Abstract
Background
Various education interventions were developed for preventing or managing OP, but the effects of those interventions on older adults were inconclusive.
Purpose
This study evaluated the effectiveness of educational interventions in preventing osteoporosis in older adults. A literature search was performed in MEDLINE (PubMed), Cochrane Library, and CBM (China BioMed Database) from the initial date of each database to Oct 2016.
Data Extraction
Two investigators independently extracted essential data from qualified studies concerning the settings, population, interventions, follow-ups, and outcomes of interest, namely effects of bone mineral density tests, changes in behavior, knowledge increase, self-efficacy, medication adherence (calcium and vitamin D), and quality of life, respectively.
Data Synthesis
A total of 17 studies met the inclusion criteria and therefore were included in the current study. The overall quality of the included studies was moderate. We were unable to carry out a meta-analysis due to the heterogeneity of these studies. We fond that compared with control groups, patients’ knowledge of osteoporosis increased significantly (p < .05) through all five interventions, which included PowerPoint presentations and discussion, class-based educational programs, osteoporosis self-management courses, revised health belief model and classes, computerized support programs and brush-up courses.
Limitation
Studies included in the present study were all conducted in Western countries and only descriptive methods were applied in synthesis due to heterogeneity in interventions and outcomes.
Conclusion
Education interventions were effective in preventing osteoporosis in older adults. Future research should focus on approaching this issue quantitatively (i.e., through meta-analysis).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis (OP) is a disease caused by multiple factors, including age, endocrine imbalance, nutrition, and genetic factors. Studies have demonstrated that a vast majority of patients remain undiagnosed and untreated because due to a lack of OP-related knowledge. They are not aware of the benefits of prevention and lack in motivation and ability to engage in OP prevention. There’s also inadequate social support and access to care for patients, and for immigrants especially, language has often been a barrier [1,2,3,4]. .Moreover, some diseases can be a risk factor for OP, such as sickle cell disease, lupus erythematosus, hypertension, and colon cancer, which can increase susceptibility to the OP by influencing the endocrine [5]. Medications such as corticosteroids, thyroid hormone, anticonvulsants, diuretics, and antacids containing aluminum may contribute to bone loss and make people more susceptible to secondary osteoporosis [6]. Studies showed that education for patients could increase their awareness of OP and improve adherence to preventive behaviors [7]. In an effort to address the importance of patients education, many studies adopted an experiment design to assess the effectiveness of various educational programs for OP patients and those who had a high risk of OP in preventing OP development and occurance. However, so far the results have been mixed. Nine studies found relatively large intervention effects [6,7,8,9,10,11,12,13,14], and two observed modest outcomes [15, 16], whereas two studies found no effect at all [17, 18]. Therefore, in the present study, we conducted a systematic review to determine the most effective strategies for OP prevention.
We found two review studies that previously assessed OP-related fractures [19], both of which focused on fracture rates, yet from different perspectives: One explored practice patterns in the diagnosis and treatment of OP after a fragility fracture, whereas the other examined a lifestyle intervention to prevent OP fractures. Kastner (2008) reviewed clinical decision support tools for OP disease management by examining randomized controlled trials (RCTs), regardless of publication language, from 1966 to July 2016 that investigated disease management interventions for patients at risk of OP [20]. A systematic review conducted in 2011 (Laliberté MC et al) assessed the effectiveness of interventions designed in improving the detection and treatment of OP for practitioners and researchers to select in primary care settings, particularly regarding the incidence of BMD testing and OP treatment initiation and fractures in patients at risk and high risk for whom OP screening or treatment is indicated based on Canadian and American guidelines [21].
Compared with Laliberté and Perreault (2001) [21] and Kastner et al. (2018) [22], the current systematic review covered a broader range of patients by including not only studies investigating diagnosed patients, but also studies looking at people who were at risk of OP or had a related fracture. Also, we added to previous studies by reviewing education interventions realized through different types of approaches (i.e., PowerPoint, RHBM, telephone counseling, OP self-management, mailed materials, etc). Furthermore, we examined a variety of outcome variables, including self-efficacy, changes in behavior, medication adherence, and quality of life, none of which were included in the two studies mentioned above. Lastly, instead of focusing on OP patients in general, the current study only concentrated on older adults.
