Abstract
Purpose
Arthroscopically assisted acromioclavicular joint (ACJ) stabilization techniques use bone tunnels in the clavicle and coracoid process. The tunnel size has been shown to have an impact on the fracture risk of clavicle and coracoid. The aim of the present study was to radiographically evaluate the alterations of the clavicular tunnel size in the early post-operative period. It was hypothesized that there would be a significant increase of tunnel size.
Methods
Twenty consecutive patients with acute high-grade ACJ (Rockwood type IV–V) injury underwent arthroscopic-assisted ACJ stabilization. The median age of the patients was 40 (26–66) years. For all patients, a single tunnel button–tape construct was used along with an additional ACJ tape cerclage. Radiologic measurements were undertaken on standardized Zanca films at two separate time points, immediate post-operative examination (IPO) and at late post-operative examination (> 4 months; LPO). The LPO radiographs were taken at a median follow-up period of 4.5 (3–6) months. Clavicular tunnel width (CT) and coracoclavicular distance (CCD) were measured using digital calipers by two independent examiners and the results are presented as median, range, and percentage.
Results
The median CCD increased significantly from 9.5 (8–13) mm at IPO to 12 (7–20) mm at LPO (p < 0.05). Median tunnel size showed significant difference from 3 (3–4) mm at IPO to 5 (4–7) mm at LPO (p < 0.05). Despite a significant increase of 2 mm (66.6%) of the initial tunnel size, there was no correlation between tunnel widening and loss of reduction.
Conclusion
Arthroscopic ACJ stabilization with the use of bone tunnels led to a significant increase of clavicular tunnel size in the early post-operative period. This phenomenon carries a higher fracture risk, especially in high-impact athletes, which needs to be considered preoperatively.
Level of evidence
IV
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acromioclavicular joint (ACJ) injuries frequently occur in the young athletic population or high-energy trauma cohorts. It accounts for 8% of all joint dislocations and has an incidence of 9.2 injuries per 1000 person-years in young athletes [29]. The Rockwood classification is widely used to grade the severity of injury [30] and provide guidance regarding the treatment plan. Surgical management is recommended for patients with high-grade injury (Rockwood type IV–VI) [22].
Evolution of arthroscopic techniques in joint surgery and advances in implant designs have made arthroscopic-assisted ACJ stabilization an increasingly popular method for surgical management of acute high-grade ACJ injuries [5, 8, 37]. It predominantly carries advantages over other surgical methods in terms of a minimally invasive approach, facilitating management of associated intraarticular lesions, good visualization of the coracoid and retaining the implant rendering a secondary surgery unnecessary [4, 8, 31, 32].
The overall principle of arthroscopic-assisted stabilization in acute ACJ injury is to use an internal bracing that provides reduction of the AC joint during the healing process of the CC and AC ligaments. Though this method is widely used, there is a lack of evidence about the ideal “golden standard” technique [4,5,6]. For internal bracing with a suture button fixation device, bone tunnels within the coracoid and the clavicle are used [8, 26, 39]. However, biomechanical studies have shown that the number and size of these tunnels have an impact on fracture risk of the clavicle and/or coracoid [6, 24, 25, 27, 35]. It has been reported that a proportion of patients undergoing these techniques has developed progressive tunnel widening that can contribute towards increasing the risk of fractures post operatively [2, 5, 34, 40, 41]. Since this phenomenon has not been the focus of investigation yet, the aim of the present study was to radiographically evaluate alterations of the clavicular tunnel size in the early postoperative period and to evaluate the association between tunnel widening and loss of reduction. It was hypothesized that there would be a significant increase of tunnel size post operatively.
