Abstract
Background
Preoperative physiological assessments are crucial for optimizing clinical outcomes, especially those of elderly esophageal cancer (EC) patients who are generally frail and at the high risk of mortality.
Methods
Patients who underwent surgery for EC between 2004 and 2018 were retrospectively reviewed. Patients were categorized into elderly (>70 years) or non-elderly (≤70 years) groups. Various physiological parameters including the Charlson Comorbidity Index (CCI), immunonutritional parameters and pulmonary functions were studied. Pulmonary functions included %vital capacity (VC) and forced expiratory volume in one second (FEV1.0) and FEV1.0%. The thresholds were set as the lowest quartile (100% for %VC and 2L for FEV1.0) in this cohort. Multivariate Cox hazards models were applied to determine independent predictors of non-EC-related deaths.
Results
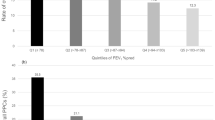
In total, 824 patients were included (elderly; n = 306, non-elderly; n = 518). Elderly patients had a significantly lower 5-year OS rate than non-elderly patients (53.3% vs. 57.2%, P = 0.03), mainly due to increased risk of death from non-EC related causes. In the elderly group, multivariate Cox hazards analysis identified 3 independent predictors of non-EC-related deaths; high CCI (HR 1.98, P=0.006), low %VC (HR 2.01, P = 0.004) and low FEV1.0 (HR 1.6, P=0.048). Elderly patients without risk factors had a significantly better 5-year OS rate (63.5%) than those with 1 (50.0%) or 2–3 (36.3%) risk factors (P <0.01). Deaths due to pulmonary disease rose significantly as the number of risk factors increased (P=0.03).
Conclusions
The severity of comorbidities and pulmonary function impairments are useful for predicting long-term outcomes, especially non-EC-related deaths, in elderly EC patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The recent substantial rise in cancer cases among older adults represents a considerable challenge for healthcare systems worldwide [1]. Declining physiological status, the high prevalence of frailty and short life expectancy of older patients complicate cancer management in this population [2]. In particular, the high possibility of mortality attributable to other causes after surgery largely impacts the survival outcomes of elderly patients with upper gastrointestinal malignancies [3, 4].
Clinicians have little evidence on which to base treatment strategies for this age group due to the limited number of clinical investigations conducted to date. Given that the health status and fitness of elderly patients are heterogeneous, chronologic age alone should not be used as the sole criterion for treatment decision-making [5]. Several geriatric assessment tools have thus been proposed by care providers for the elderly [5, 6].
Esophageal cancer (EC) constitutes the sixth leading cause of cancer deaths worldwide, despite the recent advances in diagnosis and multimodal treatments [7, 8]. Esophagectomy is a highly invasive procedure with considerable morbidity [9], and no consensus has yet been established regarding either age or frailty for identifying candidates who would be medically fit to undergo esophagectomy.
The number of elderly patients with EC has been increasing, and approximately 20% of EC patients in Japan are reportedly ≥75 years of age [10, 11]. Previous studies have revealed advanced age to be significantly associated with high short-term mortality and poor long-term survival [12, 13] and have further suggested esophagectomy to provide a small survival benefit for octogenarians [14]. Given that not only chronological age but also physiological status, as reflected by nutritional status and/or the severity of comorbidities, is reportedly associated with survival outcomes in elderly EC patients [3, 13, 15], therapeutic approaches should be tailored to each patient’s condition.
Herein, we studied the survival impact of advanced age in patients undergoing surgery for EC. Furthermore, we investigated clinical factors useful for predicting survival outcomes, especially deaths from causes other than the EC itself, in elderly EC patients.
Patients and methods
Patients
From January 2004 to December 2018, a total of 874 consecutive patients with pathologically confirmed EC underwent esophagectomy at the Saitama Cancer Center. Of the total 874 patients, 33 who died due to postoperative complications, 8 undergoing surgery for remnant EC, 3 with a history of total pharyngolaryngectomy and 6 lacking data on preoperative pulmonary functions were excluded from the analysis. The median follow-up period was 80.2 months for the survivors. This retrospective study was approved by the local ethics committee of the Saitama Cancer Center (ID: 1267).
