Abstract
Osteocalcin (OC) is the most abundant non-collagenous and osteoblast-secreted protein in bone. It consists of two forms such as carboxylated OC (cOC) and undercarboxylated OC (ucOC). While cOC promotes bone mineralization and increases bone strength, ucOC is regarded an endocrinologically active form that may have several functions in multiple end organs and tissues. Total OC (tOC) includes both of these forms (cOC and ucOC) and is considered a marker of bone turnover in clinical settings. Most of the data on OC is limited to preclinical studies and therefore may not accurately reflect the situation in clinical conditions. For the stated reason, the aim of this review was not only to summarize current knowledge of all forms of OC and characterize its role in diabetes mellitus, osteoporosis, osteopetrosis, inflammatory joint diseases, but also to provide new interpretations of its involvement in the management and treatment of aforementioned diseases. In this context, special emphasis was placed on available clinical trials. Significantly lower levels of tOC and ucOC could be associated with the risk of type 2 diabetes mellitus. On the contrary, tOC level does not seem to be a good indicator of high bone turnover status in postmenopausal osteoporosis, osteoarthritis and rheumatoid arthritis. The associations between several pharmacological drugs used to treat all disorders mentioned above and OC levels have also been provided. From this perspective, OC may serve as a medium through which certain medications can influence glucose metabolism, body weight, adiponectin secretion, and synovial inflammation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteocalcin (OC) is a major non-collagenous protein in bone synthesized by osteoblasts (bone-forming cells), but also by odontoblasts and hypertrophic chondrocytes [1]. It contains 49 amino acids in humans; while in mice it is made up of 46 amino acids. Overall, OC consists of two forms, such as carboxylated (cOC) and undercarboxylated (ucOC), and can be measured in the serum separately or as a total OC (tOC) [2, 3], which includes both aforementioned forms as well as detectable fragments released during bone resorption [4].
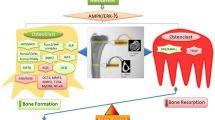
When bone is resorbed by osteoclasts (bone-resorbing cells), the acidic pH in the resorption lacuna causes the carboxyl groups on OC to be removed and ucOC to be released into the systemic circulation (Fig. 1). Therefore, circulating levels of ucOC are dependent on the rate of bone turnover (remodeling) [2, 5]. In general, serum levels of tOC, cOC, and ucOC can elevate with increasing bone formation, while ucOC level also elevates with increasing bone resorption [6].
OC biosynthesis and metabolism. Expression of the BGLAP gene produces pre-pro-osteocalcin, which contains a signal sequence, a pro-peptide, and a chain. The signal sequence is removed in the endoplasmic reticulum to form pro-osteocalcin containing a propeptide and an osteocalcin chain. Three glutamate residues located in the Gla domain can be carboxylated by γ-glutamyl carboxylase. After cleavage of the pro-peptide by proprotein convertase, mature OC is finally formed and secreted into bone microenvironment. During bone resorption by osteoclasts, the acidic pH causes decarboxylation and ucOC can be released into the systemic circulation. Circulating OC is degraded in the kidney and liver to a more stable N-MID-fragment, so intact and fragmented molecules coexist in the serum (created with BioRender.com)
The ucOC/tOC ratio is often measured in clinical studies. This parameter is higher in older adults compared to young individuals [7]. Interestingly, increased ucOC/tOC ratio was associated with reduced muscle function and elevated risk of long-term fall-related hospitalizations in elderly women, who had worse physical function, mobility, and a greater fear of falling. According to Luukinen et al. [8], higher ucOC/tOC ratio may also predict fracture risk in older men.
Overall, ucOC represents approximately one third of tOC. The serum tOC level (less than 50 ng/ml in mice and <30 ng/ml in humans) is considered a bone turnover marker in clinical conditions and reflects the osteoformation ability of osteoblasts. In mice, OC levels peak during the day and are lowest at night, whereas in humans, levels are very low in the morning, begin to increase in the afternoon, and peak at night [2, 9, 10]. These alterations may be consistent with modulation of glucocorticoid levels. Therefore, when extrapolating results from mouse studies to the human settings, the time point at which samples are collected should also be taken into account [11].
Generally, ucOC is regarded an endocrinologically active form of OC in preclinical studies [12]. The specific receptor of ucOC is G protein-coupled receptor class c group 6 member A (GPRC6A) [13]. It is broadly expressed in various organs, with the exception of the brain [14,15,16,17]. The G protein-coupled receptor 158 (GPR158) acts as ucOC receptor in the brain, and is associated with cognitive function ([18]; Fig. 2).
Schematic representation of the putative functions of ucOC. ucOC is released into the systemic circulation, binds to receptors on the cell surface (GPRC6A receptors are found in muscles, pancreas, testicles and GPR158 receptor is present in the brain) and can regulate muscle function, insulin production, male fertility and brain function (created with BioRender.com)
Based on various investigations, ucOC has been found to possess multiple functions, including increasing insulin secretion and proliferation of pancreatic β cells as well as adiponectin secretion from adipose tissue, thereby improving insulin sensitivity and reducing fat mass [19], improving skeletal muscle exercise capacity [16], enhancing testosterone secretion from testis [14], increasing glucagon-like peptide-1 (GLP-1) secretion from the intestine [15], enhancing cognitive function in the brain [20]. These various effects of ucOC have been suggested to be closely related to glucose metabolism and diabetic complications [10]. Therefore, ucOC has been proposed to act as a hormone (osteokine) with pleiotropic effects in multiple end organs and tissues, e.g. muscles, pancreas, male gonads, brain (Fig. 2) to regulate muscle mass, glucose and energy metabolism, male fertility, cognitive functions and behavior [10, 21]. The link between the skeleton and exoskeletal organs mentioned above demonstrates the importance of the endocrine function of the skeletal system. However, it is important to keep in mind that most of the data obtained has been limited to in vitro and animal model studies.
In general, OC can be clinically detected using enzyme immunoassays, chemiluminescent immunoassays or radioimmunoassays. Circulating OC has a short half-life (about 5 minutes) and is degraded in the kidney and liver, so intact and fragmented segments coexist in the serum (Fig. 1). The heterogeneity of these fragments is believed to limit its use [22]. Thus, tOC consists especially of intact OC and N-MID (N-terminal mid)-fragment. While intact OC is unstable due to protease cleavage between amino acids 43 and 44, the N-MID-fragment resulting from the cleavage, is considerably more stable. Therefore, assays usually detect a stable N-MID-fragment [23, 24]. However, assays detecting both the intact OC polypeptide and the N-MID-fragment may also be used [25,26,27]. The ucOC can be measured using hydroxyapatite binding assay (uses hydroxyapatite to bind cOC that is removed by centrifugation, and ucOC is subsequently measured) and direct immunoassays (use antibodies against ucOC; however, commercially available ucOC antibody can overestimate large ucOC fragments, leading to inaccuracies in the determination of ucOC or ucOC/tOC ratio) [4, 28, 29]. For this aim, measurement of ucOC is not straightforward, and frequently used methods do not distinguish the number and position of non-carboxylated glutamate residues, and these limitations should be considered when interpreting the results [4]. In any case, methods for the determination of circulating ucOC are nowadays gradually increasing [30], but they need to be optimized for routine use.
Despite the initial search for information on OC and the subsequent abundance of articles, to our knowledge, current information on OC with respect to all its forms (cOC, ucOC, tOC) as well as its role in most common bone-related disorders is scattered. Recent controversies regarding the proposed role of OC in skeletal development, energy metabolism, male fertility, and nervous system have been characterized by Komori [31], Manolagas [5], Wang et al. [32] primarily using animal models. Information obtained from clinical studies has not been provided. Several authors evaluated the associations of serum OC level with diabetes mellitus [2, 21, 33]; however, knowledge of which type of OC (tOC or ucOC) was analysed in patients, was not often specified. Relationships between OC levels and other bone-related diseases appear sporadically in a few articles [1, 11, 34], but they are not summarized in a dedicated review. Therefore, the main aim of this review was not only to summarize current knowledge about all forms of OC, but also to provide new interpretations of its involvement in the management of diabetes mellitus, osteoporosis, osteopetrosis and two inflammatory joint diseases (osteoarthritis and rheumatoid arthritis). In this context, special emphasis was placed on available clinical studies and accurate information on the type of OC under investigation. Less well-known associations between pharmacological treatment of all aforementioned disorders and OC levels were also provided to demonstrate the potential of OC to serve as a medium through which certain medications can influence some important indicators of a particular disease.
Molecular structure of osteocalcin
In humans, OC is encoded by a single BGLAP (bone gamma-carboxyglutamate protein) gene, located on chromosome 1 at 1q25-q31. The pre-pro-osteocalcin molecule with a length of 100 amino acids is first synthesized by gene expression (UniProtKB AC P02818; [35]). The predicted structure of the pre-pro-osteocalcin molecule with the confidence of prediction of individual parts is shown in Fig. 3a, c. Like most secreted proteins, OC has a signal sequence (amino acids 1-23) that is removed in the endoplasmic reticulum to form pro-osteocalcin containing a 28 amino acid pro-peptide and a 49-residue osteocalcin chain. The molecule contains Gla domain with three glutamate residues at positions 68, 72 and 75 that can be carboxylated (Fig. 3b), which then provide high affinity to the hydroxyapatite matrix. This modification is catalyzed by γ-glutamyl carboxylase, and uses vitamin K, O2, and CO2 as cofactors, supplied by the vitamin K cycle and circulation [11, 36]. In bone, cOC represents 15% of non-collagenous matrix proteins [2] and is essential for the alignment of apatite crystals and optimal bone strength. Bone strength is elevated by cOC [31]. The ucOC with a reduced degree of carboxylation at the glutamate residues (carboxylation is missing at one or more positions) is available with less affinity for hydroxyapatite [11]. Mature OC consisting of 49 residues is finally formed by cleavage of the pro-peptide by the proprotein convertase furin and secreted into the bone microenvironment ([37]; Fig. 1). The OC is able to interact with many molecules that have an important function in bone physiology. Predicted interactions and functional partners of OC are illustrated in Fig. 4.
