Abstract
The pathomechanism of male idiopathic osteoporosis (MIO) differs from postmenopausal osteoporosis with regard to alterations in osteoblast activity. We evaluated intravenous ibandronate (IBN) in 25 MIO patients with fragility fractures in a prospective, monocentric, single-arm, and open-label study for 24 months. The impact and changes of sclerostin (Scl), Dickkopf-1 (DKK-1), CTX, and PINP were examined. Additionally, volumetric cortical, trabecular and areal bone mineral density (BMD), trabecular bone score (TBS), and finite element analyses (FEA) were evaluated. Compared to baseline, median Scl levels were increased after 1 month (Δ 121 %, p < 0.0001) and remained elevated for 12 months. DKK-1 decreased (p < 0.001) to a lesser extent until month 9 with values comparable to baseline at study endpoint. Early changes (baseline–month 1) of Scl negatively correlated with early changes of DKK-1 (−0.72), CTX (−0.82), and PINP (−0.55; p < 0.005 for all). The overall changes over the 24 months study period of Scl negatively correlated with decreased CTX (−0.32) and DKK-1 levels (−0.57, p < 0.0001 for both); CTX and PINP changes positively correlated at each time point (p < 0.001). Volumetric hip BMD increased by 12 and 18 %, respectively (p < 0.0001 for both). Cross-sectional moment of inertia and section modulus for total hip significantly improved (p < 0.05 for all). Areal BMD at total hip, spine, and TBS increased. FEA displayed an increase in bone strength both in the hip (17 %) and vertebrae (13 %, all p < 0.0001) at anatomical sites susceptible for fragility fracture. IBN increases Scl and improves cortical and trabecular bone strength with early and ongoing vigorous suppression of bone resorption.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Male idiopathic osteoporosis (MIO) is a disease of multifactorial etiology with a distinct genetic component. This condition is characterized by low trabecular bone volume, enlarged bone marrow space, and increased fracture risk in the absence of secondary causes for osteoporosis [1]. Although the detailed pathophysiology of MIO has yet to be fully defined, evidence increasingly suggests an osteoblastic defect as the underlying cause [2]. Bone biopsies from patients with MIO showed abnormally low matrix mineralization densities and a deficit in osteoblasts suggesting an inherent mineralization defect contributing to bone fragility [3].
MIO was found to be associated with subclinical alterations in sex-hormones as well as changes in the insulin-like growth factor 1 (IGF-1) pathway [4–7] and alterations in sclerostin production [2, 8, 9]. Recently, in elderly MIO patients, extensive microstructural changes in the subcortical region of the femoral neck as well as decreased trabecular and cortical bone volume were reported with prevalent hip fractures compared to male patients with osteoarthritis. These changes were caused by altered gene expression of RUNX2 and Osterix in the osteoblast cell lineage and decreased mineralization [10, 11].
Intravenous ibandronate (IBN) is an established first line treatment in postmenopausal osteoporosis. IBN has been shown to improve bone mineral density (BMD) and reduce fragility fractures in this patient group. Furthermore, IBN improved cortical bone structure and to a lesser extent trabecular bone structure in osteopenic women as assessed by HR-pQCT [12, 13].
In a recent study, levels of sclerostin and bone turnover markers were analyzed in two trials in postmenopausal women treated with zoledronic acid with various outcomes on sclerostin levels [14, 15].
We evaluated the long-term effects of IBN in patients with MIO and prevalent fragility fractures.
Hypothesis and Objectives
We tested the hypothesis that quarterly treatment with 3 mg of intravenous IBN for 24 months in male patients with MIO and fragility fractures would strongly increase BMD and biomechanical properties of bone which is reflected by serum changes of sclerostin Scl, DKK-1, CTX, and PINP.
The primary objective of this study was to investigate changes in bone turnover markers, sclerostin, DKK-1 PINP, and CTX.
Secondary objectives included (i) monitoring changes in cortical and trabecular volumetric hip bone mineral density, (ii) changes in hip and vertebral strength using finite element analysis (FEA), (iii) changes in biomechanical hip parameters assessed by vBMD, (iv) changes in areal vertebral and hip bone mineral density assessed by DXA, (v) changes in trabecular bone score (TBS), and (vi) changes of FEA parameters and bone sites susceptible for fragility fracture during treatment (month 24 vs. baseline).
Materials and Methods
Patients and Study Design
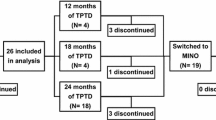
This was a prospective, monocentric, single-arm, and open-label study in patients with MIO and fragility fractures who were treated with intravenous IBN for 24 months (TOMIBA-trial, EudraCt number 2006-006692-20). Paired biopsy micro-CT data were previously reported [3, 11]. Inclusion criteria were adapted from major interventional trials in male osteoporosis and consisted of either (1) a femoral neck T-score of −2.0 or less and a lumbar spine T-score of −1.0 or less or (2) a femoral neck T-score of −1.0 or less and at least one prevalent osteoporotic fracture (i.e., at least one vertebral fracture grade I according to the Genant criteria or one low-trauma peripheral fracture). [3, 11, 16]. Patients were not included if they had at least one concomitant known disease which negatively affects bone metabolism: any systemic or local inflammatory or autoimmune disease, any type acute or chronic liver disease, type 1 or type 2 diabetes mellitus, hypo- or hyperthyroidism, depression, alcohol intake >2 IU/day, smoking >10 cigarettes/day, coronary heart disease, cardiomyopathy, ankylosing spondylitis, osteogenesis imperfecta, depression, eating disorders, chronic malnutrition or malabsorption, hemochromatosis, chronic obstructive pulmonary disease, Cushing’s disease, hypogonadism, body mass index ≤20 kg/m2, any stage of hyperparathyroidism, hypoparathyroidism, serum calcium or phosphate levels outside range of normal, any stage of chronic kidney disease, immunosuppression, any medical history of malignoma, and/or chemotherapy/radiation therapy.