Materials and methods
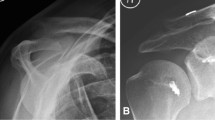
This study was conducted from June 2017 to December 2017. Due to the limited study duration, all the 20 patients who presented with acute high-grade ACJ injury (Rockwood type IV–V) and underwent arthroscopic-assisted ACJ stabilization were included in the present study. For all patients, a single tunnel (ST) button–tape construct was used supplemented with an additional ACJ tape–cerclage. Radiologic measurements were made on standardized Zanca (AP) films at two separate time points, immediate post-operative examination (IPO) and late post-operative examination (> 3 months; LPO). Clavicular tunnel (CT) width and coracoclavicular distance (CCD) were measured using digital calipers of a digital archiving system (MediDoc) (Fig. 1) with measurement accuracy of 1 mm. CT width was measured at its widest point, whilst the CCD was measured from the highest point of the coracoid’s convex surface to the lower margin of the clavicle at a 90° angle. Two surgeons independently measured each CT width and CCD twice for reliability testing. IRB was obtained from Klinikum rechts der Isar, Technical University of Munich, Germany with the number 233/14.
Zanca view of acromioclavicular joint with sample of measurements at immediate post-operative period (IPO) and late post-operative period (LPO). a IPO image showing with 3 mm clavicular tunnel size and coracoclavicular distance of 9 mm. b LPO image done at 4 months post stabilization. Clavicular tunnel widening to 6 mm and CCD measurement of 12 mm
Surgical technique
The surgical technique used for all patients was a single tunnel (ST) double button–tape construct with an additional ACJ tape–cerclage to improve horizontal stability. All surgeries were performed under general anesthesia complemented with interscalene block in a standard beach-chair position by two shoulder specialists (FM, MT). Initial glenohumeral diagnostic arthroscopy through a standard posterior portal was carried out and associated intraarticular pathologies were documented and addressed accordingly. Next, the base of coracoid was identified by opening the rotator interval using a radio frequency ablation device through an anterolateral working portal. Visualization was facilitated by changing the scope to a lateral viewing portal. The coracoid process was skeletonized to clearly identify its medial and lateral borders along with the base. A 2 cm longitudinal incision was made over the clavicular insertion of the CC ligaments. Usage of a drill guide and a 2.4 mm cannulated drill, a trans-clavicular and trans-coracoidal tunnel was created under direct visualization with the scope in the subcoracoid space, while the reduction was maintained manually. The implant was passed in a retrograde manner and the cortical button device positioned well-centered under the base of coracoid. A second button was used over the clavicle and the two high-strength suture tapes (Dog Bone; Fiber Tape; Arthrex, Naples, FL) were tightened and secured with seven half-hitches, while the reduction was confirmed by an image intensifier. Then, one limb of the tape was passed through two extra tunnels within the anterior acromion and knotted back to the remaining sutures thus providing a cerclage crossing over the ACJ, improving horizontal stabilization.
Post-operative rehabilitation: for the first 6 weeks, the shoulder joint was immobilized with a sling, allowing only elbow and wrist range of motion exercise. Gradual passive- and active-assisted movements started 2 weeks after surgery and the strengthening program started 12 weeks after surgery.
Statistical analysis
Statistical analysis was performed with SPSS 19.0 software (IBM Corp, Ehningen, Germany). The level of significance was set at p < 0.05. Differences of immediate post-operative and late post-operative nonparametric metrical data were analyzed using the Wilcoxon signed-rank test. A post hoc power analysis for Wilcoxon signed-ranked tests (matched pairs), with α 0.05, sample size 20, and effect sizes for coracoclavicular distance (CCD) d = 1.167 (r = 0.504), and for clavicular tunnel width (CT) d = 1.496 (r = 0.5041) showed power (1 − β) 0.99, and 1, respectively.
Results
All patients were males with a median age of 40 (26–66) years at the time of surgery. Median coracoclavicular displacement was 20 (range 15–25) mm at the time of diagnosis. The LPO radiographs were taken at a median follow-up period of 4.5 (range 3–6) months. The median CCD measured at IPO and LPO was 9.5 (8–13) mm and 12 (7–20) mm, respectively, representing a significant difference (p < 0.05). The median loss of reduction regarding the CCD measured at IPO and LPO was 2.5 mm. Mean tunnel size was 3 (3–4) mm at IPO and 5 (4–7) mm at LPO, again representing a significant difference (p < 0.05). Overall, a significant increase of 2 mm (66.6%) of the initial tunnel size was observed and this widening occurred in 18 cases (90%) with the median widening measuring 2 (0–4) mm. Tunnel widening did not seem to correlate with loss of reduction (n.s). Twelve (60.0%) patients with 2 mm loss of reduction or less showed a median tunnel widening of 2 (0–4) mm while six (40%) patients with more than 2 mm showed a median tunnel widening of 1.9 (0–3) mm (non-significant difference).