Human OC structure prediction according to AlphaFold Protein Structure Database [168, 169]. a – 3D visualization of OC structure prediction with colored per-residue confidence metric (pLDDT). The structures of the signal sequence (red box) and Gla domain (green box) show the highest confidence score. b - Positions of carboxylation and disulfide bond on the OC molecule (Gla domain). c - Inter-domain (inter-structure) arrangement prediction with predicted aligned error. The two dark green (low-error) squares on the 2D plot correspond to the two distinct domains (structures) highlighted in red and blue boxes. The alignment of the middle sequence (shown in gray) relative to the other residues shows a high error
Predicted interactions and functional partners of OC. The network comes from STRING, a database of known and predicted protein interactions [170]. The evidence view with a minimum interaction score of 0.9 (the highest confidence) is displayed. Different line colors represent the types of evidence for the association. ALPL - Alkaline phosphatase, tissue-nonspecific isozyme; BGLAP – Osteocalcin; BMP2 - Bone morphogenetic protein 2; FN1 – Fibronectin; GGCX - Vitamin K-dependent gamma-carboxylase; GPRC6A - G-protein coupled receptor family C group 6 member A; IBSP - Bone sialoprotein 2; MGP - Matrix Gla protein; PTH - Parathyroid hormone; RUNX2 - Runt-related transcription factor 2; SP7 - Transcription factor Sp7; SPARC – SPARC; SPP1 – Osteopontin; TNFSF11- Tumor necrosis factor ligand superfamily member 11, membrane form
Osteocalcin-deficient animal models
Due to considerable differences between mouse and human OC at both the genomic and protein level, the validity of extrapolating findings from the OC-deficient mouse model to human disease has been questioned [38]. In general, mice have a gene cluster of OC consisting of Bglap, Bglap2, and Bglap3 genes within a 23 kb span of genomic DNA, while one OC gene has been determined in rats and humans [39]. Bglap and Bglap2 are specifically expressed in bone, while Bglap3 is expressed in non-osteoid tissues (e.g. kidney, male gonadal tissues, lung) [40, 41]. OC expression is regulated by runt-related transcription factor 2 (Runx2), which is an essential transcription factor for osteoblast differentiation [42]. In fact, Runx2 deficient mice do not express any OC; its expression was reduced by Runx2 antisense oligonucleotides in rat primary osteoblasts and ROS17/2.8 osteoblastic cells, and overexpression of Runx2 induced OC expression in C3H10T1/2 multipotent mesenchymal cells [43,44,45,46].
Ducy et al. [47], generated the first OC-deficient mice (in 129Sv:C57BL/6J mixed genetic background) that had significantly elevated trabecular and cortical bone volume, cortical bone thickness, bone mineral density (BMD), and bone strength. The number of osteoclasts and bone marrow area were higher in OC-null mice. In addition, ovariectomy raised bone marrow area and reduced bone strength in this mouse model. In accordance with the findings of aforementioned study, OC has been considered a negative factor of bone formation that reduces osteoblast function and osteoclastogenesis. Moreover, OC-null mice displayed impaired glucose metabolism [28], reduced testosterone synthesis [14], and muscle mass [16]. However, the new OC-deficient mice generated by Diegel et al. [48], (in C57BL/6J,C3H mixed genetic background, the authors replaced DNA encoding Bglap and Bglap2 with a neo cassette in embryonic stem cells) and Moriishi et al. [6] (in C57BL/6N mixed genetic background, the authors used CRISPR/Cas9-mediated gene editing to remove most of the Bglap and Bglap2 protein coding regions) did not confirm the inhibition of bone formation by OC. Consistent with their findings, OC did not affect bone formation, bone resorption, and bone mass in either estrogen-deficient or estrogen-sufficient conditions. Moreover, OC was not physiologically involved in glucose metabolism, testosterone synthesis or maintenance of muscle mass. Possible explanations for these discrepancies may include modifier genes, genetic background of mice, differences in the molecular genetics of knockout alleles, sex, or breeding environment. However, both studies mentioned above [6, 48] have brought a general consensus that OC promotes bone mineralization. The rat OC gene locus shares greater synteny with the human locus. Therefore, Lambert et al. [38] generated OC-null mutant rats (using the CRISPR/Cas9 system) and reported increased trabecular thickness, BMD, and trabecular bone volume. In contrast to the findings of Ducy et al. [47], their data did not demonstrate elevated cortical bone volume and density. Also, OC-deficient rats did not develop obesity, insulin resistance, or glucose intolerance. Further investigations are therefore necessary to clearly determine the causal effect of OC.
Osteocalcin and diabetes mellitus
Diabetes mellitus (DM) represents a worldwide public health issue affecting approximately 450 million adults [49]. In addition to the most frequent secondary complications of DM (including diabetic retinopathy, nephropathy, neuropathy, cardiovascular diseases) [50], diabetic bone disorder is often diagnosed, which justifies the inclusion of DM among bone-related diseases. It is manifested by altered bone mineral density (BMD), abnormalities in bone metabolism and microarchitecture, reduced bone strength. Although both type 1 diabetes mellitus (T1DM) and type 2 diabetes mellitus (T2DM) share common features, notably hyperglycemia, the etiology of diabetic bone disorder differs between them. While reduced BMD is mainly determined in T1DM, the BMD may not be affected in T2DM patients. However, a higher risk of fractures is demonstrated in both T1DM and T2DM [51, 52].
Strong evidence suggests that ucOC could exert its metabolic effects by targeting multiple tissues essential for glucose and lipid metabolism. In the pancreas, ucOC can promote β-cell proliferation and insulin production through GPRC6A [19, 53]. The ucOC can also elevate delta like-1 (DLK1) production in pancreatic β cells, and DLK1 inhibits the insulin signaling-dependent OC production in osteoblasts [54]. Therefore, there is a positive feedback loop between pancreatic islets and bone. The ucOC can also indirectly favor insulin production by increasing GLP-1 secretion from the intestine [15]. In insulin target tissues, ucOC can increase glucose and fatty acid uptake [16, 55], insulin sensitivity [56], nutrient utilization and mitochondrial capacity [16] and reduce glycogen production in muscle and lipid synthesis in liver [16, 57].
It has been reported that circulating levels of ucOC are decreased in both humans and mice in the presence of metabolic syndromes such as insulin resistance and DM [58,59,60] and that these disorders can be alleviated by ucOC administration [28, 60,61,62]. Obese diabetic mice administered ucOC have been shown to improve systemic glucose tolerance and insulin sensitivity, concomitantly with reductions in hyperlipidemia and whole-body adiposity [61,62,63]. Accordingly, the overexpression of ucOC protected mice from obesity and glucose intolerance [28]. In insulin resistant tissues, ucOC treatment restored the impaired response to insulin stimulation, disturbed energy metabolism and reduced mitochondrial capacity [19, 60, 62, 64].
In patients with metabolic syndrome, lower tOC levels were reported compared to controls, and increases in tOC levels were associated with decreases in fasting plasma glucose, glycated hemoglobin (HbA1c), insulin resistance index (HOMA-IR) and body mass index (BMI) [58]. According to Liang et al. [65], tOC level was the highest in the normal glucose tolerance group and gradually decreased in the impaired glucose tolerance group and T2DM participants. After a four-year follow-up, group with low tOC (<23.33 ng/mL) showed an increased risk of T2DM, reduced fasting glucose and insulin resistance (IR). Many studies also confirmed significantly reduced tOC levels in individuals with T2DM versus healthy controls [65,66,67,68,69,70,71,72,73,74,75,76]. On the other hand, a minimal number of studies did not reveal any differences [77, 78]. The data are summarized in Table 1. According to Zeng et al. [79], high tOC was associated with lower blood glucose, IR, triglycerides and BMI. Thus, OC may be positively correlated with glycemic metabolic status, and reduced level of serum tOC could be consistent with incident T2DM.
Large epidemiological studies indicated that a higher level of ucOC was associated with a lower risk of DM in the community [73, 80]. Bullo et al. [81] revealed that an increase in ucOC was consistent with a decrease in HOMA-IR over two years in a community-dwelling population. However, a prospective investigation showed no evidence of an association between ucOC and incident T2DM in elderly participants [82]. On the contrary, further studies reported lower levels of ucOC in subjects with T2DM compared to controls [30, 73, 83,84,85]. The role of ucOC in T1DM remains uncertain [4].
Considering pharmacological treatment of DM, a recent meta-analysis by Hu et al. [86] revealed no significant impact of metformin (an insulin sensitizer) administration on tOC level. Similarly, vildagliptin (an incretin-based therapy) had no effect on tOC level even after 12 months of application [87]. Identical findings were also recorded in diabetic women with osteoporosis receiving metformin and sitagliptin (an incretin-based therapy) [88]. Application of thiazolidinediones (insulin sensitizers) such as pioglitazone and rosiglitazone in diabetic patients produced various effects on tOC levels, ranging from a decrease [89], through non-significant changes [90, 91] to an increase in tOC [92]. In several cases, it is possible to observe variability in the concentration of tOC over time according to the length of treatment with a given thiazolidinedione. When using rosiglitazone, no significant changes in tOC levels were found after 12 weeks; however, rapid decrease in tOC was sustained during the 2-year follow-up. In contrast, in the pioglitazone study, serum tOC first decreased at 6 months and then almost returned to baseline at 12 months. Both thiazolidinediones are peroxisome proliferator-activated receptor (PPAR) agonists. However, rosiglitazone is a specific PPARγ activator, while pioglitazone is not only a selective human PPARγ1 but also a weak human PPARα activator [93], which may result in differences in their effects. In addition, it is necessary to consider the limitations of individual studies, such as small sample sizes, different dosages or different proportions of men and women. The results of Namvaran et al. [92] deviate from the trend of decreasing tOC levels due to thiazolidinediones, the authors explain this fact by breaking IR, where the cause of increased tOC may be reduced IR in peripheral tissues and improved glucose tolerance. Regarding SGLT2 inhibitors (e.g. canagliflozin, empagliflozin), longer treatment time appears to be required to affect tOC levels (Table 2). In addition, OC may serve as a medium through which certain pharmacological drugs can affect glucose metabolism. It is known that bone resorption is closely related to glucose homeostasis. Specifically, high fasting plasma glucose levels were measured in osteoporotic women treated with medications inhibiting bone resorption, and there was a positive correlation between ucOC and urinary cross-linked N-telopeptides of type I collagen (NTx, bone resorption marker) [94, 95]. Accordingly, the use of antiresorptive drugs should increase the risk of IR and DM due to reduced levels of ucOC. However, epidemiological and clinical trials have shown that the administration of antiresorptive drugs was not consistent with changes in plasma glucose, IR and the development of DM, but was associated with a reduced risk of DM, especially with long-term treatment [96,97,98,99,100,101]. Urano et al. [74] conducted a study involving postmenopausal women; some of them were treated with bisphosphonates (antiresorptive drugs). According to their findings, tOC levels were significantly correlated with HbA1c levels. Furthermore, a decrease (<6.1 ng/mL) of tOC was associated with the future development of T2DM. However, there was no trend towards an increased incidence of T2DM in patients treated with bisphosphonates [74]. The findings by Mazzioti et al. [102] also suggested that bisphosphonate treatment does not affect glucose metabolism, although lower tOC levels were noted in bisphosphonate-treated patients. Lewis et al. [103] found that HbA1c did not change significantly, although tOC and ucOC levels were lower in elderly women after 1 year of calcium carbonate supplementation compared to untreated individuals. Serum levels of OC were measured by radioimmunoassay or immunoradiometric assay.
A low bone remodeling status has been observed in diabetic patients treated with glucocorticoids (GC) [104] and could be associated with higher BMD [105]. According to Florez et al. [75], reduced tOC levels during GC treatment represent a risk factor for the manifestation of DM. Thus, GC-treated patients with tOC levels <9.25 ng/mL presented a sixfold higher risk of DM (Table 2). However, of all bone turnover markers measured, only OC was significantly associated with increased chances of DM. Insignificantly lower values of bone alkaline phosphatase (ALP), serum procollagen type I amino-terminal propeptide (PINP), and cross-linked C-terminal and N-terminal telopeptides of type I collagen (serum CTx and urine NTx) were reported in subjects with DM. The study by van Bommel et al. [106] showed that GC decreased tOC and PINP levels in a dose-dependent manner and that these alterations were related to adverse effects of GC on glucose and lipid metabolism. Furthermore, the effect of teriparatide (anabolic drug) on serum HbA1c and fasting plasma glucose was investigated by Mazzioti et al. [102]. This therapy generally increases bone formation and thus OC values (Table 2). A significant decrease in serum HbA1c was determined in diabetic patients, suggesting that teriparatide could cause some improvement in glucose homeostasis [102, 107]. Future research may assess whether treatments with more profound effects on OC interfere with glucose metabolism.
