Abstract
Purpose
The aim of this study was to describe the epidemiology of Achilles tendon re-rupture. Secondary aims were to identify factors predisposing to increased Achilles tendon re-rupture risk, at the time of primary Achilles tendon rupture.
Methods
A retrospective review of all patients with primary Achilles tendon rupture and Achilles tendon re-rupture was undertaken. Two separate databases were compiled: the first included all Achilles tendon re-ruptures presenting during the study period and described epidemiology, mechanisms and nature of the re-rupture; the second was a case–control study analysing differences between patients with primary Achilles tendon rupture during the study period, who did, or did not, go on to develop re-rupture, with minimum review period of 1.5 years.
Results
Seven hundred and eighty-three patients (567 males, 216 females) attended with primary Achilles tendon rupture and 48 patients (41 males, 7 females) with Achilles tendon re-rupture. Median time to re-rupture was 98.5 days (IQR 82–122.5), but 8/48 re-ruptures occurred late (range 3 to 50 years) after primary Achilles tendon rupture. Males were affected more commonly (OR = 7.40, 95% CI 0.91–60.15; p = 0.034). Mean Achilles tendon re-rupture incidence was 0.94/100,000/year for all ages and 1.16/100,000/year for adults (≥ 18 years). Age distribution was bimodal for both primary Achilles tendon rupture and re-rupture, peaking in the fifth decade, with secondary peaks in older age. Incidence of re-rupture was higher in less socioeconomically deprived sub-populations (OR = 2.01, 95%CI 1.01–3.97, p = 0.04). The majority of re-ruptures were low-energy injuries. Greater risk of re-rupture was noted for patients with primary rupture aged < 45 years [adjusted odds ratio (aOR) 1.96; p = 0.037] and those treated with traditional cast immobilisation (aOR 2.20; p = 0.050).
Conclusion
The epidemiology of Achilles tendon re-rupture is described and known trends (e.g. male predilection) are confirmed, while other novel findings are described, including incidence of a small but significant number of late re-ruptures, occurring years after the primary injury and an increased incidence of re-rupture in less socioeconomically deprived patients. Younger age and traditional immobilising cast treatment of primary Achilles tendon rupture were independently associated with Achilles tendon re-rupture.
Level of evidence
III.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary Achilles tendon ruptures (ATR) are common soft tissue injuries and their incidence is rising [4, 13, 21]. Achilles tendon re-rupture (ATRR) is a much-feared and widely discussed complication of primary ATR [26, 31, 45]. Despite the significant publicity given to ATRR, the rate of which is widely reported in studies on ATR and whose occurrence has been an outcome measure of multiple randomised studies [19, 23] and meta-analyses [26, 31, 34] in the field, studies detailing the epidemiology of ATRR are lacking. This is in contrast to the epidemiology of primary ATR, which is extensively documented and whose incidence is known to have risen in recent decades [13, 21, 40]. This is surprising, given that ATRR is by far the most frequently reported complication of primary ATR [26, 31, 34] and that it is also known to be associated with poorer patient reported and functional outcomes and lower rates of return to sports [27, 45] than uncomplicated primary ATR, while patients who sustain ATRR are subjected to further treatment that often requires additional surgery and further prolonged periods of rehabilitation [25, 30, 45].
It is unclear which patients with primary ATR are at increased risk of ATRR and only a few studies have attempted to identify risk factors for ATRR [15, 17, 35, 44], with most of these unable to identify any [15, 17, 44]. Despite otherwise similar outcomes [10, 12, 24, 31], surgical repair may result in a small reduction in re-rupture rate, although the relative risk reduction is small and often only identifiable when results from individual studies are pooled into meta-analyses [31] and this potential benefit must be weighed against the risk of potential surgical complications [42]. Although it is believed that modern functional rehabilitation regimes for primary ATR may be associated with lower levels of ATRR than traditional immobilising regimes, the authors of a previous meta-analysis indicated a lack of direct evidence in this regard [26]. Subsequent randomised controlled trials comparing traditional and functional rehabilitation have suggested trends towards higher re-rupture rate with traditional immobilising techniques, but these were not statistically significant [8, 22, 23]. A better understanding of the risk factors for ATRR would allow higher risk patients to be identified and counselled accordingly and any modifiable risk factors identified may present opportunities to reduce the risk of ATRR.
The primary aim of this study was to describe the epidemiology of ATRR. The hypothesis was that males would be more commonly affected than females. The secondary aim of this study was to determine whether it is possible to identify factors that predispose patients to increased risk of ATRR at the time of primary ATR.
