Abstract
Background
Inverted nipple deformity presents an unsatisfactory appearance that may induce an unpleasant sex life, but can also be associated with psychological discomfort and increased the functional problems, such as local irritation and inflammation.
Methods
Multiple techniques have been used to correct inverted nipples, but they mostly lead to different problems such as deficiency of the nerve or duct, recurrence of the inverted nipple, and hypopigmented scars in the areola. To minimize complications and maintain the stability of the reconstructed nipple, we presented a minimal incision technique that designed four 3-mm-sized horizontal microincisions, which ran a sun-cross through the periphery and the core of the nipple to push the nipple together, then a vertical suture ran longitudinal to close the transverse incision to stabilize the projection.
Results
This technique was performed in 71 patients classified as grade II or III of the inverted nipples, comprising 53 congenital cases and 18 patients with acquired deformity. Thirty-four patients had bilateral inverted nipples, and 37 patients had unilateral inverted nipple. During a mean follow-up period of 15 months, 70 corrected nipples remained raised without recurrence, and one nipple was found retracted at the outpatient clinic after 3 months. There were no serious complications associated with surgery regarding nipple necrosis, seven patients got temporary swelling, two patients got infected after touching water, three patients got extravasated blood, eight patients indicated that they touched scar under the nipple, and two patients reflected nipple dysesthesia. In the 15 months follow-up, the patients with Grade II nipple inversion maintained a nipple average height of 9.54 ± 0.95, and the patients with Grade III nipple inversion maintained a nipple average height of 9.19 ± 1.09, and 86.63% of patients were satisfied with their results.
Conclusion
This is a simple, safe, effective and reliable technique that should be considered, providing sustained results over the long-term follow-up period with a high rate of stable eversion and low incidence of ischemia, necrosis, scarring and dysesthesia. The vertical scar of the transverse incision closure leads to an esthetic appearance without apparent scarring and minimizes the risk of an altered nipple sensation.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inverted nipple deformity is a condition in which the nipple is below the areola plane, which can be a result of congenital or acquired by infection, trauma, or surgery [1], it was first described in the early year of 1840, and corrective operation reported in 1879 [2]. Inverted nipples are classified into three grades with the severity of inversion by Han Hong [3]. According to the report, most of the inverted nipples contributed to congenital reasons, with remarkable fibrosis and short lactiferous ducts and severely retracted [4], and the prevalence of congenital inversion in women is approximately 3.26% [5]. It has been estimated that up to 10% of women are affected by this deformity in psychological and emotional [6], the inverted nipples not only present an unsatisfactory appearance that can be associated with unpleasant sex life, but also can induce breastfeeding problems, and increase the incidence of lactation mastitis [7, 8], due to chronic inflammation [9]. Therefore, timely and effective interventions are crucial to the prognosis of these patients.
Although many different surgical techniques to correct inverted nipples have been described, such as dermal and dermoglandular flaps, endoscopic release, internal suture, continuous traction, and artificial dermis, suggesting that no technique is totally successful [10,11,12,13], it is impossible to preserve all ducts and nerves, and the blood supply may be interrupted [14]. The diversity of procedures shows the lack of a technique that maintains the function of lactiferous ducts and preserves the function and sensation of the nipple [15].
In this study, we explore a novel, simple, safe and effective technique to correct severe nipple inversion, and double sutures were running through the periphery and core of the nipple. A longitudinal suture was used to close the transverse incision and support the nipple.
Patients and Methods
Patients
Patients with congenital or acquired grade II and grade III inverted nipples with or without different correction methods in other hospitals were included in this retrospective study from Sep 2019 to Aug 2022. All patients were female, 37 of them had unilateral inversion, and 34 patients had bilateral inversion. The nipple of 53 patients were inverted congenitally and 18 patients were acquired after lactiferous inflammation or breast hyperplasia, 105 nipples of 71 patients underwent corrective surgery. All patients attended routine follow-up visits approximately 3–15 months postoperatively. The height and the complications of the nipple were evaluated. This study was approved by the Ethics Committee of the Sixth Affiliated Hospital of Sun Yat-Sen University. Written consent was obtained from all patients.
