Abstract
Hemorrhagic cystitis (HC) is the major dose-limiting adverse effect of the clinical use ifosfamide (IFOS). The incidence of this side effect can be as high as 75%. Mesna has been used to reduce the risk of HC, although 5% of patients who get IFOS treatment may still suffer from HC. In previous studies, our group demonstrated that α-phellandrene (α-PHE) possesses anti-inflammatory activity, which opens the door for its study in the attenuation of HC. The objective of this study was to investigate the potential uroprotective effect of the α-PHE in the mouse model of IFOS-induced HC. In order to analyze the reduction of the urothelial damage, the bladder wet weight, hemoglobin content, and the Evans blue dye extravasation from the bladder matrix were evaluated. To investigate the involvement of neutrophil migration and lipid peroxidation and involvement of enzymatic and endogenous non-enzymatic antioxidants, the tissue markers myeloperoxidase (MPO), malondialdehyde, nitrite/nitrate (NOx), superoxide dismutase (SOD), and reduced glutathione (GSH) were evaluated. TNF-α and IL-1β were measured by ELISA immunoassay technique. The results show that pretreatment with α-PHE significantly reduced urothelial damage that was accompanied by a decrease in the activity of MPO, MDA, and NOx levels and prevention of the depletion of SOD and GSH in bladder tissues. In the assessment of cytokines, α-PHE was able to significantly reduce TNF-α level. However, it does not affect the activities of IL-1β. These data confirm that α-PHE exerts potent anti-inflammatory properties and demonstrates that α-PHE represents a promising therapeutic option for this pathological condition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cyclophosphamide (CP) and ifosfamide (IFO) (oxazaphosphorines) are among the most widely used cytotoxic drugs worldwide and are active against many types of benign and malignant neoplastic diseases (Matz and Hsieh 2017). In addition, they are also used at lower doses to treat rheumatic diseases (Yilmaz et al. 2015). Its use is based on its action as a chelator of DNA which renders cells unfeasible for cell division (Altayli et al. 2012). IFO shares with CP a toxic profile characterized by urotoxicity due to the metabolism of these drugs and it involves the formation of toxic metabolite (acrolein), which in turn has a high potential for tissue aggression when it accumulates in the bladder because it induces bladder inflammatory damage, thus constituting hemorrhagic cystitis (HC) (Decker et al. 2009).
Oxazaphosphorine-induced bladder inflammation is mediated by a variety of soluble factors, including reactive oxygen species (ROS), reactive nitrogen species (RNS), and inflammatory cytokines (IL-1β and TNF) which are widely associated with epithelial damage in the bladder tissue (Macedo et al. 2012). It is worth noting that HC occurs in up to 70% of patients exposed to high doses of chemotherapy with CP or IFO (Cannon et al. 1991). HC can cause bladder constriction or perforation, anemia, recurrent urinary tract infections, hydronephrosis, and renal failure, leading to death (Sencer et al. 1993). In addition, HC is the main dose-limiting adverse effect of oxazaphosphorines and its development compromises the continuity of cancer treatment and despite the available treatments, there is a prevalence of this disease in up to 40% of oxazaphosphorine-treated patients (Silva Junior et al. 2013).
Among the chemoprotective agents used as coadjuvants in chemotherapy treatment with cyclophosphamide, Mesna (2-mercaptoethanesulfonate) is the most widely used drug as a protector against the development of hemorrhagic cystitis (Matz and Hsieh 2017). Mesna has the ability to bind to the acrolein molecule and thus prevents its entry into the bladder cells thus preventing oxidative stress, inflammation, and necrosis from installing in these cells (Haselberger and Schwinghammer 1995; Haldar 2014). However, about 5% of patients treated with cyclophosphamide and submitted to Mesna treatment still develop hemorrhagic cystitis. This is due to the presence of other substances that do not bind to Mesna and that have the capacity to induce HC (Altayli et al. 2012). Indeed, ifosfamide also undergoes considerable chloroethyl side chain oxidation with liberation of chloroacetaldehyde (CAA). CAA may also contribute to the urotoxicity of ifosfamide, not just acrolein (Mills et al. 2019).
In this sense, several other groups of drugs have been tested in particular, anti-inflammatory drugs (Szabo et al. 2007) and antioxidants (Vieira et al. 2004; Ozcan et al. 2005; Arafa 2009; Boeira et al. 2011).
Within this scope, several substances of natural origin (ternatine, curcumin, quercetin, rutin, and gallic acid) were tested in experimental models of cyclophosphamide/ifosfamide-induced hemorrhagic cystitis (Vieira et al. 2004; Boeira et al. 2011). In our previous studies, our group demonstrated that monoterpene α-phellandrene has anti-inflammatory and antioxidant activity (Siqueira et al. 2016a), which opens the door to investigate its potential therapeutic effect on hemorrhagic cystitis.
In the present study, it was found that the α-phellandrene (2-methyl-5-propane-2-cyclohexane-1,3-diene) had important pharmacological effects, such as antinociceptive effect and antidematogenic activity (Lima et al. 2011; Siqueira et al. 2016b). The anti-inflammatory effect exerted by this monoterpene probably still involves a decrease in neutrophil migration and stabilization of mast cell degranulation (Siqueira et al. 2016a), which indicates that α-phellandrene is potentially useful in the investigation of new agents with anti-inflammatory activity. In this context, we hypothesized that α-phellandrene might prevent (H1) experimentally ifosfamide-induced hemorrhagic cystitis in mice through suppression of inflammation and oxidative stress, which paves the way for its application in the study of attenuation of inflammatory bladder damage caused by oxazaphosphorine chemotherapy in acute evaluation.
Material and methods
Animals
Non-fasted Mus musculus mice of Swiss albino lineage, males, weighing between 25 and 30 g were used. The animals were obtained from the bioterium of the Medicinal Plants Research center (NPPM) of the Federal University of Piauí. The animals were kept at 22 ± 2 °C and light/dark cycle of 12 h with water and food ad libitum. The experimental and euthanasia procedures were performed according to the ethical guidelines of animal experimentation and were approved by the Committee of Ethics in Animal Experimentation of the Federal University of Piauí through protocol No. 279/16 (CEUA-UFPI).
Drugs
The following drugs were used in this study: α-phellandrene (Sigma), ifosfamide (Holoxane – ASTA – AG – Frankfurt. Alemanha), Mesna (Mitexan®) (Baxter), Tween 80 (Riedel, Alemanha), sodium chloride (LabSynth, Brazil), o-dianisidine (Sigma), sodium thiopental (Abbots Lab, Brasil), lidocaine (Sigma), hexadecyltrimethylammonium bromide (Sigma), hydrogen peroxide (Quimesp Química), potassium chloride (LabSynth, Brazil), phosphoric acid (Sigma), thiobarbituric acid (Sigma), n-butanol, 5,5′-Dithiobis(2-nitrobenzoic acid) (DTNB) (Sigma).
