Abstract
Aims/hypothesis
Data on trends of end-stage renal disease among people with diabetes are lacking. We analysed the incidence of end-stage renal disease, defined as renal replacement therapy, among people with and without diabetes, and the corresponding relative risk. Moreover, we investigated time trends for the period 2002–2016.
Methods
In this retrospective population-based study we analysed data from one dialysis centre of a region in Germany covering a population of about 310,000 inhabitants. We estimated the age- and sex-standardised incidence rates for chronic renal replacement therapy among adults with and without diabetes and the corresponding relative risks. The time trend was analysed using Poisson regression models.
Results
Between 2002 and 2016, 1107 people (61.2% male; mean age 71.6 years; 48.7% with diabetes) had a first renal replacement therapy. During the study period, the incidence rate in the population with diabetes varied from 93.6 (95% CI 50.4, 136.7) in 2002 to 140.5 (95% CI 80.6, 200.4) in 2016 per 100,000 person-years. In the population without diabetes the incidence rate was substantially lower and reached 17.3 (95% CI 10.9, 23.6) in 2002 and 24.6 (95% CI 17.5, 31.7) in 2009. The relative risk comparing people with and without diabetes was 3.57 (95% CI 3.09, 4.13). No significant change in the incidence rates was found during the observation period, either in the population with or in the population without diabetes, and thus the relative risk also remained constant.
Conclusions/interpretation
People with diabetes have a higher risk of needing renal replacement therapy than those without diabetes, a fact that remained constant over a time period of 15 years.
Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
The increasing prevalence of diabetes mellitus worldwide [1] leads to an increase in the number of people with complications of diabetes, including diabetic nephropathy and its last stage, end-stage renal disease (ESRD) requiring renal replacement therapy (RRT). Among people starting RRT, the proportion of individuals with diabetes (as comorbidity) ranges between 28% [2] and 51% [3]. Individuals with diabetes and ESRD have poorer survival rates than people without diabetes [2, 4,5,6]. Moreover, this group of individuals brings about especially high treatment costs [7, 8]. Nevertheless, there are only a few population-based studies that have analysed the incidence of RRT in the population with diabetes compared with the population without diabetes, in particular where diabetes was taken into account as a comorbidity and not only diabetic nephropathy as a primary kidney disease leading to ESRD [3, 4, 9,10,11]. In our previous study we analysed the incidence of RRT in 2002–2008 in a German region stratified by diabetes status [9]. In this study, no temporal change regarding the incidence of RRT could be detected among people either with or without diabetes. However, the considered time period of this study was quite short. Furthermore, a national guideline was implemented in 2010 in Germany addressing treatment and healthcare of adult individuals with diabetes and renal disease [12]. This may have improved diabetes care in this patient group.
The aims of this study were: (1) to analyse the incidence of RRT among individuals with and without diabetes as well as relative risk (RR) and (2) to investigate the corresponding time trends for the period 2002–2016.
Methods
Study design and data assessment
The data analysed were sourced from one dialysis centre, which delivers dialysis to all inhabitants in a region in North Rhine-Westphalia, Western Germany (district of Mettmann excluding the cities of Ratingen, Monheim and Langenfeld), covering a population of about 310,000 inhabitants. As there is only this one dialysis centre in the region, it was assumed that nearly all individuals with RRT living in this region are treated there. This study was designed as a retrospective population-based study.
