Abstract
Introduction
This prospective study investigates sexual function in women after a tension-free vaginal tape (TVT) operation and compares short-term and long-term effects.
Methods
Sixty-three women had a TVT operation performed at Aalborg University Hospital, Department of Gynecology and Obstetrics, between November 2008 and June 2010. Patients completed the Pelvic Organ Prolapse Urinary Incontinence Sexual Questionnaire-12 (PISQ-12) and the International Consultation on Incontinence Questionnaire-Urinary Incontinence Short Form (ICIQ-UI SF) before undergoing surgery, 6 months postoperatively, and at the long-term follow-up (mean 4 years and 9 months).
Results
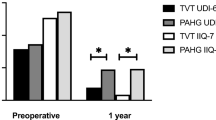
Forty-four women completed the two questionnaires all three times. Preoperatively, mean PISQ-12 was 33.8 [95% confidence interval (CI) 28.9-38.6] and the ICIQ-UI SF was 15.2 (14.4-16.0). Postoperatively the PISQ-12 increased significantly and the ICIQ-UI-SF decreased significantly, to 36.7 (31.5-41.9) and 2.5 (1.3-3.8), respectively, at the 6-months follow-up and 35.8 (33.6-38.1) and 4.9 (3.4-6.3), respectively, at the long-term follow-up. The greates improvement was in the physical domain of the PISQ-12. Women experienced less negative emotional reactions during intercourse, less coital incontinence, and less fear of being incontinent during intercourse after the TVT operation.
Conclusion
This study shows that a woman’s sex life does not deteriorate after a TVT operation, that their sexual function improves somewhat, and that results are sustained over time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stress urinary incontinence (SUI) has an adverse effect on a woman’s quality of life (QoL), and the way in which affects her sexual health is important [1]. Female sexuality is complex, and incontinence might have unfavorable effects on many factors contributing to sexual dysfunction: embarrassment, fear of odor, loss of self-esteem, psychological distress, dyspareunia because of urinary dermatitis, and urine leaking during intercourse being a nuisance are some of the effects that may lead to sexual dysfunction [2–4]. Several studies investigated the effect of incontinence surgery on sexual function, with conflicting results; some report improvement [5], some deterioration [6], and some no difference [7]. Most previous studies have a 6- to 12-month follow-up period; few have investigating the long-term effect after >12 months, and no studies compare short- and long-term effects. The aim of the study was to determine the long-term effects on women’s sexual function after a tension-free vaginal tape (TVT) operation and compare short- and long-term results.
Materials and method
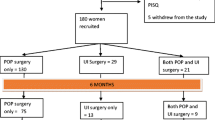
The study population consisted of 63 consecutive women who had a TVT operation between November 2008 and June 2010. Inclusion criteria were sexually active (within 6 months before operation), SUI or mixed (MUI) (predominantly stress) urinary incontinence, able to understand and write Danish. Permission from the ethical committee of Region North was obtained. All women underwent a preoperative physical examination involving gynecological examination and vaginal ultrasound, evaluation of incontinence with a 3-day voiding chart, and urinary flow assessment based on ultrasound postvoid residual (PVR) urine measurement. Preoperative data comprised age, parity, body mass index (BMI), and past medical history (Table 1). The TVT operation was performed under local anesthesia with mild sedation, according to the procedure described by Ulmsten [8]. No other procedures were performed in connection with the TVT procedure.
The women completed two standardized questionnaires: the Pelvic Organ Prolapse Urinary Incontinence Sexual Questionnaire-12 (PISQ-12) [9, 10] and the International Consultation on Incontinence Questionnaire-Urinary Incontinence Short Form (ICIQ-UI SF) [11, 12] before undergoing surgery. Each woman received a letter 6 months postoperatively with the same questionnaires; results from the short-term follow-up were previously published [13]. In June 2014, the same questionnaires were sent to the women in order to collect data for a long-term follow-up.
