Abstract
Background
Breast hypoplasia or amastia with pectoralis major muscle defect in female Poland syndrome patients always necessitates surgical intervention. This study aims to introduce an efficient endoscopic technique to perform breast reconstruction in Poland syndrome patients with a latissimus dorsi myo flap and an implant using a single transverse axillary incision (ELDM + IMPLANT) and to evaluate its safety and effectiveness.
Methods
A prospective study was designed to recruit Poland syndrome candidates for ELDM + IMPLANT breast reconstruction. Only one transaxillary incision was made to harvest the LDM flap and create the anterior chest wall pocket. The LDM flap was transposed to the front to reconstruct the breast with a silicone implant. Patient demographics, LDM area, implant size, contralateral symmetry surgery, operative time and post-operative complications were collected. The BREAST-Q reconstruction module was used to evaluate patient quality of life. The disabilities of the arm, shoulder and hand (DASH) outcome questionnaire was used to evaluate patient upper extremity disabilities.
Results
Sixteen eligible patients were recruited and received ELDM + IMPLANT-BR. Mean endoscopic time for LDM flap harvesting was 61.6 min. All of the 16 patients recovered uneventfully without any significant complications. The post-operative scores of satisfaction with breast and psychosocial well-being were significantly higher than the pre-operative ones. The score of DASH was 7.1 pre-operatively and 8.3 post-operatively with no significant difference either. The score of satisfaction with outcome was 80.0.
Conclusions
Our proposed ELDM + IMPLANT technique provides a safe and efficient way to reconstruct breasts in Poland syndrome patients with a high satisfaction rate, optimized aesthetic outcome and minimized donor site morbidity.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these evidence-based medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Poland syndrome is a rare, predominantly unilateral, congenital chest deformity with a pectoralis major muscle defect as the pathognomonic manifestation. The incidence of this anomaly ranges from 1 in 7000 to 1 in 100,000 [1]. In female patients, ipsilateral breast hypoplasia or amastia always exists. The goal of the surgical treatment for female patients is to reconstruct the missing pectoralis muscle and the breast mound. Latissimus dorsi muscle flap (LDM) transfer is the most commonly used procedure to reconstruct the pectoralis muscle defect as it can be regarded as the mirrored counterpart of the pectoralis major muscle [2,3,4,5]. However, the conventional LDM harvesting technique leaves a long unsightly scar on the back, which compromises the aesthetic outcome and patient satisfaction. In the 1990s, endoscopes started to be used to harvest a LDM flap for various reconstruction purposes via short incisions [6,7,8,9,10]. However, the initial reports showed that 3–5 h was required to harvest a LDM flap using an endoscope, which significantly hindered the spread of this technique. In the following 20 years, various endeavors have been tried to improve the efficiency and safety of this technique, including using retractors [7, 11,12,13,14,15] or external skin sutures [16] or insufflation [17,18,19] to provide better optical space, and using electrothermal vessel sealer to secure hemostasis [13]. Nevertheless, the mean flap harvest time was still around 2–4 h [12, 13, 17, 18, 20]. Even the latest da Vinci surgical robot required 2.5 h [21, 22]. Moreover, multiple incisions on the back or lateral thoracic wall were required for the surgery, which compromised the advantage of the endoscopic technique to reduce scarring. The aim of this study was to introduce an efficient endoscopic technique to perform breast reconstruction in Poland syndrome patients with a latissimus dorsi myo flap and implant using a single transverse axillary incision and to evaluate its safety and effectiveness.
Patients and Methods
A prospective study was designed to recruit Poland syndrome candidates for latissimus dorsi myo flap (LDM) plus implant breast reconstruction in the Department of Aesthetic and Reconstructive Breast Surgery, Plastic Surgery Hospital, Peking Union Medical College, Chinese Academy of Medical Sciences, from January 2012 to October 2017. The inclusion criteria were defined as: (1) female ≥ 18 years old; (2) Poland syndrome diagnosed by congenital total or partial deficiency of the unilateral pectoralis major muscle with ipsilateral amastia or breast hypoplasia; (3) existence of thoracodorsal vessels confirmed by duplex ultrasonography or enhanced CT angiography; (4) good function of ipsilateral latissimus dorsi muscle. The exclusion criteria were defined as: (1) previous surgery on the affected chest wall; (2) severe chest wall deformity with rib defect; (3) other contraindications for latissimus dorsi myocutaneous flap or implant surgery. The included patients received breast reconstruction, performed by the senior authors Dr. Chunjun Liu and Dr. Jie Luan, with an endoscopically harvested LDM and implant using a single transverse axillary incision (ELDM + IMPLANT-BR).