The study was performed at the St. Vincent Hospital, Medical Department II, in Vienna, Austria in cooperation with the Institute for Lightweight Design and Structural Biomechanics at the University of Technology in Vienna, Austria (finite element analysis and fall simulations).
The study was approved by the local ethics committee. All patients were prospectively recruited; a written informed consent document was signed prior to any study-related procedures.
Study participants were treated with IBN, 3 mg/3 mL intravenously every 3 months for 24 months. Prior to IBN treatment, patients received vitamin D loading (i.e., cholecalciferol, 16,000 IU/week and calcium carbonate 500 mg/d) for 8 weeks. This procedure was continued during the entire 24 month study period.
Serum markers of bone turnover were determined at baseline, months 1, 3, and every 3 months thereafter until study end. Quantitative computed tomography (QCT) and paired transiliac biopsies were taken at baseline and study end after 24 months. Dual Energy X-ray Absorptiometry (DXA) scans of the total hip, femoral neck, and lumbar spine were performed at baseline and months 6, 12, 18, and 24.
Blood Samples/Bone Turnover Marker
Blood sampling was performed between 8 and 10 a.m. after an overnight fast. Samples were immediately centrifuged, cooled, and stored at −70 °C for later analysis.
The sclerostin (Scl) and Dickkopf-1 (DKK-1) levels from serum were quantitatively determined using an established enzyme immunoassay (EIA) kit (intra-assay coefficient of variation (CV) is 5–6 % for sclerostin and 4–7 % for DKK-1; Biomedica, Vienna, Austria). Crosslaps (CTX), Procollagen type 1 Amino-terminal Propeptide (PINP), intact parathyroid hormone (PTH), and 25- hydroxyvitamin D (25-OH vitamin D) were measured via chemoluminescence on the IDS-iSYS microparticle immunoassay system (Immunodiagnostics Systems Ltd., Boldon, UK). The intra-/inter-assay coefficients of variation were as follows: CTX 2.1–4.9 %; PINP 2.6–3.0 %; PTH 1.1–3.7 %; and 25(OH) Vitamin D 5.5–7.1 %. Total serum calcium levels were photometrically determined on the Architect ci8200 platform (Abbott Laboratories, Abbott Park, US-IL).
Areal BMD
Areal BMD at the hip and vertebrae was measured using a DXA scanner (GE LUNAR iDXA, software version Encore 13, 50,040, GE LUNAR Corporation, Madison, WI, USA). The in vivo coefficient of variation (CV) for the spine was 0.41 and 0.53 % for total hip. All daily quality control procedures and DXA measurements were taken by two well-trained IOF-ISCD certified technicians.
Trabecular Bone Score (TBS)
The DXA files of the male study population were digitally exported; and the raw data were extracted to a specific workstation for trabecular bone score (TBS) calculation using TBS iNsight software (Medimaps SA, France). TBS was calculated as mean value of the measurement for vertebrae L1–L4 (excluding fractured vertebrae) at exactly the same region of interest at spine BMD with the manufacturer´s beta version for male reference values (to date, unreleased). TBS is an index that classifies trabecular microstructure obtained through texture patterns. Reported in vivo precision for TBS ranges from 1.1 to 1.8 % [17]. According to reference values in postmenopausal women, TBS values >1.300 were considered normal [18].
Volumetric BMD
Volumetric BMD at the hip and at the lumbar spine (reference vertebra L2) was measured with a 128 row multidetector CT scanner (MX8000, Philips, Best, Netherlands) with a CT slice thickness of 1.0 mm (ultra high resolution—UHR mode). Values of density were calibrated against the K2HPO4 standard implemented in five phantoms (from 0 to 800 mg/cm3) dedicated to perform automatic error corrections of CT field inhomogeneities as well as synchronous patient calibrations of HU values toward bone density measured in mg/cm3. The CV for total hip was 0.79 % and 0.97 for vertebral body. Variables related to bone density were retrieved using Mindways QCT Pro Version 5.0A 3D CTXA Hip for standard hip analysis, and Mindways QCT Pro BIT Version 2.0 for additional vertebral analyses. (Mindways Software, Inc., Austin, TX, USA). Non-fractured vertebral bodies (reference vertebra L2) were segmented by an automatic algorithm, and each patient-related examination was cross-checked by two independent radiologists without any knowledge of the study protocol to ensure the identical regions of interest in the baseline and follow-up measurements. The CTXA Hip module allowed after exact 3D rotation of the femur for the determination of both three-dimensional cortical and trabecular values as well as their projected areal densities. The outer cortical volumetric BMD thresholds were individually adapted to each scan to avoid partial-volume effects caused by constant threshold settings. The BIT software module was used to obtain hip variables with a biomechanical context at the cross-sectional moment of inertia (CSMI), section modulus, and cortical and trabecular variables over sectors of slices through the femur. Both CSMI and section modulus are measures of bone strength with regard to bending. In contrast to CSMI, section modulus includes the distribution of bone mass, i.e., the distance of bone mass to the center of the bone.
