Abstract
Purpose
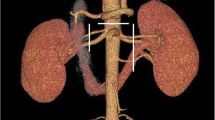
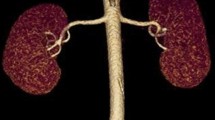
Endovascular navigation in aortic, renal and visceral procedures are based on precise knowledge of arterial anatomy. Our aim was to define the anatomical localization of the ostia of renovisceral arteries and their distribution to establish anatomical landmarks for endovascular catheterization.
Methods
Computer-assisted measurements performed on 55 CT scans and patients features (age, sex, aortic diameter) were analyzed. p values <0.05 were considered statistically significant.
Results
The mean axial angulation of CeT and the SMA origin was 21.8° ± 10.1° and 9.9° ± 10.5°, respectively. The ostia were located on the left anterior edge of the aorta in 96 % of cases for the CeT and 73 % for the SMA. CeT and SMA angles followed Gaussian distribution. Left renal artery (LRA) rose at 96° ± 15° and in 67 % of cases on the left posterior edge. The right renal artery (RRA) rose at −62° ± 16.5° and in 98 % of cases on the right anterior edge of the aorta. RRA angle measurements and cranio-caudal RRA-LRA distance measurements did not follow Gaussian distribution. The mean distances between the CeT and the SMA, LRA, and RRA were 16.7 ± 5.0, 30.7 ± 7.9 and 30.5 ± 7.7 mm, respectively. CeT-SMA distance showed correlation with age and aortic diameter (p = 0.03). CeT-LRA distance showed correlation with age (p = 0.04). The mean distance between the renal ostia was 3.75 ± 0.21 mm. The RRA ostium was higher than the LRA ostium in 52 % of cases. RRA and LRA origins were located at the same level in 7 % of cases.
Conclusion
Our results illustrate aortic elongation with ageing and high anatomical variability of renal arteries. Our findings are complementary to anatomical features previously published and might contribute to enhance endovascular procedures safety and efficacy for vascular surgeons and interventional radiologists.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Endovascular treatment is the procedure of choice for aortic aneurysms (AAA) and aorto-iliac or aortic branches occlusive disease in cases with favorable anatomy [22]. Endovascular approach can also be used as an alternative procedure in patients deemed unfit for open surgery [7]. Endovascular techniques are based on fluoroscopy-guided intra-arterial navigation. Catheterization of renal and digestive arteries is mandatory in numerous procedures such as the treatment of renovisceral arteries stenosis or aneurysms [22], para-renal and thoraco-abdominal aneurysms repair [11] and selective embolization.
Target vessels ostia localization is often possible with repeated contrast agent injections and prolonged radiation time with, however, an increased morbidity of the procedure [13, 23]. New imaging techniques with less contrast agents during interventional procedures such as image fusion techniques have been developed but remain difficult to access [25]. Therefore, knowing and using anatomical landmarks can allow faster and safer catheterization using less contrast agent. In this study, we focused on the axial orientation on the aorta of the renovisceral branches ostia and distances between these ostia, as well as their distribution. We presumed that each ostium, once catheterized, could be used to find another vessel origin. A few authors have described the distances between the aortic branches ostia, with different methodologies [1, 2, 5, 8–10, 14, 26]. We completed our study with a review of the literature concerning the vertebral level of the ostia and their distance to the iliac bifurcation, which are also helpful intraoperative landmarks.
Methods
Contrast-enhanced abdomino-pelvic computed tomography (CT) scans in 55 patients from January 2010 to December 2012 in our institution were retrospectively analyzed. All of the examinations were performed to explore a symptomatic peripheral arterial occlusive disease in our vascular surgery unit.
Patients older than 75 years, patients with history of open or endovascular aortic surgery, and patients with aortic occlusive or aneurysmal disease were not included in this study.