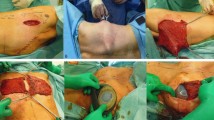
ELDM + IMPLANT-BR operative technique (see Video, Supplemental Digital Content 1) Pre-operative marking was undertaken as shown in Fig. 1 with the patient standing upright. The patient was set in a lateral decubitus position, and the surgery was performed under general anesthesia. A 5-cm incision was made along the transverse axillary crease. Thoracodorsal vessels were identified before flap elevation. Subcutaneous dissection was carried out first. A customized retractor (Fig. 2), held by the assistant, was introduced through the axillary incision, not only to provide an optical cavity but also to stretch the skin or muscle to facilitate dissection. The retractor was hooked up to a vacuum suction and had tiny holes in the tip, so it could suck out the cautery smoke and heat. A short-size retractor was used for proximal dissection, while a long-size retractor was used for distal dissection. The operator used his non-dominant hand to hold the 30 degree endoscope, which could move freely to provide the best visual field, and used the dominant hand to hold a long electrosurgical pencil to do the dissection (Fig. 3). The monopolar electrosurgical pencil had a flat tip which was useful to coagulate perforator vessels coming from underlying muscles effectively in most cases. Bipolar forceps were seldom needed for vessel coagulation. The dissection extended 1 cm beyond the lateral, caudal and medial marks, which was very helpful to detach the distal border of the LDM in the next step. Then, the retractor was inserted under the latissimus dorsi muscle, caudal to the thoracodorsal vessel pedicle. The lateral, inferior and medial portion of the LDM flap was detached from the underlying muscle by monopolar cautery, respectively. Then, the detachment of the upper medial portion of the LDM was completed as the retractor was inserted under the LDM cranial to the thoracodorsal vessel pedicle. The electrosurgical pencil was bent to follow the curved posterior thoracic wall contour. Care was taken not to place too much tension on the vessel pedicle by the retractor. So far, the submuscular detachment was well controlled to reach the pre-operative marks exactly. With the aid of the retractor stretching the distal border of the LDM from underneath the muscle, the operator could cut off the distal border of the LDM by electrosurgical pencil easily and effectively (Fig. 4). The endoscopic operation procedure was recorded as a video supplement.
Pre-operative marking. The polygon OABCDEFG indicates the subcutaneous dissection pocket in the anterior chest wall. Based on reverse design, polygon O’A’B’C’D’F’G’ was delineated to mark the range of the LDM flap to be harvested. The harvested LDM flap O’A’B’C’D’F’G’ would be rotated to the anterior chest wall to cover the pectoralis major muscle defect OABCDFG. Left: Pre-operative marking of anterior chest wall for total deficiency of pectoralis major muscle. O: anterior axillary point; A: midpoint of clavicle; B: intersection point of clavicle and sternum; C: midpoint of BD; D: intersection point of IMF and sternum; FED: IMF; F: intersection point of anterior axillary fold and IMF; G: midpoint of OF. Middle: pre-operative marking of anterior chest wall for partial deficiency of pectoralis major muscle. O: anterior axillary point; A: midpoint of AB; B: intersection point of inferior border of remnant pectoralis major muscle and sternum; C: midpoint of BD; D: intersection point of IMF and sternum; FED: IMF; F: intersection point of anterior axillary fold and IMF; G: midpoint of OF. Right: O’: posterior axillary point; O’A’B’C’D’F’G’: corresponding points of OABCDFG
Technical key point of cutting off the distal border of LDM. The subcutaneous dissection was extended 1 cm beyond the lateral, caudal and medial marks. Then, the submuscular dissection continued. With the aid of the retractor stretching the distal border of the LDM from underneath the muscle, the operator could cut off the distal border of the LDM with an electrosurgical pencil easily and effectively
Then subcutaneous pocket dissection in the anterior chest wall was performed aided by the endoscope via the same axillary incision. Special care was taken to keep dissecting in the correct plane and prevent damaging the parietal pleura, especially in patients with rib defects. Subcutaneous bands and cords were completely released to allow effective expansion of the skin envelope. Then, the LDM was transposed to the front subcutaneous pocket based on the thoracodorsal pedicle and secured to the corresponding marking points by internal sutures (Fig. 5). The lateral border of the LDM was sutured to the inferior border of the remnant clavicular head of the pectoralis major muscle or the inferior border of the clavicle. The distal end of the LDM was sutured to the periosteum or deep fascia along the lateral border of the sternum. The medial border of the LDM was sutured to rib periosteum. A silicone implant was inserted before the upper border of the LDM was sutured to the deep fascia along the pre-axillary line. Occasionally the vessel branch to the anterior serratus muscle was transected to obtain better rotation freedom. Three closed suction drains with bulb were placed, one in the front and two in the back. The axillary incision was closed in two layers. An elastic vest was used to give adequate compression on the back as well as the front.
