Abstract
Programmed cell death-1 (PD-1) and PD-1 ligand 1 (PD-L1) are target molecules for immunotherapy in non-small cell lung cancer. PD-L1 is expressed not only in cancer cells, but also on macrophages, and has been suggested to contribute to macrophage-mediated immune suppression. We examined the clinical significance of PD-L1 expression on macrophages in human lung adenocarcinoma. The mechanism of PD-L1 overexpression on macrophages was investigated by means of cell culture studies and animal studies. The results showed that high PD-L1 expression on macrophages was correlated with the presence of EGFR mutation, a lower cancer grade, and a shorter cancer-specific overall survival. In an in vitro study using lung cancer cell lines and human monocyte-derived macrophages, the conditioned medium from cancer cells was found to up-regulate PD-L1 expression on macrophages via STAT3 activation, and a cytokine array revealed that granulocyte–macrophage colony-stimulating factor (GM-CSF) was a candidate factor that induced PD-L1 expression. Culture studies using recombinant GM-CSF, neutralizing antibody, and inhibitors indicated that PD-L1 overexpression was induced via STAT3 activation by GM-CSF derived from cancer cells. In a murine Lewis lung carcinoma model, anti-GM-CSF therapy inhibited cancer development via the suppression of macrophage infiltration and the promotion of lymphocyte infiltration into cancer tissue; however, the PD-L1 expression on macrophages remained unchanged. PD-L1 overexpression on macrophages via the GM-CSF/STAT3 pathway was suggested to promote cancer progression in lung adenocarcinoma. Cancer cell-derived GM-CSF might be a promising target for anti-lung cancer therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer is one of the most common causes of cancer death, and tobacco smoking is the most well-known risk factor for lung cancer [1]. The incidence of lung cancer among never-smokers has been increasing over the past decade, and exposure to secondhand tobacco smoke, radon, and/or air pollution is considered to be a possible etiological factor [2, 3]. Although recent advances in diagnostic tools, such as computed tomography scans, have increased the detection rate of early stage lung cancer, many cases are still diagnosed at advanced stages. In addition to conventional chemotherapy/radiotherapy, immunotherapy blocking immune checkpoint molecules, such as programmed cell death protein 1 (PD-1), is now becoming one of the standard therapies for lung cancer [4].
PD-1 ligand 1 (PD-L1) expression in cancer cells is considered to be a potential predictive biomarker for anti-PD-1/PD-L1 therapy in several cancers, including lung cancer, and immunohistochemistry (IHC) using anti-PD-L1 antibodies has been performed in pathological specimens [5, 6]. Several retrospective studies have shown that PD-L1 expression in cancer cells was associated with a poor clinical course in lung adenocarcinoma, but not in lung squamous cell carcinoma and small cell carcinoma [7,8,9,10]. Although researchers have noted that PD-L1 is expressed in stromal cells in lung cancer tissues, the significance of the PD-L1 expression in stromal cells remains unclear.
It is known that myeloid cells, such as dendritic cells and macrophages, also express PD-L1 [11]. Macrophages that infiltrate cancer tissues are referred to as tumor-associated macrophages (TAMs) [12,13,14]. TAMs have protumor functions related to angiogenesis, invasion, and immunosuppression, and a high density of TAMs has been shown to be associated with a poor clinical course in many cancers, including lung cancer [15,16,17,18]. TAMs are known to express several molecules related to immune suppression, such as indoleamine 2,3-dioxygenase, interleukin (IL) 10, Siglec-15, and PD-1 ligands [19,20,21], and the immunosuppressive effect of the PD-1 ligands on TAMs has been demonstrated in a murine cancer model [22, 23]. PD-L1 expression on TAMs is correlated with the efficacy of immunotherapy in ovarian cancer and melanoma patients [24]. In the present study, we tried to accurately evaluate the expression status of PD-L1 on TAMs in pathological specimens by double IHC with anti-macrophage antibodies. The mechanisms related to PD-L1 overexpression on TAMs were also investigated in cell culture studies.
Materials and methods
Samples
Paraffin-embedded samples were prepared from specimens obtained from 231 patients diagnosed with lung adenocarcinoma between 2010 and 2013 at Kumamoto University Hospital. Two pathologists reviewed all tissue specimens, and the most representative area of a 5-mm-diameter core containing viable lung adenocarcinoma cells was carefully selected for tissue microarrays. The study design was approved by the Kumamoto University Review Board (approval #1174).
IHC
The DAKO automation system (Autostainer Link 48; DAKO, Glostrup, Denmark) was used for the immunohistochemical analysis of human PD-L1 (clone 22C3; DAKO). Anti-human CD8 antibody (clone C8/144B; Nichirei, Tokyo, Japan), anti-PU.1 antibody (clone EPR3158Y; Abcam, Cambridge, UK), and anti-Iba-1 antibody (Wako, Tokyo, Japan) were used as the primary antibodies to label the macrophages and lymphocytes in human samples. For IHC of murine tumor specimens, anti-Iba-1 antibody (Wako), anti-CD8 antibody (clone D4W2Z; Cell Signaling Technology, Danvers, MA), and anti-PD-L1 antibody (#AF1019; R&D Systems, Minneapolis, MN, USA) were used as the primary antibodies. Horseradish peroxidase (HRP)-labeled anti-rabbit immunoglobulin antibody (Nichirei) was used as the secondary antibody. 3,3’-Diaminobenzidine was used for the visualization of positive signals in the first step of double IHC. Subsequently, sections were treated by heating in 1 mM ethylenediaminetetraacetic acid (pH 8.0) buffer. Then, the sections were treated with HRP-labeled anti-rabbit immunoglobulin antibody, and positive signals were visualized with HistoGreen substrate (#AYS-E109; Linaris, Dossenheim, Germany) as the second step of double IHC. Two investigators (Y.K. and Y.S.), who were blinded to information about the samples, evaluated the PD-L1 and PU.1 expression. We also determined the macrophage proportion score (MPS), which is based on the tumor proportion score (TPS). Images of ten randomly selected 400 × fields were obtained under microscopy, and the image files were analyzed for cell counting and the evaluation of the stained areas by Image J software.
