Abstract
A loss of functioning motor units underlies many neuromuscular disorders. The facial nerve innervates the muscles of facial expression, including nasal muscles, which also play an important role in the regulation of airflow resistance. It is difficult to accurately assess motor unit number in the facial muscles, because the muscles are difficult to activate in isolation. Here, we apply the manual McComas method to estimate the number of motor units in a nasal dilator muscle. EMG of the dilator naris was recorded during graded stimulation of the zygomatic branch of the facial nerve in 26 subjects (12 males and 14 females), aged 20–41 years. Each subject was studied twice, on separate days, to estimate method reproducibility. As a check on our use of the McComas method, we also estimated motor unit number in the first dorsal interosseus muscle (FDI) of six subjects, as the muscle is also small and has been studied with the McComas method. Reproducibility was evaluated with a rigorous statistical approach, the Bland–Altman procedure. We estimate that dilator naris is composed of 75 ± 15.6 (SD) motor units, compared to 144 ± 35.5 in FDI. The coefficient of variation for test–retest reproducibility of dilator naris motor unit estimates was 29.6 %, similar to separate-day reproducibility reported for other muscles. Recording and stimulation were done with surface electrodes, and the recordings were of high quality and reproducible. This simple technique could be applied clinically to track motor neuron loss and to monitor facial nerve integrity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A reduction in the number of functioning motor units (defined here as a motoneuron and the muscle fibers it innervates) is an important early indicator of neuromuscular impairment/disease. Thus, the ability to obtain reliable estimates of motor unit number and to monitor motor unit function over time is of considerable clinical importance. Here, we used the McComas method (McComas et al. 1971) to estimate motor unit number in the principal nasal dilator muscle, dilator naris. This muscle originates on the nasal notch of the maxilla and inserts into the ala nasi cartilage, and its principal action is dilation of the external nares (for an interesting discussion of the history of this muscle’s nomenclature, see Figallo and Acosta 2001). Although this muscle is small, it is potentially clinically interesting because it is (1) quite superficial and therefore easily accessible for study via surface EMG, (2) innervated by a cranial nerve, (3) under automatic regulation by respiratory control centers in the brainstem, and (4) also under voluntary/cortical control, e.g., for sniffing and facial expression. Because both the muscle and nerve are relatively superficial, the approach uses surface electrodes for both recording and stimulation. As such, the methods described herein should be useful for the noninvasive assessment of facial nerve damage due to trauma, tumor (e.g., acoustic neuroma), or inflammation (Bell’s palsy).
Materials and methods
Motor unit number estimation (MUNE) of dilator naris was performed in 26 subjects (12 males and 14 females), 20–41 years of age. Experimental procedures were reviewed and approved by the Human Subjects Committee at The University of Arizona, and subjects gave their signed consent prior to participation in the study. All subjects were healthy with no history of neuromuscular disorders, allergies, or deviations of the nasal septum.
Each subject was studied while seated and participated in two MUNE experiments on separate days. MUNEs were made with the manual incremental method, as described by McComas et al. (1971). The EMG of the left dilator naris was recorded with two 3-mm-diameter silver–silver chloride electrodes placed over the external nares, and a ground electrode was placed on the left earlobe, as described previously (Connel and Fregosi 1993; DelloRusso et al. 2002; Schmitt et al. 2009). EMG signals were amplified (A-M Systems), filtered (5 Hz–10 kHz), digitized at 10 kHz, and stored (A.R. Vetter Co.). Stimulation of the facial nerve was delivered via two 8-mm-diameter silver–silver chloride surface electrodes. One electrode was placed over the stylomastoid foramen, just below and slightly posterior to the left ear lobe. The second electrode location was identified with a stimulus wand that was placed on the skin overlying the facial nerve while the stimulator (Grass S48) delivered 0.1-ms duration square wave pulses at a frequency of 1 Hz, as described previously (Fuller et al. 1995; DelloRusso et al. 2002; Schmitt et al. 2009). The wand was moved distally along the course of the nerve until we located the site that produced the largest evoked response with the least amount of noise upon submaximal stimulation, and the second electrode was secured at this site.
