Abstract
Cumulative evidence has established that macrophages orchestrate inflammatory responses that crucially contribute to the pathogenesis of insulin-resistant obesity and type 2 diabetes. In the present study, we examined the impact of hyperglycemia on macrophage pro-inflammatory responses under an inflammatory stimulus. To conduct this study, RAW264.7 macrophages were cultured under normal- (5.5 mM) or high-glucose (22 or 40 mM) conditions for 7 days and stimulated with lipopolysaccharide (LPS). Long-term exposure to high glucose significantly enhanced the increase in the production of pro-inflammatory cytokines, including tumor necrosis-α, interleukin (IL)-1β, and IL-6, when macrophages were stimulated with LPS. The LPS-induced increases in inducible nitric oxide (NO) synthase (iNOS) expression and NO production were also significantly enhanced by long-term exposure of macrophages to high glucose. Treatment with N-acetyl-l-cysteine, a widely used thiol-containing antioxidant, blunted the enhancement of the LPS-induced upregulation of pro-inflammatory cytokine production, iNOS expression, and NO production in macrophages. When intracellular reactive oxygen species (ROS) were visualized using the fluorescence dye 5-(and-6)-chloromethyl-2′,7′-dichlorofluorescein diacetate, acetyl ester, a significant increase in ROS generation was found after stimulation of macrophages with LPS, and this increased ROS generation was exacerbated under long-term high-glucose conditions. LPS-induced translocation of phosphorylated nuclear factor-κB (NF-κB), a transcription factor regulating many pro-inflammatory genes, into the nucleus was promoted under long-term high-glucose conditions. Altogether, the present results indicate that a long-term high-glucose environment can enhance activation of NF-κB in LPS-stimulated macrophages possibly due to excessive ROS production, thereby leading to increased macrophage pro-inflammatory responses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Macrophages are immune cells that are found virtually in every tissue of the body and play a pivotal role in host defense and homeostasis (Mosser and Edwards 2008; Ohashi et al. 2015; Thapa and Lee 2019). Macrophages display phenotypic plasticity and diversity under the influence of the surrounding microenvironment of macrophages (Shapouri-Moghaddam et al. 2018), meaning that, depending on external stimuli, they can transform into a pro-inflammatory phenotype, known as M1 macrophages, or an anti-inflammatory phenotype associated with tissue repair, known as M2 macrophages (Murray et al. 2014). Lipopolysaccharide (LPS), an outer membrane component of Gram-negative bacteria, is widely recognized as a potent macrophage activator that generates abundant inflammatory effects through Toll-like receptor-4 (TLR4). Thus, pro-inflammatory macrophages are potently activated by LPS, leading to the production of a vast number of inflammatory mediators, including oxygen and nitrogen intermediators, prostaglandins, and cytokines (MarcCavaillon 2018).
Recent evidence has revealed that hyperglycemic conditions appear to activate monocytes, precursors of tissue macrophages, which further contributes to an increase in an M1 macrophage phenotype expression, even if neither tissue damage nor infection is present (Barry et al. 2016; Torres-Castro et al. 2016), suggesting that excess high glucose may be associated with an M1/M2 imbalance. Furthermore, it has been shown that mRNA levels of tumor necrosis-α (TNF-α), interleukin (IL)-1β, IL-6, and IL-12 in murine peritoneal macrophages are increased when being exposed to high glucose (Pan et al. 2012). A significant increase in TNF-α in response to elevated glucose levels has also been observed in the mouse macrophage cell line RAW264.7 (Cheng et al. 2015). In streptozotocin-induced diabetic mice, hyperglycemia has been demonstrated to induce broad infiltration of macrophages, leading to a systemic pro-inflammatory state that, upon inflammatory challenge, can trigger a hyperinflammatory reaction and increase pro-inflammatory cytokines/chemokines (Niu et al. 2016). In line with this, high glucose–induced exacerbation of the production of pro-inflammatory cytokines, such as TNF-α and IL-6, after stimulation with LPS has been reported by an in vitro study on human THP-1 macrophages (Grosick et al. 2018). However, what is a key mechanism by which macrophages exhibit hyperproduction of pro-inflammatory cytokines in a hyperglycemic environment is poorly understood.
In this study, we initially ascertained whether pro-inflammatory responses to LPS can be actually enhanced by sustained high-glucose conditions in the environment of the macrophage cell culture. Hyperglycemia leads to excessive production of reactive oxygen species (ROS) in cells, including macrophages, a condition which referred to as oxidative stress (Choi et al. 2008; Rendra et al. 2019; Yaribexgi et al. 2019). Oxidative stress and inflammation have been documented to be linked with most of the diseases in recent times (Dandekar et al. 2015; Siti et al. 2015; Zuo et al. 2019). The goal of this study was thus to assess the role of oxidative stress in the deregulation of LPS-induced pro-inflammatory responses of RAW264.7 macrophage cells in a long-term hyperglycemic environment by using N-acetyl-l-cysteine (NAC), a widely used thiol-containing antioxidant.
Materials and methods
Cell culture
RAW264.7 cells, a mouse macrophage cell line, were cultured according to our previous studies (Wang et al. 2015; Sakamoto et al. 2018). Cells were harvested at 70–80% confluence and seeded into variable size of plates. Then, they were exposed to the experimental condition for 7 days. Specifically, cells were grouped as follows: (1) normal-glucose medium (5.5 mM), (2) high-glucose medium (22 mM), and (3) extremely high-glucose medium (40 mM). Mannitol was used to rule out the effect of osmotic pressure (Abdelzaher et al. 2016). Cells were challenged with 0.1–1000 ng/ml LPS (Escherichia coli 055:B5; List Biological Laboratories, Campbell, CA, USA). When cells were treated with NAC (Nacalai Tesque, Kyoto, Japan), it was added 30 min before LPS stimulation.
