Abstract
Purpose
The need for spinal instrumented fusion in osteoporotic patients is rising. In this review, we try to give an overview of the current spectrum of pedicle screw augmentation techniques, safety aspects and indications.
Methods
Review of literature and discussion of indications, limitations and technical aspects.
Results
Various studies have shown higher failure rates in osteoporotic patients, most probably due to reduced bone quality and a poor bone-screw interface. Augmentation of pedicle screws with bone cement, such as polymethylmethacrylate or calcium based cements, is one valid option to enhance fixation if required.
Conclusions
Crucial factors for success in the use of augmented screws are careful patient selection, a proper technique and choice of the ideal cement augmentation option.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis is a common disease in the elderly population and is continually rising. In the US the annual cost for the management of osteoporosis was estimated at $17 billion US [1]. For spine surgeons, it is, therefore, becoming part of their surgical routine to treat osteoporotic patients in need of spinal decompression and instrumented fusion. Successful fusion is more likely with rigid internal fixation [2] and such posterior internal fixation systems (PIFS) undergo important internal constraints resulting in high load bearing requirements for the pedicular screw/bone interface. Various studies have proven that the screw performance is dependent on the bone quality meaning that osteoporotic patients may be predisposed to larger PIFS failure rates [3–5]. Screw loosening techniques, cut out experiments and pullout test have been performed for different bone qualities with a common outcome: good dense quality trabecular bone enhances solid fixation while osteoporotic bone increases implants failure risks [4, 6–11].
Augmentation of the pedicle screw with bone cement, such as polymethylmethacrylate-(PMMA) or calcium-based cements, is one technique to enhance fixation if required.
In this review, we try to give an overview of the current spectrum of pedicle screw augmentation indications and technical aspects affecting the results.
Indications
Generally, there are two different conditions in which augmentation of pedicle screws could be beneficial: osteoporosis and revision surgery.
Osteoporosis
Several biomechanical studies assessed the use of PMMA cement for screw augmentation in osteoporotic bone. In lumbar [12] as well as in the thoracic spine [13], in the ilium [14] and the sacrum [15] there is 1.5- to 2-fold increase in pullout strength and energy to failure comparing augmented with not-augmented screws. After cyclic compressive loading, Hoppe et al. found no difference in screw migration in normal bone but less displacement after augmentation in osteoporotic bone [16], showing that augmentation is just beneficial if required due to insufficient bone stock.
Revision surgery in elderly
Several studies were performed in previously instrumented osteoporotic vertebrae, simulating a revision scenario.
In lumbosacral vertebrae, non-pressurized PMMA injection alone was found to restore secure screw fixation while additional cement pressurization doubled the pullout force [17]. Several similar studies showed restored (“back to baseline”) or even increased axial screw pullout strength for previous instrumented thoracolumbar vertebrae by PMMA [18] and calcium phosphate [19] augmentation.
Cyclic loading tests comparing PMMA-augmented 8- with 6-mm-diameter screws, showed increased initial and final stiffness for the larger diameter screws [20] in revision scenarios.
Technical aspects
Many studies have examined the biomechanical characteristics of primary, osteoporotic posterior lumbar spinal instrumentation. Usually two different tests for biomechanical properties of screw fixation are used: axial pullout tests or cyclic cephalo-caudal toggle displacement. In axial pullout tests, a tensile load is applied to a fixed vertebral body to determine the required force to extract the screw and the energy to failure. Although this method seems not to be the most realistic testing paradigm because resulting constraints into the system are not physiologic [21], axial testing is commonly used due to its simple set-up and consistent results.
Only few studies use quasi-physiological conditions like cyclic toggle displacement. This form of fatigue testing applies bending forces to the screw by displacing it cranially and caudally [16]. This potentially better simulates physiologic screw loading and leads to screw loosening at the tip, which is the common form of failure seen in reality [21, 22]. The specimen is usually fixed in a testing machine. A cyclic compressive force is then applied to the screw heads. Angular displacement can be measured after a certain load cycle, or loading is stopped after a certain displacement is reached.
There are some technical aspects influencing screw purchase. The main factors are injected cement volume, the timing of cementation, the screw type used and the type of cement.
Cement volume
There are several studies comparing the effect of different cement volumes on axial pullout strength. Recent literature shows that volumes around 2–3 cc maximize the initial fixation while a further increase of cement volume does not seem to have a positive effect on pullout strength, but increases the risk for cement extravasation [18, 23]. Only one study [24] compared kypho- and vertebroplasty, using higher cement volumes in the kyphoplasty group, showing a significantly higher pullout strength. If that is due to the higher cement volume or the technique itself could not finally answered.