Study population
A census-based description of the general population of the study region was obtained from the Federal Office for Statistics [13]. The population with diabetes was estimated in the adult population based on age- (30–59, 60–69, 70–79, ≥80 years) and sex-specific diabetes prevalence from two German nationwide surveys (German Health Interview and Examination Surveys, GNHIES98 and DEGS1) [14,15,16] performed in 1997–1999 and 2008–2011, respectively. In both surveys, diabetes was defined by intake of glucose-lowering medication, by self-report of physician-diagnosed diabetes or by an HbA1c value above 47.5 mmol/mol (6.5%) within the last week before the survey [17]. These two surveys are believed to be the only nationwide data sources with a comparable study design that allow the estimation of age- and sex-specific diabetes prevalence, including undetected diabetes, over more than a decade. Since both surveys were truncated at the age of 80 years, and given findings of previous studies [14], we assumed that diabetes prevalence remained constant among people above 80 years. For the main analysis we assumed that the estimated age- and sex-specific diabetes prevalence increased linearly from 2002 to 2011 and also continued to do so thereafter until 2016. Nevertheless, we repeated the main analysis with constant age- and sex-specific diabetes prevalence during the years 2011–2016 in the sensitivity analysis.
Assessment of people with incident RRT and data assessment
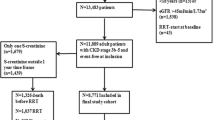
In the present analysis, we examined all people aged at least 30 years at the time of first RRT between January 2002 and December 2016. According to our previous study [9], an incident RRT was defined as the first dialysis or primary kidney or combined pancreas-kidney transplantation due to chronic kidney disease. Individuals with RRT due to typical acute kidney insufficiency due to sepsis and other agents were excluded, as were individuals with transplant failure and individuals from outside of the study region.
Demographic data such as age and sex were available for all people with a first RRT. A person was classified as having diabetes according to a history of diabetes, use of a glucose-lowering agent or having HbA1c ≥ 47.5 mmol/mol (6.5%) at the start of RRT [18]. Likewise, the reason for RRT was determined according to established classifications [19,20,21]. Diabetic nephropathy as a reason for RRT was assumed when an individual had macroalbuminuria or microalbuminuria and diabetic retinopathy, both in the absence of another disease associated with ESRD [22]. Additionally, the type of RRT was documented (i.e. peritoneal dialysis or haemodialysis).
Furthermore, several clinical variables such as GFR (using the Modification of Diet in Renal Disease [MDRD] formula or the Chronic Kidney Disease Epidemiology Collaboration formula [CKD-Epi]), HbA1c value, initial form of RRT, start of dialysis in the clinic (yes vs no), BMI, information regarding type of diabetes and diabetes duration were ascertained.
Moreover, information was obtained regarding the following comorbidities at the start of RRT: hypertension, CHD, congestive heart failure, myocardial infarction, peripheral artery occlusive disease, amputation, stroke, malignant tumour and presence of diabetic retinopathy among individuals with diabetes only.
Statistical analysis
We performed analyses for the population as a whole and separately for men and women. We estimated the number of people with diabetes by multiplying the study population with the estimated diabetes prevalence in each stratum, defined by sex and age (30–59, 60–69, 70–79, ≥80 years). Person-years (PY) were calculated by taking the estimated number of people with and without diabetes for each calendar year. We computed stratum-specific and age- and sex-standardised incidence rates (IRs) of RRT with 95% CIs in the estimated population with and without diabetes for each calendar year, using the German population of 2009 as the standard population. Moreover, we estimated the IR ratio by comparing the population with and without diabetes from the standardised IRs. Furthermore, we computed attributable risk among the population with diabetes and population attributable risk due to diabetes along with 95% CIs in order to describe what proportion of RRT could theoretically be avoided if the exposure (i.e. diabetes) was omitted. Time trends were investigated by first fitting separate Poisson regression models with IR of RRT as the dependent variable for individuals with and without diabetes. Age and year of RRT as linear continuous difference from baseline year 2002 were used as the independent variables. The lowest age group (30–59 years) was used as a reference group. Moreover, we fitted analogous Poisson models for the entire population. The variable ‘presence of diabetes’ (yes vs no) and an interaction term for diabetes and years since 2002 were also included.
Furthermore, we estimated IRs and trends of RRT due only to diabetic nephropathy in the diabetic population.
