Abstract
Autoinflammatory diseases are a family of disorders characterized by aberrant stimulation of inflammatory pathways without involvement of antigen-directed autoimmunity. They can be further divided in monogenic and polygenic types. Those without an identified genetic mutation are known as polygenic and include systemic-onset juvenile idiopathic arthritis, idiopathic recurrent acute pericarditis, Behçet syndrome, chronic recurrent multifocal osteomyelitis and inflammatory bowel disease among others. Autoinflammatory diseases are characterized by recurrent flares or persistent systemic inflammation and fever, as well as lymphadenopathy and cutaneous, abdominal, thoracic and articular symptoms. Although these syndromes can mimic infections clinically, the inflammatory lesions in autoinflammatory disorders are aseptic. However, because of their infrequency, varied and nonspecific presentation, and the new genetic identification, diagnosis is usually delayed. In this article, which is Part 2 of a two-part series, the authors review the main polygenic autoinflammatory diseases that can be seen in childhood, with special emphasis wherever applicable on imaging features that may help establish the correct diagnosis. However, the major role of imaging is to delineate organ involvement and disease extent.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As noted in Part 1 of this series, the term autoinflammatory disorders was originally used to differentiate autoimmune disorders from diseases with no specific autoantibodies or autoreactive lymphocytes, which were thought to be induced by innate rather than adaptive immune dysregulation [1]. However, today we know that there is overlap in the immunological characteristics of some of these entities with the classical autoimmune diseases [2].
Autoinflammatory diseases are further divided into monogenic and polygenic autoinflammatory syndromes, depending on whether there is an identified genetic mutation. Monogenic autoinflammatory syndromes are those with identified genetic mutations and are primarily errors of innate immunity. Those without an identified genetic mutation have a polygenic origin and include systemic-onset juvenile idiopathic arthritis, idiopathic recurrent acute pericarditis, Behçet syndrome, chronic recurrent multifocal osteomyelitis and inflammatory bowel disease [3].
The pathogenetic mechanisms underlying autoinflammation, although still unclear and different from each other from a molecular point of view, are responsible for an aberrant activation of the immune system resulting in involvement of multiple organs and systems. Symptoms are nonspecific and include recurrent flares or persistent systemic inflammation, fever, skin rashes, chest and abdominal pain, lymphadenopathy and arthritis. Because of the rarity of autoinflammatory diseases, their varied and nonspecific presentation, and the new genetic identification, diagnosis is usually delayed. Imaging can help provide clues for the diagnosis but the major role of imaging is to delineate organ involvement and disease extent.
In Part 2 of this series, we review the main polygenic autoinflammatory diseases in childhood, with special emphasis on imaging features that may be useful to reach the correct diagnosis.
Systemic-onset juvenile idiopathic arthritis
The systemic form of juvenile idiopathic arthritis is one of the most severe forms of juvenile idiopathic arthritis. According to the International League of Associations for Rheumatology criteria, systemic-onset juvenile idiopathic arthritis is characterized by arthritis with or preceded by at least 2 weeks of fevers that have been daily for at least 3 days, with at least one of the following: transitory rash, generalized lymphadenopathy, hepato- or splenomegaly, or serositis [4].
Arthritis, which is mandatory for a conclusive diagnosis, is not usually one of the presenting symptoms. In addition, the classical symmetrical and polyarticular joint involvement may not develop until late in the disease course [5]. Wrists, knees and ankles are frequently affected, although the hands, hips, cervical spine and temporomandibular joints can also be involved [6] (Fig. 1). Unlike the oligoarticular and polyarticular subtypes of juvenile idiopathic arthritis, the arthritis of systemic-onset juvenile idiopathic arthritis may start in the hips and can progress very rapidly, causing severe damage and dysfunction resulting in the need for early joint replacement surgery as well as loss of growth potential in younger patients. The imaging findings are summarized in Table 1. The main radiologic findings in systemic-onset juvenile idiopathic arthritis are juxta-articular osteopenia, joint space narrowing, erosions, growth abnormalities and even ankylosis (Fig. 2). Generalized delay in bone age is also common. Ultrasonography (US) is very helpful to evaluate tenosynovitis, which is common in children with polyarticular course and is characterized by increased fluid content within the tendon sheath and hypoechoic thickening of the synovial sheath with or without increased vascularity [6]. Magnetic resonance imaging (MRI) with intravenous contrast administration is the technique of choice to study arthritis [7]. It has the advantages of displaying both soft tissue and bone, being the most sensitive technique for detecting acute synovitis and tenosynovitis, and the only one able to identify bone marrow edema. Furthermore, it allows detection of changes in the joint over time and evaluates the effectiveness of therapeutic interventions. On MRI, tenosynovitis appears as increased fluid within the tendon sheath, with low or intermediate signal intensity on T1-weighted images and high signal intensity on T2-weighted images, or as increased enhancement of the tendon sheath. The most frequently affected tendons are the extensor tendons of the carpus, the flexor tendons of the fingers, the extensor tendons of the feet, and the posterior tibialis and peroneus tendons [6]. Occasionally, synovial cysts that communicate with the shoulder, elbow, wrist or knee joints are also seen [6]. Myositis is rare but can be identified by MRI [8].