Hemorrhagic cystitis induced by ifosfamide
The mice were distributed in 8 (eight) groups of 5 (five) animals each. Dosage and route of administration of IFOS were determined from that described in the literature (Ribeiro et al. 2002; Mota et al. 2007). The control group received pretreatment with vehicle (Tween in saline solution at 0.05%, 0.5 mL/10 g of animal weight, i.p.), the negative control (−) received only ifosfamide (400 mg/kg, i.p.), the Mesna group received two intraperitoneal doses of Mesna 80 mg/kg each, totaling 160 mg/kg, 30 min before and 6 h after the administration of ifosfamide. The groups treated with α-phellandrene received 6.25, 12.5, 25, 50, and 100 mg/kg (Polysorbate 80 0.05% + NaCl 0.9%, i.p.) 30 min before the administration of ifosfamide. For induction of hemorrhagic cystitis, the animals received intraperitoneal injection of ifosfamide at a dose of 400 mg/kg 30 min after pretreatment according to the study groups (Vieira et al. 2004; Silva-Junor 2013). After 12 h, the animals were euthanized by anesthetic overdose (sodium thiopental 150 mg/kg and lidocaine 10 mg/kg via i.p.) (Macedo et al. 2012; Silva-Junor 2013).
Macroscopic analysis
After euthanasia of the animals, exploratory laparatomy was performed, the bladder of the animal was removed, emptied, and weighed on an analytical scale, and bladder edema was reported as increased bladder wet weight (BWW), which in turn was expressed as normalized by bladder weight/20 g of animal weight after treatment (Vieira et al. 2004).
Microscopic analysis
The bladders were fixed in formalin, diaphanized, and embedded in paraffin after being weighed and after microtomy in 4 μm bands, they were stained with hematoxylin and eosin (H&E) and analyzed in an optical microscope by two experienced clinical analysts through blind evaluation.
Quantification of urinary hemoglobin by cyanomethaemoglobin method
In this test, an adaptation of the technique described by Harold and Drabkin (1935) was used. The bladders were homogenized in Drabkin reagent (100 mg of bladder tissue per mL of reagent) and after 1 h of incubation, the bladders were centrifuged at 10,000 (g) for 10 min. The supernatants were extracted and centrifuged again at 10,000g for 10 min. The absorbance of the supernatant was quantified using a microplate reader at wavelength of 450 nm and the hemoglobin concentration was calculated through the analytical curve previously constructed using hemoglobin standard (Labtest, Brazil) and the results were expressed in μg of hemoglobin/mg of tissue.
Evaluation of vascular protein leakage by the Evans blue dye technique
The animals submitted to intraperitoneal injection of ifosfamide, 30 min before euthanasia, were received (25 mg/kg) of Evans blue intravenously in the caudal plexus as adapted from Mota et al. (2007). After euthanasia, the bladders were removed, dissected, and incubated in test tubes containing formamide solution (1 mL/bladder) at 56 °C for 6 h (overnight) for dye extraction. The total dye extracted was determined using a spectrophotometer at 550 nm, followed by a standard curve to express the data in ng of Evans blue/mg of tissue.
Determination of myeloperoxidase activity in bladder tissue
The bladder tissue was homogenized in potassium phosphate buffer containing 0.5% hexadecyltrimethylammonium bromide and centrifuged at 4500 rpm for 15 min at 4 °C as proposed by Alves-Filho et al. (2006). The pellet was resuspended and the myeloperoxidase (MPO) activity was determined at 450 nm using o-dianisidine dihydrochloride and 1% hydrogen peroxide. An MPO unit was defined as the amount of MPO capable of breaking 1 mmol of peroxide/min and the data were reported in units per milligram of tissue (U/mg of tissue).
Determination of malondialdehyde levels in bladder tissue
Malondialdehyde (MDA) levels in bladder tissue were determined by the Mihara and Uchiyama method (1978). The samples were homogenized in KCL ice 1.15% to prepare a 10% homogenate. Then, aliquots of 250 μL of homogenate were added to tubes containing 1.5 mL of 1% H3PO4 and 500 μL of aqueous thiobarbituric acid (0.6%). Subsequently, the tubes were heated for a period of 45 min in a water bath at 100 °C and the reaction mixture was then cooled in a cold water bath, followed by the addition of 2 mL of n-butanol. After the addition of n-butanol, the samples were shaken with a vortex mixer for 1 min, and then centrifuged at 1500 rpm for 10 min. The supernatant was analyzed using a UV-Vis spectrophotometer at an absorbance of 520 and 535 nm, and the result was obtained by the difference in absorbance of the two readings. The results were expressed in nmol/g of bladder tissue.
Measurement of tissue nitrite and nitrate levels
Nitrite/nitrate (NOx) is measured indirectly through its metabolites, nitrite and nitrate, using the Griess reagent, according to the method described by Green et al. (1982). The tissue samples were homogenized in 0.15 M KCl (1 mL/100 mg of tissue), and the homogenate was centrifuged under refrigeration (Cunha et al. 2016). Later, 100 μL of the supernatant was mixed with 100 μL of Griess reagent. The absorbance at wavelength 540 nm was measured after 10 min of incubation. Nitrate/nitrite levels were expressed as μM nitrite and nitrate (NOx).
Determination of superoxide dismutase levels in bladder tissue
Superoxide dismutase concentration was measured using a modified spectrophotometric assay (Das et al. 2000; Cunha et al. 2016). In this method, the enzyme activity is calculated by the amount of superoxide dismutase (SOD) capable of inhibiting nitrite formation by 50%. The bladder tissue was homogenized in 1 mL/100 mg of potassium phosphate buffer (50 nM, pH 7.4). One hundred microliters of the homogenate was added to 1110 μL phosphate buffer, 75 μL L-methionine (20 mM), 40 μL Triton X-100 (1% v/v), 75 μL hydroxylamine chloride (10 mM), and 100 μL EDTA (50 μM). This solution was incubated in a 37 °C water bath for 5 min, then 80 μL of riboflavin solution (50 μM) was added and exposed to light for 10 min. From this solution, 100 μL of the sample was removed and another 100 μL of Griess reagent was added to wells, and after 10 min, the absorbance was read at 550 nm on scanning multiwell spectrophotometer ELISA reader. In addition, the amount of total protein was determined with a commercial kit (Labtest, Brazil). The results were expressed as units of SOD/μg of protein (uSOD/μg).
Determination of reduced glutathione levels in bladder tissue
The glutathione (GSH) concentration was determined according to the method proposed by Sedlak and Lindsay (1968). The determination of reduced glutathione is based on the reaction of DTNB [5.5 ditidio-bis-(acido-2-nitrobenzoic)] with free thiol giving rise to a mixed disulfide plus 2-nitro-5-benzoic acid. Samples of the bladder tissue were homogenized in 0.02 M EDTA for subsequent preparation of a 10% homogenate. Next, 400 μl aliquots of the homogenate was added to 320 μl distilled water and 80 μl 50% trichloroacetic acid (TCA). Then, the material was centrifuged at 3000 rpm for 15 min at 4 °C. After centrifugation, 400 μL of supernatant was removed and mixed with 800 μl of 0.4 M TRIS buffer (pH 8.9) and 20 μL of 0.01 M DTNB (Ellman’s reagent). The mixture was finally stirred for 3 min and the absorbance was measured at 412 nm in a spectrophotometer. Results were expressed in μg GSH/g tissue.
