Abstract
Purpose
To compare the accuracy of C-arm computed tomography (CT) and digital subtraction angiography (DSA) in detecting incomplete stent expansion (ISE) after superficial femoral artery (SFA) stenting using intravascular ultrasound (IVUS) as a gold standard.
Materials
Fifty patients with symptomatic SFA occlusive disease requiring angioplasty were prospectively included. Once technical success (<30 % residual stenosis) was obtained on post-procedural DSA, C-arm CT and IVUS were acquired. DSA and C-arm CT examinations were reviewed by 2 investigators and correlated with IVUS. C-arm CT image quality was rated on a four-point scale. Doppler ultrasound was performed at 1-year follow-up.
Results
The ankle-brachial index was 0.69 ± 0.10 and 0.99 ± 0.40, respectively, pre- and post-procedure. C-arm CT imaging quality was rated as good or excellent in 80 %. In-stent minimal luminal diameter (MLD) was evaluated at 4.71 ± 0.7 mm on DSA, 3.39 ± 0.6 mm on IVUS, and 3.12 ± 0.9 mm on C-arm CT. Compared to IVUS, DSA demonstrated an overestimation of MLD (p = 0.0001), an underestimation of ISE (DSA = 18.8 % ± 7.6; IVUS = 29.8 % ± 9) (p < 0.0001), and a poor inter-technique intra-class correlation coefficient (ICC = 0.24). No difference was observed between IVUS and C-arm CT in ISE as calculated by diameter (29.8 ± 9 vs. 28.2 ± 12.5 %, p = 0.5) and area (30.2 ± 8.4 vs. 33.3 ± 9.5 %, p = 0.2). Inter-technique ICC between C-arm CT and IVUS was 0.72 [95 %CI 0.49; 0.85] for MLA measurements. The inter-observer ICC for MLD and MLA measurements on C-arm CT were, respectively, estimated at 0.75 [95 % CI 0.40, 0.89] and 0.77 [95 % CI 0.43, 0.90)].
Conclusions
C-arm CT presents a better correlation with IVUS than DSA to determine lumen diameter and ISE immediately after percutaneous revascularization.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Percutaneous transluminal angioplasty (PTA) of femoro-popliteal arteries offers an effective and minimally invasive alternative to surgical bypass. Initially limited to focal and short lesions, PTA is now routinely conducted and applied to more extensively diseased segments [1]. Compared to PTA alone, nitinol self-expanding stents used in the femoro-popliteal region have lowered the rate of early restenosis and improved acute and long-term patency even for long and complex lesions [2]. Stenting has resolved the issues of elastic recoil and flow-limiting dissection seen during balloon angioplasty alone [3]. However, stent under-deployment has been reported as a cause of restenosis after stenting of both iliac artery and SFA [4, 5]. Evaluation of stent expansion is therefore important to optimize percutaneous interventions.
Digital subtraction angiography (DSA) is considered the overriding image modality for angioplasty and stenting; however, this technique underestimates stenosis severity [6, 7]. The inability of DSA to identify technical failure of PTA is often related to the eccentricity of the lesions [7]. Unless multiplanar angiographic views are used, DSA is of limited value in optimizing stent deployment and apposition to wall. Intravascular ultrasound imaging (IVUS) allows a 360-degree cross-sectional evaluation of the arterial lumen and wall. Compared to DSA, IVUS accurately measures cross-sectional stenosis severity and is more sensitive in detecting and grading post-angioplasty dissections [5]. The superiority of IVUS over DSA in detecting technical failure following femoro-popliteal angioplasty has been established in several reports [8, 9]. Studies have shown that stent under-deployment can be corrected by further stent expansion based on IVUS findings [10]. Although IVUS imaging may improve long-term patency rates, its routine use in the catheterization laboratory is associated with increased costs [11]. Advanced imaging modalities such as C-arm computed tomography (CT) rotational acquisition enable CT-like images of soft tissue [12]. Preliminary clinical investigations have shown that C-arm CT offers cross-sectional imaging of the arterial lumen, arterial wall, and stent [13, 14]. We hypothesized that C-arm CT could allow better evaluation of post-angioplasty/stenting results than DSA by providing information similar to that for IVUS. The goal of this study was to assess the ability of C-arm CT images to document stent expansion and technical failure during femoro-popliteal interventions in comparison with DSA, using IVUS as a gold standard.