Measures were performed on 1.25 mm CT scans slices using Aquarius intuition Edition software (ver.4.4.7.29.4070, TeraRecon, Inc, Foster City, CA, USA). This software allows multiplanar reconstructions and aortic centerline establishment, which consists of a curvilinear axis through the center of the aorta (Fig. 1a). All CT scans were analyzed by the same operator. Results were expressed in mean values ± standard deviation.
a Axial and distances measures. Green line: centerline. Plan A (blue): CeT ostium. Plan B (red): SMA ostium. Plan C (blue): RRA ostium. A–B: CeT-SMA distance. A–C: CeT-RRA distance. b CeT angle measure (plan A). c SMA angle measure (plan B). d CeT–SMA distance measure (plan A–B) (color figure online)
Axial location measurements
Angles defining the axial location of the ostia of renovisceral arteries were measured on transverse sections perpendicular to the aortic centerline. The angle between the aortic centerline and the line joining the centerline to the center of the target vessel ostium was measured after displaying a clock position dial (Fig. 1b, c). Measures were reported in degrees relative to a reference antero-posterior axis (0°). Positive angles correspond to an ostium located on the left side of the aorta and negative angles to the right side of the aorta. Anatomical variations and supernumerary arteries were excluded from the study.
Distance measurements
Distance between arteries was measured in sagittal and coronal sections between the center of the celiac trunk (CeT) ostium and superior mesenteric artery (SMA) and both right (RRA) and left (LRA) renal arteries ostia. Distances between both renal arteries were obtained by subtraction using the three measures. Distances (CeT-SMA, CeT-RRA, CeT-LRA and RRA-LRA) represent the height between two axial plans, perpendicular to the centerline (Fig. 1d). Measures obtained do not match the anatomical distances: the curve of the aorta is taken into consideration but not the axial angulation of the ostia. Anatomical variations and supernumerary arteries were excluded from the study.
Statistics
Data were analyzed using SAS/STAT® v9.3 software (SAS Institute Inc., Cary, NC, USA). Shapiro–Wilk test was used to assess normality of the distribution of CT angiography measurements. Variables with normal distribution were compared using the two-tailed Student’s t test. Non-parametric variables were compared using Wilcoxon test. Correlations were obtained after linear regression. A p value <0.05 was considered statistically significant.
Results
Fifty-five contrast-enhanced CT scans were analyzed, in 14 women and 41 men. The mean age was 58 ± 9.2 years.
Anatomical variations
Two patients (3.6 %) presented anatomical variations of the CeT with a direct aortic origin of the left gastric artery. No anatomical variation in the SMA was observed.
Among the 55 patients, twelve (22 %) had one or two supernumerary renal arteries. Two LRA and one RRA were observed in four (7.2 %) cases, two RRA and one LRA in two (3.6 %) cases and two RRA with two LRA in three (5.4 %) cases.
Axial location of the renovisceral ostia (Tables 1, 2)
Axial location of the celiac trunk
The mean axial location of the CeT was 21.8° ± 10.1° (−3° to 39°). CeT rose on the left side of the aorta in 96 % of cases (n = 51), in one case at 0° and in one case on the right side of the aorta at −3°. In 88 % of cases, the celiac trunk rose between 10° and 40° (Fig. 2a).
Axial location of the SMA
The mean axial location of the SMA was 9.9° ± 10.5° (−12° to 31°). SMA rose in 15 % of cases on the right side of the aorta (n = 8), in 12 % (n = 7) at 0° and in 73 % of cases on the left side of the aorta (n = 40). SMA took origin in 81 % between 0° and 29° (Fig. 2b).
Axial location of the LRA
The LRA had a mean ostial location at 96° ± 15° (58°–128°). LRA rose in 33 % of cases on the left anterior side of the aorta (58°–89°) and in 67 % of cases on the left posterior side of the aorta (92°–128°) (Fig. 2c).
Axial location of the RRA
The RRA had a mean ostial location at −62°± 16.5° (−8° to −96°). The RRA origin was observed in 98 % of cases (n = 49) on the right anterior side of the aorta and in one case on the right posterior side. In 74 % of cases the RRA rose between 50° and 79° (Fig. 2d).
Distances between the Ostia (Tables 3, 4)
Distance CeT-SMA
The mean distance between the celiac trunk and the SMA was 16.7 ± 5.0 mm (7.0–31.6 mm). In 85 % of cases, the distance was comprised between 10 and 24.9 mm.
