Abstract
Rationale
The behavioral and reward-related effects of stimulant drugs have been studied extensively; yet the effect of stimulants on sensory processing is still relatively unknown. Prior brain imaging studies have shown that single doses of stimulant drugs increase neural function during cognitive and attentional processes. However, it is not clear if stimulant drugs such as methamphetamine (MA) affect neural responses to novel sensory stimuli, and whether these effects depend on the visual features of the stimuli.
Objective
In this study, we examined the effects of a single dose of MA (20 mg oral) on neural activation in response to visual stimuli that varied on “non-straight edges” (NSE), a low-level visual feature that quantifies curved/fragmented edges and is related to perceived image complexity.
Methods
Healthy adult participants (n = 18) completed two sessions in which they received MA and placebo in counterbalanced order before an fMRI scan where they viewed both high and low NSE images. Participants also completed measures of subjective drug effects throughout both sessions.
Results
During both sessions, high NSE images activated primary visual cortex to a greater extent than low NSE images. Further, MA increased activation only for low NSE images in three areas of visual association cortex: left fusiform, right cingulate/precuneus, and posterior right middle temporal gyrus. This interaction was unrelated to subjective drug effects.
Conclusions
These findings suggest that stimulant drugs may change the relative sensitivity of higher order sensory processing to increase visual attention when viewing less complex stimuli. Moreover, MA-induced alterations in this type of sensory processing appear to be independent of the drugs’ ability to increase feelings of well-being.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The behavioral and neurochemical effects of stimulant drugs have been well characterized. Presumably through actions on noradrenergic and dopaminergic systems, stimulants enhance cognitive performance, reduce inattention and impulsive behavior, and improve memory (de Wit et al. 2000; Eagle et al. 2007; Jonkman et al. 1997). These actions likely underlie their therapeutic effects in the treatment of attention deficit hyperactivity disorder (Briars and Todd 2016). However, some of these same effects may contribute to their abuse potential. That is, stimulants may increase reactivity to certain sensory stimuli in ways that increase the salience of contextual stimuli.
Both noradrenergic and dopaminergic systems are involved in sensory processing of neutral stimuli and stimuli with valence, such as conditioned stimuli (Anderson et al. 2016; Berridge and Waterhouse 2003; Schultz et al. 2000; Volkow and Morales 2015). For example, in a recent study using a signal detection procedure in rats, Navarra et al. (2017) found that methylphenidate, an indirect agonist at catecholamine receptors, improved reaction times for correct responses in a signal detection task, suggesting that the drug facilitated behavioral efficiency during task performance. Navarra and Waterhouse (2016) propose that stimulants like methylphenidate enhance sensory signals and that these effects are likely to contribute to the drugs’ capacity to facilitate performance of goal-directed behaviors.
Brain imaging studies in humans have shown that single doses of stimulant drugs alter neural function in relation to both inhibitory and attentional processes. For example, methylphenidate and modafinil modulate response inhibition networks (Schmidt et al. 2017), and modafinil increases activation in the occipital lobe in the alerting network (Ikeda et al. 2017). Methylphenidate increased brain connectivity during a muscle-fatiguing exercise (King et al. 2017), and strengthened functional brain networks related to attention (Rosenberg et al. 2016). In one early study (Uftring et al. 2001), we found that a single dose of d-amphetamine (compared to placebo) increased neural activity in the visual cortex during exposure to a visual stimulus, as well as increasing activity in the motor cortex during a motor task. However, we have a limited understanding of how stimulant drugs alter neural responses to sensory stimuli in healthy humans.
In a recent drug conditioning study in healthy adults, we found that a conditioned stimulus previously paired with methamphetamine (MA) robustly activated brain regions involved in sensory processing (Van Hedger et al. 2018). Healthy volunteers received two pairings of one stimulus (nature scene with sound) with MA (20 mg oral) and another stimulus with placebo (PBO), all outside the scanner. When these stimuli were presented in the fMRI scanner (without drug administration), the stimuli previously paired with drug activated visual and auditory cortices and the insula, suggesting that the stimuli produced a conditioned response of sensory activation. However, we also found that the conditioned response might be influenced by physical features of the stimuli: One of the nature scene images yielded more robust conditioning than the other, perhaps because of differences in visual features. Thus, the present study sought to answer the questions (a) what are the direct (unconditioned) effects of MA on neural responses to sensory stimuli and (b) do these effects depend on physical characteristics of the stimuli?