Measurement of tissue levels of IL-1β and TNF-α by ELISA
Tissue concentrations of tumor necrosis factor-α (TNF-α) and interleukin-1β (IL-1β) were determined by enzyme-linked immunosorbent assay (ELISA) using commercially available kits following manufacturer’s instructions (ELISA R & D Systems, Minneapolis, MN, USA). The enzyme immunoassay was performed at room temperature 25 ± 5 °C using 100 μL of each component. Briefly, antibodies and other substrates were diluted in BSA (1% bovine serum isolated albumin in PBS pH 7.4), and the bladder tissue was homogenized at 10% in 0.5% BSA in PBS (pH 7.4). The plates were washed three times with PBS Washing Solution (pH 7.4 + 0.05% Tween 20) between steps. To perform the ELISA, each well of the plate was coated with the optimal concentration of capture antibody by overnight incubation (room temperature 25 ± 5 °C). After blocking with BSA for 1 h, followed by washing, samples and standards were distributed (duplicate standards) and incubated for 2 h. After washing, the biotinylated detection antibody was added and incubated for 2 h. After incubation time and successful washing, streptoavidin was incubated for 20 min (successful washing) and then the reaction was revealed by incubation for 20 min at room temperature and under the light of TMB chromogenic substrate (tetramethylbenzidine + hydrogen peroxide), followed by the addition of a reaction inhibitor (H2SO4 1 M 100 μL). The reading was performed at a wavelength of 450 nm in a microplate spectrophotometer and the data were calculated from the serial concentration standard curve. Results were expressed as cytokine picograms per milligram of tissue (pg/mg of protein).
Statistical analysis
Multiple comparisons of groups were carried out through analysis of variance (ANOVA) prior to Tukey’s post hoc test. Tukey’s test was used as post hoc analysis once the null hypothesis (H0) was rejected. The p value < 0.05 is considered negative in the analyses, with a significance level of 0.05. All analyses were performed using R Studio software (Version R-3.6.2).
Results
Wet weight and histopathological parameters
The administration of ifosfamide at a dose of 400 mg/kg (IFOS) induced severe changes that translated into hemorrhage and tissue edema in the bladders which could be verified by the increase in the wet weight of the bladder (BWW) by 65.87% at 12 h compared with the control group (Fig. 1). IFOS-evoked increase in BWW was significantly inhibited by pretreatment with α-phellandrene at doses of 25 and 50 mg/kg (31.59 and 29.83%, respectively, Fig. 1). However, α-phellandrene at doses of 6.25, 12.5, or 100 not was capable of inhibiting IFOS-induced edema formation (6.87, 19.74, and 6.50%). Pretreatment with the classic Mesna protocol similarly inhibited the increase in BWW (36% reduction) offering significant protection. There was nonetheless no significant difference between the inhibitory effects reached after treating animals with α-phellandrene (25 and 50 mg/kg) in relation to Mesna treatment.
Effect of α-phellandrene on bladder wet weight in ifosfamide-induced hemorrhagic cystitis in mice. Data are expressed as a ratio of wet weight of the bladders to animal weight (mg/20 g animal). The results show through Fig. 2 the analysis of variance (ANOVA) for the variable wet weight of the bladder. From ANOVA, it is observed that the variable has p value lower than the considered significance level (α = 0.05). Thus, there is a statistically significant difference between treatments regarding the behavior of the variable
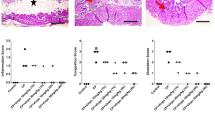
Macroscopic evaluation (Fig. 2) showed evident edema and hemorrhage with mucosal hematomas and intravesical clots, severe microscopic alterations, and the bladder presents multiple points of hemorrhage, cell loss, polymorphonucleated infiltrate, and marked ulceration (+ 3 score) in the bladder of animals treated with ifosfamide different from the control group (SHAM group) which received a score of 0 (0–0) for edema and hemorrhage. Animal groups pretreated with α-phellandrene (6.25 or 12.5 mg/kg) presents only a slight difference compared with the IFOS group (+ 2 score) (p > 0.05). The α-phellandrene 25 and 50 mg/kg groups showed a marked reduction in cell loss, hemorrhage, and edema, showing greater apparent protection compared with the negative control group (p < 0.05). Furthermore, no change was observed in the bladder of the animals when they were treated with α-phellandrene 100 mg/kg. According to the macroscopic evaluation of the bladder, the reference compound Mesna (160 mg/kg) exhibited a marked reduction in cell loss, bleeding, and edema compared with the negative control group (+ 1 score). Again, there was no significant difference between the inflammatory parameters in animals treated with α-phandandrene (25 or 50 mg/kg) compared with treatment with Mesna.
Effects of α-phellandrene (α-Phe) on macroscopic parameters of hemorrhagic cystitis induced by ifosfamide. a Group “sham,” received only saline as placebo, without induction of hemorrhagic cystitis. b Negative control group, suffered induction of hemorrhagic cystitis and was treated with the vehicle (Tween/Saline); pre and post-treatment standard. c–g Test groups, received pretreatment with monoterpene α-phe (6.25;12.5; 25; 50; 100 mg/kg) respectively. h Positive control group, received Mesna (2-mercaptoethanesulfonate sodium). All treatments were intraperitoneal (ip); the choice of the above image was through the selection of a bladder considered median among its group. The SHAM group consisted only in the administration of vehicle to untreated animals
In light of the histological analysis, the administration of ifosfamide induced severe microscopic changes besides the development of pronounced edema and multiple bleeding points, cell loss, infiltrate of polymorphos nuclear cells infiltrate, and ulceration (Fig. 3b), when compared with the control bladders (Fig. 3a). In turn, α-phellandrene attenuated the toxic effects of administering ifosfamide expressed by reducing cell loss, hemorrhage, and edema. The analysis of these results showed that the dose of 25 mg/kg of α-phellandrene exhibited greater protective capacity for microscopic lesions induced by ifosfamide (Fig. 3c). Animals that were treated with Mesna (160 mg/kg) exhibited characteristics close to those of normal animals. The pattern of tissue preservation was higher than that presented by the group treated with α-phellandrene (IFOS + α-phellandrene) (Fig. 3d).
Effects of α-phellandrene on histopathological changes in bladder tissues of mice with ifosfamide-induced hemorrhagic cystitis. Representative histological alterations of the bladders obtained from rats of different groups. a Control group. b IFOS group. c IFOS + α-phellandrene (25 mg/kg) group. d IFOS+ Mesna (160 mg/kg) group (hematoxylin and eosin staining, × 400 magnification)
It is interesting to note that despite the lack of representation of the other doses of α-phellandrene in Fig. 2, in all doses used, the pattern of tissue preservation was higher than that presented by the group treated with Mesna (IFOS + Mesna) (Fig. 3).
Effect of α-phellandrene on bleeding and bladder edema induced by ifosfamide
Contrary to the saline group, the bladder wall in IFOS-treated animals showed significantly increase hemorrhage by 62.94% as indicated in Fig. 4a, b. Pretreatment with α-phellandrene inhibited by 51.71 and 62.48% IFOS induced the hemorrhage in the bladder tissue at doses of 12.5 and 25 mg/kg, respectively (Fig. 4a). However, α-phellandrene at doses of 6.25, 50, or 100 mg/kg was unable to significantly reduce hemorrhage (32.20, 24.98, and 13.52%, respectively).