Distance CeT-LRA
The mean distance between the celiac trunk and the LRA was 30.7 ± 7.9 mm (12.7–46.5 mm). In all cases LRA was located under the level of the celiac trunk. The distance was comprised between 25 and 39.9 mm in 73 % of cases.
Distance CeT-RRA
The mean distance between the celiac trunk and the RRA was 30.5 ± 7.7 mm (14–43.5 mm). The RRA was found in all cases under the level of the celiac trunk, in 90 % of cases 20–43.5 mm from the celiac trunk.
Distance RRA-LRA
The calculated average distance between RRA and LRA was 3.75 ± 0.21 mm (−14.5 to 15.9 mm). RRA ostium was above the level of the LRA in 52 % of cases (n = 24) and below in 41 % of cases (n = 19). RRA and LRA origins were on the same level in only 7 % of cases (n = 3). Distance was comprised between −9.9 and 9.9 mm in 84 % of cases.
Measurements distribution (Table 5)
All axial locations and distances distributions were analyzed. Clock position of the CeT, SMA and LRA followed a Gaussian distribution. In contrast, RRA angle measurements and cranio-caudal RRA-LRA distance measurements did not (respectively p = 0.04 and p = 0.02) (Fig. 3).
Correlations of measures with sex, age and aortic diameter (Table 6)
Clock position of CeT, SMA, LRA did not show any statistic correlation with sex, age or aortic diameter. RRA angle showed a correlation with sex, (mean angle of −63.9°± 13.9° for men vs −62.5 ± 22.6° for women, p = 0.02). Furthermore, CeT-SMA distance and CeT-RRA distance showed correlation with aortic diameter (p = 0.03 and p = 0.01). CeT-SMA distance and CeT-LRA distance showed statistical correlation with age (p = 0.03 and p = 0.04).
Discussion
The goal of this study was to depict the topography of renovisceral arteries and analyze their distribution to ultimately facilitate their catheterization, with less radiation and contrast agent consumption during endovascular procedures. Other authors have based their studies on dissections and CT scans analysis. Patients with anatomical variations or supernumerary renal arteries were excluded of the statistical analysis in all other publications, as well as in our study. In this discussion we will combine and compare our findings with the descriptions brought by other studies to display the global anatomical characteristics, artery by artery.
Arteries ostia location
Celiac trunk ostium (Table 7)
Vertebral level
Dissections have all shown similar results with the CeT facing the superior third of L1 [1, 2, 5, 9, 10, 26]. Cauldwell et al. [5] showed that the celiac trunk always originated from the aorta between the superior third of T12 and the superior third of L2 (n = 287). In 83.2 % of cases, the celiac trunk originated between the inferior third of T12 and the inferior third of L1. There is no relationship between the length of the aorta, thus patient height, and the vertebral level of the ostia [2]. There is no difference between male and female in the variation of origin of the CeT [30].
Distance CeT-iliac bifurcation
The celiac trunk originates 12.9 ± 1.38 cm from the iliac bifurcation [5]. In 85 % of cases, the distance varies from 11.5–14.5 cm [2].
Axial location of celiac trunk ostium
Our study shows that the CeT origin is located on the left side of the aorta in 97 % of patients. CeT ostium seem to have a uniform origin since CeT angle did not show correlation with age, sex or aortic diameter. In a series of 257 dissections the CeT is left-sided in 60 % of cases, median in 30 % and right-sided in 10 % of cases [21].
On the other hand, Adachi et al. [1] reported 50 Japanese subjects dissections with the CeT originating on the left side of the aorta in only 22 % of cases, compared to 78 % on the middle and none on the right side. These differences might be due to measurement method bias. We considered the arterial ostium center as reference point, in living patients.
Our measures are consistent with results published by other authors: celiac trunk angulation varies between 24° [25] and 30° [23]. In a recent study, Mazzacaro and al. [14] found a mean celiac trunk angulation of 23.3° in 50 patients without dilatation of thoracoabdominal aorta. The celiac trunk ostium is located on the upper left of the SMA in 80 % of cases [27].
In summary, CeT ostium is globally located on the anterior side of the aorta with a slight left axial deviation (about 25°), 13 cm from the iliac bifurcation and facing the superior third of L1 in most of cases.