The PISQ-12, a validated, self-administered instrument used to evaluate sexual function in women with pelvic organ prolapse (POP) and/or incontinence, is based on 12 items that allow investigation of three different domains of sexual life: behavior (items 1–4), physical (items 5–9), and partner related (items 10–12). Scores are calculated by totalling the scores for each question, with 0 = always, 1 = often, 2 = sometimes, 3 = seldom, and 4 = never. Reversed scoring is used for items 1, 2, 3, and 4. Maximum score is 48, and higher scores indicate better sexual function. If more than two of the 12 values are missing, the short form (PISQ-12) no longer predicts the long-form scores and is therefore not valid [10]. We therefore excluded women who answered fewer than ten items. To be able to compare total scores, corrected the total score for women who answered ten or 11 items by counting the missing value as the mean value of the received values [10]. The ICIQ-UI SF is used to evaluate the severity of UI and its impact on health-related QoL. It contains three scored items and an unscored self-diagnostic item. A total score is calculated by adding them up; maximum score for worst incontinence is 21. The total score was used to evaluate incontinence pre- and postoperatively. The self-diagnostic item was used to classify the type of incontinence: SUI, urgency (UUI), or MUI. The Danish versions of the PISQ-12 and ICIQ-UI SF have been translated from English but have not been validated.
Statistical analysis
Student’s t test was used to compare groups, and one-way analysis of variance (ANOVA) was used to compare preoperative, postoperative, and follow-up scores.
Results
Sixty-three women underwent a TVT operation and fulfilled inclusion criteria; 44 (70 %) completed the PISQ-12 pre-and postoperatively and at the long-term follow-up. Nineteen women were thus excluded due to incomplete forms, including cases in which more than two of the 12 values in the PISQ-12 were missing; 12 were excluded at the 6-month postoperative follow-up and the remaining seven at the long-term follow-up. No statistically significant differences between groups were found. Demographic data are shown in Table 1. Mean long-term follow-up for the 44 women was 4 years and 9 months [standard deviation (SD) 7.2 months].
The PISQ-12 score showed an overall significant improvement in sexual function (Table 2). Preoperatively, mean PISQ-12 was 33.8 and long-term follow-up was 35.8, for a significant improvement in sexual function of 2.0 (p < 0.05). The overall PISQ-12 decreased slightly from the 6-month to the long-term follow-up, however; the difference was small and not significantly different (p > 0.05). ANOVA showed a statistically significant change in PISQ-12 over time (p < 0.05) (Table 2).
At the 6-month postoperative follow-up, 35 (80 %) women had improved sexual function compared with preoperatively. At the long-term follow-up, minor changes were noted, as 12 women reported a slightly higher score, 18 a slightly lower score, and five an unchanged score. Six women had a lower score at the 6 months postoperative follow-up, half of them had improved scores at the long-term follow-up. Three women had unchanged sexual function 6 months postoperative and one stayed unchanged, one improved and one lowered their sexual function at the long-term follow-up. Considering scores for all PISQ-12 questions, there was an increase primarily in items concerning negative emotional reactions during intercourse, incontinence during sexual intercourse, and fear of incontinence during sexual intercourse (Table 3).
The ICIQ-UI-SF score decreased postoperatively, indicating an improvement in incontinence (Table 2). Six months postoperatively, 28 (64 %) women became totally continent and reported an ICIQ- UI-SF score of 0. Sixteen (36 %) women experienced a decrease in ICIQ- UI-SF score from mean of 14.8 (13.2–16.3) to 6.9 (4.8–9.1) but not 0. At the long-term follow-up, 15 (34 %) women reported an ICIQ- UI-SF score of 0; 13 of them were continent at the 6-month follow-up; two were incontinent at the 6-month follow-up and became continent at long-term follow-up. From the first to the second follow-up, 15 (34 %) women became somewhat incontinent; however, the ICIQ- UI-SF score was significantly lower at the long-term follow-up [6.5 (4.6–8.4)], compared with preoperatively [14.8 (13.3–16.3); p < 0.05]. Of the 16 women who were still incontinent at 6 months, two became continent at the long-term follow-up, five became less incontinent, two remained unchanged, and seven became more incontinent. Of the 29 women who were somewhat incontinent at the long-term follow-up, two reported SUI, nine MUI, and 16 UUI; two had undefined UI.
The relationship between PISQ-12 and ICIQ-UI-SF was examined and is shown in Fig. 1. Preoperatively, many women had a high ICIQ- UI-SF and a low PISQ-12, indicating a substantial incontinence problem and a lower sexual function (Fig. 1a). At the 6-month follow-up, there was a clear shift downward and to the right, showing improved sexual function and decreased incontinence (Fig. 1b). Figure 1c illustrates the relationship at the long-term follow-up. When comparing Fig. 1b and c there is no clear shift in the combined group, but some women became slightly more incontinent without a significant deterioration in sexual function.