Discussion
The most important finding of the present study was that the hypothesis about a possible tunnel widening after arthroscopically assisted AC joint stabilization was confirmed. Additionally, this tunnel widening did not correlate with the investigated loss of reduction.
The arthroscopic-assisted ACJ stabilization is an accepted operative management in acute high-grade ACJ injury [1, 5, 12, 21]. Anatomic reconstruction utilizing suspensory systems predominantly use high-tensile suture material or synthetic graft in surgical management of acute ACJ instability. Most of these modern techniques use drilling of transosseous tunnels through the distal clavicle and coracoid for stabilization with suture button devices [10, 13, 43].
Several variations of these technique do exist, especially differing by the number of tunnels (single or double) or usage of additional ACJ cerclages to provide horizontal stability [3, 8, 18, 39]. While good clinical results have been shown, [12, 13, 31, 32] other studies have highlighted characteristic complications unique to this technique such as risk for fractures of the clavicle and coracoid [11, 17, 23, 25].
Apart from tunnel widening, the data from the present study showed a significant amount of re-dislocation regarding the CC distance in the early post-operative phase, which has been described as the most common complication before [44]. Shin et al. reported a loss of reduction following arthroscopic coracoclavicular reconstruction using a single tunnel in 33% of their patients, despite showing satisfactory clinical outcomes [33]. The authors recommend an alternative to address this problem with double tunnel technique to reconstruct conoid and trapezoid ligament independently to provide stronger vertical stability [14, 33]. Nonetheless, Gerhardt et al. also demonstrated loss of reduction (mean 3.6 mm) with favourable clinical results in their cohort with double tunnel technique [16, 20]. In a retrospective study, Sun et al. reported, tunnel location, button placement, and osteoporosis, as risk factors for the loss of reduction [36].
Gowd et al. [17] reported fracture complications of 5.7% form an overall pooled complication rate of 14.2% in a review and attributed the complication to the technique and specific construct used [17, 45]. Martetschläger et al. also investigated the complications following the modern reconstructive techniques for ACJ stabilization. They found a 5.5% risk to sustain fracture complication with the use of transclavicular–transcoracoid bone tunnels [24].
Thangaraju et al. recently reported on several cases of fracture complications following arthroscopically assisted ACJ reconstruction. In all cases, a widening of the bone tunnels was observed with the fracture lines running through the tunnel. This was even more interesting since the fracture complications occurred in the late post-operative phase, suggesting the fracture risk to be a persistent problem since the non-absorbing suture implants remain in place [38].
In the lab, it has been shown that fracture risk depends on the number and size of the bone tunnels. Single tunnel and smaller tunnel size have significantly lower risk compared to double tunnel and larger tunnel size (> 2.4 mm) [7, 8]. Considering these facts, a post-operative widening of the bone tunnels that has been described for AC joint graft reconstruction [2, 12, 34, 38, 40, 46] might significantly increase fracture risk over time. Therefore, in the present study, the clavicular tunnel morphology has been observed in the early post-operative phase to detect quality and quantity of a possible tunnel alteration. Besides, it can be a factor for loss of reduction.