RNA extraction and quantitative real-time polymerase chain reaction
Total RNA was isolated from cells with Sepasol®-RNA I Super G (Nacalai Tesque). ReverTra Ace qPCR RT Master Mix (Toyobo, Osaka, Japan) was used for the reverse transcription reaction, and real-time polymerase chain reaction (PCR) analyses were performed using SYBR Premix Ex Taq (Tli RNase H Plus), ROX plus, (Takara Bio, Ohtsu, Japan), or PowerUp™ SYBR® Green Master Mix (Thermo Fisher Scientific, Rockford, IL, USA), as described in the manufacturers’ instructions. Values were normalized to the housekeeping gene glyceraldehyde-3-phosphate dehydrogenase (GAPDH) according to the manufacturer’s protocol (Mx3000P real-time PCR system; Agilent Technologies Inc., Santa Clara, CA, USA). Additional details are stated by our laboratory (Abdelzaher et al. 2016; Suzuki et al. 2018; Tomita et al. 2020). The PCR primers were designed as follows: forward 5′-GTTCTATGGCCCAGACCCTCAC-3′ and reverse 5′-GGCACCACTAGTTGGTTGTCTTTG-3′ for TNF-α, forward 5′-TCCAGGATGAGGACATGAGCAC-3′ and reverse 5′-GAACGTCACACACCAGCAGGTTA-3′ for IL-1β, forward 5′-CCACTTCACAAGTCGGAGGCTTA-3′ and reverse 5′-GCAAGTGCATCATCGTTGTTCATAC-3′ for IL-6, forward 5′-ATTACCCGCCCGAGAAAGG-3′ and reverse 5′-TCGCAGCAAAGATCCACACAG-3′ for nucleotide-binding domain and leucine-rich repeat protein 3 (NLRP3), forward 5′-CTAGTTTGCTGGGGAAAGAAC-3′ and reverse 5′-CTAAGCACAGTCATTGTGAGCTC-3′ for apoptosis-associated specked-like protein (ASC), forward 5′-GCTTCAATCAGCTCCATCAGC-3′ and reverse 5′-CAGTCAGTCCTGGAAATGTGCC-3′ for caspase-1, and forward 5′-TGTGTCCGTCGTGGATCTGA-3′ and reverse 5′-TTGCTGTTGAAGTCGCAGGAG-3′ for GAPDH. The PCR program consisted of 50 °C for 2 min and 95 °C for 2 min, followed by 40 cycles of 95 °C for 15 s and 60 °C for 60 s for annealing of primers and elongation.
Enzyme immunoassay for IL-6
Levels of IL-6 in culture media were measured by the use of commercially available enzyme-linked immunosorbent assay (ELISA) kit (R&D Systems, Minneapolis, MN, USA) according to the manufacturer’s instructions. The plate was read on a FilterMax F5 microplate reader (Molecular Devices, Sunnyvale, CA, USA). Assays were performed in duplicate.
Western blot analysis
Cells were grown in a 6-well dish, harvested, and lysed in 50 μl of RIPA buffer (25 mM Tris–HCl, 150 mM NaCl, 1% NP-40, 1% sodium deoxycholate, 0.1% SDS, pH 7.4) for the whole cell and extraction buffer (20 mM HEPES [pH 7.9], 0.1 mM EDTA [pH 8.0], 0.2% NP-40, 420 mM NaCl, 1 mM dithiothreitol) for the nuclear fraction containing protease inhibitor cocktail on ice. The lysates were centrifuged at 18,000 × g for 10 min at 4 °C, and the resulting supernatants were collected. The protein concentration in the remaining supernatant was measured using BCA Protein Assay Kit (Nacalai Tesque). Blotting procedure, chemiluminescent detection, and densitometric analysis were performed as described in our previous reports (Wang et al. 2015; Abdelzaher et al. 2016; Suzuki et al. 2018). Samples (50–100 μg of protein) were run on 10% SDS-PAGE and electrotransferred to polyvinylidene difluoride filter membrane. The membrane was blocked for 60 min at room temperature in Odyssey blocking buffer (LI-COR Biosciences, Lincoln, NE, USA) followed by incubation with primary antibody at 4 °C. Primary antibody detection was performed with IRDye®-labeled secondary antibodies. Fluorescent of IRDye was analyzed by Odyssey CLx Infrared Imaging System (LI-COR Biosciences). The following antibodies, which are commercially available, were used: anti-mouse inducible nitric oxide synthase (iNOS) polyclonal antibody (1:1000; Cell Signaling, Danvers, MA, USA), anti-human IκBα (44D4) monoclonal antibody (1:1000; Cell Signaling), anti-phospho-nuclear factor- κB (NF-κB) p65 (Ser536) (93H1) monoclonal antibody (1:1000; Cell Signaling), anti-human nuclear factor erythroid 2–related factor 2 (Nrf2) (A-10) monoclonal antibody (1:200; Santa Cruz Biotechnology, Santa Cruz, CA, USA), anti-human heme oxygenase-1 (HO-1) (F-4) monoclonal antibody (1:200; Santa Cruz Biotechnology), anti-human GAPDH chicken polyclonal antibody (1:1500; EMD Millipore, Billerica, MA, USA) or mouse monoclonal antibody (1:1000; Wako Pure Chemical Industries, Osaka, Japan), and anti-laminB1 rabbit polyclonal antibody (1:1000; Proteintech, Rosemont, IL, USA).