SMA ostium (Table 7)
Vertebral level
SMA faces the lower third of L1 in most cases and is always located between the middle third of T12 and intervertebral disc L2–L3 [5, 9, 10]. For Adachi et al. [1], SMA rises regarding the middle third of L1. Other authors described SMA ostium location in 75 % of cases between the superior third of L1 and the intervertebral disc L1–L2 [5]. According to Anson and McVay [2], SMA origin is in 83 % of cases between the middle third of L1 and the superior third of L2. The SMA origin is more variable than the CeT origin (p < 0.01) [30].
SMA-Iliac bifurcation distance
SMA origin is 11.5 ± 1.31 cm from the aortic bifurcation [5]. Similar results were found in other studies where this distance varied from 10.5–12.5 cm in 80 % of cases [2].
Axial orientation of SMA ostium
According to Panagouli et al. [20], SMA origin is located at 0° (n = 62), compared to 13° ± 18° according to Pennington and Soames [20] (n = 15). Mazzacaro et al. found a mean angle of 15.1° [14]. These results are similar to ours, with a mean angulation of 9.9° ± 10.5°. Similarly to CeT, SMA angle did not show correlation with age, sex or aortic diameter.
In summary, SMA ostium is approximately located at 12 cm of the iliac bifurcation, facing the inferior third of L1 on the left anterior side of the aorta, with a slight left axial deviation, near the median line (Table 7).
Renal arteries ostia (Table 8)
Supernumerary renal arteries
In our study, 21.8 % of patients had at least one supernumerary renal artery. Other authors [1, 5, 17] found similar results with 22.8–29.5 % supernumerary renal arteries. Renal arteries always rise from the aorta. Adachi et al. [1] reported only two cases of supernumerary ectopic renal arteries: one from the right common iliac artery and one from the middle sacral artery.
Vertebral level of the renal arteries
Renal arteries are located at the superior third of L2 [5] or slightly higher, facing of the intervertebral disc L1–L2 [1]. A recent study based on 855 CT scans has shown that 98 % of the RRA and 97 % of the LRA started between the superior third of L1 and the inferior third of L2 [17].
Renal arteries-aortic bifurcation distance
RRA rises 10.0 ± 1.52 cm (3.4–14.2 cm) and the LRA 10.0 ± 1.35 cm (4.5–14.2 cm) from the aortic bifurcation [5].
Axial orientation of the RRA
Recent studies based on CT scans found a mean orientation between −63° [3] and −75° [28]. Autopsy studies showed a mean orientation from −88° [20] to −72° [12]. All studies showed a clear predominance of the anterior orientation of the RRA. Our Results were similar, with RRA ostia located at −62° ± 16.5°. Interestingly, our results, like others [14] showed that RRA angle did not follow a Gaussian distribution on the contrary of other target vessels.
Axial orientation of the LRA
Mean orientation of the LRA ostium in the literature varies from 81° (n = 52) [12] to 111° (n = 100) [3]. In Beregi et al. study [3], 80 % of the LRA began between 60° and 145° and showed a postero-lateral orientation, whereas Keen et al. [12] found a strictly lateral orientation. In our study, the LRA begins at 96° ± 15° (n = 50), consistent with previously described results [3, 12, 14]. LRA orientation was mainly posterior (67 %).
In summary, renal arteries ostia are located in regard of the superior third of L2 at approximately 10 cm from aortic bifurcation. The RRA ostium is anterolateral with a mean angulation around −70°. LRA ostium is lateral, slightly posterior with a mean angulation around 95°.
Distance between renovisceral arteries (Tables 9, 10)
Numerous authors worked on distances between visceral arteries ostia measured on cadavers. Comparison is difficult to achieve because measures were either made between the ostia centers after a longitudinal section of the posterior side of the aorta without taking into consideration the aortic curve or made between the lower edge of the CeT ostium and the superior edge of the SMA ostium [1, 2, 5]. In our study, we measured the distances between two plans that were perpendicular to the aortic centerline using the center of the ostia.