In order to take over-dispersion of the outcome variable into account, all analyses were conducted with the de-scale adjustment based on cumulated data on the covariate strata. The analysis was computed using the statistical analysis system, SAS (SAS for Windows 7, Release 9.4 TS1M1, SAS Institute, Cary, NC, USA).
Ethics
All participants were asked to provide their written, informed consent for participation when they started RRT. Individuals who declined (less than 1% of all participants) were excluded from the analysis. The study was approved by the local ethics committee.
Results
Study population
The data covered the population aged at least 30 years in the study region (2002: 219,046, 2016: 213,120). Diabetes prevalence in this region increased among men from 11.8% in 2002 to 13.7% in 2016 but remained nearly constant among women (2002: 11.4%, 2016: 11.4%).
There were 1107 people with a first RRT between 2002 and 2016. The baseline characteristics of these people regarding age, sex, clinical variables and comorbidities are shown in Table 1. The majority of the people starting RRT were men (61.2%). The age distribution of people with RRT was similar among people with and without diabetes, with a mean age of 71.6 years at the time of the first RRT. Nevertheless, the mean age increased significantly during the study period from 67.4 years in 2002 to 73.1 years in 2016 (p value linear regression: p < 0.001), with similar increases among all subgroups.
Almost half of all 1107 individuals were classified as having diabetes, with similar proportions among men and women.
The majority of individuals with diabetes had type 2 diabetes (95.6%) and the mean duration of diabetes at the time of the first RRT was 16.9 years, with similar numbers in both sexes. As expected, the mean HbA1c value was significantly higher among people with diabetes than among those without diabetes (HbA1c: 47.7 mmol/mol [6.5%] vs HbA1c: 36.5 mmol/mol [5.5%], p value t test <0.001), with similar values in men and women.
In almost half of the people with diabetes, diabetic nephropathy was the reason for RRT (49.1%). Vascular nephropathy (kidney disease due to hypertension and micro- and macrovascular diseases) was the reason for RRT in about one-third (33.8%). In the population without diabetes, the most common reason for RRT was vascular nephropathy (39.8%). The majority of people who started RRT began with haemodialysis (61.5%) followed by peritoneal dialysis (38.5%), with similar numbers in all subgroups, while only one person underwent transplantation as the first RRT.
The majority of dialyses started in the clinic (78.6%), with similar proportions in all subgroups. The GFR value was significantly higher in men with diabetes than in those without (p value = 0.0012). In women, this difference was not significant (p value = 0.427).
People with diabetes had significantly more comorbidities and higher BMI at the time of first RRT than those without diabetes (p values χ2 test and t test <0.05, respectively), with the exception of malignant tumour, where an inverse association was observed (p value < 0.001). The proportion of comorbidities was higher among men for all comorbidities except diabetic retinopathy.
IR, relative and attributable risk
The age- and sex-standardised IRs of the first RRT are shown in Table 2 and Fig. 1. There were some fluctuations, which were particularly evident in the population with diabetes. During the observation period, the IR in the population with diabetes ranged from 56.2 per 100,000 PY (95% CI 31.1, 81.4) in 2008 to 140.5 per 100,000 PY (95% CI 80.6, 200.4) in 2016, without sex differences. This rate was substantially lower in the population without diabetes, with values between 17.2 (95% CI 11.0, 23.4) in 2002 and 29.5 (95% CI 21.5, 37.5) in 2009. The RR comparing the IRs among the populations with diabetes and without diabetes ranged between 2.5 (95% CI 1.4, 4.4) in 2009 and 6.0 (95% CI 3.3, 10.8) in 2004. In people with diabetes, 78% of the RRT incidence was attributable to diabetes. In the entire population, one-third of the RRT incidence was attributable to diabetes. The IR was twice as high among men compared with women in subpopulations both with and without diabetes.