Measurement of NOx production
To assess nitric oxide (NO) production by RAW264.7 cells, the NOx (nitrite and nitrate) content of the medium was measured with NO2/NO3 Assay Kit-FX (Fluorometric) (Dojindo, Kumamoto, Japan), according to the manufacturer’s instructions. For final medium change, we used phenol red-free DMEM (Nacalai Tesque) without fetal bovine serum.
Measurement of ROS production
Intracellular ROS was detected as previously described (Kawakami et al. 2018). RAW264.7 cells were loaded with the fluorescent probe 5-(and-6)-chloromethyl-2′,7′-dichlorofluorescein diacetate, acetyl ester (CM-H2DCFDA; Thermo Fisher Scientific) to a final concentration of 10 μM for 30 min at 37 °C. Cells were harvested by TrypLE and then analyzed on a FACS Accuri (BD Biosciences, Franklin Lakes, NJ, USA).
Statistical analysis
Values are presented as means ± standard error. Student’s t test was used to evaluate the differences between two groups. One-way analysis of variance (ANOVA) followed by Tukey’s test was used to compare the means of more than two independent groups. Data were analyzed by the use of GraphPad Prism® version 6.0 software (San Diego, CA, USA). P < 0.05 was considered statistically significant.
Results
Effect of long-term high-glucose exposure on LPS-induced pro-inflammatory responses in macrophages
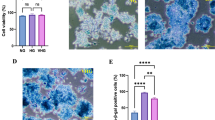
Previous studies have shown that short-term high-glucose exposure (3–48 h) enhances LPS-induced RAW264.7 macrophage activation (Chen et al. 2006; Hua et al. 2012; Hwang et al. 2017; Cantuária et al. 2018). In this study, we investigated the impact of high-glucose exposure over a longer period of time (7 days) on pro-inflammatory cytokine expression in RAW264.7 cells stimulated with LPS. When LPS (30 ng/ml) was applied to RAW264.7 cells for 12 h, the mRNA levels of TNF-α, IL-1β, and IL-6 were greatly upregulated (Fig. 1a). Exposure of RAW264.7 cells to high glucose (22 or 40 mM) for 7 days showed an increase in the mRNA expression levels of TNF-α, IL-1β, and IL-6 regardless of whether LPS was challenged. However, the enhancing effect of long-term high-glucose exposure on the gene levels of pro-inflammatory cytokines was more evident when macrophages were stimulated with LPS. Treatment with NAC, a widely used thiol-containing antioxidant, at a concentration of 10 mM blunted the increase in pro-inflammatory cytokine responses in RAW264.7 cells stimulated with LPS under the high-glucose conditions. When the amounts of IL-6 in culture media were measured by ELISA, long-term high-glucose exposure resulted in a significant enhancement of the elevation in IL-6 protein levels secreted by RAW264.7 cells after 100 ng/ml LPS challenge, and this enhancing effect was negated by treatment with NAC (Fig. 1b).
Effect of long-term high glucose on expression of pro-inflammatory cytokines in LPS-stimulated RAW264.7 cells. Cells were cultured with normal glucose (NG), 22 mM glucose (HG), or 40 mM glucose (EHG) for 7 days. Then, cells were challenged with LPS. NAC (10 mM) was given 30 min before LPS. a–c The mRNA levels of TNFα, IL-1β, and IL-6 were quantified by real-time PCR after stimulation with 30 ng/ml LPS for 3 h. The values were expressed as a fold increase above NG control normalized to GAPDH (n = 3–5). d Cell culture media were collected at 12 h after 100 ng/ml LPS challenge, and then IL-6 was measured by ELISA (n = 4). *P < 0.05, **P < 0.01, and ***P < 0.001. $P < 0.05 vs HG + LPS. &P < 0.05 vs EHG + LPS
In inflammation, NO is produced by iNOS which is induced by bacterial products, such as LPS, and cytokines, and NO acts as a regulatory and pro-inflammatory mediator (Cinelli et al. 2020). Challenge with 100 ng/ml LPS resulted in a significant upregulation of iNOS protein in RAW264.7 cells (Fig. 2a). The increase in iNOS protein expression in LPS-stimulated RAW264.7 cells was significantly augmented by high glucose (22 or 40 mM) for 7 days. Treatment with NAC blunted the augmented response of the LPS-induced iNOS upregulation when RAW264.7 cells were exposed to high glucose. In line with the finding that the increase in iNOS expression after LPS stimulation was enhanced in a high-glucose environment, an increase in NOx after challenge with LPS was significantly enhanced under high-glucose conditions (Fig. 2b). This enhancement of LPS-induced NOx production was less pronounced in the presence of NAC.