CeT-SMA distance
Mean distance varies from 1.32 cm [5] to 1.9 cm [19]. In 71 % of cases, this value ranges between 1 and 2 cm [2]. Similarly, the CeT-SMA distance in our study ranged between those values in 66 % of cases. Adachi et al. [1] found that the distance between the inferior edge of CT ostia and superior edge of the SMA ostia ranged between 5 and 10 mm in 65 % of the studied population (n = 15). Our results confirm that SMA begins at 1.67 cm from the CeT. The maximal distance was 3.16 cm. Maximal distance in other studies was 4.1 cm [2]. Interestingly, Cet-SMA distance showed statistical correlation with age and aortic diameter. Such observations could be explained by aortic remodeling with ageing associated with an increase of length and diameter, as described by Kamenskyi et al. [11]. Ozkurt et al. [18] found that there was also a correlation between the CeT-SMA distance and the body mass index (BMI) in both genders (p < 0.001).
CeT-RRA distance
The mean reported CeT-RRA distance is between 2.85 [5] and 3.2 cm [19]. According to Cauldwell et al. [5], RRA ostia were located between 1.0 and 4.4 cm below the CeT in 90 % of cases. In our series, distance between the CeT and the RRA was always included in this range (1.4–4.35 cm). CeT-RRA distance showed a correlation with aortic diameter (i.e., proportional to aortic diameter).
CeT-LRA distance
The Mean reported CeT-LRA distance between the ostia varies from 2.7 [5] to 3.6 cm [19]. LRA always begins under the CT. Our results were similar with a mean distance of 3.07 cm. Furthermore, similarly to CeT-SMA distance, CeT-LRA distance showed statistical correlation with age, possibly related to aortic elongation.
RRA-LRA distance
Different studies reported heterogeneous results: In Cauldwell et al. [5] study, RRA rose in 41 % of cases above the LRA, 23.3 % under the LRA and at the same level in 35.7 % of cases. According to Adachi et al. [1], RRA began above LRA level in 61.3 %, under it in 22.5 % and at the same level in 16.2 %.
RRA and LRA rose in the same level in 30 % of cases for Bergman et al. [4] and 50 % of cases for Beregi et al. [3] RRA seems to begin higher than LRA in most cases. Our series found that RRA ostium was higher than LRA in 52 % of cases. LRA and RRA rose at the same level in only 7 % of cases (n = 3). Similarly to RRA angle, RRA-LRA distance measurements do not follow a Gaussian distribution in our study, thus illustrating important anatomic variability of renal arteries.
Clinical applications Endovascular procedures that might be facilitated by a rigorous arterial anatomical knowledge are numerous: renovisceral arteries angioplasty [6], endovascular aortic aneurysm repair, fenestrated and branched aortic grafts deployment [11], embolization procedures. Simple landmarks such as vertebral levels exist but are often insufficient to locate ostia precisely. Accurate topographic knowledge of arterial ostia location could decrease contrast agent injections with related toxicity (contrast agents allergy, chronic renal failure, lactic acidosis [15]) as well as radiation amount, both patient and physician exposure, and procedure duration. More specifically, in vascular surgery, the endovascular treatment of thoraco-abdominal aneurysms requires branched stent-grafts which are aortic endografts equipped with branches intended to the CeT, SMA, and renal arteries that are involved in the aneurysm. In the vast majority of cases, the graft has to be manufactured in about 8–12 weeks according to the patients CT scan. These custom-made devices are not adapted to large or urgent aneurysms that require prompt management. For this reason, off-the-shelf branched aortic stent-grafts have been developed by the industry to cope with the widest range of renovisceral arteries anatomical disposition: the Zenith T-branch thoraco-abdominal stent-graft (Cook Inc. Bloomington, IN) and the branched Excluder device (W.L. Gore, Flagstaff, AZ, USA). The branches in these devices are already positioned to statistically allow to bridge-stent the renovisceral arteries in the largest number of patients. For this purpose, the knowledge of the most common disposition of renal and digestive arteries is mandatory.
Our study shows that RRA angle and RRA-LRA cranio-caudal distance have a non-gaussian distribution. Such characteristics might be factors limiting the use of some fenestrated stent-grafts in EVAR in particular off the shelf stent-grafts. As a matter of fact, RRA was the primary cause of non-feasibility among the 28 % of patients unfit for off the shelf stent-grafts for juxta and pararenal aortic aneurysms in Sobocinski et al. study [24]. Such anatomical features could require increased focus on renal arteries during preoperative course.