Relationship between Pelvic Organ Prolapse Urinary Incontinence Sexual Questionnaire-12 (PISQ-12) and International Consultation on Incontinence Questionnaire-Urinary Incontinence Short Form (ICIQ-UI SF) scores for the 44 women assessed: a preoperative, b 6 months postoperative, c Long-term follow-up
Discussion
This study adds further evidence to the fact that sexual function improves in women with SUI who a TVT operation: the 44 women assessed presented a statistically significant increase in PISQ-12 score. Both the 6-month and long-term follow-up data show a decrease in negative emotional reactions during intercourse, coital urinary incontinence, and fear of being incontinent during intercourse. A slightly lower PISQ-12 score was observed at the long-term follow-up, and scores went both up and down. This probably indicates that many factors concerning their sex life occurred over the mean 4 years and 9 months. Some women entered menopause and may suffer from urogenital atrophy, some ageing partners may suffer from impotence because of prostatic disease, some patients may have been divorced, etc. We did not investigate these factors. Unchanged orgasm intensity (question 3 in PISQ-12) argues for maintained normal sensibility in the genital area after the operation. The clinically minimum important difference (MID) in changes in PISQ-12 has not been widely investigated. In an article by Mamik et all [14], however, a figure of 6 was considered clinically important. More studies on this important subject are needed. Our study shows an improvement in sexual function of 2, but very importantly, that number did not worsen over time.
We defined continent women as an ICIQ- UI SF score of 0, and one could probably argue it is an unrealistic low score. It seems, however, that more women experienced episodes of UUI at the long-term follow-up. Strengths of our study are its prospective design, use of standardized questionnaires concerning sexual function and incontinence, and a long-term follow-up. Weaknesses are the small study population and that we did not use the new PISQ-IR [15], as the form was not available when the study was performed.
The previous study by Glavind et al. [13] showed that women’s sexual function improved 6 months after a TVT operation; these new data show that this effect is maintained up to >4 years after the operation. In agreement with our results, in their prospective study, Jha et al. reported an overall improvement in sexual function after TVT/TVT-obturator operation as assessed using the PISQ-31 [16]. Improvements were foremost in the physical and partner-related domain. Two other studies suggest that TVT and other SUI surgeries do not affect sexuality postoperatively. In those studies, no standardized questionnaires were used: Maaita et al. found that the majority (72 %) of women experienced no change in sexual function after a successful TVT operation [7]. Lemarch et al. came to a similar conclusion when investigating women’s sexual function after different SUI surgeries [17]. Neither study indicated that SUI led to deterioration in sexual function. Yeni et al., using the Index of Female Sexual Function (IFSF) scale, reported decreased genital sensation and vaginal lubrication after TVT surgery, which might inhibit orgasm and consequently decrease sexual function [6]; our results do not indicate this. Sexual dysfunction was reported as being a risk factor following TVT operation. The study population of 55 (100 %) women had normal sexual function before TVT operation, which dropped to 58.2 % after the operation [7]; 20 % reported this being due to dyspareunia and loss of libido. The questionnaire used in the study was not standardized, and there was only one question concerning sexual satisfaction.
Concerns that the tape may shrink, lose strength, or change properties over time and thereby cause pain have been discussed [18]. Our study found no evidence suggesting that a TVT operation would lead to increased pain during sexual intercourse (question 5 in PISQ-12). Rogers et al. [19] expressed concerns that fear of damaging the positive results of the operation when engaging intercourse might be a possible adverse effect for the woman and her partner. Our results show a postoperative improvement in results concerning the partner domain, suggesting that surgery does not have an adverse effect on the partner; however, it must be emphasized that the woman filled out the questionnaire. Also improvement in the question concerning women’s negative emotions during sexual activity (question 9) contradict the idea that they may be afraid sexual activity would harm results of surgery and thus harm sexual function. We agree with Rogers et al. that providing women with sufficient information pre- and postoperatively is highly important in order to avoid unnecessary concerns. The fact that there is no exact correlation between incontinence and sexual dysfunction adds evidence to the fact that sexuality is multidimensional and that dysfunction is multicausal.
This study shows that sexual function does not deteriorate after a TVT operation and that women’s sexual function actually improved over both the short- and long-term. Comparing the short- and the long-term follow-up results shows that improved sexual function can be maintained even though some women become somewhat more incontinent over time.