Effect of long-term high glucose on iNOS responses in LPS-stimulated RAW264.7 cells. Cells were cultured with normal glucose (NG), 22 mM glucose (HG), or 40 mM glucose (EHG) for 7 days. Then, cells were challenged with LPS. NAC (10 mM) was given 30 min before LPS. a Expression of iNOS protein after stimulation with 100 ng/ml LPS for 18 h (n = 3). GAPDH served as loading control. Typical Western blots are shown in the top trace. GAPDH served as loading control. b NOx levels in the culture medium at 18 h after 100 ng/ml LPS (n = 3–4). *P < 0.05 and **P < 0.01
The NLRP3 inflammasome is a critical intracellular sensor of the innate immune system that plays a vital role in regulating inflammation (Haneklaus et al. 2013). It is composed of the sensor molecule NLRP3 protein, the adaptor protein ASC, and the effector pro-caspase-1 (Jin and Flavell 2010). When RAW264.7 cells were challenged with 30 ng/ml LPS, a marked upregulation of NLRP3 transcript expression was observed (Fig. 3a). Exposure to high glucose (22 or 40 mM) for 7 days did not substantially affect the LPS-induced mRNA expression of NLRP3 in RAW264.7 cells. The expression level of ASC mRNA was also upregulated by LPS stimulation (Fig. 3b). ASC mRNA expression showed an increasing trend when cells were exposed to high glucose in both the presence and absence of LPS, although no significant difference in its expression levels was found between the normal- and high-glucose exposure groups. Caspase-1 mRNA expression levels remained unchanged with LPS challenge and high-glucose exposure (Fig. 3c). Taken together, these results indicate that the impact of a high-glucose environment on the NLRP3/ASC/caspase-1 axis appears to be minimal.
Effect of long-term high glucose on the NLRP3/ASC/caspase-1 axis in LPS-stimulated RAW264.7 cells. Cells were cultured with normal glucose (NG), 22 mM glucose (HG), or 40 mM glucose (EHG) for 7 days. Then, cells were challenged with LPS. The mRNA levels of NLRP3 (a), ASC (b), and caspase-1 (c) were quantified by real-time PCR after stimulation with 30 ng/ml LPS for 3 h. The values were expressed as a fold increase above NG control normalized to GAPDH (n = 3–4)
Effect of long-term high-glucose exposure on LPS-induced ROS generation in macrophages
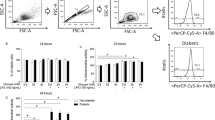
When intracellular ROS in RAW264.7 cells were measured using the fluorescence dye CM-H2DCFDA, exposure to high glucose (22 or 40 mM) for 7 days showed no change in intracellular fluorescence without LPS stimulation (Fig. 4). Application of LPS for 18 h led to a significant increase in intracellular fluorescence at doses ≥ 10 ng/ml. The increases in intracellular fluorescence after stimulation with 10 and 100 ng/ml LPS were significantly enhanced under high-glucose conditions.
Effect of long-term high-glucose exposure on NF- κB activation and the Nrf2/HO-1 axis in macrophages stimulated with LPS
The transcription factor NF- κB is well recognized as a pivotal player in regulating genes involved in immune and inflammatory responses (Li and Verma 2002; Mitchell and Carmody 2018). Since the activity of NF- κB is primarily regulated by interaction with inhibitory I κBα protein, degradation of I κBα in RAW264.7 cells after stimulation with 1 μg/ml LPS was monitored by Western blot (Fig. 5a). LPS challenge led to greatly accelerated degradation of I κBα. A peak decrease in I κBα was observed at 15–30 min after challenge with LPS. In a high-glucose environment, the degradation levels of I κBα were more transient than under normal glucose and returned to the baseline value at 30 min. The liberated NF- κB dimer then translocates into the nucleus where it recognizes and binds to specific DNA sequences termed κB sites, thereby leading to the transcription of target genes (Karin and Ben-Neriah 2000; Sharif et al. 2007). In addition, in the NF- κB signaling cascade, serine phosphorylation of NF- κB p65 is required for nuclear translocation and transcriptional activation (Kwon et al. 2016). When phosphorylated NF- κB p65 in the nuclear fractions was detected by Western blot, LPS resulted in translocation of phosphorylated NF-κB p65 into the nucleus at 30 min under normal glucose (Fig. 5b). On the other hand, nuclear translocation of phosphorylated NF- κB p65 under high-glucose conditions appeared earlier: it was evidently identified at 15 min after LPS stimulation under 22 and 40 mM high glucose.
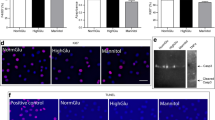
Effect of long-term high glucose on NF-κB activation and the Nrf2/HO-1 axis in LPS-stimulated RAW264.7 cells. Cells were cultured with normal glucose (NG), 22 mM glucose (HG), or 40 mM glucose (EHG) for 7 days. Then, cells were challenged with LPS for 18 h. a IκBα degradation after challenge with 1 μg/ml LPS. Western blot analysis was performed using anti-IκBα monoclonal antibody. GAPDH served as loading control. b NF-κB nuclear translocation after challenge with 1 μg/ml LPS. Nuclear proteins were extracted, and then phosphorylated NF-κB p65 was detected by Western blot. Lamin B served as a nuclear marker. c Expression of Nrf2 in nuclear fractions from cells after stimulation with 1 μg/ml LPS. Lamin B was used as nuclear loading controls. d Expression of HO-1 after 1 μg/ml LPS stimulation. As a loading control, GAPDH was employed. Shown are representative data from two independent experiments in which the same results were obtained
Nrf2 is a potent transcriptional activator that upregulates expression of cytoprotective genes, such as HO-1, to protect the cells against oxidative stress. Thus, the Nrf2/HO-1 axis is one of the antioxidant systems which play a critical role in the maintenance of the redox state for the defense of intracellular oxidative stress (Loboda et al. 2016). When RAW264.7 cells were stimulated with 1 μg/ml LPS for 18 h under normal glucose, the Nrf2 level in the nucleus was greatly decreased (Fig. 5c). In a high-glucose environment, the decrease in nuclear Nrf2 levels after LPS stimulation became less marked. HO-1 levels under normal glucose were also reduced in cells stimulated with LPS (Fig. 5d). The LPS-induced reduction in HO-1 levels was inappreciable under high-glucose conditions. These findings suggest that increased ROS generation in RAW264.7 cells under high glucose is not attributed to an impairment of the Nrf2/HO-1 axis.