The protocol began and ended with three supramaximal stimulations to obtain maximal evoked potentials (M-waves). Equivalent M-wave amplitudes at the beginning and end of the experiment ensured that the electrical properties of the recording and stimulating electrodes did not change. In three trials, the M-wave amplitude differed, the data were discarded, and the experiment was repeated after re-applying all electrodes. The intervening procedure entailed a series of progressively larger submaximal stimulations to recruit unique motor units (see Fig. 1a). The stimulator was set to deliver pulses at 1–1.5 Hz, while the voltage was gradually increased. Once a motor unit was recruited, we alternately increased and decreased the stimulus voltage to values just above and just below the motor unit’s activation threshold. This ensured that the unit was recruited at the same activation threshold and thus was a single unit (see “Discussion” section). Once this criterion was met, the voltage was increased further to recruit a different, larger motor unit. This procedure continued until the maximal number of distinct, reproducible increments was obtained. Based on previously published data, our initial aim was to attain 10 such increments (McComas 1991), but our actual yield ranged from 8 to 16 increments across the 52 trials (two trials per subject).
Estimates of motor unit number in dilator naris and FDI. a Representative record showing increments in the dilator naris EMG obtained by graded, submaximal stimulation of the facial nerve (upper recordings) in (a). The lower recording in a shows the maximal evoked potential (M-wave) in the same subject. As discussed in section “Results,” we estimated 53 motor units in this subject. b Bland–Altman plot showing the difference in motor unit number estimates in dilator naris (trial 1− trial 2), plotted as a function of the average number of motor units for that subject [(mean trial 1 + mean trial 2)/2]. The solid line shows a difference of zero, and the dashed lines represent ±2 SDs of the differences (see text for explanation). c Bland–Altman plot for dilator naris M-waves recorded in each subject. d Motor unit number estimates in dilator naris and FDI in six subjects. Numbers inside rectangles show the group average value for dilator naris and FDI
For comparison with MUNEs made by others, we also made estimates in the left first dorsal interosseus muscle (FDI) in 6 of the 26 subjects. The EMG was recorded with two 3-mm disk electrodes over the belly of the muscle, on the radial side of metacarpal II. The ground electrode was placed on the back of the hand. An 8-mm stimulating electrode was positioned on the ventromedial forearm, about 3 in. proximal to the wrist. The second electrode was positioned as described above, in this case by moving the wand over the ulnar nerve on the ventromedial forearm. The electrode was placed at the point where the largest EMG response was evoked in response to submaximal stimulation. The protocol used for MUNE in FDI was as described above. The number of reproducible increments recorded in these experiments ranged from 7 to 16.
Using commercial software (R.C. Electronics, Computer Scope), all clearly identified and reproducible submaximal increments were overlaid, as shown in the top panel of Fig. 1a. To estimate the average size of motor units in the muscle, the peak-to-peak voltage of the largest of these evoked increments was measured and divided by the number of increments (Fig. 1a, top panel). The M-wave voltage (Fig. 1a, lower panel), representing the synchronous activation of all motor units in the muscle, was then divided by this average value to estimate the total number of motor units in the muscle.
In addition to reporting average MUNE values, we used Bland–Altman plots (Bland and Altman 1986) to assess reproducibility of MUNE and M-wave amplitude. This approach computes the bias, which is the difference between measures obtained in the first and second trials. When the entire subject population is considered, the difference values should be evenly distributed around zero, indicating minimal bias (see Fig. 1, panels b and c). In contrast, test–retest bias in the method is evident if the inter-trial difference is systematically positive or negative. Standard t tests are used to determine whether the bias differs from zero. This analysis also provides a quantitative assessment of test–retest reproducibility by computation of the limit of agreement. If the data are normally distributed, 95 % of the differences will lie between the limits of agreement, defined as:
where D is the mean difference, SD is the standard deviation of the mean differences, and 1.96 is the z score for the 95 % confidence interval. If the assumption of normality is realized, the coefficient of reproducibility is simply twice the standard deviation of the differences obtained between trial 1 and trial 2. The coefficient of variation can then be computed by dividing this value by the overall mean: [mean trial 1 + mean trial 2]/2.