The purpose of this study was to evaluate the effectiveness of educational interventions in preventing OP in older adults. Specifically, the study sought to identify the most effective educational program for practitioners and researchers to adopt in order to (a) improve the accuracy of BMD tests, (b) change patients’ health-related behaviors, (c) increase patients’ knowledge and self-efficacy, (d) improve patients’ adherence to medication (calcium and vitamin D intake), and (e) improve the quality of life among older adults with OP.
Methods
Databases for literature search
We did a thorough literature search in the following databases: MEDLINE-(PubMed), Cochrane Library, and CBM.
Search strategy
To select search terms, we performed a preliminary search in the aforementioned databases using various combinations of terms and their synonyms. We also reviewed medical subject heading terms to cover a wider range of literature. In MEDLINE, we searched for headlines containing both “osteoporosis” and “education” between 1987 and Oct. 2016. The same combination of keywords was also used in Cochrane Library’s Cochrane Center Register of Controlled Trials. The RCTs filter search strategy was used to further select studies that met the inclusion criteria. Same strategies were applied when we searched in the CBM database.
Inclusion criteria
The educational interventions were defined as interventions, regardless of form, designed to improve knowledge and awareness of older adults with OP the treatment and prevention of the disease. Studies were included if they were RCTs assessing educational interventions for older adults at risk of OP, with a confirmed diagnosis of OP, or with an existing or previous fragility fracture. Interventions could be carried out in any form (e.g., telephone-based education, mailed education materials, group-based education). All identified papers were screened by two investigators independently. For each publication, the investigators first reviewed the title and the abstract, and then indicated using a standardized form if it met the inclusion/exclusion criteria. Each investigator came up with a list of papers to be included in the current study, and disagreements were resolved through discussion and consensus. The third investigator was brought in when necessary.
Data extraction and quality assessment
The data extraction was performed by two independent investigators using a standardized data extraction form. Study setting (i.e., location and enrollment dates), study design (i.e., method of randomization, allocation concealment, and blinding), population characteristics (i.e., inclusion and exclusion criteria, sample size, number of patients assessed for eligibility and who met the inclusion criteria), interventions (i.e., components, format, aspect of OP disease management evaluated, and expected outcomes), outcomes, results, and other information (i.e., duration of follow-up, intention-to-treat analysis, withdrawal, and reasons for dropout) were extracted. Trial quality was summarized based on the risk of bias tools from the Cochrane Handbook. Each trial included was independently assessed for risk of bias (i.e., yes, no, or unclear) by two investigators. Any discrepancy was solved by consulting with a third investigator.
Data synthesis and analysis
Analyses were stratified according to the outcome variables of the studies included in the current study. Possible methodological heterogeneity of the selected studies were evaluated based on study quality, participants, interventions, and outcome variables. We concluded that the heterogeneity of the selected studies was too high to conduct a quantitative analysis, and thus a descriptive method was adopted.
Results
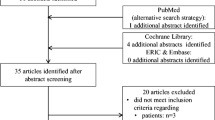
We identified 218 potentially relevant publications, and after further screening for relevance, we ended up with 141 items for further analysis (Fig. 1), indicating that a total of 17 reports met the inclusion criteria and therefore were included in the systematic review [6,7,8,9,10,11,12,13,14,15,16,17,18, 23,24,25]. Studies were excluded for failing to meet the inclusion criteria (i.e., RCT, educational intervention, older adults, and confirmed diagnosis of OP or fragility fracture) after either the titles and abstracts (113 studies) or the full text (11 studies) was examined Fig 2. All 17 studies that were eventually selected were published in English (see Tables 1 and 2 for the characteristics of these studies). The kappa agreement is 0.81 between the two investigators responsible for study screening.
Study quality
Overall, the quality of the selected studies was moderate. Table 1 provided an overview of the methods adopted in these studies. All studies were RCTs. Three of them adopted allocation concealment [7, 15, 23]. Only four studies were blinded [10, 12, 14, 23]. Data integrity was reported explicitly in all 17 trials, while only four studies reported selective results [11, 12, 16, 23].
