Abstract
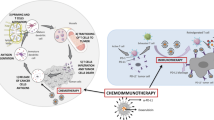
Surface exposed phosphatidylserine (PS) of cancer aids it to evade immune surveillance and thereby results in tumor progression. Earlier, we reported that PS targeting cationic liposomes, phosphatidylcholine–stearylamine (PC-SA), alone and in combination with doxorubicin can result in complete remission of B16F10 melanoma in C57BL/6 mice without signs of toxicity. Inducing an immunogenic response is highly crucial for any cancer therapy as it is essential in improving the tumor microenvironment for any drug to act. Herein, we demonstrate that PC-SA, besides having tumor reducing ability, elicits a strong immune response. The combination therapy (PC-SA-DOX) is superior to free DOX in enhancing the anti-tumor immune effect on CD4-positive and CD8-positive T cells for IFN-γ, IL-2 and TNF-α production in sera and splenic culture supernatants of B16F10 tumor-induced mice. An upregulation of IL-12 and NO production is evidenced in spleen cultures of these mice, thereby showing a promising role of both Th1 type and innate immune response for host anti-tumor activity. Complete elimination of cancer is sometimes accomplished by surgery, but its effectiveness is often limited due to the propensity of cancers to spread to distant organs by metastasis. In our present study, we show that in PC-SA-DOX treated mice, the elevated Th1 cytokine levels create an immuno-protective environment which thereby facilitates in curing lung metastasis. Our results, therefore, warrant the need of effective immune stimulation by anticancer formulations for inhibition of solid tumors and metastasis, demonstrated by the liposomal DOX formulation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
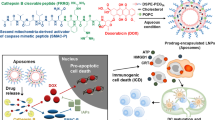
Phosphatidylserine (PS), an anionic phospholipid, is generally exposed on the surface of cancer cells and tumor vasculature [1, 2]. This increased PS exposure leads to shedding of soluble phosphatidylserine (sPS) which may interact with PS receptors on antigen presenting cells (APCs) to initiate an immunosuppressive response [3]. Anti-PS antibodies, first developed by Thorpe’s group, bind to exposed PS on tumor cell surface [4, 5]. These antibodies are reported to show anti-tumor innate immune response when combined with irradiation therapy, and in combination with immune check point blocker, anti-PD1 antibody, result in increased number of CD4+ and CD8+ tumor infiltrating lymphocytes, thereby elevating proinflammatory cytokines such as IFN-γ, IL-2 and TNF-α [6]. Cationic lipid nanoparticles (LNPs) used mainly for drug delivery, are also reported to induce proinflammatory Th1 cytokine expression (IL-2, IFN-γ and TNF-α) ten to seventy five times greater than treatment with neutral or negatively charged particles [7]. Immuno-stimulatory oligonucleotides (ODNs) with CpG motifs when selectively delivered by liposome-based agent into the tumor environment showed a marked inflammatory response with enhanced CD8+ and CD4+ T cell infiltration and activation of anti-tumor activity [8]. Herein we report, our PC-SA liposome alone and in combination to DOX have an immuno-stimulatory activity in addition to its previously reported tumor killing ability [1].
We have recently reported that PC-SA itself has anticancer property due to its specificity toward surface exposed PS, on cancer cells. DOX is majorly administered in multiple high doses (5 mg/kg on day 1, day 7, day 14 and day 21) which results in hepatotoxicity and cardiotoxicity. Therefore, a low amount (2.8 mg/kg of DOX injected twice, i.e., on day 7 and 14) of anticancer drugs, such as DOX and camptothecin, in this SA-bearing cationic liposome, through single or double dose administration, demonstrated almost complete clearance of tumors across different in vivo tumor models [1]. In addition to a formulation having ability to kill tumor, it is beneficial that it has some immunomodulatory activity to be able to improve the tumor microenvironment. Herein, experiments have been designed to investigate the possible mechanistic approach of the PC-SA-DOX liposomal formulation in redirecting the disease related immunological activity to establish and sustain a remedial effect against tumor and metastatic cancers. In the present study, we report that DOX encapsulated in these PC-SA liposome vesicles is efficient in sustaining and upregulating the inherent immunological effect of the drug in B16F10 solid tumor-induced mice. We found that administration of cationic liposome-associated low dose of DOX permitted outstanding anticancer activity, through enhancement of a Th1-biased curative immune response by exerting its immunomodulatory effect for IL-12 secretion, and additionally on CD4+ and CD8+ T cells for IFN-γ, IL-2, TNF-α and IL-12 secretion.
Development of metastasis correlates with the impact of therapy on immune cell subsets [9]. Our in vivo experiments on normal mice clearly demonstrate that drug-free PC-SA and PC-SA-DOX exerted an inducing effect on concanavalin A (ConA)-specific Th1 cytokines production thus promoting the T cell immune activity. Additionally, we report antimetastatic effect of our formulation against an in vivo lung metastatic model.