In a retrospective review, Cook et al. used the GraftRope (Arthrex Inc., Naples, FL) in 10 patients and reported loss of reduction to be as high as 50% and an unexpected finding of tunnel widening. There was 60% increase in the size of clavicle tunnels (initial diameter of 6 mm to an average increase to 9.6 mm). This was suggested to be caused by motion at the graft–bone interface. However, they did not correlate the tunnel widening with loss of reduction [12]. Similarly, in a case report of coracoclavicular ligament reconstruction with semitendinosus tendon, Yoo et al. postulated a mechanical theory for tunnel widening based on findings from ACL surgery. Constant multiplane motion occurring at the ACJ contributes to more motion of the graft within the tunnel that leads to a windshield-wiper or bungee-cord effect as occurring in ACL surgeries with hamstring graft increased tunnel width. The widening was noticed retrospectively as early as 3 months after the surgery. However, the patient showed good clinical outcomes and had maintained reduction despite this phenomenon at more than 2 years of follow-up [46]. In a prospective study reporting early failure of coracoclavicular ligament reconstruction using TightRope and GraftRope (Arthrex Inc., Naples, FL), Singh et al. have documented tunnel widening in most of their nine patients. They attribute this to the anatomic and biomechanical forces acting of ACJ during shoulder movement leading to ‘windshield-wiper’ micromotion and suggested in-vivo studies to support this theory [34]. In their study, Virtanen et al. concluded that lateral clavicle osteolysis and tunnel widening are a common occurrence and may influence the results of treatment of chronic acromioclavicular joint dislocation with autogenous tendon grafts that was stabilized with tenodesis screws [40]. Baran et al. demonstrated clavicle tunnel widening in all their patients undergoing open anatomic coracoclavicular reconstruction using hamstring allograft with high-strength suture augmentation and knotted graft fixation without interference screws [2].
The results of the present study showed that 18 patients (90%) among the patients after arthroscopically assisted AC joint stabilization showed clavicular tunnel widening. The use of cortical button and highstrength suture (Dog Bone; Fiber Tape; Arthrex, Naples, FL) using a single tunnel technique resulted in a median 2 mm (66.6%) increase of tunnel width. These changes already occurred at median follow-up period of 4.5 months after surgery.
Hence, it is speculated that the ACJ micromotion contributing to tunnel widening is time dependent. Theoretically, the micromotion is most at the initial period after stabilization surgery, which gradually reduces as healing of the native CC ligaments occur.
The drilling of the bone tunnels itself might also contribute to early tunnel widening of the tunnels which might lead to heatinduced bone necrosis following osteolysis [7, 9]. Another possibility that can be attributed to widening is the direction of the tunnel created [36]. Eccentric drilling of the bone can lead to an oblique tunnel which can further lead to abrasion by the vertical suture that contributes to a widened tunnel [15, 42]. In cadaveric model testing suture materials in repetitive rotatory motion of reconstructed ACJ, Kipple et al. conferred that relative motion between the bone and suture material resulted in a sawing motion to cause preferential wear and raised the need to consider associated abrasive properties of high-tensile suture material [19].
The use of sharp drills, continuous irrigation to dampen the heat produced along with perpendicular drill position is paramount in reducing the possibility on initial tunnel widening. To our knowledge, this is the first study directly focusing on bone tunnel alteration after a single tunnel AC joint stabilization with additional AC cerclage emphasizing this phenomenon to occur with high-tensile sutures as well. It was thought that widening might be another risk factor for loss of reduction, nevertheless, it was not confirmed by this investigation.
Several limitations of the present study need to be mentioned. Since a retrospective study was performed, the late post-operative radiographies do vary and are not consistently taken at exactly 3 months post operatively. However, the alterations within the first month after surgery could be shown, which was the goal of the study. As for all studies using radiographic measurement, possible measure variances due to projection of the radiographs are possible, which need to be mentioned as further limitation. However, all patients have been checked for consistent projection and correct radiographs before inclusion. Furthermore, since a simple measurement of the clavicular bone tunnels was performed with a digital ruler, no previous validation study was performed, but the inter-rater reliability was calculated to provide reliable data. Since this study was of preliminary in nature, all the LPO measurements of tunnel size, regardless of the time points were grouped into one category to give an overall assessment of bone tunnel size in arthroscopic-assisted acute ACJ stabilization surgery. However, a second study including larger sample size is deemed necessary to better understand the phenomenon of tunnel widening and its clinical impact. Especially, additional investigations are necessary to compare tunnel alteration in single and double tunnel techniques and to study the long-term characteristic changes since most of the implants are not removed and consist of non-absorbable suture material. Despite the mentioned limitations, this study reliably demonstrated the existence of a tunnel widening phenomenon even in the early post-operative period. This information should be taken into consideration by clinicians when creating transosseous tunnels in managing acute ACJ injuries.