Finite Element Analysis (FEA)
Baseline and follow-up hip and spine UHR-QCT scans were evaluated for FEA simulations with a recently published model [19, 20]. The unfractured L2 vertebra was selected for the analysis of the spine. The left hip was selected as the reference site. For patients with previous hip fracture, the right femur was calculated. The QCT images were calibrated, segmented, and converted into finite element models, using linear hexahedral elements. The initial image resolution of 0.37 × 0.37 × 0.4 mm was resampled to a finite element size of 2.97 × 2.97 × 3.2 mm (femur) and 1.48 × 1.48 × 1.60 mm (vertebra). Density-dependent bone material behavior was assigned to each element based on local QCT BMD values and a published calibration law [24]. Baseline and follow-up QCT images of hip and spine were segmented, masked, cross-linked, and registered. The axes of femoral neck/shaft and the vertebral bodies were rotated to ensure the exact rotation angle and orientation for evaluation of both measurements. Simulated falls on the trochanter major region and uniaxial compression forces on the vertebral head endplates were calculated for the estimation of bone strength and resistance toward virtually applied force. Relations between bone volume fraction (BV/TV) and material parameters as well as the material constants were calculated.
Statistical Analyses
The study was designed to enroll approximately 25 patients. Twenty finishers would have at least 80 % power to detect a mean within a group difference of 0.0225 g/cm2 in areal lumbar spine BMD, assuming a standard deviation (SD) of 0.043 g/cm2. Continuous outcome variables were described by the median [interquartile range]. Cumulative changes in variable values from baseline measurements up to 24 months were tested for statistical significance using the unpaired t test or the nonparametric Wilcoxon signed-rank test in case of non-normally distributed differences. When analyzing the complete time course of biochemical markers, repeated measures ANOVA models with bias corrections were performed. Multiple evaluations were done using the Dunnett test, comparing the values at each visit to the baseline measurement. The Pearson correlation coefficients were calculated and used to describe correlations between the relevant outcome variables and to evaluate the association between the changes in these variables. The partial Pearson correlation coefficient was also calculated for the early changes between baseline values and month 1. Log-transformed values were used for statistical analyses of variables with skewed distributions.
Two-sided p values <0.05 were considered as indicating statistical significance. The SAS software (version 9.4, SAS Institute Inc., 2002–2012; Cary, NC, USA) was used for data analyses.
Results
Patient Characteristics
Twenty-five patients with MIO participated in this study. Baseline characteristics of these patients are given in Table 1. T-scores at the lumbar spine, femoral neck, and total hip were in the osteoporotic or osteopenic range. Seventeen patients (68 %) had sustained at least one vertebral fracture, ten (40 %) at least one non-vertebral fracture, and two subjects (8 %) a hip fracture.
All investigated median serum laboratory values, sexual hormone concentrations, and prostate-specific antigen (PSA) were within the normal ranges. Serum markers of bone turnover marker revealed median Scl, DKK-1, CTX, and PINP levels within the lower normal male reference range. After 8 weeks of loading, all vitamin D levels were above the threshold of 30 ng/mL. (Table 1). The mean time from fragility fracture to initiation of treatment was 8 ± 2 months.
Volumetric BMD Hip
Biomechanical bone parameters were evaluated by QCT at baseline and month 24. During this period, cortical and trabecular volumetric hip BMD increased by 12 and 18 %, respectively (p < 0.0001 for both; Fig. 1; Table 2). Concurrently, average trabecular vertebral vBMD increased by 18 % (p < 0.05). After 24 months of IBN therapy, CSMI and section modulus for total and for cortical hip were significantly increased (p < 0.05 for all values; Table 2). Cross-sectional area of cortical total hip structures (after exclusion of trabecular structures) improved (+4.3 %, p < 0.001), but not so for CSA of total hip (+2.1 %, p = 0.138).
Median concentration (25:75 % quartile) of fasting serum bone turnover markers. a sclerostin; b Dickkopf-1 (DKK-1); c serum type 1 collagen cross-linked C-telopeptide (CTX); d intact amino-terminal propeptide of type I procollagen (PINP). Repeated measures (ANOVA); *p < 0.0001 versus baseline; #p < 0.001 versus baseline; †p < 0.005 versus baseline
Bone Turnover Markers
One month after the first IBN infusion, median sclerostin levels increased by Δ + 121 % (p < 0.0001) and linearly decreased thereafter (Fig. 2). Compared to baseline, Scl concentration continued to be higher throughout the 24 month study period, with a non-significant 16 % increase at month 24 versus baseline (Table 2). DKK-1 levels declined and remained low for 6 months after the first IBN injection (p < 0.0001 vs. baseline) and then increased to serum values comparable to baseline (Δ 21 %, p = n.s.).
Within 1 month of the initiation of IBN therapy, values of serum CTX (Δ − 60 %, p < 0.001) and to lesser extent PINP (Δ − 28 %, p < 0.05) decreased and remained at a lower level throughout the study (Fig. 2). After 24 months of IBN therapy, median CTX and PINP concentrations were significantly lower compared to baseline of 48 and 60 %, respectively (p < 0.0001 and p < 0.001; Table 2).
Calcium, albumin-adjusted calcium, iPTH, 25(OH) vitamin D, and alkaline phosphatase levels decreased during the study. These changes were not significant and values remained within the normal range. Likewise, phosphate levels slightly increased. In addition, there were no changes in testosterone and SHBG levels during the study (Table 2).