Discussion
In this study, we showed that exposure to high glucose for 7 days significantly enhanced the increase in pro-inflammatory cytokine production when RAW264.7 macrophages were stimulated with LPS. We also found that the LPS-induced increases in iNOS expression and NOx production were significantly enhanced by exposure of RAW264.7 macrophages to high glucose for 7 days. Thus, the present study represents that long-term high-glucose exposure can intensify pro-inflammatory responses in macrophages stimulated with LPS. Our results are consistent with previous studies showing the increase in LPS-induced RAW264.7 macrophage activation when exposed to high glucose (Chen et al. 2006; Hua et al. 2012; Hwang et al. 2017; Cantuária et al. 2018), but those studies were conducted under short-term high-glucose conditions (3–48 h). Given that our longer-term incubation with high glucose may place macrophages in an environment that resembles hyperglycemic conditions in diabetic animals and patients, we believe that our system would be a good in vitro model to study the behavior of macrophages in diabetes.
We observed a significant increase in intracellular ROS generation after stimulation of RAW264.7 macrophages with LPS at doses of ≥ 10 ng/ml when intracellular ROS were visualized using the fluorescence dye CM-H2DCFDA. LPS-stimulated macrophages that were cultured under high-glucose conditions exhibited greater amounts of ROS as compared with normal-glucose conditions. Treatment with NAC, a powerful antioxidant, blunted the enhancement of the LPS-induced upregulation of pro-inflammatory cytokine production, iNOS expression, and NOx generation in RAW264.7 macrophages. Our results thus suggest that the high glucose–induced increase in ROS generation may contribute to the enhancing effect of long-term high-glucose exposure on the pro-inflammatory responses in LPS-stimulated macrophages.
The Nrf2/HO-1 signaling axis is a multiple organ protection chain that protects against oxidative stress injury. Nrf2 is a transcription factor that upregulates expression of genes encoding detoxifying and antioxidant enzymes, including HO-1, to protect against cellular oxidative stress (Loboda et al. 2016). In the present study, LPS stimulation resulted in reductions in nucleus translocation of Nrf2 and expression of HO-1 protein in RAW264.7 cells, indicating that LPS downregulates the Nrf2/HO-1 pathway in macrophages. With due consideration of the above, these results imply that LPS stimulates the production of ROS and leads to an imbalance between oxidants and endogenous antioxidants, such as the Nrf2/HO-1 pathway, thereby resulting in the buildup of oxidative stress similar to that seen in previous studies (Thimmulappa et al. 2006; Naeem et al. 2021). The LPS-induced downregulation of the Nrf2/HO-1 axis was found to be dismissed by long-term exposure to high glucose. This may be merely attributable to the result that oxidative stress caused by excessive ROS production activated the endogenous antioxidant defense system in macrophages. Alternatively, we may consider the changes in the Nrf2/HO-1 axis not to contribute to the mechanism(s) underlying the enhancement by long-term high-glucose exposure of LPS-induced increase in ROS production in macrophages.
NF- κB acts as a critical transcriptional activator of iNOS (Xie et al. 1994), and many of pro-inflammatory cytokine genes are regulated by κB sites in the DNA and have putative binding sites for NF- κB at their promoter sites to activate gene expression (Libermann and Baltimore 1990; Trede et al. 1995). After LPS binds to TLR4, which is primarily associated with the accessory protein MD-2 and the co-receptor CD-14 to recognize LPS, activation of downstream kinases results in phosphorylation, ubiquitination, and ultimately proteolytic degradation of I κBα, leading to liberation of NF- κB from degraded I κBα and then translocation of NF- κB to the nucleus where it can cause activation of many pro-inflammatory genes (Karin and Ben-Neriah 2000; Sharif et al. 2007). In this study, long-term high-glucose exposure neither accelerated nor sustained I κBα degradation in LPS-stimulated macrophages. However, we found that LPS-induced nuclear translocation of phosphorylated NF- κB was promoted under long-term high-glucose conditions. In this regard, it may be noted that translocation of phosphorylated NF- κB to the nucleus is occasionally independent of I κBα regulation (Sasaki et al. 2005). Previous studies have proposed that ROS is involved in activation of NF- κB in a wide variety of cell types, although ROS can also have the potential to repress NF-κB activity (Nakajima and Kitamura 2013; Lingappan 2018). Collectively, we interpret our present results to indicate that a long-term high-glucose environment leads to an enhancement of NF- κB activation in LPS-stimulated macrophages possibly due to excessive ROS production, thereby more highly upregulating pro-inflammatory gene expression (Fig. 6).