Cell culture of macrophages, cancer cell lines, and lymphocytes
Monocytes were isolated using RosetteSep Human Monocyte Enrichment Cocktail (STEMCELL Technologies, Vancouver, Canada). Peripheral blood mononuclear cells were obtained from three healthy voluntary donors in accordance with protocols approved by the Kumamoto University Hospital Review Board (#1169). These monocytes were plated on UpCELL 6-well plates (2 × 105 cells/well; CellSeed, Tokyo, Japan) and cultured in AIM-V medium (Thermo Fisher, Waltham, MA, USA) supplemented with 2% human serum macrophage-colony stimulating factor (M-CSF; 100 ng/mL; Wako) for 7 days to induce the differentiation of macrophages.
Three human lung adenocarcinoma cell lines (NCI-H23, H358, and H1975) were obtained from Tomoya Yamaguchi (Kumamoto University, Kumamoto, Japan). A549 and PC9 were obtained from the Japanese Collection of Research Bioresources Cell Bank (Osaka, Japan). Murine Lewis lung carcinoma (LLC) cells were kindly gifted from Keizo Takenaga (Chiba Cancer Center, Chiba, Japan). All cells were cultured in RPMI1640 (Wako) supplemented with 10% fetal bovine serum. The conditioned medium (CM) of the cell lines was collected as previously described [21]. For the cell culture study using mouse macrophages, bone marrow cells were cultured in RPMI1640 supplemented with 10% fetal bovine serum and M-CSF (100 ng/mL) for 5 days, and adherent cells were used as macrophages.
Lymphocytes, isolated from healthy donors using RosetteSep Human T-cell Enrichment Cocktail (STEMCELL Technologies), were cultured in a cell-culture plate coated with anti-human CD3 antibody (OKT3; eBiosciences, San Diego, CA, USA), human CD28 antibody (BioLegend, San Diego, CA, USA). The proliferation of lymphocytes was tested by BrdU incorporation assay (Cell proliferation ELISA kit, Roche, Basel, Switzerland). Anti-PD-1 antibody (clone EH12.2H7) and isotype matched IgG were obtained from BioLegend (San Diego, CA, USA).
Cell enzyme-linked immunosorbent assay (ELISA)
Macrophages were cultured in a 96-well microplate and stimulated with the CM of the adenocarcinoma cell lines for 1 day. After fixation with 1% paraformaldehyde, cells were reacted with anti-PD-L1 antibody (clone 29E.2A3; BioLegend, San Diego, CA, USA) or isotype-matched control antibody (BioLegend). After the cells were washed with phosphate-buffered saline, HRP-labeled anti-mouse immunoglobulin antibody (Nichirei) was added. Then, the plate was washed with phosphate-buffered saline, and tetramethylbenzidine developing solution (BioLegend) was used to visualize the positive signals.
Phospho-receptor tyrosine kinase (RTK) array
Phospho-RTK array analysis was performed using the Human Phospho-RTK Array Kit (ARY 001; R&D Systems) according to the manufacturer’s instructions.
Cytokine array
Cytokine array analysis was performed using the Human XL Cytokine Array Kit (ARY 022; R&D Systems) according to the manufacturer’s instructions.
ELISA for granulocyte–macrophage colony-stimulating factor (GM-CSF)
ELISA for GM-CSF was performed using the Human GM-CSF ELISA Kit (Cat. No. 432007; BioLegend) according to the manufacturer’s instructions.
Recombinant proteins, anti-cancer chemicals, and inhibitors
IL-6 and GM-CSF recombinant proteins were purchased from Wako. The following inhibitors were used at a final concentration of 10 nM: Stat1 (Fludarabine; Wako), Stat3 (WP1066; Santa Cruz, Dallas, TX, USA), Stat5 (573,108; Merck KGaA, Darmstadt, Germany), JNK (SP600125; Santa Cruz), ERK (FR180204; Santa Cruz), and JAK (Ruxolitinib; ChemScene LLC, Monmouth Junction, NJ, USA). Paclitaxel, docetaxel, carboplatin, and pemetrexed were obtained from Wako.