Studied criteria
Demographic data were collected prior to treatment. Comorbidities were categorized according to the Charlson Comorbidity Index (CCI) [16]. Clinical and histological tumor staging was based on the TNM classification (UICC, 8th edition) [17]. As a nutritional parameter, Onodera's prognostic nutritional index (PNI: 10 × albumin + 0.005 × total lymphocyte count) was calculated [18]. The Glasgow prognostic score (GPS) was estimated as an inflammatory marker, as previously described [19].
Evaluation of preoperative pulmonary function
Pulmonary functions were measured using spirometry. Vital capacity (VC), as a percent of predicted (%VC), and the forced expiratory volume in one second (FEV1.0)/forced VC ratio (FEV1.0%) were employed to evaluate ventilatory functions [4, 20]. The cut-off values for %VC and FEV1.0 were set as the lowest quartile (100% for %VC and 2L for FEV1.0) in this cohort.
Treatment strategy
Prior to treatment, the clinical stage was determined by the relevant Multidisciplinary Tumor Board. All patients selected their own treatment modality after consulting with surgeons, medical oncologists and radiologists. Patients were treated according to the Japan Esophageal Society guideline [21]. For patients with T1N1-3 or T2-4a (any N) disease, neoadjuvant chemotherapy followed by surgery was generally performed. As a preoperative treatment, cisplatin (CDDP) plus 5-fluorouracil (5-FU) (CF) therapy was the standard regimen [22], while one consisting of three drugs (CDDP, 5-FU, and docetaxel; DCF therapy) was optional [23]. As chemoradiotherapy (CRT), the CF regimen was added to radiation. For patients clinically diagnosed as having cT4b and/or unresectable lymph node metastasis, definitive CRT (dCRT) was indicated as an initial treatment. dCRT was also administered to those who preferred nonsurgical treatment, regardless of the tumor stage. The patients who failed dCRT were candidates for salvage esophagectomy, if curative resection was considered to be clinically feasible.
Surgical treatment and perioperative management
With the patient under general anesthesia, we placed a single lumen spiral endotracheal tube with a blocker into the right bronchus for one-lung anesthesia to avoid fixing the trachea to the mediastinum. Our standard procedures consisted of subtotal esophagectomy along with en bloc lymph node dissection using a cervico-thoraco-abdominal approach. The operative thoracic approach was by video-assisted thoracoscopic surgery (VATS) or thoracotomy. A gastric conduit was conveyed through the retrosternal or posterior mediastinal route, and esophagogastric anastomosis was usually performed at the neck. The transmediastinal esophagectomy (abdominal-cervical approach) was selected for high-risk patients. Tube duodenostomy was added before abdominal closure to allow early postoperative jejunal feeding. The Clavien–Dindo (C-D) scale was used to grade the severity of all postoperative morbidities [24]. Postoperative surveillance was performed based on the Guidelines for Diagnosis and Treatment of Carcinoma of the Esophagus [21].
Statistical analysis
Categorical variables were expressed in numerical figures and percentages and compared using Fisher’s exact test or the χ2 test, as appropriate. Continuous variables were expressed as the median values (range) and compared using Wilcoxon’s rank-sum test (A Mann–Whitney U test). Overall survival (OS) was calculated from the operation date. Cancer-specific survival (CSS) was defined as the period from the date of surgery until death due to EC. Non-EC-related deaths included those from both non-malignant diseases and malignancies other than EC. Survival curves were constructed using the Kaplan–Meier method, and either the log-rank test (for comparisons of 2 groups) or the log-rank test followed by Holm's sequential Bonferroni corrections (for comparisons of ≥ 3 groups) was used to determine statistical significance, as appropriate. A multivariate Cox proportional-hazards analysis was performed to identify independent prognostic factors. Clinically meaningful factors with p <0.05 in a Cox proportional hazard model with univariable analysis were regarded as potential risk factors and were further analyzed by applying a multivariable Cox model. Statistical analyses were carried out using JMP 16.0.0 (SAS Institute, Cary, NC, USA).