To address these questions, we examined the direct effects of MA (20 mg) or PBO on brain activity during presentation of visual stimuli. We used six visual stimuli consisting of different nature scenes, including the two that were used in our previous study (Van Hedger et al. 2018). To investigate whether the effects of MA on neural responses to the stimuli depended on their low-level visual features, we presented images that varied on “non-straight edges” (NSE; Berman et al. 2014; Kardan et al. 2015; Kotabe et al. 2016). NSE provides an index of the number of curved or fragmented edges in an image, and is known to influence judgments (Kardan et al. 2015), behavior (Kotabe et al. 2016), and thought content (Schertz et al. 2018). Three high NSE images, including one of our original images, and three low NSE images, including the other image used previously, were used in this study. Thus, we examined the effects of MA on neural activation in response to stimuli that varied in physical features to investigate the interaction between the sensory input and the effects of the drug. We predicted that high NSE images would result in great activation in sensory areas (e.g., visual cortex) than low NSE images, and this effect would be enhanced by MA.
Methods and materials
Participants
Healthy adults (N = 22, 12 women) were recruited via flyers and online advertisements. Participants completed an initial in-person screening that involved a physical examination, electrocardiogram (EKG), psychiatric interview, and nonmedical drug use history (current and lifetime). Inclusion criteria consisted of age between 18 and 35, BMI of 19–26 kg/m2, minimum of high school education, fluency in English, and < 4 caffeinated or alcoholic drinks per day. We excluded individuals with an abnormal EKG, current use of prescription medication (excluding hormonal birth control), current psychiatric disorders (DSM 5; APA 2013) or substance-related disorders except tobacco use disorder within the past year, and contraindications for fMRI scanning (e.g., claustrophobia, copper IUD). All participants were right handed. Of the 22 participants, 4 were excluded for excessive movement during at least one of the two fMRI scans (both scans were excluded if one was of poor quality). The final study sample consisted of 18 participants. The University of Chicago Biological Sciences Division Institutional Review Board approved this study. Table 1 contains study sample demographics and drug use history.
Study design
Participants completed two fMRI scanning sessions. Before each scan, participants received either 20 mg of MA or PBO under double-blind conditions. Drug order was counter balanced across participants. During the scan, participants passively viewed six nature images that varied in physical features (i.e., high or low NSE). They also completed other, unrelated tasks reported elsewhere. We compared image-induced patterns of brain activation between MA and PBO sessions.
Session procedures
Orientation
During an initial orientation session, participants provided informed consent, and viewed and rated images similar to the ones to be used in the test sessions. They were informed that they could receive a placebo, stimulant, or sedative at each session, and were instructed to abstain from alcohol and recreational drug use for 24 and 48 h, respectively, before each session. Participants were also instructed to maintain their normal amount of use for caffeine and tobacco on the days of their sessions with the stipulation that consumption should be discontinued 1 h before their study session began.
fMRI sessions
Participants completed two 4-h study sessions between 9 a.m. and 1 p.m. and separated by at least 48 h. At each session, participants provided breath samples (Alco-SensorIII, Intoximeters, St. Louis, MO) and completed a urine drug screen (ToxCup, Branan Medical Corporation, Irvine, CA) to verify recent abstinence from drugs and alcohol. Women were screened for pregnancy (AimStickPBD, hCG professional, Craig Medical distribution, Vista, CA). Then, participants completed baseline subjective, and cardiovascular measures were obtained. At 9:30 a.m., participants received a dose of MA or PBO (see below) under double-blind conditions. Subjective and cardiovascular measures were collected again 15, 30, 75, 115, and 200 min after drug administration. At 10 a.m., participants were escorted to the MRI research facility where they completed an hour long scan (details below). After the scan, participants were escorted back to the lab where remained until the drug effects wore off. After completing both sessions, the experimenter explained the purpose of the study and which drug they received at each session, and the subjects were paid.
