Abstract
Temporal lobe epilepsy (TLE) is the most common type of intractable epilepsy and is refractory to medications. However, the role and mechanism of H19 in regulating TLE remains largely undefined. Expression of H19 and miR-206 was detected using real-time quantitative PCR (RT-qPCR). Cell apoptosis, autophagy and inflammatory response were determined by flow cytometry, western blotting and enzyme-linked immunosorbent assay (ELISA). The interaction between H19 and miR-206 was predicted on the miRcode database and confirmed by luciferase reporter assay, RNA immunoprecipitation (RIP) and RNA pull-down. H19 was upregulated and miR-206 was downregulated in the rat hippocampus neurons after kainic acid (KA) treatment. Functionally, both H19 knockdown and miR-206 overexpression weakened KA-induced apoptosis, autophagy, inflammatory response, and oxidative stress in hippocampus neurons. Mechanically, the phosphatidylinositol 3-kinase (PI3K)/AKT signaling pathway was activated by H19 knockdown and miR-206 was confirmed to be targeted and negatively regulated by H19. Moreover, downregulation of miR-206 could counteract the effects of H19 knockdown in KA-induced hippocampus neurons. Knockdown of H19 suppressed hippocampus neuronal apoptosis, autophagy and inflammatory response presumably through directly upregulating miR-206 and activating the PI3K/AKT signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Epilepsy is one of the most common neurological disorders, with an estimated 5 million people diagnosed with the disease worldwide (Saud et al. 2020; Kwon and Wagner 2022). The predominant feature of epilepsy includes recurrent and unprovoked seizures. Moreover, up to 40% of cases are refractory to conventional medical treatment due to its adverse effects and drug-resistance (Trinka et al. 2016). Temporal lobe epilepsy (TLE) is the most common type of acquired and refractory epilepsy (Tellez-Zenteno and Hernandez-Ronquillo 2012), and loss and sclerosis of hippocampus neurons are the general pathologic hallmarks of TLE (Tai et al. 2018). TLE experiences a latent period from the initial precipitating injury to recurrent seizures (Pitkanen et al. 2015). It has been well-recognized that the hippocampus undergoes plenty of cellular changes during the latent period, including apoptosis and inflammation (Wu et al. 2018; Xia et al. 2018). However, the exact mechanism underlying the process of epileptogenesis remains disappointed.
Role of non-coding RNAs has emerged in regulating brain excitability and seizure thresholds, including long ncRNAs (lncRNAs) and microRNAs (miRNAs) (Henshall and Kobow 2015). Containing 20–25 highly conserved nucleotides, miRNAs have been proposed as diagnostic biomarkers and treatment targets for SE and adult hippocampal neurogenesis (Bielefeld et al. 2017; Brindley et al. 2019). Four abnormal expressed miRNAs including miRNA-206-3p (miR-206), miR-374, miR-468 and miR-142-5p have been identified in drug-resistant epileptic mice (Moon et al. 2014). Very recently, miR-206 expression was associated with protection from seizure activity and hippocampus neuron loss (Wu et al. 2019). Nevertheless, the mechanism which miR-206 suppresses neuronal loss remains unclear.
LncRNAs are a class of endogenous transcripts defined to be greater than 200 nucleotides in length. LncRNAs can alter gene transcription in all orientations through multiple mechanisms, such as acting as a sponge for miRNAs. Lately, genome-wide lncRNA profiles have been declared in TLE mouse models induced by pilocarpine and kainate acid (KA) (Lee et al. 2015). At present, the functions and regulatory mechanisms of lncRNAs in epileptogenesis remain largely unexplored (Hauser et al. 2018). LncRNA H19 (H19) H19, originally described as an oncofetal transcript, has been revealed to be involved in the progression of many diseases (Chen et al. 2021; Ghafouri-Fard et al. 2020; Thomas et al. 2019). Studies have shown that H19 is involved in the activation of hippocampal glial cells during epileptogenesis (Han et al. 2017, 2018a). However, the role of H19 in hippocampal neuron loss and its underlying mechanisms have not been fully elucidated.
KA-induced epilepsy in rat is a popular model to investigate the pathogenesis of epilepsy (Nieuwenhuyse et al. 2015). However, we’re not able to study epilepsy in an in vivo model, but a cell model of epilepsy induced by KA in primary hippocampus neurons was utilized. And, KA-induced neurons have also been used in epilepsy research (Kaneko et al. 2016, 2017; Lu et al. 2019). Thus, we constructed a TLE model using KA in primary hippocampus neurons to investigate the expression and relationship of H19 and miR-206. Ultimately, the H19/miR-206 axis was confirmed to be associated with KA-induced hippocampus neuron injury.
Materials and methods
Patients and clinical samples
The cerebrospinal fluid of patients (n = 5) with TLE was collected from patients using a standard lumbar puncture procedure from a sitting position or lying on their side. After centrifugation of 300×g for 10 min at 4 °C, the supernatant was collected and stored at − 80 °C for total RNA isolation. Serums derived from patients with a temporal vascular malformation (n = 5) but no history of epilepsy or other neurological diseases were recruited as normal controls. This study was approved by the Research Ethics Committee of the Weihai Central Hospital and written consent from patients was received.