Materials and methods
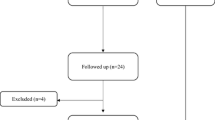
This study was part of a departmentally approved service review of ATR which was reviewed by the scientific officer for the regional ethics committee (REC) who advised that REC review was not necessary. A retrospective electronic search of all health-board medical records was undertaken to identify patients treated for primary ATR and ATRR between 1st January 2011 and 31st December 2016. All records in the health board are electronically recorded and were searched for the following search terms: “Achilles”, “tendoachilles”, “TA”, “rupture”, “tear”, “torn”. The search returned 4521 records. Each was screened according to the inclusion and exclusion criteria (Table 1), leaving 791 patients eligible for inclusion in this study. Records were assessed up to the time of study, with a minimum review period of 1.5 years after primary ATR. The nature and circumstances of primary ATR and ATRR were recorded. ATR was diagnosed clinically, with ultrasound used at the discretion of the treating physician if there was doubt as to the diagnosis. Two separate databases were compiled from this data (Fig. 1): the first, consisting of 791 entries, which included any patient presenting with a rupture (either primary ATR or ATRR) between 2011 and 2016, for the epidemiological study of ATRR; the second database, consisting of 779 entries, included only patients presenting with a primary ATR during the study period and completing treatment for this at the study institution and recorded re-ruptures occurring at any subsequent time point (which thereby permitted analysis of factors that might predict ATRR at the time of presentation with primary ATR), with a minimum review period of 1.5 years from the date of primary injury. Seasonality was defined according to the Northern Hemisphere meteorological system.
Flow diagram for the study. Part 1 consists of 791 acutely presenting ATR, including eight patients whose first presentation during the study period was with a re-rupture and 783 who first presented with a primary ATR. Of these 783, 40 developed a subsequent re-rupture between January 2011 and December 2016. Thus, there were 48 ATRR in total, occurring between January 2011 and December 2016. This data was used for epidemiological descriptions relating to ATRR during the study period and for comparison of presenting features of the 48 identified ATRR with those of primary ATR injuries. Part 2 consists of 779 patients presenting with acute primary ATR between January 2011 and December 2016, who completed treatment for the primary injury at the study institution. In this group, there were 42 patients with ATRR, comprising the 40 patients mentioned previously in part 1 and a further 2 patients who had presented with primary ATR before December 2016, but who developed an ATRR during the review period after 1st January 2017. This data was used to compare variables at primary ATR presentation for patients who did and did not go on to develop ATRR to determine whether any risk factors for ATRR at the time of presentation with primary ATR could be identified
Setting
The health board is the only authority overseeing delivery of regional healthcare services and there are no other National Health Service (NHS) providers in this region. Emergency services are provided through three emergency departments and one minor injuries unit; orthopaedic surgery is performed at two locations and outpatient clinics are based at five locations. There are two private hospitals in the region, but none of these have an emergency department and therefore acute presentations are routed through the NHS and should be securely identified by the search algorithm employed.
Population definitions
The health-board population (total, gender specific and with reference to age brackets) for each year of study was determined using Scottish Government population data from the National Records of Scotland, which issues annual mid-year population estimates for each health board [28]. Socioeconomic deprivation status was determined using the Scottish Index of Multiple Deprivation (SIMD-16), an official Scottish government resource that takes into account employment, income, crime, housing, health, education and access to services to assess and classify population socioeconomic deprivation status (SEDS) across 6,500 data zones nationwide. Each data zone is ranked by SEDS and placed into the appropriate quintile of the national population. SEDS data are published for each data zone and the health-board population serves a geographic region made up of 1083 data zones. Data for these data zones were combined to determine the socioeconomic deprivation status characteristics of the health-board population. SIMD data are published quadrennially, unlike the mid-year population estimates and, therefore, for the socioeconomic deprivation analysis only, the SIMD-16 health-board population data was used to determine the size of more and less deprived components of the health-board population, which were assumed to be static during the period of study. Patients were matched to their corresponding data zone using their postcode, and SEDS data was available for all patients. They were categorised into biquintiles, each comprising patients from data zones in the most deprived 40% and least deprived 40% bands of the national population.
Treatment of ATR
Non-operative management is routinely employed at the study institution unless there are specific indications for surgery (e.g. delayed presentation or patient request), and the period of study straddled a move from traditional immobilising cast treatment (with 10 weeks of cast immobilisation comprising 4 weeks in equinus and 4 weeks in semi-equinus, non-weight bearing, followed by 2 weeks in a neutral, weight-bearing cast and then a further 2 weeks with a shoe heel raise) to a modern functional early weight-bearing regime (with immediate weight bearing in a walking boot orthosis and progressive reduction of heel wedges such that the foot was in neutral position by 6 weeks and the boot removed at 8 weeks) as the standard treatment for primary ATR. Surgical treatment, when performed, was by open means. For the purposes of statistical analysis, treatment type was defined as the first commenced definitive treatment after the initial A&E treatment (A&E management usually comprises an equinus backslab).