IR relating only to diabetic nephropathy tended to decrease, with the highest value in 2003 (87.4; 95% CI 42.6, 132.1) and the lowest value in 2010 (32.1; 95% CI 9.7, 54.5), and was about twofold higher among men than among women (see electronic supplementary material [ESM] Table 1, ESM Fig. 1).
Analysis of time trend and other covariates
The results of the incidence trend from the fully adjusted Poisson models are shown in Table 3. The RRs in the population stratified by diabetes status are presented in models 1a and 1b. During the observation period, no change in the IR was observed in the population with diabetes (RR per calendar year, 1.02; 95% CI 0.99, 1.04) for either sex. Likewise, the IR remained nearly constant in the population without diabetes (RR 1.01; 95% CI 0.99, 1.03) both in men and in women. The IR increased substantially with increasing age, with a particularly strong increase in the population without diabetes.
Taking the entire population in model 2, the IR in the population with diabetes was almost fourfold that of the population without diabetes (RR 3.57; 95% CI 3.09, 4.13), with a higher difference among men (RR 4.14; 95% CI 3.39, 5.06). This pattern was particularly strong in the younger population but also persisted in the oldest age group (RR diabetes vs no diabetes <60 years, 12.60; 95% CI 9.04, 17.55; 80+ years: 2.04; 95% CI 1.58, 2.62) (data not shown). The interaction diabetes × calendar year as considered in model 3 was nonsignificant, indicating that the RR between the subpopulations with and without diabetes remained constant in both sexes. Results from the sensitivity analysis assumed that diabetes prevalence remained constant after 2011, meaning that they were similar to those from the main analysis (ESM Tables 2, 3).
When RRT due only to diabetic nephropathy was counted, the IR of RRT significantly decreased in the male population with diabetes (RR per calendar year, 0.96; 95% CI 0.93, 0.997) but not in the female population (RR per calendar year, 0.97; 95% CI 0.93, 1.02) (ESM Table 4).
Discussion
Statement of principal findings
This is one of the few studies analysing the incidence of RRT in the population with diabetes compared with the population without diabetes. This study also evaluated the trend of the incidence of RRT over a time period of 15 years. As expected, the IRs were substantially higher among people with diabetes, with an almost fourfold-increased IR. Men had twice as high a risk of RRT compared with women. The IRs in subpopulations both with and without diabetes and, thus, the corresponding RRs, mainly remained constant throughout the study period, with consistent results in both sexes.
Discussion of important differences in results
A comparison with other studies is very difficult. We found only a few population-based studies analysing age- and sex-standardised IRs among people with and without diabetes. Furthermore, most of the studies investigating the IR of RRT in the population with diabetes only considered diabetic nephropathy as a primary reason for RRT, and not diabetes as a comorbidity.
The IRs among people with diabetes in the current study were somewhat lower than in the previous study in the same study region [9], which included the years 2002–2008: IR 97.9 (95% CI 86.7, 109.1) vs 167 (95% CI 125, 208) per 100,000 PY. This discrepancy is mainly the result of a different methodological approach regarding the estimation of the diabetic population as a population at risk. In the previous study, diabetes prevalence was estimated using the former East German diabetes registry, the data of which are from the late 1980s when prevalence was quite low [23]. In contrast, diabetes prevalence was estimated in the current study using more recent data from nationwide German surveys with a substantially higher diabetes prevalence, partly due to the inclusion of undetected diabetes cases [14, 17]. However, the IRs among people without diabetes were comparable between the two studies (21.8 [95% CI 20.0, 23.6] in the present study vs 20 [95% CI 18, 23] in the previous study). Therefore, when comparing the incidence of RRT among people with and without diabetes, relative risk was considerably lower in the current study (almost fourfold) than in the previous study (almost eightfold).
An international comparison revealed one population-based study from Canada conducted in 1999–2000 with a comparable study design. The age- and sex-adjusted IR in the population with diabetes in that study was 132.9 per 100,000 PY and thus in line with our findings. In contrast, the IR among people without diabetes in the Canadian study was 11.0 and therefore much lower than our results, with a resulting higher corresponding RR of 12 [3].