Western blot analysis
The macrophages were stimulated with the CM of the lung adenocarcinoma cell lines (concentration: 50%) for 10 min, 30 min, 1 h, 3 h, or 1 day. Then, the macrophages were collected, and the cellular proteins were solubilized in Tris buffer containing 2% sodium dodecyl sulfate and 10% glycerol. The amount of protein was quantified using the bicinchoninic acid assay. Equal amounts of protein were then separated by sodium dodecyl sulfate polyacrylamide gel electrophoresis and subsequently transferred to a polyvinylidene fluoride membrane. The following rabbit antibodies were used for western blotting: anti-PD-L1 antibody (clone E1L3N; Cell Signaling Technology), anti-STAT3 antibody (clone 124H6; Cell Signaling Technology), and anti-pSTAT3 antibody (clone Y705; Cell Signaling Technology).
Flow cytometry
Human monocyte-derived macrophages were treated with human FcR-blocking reagent (BioLegend) and then reacted with phycoerythrin-labeled or Alexa 488-labeled anti-human PD-L1 antibody (BioLegend) or isotype-matched control antibody (BioLegend). For analysis of murine subcutaneous tumor, anti-CD11b antibody, anti-PD-L1 antibody, and isotype-matched antibodies (BioLegend) were used. The stained cell samples were analyzed on a FACSverse (Becton Dickinson, Franklin Lake, NJ, USA) flow cytometer with FACSuite (Becton Dickinson) software.
Animal studies
C57BL/6 J mice were obtained from CLEA Japan (Shizuoka, Japan). LLC cells (5 × 105 cells/mouse) suspended in 50 µL of RPMI1640 medium were subcutaneously injected into the mice. Anti-GM-CSF antibody (clone MP1-22E9) and isotype-matched control antibody were purchased from BioXel (New Haven, CT, USA). Hamster anti-mouse PD-L1 antibody (clone 10B5; 100 mg/mice) was established previously [22], and control hamster immunoglobulin G was obtained from Sigma (St. Louis, MO, USA). All animal experiments were approved by the Ethics Committee for Animal Experiments of Kumamoto University (#A2019-176) and conducted in accordance with the guidelines of the Institutional Animal Care and Use Committee.
Statistical analysis
Statistical analysis was carried out using GraphPad Prism9 (https://www.graphpad.com/) and JMP7 (SAS Institute, Chicago, IL, USA) software. Differences were considered to be statistically significant at p < 0.05.
Results
PD-L1 overexpression on TAMs was associated with a worse cancer-specific survival (CSS)
We tried to evaluate the PD-L1 that is specifically expressed on TAMs in tumor tissues by double IHC using macrophage-specific markers and anti-PD-L1 antibody. Since PU.1 is a critical molecule involved in macrophage differentiation and is expressed in the nucleus of Iba-1 (a pan-macrophage marker)-positive cells (Fig. 1A), double IHC of PD-L1 and PU.1 was performed to accurately determine the expression on TAMs (Fig. 1B). PD-L1 expression was scored based on the percentage of positive staining, and referred to as the MPS, as follows: low, < 50% positive cells; high, ≥ 50% positive cells. Of the 231 cases, PD-L1 expression was low in 114 cases (49.4%) and high in 117 cases (50.6%). Although a high MPS was associated with female sex, the presence of epidermal growth factor receptor (EGFR) mutation, and a lower grade of cancer cells, it was not correlated with age or smoking (Table 1). The MPS did not affect the progression-free survival or CSS in the total cases (Fig. 1C, Table S1, Table S2). The cases were divided into two groups according to the cancer stage, and statistical analysis was performed. Log-rank analysis showed that among the patients with a higher stage, the CSS was significantly shorter in the high MPS group than in the low MPS group (p = 0.0409; Fig. 1C). The statistical significance was more obvious in patients without EGFR mutation (Fig. 1D). The MPS was not associated with progression-free survival, as shown in Supporting Fig. 1A. In addition, there was no significant relationship between the MPS and the number of CD8-positive T cells in cancer tissues (Supporting Fig. 1B).
Double immunohistochemistry (IHC) using anti-programmed death ligand 1 (PD-L1) and macrophage-specific markers. (A) Double IHC of Iba-1 (a pan-macrophage marker) and PU.1 (a nuclear transcription factor in macrophages) in lung tumor tissue and non-tumor tissue. Iba-1 and PU.1 signals are labeled as brown and green, respectively. (B) Representative images of double IHC from a high PD-L1 case (left side) and a low PD-L1 case (right side). PD-L1 and PU.1 signals are labeled as brown and green, respectively. (C) PD-L1 expression was divided into two groups according to the macrophage proportion score (MPS). Statistical analyses related to cancer-specific overall survival (CSS) were performed. (D) Cases were divided into two groups dependent on EGFR mutation, and statistical analyses related to cancer-specific overall survival (CSS) were performed
Cancer cell-derived factors induced PD-L1 overexpression on cultured macrophages
From the above results, PD-L1 expression on the TAMs in lung adenocarcinoma tissues was more likely to be affected by cancer cells than lymphocytes. Therefore, we hypothesized that cancer cell-derived factors influenced the PD-L1 expression on TAMs. To test this hypothesis, the CM of lung adenocarcinoma cell lines was added to human monocyte-derived macrophages, and PD-L1 expression was tested by immunocytostaining and cell ELISA. The expression intensity of PD-L1 was increased by the CM of the PC9, H23, H358, and H1975 cell lines (Fig. 2A, B). We confirmed by fluorescence-activated cell sorting that the surface expression of PD-L1 on macrophages was induced by the CM of the H358 cells and H1975 cells (Fig. 2C). Macrophages suppressed anti-CD3/CD28 antibody-induced lymphocytes proliferation, and this suppression was recovered by anti-PD-1 antibody (Fig. 2D).
