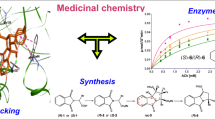
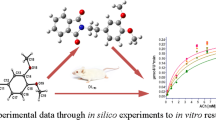
Abstract
Alzheimer’s disease (AD), the most common form of dementia, is characterized by a progressive degeneration of the brain that leads to loss of memory and deterioration of others cognitive functions. The only drugs currently approved for treating AD are AChE inhibitors (AChEIs). We previously tested a novel isoindoline-1,3-dione, finding potent inhibition of AChE, in part because the two carbonyl groups of phthalimide facilitate hydrogen bonds with the enzyme. The aims of the present study were: (A) To achieve a faster and cheaper technique with a reduced quantity of reactive, without significant difference in the validation of the results, by modifying the version of the method described by Bonting and Featherstone. (B) To test new isoindolines and dioxoisoindolines as AChEIs and see if the carbonyl group is really important for affinity. Both families of compounds (isoindolines and dioxoisoindolines) had an inhibitory effect. The enzymatic inhibitions produced by isoindolines were uncompetitive, whereas that evoked by dioxoisoindolines were competitive. One of the isoindoline derivatives (IsoB with a Ki of 88–160µM) showed about 5-fold greater inhibition of AChE than its corresponding dioxoisoindoline. According to molecular docking performed, dioxoisoindolines apparently interact with the catalytic active site, the peripheral anionic site, and the aromatic patch, which can explain the kind of inhibition observed. Due to the uncompetitive inhibition of isoindolines, their inhibitory behavior could not be explored in silico. We afforded a faster and more efficient method, while yielding similar results than Bonting and Featherstone method. Additionally, we demonstrated that carbonyl group affects the kind of inhibition and the affinity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is the most common form of dementia, constituting up to 80% of all cases (Duthey 2013; Korolev 2014). It is expected to affect around 66 million people by 2030. Today, the prevalence of AD is reported to be about 3.5% of the world population (>20 million people), with some authors estimating 6% (~35 million people). This disease mostly afflicts the elderly, including 10% of people over 65 and nearly 50% of those over 85. Since life expectancy is on the rise, prevalence is expected to increase (Musiał et al. 2007; Aliabadi et al. 2013; Anand and Singh 2013; Guzior et al. 2014). In 2010, 58% of all AD patients had low or middle incomes and this is projected to reach 63% in 2030 (Prince et al. 2013).
AD is characterized by a progressive degeneration of the brain that leads to loss of memory, disorientation, anxiety, delusion, depression, insomnia, wandering, learning impairment, and deterioration of cognitive functions. Although the etiology of AD is not well understood, various factors contribute to the development of this disease, such as an increase in β-amyloid plaques, an accumulation of neurofibrillary tangles, hyperphosphorylation of tau protein, chronic neuroinflammation, oxidative stress, inflammatory processes, dyshomeostasis of biometals, and decreased levels of acetylcholine caused by a depletion of the cholinergic system (Mandelkow and Mandelkow 1994; Grathwohl et al. 2009; Murphy and LeVine 2010; Iqbal et al. 2010; Heneka et al. 2015; Czarnecka et al. 2017).
All the manifestations of this disorder are linked to a reduction in acetylcholine levels in the brain, resulting from the degeneration of the cholinergic neurons (Ignasik et al. 2012) and the deposition of the β-amyloid peptide as plaque and neurofibrillary tangles in the brain (Lahiri et al. 2002; Wenk 2003; Musiał et al. 2007; Aliabadi et al. 2013; Anand and Singh 2013; Guzior et al. 2014). It is thought that these peptides and protein accumulations are toxic to neurons and contribute to their death, producing cerebral atrophy (Nwidu et al. 2017). Fourteen years ago, the degeneration of cholinergic nuclei was detected in the basal forebrain during the course of AD (Ibach and Haen 2004). Several theories now exist to explain the origin of AD, including the cholinergic theory, the β-amyloid theory (extracellular deposits of β-amyloid in brain parenchyma and neurofibrillary intracellular tangles, which is the most studied hypothesis), the tau hypothesis, and the inflammation theory (Kumar et al. 2015).