Methods
The institutional review board and local ethics committee approved this Health Insurance Portability and Accountability Act (HIPAA)-compliant study. All participants gave informed consent prior to their enrolment.
Patient Enrolment
This was a prospective comparative diagnostic study. Eligible patients included those older than 30 years of age referred for percutaneous revascularization of symptomatic femoro-popliteal artery disease (Rutherford stage 3 or more). All lesions treated in this study were classified as TASC (transatlantic intersociety consensus) A, B, and C lesions: >70 % obstruction or occlusion de novo or restenotic lesions in the SFA, with a target lesion length ranging from 5 to 20 cm [15]. Exclusion criteria included acute critical limb ischemia, poor ipsilateral iliac or femoral artery inflow, aneurysm in the target SFA lesions, renal failure, known intolerance to study medication (aspirin, heparin, nitinol, anticoagulant, and clopidogrel), or contrast agents.
A total of 54 % (27) of patients were also enrolled in another ongoing blinded randomized trial evaluating the effect of external beam radiation for the prevention of stent restenosis after femoral-popliteal stenting RXTX study (http://www.controlled-trials.com/ISRCTN74370657).
Under this protocol, patients were randomized to conventional angioplasty and stenting followed or not by external beam radiation 24 h after stenting to prevent restenosis. A total of 28 % of our patients actually received external radiotherapy. Finally, three patients previously stented were enrolled because in-stent stenosis was suspected.
Angioplasty/Stenting Procedure
Self-expandable Nitinol stents (Smart stent, Cordis Corporation, Warren, NJ, USA) were deployed under fluoroscopic guidance through a 6-F introducer sheath either before or after conventional balloon angioplasty. Stents were oversized by 1 mm in comparison with the reference diameter, while PTA balloon diameter was equivalent to the SFA reference diameter. A maximum of two stents were implanted per patient. Patients presenting with in-stent restenosis underwent either angioplasty or additional stenting. All patients received intra-arterial heparin boluses (3000–5000 U) at the time of the procedure. Following revascularization, patients under the RXTX protocol were given both clopidogrel and aspirin for 12 months, whereas patients enrolled outside the RXTX study received clopidogrel and aspirin for 3 months.
Per-procedure Technical Assessment
DSA was performed before and after angioplasty and stenting, and aimed at achieving technical success as recommended in the guidelines of the Society of Interventional Radiology (less than 30 % residual stenosis) [16]. Two views were systematically performed, an anteroposterior and an additional right or left anterior oblique projection (at the discretion of the operator) to better depict residual stenosis and stent expansion. After stenting, all patients underwent IVUS and C-arm CT evaluation. In the presence of residual stenosis greater than 50 % on IVUS, further angioplasty or additional stenting was performed if possible. Then, final DSA, C-arm CT, and IVUS were repeated.
Image Acquisition and Segmentation
DSA acquisition was performed using the recognized standard of practice [17]. Quantitative analyses of the baseline and post-angioplasty DSA acquisitions were performed by an independent core laboratory (angiography core lab at the Montreal Heart Institute) with automatic edge detection software (Medis, Leiden, NL). This software automatically calculates the minimal lumen diameter (MLD), mean diameter, and percent diameter stenosis [18].
IVUS evaluation was performed using 20 MHz catheters and an In-Vision Gold imaging unit (Volcano Therapeutics, San Diego, CA) with an automated pullback speed of 1 mm/s. A 3D automatic segmentation of the stent and its margins were performed on IVUS images using software developed and validated by our group [19]. The quality of segmentation was assessed visually in all patients on each cross-section and corrected manually when necessary.