Although some other studies also analysed the IR of RRT among people with diabetes and took into account diabetes as a comorbidity, they represented only the crude IRs [10, 11] or crude RRs [2], and were therefore not wholly comparable with our results.
Due to the fact that renal registers usually record only the primary cause for RRT, the epidemiological studies based on these data sources are only able to estimate the incidence of RRT that was due to diabetic nephropathy [5, 24,25,26,27,28]. Moreover, most of these studies reported IRs of diabetic nephropathy by using the total population as a denominator and not the population with diabetes at risk [5, 24, 26, 28]. This approach has limitations since it does not consider the prevalence of diabetes in the background population. These studies are therefore not comparable with the current study. Only one study from the USA [25] reported age-standardised IRs of diabetic nephropathy including estimation of the population with diabetes at risk: the IR varied between 260.2 per 100,000 PY in 2000 and 173.9 in 2014 [25]. A study from Catalonia, Spain, reported that the crude IR changed from 48.95 per 100,000 PY in 1994 to 59.36 in 2010 [27].
The incidence of RRT considering only diabetic nephropathy in the current study was largely comparable to the study results from Catalonia, Spain [27], but approximately five times lower than the study from the USA [25].
We did not find any significant time trend regarding IRs or RRs during the study period 2002–2016.
Our results are in line with a study from Italy, which analysed the incidence of dialysis during the years 2004–2013 in the populations with and without diabetes and did not observe a significant change [2]. In contrast, a study from Hong Kong reported a significant decrease in the incidence of ESRD (4% per year in the fully adjusted model) among individuals with type 2 diabetes during the years 2000–2012 [11].
The studies that only counted diabetic nephropathy as a reason for RRT reported a decrease of RRT incidence. A study from the USA reported a reduction of about a third between 2000 and 2014 [25] and the study from Catalonia, Spain, reported a slight decrease since 2002 [27]. In our study we observed a significant decrease among men but not among women with diabetes (ESM Table 4).
Strengths and weaknesses of the study
Several limitations have to be considered. First, we analysed the data from one regional dialysis centre in Germany that covered a population of about 310,000 inhabitants. Therefore, only a restricted generalisation of the data to the whole German population was possible. However, the results of RRT incidence with respect to the whole population of the study region in 2006 were justifiably comparable to national German data: 254 per million population vs 213 per million population [20]. Second, the diabetic population as a population at risk was estimated using data from two nationwide German surveys performed in 1997–1999 and 2008–2011. Although regional differences are reported in diabetes prevalence in Germany, a recent analysis based on nationwide claims data revealed that the prevalence of diabetes in the study region was highly comparable to national diabetes prevalence [29]. Third, diabetes prevalence could only be estimated up until 2011, and thus for the main analysis we assumed that diabetes prevalence increased linearly as of 2011. Nevertheless, we also performed a sensitivity analysis using constant diabetes prevalence for the years 2011–2016 with no effect on the main results. Finally, we cannot rule out that some people from the study region started RRT outside of the study region, which would lead to an underestimation. However, individuals with ESRD receive dialysis at least once a week over a long time period. Most therefore prefer to travel only a short distance within the study region. We therefore assume that the collection of RRT cases in the study region is largely complete.