Correlations Between Bone Turnover Markers
Partial correlations and cumulative correlations between bone turnover markers were calculated for early changes (baseline–month 1) as well as for changes from baseline over the entire study period. Partial correlation analysis of changes from baseline to week 4 revealed a significant negative correlation between Scl in one case and CTX and PINP in the other, −0.83 and −0.56, respectively (p < 0.0001 and p = 0.0032). DKK-1 negatively correlated with Scl (−0.72, p < 0.0001) and positively correlated with CTX (0.63, p = 0.0006), but not with PINP. Patients with a strong reduction in CTX and/or PINP tended to have a much more pronounced increase in Scl levels, though the correlation was stronger for CTX compared to PINP. No correlation was detected between iPTH and Scl, but a negative correlation was observed between iPTH and PINP (−0.52; p = 0.007). In addition, CTX and PINP correlated both at month 1 and after 24 months (0.59 and 0.51, p < 0.005, respectively).
Over the entire study period, an ongoing significant negative correlation between Scl and CTX was still present, but at a much lower level (−0.32, p < 0.0001) when compared the early correlations. Scl negatively correlated with DKK-1 (−0.57, p < 0.0001), but correlations between Scl and PINP, and PINP and iPTH were no longer significant (Table 3).
Finite Element Analysis (FEA)
FEA of the UHR-QCT scans showed an increase in bone strength both at hip and vertebrae of 17 % (p < 0.001 for both; Table 2). Correspondingly, bone volume fraction (BT/TV) increased at hip and vertebrae by 13 and 8 %, respectively (both p < 0.0001; Table 2).
These findings are illustrated by force–displacement curves and bone damage images in Fig. 2. Force–displacement curves of both hip and vertebra were steeper after 24 months (blue line) compared to baseline (red line), corresponding to an increase in bone strength. A simulation of osteoporotic fragility fracture indicated damaged regions (red squares) at the femoral neck and trochanter major when strained. In the case of a validated simulated lateral fall model, the hip would break at these typical fracture sites. Similar outcomes were observed for compression simulations at the reference vertebral body. After 24 months, these regions showed increased biomechanical bone strength in the FEA model (increases in blue squares with decreases in red squares) compared to baseline.
Areal BMD and Trabecular Bone Score (TBS)
Compared to baseline, areal BMD at the lumbar spine and total hip was significantly higher at month 24: lumbar spine +3.4 % (p = 0.0002) and total hip +4.1 % (p < 0.0001; Table 2).
The TBS increased significantly from 1.235 at baseline to 1.289 at month 24 (p = 0.0130; Table 2). At study end, the 75th percentile, i.e., the upper 25 % of patients, was 1.341, a score above the lower normal limit of TBS scores (normal TBS > 1.300).
Safety and Tolerability
Ibandronate infusions were generally well tolerated by the patients. Five patients developed mild flu-like symptoms after the first injection and three patients after the second injection. During the 24 month study period, one new non-vertebral fragility fracture occurred. Neither alterations in creatinine levels nor hyper- or hypocalcaemia or hyperparathyroidism were observed during the study.
Discussion
This was a prospective study in male patients with idiopathic osteoporosis and prevalent fragility fractures treated with quarterly IBN injections for 24 months. To date, scarce data are available for treatment of MIO with IBN, particularly with regard to changes of serum Scl and DKK-1 levels. Using non-invasive diagnostic measures, we were able to show marked improvements in hip and vertebral BMD and biomechanical properties at typical fracture sites in IBN-treated patients with MIO.
We observed an increase of Scl levels with a peak after 1 month followed by a constant decline during the first 12 months without changes in the second year of treatment. In contrast, DKK-1 levels were significantly decreased after 4 weeks with a continuous decline until month 6 and an increase to levels comparable to baseline at the end of the first year of treatment. Scl and DKK-1 levels were negatively correlated at each time point, but the correlations were weaker at study endpoint compared to the early phases of this study.
Previous studies on BP, raloxifene, or denosumab in postmenopausal women with different durations of treatment (ranging from 3 to 27 months) demonstrated an early increase of, or no association with, circulating Scl levels. [14, 17, 21, 22]. A preclinical study on murine osteoclasts revealed that osteoclast precursor cells receiving denosumab, which are primarily not affected by BP induced apoptosis, were able to secrete Scl leading to increased serum levels [23].
Zoledronic acid is known to reduce both Scl and DKK-1 in postmenopausal osteoporosis, but this effect was not shown for diverse oral BP, suggesting different potencies or affinities to bone responsible for these differing results [15, 24]. However, when Scl and DKK-1 were used in a comparable study population, levels increased during yearly zoledronic acid treatment, while in patients treated weekly with intramuscular clodronate, only Scl increased and DKK-1 remained stable [25].
We recently published an osteoblast dysfunction with reduced WNT10B, RUNX2, RANKL, and SOST expression as the most likely pathomechanism of MIO, but it cannot be specified that the IBN observed changes of sclerostin and DKK-1 can be solely explained by osteoblast dysfunction [2]. While the effect on bone resorption is mediated by connexin43 (Cx43) modulation of osteoprotegerin, the mechanisms by which Cx43 affects the function of bone forming cells and the secretion of diverse specific serum markers still need to be clarified. Direct autonomous osteoblast activity, which is chiefly regulated by Scl, and paracrine mechanisms via osteocytes, has been suggested. Several in vitro studies have also shown a direct stimulating effect of BP on osteoblast and osteocyte activity and consecutive changes in Scl levels. [26–28]. Although BP bind with high affinity to bone mineral, there is a continuous release of low levels of the drug, which results in a constant supply of BP at low concentrations. This maintains a Cx43 dependent osteoblast and osteocyte viability and activity beyond mere osteoclast influence, regardless of the type of BP [29, 30].