Effect of α-phellandrene on the parameters of hemorrhage and tissue edema. a The hemorrhage was indirectly assessed by tissue hemoglobin levels and the data are expressed as tissue hemoglobin levels (μg/mg of tissue). b Bladder edema was evaluated by tissue Evans blue content and results are expressed as nanogram of color per mg of tissue (ng/mg of tissue). The results indicate that the p value < 0.05 the control group (treated with saline alone) and the ifosfamide group present statistically significant difference, that is, there is a statistically significant difference between treatments regarding the behavior of the variable
Confirming the literature data (Gray et al. 1986) of edema in the IFOS group was significantly higher than the saline group (by 75.60%) (Fig. 4b). Treatment with the α-phellandrene (6.25, 12.5, 25, or 50 mg/kg), significantly reduced the bladder edema scores in 34.67, 34.66, 39.3, and 33.06%, respectively. Nonetheless, α-phellandrene at doses of 100 mg/kg showed non-significant changes in bladder edema when compared with IFOS group 22.49%, respectively. The intraperitoneal treatment with Mesna (160 mg/kg) caused a significant inhibition of hemorrhage (51.97%; Fig. 4a) and edema (34.94%; Fig. 4b) induced by this chemotherapeutic agent. Furthermore, there was no statistical difference (p > 0.05) between the Mesna group and the animals that received felandrene on bleeding or bladder edema induced by ifosfamide.
To delineate the mechanisms by which the effect of monoterpene α-phellandrene is capable of attenuating the bladder damage induced by ifosfamide, the dose that showed the best effect in the tests (25 mg/kg) was used to investigate the neutrophil migration, oxidative stress, and the presence of inflammatory cytokines.
Myeloperoxidase activity
Massive neutrophil migration is also a characteristic of cystitis induced by cyclophosphamide administration, as indicated by increased MPO activity in the bladder tissue, by 77.33%, when compared with the control group (p < 0.05). The administration of α-phellandrene (25 mg/kg) produced a significant (p < 0.05) reduction of MPO levels (75.70%) compared with the mice treated with IFOS and no significant difference was observed when compared with Mesna administration. Pretreatment with Mesna (160 mg/kg, the drug used as the standard therapy) partially but significantly reduced (p < 0.05) IFOS-induced increase in MPO (45.54%) (Fig. 5). Additionally, there was no statistical difference between the effects of the Phellandreno or Mesna groups when compared with the control.
Effect of α-phellandrene on the myeloperoxidase activity (MPO) (U/mg of tissue). The results indicate that the p value < 0.05 the control group (treated with saline) and the ifosfamide group present statistically significant difference, that is, there is a statistically significant difference between treatments regarding the behavior of the variable
Tissue malondialdehyde levels
The administration of ifosfamide significantly increased the levels of MDA (34.35%, p < 0.05) in the urinary bladder when compared with control group. Pretreatment with α-phellandrene (25 mg/kg) was able to prevent this increase (34.21%, p < 0.05), suggesting that this monoterpene is capable of reducing oxidative damage including lipid peroxidation in ifosfamide-induced hemorrhagic cystitis (Fig. 6a). Treatment with Mesna also decreased significantly MDA levels when compared with IFOS-treated mice (26%); however, there was no difference when compared with the group treated with felandrene (p > 0.05). Meanwhile, the levels of MDA from mice treated with both α-phellandrene and Mesna were not significantly different from the responses of the control group.
Effect of α-phellandrene on tissue levels of oxidative stress markers. a Malondialdehyde (MDA) levels were increased with cystitis induction and this increase was significantly inhibited by pretreatment with monoterpene α-phellandrene. b α-Phellandrene has prevented increased tissue levels of reactive nitrogen (NOx) species. c The pretreatment with monoterpene (25 mg/kg) and Mesna (160 mg/kg) was able to prevent depletion of superoxide dismutase (SOD) activity d The pretreatment with monoterpene was able to prevent depletion of reduced glutathione (GSH) tissue levels. The results indicate that according to p < 0.05 in the four stress markers, there is a difference between the treatments with the control group (treated with saline alone) and the ifosfamide group by the ANOVA and Tukey
Tissue of nitrite and nitrate levels
Ifosfamide (IFOS) induced a significant increase in tissue nitrite and nitrate concentration and indirect markers of nitric oxide (NO) synthesis (p < 0.05) by 18.75% when compared with the control group. Pretreatment with α-phellandrene monoterpene (25 mg/kg) was able to significantly attenuate (p < 0.05) this increase (25%) when compared with the IFOS group and significant difference was observed towards to the Mesna group, postulating that this monoterpene has the potential to act as a modulator of important inflammatory pathways. Treatment with Mesna (160 mg/kg) did not differ significantly the NO formation in the bladder (6.25%, Fig. 6b) of IFOS group.
Tissue superoxide dismutase activity
The depletion of tissue SOD activity by ifosfamide (IFOS)-induced tissue oxidative stress is statistically significant compared with the control group, by 69%, which indicates that this process is highly linked to the lack of control of redox balance. IFOS-induced mice pretreated with α-phellandrene (25 mg/kg) or Mesna (160 mg/kg) showed a significant (p < 0.05) improvement in the activity of SOD (49.1% and 68.78%, respectively) when compared with the IFOS control rats. No significant differences were observed between the SOD levels of α-phellandrene group compared with Mesna group (p > 0.05). Furthermore, there were no statistical differences between α-phellandrene and Mesna compared with control group. These data indicate that this monoterpene has promising protective activity on endogenous antioxidant defense machinery (Fig. 6c).
Reduced glutathione tissue levels
A significant reduction in bladder levels of GSH was detected in IFOS-treated mice by 190% when compared with control group (SHAM group). Administration of α-phellandrene (25 mg/kg) induced more significant increase (p < 0.05) in the antioxidant parameter (49.1%) than Mesna group (160 mg/kg) when compared with the IFOS-treated mice (68.78%) (Fig. 6d). Furthermore, it is interesting to note that GSH levels were more significantly expressive in the group treated with felandrene when compared with the Mesna group.
Cytokine levels in bladder tissue
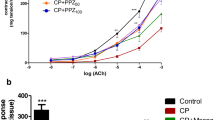
The increase in tissue levels of inflammatory cytokines in response to ifosfamide-induced hemorrhagic cystitis demonstrates that these cytokines are involved in the progression of tissue damage. The data revealed a significant (p < 0.05) increase in bladder levels of the inflammatory biomarkers IL-1β and TNF-α (62.74 and 19.46%) respectively in group IFOS-treated mice when compared with the respective control groups (SHAM groups). α-Phellandrene (25 mg/kg) and Mesna (160 mg/kg) pretreatment have restored the levels of IL-1β (19.35 and 21.58%, respectively) and TNF-α (28.44 and 14.31%, respectively) significantly (p < 0.05) in the bladder tissue of animals that were submitted to chemotherapy with high doses of ifosfamide (Figs. 7 and 8). Finally, it was also noted that there was a significant difference (p < 0.05) in the levels of TNF in the animals treated with α-phellandrene in relation to the treatment with Mesna.