PD-L1 expression on macrophages. Human monocyte-derived macrophages were stimulated with the conditioned medium (CM) of lung adenocarcinoma cell lines for 24 h, and PD-L1 expression was evaluated by immunocytochemistry (A) and cell enzyme-linked immunosorbent assay (cell-ELISA) (B). The surface expression of PD-L1 on CM-stimulated macrophages was tested by flow cytometry (C). Human lymphocytes were cultured in culture plate coated with anti-CD3/CD28 antibodies *: statistically significant (n = 3 to 4 each), p value < 0.05
PD-L1 overexpression on macrophages was dependent on Stat3 activation
The phosphorylation kinase array was then performed to elucidate the PD-L1 expression-inducing mechanism of the cancer cell-derived factors. The levels of some phosphorylation kinases were elevated; in particular, the levels of STAT3, STAT5, and c-Jun were significantly elevated (Fig. 3A, Supporting Fig. 2A). Next, we investigated which pathway contributes to PD-L1 expression by using inhibitors against these molecules. No direct inhibitor was available for c-Jun, so inhibitors of its upstream kinases, JNK and ERK, were used instead. In addition, since it has been reported that STAT1 induced PD-L1 expression in cancer cells [22], we added a STAT1 inhibitor. The results showed that PD-L1 expression was strongly suppressed by the STAT3 inhibitor and was slightly suppressed by the STAT1 inhibitor and JNK inhibitor (Fig. 3B). From Western blotting, STAT3 activation was observed in the macrophages within 30 min after CM stimulation, and the PD-L1 expression level was increased 1 h after CM stimulation (Fig. 3C). Since JAK signals are located upstream of STAT3, we additionally tested whether the JAK inhibitor suppressed PD-L1 overexpression. The results showed that the PD-L1 protein expression level was significantly suppressed by the JAK inhibitor as well as the STAT3 inhibitor (Fig. 3D). Similar results were confirmed by flow cytometry (Fig. 3E).
PD-L1 expression on macrophages and related signaling pathways. Human macrophages were stimulated with the CM of the NCI-H358 and H1975 cell lines, and the upstream signals related to PD-L1 expression on macrophages were analyzed using a phospho-receptor tyrosine kinase array. Each of the signal densities was evaluated by Image J software (A). The inhibitory effects of inhibitors on the up-regulation of PD-L1 were tested by cell-ELISA (B). Western blot analysis of PD-L1, pSTAT3, and STAT3 performed using macrophages stimulated with the conditioned medium of the NCI-H358 cell line (C). The suppressive effects of inhibitors of STAT3 and JAK signals were tested by cell-ELISA (D) and flow cytometry (E) using macrophages stimulated with the CM of the NCI-H358 cell line. The bar graph shows the mean fluorescence intensity (MFI) for PD-L1. *: statistically significant (n = 3 to 4 each), p value < 0.05
Cancer cell-derived GM-CSF induced PD-L1 expression on macrophages
Although it has been revealed that STAT3 is involved in PD-L1 expression on macrophages, the cancer cell-derived factors that induce STAT3 activation are unclear. Therefore, we used a cytokine array to try to identify the cytokines that activate the STAT3 pathway. The CM of NCI-H358 and NCI-H1975, which increased PD-L1 expression, and the CM of A549, which did not increase PD-L1 expression, were used. GM-CSF and IL-6 were identified as cytokines that were abundantly contained in the CM of NCI-H358 and NCI-H1975, and were scarce in the CM of A549 (Fig. 4A, Supporting Fig. 2B). Cell ELISA analysis (Fig. 4B) and flow cytometry (Fig. 4C) results showed that PD-L1 expression was increased by GM-CSF, but not by IL-6. No synergistic effect of IL-6 and GM-CSF was observed. Among the CM of the macrophages and cell lines, GM-CSF production was detected in the CM of PC9, NCI-H358, and NCI-H1975 (Fig. 4D). GM-CSF production was not associated with EGFR mutation. Recombinant GM-CSF induced STAT3 activation in macrophages within 30 min and PD-L1 expression after 1 day (Fig. 4E).
Cytokines produced from the cell lines. Cancer cell-derived factors that promote PD-L1 expression on macrophages were tested using a cytokine array. The signal density was evaluated by Image J software (A). Human macrophages were stimulated with IL-6 (10 ng/mL) and GM-CSF (10 ng/mL), and PD-L1 expression was measured by cell-ELISA (B) and flow cytometry (C). The concentration of GM-CSF in the CM of macrophages (three donors) and cell lines was tested by ELISA (D). Macrophages were stimulated by GM-CSF (10 ng/mL), and subsequently, STAT3 activation and PD-L1 expression were evaluated by western blot analysis (E). *: statistically significant (n = 3 to 4 each), p value < 0.05
The CM-induced PD-L1 overexpression was significantly suppressed by the STAT3 inhibitor and anti-GM-CSF antibody (Fig. 5A, B). Gene expression data from a lung adenocarcinoma cohort in The Cancer Genome Atlas (https://www.proteinatlas.org/) showed that PD-L1 expression was significantly associated with the expression of GM-CSF and IL-6, and a more significant correlation was seen between GM-CSF and PD-L1 (Fig. 5C). Next the correlation between GM-CSF and PD-L1 expression was tested using 15 adenocarcinoma cases. In situ hybridization of GM-CSF indicated GM-CSF mRNA expression in cancer cells was detected in 4 cases (27%), and not detected in stromal cells (Supporting Fig. 3). Although the association was not statistically significant, MPS score was high in all GM-CSF-positive cases while MPS score was high in 55% of GM-CSF-negative cases (Supporting Fig. 3).