Statistical analysis
The annual incidence of ATRR per 100,000 was calculated as the number of cases occurring between 1st January and 31st December, divided by the health-board population (or relevant population bracket), as defined in the government mid-year population estimate for that year. The resulting figure was multiplied by 100,000. The occurrence of ATRR was reported in the most and least socioeconomically deprived national biquintiles (40% bands) in the health-board population, over the period of study, as described above.
Data parametricity in the ATR cohorts was assessed using Kolmogorov–Smirnov testing. Non-parametric data was compared using independent samples Mann–Whitney U tests. Nominal variables were compared using Chi-squared tests (or Fisher’s Exact test if cell count was < 5 in any cell). Binary logistic regression was undertaken to identify variables that were independently associated with ATRR at the time of primary ATR. Variables with a p value of ≤ 0.05 on initial analysis were included in the regression model. The threshold for age used in the regression analysis was determined using a receiver operator characteristic curve to identify the threshold value that predicted ATRR with maximum combined sensitivity and specificity. A p value of ≤ 0.05 was considered significant [6].
Results
Part 1 (primary outcome): epidemiology of re-rupture of the Achilles tendon
Seven hundred and eighty-three patients (567 males, 72.4%; 216 females, 27.6%) residing in the health-board catchment population presented with a primary ATR and 48 patients (41 males, 85.4% and 7 females, 14.6%) with an ATRR between January 2011 and December 2016. Median time between primary ATR and ATRR was 99.5 days (IQR 82.25–130.75), although 8 ATRR (16.7%) occurred late, between 3 and 50 years after the primary injury (Fig. 2). Males (mean 6.83 cases per year, range 2–10; in an average male population of 416,096) were affected more commonly than females (mean 1.17 cases per year, range 0–3; in an average female population of 439,902; p = 0.034 FET; OR = 7.40, 95% CI 0.91–60.15).
Median age at the time of ATRR was 44 years (IQR 33–54) and there was a trend trend towards older age in females (median age 47, IQR 42–66 vs 41, IQR 33–52; p = 0.10). Male preponderance for ATRR was more pronounced than for primary ATR (p = 0.048; OR = 2.23, 95% CI 0.99–5.05).
The mean incidence of ATRR over the study period was 0.94/100,000 per year (range 0.45 to 1.17/100,000 per year) for all ages (Fig. 3) and 1.16/100,000 per year (range 0.56–1.44/100,000 per year) for the adult population (≥ 18 years). This compares to a mean incidence of primary ATR of 15.26/100,000 per year (range 13.51 to 19.07) for all ages and 18.75/100,000 per year (range 16.56–23.57) in adults (≥ 18 years). Peak incidence of both primary ATR and ATRR was in the fifth decade (Fig. 4a, b).
Incidence of ATRR was higher in the least socioeconomically deprived population biquintile (33 cases in a population of 425,254) compared to the most deprived biquintile (11 of 294,239; OR = 2.01, 95% CI 1.01–3.97, p = 0.04). ATRR occurred most frequently in summer (Fig. 5a, b), but there was no statistically demonstrable seasonal variation (p ≥ 0.13; Appendix 1). The majority of ATRR were low-energy injuries and two ATRR (4.2%) occurred while undertaking primary ATR rehabilitation exercises (Table 2).
Treatment of ATRR was surgical in 36 cases (75%), while 5 patients (10.4%) were advised surgical management but declined. Three patients were treated using the casting regime and three with a walking boot regime; one patient was lost to follow-up after radiological confirmation of re-rupture.
A repeat analysis was undertaken, with ATRR defined as re-rupture occurring ≤ 3 years from primary injury (Appendix 2).
Part 2 (secondary outcomes): predictors of re-rupture at the time of first presentation
Patient factors
Males presenting with primary ATR were more likely to sustain ATRR than females (OR = 2.97, 95% CI 1.15–7.66, p < 0.001) and patients who went on to develop ATRR were younger at first presentation than those who did not (p = 0.019); however, there were no other demographic differences (Table 3) or other identifiable patient factors (Table 4).
Mechanism and seasonality of injury
No mechanism (Table 5) or season (Table 6) of primary ATR was shown to be associated with increased risk of ATRR.
Primary ATR treatment
Immobilising cast treatment for primary ATR was associated with increased risk of ATRR (Table 7).
Regression model
Patients sustaining a primary ATR under the age of 45 years and those treated with traditional cast immobilisation were more likely to sustain ATRR (Table 8).