Sun-Cross Running Suture Technique
The technique is designed to reduce surgical damage to the lactiferous ducts, while providing a relatively easy and feasible method to correct nipple inversion. As the suture came into and out of the dermis through the microincision, a double track sun-cross running suture was made: The first sun track was running in the direction of 6–12–9–6–3–12–6 o’clock, and the second sun track was running in the direction of 3–9–6–3–12–9–3 o’clock (Fig. 1a, b). Before the operation, all patients were informed of the technique and detailed steps. The grade of inversion and the diameter of the areola were measured. Questionnaires were used to investigate patients’ age, menopausal status, reproductive status, and breastfeeding needs, and to understand patients’ wishes and target effects. Preoperative anteroposterior and double oblique photos were taken before the operation.
Four 3-mm microincisions are made at 3, 6, 9, and 12 o’clock position. a, b Two 4-0 PDS suture walk through the base of the nipple in order by serial number, the first sun track was running in a direction of 6–12–9–6–3–12–6 o’clock; the second sun track was running in a direction of 3–9–6–3–12–9–3 o’clock. c, d Vertical closure of transverse incision
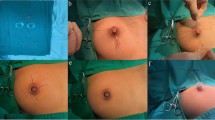
The surgery was performed with the patient under local anesthesia using 1% lidocaine with 1:200,000 adrenaline. The nipple was then temporarily lifted up with a 4-0 PROLENE suture (Fig. 2a), and the loose tissue under the nipple was released, and the new base of the nipple was marked according to the diameter of the areola and the desired height of the nipple (Fig. 2b). The micro-knife (no.11 blade) was used to make a 3-mm incision in the 3, 6, 9, and 12 o’clock position around the base of the nipple; the incisions are made 1–2 mm beyond the nipple–areolar transition point to lower the risk of devascularization [16]. PDS sutures were used around the circumference of the nipple base in the internal wall of the cylinder of the nipple; a double track sun-cross running suture was made (Fig. 2c). The sutures were tied, and the knots were placed within the interior of the nipple cylinder at the 6 and 9 o’clock positions (Fig. 2d). The transverse incisions were closed, tissue glue was used to cover the incisions and maintain the eversion of the nipple (Fig. 2e, f), and the height and width of the nipple were measured afterward.
Surgical procedure diagram. a The nipple was temporarily lifted up with 4-0 PROLENE suture and the loose tissue under the nipple was released, the new base of the nipple was marked according to the diameter of the areola and the desired height of the nipple. b Four length of 3-mm microincision was made which located on 3 o’clock, 6 o’clock, 9 o’clock, and 12 o’clock around the base of nipple. c Sun-cross running suture. d The running sutures are tied under the skin. e The transverse incisions are closed in longitudinal. f Postoperative effect
Transverse to Vertical Skin Closure
Four 3 mm length of transverse incisions were made that were located at 3 o’clock, 6 o’clock, 9 o’clock, and 12 o’clock around the base of nipple; each incision site was closed a 5-0 Monosyn Synthetic absorbable surgical suture, and the transverse incision was stitched in the longitudinal direction, converting the horizontal cut into a vertical scar, thus providing additional support to the corrected nipple (Fig. 1c, d).
Measurements
During the first week, the suture was carefully monitored, and the patient could not shower. The diameter of the areola and width and height of the nipple were measured immediately after surgery and at 3, 9 and 15 months postoperatively. The operation time, blood loss, incision size, length of hospital stays, and operation costs were counted. Three months after the operation, questionnaires were given to evaluate patient satisfaction, quality of life, sensory and erection of the nipple.
Statistical Analysis
SPSS software (version 22.0; SPSS Inc., Chicago, IL, USA) was used for the data analysis. Normally distributed data are represented as mean ± standard deviation, and the Kruskal–Wallis test was used to compare categorical data. The data were evaluated with a 95% confidence interval and 5% significance level. Statistically significance was set at p < 0.05.
Results
Clinical Demographics
A total of 71 patients with nipple inversion underwent surgery between Sep 2019 and Aug 2022, the age of the patients at the time of the operation ranged from 21 to 66 years (mean age 36.40 ± 10.15), we identified 35 patients with Grade II nipple inversion and 36 patients with Grade III nipple inversion, 87.3% of them were premenopausal, 52.1% of the nipples were unilateral, 74.6% of the inverted nipple were congenital, and the operation duration in Grade III nipple inversion was 21.75 ± 7.90 min which was longer than 19.46 ± 7.19 min in Grade II nipple inversion (shown in Table 1).