C-arm CT image acquisition (Artis, DTA, Siemens, Forchheim, Germany) was performed using an 8-s digital radiography acquisition with a 2-s delay between injection and start of acquisition. 35 ml of contrast solution (10 ml Visipaque 270 mixed with 25 ml saline 0.9 %) was injected through the arterial sheath at 3.5 ml/s for 10 s. Segmentation of stent lumen and stent margins (15 mm proximal and distal to the stent) on C-arm CT images was performed independently on a specialized workstation (Object Research System, Montreal, Quebec, Canada) with semi-automatic software by two observers blinded to IVUS and DSA results.
The quality of DSA, IVUS, and C-arm CT images was rated by 2 independent investigators on a four-point scale: 1 Excellent, 2 Good, 3 Fair, and 4 Poor.
One-year Follow-up
Clinical assessment (before and 1 year after the intervention) included physical examination, symptom evaluation using the Rutherford classification, ankle-brachial index (ABI) measurements, and the walking impairment questionnaire. Adverse events were evaluated at baseline, 6 and 12 months post-intervention. Doppler ultrasonography of the treated lesions was performed for all patients at 6 months and 1-year post-angioplasty by experienced radiologists, blinded to the results of the other imaging modalities.
Study Endpoints
The primary endpoint of this study was incomplete stent expansion (ISE) at the end of the intervention assessed by minimal lumen diameter (MLD) and minimal lumen area (MLA) on DSA, IVUS, and C-arm CT images. Calculations of MLD, and ISE were compared between the 3 techniques and MLA between IVUS and C-arm CT.
ISE was determined by comparing the minimal stent dimension with the mean expansion of the stent in diameter (1-stent MLD/mean stent lumen diameter) and area (1-stent MLA/mean stent lumen area) as previously reported in remodeling studies (Fig. 1) [20]. This endpoint was then referred as stent ISE.
To minimize blooming artifacts due to stent edge, reference segment morphometry was evaluated in a 10-mm segment with a 5-mm margin proximal and distal to the stent. Again MLD (DSA, IVUS, and C-arm CT) and MLA (IVUS, C-arm CT) were calculated in the reference segments [21]. Finally, in-stent stenosis (ISS) was also calculated using the proximal and distal reference segments with the following formula in diameter (1-(stent MLD/mean proximal reference + mean distal reference lumen diameter)/2) and area (1-(stent MLA/mean proximal reference + mean distal reference lumen area)/2).
Other secondary endpoints were the evaluation of clinical success and stent patency at Doppler ultrasound examination after 1 year of follow-up. Patency was assessed by Doppler examination using the following criteria: 1. Stent thrombosis: the absence of duplex signal inside the stent; 2. in-stent stenosis of more than 50 %: peak systolic velocity (PSV) ratio of more than 2 in the area of greatest stenosis, when compared to the proximal and distal reference segment; and 3. Stent patency defined as freedom of restenosis and thrombosis [22].
Statistical Analysis
Patient variables were expressed as mean ± standard deviation for continuous variables. Descriptive statistics of the main study parameters in the stented (MLD, MLA, and ISE) and reference segments (MLD, MLA) were presented for each imaging technique as well as for the difference between imaging techniques. Differences between DSA, IVUS and C-arm CT parameters were determined by paired t test and inter-technique intra-class correlation coefficient (ICC). Inter-observer agreements between two observers for C-arm CT analyses were evaluated by ICC. Agreement on C-arm CT image quality between the two observers was evaluated with the Kappa statistic.
Technical failure was defined as stent ISE greater than 30 %. The ability of C-arm CT and DSA to detect technical failure as determined by IVUS was evaluated by calculating sensitivity and specificity with 95 % confidence interval. Receiver operating characteristic (ROC) curves were generated for the detection of 30 % stent ISE by diameter and 50 % by areas (50 % surface reduction roughly corresponds to 30 % diameter reduction).
Inter-technique accuracy was also evaluated by Bland–Altman analysis [23, 24].