Isolation of hippocampus neurons and cell culture
The hippocampus tissues from neonatal rats (Sprague–Dawley, 18th embryonic day) were micro-dissected and cut into pieces from the isolated brain in D-Hank’s buffer on ice. The hippocampus neurons were isolated from tissues as previous report (Wang et al. 2018). Briefly, tissues were then treated with 0.25% trypsin (Gibco, Grand Island, NY, USA) at 37 °C for 15 min, which was terminated by adding low glucose Dulbecco minimum essential medium (DMEM; Gibco) containing 10% fetal bovine serum (FBS; Gibco). The digested tissues were centrifuged at 700 rpm for 5 min with the supernatant discarded, then planted on 6-well plate dishes (Corning, NY, USA) in Neuron-basal medium (Invitrogen, Carlsbad, CA, USA.) containing 2% B27 (Gibco), 0.5 mM glutamine and 100 U/mL penicillin/streptomycin for 4–6 h. Additionally, the cell cultures were treated with cytosine arabinoside (5 μg/mL) to inhibit glial proliferation. The culture medium was refreshed every 2 days and hippocampal neurons were passaged when reached to 80–90% confluence. Hippocampal neurons were treated with KA (50 μM) for 48 h to induce injury.
Lentivirus infection
Small hairpin RNA (shRNA) against H19 (sh-H19), miR-206 mimic and miR-206 inhibitor (anti-miR-206) were synthesized by GenePharma (Shanghai, China), as well as their negative controls. The isolated hippocampus neurons (8 × 104 cells) were plated into 6-well plates (Corning) and the cells at 50% confluence were ready for lentivirus infection. Above nucleotides and PCR product of the full length of H19 were sub-cloned into a pGLVU6/Puro lentiviral vector (GenePharma) to general lentivirus, respectively. After inoculating the neurons with lentivirus suspension for 48 h, a fresh complete medium containing appropriate concentrations of puromycin (5 μg/mL) was used to screen stably transfected cell lines. These sequences were provided in Table 1.
Real-time quantitative PCR (RT-qPCR)
Total RNA was extracted with Trizol (Invitrogen) following the operation guidance. Next, 1 μg RNA was used to synthesize complementary DNA (cDNA) using First Strand DNA Synthesis Kit (Takara, Kyoto, Shiga, Japan). The RT-qPCR experiment was conducted with SYBR Premix Tap (2×; Takara) on a quantitative PCR system. Each sample was performed in triplicate. The primers used in this study were provided by GENEWIZ (Suzhou, China) and the sequences were shown in Table 2. The multiple proportions of gene expression were analyzed with the 2−ΔΔCt method and the internal control was β-actin (for lncRNA) and U6 (for miRNA).
EdU assay
EdU staining proliferation assay kit (iFluor 488; Abcam, Cambridge, UK) was employed to detect cell proliferation on a fluorescence microscope. EdU could be incorporated into the newly synthesized DNA in cells, and re-reacted with iFluor 488 (generates green fluorescence); eventually DNAs in all cells were double-stained with DAPI staining solution (Abcam) (generates blue fluorescence). Stained cells were observed under fluorescence microscopy, and the percentage of EdU positive cells in DAPI positive cells was calculated from five randomly selected fields (bar scale: 50 μm).
Flow cytometry
Hippocampus neurons and KA-induced transfected hippocampus neurons were collected and analyzed by Annexin V-Fluorescein isothiocyanate (FITC) apoptosis detection kit (Sigma-Aldrich) on a flow cytometry. Apoptotic cells were labeled complying with the protocol. In brief, the adherent and floating cells were harvested and washed with phosphate buffer solution twice. Then, 100 μL cells (1 × 105 cells) of each group were stained in the buffer containing FITC-Annexin V and PI for 30 min in the dark. Fluorescence was analyzed on cytoFLEX LX flow cytometer (Beckman-Coulter, CA, USA) using a CytExpert software. Quadrants were positioned on Annexin V/PI plots to distinguish normal cells (Annexin V−/PI−) and apoptotic cells (Annexin V+/PI− and Annexin V+/PI+). Cell apoptotic rate = apoptotic cells/(apoptotic cells + normal cells).
Western blotting
Hippocampus neurons and KA-induced transfected hippocampus neurons were acquired to extract total protein with RIPA lysis buffer (Millipore, Billerica, MA, USA) containing protease inhibitor cocktail (Millipore), a protease inhibitor. According to the Bradford protein assay reagent (Bio-Rad, Shanghai, China), equal amounts of protein (20 μg) from each sample were loaded for the standard procedures of western blot assay. The primary antibodies were shown in Table 3. Image-Pro Plus (version 6.0; Media Cybernetics, Rockville, MD, USA) was used to quantify the densities of the protein signals. The relative expression of B cell lymphoma (Bcl-2), Bcl-2 associated X6A7 protein (BAX6A7), cleaved caspase 3 (C-cleaved 3) and Beclin 1 was normalized to the internal reference glyceraldehyde-phosphate dehydrogenase (GAPDH), and expression levels of LC3-II, phosphorylated phosphatidylinositol 3-kinase (p-PI3K) and p-AKT were respectively compared to LC3-I, PI3K and AKT.
Enzyme-linked immunosorbent assay (ELISA)
Isolated hippocampus neurons were transfected and then implanted and cultured in 96-well plates (Corning). The culture supernatant was collected at 24 h. Commercial kits for tumor necrosis factor (TNF)-α (#ab100785), interleukin (IL)-1β (#ab100768) and IL-6 (#ab100772) were obtained from Abcam. All operations were carried out according to the instructions.
Malondialdehyde (MDA) and superoxide dismutase (SOD) assay kits
After KA treatment, hippocampus neurons were collected. The productions of MDA and SOD were examined using Lipid Peroxidation MDA Assay Kit (Beyotime, Shanghai, China) and Total SOD Assay Kit with WST-8 (Beyotime) according to the manufacturers’ instructions. The relative MDA level and SOD level were normalized to the control group.