Involvement of GM-CSF in PD-L1 overexpression. The inhibitory effect of the STAT3 inhibitor and anti-GM-CSF antibody (Ab) on PD-L1 overexpression was tested by flow cytometry (A). Bar graph showing the mean fluorescence intensity (MFI) for PD-L1 (B). Gene expression data (fragments per kilobase of exon model per million reads mapped) of PD-L1, GM-CSF, and IL-6 in lung adenocarcinoma were obtained from the Protein Atlas (TCGA) website, and Spearman’s correlation tests were performed to examine the correlation of the expression of each gene (C). *: statistically significant (n = 3 to 4 each), p value < 0.05
Anti-cancer compounds increased GM-CSF overexpression in cancer cells
A previous study demonstrated that chemotherapy stimulated GM-CSF production in pancreatic cancer cells, which accelerated the infiltration of immunosuppressive myeloid cells into the microenvironment [23]. Therefore, we next tested whether anti-cancer drugs induced GM-CSF overexpression in cancer cells. A549 and PC9 cells were stimulated with paclitaxel, docetaxel, carboplatin, and pemetrexed for 24 h at the same concentration (40 µM), and the mRNA expression of GM-CSF was evaluated by real-time polymerase chain reaction (Fig. 6A). Strong overexpression was induced by pemetrexed in the A549 and PC9 cells, and by carboplatin in the PC9 cells (Fig. 6B). The cells were subsequently cultured for another day, and the concentration of GM-CSF in the medium was tested by ELISA (Fig. 6A). The concentration of GM-CSF was significantly increased in the medium of the PC9 cells treated with carboplatin and pemetrexed (Fig. 6C). Although the concentration of GM-CSF was low in the medium of all of the treated A549 cells, pemetrexed induced an increase in the production of GM-CSF (Fig. 6C). PD-L1 expression on macrophages was increased by the CM of the pemetrexed-treated PC9 cells (Fig. 6D), and the PD-L1 overexpression was suppressed by anti-GM-CSF antibody (Fig. 6E).
Effect of anti-cancer compounds in cell lines. A schematic diagram of the cell cultures and methods (A). A549 and PC9 cells were cultured with dimethyl sulfoxide (DMSO), paclitaxel (PTX), docetaxel (DOC), carboplatin (CBDCA), and pemetrexed (PMET) for 24 h at the same concentration (40 µM), and the mRNA expression of GM-CSF was evaluated by real-time polymerase chain reaction (B). The cells were subsequently cultured for another day, and the concentration of GM-CSF in the medium was tested by ELISA (C). Macrophages were stimulated with the CM of control PC9 cells or PEMT-treated PC9 cells, and surface PD-L1 expression was detected by fluorescence-activated cell sorting (D). Macrophages were stimulated with the CM of PEMT-treated PC9 cells with control immunoglobulin G or anti-GM-CSF antibody (20 µg/mL) (E). *: statistically significant (n = 3 to 4 each), p value < 0.05
Blocking of GM-CSF inhibited tumor development in a mouse LLC tumor model
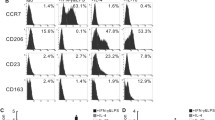
We tested whether GM-CSF influenced PD-L1 expression on mouse cells. Mouse bone marrow-derived macrophages (BMDMs) were stimulated with the CM of LLC cells, and the results of immunocytochemistry indicated that the PD-L1 expression on BMDMs was increased by the CM (Supporting Fig. 4A). LLC cells expressed GM-CSF (Supporting Fig. 4B). Flow cytometry showed that the PD-L1 on BMDMs was up-regulated by the CM, and the CM-induced overexpression was cancelled out by anti-GM-CSF antibody (Supporting Fig. 4C). We also tested whether anti-GM-CSF antibody would be effective in the LLC mouse tumor model, and the results showed that subcutaneous tumor growth was significantly inhibited by the anti-GM-CSF antibody (Fig. 7A). By means of flow cytometry, PD-L1 expression was higher in CD11b+ myeloid cells than that in CD11b− tumor cells. Double IHC of PD-L1 and Iba-1 showed that PD-L1 expression was predominantly restricted to TAMs (Fig. 7C); however, anti-GM-CSF therapy did not affect the PD-L1 expression in tumor tissues (Fig. 7D). Notably, anti-GM-CSF antibody therapy decreased the infiltration of Iba-1-positive TAMs and CD206-positive TAMs and increased the infiltration of CD8-positive T cells (Fig. 7E). The size of TAMs was also reduced by anti-GM-CSF antibody therapy (Fig. 7F).