Systemic-onset juvenile idiopathic arthritis in a 10-year-old girl with daily fever, arthralgias for 1 year and a history of pericarditis. a Posteroanterior radiograph of the chest and abdomen shows mediastinal widening (arrow) and hepatosplenomegaly (asterisks). b Axial contrast-enhanced computed tomography (CT) image of the chest confirms multiple enlarged mediastinal lymph nodes (arrows). c Axial contrast-enhanced CT image of the abdomen shows several enlarged lymph nodes at the splenic hilum (arrowheads). d, e Four years later, the child presented with deviation of the mandible to the right on the mouth opening. Sagittal T2-weighted gradient echo magnetic resonance imaging (MRI) of the right temporomandibular joint (d) shows an erosion in the mandibular condyle (arrowhead), bone marrow edema (arrow) and intra-articular high signal intensity that may represent joint effusion or synovial thickening (curved arrow). Axial contrast-enhanced fat-suppressed T1-weighted MRI of both temporomandibular joints (e) shows thickening and enhancement of the synovium on the right, consistent with active synovitis (curved arrow) combined with joint effusion (arrowhead). f Three years later, the child presented with left hip pain. Coronal contrast-enhanced fat-suppressed T1-weighted MRI of the hips shows left proximal femoral bone marrow enhancement and marked synovial thickening and enhancement of the left hip joint (arrow)
Systemic-onset juvenile idiopathic arthritis in an 11-year-old boy with left hand pain on flexion. a, b Anteroposterior radiograph (a) and coronal T1-weighted MRI (b) of the left hand show carpal and carpometacarpal joint bony ankylosis (arrowheads). There is also shortening and deformity of the left ulna (arrow in a). These are all sequelae of synovitis and erosive changes
Pericardial effusion is common and frequently asymptomatic, with no obvious cardiomegaly or typical electrocardiographic findings [9]. Myocarditis is much less common.
Pleural effusion, the most common chest manifestation, is frequently found incidentally on chest radiographs [6]. Interstitial lung disease, alveolar proteinosis and pulmonary hypertension are rare but are being reported with increasing frequency [10].
Lymphadenopathy and splenomegaly may occur alone or together and are characteristic of systemic-onset juvenile idiopathic arthritis (Fig. 1). Lymphadenopathy might be markedly enlarged and symmetrically distributed, especially in the cervical, axillary and inguinal regions, and thus it mimics the appearance of lymphoma [6]. Hepatomegaly is not as frequent as splenomegaly [6] (Fig. 1). Occasionally, a fatty liver can be seen secondary to glucocorticoid administration, but chronic hepatic disease generally does not occur.
Acute neurological episodes such as macrophage activation syndrome and posterior reversible encephalopathy syndrome are uncommon but serious complications in children with systemic-onset juvenile idiopathic arthritis [6]. Macrophage activation syndrome is an acute, life-threatening condition characterized by pancytopenia, disseminated intravascular coagulopathy, hepatic dysfunction and persistent fever resulting in multiorgan failure. Brain MRI may show intracranial hemorrhages and cerebral edema [11]. Posterior reversible encephalopathy syndrome consists of a neurotoxic state secondary to the inability of the circulation to autoregulate in response to acute changes in blood pressure [12]. MRI shows symmetrical brain edema at the watershed zones, most common in the parietal and occipital cortical and subcortical areas (Fig. 3). These findings are usually reversible.
Systemic-onset juvenile idiopathic arthritis and macrophage activation syndrome in a 10-year-old girl with seizures. a Coronal fluid-attenuated inversion recovery (FLAIR) MRI of the brain shows bilateral occipital cortical high signal intensity (arrows). b Axial diffusion-weighted MRI shows diffusion restriction of the bilateral occipital lesions (arrows). These findings are in keeping with posterior reversible encephalopathy syndrome
Treatment of systemic-onset juvenile idiopathic arthritis includes the use of nonsteroidal anti-inflammatory drugs, oral or intravenous glucocorticoids and biological agents.
Idiopathic recurrent acute pericarditis
The term recurrent pericarditis is used when there is a second episode of acute pericarditis after a period of at least 4 to 6 weeks from an initial episode with no symptoms in between [13]. If the symptoms last more than 3 months, it is then called chronic pericarditis [14].