Abbreviations
- ICIQ-UI-SF:
-
International Consultation on Incontinence Questionnaire-Urinary Incontinence Short Form
- PISQ-12:
-
Pelvic Organ Prolapse Urinary Incontinence Sexual Questionnaire-12
- SUI:
-
Stress urinary incontinence
- TVT:
-
Tension-free vaginal tape
References
Naumann G, Steetskamp J, Meyer M, Laterza R, Skala C, Albrich S, Koelbl H (2013) Changes in sexual function and quality of life after single-incision mid-urethral sling for treatment of female stress urinary incontinence. Eur J Obstet Gynecol Reprod Biol 168(2):231–235
Jha S, Ammenbal M, Metwally M (2012) Impact of incontinence surgery on sexual function: a systematic review and metaanalysis. J Sex Med 9:34–43
Barber MD, Visco AG, Wyman JF, Fantl JA, Bump RC (2002) Sexual function in women with urinary incontinence and pelvic organ prolapse. Obstet Gynecol 99:281–289
Shaw C (2002) A systematic review of the literature on the prevalence of sexual impairment in women with urinary incontinence and the prevalence of urinary leakage during sexual activity. Eur Urol 42:432–440
De Souza A, Dwyer PL, Rosamilia A, Hiscock R, Lim YN, Murray C, Thomas E, Conway C, Schierlitz L (2012) Sexual function following retropubic TVT and transobturator Monarc sling in women with intrinsicsphincter deficiency: a multicentre prospective study. Int Urogynecol J 23:153–158
Yeni E1, Unal D, Verit A, Kafali H, Ciftci H, Gulum M (2003) The effect of tension-free vaginal tape (TVT) procedure on sexual function in women with stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 14(6):390-4. Epub 2003 Nov 25
Maaita M, Bhaumik J, Davies AE (2002) Sexual function after using tension-free vaginal tape for the surgical treatment of genuine stress incontinence. BJU Int 90:540–543
Ulmsten U, Henriksson L, Johnson P, Varhos G (1996) An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J 7:81–86
Rogers RG, Kammerer-Doak D, Villarreal A, Coates K, Qualls C (2001) A new instrument to measure sexual function in women with urinary incontinence or pelvic organ prolapse. Am J Obstet Gynecol 184:552–558
Rogers RG, Coates KW, Kammerer-Doak D, Khalsa S, Qualls C (2003) A short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). Int Urogynecol J Pelvic Floor Dysfunct 14:164–168
Abrams P, Avery K, Gardener N, Donovan J (2006) ICIQ Advisory Board. The International Consultation on Incontinence Modular Questionnaire: www.iciq.net. J Urol 175:1063–1066
Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P (2004) ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn 23:322–330
Glavind K, Larsen T, Lindquist ASI (2014) Sexual function in women before and after tension-free vaginal tape operation for stress urinary incontinence. Acta Obstet Gynecol Scand 93:986–990
Mamik MM, Rogers RG, Qualls CR, Morrow JD (2014) The minimum important difference for the Pelvic Organ Prolapse- Urinary Incontinence Sexual Function Questionnaire. Int Urogynecol J 25:1321–1326
Rogers RG, Rockwood TH, Constantine ML, Thakar R, Kammerer-Doak DN, Pauls RN et al (2013) A new measure of sexual function in women with pelvic floor disorders (PFD): the Pelvic Organ Prolapse/Incontinence Sexual Questionnaire, IUGA-Revised (PISQ-IR). Int Urogynecol J 24(7):1091–1103
Jha S, Moran P, Greenham H, Ford C (2007) Sexual function following surgery for urodynamic stress incontinence. Int Urogynecol J Pelvic Floor Dysfunct 18(8):845–850, Epub 2006 Nov 18
Lemack GE, Zimmern PE (2000) Sexual function after vaginal surgery for stress incontinence: results of a mailed questionnaire. Urology 1;56(2):223–227
Kasyan G, Abramyan K, Popov AA, Gvozdev M, Pushkar D (2014) Mesh-related and intraoperative complications of pelvic organ prolapse repair. Cent Eur J Urol 67(3):296–301
Rogers RG, Kammerer-Doak D, Darrow A, Murray K, Qualls C, Olsen A, Barber M (2006) Does sexual function change after surgery for stress urinary incontinence and/or pelvic organ prolapse? A multicenter prospective study. Am J Obstet Gynecol 195(5):e1-4
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Lindquist, A.S.I., Glavind, K. Long-term follow-up of sexual function in women before and after tension-free vaginal tape operation for stress urinary incontinence. Int Urogynecol J 27, 1571–1576 (2016). https://doi.org/10.1007/s00192-016-3004-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-3004-x