Discussion
This most important finding of this study was the description of the epidemiology of ATRR. Risk factors for ATRR are also described. A male predilection for these injuries was confirmed and the hypothesis accepted. An association with younger age at the time of primary ATR, previously alluded to in a single small study with four re-ruptures [36], was confirmed while other, novel findings were described, including the incidence of a small, but significant number of late ATRR, occurring years after the primary injury and a greater incidence of ATRR in patients with lower levels of socioeconomic deprivation. Mechanisms of injury are contrasted between primary ATR and ATRR. Associations between ATRR risk and male gender, younger age and traditional immobilising cast treatment at the time of primary ATR were observed.
Epidemiological studies of ATRR are lacking, with only one description of population-level incidence noted on literature review, in a study focussing primarily on comparison of patient characteristics between patients who developed either infection or a re-rupture after surgical repair of ATR [33]. This is in contradistinction to the epidemiology of primary ATR, which is widely documented [13, 21, 40]. Previous epidemiological studies have shown that primary ATR occurs more frequently in males [13, 21], but the only report of male predilection to ATRR is based on comparisons of ATRR relative to a primary ATR cohort [35] and there is no population-level data in this regard. This study demonstrated a male predilection both at population level (OR = 7.40) and also relative to primary ATR. Furthermore, age-specific incidence is reported, which, similarly to primary ATR [21], demonstrates a bimodal age-related incidence of ATRR, with peak incidence in the fifth decade of life.
An original finding of the current study was the increased incidence in those with lower levels of socioeconomic deprivation. These findings are the opposite of trends observed for many traumatic injuries [5, 7, 9] and other musculoskeletal [16, 37, 43] and medical [3] conditions, where increasing incidence correlates with increasing levels of socioeconomic deprivation.
ATRR is generally thought to occur early on in the course of rehabilitation, usually within weeks of completing immobilisation [1, 11, 14, 15, 35, 36, 39, 44]. While this study found that the median time to ATRR was 14 weeks after primary injury and that most re-ruptures occurred early, it also found that 1 in 6 ATRR (8 of 48) occurred years after the primary injury, ranging from over 3 years through to 50 years. Studies designed to follow patients prospectively [8, 23, 29] or to retrospectively review patients with primary ATR in recent years [15, 35, 36], would be unable to pick up on this phenomenon and this is probably why it has not been previously recognised. However it has potentially significant implications for studies using re-ruptures as an end point and for patients sustaining an ATR, who should not assume that they are “in the clear” after navigating the early post-injury rehabilitation period uneventfully. It is possible that some authors may consider re-ruptures occurring many years after the primary injury as a new primary injury and we have therefore also presented full epidemiological results defining ATRR as a rupture occurring ≤ 3 years after primary ATR (Appendix 2): similar demographic trends were observed. Further study of ‘late’ ATRR is warranted to determine whether they differ in nature from traditionally described ‘early’ ATRR.
The majority of ATRRs were low-energy injuries, occurring during the course of simple walking, navigating stairs or even spontaneously with no precipitating event. Only two injuries were sustained during rehabilitation exercises. Reito et al. pondered whether the identification of individuals at increased risk of re-rupture would allow for less vigorous rehabilitation to reduce their risk of re-rupture, but ultimately found, in keeping with this study, that most injuries were low-energy injuries and questioned whether less vigorous rehabilitation regimes would have any bearing on these ATRR [35].
To date, only a small number of studies have attempted to identify predictors of ATRR at the time of presentation with a primary ATR [15, 17, 35, 44] and most were unable to identify any risk factors [15, 17, 44]. This may be the result of type II error due to relatively small numbers of ATRR in the studies. Male sex is a well-known risk factor for primary ATR [13, 21], but the nature of any association with ATRR has remained poorly understood—it was found to predict ATRR in patients presenting with a primary ATR in one other study (albeit without correction for confounding factors)[35]. but not in other studies [15, 36, 44]. Part of this disparity is explained by the predisposition of males for primary ATR; which is a pre-requisite for subsequent ATRR, however even within the group of patients with primary ATR, there was a trend towards increased incidence of re-rupture in males, which was just outside statistical significance (p = 0.052), suggesting an additional predisposition to repeat rupture that is independent of that to primary ruptures.
Younger patients presenting with primary ATR were at increased risk of subsequent re-rupture. One other study reported a higher incidence of re-rupture in younger patients, although this was based on a series of only four ATRR, in a selected group of athletes undergoing surgical repair [36]. Another study was unable to demonstrate an association between younger age and overall ATRR risk, despite reporting a younger mean age in patients with ATRR [35]. In the current study, increased odds of ATRR in younger patients were confirmed, even after adjusting for confounding factors.