Since the 1970s, the stimulation of cholinergic neurotransmission has been the principal strategy of many researchers (Ozadali-Sari et al. 2017), mainly carried out by inhibiting acetylcholinesterase (AChE, EC 3.1.1.7), an enzyme that hydrolyzes the neurotransmitter acetylcholine at cholinergic synapses and thus terminates nerve transmission (Barnard 1974; Kamkwalala and Newhouse 2016; Li et al. 2017). Another non-specific cholinesterase enzyme, butyrylcholinesterase (BuChE), is also a target for treating AD. In the late phases of the disease, antagonizing NMDA forms part of this same strategy (Musiał et al. 2007; Bajda et al. 2013; Anand and Singh 2013; Guzior et al. 2014).
Currently, AChEIs are the only drugs approved by the FDA for the treatment of AD (Musiał et al. 2007). Of these drugs, the most widely used are tacrine, donepezil, rivastigmine, galantamine, and memantine (Musiał et al. 2007; Anand and Singh 2013; Guzior et al. 2014; Kumar et al. 2015). Others such as phenserine are currently in clinical trials (Lahiri et al. 2002; Ozadali-Sari et al. 2017). The most promising agents for AD treatment are dual-binding AChEIs (Ignasik et al. 2012). Diverse studies indicate that the inhibition of AChE in AD patients can improve cognitive function, delay the progression of mental deterioration, and reduce neuropsychiatric symptoms (Lahiri et al. 2002; Ozadali-Sari et al. 2017; Nwidu et al. 2017; Li et al. 2017). Certainly, AChEIs are still the best established treatment for mild to moderate AD, although they do not represent a cure.
Since the AChEIs currently on the market have adverse effects (Birks 2006), there are ongoing efforts to seek new drugs with greater potency and less toxicity. As demonstrated by different crystals, AChE is characterized by a deep gorge with the catalytic active site inside. This site is surrounded by numerous other ligand recognition sites, the nearest oxyanionic hole, an aromatic patch, an anionic site, and a peripheral anionic site (Dvir et al. 2010; Shazi 2012; Kiametis et al. 2017). The peripheral anionic site mediates the aggregation rate of β-amyloid. Hence, a moiety or molecule that binds to the latter site could possibly modify the physiopathology of AD (Gupta and Mohan 2014).
The catalytic site for Torpedo californica AChE has been described as having a gorge 20 Å deep and 5 Å wide. The most important part (the stearic site) is surrounded by three essential aminoacids, Ser200, His440, and Gly327, creating the catalytic triad. The anionic site is composed of Trp84, Tyr130, Phe330, and Phe331. The stabilizing transition complex is formed by Gly118, Gly119, and Ala201, while the peripheral anionic site consists of five aminoacids: Tyr70, Asp72, Tyr121, Trp279, and Tyr334 (Bajda et al. 2013).
Isoindolines and isoindolines-1,3-diones, potent pharmacophore groups found in natural and non-natural products, have shown anticonvulsant, anti-inflammatory, analgesic, anti-hypertensive, and antibacterial activity (Kukkola et al. 2001; Kim et al. 2007; Van Goethem et al. 2011; Çizmecioğlu et al. 2011; Davood et al. 2012; Shakir et al. 2012; Raveendra et al. 2014; Barrio et al. 2015; Achary et al. 2017). According to various research teams, isoindoline-1,3-diones are potent and novel inhibitors of AChE with two carbonyl groups of phthalimide that facilitate hydrogen bonds with the catalytic active site and the peripheral anionic site simultaneously. Consequently, this molecule can inhibit both the formation of β-amyloid fibrils and the hydrolytic activity of AChE on acetylcholine. The main interactions with AChE carried out by isoindolines-1,3-diones and their analogs are π–π and π–cation (Mohammadi-Farani et al. 2017). Additionally, isoindolines-1,3-diones are considered to provide neuroprotection (Mary et al. 1998; Zhao et al. 2009; Alipour et al. 2012; Mohammadi-Farani et al. 2013; Guzior et al. 2015; Hebda et al. 2016; Si et al. 2016).