The most frequent imaging finding is pericardial effusion (Table 1) (Fig. 4). Transthoracic echocardiography is generally the initial diagnostic imaging study performed in these children, but cardiac MRI is better suited to evaluate inflammatory changes. The presence and extent of late gadolinium enhancement of the pericardium are indicators of pericarditis and are useful in guiding the anti-inflammatory treatment [15].
Acute recurrent pericarditis in a 15-year-old boy with recurrent episodes of asthenia, fever and dyspnea. a Anteroposterior radiograph of the chest shows enlargement of the cardiac silhouette. b Axial contrast-enhanced CT image of the chest shows a large pericardial effusion (arrows) and bilateral pleural effusions (arrowheads). c Posteroanterior radiograph of the chest after treatment shows normal cardiac silhouette
In contrast to the first episode of acute pericarditis, treatment of idiopathic recurrent acute pericarditis should include a new course of nonsteroidal anti-inflammatory drugs with additional colchicine for 6 months. Anti-tumor necrosis factor-alpha drugs and Interleukin-1 blockade have also been used with good clinical response [16].
Behçet disease
Behçet disease is categorized as an inflammatory vascular disease affecting arteries and veins of all kinds and sizes, and is characterized by recurrent oral and genital aphthae, ocular, cutaneous, gastrointestinal, neurological, vascular and/or articular involvement [17].
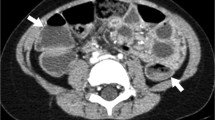
One of the major characteristic features of Behçet disease is the heterogeneity of the clinical presentation. Imaging findings in Behçet disease are summarized in Table 1. Barium study was traditionally useful in demonstrating the presence of deep, penetrating ulcers, which are characteristic radiographic features of this disease in the gastrointestinal tract. The progression of this penetrating disease may result in multiple complications, including perforation, fistula, hemorrhage and peritonitis [18]. Currently, computed tomography (CT) and MR enterography are used to diagnose Behçet disease, with typical findings including bowel wall thickening and enhancement associated with deep penetrating ulcers, particularly in the ileocecal region. Polypoid appearance of the intestinal surface and homogeneous enhancement of the small-bowel wall are more common in children with Behçet disease than in patients with Crohn disease [19]. A layered or stratified enhancement pattern, the presence of strictures, and the involvement of a long segment and, particularly, of more proximal ileal segments favor Crohn disease [19]. However, in the absence of extraintestinal manifestations, it may be impossible to differentiate intestinal Behçet disease from Crohn disease. On occasion, Behçet disease can manifest as a cecal mass or an aneurysmal dilatation of the terminal ileum mimicking a malignant tumor, particularly lymphoma [20,21,22].
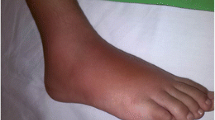
Cardiopulmonary and renal involvement is rare in children. Neurological manifestations may include encephalomyelitis or aseptic meningitis (Fig. 5), as well as dural sinus thrombosis (Fig. 6). Oligoarthritis is common, usually asymmetrical and nonerosive and most frequently affects medium and large joints including the knees, ankles, wrists and elbows. Myositis is uncommon. The vasculitis of Behçet disease is characterized by venous thrombosis and arterial occlusions or aneurysms [23, 24]. Thrombosis of the hepatic veins can result in Budd-Chiari syndrome [23, 24].
Behçet disease in a 10-year-old girl with recurrent fever and meningoencephalitis. a Coronal fluid-attenuated inversion recovery (FLAIR) MRI of the brain at presentation shows high signal intensity in the midbrain, extending into the cerebral peduncles and pons (arrow). There was associated leptomeningeal enhancement and central punctate enhancement at the right cerebral peduncle (not shown). b Coronal FLAIR MRI of the brain at the 7-month follow-up shows a normal appearance with resolution of the previous findings
Treatment of Behçet disease is variable, depending on the location and severity of involvement. Topical treatment with sucralfate suspension or corticosteroids is used initially for ulcers [23]. Prednisone is frequently the first treatment option for multiple manifestations. Azathioprine and biologics, mainly tumor necrosis factor-alpha blocking agents, are useful for uveitis. Low-dose methotrexate, azathioprine, anti-tumor necrosis factor agents and cyclophosphamide are helpful for central nervous system disease [23].
Chronic recurrent multifocal osteomyelitis
Chronic recurrent multifocal osteomyelitis, also named chronic nonbacterial osteomyelitis, is a rare type of skeletal inflammation that occurs mainly in children and adolescents, affects females more frequently and shows a worldwide distribution.