The Nipple Height Form and Recurrence
In the 15 months follow-up, the patient with Grade II nipple inversion kept the nipple height of 9.54 ± 0.95 and the patient with Grade III nipple inversion kept the nipple height of 9.19 ± 1.09, and 86.63% of patients were satisfied with their results. Grade II and III nipples achieved an increase in height postoperatively. There is one recurrence in grade II nipple inversion at 3 months postoperative follow-up. However, the shape and length had improved significantly compared to the preoperative appearance, the nipple could easily be pulled out manually and could maintain its projection without traction, and the nipple had been converted from grade II to grade I (shown in Table 2, Fig 3).
Complications
No serious complications after occurred postoperatively. No necrosis was observed after the surgery. Seven patients developed wild swelling and three patients had extravasated blood because the sutures were pulled too tight and recovered after appropriate treatment; two patients were got infected with the touched water after discharge. Nipple sensation persisted in 97.2% patients. After 15 months of follow-up, there was one patient had recurrence of inversion nipple. Eight patients reflected that they touched scar under the nipple after operation (shown in Table 3).
Questionnaire Results
Of the patients who underwent sun-cross running suture combined with transverse to longitudinal skin closure technique to correct severe inverted nipple, 86.63% were satisfied with their results. (Fig. 4, 5, and 6 show the preoperative and postoperative views.) The satisfaction rates of nipple shape and sensory function were 84.5% and 87.3%, wound scar satisfaction rate was 85.9%, and confidence of breasts after operation rate was 88.7% (shown in Table 4).
Discussion
The results obtained from our study demonstrated that the proposed technique is safe and effective. The nipple height gains can be accepted as adequate based on the satisfaction of included patients, the postoperative mean measurements of the nipple were between 7.0 and 11.0 mm, the average height of Grade II inverted nipple at 9 month and 15 months was 9.48 ± 1.09 and 9.54 ± 0.95, and the average height of Grade III inverted nipple at 9 month and 15 months was 9.50 ± 1.00 and 9.19 ± 1.09, respectively. These data show that all grades of inverted nipples were corrected efficiently.
An inverted nipple is a frequent pathologic condition in which the entire nipple, or a portion of it, is buried inward toward the lactiferous duct and lies below the plane of the areola [17], which is always accompanied by insufficient soft tissue, resulting in both psychological and functional problems. The first surgery to correct the inversion of the nipple was reported in 1889 by Axford [18]. Since then, various typical surgical approaches have described different methods of reconstructed dermo flaps [19, 20], purse-string suture techniques [21, 22], and the unique telescope technique in which a circumferential incision is made, the nipple is pulled, and the base is tightened [23]. However, many complications have been reported including visible and undesirable hypopigmented scars in the areola, removal of a portion of the nerve or duct [24], the use of the purse-string suture interrupted the blood supply of the nipple, sometimes causing ischemia [25]. In this modified technique, the sun-cross running suture involved two cross sutures through the periphery and core of the nipple that the configuration of the suture line runs in counterclockwise direction; the PDS suture line advances the nipple from the outside in and encircles the areolar tissue together instead of skin excision. There was no serious complication after the operation, 13 patients got mild complications which recovered quickly after appropriate treatment, two patients got infected cause the inappropriate home care, and nipple sensation persisted in 97.2% patients. Our technique combined a sun-crossing running suture with the longitudinal seam of the transverse incision, in which the transverse incisions were closed longitudinally. The PDS suture run through the core serves as a buttress, block any inverting forces acting on the nipple and support the projection of the nipple, the corrected nipple is supported by an internal sun-cross running suture, and the absorption of suture is by simple hydrolysis within 180 days. The transverse incision is closed longitudinally with the 5-0 Monosyn Synthetic absorbable surgical suture which is absorbed in 60 days and recruits surrounding the areolar skin to increase the projection of the nipple. The vertical closure of the areola tightened the base of the nipple without the use of a purse-string suture, provided stable results with minimal complications.