Materials and methods
Liposomes
PC-SA liposomes (7:2 molar ratio) and PC-SA-DOX liposomes were prepared as described earlier [1]. Particle size distribution and zeta potential of PC-SA liposome were measured by laser DLS (Malvern Instrument, Zeta sizer, Nano-ZS, model ZEN 3600) as described earlier [1].
Enzyme-linked immunosorbent
Enzyme-linked immunosorbent assay (ELISA) was performed as recommended by the manufacturers, (eBioscience) [10]. Briefly, 96-well maxisorp (Nunc) microplates were coated overnight with capture antibody. Blocking reagents were added and incubated for 1 h followed by incubation with cell-free supernatant or serum samples for 2 h. Biotinylated detection antibody and streptavidine horse radish peroxidase (HRP) were added and kept for 1 h followed by substrate solution (TMB) and then stop solution (2 N H2SO4) added. Each step was followed by a three-step washing with PBS buffer. The limits of detection for IFN-γ and TNF-α were 31.25–2000 pg/ml, and for IL-2, IL-4, IL-12p40 and IL-13, they were 4.6–300 pg/ml, 8–500 pg/ml, 2–300 pg/ml and 62.5–4000 pg/ml, respectively.
Cytokine production from splenocytes of normal mice
Normal C57BL/6 mice were injected subcutaneously with double doses (with 7-day interval) of 60 mg/kg of PC-SA liposomes alone, 2.8 mg/kg of free DOX and 2.8 mg/kg of DOX entrapped in 60 mg/kg of PC-SA liposomes on day 0. On day 14, from the start of the experiments, animals were killed. IFN-γ and TNF-α cytokine levels in the splenocyte culture supernatants of the various treated groups, in response to Concanavalin A (ConA) (2.5 µg/ml) incubation for 48 h, were determined by sandwich ELISA (eBioscience) as recommended by the manufacturers [10].
Cell culture
B16F10 cells purchased from NCCS Pune were maintained in DMEM (Gibco) supplemented with 10% fetal bovine serum (MP Biomedicals), sodium pyruvate, 2 mM l-glutamine, penicillin and streptomycin [1].
Animals
Animal ethical clearance was approved by ethical committee at IICB (147/1999/CPSCEA). Female C57BL/6 of 3–4 weeks age was maintained at the animal house facility at IICB. The mice were supplied filtered air, appropriate food supplements water and they were kept in ample light supply. The animals (n = 3 or n = 6) were randomly grouped.
Tumor induction and treatment
1 × 106 B16F10 cells were suspended in 100 μl of 0.02 M PBS and injected on day 0 in the left flank of female C57BL/6 mice. On days 7 and 16, mice were treated with 60 mg/kg of PC-SA liposome, 2.8 mg/kg of DOX and 2.8 mg/kg of DOX entrapped in 60 mg/kg of PC-SA liposome. Untreated mice injected with B16F10 cells were kept as controls. On day 24 of tumor inoculation, mice were killed and tumors were taken out, and measured as previously done [1].
Splenocyte culture
The spleens were aseptically removed from the treated and untreated mice on day 24 of B16F10 solid tumor induction, and cells were suspended in RPMI 1640. This was followed by washing the splenocytes twice, resuspending in the culture medium and viable mononuclear cell number was determined by Trypan blue exclusion [10].
Cell proliferation assay
Splenocytes were then labeled with carboxyfluoresceinsuccinimidyl ester (CFSE) (Molecular Probes) using a modified technique, originally devised by Lyon et al. [11, 12]. Briefly, 1x106 cells/ml were incubated with 2 mM CFSE for 30 min at 37 °C. The labeling was quenched by adding 5 volumes of cold RPMI and keeping on ice for 10 min followed by washing twice in cold RPMI 1640 (Sigma). Cells (1 × 106 cells/well) were then cultured in triplicates in 24-well flat-bottomed tissue culture plates in a final volume of 1 ml and stimulated with tumor lysate (50 µg/ml). After 5 days, the cells were collected and analyzed on BDLSRFortessa™ Cell Analyser (BD) using the FACS Diva software.
Cytokine assays in B16F10 solid tumor model
Serum samples were collected after termination of experiments (i.e., on day 24 of tumor inoculation) from B16F10 tumor implanted C57BL/6 mice treated (s.c) on days 7 and 16 of tumor induction, with 60 mg/kg of PC-SA liposomes alone, 2.8 mg/kg of free DOX and 2.8 mg/kg of DOX entrapped in 60 mg/kg of PC-SA liposomes [1]. Blood was collected via tail vein, allowed to clot at room temperature and centrifuged (10,000 g for 10 min) to separate serum. Cytokine amounts in sera (1:2 dilutions) were determined by ELISA (eBioscience).
Depletion of CD4+ and CD8+ T cells
Single-cell suspensions of splenocytes were isolated as above from different groups of mice. T cell subsets from the splenocytes were depleted using monoclonal antibodies (Biolegend) for CD4+ T cells, CD8+ T cells and both CD4+ CD8+ T cells for 60–90 min (1 µg/106 cells) at 4 °C followed by washing [13].