The relationship between stent ISE and 1-year patency was assessed using paired t test. We used multiple logistic regression analysis to stratify for the confounding factor “radiotherapy arm” in patients who were also enrolled in the RXTX trial. Statistical significance was set at p < 0.05. All statistical analyses were performed with SAS 9.2. (SAS Institute Inc., Cary, North Carolina, USA).
Results
Clinical Characteristics
Fifty patients (34 males/16 females, aged 65.4 ± 8.6 years) with symptomatic lesion of the superficial femoral artery were enrolled, including 74 % stenotic and 26 % chronic occlusion lesions. The mean lesion length was evaluated at 52.2 ± 42.2 mm on DSA. Patient characteristics are shown in Table 1. Most patients (47) underwent angioplasty and stenting of the SFA; three patients who presented with intra-stent restenosis underwent angioplasty alone (one patient) or additional stenting (two patients). Among patients (43/50) where final DSA showed less than 30 % residual stenosis by diameter, two had additional angioplasty and re-stenting based on significant in-stent stenosis found during post-procedural IVUS examination.
The mean ABI improved from 0.69 ± 0.10 to 0.99 ± 0.40 after the procedures. One-year follow-up data were obtained for all enrolled patients with a mean follow-up period of 12.6 ± 1.6 months. Mean ABI was still improved at 1-year follow-up (0.90 ± 0.06) compared to baseline. The mean walking distance remained slightly but significantly improved (298 ± 125 m at baseline vs. 332 ± 93 m at 1 year; p < 0.02). Positive Doppler criteria of stent stenosis or occlusion were present in 28 % of patients (14/50) at one-year follow-up and 6/50 patients (12 %) had stent occlusion. Interestingly, these six patients presented either a stent fracture (two patients) or clopidogrel non-adherence (four patients).
Image Quality
C-arm CT image quality was rated as excellent in 62 %, good in 18 %, and fair in 20 % of cases by the first observer, with a very good agreement between both observers (Kappa = 0.85 (p < 0.001), 95 % CI 0.67, 0.96). Blooming artifacts related to stent markers were frequently observed at stent extremities.
Evaluation of Stented Segment
Stent length was estimated at 99 ± 55, 101 ± 46, and 108 ± 47 mm, respectively, on IVUS, C-arm CT, and DSA (p = 0.53). When compared with IVUS examination, in-stent MLD was overestimated on DSA by more than 39 % (DSA: 4.71 ± 0.70 mm vs. IVUS: 3.39 ± 0.60 mm; p < 0.0001), whereas less than 10 % underestimation was observed on C-arm CT for MLD (3.11 ± 0.9 mm; p = 0.1) and MLA (p = 0.4, Table 2; Fig. 2). The average absolute differences of MLD between IVUS and DSA and between IVUS and C-arm CT were, respectively, 1.3 mm [95 % CI 0.27; 2.33] and 0.28 mm [95 % CI −1.75; 1.20] (Fig. 3A, B). ISE was significantly underestimated on angiography as compared to IVUS (DSA: 18.8 ± 7.6 % vs. IVUS: 29.8 ± 9.0 %; p < 0.0001). No difference in ISE was observed between IVUS and C-arm CT as calculated by diameter (29.8 ± 9 vs. 28.2 ± 12.5 %, p = 0.5) and area (30.2 ± 8.4 vs. 33.3 ± 9.5 %, p = 0.2). C-arm CT provided good delineation of structural details of plaque and stent struts (Figs. 4, 5).
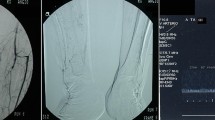
C-arm CT evaluation of stent apposition. DSA post-SFA stenting (A, B) showing an ISE estimated at 26 % (arrow). Corresponding C-arm CT coronal (C) and multiple 2D axial reformations along the stent axis demonstrated an ISE estimated at 49 % (D). It is possible to observe the relationships between stent lumen, soft, and calcified plaque on IVUS (E)
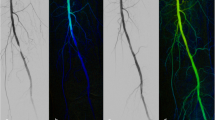
Blooming artifact. A and B Patient presenting with in-stent restenosis who underwent angioplasty and stenting. C and D DSA after additional stenting showing adequate stent expansion. E Severe blooming artifact impairing lumen analysis at the level of distal markers of the first stent (zone of stent overlap). F Complete stent expansion is seen on corresponding IVUS acquisition
Inter-technique and Inter-observer Agreement
Inter-technique ICC between C-arm CT and IVUS was estimated at 0.72 [95 % CI 0.49, 0.85] for MLA and 0.62 [95 % CI 0.4, 0.77] for MLD. Lesser agreement was observed between IVUS and DSA with an ICC value of 0.24 for MLD [95 % CI 0.06, 0.60].