Results
Survival outcomes according to age
In total, 824 EC patients were included in this study. First, we classified patients into 3 groups according to age (≤70, 71–75 and >75 years of age) and compared the survival outcomes among these 3 groups. OS curves were significantly demarcated according to the age group (P=0.02, Fig. 1a); however, the 5-year OS rate of patients 71–75 years of age was essentially equivalent to that of patients ≤70 years of age and also that of patients >75 years of age (57.6% vs. 57.2%, P=0.98; 57.6% vs. 48.7%, P=0.18). CSS was not significantly demarcated according to age (P=0.31, Fig. 1b). In contrast, survival was well-demarcated when death from non-EC-related disease was taken as the event of interest (P <0.01, Fig. 1c). Patients >70 years of age had a significantly higher risk of non-EC-related death than those ≤70 years of age (P=0.01, Fig. 1c). Overall, advanced age (>70 years) was associated with significantly increased non-EC-related deaths as compared to younger age (≤70 years) in our cohort. We thus subsequently divided our cohort into elderly (>70 years) and non-elderly (≤70 years) EC patients.
Comparison of clinicopathological and demographic characteristics and survival between elderly and non-elderly EC patients
Clinicopathological features according to age are shown in Table 1. Advanced age was significantly associated with poorer pulmonary functions (P <0.01), lower PNI (P <0.01) and lower rate of pStage III-IV disease (P=0.03). OS curves were significantly stratified by age (P=0.03, Fig. 2a). Importantly, no significant survival difference was found when the event was EC (P=0.19, Fig. 2b), but survival was well-demarcated when death from non-EC-related disease was taken as the event of interest (P <0.01, Fig. 2c). Elderly patients had a significantly higher incidence of death due to pulmonary diseases than non-elderly patients (9.5% vs. 3.7%, P <0.01, Supplementary Fig. 1).
Comparison of survival outcomes between elderly and non-elderly patients. (a) Elderly (>70 years of age) patients had significantly poorer OS than non-elderly patients (P=0.03). (b) No significant survival difference was found when the event was EC (P = 0.19), but (c) Survival was well-demarcated when death from non-EC-related disease was taken as the event of interest (P <0.01)
Predictors of non-EC-related deaths in elderly patients
Univariable analysis and subsequent application of the multivariable Cox proportional hazards model revealed high CCI (≥ 2), low %VC (<100%) and pStage III–IV disease to be independently associated with poor OS outcomes in the elderly group (Table 2). Notably, multivariate Cox hazards model analysis focusing on non-EC-related deaths showed high CCI (≥2) (HR 1.98, 95% CI 1.22–3.22, P=0.006), low %VC (<100%) (HR 2.01, 95% CI 1.24–3.24, P=0.004) and low FEV1.0 (<2L) (HR 1.6, 95% CI 1.00–2.57, P=0.048) to be independent predictors of non-EC-related deaths (Table 3).
Next, we stratified patients into 3 groups according to the number of the 3 identified variables present (high CCI, low %VC and low FEV1.0; 0, low risk; 1, intermediate risk; 2–3, high risk). Age and the rate of female sex increased as the number of risk factors increased in the elderly group (Table 3). Neither the incidence of postoperative complications nor pStage differed significantly among the 3 groups (Table 4).
Survival outcomes according to the number of factors predicting non-EC-related deaths
Patients without risk factors had a significantly better 5-year OS rate (63.5%) than those with 1 (50.0%) or 2–3 (36.3%) risk factors (P<0.01, Fig. 3a). The survival difference among the 3 groups was attributable mainly to non-EC-related deaths (Fig. 3b, c). The incidence of deaths due to pulmonary disease rose significantly as the number of risk factors increased in the elderly group (P = 0.03, Supplementary Figure 2).
Survival outcomes according to the number of risk factors. (a) Patients without risk factors had a significantly better 5-year OS rate (63.5%) than those with 1 (50.0%) or 2–3 (36.3%) risk factors (P <0.01). (b) Cancer-specific survival and (c) non-EC-related deaths according to the number of risk factors
Discussion
This study demonstrated poor survival outcomes of elderly EC patients to be attributable mainly to the high incidence of death from non-EC-related causes in this population. We identified several physiological parameters which were useful for predicting non-EC-related deaths in elderly EC patients, and devised a novel tool applicable to stratifying the survival outcomes of elderly EC patients.
Previous studies have highlighted the relatively poor short- and long-term outcomes of elderly EC patients as compared with their non-elderly counterparts [11, 12, 25]. It is noteworthy that the survival impacts of physiological status, as reflected by frailty, nutritional status, comorbidities and/or BMI outside of normal range, are more evident in elderly than in non-elderly patients [3, 13, 15, 26]. As such, preoperative evaluation of multidimensional health status is of major importance for improving the survival outcomes of elderly EC patients [2].