Tumor-specific cytokine production in B16F10 solid tumor model
B16F10 cells were grown and lysed by five freeze/thaw cycles in liquid nitrogen and then in 37 °C water-bath, centrifuged at 10,000g for 15 min. The supernatant (lysate) was filtered, and the protein concentration was determined by Lowry’s assay. Tumor-induced control and treated mice were killed and undepleted, and depleted splenocytes (0.5 × 106) were restimulated in vitro with 50 µg/ml of tumor lysate for 72 h. Cell-free supernatants were harvested at 72 h, and IFN-γ, IL-2, IL-12 p40, TNF-α, IL-4 and IL-13 amounts were analyzed by ELISA (eBioscience) [13].
Quantification of NO
Splenocytes (0.5 × 106) from differently treated groups of experimental B16F10 solid tumor model were incubated with or without 50 µg/ml tumor lysate for 72 h in 5%CO2 at 37 °C. The culture supernatants were tested for NO2− levels according to the method of Ding et al. Briefly, the mixture of Greiss reagent (1% sulfanilamide and 0.1% N-(1-naphthyl) ethylenediaminedihydrochloride in 2.5% H3PO4) and culture supernatant at 1:1 ratio were incubated for 15 min at room temperature, and the OD was determined at 550 nm by ELISA reader (Thermo). Sodium nitrite (NaNO2) diluted in culture medium served as standard [1, 14].
Flow cytometry
Splenocytes (1 × 106) from differently treated B16F10 solid tumor implanted mice were stimulated with 50 µg/ml tumor lysate and cultured overnight in 24 well cell culture plates. BFA (Brefeldin A) (10 µg/ml) was added to the cultures 2 h prior to harvesting. This was followed by washing the cells with 20 mM PBS containing 0.1% NaN3 and 1% FCS (staining buffer) at 4 °C and then stained with PerCp-Cy5.5-conjugated anti-CD4, APC-Cy7 conjugated anti-CD3 and FITC-conjugated anti-CD8 mAb at 4 °C for 30 min. The cells were then fixed and permeabilized with Cytofix/Cytoperm (BD Biosciences, San Diego, CA) solution for 20 min at 4 °C, and stained with APC-conjugated anti-mouse IFN-γ, PE-Cy7-conjugated IL-2 and PE-conjugated TNF-α mAb. After incubation at 4 °C for 1 h in the dark, cells were washed with permeabilization buffer (0.1% saponin in PBS) and re-suspended in staining buffer prior to analysis [10]. At least 50,000 events were acquired in a BDLSRFortessa™ Cell Analyser (BD) using the FACS Diva software.
In vivo experimental pulmonary metastasis assay
For the in vivo experimental pulmonary metastasis study, 0.2 ml of B16F10 cell (1x106 per animal in 20 mM PBS) was injected into the tail veins of C57BL6 mice. The viability of cells was > 90% as determined by trypan blue exclusion. On day 7 of tumor inoculation, mice were injected intravenously with 22 mg of PC-SA per mouse, 0.125 mg (i.e., 5 mg/kg body weight) of DOX or 0.125 mg (i.e., 5 mg/kg body weight) of DOX entrapped in 22 mg of PC-SA liposomes. Since treatment in metastatic model is through intravenous route we used as higher dose of our formulation because there are chances of biodistribution of the drug in other organs. Control mice received PBS. Each group consisted of three mice. Mice were killed on day 24 of cell inoculation. The lungs were removed, and visible nodules on the surfaces were counted with the help of dissecting forceps.
Tumor-specific cytokine production in B16F10 lung metastasis model
Pulmonary metastasis was induced by injecting B16F10 cells and treated as described above. Control mice received PBS. On day 24 of B16F10 inoculation, mice were killed and spleen cells were isolated as described above. Splenocytes (0.5 × 106) were restimulated in vitro with 50 μg/ml tumor lysate for 72 h. Cell-free supernatants were harvested at 72 h, and IFN-γ, IL-2, IL-12 p40 and TNF-α amounts were analyzed by ELISA (eBioscience).
Statistical analysis
Statistics was performed using GraphPad Prism 5 software (https://www.graphpad.com) software. Statistical significance (***p < 0.0001, all other p values as stated) was calculated using ANOVA with Tukey’s correction and Student’s t test.
Results
Size and Zeta potential of PC-SA
Hydrodynamic diameter of PC-SA-DOX was 148 nm, and Zeta potential was + 43.1 mV.
Immunomodulatory activity of DOX entrapped in PC-SA liposomes on splenic cells of normal mice, in vitro
Our strategy was to study whether PC-SA-DOX treatment can induce Th1 cytokines such as IFN-γ, IL-12 p40 and TNF-α from splenocytes of healthy normal C57BL/6 mice. Fourteen days after treatment, mice were killed. Splenocytes (stimulated with ConA) from PC-SA-DOX treated mice caused significant elevation of IFN-γ (p < 0.001), IL-12 p40 (p < 0.01) and TNF-α (p < 0.0001) levels in comparison with untreated controls. IL-12p40, a subunit of IL-12 or IL-23, has multiple role in anticancer immune response. PC-SA-DOX treatment also significantly increased IFN-γ and TNF-α levels (p < 0.01) when compared with free DOX treated mice (Fig. 1a). These results exhibit that PC-SA-DOX liposomes have the ability to impart beneficial immunomodulatory effects, by enhancing the secretion of Th1 cytokines.
