Abstract
Five types of persistent primitive olfactory artery (PPOA), a rare variation of the proximal anterior cerebral artery (ACA), have been reported. Type 1 is most common, generally following an extreme anteroinferior course and taking a hairpin turn before continuing to the distal A2 segment of the ACA. Triple ACAs are a common variation of the A2 segment of the ACA, and a centrally located artery is called an “accessory ACA” or “median artery of the corpus callosum”. This artery usually does not bifurcate or else bifurcates distally and continues to the pericallosal artery. We herein report a 74-year-old woman with type 1 PPOA and early bifurcated accessory ACA, an extremely rare combination of ACA variations, that was diagnosed using magnetic resonance angiography.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rarely, the proximal segment of the anterior cerebral artery (ACA) courses extremely anteroinferiorly, makes a hairpin turn, and runs posterosuperiorly to connect to the distal normal A2 segment. This is regarded as type 1 persistent primitive olfactory artery (PPOA) [3, 11]. The POA normally regresses during early gestation [5]. There are five types of PPOA [10].
Triple ACAs are common variations of the A2 segment of the ACA [6, 9]. The centrally located artery is called the “accessory ACA” or “median artery of the corpus callosum”. The accessory ACA arises from the anterior communicating artery (ACoA) and usually does not bifurcate or bifurcates distally.
We herein report a case of type 1 PPOA associated with an accessory ACA that bifurcated immediately after the origin. This extremely rare combination of ACA variations was diagnosed using magnetic resonance (MR) angiography.
Case report
A 74-year-old woman with Parkinson’s disease underwent cranial MR imaging and MR angiography using a 3-Tesla scanner (Magnetom Skyra, Siemens Medical System, Erlangen, Germany) for the evaluation of brain diseases. Her chief complaints were bradykinesia of the colon and left side dominant rigidity. MR angiography was obtained using a standard three-dimensional time-of-flight technique. The imaging parameters were a flip angle of 18°, repetition time of 21.0 s, echo time of 3.69 s, and slice thickness of 0.6 mm.
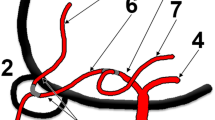
MR imaging revealed no significant abnormality except for multiple small ischemic white matter lesions in the bilateral cerebral hemispheres (not shown). MR angiography showed an anomalous course of the A2 segment of the right ACA (Fig. 1). Normally, the A2 segment of ACA takes a cephalad course. The present case showed a right ACA with an anteroinferior course along the midline anterior cranial fossa, followed by a posterosuperior course with a hairpin turn, indicative of type 1 PPOA. At the A2 segment of the ACA, there were three arteries (triple ACAs), and the centrally located largest artery was regarded as an accessory ACA that bifurcated soon after its origin from the ACoA. These findings were obvious on partial volume rendering images (Fig. 2). Figure 3 is schematic illustration of this ACA variation.
Left lateral (a) and anteroinferior–posterosuperior (b) projections of cranial magnetic resonance (MR) angiography show an anomalous anteroinferior course of the A2 segment of the right anterior cerebral artery (ACA). The artery then takes a posterosuperior course with a hairpin turn (long arrows), connecting to the distal A2 segment of the right ACA, indicative of type 1 persistent primitive olfactory artery (PPOA). There are three A2 segments of the ACA, and the centrally located accessory ACA bifurcates early (short arrows)
Right lateral (a), anteroinferior–posterosuperior (b) and slightly right anterior oblique (c) projections of partial volume rendering images of the bilateral internal carotid arteries (ICAs) and ACAs clearly reveal the anomalous A2 segment of right ACA. Long arrows indicate hairpin turn. There are three A2 segments, and the centrally located largest artery (accessory ACA) bifurcates immediately after its origin (short arrows). Dotted arrows indicate tiny aneurysm arising at the paraclinoid segment of the left ICA
Discussion
According to Padget [5], the ACA begins to develop at the formation of a secondary branch of the POA at 5 weeks’ gestation. The rostral division of the primitive internal carotid artery (ICA) constitutes the POA. The secondary branch of the POA is the medial olfactory artery, which constitutes the future ACA. If regression of the medial branch of the POA does not occur normally, an anomalous course and/or anomalous branching of the ACA develops.