The present study showed the poor survival outcomes of elderly EC patients to be attributable mainly to the high probability of non-cancer-related deaths. Therefore, we performed multivariable Cox hazards analysis focusing on non-EC-related deaths and identified three physiological factors (low %VC, low FEV1.0 and comorbidity) impacting non-EC-related deaths. Only a few studies have focused on non-cancer-related deaths in EC patients [20, 27], although this is a highly relevant issue from a public health perspective [28]. Our newly proposed tool based on physiological status is useful for stratifying long-term outcomes of elderly EC patients, especially predicting the risk of non-cancer mortality.
Lung elasticity and intercostal muscle mass both deteriorate with advancing age, resulting in lung function impairments in the elderly population [29]. Notably, the presence of impaired lung functions is reportedly associated with high general mortality [30], and poor survival outcomes of patients who underwent surgery for upper gastrointestinal malignancies [4, 20]. Furthermore, a recent study highlighted the survival impacts of the difference between lung age and chronological age in EC patients [31]. Our observations, together with those made in previous studies, suggest pulmonary function evaluation to be useful for predicting frailty in elderly patients [4, 20, 32]. The severity of comorbidities is also reportedly associated with survival outcomes and non-cancer mortality of EC patients undergoing surgery [27, 33, 34]. Overall, our observation that elderly patients with both lung function impairments and high CCI have very poor survival outcomes is reasonable.
In our present study, oncological outcomes did not differ significantly between elderly and non-elderly patients. Previous studies have shown less aggressive treatments, such as omission of neoadjuvant chemotherapy or limited lymphadenectomy, to often be applied to the elderly, leading to poor oncological outcomes for these patients [13, 35]. In our present study, however, the NAC administration rates did not differ significantly between the elderly and the non-elderly, possibly accounting for the similar oncological outcomes of these two groups. On the other hand, a recent study suggested the negative survival impact of postoperative complications to be particularly apparent in elderly patients who received triplet chemotherapy [36]. Further investigation is required to determine the optimal treatment intensity for elderly patients. Taken together, these observations highlight why the individual oncological impacts of age remain controversial in ESCC patients.
The incidence of postoperative complications did not rise significantly as the number of risk factors increased. This observation, together with a recent study which showed frailty to not necessarily be associated with morbidity [26], suggests esophagectomy to potentially be feasible even for frail patients. However, the survival benefit of esophagectomy remains controversial in elderly patients with EC [14], especially those with significant comorbidities [37]. While less invasive treatment strategies, such as endoscopic resection or chemoradiotherapy, are reportedly indicated for frail elderly patients [38, 39], the benefit of CRT remains controversial, especially for super-elderly patients with EC [40]. In general, surgical indications should not be determined based solely on chronological age [14], although optimal selection criteria have yet to be established [10]. Whether our newly proposed survival prediction model is useful for determining surgical indications merits further study.
Our model might help clinicians optimize perioperative managements for patients with impaired physiological functions. Pharmacological interventions are reportedly useful for improving the survival of patients with pulmonary diseases [41]. High-risk patients might be good candidates for long-term rehabilitation programs. Notably, recent randomized trails revealed a supervised exercise program and a health education informatics program to improve both cardiorespiratory fitness and quality of life for EC patients after esophagectomy [42, 43]. The combination of pre-habilitation and pre-nutrition therapy reportedly improves perioperative functional capacity, thereby reducing the incidence of postoperative complications [44].
Pulmonary morbidity after esophagectomy can be avoided by perioperative management strategies such as pre-operative smoking cessation, respiratory rehabilitation, maintaining oral hygiene, perioperative nutritional interventions and applying less invasive surgery [45]. In our institution, all patients start a rehabilitation program and visit a dentist at the outpatient clinic. Furthermore, MIE was generally performed (85%) during the study period, and enteral nutrition was given via the jejunostomy postoperatively. In addition to these managements, further surgical approaches can be modified in frail patients. Transmediastinal esophagectomy can avoid one-lung ventilation and can be performed on frail people, such as the elderly or patients with pulmonary comorbidities [46]. Also, robot-assisted minimally invasive esophagectomy can reportedly improve postoperative outcomes [47].