There was no demonstrable association between season of primary ATR and ATRR risk. This is in contrast to the findings of Saarensilta et al. [38], who reported that patients sustaining primary ATR in summer were more likely to develop ATRR. The reasons for this discrepancy are unknown but may relate to that analysis being based on a small series of five re-ruptures which may therefore be prone to error, or the authors’ decision to use percentages in the place of actual re-rupture numbers in that analysis, thereby increasing the cell counts in the cross table analysis and the apparent statistical power without increasing patient numbers [38].
Re-rupture rate after functional non-operative rehabilitation was 3.8%, which is in keeping with the published literature [26, 31] and it was similar to that for surgically treated cases, while after traditional cast immobilisation, it was 6.7%. It is acknowledged that inclusion of a small number of surgically treated patients may result in some heterogeneity of the group under study, however it appears that our experience reflects that of other units adopting predominantly non-operative management of ATR, where small numbers of patients continue to undergo surgery [1, 11, 14, 44]. No difference was demonstrated between operative and other regimes, although this may be related to the small numbers of surgically treated patients in this study and the relative rarity of ATRR. In fact, the majority of studies similarly show no difference in this regard, although pooling of data in meta-analyses suggests that there is a small clinical difference in re-rupture rates in favour of surgery [31]. This study provides evidence that traditional immobilising cast regimes are associated with higher re-rupture rates, even after adjusting for confounding variables that may influence re-rupture rate and they should therefore be avoided. This is a belief that is widely held among the medical community and is said to have driven recent trends towards functional rehabilitation [26, 41]; however, a previous meta-analysis lamented the paucity of direct evidence in this regard [26]. Surveys have shown that management of ATR often does not follow the evidence base [2] and that plaster cast immobilisation continued to be employed by some practitioners [20], even after the publication of high-quality studies favouring functional rehabilitation [18, 29, 32, 41, 46].
Primary ATR is a pre-requisite for ATRR. Factors that appear to influence incidence of ATRR may therefore be associated directly with ATRR, or mediated indirectly, in part or in full, through a propensity for the primary injury. SEDS appears to be associated with ATRR risk in the general population, but was not found to predict increased re-rupture risk in patients presenting with primary ATR and this effect may therefore be mediated indirectly. Conversely, male sex appears to exert additive risk of re-rupture through direct and indirect means. Furthermore, while some factors that are associated with ATRR are non-modifiable (e.g. younger age at time of primary injury), others (e.g. choice of treatment regime) are potentially modifiable and present opportunities for intervention to reduce patients’ risk of ATRR.
This study does have limitations including its retrospective nature and with this, the possibility of loss to follow-up. Despite being a large series of ATRR, the potential for type II error remains, particularly for less common variables, although this would relate to secondary aims of the study and multiple statistically significant relationships have nonetheless been identified. Furthermore, as with all epidemiological studies, individuals who did not seek medical care for their injuries or were misdiagnosed will have been missed, as may have been others. The strengths of the study design include reporting in two parts with different scope. The first part was able to demonstrate important information about ATRR epidemiology and in particular, late re-ruptures, which would not otherwise be possible. As with all retrospective reviews, a minimum follow-up time had to be defined in the second part of the study, although the minimum 1.5 year threshold chosen is longer than that used in other studies on the topic [15, 35]. Additionally, most patients had a significantly longer review period than the minimum period and data from part 1 suggests that over 80% of ATRR would have occurred within this minimum timeframe. Targeted data collection in this study permitted detailed analysis of all primary ATR and re-ruptures, in contrast to some registry-based studies which are limited to the demographic data collected in the registry and may be unable to differentiate between primary ATR and ATRR [13].
Conclusions
The epidemiology of ATRR is described and the hypothesis confirmed. Other novel findings are described, including incidence of a small but significant number of late ATRR, occurring years after the primary injury and increased incidence of ATRR in less socioeconomically deprived patients. Younger age and traditional immobilising cast treatment of primary ATR were independently associated with ATRR. Traditional immobilising rehabilitation regimes should be avoided to reduce re-rupture risk.