Results
The results of a representative experiment performed on the dilator naris muscle are shown in Fig. 1a. In this example, we identified 13 increments, with the largest increment about 0.96 mV (top panel in Fig. 1a). Dividing 0.96 mV by 13 increments yields an estimated average motor unit size of 74 µV. Dividing the M-wave amplitude (3.94 mV) by the average motor unit size (74 µV) gives an estimate of 53 motor units; the data point from this experiment is indicated by the arrow in Fig. 1b. Note that reproducibility in this subject was perfect, with a MUNE of 53 on both days. The MUNE for the dilator naris in all 26 subjects averaged 74.9 ± 15.6 for trial 1 and 74.3 ± 15.1 for trial 2 (mean ± SD). Bland–Altman analysis of reliability (Fig. 1b) revealed a bias of 0.62 ± 10.9, which is not significantly different from zero (t = 0.29, P = 0.775, df = 25), indicating that there were no systematic errors in day-to-day reproducibility. In addition, the difference values were not systematically related to the average MUNE (x-axis in Fig. 1b), indicating that reproducibility does not depend on the number of motor units in the muscle. The 95 % limits of agreement extend from −20.8 to 22.0 (horizontal dashed lines in Fig. 1b), and even with the one outlier, more than 95 % of the data points lie within the limits of agreement expected for normally distributed data. The coefficient of reproducibility averaged 22 motor units (10.9 × 2), which translates into a coefficient of variation of 29.5 % (22 divided by 74.6, which is the average of the means computed on day 1 and day 2).
The M-wave amplitude averaged 3.4 ± 1.9 mV for trial 1 and 3.3 ± 1.5 mV for trial 2. Because of the small size of the myofibers, positioning of both recording and stimulating electrodes for each experimental session likely entailed changes in their location, impedance, and other biophysical properties, which may explain why reproducibility of M-wave amplitude was relatively poor (Fig. 1c); the 95 % limit of agreement extended from −3.7 to 4.0 (horizontal dashed lines in Fig. 1c). Nonetheless, 95 % of the 26 difference values were within the limits of agreement, consistent with normally distributed data. The bias averaged 0.14 ± 1.9, which was not significantly different than zero (t = 0.37, P = 0.72, df = 25), indicating that between-experiment variability was random, not systematic. The lack of correlation in Fig. 1c indicates that reproducibility is independent of absolute M-wave amplitude. The coefficient of reproducibility averaged 3.96 mV, which translates into a coefficient of variation of 118.5 % (3.96 divided by 3.34, which is the average of the means computed on day 1 and day 2).
We carried out MUNE on both dilator naris and the FDI in six of the subjects (Fig. 1d). The number of dilator naris motor units in these six subjects averaged 78.8 ± 11.4, compared to 144 ± 35.5 in the FDI (paired t test, t = 3.87, P = 0.0118).
Discussion
The nasal dilator muscles are unique in several ways. They participate in both automatic (respiration-related drive) and voluntary behaviors (sniffing and facial expression), have very small myofibers, do not cross a joint, lack muscle spindles and fascia, etc. (see Cattaneo and Pavesi 2014 for review). The muscles originate on bone or cartilage and insert into cartilage, skin, other muscles, or connective tissue (Griesman 1944) and are grouped functionally as elevators (shorten the nose while dilating the nostrils); depressors (lengthen and dilate); compressors (lengthen and narrow); and dilators (dilate the external nares). Thus, with the exception of the compressor muscles, all nasal muscles assist in widening the nasal opening, especially during labored breathing (Bridger 1970; Bridger and Proctor 1970; Haight and Cole 1983; Connel and Fregosi 1993; Fregosi and Lansing 1995; Sullivan et al. 1996). The zygomatic branch of the facial nerve innervates the nasal muscles. Here, we applied the McComas method (McComas et al. 1971) to estimate the number of motor units in the dilator naris, providing the first estimates of motor unit number in this muscle, and showing that this unique nerve-muscle preparation can be used to track the loss of motor units in facial muscles and to evaluate facial nerve integrity.
Critique of Method
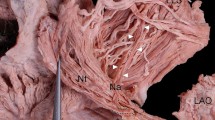
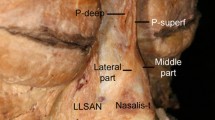
The manual incremental method rests upon the following assumptions (McComas et al. 1971). The first is that the EMG reflects activity in only the muscle of interest. Based upon our previous studies (Fuller et al. 1995), showing that the dilating force produced by the external nares during incremental exercise was highly correlated with dilator naris EMG activity (r = 0.90), this assumption seems well supported. Although we cannot rule out contamination from other small nasal muscles, we note that the muscles are separated by cartilage, and the nasalis, which lies closest to dilator naris, is considered a nasal compressor rather than a dilator (Griesman 1944). Inasmuch as facial nerve stimulation always evoked dilation of the nares, we assume that this is the result of specific activation of dilator naris.