Patient position changing from lateral decubitus to supine was not needed except in four patients receiving contralateral symmetrical surgery. Two patients received transaxillary implant breast augmentation and the other two received fat grafting.
Post-operative care. Drains were removed when output was less than 50 ml per day. The elastic vest was worn for 4 weeks. The patient was encouraged to restore shoulder movement range gradually after 6 weeks and normal activities after 8 weeks.
Patient demographics, LDM area, implant size, contralateral symmetry surgery, operative time and post-operative complications were collected. The LDM area was defined as 1/2 length × width. Operation time included LDM harvesting time, anterior subcutaneous pocket creating time and total time. Patients were followed up 6 months after surgery. The BREAST-Q reconstruction module, a validated patient-reported outcome instrument, was used to evaluate patient quality of life and satisfaction (score 0–100, the higher score the better satisfaction and quality of life) [23]. The disabilities of the arm, shoulder and hand (DASH) outcome questionnaire was used to evaluated patient upper extremity disabilities (score 0–100, the higher score the greater disability) [24]. Both questionnaires were completed by patients pre-operatively and at 6-month follow-up. A Chi-square test or Fisher’s exact test was utilized to analyze categorical data, while a t test was utilized to analyze numerical data. Statistical Product and Service Solutions (SPSS) 16 was utilized for statistical analysis. A p value < 0.05 was regarded statistically significant. IRB approval was obtained prior to the study. Informed consent was obtained from each patient.
Results
Sixteen eligible patients were recruited and received ELDM + IMPLANT-BR (Table 1). Mean age was 21.3 years old. Mean BMI was 19.7. LDM flap dimensions ranged from 18 cm × 11 cm to 25 cm × 20 cm, with the mean area as 177.4 cm2. Mean endoscopic time for LDM flap harvesting was 61.6 min. Mean total operation time was 175.0 min for patients without contralateral symmetrical surgery and 228.9 min for patients with contralateral symmetrical surgery. The size of the implant used for breast reconstruction ranged from 180 ml to 350 ml, with the average as 242.3 ml. There was no conversion from endoscopic surgery to open surgery in any patient. The average drain time was 8.0 days. Four patients received contralateral symmetrical surgery: two implant augmentation and two fat grafting. Four patients received additional fat grafting afterward. All of the 16 patients recovered uneventfully without any significant complications. One patient had minor axillary wound dehiscence but healed after dressing changes. All of the 16 patients took the questionnaire of BREAST-Q and the DASH pre-operatively; however, 13 took the post-operative questionnaire at 6 months. Post-operative scores of satisfaction with breast score and psychosocial well-being were 61.7 and 63.7, respectively, which was significantly higher than the pre-operative score 23.1 and 47.8, respectively. (Table 2) The score of chest physical well-being was 76.8 pre-operatively and 72.8 post-operatively with no significant difference. The score of DASH was 7.1 pre-operatively and 8.3 post-operatively with no significant difference either. The score of satisfaction with outcome was 80.0. Pre-/post-operative photographs of four patients are shown in Figs. 6, 7, 8, 9 and 10.