The occurrence of tunnel widening and a possible fracture risk was highlighted during informed consent procedure in our current clinical practice. Furthermore, different surgical techniques that do not use tunnels are discussed for high-risk individuals such as contact athletes.
Conclusion
Arthroscopic ACJ stabilization with the use of bone tunnels leads to a significant increase of the clavicular tunnel size in the early post-operative period. This phenomenon carries a higher fracture risk, especially in high-impact athletes which needs to be considered preoperatively.
References
Balke M (2017) Diagnosis and treatment of acute acromioclavicular joint injuries. Arch Trauma Res 2017:1–7
Baran S, Belisle JG, Granger EK, Tashjian RZ (2018) Functional and radiographic outcomes after allograft anatomic coracoclavicular ligament reconstruction. J Orthop Trauma 32(4):204–210
Barth J, Duparc F, Andrieu K, Duport M, Toussaint B, Bertiaux S et al (2015) French Society of Arthroscopy. Is coracoclavicular stabilisation alone sufficient for the endoscopic treatment of severe acromioclavicular joint dislocation (Rockwood types III, IV, and V). Orthop Traumatol Surg Res 101(8 Suppl):S297–303
Baumgarten KM, Altchek DW, Cordasco FA (2006) Arthroscopically assisted acromioclavicular joint reconstruction. Arthroscopy 22(2):2281e1–3228
Beitzel K, Cote MP, Apostolakos J, Solovyova O, Judson CH, Ziegler CG et al (2013) Current concepts in the treatment of acromioclavicular joint dislocations. Arthroscopy 29(2):387–397
Beitzel K, Obopilwe E, Chowaniec DM, Niver GE, Nowak MD, Hanypsiak BT et al (2011) Biomechanical comparison of arthroscopic repairs for acromioclavicular joint instability: suture button systems without biological augmentation. Am J Sports Med 39(10):2218–2225
Bhullar R, Habib A, Zhang K, de Sa D, Horner NS, Duong A et al (2019) Tunnel osteolysis post-ACL reconstruction: a systematic review examining select diagnostic modalities, treatment options and rehabilitation protocols. Knee Surg Sports Traumatol Arthrosc 27(2):524–533
Braun S, Beitzel K, Buchmann S, Imhoff AB (2015) Arthroscopically assisted treatment of acute dislocations of the acromioclavicular joint. Arthrosc Tech 4(6):e681–e685
Chen YC, Tu YK, Tsai YJ, Tsai YS, Yen CY, Yang SC et al (2018) Assessment of thermal necrosis risk regions for different bone qualities as a function of drilling parameters. Comput Methods Programs Biomed 162:253–261
Chernchujit B, Tischer T, Imhoff AB (2006) Arthroscopic reconstruction of the acromioclavicular joint disruption: surgical technique and preliminary results. Arch Orthop Trauma Surg 126(9):575–581
Clavert P, Meyer A, Boyer P, Gastaud O, Barth J, Duparc F, SFA (2015) Complication rates and types of failure after arthroscopic acute acromioclavicular dislocation fixation. Prospective multicentre study of 116 cases. Orthop Traumatol Surg Res 101(8 Suppl):S313–316
Cook JB, Shaha JS, Rowles DJ, Bottoni CR, Shaha SH, Tokish JM (2012) Early failures with single clavicular transosseous coracoclavicular ligament reconstruction. J Shoulder Elbow Surg 21(12):1746–1752
DeBerardino TM, Pensak MJ, Ferreira J, Mazzocca AD (2010) Arthroscopic stabilization of acromioclavicular joint dislocation using the AC graftrope system. J Shoulder Elbow Surg 19:47–52
El Sallakh SA (2012) Evaluation of arthroscopic stabilization of acute acromioclavicular joint dislocation using the Tight-Rope system. Orthopedics 35:e18–e22