PC-SA-DOX treatment induces a Th1 cytokine response in normal and B16F10 tumor-induced mice (a). Normal mice were treated twice (with 7 day interval) with 60 mg/kg of PC-SA liposomes alone, 2.8 mg/kg of free DOX, 2.8 mg/kg of DOX entrapped in 60 mg/kg of PC-SA liposomes. After 14 days, spleens were taken out from differently treated animals, and splenocytes were isolated, seeded in 24-well plate (5 × 105 cells/well) and stimulated with 2.5 µg/ml of Con A for 48 h. Cell-free culture supernatants were collected to determine the secretion of Con A-specific IFN-γ, IL-12p40 and TNF-α by ELISA (b). Mice treated with the doses mentioned above of PC-SA, DOX or PC-SA-DOX on days 7 and 16 of B16F10 solid tumor induction were killed on day 24 post-inoculation of B16F10 cells, tumors were taken out (for PC-SA-DOX, figure is a representative of tumors isolated from two different mice), and c serum amounts of IFN-γ, IL-2 and TNF-α cytokines were detected by ELISA. Data were tested by ANOVA. Differences between mean were assessed for statistical significance by Tukey’s test (*p < 0.01; **p < 0.001; ***p < 0.0001) each group having 3 C57BL6 mice
Evaluation of antigen-specific lympho-proliferation in differently treated B16F10 solid tumor-induced mice
A leftward shift to the x axis in CFSE fluorescence indicates proliferation of cells. Negligible shift in numbers of CFSE positive population was seen in control mice (0.8%). The percentage of free DOX and free PC-SA treated cells that underwent division was 1.7%. PC-SA-DOX treated mice exhibited greater lympho-proliferation of 6.5%, compared to untreated controls, DOX and PC-SA treated groups. Taken together, these findings suggest that PC-SA-DOX treatment caused better lympho-proliferation to rule out the impaired T cells response for better protection against cancer. (Supporting Information Fig. S1).
PC-SA-DOX treatment increases Th1 cytokine levels in C57BL6 mice bearing B16F10 solid tumor
To evaluate whether PC-SA, DOX and PC-SA-DOX treatment modulated cytokine amounts in tumor-bearing mice, mice treated with PC-SA, DOX or PC-SA-DOX were killed and tumors isolated on day 24 after implantation of B16F10 solid tumor. Maximal tumor growth inhibition was observed in mice treated with PC-SA-DOX followed by PC-SA (Fig. 1b and Supporting Information Fig. S2). Interestingly, the levels of the three T helper 1 (Th1)-type cytokines, IFN-γ (p < 0.001 and p < 0.001), IL-2 (p < 0.01 and p < 0.01) and TNF-α (p < 0.0001 and p < 0.0001) were significantly increased in the sera of mice receiving PC-SA-DOX compared to untreated and DOX treated mice, respectively (Fig. 1c).
Tumor antigen-specific cytokine secretion by CD4+ T cells and CD8+ T cells in B16F10 solid tumor-induced mice
To investigate the ability of PC-SA-DOX treatment to show immune response specific to tumor, isolated splenic cells were stimulated in vitro with B16F10 tumor lysates. After 72 h, cell-free supernatants were collected for cytokine assays. B16F10 tumor lysate-stimulated splenocytes isolated from PC-SA-DOX treated mice produced significantly higher amounts of IFN-γ (p < 0.01), IL-2 (p < 0.01), IL-12 p40 (p < 0.0001) and TNF-α (p < 0.01) in comparison with untreated control B16F10 solid tumor-induced mice. Interestingly, in PC-SA-DOX treated tumor-induced mice, levels of IFN-γ, and TNF-α were considerably downregulated in CD4+ T cells, CD8+ T cells or both CD4+ and CD8+ T depleted cells, indicating that CD4 and CD8 T cells play a key role in the secretion of these cytokines from PC-SA-DOX treated mice (Fig. 2a–d). In addition, we also studied the secretion level IL-4 and IL-13 cytokines from undepleted splenocytes and found that PC-SA-DOX could decrease the levels of IL-4 and IL-13 in comparison with controls (p < 0.05) and as well as that of DOX and PC-SA treated mice (Supporting Information Fig. S3). Ratios of IFN-γ:IL-4 and IFN-γ:IL-13 indicate that there is a Th1 biased response in PC-SA-DOX treated mice (Supporting Information Fig. S4).