Osteocalcin and osteoporosis
Osteoporosis is the most common skeletal disorder affecting approximately 200 million individuals worldwide [108]. It is characterized primarily by reduced BMD, alterations in bone microstucture and elevated risk of fragility fractures. At the microstructural level, increased bone resorption and decreased bone formation occur simultaneously, leading to bone loss. Age is one of the main risk factors for primary type 1 (postmenopausal) osteoporosis. Primary osteoporosis of type 2 (senile) occurs after the age of 75 and is diagnosed in a ratio of 2:1 in women and men [109, 110].
Although serum tOC is widely used as a bone turnover marker to indicate high remodeling status in postmenopausal osteoporosis (PMO) [22, 111, 112], alterations in tOC level in individuals with PMO compared to healthy controls remain controversial. Several studies indicated a higher level of tOC in PMO cases [113,114,115,116,117,118,119,120,121]. However, there are also researches reporting the same or even lower tOC level in osteoporotic patients [122,123,124,125]. Biver et al. [126] and Liu et al. [127] performed meta-analyses to compare several markers of bone turnover and found no significant difference in tOC level between osteoporotic and healthy individuals. Therefore, tOC does not appear to be a good indicator of high bone turnover status in PMO unless new techniques for standardized assessment of circulating OC are used. Despite remaining issues with reference intervals and assay harmonization, tOC has been shown to be useful in elucidating the pharmacodynamics and efficacy of osteoporosis drugs in clinical trials [128].
Vergnaud et al. [123] revealed that a higher ucOC level predicted hip fracture risk independently of femoral neck BMD in older women. Conversely, tOC was not associated with hip fracture risk [124]. However, significant changes in ucOC level were observed in both osteoporotic and diabetic patients with osteoporosis (Table 1). According to Xu et al. [129], elevated ucOC level correlated with lower BMD at the lumbar spine, femoral neck, and total hip in both elderly women and men. Similar to these findings, Szulc et al. [130] and Emmaus et al. [131] reported that older women with abnormally high serum ucOC had lower BMD values at all sites. Cummings et al. [132] identified a 26% decrease of femoral neck BMD in patients with abnormal ucOC levels, which corresponded to a five- to sevenfold increase in hip fracture. Horiuchi et al. [124] found that ucOC levels were significantly higher in subjects with osteoporosis versus non-osteoporotic individuals (Table 1).
Interestingly, lower levels of dietary vitamin K are consistent with higher ucOC levels, while vitamin K supplements reduce ucOC levels [133]. Therefore, ucOC can be used as a marker to determine whether vitamin K preparations should be given to patients with osteoporosis [10]. Menatetrenone is the form of a synthetic vitamin K2 that is widely used in clinical practice. In the study by Shiraki et al. [134], serum level of ucOC was lower and cOC higher after 1 month of menatetrenone treatment. Differences in ucOC and cOC levels persisted during 6 months of the therapy. In addition, a higher tOC level was reported after 6 months of menatetrenone administration. Conversely, Jiang et al. [135] identified a reduction for both tOC and ucOC as well as the ucOC/tOC ratio after 12 months of menatetrenone treatment. A meta-analysis by Su et al. [136] demonstrated nonsignificantly reduced ucOC and a lower ucOC/tOC ratio in patients treated with menatetrenone (as part of combination therapy) compared to the placebo group. On the other hand, warfarin, an anticoagulant drug, inhibits vitamin K-dependent carboxylase, prevents post-translational carboxylation of factors in the coagulation cascade and OC, thereby increasing the levels of ucOC and lowering blood glucose levels in mice. However, warfarin also regulates OC gene expression, so warfarin treatment interferes with the interpretation of studies of this protein and its role in carbohydrate metabolism [137].
In this context, a clinical study by Fernandez-Real et al. [138] evaluated the effect of a high-calorie diet and regular physical activity on tOC levels. According to their findings, weight loss through diet and physical activity can cause increase in tOC level associated with changes in visceral fat mass.
Lower tOC levels were found in osteoporotic patients treated with bisphosphonates including risedronate, as well as in those treated with denosumab, a RANKL-binding monoclonal antibody [102, 139, 140]. On the other hand, treatment with teriparatide resulted in an increase in tOC [102]. The relationship between ucOC levels in postmenopausal osteoporotic women treated with parathyroid hormone (PTH) or alendronate (a bisphosphonate) and alterations in metabolic parameters were investigated by Schafer et al. [141]. The ucOC levels were increased after PTH and decreased after alendronate administration (Table 2). The ucOC/tOC ratio was increased with PTH treatment and unchanged with alendronate administration. Patients treated with PTH had reduced body weight after 12 months, while those treated with alendronate showed no significant changes. In addition, alterations in ucOC were positively correlated with changes in adiponectin, but no association was found with insulin, glucose, leptin, or the insulin/glucose ratio. On the contrary, no significant difference in ucOC level was detected during treatment with risedronate [139].
Secondary osteoporosis is also an important health problem, the most common form being glucocorticoid-induced osteoporosis (GIO). Impaired bone formation is a central pathophysiological mechanism of GIO-related bone loss [102]. At the molecular level, excess glucocorticoids inhibit Wnt protein production, causing mesenchymal progenitor cells to differentiate into adipocytes rather than osteoblasts. Excessive glucocorticoids also interfere with the canonical BMP (bone morphogenetic protein) pathway [142]. Consequently, serum tOC levels were reduced in patients receiving glucocorticoids, even when administered at lower doses [143, 144]. In the study by Shikano et al. [145], serum ucOC levels showed a decrease during glucocorticoid treatment from the first week and remained decreased for four weeks. Menatetrenone treatment improved tOC levels in the third and fourth weeks.
Osteocalcin and osteopetrosis
Osteopetrosis is a group of rare bone disorders within the family of sclerosing bone dysplasias, characterized by reduced bone resorption leading to high bone mass. An overly dense bone architecture, instead of providing strength, negates structural fragility that predisposes to fractures. Disruption of normal bone remodeling can lead to skeletal deformation and can interfere with mineral homeostasis [146]. Interestingly, mice lacking OC have severe osteopetrosis [147]. In general, three different types of osteopetrosis can be classified in humans: autosomal recessive (ARO), intermediate recessive (IRO) and autosomal dominant (ADO). They are characterized by different modes of inheritance and severity, from asymptomatic to fatal [11, 148].
Overall, individuals with ADO had increased level of tOC in cortical bone [149], reduced ucOC/tOC ratio (Table 1) and hypoinsulinemia [150]. In osteopetrotic children, serum OC levels were reported as normal or low. However, in a subset of six children, osteoblast activity (assessed by circulating ALP and OC) and osteoblast number did not increase despite hyperparathyroidism, suggesting PTH resistance or defective osteoblasts [151].
Osteopetrosis can be generally treated with calcium and vitamin D (first-line therapy), calcitriol, red blood cell transfusion, interferon γ-1b, and corticosteroids [146], however, there is no known link between these medications and OC level.
Osteocalcin and inflammatory joint diseases
Inflammatory diseases affecting bones and joints are very common in the world, as 250 million and 14 million people worldwide suffer from osteoarthritis (OA) and rheumatoid arthritis (RA), respectively [152, 153]. Primary joint diseases are characterized by systemic osteoporosis and higher incidence of fractures [154]. These disorders are also associated with the presence of inflammatory process targeting the joints with adverse effects on their structure and function [155]. From this group, OA and RA are described in this review.
OA can be defined by joint symptoms, structural pathology, or both [156]. It is characterized by excessive cartilage degradation, abnormal bone growth, sclerosis, and synovial inflammation [157].
Campion et al. [158] determined reduced tOC levels in patients with non-destructive OA and a non-significant increase in those with destructive OA. On the contrary, Naito et al. [159] revealed elevated ucOC levels in subjects with bilateral knee OA versus healthy controls. The data are summarized in Table 1. An increased OC expression in articular cartilage and subchondral bone was detected in OA joints [158, 160, 161]. Karsdal et al. [162] found a 12% reduction in tOC levels in patients with symptomatic knee OA treated with salmon calcitonin compared to untreated individuals; however, this decrease was transient and only a 2% decrease was noted at the end of the study (Table 2).
RA is a systemic inflammatory autoimmune disease characterized by synovial inflammation and hyperplasia, autoantibodies production, and systemic features (cardiovascular, pulmonary, and psychological disorders) [163]. It is also responsible for joint destruction consistent with bone complications, which include periarticular bone loss, bone erosion, and systemic osteoporosis [155].
Non-significantly lower tOC levels were found in patients with RA [158]. Seriolo et al. [164] reported decreased tOC levels in individuals with active RA compared to those without active disease (Table 1). Although the physiological significance of alterations in tOC levels in OA and RA is still unknown, they may reflect distinct bone phenotypes between these diseases [1]. While OA is more characterized by an increase in subchondral bone mass, RA involves bone resorption and subchondral bone loss [164, 165].
According to Peretz et al. [166], tOC levels have not been shown to be a useful index of abnormal bone turnover in RA, except in some patients with vertebral fractures treated with low doses of corticosteroids. No significant differences in tOC levels were recorded in individuals with RA treated with low-dose corticosteroids or non-steroidal antiinflammatory drugs and untreated controls (Table 2). In the study by Tamai et al. [167], tOC levels in RA patients with erosion progression were significantly increased in the tocilizumab (anti-interleukin-6 receptor antibody)-treated group than in the infliximab (anti-tumor necrosis factor drug)-treated group.
Conclusions and perspectives
Three forms of OC (cOC, ucOC, tOC) can be generally determined. In clinical conditions, ucOC/tOC ratio is often measured because it allows early identification of individuals at risk of low physical function and thus prevent future falls. Overall, cOC is required for optimal bone strength, ucOC is considered an endocrinologically active form, and tOC is regarded a marker of bone turnover. The vast majority of information on OC is limited to in vitro and animal model studies and therefore may not accurately reflect the situation in humans. Moreover, most clinical trials investigated groups pre-defined according to age, ethnicity or gender, which may also distort the data obtained. Limitations of existing knowledge also include technical problems with commonly used serum ucOC assays. Therefore, the medical-scientific community must continue efforts to elucidate the involvement of ucOCs in human health and disease and its clinical applications.
In addition to current knowledge of OC, this review also described its role in the management of DM, osteoporosis, osteopetrosis, OA and RA, focusing mainly on available clinical studies. Significantly reduced levels of tOC and ucOC could be associated with the risk of T2DM. The role of tOC and ucOC in T1DM remains uncertain. The tOC level does not seem to be a good indicator of high bone turnover status in PMO, OA and RA due to controversial findings. It is also worth noting that the correlation does not imply a direct function of OC in humans, so investigation of larger patient cohorts as well as carefully performed genetic studies are needed to gain more mechanistic insights. Additionally, associations between several pharmacological drugs used to treat all aforementioned bone-related disorders and OC levels were revealed. From this point of view, OC may serve as a medium through which some medications can affect glucose metabolism (e.g. glucocorticoids, teriparatide), body weight (e.g. PTH), adiponectin secretion (e.g. PTH), and synovial inflammation (e.g. tocilizumab). Last but not least, this review can contribute to a better use of OC in clinical applications as well as in further research and thus enrich current scientific literature.