Drug
Oral MA tablets (5 mg, total dose 20 mg; Desoxyn, Lundbeck) were crushed and mixed with 10 ml of combined Ora-Plus and Ora-Sweet syrups (Paddock Laboratories, Minneapolis, MN; for a similar procedure, see Mayo and de Wit 2015). PBO consisted of 10 ml of equal parts Ora-Plus and Ora-Sweet. Syrups were administered in 1 oz. plastic cups.
Drug effect measures
Subjective measures
Subjective effects were assessed using the Drug Effects Questionnaire (DEQ; Johanson and Uhlenhuth 1980; Morean et al. 2013), and the Addiction Research Center Inventory (ARCI; Haertzen 1966). We focused on the morphine-benzedrine group (MBG) and amphetamine (A) subscales, which index euphoria and stimulation, respectively. Measurements were completed before and 15, 30, 75, 115, and 200 min after drug administration. DEQ data were not collected at one timepoint for one participant during an MA session nor at two timepoints for two additional participants during PBO sessions due to computer failure. Similarly, ARCI data were not collected at three timepoints for two participants during MA sessions nor at three timepoints for two additional participants during PBO sessions.
Cardiovascular measures
Heart rate (HR) and blood pressure (BP) were monitored (Omron, Lake Forest, IL) at the same intervals as the subjective measures. Mean arterial pressure (MAP) was calculated using the following formula:
fMRI measures and stimuli
Imaging was done on a Philips Achieva 3.0T scanner using a 32-channel headcoil and a gradient-echo echo-planar imaging sequence with the following acquisition parameters: TR = 2000; TE = 28; 39 3-mm-thick axial slices aligned to the AC-PC line, 0.6-mm slice gap; 19.2 × 19.2 cm FOV; SENSE factor = 2, flip angle = 77°. Four images were acquired and discarded just prior to task start. A high-resolution T1-weighted image (MPRAGE sequence) was also acquired to assess for incidental findings, and for alignment and spatial standardization of the functional data. Subject head motion was minimized with foam packing around the head. Stimuli were viewed via projection onto a mirror mounted on the headcoil.
Nature images
The images used for this study were six nature scenes that varied on low-level visual features. Three of the images were high in NSE (0.085–0.095), and the other three were low in NSE (0.007–0.03). The high NSE images were more visually complex and contained vegetation (e.g., a mountain scene with wildflowers), whereas none of the low NSE images contained vegetation (e.g., sand dunes in a desert). Two of the images were previously used for the task reported in Van Hedger et al. (2018), one in the high NSE category and one low NSE. Among the pictures, there were no systematic differences in preference ratings between high NSE and low NSE images.
During the scan, the six pictures were presented twice for 12 s each, in a random order. Each presentation was followed by a fixation stimulus consisting of a white cross on a dark background. Most fixation periods were 16 s except the third and eighth were 36 s, and the final one was 46 s. Image duration was similar to that used in a previous conditioning study (Van Hedger et al. 2018), and fixation intervals were included to allow activity from the previous image to resolve before presentation of the next image. The two longer fixation blocks served as a contrast condition for the two image types (i.e., each image was compared to fixation, and comparisons were averaged within high NSE and low NSE).
Subject-level functional image processing
Neuroimaging data analysis was conducted with AFNI (Cox 1996). Preprocessing steps included alignment of the time series to the volume with the minimum outlier fraction, spatial registration of the aligned time series data to the anatomical scan, anatomical scan warping to Talairach space and warp applied to functional data, resampled to 3 mm3, smoothed with a 4-mm FWHM Gaussian kernel, and intensity normalization. Volumes exceeding a motion-related displacement of > 3 mm were excluded from analysis. Voxelwise neural activation was then estimated for each subject using a linear regression analysis as implemented in AFNI’s 3dDeconvolve, with the low NSE and high NSE stimuli and long fixation blocks modeled as block functions. De-meaned and derivatives of motion parameters were estimated and included as covariates of no interest. First-level analyses included contrasts of each stimulus type relative to the long fixation blocks. Additional analyses were conducted to verify the assumed insensitivity of the fixation blocks to drug effects. Extractions from any significant findings were planned for use as correlates with behavioral and self-report data.