The second assumption is that the evoked responses are from single motor units, not a combination of two or more units that may or may not be activated simultaneously, a phenomenon that has been termed “alternation.” McComas et al. (1971) and Brown and Milner-Brown (1976; Brown et al. 1988) concluded that an incremental action potential response can be assumed to arise from a unique motor unit only if the same stimulation voltage activates the unit on two or more occasions. We applied this rule here and in most cases were successful in evoking each unit at the same voltage on more than two occasions, indicating that alternation was minimized. Nonetheless, (Stein and Yang 1990) compared the McComas method with spike-triggered averaging and intramuscular microstimulation to estimate the number of motor units in the thenar muscle of 10 healthy subjects. Although there were no significant differences between methods, the number of motor units averaged 170, 135, and 122 with the McComas method, spike-triggered averaging, and microstimulation, respectively. Simulation studies showed that by the tenth motor unit recruitment, the probability of alternation was 65 %; from these data, Stein and Yang concluded that because of alternation the McComas method underestimates average motor unit size and overestimates motor unit number. Thus, it is likely that at least some alternation occurred in our studies and may have lead to an overestimation of motor unit number.
A third assumption is that the amplitude of the evoked responses used in the calculation of the average motor unit number sums additively. If, however, the negative phase of one motor unit potential overlaps with the positive phase of another, the units can “cancel” each other (Day and Hulliger 2001; Keenan et al. 2006). For the technique used here, cancelation would most likely occur if there were differences in motor unit conduction velocity (Keenan et al. 2006). Although cancelation can be minimized by stimulating over the muscle’s end-plate zone, this is not possible in the dilator naris muscle, because like most facial muscles it has diffusely distributed end plates, rather than the single band observed in most limb muscles (Happak et al. 1997). Nonetheless, as shown in Fig. 1a, each of the evoked motor unit potentials dip negatively before the large positive deflection, suggesting—though not proving—that the evoked potentials should sum additively. This pattern of activation was observed in all subjects and trials.
The final assumption is that motor unit potentials used to determine the average motor unit size are representative of the total motor unit population and not biased toward recruitment of smaller or larger motor units. Several factors influence whether or not a given axon will be brought to firing threshold during stimulation of muscle nerves, including the tendency for large-diameter axons to be preferentially recruited, the relative positions of the axons in the nerve trunk, and the distribution of blood vessels and connective tissue within and around the nerve. Examination of our records (see Fig. 1a) showed that the size of individual increments is fairly close, though a size distribution is obvious. However, with the exception of the very first increments, the size distribution was randomly distributed, and not biased by smaller increments early in the procedure (i.e., at low stimulation voltage) or larger increments later.
Reproducibility
Confidence in a method depends largely on its reproducibility. Here, we used the Bland–Altman approach to assay the reproducibility of the technique (Bland and Altman 1986). With this approach, the coefficient of variation is computed on the average and SD of the differences measured on trial 1 and trial 2, rather than using the population mean and SD of the absolute measurements, as the latter underestimates the variability unless the sample is very large (Sokal and Rohlf 1995). The distinction between the two approaches is best illustrated by our own data, where the coefficient of variation using population average and SD data is 21 %, compared to 29.6 % using the Bland–Altman approach (29.6 %). Similarly, the population coefficient of variation for our M-wave data was 59 %, compared to 118.5 % using the Bland–Altman approach. We were unable to find other studies that used the Bland–Altman approach to estimate day-to-day reproducibility of motor unit number estimation. Nevertheless, if we rely only on conventionally computed coefficient of variation values, our data are well within values reported by others in limb and facial muscles (for review, see McComas 1991).