Data availability
No original datasets were generated for this review. All data supporting the information given here can be found in the references cited within the paper.
References
Stock M, Schett G (2021) Vitamin K-dependent proteins in skeletal development and disease. Int J Mol Sci 22:9328. https://doi.org/10.3390/ijms22179328
Diaz-Franco MC, Franco-Diaz de Leon R, Villafan-Bernal JR (2019) Osteocalcin-GPRC6A: An update of its clinical and biological multi-organic interactions (Review). Mol Med Rep 19:15–22. https://doi.org/10.3892/mmr.2018.9627
Komori T (2020) Molecular mechanism of runx2-dependent bone development. Mol Cells 43:168–175. https://doi.org/10.14348/molcells.2019.0244
Lin X, Brennan-Speranza TC, Levinger I, Yeap BB (2018) Undercarboxylated Osteocalcin: Experimental and Human Evidence for a Role in Glucose Homeostasis and Muscle Regulation of Insulin Sensitivity. Nutrients 10:847. https://doi.org/10.3390/nu10070847
Manolagas SC (2020) Osteocalcin promotes bone mineralization but is not a hormone. PLoS Genet 16
Moriishi T, Ozasa R, Ishimoto T, Nakano T, Hasegawa T, Miyazaki T, Liu W, Fukuyama R, Wang Y, Komori H, Qin X, Amizuka N, Komori T (2020) Osteocalcin is necessary for the alignment of apatite crystallites, but not glucose metabolism, testosterone synthesis, or muscle mass. PLOS Gen 16
Smith C, Voisin S, Al Saedi A, Phu S, Brennan-Speranza T, Parker L, Eynon N, Hiam D, Yan X, Scott D, Blekkenhorst LC (2020)Osteocalcin and its forms across the lifespan in adult men. Bone 130:115085. https://doi.org/10.1016/j.bone.2019.115085.
Luukinen H, Käkönen SM, Pettersson K, Koski K, Laippala P, Lövgren T, Kivelä SL, Väänänen HK (2000) Strong prediction of fractures among older adults by the ratio of carboxylated to total serum osteocalcin. J Bone Miner Res 15:2473–2478. https://doi.org/10.1359/jbmr.2000.15.12.2473
Vitale JA, Sansoni V, Faraldi M, Messina C, Verdelli C, Lombardi G, Corbetta S (2021) Circulating carboxylated osteocalcin correlates with skeletal muscle mass and risk of fall in postmenopausal osteoporotic women. Front Endocrinol 12. https://www.frontiersin.org/articles/10.3389/fendo.2021.669704. Accessed 7 Sep 2022
Takashi Y, Kawanami D (2022) The role of bone-derived hormones in glucose metabolism, diabetic kidney disease, and cardiovascular disorders. Int J Mol Sci 23:2376. https://doi.org/10.3390/ijms23042376
Rossi M, Battafarano G, Pepe J, Minisola S, Del Fattore A (2019) The endocrine function of osteocalcin regulated by bone resorption: a lesson from reduced and increased bone mass diseases. Int J Mol Sci 20:4502. https://doi.org/10.3390/ijms20184502
Wei J, Karsenty G (2015) An overview of the metabolic functions of osteocalcin. Rev Endocr Metab Disord 16:93–98. https://doi.org/10.1007/s11154-014-9307-7
Wei J, Hanna T, Suda N, Karsenty G, Ducy P (2014) Osteocalcin promotes β-cell proliferation during development and adulthood through Gprc6a. Diabetes 63:1021–1031. https://doi.org/10.2337/db13-0887
Oury F, Sumara G, Sumara O, Ferron M, Chang H, Smith CE, Hermo L, Suarez S, Roth BL, Ducy P, Karsenty G (2011) Endocrine regulation of male fertility by the skeleton. Cell 144:796–809. https://doi.org/10.1016/j.cell.2011.02.004
Mizokami A, Yasutake Y, Gao J, Matsuda M, Takahashi I, Takeuchi H, Hirata M (2013) Osteocalcin induces release of glucagon-like peptide-1 and thereby stimulates insulin secretion in mice. PLoS ONE 8
Mera P, Laue K, Ferron M, Confavreux C, Wei J, Galán-Díez M, Lacampagne A, Mitchell SJ, Mattison JA, Chen Y, Bacchetta J, Szulc P, Kitsis RN, de Cabo R, Friedman RA, Torsitano C, McGraw TE, Puchowicz M, Kurland I, Karsenty G (2016) Osteocalcin signaling in myofibers is necessary and sufficient for optimum adaptation to exercise. Cell Metabol 23:1078–1092. https://doi.org/10.1016/j.cmet.2016.05.004
Otani T, Mizokami A, Hayashi Y, Gao J, Mori Y, Nakamura S, Takeuchi H, Hirata M (2015) Signaling pathway for adiponectin expression in adipocytes by osteocalcin. Cell Signal 27:532–544. https://doi.org/10.1016/j.cellsig.2014.12.018
Khrimian L, Obri A, Ramos-Brossier M, Rousseaud A, Moriceau S, Nicot A-S, Mera P, Kosmidis S, Karnavas T, Saudou F, Gao X-B, Oury F, Kandel E, Karsenty G (2017) Gpr158 mediates osteocalcin’s regulation of cognition. J Exp Med 214:2859–2873. https://doi.org/10.1084/jem.20171320
Ferron M, Hinoi E, Karsenty G, Ducy P (2008) Osteocalcin differentially regulates β cell and adipocyte gene expression and affects the development of metabolic diseases in wild-type mice. Proc Nat Acad Sci 105:5266–5270. https://doi.org/10.1073/pnas.0711119105
Oury F, Khrimian L, Denny CA, Gardin A, Chamouni A, Goeden N, Huang YY, Lee H, Srinivas P, Gao XB, Suyama S, Langer T, John J, Mann TL, Horvath A, Bonnin G (2013) Maternal and offspring pools of osteocalcin influence brain development and functions. Cell 155:228–241. https://doi.org/10.1016/j.cell.2013.08.042.
Li Y, Gu Z, Wang J, Wang Y, Chen X, Dong B (2022) The emerging role of bone-derived hormones in diabetes mellitus and diabetic kidney disease. Front Endocrinol (Lausanne) 13
Burch J, Rice S, Yang H, Neilson A, Stirk L, Francis R, Holloway P, Selby P, Craig D (2014) Systematic review of the use of bone turnover markers for monitoring the response to osteoporosis treatment: the secondary prevention of fractures, and primary prevention of fractures in high-risk groups. Health Technol Assess 18:1–180. https://doi.org/10.3310/hta18110
Lee AJ, Hodges S, Eastell R (2000) Measurement of osteocalcin. Ann Clin Biochem 37:432–446. https://doi.org/10.1177/000456320003700402
Cui R, Su B, Sheng C, Cheng X, Yang P, Bu L, Li H, Wang J, Sheng H, Qu S (2014) Total osteocalcin in serum predicts testosterone level in male type 2 diabetes mellitus. Int J Clin Exp Med 7:1145–1149
Glover SJ, Garnero P, Naylor K, Rogers A, Eastell R (2008) Establishing a reference range for bone turnover markers in young, healthy women. Bone 42:623–630. https://doi.org/10.1016/j.bone.2007.12.218
Adami S, Bianchi G, Brandi ML, Giannini S, Ortolani S, DiMunno O, Frediani B, Rossini M (2008) On behalf of the BONTURNO study group, determinants of bone turnover markers in healthy premenopausal women. Calcif Tissue Int 82:341–347. https://doi.org/10.1007/s00223-008-9126-5
Hannemann A, Friedrich N, Spielhagen C, Rettig R, Ittermann T, Nauck M, Wallaschofski H (2013) Reference intervals for serum osteocalcin concentrations in adult men and women from the study of health in Pomerania. BMC Endocrine Disord 13:11. https://doi.org/10.1186/1472-6823-13-11
Lee NK, Sowa H, Hinoi E, Ferron M, Ahn JD, Confavreux C, Dacquin R, Mee PJ, McKee MD, Jung DY, Zhang Z, Kim JK, Mauvais-Jarvis F, Ducy P, Karsenty G (2007) Endocrine regulation of energy metabolism by the skeleton. Cell 130:456–469. https://doi.org/10.1016/j.cell.2007.05.047
Gundberg CM, Nieman SD, Abrams S, Rosen H (1998) Vitamin K status and bone health: an analysis of methods for determination of undercarboxylated osteocalcin1. J Clin Endocrinol Metabol 83:3258–3266. https://doi.org/10.1210/jcem.83.9.5126
Lacombe J, Al Rifai O, Loter L, Moran T, Turcotte AF, Grenier-Larouche T, Tchernof A, Biertho L, Carpentier AC, Prud’homme D, Rabasa-Lhoret R, Karsenty G, Gagnon C, Jiang W, Ferron M (2020) Measurement of bioactive osteocalcin in humans using a novel immunoassay reveals association with glucose metabolism and β-cell function. Am J Physiol Endocrinol Metab 318:E381–E391. https://doi.org/10.1152/ajpendo.00321.2019.
Komori T (2020) Functions of osteocalcin in bone, pancreas, testis, and muscle. Int J Mol Sci 21:7513. https://doi.org/10.3390/ijms21207513
Wang JS, Mazur CM, Wein MN (2021) Sclerostin and osteocalcin: candidate bone-produced hormones. Front Endocrinol (Lausanne) 12
Liu Y, Liu X, Lewis JR, Brock K, Brennan-Speranza TC, Teixeira-Pinto A (2019) Relationship between serum osteocalcin/undercarboxylated osteocalcin and type 2 diabetes: a systematic review/meta-analysis study protocol. BMJ Open 9
Rubert M, De la Piedra C, Rubert M, De la Piedra C (2020) La osteocalcina: de marcador de formación ósea a hormona; y el hueso, un órgano endocrino. Revista de Osteoporosis y Metabolismo Mineral 12:146–151. https://doi.org/10.4321/s1889-836x2020000400007
UniProt Consortium (2023) UniProt: The universal protein knowledgebase in 2023. Nucleic Acids Res 51:D523–D531. https://doi.org/10.1093/nar/gkac1052
Zoch ML, Clemens TL, Riddle RC (2016) New insights into the biology of osteocalcin. Bone 82:42–49. https://doi.org/10.1016/j.bone.2015.05.046
Al Rifai O, Chow J, Lacombe J, Julien C, Faubert D, Susan-Resiga D, Essalmani R, Creemers JW, Seidah NG, Ferron M (2017) Proprotein convertase furin regulates osteocalcin and bone endocrine function. J Clin Invest 127:4104–4117. https://doi.org/10.1172/JCI93437.