Double-track sun-cross running suture has been described as a suture ran a single circle around the nipple, and the suture line crossed the nipple and four quarter; then, surgeon tied a knot at the end [26]. We improve this method by using two sutures cross the nipple; each suture run in a cross-shaped and semicircle of the nipple individually (Fig. 1a, b), and the two sutures are perpendicular to each other, which minimize the circulation problem and necrosis of the nipple. The method of cross vertical mattress suturing used two loop stitches with a vertical mattress-shape to correct the inverted nipple, four sutures were used to run across to cover the most part of nipple, but lacked a circle suture to keep the esthetic effect [27]. The technique of integrated repair approach minimized the damage of lactiferous ducts, but the used of internal sutures to put the opposite nipple wall together may increase the risk of necrosis, and the big incision may affect esthetics result [28]. The research of double triangle suture technique avoided the milk duct and reduced the number of incisions, but the lack of cross-fixation increased the possibility of inversion recurrence [29]. By combining the strength of the sun-cross running suture and the transverse-to-longitudinal skin closure technique, we improved the stability of the nipple and minimized trauma to preserve the lactiferous ducts and nerve system as much as possible. The questionnaire survey showed 86.63% of patients were satisfied with the operation results. The combined efforts of the periphery and core sutures prevent recurrence of nipple inversion; the transverse-to-longitudinal skin closure technique recruits the areolar skin and stiffens the base of the nipple to provide additional support. Therefore, this technique is a novel concept that is different from the conventional suture technique and produces consistent results. With the described technique, the goals of inverted nipple reconstruction have been achieved, and the risk of ischemia postoperatively is considered to distinguish this method from purse-string suture.
Conclusion
We described a minimally invasive procedure consisting of a small incision followed by a sun-crossing suture and longitudinal closure of the transverse incision. Scars are minimal, provide a good nipple shape, and minimize the risk of recurrence, and cosmetic expectations are achieved. It is a simple, safe, and inexpensive technique that should be considered a reliable method for long-term correction of nipple inversion.
Data Availability
All data generated or analyzed during this study are included in this article. Further inquiries can be directed to the corresponding author.
References
Durgun M, Ozakpinar HR, Selcuk CT, Sarici M, Ceran C, Seven E (2014) Inverted nipple correction with dermal flaps and traction. Aesthet Plast Surg 38(3):533–539
Jeong HS, Lee HK (2015) Correction of inverted nipple using subcutaneous turn-over flaps to create a tent suspension-like effect. PLoS ONE 10(7):e0133588
Han S, Hong YG (1999) The inverted nipple: its grading and surgical correction. Plast reconstr Surg 104(2):389–395
Kim DY, Jeong EC, Eo SR, Kim KS, Lee SY, Cho BH (2003) Correction of inverted nipple: an alternative method using two triangular areolar dermal flaps. Ann Plast Surg 51(6):636–640
Park HS, Yoon CH, Kim HJ (1999) The prevalence of congenital inverted nipple. Aesthetic Plast Surg 23:144–146
Kolker AR, Torina PJ (2009) Minimally invasive correction of inverted nipples: a safe and simple technique for reliable, sustainable projection. Ann Plast Surg 62(5):549–553
Hwang K, Kim DH (2013) Half Z-plasty, band release, and cavity filling for correction of inverted nipple. J Plast Surg Hand Surg 47(2):93–96
Teng L, Wu GP, Sun XM, Lu JJ, Ding B, Ren M et al (2005) Correction of inverted nipple: an alternative method using continuous elastic outside distraction. Ann Plast Surg 54(2):120–123
Hwang K, Kim DH (2013) Half Z-plasty, band release, and cavity filling for correction of inverted nipple. J Plast Surg Hand Surg 47:93–96
Sapountzis S, Kim JH, Minh P et al (2012) Correction of inverted nipple with “arabesque”-shape sutures. Aesthet Plast Surg 36:339–342
Chen SH, Gedebou T, Chen PH (2007) The endoscope as an adjunct to correction of nipple inversion deformity. Plast Reconstr Surg 119:1178–1182