A main strength of our study was that we estimated the incidence of RRT in people with diabetes compared with people without diabetes independently of the underlying reason for RRT. The majority of studies published were able to identify only people with diabetes in whom diabetic nephropathy was the main reason for RRT. This methodological approach could lead to an underestimation of people with diabetes, since diabetic nephropathy was only reported as primary renal disease in approximately half of the individuals with type 2 diabetes [30]. An additional problem is that although diagnosis of diabetic nephropathy is based on established guidelines [22], in practice it is not always easy (especially among individuals with type 2 diabetes) to differentiate between diabetic nephropathy as a main reason for ESRD and diabetes as a comorbidity when other diseases in individuals with diabetes co-exist, e.g. hypertension or renal disease with nondiabetic pathogenesis [30, 31]. A biopsy could clarify the diagnosis of diabetic nephropathy but is usually only performed among a small group of individuals [30, 31]. All of these factors could lead to an over- or underestimation of diabetic nephropathy as a reason for ESRD. A further strength of our study was the population-based design. We conducted our study using valid data from one well-documented regional dialysis centre. We were therefore able to report clinical data relating to diabetes type and diabetes duration as well as comorbidities upon commencement of RRT. Finally, we estimated the IR over a long study period which allowed us to evaluate a time trend of 15 years.
Unanswered questions and future research
The IR of RRT remained substantially higher among people with diabetes, with an almost fourfold-increased RR. Men have a twofold-increased risk of RRT compared with women. The IRs among the subpopulations with and without diabetes and the RRs during the study period largely remained mainly constant, with consistent results in both sexes. However, the considered study region was fairly small. Therefore, future research in a nationwide population is needed to confirm these findings.
Data availability
The data that support the findings of this study are available from the authors upon reasonable request and with permission of the dialysis centre of Mettmann.
Abbreviations
- ESRD:
-
End-stage renal disease
- IR:
-
Incidence rate
- PY:
-
Person-years
- RRT:
-
Renal replacement therapy
References
International Diabetes Federation (2019) IDF diabetes atlas, 8th edition. Available from http://www.idf.org/diabetesatlas. Accessed 23 June 2019
Giorda CB, Carna P, Salomone M et al (2018) Ten-year comparative analysis of incidence, prognosis, and associated factors for dialysis and renal transplantation in type 1 and type 2 diabetes versus non-diabetes. Acta Diabetol 55(7):733–740. https://doi.org/10.1007/s00592-018-1142-y
Lok CE, Oliver MJ, Rothwell DM, Hux JE (2004) The growing volume of diabetes-related dialysis: a population based study. Nephrol Dial Transplant 19(12):3098–3103. https://doi.org/10.1093/ndt/gfh540
Hoffmann F, Haastert B, Koch M, Giani G, Glaeske G, Icks A (2011) The effect of diabetes on incidence and mortality in end-stage renal disease in Germany. Nephrol Dial Transplant 26(5):1634–1640. https://doi.org/10.1093/ndt/gfq609
Villar E, Chang SH, McDonald SP (2007) Incidences, treatments, outcomes, and sex effect on survival in patients with end-stage renal disease by diabetes status in Australia and New Zealand (1991-2005). Diabetes Care 30(12):3070–3076. https://doi.org/10.2337/dc07-0895
Sattar A, Argyropoulos C, Weissfeld L et al (2012) All-cause and cause-specific mortality associated with diabetes in prevalent hemodialysis patients. BMC Nephrol 13:130. https://doi.org/10.1186/1471-2369-13-130
Icks A, Haastert B, Gandjour A et al (2010) Costs of dialysis - a regional population-based analysis. Nephrol Dial Transplant 25(5):1647–1652. https://doi.org/10.1093/ndt/gfp672