Timing of cementation
In most studies fixed screw insertion times, immediately after PMMA cement injection, were used. Just few studies [25, 26] compare different cement curing times before screw insertion. In general, if PMMA had not totally solidified before screw placement, no significant differences in pullout strength depending on screw insertion times could be noted.
However looking at the failure mode, the failure is more likely to be at the bone–cement interface in “soft” cement and the screw–cement interface for “hard” cement. This indicates that there my be a better integration of the screw threads and surrounding trabecular bone with the use of “soft” PMMA cement.
No changes could be found for calcium phosphate (CP) cements [27]; however, these cements usually require 24 h to be fully cured. For these cements the effects of small variations in initial curing time are probably too small to be detected on immediate fixation tests.
Screw type and augmentation technique
Beside minor variations there are basically two different augmentation techniques depending on the used screw design.
Firstly, cement is injected into the vertebral body using a standard vertebroplasty or kyphoplasty technique. Afterwards a solid standard pedicle screw is inserted and the cement cures around the screw. The other option is to use a fenestrated or cannulated pedicle screw. In this technique the cement gets injected through the fenestrations in the screw into the vertebral body.
The actual published data are somehow controversial: while all studies found a significant improvement compared to non-augmented vertebrae, some found a higher initial fixation strength and motion reduction in solid screws with cement preinjection [7, 28], other studies showed oppositional results [21, 29]. One advantage of cannulated screws seems to be shorter operation times and lower risks of cement leakage [30], but larger studies are still missing.
The design of the pedicle screw fenestrations (number and position of fenestration) seems to influence fixation strength [31], although final conclusions cannot be made so far.
Cement materials
Polymethylmethacrylate has been commonly used since the 1960s due to its good biocompatibility, minimal complications at long term and relative low costs. But PMMA also may have some disadvantages. Its bone remodeling and osseointegration capacity are limited because it is bioinert. Furthermore as a monomer, cardiovascular complications can occur. Based on that, alterative, calcium-based cement materials like calcium phosphate (CP), calcium sulfate (CS) and calcium triglyceride (CT) have been implemented.
CP converts into hydroxyapatite, and has, due to its osteoconductivity and osteoinductivity, a high potential for bone remodeling and osseointegration [32, 33].
CS and CT can although be used as a bone substitutes but both have some limitations. While CS it is quickly resorbed [34], CT expands during polymerization what may increase the risk of extravasation [35]. Moreover all new cements have a lower viscosity during injection compared to PMMA, which potentially although increases the risk of extravasation. The biggest disadvantage is that they require 24 h for curing and therefore do not provide enhanced fixation at the time of surgery.
While different studies have shown biomechanical benefits for calcium ceramics compared with no augmented screws [36, 37], PMMA often performs better in direct comparison to ceramic cements for enhancing pullout strengths and resistance to failure [19, 35, 38].
Discussion
Many studies have examined the biomechanical characteristics of primary, osteoporotic posterior lumbar spinal instrumentation. Primarily or after failure of spinal instrumentation in osteoporotic spine, screw augmentation may be one option to secure adequate screw purchase in the vertebral body. Nevertheless, the clinical data is spare so far. A “pubmed” search using the search terms “pedicle”, “screw” and “augmentation” reveals actually 220 articles, only 26 of them showing clinical results, most of them case reports or case series! El Saman et al. [39] showed a significant reduction of screw loosening rates in augmented vs. non-augmented screws (4.3 vs. 62.8%) with a lower loss of reduction (1.1° vs. 5°) in the treatment vertebral fractures in the elderly. Similar clinical results were reported by Sawakami et al. in a retrospective study, showing a significant decrease in loss of reduction (3° vs. 7°), higher fusion rates (94 vs. 77%) and less clear zones (29 vs. 71%), as sign for screw loosening, for PMMA-augmented compared to non-augmented screws [40].
In preselected cases a minimal-invasive, percutaneous stabilization, in combination with vertebra or kyphoplasty is a possible option (Fig. 1). In the treatment of fractures in the elderly two different scenarios should be differentiated: osteoporotic vertebral fractures, caused by low energy trauma, which usually can be treated by vertebral bode augmentation, like vertebroplasty or kyphoplasty, alone. On the other hand, vertebral fractures in osteoporotic bone, caused by an adequate trauma, often require dorsal augmented instrumentation in combination with vertebro- or kyphoyplasty.