Our study has limitations. First, we did not include patients who underwent dCRT, which is reportedly a less-invasive and efficacious treatment option for elderly EC patients [39]. Accordingly, our cohort included only patients deemed fit for an esophagectomy. Although the proportion of ESCC patients who received dCRT did not differ according to the age category in our study (data not shown), selection bias might influence the results. Second, the definition of elderly differs among investigations. We defined advanced age as >70 years considering that patients older than 70 had significantly poorer survival outcomes. Several prior investigations have employed the same age threshold [13, 15, 25], while others used different cut-off values [12, 35]. A recent study suggested that rather than >70 years, >75 years would be the most useful age cut-off value for indicating poor survival [12]. Differences in standard care regimens during the study period, the NAC administration rate and tumor histology might have influenced the survival impacts of aging. The optimal age cut-off in EC patients merits further research. Third, the thresholds for %VC and FEV1.0 were set as the lowest quartile (100% for %VC and 2L for FEV1.0) in our cohort. In general, pulmonary dysfunction is defined as %VC <80% or FEV1.0%<70%. In our cohort, the proportion of patients with %VC <80% was very small (3.3%), a finding consistent with prior studies [48], because thoracic surgery is not feasible for patients with extremely poor pulmonary functions. Finally, this was a single-institution study with a relatively small number of patients. Further studies with larger cohorts are needed to achieve more convincing results.
In conclusion, elderly EC patients are at high risk of death from non-EC-related causes, which worsens the overall survival outcomes of this population. A survival prediction model based on physiological status is useful for stratifying the survival outcomes of elderly EC patients, thus aiding clinicians in optimizing treatment strategies.
Abbreviations
- EC:
-
Esophageal cancer
- CCI:
-
Charlson comorbidity index
- VC:
-
Vital capacity
- FEV1.0:
-
Forced expiratory volume in one second
- PNI:
-
Prognostic nutritional index
- GPS:
-
Glasgow prognostic score
- CDDP:
-
Cisplatin
- 5-FU:
-
5-Fluorouracil
- dCRT:
-
Definitive chemoradiotherapy
- VATS:
-
Video-assisted transthoracic surgery
- C-D:
-
Clavien–Dindo
- OS:
-
Overall survival
- CSS:
-
Cancer-specific survival
- HR:
-
Hazard ratios
- CI:
-
Confidence intervals
References
DuMontier C, Loh KP, Bain PA et al (2020) Defining undertreatment and overtreatment in older adults with cancer: a scoping literature review. J Clin Oncol 38:2558–2569
Soto-Perez-de-Celis E, Li D, Yuan Y et al (2018) Functional versus chronological age: geriatric assessments to guide decision making in older patients with cancer. Lancet Oncol 19:e305–e316
Sugawara K, Yamashita H, Okumura Y et al (2020) Age-dependent survival impact of body mass index in patients with oesophageal squamous cell carcinoma. Eur J Surg Oncol 46:1948–1955
Sugawara K, Yamashita H, Yajima S et al (2020) Preoperative restrictive pulmonary dysfunction influences the survival after gastrectomy for elderly patients with gastric carcinoma. Surg Today 50:1065–1073
Montroni I, Saur NM, Shahrokni A et al (2021) Surgical considerations for older adults with cancer: a multidimensional, multiphase pathway to improve care. J Clin Oncol 39:2090–2101
Wildiers H, Heeren P, Puts M et al (2014) International society of geriatric oncology consensus on geriatric assessment in older patients with cancer. J Clin Oncol 32:2595–2603
Uhlenhopp DJ, Then EO, Sunkara T et al (2020) Epidemiology of esophageal cancer: update in global trends, etiology and risk factors. Clin J Gastroenterol 13:1010–1021
Smyth EC, Lagergren J, Fitzgerald RC et al (2017) Oesophageal cancer. Nat Rev Dis Primers 3:17048
Kuppusamy MK, Low DE (2022) Evaluation of international contemporary operative outcomes and management trends associated with esophagectomy: a 4-year study of >6000 patients using ECCG definitions and the online esodata database. Ann Surg 275:515–525
Hamamoto Y, Murakami K, Kato K et al (2022) Management of elderly patients with esophageal squamous cell cancer. Jpn J Clin Oncol 52:816–824
Murakami K, Akutsu Y, Miyata H et al (2023) Essential risk factors for operative mortality in elderly esophageal cancer patients registered in the national clinical database of Japan. Esophagus Off J Jpn Esophageal Soc 20:39–47