Statistical analysis
Non-imaging drug effects
We used repeated-measures ANOVA (RM-ANOVA) to examine subjective and cardiovascular effects of MA and PBO. Time (15 min before and 15, 30, 75, 115, and 200 min after drug administration) and drug (MA, PBO) were treated as within-subject factors. To explore relationships between subjective and cardiovascular drug effects (e.g., drug liking, HR) and our neural measures, we calculated peak change scores from baseline after MA and PBO and then subtracted the PBO score from the MA score to create a difference score.
Imaging
Whole brain analyses were conducted using AFNI’s 3dmvm, also implementing an ANCOVA (age, sex covariates) and assessing for interactions and main effects of NSE type (high, low) and drug (MA, PBO) on a voxelwise basis. Voxels that were high-probability white matter or CSF were excluded prior to cluster thresholding, using a mask generated from the study subjects’ tissue-segmented anatomical scans. Significant clusters of voxels were identified if they met a p < .05 familywise error correction threshold. This threshold was determined using 3dClustSim, which ran Monte Carlo simulations of randomly generated data of the same resolution as the analyzed data, spatially smoothed with the group average smoothing parameters estimated using a spatial autocorrelation function, and masked with the same white matter and CSF mask as applied to the group analysis. These procedures implement current methods recommended to address high false positive rates in fMRI particularly due to improper assumptions regarding spatial smoothness of the data (Cox et al. 2017; Eklund et al. 2016).
Results
Drug effects
In line with prior studies (e.g., Mayo and de Wit 2015; Van Hedger et al. 2018), MA produced its expected effects on both subjective and cardiovascular measures. The drug increased ratings of “feel drug” (drug × time; F(5, 75) = 5.99, p < .001), “like drug” (drug × time; F(5, 70) = 5.98, p < .001), ARCI A (drug × time; F(5, 65) = 8.77, p < .001), and ARCI MBG (drug × time; F(5, 75) = 7.47, p < .001). It also increased HR (drug × time; F(5, 85) = 13.71, p < .001) and MAP (drug × time; F(5, 85) = 5.84, p < .001).
Imaging
Quality check
The number of excluded volumes did not differ for either the NSE types or the two drug conditions. There was no effect of drug condition on the fixation blocks.
Imaging findings
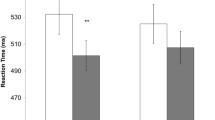
Overall, stimulus-induced activation after MA did not differ from activation after PBO. However, high NSE images yielded greater activation in primary visual cortex than low NSE (Fig. 1, Table 2), and there was a significant interaction between NSE type and drug in three clusters (Table 2). The clusters involved in the interaction did not overlap with the main effect cluster for NSE type. The NSE type and drug interactions were detected in areas of heteromodal association cortex involved in tertiary visual processing: left fusiform (BA 37), right cingulate/precuneus, and posterior right middle temporal gyrus (BA 21/37). Pairwise comparisons of extracted activations indicated that in all three clusters, participants showed greater activation during high NSE images relative to low NSE during the PBO session, but greater activation for low NSE relative to high NSE during the MA session (t values > 2.81, p values < .05; Fig. 2). There was also a significant difference in left fusiform and right cingulate/precuneus showing significantly greater activation during the MA session relative to PBO for low NSE images (t(17) = 2.68, p < .05, and t(17) = 2.17, p < .05, respectively).
Interaction between NSE (high, low) and drug (MA, PBO). Beta weights quantify the fit of the measured BOLD response with the idealized BOLD response model are on the Y-axis for all graphs, and graphs represent change relative to fixation. The areas where there was a significant interaction: left fusiform (a), right cingulate/precuneus (b), and posterior right middle temporal gyrus (c). For all three clusters, there were significant differences between high NSE and low NSE during both sessions; however, during the PBO session, high NSE images produced greater activation, while low NSE images produced greater activation during the MA session. Clusters are thresholded 3 × 3 × 3 mm voxels taken directly from the results map of the analysis. Underlay is an average of all participants’ structural scans. *p < .05; **p < .01; ***p < .001
Relationship between drug effects and imaging
Activations in the three interaction clusters were not correlated with either subjective or cardiovascular effects of the drug (r values = − .30–.41, all p values > .05, uncorrected).