Lambert LJ, Challa AK, Niu A, Zhou L, Tucholski J, Johnson MS, Nagy TR, Eberhardt AW, Estep PN, Kesterson RA, Grams JM (2016) Increased trabecular bone and improved biomechanics in an osteocalcin-null rat model created by CRISPR/Cas9 technology. Dis Models Mechan 9:1169–1179. https://doi.org/10.1242/dmm.025247
Rahman S, Oberdorf A, Montecino M, Tanhauser SM, Lian JB, Stein GS, Laipis PJ, Stein JL (1993) Multiple copies of the bone-specific osteocalcin gene in mouse and rat. Endocrinology 133:3050–3053. https://doi.org/10.1210/endo.133.6.8243336
Desbois C, Hogue DA, Karsenty G (1994) The mouse osteocalcin gene cluster contains three genes with two separate spatial and temporal patterns of expression. J Biol Chem 269:1183–1190
Sato M, Tada N (1995) Preferential expression of osteocalcin-related protein mRNA in gonadal tissues of male mice. Biochem Biophys Res Commun 215:412–421. https://doi.org/10.1006/bbrc.1995.2480
Komori T (2019) Regulation of proliferation, differentiation and functions of osteoblasts by runx 2. Int J Mol Sci 20:E1694. https://doi.org/10.3390/ijms20071694
Komori T, Yagi H, Nomura S, Yamaguchi A, Sasaki K, Deguchi K, Shimizu Y, Bronson RT, Gao Y-H, Inada M, Sato M, Okamoto R, Kitamura Y, Yoshiki S, Kishimoto T (1997) Targeted disruption of cbfa1 results in a complete lack of bone formation owing to maturational arrest of osteoblasts. Cell 89:755–764. https://doi.org/10.1016/S0092-8674(00)80258-5
Banerjee C, McCabe LR, Choi J-Y, Hiebert SW, Stein JL, Stein GS, Lian JB (1997) Runt homology domain proteins in osteoblast differentiation: AML3/CBFA1 is a major component of a bone-specific complex. J Cellular Biochem 66:1–8. https://doi.org/10.1002/(SICI)1097-4644(19970701)66:1<1::AID-JCB1>3.0.CO;2-V
Ducy P, Zhang R, Geoffroy V, Ridall AL, Karsenty G (1997) Osf2/Cbfa1: A Transcriptional Activator of Osteoblast Differentiation. Cell 89:747–754. https://doi.org/10.1016/S0092-8674(00)80257-3
Harada H, Tagashira S, Fujiwara M, Ogawa S, Katsumata T, Yamaguchi A, Komori T, Nakatsuka M (1999) Cbfa1 isoforms exert functional differences in osteoblast differentiation. J Biol Chem 274:6972–6978. https://doi.org/10.1074/jbc.274.11.6972
Ducy P, Desbois C, Boyce B, Pinero G, Story B, Dunstan C, Smith E, Bonadio J, Goldstein S, Gundberg C, Bradley A, Karsenty G (1996) Increased bone formation in osteocalcin-deficient mice. Nature 382:448–452. https://doi.org/10.1038/382448a0
Diegel CR, Hann S, Ayturk UM, Hu JC, Lim KE, Droscha CJ, Madaj ZB, Foxa GE, Izaguirre I, Transgenics Core VV, Paracha N,Pidhaynyy B, Dowd TL, Robling AG, Warman ML, Williams BO (2020) An osteocalcin-deficient mouse strain without endocrine abnormalities. PLOS Gen 16:e1008361. https://doi.org/10.1371/journal.pgen.1008361.
Lin X, Xu Y, Pan X, Xu J, Ding Y, Sun X, Song X, Ren Y, Shan P-F (2020) Global, regional, and national burden and trend of diabetes in 195 countries and territories: an analysis from 1990 to 2025. Sci Rep. 10:14790. https://doi.org/10.1038/s41598-020-71908-9
Lv Q, Li Z, Sui A, Yang X, Han Y, Yao R (2022) The role and mechanisms of gut microbiota in diabetic nephropathy, diabetic retinopathy and cardiovascular diseases. Front Microbiol. 13. https://doi.org/10.3389/fmicb.2022.977187
Martiniakova M, Blahova J, Kovacova V, Babikova M, Mondockova V, Kalafova A, Capcarova M, Omelka R (2021) Bee bread can alleviate lipid abnormalities and impaired bone morphology in obese zucker diabetic rats. Molecules 26:2616. https://doi.org/10.3390/molecules26092616
Blahova J, Martiniakova M, Babikova M, Kovacova V, Mondockova V, Omelka R (2021) Pharmaceutical drugs and natural therapeutic products for the treatment of type 2 diabetes mellitus. Pharmaceuticals. 14:806. https://doi.org/10.3390/ph14080806
Pi M, Chen L, Huang M-Z, Zhu W, Ringhofer B, Luo J, Christenson L, Li B, Zhang J, Jackson PD, Faber P, Brunden KR, Harrington JJ, Quarles LD (2008) GPRC6A null mice exhibit osteopenia. Feminization and Metabolic Syndrome, PLOS ONE. 3. https://doi.org/10.1371/journal.pone.0003858
Abdallah BM, Ditzel N, Laborda J, Karsenty G, Kassem M (2015) DLK1 regulates whole-body glucose metabolism: A negative feedback regulation of the osteocalcin-insulin loop. Diabetes. 64:3069–3080. https://doi.org/10.2337/db14-1642
Lin X, Parker L, Mclennan E, Zhang X, Hayes A, McConell G, Brennan-Speranza TC, Levinger I (2017) Recombinant uncarboxylated osteocalcin per se enhances mouse skeletal muscle glucose uptake in both extensor digitorum longus and soleus muscles. Front Endocrinol (Lausanne). 8:330. https://doi.org/10.3389/fendo.2017.00330
Levinger I, Lin X, Zhang X, Brennan-Speranza TC, Volpato B, Hayes A, Jerums G, Seeman E, McConell G (2016) The effects of muscle contraction and recombinant osteocalcin on insulin sensitivity ex vivo. Osteoporos Int. 27:653–663. https://doi.org/10.1007/s00198-015-3273-0
Zhang X-L, Wang Y-N, Ma L-Y, Liu Z-S, Ye F, Yang J-H (2020) Uncarboxylated osteocalcin ameliorates hepatic glucose and lipid metabolism in KKAy mice via activating insulin signaling pathway. Acta Pharmacol Sin. 41:383–393. https://doi.org/10.1038/s41401-019-0311-z
Kunutsor SK, Apekey TA, Laukkanen JA (2015) Association of serum total osteocalcin with type 2 diabetes and intermediate metabolic phenotypes: systematic review and meta-analysis of observational evidence. Eur J Epidemiol. 30:599–614. https://doi.org/10.1007/s10654-015-0058-x
Liu C, Wo J, Zhao Q, Wang Y, Wang B, Zhao W (2015) Association between serum total osteocalcin level and type 2 diabetes mellitus: A systematic review and meta-analysis. Horm Metab Res. 47:813–819. https://doi.org/10.1055/s-0035-1564134
Lin X, Parker L, McLennan E, Hayes A, McConell G, Brennan-Speranza TC, Levinger I (2019) Undercarboxylated osteocalcin improves insulin-stimulated glucose uptake in muscles of corticosterone-treated mice. J Bone Miner Res. 34:1517–1530. https://doi.org/10.1002/jbmr.3731
Ferron M, McKee MD, Levine RL, Ducy P, Karsenty G (2012) Intermittent injections of osteocalcin improve glucose metabolism and prevent type 2 diabetes in mice. Bone. 50:568–575. https://doi.org/10.1016/j.bone.2011.04.017
Zhou B, Li H, Xu L, Zang W, Wu S, Sun H (2013) Osteocalcin reverses endoplasmic reticulum stress and improves impaired insulin sensitivity secondary to diet-induced obesity through nuclear factor-κB signaling pathway. Endocrinology. 154:1055–1068. https://doi.org/10.1210/en.2012-2144
Brennan-Speranza TC, Henneicke H, Gasparini SJ, Blankenstein KI, Heinevetter U, Cogger VC, Svistounov D, Zhang Y, Cooney GJ, Buttgereit F, Dunstan CR, Gundberg C, Zhou H, Seibel MJ (2012) Osteoblasts mediate the adverse effects of glucocorticoids on fuel metabolism. J Clin Invest. 122:4172–4189. https://doi.org/10.1172/JCI63377
Zhou B, Li H, Liu J, Xu L, Zang W, Wu S, Sun H (2013) Intermittent injections of osteocalcin reverse autophagic dysfunction and endoplasmic reticulum stress resulting from diet-induced obesity in the vascular tissue via the NFκB-p65-dependent mechanism. Cell Cycle. 12:1901–1913. https://doi.org/10.4161/cc.24929
Liang Y, Tan A, Liang D, Yang X, Liao M, Gao Y, Jiang Y, Yao Z, Lin X, Lu Z, Wu C, Zhang S, Hu Y, Qin X, Mo Z, Li H, Zhang H (2016) Low osteocalcin level is a risk factor for impaired glucose metabolism in a Chinese male population. J Diabetes Investig. 7:522–528. https://doi.org/10.1111/jdi.12439
Rosato MT, Schneider SH, Shapses SA (1998) Bone Turnover and Insulin-like Growth Factor I Levels Increase After Improved Glycemic Control in Noninsulin-dependent Diabetes Mellitus. Calcif Tissue Int. 63:107–111. https://doi.org/10.1007/s002239900498
Akin O, Göl K, Aktürk M, Erkaya S (2003) Evaluation of bone turnover in postmenopausal patients with type 2 diabetes mellitus using biochemical markers and bone mineral density measurements. Gynecological Endocrinology. 17:19–29. https://doi.org/10.1080/gye.17.1.19.29
Achemlal L, Tellal S, Rkiouak F, Nouijai A, Bezza A, Derouiche EM, Ghafir D, El Maghraoui A (2005) Bone metabolism in male patients with type 2 diabetes. Clin Rheumatol. 24:493–496. https://doi.org/10.1007/s10067-004-1070-9
Im J-A, Yu B-P, Jeon JY, Kim S-H (2008) Relationship between osteocalcin and glucose metabolism in postmenopausal women. Clinica Chimica Acta. 396:66–69. https://doi.org/10.1016/j.cca.2008.07.001
Zhou M, Ma X, Li H, Pan X, Tang J, Gao Y, Hou X, Lu H, Bao Y, Jia W (2009) Serum osteocalcin concentrations in relation to glucose and lipid metabolism in Chinese individuals. European Journal of Endocrinology. 161:723–729. https://doi.org/10.1530/EJE-09-0585
Kindblom JM, Ohlsson C, Ljunggren Ö, Karlsson MK, Tivesten Å, Smith U, Mellström D (2009) Plasma Osteocalcin Is Inversely Related to Fat Mass and Plasma Glucose in Elderly Swedish Men, Journal of Bone and Mineral. Research. 24:785–791. https://doi.org/10.1359/jbmr.081234
Zhou Y, Li Y, Zhang D, Wang J, Yang H (2010) Prevalence and predictors of osteopenia and osteoporosis in postmenopausal Chinese women with type 2 diabetes. Diabetes Research and Clinical Practice. 90:261–269. https://doi.org/10.1016/j.diabres.2010.09.013
Yeap BB, Alfonso H, Chubb SAP, Gauci R, Byrnes E, Beilby JP, Ebeling PR, Handelsman DJ, Allan CA, Grossmann M, Norman PE, Flicker L (2015) Higher serum undercarboxylated osteocalcin and other bone turnover markers are associated with reduced diabetes risk and lower estradiol concentrations in older men. J Clin Endocrinol Metabol 100:63–71. https://doi.org/10.1210/jc.2014-3019
Urano T, Shiraki M, Kuroda T, Tanaka S, Urano F, Uenishi K, Inoue S (2018) Low serum osteocalcin concentration is associated with incident type 2 diabetes mellitus in Japanese women. J Bone Miner Metab. 36:470–477. https://doi.org/10.1007/s00774-017-0857-0
Florez H, Hernández-Rodríguez J, Carrasco JL, Filella X, Prieto-González S, Monegal A, Guañabens N, Peris P (2022) Low serum osteocalcin levels are associated with diabetes mellitus in glucocorticoid treated patients. Osteoporos Int 33:745–750. https://doi.org/10.1007/s00198-021-06167-z
Ye X, Yu R, Jiang F, Hou X, Wei L, Bao Y, Jia W (2022) Osteocalcin and Risks of Incident Diabetes and Diabetic Kidney Disease: A 4.6-Year Prospective Cohort Study. Diabetes Care 45:830–836. https://doi.org/10.2337/dc21-2113.