Fauno P, Kaalund S (2005) Tunnel widening after hamstring anterior cruciate ligament reconstruction is influenced by the type of graft fixation used: a prospective randomized study. Arthroscopy 21(11):1337–1341
Gerhardt C, Kraus N, Pauly S, Scheibel M (2013) Arthroscopically assisted stabilization of acute injury to the acromioclavicular joint with the double TightRope™ technique: one-year results. Unfallchirurg 116(2):125–130
Gowd AK, Liu JN, Cabarcas BC, Cvetanovich GL, Garcia GH, Manderle BJ et al (2018) Current concepts in the operative management of acromioclavicular dislocations: a systematic review and meta-analysis of operative techniques. Am J Sports Med 2018:1–15
Hou Z, Graham J, Zhang Y, Strohecker K, Feldmann D, Bowen TR et al (2014) Comparison of single and two-tunnel techniques during open treatment of acromioclavicular joint disruption. BMC Surg 14(53):1–7
Kippe MA, Demetropoulos CK, Baker KC, Jurist KA, Guettler JH (2009) Failure of coracoclavicular artificial graft reconstructions from repetitive rotation. Arthroscopy 25(9):975–982
Kraus N, Haas NP, Scheibel M, Gerhardt C (2013) Arthroscopically assisted stabilization of acute high-grade acromioclavicular joint separations in a coracoclavicular Double-Tight Rope technique: V-shaped versus parallel drill hole orientation. Arch Orthop Trauma Surg 133(10):1431–1440
Lee S, Bedi A (2016) Shoulder acromioclavicular joint reconstruction options and outcomes. Curr Rev Musculoskelet Med 9(4):368–377
Li X, Ma R, Bedi A et al (2014) Management of acromioclavicular joint injuries. J Bone Jt Surg Am 96(1):73–84
Lim TK, Oh WK (2019) Intraoperative and postoperative complications after arthroscopic coracoclavicular stabilization. Clin Orthop Surg 11(1):103–111
Martetschläger F, Horan MP, Warth RJ, Millett PJ (2013) Complications after anatomic fixation and reconstruction of the coracoclavicular ligaments. Am J Sports Med 41(12):2896–2903
Martetschläger F, Saier T, Weigert A, Herbst E, Winkler M, Henschel J et al (2016) Effect of coracoid drilling for acromioclavicular joint reconstruction techniques on coracoid fracture risk: a biomechanical study. Arthroscopy 32(6):982–987
Martetschläger F, Tauber M, Habermeyer P, Hawi N (2016) Arthroscopically assisted acromioclavicular and coracoclavicular ligament reconstruction for chronic acromioclavicular joint instability. Arthrosc Tech 5(6):e1239–e1246
Milewski MD, Tompkins M, Giugale JM, Carson EW, Miller MD, Diduch DR (2012) Complications related to anatomic reconstruction of the coracoclavicular ligaments. Am J Sports Med 40(7):1628–1634
Millett PJ, Horan MP, Warth RJ (2015) Two-year outcomes after primary anatomic coracoclavicular ligament reconstruction. Arthroscopy 31(10):1962–1973
Pallis M, Cameron KL, Svoboda SJ, Owens BD (2012) Epidemiology of acromioclavicular joint injury in young athletes. Am J Sports Med 40:2072–2077
Rockwood CJ, Williams G, Young D (2004) Disorders of the acromioclavicular joint. In: Rockwood CA, Matsen FA, Wirth MA, Lippitt SB (eds) The shoulder, 3rd edn. WB Saunders, Philadelphia, pp 521–595
Salzmann GM, Walz L, Buchmann S, Glabgly P, Venjakob A, Imhoff AB (2010) Arthroscopically assisted 2-bundle anatomical reduction of acute acromioclavicular joint separations. Am J Sports Med 38(6):1179–1187
Scheibel M, Dröschel S, Gerhardt C, Kraus N (2011) Arthroscopically assisted stabilization of acute high-grade acromioclavicular joint separations. Am J Sports Med 39(7):1507–1516
Shin SJ, Kim NK (2015) Complications after arthroscopic coracoclavicular reconstruction using a single adjustable-loop-length suspensory fixation device in acute acromioclavicular joint dislocation. Arthroscopy 31(5):816–824