Schematic diagram of the long-term high-glucose environment–induced enhancement of pro-inflammatory gene expression in macrophages stimulated with LPS. Upon stimulation of TLR4 with LPS, IκBα is phosphorylated by IκB kinase (IKK), ubiquitinated proteolytically, and degraded, freeing NF-κB to the nucleus where it binds to DNA at its cognate regulatory sites and regulates pro-inflammatory gene activity. Long-term high-glucose exposure enhances nuclear translocation of phosphorylated NF-κB due to excess ROS generation. See text for details
The NLRP3 inflammasome is an intracellular sensor consisting of the sensor molecule NLRP3 protein, the adaptor protein ASC, and the effector pro-caspase-1 and has now emerged as a critical regulator in the inflammatory process. NLRP3 initiates the formation of the inflammasome by interacting with ASC, which recruits and activates pro-caspase-1 and then converts the cytokine precursor pro-IL-1β into mature and biologically active IL-1β (Jin and Flavell 2010; Haneklaus et al. 2013). In this study, changes in transcript levels of NLRP3, ASC, and caspase-1 were found to vary in macrophages stimulated with LPS. Moreover, long-term exposure to high glucose failed to substantially upregulate gene expression of these components in LPS-stimulated macrophages. These findings indicate that the NLRP3/ASC/caspase-1 axis is not totally involved in the enhancement of the LPS-induced upregulation of IL-1β expression in macrophages under long-term high-glucose conditions.
The limitation of this study is that RAW264.7 macrophages in our in vitro approach may not accurately reflect their in vivo counterparts in diabetic states. Indeed, isolated and cultivated primary cells could be criticized for being different from the corresponding cell type in an organism. However, it should be noted that in vitro assays allow the research of isolated molecular steps that contribute to macrophage activation. The present study did not examine a possible role of targeting hyperglycemia-induced macrophage activation as the mechanism of drug action. In this regard, metformin, a widely used antidiabetic drug, has been shown to reduce LPS-stimulated pro-inflammatory cytokines in macrophages (Kim et al. 2014), and the anti-inflammatory benefits of metformin from targeting macrophages may contribute, at least in part, to its prevention of diabetic cardiovascular complications beyond glucose lowering (Hattori et al. 2015). Thus, whether metformin can curb the enhancement by long-term high-glucose exposure of LPS-induced pro-inflammatory responses in macrophages may well deserve further study. Given the possible role of ROS in the long-term high glucose–increased pro-inflammatory responses in macrophages stimulated with LPS, anti-inflammatory agents with antioxidant properties may also be worth of careful study.
In conclusion, our in vitro cell-based study demonstrated that long-term high glucose exacerbated the pro-inflammatory responses of macrophages when challenged with LPS. The impact of a long period of high-glucose exposure on LPS-stimulated macrophage pro-inflammatory responses appears to stem from increased activation of NF- κB due to excess ROS generation. It is now becoming clear that low-grade inflammation is associated with the development of obesity-related insulin resistance and type 2 diabetes (Saltiel and Olefsky 2017). Activation of macrophages is considered to contribute to a significant amplification of the inflammatory states via release of a variety of pro-inflammatory cytokines, leading to the impairment of insulin signaling (Greenberg and McDaniel 2002; Fujisaka et al. 2009). People with diabetes are highly susceptible to bacterial infections (Peleg et al. 2007). We indicated that hyperglycemia sensitizes macrophages to LPS stimulation, which may play a potential role in the defects in the insulin-signaling cascade in diabetic patients with infection events. Additional work is needed to further establish the molecular mechanisms through which hyperglycemia is able to promote the production of pro-inflammatory cytokines and chemicals in macrophages, and the development of strategies aiming to limit macrophage activation in a hyperglycemic environment may have a potential value for controlling diabetic complications in conjunction with hyperglycemia-associated macrophage activation.
References
Abdelzaher LA, Imaizumi T, Suzuki T, Tomita K, Takashina M, Hattori Y (2016) Astaxanthin alleviates oxidative stress insults-related derangements in human vascular endothelial cells exposed to glucose fluctuations. Life Sci 150:24–31
Barry JC, Shakibakho S, Durrer C, Simtchouk S, Jawanda KK, Cheung ST, Mui AL, Little JP (2016) Hyporesponsiveness to the anti-inflammatory action of interleukin-10 in type 2 diabetes. Sci Rep 6:21244
Cantuária APC, Figueiredo TM, Freire MS, Lima SMF, Almeida JA, Franco OL, Rezende TMB (2018) The effects of glucose concentrations associated with lipopolysaccharide and interferon-gamma stimulus on mediators’ production of RAW 264.7 cells. Cytokine 107:18–25