Chronic recurrent multifocal osteomyelitis remains a diagnosis of exclusion, as no specific diagnostic test is available [25]. Infectious osteomyelitis and neoplasms such as osteosarcoma, Ewing sarcoma, lymphoma, neuroblastoma, leukemia, Langerhans cell histiocytosis, osteoid osteoma and osteoblastoma are often part of the differential diagnosis (Table 2) [4, 25,26,27,28,29,30,31,32,33,34,35,36,37,38]. Multiple bone lesions, a relapsing-remittent course, involvement of locations not typical for infectious osteomyelitis, such as the clavicle, imaging findings in keeping with subacute or chronic osteomyelitis but with no abscess, fistula or sequestrum, absence of an infectious microorganism and improvement with nonsteroidal anti-inflammatory drugs but not antibiotics suggest the diagnosis [25, 39, 40]. In addition, chronic recurrent multifocal osteomyelitis may be associated with other inflammatory disorders of the skin, such as pustulosis palmoplantaris or acne, as well as gastrointestinal tract diseases, including inflammatory bowel disease, and vasculitis such as Takayasu arteritis and granulomatosis with polyangiitis (formerly known as Wegener granulomatosis) [25].
Chronic recurrent multifocal osteomyelitis is usually bilateral and multifocal at presentation but often lacks clinical and temporal symmetry [25]. Typical imaging findings (Table 1) consist of lytic and sclerotic metaphyseal lesions in the long bones, especially involving the lower extremities and the medial aspect of the clavicles (Fig. 7) [39]. In fact, involvement of the clavicles is one of the distinctive features of chronic recurrent multifocal osteomyelitis, which is a rare location for hematogenous osteomyelitis. In addition, excluding neoplastic processes, chronic recurrent multifocal osteomyelitis is the most frequent disease affecting the clavicle in children and young adults, as well as the most frequent pathology involving the medial third of the clavicle at any age [25]. As opposed to synovitis-acne-pustulosis-hyperostosis-osteitis (SAPHO) syndrome, clavicular disease in chronic recurrent multifocal osteomyelitis is not associated with the sternoclavicular joint. In addition to the clavicle and long bones, involvement of the vertebral bodies, pelvis, ribs, and mandible is also common [25].
Chronic recurrent multifocal osteomyelitis in a 15-year-old girl with left shoulder pain. a Posteroanterior radiograph of the upper chest shows enlargement and sclerosis of the medial aspect of the left clavicle (arrow), a common site of involvement in chronic recurrent multifocal osteomyelitis. b Axial CT image shows thickening of the left clavicle with a mixed pattern of lysis and sclerosis
At presentation, radiographs may be completely normal or show only osteopenia, however, MRI may show bone marrow edema at this stage. With time, radiographs typically show a metaphyseal osteolytic lesion abutting the growth plate demarcated by a thin sclerotic rim (Fig. 8) [41]. With disease progression, sclerosis gradually increases around the lytic lesion and therefore chronic lesions usually become mainly sclerotic with associated hyperostosis [25]. Lesions also occur in nontubular bones, in metaphyseal-equivalent regions adjacent to cartilage.
Chronic recurrent multifocal osteomyelitis in a 15-year-old boy with polyarticular pain that is more prominent in the right knee. a Anteroposterior radiograph of the right knee shows widening and irregularity of the medial aspect of the proximal tibial physis (arrowhead) and an ill-defined lesion in the adjacent metaphysis (arrow). b Coronal reformatted CT image of the right proximal tibia shows a focal lytic lesion at the medial aspect of the proximal metaphysis (arrow). c Coronal short tau inversion recovery (STIR) MRI of the knees shows increased signal intensity involving the proximal epiphysis, metaphysis and diaphysis of the right tibia (arrow), as well as the distal epiphysis of both femurs (arrowheads), more extensive on the left
MRI may suggest the diagnosis and show the typical periphyseal, multifocal pattern [42]. It can also detect clinically occult involvement and show the extension of the bone and soft-tissue lesions (Fig. 9). Whole-body MRI with short tau inversion recovery (STIR) images is the imaging technique of choice used at our institution as it allows identification of asymptomatic lesions and establishes a baseline of disease burden [43]. The protocol includes coronal images of the whole body and sagittal images of the spine. Whole-body imaging can also be done with Technetium-99 bone scintigraphy, which shows areas of increased uptake. However, MRI is preferred because of the lack of radiation and the better assessment of the anatomy and soft tissues [44]. Furthermore, the physiological uptake of the physis seen on the bone scan can be misleading. Positron emission tomography has been used clinically to detect chronic osteomyelitis, but its use in chronic recurrent multifocal osteomyelitis has not been described [45]. In addition to the typical metaphyseal involvement, accompanying epiphyseal lesions are also frequent [42]. Recognizing transphyseal involvement and secondary physeal bars is important as it allows identifying children at higher risk for growth deformities [25]. Diaphyseal involvement is rare, although it usually occurs next to the affected metaphyses [46]. MRI may show periostitis, inflammatory changes in the adjacent soft tissues, involvement of the physis and articular inflammation with synovitis, joint effusion and destructive changes within the joint cartilage and subchondral bone [25]. Active lesions typically show increased signal intensity on STIR and fat-suppressed T2-weighted images, decreased signal intensity on T1-weighted images, and increased apparent diffusion coefficient values on diffusion-weighted imaging [47]. MRI is also useful for follow-up, particularly when there is suspicion for inflammatory activity in children with marked sclerosis or hyperostosis. In these patients, areas of sclerosis with no superimposed inflammation appear hypointense on T1- and T2-weighted images [25]. Findings such as abscess, fistula or sequestrum are more characteristic of infectious osteomyelitis rather than chronic recurrent multifocal osteomyelitis.