Effect of α-phellandrene on inflammatory cytokines. The induction of hemorrhagic cystitis was able to cause a significant increase in the tissue levels of the cytokines IL-1β and TNF-α. Pretreatment with monoterpene α-phellandrene (25 mg/kg) or Mesna (160 mg/kg; standard for the prevention of cystitis) significantly reduced IL-1β (a) and TNF-α (b) levels in the bladders of IFOS-induced mice. The results are confirmed by ANOVA and Tukey tests, as shown in Fig. 8a and b illustrating the IL-1β and TNF-α cytokines
Representation of the variables for inflammatory cytokines, by the criterion used, if the interval between the levels of cytokines IL-1β (a) and TNF-α (b) contains the lower limit greater than zero, means that those levels do not present significant differences capable of altering the response variable. The control, α- phandandrene, and Mesna groups are represented by control A, B, and C, respectively. Analyzing IL-1β data (a), we note that none of the intervals (− 100; − 80; − 60; − 40; − 20; 0, 20) contains zero, which means that the mean levels are significantly different, as is the case with TNF-α (b), but in the Mesna and α-phandandrene groups, there is a significant difference however so small that it does not influence the response variable
Discussion
Oxazaphosphorine-induced hemorrhagic cystitis is well characterized and the etiology of this harmful adverse effect is related to its toxic metabolite (acrolein) of oxazaphosphorine, which promotes a rupture of the intraluminal membrane, enabling contact with the deeper epithelial layers, which in turn induces displacement of the urothelial cells to develop a typical robust inflammatory process, resulting histologically in subepithelial edema, neutrophil infiltration, hemorrhage, and endothelial tissue destruction (Brock et al. 1979; Theman et al. 1987; Gonzalez et al. 2005; Macedo et al. 2012; Silva Junior et al. 2013). In hemorrhagic cystitis, three factors can be highlighted in its pathophysiology: oxidative stress caused by acrolein in the bladder lumen, the inflammatory process that is installed with emphasis on edema, since it is a measurable factor, and bleeding that characterizes the general clinical aspect of this condition (Haldar et al. 2014). Regarding this, the protocols developed in this research sought to elucidate the effective participation of α-phellandrene in the different stages of the disease mentioned above.
Results of the present study indicate that IFOS induces marked urinary bladder toxicity (characterized by increased bladder wet weight, vascular permeability, macroscopic and microscopic damage, inflammatory cell infiltration) is prevented by α-phellandrene pretreatment. The formation of edema which is characteristic of HC was observed in this investigation. The edema was accessed indirectly through the evaluation of the mean bladder wet weight and it was observed that both Mesna and α-phellandrene showed that they were capable of preventing the appearance of edema. For α-phellandrene, only doses of 25 and 50 mg/kg showed significant results in this aspect. In this regard, studies have shown that extracts of medicinal plants or compounds isolated from these plants can reduce cystitis induced by oxazophorines in rodents (Boeira et al. 2011; Hamsa and Kuttan 2011; Rezvanfar et al. 2010). In this context of inflammatory induction, in contrast to the results observed with the macroscopic parameters, an edema reduction response at doses of 25 and 50 mg/kg was obtained, but the activity of α-phellandrene on bleeding was only significantly pronounced at the dose of 25 mg/kg. These same results can be observed visually through the macroscopic parameters that represent the median of its group.
In order to quantify more precisely the extent of bladder tissue edema, Evans blue dye was used because this chromogenic substrate binds with high affinity to serum albumin and this complex has frequently been used to quantitatively evaluate the extent of vascular leakage that accompanies tissue inflammation, consisting of a cheap, accurate, and efficient method, and which can be adapted to assess leakage in a variety of experimental pathological conditions, in particular inflammatory conditions (Krzyzanowska et al. 2010; Ramesh et al. 2014).
Thus, the results of the evaluation of the extension of hemorrhagic cystitis using Evans blue dye demonstrated that α-phellandrene at doses of 12.5, 25, and 50 mg/kg is capable of reducing the vascular protein leakage, thus consolidating that α-phellandrene has protective potential against the progression of hemorrhagic cystitis induced by ifosfamide. This finding is compatible with the pattern of anti-inflammatory activities expressed by monoterpenes that consist of chemical structures related to α-phellandrene (Romero and Romero 2014) such as thymol (Riella et al. 2012), carvacrol (Silva et al. 2013; Lima et al. 2013), and linalol (Peana et al. 2002). Boeira et al. (2011) evaluated the effect of flavonoids rutin, gallic acid, and quercetin on the edema formed in the bladder of mice related to cyclophosphamide-induced hemorrhagic cystitis and observed an anti-edematogenic action in all tested substances. Interestingly, our results show that α-phellandrene at lower doses prevents the damage caused by ifosfamide, but at the highest dose (100 mg/kg) appears to be ineffective. These profile changes are characteristic of a phenomenon called hormesis, described as an effect of some substances, which show biphasic dose responses displaying a “U” shape (Calabrese 2004). This pharmacological response (U shape) is observed in vitamins, minerals, and herbal medicines and that health benefits of many phytochemicals may also be conferred by hormesis mechanisms in which a phytochemical activates one or more adaptive cellular stress response pathways (Son et al., 2008; Calabrese 2008). Furthermore, this finding has importance with respect to the use of low doses of α-phellandrene highlighting the potential therapeutic effects of this drug as a promising approach to develop new anti-inflammatory agent.
Concerning the inflammatory process, the findings related to edema corroborate the results associated with the decrease in cytokine TNF-α as well as the reduction in NOx concentration and myeloperoxidase activity. These results corroborate the findings of Siqueira et al. (2016a) who evaluated the anti-inflammatory action of α-phellandrene in different inflammatory models and observed a reduction in the levels of TNF-α and IL-1 in addition to lower leukocyte migration in mice observed by intravital microscopy.
Another classic finding of oxazaphosphorine-induced hemorrhagic cystitis is the marked presence of extravasation of mature RBCs and reticulocytes characterized by the presence of macro- and microhematuria (Campobasso and Berrino 1972; Fu et al. 2016). This parameter of hemorrhage was quantitatively approached through the dosage of tissue hemoglobin, which in turn is directly proportional to the vascular ruptures that occurred in the bladder. Thus, the amount and size of these hemoglobin deposits in the extracellular matrix of bladder tissue is proportional to the extent of bladder damage caused by the ifosfamide metabolite. The data from this study revealed protective activity of α-phellandrene at doses of 12.5 and 25 mg/kg in bladder hemorrhage. Other substances of natural origin such as rutin, gallic acid, and ternatin had the same effects as those exhibited by α-phellandrene in this study (Boeira et al. 2011; Vieira et al. 2004).
Thus, in the context of the characterization of the cytoprotective activity of α-phellandrene, the investigation of the effect of this monoterpene on the presence of tissue degeneration markers in the progression of hemorrhagic cystitis was evaluated through the dosage of tissue MPO, MDA, and NOx levels because these markers provide (indirectly) a panoramic view of the process of neutrophil migration (Abraham and Rabi 2011), lipid peroxidation (Godinho et al. 2018), and oxidative stress, especially regarding the appearance of peroxynitrite in the intracellular environment (Korkmaz et al. 2007), respectively. In this sense, the findings of this study point to the modulating activity of cellular aggression resulting from inhibition of lipid peroxidation by α-phellandrene. Boeira et al. (2011) evaluated the effect of flavonoids rutin, gallic acid, and quercetin on MDA levels in the bladder of mice with cyclophosphamide-induced hemorrhagic cystitis and observed decreased concentrations in all substances tested. This activity displays these substances advantages over Mesna, because it is activated only by means of hydrolysis in an acid environment (in urine) and acts as a chemical chelator of acrolein, forming a stable and non-toxic product, which in turn is eliminated by urine, not causing damage to bladder tissue (Takamoto et al. 2004; Chabner and Longo 2015; Teles et al. 2017). In addition, despite demonstrating antioxidant activity, inhibiting MPO activity and buffering ROS at doses from 300 to 400 mg/kg (Macallister et al. 2013; Miller et al. 1981; Triantafyllidis et al. 2015), Mesna has protective activity against ifosfamide-induced hemorrhagic cystitis reduced due to its low half-life (> 0.5 h) and high cost (Rosa 2004).