CD4+ T and CD8+ T cells from PC-SA-DOX treated B16F10 solid tumor-induced mice produce high amounts of IFN-γ, IL-2, IL-12 p40 and TNF-α in a tumor-specific manner. Twenty four days after transplantation of B16F10 solid tumor, isolated splenocytes from differently treated and untreated mice were incubated with anti CD4 or anti CD8 or anti CD4 and CD8 monoclonal antibodies to deplete specific T cell populations and stimulated in vitro with B16F10 (specific) tumor lysates (50 µg/ml). Culture supernatants from undepleted, CD4+ T cells depleted, CD8+ T cells depleted, and both CD4+ and CD8+T cells depleted splenocytes were collected after 72 h, and a IFN-γ, b IL-2, c IL-12 and d TNF-α cytokines were measured by ELISA. Each group had 3 C57BL6 mice. Data were tested by ANOVA. Differences between mean were assessed for statistical significance by Tukey’s test (*p < 0.01; **p < 0.001; ***p < 0.0001)
PC-SA-DOX treated tumorigenic mice produce more nitrite (NO) after cure
In PC-SA-DOX treated B16F10 solid tumor-induced mice, we found ~ 3-, ~ 2- and ~ 2.5- fold higher and significant levels of NO production (from splenocytes stimulated in vitro with tumor lysates) in comparison with untreated tumor-bearing controls (p < 0.001), free PC-SA (p < 0.01) and free DOX (p < 0.001) treatment (Supporting Information Fig. S5).
PC-SA liposome-associated DOX treatment in B16F10 solid tumor-bearing mice elicits a high frequency of IFN-γ, IL-2 and TNF-α-secreting CD4+ and CD8+ T cells
Intra cellular cytokines were analyzed through flow cytometry to compare the T cell population present in the spleen of control untreated tumor-bearing and treated groups. Populations of CD3+, CD4+ and CD8+ T cells in the splenocytes of PC-SA-DOX treated mice significantly increased compared to that of untreated tumor-bearing mice (p < 0.01) (Supporting Information Fig. S6). The frequencies of IFN-γ, IL-2 and TNF-α-producing CD4+ and CD8+ T cells, respectively, increased after free PC-SA liposome and free DOX treatment in comparison with control (Fig. 3). However, the magnitude of IFN-γ, IL-2 and TNF-α-producing CD4+ and CD8+ T cells, respectively, were highest with PC-SA-DOX treatment. These results are consistent with enhanced IFN-γ, IL-2 and TNF-α in serum as well as from splenocytes. These results also demonstrate a promising role of both CD4+ and CD8+ T cells producing Th1 cytokines like IFN-γ, IL-2 and TNF-α leading to effective cure.
Intracellular T cell response to PC-SA-DOX in B16F10 tumor-induced mice. Percentage of tumor lysate-stimulated CD4+ and CD8+T cells of various control and treated B16F10 solid tumor-induced mice producing IFN-γ, IL-2 and TNF-α was determined by flow cytometry. Splenocytes were stimulated with B16F10 tumor lysate (50 µg/ml). Surface phenotyping and intracellular staining were performed, and cells were analyzed by flow cytometer. Dot-plot and mean percentage of a, b CD4+ and c, d CD8+cells producing IFN-γ, IL-2 and TNF-α in each group of control and treated (n = 3) C57BL6 mice. The significance of difference was determined by Tukey’s test (*p < 0.01; **p < 0.001; ***p < 0.0001)
In vivo lung colonization
B16F10 cells were injected intravenously in C57BL6 mice. Treatment with 0.125 mg/kg of DOX in association with 22 mg of PC-SA (i.v) on day 7 of cell inoculation resulted in complete clearance of pulmonary nodules. Lung colony count was reduced by 76% and 99% with free PC-SA and DOX entrapped in PC-SA, respectively. Free DOX could reduce only 24% of lung colonies. Thus, PC-SA and DOX entrapped in PC-SA liposomes were found to be effective against lung metastasis also (Fig. 4a, b).
PC-SA-DOX treatment inhibits growth of lung metastasis and releases B16F10 tumor antigen-specific Th1 cytokines from splenocytes in a pulmonary metastasis mouse Lungs from B16F10 cell inoculated mice (i.v) treated with 22 mg of PC-SA, 0.125 mg of DOX, 0.125 mg DOX entrapped in 22 mg of PC-SA and untreated mice were taken out and photographed (a) for counting the nodules (b). Splenocytes from the above treated mice were stimulated in vitro with B16F10 (specific) tumor lysates (50 μg/ml) for 72 h, and IL-12p40, IFN-γ, IL-2 and TNF-α cytokines were determined by ELISA from the culture supernatants (c). (mean ± SE for three animals per group performed in duplicate, n = 6). Data were tested by ANOVA. Differences between mean were assessed for statistical significance by Tukey’s test (*p < 0.01; **p < 0.001; ***p < 0.0001) (c) (mean ± SE for three animals per group performed in duplicate)
Tumor antigen-specific cytokine secretion by splenocytes in the pulmonary metastasis mouse model
To investigate the ability of PC-SA-DOX treatment to induce tumor-specific recall responses in the pulmonary metastasis mouse model, cultured splenocytes were stimulated with B16F10 cell lysates and cell-free supernatants were used for determining different levels of cytokines. PC-SA-DOX treated mice showed significantly higher levels of IFN-γ, IL-2, IL-12 p40 and TNF-α production upon incubation of the cultured splenocytes with B16F10 cell lysate as compared with untreated control and DOX treated B16F10 pulmonary metastasis-bearing mice (Fig. 4c).