Luciferase reporter assay
The fragment of H19 containing the predicted miR-206 binding site or its mismatched sequence was cloned into the pGL3 plasmid (Promega, Madison, Wisconsin, USA). The mutation of wild type H19 (H19-WT) was performed by site-directed mutagenesis. 50 nM of miR-206 mimic, miR-NC mimic, anti-miR-206 or anti-NC was co-transfected into 293T cells (PTA-5077; ATCC, Manassas, VA, USA) with 5 ng of Renilla plasmid (Promega) and 100 ng of the constructed plasmid H19-WT or H19-MUT. After transfection for 24 h, luciferase assay was detected using a dual-luciferase reporter assay system (Promega) and relative Firefly luciferase activity of H19-WT/MUT was normalized to Renilla.
RNA immunoprecipitation (RIP)
Magna RIP™ RNA-binding protein immunoprecipitation kit (Millipore) was used to conduct the RIP assay. Hippocampus neurons were collected and lysed in a complete RIP lysis buffer, and then the cell extract was incubated with magnetic beads conjugated with human Ago2 or IgG antibody in RIP buffer. After incubation of proteinase K, the immunoprecipitated RNAs including miR-206 and H19 were extracted and detected by RT-qPCR.
RNA pull-down assay
Oligonucleotides miR-206 and miR-NC were biotinylated using a biotin-labeled RNA labeling mix (Roche, Basel, Switzerland). An equal amount of biotinylated miRNA (bio-miRNA) was added to streptavidin dynabeads. 293T cells were transfected with bio-miR-206/NC for 24 h. Then the lysates of transfected neurons were incubated at room temperature for 15 min to immobilize RNA on the streptavidin dynabeads. After removing the supernatant and washing the magnetic beads with wash buffer, the H19 level in RNA complexes was measured using RT-qPCR.
Statistical analysis
All data were presented as mean ± standard error of the mean from three independent studies and the statistical analysis was performed on Graphpad Prism 5 (GraphPad, San Diego, CA, USA). The comparisons were made using two-tailed Student t-test in two groups and using one-way analysis of variance followed by a Bonferroni-Dunn test in multiple groups. The significant differences were acknowledged as a P value < 0.05.
Results
Knockdown of H19 suppressed KA-induced primary hippocampus neuron apoptosis, autophagy, inflammatory response, and oxidative stress in vitro
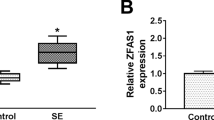
Expression level of H19 was distinctively higher in cerebrospinal fluid of patients with epilepsy compared with control people (Fig. 1A). This data suggested a potential role of both in epileptogenesis. Thus, the biological role of H19 dysregulation was further investigated in hippocampus neurons in the latent period of epilepsy. RT-qPCR revealed that H19 expression level was increased in KA-treated neurons (Fig. 1B). Then, we forcedly silenced H19 expression via lentivirus infection, and silencing efficiency was determined by RT-qPCR (Figure S1A). Similarly, relative expression of H19 was extremely decreased after sh-H19 lentivirus infection in KA-induced cells (Fig. 1B). Then, neuron injury was evaluated with cell apoptosis, autophagy, inflammation response, and oxidative stress. In this present study, cell apoptosis was testified with cell proliferation, apoptotic rate and apoptosis-related protein expression. EdU assay and flow cytometry demonstrated that EdU positive cells were remarkably reduced and the apoptotic rate was dramatically induced in hippocampus cells under KA treatment, while these effects were inhibited when H19 was silenced (Fig. 1C, D). Western blotting indicated that BAX6A7 and C-caspase 3 protein levels were increased and the Bcl-2 protein level was decreased in KA-induced hippocampus neurons; whereas that effect was significantly reversed by sh-H19 lentivirus infection (Fig. 1E). Moreover, western blotting data showed that KA-induced promotion on LC3-II/I and Beclin 1 proteins were also attenuated by H19 silencing (Fig. 1F). The production of pro-inflammatory factors secreted in the culture supernatant was assessed by ELISA, and we found that highly expressed TNF-α, IL-1β and IL-6 in KA-treated neurons were overall declined with sh-H19 lentivirus infection (Fig. 1G–I). Besides, H19 silencing decreased the production of MDA and increased the activity of SOD in hippocampus neurons treated with KA, as determined by special kits (Fig. 1J, K). Collectively, these results showed that knockdown of H19 could suppress KA-induced hippocampus neuron apoptosis, autophagy, inflammatory response, and oxidative stress, suggesting a protective role of H19 silencing in KA-induced epilepsy in hippocampus neurons in vitro. By the way, H19 knockdown did not affect apoptosis and inflammatory response of control hippocampus neurons (Fig. S2A–S2E).