Some researchers have examined the AChE inhibitory capacity of phthalimide derivatives, identifying inhibitory concentrations 50 (IC50) at a micromolar scale (16.42µM) (Mohammadi-Farani et al. 2013). Michalina et al. designed and tested a series of 2-(diethylaminoalkyl)-isoindoline-1,3-dione derivatives, establishing that they bind to the catalytic active site and the peripheral anionic site. The IC50 of the best compound ranged from 0.9 to 19.5µM (Ignasik et al. 2012). Bajda et al. (2013) evaluated different structures of AChEIs by performing fragment-based design, finding 2-(5-(2-fluorobenzylamino)pentyl)isoindoline-1,3-dione to be the most active compound, with an IC50 of 87 nm.
The in silico studies on the latter compounds revealed a CH–π interaction with Trp84, a π–cation interaction with Phe330, an H-bond with Tyr121, hydrophobic interactions in the middle of the active gorge with Phe290, Phe331, and Tyr334, π–π interactions with Trp279, and a CH–π with Tyr70 by the phthalimide moiety residues (Bajda et al. 2013). Others studies with phthalimide have shown that this kind of compound can interact by π–π stacking and CH–π interactions with aromatic amino acids at the anionic subsite (Phe330, Phe331, and Trp84), and/or with residues at the peripheral anionic site (Trp279, Tyr334) of AChE (Ignasik et al. 2012).
Due to the importance of measuring ACh levels, during the last few decades, many techniques have been elaborated to measure AChE activity in experiments. In 1955, Bonting and Featherstone presented their ultramicro assay of cholinesterase, which was an adaptation of the hydroxamic acid method for the determination of choline esters (Bonting and Featherstone 1956). The method is time-consuming and costly in materials. In 1961, Ellman et al. developed the colorimetric analysis of AChE activity, measuring the enzymatic activity based on the intensification of the color yellow produced by thiocholine upon reacting with the dithiobisnitrobenzoate ion (Ellman et al. 1961). Though sensitive, this method can generate errors if the compounds tested are α,β-unsaturated carbonyls or good electrophiles, because these compounds tend to react with the analytical substance.
For the present study, it was decided to improve the 1956 technique by Bonting and Featherstone because of its accuracy and easiness AChE catalytic activity detection. Hence, it was modified to make it inexpensive and straightforward. In a previous investigation based on this method, we crystallized and tested an isoindoline-1,3-dione as an AChEI (paper in peer review), finding good inhibitory activity (inhibitory constant Ki = 330–930 µM; p < 0.05). Therefore, new isoindolines and dioxoisoindolines with were herein evaluated in terms of their inhibition of AChE. Both sets of compounds were compared in order to elucidate how carbonyl groups influence the inhibition of the enzyme.
Materials and methods
Synthesis and characterization of 2,3-dihydro-1H-isoindoles and N-substituted phthalimide
Our previously reported synthetic methodology was followed without any modifications (Andrade-Jorge et al. 2017). In brief, reagents and solvents from Sigma-Aldrich were used as received. The reactions were carried out in a flask at the melting point of the starting material and agitated with a stirring bar for a few minutes in solventless conditions (green chemistry), and then the products were purified as described (Andrade-Jorge et al. 2017). The reactions were monitored by TLC (0.25 mm thick silica gel, 60 F254 plates) and the products were characterized by nuclear magnetic resonance (NMR) spectra, recorded on a Varian Mercury 300 spectrometer at 300MHz for 1H and 75MHz for 13C, with tetramethylsilane as internal reference.
Solutions
For the phosphate buffer (0.1 M, pH 8), 7.48 g of K2HPO4 were weighed and added to 430 mL of distilled water, while 0.916 g of KH2PO4 were mixed with 70 mL of distilled water. Then both solutions were combined to provide the buffer solution, which had a final volume of 500 mL and a pH of 8 (monitoring pH with a potentiometer). For the sodium hydroxide solution (4.2 M NaOH), 16.96 g NaOH were dissolved in distilled water to attain a final volume of 100 mL. For the hydroxylamine solution (2.4 M NH2OH), 16.84 g NH2OH·HCl were dissolved in distilled water to obtain a final volume of 100 mL. For the alkaline hydroxylamine solution, equal volumes of sodium hydroxide and hydroxylamine solution were mixed immediately before use. For the ferric chloride (FeCl3) solution, 20.31 g FeCl3·6H2O were slowly mixed (to avoid any damage) with an HCl solution (61.95%) to reach a final volume of 100 mL. For the stock acetylcholine solution, 50 mg ACh iodide were dissolved in 0.695 mL phosphate buffer to afford a solution of 256 mM. Subsequently, different dilutions were prepared for the kinetic experiment (Scheme 1a). For the stock AChE solution, 10 U/mL lyophilized powder of AChE from Electric electricus (EE-AChE, Sigma Chemical Co. C1682) were prepared from the original source, and the solutions were kept at −20 °C. The three synthesized compounds and neostigmine were prepared at concentrations of 2, 4, and 8 mM, with DMSO (<1%) or distilled water as the dissolution medium. The dilutions were stored at −20 °C.