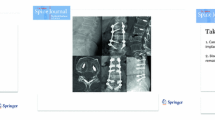
Pincer fracture in an 81-year old female with osteoporosis treated with percutaneous cement augmented dorsal instrumentation with vertebroplasty (a). A.-p. view: Jamshidi needles are placed in the vertebra above and below the fractured one, which is accessed with k-wires only (b). Lateral view: after vertebroplasty of the adjacent segments, guide wires are inserted into the preformed canal, two vertebroplasty needles are placed into the fractured vertebra (c). Then pedicle screws are percutaneously inserted into the augmented vertebra and connected via 2 rods (d). Lateral view after vertebroplasty of the fractured vertebra (e). A.-p. and lateral standing radiographs 2 months postoperatively (f)
Especially in a revision scenario in osteoporotic bone, where a long, more segmental instrumentation is needed, augmentation of pedicle screws might be beneficial. Under cranio-caudal cyclic loading, screw typically cut out through the superior endplate. This so called “windshield-wiper effect” can be typically observed in long instrumentations in osteoporotic bone. The extent of fixation, including the level at which the construct ends, is critical because increased junctional strain at the termination of the construct may lead to accelerated deformity. Moreover, transition points, the cervicothoracic and thoracolumbar junctions, are predisposed to kyphotic collapse, especially in osteoporotic patients. Therefore, multiple points of fixation, above and below the transition zone, should be used. Moreover longer instrumentations have the benefit of a lower failure rates compared to shorter constructs [41]. Additionally, to these biomechanical considerations augmentation is an option to prevent screw pullout and implant failure in these constructs long constructs, revision scenarios or in osteoporotic bone per se (Figs. 2, 3).
An 80-year-old female with sagittal imbalance. Lateral X-ray after posterior stabilization T12-pelvis with pedicle subtraction osteotomy L2 and L4, the instrumentation was stopped at the thoracolumbar junctional zone (a). Lateral X-ray 2 months postoperatively: pullout of T12 pedicle screws (b) Extension of the posterior instrumentation to T4, PMMA augmentation pedicle screws in T10 and T11 (c)
An 82-year-old female with total collapse of a initially conservatively treated L3 fracture. Sagittal CT: collapsed L3 fracture with posterior wall fragments compromising the spinal canal (a). Lateral standing X-ray after posterior open decompression, cement augmented dorsal spondylodesis L1–4 and anterior vertebrectomy and cage implantation L3 (b). Subsidence of the anterior cage into the vertebral body of L4, most probably due to insufficient cement volume in L4 and too short caudal instrumentation (c). Lateral X-ray after extension of the posterior stabilization to the ilium (d)
Conclusions
Polymethylmethacrylate, along with several calcium ceramic materials, are effective materials for enhancing pedicle screw fixation in both osteoporosis and revision spine surgery. This effect is maintained whether the cement is placed first, followed by a solid screw, or the cement is injected through a cannulated screw. Regardless of the technique, there is a remaining risks of cement extravasation into the venous system, spinal canal, or disk space. Due to the lack of clinical studies valid recommendations for the optimal treatment cannot be made so far.
References
Keen RW. Burden of osteoporosis and fractures. Curr Osteoporos Rep. 2003;1–2:66–70.
Bernhardt M, Swartz DE, Clothiaux PL, Crowell RR, White Iii AA. Posterolateral lumbar and lumbosacral fusion with and without pedicle screw internal fixation. Clin Orthop Relat Res. 1992;284:109–15.
Goldhahn J, Suhm N, Goldhahn S, Blauth M, Hanson B. Influence of osteoporosis on fracture fixation—a systematic literature review. Osteoporos Int. 2008;19–6:761–72.
Halvorson TL, Kelley LA, Thomas KA, Whitecloud Iii TS, Cook SD. Effects of bone mineral density on pedicle screw fixation. Spine. 1994;19–21:2415–20.
Yamagata M, Kitahara H, Minami S, Takahashi K, Isobe K, Moriya H, Tamaki T. Mechanical stability of the pedicle screw fixation systems for the lumbar spine. Spine (Phila Pa 1976). 1992;17(3 Suppl):S51–4.
Law M, Tencer AF, Anderson PA. Caudo-cephalad loading of pedicle screws: mechanisms of loosening and methods of augmentation. Spine. 1993;18–16:2438–43.
Chao KH, Lai YS, Chen WC, Chang CM, McClean CJ, Fan CY, Chang CH, Lin LC, Cheng CK. Biomechanical analysis of different types of pedicle screw augmentation: a cadaveric and synthetic bone sample study of instrumented vertebral specimens. Med Eng Phys. 2013;35–10:1506–12.
Higashino K, Kim JH, Horton WC, Hutton WC. A biomechanical study of two different pedicle screw methods for fixation in osteoporotic and nonosteoporotic vertebrae. J Surg Orthop Adv. 2012;21–4:198–203.