Kahm K, Laxy M, Schneider U, Rogowski WH, Lhachimi SK, Holle R (2018) Health care costs associated with incident complications in patients with type 2 diabetes in Germany. Diabetes Care 41(5):971–978. https://doi.org/10.2337/dc17-1763
Icks A, Haastert B, Genz J et al (2011) Incidence of renal replacement therapy (RRT) in the diabetic compared with the non-diabetic population in a German region, 2002–08. Nephrol Dial Transplant 26(1):264–269. https://doi.org/10.1093/ndt/gfq398
Chu YW, Wu WS, Hsu CF, Wang JJ, Weng SF, Chien CC (2017) Bidirectional association between ESRD dialysis and diabetes: national cohort study. PLoS One 12(3):e0173785. https://doi.org/10.1371/journal.pone.0173785
Luk AOY, Hui EMT, Sin MC et al (2017) Declining trends of cardiovascular-renal complications and mortality in type 2 diabetes: the Hong Kong Diabetes Database. Diabetes Care 40(7):928–935. https://doi.org/10.2337/dc16-2354
Nationale VersorgungsLeitlinie (2010. Zuletzt geändert: September 2015) Nierenerkrankungen bei Diabetes im Erwachsenenalter. Langfassung. Available from https://www.leitlinien.de/mdb/downloads/nvl/diabetes-mellitus/dm-nierenerkrankungen-1aufl-vers6-lang.pdf. Accessed 20 June 2019 [document in German]
Federal Office for Statistics (2017) Statistisches Bundesamt. Bevölkerung auf Grundlage des Zensus 2016. Available from https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Bevoelkerung/_inhalt.html. Accessed 14 May 2019 [document in German]
Heidemann C, Du Y, Schubert I, Rathmann W, Scheidt-Nave C (2013) Prevalence and temporal trend of known diabetes mellitus: results of the German Health Interview and Examination Survey for Adults (DEGS1). Bundesgesundheitsblatt, Gesundheitsforschung, Gesundheitsschutz 56(5–6):668–677. https://doi.org/10.1007/s00103-012-1662-5
Kamtsiuris P, Lange M, Hoffmann R et al (2013) The first wave of the German Health Interview and Examination Survey for Adults (DEGS1): sample design, response, weighting and representativeness. Bundesgesundheitsblatt, Gesundheitsforschung, Gesundheitsschutz 56(5–6):620–630. https://doi.org/10.1007/s00103-012-1650-9
Gosswald A, Lange M, Kamtsiuris P, Kurth BM (2012) DEGS: German Health Interview and Examination Survey for Adults. A nationwide cross-sectional and longitudinal study within the framework of health monitoring conducted by the Robert Koch institute. Bundesgesundheitsblatt, Gesundheitsforschung, Gesundheitsschutz 55(6–7):775–780. https://doi.org/10.1007/s00103-012-1498-z
Heidemann C, Du Y, Paprott R, Haftenberger M, Rathmann W, Scheidt-Nave C (2016) Temporal changes in the prevalence of diagnosed diabetes, undiagnosed diabetes and prediabetes: findings from the German Health Interview and Examination Surveys in 1997–1999 and 2008–2011. Diabet Med 33(10):1406–1414. https://doi.org/10.1111/dme.13008
Nationale VersorgungsLeitlinie Therapie des Typ-2-Diabetes (August 2013. Zuletz geändert: April 2014) Langfassung. Version 3. Available from http://www.deutsche-diabetes-gesellschaft.de/fileadmin/Redakteur/Leitlinien/Evidenzbasierte_Leitlinien/NVL_Typ-2_Therapie-lang_Apr_2014.pdf. Accessed 20 June 2019 [document in German]
Boddana P, Caskey F, Casula A, Ansell D (2009) UK Renal Registry 11th annual report (December 2008): chapter 14: UK Renal Registry and international comparisons. Nephron Clin Pract 111(Suppl 1):c269–c276. https://doi.org/10.1159/000210003
Frei U, Schober-Halstenberg H-J (2006) Nierenersatztherapie in Deutschland. Bericht 2005/2006. QuaSi Niere. Available from https://www.bundesverband-niere.de/wp/wp-content/uploads/2019/02/QuaSi-Niere-Bericht_2005-2006.pdf. Accessed 20 June 2019 [document in German]
United States Renal Data System (2009) Atlas of end-stage renal disease in the United States. Available from https://www.usrds.org/atlas09.aspx. Accessed 20 June 2019