Discussion
The innovation of the study is the technical refinements to use an endoscope to harvest the LDM flap, creating a subcutaneous pocket in the anterior chest wall, and reconstructing the breast with a LDM flap and silicone implant via only one incision as short as 5 cm in the horizontal axillary crease. Although a vertical incision is much easier to get access to the surgical field [25], a transverse incision is preferred for its better cosmetic outcome. Typically an average of 60 min was used to harvest a LDM flap as large as 177 cm2. The total operation time was less than 3 h for patients without contralateral symmetrical surgery. Four technical refinements were crucial for improving efficiency: (1) A customize-designed retractor linked with a suction vacuum could provide optical cavity, suck out heated smoke and facilitate electrocautery dissection by stretching. A well-trained assistant knew the best way to use the retractor to help the operator; (2) optimization of the operation workflow. The key philosophy was to perform the dissection by utilizing the anatomical attachments. First, the retractor was introduced through the axillary incision to retract the subcutaneous skin envelope. Because the LDM was still attached to the underlying tissue, the subcutaneous dissection was easily carried out using electrocautery. Then, the retractor was inserted under the LDM and submuscular dissection was carried out in the same way. This process was opposite from using external suture retraction [26], where submuscular dissection was done before subcutaneous dissection. Keep the lateral, inferior, medial and superior border of the LDM attached until the subcutaneous and submuscular dissection was completed. (3) The subcutaneous dissection must extend 1 cm beyond the submuscular dissection, which made it much easier to detach the distal border of LDM by using an electrocautery with the muscle stretched by the retractor from beneath the muscle. The border of the LDM was released “from lateral to inferior” and “from superior to medial.” (4) A bendable electrosurgical pencil with a flat tip was used to perform both dissection and vessel coagulation. Although endoscopic bipolar forceps were routinely prepared as backup, they have never been used. The electrosurgical pencil could be bent to follow the rib contour, which was very useful in dissecting the medial inferior portion. By using the four key refinements, our transaxillary endoscopic technique has demonstrated much more efficient than the previously reported techniques [7, 11,12,13,14, 17, 18, 20, 27]. Since harvesting the LDM is a superficial procedure beneath the skin, the advantages of using a surgical robot in a deep complex cavity do not fully show up. Compared with the high cost, long docking time and multiple ports needed on the back for the robot technique [21, 22], our proposed endoscopic technique is much more cost-effective and efficient.
The endoscopic technique is also very useful in creating the anterior chest wall subcutaneous pocket. Compared with the blind blunt dissection technique, it provided precise pocket space and effective bleeding control. Moreover, it is important to release the subcutaneous fibrous bands completely with an electrocautery so that the skin envelope can be fully expanded. As long as the subcutaneous constrictions are released, pre-expansion with a tissue expander is not necessary and one-stage implant insertion works well. However, sharp dissection with a cautery should be performed carefully, especially in cases with rib aplasia, avoiding damage of the parietal pleural.
Our study showed that all the patients had very good post-operative satisfaction, which was mainly attributed to reduced scar length and concealed scar location. Unlike other reports making the incision in the vertical posterior axillary line [9, 12, 13, 21], we put the incision along the transverse axillary fold, which could be better hidden in the axillary fossa. Compared with the traditional open technique, which usually took 40–50 min to harvest the LDM based on our experience, only an extra 10–20 min was needed for the endoscopic technique. Moreover, considering the much longer incision left by the traditional open technique would cost more time for wound closure, the endoscopic technique is competitive in efficiency. So we believe that it was absolutely worth spending the additional 10–20 min to save the patient from having a long unsightly scar on the back. However, the traditional open technique does have the merit of being able to harvest a larger flap with the posterior iliac fat tissue, as well as a skin paddle, which is helpful to provide more volume and skin coverage to the breast for female patients. Therefore, the traditional latissimus dorsi myocutaneous flap is still indicated in cases in which a skin paddle is need or the patient refuses using an implant.
Our study showed that the post-operative complications and morbidity were minimal. The seroma rate was zero, which was significantly lower than our experience with the traditional open technique, which was 15%. A recent study revealed that the seroma rate in latissimus dorsi myocutaneous flaps without lumbar fat extension (3.6%) was significantly lower than that with lumbar extension (42.6%) [28]. It indicated that the lumbar fat extension, which was usually harvested together with the latissimus dorsi myocutaneous flap to provide more volume for breast reconstruction in the traditional open technique, could be the main reason for seroma formation [29, 30]. In our 16 cases, the LDM alone without the lumbar fat extension was harvested, which explained the low seroma rate. At the 6-month follow-up, all the patients recovered completely to normal activities before surgery, such as swimming and playing basketball, which is confirmed by the measurement of the BREAST-Q Chest Physical Well-being and DASH.