Role of H19 dysregulation in cell injury in kainic acid (KA)-induced epilepsy in primary hippocampus neurons in vitro. A RT-qPCR analysis detected expression of H19 in cerebrospinal fluid of epilepsy patients and normal people. B–K Hippocampus neurons were transfected with shRNA against H19 (sh-H19) or its negative control (si-NC) via lentiviral vector, and then treated with KA for 24 h. B Level of H19 was measured using RT-qPCR. C Cell proliferation was measured by EdU assay. The percentage of EdU positive cells in DAPI positive cells was calculated. D Apoptotic rate was determined by flow cytometry. The percentage of cells in quadrants of Annexin V+/PI− and Annexin V+/PI+ was statistically recorded. Expression of E apoptosis-related proteins and F autophagy-related markers was evaluated by western blotting. Protein bands of B cell lymphoma (Bcl-2), active Bcl-2 associated X protein 6A7 (BAX6A7), cleaved caspase 3 (C-caspase 3), Beclin 1 and LC3-II/I were quantified by densitometry and normalized to the level of glyceraldehyde-phosphate dehydrogenase (GAPDH). G–I Secreted pro-inflammatory factors tumor necrosis factor (TNF)-α, interleukin (IL)-1β and IL-6 were examined utilizing enzyme-linked immunosorbent assay (ELISA). J, K Level of oxidative stress-related factors MDA and SOD was determined by commercial kits. Data represent mean ± standard error of the mean (SEM). *P < 0.05
Overexpression of miR-206 remitted KA-induced apoptosis, autophagy, inflammatory response, and oxidative stress in primary hippocampus neurons
Moreover, miR-206 was lower expressed in cerebrospinal fluid of epilepsy patients (Fig. 2A). This data suggested a potential role of both in epileptogenesis. The biological role of miR-206 dysregulation was also investigated in hippocampus during epilepsy latency. Expression of miR-206 was downregulated in KA-induced primary hippocampus neurons (Fig. 2B), and mimic lentivirus infection was used to overexpress its expression. The high overexpression efficiency was identified in primary hippocampus neurons (Figure S1B), and this lentivirus infection was also rescued by miR-206 expression in neurons under KA stimuli (Fig. 2B). Ectopic expression of miR-206 could inhibit cell apoptosis of KA-treated hippocampus neurons, as depicted by the decrease of protein apoptotic rate and the protein levels of BAX6A7 and C-caspase 3, as well as the increase of EdU positive cells and the Bcl-2 protein level (Fig. 2C–E). The autophagy-related markers LC3II/I and Beclin 1 were highly expressed in KA-treated hippocampus cells, and this effect was reversed by the presence of miR-206 mimic (Fig. 2F), suggesting that the inhibiting effect miR-206 on KA-induced autophagy. ELISA indicated a high level of TNF-α, IL-1β and IL-6 in response to KA, which was then declined in miR-206 mimic-transfected hippocampus neurons (Fig. 2G–I), hinting a diminishing effect of miR-206 on KA-induced inflammation. Besides, oxidative stress of KA-induced neurons was consistently attenuated by miR-206 overexpression, as evidenced by decreased MDA and increased SOD (Fig. 2J, K). Taken together, these results showed that overexpression of miR-206 could also suppress KA-induced hippocampus cell injuries in vitro, implying a protective role of miR-206 upregulation in KA-induced hippocampus neurons in epilepsy. By the way, miR-206 overexpression failed to alter apoptosis and inflammatory response of control hippocampus neurons (Figure S2F–S2J).
Effect of miR-206 dysregulation on KA-induced cell injury in epilepsy in primary hippocampus neurons in vitro. A RT-qPCR analysis detected expression of miR-206 in cerebrospinal fluid of epilepsy patients and normal people. B–K Hippocampus neurons were transfected with miR-206 mimic (miR-206) or its negative control (NC) for 24 h via lentiviral vector, and then treated with KA for 24 h. B RT-qPCR measured miR-206 level. C EdU-positive cells were measured by EdU assay. D Apoptotic rate was determined by flow cytometry. E, F Western blotting evaluated protein levels of Bcl-2, BAX6A7, C-caspase 3, Beclin 1, and LC3. (G-I) ELISA examined secretions of TNF-α, IL-1β and IL-6. J, K Commercial assay kits determined MDA and SOD products. Data represent mean ± SEM. *P < 0.05
H19 directly interacted with miR-206
Therefore, we wondered about the relationship between H19 and miR-206. Online bioinformatics software miRcode (http://www.mircode.org/) predicted that H19 contained the complementary binding sequence of miR-206, as shown in Fig. 3A. To determine this potential interaction, a luciferase reporter assay was conducted in SE-induced hippocampus cells. As a result, the luciferase activity of a luciferase vector containing H19-wt was consistently reduced by upregulating miR-206 via miR-206 mimic transfection, whereas accelerated by downregulating miR-206 via anti-miR-206 transfection in 293T cells (Fig. 3B, C, Fig. S1B). Additionally, no significant changes were observed in luciferase activity of the H19-mut vector after any transfection. Furthermore, miR-206 and H19 were simultaneously enriched in RIP derived from Ago2 antibody in cell extract of primary hippocampus neurons (Fig. 3D); moreover, Bio-miR-206 mimic could abundantly enrich H19 expression in 293FT cells (Fig. 3E). These outcomes suggested a direct target relationship between H19 and miR-206. Besides, miR-206 expression levels were induced by H19 knockdown via sh-H19 lentivirus infection and descended by H19 overexpression via H19 lentivirus infection in hippocampus neurons (Fig. 3F, Fig. S1A). These results showed that H19 could negatively regulate miR-206 expression via acting as a miR-206 decoy.