Discussion
The primary findings from this study were that less complex images with fewer curved or fragmented edges (low NSE) produced less activation in visual cortex than more complex images with more curved or fragmented edges (high NSE) and that MA preferentially increased neural responses elicited by the less complex images in three regions of heteromodal association cortex. Overall, high NSE images activated the primary visual cortex to a greater extent than low NSE images, consistent with what might be expected from perceptual theory (Hubel and Wiesel 1962; Vinberg and Grill-Spector 2008). This finding is also consistent with our prior findings where the higher NSE stimulus used in our previous study with MA conditioning resulted in stronger conditioned responses in primary visual cortex. The second finding, that MA preferentially increased neural responses to low NSE images in heteromodal association cortex, provides support for the idea that stimulant drugs facilitate sensory processing (Uftring et al. 2001), with new insights suggesting that stimuli of lower complexity may be more susceptible to the drug effect.
We found significant interactions between stimulus type (low NSE and high NSE) and drug (MA and PBO) in heteromodal, or integrative, cortical regions. While our passive viewing task likely engaged these regions via the higher order physical (spatial or semantic) characteristics of the stimuli, these characteristics are also thought to partly comprise bottom-up attention mechanisms, bridging perception and attention (Arnsten 2009), and in that way, also serve as early signals contributing to salience valuations (Braga et al. 2013). Our data suggest MA increases this higher order processing of less complex sensory input.
The interaction of stimulus type and drug in three higher order visual processing cortical regions provides insight into the nature of the direct effect of MA on processing visual images. As predicted, during the PBO sessions, the more complex high NSE stimuli resulted in stronger activation in primary visual processing regions of the brain. Interestingly, MA increased activation only for the low NSE, or less complex, stimuli, and the drug did not increase activation in any regions when viewing high NSE images. One interpretation of this interaction is that the low NSE stimuli were more susceptible to a drug-related enhanced bottom-up attentional response, whereas high NSE images were less susceptible to such drug-related enhancements due to ceiling effects. Alternatively, stimulant drugs may change the relative sensitivity of higher order sensory processing regions, or otherwise cause changes resulting in greater resource being needed to process the low NSE stimuli.
MA enhanced higher order sensory processing for low NSE images in associative cortex in both temporal and parietal cortices, which have previously been described as the dorsal and ventral streams of attention processing. Dorsal areas, like our finding in the posterior cingulate/precuneus, encode “where” visual input occurs, whereas ventral areas located more in the temporal lobe encode “what” (Ungerleider and Haxby 1994). Our findings suggest that MA affects both of these kinds of higher order visual processing. The posterior cingulate/precuneus cluster is located further downstream in the where path. This region serves a role of integrating the visual spatial information about a stimulus with self-referential and episodic memory information, contributing to calculations of demand for attentional allocation. The top 5 functional (rather than anatomical) terms associated with the peak voxel from this cluster (first converted to MNI space) at Neurosynth.org were “cognitive emotional,” “multisensory,” “visual motion,” “abstract,” and “action observation,” attesting to the complex set of functions subserved by this region.
Both portions of the what stream enhanced by MA were clusters within Brodmann area 37, thought to serve a role integrating visual perceptual information with orthographic and other types of semantic information (Ardila et al. 2015). Specific portions of the what stream are often identified as category specific, such as for faces, words, or place, However, recent work examining downstream specialized categorical processing of visual input suggests that low level visual properties of images within categories drive these seemingly category-specific cortical responses in the what stream (Watson et al. 2014). The top 5 functional terms found at Neurosynth.org for the left temporal cluster were “objects,” “visual,” “faces,” “photographs,” and “encoding,” and for the right cluster, terms were “object,” “visual,” “characters,” “visual word,” and “multisensory.”