Hamasaki T, Tanaka N, Kim J, Okada M, Ochi M, Hutton WC. Pedicle screw augmentation with polyethylene tape: a biomechanical study in the osteoporotic thoracolumbar spine. J Spinal Disord Technol. 2010;23–2:127–32.
Tsai KJ, Murakami H, Horton WC, Fei Q, Hutton WC. Pedicle screw fixation strength: a biomechanical comparison between 4.5- and 5.5-mm diameter screws in osteoporotic upper thoracic vertebrae. J Surg Orthop Adv. 2009;18–1:23–7.
Becker S, Chavanne A, Spitaler R, Kropik K, Aigner N, Ogon M, Redl H. Assessment of different screw augmentation techniques and screw designs in osteoporotic spines. Eur Spine J. 2008;17–11:1462–9.
Liu D, Wu ZX, Pan XM, Fu SC, Gao MX, Shi L, Lei W. Biomechanical comparison of different techniques in primary spinal surgery in osteoporotic cadaveric lumbar vertebrae: expansive pedicle screw versus polymethylmethacrylate-augmented pedicle screw. Arch Orthop Trauma Surg. 2011;131–9:1227–32.
Sarzier JS, Evans AJ, Cahill DW. Increased pedicle screw pullout strength with vertebroplasty augmentation in osteoporotic spines. J Neurosurg. 2002;96–3(Suppl):309–12.
Yu BS, Li ZM, Zhou ZY, Zeng LW, Wang LB, Zheng ZM, Lu WW. Biomechanical effects of insertion location and bone cement augmentation on the anchoring strength of iliac screw. Clin Biomech (Bristol, Avon). 2011;26–6:556–61.
Yu BS, Zhuang XM, Zheng ZM, Zhang JF, Li ZM, Lu WW. Biomechanical comparison of 4 fixation techniques of sacral pedicle screw in osteoporotic condition. J Spinal Disord Technol. 2010;23–6:404–9.
Hoppe S, Loosli Y, Baumgartner D, Heini P, Benneker L. Influence of screw augmentation in posterior dynamic and rigid stabilization systems in osteoporotic lumbar vertebrae: a biomechanical cadaveric study. Spine (Phila Pa 1976). 2014;39(6):E384–9.
Zindrick MR, Wiltse LL, Widell EH, Thomas JC, Holland WR, Field BT, Spencer CW. A biomechanical study of intrapeduncular screw fixation in the lumbosacral spine. Clin Orthop Relat Res. 1986;203:99–112.
Frankel BM, D’Agostino S, Wang C. A biomechanical cadaveric analysis of polymethylmethacrylate-augmented pedicle screw fixation. J Neurosurg Spine. 2007;7–1:47–53.
Renner SM, Lim TH, Kim WJ, Katolik L, An HS, Andersson GB. Augmentation of pedicle screw fixation strength using an injectable calcium phosphate cement as a function of injection timing and method. Spine (Phila Pa 1976). 2004;29(11):E212–6.
Kiner DW, Wybo CD, Sterba W, Yeni YN, Bartol SW, Vaidya R. Biomechanical analysis of different techniques in revision spinal instrumentation: larger diameter screws versus cement augmentation. Spine (Phila Pa 1976). 2008;33(24):2618–22.
Kueny RA, Kolb JP, Lehmann W, Puschel K, Morlock MM, Huber G. Influence of the screw augmentation technique and a diameter increase on pedicle screw fixation in the osteoporotic spine: pullout versus fatigue testing. Eur Spine J. 2014;23–10:2196–202.
Law M, Tencer AF, Anderson PA. Caudo-cephalad loading of pedicle screws: mechanisms of loosening and methods of augmentation. Spine (Phila Pa 1976). 1993;18–16:2438–43.
Folsch C, Goost H, Figiel J, Paletta JR, Schultz W, Lakemeier S. Correlation of pull-out strength of cement-augmented pedicle screws with CT-volumetric measurement of cement. Biomed Technol (Berl). 2012;57–6:473–80.
Burval DJ, McLain RF, Milks R, Inceoglu S. Primary pedicle screw augmentation in osteoporotic lumbar vertebrae: biomechanical analysis of pedicle fixation strength. Spine (Phila Pa 1976). 2007;32(10):1077–83.
Linhardt O, Luring C, Matussek J, Hamberger C, Herold T, Plitz W, Grifka J. Stability of anterior vertebral body screws after kyphoplasty augmentation. An experimental study to compare anterior vertebral body screw fixation in soft and cured kyphoplasty cement. Int Orthop. 2006;30–5:366–70.