The inter-observer ICC for C-arm CT was calculated at 0.75 [95 % CI 0.40, 0.89] for MLD and 0.77 [95 % CI 0.43, 0.9] for MLA.
Reference Segment Evaluation
In contrast to stented segments, MLD of reference segments by DSA and IVUS was similar. An underestimation of MLD was observed for C-arm CT for both proximal and distal reference segments in comparison with IVUS (p ≤ 0.002, Table 3).
Technical Failure Detection
DSA and C-arm CT (two observers) had similar accuracy in detecting technical failure (ISE >30 %) as observed on IVUS (DSA: 0.70 vs. C-arm CT: 0.60) with a better sensitivity of C-arm CT (DSA = 31.6 % vs. C-arm CT = 57.9 %) but a lower specificity (DSA = 100 % vs. C-arm CT = 74.1 %) (Table 4).
Links with Clinical Outcomes
There were no differences in ISE, MLD, and MLA as measured post-procedure among patients with patent stent and those presenting with restenosis or thrombosis on Doppler ultrasound at 1-year follow-up (Table 5). Analyses were adjusted for the radiotherapy factor. Binary logistic regression analyses for patency assessment at 1 year by Doppler did not show a significant effect of radiotherapy in our model (OR 0.18 p = 0.29).
Discussion
There has been a remarkable increase in the number of SFA endovascular revascularizations performed annually over the last decade, due essentially to advancements in the development of second and third generations of nitinol stents [25–27]. Because stenting is subject to complex and varied mechanical stresses in long and calcified atherosclerotic lesions, detecting technical failure after stenting remains challenging. In-vitro testing and preliminary clinical investigation have shown that C-arm CT offers cross-sectional imaging of the arterial lumen, arterial wall, and stent [13]. C-arm CT is capable of visualizing small Nitinol stents with low radio opacity and strut diameters of 70 µm [28].
In the present study, C-arm CT was compared for the first time with DSA, using IVUS as a gold standard during SFA stenting. C-arm CT and IVUS provided concordant data on MLD and MLA measurements inside the stent. Our data are consistent with previous work [10] showing an overestimation of in-stent MLD for DSA compared to IVUS. This discrepancy may be accounted for by the availability of cross-sectional images obtained from C-arm CT and IVUS, thus providing the best defined plane to identify the MLD in contrast to only two cranio-caudal projections acquired routinely at the end of the procedure on DSA examinations. This fact may also explain why our results showed more ISE with IVUS and C-arm CT than with DSA.
The underestimation of the reference segment MLD observed on C-arm CT could be explained by blooming artifacts at the level of edge stent markers (see Fig. 5). However, this discordance was not observed between C-arm CT and IVUS for measurements of the reference segment MLA. One of the major drawbacks of the C-arm CT evaluation was indeed the blooming artifacts, especially at stent extremities (radio-opaque markers). This artifact can generate a thickening of stent struts and artificially minimize MLD, which could explain the loss of specificity of C-arm CT in this study.
The restenosis rate (approximately 30 % at 1 year) observed in this study is in accordance with prior observations [29] which showed that self-expanding nitinol stents translate into a substantial benefit. However, the follow-up period of 1 year is not sufficient to properly evaluate in-stent restenosis [30–32]. No link was observed between ISE and stent patency at 1 year, and 66.7 % of patients presenting with stent thrombosis discontinued clopidogrel before 1 year of follow-up. Thus, adherence to medication may be a confounding factor that could have influenced the occurrence of in-stent stenosis or thrombosis.