Findings in the literature make the cytoprotective potential of α-phellandrene more consistent, because in our previous designs, it was demonstrated that this monoterpene has the potential to reduce levels of pro-inflammatory cytokines (IL-1β and TNF-α) (Siqueira et al. 2016a) and antidematogenic activity in acute inflammation models (Siqueira et al. 2016b), which provides subsidies to theorize that the reduction of hemorrhagic cystitis by α-phellandrene has a positive relationship with the modulation of endogenous systems of inflammatory regulation and antioxidant protection. In this context, the research of a drug that brings cytoprotective activities dependent on modulations of endogenous antioxidant defenses is a proposal with good premises (Dobrek and Thor 2012).
Cells have complex systems for endogenous defense and protection generally related to barriers against oxidative stress, highlighting systems such as superoxide dismutase (SOD) and the glutathione system (Kurutas 2015). SOD has a prominent capacity among antioxidant agents since its action on the superoxide anions (O2−) results in a decrease in the formation of peroxynitrite (ONOO2−−), a radical that is widely involved in the pathophysiology of hemorrhagic cystitis (Vasconcelos et al. 2011; Abo-Salem 2013; Matz and Hsieh 2017). The results expressed here show that both the monoterpenes α-phellandrene and Mesna were able to attenuate the depletion of SOD caused by cystitis induction, which suggests antioxidant activity, a finding that corroborates other monoterpenes such as cineole, geraniol, and linalool (Noacco et al. 2018).
Another barrier of defense against free radicals, glutathione (GSH), is an agent of great importance in the biotransformation and elimination of free radicals (Huber et al. 2008). Batista et al. (2007) demonstrated that the administration of glutathione to animals submitted to induction of hemorrhagic cystitis by acrolein diminished the observed effects of hemorrhage and edema. In this regard, this research quantified the tissue levels of GSH in bladder of rats with hemorrhagic cystitis and the findings showed that the α-phellandrene (25 mg/kg) was able to maintain the levels of GSH similar to the control group (p > 0.05); this protective potential corroborates the antioxidant activities attributed to this monoterpene (Cabral et al. 2015).
Conclusion
In conclusion, the results presented in this study provide evidence that α-phellandrene negatively modulates the inflammatory process of ifosfamide-induced hemorrhagic cystitis. The evidence presented here suggests that this modulation is associated with decreased migration of polymorphonuclear cells, decreased oxidative stress, and decreased TNF-α concentration. In summary, these results indicate that systemic treatment with α-phellandrene is able to prevent inflammatory events associated with HC and it may be useful for the prevention against ifosfamide-induced hemorrhagic cystitis.
Change history
16 October 2020
The published online version contains figure in poor quality.
References
Abo-Salem OM (2013) Uroprotective effect of pentoxifylline incyclophosphamide-induced hemorrhagic cystitisin rats. J Biochem Mol Toxicol 27:7–350. https://doi.org/10.1002/jbt.21494
Abraham P, Rabi S (2011) Protective effect of aminoguanidine against cyclophosphamide-induced oxidative stress and renal damage in rats. Redox Rep 16(1):8–14. https://doi.org/10.1179/174329211X12968219310837
Altayli E, Malkoc E, Alp BF, Korkmaz A (2012) Prevention and treatment of cyclophosphamide and ifosfamide-induced hemorrhagic cystitis. J Mol Pathophysiol 1(1):53–62. https://doi.org/10.5455/jmp.20120321060902
Alves-Filho JC, Freitas A, Russo M, Cunha FQ (2006) Toll-like receptor 4 signaling leads to neutrophil migration impairment in polymicrobial sepsis. Crit Care Med 34:461–470. https://doi.org/10.1097/01.ccm.0000198527.71819.e1
Arafa HM (2009) Uroprotective effects of curcumin in cyclophosphamide-induced haemorrhagic cystitis paradigm. Basic Clin Pharmacol Toxicol 104:393–399. https://doi.org/10.1111/j.1742-7843.2009.00379.x
Batista CK, Mota JM, Souza ML, Leitão BT, Souza MH, Brito GA, Cunha FQ, Ribeiro RA (2007) Amifostine and glutathione prevent ifosfamide- and acrolein-induced hemorrhagic cystitis. Cancer Chemother Pharmacol 59(1):71–77. https://doi.org/10.1007/s00280-006-0248-z
Boeira VT, Leite CE, Santos AA Jr, Edelweiss MI, Calixto JB, Campos MM, Morrone FB (2011) Effects of the hydroalcoholic extract of Phyllanthus niruri and its isolated compounds on cyclophosphamide-induced hemorrhagic cystitis in mouse. Naunyn Schmiedeberg's Arch Pharmacol 384:265–275. https://doi.org/10.1007/s00210-011-0668-0
Brock N, Stekar J, Pohl J, Niemeyer U, Scheffler G (1979) Acrolein, the causative factor of urotoxic side-effects of cyclophosphamide, ifosfamide, trofosfamide and sufosfamide. Arzneimittel-Forschung 29(4):659–661
Cabral C, Poças J, Gonçalves MJ, Cavaleiro C, Cruz MT, Salgueiro L (2015) Ridolfia segetum (L.) Moris (Apiaceae) from Portugal: a source of safe antioxidant and anti-inflammatory essential oil. Ind Crop Prod 65(1):56–61. https://doi.org/10.1016/j.indcrop.2014.11.041
Calabrese EJ (2004) Hormesis: a revolution in toxicology, risk assessment and medicine. EMBO Rep 5(1):S37–S40. https://doi.org/10.1038/sj.embor.7400222
Calabrese EJ (2008) Hormesis and medicine. Br J Clin Pharmacol 66(5):594–617. https://doi.org/10.1111/j.1365-2125.2008.03243
Campobasso O, Berrino F (1972) Early effects of cyclophosphamide on mouse bladder epithelium. Pathol Microbiol 38(2):144–157
Cannon J, Linke CA, Cos LR (1991) Cyclophosphamide-associated carcinoma of urothelium: modalities for prevention. Urology 38(5):413–416. https://doi.org/10.1016/0090-4295(91)80228-y
Chabner BA, Longo DL (2015) Manual de Oncologia de Harrison, 2nd edn. Amgh Editora, Porto Alegre
Cunha FV, Gomes Bde S, Neto Bde S, Ferreira AR, de Sousa DP, de Carvalho e Martins Mdo C, Oliveira Fde A (2016) Ferulic acid ethyl ester diminished Complete Freund’s Adjuvant-induced incapacitation through antioxidant and anti-inflammatory activity. Naunyn Schmiedebergs Arch Pharmacol 389(1):117–130. Chttps://doi.org/10.1007/s00210-015-1180-8
Das K, Samanta L, Chainy GBD (2000) A modified spectrophotometric assay of superoxide dismutase using nitrite formation by superoxide radicals. Indian J Biochem Biophys 37:201–204
Decker DB, Karam JA, Wilcox DT (2009) Pediatric hemorrhagic cystitis. J Pediatr Urol 5:254–264. https://doi.org/10.1016/j.jpurol.2009.02.199
Dobrek Ł, Thor PJ (2012) Bladder urotoxicity pathophysiology induced by the oxazaphosphorine alkylating agents and its chemoprevention. Postepy Hig Med Dosw (Online) 66:592–602. https://doi.org/10.5604/17322693.1009703
Fu D, Ye S, Xiao C, Xie Y, Gao J, Liang L, Yang X (2016) Incidence of cyclophosphamide-induced hemorrhagic cystitis in Chinese Han population with autoimmune disease. Int J Clin Exp Med 9(7):13160–13165 ISSN:1940-5901/IJCEM0020702