The limitation of the study is discussed below. Our proposed ELDM + IMPLANT-BR operative technique requires a long learning curve to achieve efficiency and safety. Both the senior authors have performed over 200 cases of transaxillary endoscopic augmentation mammoplasty surgeries. The lack of endoscopic surgery experience might hinder the popularization of this technique. Second, this research involved only 16 cases. Research of larger volume of cases needs to be done to evaluate the safety and effectiveness of this technique in the future.
Conclusions
Our proposed surgical technique is a safe and efficient method to harvest the LDM flap to correct chest wall deformity in Poland syndrome patients with an endoscopic technique via a single axillary incision. It provides a lower complication rate, better patient satisfaction and optimized aesthetic outcome.
References
Fokin AA, Robicsek F (2002) Poland’s syndrome revisited. Ann Thorac Surg 74(6):2218–2225
Fodor PB, Khoury F (1980) Latissimus dorsi muscle flap in reconstruction of congenitally absent breast and pectoralis muscle. Ann Plast Surg 4(5):422–425
Fodor PB (1981) Latissimus dorsi flap in Poland’s syndrome. Ann Plast Surg 7(3):258
Seyfer AE, Fox JP, Hamilton CG (2010) Poland syndrome: evaluation and treatment of the chest wall in 63 patients. Plast Reconstr Surg 126(3):902–911
Yiyit N, Isitmangil T, Oksuz S (2015) Clinical analysis of 113 patients with Poland syndrome. Ann Thorac Surg 99(3):999–1004
Monticciolo DL, Ross D, Bostwick J 3rd, Eaves F, Styblo T (1996) Autologous breast reconstruction with endoscopic latissimus dorsi musculosubcutaneous flaps in patients choosing breast-conserving therapy: mammographic appearance. AJR Am J Roentgenol 167(2):385–389
Cho BC, Lee JH, Ramasastry SS, Baik BS (1997) Free latissimus dorsi muscle transfer using an endoscopic technique. Ann Plast Surg 38(6):586–593
Karp NS, Bass LS, Kasabian AK, Eidelman Y, Hausman MR (1997) Balloon assisted endoscopic harvest of the latissimus dorsi muscle. Plast Reconstr Surg 100(5):1161–1167
Van Buskirk ER, Rehnke RD, Montgomery RL, Eubanks S, Ferraro FJ, Levin LS (1997) Endoscopic harvest of the latissimus dorsi muscle using the balloon dissection technique. Plast Reconstr Surg 99(3):899–903 (discussion 4-5)
Masuoka T, Fujikawa M, Yamamoto H, Ohyama T, Inoue Y, Takao T et al (1998) Breast reconstruction after mastectomy without additional scarring: application of endoscopic latissimus dorsi muscle harvest. Ann Plast Surg 40(2):123–127
Cha W, Jeong WJ, Ahn SH (2013) Latissimus dorsi muscle free flap revisited: a novel endoscope-assisted approach. Laryngoscope 123(3):613–617
Lin CH, Wei FC, Levin LS, Chen MC (1999) Donor-site morbidity comparison between endoscopically assisted and traditional harvest of free latissimus dorsi muscle flap. Plast Reconstr Surg 104(4):1070–1077 (quiz 8)
Guven E, Basaran K, Yazar M, Ozden BC, Kuvat SV, Aydin H (2010) Electrothermal bipolar vessel sealer in endoscope-assisted latissumus dorsi flap harvesting. J Laparoendosc Adv Surg Tech Part A 20(9):735–742
Lee MA, Miteff KG (2014) The scarless latissimus dorsi flap provides effective lower pole prosthetic coverage in breast reconstruction. Plast Reconstr Surg Glob Open 2(5):e147
Yang CE, Roh TS, Yun IS, Kim YS, Lew DH (2014) Immediate partial breast reconstruction with endoscopic latissimus dorsi muscle flap harvest. Arch Plast Surg 41(5):513–519
Serra-Renom JM, Serra-Mestre JM, Martinez L, D’Andrea F (2013) Endoscopic reconstruction of partial mastectomy defects using latissimus dorsi muscle flap without causing scars on the back. Aesthet Plast Surg 37(5):941–949
Missana MC, Pomel C (2007) Endoscopic latissimus dorsi flap harvesting. Am J Surg 194(2):164–169
Iglesias M, Gonzalez-Chapa DR (2013) Endoscopic latissimus dorsi muscle flap for breast reconstruction after skin-sparing total mastectomy: report of 14 cases. Aesthet Plast Surg 37(4):719–727