Radiation exposure remains an important issue for C-arm CT. Substantial changes have been made in C-arm CT technology with the aim of reducing radiation doses. With a rotation time of 8 s (the protocol used in our study), the amount of radiation is similar to a biplane DSA during a cerebral angiogram (9 mGy) [33]. However, improving clinical imaging protocols as well as rotation time may reduce radiation doses. In this setting, a compromise between image quality and dose needs to be defined.
The main limitations of this study are its small sample size and the absence of long-term follow-up. Thus, we have observed a low restenosis rate but we cannot draw a definitive conclusion about the link between in-stent MLD and ISE and long-term patency. We also decided to evaluate ISE by comparing MLD or MLA within the stent with mean stent diameter or area (instead of reference segments outside the stent). This approach was selected to estimate homogeneity of stent expansion and take into consideration self-expandable stent oversizing that will artificially over-expand the stented segment. This approach is more sensitive in detecting areas of stent under expansion caused by calcified plaques just after deployment. Finally, in our work, 54 % of patients were also enrolled in a study investigating the efficacy of external beam radiation on restenosis. This may have lowered the occurrence of stenosis and occlusion and minimized the clinical impact of C-arm CT findings in comparison to conventional DSA.
In conclusion, this is the first study showing the clinical feasibility of C-arm CT imaging to assess technical success after femoro-popliteal stenting. The first correlation analysis between IVUS and C-arm CT is encouraging, with high inter-technique correlation for in-stent MLD, MLA, and ISE. Thus, C-arm CT could replace IVUS to analyze these endpoints in particular for research studies.
References
Dorrucci V. Treatment of superficial femoral artery occlusive disease. J Cardiovasc Surg (Torino). 2004;45(3):193–201.
Dick P, Wallner H, Sabeti S, Loewe C, Mlekusch W, Lammer J, Koppensteiner R, Minar E, Schillinger M. Balloon angioplasty versus stenting with nitinol stents in intermediate length superficial femoral artery lesions. Catheter Cardiovasc Interv. 2009;74(7):1090–5.
Lyden SP, Shimshak TM. Contemporary endovascular treatment for disease of the superficial femoral and popliteal arteries: an integrated device-based strategy. J Endovasc Ther. 2006;13(Suppl 2):II41–51.
Rosenfield K, Schainfeld R, Pieczek A, Haley L, Isner JM. Restenosis of endovascular stents from stent compression. J Am Coll Cardiol. 1997;29(2):328–38.
Buckley CJ, Arko FR, Lee S, Mettauer M, Little D, Atkins M, Manning LG, Patterson DE. Intravascular ultrasound scanning improves long-term patency of iliac lesions treated with balloon angioplasty and primary stenting. J Vasc Surg. 2002;35(2):316–23.
Willoteaux S, Moranne O, Duda SH, Lions C, Gaxotte V, Durand F, Negawi Z, Beregi JP. Multislice computed tomographic angiography versus digital subtraction angiography in the follow-up of nitinol stents in the superficial femoral artery. J Endovasc Ther. 2006;13(5):609–15.
Arthurs ZM, Bishop PD, Feiten LE, Eagleton MJ, Clair DG, Kashyap VS. Evaluation of peripheral atherosclerosis: a comparative analysis of angiography and intravascular ultrasound imaging. J Vasc Surg. 2010;51(4):933–8 (discussion 939).
Laird JR, Katzen BT, Scheinert D, Lammer J, Carpenter J, Buchbinder M, Dave R, Ansel G, Lansky A, Cristea E, Collins TJ, Goldstein J, Cao AY, Jaff MR, Investigators R. Nitinol stent implantation vs. Balloon angioplasty for lesions in the superficial femoral and proximal popliteal arteries of patients with claudication: three-year follow-up from the resilient randomized trial. J Endovasc Ther. 2012;19(1):1–9.