This study has several limits. First, the absence of totally automated measurements may have induced biases in our findings. Such biases were limited by using thin 1.25 mm slices when measuring parameters on CT scans. Reconstruction software allowed automated design of the aortic centerline and use of curved planar reconstruction thus allowing precise distances and angles calculation by minimizing manual measurement. On the other hand, measurements were performed on non-dynamic CT scans: axial and longitudinal aortic pulsatility may have induced measurements errors, this impact has not been studied in this paper. Use of dynamic CT may limit this last bias. Precise study of renovisceral arteries’ anatomic variability during cardiac cycle could be interesting.
Conclusion
Imaging techniques and software allowed us to establish precise anatomical measures that are complementary to the results of previously published studies. This computer-assisted anatomy helps to define anatomical landmarks that might facilitate target vessels catheterization, and thus reduce procedure-related morbidity. CeT and SMA angles follow Gaussian distribution and were not correlated with age, sex or aortic diameter. RRA angle and RRA-LRA cranio-caudal distance measurements distribution did not follow Gaussian distribution and illustrate renal arteries high anatomical variability. Aortic remodeling with ageing and important heterogeneity of renal vessels distribution should be carefully studied in preoperative course.
The authors declare that they have no conflict of interest and that the study complies with the current French laws.
References
Adachi B (1928) Anatomie der Japaner I. Das Arteriensystem der Japaner. Band II. Verlag der Kaiserlich-Japanischen Universität zu Kyoto. Maruzen Publishing Co., Kyoto
Anson BJ, McVay CB (1936) The topographical positions and the mutual relations of the visceral branches of the abdominal aorta. A study of 100 consecutive cadavers. Anat Rec 67(1):7–15
Beregi JP, Mauroy B, Willoteaux S, Mounier-Vehier C, Rémy-Jardin M, Francke J (1998) Anatomic variation in the origin of the main renal arteries: spiral CTA evaluation. Eur Radiol 9(7):1330–1334
Bergman RA, Thomson SA, Afifi AK, Saadeh FA (1988) Compendium of human anatomic variation. Urban & Schwarzenberg, Baltimore, pp 81–82
Cauldwell EW, Anson BJ (1943) The visceral branches of the abdominal aorta: topographical relationships. Am J Anat 73(1):27–57
Cooper CJ, Murphy TP, Cutlip DE, Jamerson K, Henrich W, Reid DM et al (2014) Stenting and medical therapy for atherosclerotic renal-artery stenosis. N Engl J Med 370(1):13–22. doi:10.1056/NEJMoa1310753
Coscas R, Kobeiter H, Desgranges P, Becquemin J-P (2011) Technical aspects, current indications, and results of chimney grafts for juxtarenal aortic aneurysms. J Vasc Surg 53(6):1520–1527. doi:10.1016/j.jvs.2011.01.067
Garcier J-M, De Fraissinette B, Filaire M, Gayard P, Therre T, Ravel A et al (2001) Origin and initial course of the renal arteries a radiological study. Surg Radiol Anat 23(1):51–55
George R (1935) Topography of the unpaired visceral branches of the abdominal aorta. J Anat 69(Pt 2):196–205
Heidsieck E (1928) Zur Skeletopie der grossen Aste der Bauchaorta. Anat Anz 66:6–24
Kamenskiy A, Miserlis D, Adamson P, Adamson M, Knowles T, Neme J et al (2015) Patient demographics and cardiovascular risk factors differentially influence geometric remodeling of the aorta compared with the peripheral arteries. Surgery 158(6):1617–1627. doi:10.1016/j.surg.2015.05.013
Keen EN (1981) Origin of the renal arteries from the aorta. Acta Anat 110:285–286