Lagergren J, Bottai M, Santoni G (2021) Patient age and survival after surgery for esophageal cancer. Ann Surg Oncol 28:159–166
Miyata H, Yamasaki M, Makino T et al (2015) Clinical outcome of esophagectomy in elderly patients with and without neoadjuvant therapy for thoracic esophageal cancer. Ann Surg Oncol 22(Suppl 3):S794-801
Motoyama S, Maeda E, Iijima K et al (2020) Does esophagectomy provide a survival advantage to patients aged 80 years or older? analyzing 5,066 patients in the national database of hospital-based cancer registries in Japan. Ann Surg 276:16–23
Scarpa M, Filip B, Cavallin F et al (2016) Esophagectomy in elderly patients: which is the best prognostic score? Dis Esophagus 29:589–597
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Brierley JGMKWC, TNM classification of malignant tumours, 8th Edition (2017)
Sugawara K, Yagi K, Okumura Y et al (2022) Survival prediction capabilities of preoperative inflammatory and nutritional status in esophageal squamous cell carcinoma patients. World J Surg 46:639–647
Sugawara K, Mori K, Yagi K et al (2019) Association of preoperative inflammation-based prognostic score with survival in patients undergoing salvage esophagectomy. Dis Esophagus 32:66
Sugawara K, Mori K, Okumura Y et al (2020) Preoperative low vital capacity influences survival after esophagectomy for patients with esophageal carcinoma. World J Surg 44:2305–2313
Kitagawa Y, Uno T, Oyama T et al (2019) Esophageal cancer practice guidelines 2017 edited by the Japan esophageal society: part 1. Esophagus Off J Jpn Esophageal Soc 16:1–24
Ando N, Kato H, Igaki H et al (2012) A randomized trial comparing postoperative adjuvant chemotherapy with cisplatin and 5-fluorouracil versus preoperative chemotherapy for localized advanced squamous cell carcinoma of the thoracic esophagus (JCOG9907). Ann Surg Oncol 19:68–74
Hara H, Tahara M, Daiko H et al (2013) Phase II feasibility study of preoperative chemotherapy with docetaxel, cisplatin, and fluorouracil for esophageal squamous cell carcinoma. Cancer Sci 104:1455–1460
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Tapias LF, Muniappan A, Wright CD et al (2013) Short and long-term outcomes after esophagectomy for cancer in elderly patients. Ann Thorac Surg 95:1741–1748
Morito A, Harada K, Iwatsuki M et al (2023) Frailty assessed by the clinical frailty scale is associated with prognosis after esophagectomy. Ann Surg Oncol 30:3725–3732
Ichikawa H, Kosugi SI, Kanda T et al (2016) Surgical and long-term outcomes following oesophagectomy in oesophageal cancer patients with comorbidity. Int J Surg 36:212–218
Cho H, Mariotto AB, Mann BS et al (2013) Assessing non-cancer-related health status of US cancer patients: other-cause survival and comorbidity prevalence. Am J Epidemiol 178:339–349
Jeon YK, Shin MJ, Kim MH et al (2015) Low pulmonary function is related with a high risk of sarcopenia in community-dwelling older adults: the Korea national health and nutrition examination survey (KNHANES) 2008–2011. Osteoporos Int 26:2423–2429
Burney PG, Hooper R (2011) Forced vital capacity, airway obstruction and survival in a general population sample from the USA. Thorax 66:49–54
Hong ZN, Weng K, Chen Z et al (2022) Difference between “lung age” and real age as a novel predictor of postoperative complications, long-term survival for patients with esophageal cancer after minimally invasive esophagectomy. Front Surg 9:794553
Dos Santos NLO, Pegorari MS, Silva CFR et al (2023) Pulmonary function as a predictor of frailty syndrome in community-dwelling older adults. J Geriatr Phys Ther 46:64–70
Yamashita K, Watanabe M, Mine S et al (2018) The impact of the Charlson comorbidity index on the prognosis of esophageal cancer patients who underwent esophagectomy with curative intent. Surg Today 48:632–639
Backemar L, Lagergren P, Johar A et al (2015) Impact of co-morbidity on mortality after oesophageal cancer surgery. Br J Surg 102:1097–1105
Kozuki R, Watanabe M, Toihata T et al (2022) Treatment strategies and outcomes for elderly patients with locally advanced squamous cell carcinoma of the esophagus. Surg Today 52:377–384
Matsuda S, Kitagawa Y, Okui J et al (2023) Old age and intense chemotherapy exacerbate negative prognostic impact of postoperative complication on survival in patients with esophageal cancer who received neoadjuvant therapy: a nationwide study from 85 Japanese esophageal centers. Esophagus Off J Jpn Esophageal Soc 20:445–454