Chen YJ, Hsu KW, Chen YL (2006) Acute glucose overload potentiates nitric oxide production in lipopolysaccharide-stimulated macrophages: the role of purinergic receptor activation. Cell Biol Int 30:817–822
Cheng CI, Chen PH, Lin YC, Kao YH (2015) High glucose activates Raw264.7 macrophages through RhoA kinase-mediated signaling pathway. Cell Signal 27:283–292
Choi S-W, Benzie IFF, Ma S-W, Strain JJ, Hannigan BM (2008) Acute hyperglycemia and oxidative stress: direct cause and effect? Free Radic Biol Med 44:1217–1231
Cinelli MA, Do HT, Miley GP, Silverman RB (2020) Inducible nitric oxide synthase: regulation, structure, and inhibition. Med Res Rev 40:158–189
Dandekar A, Mendez R, Zhang K (2015) Crosstalk between ER stress, oxidative stress, and inflammation in health and disease. Methods Mol Biol 1292:205–214
Fujisaka S, Usui I, Bukhari A, Ikutani M, Oya T, Kanatani Y, Tsuneyama K, Nagai Y, Takatsu K, Urakaze M, Kobayashi M, Tobe K (2009) Regulatory mechanisms for adipose tissue M1 and M2 macrophages in diet-induced obese mice. Diabetes 58:2574–2582
Greenberg AS, McDaniel ML (2002) Identifying the links between obesity, insulin resistance and β cell function: potential role of adipocyte-derived cytokines in the pathogenesis of type 2 diabetes. Eur J Clin Invest 32(Suppl 3):24–34
Grosick R, Alvarado-Vazquez PA, Messersmith AR, Romero-Sandoval EA (2018) High glucose induces a priming effect in macrophages and exacerbates the production of pro-inflammatory cytokines after a challenge. J Pain Res 11:1769–1778
Haneklaus M, O’Neill LA, Coll RC (2013) Modulatory mechanisms controlling the NLRP3 inflammasome in inflammation: recent developments. Curr Opin Immunol 25:40–45
Hattori Y, Hattori K, Hayashi T (2015) Pleiotropic benefits of metformin: macrophage targeting its anti-inflammatory mechanisms. Diabetes 64:1907–1909
Hua KF, Wang SH, Dong WC, Lin CY, Ho CL, Wu TH (2012) High glucose increases nitric oxide generation in lipopolysaccharide-activated macrophages by enhancing activity of protein kinase C-α/ δ and NF-κB. Inflamm Res 61:1107–1116
Hwang JS, Kwon MY, Kim KH, Lee Y, Lyoo IK, Kim JE, Oh ES, Han IO (2017) Lipopolysaccharide (LPS)-stimulated iNOS induction is increased by glucosamine under normal glucose conditions but is inhibited by glucosamine under high glucose conditions in macrophage cells. J Biol Chem 292:1724–1736
Jin C, Flavell RA (2010) Molecular mechanism of NLRP3 inflammasome activation. J Clin Immunol 30:628–631
Karin M, Ben-Neriah Y (2000) Phosphorylation meets ubiquitination: the control of NF-κB activity. Annu Rev Immunol 18:621–663
Kawakami M, Hattori M, Ohashi W, Fujimori T, Hattori K, Takebe M, Tomita K, Yokoo H, Matsuda N, Yamazaki M, Hattori Y (2018) Role of G protein-coupled receptor kinase 2 in oxidative stress and nitrosative stress-related neurohistopathological changes in a mouse model of sepsis-associated encephalopathy. J Neurochem 145:474–488
Kim J, Kwak HJ, Cha J-Y, Jeong Y-S, Rhee SD, Kim KR, Cheon HG (2014) Metformin suppresses lipopolysaccharide (LPS)-induced inflammatory response in murine macrophages via activating transcription factor-3 (ATF-3) induction. J Biol Chem 289:23246–23255
Kwon H-J, Choi G-E, Ryu S, Kwon SJ, Kim SC, Booth C, Nichols KE, Kim HS (2016) Stepwise phosphorylation of p65 promotes NF-κB activation and NK cell responses during target cell recognition. Nat Commun 7:11686
Li Q, Verma IM (2002) NF-kappaB regulation in the immune system. Nat Rev Immunol 2:725–734
Libermann TA, Baltimore D (1990) Activation of interleukin-6 gene expression through the NF-κB transcription factor. Mol Cell Biol 10:2327–2334
Lingappan A (2018) NF-κB in oxidative stress. Curr Opin Toxicol 7:81–86
Loboda A, Damulewicz M, Pyza E, Jozkowicz A, Dulak J (2016) Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: an evolutionarily conserved mechanism. Cell Mol Life Sci 73:3221–3247
MarcCavaillon J (2018) Exotoxins and endotoxins: inducers of inflammatory cytokines. Toxicon 149:45–53
Mitchell JP, Carmody RJ (2018) NF-κB and the transcriptional control of inflammation. Int Rev Cell Mol Biol 335:41–84
Mosser DM, Edwards JP (2008) Exploring the full spectrum of macrophage activation. Nat Rev Immunol 8:858–869
Murray PJ, Allen JE, Biswas SK, Fisher EA, Gilroy DW, Goerdt S, Gordon S, Hamilton DM, Ivashkiv LB, Lawrence T, Locati M, Mantovani A, Martinez FO, Mege JL, Mosser DM, Natoli G, Saeij JP, Schultze JL, Shirey KA, Sica A, Suttles J, Udalova I, van Ginderachter JA, Vogel SN, Wynn TA (2014) Macrophage activation and polarization: nomenclature and experimental guidelines. Immunity 41:14–20
Naeem K, Kury L, Nasar F, Alattar A, Alshaman R, Shah FA, Khan A-U, Li S (2021) Natural dietary supplement, carvacrol, alleviates LPS-induced oxidative stress, neurodegeneration, and depressive-like behaviors via the Nrf2/HO-1 pathway. J Inflamm Res 14:1313–1329
Nakajima S, Kitamura M (2013) Bidirectional regulation of NF-κB by reactive oxygen species : a role of unfolded protein response. Free Radic Biol Med 65:162–174
Niu S, Bian Z, Tremblay A, Luo Y, Kidder K, Mansour A, Zen K, Liu Y (2016) Broad infiltration of macrophages leads to a proinflammatory sate in streptozotocin-induced hyperglycemic mice. J Immunol 197:3293–3301