Discussion
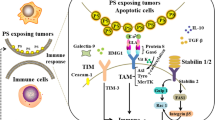
Expression of elevated levels of PS on the surface of tumor cells in the tumor microenvironment has an innate immunosuppressive property by inducing secretion of immune-suppressive cytokines, interleukin-10 (IL-10) and TGF-β, thereby facilitates tumor growth and metastasis [15, 16]. Several studies have shown that the induction of a Th1 response, with IFN-γ, IL-2 and TNF-α as principal cytokines, plays a crucial role in overcoming the immune-suppressive tumor microenvironment in cancer [17,18,19,20]. DOX, a potent drug used against solid tumor, also induces a lymphocyte-mediated Th1 cytokine response [21]. However, due to several acute and chronic side effects of DOX, its clinical use is limited. Herein, we evaluated the immunomodulatory role of our liposomal DOX formulation (PC-SA-DOX) and report that treatment results in a Th1 biased immune response.
In our recently published work, the tumor clearance efficiency of DOX in combination with PC-SA liposome was shown against B16F10 melanoma in C57BL/6 mice [1]. In an earlier study from our group, treatment of visceral leishmaniasis (VL) with free PC-SA liposome, and in combination with amphotericin B, could induce immunomodulation in normal healthy mice [10]. Based on these, we wanted to investigate whether the therapeutic dose of PC-SA (60 mg/kg, i.e., 1.5 mg/mouse, s.c injection) used against B16F10 tumor-induced mice [1], could elicit any curative immunomodulation. As observed earlier, herein also we found that drug-free PC-SA liposomes induced some level of ConA specific IFN-γ, IL-12 p40 and TNF-α in normal mice. Treatment with DOX entrapped PC-SA increased the levels of IFN-γ, IL-12 p40 and TNF-α in comparison with free liposome as well as free DOX. Regulation of cytokines is reported to occur with progression of tumor [22]. Earlier studies on DOX treatment in mice induced with ovarian cancer, or in carcinogen-induced adenocarcinomas and fibrosarcomas, showed CD4 T cell dependent anti-tumor immune response [19]. DOX treatment prolongs survival and enhances tumor-specific proliferation of CD8 T cells in tumor-draining lymph nodes (LNs) producing IFN-γ [23]. Notably, upregulation of Th1 cytokines was observed in the sera of tumorigenic mice treated with PC-SA-DOX treatment. Increase in the secretion of IFN-γ, IL-2 and TNF-α in the sera of treated mice suggests that it is a pro-Th1 inducer. These observations are consistent with reports that secretion of these cytokines is elevated during anti-tumor responses [21, 24, 25]. PC-SA-DOX induces protective cell-mediated immune effects principally through the production of IFN-γ, IL-2 and TNF-α from both CD4+ and CD8+splenocyte T cells. Although in small quantity, free DOX and free PC-SA also triggered CD4+ and CD8+ T cells to produce IFN-γ, IL-2 and TNF-α. In vitro depletion of CD4+ and CD8+ cells using anti-CD4 or anti-CD8 mAb [26, 27] led to reduced IFN-γ, IL-2 and TNF-α production, further validating the role of CD4 and CD8 T cells in promoting a sustained T cell response. On the other hand, no significant decrease in the production of IL-12 cytokine was observed in CD4+, CD8+ or both CD4+ and CD8+ depleted T cells by the treated groups, indicating that IL-12 is not produced by CD4+ and CD8+ T cells. IL-12 is primarily produced by antigen presenting cells. It induces Th1 response, increases the generation of CD8 T cells, enhances the proliferation of activated T and natural killer (NK) cells and induces the production and stabilization of IFN-γ [25, 28]. Additionally, we observed decrease in IL-4 and IL-13 secretion upon treatment with PC-SA-DOX, confirming that it is a Th1-driven response. We also found an upregulation of NO production from splenocytes of PC-SA-DOX treated mice. High concentration of NO levels results in cancer cell cytotoxicity [29]; thus, it could be one of the reasons for the control of tumor growth in the successfully treated animals. It can therefore be inferred that the PS-driven immunosuppression in the microenvironment is reversed to a Th1 inducing response through the blocking of the PS by our formulation.
Th1 cytokines are known to show protection against metastatic cancer. Remarkably, IL-12 has been found to play an important role in primary and metastatic tumor suppression in different tumor models and human clinical trials [25, 30,31,32,33]. The increase in Th1 response in normal mice treated with our formulation gave us an insight into the feasibility of this formulation for the treatment of metastatic tumor model. Interestingly, we found a reduction in the number of lung nodules in lung metastatic model treated with PC-SA-DOX. The treated animals corresponded with elevated secretion of Th1 cytokines like IFN-γ, IL-2, IL-12 p40 and TNF-α. These could be reasoned to improve the overall tumor suppression in the microenvironment and also aid in preventing metastasis.