Chronic recurrent multifocal osteomyelitis in an 11-year-old girl with a 3-week history of persistent left hip pain, daily fevers and weight loss. a Coronal STIR whole-body MRI at presentation shows hyperintense foci in the left acetabulum and adjacent iliac bone (long arrow) and ischium, adjacent soft tissues (arrowhead) and right medial femoral condyle (short arrow). There is also a small left-side hip joint effusion (curved arrow). b Coronal STIR whole-body MRI 4 months later shows significant improvement in the signal abnormality within the left acetabulum and ischium (arrow) and resolution of the signal abnormality within the right distal femoral epiphysis. New bone marrow hyperintense foci are seen in the bilateral proximal tibial metaphyses (arrowheads)
Nonsteroidal anti-inflammatory drugs represent the initial treatment option. Second-line treatment agents include corticosteroids, azathioprine, disease-modifying antirheumatic drugs, bisphosphonates, biologics, mainly tumor necrosis factor-alpha and Interleukin-1 blocking agents, and other immune modulators [41].
Inflammatory bowel disease
Inflammatory bowel disease is a chronic, relapsing autoinflammatory disease of the gastrointestinal tract, and is often categorized in three subtypes: Crohn disease, ulcerative colitis and unclassified [48]. Inflammatory bowel disease has a prevalence of 1 in 1,000 inhabitants in Western countries [48]. Approximately 25% of inflammatory bowel disease occurs in children [49], in whom Crohn disease tends to be more common than ulcerative colitis, especially in males [48].
Symptoms at presentation in children are diverse and include abdominal pain, diarrhea (with or without bloody stools), perianal lesions, growth retardation and weight loss [48]. Extraintestinal manifestations may be seen, including hepatobiliary, pancreatic, genitourinary, musculoskeletal, pulmonary, cardiac, ocular and dermatological symptoms.
Ulcerative colitis and Crohn disease have distinctive characteristics that help to establish a specific diagnosis. Crohn disease can involve the gastrointestinal tract from mouth to anus with multiple inflammatory lesions separated by normal bowel segments. In addition, these lesions may involve the entire bowel wall from the mucosa to serosa causing deep ulcerations and local complications, such as abscesses and fistulas [48]. Bowel strictures are also relatively frequent in Crohn disease. In contrast, in ulcerative colitis, lesions are limited to the mucosa and to the large bowel, and perianal lesions are uncommon and limited [48]. Unclassified inflammatory bowel disease refers to colitis with equivocal features for Crohn disease or ulcerative colitis.
The diagnosis of inflammatory bowel disease requires correlation of clinical, biological, endoscopic, histological and imaging findings [48] as shown in the revised Porto criteria proposed by the European Society for Paediatric Gastroenterology Hepatology and Nutrition [50, 51] and exclusion of potential mimickers (Table 3) [19, 52,53,54,55,56,57,58]. US and MRI are the imaging techniques most frequently used to diagnose and manage inflammatory bowel disease in children, although radiography, fluoroscopic studies and CT may also be useful [59]. The imaging findings in inflammatory bowel disease are summarized in Table 1. Transabdominal US may detect bowel inflammation and evaluate the severity and extent of the disease although its value is limited for the small bowel compared to MR enterography. Increased bowel wall thickness (>3 mm) is the main sonographic finding (Fig. 10) [60]. Other sonographic findings include hyperemia, abnormal bowel wall echogenicity, abnormal bowel margin, increased echogenicity of the surrounding fat and lymphadenopathy [50]. US may also depict complications such as inflammatory mass (phlegmon/abscess), stricture, sinus tract and fistula. MR enterography and CT have similar indications and diagnostic performance, but MR enterography is preferred in children due to the lack of ionizing radiation [50, 60]. MRI of the bowel needs fast acquisition techniques and luminal distension [61]. The main MRI findings are mural enhancement, wall thickening, intramural edema (T2 hyperintensity), ulcerations, sacculations, stricture, fistula, sinus tract, inflammatory phlegmon, abscess (fluid collection with enhancing rim with or without air, with diffusion restriction), perienteric edema/engorged vasa recta (comb sign), and mesenteric venous thrombosis [60] (Fig. 11). Diminished peristalsis may also be present in small bowel Crohn disease [62]. Extraintestinal findings such as sacroiliitis, sclerosing cholangitis, avascular necrosis, pancreatitis, nephrolithiasis, cholelithiasis and perianal disease can also be depicted.