A primary neurochemical effect of stimulant drugs is increased dopamine availability, which is thought to account for several different aspects of the drugs’ “rewarding” properties (Schultz 2002; Volkow et al. 2001). In studies with human volunteers, drug reward typically refers to feelings of well-being that may reflect “tonic” increases in dopamine levels (Volkow et al. 1999). In preclinical studies and some clinical studies (Volkow et al. 2004), it has been proposed that dopamine enhances the brain reward signal that accompanies unexpected rewards or signals for upcoming rewards. Thus, in addition to these reward-related effects of MA, our study further shows that an integrative sensory-attentional enhancement can occur and is independent of the subjective drug experience. Increasing sensory salience of particular types of stimuli in the absence of increased positive drug effects is a key aspect of certain models of drug conditioning (Berridge and Robinson 2016).
The present results should be considered in light of several limitations. First, this study only examined a single dose of MA, and as such cannot describe whether the interaction we observed between stimulus type and drug is dose-dependent. Future studies using similar paradigms should include multiple drug doses to address this issue. Second, this study tested a sufficient, given the within-subject design, but modestly sized sample. Lastly, participants in the study were selected from a population of healthy control subjects with limited prior experience with stimulant drugs. It is possible that the effects of MA on higher order sensory processing of novel stimuli observed in this study would differ from effects experienced by individuals who use the drug regularly and/or suffer from stimulant use disorder. However, a recent fMRI study by Courtney et al. (2016) of MA-addicted individuals viewing MA-associated cues reported that the areas of the greatest cue-induced activation were the primary and higher order visual cortex.
Taken together with our prior conditioning study, these results suggest that MA may alter neural response to visual stimuli in addition to its other well-known effects on cognitive and attentional processes. This research highlights the need for a better understanding of the sensory processing effects that MA might have in chronic users, and the trajectory of the development of these effects. Our results indicate that acute MA exposure does have effects on higher order sensory processing, but it is still unknown whether these effects contribute separately or interact with alterations to the reward system over time in the development of stimulant use disorder.
References
Anderson BA, Kuwabara H, Wong DF, Gean EG, Rahmim A, Brašić JR, George N, Frolov B, Courtney SM, Yantis S (2016) The role of dopamine in value-based attentional orienting. Curr Biol 26(4):550–555. https://doi.org/10.1016/j.cub.2015.12.062
APA (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Publishing, Washington, DC
Ardila A, Bernal B, Rosselli M (2015) Language and visual perception associations: meta-analytic connectivity modeling of Brodmann area 37. Behav Neurol 2015:1–14. https://doi.org/10.1155/2015/565871
Arnsten AFT (2009) Toward a new understanding of attention-deficit hyperactivity disorder pathophysiology. CNS Drugs 23(Supplement 1):33–41. https://doi.org/10.2165/00023210-200923000-00005
Berman MG, Hout MC, Kardan O, Hunter MR, Yourganov G, Henderson JM, Hanayik T, Karimi H, Jonides J (2014) The perception of naturalness correlates with low-level visual features of environmental scenes. PLoS One 9(12):e114572. https://doi.org/10.1371/journal.pone.0114572
Berridge KC, Robinson TE (2016) Liking, wanting, and the incentive-sensitization theory of addiction. Am Psychol 71(8):670–679. https://doi.org/10.1037/amp0000059
Berridge CW, Waterhouse BD (2003) The locus coeruleus-noradrenergic system: modulation of behavioral state and state-dependent cognitive processes. Brain Res Rev 42(1):33–84