The interaction between H19 and miR-206. A The in silicon data on miRcode showed the complementary binding sites between H19 and miR-206. The wild type of H19 (H19-wt) was mutated and named as H19-mut. B, C Relative luciferase activity of H19-wt/mut was measured by luciferase reporter assay in 293T cells co-transfected with H19-wt/mut and either miR-206/NC or miR-206/NC inhibitor (anti-miR-206/NC). D RNA immunoprecipitation assay examined relative enrichment of H19 in primary hippocampus neurons. E RNA pull-down assay detected relative enrichment of H19 in 293T cells transfected with biotin-labeled miR-206 (Bio-miR-206) or its control Bio-NC. F RT-qPCR detected miR-206 expression level in hippocampus neurons lentivirus infected with sh-H19, si-NC, H19 or empty lentiviral vector (vector). Data represent mean ± SEM. *P < 0.05
Knockdown of miR-206 counteracted the suppressive role of H19 silencing in KA-induced hippocampus neurons in vitro
Rescue experiments with transfection of sh-H19 alone or combined with anti-miR-206 were carried out, and expression of miR-206 was upregulated in sh-H19-transfected hippocampus neurons under KA treatment, which was abolished by co-infected of anti-miR-206 (Fig. 4A). The silence of miR-206 abated the inhibition of H19 knockdown on EdU positive cells (Fig. 4B) and apoptotic rate (Fig. 4C), as well as expression of BAX6A7 and cleaved caspase 3 expression (Fig. 4D), and LC3-II/I and Beclin 1 (Fig. 4E) in KA-treated neurons. In addition, the protection of sh-H19 lentivirus infection against pro-inflammatory factors TNF-α, IL-1β and IL-6 secretions (Fig. 4F–H), and MDA production (Fig. 4I) was impaired in KA + sh-H19 + anti-miR-206 group than KA + sh-H19 + anti-NC group. By the way, H19 silencing promoted Bcl-2 expression and SOD production in KA-challenged hippocampus neurons, and this promotion was abrogated by simultaneous downregulation of H19 and miR-206 (Fig. 4D, J). These data indicated the suppressive role of H19 knockdown in KA-induced apoptosis, autophagy, inflammatory response, and oxidative stress presumably through upregulating its target miR-206, indicating that the H19/miR-206 axis took part in KA-induced hippocampal neurons injury.
Influence of miR-206 expression on the suppressive role of H19 knockdown in KA-induced epilepsy in primary hippocampus neurons in vitro. Hippocampus neurons were lentivirus infected with sh-H19 or si-NC, or co-infected with sh-H19 and anti-miR-206/NC prior to KA treatment. A RT-qPCR measured miR-206 level. B EdU-positive cells were measured by EdU assay. C Flow cytometry determined apoptotic rate. D, E Western blotting evaluated Bcl-2, BAX6A7, C-caspase 3, Beclin 1, and LC3 levels. F–H ELISA examined TNF-α, IL-1β and IL-6 secretions. I, J Commercial assay kits determined MDA and SOD products. Data represent mean ± SEM. *P < 0.05
H19 knockdown promoted the activation of the PI3K-AKT signaling pathway through upregulating miR-206 in hippocampus neurons under KA treatment
The involved signaling pathways were dug out, and western blotting was performed to examine the key protein levels in PI3K/AKT signaling. According to the results in Fig. 5A, B, p-PI3K and p-AKT expression levels were lower in KA-induced hippocampus cells, implying that KA caused PI3K/AKT signaling inhibition in the latent period of epilepsy; while knockdown of H19 by transfecting sh-H19 could apparently recover its activation. Co-infection of anti-miR-206 lentivirus counteracted the promoting effect of sh-H19 lentivirus infection on p-PI3K and p-AKT expression in KA-induced hippocampus neurons, which was in line with the impact of LY, an inhibitor of the PI3K-AKT signaling pathway (Fig. 5A, B). Thus, we considered that H19 knockdown activated the PI3K/AKT signaling pathway in KA-induced hippocampus neurons via liberating miR-206.
The H19/miR-206 axis promoted the activation of phosphatidylinositol 3-kinase (PI3K)/AKT signaling pathway in KA-induced epilepsy in primary hippocampus neurons in vitro. Hippocampus neurons were lentivirus infected with sh-H19 or si-NC, and co-infected with sh-H19 and anti-miR-206/NC. 25 μM of LY294002 (LY), a PI3K/AKT inhibitor, was simultaneously exposed to sh-H19-transfected neurons for 24 h. A Expression of phosphorylated PI3K and AKT (p-PI3K and p-AKT) and total PI3K and AKT (PI3K and AKT) was evaluated by western blotting. B Protein bands of p-PI3K and p-AKT were quantified by densitometry, normalized to PI3K and AKT, respectively. Data represent mean ± SEM. *P < 0.05
Discussion
Emerging pieces of evidence had gained attention to lncRNAs for the treatment of epilepsy. For example, several dysregulations of vitamin D receptor-related lncRNAs had been revealed in the peripheral blood of epileptic patients compared to healthy subjects (Mazdeh et al. 2019). High-throughput sequencing was also used to profile the transcriptome of deregulated circRNAs (Li et al. 2018), a type of lncRNAs with a closed-loop structure. In an animal model with chronic epilepsy, comprehensive profiling of lncRNAs and mRNAs was performed in mouse models induced by pilocarpine and KA (Lee et al. 2015; Jang et al. 2018). Moreover, the lncRNA-mRNA network and lncRNA-miRNA-mRNA network had been well-established in epilepsy (Lee et al. 2015; Jang et al. 2018; Luo et al. 2019). In this present study, we discussed the function and regulatory mechanism of H19 in epilepsy patients and KA-induced hippocampus neurons isolated from neonatal rats. Notably, a direct interaction between H19 and miR-206 was further confirmed in hippocampal neurons under KA treatment.
