Abstract
Background
Persistent trigeminal artery or persistent primitive trigeminal artery (PTA) is the most common carotid-basilar anastomosis in both cadaveric and live patient studies, followed by persistent hypoglossal and persistent otic arteries. Approximately 0.2% of all angiographies reported this finding.
Case report: We present the case of a 21-year-old male who arrived at the emergency department with tonic‒clonic seizures. After performing diagnostic contrast magnetic resonance imaging and digital subtraction angiography, the patient was diagnosed with a right occipital arteriovenous malformations (AVM) fed by the right calcarine artery associated with an ipsilateral PTA. After considering surgical and endovascular treatment options, the patient was selected for watchful waiting. We included a literature review of the PTA, the results of a PubMed search regarding the combined presence of these findings, and a brief discussion providing insight into the implications for treatment.
Conclusions
Although several studies have linked PTA to different vascular pathologies, such as cerebral aneurysms, the association between PTA and AVMs remains scarce. This case, along with the literature review, shows that further research is needed to characterize the relationship between these findings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The persistent trigeminal artery (PTA) is the most common carotid-basilar anastomosis. Eighty-five percent of the reported literature of carotid-basilar anastomosis concerns PTA [16]. PTA was described in live patients by Sutton in 1950 using cerebral angiography [2].
It is not uncommon for PTA to be associated with intracranial vascular pathology, especially intracranial aneurysms [15]. However, arteriovenous malformations (AVMs) remain a much less studied subject, with only a few cases reported. Herein, we present a case of a young male patient with a right occipital AVM associated with an ipsilateral PTA.
Case report
A 21-year-old male with a medical history of smoking and a remitted case of acute lymphoblastic leukemia was brought to the emergency department after presenting with a generalized tonic‒clonic seizure with loss of consciousness of unknown length. The patient denied any previous history of seizures or family history of epilepsy.
Initial magnetic resonance imaging (MRI) of the patient revealed a right posterior AVM (Fig. 1). The patient was started on antiepileptic medication and was scheduled for further testing.
Three-dimensional time-of-flight magnetic resonance angiography of the brain in sagittal (A), axial (B) and coronal (C) reformatted images show the presence of the persistent trigeminal artery arising from the right internal carotid artery and ending in the vertebrobasilar circulation. In the sagittal image, the right calcarine artery as well as the arteriovenous nidus can be identified
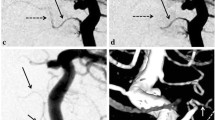
Diagnostic subtraction angiography (DSA) demonstrated an occipital AVM fed by the calcarine artery measuring 11 mm in the dorsoventral axis and 17 mm in the lateral–lateral axis (Fig. 2b); it drained into the right occipital cortical vein and further into the superior sagittal sinus. The AVM was scored as grade II using the Spetzler–Martin classification (1 point for the nest size and 1 point for the eloquent area) and as grade I using the Buffalo classification (1 point for eloquence). DSA also revealed a persistent trigeminal artery type Saltzman 1 in the anterior and posterior projections (Fig. 2a).
Lateral projections of digital subtraction angiography of the right internal carotid (A) and vertebral (B) arteries show the presence of the persistent trigeminal artery (PTA) arising from the cavernous segments of the right internal carotid artery (ICA) and ending in the posterior circulation, from which the right posterior cerebral artery (R-PCA) arises. Vertebral angiography shows the basilar artery (BA) bifurcating into the posterior cerebral arteries; the right PCA divides into the right calcarine artery (Calcarine A) which feeds the AVM nidus (Nidus). The nidus drains into the Right Occipital Vein (Occ. vein)
At the moment that this article was written, the patient had adequate control of epileptic seizures and was selected for watchful waiting by consensus of the Interventional Neuroradiology and Vascular Neurosurgery departments.
Discussion
PTA is a carotid-basilar anastomosis that emerges in the early days of the embryologic development phase and disappears when the embryo reaches 11.5–14 mm [2]. It is the most common carotid-basilar anastomosis and is found in between 0.1 and 3% of the general population [7]. There are two kinds of the PTA: lateral (usual) type and medial (intrasellar) type. The latter one is rare.