Effect of anti-GM-CSF antibody on the mouse LLC model. The protocol of anti-GM-CSF antibody therapy. The tumor weight was evaluated and compared between the anti-GM-CSF antibody-treated group and the control antibody-treated group (A). Flow cytometry of CD11b and PD-L1 was performed using subcutaneous tumor nodule (B). Double IHC of Iba-1 (green) and PD-L1 (brown) in a LLC tumor was performed to test whether PD-L1 was expressed on tumor-associated macrophages (TAMs) (C). The PD-L1-positive area (%) was examined by Image J software (D). The infiltration of CD8-positive T cells (cells/mm2) and the area (%) with Iba-1-positive and CD206-positive TAMs were analyzed by Image J software (E). The cell size of infiltrating macrophages was evaluated by Image J software (F)
Lastly, we tested whether anti-PD-L1 antibody would affect anti-GM-CSF therapy in the LLC mouse tumor model; however, anti-PD-L1 antibody did not affect the anti-tumor effect of anti-GM-CSF therapy (Supporting Fig. 5).
Discussion
PD-L1 is highly expressed not only in cancer cells, but also in immune cells, mostly TAMs, in lung cancer tissues. A previous study reported that PD-L1 expression in tumor cells (the PD-L1 TPS) was strongly associated with the effects of anti-PD-1 therapy in non-small cell lung cancer (NSCLC) [24,25,26,27]. On the other hand, it has been reported that PD-L1 expression in tumor cells and immune cells independently predicts the efficacy of anti-PD-L1 therapy [25, 26]. In any case, there have been no reports evaluating PD-L1 expression on TAMs using the clone 22C3 antibody, which is the most commonly used antibody for lung cancer in clinical practice. Therefore, in the present study, PD-L1 expression on TAMs in lung adenocarcinoma tissue was evaluated by double-IHC using 22C3 antibody and anti-PU.1 antibody (as a marker for TAMs). In a previous study, we reported that the PD-L1 TPS could be accurately determined by double IHC using clone 22C3 and anti-Iba-1 antibodies [7]. Since positive signals of PD-L1 and Iba-1 were both observed in the cell membrane and cytoplasm, we could not accurately determine the MPS by double IHC of PD-L1 and Iba-1. PU.1 is expressed on the nucleus of macrophages; therefore, we newly performed double IHC of PD-L1 and PU.1. The present study results suggested that double IHC using anti-PD-L1 and PU.1 antibodies is an adequate method for accurately determining the MPS in human samples.
In this study, PD-L1 expression on TAMs in the primary lesion of lung adenocarcinoma was seen in 90.0% of the cases, whereas in a previous study, PD-L1 expression in tumor cells was seen in 26.8% of the cases [7]. Consistent with the present study, it was reported that PD-L1 expression was observed in TAMs more frequently than in cancer cells in ovarian cancer and gastric cancer [28, 29]. Sumitomo et al. reported that high PD-L1 expression in tumor-infiltrating immune cells was associated with a high density of M2-like TAMs and a shorter progression-free survival and overall survival in NSCLC [30]. Since TAMs are the main component of PD-L1-expressing stromal cells, the “PD-L1 expression in immune cells” is considered to be very similar to the “MPS.” In our cases, although the CSS in the lung adenocarcinoma patients with pathological stage II cancer or higher was significantly shorter in the high MPS group, there was no association between the MPS and relapse-free survival. This discrepancy might be due to the differences in the histological subtypes of lung cancer. Since the significance of PD-L1 expression is potentially different between lung adenocarcinoma and squamous cell carcinoma [31, 32], studies on PD-L1 in NSCLC should be separated by histological subtypes.
PD-L1 expression on macrophages has been shown to be regulated by STAT1 and STAT3 signals [25, 26]. PD-L1 overexpression in cancer cells may be induced by several mechanisms. Copy number amplification of 9p24.1 and 3’-untranslated region disruption were associated with increased PD-L1 expression in several cancers [33, 34]. Several oncogenic transcription factors, including MYC, RAS, and JAK2/STAT3, also contribute to PD-L1 overexpression in cancer cells [25, 26]. Hypoxia inducible factor 1a is also known to mediate PD-L1 expression in both cancer cells and myeloid cells. In this study, we showed that GM-CSF derived from cancer cells increased PD-L1 expression on TAMs via the JAK/STAT3 pathway in macrophages. Blockade of GM-CSF improved the anti-cancer effect of chemotherapy by modulating the immunosuppressive tumor microenvironment [23, 35]. The PD-L1 expression on TAMs induced by GM-CSF might be involved in the immunosuppressive microenvironment.
In the present study, the experiment in the LLC tumor model using anti-GM-CSF antibody indicated that GM-CSF-blocking inhibited tumor development by inducing anti-tumor immune responses. Although PD-L1 expression in tumor tissues was not influenced by GM-CSF-blocking, the density and maturation of TAMs were significantly suppressed by GM-CSF-blocking. Double IHC data suggested that PD-L1-positive cells in tumor tissues are predominantly TAMs. Inflammatory cytokines, such as interferons and tumor necrosis factor-alpha, that are secreted by activated lymphocytes may up-regulate PD-L1 expression. PD-L1 expression on TAMs is suggested to be mediated by not only cancer-derived GM-CSF, but also inflammatory cytokines secreted from lymphocytes in the mouse model.
It is well known that anti-GM-CSF autoantibody in human was involved in pulmonary alveolar proteinosis (PAP) [36]. However, anti-GM-CSF therapy using therapeutic monoclonal antibody was tested under clinical trial of COVID-19 infection and rheumatoid arthritis [37, 38]. No patients suffered from PAP in these clinical trials, and this indicated monoclonal antibody for GM-CSF was insufficient for the PAP development.