Godinho J, Sa-Nakanishi ABDE, Moreira LS, Oliveira RMW, Huzita CH, Mello JCP, Silva AOF, Nakamura CV, Previdelli IS, Ribeiro MHDM, Milani H (2018) Ethyl-acetate fraction of Trichilia catigua protects against oxidative stress and neuroinflammation after cerebral ischemia/reperfusion. J Ethnopharmacol 221:109–118. https://doi.org/10.1016/j.jep.2018.04.018
Gonzalez RR, Fong T, Belmar N, Saban M, Felsen D, Te A (2005) Modulating bladder neuro-inflammation: RDP58, a novel anti-inflammatory peptide, decreases inflammation and nerve growth factor production in experimental cystitis. J Urol 173(2):630–634. https://doi.org/10.1097/01.ju.0000143192.68223.f7
Gray KJ, Engelmann UH, Johnson EH, Fishman IJ (1986) Evaluation of misoprostol cytoprotection of the bladder with cyclophosphamide (Cytoxan) therapy. J Urol 136(2):497–500. https://doi.org/10.1016/s0022-5347(17)44929-9
Green LC, Wagner DA, Glogowski J, Skipper PL, Wishnok JS, Tannenbaum SR (1982) Analysis of nitrate, nitrite, and [15N]nitrate in biological fluids. Anal Biochem 126(1):131–138. https://doi.org/10.1016/0003-2697(82)90118-x
Haldar S, Dru C, Bhowmick NA (2014) Mechanisms of hemorrhagic cystitis. Am J Clin Exp Urol 2(3):199–208
Hamsa TP, Kuttan G (2011) Protective role of Ipomoea obscura (L.) on cyclophosphamide-induced uro- and nephrotoxicities by modulating antioxidant status and pro-inflammatory cytokine levels. Inflammopharmacology 19(3):155–167. https://doi.org/10.1007/s10787-010-0055-3
Harold J, Drabkin L (1935) Spectrophotometric studies. J Biol Chem 112(1):51–65
Haselberger MB, Schwinghammer TL (1995) Efficacy of mesna for prevention of hemorrhagic cystitis after high-dose cyclophosphamide therapy. Ann Pharmacother 29:918–921. https://doi.org/10.1177/106002809502900914
Huber PC, Almeida WP, Fátima A (2008) Glutationa e enzimas relacionadas: papel biológico e importância em processos patológicos. Química Nova 31(5):1170–1179. https://doi.org/10.1590/S0100-40422008000500046
Korkmaz A, Topal T, Oter S (2007) Pathophysiological aspects of cyclophosphamide and ifosfamide induced hemorrhagic cystitis; implication of reactive oxygen and nitrogen species as well as PARP activation. Cell Biol Toxicol 23:303–312. https://doi.org/10.1007/s10565-006-0078-0
Krzyzanowska AGI, Martin Y, Avendano C, Piedras MJ (2010) Evaluation of Evans blue extravasation as a measure of peripheral inflammation. Protoc Exch. https://doi.org/10.1038/protex.2010.209
Kurutas EB (2015) The importance of antioxidants which play the role in cellular response against oxidative/nitrosative stress: current state. Nutr J 15(1):71. https://doi.org/10.1186/s12937-016-0186-5
Lima DF, Brandão MS, Moura JB, Leitão JMRS, Carvalho FAA, Miúra LMCV, Leite JRSA, Sousa DP, Almeida FRC (2011) Antinociceptive activity of the monoterpene alpha-phellandrene in rodents: possible mechanisms of action. J Pharm Pharmacol 64:283–292. https://doi.org/10.1111/j.2042-7158.2011.01401.x
Lima MS, Quintans-Júnior LJ, Santana WA, Martins KC, Pereira SMB, Villarreal CF (2013) Anti-inflammatory effects of carvacrol: evidence for a key role of interleukin-10. Eur J Pharmacol 699(1-3):112–117. https://doi.org/10.1016/j.ejphar.2012.11.040
Macallister SL, Martin-Brisac N, Lau V, Yang K, O’brien PJ (2013) Acrolein and chloroacetaldehyde: an examination of the cell and cell-free biomarkers of toxicity. Chem Biol Interact 202(1–3):259–266. https://doi.org/10.1016/j.cbi.2012.11.017
Macedo FYB, Mourão LTC, Freitas HC, Lima RC Jr, Wong DV, Oriá RB, Vale ML, Brito GA, Cunha FQ, Ribeiro RA (2012) Interleukin-4 modulates the inflammatory response in ifosfamide-induced hemorrhagic cystitis. Inflammation 35:297–307. https://doi.org/10.1007/s10753-011-9319-3
Matz EL, Hsieh MH (2017) Review of advances in uroprotective agents for cyclophosphamide- and ifosfamide-induced hemorrhagic cystitis. Urology 100:16–19. https://doi.org/10.1016/j.urology.2016.07.030
Mihara M, Uchiyama M (1978) Determination of malonaldehyde precursor in tissues by thiobarbituric acid test. Anal Biochem 86(1):271–278. https://doi.org/10.1016/0003-2697(78)90342-1
Miller AB, Hoogstraten B, Staquet M, Winkler A (1981) Reporting results of cancer treatment. Cancer 47:207–214. https://doi.org/10.1002/1097-0142(19810101)
Mills KA, Chess-Williams R, McDermott C (2019) Novel insights into the mechanism of cyclophosphamide-induced bladder toxicity: chloroacetaldehyde’s contribution to urothelial dysfunction in vitro. Arch Toxicol 93:3291–3303. https://doi.org/10.1007/s00204-019-02589-1
Mota JM, Brito GA, Loiola RT, Cunha FQ, Ribeiro RA (2007) Interleukin-11 attenuates ifosfamide-induced hemorrhagic cystitis. Int Braz J Urol 33:704–710. https://doi.org/10.1590/S1677-55382007000500013
Noacco N, Rodenak-Kladniew B, de Bravo MG, Castro GR, Islan GA (2018) Simple colorimetric method to determine the in vitro antioxidant activity of different monoterpenes. Anal Biochem 555:59–66. https://doi.org/10.1016/j.ab.2018.06.007
Ozcan A, Korkmaz A, Oter S, Coskun O (2005) Contribution of flavonoid antioxidants to the preventive effect of mesna in cyclophosphamide-induced cystitis in rats. Arch Toxicol 79:461–465. https://doi.org/10.1007/s00204-005-0647-7
Peana AT, D’aquila PS, Panin F, Serra G, Pippia P, Moretti MDL (2002) Anti-inflammatory activity of linalool and linalyl acetate constituents of essential oils. Phytomedicine 9(8):721–726. https://doi.org/10.1078/094471102321621322
Ramesh BN, Mahalakshmi AM, Shalawadi M (2014) Vascular permeability and Evans blue dye: a physiological and pharmacological approach. J Appl Pharm Sci 11(4):106–113. https://doi.org/10.7324/JAPS.2014.41119
Rezvanfar MA, Farshid AA, Sadrkhanlou RA, Ahmadi A, Rezvanfar MA, Salehnia A, Abdollahi M (2010) Benefit of Satureja khuzestanica in subchronically rat model of cyclophosphamide-induced hemorrhagic cystitis. Exp Toxicol Pathol 62(3):323–330. https://doi.org/10.1016/j.etp.2009.05.005
Ribeiro RA, Freitas HC, Campos MC, Santos CC, Figueiredo FC, Brito GAC, Cunha FQ (2002) Tumor necrosis factor-α and interleukin-1β mediate the production of nitric oxide involved in the pathogenesis of ifosfamide induced hemorrhagic cystitis in mice. J Urol 167:2229–2234
Riella KR, Marinho RR, Santos JS, Pereira-Filho RN, Cardoso JC, Albuquerque-Junior RLC, Thomazzi SM (2012) Anti-inflammatory and cicatrizing activities of thymol, a monoterpene of the essential oil from Lippia gracilis, in rodents. J Ethnopharmacol 143(2):656–663. https://doi.org/10.1016/j.jep.2012.07.028
Romero RB, Romero AL (2014) Inibição de ciclooxigenases 1 (COX-1) e 2 (COX-2) por monoterpenos : um estudo in silico; Cyclooxygenase 1 (COX-1) and 2 (COX-2) Inhibition by monoterpenes : an in silico study. UNOPAR Científica. Ciências Biológicas e Saúde 16(4):307–316. https://doi.org/10.17921/2447-8938.2014v16n4p%25p
Rosa DD (2004) Uso de citoprotetores [Use of cytoprotectans]. Oncologia Baseada em Provas 1(1):43–50.