The systematic functions and downstream targets of H19 had been explored using high-throughput microarray analysis, as well as signaling pathways. As a result, H19 dysregulation exhibited diverse cellular functions related to SE-induced hippocampus cell injury including inflammatory response, apoptosis, immune response and demyelination (Han et al. 2017). In the present study, our data supported the notion that H19 was associated with hippocampus injuries, and knockdown of H19 resulted in lowered apoptosis, autophagy, inflammatory response and oxidative stress in hippocampus neurons under KA treatment. As previously reported, H19 accentuated neuron apoptosis in a rat model of epilepsy, suggesting a promoting role of H19 in epileptogenesis (Han et al. 2018a). Besides, H19 upregulation might underlay epileptogenesis by promoting hippocampal glial cell activation and inflammatory response (Han et al. 2018b). Moreover, downregulation of H19 was also demonstrated to suppress streptozotocin-induced hippocampus neuron apoptosis and oxidative stress in mice model of diabetes mellitus (Yu et al. 2019). These findings together suggest that H19 expression might contribute to hippocampal neurodegeneration through multiple mechanisms, including signaling pathways and H19/miRNAs axis. Here, we confirmed that miR-206 was sponged by H19 via target binding, and thereby participated in epileptogenesis, at least, through PI3K/AKT signaling pathway (Fig. 6), a well-documented pathway in epilepsy (Duan et al. 2018; Liu et al. 2019; Wu and Yi 2018). However, the influence of the H19/miR-206 axis on downstream gene expression remained to be further investigated.
miR-206 had been implicated in hippocampus neurons in a broad spectrum of neurological disorders, such as Alzheimer’s disease (Tian et al. 2014), depression (Yang et al. 2014), as well as epilepsy (Wu et al. 2019). In epilepsy, expression of miR-206 was found to be lower in hippocampus tissues compared to the cortex during KA-induced SE, and injection of miR-206 agomir led to inhibition of seizure activity, neuron loss and IL-1β expression through targeting C–C Motif chemokine ligand 2 (CCL2). Intriguingly, the linking between miR-206 and drug resistance was explained in epilepsy models (Moon et al. 2014). By the way, the brain-derived neurotrophic factor (BDNF) gene was wildly recognized to be a target for miR-206 ranging from cancers to neurological diseases (Tajbakhsh et al. 2017). Even though CCL2 and BDNF played a vital role in epileptogenesis (Tian et al. 2017; Soysal et al. 2016), it was unclear that miR-206 is involved in epilepsy. Here, we uncovered that miR-206 upregulation showed a suppressive effect on cell apoptosis, autophagy, inflammatory response, and oxidative stress in hippocampus neurons under KA treatment (Fig. 6).
Recently, several lncRNAs including H19 (Han et al. 2018a) had been uncovered to take part in the inflammatory response and hippocampus neuronal apoptosis. Meanwhile, autophagy, another cellular process, was also discovered to lead to neuronal loss. Codogno and Meijer (2005) observed that epilepsy was accompanied by increased oxidative stress, ATP exhaust, TNF-α and unbalanced ion fluxes, thereby inducing and aggravating the autophagy. However, the autophagy-related miRNAs and lncRNAs in epilepsy remained poorly investigated, even though these informative RNAs were popular in cancers (Gan et al. 2015). In this study, we demonstrated a novel H19/miR-206 axis in KA-induced cellular events alterations in hippocampus neurons including autophagy and oxidative stress. Moreover, the inhibition of the PI3K/AKT signaling pathway was confirmed to be activated when H19 silence and/or miR-206 upregulation exerted the protective role in KA-induced primary hippocampal neurons. Coincidently, Wu and Yi (2018) put forward a protective role of MALAT1 downregulation from excessive autophagy and apoptosis through activating PI3K/AKT signaling pathway in pilocarpine-injected rats with epilepsy. miR-206 had been documented to control PI3K/AKT signaling pathway probably by targeting functional genes and regulating downstream signals in human cells (Liu et al. 2018; Ma et al. 2018). However, the association between miR-206 and PI3K/AKT seemed to be firstly exploited in this study, but unluckily it was still unclear how H19/miR-206 regulated PI3K/AKT signaling yet. This underlying mechanism should be further studied in the near further.
Conclusion
In conclusion, we proposed an upregulation of H19 and a downregulation of miR-206 in hippocampus neurons in KA-induced epilepsy in vitro. Knockdown of H19 or overexpression of miR-206 could suppress KA-induced apoptosis, autophagy, inflammatory response, and oxidative stress in hippocampus neurons via H19/miR-206 axis and PI3K/AKT signaling pathway (Fig. 6). Our data provided a novel H19/miR-206 axis in epileptogenesis, and it could be a target for epilepsy therapy.
Availability of data and materials
The analyzed data sets generated during the present study are available from the corresponding author on reasonable request.