PPOA is a well-known variation of the proximal ACA, with a reported prevalence of 0.14% [11] and 0.26% [3]. Its bilaterality is extremely rare. There is no gender or laterality predominance [11]. The existence of five types of PPOA was recently reported [10]. Type 1 is the most common, and its configuration is just like in the present case. Type 2 is a small artery that connects to the ethmoidal artery. Type 3 supplies both the distal ACA and ethmoidal artery [2]. Type 4 continues to the accessory middle cerebral artery, not to the ACA [3]. Type 5 connects to the A3 segment of the ACA without a hairpin turn [10]. An aneurysm can occur at the hairpin turn because of hemodynamic stress [8, 12], but its prevalence is not very high [11]. The clinical significance of a PPOA is limited, but recognition of the presence of this variation is important before performing midline anterior skull base surgery to prevent complications.
Normally, the A2 segment of the ACA is paired (two arteries). An unpaired A2 segment is known as an azygous ACA. The presence of three A2 segments is regarded as triple ACA. This variation is relatively common, with a reported MR angiographic prevalence of 3% [9]. Using anatomical dissection, Stefani et al. [6] reported 3 triple ACAs among 38 cadavers (8%). The third artery, which arises from the ACoA, is called an accessory ACA or median artery of the corpus callosum; the latter is usually used in cases of a tiny artery supplying only the corpus callosum. The present patient had a large artery supplying not only the corpus callosum but also the medial surface of the bilateral frontoparietal lobes. Thus, we used the term “accessory ACA” in this paper.
The accessory ACA usually does not bifurcate or else bifurcates distally and continues to the pericallosal artery. In the present case, the accessory ACA bifurcated soon after arising from the ACoA. A similar case was reported by Altafulla et al. [1] using anatomical dissection. In contrast, Kornieieva et al. [4] reported a case of accessory ACA with a double proximal origin. An aneurysm can occur at the origin or at the bifurcation of the accessory ACA, although its prevalence is not very high [7].
Conclusions
We encountered an extremely rare combination of ACA variation, type 1 PPOA and early bifurcated accessory ACA. Although the clinical significance of these variations is limited, aneurysms can occur in such cases. A correct diagnosis is, therefore, important when interpreting of cranial MR angiography findings.
References
Altafulla JJ, Simonds EA, Dupont G, Lachkar S, Litvack Z, Iwanaga J, Tubbs RS (2018) A median artery of the corpus callosum. Cureus 10:
Horie N, Morikawa M, Fukuda S, Hayashi K, Suyama K, Nagata I (2012) New variant of persistent primitive olfactory artery associated with a ruptured aneurysm. J Neurosurg 117:26–28
Kim MS, Lee GJ (2014) Persistent primitive olfactory artery: CT angiographic diagnosis and literature review for classification and clinical significance. Surg Radiol Anat 36:663–667
Kornieieva MA, Hadidy AM, Hinno SH (2017) Median pericallosal artery with double proximal origin: case report. Surg Radiol Anat 39:1169–1173
Padget DH (1948) Development of cranial arteries in human embryo. Contrib Embryol 32:205–262
Stefani MA, Schneider FL, Marrone AC, Severino AG, Jackowski AP, Wallace MC (2000) Anatomic variations of anterior cerebral artery cortical branches. Clin Anat 13:231–236
Sun C, Xv ZD, Yuan ZG, Wang XM, Wang LJ, Liu C (2012) MSCT diagnosis of aneurysms associated with an unusual variant: atypical triplication anterior cerebral artery. Surg Radiol Anat 34:777–780
Tsuji T, Abe M, Tabuchi K (1995) Aneurysm of a persistent primitive olfactory artery. Case report. J Neurosurg 83:138–140
Uchino A, Nomiyama K, Takase Y, Kudo S (2006) Anterior cerebral artery variations detected by MR angiography. Neuroradiology 48:647–652
Uchino A, Ohno H, Ogiichi T (2021) Persistent primitive olfactory artery without a hairpin turn. Surg Radiol Anat 43:231–234. https://doi.org/10.1007/s00276-020-02595-4
Uchino A, Saito N, Kozawa E, Mizukoshi W, Inoue K (2011) Persistent primitive olfactory artery: MR angiographic diagnosis. Surg Radiol Anat 33:197–201
Yamamoto T, Suzuki K, Yamazaki T, Tsuruta W, Tsurubuchi T, Matsumura A (2009) Persistent primitive olfactory artery aneurysm. Neurol Med Chir 49:303–305
Author information
Authors and Affiliations
Contributions
AU carried out the study design and drafted the manuscript. All authors reviewed the manuscript critically, and have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Uchino, A., Mochizuki, A. Persistent primitive olfactory artery associated with early bifurcated accessory anterior cerebral artery. Surg Radiol Anat 43, 1731–1733 (2021). https://doi.org/10.1007/s00276-021-02744-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-021-02744-3