Setting
Out of the 17 studies, two incorporated inpatients as participants [17, 26], two included outpatients [10, 24], one featured both [23], and five included community residents [9,10,11, 14, 25]. Regarding setting, 14 studies were conducted in the United States [6, 7, 10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25], two in Europe [8, 23], and one in Australia [9].
Participants
Overall, the inclusion and exclusion criteria in these studies varied greatly. Most studies focused primarily on older adults, although some investigated postmenopausal women [11, 15, 16] and thus included a smaller proportion of individuals aged 45 years or older. All other studies were in accordance with the inclusion criterion for age (i.e., 50 years old or older). The sample sizes ranged from 80 [25] to 1847 [17]. Participants in some studies had a confirmed diagnosis of OP [8, 10, 14, 16, 23, 24], whereas other studies focused on individuals at risk of OP [6, 7, 18] or with a fracture [13, 17, 18, 24, 25]. Follow-up ranged from less than or equal to 6 months (n = 8) [6, 7, 9, 10, 14, 23,24,25] through 6 months and 12 months (n = 5) [11, 15, 17, 18, 20] to more than 12 months (n = 3) [8, 12, 13]. The follow-up period was unclear in one study [24].
Effects of BMD tests
Five studies reported that there was a statistically significant difference in the BMD test between the education group and the control group (e.g., individuals received printed educational materials or usual care) [10, 13, 14, 18, 23]. Another study reported spinal and femoral BMD results [16], where participants completed a dual X-ray absorptiometry evaluation to assess osteoporosis. Participants in the education group also performed weight-bearing exercises, aerobic dancing, and flexibility exercises, and intervention was found to have improved spinal BMD (p = .031), but not femoral BMD (p = .579) [16].
Changes in behavior
There were three studies which reported changes in OP-related preventive, health-directed, and diet behaviors. In three study where different interventions (i.e., PowerPoint presentation and discussion, OP self-management course, education group plus BMD therapy) were adopted for participants with high risk of OP and uninvolved in preventive therapy, a significant difference in the behaviors mentioned above was found between the PowerPoint health promotion education group and the control group (p < .05) [7, 9, 11].
Another study (Qi BB et al., 2011) concluded that Mandarin-speaking Asian adults exposed to the self-efficacy-based OP preventive Educational (SEOPE) intervention would exhibit improvement at 2 weeks post-intervention with respect to (a) increased time spent exercising, and using OP medications, (b) self-efficacy for exercise, and (c) outcome expectations for exercise [7].
One study (Francis KL et al.,2009) reported that the OP self-management course (OPSMC) attendance improved osteoporosis knowledge, self-efficacy, and self-management skills/behaviors. During follow-up, compared with the control group, the experiment group displayed significantly larger improvements in health-directed behaviors (mean difference = 0.16, p = 0.020], positive and active engagement in life [mean difference = 0.14, p = 0.048], skill and technique acquisition [mean difference = 0.22, p = 0.006] and social integration and support [mean difference = 0.17, p = 0.033] [9].
Another study (Feldstein A et al., 2006) found that providing patient-specific post fracture advice to providers through an EMR message significantly increased BMD measurement accuracy and osteoporosis medication usage [10].
Knowledge increase
Out of the studies included, six measured outcome variables related to increased OP-related knowledge. The knowledge change was defined by Patients Viden om OSteoporose (i.e., PAVIOS), meaning “Patients’ knowledge of osteoporosis” [23]. PAVIOSwas measured using the Osteoporosis Knowledge Test, which is a 24-item measure with a 4-point rating scale [6].
One study (Yuksel N et al., 2010) conducted in 15 community pharmacies of Alberta, Canada did not find any difference in OP knowledge between the experiment group where participants received follow-up phone calls at the 2nd and the 8th week asking them to return to the pharmacy at the 16th week and the control group where participants received only printed educational materials (p = .31) [14]. Other forms of education programs, however, were found to be effective in improving participants’ OP-related knowledge, and these programs included PowerPoint presentations and discussion for individuals at high risk of OP [8], the revised health belief model (RHBM) for those at risk of OP [6], computerized support programs and brush-up courses [8], an OP prevention and self-management course [9], and a class-based educational program [23].