As described by Saltzman, PTA might be classified as one of three types. In type 1, as in our case, PTA supplies most of the vertebrobasilar circulation, whereas type 2 PTA supplies only the superior cerebellar arteries. Type 3 usually refers to a PTA that ends in a cerebellar artery completely bypassing the basilar artery [9].
We performed a PubMed search using the following MESH terms: Persistent Trigeminal Artery, Persistent Primitive Trigeminal Artery, and Arteriovenous Malformation. We found 13 studies published from 1962 to 2015 (Table 1). A majority of cases were treated by surgery, and all articles reported a stable or improved clinical condition when the patient underwent treatment or conservative management.
Our case is a very particular case due to its clinical presentation. On the one hand, most AVMs associated with PTA presented as hemorrhagic stroke, either by intracerebral hemorrhage or subarachnoid hemorrhage. A small subset also presented as trigeminal neuralgia due to the location of the AVM [4, 8]. On the other hand, our case presented with epileptic seizures; to our knowledge, this is the only case of AVM with PTA that had this unusual clinical presentation.
The location of the AVMs is another point of discussion. Although they were once considered rare, the last published case reports have presented more posterior circulation AVMs, especially in the cerebellum and brainstem. Two of the reported AVMs were located in the corpus callosum; one had bilateral blood supply, and the other was only fed by the left circulation [9, 14]. Other sites where the AVMs were located include the occipital, temporal, and parietal regions.
Almost all the described associations of AVMs with PTA were incidental. In two cases, the PTA provided a direct blood supply to the AVM. In one case, the PTA was the main pedicle to an AVM located on the left side of the cerebellum [8], whereas in a second case, the PTA fed a right cerebellopontine AVM along with the ipsilateral anterior inferior cerebellar artery (AICA) [4].
Although a strong association of PTA with saccular aneurysms has been described, no formal studies have analyzed this phenomenon with AVMs. It has been theorized that the abnormal blood flow caused by AVMs may create an environment in which the PTA cannot be closed at birth [10]. Another theory states that both the failure to close the trigeminal artery and the emergence of the AVM are the result of maldevelopment in the fetal period [1]. This may be supported by the fact that most of the reported AVMs were located ipsilateral to the anatomical variant. Despite this, some dismiss these findings as purely coincidental.
Treatment of these malformations remains a difficult challenge. AVMs can be treated by surgical resection, endovascular embolization, and radiation surgery. In the case of endovascular treatment, PTA presents both an advantage and a disadvantage.
PTA acts as a communication mechanism between the anterior and posterior circulation. This elevates the risk of vessel occlusion when presented with embolizing material backflow [8]. However, in this particular case, PTA may also serve as an access pathway by which AVM catheterization may occur. Therefore, when anatomical variants are encountered, a thorough characterization of the anatomy using a diagnostic angiogram must be done before discussing treatment options.
Availability of data and materials
Clinical data related to the case are available upon request.