The key role of Scl produced primarily by osteocytes as a major mediator of the molecular mechanisms involved in the process of adaptive bone remodeling is reported by the majority of studies. Bone remodeling is mediated by altered sclerostin levels through different expressions of RANKL, OPG, and likely FGF23, which are also secreted by osteocytes. Antiresorptive treatment may be responsible for dynamic RANKL/OPG ratios, leading either to osteocyte-mediated early bone formation or prolonged resorption at a later point [31].
Although compelling evidence exists for the involvement of Scl in the homeostasis of the growing and adult skeleton, limited data exist on the postnatal role of DKK-1. Since DKK-1 is secreted in different tissues and states, the observed changes of this serum marker should not be interpreted without focusing on other markers of bone metabolism. The decrease of DKK-1 levels in the early phase with its nadir after 6 months is transient, and the promising correlations at early time points could lead to an over interpretation. This is also supported by stronger correlations of Scl and bone turnover markers of resorption and formation compared to DKK-1 in this and other studies [32, 33].
Using paired biopsies, we recently demonstrated in the same cohort of MIO patients that mineralization improved within 24 months of IBN therapy [11].
However, histomorphometric analysis of the biopsies did not show significant changes in trabecular volume (BV/TV), thickness, or number. Rather, we found significant improvement or even normalization of TBS during IBN therapy in the same study cohort.
Enhanced mineralization is likely to be the reason for the effects seen in the paired transiliac bone biopsies after 24 months at an anatomical bone site, which does not reflect mechanical strain [11]. However, IBN exerts antiresorptive effects throughout the whole skeleton and our data confirm these positive effects in MIO patients regardless of the weight-bearing or non-weight-bearing bone sites. Several studies have investigated the effects of oral and intravenous IBN compared to calcium/vitamin D only in male populations. Improvements of geometrical parameters, a reduction of bone turnover marker, and a reduction of fragility fracture risk were only reported for IBN [34–36].
Most studies on male osteoporosis focused on changes in areal BMD as a surrogate parameter of enhanced bone strength [37, 38]. Intravenous IBN also enhanced changes in trabecular bone structures, cortical bone, and hip geometrical parameters as previously reported for monthly oral IBN in men with low aBMD measured by DXA [34]. Voxel-based FEA models of the proximal femur and vertebral body showed promising strength increases during the 24 months of treatment. Similar improvements of femoral and vertebral strength were recently published in postmenopausal women with osteoporosis treated with denosumab over 36 months [39]. In general, increases in bone strength and density showed similar trends at both the femur and the vertebral body. The even strain of the vertebral body and BMD increased in both trabecular and cortical hip compartments correspond well with an increase in strength, BMD, and BV/TV. The strain situation in the lateral fall configuration of the femur is inhomogeneous and involves tension/compression combined with bending and shears forces. Furthermore, fractures mainly occur at the neck or trochanteric region, and the strain bearing capacity of the weakest part finally determines strength. Thus, for the proximal femur—and especially in the analyzed lateral fall scenario—the location where new bone is formed or where BMD is increased by the treatment has a crucial effect on strength increase. Since fractures at baseline and follow-up occurred at the same position, a strength increase is achieved by local density changes at the hip or vertebral body, which seem more important than general changes.
Direct interrelations between serum markers of bone metabolism and bone architecture play an important role for bone strength and low fracture risk. Recent literature indicates a direct relationship between circulating Scl levels and age as well as positive correlations between Scl levels with trabecular density, number and thickness in both genders. Especially in non-osteoporotic young men (age ≤ 43 years), higher Scl levels are associated with higher aBMD and better bone microarchitecture assessed by HR-pQCT. Even stronger correlations of Scl in levels and trabecular bone structure were confirmed for males at the age of 63 years or older. The frequency of prevalent fractures was lower for these subjects with Scl levels in the higher quartiles compared to the lowest quartile, suggesting a lower fracture risk in men with higher sclerostin levels. Positive correlations between changes in a biochemical marker and improvement of biomechanical properties support the use of markers as a potential surrogate of bone strength in teriparatide-treated male GIO patients [15, 22, 40–42]. In this study population, median baseline Scl levels of 22.8 pmol/L were in the lowest quartile of healthy age-comparable female and male individuals suggesting low bone strength. The increase of Scl and the decrease of CTX levels caused by ibandronate treatment resulted in low bone turnover and in improvements of vBMD as well as biomechanical strength in MIO patients.
Limitations
Non-invasive measurements of bone microarchitecture with high-resolution peripheral QCT (HR-pQCT) were not obtained. However, TBS and QCT parameters indicated improvements in cortical and trabecular properties during the study period. There is always concern that improvements of geometrical parameters measured by DXA or QCT are likely due to enhanced mineralization or beam hardening, but both non-invasive methods are well established in clinical routine. Additional bone biopsies after 4 weeks of IBN therapy would have been useful to investigate the effects of the observed changes. However, patients are unlikely to agree to this biopsy. Furthermore, there is no mouse model available yet to confirm our findings at tissue levels at different time points of IBN treatment, and there are doubts that systemic serum bone marker reflects the microenvironment of bone tissue.
To prove the impact of changes in BTMs and their respective correlations, a control group would be useful. However, this was not considered due to the severity of osteoporosis (each patient had sustained at least one fragility fracture).
There is always a potential bias in an open‐label clinical trial. Since each IBN dose was administered by the investigators, we believe that this effect is unlikely to affect the evaluation of BMD and biochemical values.