Laird JR, Katzen BT, Scheinert D, Lammer J, Carpenter J, Buchbinder M, Dave R, Ansel G, Lansky A, Cristea E, Collins TJ, Goldstein J, Jaff MR, Investigators R. Nitinol stent implantation versus balloon angioplasty for lesions in the superficial femoral artery and proximal popliteal artery: twelve-month results from the resilient randomized trial. Circ Cardiovasc Interv. 2010;3(3):267–76.
Kuribayashi S, Takamiya M, Homma S. Intravascular ultrasound observations during iliac stent deployment. Int Angiol. 1999;18(4):263–70.
Gaster AL, Slothuus U, Larsen J, Thayssen P, Haghfelt T. Cost-effectiveness analysis of intravascular ultrasound guided percutaneous coronary intervention versus conventional percutaneous coronary intervention. Scand Cardiovasc J. 2001;35(2):80–5.
Akpek S, Brunner T, Benndorf G, Strother C. Three-dimensional imaging and cone beam volume ct in c-arm angiography with flat panel detector. Diagn Interv Radiol. 2005;11(1):10–3.
Wallace MJ, Kuo MD, Glaiberman C, Binkert CA, Orth RC, Soulez G. Three-dimensional c-arm cone-beam ct: applications in the interventional suite. J Vasc Interv Radiol. 2009;20(7 suppl):S523–37.
Wallace MJ, Kuo MD, Glaiberman C, Binkert CA, Orth RC, Soulez G. Three-dimensional c-arm cone-beam ct: applications in the interventional suite. J Vasc Interv Radiol. 2008;19(6):799–813.
Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, Fowkes FG. Inter-society consensus for the management of peripheral arterial disease (TASCII). J Vasc Surg. 2007;45(Suppl S):S5–67.
Hirsch AT, Haskal ZJ, Hertzer NR, Bakal CW, Creager MA, Halperin JL, Hiratzka LF, Murphy WR, Olin JW, Puschett JB, Rosenfield KA, Sacks D, Stanley JC, Taylor LM Jr, White CJ, White J, White RA, Antman EM, Smith SC Jr, Adams CD, Anderson JL, Faxon DP, Fuster V, Gibbons RJ, Hunt SA, Jacobs AK, Nishimura R, Ornato JP, Page RL, Riegel B. ACC/AHA 2005 practice guidelines for the management of patients with peripheral arterial disease (lower extremity, renal, mesenteric, and abdominal aortic): a collaborative report from the American Association for Vascular Surgery/Society for Vascular Surgery, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA task force on practice guidelines (writing committee to develop guidelines for the management of patients with peripheral arterial disease). Circulation. 2006;113(11):e463–654.
Singh H, Cardella JF, Cole PE, Grassi CJ, McCowan TC, Swan TL, Sacks D, Lewis CA. Quality improvement guidelines for diagnostic arteriography. J Vasc Interv Radiol. 2003;14(9 Pt2):S283–8.
Berry C, L’Allier PL, Gregoire J, Lesperance J, Levesque S, Ibrahim R, Tardif JC. Comparison of intravascular ultrasound and quantitative coronary angiography for the assessment of coronary artery disease progression. Circulation. 2007;115(14):1851–7.
Cardinal MH, Meunier J, Soulez G, Maurice RL, Therasse E, Cloutier G. Intravascular ultrasound image segmentation: a three-dimensional fast-marching method based on gray level distributions. IEEE Transmed Imaging. 2006;25(5):590–601.
Schwartz RS, Edelman ER, Carter A, Chronos N, Rogers C, Robinson KA, Waksman R, Weinberger J, Wilensky RL, Jensen DN, Zuckerman BD, Virmani R. Consensus Committee. Drug-eluting stents in preclinical studies: recommended evaluation from a consensus group. Circulation. 2002;106(14):1867–73.
Schlager O, Dick P, Sabeti S, Amighi J, Mlekusch W, Minar E, Schillinger M. Long-segment SFA stenting–the dark sides: in-stent restenosis, clinical deterioration, and stent fractures. J Endovasc Therapy. 2005;12(6):676–84.