Crohn disease in a 16-year-old boy with symptoms of small bowel obstruction. a Transverse sonogram of the right lower quadrant of the abdomen shows marked wall thickening of the terminal ileum (arrow), measuring 0.61 cm, with increased echogenicity of the adjacent fat (asterisk). b Transverse sonogram with color Doppler interrogation shows marked hyperemia of the thickened bowel wall, which is considered a sign of disease activity
Crohn disease in a 9-year-old girl with abdominal pain and diarrhea. a Coronal fat-suppressed T2-weighted image shows marked wall thickening and edema of the terminal ileum (arrow). b Coronal diffusion-weighted MRI (b=800 s/mm2) shows thickening and increased signal intensity of the terminal ileum (arrowhead). c Coronal apparent diffusion coefficient map MRI shows the corresponding hypointensity of the terminal ileum consistent with marked diffusion restriction (arrowhead). d Axial fat-suppressed contrast-enhanced T1-weighted MRI shows increased enhancement of the thickened terminal ileum (curved arrow) denoting inflammation
The current goals of treatment in inflammatory bowel disease are to eliminate symptoms and restore quality of life, restore normal growth and eliminate complications. Corticosteroids, enteral nutrition therapy, aminosalicylates, immunomodulators, anti-tumor necrosis factor therapy and surgery are the main therapeutic options [63].
Conclusion
Autoinflammatory diseases include a broad spectrum of disorders with a wide variety and, often, nonspecific presentations. Imaging provides clues for diagnosis and is useful to assess organ involvement and disease extent. Systemic-onset juvenile idiopathic arthritis is associated with arthritis, lymphadenopathy, hepatosplenomegaly and serositis. Idiopathic recurrent pericarditis is characterized by recurrent pericardial effusions. Behçet disease is characterized by deep penetrating ulcers, particularly in the ileocecal region, neurological vascular and articular involvement. Multiple bone lesions with predilection for the metaphyses of the lower extremities and the medial clavicles are typical of chronic recurrent multifocal osteomyelitis. Bowel wall thickening is the main finding in inflammatory bowel disease, although abdominal complications and extraintestinal findings may be detected on imaging.
References
McDermott MF, Aksentijevich I, Galon J et al (1999) Germline mutations in the extracellular domains of the 55 kda TNF receptor, TNFR1, define a family of dominantly inherited autoinflammatory syndromes. Cell 97:133–144
Almeida de Jesus A, Goldbach-Mansky R (2013) Monogenic autoinflammatory diseases: concept and clinical manifestations. Clin Immunol 147:155–174
Masters SL, Simon A, Aksentijevich I, Kastner DL (2009) Horror autoinflammaticus: the molecular pathophysiology of autoinflammatory disease. Annu Rev Immunol 27:621–668
Petty RE, Southwood TR, Manners P et al (2004) International league of associations for rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 31:390–392
Sheybani EF, Khanna G, White AJ, Demertzis JL (2013) Imaging of juvenile idiopathic arthritis: a multimodality approach. Radiographics 33:1253–1273
De Benedetti F, Schneider R (2016) Systemic juvenile idiopathic arthritis. In: Petty RE, Laxer RM, Lindsley CB, Wedderburn LR (eds) Textbook of pediatric rheumatology, 7th edn. Elsevier, Philadelphia, pp 205–216
Sudoł-Szopińska I, Jurik AG, Eshed I et al (2015) Recommendations of the ESSR arthritis subcommittee for the use of magnetic resonance imaging in musculoskeletal rheumatic diseases. Semin Musculoskelet Radiol 19:396–411
Miller ML, Levinson L, Pachman LM, Poznanski A (1995) Abnormal muscle MRI in a patient with systemic juvenile arthritis. Pediatr Radiol 25:S107–S108
Bernstein B, Takahashi M, Hanson V (1974) Cardiac involvement in juvenile rheumatoid arthritis. J Pediatr 85:313–317
Kimura Y, Weiss JE, Haroldson KL et al (2013) Pulmonary hypertension and other potentially fatal pulmonary complications in systemic juvenile idiopathic arthritis. Arthritis Care Res 65:745–752
Bennett TD, Fluchel M, Hersh AO et al (2012) Macrophage activation syndrome in children with systemic lupus erythematosus and children with juvenile idiopathic arthritis. Arthritis Rheum 64:4135–4142