National Kidney Foundation (2007) KDOQI clinical practice guideline diabetes and CKD. Guidelines 1.3 and 1.4. Screening and diagnosis of DKD. Am J Kidney Dis 49:1–180
Ratzmann KP (1991) Eine Analyse von alters- und geschlechts-spezifischer Diabetesprävalenz sowie Behandlungsart: Die Berlin-Studie. Akt Endokr Stoffw 12:220–223 [document in German]
van Dijk PR, Kramer A, Logtenberg SJ et al (2015) Incidence of renal replacement therapy for diabetic nephropathy in the Netherlands: Dutch diabetes estimates (DUDE)-3. BMJ Open 5(1):e005624. https://doi.org/10.1136/bmjopen-2014-005624
Burrows NR, Hora I, Geiss LS, Gregg EW, Albright A (2017) Incidence of end-stage renal disease attributed to diabetes among persons with diagnosed diabetes––United States and Puerto Rico, 2000–2014. MMWR Morb Mortal Wkly Rep 66(43):1165–1170. https://doi.org/10.15585/mmwr.mm6643a2
Prischl FC, Auinger M, Saemann M et al (2015) Diabetes-related end-stage renal disease in Austria 1965–2013. Nephrol Dial Transplant 30(11):1920–1927. https://doi.org/10.1093/ndt/gfv113
Comas J, Arcos E, Castell C et al (2013) Evolution of the incidence of chronic kidney disease stage 5 requiring renal replacement therapy in the diabetic population of Catalonia. Nephrol Dial Transplant 28(5):1191–1198. https://doi.org/10.1093/ndt/gfs507
Assogba FG, Couchoud C, Hannedouche T et al (2014) Trends in the epidemiology and care of diabetes mellitus-related end-stage renal disease in France, 2007–2011. Diabetologia 57(4):718–728. https://doi.org/10.1007/s00125-014-3160-9
Goffrier B, Bätzing J, Holstigee J (2017) Entwicklung der administrativen Prävalenz des Diabetes mellitus von 2009 bis 2015. Monitor Versorgungsforschung 05:46–49. https://doi.org/10.24945/MVF.05.17.1866-0533.2040 [document in German]
Villar E, McDonald SP, Couchoud C (2010) Incidence of treatment for end-stage renal disease among individuals with diabetes in the U.S. continues to decline: response to Burrows, Li, and Geiss. Diabetes Care 33(5):e69; author reply e70. https://doi.org/10.2337/dc10-0074
Yuan CM, Nee R, Ceckowski KA, Knight KR, Abbott KC (2017) Diabetic nephropathy as the cause of end-stage kidney disease reported on the medical evidence form CMS2728 at a single center. Clin Kidney J 10(2):257–262. https://doi.org/10.1093/ckj/sfw112
Acknowledgements
We thank J. Groves (Conference interpreter, Cologne, Germany) for editing the paper and revising the English language used in this manuscript. Some of the data were presented as an abstract at the EASD Annual Meeting, Barcelona, 2019.
Funding
The project was supported by the German Federal Ministry of Health (grant number ZMV I 5-2514FSB505). We also thank the Nieren- und Hochdruckforschung e.V. Mettmann Foundation for their unrestricted grant. The funders had no role in study design, data collection and analysis, decision to publish or the preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
AI and MK designed the study and co-drafted the first version of the article. MK collected and provided data. TK, TW, LCR and MN contributed to the overall coordination, data collection and research data. HC and MN analysed and interpreted the findings and drafted the first version of the article. All authors interpreted the analysis, and reviewed and provided input into the final manuscript and gave their final approval of the version to be published. AI is the guarantor of this work and, as such, had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
The authors declare that there is no duality of interest associated with this manuscript.
Open access
This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 357 kb)
Rights and permissions
About this article
Cite this article
Narres, M., Claessen, H., Kvitkina, T. et al. Incidence and relative risk of renal replacement therapy in people with and without diabetes between 2002 and 2016 in a German region. Diabetologia 63, 648–658 (2020). https://doi.org/10.1007/s00125-019-05067-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-019-05067-6