Duda SH, Bosiers M, Lammer J, Scheinert D, Zeller T, Tielbeek A, Anderson J, Wiesinger B, Tepe G, Lansky A, Mudde C, Tielemans H, Beregi JP. Sirolimus-eluting versus bare nitinol stent for obstructive superficial femoral artery disease: the sirocco ii trial. J Vasc Interv Radiol. 2005;3(16):331–8.
Bland JM, Altman DG. Comparing methods of measurement: why plotting difference against standard method is misleading. Lancet. 1995;346(8982):1085–7.
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1(8476):307–10.
Baril DT, Marone LK, Kim J, Go MR, Chaer RA, Rhee RY. Outcomes of endovascular interventions for TASC II B and C femoropopliteal lesions. J Vasc Surg. 2008;48(3):627–33.
Bosiers M, Deloose K, Callaert J, Moreels N, Keirse K, Verbist J, Peeters P. Results of the protege everflex 200-mm-long nitinol stent (ev3) in TASC C and D femoropopliteal lesions. J Vasc Surg. 2011;54(4):1042–50.
Scheinert D, Grummt L, Piorkowski M, Sax J, Scheinert S, Ulrich M, Werner M, Bausback Y, Braunlich S, Schmidt A. A novel self-expanding interwoven nitinol stent for complex femoropopliteal lesions: 24-month results of the supera sfa registry. J Endovasc Ther. 2011;18(6):745–52.
Ebrahimi N, Claus B, Lee CY, Biondi A, Benndorf G. Stent conformity in curved vascular models with simulated aneurysm necks using flat-panel ct: an in vitro study. Am J Neuroradiol. 2007;28(5):823–9.
Ferreira M, Lanziotti L, Monteiro M, Abuhadba G, Capotorto LF, Nolte L, Fearnot N. Superficial femoral artery recanalization with self-expanding nitinol stents: long-term follow-up results. Eur J Vasc Endovasc Surg. 2007;34(6):702–8.
Kastrati A, Schomig A, Dietz R, Neumann FJ, Richardt G. Time course of restenosis during the first year after emergency coronary stenting. Circulation. 1993;87(5):1498–505.
Schillinger M, Mlekusch W, Haumer M, Sabeti S, Ahmadi R, Minar E. Angioplasty and elective stenting of de novo versus recurrent femoropopliteal lesions: 1-year follow-up. J Endovasc Therapy. 2003;10(2):288–97.
Schillinger M, Minar E. Endovascular stent implantation for treatment of peripheral artery disease. Eur J Clin Invest. 2007;37(3):165–70.
Fahrig R, Dixon R, Payne T, Morin RL, Ganguly A, Strobel N. Dose and image quality for a cone-beam c-arm CT system. Med Phys. 2006;33(12):4541–50.
Coyne KS, Margolis MK, Gilchrist KA, Grandy SP, Hiatt WR, Ratchford A, Revicki DA, Weintraub WS, Regensteiner JG. Evaluating effects of method of administration on walking impairment questionnaire. J Vasc Surg. 2003;8(2):296–304.
Acknowledgments
Gilles Soulez was supported for this work by the Canadian Institutes of Health Research through a collaborative research program with Siemens Medical Germany (Grant Number: CIHR ISO-83052), and a senior clinical research scholarship (to Gilles Soulez from the Fonds de la Recherche en Santé du Québec (FRSQ, Grant Ref: 9958)).
Conflict of Interest
Gerald Gahide, Sofian Hadjaj, Eric Therasse, Claude Kauffmann, Patrick Gilbert, Vincent L Oliva, Jean-Claude Tardif, Jacques Lesperance, and Guy Cloutier have no conflict of interest.
Statement of Human and Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gahide, G., Hadjadj, S., Therasse, E. et al. Value of C-Arm Computed Tomography to Evaluate Stent Deployment During Femoro-Popliteal Revascularization. Cardiovasc Intervent Radiol 38, 1458–1467 (2015). https://doi.org/10.1007/s00270-015-1108-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-015-1108-1