MUNE in other muscles
To our knowledge, the only electrophysiologic measures of motor unit number in muscles innervated by cranial nerves have been made in facial muscles. Delbeke (Delbeke 1982) used the manual incremental method to determine the MUNE in facial muscles. Using broad categorizations including the “eyelid and mouth areas,” it was estimated that there were 156 motor units in the former and 187 in the latter. Defaria et al. (1979) focused more specifically on orbicularis oculi and found 73 motor units, supporting the idea that the estimates of Delbeke included motor units from multiple muscles around the eye. There have been several estimates of axon number in cranial nerve branches innervating laryngeal muscles (cricothyroid, posterior cricoarytenoid, and transverse arytenoid), the masseter, and the rectus lateralis. The number of motor axons estimated was 112–140 in the laryngeal muscles, 1452 in masseter, and 4150 in rectus lateralis (summarized in Enoka 1995). Although estimating the number of motor axons in a nerve specimen is based on the assumption that about 50 % of the fibers are motor, such data are considered reasonable approximations (Enoka 1995). If we accept these estimates, our findings are well within the range for small laryngeal muscles and very consistent with data in orbicularis oculi, which increases our confidence in the method. Given that facial muscle fibers show polyneuronal innervation (Happak et al. 1997), it would be extremely interesting to learn how many motor axons supply the fibers of the dilator naris and other facial muscles. Many estimates of motor unit number have been made in small hand muscles, including the thenar group (116–342 motor units), the hypothenar group (300–390 units), abductor digiti minimi (50–100 units), FDI (130 units) and abductor pollicis longus (421 units) (reviewed in McComas 1991). The reported value for FDI compares favorably with our own data, showing an average of 144 units. Moreover, estimates in a single male subject show that there are 119 motor axons supplying the FDI (Enoka 1995), which is consistent with physiological estimates of motor unit number.
Significance
Facial nerve stimulation has been used to evaluate nerve integrity, including intra-operative monitoring during tumor removal and other procedures that may damage the facial nerve (Devi et al. 1978; Kirkpatrick et al. 1991; Wedekind and Klug 2001). Interestingly, the quality of compound muscle action potentials recorded from the nasalis muscle was considered far superior to that obtained from orbicularis oculi, owing to much better signal to noise ratio (Rosler et al. 1989). Our earlier studies confirm this, with very high signal/noise ratios in surface EMG recordings, whether contractions are volitional (voluntary flaring Fuller et al. 1995; DelloRusso et al. 2002; Schmitt et al. 2009), automatic (evoked by exercise or carbon dioxide stimulation) (Connel and Fregosi 1993; Fregosi and Lansing 1995; Fuller et al. 1995; Sullivan et al. 1996), or evoked electrically (Fuller et al. 1995; Mateika et al. 1998; DelloRusso et al. 2002; Schmitt et al. 2009). Given the high quality of the recordings, the ease of recording and stimulation, the minimal equipment necessary, and the ability to collect the data without requiring effort by the subject, we are hopeful that this method will be utilized clinically to track motor unit loss and facial nerve integrity. Applications may include motor unit loss due to aging and disease, and facial nerve damage due to trauma, tumor (e.g., acoustic neuroma), or inflammation (Bell’s palsy). Nonetheless, given that the inter-trial variability is in the range of 20–30 %, small changes in motor unit number will not be easily detected, and it will be critical to have a substantial amount of normative data for comparison.
References
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Bridger GP (1970) Physiology of the nasal valve. Arch Otolaryngol 92:543–553
Bridger GP, Proctor DF (1970) Maximum nasal inspiratory flow and nasal resistance. Ann Otol Rhinol Laryngol 79:481–488
Brown WF, Milner-Brown HS (1976) Some electrical properties of motor units and their effects on the methods of estimating motor unit numbers. J Neurol Neurosurg Psychiatry 39:249–257
Brown WF, Strong MJ, Snow R (1988) Methods for estimating numbers of motor units in biceps-brachialis muscles and losses of motor units with aging. Muscle Nerv 11:423–432. doi:10.1002/mus.880110503