Self-efficacy
Out of the three studies that assessed self-efficacy, all of them discovered a significant difference between the experiment and the control group, although the interventions adopted varied.
Babatunde et al. (2011) recruited individuals who were at risk of OP, and assessed the effects of RHBM by comparing them with a waiting-list control group. They found that RHBM significantly improved self-efficacy in the experiment group (p < .001) [6]. Solomon et al. (2006), on the other hand, applied a mailed education intervention in the experiment group, and found that compared to the control group receiving only usual care, participants with a prior fracture in the had significantly higher self-efficacy (p = .03) [25]. Gardner et al. (2005) found that a discussion education brochure on fall prevention was also able to improve self-efficacy among participants (p = .036) [26].
Medication adherence (calcium and vitamin D)
Six studies examined adherence to a calcium and vitamin D regimen after education interventions [6, 11, 14, 15, 18, 23], and found that at the end of a 6-week, theory-driven intervention, compared to the control group, participants in the experimental group displayed significant improvement in their calcium intake (Wilks λ = 0.47, F1,108 = 122.97, P < .001, η2 = 0.53) [6]. It was also found that the EMR reminder led to greater self-reported total calcium intake than usual care, although the difference was small and not likely to be of clinical significance. These data should be interpreted with caution because although the results were statistically significant, they likely were due in part to the decrease in the control group’s reported intake. Total calcium intake increased from 1116.5 mg/d to 1311.4 mg/d in the EMR reminder group (p = .02 when compared with the change in usual care) and increased from 1221.5 mg/d to 1224.7 mg/d in the patient reminder group (p = .05 when compared with the change in usual care). Total reported calcium intake in the usual care group decreased from 1308.6 mg/d to 851.2 mg/d [11]. Another study (Yuksel N et al., 2010) reported that compare with the usual care group, calcium intake in the experiment group significantly improved (p = .011), where participants were reminded to return to the pharmacy at the 16th week [14], whereas no such effects were found for vitamin D intake (p = .66). Nurse education along with phone care follow-up was found helpful in improving self- reported calcium intake in this cohort of older postmenopausal women. At the 12th month follow-up, women in the nurse care group were significantly more likely to report that they had increased calcium intake via supplements and/or calcium-rich foods compared with the usual care group(nurse education group (n = 147),usual care group (n = 140),The number of patients in the two groups who increased their daily calcium intake was 86 (58.5%) and 55 (39.3%), respectively) [15]. However, no effect was found with a combination of personalized counseling and educational materials on medication adherence among people at risk of future fracture (p = .48) [18]. One study (Majumdar SR et al., 2008) examined the effectiveness of a multifaceted intervention and found that intervened participants reported greater use of calcium (p = .04) and vitamin D (p = .06), although at the same time they were somewhat more likely to report acid peptic disease (p = .06), osteoarthritis (p = .03) and current smoking (p = .06) [24].
Quality of life
In all studies, the purpose of education interventions was to improve the quality of life. However, only two studies (Majumdar SR et al., 2008) (Ciaschini PM et al., 2010) measured this variable. Interventions in both studies consisted of a combination of personalized counseling and educational materials compared to usual care [24] or follow-up phone calls at 2 and 8 weeks and a request to return to the pharmacy at 16 weeks compared to receiving printed educational materials [18]. Results suggested that neither approach had a significant effect on the quality of life relative to control groups (p > .05).
One study (Ciaschini PM et al., 2010) recruited community-dwelling individuals who were over 54 years old and at risk of osteoporosis-related fractures. The quality of life, measured using the OPTQoL questionnaire (osteoporosis-targeted quality of life questionnaire), remained similar within the immediate intervention protocol(i.e., IIP)group (p = .58) and delayed intervention protocol (i.e., DIP) group (p = .26) over the course of the study [18].