Gennari L, Merlotti D, Valenti R, Ceccarelli E, Ruvio M, Pietrini MG, Capodarca C, Franci MB, Campagna MS, Calabrò A, Cataldo D, Stolakis K, Dotta F, Nuti R (2012) Circulating sclerostin levels and bone turnover in type 1 and type 2 diabetes. J Clin Endocrinol Metabol 97:1737–1744. https://doi.org/10.1210/jc.2011-2958
Buday B, Pach FP, Literati-Nagy B, Vitai M, Vecsei Z, Koranyi L (2013) Serum osteocalcin is associated with improved metabolic state via adiponectin in females versus testosterone in males. Gender specific nature of the bone–energy homeostasis axis. Bone 57:98–104. https://doi.org/10.1016/j.bone.2013.07.018.
Zeng H, Ge J, Xu W, Ma H, Chen L, Xia M, Pan B, Lin H, Wang S, Gao X (2021) Type 2 diabetes is causally associated with reduced serum osteocalcin: A genomewide association and mendelian randomization study. J Bone Miner Res. 36:1694–1707. https://doi.org/10.1002/jbmr.4330
Iki M, Tamaki J, Fujita Y, Kouda K, Yura A, Kadowaki E, Sato Y, Moon JS, Tomioka K, Okamoto N, Kurumatani N (2012) Serum undercarboxylated osteocalcin levels are inversely associated with glycemic status and insulin resistance in an elderly Japanese male population: Fujiwara-kyo Osteoporosis Risk in Men (FORMEN) Study. Osteoporos Int. 23:761–770. https://doi.org/10.1007/s00198-011-1600-7
Bulló M, Moreno-Navarrete JM, Fernández-Real JM, Salas-Salvadó J (2012) Total and undercarboxylated osteocalcin predict changes in insulin sensitivity and β cell function in elderly men at high cardiovascular risk. Am J Clin Nutr 95:249–255. https://doi.org/10.3945/ajcn.111.016642
Samadfam R, Richard C, Nguyen-Yamamoto L, Bolivar I, Goltzman D (2009) Bone formation regulates circulating concentrations of fibroblast growth factor 23. Endocrinology. 150:4835–4845. https://doi.org/10.1210/en.2009-0472
Díaz-López A, Bulló M, Juanola-Falgarona M, Martínez-González MA, Estruch R, Covas M-I, Arós F, Salas-Salvadó J (2013) Reduced serum concentrations of carboxylated and undercarboxylated osteocalcin are associated with risk of developing type 2 diabetes mellitus in a high cardiovascular risk population: A nested case-control study. J Clin Endocrinol Metabol 98:4524–4531. https://doi.org/10.1210/jc.2013-2472
Razny U, Fedak D, Kiec-Wilk B, Goralska J, Gruca A, Zdzienicka A, Kiec-Klimczak M, Solnica B, Hubalewska-Dydejczyk A, Malczewska-Malec M (2017) Carboxylated and undercarboxylated osteocalcin in metabolic complications of human obesity and prediabetes. Diabetes/Metabolism Res Rev 33
Sanchez-Enriquez S, Ballesteros-Gonzalez IT, Villafán-Bernal JR, Pascoe-Gonzalez S, Rivera-Leon EA, Bastidas-Ramirez BE, Rivas-Carrillo JD, Alcala-Zermeno JL, Armendariz-Borunda J, Llamas-Covarrubias IM, Zepeda-Moreno A (2017) Serum levels of undercarboxylated osteocalcin are related to cardiovascular risk factors in patients with type 2 diabetes mellitus and healthy subjects, World. J Diabetes. 8:11–17. https://doi.org/10.4239/wjd.v8.i1.11
Hu J, Han J, Jin M, Jin J, Zhu J (2023) Effects of metformin on bone mineral density and bone turnover markers: a systematic review and meta-analysis. BMJ Open. 13. https://doi.org/10.1136/bmjopen-2023-072904
Vianna AG, de Lacerda CS, Pechmann LM, Polesel MG, Marino EC, Borba VZ, Barreto FD (2017) Vildagliptin has the same safety profile as a sulfonylurea on bone metabolism and bone mineral density in post-menopausal women with type 2 diabetes: a randomized controlled trial. Diabetol Metab Syndr 9:35. https://doi.org/10.1186/s13098-017-0232-2.
Hegazy SK (2015) Evaluation of the anti-osteoporotic effects of metformin and sitagliptin in postmenopausal diabetic women. J Bone Miner Metab. 33:207–212. https://doi.org/10.1007/s00774-014-0581-y
Berberoglu Z, Yazici AC, Demirag NG (2010) Effects of rosiglitazone on bone mineral density and remodelling parameters in Postmenopausal diabetic women: a 2-year follow-up study. Clin Endocrinol (Oxf). 73:305–312. https://doi.org/10.1111/j.1365-2265.2010.03784.x
Berberoglu Z, Gursoy A, Bayraktar N, Yazici AC, Bascil Tutuncu N, Guvener Demirag N (2007) Rosiglitazone decreases serum bone-specific alkaline phosphatase activity in postmenopausal diabetic women. J Clin Endocrinol Metab 92:3523–3530. https://doi.org/10.1210/jc.2007-0431.
Kanazawa I, Yamaguchi T, Yano S, Yamamoto M, Yamauchi M, Kurioka S, Sugimoto T (2010) Baseline atherosclerosis parameter could assess the risk of bone loss during pioglitazone treatment in type 2 diabetes mellitus. Osteoporos Int. 21:2013–2018. https://doi.org/10.1007/s00198-009-1161-1
Namvaran F, Rahimi-Moghaddam P, Azarpira N, Dabbaghmanesh MH, Bakhshayeshkaram M, Namvaran MM (2013) Changes in bone biological markers after treatment of Iranian diabetic patients with pioglitazone: No relation to polymorphism of PPAR-γ (Pro12Ala). J Res Med Sci. 18:277–282
Sakamoto J, Kimura H, Moriyama S, Odaka H, Momose Y, Sugiyama Y, Sawada H (2000) Activation of human peroxisome proliferator-activated receptor (PPAR) subtypes by pioglitazone. Biochem Biophys Res Commun. 278:704–711. https://doi.org/10.1006/bbrc.2000.3868
Kaji H, Kuroki Y, Murakawa Y, Funakawa I, Funasaka Y, Kanda F, Sugimoto T (2010) Effect of alendronate on bone metabolic indices and bone mineral density in patients treated with high-dose glucocorticoid: a prospective study. Osteoporos Int. 21:1565–1571. https://doi.org/10.1007/s00198-009-1110-z
Yamauchi M, Yamaguchi T, Nawata K, Takaoka S, Sugimoto T (2010) Relationships between undercarboxylated osteocalcin and vitamin K intakes, bone turnover, and bone mineral density in healthy women. Clin Nutr. 29:761–765. https://doi.org/10.1016/j.clnu.2010.02.010
Karimi Fard M, Aminorroaya A, Kachuei A, Salamat MR, Hadi Alijanvand M, Aminorroaya Yamini S, Karimifar M, Feizi A, Amini M (2019) Alendronate improves fasting plasma glucose and insulin sensitivity, and decreases insulin resistance in prediabetic osteopenic postmenopausal women: A randomized triple-blind clinical trial. Diabetes Investig 10:731–737. https://doi.org/10.1111/jdi.12944.