Zhang P, Li X, Li Y et al (2015) Reversible posterior leukoencephalopathy syndrome secondary to systemic-onset juvenile idiopathic arthritis: a case report and review of the literature. Biomed Rep 3:55–58
Adler Y, Charron P, Imazio M et al (2015) 2015 ESC guidelines for the diagnosis and management of pericardial diseases. Rev Esp Cardiol (Engl Ed) 68:1126
Xu B, Kwon DH, Klein AL (2017) Imaging of the pericardium: a multimodality cardiovascular imaging update. Cardiol Clin 35:491–503
Cremer PC, Tariq MU, Karwa A et al (2015) Quantitative assessment of pericardial delayed hyperenhancement predicts clinical improvement in patients with constrictive pericarditis treated with anti-inflammatory therapy. Circ Cardiovasc Imaging 8:e003125
Lilly LS (2013) Treatment of acute and recurrent idiopathic pericarditis. Circulation 127:1723–1726
Siddiqui B, Fernandes D, Chaucer B et al (2016) Behcet's disease in acquired immune deficiency syndrome. IDCases 3:3–4
Chung SY, Ha HK, Kim JH et al (2001) Radiologic findings of Behçet syndrome involving the gastrointestinal tract. Radiographics 21:911–924
Peker E, Erden A, Erden İ, Düzgün N (2018) Intestinal Behçet disease: evaluation with MR enterography–a case-control study. AJR Am J Roentgenol 211:767–775
Chae EJ, Do KH, Seo JB et al (2008) Radiologic and clinical findings of Behçet disease: comprehensive review of multisystemic involvement. Radiographics 28:e31
Park MJ, Lim JS (2013) Computed tomography enterography for evaluation of inflammatory bowel disease. Clin Endosc 46:327–366
D'Angelo T, Gallizzi R, Romano C et al (2017) Magnetic resonance enterography findings of intestinal behçet disease in a child. Case Rep Radiol 2017:8061648
Ozen S (2016) Behçet disease. In: Petty RE, Laxer RM, Lindsley CB, Wedderburn LR (eds) Textbook of pediatric rheumatology, 7th edn. Elsevier, Philadelphia, pp 526–532
Krupa B, Cimaz R, Ozen S et al (2011) Pediatric Behcet's disease and thromboses. J Rheumatol 38:387–390
Khanna G, Sato TS, Ferguson P (2009) Imaging of chronic recurrent multifocal osteomyelitis. Radiographics 29:1159–1177
Girschick HJ, Zimmer C, Klaus G et al (2007) Chronic recurrent multifocal osteomyelitis: what is it and how should it be treated? Nat Clin Pract Rheumatol 3:733–738
Chang CY, Rosenthal DI, Mitchell DM et al (2016) Imaging findings of metabolic bone disease. Radiographics 36:1871–1887
Offiah AC, Vockley J, Munns CF, Murotsuki J (2019) Differential diagnosis of perinatal hypophosphatasia: radiologic perspectives. Pediatr Radiol 49:3–22
Jaramillo D, Dormans JP, Delgado J et al (2017) Hematogenous osteomyelitis in infants and children: imaging of a changing disease. Radiology 283:629–643
Chai JW, Hong SH, Choi JY et al (2010) Radiologic diagnosis of osteoid osteoma: from simple to challenging findings. Radiographics 30:737–749
Murphey MD, Senchak LT, Mambalam PK et al (2013) From the radiologic pathology archives: Ewing sarcoma family of tumors: radiologic-pathologic correlation. Radiographics 33:803–831
Murphey MD, Robbin MR, McRae GA et al (1997) The many faces of osteosarcoma. Radiographics 17:1205–1231
Glotzbecker MP, Kersun LS, Choi JK et al (2006) Primary non-Hodgkin's lymphoma of bone in children. J Bone Joint Surg Am 88:583–594
Krishnan A, Shirkhoda A, Tehranzadeh J et al (2003) Primary bone lymphoma: radiographic-MR imaging correlation. Radiographics 23:1371–1383
Spijkers S, Littooij AS, Humphries PD et al (2019) Imaging features of extranodal involvement in paediatric Hodgkin lymphoma. Pediatr Radiol 49:266–276
Navarro SM, Matcuk GR, Patel DB et al (2017) Musculoskeletal imaging findings of hematologic malignancies. Radiographics 37:881–900
Chu CM, Rasalkar DD, Hu YJ et al (2011) Clinical presentations and imaging findings of neuroblastoma beyond abdominal mass and a review of imaging algorithm. Br J Radiol 84:81–91
Zaveri J, La Q, Yarmish G, Neuman J (2014) More than just Langerhans cell histiocytosis: a radiologic review of histiocytic disorders. Radiographics 34:2008–2024
Falip C, Alison M, Boutry N et al (2013) Chronic recurrent multifocal osteomyelitis (CRMO): a longitudinal case series review. Pediatr Radiol 43:355–375