In another study (Majumdar SR et al., 2008) conducted in Edmonton, Alberta, Canada, participants were 50 years old with the experienced of a wrist fracture and visited the emergency department and fracture clinics. The quality of life was measured by the 22-item Osteoporosis-Related Quality of Life instrument. Overall, there was no significant difference between the experiment and the control groups in self-reported outcome variables such as health status, upper extremity disability, and osteoporosis-related quality of life or knowledge [24].
Discussion
Limitations
The quality of the studies in the current systematic review was moderate. All studies were RCTs, with clear data integrity, with seven studies adopting a blinded [10, 12, 14, 23] or allocation concealment [7, 15, 23] design. Selective reporting and other biases were rarely reported. Sample sizes varied greatly across samples, so did the type of interventions and the duration of follow-up.
Substantial heterogeneity existed among the identified trials in terms of participant characteristics, settings, the amount and duration of the intervention and control comparators, methods of intervention delivery, and the timing of outcome measures. Therefore, we failed to carry out a meta-analysis with effect sizes reported, and instead had to turn to systematic review in order to determine the effectiveness of various education interventions under various conditions.
Most studies selected were conducted in North America and Europe, and thus this systematic review may be susceptible to publication bias.
Despite the limitations mentioned above, we believe this review provides a relatively concise and informative summary of the effectiveness of education interventions designed to improve various aspects of the life quality among older adults with OP. We concluded in real-world practice, several interventions(i.e.,PowerPoint presentations and discussion, class-based educational programs, osteoporosis self-management courses, revised health belief model and classes, computerized support programs and brush-up courses) were beneficial or at least promising. Results showed that certain interventions(i.e., PowerPoint presentation and discussion, OP self-management course, education group plus BMD therapy) had significantly improved OP-related health behaviors and self-efficacy.
We found that interventions that had a positive effect on BMD for patients with OP or at risk of fractures were: (1) electronic medical records combined with an educational letter and follow-up phone calls, (2) one-on-one educational visits with primary care physicians along with lectures, and (3) weight-bearing exercises, aerobic dancing, and flexibility exercises. Moreover, knowledge about OP among older adults could be strengthened through both PowerPoint presentations and discussion and class-based educational programs. Medication adherence (calcium and vitamin D) could be enhanced through RHBM and counseling sessions via telephone for individuals with or at risk of OP.
The effectiveness of interventions also differed across populations. For patients in care organizations, the most effective intervention was patient-specific post-fracture advice received by providers through EMR messages, which we found significantly raised BMD measurement accuracy and osteoporosis medication intake, which lasted for as long as 6 months.
As to community residents, the most effective intervention turned out to be a multi-faceted community-based intervention directing towards primary care physicians and patients, consisting of facilitated bone mineral density testing, patient education, and patient-specific recommendations for osteoporosis treatment. The intervention lasted for 12 months.
When participants were inpatients, we found that the most effective intervention was a multifaceted one consisting of 3 components: (1) a brief counseling session to intervene patients by telephone, (2) a patient-specific reminder sent by fax or mail to the physicians of the patients being intervened, and (3) evidence-based treatment guidelines sent to these physicians. The interventions which lasted for 6 months.
The current systematic review focused on RCT method, which is the least likely to generate biased estimates. Through a comprehensive literature search, we were able to identify relevant systematic reviews and trials involving education interventions for older adults with OP. In order to reduce potential biases, two investigators evaluated each study independently using a standardized form before a decision to include/exclude a study was made.
A previous systematic review by Laliberté and Perreault (2001) [21] centered on the effectiveness of interventions to improve the detection and treatment of OP in primary care settings. The study assessed patients at risk (i.e., women ≥65 years old, men ≥70 years old, and men or women ≥50 years old with at least one major risk factor for OP) or with high risk (i.e., men or women using oral glucocorticoids or with previous fragility fractures) of OP and fractures. Therefore, compared with Laliberté and Perreault (2001), the current systematic review included a broader range of patients (i.e., those diagnosed with OP, at risk of OP, or with a related fracture). Also, Laliberté and Perreault (2001) largely focused on mailed materials sent to subjects, whereas our study included education interventions realized through a variety of approaches (e.g., PowerPoint, RHBM, telephone counseling, OP self-management, and mailed materials) [21]. In terms of outcome variables, Laliberté and Perreault (2001) only examined the effectiveness of BMD testing and fractures, while in the present review, we also looked at self-efficacy, knowledge increase, changes in behavior, medication adherence, and quality of life.