Abbreviations
- ATR:
-
Achilles tendon rupture
- ATRR:
-
Achilles tendon re-rupture
- FET:
-
Fisher’s exact test
- NHS:
-
National Health Service
- REC:
-
Regional ethics committee
- SEDS:
-
Socioeconomic deprivation status
- SIMD:
-
Scottish Index of Multiple Deprivation
References
Aujla RS, Patel S, Jones A, Bhatia M (2019) Non-operative functional treatment for acute Achilles tendon ruptures: the Leicester Achilles Management Protocol (LAMP). Injury 50(4):995–999
Barfod KW, Nielsen F, Helander KN, Mattila VM, Tingby O, Boesen A et al (2013) Treatment of acute Achilles tendon rupture in Scandinavia does not adhere to evidence-based guidelines: a cross-sectional questionnaire-based study of 138 departments. J Foot Ankle Surg 52(5):629–633
Cassell A, Edwards D, Harshfield A, Rhodes K, Brimicombe J, Payne R et al (2018) The epidemiology of multimorbidity in primary care: a retrospective cohort study. Br J Gen Pract 68(669):e245–e251
Clayton RA, Court-Brown CM (2008) The epidemiology of musculoskeletal tendinous and ligamentous injuries. Injury 39(12):1338–1344
Clement ND, McQueen MM, Court-Brown CM (2014) Social deprivation influences the epidemiology and outcome of proximal humeral fractures in adults for a defined urban population of Scotland. Eur J Orthop Surg Traumatol 24(7):1039–1046
Concato J, Hartigan JA (2016) P values: from suggestion to superstition. J Investig Med 64(7):1166–1171
Corfield AR, MacKay DF, Pell JP (2016) Association between trauma and socioeconomic deprivation: a registry-based, Scotland-wide retrospective cohort study of 9,238 patients. Scand J Trauma Resusc Emerg Med 24(1):90
Costa ML, Achten J, Marian IR, Dutton SJ, Lamb SE, Ollivere B et al (2020) Plaster cast versus functional brace for non-surgical treatment of Achilles tendon rupture (UKSTAR): a multicentre randomised controlled trial and economic evaluation. Lancet 395(10222):441–448
Court-Brown CM, Aitken SA, Duckworth AD, Clement ND, McQueen MM (2013) The relationship between social deprivation and the incidence of adult fractures. J Bone Jt Surg Am 95(6):e321–e327
Cramer A, Rahdi E, Hansen MS, Sandholdt H, Holmich P, Barfod KW (2021) No clinically relevant difference between operative and non-operative treatment in tendon elongation measured with the Achilles tendon resting angle (ATRA) 1 year after acute Achilles tendon rupture. Knee Surg Sports Traumatol Arthrosc 29(5):1617–1626
Ecker TM, Bremer AK, Krause FG, Muller T, Weber M (2016) Prospective use of a standardized nonoperative early weightbearing protocol for achilles tendon rupture: 17 years of experience. Am J Sports Med 44(4):1004–1010
Fischer S, Colcuc C, Gramlich Y, Stein T, Abdulazim A et al (2021) Prospective randomized clinical trial of open operative, minimally invasive and conservative treatments of acute Achilles tendon tear. Arch Orthop Trauma Surg 141(5):751–760
Ganestam A, Kallemose T, Troelsen A, Barfod KW (2016) Increasing incidence of acute Achilles tendon rupture and a noticeable decline in surgical treatment from A nationwide registry study of 33,160 patients. Knee Surg Sports Traumatol Arthrosc 24(12):3730–3737
Hutchison AM, Topliss C, Beard D, Evans RM, Williams P (2015) The treatment of a rupture of the Achilles tendon using a dedicated management programme. Bone Jt J 97(4):510–515
Ingvar J, Tagil M, Eneroth M (2005) Nonoperative treatment of Achilles tendon rupture: 196 consecutive patients with a 7% re-rupture rate. Acta Orthop 76(4):597–601
Jenkins PJ, Watts AC, Duckworth AD, McEachan JE (2012) Socioeconomic deprivation and the epidemiology of carpal tunnel syndrome. J Hand Surg Eur 37(2):123–129
Jildeh TR, Okoroha KR, Marshall NE, Abdul-Hak A, Zeni F, Moutzouros V (2018) Infection and rerupture after surgical repair of Achilles tendons. Orthop J Sports Med 6(5):2325967118774302
Kangas J, Pajala A, Ohtonen P, Leppilahti J (2007) Achilles tendon elongation after rupture repair: a randomized comparison of 2 postoperative regimens. Am J Sports Med 35(1):59–64
Kastoft R, Bencke J, Speedtsberg MB, Penny JO, Barfod K (2019) Early weight-bearing in nonoperative treatment of acute Achilles tendon rupture did not influence mid-term outcome: a blinded, randomised controlled trial. Knee Surg Sports Traumatol Arthrosc 27(9):2781–2788
Kearney RS, Parsons N, Underwood M, Costa ML (2015) Achilles tendon rupture rehabilitation: a mixed methods investigation of current practice among orthopaedic surgeons in the United Kingdom. Bone Jt Res 4(4):65–69