Singh B, Mohanlal P, Bawale R (2016) Early failure of coracoclavicular ligament reconstruction using TightRope system. Acta Orthop Belg 82(1):119–123
Spiegl UJ, Smith SD, Euler SA, Dornan GJ, Millett PJ, Wijdicks CA (2014) Biomechanical consequences of coracoclavicular reconstruction techniques on clavicle strength. Am J Sports Med 42(7):1724–1730
Sun LJ, Lu D, Tao ZY, Yu XB, Hu W, Ma YF et al (2019) Analysis of risk factors for loss of reduction after acromioclavicular joint dislocation treated with the suture-button. J Orthop Sci 1:4. https://doi.org/10.1016/j.jos.2019.01.014
Tauber M (2013) Management of acute acromioclavicular joint dislocations: current concepts. Arch Orthop Trauma Surg 133(7):985–995
Thangaraju S, Tauber M, Habermeyer P, Martetschläger F (2019) Clavicle and coracoid process periprosthetic fractures as late post-operative complications in arthroscopically assisted acromioclavicular joint stabilization. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05482-7
Venjakob AJ, Salzmann GM, Gabel F, Buchmann S, Walz L, Spang JT et al (2013) Arthroscopically assisted 2-bundle anatomic reduction of acute acromioclavicular joint separations: 58-month findings. Am J Sports Med 41(3):615–621
Virtanen KJ, Savolainen V, Tulikoura I, Remes V, Haapamäki V, Pajarinen J et al (2014) Surgical treatment of chronic acromioclavicular joint dislocation with autogenous tendon grafts. Springerplus 3(420):1–8
Voss A, Beitzel K, Alaee F, Dukas A, Herbst E, Obopilwe E et al (2016) A Biomechanical analysis of different clavicular tunnel diameters in anatomic acromioclavicular ligament reconstruction. Arthroscopy 32(8):1551–1557
Wellmann M, Zantop T, Petersen W (2007) Minimally invasive coracoclavicular ligament augmentation with a flip button/polydioxanone repair for treatment of total acromioclavicular joint dislocation. Arthroscopy 23(10):1132.e1–5
Wolf EM, Pennington WT (2001) Arthroscopic reconstruction for acromioclavicular joint dislocation. Arthroscopy 17(5):558–563
Woodmass JM, Esposito JG, Ono Y, Nelson AA, Boorman RS, Thornton GM et al (2015) Complications following arthroscopic fixation of acromioclavicular separations: a systematic review of the literature. Open Access J Sports Med 10(6):97–107
Wylie JD, Johnson JD, DiVenere J, Mazzocca AD (2018) Shoulder acromioclavicular and coracoclavicular ligament injuries: common problems and solutions. Clin Sports Med 37(2):197–207
Yoo JC, Choi NH, Kim SY, Lim TK (2006) Distal clavicle tunnel widening after coracoclavicular ligament reconstruction with semitendinosus tendon: a case report. J Shoulder Elbow Surg 15(2):256–259
Acknowledgements
The first author acknowledges the fellowship provided by the Ministry of Health, Malaysia which enabled the attachment at the ATOS Clinic in Munich.
Funding
No funding was received for the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conlict of interest
The authors declare that there is no conflict of interest.
Ethical approval
Institutional Review Board (IRB) or Ethical Committee approval obtained at Technical University of Munich (number 233/14).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Thangaraju, S., Cepni, S., Magosch, P. et al. Arthroscopically assisted acromioclavicular joint stabilization leads to significant clavicular tunnel widening in the early post-operative period. Knee Surg Sports Traumatol Arthrosc 27, 3821–3826 (2019). https://doi.org/10.1007/s00167-019-05662-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05662-5