Schwartz AV, Schafer AL, Grey A, Vittinghoff E, Palermo L, Lui L-YL, Wallace RB, Cummings SR, Black DM, Bauer DC, Reid IR (2013) Effects of antiresorptive therapies on glucose metabolism: results from the FIT, HORIZON-PFT, and FREEDOM trials. J Bone Miner Res. 28:1348–1354. https://doi.org/10.1002/jbmr.1865
Toulis KA, Nirantharakumar K, Ryan R, Marshall T, Hemming K (2015) Bisphosphonates and glucose homeostasis: a population-based, retrospective cohort study. J Clin Endocrinol Metab. 100:1933–1940. https://doi.org/10.1210/jc.2014-3481
Vestergaard P, Rejnmark L, Mosekilde L (2011) Are antiresorptive drugs effective against fractures in patients with diabetes? Calcif Tissue Int. 88:209–214. https://doi.org/10.1007/s00223-010-9450-4
Xuan Y, Sun L-H, Liu D-M, Zhao L, Tao B, Wang W-Q, Zhao H-Y, Liu J-M, Ning G (2015) Positive association between serum levels of bone resorption marker CTX and HbA1c in women with normal glucose tolerance. J Clin Endocrinol Metab. 100:274–281. https://doi.org/10.1210/jc.2014-2583
Yang S, Leslie WD, Morin SN, Majumdar SR, Lix LM (2016) Antiresorptive therapy and newly diagnosed diabetes in women: a historical cohort study. Diabetes Obes Metab. 18:875–881. https://doi.org/10.1111/dom.12678
Mazziotti G, Maffezzoni F, Doga M, Hofbauer LC, Adler RA, Giustina A (2014) Outcome of glucose homeostasis in patients with glucocorticoid-induced osteoporosis undergoing treatment with bone active-drugs. Bone. 67:175–180. https://doi.org/10.1016/j.bone.2014.07.008
Lewis JR, Brennan-Speranza TC, Levinger I, Byrnes E, Lim EM, Blekkenhorst LC, Sim M, Hodgson JM, Zhu K, Lim WH, Adams LA, Prince RL (2019) Effects of calcium supplementation on circulating osteocalcin and glycated haemoglobin in older women. Osteoporos Int. 30:2065–2072. https://doi.org/10.1007/s00198-019-05087-3
Hygum K, Starup-Linde J, Harsløf T, Vestergaard P, Langdahl BL (2017) MECHANISMS IN ENDOCRINOLOGY: Diabetes mellitus, a state of low bone turnover – a systematic review and meta-analysis. European Journal of Endocrinology. 176:R137–R157. https://doi.org/10.1530/EJE-16-0652
Krakauer JC, McKenna MJ, Buderer NF, Rao DS, Whitehouse FW, Parfitt AM (1995) Bone loss and bone turnover in diabetes. Diabetes. 44:775–782. https://doi.org/10.2337/diab.44.7.775
van Bommel EJM, de Jongh RT, Brands M, Heijboer AC, den Heijer M, Serlie MJ, van Raalte DH (2018) The osteoblast: Linking glucocorticoid-induced osteoporosis and hyperglycaemia? A post-hoc analysis of a randomised clinical trial, Bone. 112:173–176. https://doi.org/10.1016/j.bone.2018.04.025
Cooper MS, Seibel MJ, Zhou H (2016) Glucocorticoids, bone and energy metabolism. Bone. 82:64–68. https://doi.org/10.1016/j.bone.2015.05.038
Oton-Gonzalez L, Mazziotta C, Iaquinta MR, Mazzoni E, Nocini R, Trevisiol L, D’Agostino A, Tognon M, Rotondo JC, Martini F (2022) Genetics and epigenetics of bone remodeling and metabolic bone diseases. Int J Mol Sci 23:1500. https://doi.org/10.3390/ijms23031500
Martiniakova M, Babikova M, Mondockova V, Blahova J, Kovacova V, Omelka R (2022) The role of macronutrients, micronutrients and flavonoid polyphenols in the prevention and treatment of osteoporosis. Nutrients 14:523. https://doi.org/10.3390/nu14030523
Compston JE, McClung MR, Leslie WD (2019) Osteoporosis. The Lancet. 393:364–376. https://doi.org/10.1016/S0140-6736(18)32112-3
Park SG, Jeong SU, Lee JH, Ryu SH, Jeong HJ, Sim YJ, Kim DK, Kim GC (2018) The Changes of CTX. DPD, Osteocalcin, and Bone Mineral Density During the Postmenopausal Period, Ann Rehabil Med. 42:441–448. https://doi.org/10.5535/arm.2018.42.3.441
Boyacioglu O, Orenay-Boyacioglu S, Yildirim H, Korkmaz M (2018) Boron intake, osteocalcin polymorphism and serum level in postmenopausal osteoporosis. J Trace Elem Med Biol. 48:52–56. https://doi.org/10.1016/j.jtemb.2018.03.005
Kim JG, Lee JY (1996) Serum insulin-like growth factor binding protein profiles in postmenopausal women: Their correlation with bone mineral density. Am J Obstetrics Gynecol 174:1511–1517. https://doi.org/10.1016/S0002-9378(96)70598-7
Cabrera CD, Henríquez MS, Traba ML, Villafañe EA, de la Piedra C (1998) Biochemical markers of bone formation in the study of postmenopausal osteoporosis. Osteoporosis Int. 8:147–151. https://doi.org/10.1007/BF02672511
Duman BS, Tanakol R, Erensoy N, Öztürk M, Yilmazer S (2004) Vitamin D receptor alleles, bone mineral density and turnover in postmenopausal osteoporotic and healthy women. Med Princ Pract 13:260–266. https://doi.org/10.1159/000079524
Luo X-H, Guo L-J, Shan P-F, Xie H, Wu X-P, Zhang H, Cao X-Z, Yuan L-Q, Liao E-Y (2006) Relationship of circulating MMP–2, MMP–1, and TIMP–1 levels with bone biochemical markers and bone mineral density in postmenopausal Chinese women. Osteoporos Int. 17:521–526. https://doi.org/10.1007/s00198-005-0017-6
Pouillès J-M, Trémollieres FA, Ribot C (2006) Osteoporosis in otherwise healthy perimenopausal and early postmenopausal women: Physical and biochemical characteristics. Osteoporos Int. 17:193–200. https://doi.org/10.1007/s00198-005-1954-9
Verit FF, Geyikli I, Yazgan P, Celik A (2006) Correlations of serum prolidase activity between bone turnover markers and mineral density in postmenopausal osteoporosis. Arch Gynecol Obstet. 274:133–137. https://doi.org/10.1007/s00404-006-0148-9
Jabbar S, Drury J, Fordham JN, Datta HK, Francis RM, Tuck SP (2011) Osteoprotegerin, RANKL and bone turnover in postmenopausal osteoporosis. J Clin Pathol 64:354–357. https://doi.org/10.1136/jcp.2010.086595
Mondockova V, Adamkovicova M, Lukacova M, Grosskopf B, Babosova R, Galbavy D, Martiniakova M, Omelka R (2018) The estrogen receptor 1 gene affects bone mineral density and osteoporosis treatment efficiency in Slovak postmenopausal women. BMC Med Genet. 19:174. https://doi.org/10.1186/s12881-018-0684-8
Atalay S, Elci A, Kayadibi H, Onder CB, Aka N (2012) Diagnostic utility of osteocalcin, undercarboxylated osteocalcin, and alkaline phosphatase for osteoporosis in premenopausal and postmenopausal women. Ann Lab Med. 32:23–30. https://doi.org/10.3343/alm.2012.32.1.23
Diego EMD, Martín MAD, de la Piedra C, Rapado A (1995) Lack of correlation between levels of osteocalcin and bone alkaline phosphatase in healthy control and postmenopausal osteoporotic women. Horm Metab Res. 27:151–154. https://doi.org/10.1055/s-2007-979928
Vergnaud P, Garnero P, Meunier PJ, Bréart G, Kamihagi K, Delmas PD (1997) Undercarboxylated osteocalcin measured with a specific immunoassay predicts hip fracture in elderly women: The EPIDOS study1. J Clin Endocrinol Metabol 82:719–724. https://doi.org/10.1210/jcem.82.3.3805
Horiuchi T, Kazama H, Araki A, Inoue J, Hosoi T, Onouchi T, Mizuno S, Ito H, Orimo H (2004) Impaired gamma carboxylation of osteocalcin in elderly women with type II diabetes mellitus: relationship between increase in undercarboxylated osteocalcin levels and low bone mineral density. J Bone Miner Metab. 22:236–240. https://doi.org/10.1007/s00774-003-0473-z
Al-Daghri NM, Yakout S, Al-Shehri E, Al-Fawaz H, Aljohani N, Al-Saleh Y (2014) Inflammatory and bone turnover markers in relation to PTH and vitamin D status among Saudi postmenopausal women with and without osteoporosis. Int J Clin Exp Med. 7:2812–2819
Biver E, Chopin F, Coiffier G, Brentano TF, Bouvard B, Garnero P, Cortet B (2012) Bone turnover markers for osteoporotic status assessment? A systematic review of their diagnosis value at baseline in osteoporosis, Joint Bone Spine. 79:20–25. https://doi.org/10.1016/j.jbspin.2011.05.003
Liu Z, Chen R, Jiang Y, Yang Y, He L, Luo C, Dong J, Rong L (2019) A meta-analysis of serum osteocalcin level in postmenopausal osteoporotic women compared to controls. BMC Musculoskeletal Disorders. 20:532. https://doi.org/10.1186/s12891-019-2863-y
Brown JP, Don-Wauchope A, Douville P, Albert C, Vasikaran SD (2022) Current use of bone turnover markers in the management of osteoporosis. Clin Biochem. S0009–9120(22):00204–1. https://doi.org/10.1016/j.clinbiochem.2022.09.002
Xu Y, Shen L, Liu L, Zhang Z, Hu W (2022) Undercarboxylated osteocalcin and its associations with bone mineral density, bone turnover markers, and prevalence of osteopenia and osteoporosis in chinese population: A cross-sectional study. Front Endocrinol 13. https://doi.org/10.3389/fendo.2022.843912.
Szulc P, Arlot M, Chapuy M-C, Duboeuf F, Meunier PJ, Delmas PD (1994) Serum undercarboxylated osteocalcin correlates with hip bone mineral density in elderly women, Journal of Bone and Mineral. Research. 9:1591–1595. https://doi.org/10.1002/jbmr.5650091012
Emaus N, Nguyen ND, Almaas B, Berntsen GK, Center JR, Christensen M, Gjesdal CG, Grimsgaard AS, Nguyen TV, Salomonsen L, Eisman JA, Fønnebø VM (2013) Serum level of under-carboxylated osteocalcin and bone mineral density in early menopausal Norwegian women. Eur J Nutr. 52:49–55. https://doi.org/10.1007/s00394-011-0285-1
Cummings SR, Browner W, Cummings SR, Black DM, Nevitt MC, Browner W, Genant HK, Cauley J, Ensrud K, Scott J, Vogt TM (1993) Bone density at various sites for prediction of hip fractures. The Lancet. 341:72–75. https://doi.org/10.1016/0140-6736(93)92555-8
Sokoll LJ, Sadowski JA (1996) Comparison of biochemical indexes for assessing vitamin K nutritional status in a healthy adult population. The American Journal of Clinical Nutrition. 63:566–573. https://doi.org/10.1093/ajcn/63.4.566
Shiraki M, Itabashi A (2009) Short-term menatetrenone therapy increases gamma-carboxylation of osteocalcin with a moderate increase of bone turnover in postmenopausal osteoporosis: a randomized prospective study. J Bone Miner Metab. 27:333–340. https://doi.org/10.1007/s00774-008-0034-6
Jiang Y, Zhang Z-L, Zhang Z-L, Zhu H-M, Wu Y-Y, Cheng Q, Wu F-L, Xing X-P, Liu J-L, Yu W, Meng X-W (2014) Menatetrenone versus alfacalcidol in the treatment of Chinese postmenopausal women with osteoporosis: a multicenter, randomized, double-blinded, double-dummy, positive drug-controlled clinical trial. Clin Interv Aging. 9:121–127. https://doi.org/10.2147/CIA.S54107
Su S, He N, Men P, Song C, Zhai S (2019) The efficacy and safety of menatetrenone in the management of osteoporosis: a systematic review and meta-analysis of randomized controlled trials. Osteoporos Int. 30:1175–1186. https://doi.org/10.1007/s00198-019-04853-7
Barone LM, Aronow MA, Tassinari MS, Conlon D, Stein GS, Lian JB, Canalis E (1994) Differential effects of warfarin on mRNA levels of developmentally regulated vitamin K dependent proteins, osteocalcin, and matrix Gla protein in vitro. Journal of Cellular Physiology. 160:255–264. https://doi.org/10.1002/jcp.1041600207