Conclusion
Our results suggest that in MIO patients the treatment with quarterly intravenous IBN reduces bone resorption and improves cortical and trabecular bone strength. These changes result in improvements of biomechanical properties of cortical and trabecular bone sites susceptible to fragility fractures and are associated with an early and ongoing increase of serum Scl and temporarily reduced DKK-1 levels.
References
Orwoll ES, Klein RF (2008) Osteoporosis in men: epidemiology, pathophysiology, and clinical characterization. In: Marcus R, Feldman D, Nelson DA, Rosen CJ (eds) Osteoporosis, vol 2, 3rd edn. Academic Press, New York
Patsch JM, Kohler T, Berzlanovich A, Muschitz C, Bieglmayr C, Roschger P, Resch H, Pietschmann P (2011) Trabecular bone microstructure and local gene expression in iliac crest biopsies of men with idiopathic osteoporosis. J Bone Miner Res 26:1584–1592. doi:10.1002/jbmr.344
Fratzl-Zelman N, Roschger P, Misof BM, Nawrot-Wawrzyniak K, Pötter-Lang S, Muschitz C, Resch H, Klaushofer K, Zwettler E (2011) Fragility fractures in men with idiopathic osteoporosis are associated with undermineralization of the bone matrix without evidence of increased bone turnover. Calcif Tissue Int 88:378–387. doi:10.1007/s00223-011-9466-4
Legrand E, Hedde C, Gallois Y, Degasne I, Boux de Casson F, Mathieu E, Baslé MF, Chappard D, Audran M (2011) Osteoporosis in men: a potential role for the sex hormone binding globulin. Bone 29:90–95
Van Pottelbergh I, Goemaere S, Zmierczak H, Kaufman JM (2004) Perturbed sex steroid status in men with idiopathic osteoporosis and their sons. J Clin Endocrinol Metab 89:4949–4953. doi:10.1210/jc.2003-032081
Johansson AG, Eriksen EF, Lindh E, Langdahl B, Blum WF, Lindahl A, Ljunggren O, Ljunghall S (1997) Reduced serum levels of the growth hormone dependent insulin-like growth factor binding protein and a negative bone balance at the level of individual remodeling units in idiopathic osteoporosis in men. J Clin Endocrinol Metab 82:2795–2798. doi:10.1210/jcem.82.9.4148
Kurland ES, Rosen CJ, Cosman F, McMahon D, Chan F, Shane E, Lindsay R, Dempster D, Bilezikian JP (1997) Insulin-like growth factor-I in men with idiopathic osteoporosis. J Clin Endocrinol Metab 82:2799–2805. doi:10.1210/jcem.82.9.4253
Patel MB, Arden NK, Masterson LM, Phillips DI, Swaminathan R, Syddall HE, Byrne CD, Wood PJ, Cooper C, Holt RI et al (2005) Investigating the role of the growth hormone-insulin-like growth factor (GH-IGF) axis as a determinant of male bone mineral density (BMD). Bone 37:833–841. doi:10.1016/j.bone.2005.06.016
Gillberg P, Mallmin H, Petrén-Mallmin M, Ljunghall S, Nilsson AG (2002) Two years of treatment with recombinant human growth hormone increases bone mineral density in men with idiopathic osteoporosis. J Clin Endocrinol Metab 87:4900–4906. doi:10.1210/jc.2002-020231
Föger-Samwald U, Patsch JM, Schamall D, Alaghebandan A, Deutschmann J, Salem S, Mousavi M, Pietschmann P (2014) Molecular evidence of osteoblast dysfunction in elderly men with osteoporotic hip fractures. Exp Gerontol 57:114–121. doi:10.1016/j.exger.2014.05.014
Misof BM, Patsch JM, Roschger P, Muschitz C, Gamsjaeger S, Paschalis EP, Prokop E, Klaushofer K, Zwettler E (2014) Intravenous treatment with ibandronate normalizes bone matrix mineralization and reduces cortical porosity after two years in male osteoporosis: a paired biopsy study. J Bone Miner Res 29:440–449. doi:10.1002/jbmr.2035
Mosekilde L, Vestergaard P, Rejnmark L (2013) The pathogenesis, treatment and prevention of osteoporosis in men. Drugs 73:15–29. doi:10.1007/s40265-012-0003-1
Chapurlat RD, Laroche M, Thomas T, Rouanet S, Delmas PD, de Vernejoul MC (2013) Effect of oral monthly ibandronate on bone microarchitecture in women with osteopenia-a randomized placebo-controlled trial. Osteoporos Int 24:311–320. doi:10.1007/s00198-012-1947-4
Catalano A, Morabito N, Basile G, Brancatelli S, Cucinotta D, Lasco A (2013) Zoledronic acid acutely increases sclerostin serum levels in women with postmenopausal osteoporosis. J Clin Endocrinol Metab 98:1911–1915. doi:10.1210/jc.2012-4039
Anastasilakis AD, Polyzos SA, Gkiomisi A, Bisbinas I, Gerou S, Makras P (2013) Comparative effect of zoledronic acid versus denosumab on serum sclerostin and dickkopf-1 levels of naive postmenopausal women with low bone mass: a randomized, head-to-head clinical trial. J Clin Endocrinol Metab 98:3206–3212. doi:10.1210/jc.2013-1402
Orwoll E, Ettinger M, Weiss S, Miller P, Kendler D, Graham J, Adami S, Weber K, Lorenc R, Pietschmann P, Vandormael K, Lombardi A (2000) Alendronate for the treatment of osteoporosis in men. N Engl J Med 343:604–610. doi:10.1056/NEJM200008313430902