Braga RM, Sharp DJ, Leeson C, Wise RJS, Leech R (2013) Echoes of the brain within default mode, association, and heteromodal cortices. J Neurosci 33(35):14031–14039. https://doi.org/10.1523/JNEUROSCI.0570-13.2013
Briars L, Todd T (2016) A review of pharmacological management of attention-deficit/hyperactivity disorder. J Pediatr Pharmacol Ther 21(3):192–206. https://doi.org/10.5863/1551-6776-21.3.192
Courtney KE, Ghahremani DG, Ray LA (2016) The effects of pharmacological opioid blockade on neural measures of drug cue-reactivity in humans. Neuropsychopharmacology 41(12):2872–2881. https://doi.org/10.1038/npp.2016.99
Cox RW (1996) AFNI: software for analysis and visualization of functional magnetic resonance neuroimages. Comput Biomed Res 29(3):162–173
Cox RW, Chen G, Glen DR, Reynolds RC, Taylor PA (2017) fMRI clustering and false-positive rates. Proc Natl Acad Sci U S A 114(17):E3370–E3371. https://doi.org/10.1073/pnas.1614961114
de Wit H, Crean J, Richards JB (2000) Effects of d-amphetamine and ethanol on a measure of behavioral inhibition in humans. Behav Neurosci 114(4):830–837
Eagle DM, Tufft MRA, Goodchild HL, Robbins TW (2007) Differential effects of modafinil and methylphenidate on stop-signal reaction time task performance in the rat, and interactions with the dopamine receptor antagonist cis-flupenthixol. Psychopharmacology 192(2):193–206. https://doi.org/10.1007/s00213-007-0701-7
Eklund A, Nichols TE, Knutsson H (2016) Cluster failure: why fMRI inferences for spatial extent have inflated false-positive rates. Proc Natl Acad Sci U S A 113(28):7900–7905. https://doi.org/10.1073/pnas.1602413113
Haertzen CA (1966) Development of scales based on patterns of drug effects, using the addiction research center inventory (ARCI). Psychol Rep 18(1):163–194. https://doi.org/10.2466/pr0.1966.18.1.163
Hubel DH, Wiesel TN (1962) Receptive fields, binocular interaction and functional architecture in the cat’s visual cortex. J Physiol 160:106–154
Ikeda Y, Funayama T, Tateno A, Fukayama H, Okubo Y, Suzuki H (2017) Modafinil enhances alerting-related brain activity in attention networks. Psychopharmacology 234(14):2077–2089. https://doi.org/10.1007/s00213-017-4614-9
Johanson CE, Uhlenhuth EH (1980) Drug preference and mood in humans: diazepam. Psychopharmacology 71(3):269–273. https://doi.org/10.1007/BF00433061
Jonkman LM, Kemner C, Verbaten MN, Koelega HS, Camfferman G, vd Gaag R J, …, van Engeland H (1997) Effects of methylphenidate on event-related potentials and performance of attention-deficit hyperactivity disorder children in auditory and visual selective attention tasks. Biol Psychiatry, 41(6):690–702
Kardan O, Demiralp E, Hout MC, Hunter MR, Karimi H, Hanayik T, Yourganov G, Jonides J, Berman MG (2015) Is the preference of natural versus man-made scenes driven by bottom–up processing of the visual features of nature? Front Psychol 6(471). https://doi.org/10.3389/fpsyg.2015.00471
King M, Rauch LHG, Brooks SJ, Stein DJ, Lutz K (2017) Methylphenidate enhances grip force and alters brain connectivity. Med Sci Sports Exerc 49(7):1443–1451. https://doi.org/10.1249/MSS.0000000000001252
Kotabe HP, Kardan O, Berman MG (2016) The order of disorder: deconstructing visual disorder and its effect on rule-breaking. J Exp Psychol Gen 145(12):1713–1727. https://doi.org/10.1037/xge0000240
Mayo LM, de Wit H (2015) Acquisition of responses to a methamphetamine-associated cue in healthy humans: self-report, behavioral, and psychophysiological measures. Neuropsychopharmacology 40(7):1734–1741. https://doi.org/10.1038/npp.2015.21
Morean ME, de Wit H, King AC, Sofuoglu M, Rueger SY, O’Malley SS (2013) The drug effects questionnaire: psychometric support across three drug types. Psychopharmacology 227(1):177–192. https://doi.org/10.1007/s00213-012-2954-z
Navarra R, Waterhouse B (2016) “What have we GANEd” a theoretical construct to explain experimental evidence for noradrenergic regulation of sensory signal processing. Behav Brain Sci 39:e219. https://doi.org/10.1017/S0140525X15001909