Flahiff CM, Gober GA, Nicholas RW. Pullout strength of fixation screws from polymethylmethacrylate bone cement. Biomaterials. 1995;16–7:533–6.
Cho W, Wu C, Erkan S, Kang MM, Mehbod AA, Transfeldt EE. The effect on the pullout strength by the timing of pedicle screw insertion after calcium phosphate cement injection. J Spinal Disord Technol. 2011;24–2:116–20.
Chen LH, Tai CL, Lee DM, Lai PL, Lee YC, Niu CC, Chen WJ. Pullout strength of pedicle screws with cement augmentation in severe osteoporosis: a comparative study between cannulated screws with cement injection and solid screws with cement pre-filling. BMC Musculoskelet Disord. 2011;12:33.
Choma TJ, Pfeiffer FM, Swope RW, Hirner JP. Pedicle screw design and cement augmentation in osteoporotic vertebrae: effects of fenestrations and cement viscosity on fixation and extraction. Spine (Phila Pa 1976). 2012;37(26):E1628–32.
Chang MC, Kao HC, Ying SH, Liu CL. Polymethylmethacrylate augmentation of cannulated pedicle screws for fixation in osteoporotic spines and comparison of its clinical results and biomechanical characteristics with the needle injection method. J Spinal Disord Technol. 2013;26–6:305–15.
Tan QC, Wu JW, Peng F, Zang Y, Li Y, Zhao X, Lei W, Wu ZX. Augmented PMMA distribution: improvement of mechanical property and reduction of leakage rate of a fenestrated pedicle screw with diameter-tapered perforations. J Neurosurg Spine. 2016;24(6):971–7. doi:10.3171/2015.10.SPINE141275.
Kobayashi H, Fujishiro T, Belkoff SM, Kobayashi N, Turner AS, Seim HB 3rd, Zitelli J, Hawkins M, Bauer TW. Long-term evaluation of a calcium phosphate bone cement with carboxymethyl cellulose in a vertebral defect model. J Biomed Mater Res A. 2009;88–4:880–8.
Larsson S, Bauer TW. Use of injectable calcium phosphate cement for fracture fixation: a review. Clin Orthop Relat Res. 2002;395:23–32.
Walsh WR, Morberg P, Yu Y, Yang JL, Haggard W, Sheath PC, Svehla M, Bruce WJ. Response of a calcium sulfate bone graft substitute in a confined cancellous defect. Clin Orthop Relat Res. 2003;406:228–36.
McLachlin SD, Al Saleh K, Gurr KR, Bailey SI, Bailey CS, Dunning CE. Comparative assessment of sacral screw loosening augmented with PMMA versus a calcium triglyceride bone cement. Spine (Phila Pa 1976). 2011;36(11):E699–704.
Gao M, Lei W, Wu Z, Liu D, Shi L. Biomechanical evaluation of fixation strength of conventional and expansive pedicle screws with or without calcium based cement augmentation. Clin Biomech (Bristol, Avon). 2011;26–3:238–44.
Hashemi A, Bednar D, Ziada S. Pullout strength of pedicle screws augmented with particulate calcium phosphate: an experimental study. Spine J. 2009;9–5:404–10.
Moore DC, Maitra RS, Farjo LA, Graziano GP, Goldstein SA. Restoration of pedicle screw fixation with an in situ setting calcium phosphate cement. Spine (Phila Pa 1976). 1997;22(15):1696–705.
El Saman A, Meier S, Sander A, Kelm A, Marzi I, Laurer H. Reduced loosening rate and loss of correction following posterior stabilization with or without PMMA augmentation of pedicle screws in vertebral fractures in the elderly. Eur J Trauma Emerg Surg. 2013;39–5:455–60.
Sawakami K, Yamazaki A, Ishikawa S, Ito T, Watanabe K, Endo N. Polymethylmethacrylate augmentation of pedicle screws increases the initial fixation in osteoporotic spine patients. J Spinal Disord Tech. 2012;25–2:E28–35.
Weiser L, Dreimann M, Huber G, Sellenschloh K, Puschel K, Morlock MM, Rueger JM, Lehmann W. Cement augmentation versus extended dorsal instrumentation in the treatment of osteoporotic vertebral fractures: a biomechanical comparison. Bone Jt J. 2016;98-B(8):1099–105.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Sven Hoppe and Marius J.B. Keel declare that they have no conflict of interest .
Rights and permissions
About this article
Cite this article
Hoppe, S., Keel, M.J.B. Pedicle screw augmentation in osteoporotic spine: indications, limitations and technical aspects. Eur J Trauma Emerg Surg 43, 3–8 (2017). https://doi.org/10.1007/s00068-016-0750-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-016-0750-x