Sedlak J, Lindsay RH (1968) Estimation of total, protein-bound, and nonprotein sulfhydryl groups in tissue with Ellman’s reagent. Anal Biochem 25:192–205. https://doi.org/10.1016/0003-2697(68)90092-4
Sencer SF, Haake RJ, Weisdorf DJ (1993) Hemorrhagic cystitis after bone marrow transplantation. Transplantation 56:875–879. https://doi.org/10.1182/blood-2003-08-2815
Silva Junior RNC, Fialho SEM, Assunção AKM, Machado JL, Arruda D, Furtado PGR, Gonçalves Filho A, Nascimento FRF (2013) Caracterização do modelo inflamatório de cistite induzida por ciclofosfamida em camundongos Swiss. Revista de Ciências da Saúde 15(1):55–67. http://www.periodicoseletronicos.ufma.br/index.php/rcisaude/article/view/1922
Siqueira HDS, Neto BS, Sousa DP, Gomes BS, Cunha FVM, Oliveira F (2016b) Antiedematogenic effect of alpha-phellandrene in animal models. Curr Bioact Compd 12(2):107–113. https://doi.org/10.2174/1573407212666160210231052
Siqueira HDS, Neto BS, Sousa DP, Gomes BS, Silva FV, Cunha FVM, Wanderley CWS, Pinheiro G, Cândido AGF, Wong DVT, Ribeiro RA, Lima-Júnior RCP, Oliveira FA (2016a) α-Phellandrene, a cyclic monoterpene, attenuates inflammatory response through neutrophil migration inhibition and mast cell degranulation. Life Sci 160:27–33. https://doi.org/10.1016/j.lfs.2016.07.008
Son TG, Camandola S, Mattson MP (2008) Hormetic dietary phytochemicals. Neuromolecular Med 10(4):236–246. https://doi.org/10.1007/s12017-008-8037-y
Szabo C, Ischiropoulos H, Radi R (2007) Peroxynitrite: biochemistry, pathophysiology and development of therapeutics. Nat Rev Drug Discov 6:662–680. https://doi.org/10.1038/nrd2222
Takamoto S, Sakura N, Namere A (2004) Monitoring of urinary acroleín concentration in patients receiving cyclophosphamide and ifosfamide. J Chromatogr B Anal Technol Biomed Life Sci 806:59–63. https://doi.org/10.1016/j.jchromb.2004.02.008
Teles KA, Souza PM, Lima FAC, Araújo GA (2017) Rotina de administração de ciclofosfamida em doenças autoimunes reumáticas: uma revisão. Rev Bras Reumatol 57(6):596–604. https://doi.org/10.1016/j.rbre.2016.09.008
Theman H, Oberdorf E, Brock N, Pohl J (1987) Electron microscopic investigations of cyclophosphamide-induced lesions of the urinary bladder of the rat and their prevention by mesna. Urol Int 42(1):37–43. https://doi.org/10.1159/000281847
Triantafyllidis I, Poutahidis T, Taitzoglou I, Kesisoglou I, Lazaridis C, Botsios D (2015) Treatment with Mesna and n-3 polyunsaturated fatty acids ameliorates experimental ulcerative colitis in rats. Int J Exp Pathol 96(6):433–443. https://doi.org/10.1111/iep.12163
Vasconcelos SML, Goulart MOF, Silva MAM, Manfredini V, Benfato MS, Rabelo LA, Fontes G (2011) Markers of redox imbalance in the blood of hypertensive patients of a community in northeastern Brazil. Arq Bras Cardiol 97(2):141–147. https://doi.org/10.1590/S0066-782X2011001100008
Vieira MM, Macedo FY, Filho JN, Costa AC, Cunha AN, Silveira ER, Brito GA, Ribeiro RA (2004) Ternatin, a flavonoid, prevents cyclophosphamide and ifosfamide-induced hemorrhagic cystitis in rats. Phytother Res 18(2):135–141. https://doi.org/10.1002/ptr.1379
Yilmaz N, Emmungil H, Gucenmez S, Ozen G, Yildiz F, Balkarli A, Yavuz S (2015) Incidence of cyclophosphamide-induced urotoxicity and protective effect of mesna in rheumatic diseases. J Rheumatol 42(9):1661–1666. https://doi.org/10.3899/jrheum.150065
Funding
This work was financially supported by the FAPEPI - Fundação de Amparo a Pesquisa do Piauí (Research Support Foundation of Piauí/Brazil) EDITAL FAPEPI/MSDECIT/CNPq/SESAPI No 002/2016 – PPSUS (Projeto PPSUS EFP_00012091) and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES/Brazil).
Author information
Authors and Affiliations
Contributions
Oliveira FA, Almeida FRC, Sousa DP, and Lima-Júnior RC conceived and designed the research. Gonçalves RLG, Oliveira LSA, Lopes ME, Rezende DC, Nogueira KM, Pereira VMP, Souza LKM, Medeiros JVR, Wong DV, and Oliveira CPC conducted experiments and analyzed data. Gonçalves RLG, Cunha FVM, Neto BS, and Oliveira FA wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
The study was done with compliance to the ethics standards and approval from the Institutional Committee for Ethics in Animal Research of UFPI (protocol no. 279/16).
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gonçalves, R.L.G., Cunha, F.V.M., Sousa-Neto, B.P.S. et al. α-Phellandrene attenuates tissular damage, oxidative stress, and TNF-α levels on acute model ifosfamide-induced hemorrhagic cystitis in mice. Naunyn-Schmiedeberg's Arch Pharmacol 393, 1835–1848 (2020). https://doi.org/10.1007/s00210-020-01869-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-020-01869-3