In conclusion, high PD-L1 expression on TAMs was associated with a poor clinical course in advanced cases of lung adenocarcinoma, and cancer cell-derived GM-CSF was suggested to induce PD-L1 overexpression on TAMs via the STAT3 pathway. Results from the preclinical model using the LLC cell line indicated that the blocking of GM-CSF significantly suppressed tumor development, although anti-PD-L1 did not influence anti-GM-CSF therapy. Anti-GM-CSF therapy inhibited the infiltration and maturation of TAMs, and increased T-cell infiltration, suggesting alternative mechanisms of TAM-related immune suppression and PD-L1 overexpression on TAMs in the murine model. Although further studies are necessary to uncover the detailed mechanisms of GM-CSF-induced immune suppression in humans and mice, cancer cell-derived GM-CSF appears to be a promising target for anti-cancer therapy.
References
Li X, Ren F, Wang S et al (2020) The epidemiology of ground glass opacity lung adenocarcinoma: a network-based cumulative meta-analysis. Front Oncol 10:1059
Casal-Mouriño A, Valdés L, Barros-Dios JM, Ruano-Ravina A (2019) Lung cancer survival among never smokers. Cancer Lett 451:142–149
Lim SM, Choi JW, Hong MH et al (2019) Indoor radon exposure increases tumor mutation burden in never-smoker patients with lung adenocarcinoma. Lung Cancer 131:139–146
Borghaei H, Langer CJ, Paz-Ares L et al (2020) Pembrolizumab plus chemotherapy versus chemotherapy alone in patients with advanced non-small cell lung cancer without tumor PD-L1 expression: a pooled analysis of 3 randomized controlled trials. Cancer 126:4867–4877
Topalian SL, Taube JM, Pardoll DM. (2020) Neoadjuvant checkpoint blockade for cancer immunotherapy. Science. 367:eaax0182.
Koomen BM, Badrising SK, van den Heuvel MM, Willems SM (2020) Comparability of PD-L1 immunohistochemistry assays for non-small-cell lung cancer: a systematic review. Histopathology 76:793–802
Shinchi Y, Komohara Y, Yonemitsu K et al (2019) Accurate expression of PD-L1/L2 in lung adenocarcinoma cells: a retrospective study by double immunohistochemistry. Cancer Sci 110:2711–2721
Kozuma Y, Takada K, Toyokawa G et al (2018) Indoleamine 2,3-dioxygenase 1 and programmed cell death-ligand 1 co-expression correlates with aggressive features in lung adenocarcinoma. Eur J Cancer 101:20–29
Takamori S, Takada K, Azuma K et al (2018) Prognostic impact of PD-L2 expression and association with PD-L1 in patients with small-cell lung cancer. Anticancer Res 38:5903–5907
Yu H, Chen Z, Ballman KV et al (2019) Correlation of PD-L1 expression with tumor mutation burden and gene signatures for prognosis in early-stage squamous cell lung carcinoma. J Thorac Oncol 14:25–36
Santoni M, Romagnoli E, Saladino T et al (2018) Triple negative breast cancer: Key role of Tumor-Associated Macrophages in regulating the activity of anti-PD-1/PD-L1 agents. Biochim Biophys Acta Rev Cancer 1869:78–84
Komohara Y, Jinushi M, Takeya M (2014) Clinical significance of macrophage heterogeneity in human malignant tumors. Cancer Sci 105:1–8
Lewis CE, Pollard JW (2006) Distinct role of macrophages in different tumor microenvironments. Cancer Res 66:605–612
Qian BZ, Pollard JW (2010) Macrophage diversity enhances tumor progression and metastasis. Cell 141:39–51
Zhang QW, Liu L, Gong CY et al (2012) Prognostic significance of tumor-associated macrophages in solid tumor: a meta-analysis of the literature. PLoS ONE 7:e50946
Hirayama S, Ishii G, Nagai K et al (2012) Prognostic impact of CD204-positive macrophages in lung squamous cell carcinoma: possible contribution of Cd204-positive macrophages to the tumor-promoting microenvironment. J Thorac Oncol 7:1790–1797
Ohtaki Y, Ishii G, Nagai K et al (2010) Stromal macrophage expressing CD204 is associated with tumor aggressiveness in lung adenocarcinoma. J Thorac Oncol 5:1507–1515
Rakaee M, Busund LR, Jamaly S et al (2019) Prognostic value of macrophage phenotypes in resectable non-small cell lung cancer assessed by multiplex immunohistochemistry. Neoplasia 21:282–293
Grzywa TM, Justyniarska M, Nowis D, Golab J (2021) Tumor immune evasion induced by dysregulation of erythroid progenitor cells development. Cancers (Basel) 13:870
Wang J, Sun J, Liu LN et al (2019) Siglec-15 as an immune suppressor and potential target for normalization cancer immunotherapy. Nat Med 25:656–666
Horlad H, Ma C, Yano H et al (2016) An IL-27/Stat3 axis induces expression of programmed cell death 1 ligands (PD-L1/2) on infiltrating macrophages in lymphoma. Cancer Sci 107:1696–1704
Dong H, Strome SE, Salomao DR et al (2002) Tumor-associated B7–H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat Med 8:793–800
Takeuchi S, Baghdadi M, Tsuchikawa T et al (2015) Chemotherapy-derived inflammatory responses accelerate the formation of immunosuppressive myeloid cells in the tissue microenvironment of human pancreatic cancer. Cancer Res 75:2629–2640