Silva BC, Boutroy S, Zhang C, McMahon DJ, Zhou B, Wang J et al (2013) Trabecular bone score (TBS)—a novel method to evaluate bone microarchitectural texture in patients with primary hyperparathyroidism. J Clin Endocrinol Metab 98:1963–1970. doi:10.1210/jc.2012-4255
Silva BC, Leslie WD, Resch H, Lamy O, Lesnyak O, Binkley N, McCloskey EV, Kanis JA, Bilezikian JP (2014) Trabecular bone score: a noninvasive analytical method based upon the DXA image. J Bone Miner Res 29:518–530. doi:10.1002/jbmr.2176
Dall’Ara E, Schmidt R, Pahr D, Varga P, Chevalier Y, Patsch J, Kainberger F, Zysset P (2010) A nonlinear finite element model validation study based on a novel experimental technique for inducing anterior wedge-shape fractures in human vertebral bodies in vitro. J Biomech 43:2374–2380. doi:10.1016/j.jbiomech.2010.04.023
Dall’Ara E, Luisier B, Schmidt R, Kainberger F, Zysset P, Pahr D (2013) A nonlinear QCT-based finite element model validation study for the human femur tested in two configurations in vitro. Bone 52:27–38. doi:10.1016/j.bone.2012.09.006
Chung YE, Lee SH, Lee SY, Kim SY, Kim HH, Mirza FS, Lee SK, Lorenzo JA, Kim GS, Koh JM (2012) Long-term treatment with raloxifene, but not bisphosphonates, reduces circulating sclerostin levels in postmenopausal women. Osteoporos Int 23:1235–1243. doi:10.1007/s00198-011-1675-1
Polyzos SA, Anastasilakis AD, Bratengeier C, Woloszczuk W, Papatheodorou A, Terpos E (2012) Serum sclerostin levels positively correlate with lumbar spinal bone mineral density in postmenopausal women-the six-month effect of risedronate and teriparatide. Osteoporos Int 23:1171–1176. doi:10.1007/s00198-010-1525-6
Ota K, Quint P, Ruan M, Pederson L, Westendorf JJ, Khosla S, Oursler MJ (2013) Sclerostin is expressed in osteoclasts from aged mice and reduces osteoclast-mediated stimulation of mineralization. J Cell Biochem 114:1901–1907. doi:10.1002/jcb.24537
Russel RG, Watts NB, Ebetino FH, Rogers MJ (2008) Mechanisms of action of bisphosphonates: similarities and differences and their potential influence on clinical efficacy. Osteoporos Int 19:733–759. doi:10.1007/s00198-007-0540-8
Gatti D, Viapiana O, Idolazzi L, Fracassi E, Ionescu C, Dartizio C, Troplini S, Kunnathully V, Adami S, Rossini M (2014) Distinct effect of zoledronate and clodronate on circulating levels of DKK1 and sclerostin in women with postmenopausal osteoporosis. Bone 67:189–192. doi:10.1016/j.bone.2014.06.037
Stains JP, Watkins MP, Grimston SK, Hebert C, Civitelli R (2014) Molecular mechanisms of osteoblast/osteocyte regulation by connexin43. Calcif Tissue Int 94:55–67. doi:10.1007/s00223-013-9742-6
Plotkin LI, Bellido T (2013) Beyond gap junctions: connexin43 and bone cell signaling. Bone 52:157–166. doi:10.1016/j.bone.2012.09.030
Bivi N, Nelson MT, Faillace ME, Li J, Miller LM, Plotkin LI (2012) Deletion of Cx43 from osteocytes results in defective bone material properties but does not decrease extrinsic strength in cortical bone. Calcif Tissue Int 91:215–224. doi:10.1007/s00223-012-9628-z
Bellido T, Plotkin LI (2011) Novel actions of bisphosphonates in bone: preservation of osteoblast and osteocyte viability. Bone 49:50–55. doi:10.1016/j.bone.2010.08.008
Maruotti N, Corrado A, Neve A, Cantatore FP (2012) Bisphosphonates: effects on osteoblast. Eur J Clin Pharmacol 68:1013–1018. doi:10.1007/s00228-012-1216-7
Sapir-Koren R, Livshits G (2014) Osteocyte control of bone remodeling: is sclerostin a key molecular coordinator of the balanced bone resorption-formation cycles? Osteoporos Int 25:2685–2700. doi:10.1007/s00198-014-2808-0
Li X, Grisanti M, Fan W, Asuncion FJ, Tan HL, Dwyer D et al (2011) Dickkopf-1 regulates bone formation in young growing rodents and upon traumatic injury. J Bone Miner Res 26:2610–2621. doi:10.1002/jbmr.472
Muschitz C, Kocijan R, Fahrleitner-Pammer A, Pavo I, Haschka J, Schima W, Kapiotis S, Resch H (2014) Overlapping and continued alendronate or raloxifene administration in patients on teriparatide: effects on areal and volumetric bone mineral density—the CONFORS Study. J Bone Miner Res 29:1777–1785. doi:10.1002/jbmr.2216
Genant HK, Lewiecki EM, Fuerst T, Fries M (2012) Effect of monthly ibandronate on hip structural geometry in men with low bone density. Osteoporos Int 23:257–265. doi:10.1007/s00198-011-1732-9
Orwoll ES, Binkley NC, Lewiecki EM, Gruntmanis U, Fries MA, Dasic G (2010) Efficacy and safety of monthly ibandronate in men with low bone density. Bone 46:970–976. doi:10.1016/j.bone.2009.12.034
Fahrleitner-Pammer A, Piswanger-Soelkner JC, Pieber TR, Obermayer-Pietsch BM, Pilz S, Dimai HP, Prenner G, Tscheliessnigg KH, Hauge E, Portugaller RH, Dobnig H (2009) Ibandronate prevents bone loss and reduces vertebral fracture risk in male cardiac transplant patients: a randomized double-blind, placebo-controlled trial. J Bone Miner Res 24(7):1335–1344. doi:10.1359/jbmr.090216