Serra-Reom J, Fontdevila J, Monner J (2004) Correction of the inverted nipple with an internal 5-point star suture. Ann Plast Surg 53:293–296
Durgun M, Ozakpinar HR, Selçuk CT et al (2014) Inverted nipple correction with dermal flaps and traction. Aesthet Plast Surg 38:533–539
Ma N, Fu S, Luan J (2022) A two-step technique for correction of severe inverted nipples with minimally invasive procedures. Aesthet Plast Surg 46(6):2735–2741. https://doi.org/10.1007/s00266-022-02925-4
Mathur B, Loh CYY (2019) Sensation-sparing correction of inverted nipples using the “drawbridge” flap approach. Aesthet Plast Surg 43:348–353
Cabalag MS, Chui CH, Tan BK (2010) Correction of nipple inversion using a micro-knife and transverse to longitudinal skin closure. J Plast Reconstr Aesthet Surg 63:e627–e630
Dessena L, Dast S, Perez S, Mercut R, Herlin C, Sinna R (2018) Inverted nipple treatment and poliglecaprone spacer. Aesthet Plast Surg 42(4):958–963. https://doi.org/10.1007/s00266-018-1139-5
Axford WL (1889) Mammillaplasty. Ann Surg 9:277–279
Burm JS, Kim YW (2007) Correction of inverted nipples by strong suspension with areola-based dermal flaps. Plast Reconstr Surg 120:1483–1486
Jeong HS, Lee HK (2015) Correction of inverted nipple using subcutaneous turn-over flaps to create a tent suspension-like effect. PLoS ONE 2410:e0133588
Sapountzis S, Kim JH, Minh P et al (2012) Correction of inverted nipple with “arabesque”-shape sutures. Aesthet Plast Surg 36:339–342
Gould DJ, Nadeau MH, Macias LH et al (2015) Inverted nipple repair revisited: a 7-year experience. Aesthet Surg J 35:156–164
Yukun L, Ke G, Jiaming S (2016) Application of nipple retractor for correction of nipple inversion: a 10-year experience. Aesthet Plast Surg 40:707–715
Aysal BK, Sever C (2022) A new technique in correction of nipple inversion using dermal C flaps. Aesthet Plast Surg 46(1):101–107. https://doi.org/10.1007/s00266-021-02521-y
Sapountzis S, Kim JH, Minh P, Hwang YS, Baek RM, Heo CY (2012) Correction of inverted nipple with “arabesque”-shape sutures. Aesthet Plast Surg 36(2):339–342. https://doi.org/10.1007/s00266-011-9827-4
Jeong JH, Park I, Han J, Park JU (2018) Correction of inverted nipples with the double-track sun-cross running suture technique. J Plast Surg Hand Surg 52(2):87–93. https://doi.org/10.1080/2000656X.2017.1338184
Liang W, Zhao Z, Liu S, Gu T (2017) Cross vertical mattress suturing with basilar tightening during the correction of inverted nipple in 30 cases. Aesthet Plast Surg 41(4):782–787. https://doi.org/10.1007/s00266-017-0856-5
Stevens WG, Fellows DR, Vath SD, Stoker DA (2004) An integrated approach to the repair of inverted nipples. Aesthet Surg J 24(3):211–215. https://doi.org/10.1016/j.asj.2004.03.003
Byun IH, Koo HK, Kim SJ, Kim HJ, Lee SW (2022) Double triangle suture technique for inverted nipple correction while preserving the lactiferous ducts. J Cutan Aesthet Surg 15(4):371–374. https://doi.org/10.4103/JCAS.JCAS_85_21
Funding
This study was supported by the Natural Science Foundation of Guangdong Province, 2020A1515010424, 2022 Beijing Health Promotion Association-support of the China Breast Surgery Young Physician Research Project, CJBSRAF-2022, and the Sixth Affiliated Hospital of Sun Yat-Sen University Clinical Research - 1010 Program: 1010PY (2020)-65.
Author information
Authors and Affiliations
Contributions
QW contributed to the conception of the study. XZ contributed to the acquisition of clinical pictures. HL contributed to the conception and design of the study. All authors contributed to the drafting of the manuscript, critical reversion, and approval of the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
Written informed consent was obtained from the patient for the publication of this case report and any accompanying images. This study protocol was reviewed and approved by the Ethics Committee of the Sixth Affiliated Hospital of Sun Yat-Sen University, approval number 2021ZSLYEC-406. Supported by National Key Clinical Discipline.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Q., Zhong, X., Yang, Q. et al. Sun-Cross Running Suture Combined with Transverse to Longitudinal Skin Closure to Correct Severe Inverted Nipple. Aesth Plast Surg 48, 2842–2850 (2024). https://doi.org/10.1007/s00266-023-03767-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03767-4