Pomel C, Missana MC, Atallah D, Lasser P (2003) Endoscopic muscular latissimus dorsi flap harvesting for immediate breast reconstruction after skin sparing mastectomy. Eur J Surg Oncol J Eur Soc Surg Oncol Br Assoc Surg Oncol 29(2):127–131
Pomel C, Missana MC, Lasser P (2002) Endoscopic harvesting of the latissimus dorsi flap in breast reconstructive surgery. Feasibility study and review of the literature. Ann Chir 127(5):337–342
Selber JC, Baumann DP, Holsinger FC (2012) Robotic latissimus dorsi muscle harvest: a case series. Plast Reconstr Surg 129(6):1305–1312
Chung JH, You HJ, Kim HS, Lee BI, Park SH, Yoon ES (2015) A novel technique for robot assisted latissimus dorsi flap harvest. J Plas Reconstr Aesthet Surg JPRAS 68(7):966–972
Pusic AL, Klassen AF, Scott AM, Klok JA, Cordeiro PG, Cano SJ (2009) Development of a new patient-reported outcome measure for breast surgery: the BREAST-Q. Plast Reconstr Surg 124(2):345–353
Hudak PL, Amadio PC, Bombardier C (1996) Development of an upper extremity outcome measure: the DASH (disabilities of the arm, shoulder and hand) [corrected] The Upper Extremity Collaborative Group (UECG). Am J Ind Med 29(6):602–608
Watfa W, di Summa PG, Raffoul W (2016) Bipolar latissimus dorsi transfer through a single incision: first key-step in poland syndrome chest deformity. Plast Reconstr Surg Glob Open 4(8):e847
Fine NA, Orgill DP, Pribaz JJ (1994) Early clinical experience in endoscopic-assisted muscle flap harvest. Ann Plast Surg 33(5):465–469 (discussion 9-72)
Munoz IVJ, Rodrigues TA, Serra Payro JM, Vinals Vinals JM, Dewever M (2014) Immediate single-stage endoscopic latissimus dorsi breast and nipple reconstruction. Plast Reconstr Surg Glob Open 2(3):e122
Arikawa M, Miyamoto S, Fujiki M, Higashino T, Oshima A, Sakuraba M (2017) Comparison of donor site drainage duration and seroma rate between latissimus dorsi musculocutaneous flaps and thoracodorsal artery perforator flaps. Ann Plast Surg 79(2):183–185
di Santanelli Pompeo F, Laporta R, Sorotos M, Pagnoni M, Falesiedi F, Longo B (2014) Latissimus dorsi flap for total autologous immediate breast reconstruction without implants. Plast Reconstr Surg 134(6):871e–879e
Branford OA, Kelemen N, Hartmann CE, Holt R, Floyd D (2013) Subfascial harvest of the extended latissimus dorsi myocutaneous flap in breast reconstruction: a comparative analysis of two techniques. Plast Reconstr Surg 132(4):737–748
Acknowledgements
This study was supported by Captital’s Funds for Health Improvement and Research 2016-2-4041, PUMC Youth Fund & the Fundamental Research Funds for the Central Universities 3332015156, to Dr. Chunjun Liu, and CAMS Initiative for Innovative Medicine (CAMS-I2M) (2017-I2M-3-006) to Dr. Jie Luan.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Human and Animal Rights or Ethical Approval
The study has obtained IRB approval from the Ethical Committee of Plastic Surgery Hospital, Peking Union Medical College, Chinese Academy of Medical Sciences.
Informed Consent
Written informed consent was obtained from each patient prior to the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Dr. Chunjun Liu and Dr. Jie Luan contribute equally as co-corresponding author to this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Endoscopic video of harvesting LDM via transaxillary incision. (MP4 88408 kb)
Rights and permissions
About this article
Cite this article
Liu, C., Luan, J., Ouyang, Y. et al. Breast Reconstruction in Poland Syndrome Patients with Latissimus Dorsi Myo Flap and Implant: An Efficient Endoscopic Approach Using Single Transverse Axillary Incision. Aesth Plast Surg 43, 1186–1194 (2019). https://doi.org/10.1007/s00266-019-01346-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-019-01346-0