References
Bielefeld P, Mooney C, Henshall DC, Fitzsimons CP (2017) miRNA-mediated regulation of adult hippocampal neurogenesis; implications for epilepsy. Brain Plast 3(1):43–59
Brindley E, Hill TDM, Henshall DC (2019) MicroRNAs as biomarkers and treatment targets in status epilepticus. Epilepsy Behav 101(Pt B):106272
Chen S, Liu D, Zhou Z, Qin S (2021) Role of long non-coding RNA H19 in the development of osteoporosis. Mol Med (cambridge, Mass) 27(1):122
Codogno P, Meijer AJ (2005) Autophagy and signaling: their role in cell survival and cell death. Cell Death Differ 12(Suppl 2):1509–1518
Duan W, Chen Y, Wang XR (2018) MicroRNA155 contributes to the occurrence of epilepsy through the PI3K/Akt/mTOR signaling pathway. Int J Mol Med 42(3):1577–1584
Gan J, Qu Y, Li J, Zhao F, Mu D (2015) An evaluation of the links between microRNA, autophagy, and epilepsy. Rev Neurosci 26(2):225–237
Ghafouri-Fard S, Esmaeili M, Taheri M (2020) H19 lncRNA: roles in tumorigenesis. Biomed Pharmacother 123:109774
Han CL, Liu YP, Zhao XM, Wang KL, Chen N, Hu W, Zhang JG, Ge M, Meng FG (2017) Whole-transcriptome screening reveals the regulatory targets and functions of long non-coding RNA H19 in epileptic rats. Biochem Biophys Res Commun 489(2):262–269
Han CL, Ge M, Liu YP, Zhao XM, Wang KL, Chen N, Hu W, Zhang JG, Li L, Meng FG (2018a) Long non-coding RNA H19 contributes to apoptosis of hippocampal neurons by inhibiting let-7b in a rat model of temporal lobe epilepsy. Cell Death Dis 9(6):617
Han CL, Ge M, Liu YP, Zhao XM, Wang KL, Chen N, Meng WJ, Hu W, Zhang JG, Li L et al (2018b) LncRNA H19 contributes to hippocampal glial cell activation via JAK/STAT signaling in a rat model of temporal lobe epilepsy. J Neuroinflamm 15(1):103
Hauser RM, Henshall DC, Lubin FD (2018) The epigenetics of epilepsy and its progression. Neuroscientist 24(2):186–200
Henshall DC, Kobow K (2015) Epigenetics and epilepsy. Cold Spring Harbor Perspect Med 5(12):a022731
Jang Y, Moon J, Lee ST, Jun JS, Kim TJ, Lim JA, Park BS, Yu JS, Park DK, Yang AR et al (2018) Dysregulated long non-coding RNAs in the temporal lobe epilepsy mouse model. Seizure 58:110–119
Kaneko Y, Sullivan R, Dailey T, Vale FL, Tajiri N, Borlongan CV (2016) Kainic acid-induced golgi complex fragmentation/dispersal shifts the proteolysis of reelin in primary rat neuronal cells: an in vitro model of early stage epilepsy. Mol Neurobiol 53(3):1874–1883
Kaneko Y, Pappas C, Malapira T, Vale FL, Tajiri N, Borlongan CV (2017) Extracellular HMGB1 modulates glutamate metabolism associated with kainic acid-induced epilepsy-like hyperactivity in primary rat neural cells. Cell Physiol Biochem 41(3):947–959
Kwon CS, Wagner RG (2022) The worldwide epilepsy treatment gap: a systematic review and recommendations for revised definitions—a report from the ILAE Epidemiology Commission. Epilepsia 63(3):551–564
Lee DY, Moon J, Lee ST, Jung KH, Park DK, Yoo JS, Sunwoo JS, Byun JI, Lim JA, Kim TJ et al (2015) Dysregulation of long non-coding RNAs in mouse models of localization-related epilepsy. Biochem Biophys Res Commun 462(4):433–440
Li J, Lin H, Sun Z, Kong G, Yan X, Wang Y, Wang X, Wen Y, Liu X, Zheng H et al (2018) High-throughput data of circular RNA profiles in human temporal cortex tissue reveals novel insights into temporal lobe epilepsy. Cell Physiol Biochem 45(2):677–691
Liu TJ, Wang B, Li QX, Dong XL, Han XL, Zhang SB (2018) Effects of microRNA-206 and its target gene IGF-1 on sevoflurane-induced activation of hippocampal astrocytes in aged rats through the PI3K/AKT/CREB signaling pathway. J Cell Physiol 233(5):4294–4306
Liu AH, Chu M, Wang YP (2019) Up-regulation of Trem2 inhibits hippocampal neuronal apoptosis and alleviates oxidative stress in epilepsy via the PI3K/Akt pathway in mice. Neurosci Bull 35(3):471–485
Lu J, Zhou N, Yang P, Deng L, Liu G (2019) MicroRNA-27a-3p downregulation inhibits inflammatory response and hippocampal neuronal cell apoptosis by upregulating mitogen-activated protein kinase 4 (MAP2K4) expression in epilepsy: in vivo and in vitro studies. Med Sci Monit 25:8499–8508
Luo ZH, Walid AA, Xie Y, Long H, Xiao W, Xu L, Fu Y, Feng L, Xiao B (2019) Construction and analysis of a dysregulated lncRNA-associated ceRNA network in a rat model of temporal lobe epilepsy. Seizure 69:105–114
Ma Y, Zhou G, Li M, Hu D, Zhang L, Liu P, Lin K (2018) Long noncoding RNA DANCR mediates cisplatin resistance in glioma cells via activating AXL/PI3K/Akt/NF-kappaB signaling pathway. Neurochem Int 118:233–241
Mazdeh M, Zamani M, Eftekharian MM, Komaki A, Arsang-Jang S, Taheri M, Ghafouri-Fard S (2019) Expression analysis of vitamin D receptor-associated lncRNAs in epileptic patients. Metab Brain Dis 34(5):1457–1465
Moon J, Lee ST, Choi J, Jung KH, Yang H, Khalid A, Kim JM, Park KI, Shin JW, Ban JJ et al (2014) Unique behavioral characteristics and microRNA signatures in a drug resistant epilepsy model. PLoS ONE 9(1):e85617
Pitkanen A, Lukasiuk K, Dudek FE, Staley KJ (2015) Epileptogenesis. Cold Spring Harbor Perspect Med 5(10):a022822
Saud AM, Mater HN, Abd-Alrehman RM (2020) Epidemiology, diagnosis and etiology of epilepsy: a review