Cattaneo L, Pavesi G (2014) The facial motor system. Neurosci Biobehav Rev 38:135–159
Connel DC, Fregosi RF (1993) Influence of nasal airflow and resistance on nasal dilator muscle activities during exercise. J Appl Physiol 74:2529–2536
Day SJ, Hulliger M (2001) Experimental simulation of cat electromyogram: evidence for algebraic summation of motor-unit action-potential trains. J Neurophysiol 86:2144–2158
Defaria CR, de Melo-Souza SE, Lima AF (1979) Motor unit estimation in the orbicularis oculi muscle. In: 6th International congress of electromyography, vol 60. Acta Neurologica Scandinavica, Supplement, Stockholm, p 73
Delbeke J (1982) Reliability of the motor unit count in the facial muscles. Electromyogr Clin Neurophysiol 22:277–290
DelloRusso C, Khurana N, Rankin L, Sullivan J, Fregosi RF (2002) Mechanisms of force failure during repetitive maximal efforts in a human upper airway muscle. Muscle Nerv 26:94–100
Devi S, Challenor Y, Duarte N, Lovelace RE (1978) Prognostic value of minimal excitability of facial nerve in Bell’s palsy. J Neurol Neurosurg Psychiatry 41:649–652
Enoka RM (1995) Morphological features and activation patterns of motor units. J Clin Neurophysiol 12:538–559
Figallo EE, Acosta JA (2001) Nose muscular dynamics: the tip trigonum. Plast Reconstr Surg 108:1118–1126
Fregosi RF, Lansing RW (1995) Neural drive to nasal dilator muscles: influence of exercise intensity and oronasal flow partitioning. J Appl Physiol 79:1330–1337
Fuller D, Sullivan J, Essif E, Personius K, Fregosi RF (1995) Measurement of the EMG–force relationship in a human upper airway muscle. J Appl Physiol 79:270–278
Griesman B (1944) Muscles and cartilages of the nose from the standpoint of a typical rhinoplasty. Arch Otolaryngol 39:334–341
Haight JS, Cole P (1983) The site and function of the nasal valve. Laryngoscope 93:49–55
Happak W, Liu J, Burggasser G, Flowers A, Gruber H, Freilinger G (1997) Human facial muscles: dimensions, motor endplate distribution, and presence of muscle fibers with multiple motor endplates. Anat Rec 249:276–284
Keenan KG, Farina D, Merletti R, Enoka RM (2006) Amplitude cancellation reduces the size of motor unit potentials averaged from the surface EMG. J Appl Physiol 100:1928–1937. doi:10.1152/japplphysiol.01282.2005
Kirkpatrick PJ, Watters G, Strong AJ, Walliker JR, Gleeson MJ (1991) Prediction of facial nerve function after surgery for cerebellopontine angle tumors: use of a facial nerve stimulator and monitor. Skull Base Surg 1:171–176
Mateika JH, Essif EG, Dellorusso C, Fregosi RF (1998) Contractile properties of human nasal dilator motor units. J Neurophysiol 79:371–378
McComas AJ (1991) Invited review: motor unit estimation: methods, results, and present status. Muscle Nerv 14:585–597. doi:10.1002/mus.880140702
McComas AJ, Fawcett PR, Campbell MJ, Sica RE (1971) Electrophysiological estimation of the number of motor units within a human muscle. J Neurol Neurosurg Psychiatry 34:121–131
Rosler KM, Hess CW, Schmid UD (1989) Investigation of facial motor pathways by electrical and magnetic stimulation: sites and mechanisms of excitation. J Neurol Neurosurg Psychiatry 52:1149–1156
Schmitt K, DelloRusso C, Fregosi RF (2009) Force–EMG changes during sustained contractions of a human upper airway muscle. J Neurophysiol 101:558–568. doi:10.1152/jn.90922.2008
Sokal RR, Rohlf FJ (1995) Biometry. Freeman, New York
Stein RB, Yang JF (1990) Methods for estimating the number of motor units in human muscles. Ann Neurol 28:487–495. doi:10.1002/ana.410280404
Sullivan J, Fuller D, Fregosi RF (1996) Control of nasal dilator muscle activities during exercise: role of nasopharyngeal afferents. J Appl Physiol 80:1520–1527
Wedekind C, Klug N (2001) Recording nasal muscle F waves and electromyographic activity of the facial muscles: a comparison of two methods used for intraoperative monitoring of facial nerve function. J Neurosurg 95:974–978. doi:10.3171/jns.2001.95.6.0974
Acknowledgments
We thank Alan McComas, M.D., for advice with the method and interpretation of the data, E. Fiona Bailey, Ph.D., for a critical evaluation of the manuscript and Elik Essif, M.S. for technical support. These studies were supported by NIH Grant HL 51056.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Patel-Khurana, N., Fregosi, R.F. Motor unit number in a small facial muscle, dilator naris . Exp Brain Res 233, 2897–2902 (2015). https://doi.org/10.1007/s00221-015-4359-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-015-4359-9