Navarra RL, Clark BD, Gargiulo AT, Waterhouse BD (2017) Methylphenidate enhances early-stage sensory processing and rodent performance of a visual signal detection task. Neuropsychopharmacology 42(6):1326–1337. https://doi.org/10.1038/npp.2016.267
Rosenberg MD, Zhang S, Hsu W-T, Scheinost D, Finn ES, Shen X, Constable RT, Li CSR, Chun MM (2016) Methylphenidate modulates functional network connectivity to enhance attention. J Neurosci 36(37):9547–9557. https://doi.org/10.1523/JNEUROSCI.1746-16.2016
Schertz KE, Sachdeva S, Kardan O, Kotabe HP, Wolf KL, Berman MG (2018) A thought in the park: the influence of naturalness and low-level visual features on expressed thoughts. Cognition 174:82–93. https://doi.org/10.1016/j.cognition.2018.01.011
Schmidt A, Müller F, Dolder PC, Schmid Y, Zanchi D, Liechti ME, Borgwardt S (2017) Comparative effects of methylphenidate, modafinil, and MDMA on response inhibition neural networks in healthy subjects. Int J Neuropsychopharmacol 20(9):712–720. https://doi.org/10.1093/ijnp/pyx037
Schultz W (2002) Getting formal with dopamine and reward. Neuron 36(2):241–263. https://doi.org/10.1016/S0896-6273(02)00967-4
Schultz W, Tremblay L, Hollerman JR (2000) Reward processing in primate orbitofrontal cortex and basal ganglia. Cereb Cortex 10(3):272–284
Uftring S, Wachtel SR, Chu D, McCandless C, Levin DN, de Wit H (2001) An fMRI study of the effect of amphetamine on brain activity. Neuropsychopharmacology 25(6):925–935. https://doi.org/10.1016/S0893-133X(01)00311-6
Ungerleider LG, Haxby JV (1994) What’ and ‘where’ in the human brain. Curr Opin Neurobiol 4(2):157–165. https://doi.org/10.1016/0959-4388(94)90066-3
Van Hedger K, Keedy SK, Mayo LM, Heilig M, de Wit H (2018) Neural responses to cues paired with methamphetamine in healthy volunteers. Neuropsychopharmacology 43(8):1732–1737. https://doi.org/10.1038/s41386-017-0005-5
Vinberg J, Grill-Spector K (2008) Representation of shapes, edges, and surfaces across multiple cues in the human visual cortex. J Neurophysiol 99:1380–1393. https://doi.org/10.1152/jn.01223.2007
Volkow ND, Morales M (2015) The brain on drugs: from reward to addiction. Cell 162(4):712–725. https://doi.org/10.1016/j.cell.2015.07.046
Volkow ND, Wang GJ, Fowler JS, Logan J, Gatley SJ, Wong C, Hitzemann R, Pappas NR (1999) Reinforcing effects of psychostimulants in humans are associated with increases in brain dopamine and occupancy of D(2) receptors. J Pharmacol Exp Ther 291(1):409–415
Volkow ND, Wang G, Fowler JS, Logan J, Gerasimov M, Maynard L et al (2001) Therapeutic doses of oral methylphenidate significantly increase extracellular dopamine in the human brain. J Neurosci 21(2):RC121
Volkow ND, Wang G-J, Fowler JS, Telang F, Maynard L, Logan J, Gatley SJ, Pappas N, Wong C, Vaska P, Zhu W, Swanson JM (2004) Evidence that methylphenidate enhances the saliency of a mathematical task by increasing dopamine in the human brain. Am J Psychiatr 161(7):1173–1180. https://doi.org/10.1176/appi.ajp.161.7.1173
Watson DM, Hartley T, Andrews TJ (2014) Patterns of response to visual scenes are linked to the low-level properties of the image. NeuroImage 99:402–410. https://doi.org/10.1016/j.neuroimage.2014.05.045
Funding
This research is financially supported by National Institute on Drug Abuse Grant R01 DA037011 (HdW), and benefitted from S10OD018448 awarded to the University of Chicago MRI Research Center. KVH was supported by National Institute of Mental Health training grant T32MH020065. MGB was partially supported by a National Science Foundation Grant (NSF-BCS-1632445), and KES was partially supported by a NSF Graduate Research Fellowship. The funding agencies had no involvement in the research other than financial support.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Van Hedger, K., Keedy, S.K., Schertz, K.E. et al. Effects of methamphetamine on neural responses to visual stimuli. Psychopharmacology 236, 1741–1748 (2019). https://doi.org/10.1007/s00213-018-5156-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-018-5156-5