Lin H, Wei S, Hurt EM et al (2018) Host expression of PD-L1 determines efficacy of PD-L1 pathway blockade-mediated tumor regression. J Clin Invest 128:805–815
Chen S, Crabill GA, Pritchard TS et al (2019) Mechanisms regulating PD-L1 expression on tumor and immune cells. J Immunother Cancer 7:305
Shklovskaya E, Rizos H (2020) Spatial and Temporal Changes in PD-L1 Expression in Cancer: The Role of Genetic Drivers, Tumor Microenvironment and Resistance to Therapy. Int J Mol Sci 21:7139
Hu-Lieskovan S, Lisberg A, Zaretsky JM et al (2019) Tumor characteristics associated with benefit from pembrolizumab in advanced non-small cell lung cancer. Clin Cancer Res 25:5061–5068
Gottlieb CE, Mills AM, Cross JV, Ring KL (2017) Tumor-associated macrophage expression of PD-L1 in implants of high grade serous ovarian carcinoma: A comparison of matched primary and metastatic tumors. Gynecol Oncol 144:607–612
Yamashita K, Iwatsuki M, Harada K et al (2020) Prognostic impacts of the combined positive score and the tumor proportion score for programmed death ligand-1 expression by double immunohistochemical staining in patients with advanced gastric cancer. Gastric Cancer 23:95–104
Sumitomo R, Hirai T, Fujita M et al (2019) PD-L1 expression on tumor-infiltrating immune cells is highly associated with M2 TAM and aggressive malignant potential in patients with resected non-small cell lung cancer. Lung Cancer 136:136–144
Lau J, Cheung J, Navarro A et al (2017) Tumour and host cell PD-L1 is required to mediate suppression of anti-tumour immunity in mice. Nat Commun 8:14572
Kowanetz M, Zou W, Gettinger SN et al (2018) Differential regulation of PD-L1 expression by immune and tumor cells in NSCLC and the response to treatment with atezolizumab (anti-PD-L1). Proc Natl Acad Sci U S A 115:E10119–E10126
Green MR, Monti S, Rodig SJ et al (2010) Integrative analysis reveals selective 9p24 1 amplification, increased PD-1 ligand expression, and further induction via JAK2 in nodular sclerosing Hodgkin lymphoma and primary mediastinal large B-cell lymphoma. Blood 116:3268–3277
Kataoka K, Shiraishi Y, Takeda Y et al (2016) Aberrant PD-L1 expression through 3’-UTR disruption in multiple cancers. Nature 534:402–406
Liu Q, Wu H, Li Y et al (2020) Combined blockade of TGf-β1 and GM-CSF improves chemotherapeutic effects for pancreatic cancer by modulating tumor microenvironment. Cancer Immunol Immunother 69:1477–1492
Sakagami T, Beck D, Uchida K et al (2010) Patient-derived granulocyte/macrophage colony-stimulating factor autoantibodies reproduce pulmonary alveolar proteinosis in nonhuman primates. Am J Respir Crit Care Med 182:49–61
Fisher BA, Veenith T, Slade D, et al. (2021) Namilumab or infliximab compared with standard of care in hospitalised patients with COVID-19 (CATALYST): a randomised, multicentre, multi-arm, multistage, open-label, adaptive, phase 2, proof-of-concept trial. Lancet Respir Med. in press
Taylor PC, Saurigny D, Vencovsky J et al (2019) Efficacy and safety of namilumab, a human monoclonal antibody against granulocyte-macrophage colony-stimulating factor (GM-CSF) ligand in patients with rheumatoid arthritis (RA) with either an inadequate response to background methotrexate therapy or an inadequate response or intolerance to an anti-TNF (tumour necrosis factor) biologic therapy: a randomized, controlled trial. Arthritis Res Ther 21:101
Acknowledgements
We thank Mr. Takenobu Nakagawa, Ms. Michiyo Tokunaga, and K. I. Steiner Inc (Kumamoto, Japan) for technical assistance. This work was supported by grants from the Ministry of Education, Culture, Sports, Science, and Technology of Japan (Nos. 16H05162 and 20H03459).
Author information
Authors and Affiliations
Contributions
Yusuke Shinchi, Shiho Ishizuka, Yoshihiro Komohara, and Yukio Fujiwara involved in data curation; Eri Matsubara took part in formal analysis; Yoshihiro Komohara involved in funding acquisition; Eri Matsubara took part in investigation; Kimihiro Yonemitsu and Daiki Yoshii involved in methodology; Yukio Fujiwara took part in project administration; Koei Ikeda, Koji Tamada, and Makoto Suzuki involved in resources; Yoshihiro Komohara took part in supervision; Yusuke Shinchi involved in writing—original draft; Takuro Sakagami, Yoshihiro Komohara, and Makoto Suzuki took part in writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. All authors have no financial competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shinchi, Y., Ishizuka, S., Komohara, Y. et al. The expression of PD-1 ligand 1 on macrophages and its clinical impacts and mechanisms in lung adenocarcinoma. Cancer Immunol Immunother 71, 2645–2661 (2022). https://doi.org/10.1007/s00262-022-03187-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-022-03187-4