Kirkwood ML, Guild JB, Arbique GM, Anderson JA, Valentine RJ, Timaran C (2015) Surgeon radiation dose during complex endovascular procedures. J Vasc Surg 62(2):457–463. doi:10.1016/j.jvs.2015.02.050
Mazzaccaro D, Malacrida G, Nano G (2015) Variability of origin of splanchnic and renal vessels from the thoracoabdominal aorta. Eur J Vasc Endovasc Surg 49(1):33–38
Mehran R, Nikolsky E (2006) Contrast-induced nephropathy: definition, epidemiology, and patients at risk. Kidney Int Suppl (100):S11–S5
Ozan H, Alemdaroglu A, Sinav A, Gümüsalan Y (1997) Location of the ostia of the renal arteries in the aorta. Surg Radiol Anat 19:245–247
Ozkan U, Oguzkurt L, Tercan F, Kizilkilic O, Koç Z, Koca N (2006) Renal artery origins and variations: angiographic evaluation of 855 consecutive patients. Diagn Interv Radiol 12(4):183–186
Ozkurt H, Cenker MM, Bas N, Erturk SM, Basak M (2007) Measurement of the distance and angle between the aorta and superior mesenteric artery: normal values in different BMI categories. Surg Radiol Anat 29(7):595–599
Panagouli E, Lolis E, Venieratos DA (2011) Morphometric study concerning the branching points of the main arteries in humans: relationships and correlations. Ann Anat 193(2):86–99. doi:10.1016/j.aanat.2010.10.009
Pennington N, Soames RW (2005) The anterior visceral branches of the abdominal aorta and their relationship to the renal arteries. Surg Radiol Anat 27(5):395–403
Rio Branco P (1912) Essai sur l’anatomie et la médecine opératoire du tronc cœliaque et de l’artère hépatique. G. Steinheil (ed), pp. 65–66
Saltzberg SS, Maldonado TS, Lamparello PJ, Cayne NS, Nalbandian MM, Rosen RJ, Jacobowitz GR, Adelman MA, Gagne PJ, Riles TS, Rockman CB (2005) Is endovascular therapy the preferred treatment for all visceral artery aneurysms? Ann Vasc Surg 19(4):507–515
Saratzis AN, Goodyear S, Sur H, Saedon M, Imray C, Mahmood A (2013) Acute kidney injury after endovascular repair of abdominal aortic aneurysm. J Endovasc Ther 20(3):315–330. doi:10.1583/12-4104MR2.1
Sobocinski Jonathan, d’Utra Guillerme, O’Brien Noel, Midulla Marco, Maurel Blandine, Guillou Matthieu, Azzaoui Richard, Roeder Blayne, Resch Timothy A, Haulon Stéphan (2012) Off-the-shelf fenestrated endografts: a realistic option for more than 70 % of patients with juxtarenal aneurysms. Endovasc Ther 19:165–172. doi:10.1583/11-3772.1
Tacher V, Lin M, Desgranges P, Deux JF, Grünhagen T, Becquemin JP, Luciani A, Rahmouni A, Kobeiter H (2013) Image guidance for endovascular repair of complex aortic aneurysms: comparison of two-dimensional and three-dimensional angiography and image fusion. J Vasc Interv Radiol 24(11):1698–1706. doi:10.1016/j.jvir.2013.07.016
Taniguchi J (1931) Beitrag zur Topographie der grossen Aste der Bauchaorta. Folia Anat Jpn 9:201–214
Tokue H, Tokue A, Tsushima Y (2012) Multidetector-row computed tomography for evaluating the branching angle of the celiac artery: a descriptive study. BMC Med Imaging 21(12):36. doi:10.1186/1471-2342-12-36
Wozniak WT (2000) Origin of the renal arteries from sides of aorta. Folia Morphol (Warsz) 58:259–261
Yahel J, Arensburg B (1998) The topographic relationships of the unpaired visceral branches of the aorta. Clin Anat 11(5):304–309
Yan H (1994) Relationship of the celiac and superior mesenteric arteries to the vertebral bodies and its clinical relevance. Radiat Med 12:105–109
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lawton, J., Touma, J., Sénémaud, J. et al. Computer-assisted study of the axial orientation and distances between renovisceral arteries ostia. Surg Radiol Anat 39, 149–160 (2017). https://doi.org/10.1007/s00276-016-1718-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-016-1718-6