Soysal H, Dogan Z, Kamisli O (2016) Effects of phenytoin and lamotrigine treatment on serum BDNF levels in offsprings of epileptic rats. Neuropeptides 56:1–8
Tai XY, Bernhardt B, Thom M, Thompson P, Baxendale S, Koepp M, Bernasconi N (2018) Review: Neurodegenerative processes in temporal lobe epilepsy with hippocampal sclerosis: clinical, pathological and neuroimaging evidence. Neuropathol Appl Neurobiol 44(1):70–90
Tajbakhsh A, Mokhtari-Zaer A, Rezaee M, Afzaljavan F, Rivandi M, Hassanian SM, Ferns GA, Pasdar A, Avan A (2017) Therapeutic potentials of BDNF/TrkB in breast cancer; current status and perspectives. J Cell Biochem 118(9):2502–2515
Tellez-Zenteno JF, Hernandez-Ronquillo L (2012) A review of the epidemiology of temporal lobe epilepsy. Epilepsy Res Treat 2012:630853
Thomas AA, Biswas S, Feng B, Chen S, Gonder J, Chakrabarti S (2019) lncRNA H19 prevents endothelial-mesenchymal transition in diabetic retinopathy. Diabetologia 62(3):517–530
Tian N, Cao Z, Zhang Y (2014) MiR-206 decreases brain-derived neurotrophic factor levels in a transgenic mouse model of Alzheimer’s disease. Neurosci Bull 30(2):191–197
Tian DS, Peng J, Murugan M, Feng LJ, Liu JL, Eyo UB, Zhou LJ, Mogilevsky R, Wang W, Wu LJ (2017) Chemokine CCL2-CCR2 signaling induces neuronal cell death via STAT3 activation and IL-1beta production after status epilepticus. J Neurosci 37(33):7878–7892
Trinka E, Brigo F, Shorvon S (2016) Recent advances in status epilepticus. Curr Opin Neurol 29(2):189–198
Van Nieuwenhuyse B, Raedt R, Sprengers M, Dauwe I, Gadeyne S, Carrette E, Delbeke J, Wadman WJ, Boon P, Vonck K (2015) The systemic kainic acid rat model of temporal lobe epilepsy: Long-term EEG monitoring. Brain Res 1627:1–11
Wang L, Liu Y, Lu R, Dong G, Chen X, Yun W, Zhou X (2018) The role of S-nitrosylation of kainate-type of ionotropic glutamate receptor 2 in epilepsy induced by kainic acid. J Neurochem 144(3):255–270
Wu Q, Yi X (2018) Down-regulation of long noncoding RNA MALAT1 protects hippocampal neurons against excessive autophagy and apoptosis via the PI3K/Akt signaling pathway in rats with epilepsy. J Mol Neurosci 65(2):234–245
Wu L, Li Y, Yu M, Yang F, Tu M, Xu H (2018) Notch signaling regulates microglial activation and inflammatory reactions in a rat model of temporal lobe epilepsy. Neurochem Res 43(6):1269–1282
Wu Z, Liu Y, Huang J, Huang Y, Fan L (2019) MiR-206 inhibits epilepsy and seizure-induced brain injury by targeting CCL2. Cytotechnology 71:809–818
Xia J, Li CY, Wang H, Zhang QM, Han ZM (2018) Therapeutic effects of scoparone on pilocarpine (Pilo)-induced seizures in mice. Biomed Pharmacother 97:1501–1513
Yang X, Yang Q, Wang X, Luo C, Wan Y, Li J, Liu K, Zhou M, Zhang C (2014) MicroRNA expression profile and functional analysis reveal that miR-206 is a critical novel gene for the expression of BDNF induced by ketamine. NeuroMol Med 16(3):594–605
Yu JL, Li C, Che LH, Zhao YH, Guo YB (2019) Downregulation of long noncoding RNA H19 rescues hippocampal neurons from apoptosis and oxidative stress by inhibiting IGF2 methylation in mice with streptozotocin-induced diabetes mellitus. J Cell Physiol 234(7):10655–10670
Funding
No funding was received.
Author information
Authors and Affiliations
Contributions
HJ and ZY are totally responsible for this work, including the conceptualization, methodology, formal analysis, data curation, validation, investigation, writing—original draft preparation and writing—review and editing of this work. Both of them approved this manuscript to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval and consent to participate
The present study was approved by the ethical review committee of Weihai Central Hospital. Written informed consent was obtained from all enrolled patients.
Patient consent for publication
Not applicable.
Additional information
Communicated by Sreedharan Sajikumar.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
221_2022_6392_MOESM1_ESM.tif
Supplementary file1 Figure S1. The gene manipulation efficiency of exogenous nucleotides was used in this study. RT-qPCR measured relative expression of (A) H19 and (B) miR-206 in primary hippocampus neurons lentivirus infected with H19, sh-H19, miR-206, anti-miR-206, or the negative controls. Data represent mean ± SEM. *P < 0.05 (TIF 5746 KB)
221_2022_6392_MOESM2_ESM.tif
Supplementary file2 Figure S2. The effects of H19 and miR-206 in primary hippocampus neurons. (A, F) RT-qPCR measured H19 and miR-206 levels in primary hippocampus neurons lentivirus infected with si-NC, sh-H19, miR-206, or NC. (B, G) Flow cytometry examined apoptotic rate after lentivirus infection. (C-E and H-J) ELISA kits measured TNF-α, IL-1β and IL-6 secretions after lentivirus infection. Data represent mean ± SEM. *P < 0.05 (TIF 15432 KB)
Rights and permissions
About this article
Cite this article
Ju, H., Yang, Z. H19 silencing decreases kainic acid-induced hippocampus neuron injury via activating the PI3K/AKT pathway via the H19/miR-206 axis. Exp Brain Res 240, 2109–2120 (2022). https://doi.org/10.1007/s00221-022-06392-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-022-06392-w