Lantto I, Heikkinen J, Flinkkila T, Ohtonen P, Leppilahti J (2015) Epidemiology of Achilles tendon ruptures: increasing incidence over a 33-year period. Scand J Med Sci Sports 25(1):e133–e138
Lu J, Liang X, Ma Q (2019) Early functional rehabilitation for acute achilles tendon ruptures: an update meta-analysis of randomized controlled trials. J Foot Ankle Surg 58(5):938–945
Maempel JF, Clement ND, Duckworth AD, Keenan OJF, White TO, Biant LC (2020) A randomized controlled trial comparing traditional plaster cast rehabilitation with functional walking boot rehabilitation for acute achilles tendon ruptures. Am J Sports Med 48(11):2755–2764
Maempel JF, Clement ND, Wickramasinghe NR, Duckworth AD, Keating JF (2020) Operative repair of acute Achilles tendon rupture does not give superior patient-reported outcomes to nonoperative management. Bone Jt J 102(7):933–940
Maffulli N, Oliva F (2020) Achilles tendon re-rupture. Knee Surg Sports Traumatol Arthrosc 28(5):1673–1674
Mark-Christensen T, Troelsen A, Kallemose T, Barfod KW (2016) Functional rehabilitation of patients with acute Achilles tendon rupture: a meta-analysis of current evidence. Knee Surg Sports Traumatol Arthrosc 24(6):1852–1859
Metz R, van der Heijden GJ, Verleisdonk EJ, Andrlik M, van der Werken C (2011) Persistent disability despite sufficient calf muscle strength after rerupture of surgically treated acute achilles tendon ruptures. Foot Ankle Spec 4(2):77–81
National Records of Scotland (NRS). (2021) Mid-year population estimates for Scotland. https://www.nrscotland.gov.uk/statistics-and-data/statistics/statistics-by-theme/population/population-estimates/mid-year-population-estimates.
Nilsson-Helander K, Silbernagel KG, Thomee R, Faxen E, Olsson N, Eriksson BI et al (2010) Acute achilles tendon rupture: a randomized, controlled study comparing surgical and nonsurgical treatments using validated outcome measures. Am J Sports Med 38(11):2186–2193
Nilsson-Helander K, Sward L, Silbernagel KG, Thomee R, Eriksson BI, Karlsson J (2008) A new surgical method to treat chronic ruptures and reruptures of the Achilles tendon. Knee Surg Sports Traumatol Arthrosc 16(6):614–620
Ochen Y, Beks RB, Van HM, Hietbrink F, Leenen LPH, Vand V et al (2019) Operative treatment versus nonoperative treatment of Achilles tendon ruptures: systematic review and meta-analysis. BMJ 364:5120
Olsson N, Silbernagel KG, Eriksson BI, Sansone M, Brorsson A, Nilsson-Helander K et al (2013) Stable surgical repair with accelerated rehabilitation versus nonsurgical treatment for acute Achilles tendon ruptures: a randomized controlled study. Am J Sports Med 41(12):2867–2876
Pajala A, Kangas J, Ohtonen P, Leppilahti J (2002) Rerupture and deep infection following treatment of total Achilles tendon rupture. J Bone Jt Surg Am 84(11):2016–2021
Reda Y, Farouk A, Abdelmonem I, El Shazly OA (2020) Surgical versus non-surgical treatment for acute Achilles’ tendon rupture. A systematic review of literature and meta-analysis. Foot Ankle Surg 26(3):280–288
Reito A, Logren HL, Ahonen K, Nurmi H, Paloneva J (2018) Risk factors for failed nonoperative treatment and rerupture in acute Achilles tendon rupture. Foot Ankle Int 39(6):694–703
Rettig AC, Liotta FJ, Klootwyk TE, Porter DA, Mieling P (2005) Potential risk of rerupture in primary achilles tendon repair in athletes younger than 30 years of age. Am J Sports Med 33(1):119–123
Reyes C, Garcia-Gil M, Elorza JM, Mendez-Boo L, Hermosilla E, Javaid MK et al (2015) Socio-economic status and the risk of developing hand, hip or knee osteoarthritis: a region-wide ecological study. Osteoarthr Cartil 23(8):1323–1329
Saarensilta IA, Edman G, Ackermann PW (2020) Achilles tendon ruptures during summer show the lowest incidence, but exhibit an increased risk of re-rupture. Knee Surg Sports Traumatol Arthrosc 28(12):3978–3986
Scott WN, Inglis AE, Sculco TP (1979) Surgical treatment of reruptures of the tendoachilles following nonsurgical treatment. Clin Orthop Relat Res 140:175–177
Sheth U, Wasserstein D, Jenkinson R, Moineddin R, Kreder H, Jaglal SB (2017) The epidemiology and trends in management of acute Achilles tendon ruptures in Ontario, Canada: a population-based study of 27 607 patients. Bone Jt J 99(1):78–86
Soroceanu A, Sidhwa F, Aarabi S, Kaufman A, Glazebrook M (2012) Surgical versus nonsurgical treatment of acute Achilles tendon rupture: a meta-analysis of randomized trials. J Bone Jt Surg Am 94(23):2136–2143