Taken together, these findings support the view that our PC-SA-DOX liposomal formulation which we recently demonstrated to have anticancer activity with almost no toxicity [1], also depicts strong anti-tumor immune activities. Here, we have successfully shown that PC-SA-DOX regulates immune function cells and promotes Th1 response, indicating that the liposomes targets PS to block immunosuppressive effect of PS. A Th1 response is critical for tumor destruction and inducing a strong anti-tumor immunity [9, 33, 34]. Herein, we report a similar Th1 response, as a consequence of which metastasis may have been prevented. Therefore, our results are suggestive that this formulation has the ability to enhance Th1 biased anti-tumor immunity thereby having a role in limiting lung metastasis. Thus, we believe the combination therapy, designed herein, not only directly kills cancer cells, but also simultaneously causes generation of immunity against the disease offering a new strategy for treating solid tumors.
Abbreviations
- ANOVA:
-
Analysis of variance
- APC:
-
Allophycocyanin
- APCs:
-
Antigen presenting cells
- BFA:
-
Brefeldin A
- CD:
-
Cluster of differentiation
- CFSE:
-
Carboxyfluoresceinsuccinimidyl ester
- ConA:
-
Concanavalin A
- DLS:
-
Dynamic light scattering
- DOX:
-
Doxorubicin
- ELISA:
-
Enzyme-linked immunosorbent assay
- FITC:
-
Fluorescein isothiocyanate
- i.v:
-
Intravenous
- IFN-γ:
-
Interferon-gamma
- IL:
-
Interleukin
- mAb:
-
Monoclonal antibody
- NaN3 :
-
Sodium azide
- NCCS:
-
National Centre or Cell Science
- NIN:
-
National Institute of Nutrition
- NK:
-
Natural killer
- NO:
-
Nitric oxide
- ODNs:
-
Immunostimulatory oligonucleotides
- PC-SA:
-
Phosphatidylcholine–stearylamine
- PE:
-
Phycoerythrin
- PS:
-
Phosphatidylserine
- s.c:
-
Subcutaneous
- SE:
-
Standard error
- Streptavidine HRP:
-
Streptavidine horse raddish peroxidase
- Th:
-
T helper
- TMB:
-
3,3′,5,5′-Tetramethylbenzidine
- TNFα:
-
Tumor necrosis factor-alpha
References
De M et al (2018) A novel therapeutic strategy for cancer using phosphatidylserine targeting stearylamine-bearing cationic liposomes. Mol Ther Nucleic Acids 10:9–27
Ran S, Downes A, Thorpe PE (2002) Increased exposure of anionic phospholipids on the surface of tumor blood vessels. Cancer Res 62(21):6132–6140
Kim R, Emi M, Tanabe K (2005) Cancer cell immune escape and tumor progression by exploitation of anti-inflammatory and pro-inflammatory responses. Cancer Biol Ther 4(9):924–933
DeRose P, Thorpe PE, Gerber DE (2011) Development of bavituximab, a vascular targeting agent with immune-modulating properties, for lung cancer treatment. Immunotherapy 3(8):933–944
Huang X, Bennett M, Thorpe PE (2005) A monoclonal antibody that binds anionic phospholipids on tumor blood vessels enhances the antitumor effect of docetaxel on human breast tumors in mice. Cancer Res 65(10):4408–4416
Birge RB et al (2016) Phosphatidylserine is a global immunosuppressive signal in efferocytosis, infectious disease, and cancer. Cell Death Differ 23(6):962–978
Peer D (2012) Immunotoxicity derived from manipulating leukocytes with lipid-based nanoparticles. Adv Drug Deliv Rev 64(15):1738–1748
Hamzah J et al (2009) Targeted liposomal delivery of TLR9 ligands activates spontaneous antitumor immunity in an autochthonous cancer model. J Immunol 183(2):1091–1098
Janssen LME et al (2017) The immune system in cancer metastasis: friend or foe? J Immunother Cancer 5(1):79
Banerjee A, De M, Ali N (2008) Complete cure of experimental visceral leishmaniasis with amphotericin B in stearylamine-bearing cationic liposomes involves down-regulation of IL-10 and favorable T cell responses. J Immunol 181(2):1386–1398
Lyons AB (2000) Analysing cell division in vivo and in vitro using flow cytometric measurement of CFSE dye dilution. J Immunol Methods 243(1–2):147–154
Das A, Ali N (2014) Combining cationic liposomal delivery with MPL-TDM for cysteine protease cocktail vaccination against Leishmania donovani: evidence for antigen synergy and protection. PLoS Negl Trop Dis 8(8):e3091
Rakshit S et al (2012) Immunotherapeutic efficacy of Mycobacterium indicus pranii in eliciting anti-tumor T cell responses: critical roles of IFNgamma. Int J Cancer 130(4):865–875
Ding AH, Nathan CF, Stuehr DJ (1988) Release of reactive nitrogen intermediates and reactive oxygen intermediates from mouse peritoneal macrophages. Comparison of activating cytokines and evidence for independent production. J Immunol 141(7):2407–2412
Huang X, Ye D, Thorpe PE (2011) Enhancing the potency of a whole-cell breast cancer vaccine in mice with an antibody-IL-2 immunocytokine that targets exposed phosphatidylserine. Vaccine 29(29–30):4785–4793