Most of the feasibility studies failed to test all proposed hypotheses due to small sample sizes, short duration, and insufficient power, and thus some of the results of these studies should be interpreted with caution. In some studies, participants had already been quite knowledgeable about OP to begin with, which may account for the minimal knowledge change after the education interventions [11]. Future research is needed to consider the long-term impact of these changes in order to evaluate the long-range benefits of improved bone health and fracture reduction, so that the reliability and validity could be established of various measures in a more heterogeneous sample.
Conclusion
Education via mailed materials and in-person discussion sessions could reduce the risk of osteoporosis among patients with a current fragility fracture or at risk of a second fracture. Interventions such as a combination of education group and BMD tests or OP brochures combining one-on-one education could change patients’ diets and exercise behaviors. An intervention containing class-based educational programs and OP self-management courses could increase OP-related knowledge. Future research should search for studies with larger sample sizes, more structured education interventions and other relevant outcome variables in order to add more solid evidence to this area of research.
References
Babbar RK, Handa AB, Lo CM (2006) Bone health of immigrant Chinese women living in new York City. J Community Health 31:7–23
Chan MF,Ko CY (2006) Osteoporosis prevention education program for women. J Journal of advanced nursing 54:159–170
Tan S, Ji L, Tsai J (2009) Greater osteoporosis educational outreach is desirable among Chinese immigrants in Chinatown, Chicago. Osteoporos Int 20:1517–1522
Taylor-Piliae RE, Haskell WL, Froelicher ES (2006) Hemodynamic responses to a community-based tai chi exercise intervention in ethnic Chinese adults with cardiovascular disease risk factors. Eur J Cardiovasc Nurs 5(2):165–174
Weaver CM, Gordon CM, Janz KF, Kalkwarf HJ, Lappe JM, Lewis R (2016) The National Osteoporosis Foundation’s position statement on peak bone mass development and lifestyle factors: a systematic review and implementation recommendations. Osteoporos Int 27:1281–1386
Babatunde OT, Himburg SP, Newman FL (2011) Theory-driven intervention improves calcium intake, osteoporosis knowledge, and self-efficacy in community-dwelling older black adults. J Nutr Educ Behav 43:434–440
Qi BB, Resnick B, Smeltzer SC, Bausell B (2011) Self-efficacy program to prevent osteoporosis among Chinese immigrants: a randomized controlled trial. Nurs Res 60:393–404
Nielsen D, Ryg J, Nielsen W, Knold B, Nissen N, Brixen K (2010) Patient education in groups increases knowledge of osteoporosis and adherence to treatment: a two-year randomized controlled trial. Patient Educ Couns 81:155–160
Francis KL, Matthews BL, Van MW, Bennell KL, Osborne RH (2009) Effectiveness of a community-based osteoporosis education and self-management course: a wait list controlled trial. Osteoporos Int 20:1563–1570
Feldstein A, Elmer PJ, Smith DH (2006) Electronic medical record reminder improves osteoporosis management after a fracture: a randomized, controlled trial. J Am Geriatr Soc 54:450–457
Rolnick SJ, Kopher R, Jackson J, Fischer LR, Compo R (2001) What is the impact of osteoporosis education and bone mineral density testing for postmenopausal women in a managed care setting? Menopause 8:141–148
Solomon DH, Gleeson T, Iversen M, Avorn J, Brookhart MA, Lii J, Losina E, May F, Patrick A, Shrank WH, Katz JN (2010) A blinded randomized controlled trial of motivational interviewing to improve adherence with osteoporosis medications: design of the OPTIMA trial. Osteoporos Int 21:137–144