Jensen GL, Hammonds KP, Haque W (2023) Neoadjuvant versus definitive chemoradiation in locally advanced esophageal cancer for patients of advanced age or significant comorbidities. Dis Esophagus 36(2):50
Nakajo K, Abe S, Oda I et al (2019) Impact of the charlson comorbidity index on the treatment strategy and survival in elderly patients after non-curative endoscopic submucosal dissection for esophageal squamous cell carcinoma: a multicenter retrospective study. J Gastroenterol 54:871–880
Faiz Z, van Putten M, Verhoeven RHA et al (2019) Impact of age and comorbidity on choice and outcome of two different treatment options for patients with potentially curable esophageal cancer. Ann Surg Oncol 26:986–995
Jingu K, Takahashi N, Umezawa R et al (2022) The benefit of concurrent chemotherapy with radiotherapy for esophageal cancer is limited in Asian patients aged 80 years or older: a seer database analysis. Esophagus Off J Jpn Esophageal Soc 19:653–659
Celi A, Latorre M, Paggiaro P et al (2021) Chronic obstructive pulmonary disease: moving from symptom relief to mortality reduction. Ther Adv Chronic Dis 14:20406223211014028
van Vulpen JK, Hiensch AE, van Hillegersberg R et al (2021) Supervised exercise after oesophageal cancer surgery: the perfect multicentre randomized clinical trial. Br J Surg 108:786–796
Chang YL, Tsai YF, Hsu CL et al (2020) The effectiveness of a nurse-led exercise and health education informatics program on exercise capacity and quality of life among cancer survivors after esophagectomy: a randomized controlled trial. Int J Nurs Stud 101:103418
Minnella EM, Awasthi R, Loiselle SE et al (2018) Effect of exercise and nutrition prehabilitation on functional capacity in esophagogastric cancer surgery: a randomized clinical trial. JAMA Surg 153:1081–1089
Yoshida N, Harada K, Iwatsuki M et al (2020) Precautions for avoiding pulmonary morbidity after esophagectomy. Ann Gastroenterol Surg 4:480–484
Sugawara K, Yoshimura S, Yagi K et al (2019) Long-term health-related quality of life following robot-assisted radical transmediastinal esophagectomy. Surg Endosc 34:1602–1611
Tsunoda S, Obama K, Hisamori S et al (2021) Lower incidence of postoperative pulmonary complications following robot-assisted minimally invasive esophagectomy for esophageal cancer: propensity score-matched comparison to conventional minimally invasive esophagectomy. Ann Surg Oncol 28:639–647
Ohi M, Toiyama Y, Omura Y et al (2019) Risk factors and measures of pulmonary complications after thoracoscopic esophagectomy for esophageal cancer. Surg Today 49:176–186
Funding
This research received no specific grants from any funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
The contributions of the authors to this study are as follows: K.S. and T.F. are the authors mainly responsible for the study’s conception and design, acquisition of data, and analysis and interpretation of data. H.H., T.Y. and D.O. contributed mainly to the drafting of the article and to revising it critically for important intellectual content. All authors have no conflicts of interest or financial ties to disclose.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Ethical approval
All procedures were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions.
Informed consent
Informed consent was obtained from all individual participants in the form of opt-out on the website. Those who rejected participation were excluded.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
268_2023_7195_MOESM1_ESM.tiff
Supplementary Figure 1. Causes of death according to age elderly patients had a significantly higher death rate due to pulmonary diseases than non-elderly patients (9.5% vs. 3.7%, P<0.01). (Tiff 7274 kb)
268_2023_7195_MOESM2_ESM.tiff
Supplementary Figure 2. Causes of death according to the number of risk factors in elderly patients deaths due to pulmonary disease rose significantly as the number of risk factors increased. (Tiff 7274 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sugawara, K., Oka, D., Hara, H. et al. Survival Impacts of Impaired Lung Functions and Comorbidities on Elderly Esophageal Cancer Patients. World J Surg 47, 3229–3239 (2023). https://doi.org/10.1007/s00268-023-07195-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-07195-y