Ohashi W, Hattori K, Hattori Y (2015) Control of macrophage dynamics as a potential therapeutic approach for clinical disorders involving chronic inflammation. J Pharmacol Exp Ther 354:240–250
Pan Y, Wang Y, Cai L, Cai Y, Hu J, Yu C, Li J, Feng Z, Yang S, Li X, Liang G (2012) Inhibition of high glucose-induced inflammatory response and macrophage infiltration by a novel curcumin derivative prevents renal injury in diabetic rats. Br J Pharmacol 166:1169–1182
Peleg AY, Weerarathna T, McCarthy JS, Davis TM (2007) Common infections in diabetes: pathogenesis, management and relationship to glycaemic control. Diabetes Metab Res Rev 23:3–13
Rendra E, Riabov V, Mossel DM, Sevastyanova T, Harmsen MC, Kzhyshkowska J (2019) Reactive oxygen species (ROS) in macrophage activation and function in diabetes. Immunobiology 224:242–253
Sakamoto T, Ohashi W, Tomita K, Hattori K, Matsuda N (2018) Anti-inflammatory properties of cilostazil: its interruption of DNA binding activity of NF-κB from the Toll-like receptor signaling pathways. Int Immunopharmacol 62:120–131
Saltiel AS, Olefsky JM (2017) Inflammatory mechanisms linking obesity and metabolic disease. J Clin Invest 127:1–4
Sasaki CY, Barberi TJ, Ghosh P, Longo DL (2005) Phosphorylation of RelA/p65 on serine 536 defines an IκBα-independent NF-κB pathway. J Biol Chem 280:34538–34547
Shapouri-Moghaddam A, Mohammadian S, Vazini H, Taghadosi M, Esmaeili S-A, Mardani F, Seifi B, Mohammadi A, Afshari JT, Sahebkar A (2018) Macrophage plasticity, polarization, and function in health and disease. J Cell Physiol 233:6425–6440
Sharif O, Bolshakov VN, Raines S, Newham P, Perkins ND (2007) Transcriptional profiling of the LPS induced NF-κB response in macrophages. BMC Immunol 8:1
Siti HW, Kamisah Y, Kamsiah J (2015) The role of oxidative stress, antioxidants, and vascular inflammation in cardiovascular disease (a review). Vascul Pharmacol 71:40–56
Suzuki T, Sakata K, Mizuno N, Palikhe S, Yamashita S, Hattori K, Matsuda N, Hattori Y (2018) Different involvement of the MAPK family in inflammatory regulation in human pulmonary microvascular endothelial cells stimulated with LPS and IFN-γ. Immunobiology 223:777–785
Thapa B, Lee K (2019) Metabolic influence on macrophage polarization and pathogenesis. BMB Rep 52:360–372
Thimmulappa RK, Scollick C, Traore K, Yates M, Trush MA, Liby KT, Sporn MB, Yamamoto M, Kensler TW, Biswal S (2006) Nrf2-dependent protection from LPS induced inflammatory response and mortality by CDDO-Imidazolide. Biochem Biophys Res Commun 351:883–889
Tomita K, Saito Y, Suzuki T, Imbaby S, Hattori K, Matsuda N, Hattori Y (2020) Vascular endothelial growth factor contributes to lung vascular hyperpermeability in sepsis-associated acute lung injury. Naunyn-Schmiedeberg’s Arch Pharmacol 393:2365–2374
Torres-Castro I, Arroyo-Camarena ÚD, Martínez-Reyes CP, Gómez-Arauz AY, Dueñas-Andrade Y, Hernández-Ruiz J, Béjar YL, Zaga-Clavellina V, Morales-Montor J, Terrazas LI, Kzhyshkowska J, Escobedo G (2016) Human monocytes and macrophages undergo M1-type inflammatory polarization in response to high levels of glucose. Immuno Lett 176:81–89
Trede NS, Tsytsykova AV, Chatila T, Goldfield AE, Geha RS (1995) Transcriptional activation of the human TNF-a promoter by superantigen in human monocytic cells: role of NF-κB. J Immunol 155:902–908
Wang Q, Yokoo H, Takashina M, Sakata K, Ohashi W, Abedelzaher LA, Imaizumi T, Sakamoto T, Hattori K, Matsuda N, Hattori Y (2015) Anti-inflammatory profile of levosimendan in cecal ligation-induced septic mice and in lipopolysaccharide-stimulated macrophages. Crit Care Med 43:e508–e520
Xie Q, Kashiwabara Y, Nathan C (1994) Role of transcription factor NF-κB/Rel in induction of nitric oxide. J Biol Chem 269:4705–4708
Yaribexgi H, Atkin SL, Sahebkar A (2019) A review of the molecular mechanisms of hyperglycemia-induced free radical generation leading to oxidative stress. J Cell Physiol 234:1300–1312
Zuo L, Prather ER, Stetskiv M, Garrison DE, Meode JR, Peace TI, Zhout T (2019) Inflammaging and oxidative stress in human diseases: from molecular mechanisms to novel treatments. Int J Mol Sci 20:4472
Acknowledgements
We wish to thank Prof. Naoki Yoshimura for giving Shigeyuki Yamashita the opportunity to work at the Department of Molecular and Medical Pharmacology, University of Toyama.
Funding
This study was supported by Grant-in-Aid for Scientific Research (16K19015, 17K08586, 19H03757) and for Young Scientists (20K17776) from the Japan Society for Promotion of Science.
Author information
Authors and Affiliations
Contributions
T.S., N.M., and Y.H. conceived and designed the experiments. T.S. and S.Y. performed the experiments and analyzed data. T.S., K.H., and Y.H. wrote the article. All authors read and approved the manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Suzuki, T., Yamashita, S., Hattori, K. et al. Impact of a long-term high-glucose environment on pro-inflammatory responses in macrophages stimulated with lipopolysaccharide. Naunyn-Schmiedeberg's Arch Pharmacol 394, 2129–2139 (2021). https://doi.org/10.1007/s00210-021-02137-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-021-02137-8