References
Abe T, Matsumoto K, Aruga T (1994) Primitive trigeminal artery variant associated with intracranial ruptured aneurysm and cerebral arteriovenous malformation. Case report. Neurol Med Chir (Tokyo) 34:104–107
Azab W, Delashaw J, Mohammed M (2012) Persistent primitive trigeminal artery: a review. Turk Neurosurg 22(4):399–406. https://doi.org/10.5137/1019-5149.JTN.4427-11.1
Brick JF, Roberts T (1987) Cerebral arteriovenous malformation coexistent with intracranial aneurysm and persistent trigeminal artery. South Med J 80(3):398–400. https://doi.org/10.1097/00007611-198703000-00036
Choudhri O, Heit JJ, Feroze AH, Chang SD, Dodd RL, Steinberg GK (2015) Persistent trigeminal artery supply to an intrinsic trigeminal nerve arteriovenous malformation: a rare cause of trigeminal neuralgia. J Clin Neurosci 22(2):409–412. https://doi.org/10.1016/j.jocn.2014.06.007
Gannon WE (1962) Malformation of the brain. Persistent trigeminal artery and arteriovenous malformation. Arch Neurol 6:496–498. https://doi.org/10.1001/archneur.1962.00450240074009
Jayaraman A, Garofalo M, Brinker RA, Chusid JG (1977) Cerebral arteriovenous malformation and the primitive trigeminal artery. Arch Neurol 34(2):96–98. https://doi.org/10.1001/archneur.1977.00500140050009
Komiyama M (2019) Persistent trigeminal artery and its variants. Interv Neuroradiol 25(6):635–637. https://doi.org/10.1177/1591019919863110
Kono K, Matsuda Y, Terada T (2013) Resolution of trigeminal neuralgia following minimal coil embolization of a primitive trigeminal artery associated with a cerebellar arteriovenous malformation. Acta Neurochir (Wien) 155(9):1699–1701. https://doi.org/10.1007/s00701-013-1753-6
Mohanty CB, Devi BI, Somanna S, Bhat DI, Dawn R (2011) Corpus callosum arteriovenous malformation with persistent trigeminal artery. Br J Neurosurg 25(6):736–740. https://doi.org/10.3109/02688697.2011.554583
Nakai Y, Yasuda S, Hyodo A, Yanaka K, Nose T (2000) Infratentorial arteriovenous malformation associated with persistent primitive trigeminal artery—case report. Neurol Med Chir (Tokyo) 40(11):572–574. https://doi.org/10.2176/nmc.40.572
Oran I, Parildar M, Memis A, Yunten N (2000) Catheter and MR angiography of persistent trigeminal artery associated with occipital arteriovenous malformation. Comput Med Imaging Graph 24(1):33–35. https://doi.org/10.1016/s0895-6111(99)00040-3
Perret G, Nishioka H (1966) Report on the cooperative study of intracranial aneurysms and subarachnoid hemorrhage. Section VI. Arteriovenous malformations. An analysis of 545 cases of cranio-cerebral arteriovenous malformations and fistulae reported to the cooperative study. J Neurosurg 25(4):467–490. https://doi.org/10.3171/jns.1966.25.4.0467
Tomsick TA, Lukin RR, Chambers AA (1979) Persistent trigeminal artery: unusual associated abnormalities. Neuroradiology 17(5):253–257. https://doi.org/10.1007/BF00337535
Uchino A, Matsunaga M, Ohno M (1989) Arteriovenous malformation of the corpus callosum associated with persistent primitive trigeminal artery—case report. Neurol Med Chir (Tokyo) 29(5):429–432. https://doi.org/10.2176/nmc.29.429
Wan Z, Meng H, Xu N et al (2019) Coil embolisation of multiple cerebral aneurysms with lateral type I persistent primitive trigeminal artery: a case report and literature review. Interv Neuroradiol 25(6):628–634. https://doi.org/10.1177/1591019919859507
Yilmaz E, Ilgit E, Taner D (1995) Primitive persistent carotid-basilar and carotid-vertebral anastomoses: a report of seven cases and a review of the literature. Clin Anat 8(1):36–43. https://doi.org/10.1002/ca.980080107
Funding
This manuscript was written using internal funding. No external private, commercial, or governmental funding sources were used.
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
All procedures were carried out in accordance with the ethical standards of the Institutional Research Board, The General Health Law in Mexico and the Helsinki Declaration. The study was approved by the Internal Research Board.
Consent to participate
Informed consent was obtained from the patient.
Consent for publication
The patient consented to the use of their personal data included in this case report.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rodriguez-Hernandez, L.A., Martinez, P., Baracaldo, I. et al. Persistent trigeminal artery associated with an occipital arteriovenous malformation: a case report and literature review. Surg Radiol Anat 44, 1271–1275 (2022). https://doi.org/10.1007/s00276-022-03003-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-022-03003-9