Ringe JD, Faber H, Dorst A (2001) Alendronate treatment of established primary osteoporosis in men: results of a 2-year prospective study. J Clin Endocrinol Metab 86:5252–5255. doi:10.1210/jcem.86.11.7988
Orwoll ES, Miller PD, Adachi JD, Brown J, Adler RA, Kendler D, Bucci-Rechtweg C, Readie A, Mesenbrink P, Weinstein RS (2010) Efficacy and safety of a once-yearly i.v. Infusion of zoledronic acid 5 mg versus a once-weekly 70-mg oral alendronate in the treatment of male osteoporosis: a randomized, multicenter, double-blind, active-controlled study. J Bone Miner Res 25:2239–2250. doi:10.1002/jbmr.119
Keaveny TM, McClung MR, Genant HK, Zanchetta JR, Kendler D, Brown JP et al (2014) Femoral and vertebral strength improvements in postmenopausal women with osteoporosis treated with denosumab. J Bone Miner Res 29:158–165. doi:10.1002/jbmr.2024
Amrein K, Amrein S, Drexler C, Dimai HP, Dobnig H, Pfeifer K, Fahrleitner-Pammer A (2012) Sclerostin and its association with physical activity, age, gender, body composition, and bone mineral content in healthy adults. J Clin Endocrinol Metab 97:148–154. doi:10.1210/jc.2011-2152
Kocijan R, Muschitz C, Fahrleitner-Pammer A, Amrein K, Pietschmann P, Haschka J, Dinu S, Kapiotis S, Resch H (2014) Serum sclerostin levels are decreased in adult patients with different types of osteogenesis imperfecta. J Clin Endocrinol Metab 99:E311–E319. doi:10.1210/jc.2013-2244
Szulc P, Boutroy S, Vilayphiou N, Schoppet M, Rauner M, Chapurlat R, Hamann C, Hofbauer LC (2013) Correlates of bone microarchitectural parameters and serum sclerostin levels in men: the STRAMBO study. J Bone Miner Res 28(8):1760–1770. doi:10.1002/jbmr.1888
Acknowledgements
The authors cordially thank Dr. Heike von Krempelhuber at Tutzing/Germany for assistance in editing the manuscript, Sabine Klauss and Xenia Steiner at Ulm/Germany for graphic design of the figures. The authors further acknowledge the work of the staff of the central laboratory and of the Department of Diagnostic and Interventional Radiology at St. Vincent Hospital Vienna, Austria. QCT DICOM data were calculated without knowledge of the study protocol by Dr. Wolfram Timm at Kiel/Germany. FEA calculations were performed by Dr. Enrico Dall’Ara at the Institute of Lightweight Design and Structural Biomechanics, University of Technology, Vienna, Austria. TBS scores were calculated without knowledge of the study protocol by Prf. Didier Hans at Lausanne/CH.
Conflict of interest
Christian Muschitz has received speaker honoraria from Amgen, Novartis, Servier, Eli Lilly, Nycomed/Takeda, and has received educational grants/research support from the Austrian Society for Bone and Mineral Research, Roche Austria, Eli Lilly Austria, and Amgen Austria. Heinrich Resch has received speaker honoraria from Amgen, Novartis, Servier, Eli Lilly, Nycomed/Takeda, Merck (MSD), and has received educational grants/research support from Eli Lilly and Roche Austria. Peter Pietschmann has received research support and/or honoraria from Amgen GmbH, Eli Lilly GmbH, Fresenius Kabi Austria GmbH, Merck, Sharp and Dohme GmbH, Novartis Pharma, Nycomed Pharma, Roche Austria, Servier Austria, Sanofi-Austria, and Sinapharm. Karin Amrein reports scientific support from Fresenius Kabi Austria. Dieter Pahr is the owner of a consultancy company for FEA calculations and has received a fee for the QCT segmentation, but not for the FEA calculations in this study. Roland Kocijan, Janina M. Patsch, Barbara M. Misof, and Alexandra Kaider have nothing to disclose.
Human and Animal Rights and Informed Consent
This study was planned and conducted according to the Helsinki Declaration of 2000 and was approved by the Ethics Committee of the Medical University of Vienna/Austria (AUT – 25/2006) and by the Ethics Committee of the St. Vincent Hospital Vienna/Austria (EK-Nr: 2006/12). The study was also registered at EudraCT:2006-006692-20. Informed and written consent was obtained from all patients prior to any study related procedure.
Competing interest
This investigator-initiated study was supported by an independent research grant from Roche Austria. Roche Austria was not involved in the study design or had any admission to patient-related data and findings.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Muschitz, C., Kocijan, R., Pahr, D. et al. Ibandronate Increases Sclerostin Levels and Bone Strength in Male Patients with Idiopathic Osteoporosis. Calcif Tissue Int 96, 477–489 (2015). https://doi.org/10.1007/s00223-015-0003-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-015-0003-8