Tse E, Kwong YL (2015) T-cell lymphoma: microenvironment-related biomarkers. Semin Cancer Biol 34:46–51
Yu WG et al (1997) IL-12-induced tumor regression correlates with in situ activity of IFN-gamma produced by tumor-infiltrating cells and its secondary induction of anti-tumor pathways. J Leukoc Biol 62(4):450–457
Lee CM et al (2002) Novel chondroitin sulfate-binding cationic liposomes loaded with cisplatin efficiently suppress the local growth and liver metastasis of tumor cells in vivo. Cancer Res 62(15):4282–4288
Bracci L et al (2014) Immune-based mechanisms of cytotoxic chemotherapy: implications for the design of novel and rationale-based combined treatments against cancer. Cell Death Differ 21(1):15–25
Ahmad F et al (2011) Activation of anti-tumor immune response and reduction of regulatory T cells with Mycobacterium indicus pranii (MIP) therapy in tumor bearing mice. PLoS ONE 6(9):e25424
Santos RV et al (2010) Effect of doxorubicin on cytokine production by lymphocytes and the Th1/Th2 balance. Biomed Pharmacother 64(8):579–581
Dranoff G (2004) Cytokines in cancer pathogenesis and cancer therapy. Nat Rev Cancer 4(1):11–22
Kim JE et al (2012) Cancer cells containing nanoscale chemotherapeutic drugs generate antiovarian cancer-specific CD4+ T cells in peritoneal space. J Immunother 35(1):1–13
Saha B et al (2010) Gene modulation and immunoregulatory roles of interferon gamma. Cytokine 50(1):1–14
Tugues S et al (2015) New insights into IL-12-mediated tumor suppression. Cell Death Differ 22(2):237–246
Hanson HL et al (2000) Eradication of established tumors by CD8+ T cell adoptive immunotherapy. Immunity 13(2):265–276
Corthay A et al (2005) Primary antitumor immune response mediated by CD4+ T cells. Immunity 22(3):371–383
Trinchieri G (1998) Interleukin-12: a cytokine at the interface of inflammation and immunity. Adv Immunol 70:83–243
Vahora H et al (2016) The potential role of nitric oxide in halting cancer progression through chemoprevention. J Cancer Prev 21(1):1–12
Yoon SJ et al (1999) Combination gene therapy of IL-12 and allogeneic MHC class I gene via stimulating NK cytolytic activity. Anticancer Res 19(5B):4337–4342
DiMeco F et al (2000) Paracrine delivery of IL-12 against intracranial 9L gliosarcoma in rats. J Neurosurg 92(3):419–427
Lechanteur C et al (2000) Antitumoral vaccination with granulocyte-macrophage colony-stimulating factor or interleukin-12-expressing DHD/K12 colon adenocarcinoma cells. Cancer Gene Ther 7(5):676–682
Nishimura T et al (2000) The critical role of Th1-dominant immunity in tumor immunology. Cancer Chemother Pharmacol 46(Suppl):S52–S61
Dai M et al (2018) Tumor regression and cure depends on sustained Th1 responses. J Immunother 41(8):369–378
Acknowledgements
The authors are thankful to Director of CSIR-IICB, Kolkata, Dr. Samit Chattopadhyay for supporting this work. The authors are also thankful to Mr. Tanmoy Dalui and Debalina Chakraabarty for flow cytometry.
Funding
Grant sponsor: Department of Science Technology (DST)-J. C. Bose National Fellowship (Grant No. SB/S2/JCB-021/2015).
Author information
Authors and Affiliations
Contributions
MD and NA designed the experiments. MD, IB and SG carried out the experiments. MD and MA analyzed the data. MD, NA and SG wrote the manuscript. NA supervised the project.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Animal ethical clearance
The studies with mice were performed according to the guidelines of the Indian Animal Ethics Committee (IAEC) and Committee for the Purpose of Control and Supervision of Experiments on Animals (147/1999/CPSCEA).
Animal source
C57BL/6 mice were purchased from National Institute of Nutrition (NIN), Hyderabad, and reared in the Indian Institute of Chemical Biology animal house facility.
Cell line authentication
B16F10 cells were purchased from cell line repository of NCCS (National Centre for Cell Science), Pune, and maintained according to their recommendations.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional information This is a first-in-class report of a cationic liposome, PC-SA, depicting immune-regulating properties which are further increased when administered in combination with low doses of doxorubicin, thereby making a unique formulation, having the potential to cure metastasis.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
De, M., Ghosh, S., Asad, M. et al. Combining doxorubicin with stearylamine-bearing liposomes elicits Th1 cytokine responses and cures metastasis in a mouse model. Cancer Immunol Immunother 69, 1725–1735 (2020). https://doi.org/10.1007/s00262-020-02578-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-020-02578-9