Rossi A (2015) Infectious and inflammatory diseases of the spine in children. In: Rossi A (ed) Pediatric neuroradiology. Springer, Berlin, Heidelberg, pp 1–55
Ferguson PJ, Laxer RM (2016) Autoinflammatory bone disorders. In: Petty RE, Laxer RM, Lindsley CB, Wedderburn LR (eds) Textbook of pediatric rheumatology, 7th edn. Elsevier, Philadelphia, pp 627–641
Fritz J, Tzaribatchev N, Claussen CD et al (2009) Chronic recurrent multifocal osteomyelitis: comparison of whole-body MR imaging with radiography and correlation with clinical and laboratory data. Radiology 252:842–851
Chen HC, Wuerdeman MF, Chang JH, Nieves-Robbins NM (2018) The role of whole-body magnetic resonance imaging in diagnosing chronic recurrent multifocal osteomyelitis. Radiol Case Rep 13:485–489
Kennedy MT, Murphy T, Murphy M et al (2012) Whole body MRI in the diagnosis of chronic recurrent multifocal osteomyelitis. Orthop Traumatol Surg Res 98:461–464
Jurriaans E, Singh NP, Finlay K, Friedman L (2001) Imaging of chronic recurrent multifocal osteomyelitis. Radiol Clin N Am 39:305–327
Jurik AG (2004) Chronic recurrent multifocal osteomyelitis. Semin Musculoskelet Radiol 8:243–253
Leclair N, Thörmer G, Sorge I et al (2016) Whole-body diffusion-weighted imaging in chronic recurrent multifocal osteomyelitis in children. PLoS One 11:e0147523
Hugot JP, Bellaiche M (2007) Inflammatory bowel diseases: the paediatric gastroenterologist's perspective. Pediatr Radiol 37:1065–1070
Griffiths AM (2004) Specificities of inflammatory bowel disease in childhood. Best Pract Res Clin Gastroenterol 18:509–523
Levine A, Koletzko S, Turner D et al (2014) ESPGHAN revised Porto criteria for the diagnosis of inflammatory bowel disease in children and adolescents. J Pediatr Gastroenterol Nutr 58:795–806
Athanasakos A, Mazioti A, Economopoulos N et al (2015) Inflammatory bowel disease-the role of cross-sectional imaging techniques in the investigation of the small bowel. Insights Imaging 6:73–83
Navarro OM, Siegel MJ (2019) Gastrointestinal tract. In: Siegel MJ (ed) Pediatric sonography, 5th edn. Wolters Kluwer Health, Philadelphia, pp 346–395
Khanna G, Kao SC, Kirby P, Sato Y (2005) Imaging of chronic granulomatous disease in children. Radiographics 25:1183–1195
Katre RS, Sunnapwar A, Restrepo CS et al (2016) Cardiopulmonary and gastrointestinal manifestations of eosinophil-associated diseases and idiopathic hypereosinophilic syndromes: multimodality imaging approach. Radiographics 36:433–451
Khanna G, Sargar K, Baszis KW (2015) Pediatric vasculitis: recognizing multisystemic manifestations at body imaging. Radiographics 35:849–865
Bandyopadhyay R, Sinha SK, Chatterjee U et al (2011) Primary pediatric gastrointestinal lymphoma. Indian J Med Paediatr Oncol 32:92–95
Abramson SJ, Price AP (2008) Imaging of pediatric lymphomas. Radiol Clin N Am 46:313–338
Stringer DA, Cleghorn GJ, Durie PR et al (1986) Behçet's syndrome involving the gastrointestinal tract - a diagnostic dilemma in childhood. Pediatr Radiol 16:131–134
Masselli G, Mastroiacovo I, De Marco E et al (2016) Current tecniques and new perpectives research of magnetic resonance enterography in pediatric Crohn's disease. World J Radiol 8:668–682
Panes J, Bouhnik Y, Reinisch W et al (2013) Imaging techniques for assessment of inflammatory bowel disease: joint ECCO and ESGAR evidence-based consensus guidelines. J Crohns Colitis 7:556–585
Greer ML (2016) How we do it: MR enterography. Pediatr Radiol 46:818–828
Bruining DH, Zimmermann EM, Loftus EV Jr et al (2018) Consensus recommendations for evaluation, interpretation, and utilization of computed tomography and magnetic resonance enterography in patients with small bowel Crohn's disease. Gastroenterology 154:1172–1194
Rosen MJ, Dhawan A, Saeed SA (2015) Inflammatory bowel disease in children and adolescents. JAMA Pediatr 169:1053–1060
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Navallas, M., Inarejos Clemente, E.J., Iglesias, E. et al. Autoinflammatory diseases in childhood, part 2: polygenic syndromes. Pediatr Radiol 50, 431–444 (2020). https://doi.org/10.1007/s00247-019-04544-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-019-04544-9