Stavenuiter XJR, Lubberts B, Prince RM III, Johnson AH, DiGiovanni CW, Guss D (2019) Postoperative complications following repair of acute achilles tendon Rupture. Foot Ankle Int 40(6):679–686
Urwin M, Symmons D, Allison T, Brammah T, Busby H, Roxby M et al (1998) Estimating the burden of musculoskeletal disorders in the community: the comparative prevalence of symptoms at different anatomical sites, and the relation to social deprivation. Ann Rheum Dis 57(11):649–655
Wallace RG, Heyes GJ, Michael AL (2011) The non-operative functional management of patients with a rupture of the tendo Achillis leads to low rates of re-rupture. J Bone Jt Surg Br 93(10):1362–1366
Westin O, Nilsson HK, Gravare SK, Samuelsson K, Brorsson A, Karlsson J (2018) Patients with an Achilles tendon re-rupture have long-term functional deficits and worse patient-reported outcome than primary ruptures. Knee Surg Sports Traumatol Arthrosc 26(10):3063–3072
Willits K, Amendola A, Bryant D, Mohtadi NG, Giffin JR, Fowler P et al (2010) Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation. J Bone Joint Surg Am 92(17):2767–2775
Funding
None received.
Author information
Authors and Affiliations
Contributions
JM—concept/idea for study, data collection, review and statistical analysis, drafting of manuscript and editing of manuscript; TOW—guidance with initial study design and with manuscript; SPM—data collection, manuscript editing; CMcC—data collection, manuscript editing; NDC—guidance with study design, assistance with statistical analysis and editing of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
This study was part of a departmentally approved service review of ATR which was reviewed by the scientific officer for the regional ethics committee (REC) who advised that REC review was not necessary.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix 1
See Table
9.
Appendix 2
For the purposes of this sub-analysis, only patients presenting with a second Achilles tendon rupture within 3 years of their primary rupture (n = 40) were considered to have re-ruptures. All other presenters with ATR (n = 791) were considered to have primary ruptures. The median time between primary ATR and ATRR was 92.5 days (IQR 82–106). Males (mean 6 cases per year, range 2–9; in an average male population of 416,096) were affected more commonly than females (mean 0.67 cases per year, range 0–3; in an average female population of 439,902; p = 0.063 FET; OR = 6.34, 95% CI 0.76–52.69).
Median age at the time of ATRR was 41 years (IQR 33–47). Male preponderance for ATRR was more pronounced than for primary ATR (p = 0.014; OR = 3.43, 95% CI 1.21–9.75). The mean incidence of ATRR over the study period was 0.78/100,000 per year (range 0.34–1.05/100,000 per year) for all ages and 0.96/100,000 per year (range 0.42–1.30/100,000 per year) for the adult population (≥ 18 years). This compares to a mean incidence of primary ATR of 15.41/100,000 per year (range 13.63 to 19.18) for all ages and 19.04/100,000 per year (range 16.86–23.71) in adults (≥ 18 years). Peak incidence of both primary ATR and ATRR was in the fifth decade (Appendix 2, Fig.
6a, b). ****NOTE THE END OF THIS SENTECE...i.e. "6a, b)." should be BEFORE Figure 6, with the beginning of the sentence and not over here***
Incidence of ATRR was higher in the least socioeconomically deprived population biquintile (26 cases in a population of 425,254) compared to the most deprived biquintile (10 of 294,239) but this finding did not reach statistical significance after excluding late re-ruptures (OR = 1.74, 95%CI 0.84–3.60, p = 0.13). ATRR occurred most frequently during the summer, but there was no statistically demonstrable seasonal variation (p ≥ 0.15; Appendix 2, Table ***NOTE that throughout this section, as above with figure 6, the end of the sentence linking to the appropriate figure or table has been separated and inserted after the relevant figure or table.***
10). The majority of ATRR were low-energy injuries and two ATRR (5%) occurred while undertaking primary ATR rehabilitation exercises (Appendix 2, Table
11).
Rights and permissions
About this article
Cite this article
Maempel, J.F., White, T.O., Mackenzie, S.P. et al. The epidemiology of Achilles tendon re-rupture and associated risk factors: male gender, younger age and traditional immobilising rehabilitation are risk factors. Knee Surg Sports Traumatol Arthrosc 30, 2457–2469 (2022). https://doi.org/10.1007/s00167-021-06824-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06824-0