Solomon DH, Polinski JM, Stedman M, Truppo C, Breiner L, Egan C, Jan S, Patel M, Weiss TW, Chen YT, Brookhart MA (2007) Improving care of patients at-risk for osteoporosis: a randomized controlled trial. J Gen Intern Med 22:362–367
Yuksel N, Majumdar SR, Biggs C, Tsuyuki RT (2010) Community pharmacist-initiated screening program for osteoporosis: randomized controlled trial. Osteoporos Int 21:391–398
Schousboe DJT, Debold RC, Kuno LS, Weiss TW, Chen YT, Iii TAA (2005) Education and phone follow-up in postmenopausal women at risk for osteoporosis. Disease Management & Health Outcomes 13:395–404
Bravo G, Gauthier P, Roy PM, Payette H, Gaulin P, Harvey M, Péloquin L, Dubois MF (1996) Impact of a 12-month exercise program on the physical and psychological health of osteopenic women. J Am Geriatr Soc 44:756–762
Shu DH, Stedman MR, Polinski JM, Jan SA, Patel M, Truppo C (2009) Adherence to osteoporosis medications after patient and physician brief education: post hoc analysis of a randomized controlled trial. Am J Manag Care 15:417–424
Ciaschini PM, Straus SE, Dolovich LR, Goeree RA, Leung KM, Woods CR, Zimmerman GM, Majumdar SR, Spadafora S, Fera LA, Lee HN (2010) Community based intervention to optimize osteoporosis management: randomized controlled trial. BMC Geriatrics 10:60
Elliot-Gibson V, Bogoch ER, Jamal SA (2004) Practice patterns in the diagnosis and treatment of osteoporosis after a fragility fracture: a systematic review. Osteoporos Int 15:767–778
Kastner M, Straus SE (2008) Clinical decision support tools for osteoporosis disease management: a systematic review of randomized controlled trials. J Gen Intern Med 23:2095–2105
Laliberté MC, Perreault S, Jouini G, Shea BJ, Lalonde L (2011) Effectiveness of interventions to improve the detection and treatment of osteoporosis in primary care settings: a systematic review and meta-analysis. Osteoporos Int 22:2743–2768
Kastner M, Perrier L, Munce SEP, Adhihetty CC, Lau A, Hamid J, Treister MV, Chan J, Lai Y, Straus SE (2017) Complex interventions can increase osteoporosis investigations and treatment: a systematic review and meta-analysis. Osteoporos Int 29:5–17
Nielsen D, Ryg J, Nissen N, Nielsen W, Knold B, Brixen K (2008) Multidisciplinary patient education in groups increases knowledge on osteoporosis: a randomized controlled trial. Scand J Public Health 36:346–352
Majumdar SR, Johnson JA, McAlister FA (2008) Multifaceted intervention to improve diagnosis and treatment of osteoporosis in patients with recent wrist fracture: a randomized controlled trial. CMAJ 178:569–575
Solomon DH, Finkelstein JS, Polinski JM, Arnold M, Licari A, Cabral DA, Canning C, Avorn J, Katz JN (2006) Randomized controlled trial of mailed osteoporosis education to older adults. Osteoporos Int 17:760–767
Gardner MJ, Brophy RH, Demetrakopoulos D, Koob J, Hong R, Rana A, Lin JT, Lane JM (2005) Interventions to improve osteoporosis treatment following hip fracture: a prospective, randomized trial. J Bone Joint Surg Am 87:3–7
Acknowledgements
The study was funded by the supported by “The Fundamental Research Funds for the Central Universities, No. 30918013115”.
Author information
Authors and Affiliations
Contributions
Iris Chi (School of Social Work, University of Southern California) contribute the language editing and suggestions for this version.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no conflicts to report.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
H. Lv the co-first author contributed equally to this manuscript.
Electronic supplementary material
ESM 1
(DOCX 13 kb)
Rights and permissions
About this article
Cite this article
Gai, Q.Y., Lv, H., Li, Y.P. et al. Education intervention for older adults with osteoporosis: a systematic review. Osteoporos Int 31, 625–635 (2020). https://doi.org/10.1007/s00198-019-05166-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05166-5