Fernández-Real JM, Izquierdo M, Ortega F, Gorostiaga E, Gómez-Ambrosi J, Moreno-Navarrete JM, Frühbeck G, Martínez C, Idoate F, Salvador J, Forga L, Ricart W, Ibañez J (2009) The relationship of serum osteocalcin concentration to insulin secretion, sensitivity, and disposal with hypocaloric diet and resistance training. J Clin Endocrinol Metabol 94:237–245. https://doi.org/10.1210/jc.2008-0270
Kasukawa Y, Miyakoshi N, Ebina T, Aizawa T, Hongo M, Nozaka K, Ishikawa Y, Saito H, Chida S, Shimada Y (2014) Effects of risedronate alone or combined with vitamin K2 on serum undercarboxylated osteocalcin and osteocalcin levels in postmenopausal osteoporosis. J Bone Miner Metab. 32:290–297. https://doi.org/10.1007/s00774-013-0490-5
Lasco A, Morabito N, Basile G, Atteritano M, Gaudio A, Giorgianni GM, Morini E, Faraci B, Bellone F, Catalano A (2016) Denosumab Inhibition of RANKL and Insulin Resistance in Postmenopausal Women with Osteoporosis. Calcif Tissue Int. 98:123–128. https://doi.org/10.1007/s00223-015-0075-5
Schafer AL, Sellmeyer DE, Schwartz AV, Rosen CJ, Vittinghoff E, Palermo L, Bilezikian JP, Shoback DM, Black DM (2011) Change in undercarboxylated osteocalcin is associated with changes in body weight, fat mass, and adiponectin: Parathyroid hormone (1–84) or alendronate therapy in postmenopausal women with osteoporosis (the PaTH Study). J Clin Endocrinol Metabol 96:E1982–E1989. https://doi.org/10.1210/jc.2011-0587
Cheng C-H, Chen L-R, Chen K-H (2022) Osteoporosis due to hormone imbalance: An overview of the effects of estrogen deficiency and glucocorticoid overuse on bone turnover. Int J Mol Sci 23:1376. https://doi.org/10.3390/ijms23031376
Reid IR, Chapman GE, Fraser TR, Davies AD, Surus AS, Meyer J, Huq NL, Ibbertson HK (1986) Low serum osteocalcin levels in glucocorticoid-treated asthmatics. J Clin Endocrinol Metab. 62:379–383. https://doi.org/10.1210/jcem-62-2-379
Prummel MF, Wiersinga WM, Lips P, Sanders GT, Sauerwein HP (1991) The course of biochemical parameters of bone turnover during treatment with corticosteroids. J Clin Endocrinol Metab. 72:382–386. https://doi.org/10.1210/jcem-72-2-382
Shikano K, Kaneko K, Kawazoe M, Kaburaki M, Hasunuma T, Kawai S (2016) Efficacy of vitamin K2 for glucocorticoid-induced osteoporosis in patients with systemic autoimmune diseases. Intern Med 55:1997–2003. https://doi.org/10.2169/internalmedicine.55.6230
Wu CC, Econs MJ, DiMeglio LA, Insogna KL, Levine MA, Orchard PJ, Miller WP, Petryk A, Rush ET, Shoback DM, Ward LM, Polgreen LE (2017) Diagnosis and management of osteopetrosis: Consensus guidelines from the osteopetrosis working group. J Clin Endocrinol Metabol 102:3111–3123. https://doi.org/10.1210/jc.2017-01127
Burr DB, Allen MR (2019) Basic and applied bone biology, 2nd ed., Academic Press
Del Fattore A, Cappariello A, Teti A (2008) Genetics, pathogenesis and complications of osteopetrosis. Bone. 42:19–29. https://doi.org/10.1016/j.bone.2007.08.029
Bollerslev J, Marks SC, Mosekilde L, Lian JB, Stein GS, Mosekilde L (1994) Cortical bone osteocalcin content and matrix composition in autosomal dominant osteopetrosis type I. Eur J Endocrinol. 130:592–594. https://doi.org/10.1530/eje.0.1300592
Ferron M, Wei J, Yoshizawa T, Del Fattore A, DePinho RA, Teti A, Ducy P, Karsenty G (2010) Insulin signaling in osteoblasts integrates bone remodeling and energy metabolism. Cell. 142:296–308. https://doi.org/10.1016/j.cell.2010.06.003
Cournot G, Trubert-Thil CL, Petrovic M, Boyle A, Cormier C, Girault D, Fischer A, Garabedian M (1992) Mineral metabolism in infants with malignant osteopetrosis: Heterogeneity in plasma 1,25-dihydroxyvitamin D levels and bone histology, Journal of Bone and Mineral. Research. 7:1–10. https://doi.org/10.1002/jbmr.5650070103
Bihlet AR, Byrjalsen I, Bay-Jensen A-C, Andersen JR, Christiansen C, Riis BJ, Karsdal MA (2019) Associations between biomarkers of bone and cartilage turnover, gender, pain categories and radiographic severity in knee osteoarthritis. Arthritis Res Ther. 21:203. https://doi.org/10.1186/s13075-019-1987-7
Zemanova N, Omelka R, Mondockova V, Kovacova V, Martiniakova M (2022) Roles of gut microbiome in bone homeostasis and its relationship with bone-related diseases. Biology 11:1402. https://doi.org/10.3390/biology11101402
Briot K, Geusens P, Em Bultink I, Lems WF, Roux C (2017) Inflammatory diseases and bone fragility. Osteoporos Int 28:3301–3314. https://doi.org/10.1007/s00198-017-4189-7.
Roux C (2011) Osteoporosis in inflammatory joint diseases. Osteoporos Int. 22:421–433. https://doi.org/10.1007/s00198-010-1319-x
Arden N, Nevitt MC (2006) Osteoarthritis: Epidemiology, best practice & research. Clin Rheumatol 20:3–25. https://doi.org/10.1016/j.berh.2005.09.007
Wei Z, Li F, Pi G (2022) Association between gut microbiota and osteoarthritis: a review of evidence for potential mechanisms and therapeutics. Front Cell Infect Microbiol 12
Campion GV, Delmas PD, Dieppe PA (1989) Serum and synovial fluid osteocalcin (bone gla protein) levels in joint disease. Rheumatology. 28:393–398. https://doi.org/10.1093/rheumatology/28.5.393
Naito K, Watari T, Obayashi O, Katsube S, Nagaoka I, Kaneko K (2012) Relationship between serum undercarboxylated osteocalcin and hyaluronan levels in patients with bilateral knee osteoarthritis. Int J Mol Med 29:756–760. https://doi.org/10.3892/ijmm.2012.897
Booth SL, Tucker KL, Chen H, Hannan MT, Gagnon DR, Cupples LA, Wilson PW, Ordovas J, Schaefer EJ, Dawson-Hughes B, Kiel DP (2000) Dietary vitamin K intakes are associated with hip fracture but not with bone mineral density in elderly men and women. Am J Clin Nutr 71:1201–1208. https://doi.org/10.1093/ajcn/71.5.1201
Pullig O, Weseloh G, Ronneberger D-L, Käkönen S-M, Swoboda B (2000) Chondrocyte differentiation in human osteoarthritis: Expression of osteocalcin in normal and osteoarthritic cartilage and bone. Calcif Tissue Int 67:230–240. https://doi.org/10.1007/s002230001108
Karsdal MA, Byrjalsen I, Alexandersen P, Bihlet A, Andersen JR, Riis BJ, Bay-Jensen AC, Christiansen C (2015) CSMC021C2301/2 investigators, Treatment of symptomatic knee osteoarthritis with oral salmon calcitonin: results from two phase 3 trials. Osteoarthritis Cartilage. 23:532–543. https://doi.org/10.1016/j.joca.2014.12.019
McInnes IB, Schett G (2011) The pathogenesis of rheumatoid arthritis. New England J Med 365:2205–2219. https://doi.org/10.1056/NEJMra1004965
Seriolo B, Ferretti V, Sulli A, Caratto E, Fasciolo D, Cutolo M (2002) Serum osteocalcin levels in premenopausal rheumatoid arthritis patients. Ann N Y Acad Sci. 966:502–507. https://doi.org/10.1111/j.1749-6632.2002.tb04254.x
Igarashi M, Yogiashi Y, Mihara M, Takada I, Kitagawa H, Kato S (2007) Vitamin K induces osteoblast differentiation through pregnane X receptor-mediated transcriptional control of the Msx2 gene. Mol Cell Biol. 27:7947–7954. https://doi.org/10.1128/MCB.00813-07
Peretz A, Praet JP, Rozenberg S, Bosson D, Famaey JP, Bourdoux P (1989) Osteocalcin and bone mineral content in rheumatoid arthritis. Clin Rheumatol. 8:42–48. https://doi.org/10.1007/BF02031067
Tamai H, Nishina N, Kikuchi J, Izumi K, Otomo K, Yoshimoto K, Yamaoka K, Takeuchi T, Kaneko Y (2022) Serum cytokines and bone metabolic markers in patients with rheumatoid arthritis treated with biological disease modifying anti-rheumatic drugs. Clin Rheumatol. https://doi.org/10.1007/s10067-022-06390-x
Jumper J, Evans R, Pritzel A, Green T, Figurnov M, Ronneberger O, Tunyasuvunakool K, Bates R, Žídek A, Potapenko A, Bridgland A, Meyer C, Kohl SAA, Ballard AJ, Cowie A, Romera-Paredes B, Nikolov S, Jain R, Adler J, Back T, Petersen S, Reiman D, Clancy E, Zielinski M, Steinegger M, Pacholska M, Berghammer T, Bodenstein S, Silver D, Vinyals O, Senior AW, Kavukcuoglu K, Kohli P, Hassabis D (2021) Highly accurate protein structure prediction with AlphaFold. Nature. 596:583–589. https://doi.org/10.1038/s41586-021-03819-2
Varadi M, Anyango S, Deshpande M, Nair S, Natassia C, Yordanova G, Yuan D, Stroe O, Wood G, Laydon A, Žídek A, Green T, Tunyasuvunakool K, Petersen S, Jumper J, Clancy E, Green R, Vora A, Lutfi M, Figurnov M, Cowie A, Hobbs N, Kohli P, Kleywegt G, Birney E, Hassabis D, Velankar S (2022) AlphaFold Protein Structure Database: massively expanding the structural coverage of protein-sequence space with high-accuracy models. Nucleic Acids Res. 50:D439–D444. https://doi.org/10.1093/nar/gkab1061
Szklarczyk D, Kirsch R, Koutrouli M, Nastou K, Mehryary F, Hachilif R, Gable AL, Fang T, Doncheva NT, Pyysalo S, Bork P, Jensen LJ, von Mering C, The STRING, database in, (2023) protein-protein association networks and functional enrichment analyses for any sequenced genome of interest. Nucleic Acids Res. 51(2023):D638–D646. https://doi.org/10.1093/nar/gkac1000
Bilezikian JP, Watts NB, Usiskin K, Polidori D, Fung A, Sullivan D, Rosenthal N (2016) Evaluation of bone mineral density and bone biomarkers in patients with type 2 diabetes treated with canagliflozin. J Clin Endocrinol Metab 101:44–51. https://doi.org/10.1210/jc.2015-1860
Rau M, Thiele K, Hartmann N-UK, Möllmann J, Wied S, Hohl M, Marx N, Lehrke M (2022) Effects of empagliflozin on markers of calcium and phosphate homeostasis in patients with type 2 diabetes - Data from a randomized, placebo-controlled study. Bone Rep. 16. https://doi.org/10.1016/j.bonr.2022.101175
Funding
Open access funding provided by The Ministry of Education, Science, Research and Sport of the Slovak Republic in cooperation with Centre for Scientific and Technical Information of the Slovak Republic This work was supported by the Ministry of Education, Science, Research and Sport of the Slovak Republic, grant numbers VEGA 1/0416/22 and VEGA 1/0328/24.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. M. Martiniakova and R. Omelka were responsible for conceptualization, methodology, supervision, writing – original draft, writing – review & editing, and funding acquisition. R. Biro was responsible for formal analysis and visualization. V. Kovacova and M. Babikova were responsible for formal analysis. N. Zemanova and V. Mondockova were responsible for visualization. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval, consent to participate, and consent to publish
Not applicable.
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Martiniakova, M., Biro, R., Kovacova, V. et al. Current knowledge of bone-derived factor osteocalcin: its role in the management and treatment of diabetes mellitus, osteoporosis, osteopetrosis and inflammatory joint diseases. J Mol Med 102, 435–452 (2024). https://doi.org/10.1007/s00109-024-02418-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-024-02418-8