Docking
The ligands were modeled on GaussView 5.0.9 software and the protonation state was considered at physiological conditions (pH 7.4). Conformational analysis was performed on Gaussian 09 (Frisch et al. 2009) with a semi-empirical method (PM3). The rotating bonds, torsional degree of freedom, atomic partial charges, and non-polar H-bonds were assigned with AutoDock tools 1.5.4. (Morris et al. 2009). One of the crystal structures of AChE of Electrophorus electricus was downloaded from the Protein Data Bank (PDB code: 1C2O) (Bourne et al. 1999).
Docking conditions were programmed with AutoDock tools 1.5.4 and Raccoon (Forli et al. 2016), by utilizing a hybrid Lamarckian Genetic Algorithm (Morris et al. 1998), an initial population of 100 randomly placed individuals, Kollmann partial charges for all protein atoms, and Gasteiger charges for ligands. Subsequently, the grid parameter file was established, using a 60 × 60 × 60 Å gridbox with the coordinates X = 42.095, Y = 66.809, and Z = −81.47 and a mesh spacing of 0.375 Å. The calculations were run on AutoDock4 software in a Linux operative system (Fedora 22).
Finally, the lowest energy state, expressed as Gibbs free energy (∆G), was obtained for each compound. The dissociation constant (Kd), the –log(10) dissociation constant (pKd), the number of interactions, and the distance and type of binding were determined with the Visual Molecular Dynamics program (VMD v.1.8.6) (Humphrey et al. 1996).
Anticholinesterase activity assay
Dilutions of ACh were made to prepare different concentrations, which were mixed in an Analog Vortex Mixer (Thomas Scientific). Twenty μL of each solution (at 128, 96, 64, 48, 32, 16, 8, and 2mM) were placed in each well of a 96-well microplate, following the pattern described in Scheme 1b. The microplate was allowed to incubate for 20min at 37°C in a water bath (Felisa). Completing this period, the reaction was stopped with 40μL alkaline hydroxylamine solution and then 100μL of FeCl3 solution was added to each well and the optical density was read at 540nm in a microplate reader (Benchmark BIO-RAD), with a pre-mixed of 40 s. The standard curve of ACh was constructed with these values.
The same dilutions as well as incubation and reading procedures were employed to construct the standard curve for AChE, with 20μL of AChE in the starting mixture (utilized to make subsequent dilutions, see Scheme 1b). The standard and test compounds were used at 2, 4, and 8mM. The process for evaluating AChE activity was repeated, this time including 20μL of the test compounds before adding AChE. All experiments were performed in triplicate and data are expressed as the average of three values. The AChE activity/inhibition analysis was made with a Michaelis–Menten plot and non-linear regression to find the characteristic parameters. To compare the modified method with the original one, additional experiments adhered to the latter (Bonting and Featherstone 1956) and a curve was constructed for AChE activity as well as AChE inhibition elicited by neostigmine.
Statistical analysis
The data from the anticholinesterase activity assay are expressed as the mean ± 95% confidence intervals. Each treatment was compared to the control group (AChE+ACh). Non-linear regression analysis was carried out with 95% confidence intervals on GraphPad Prism statistical software with the enzyme kinetic module.
Results and discussion
Synthesis
IsoA, IsoB, and DioxoA were synthesized (Table 1 and Scheme 2). These are derived from isoindoline and dioxoisoindoline following our previously described above green chemistry technique (Andrade-Jorge et al. 2017) without modifications. Thus, the chemical characterization is in agreement with those reported in our previous report.
Structure and route for the synthesis of isoindoline/isoindoline-1,3-dione (Andrade-Jorge et al. 2017)
2-(2-Phenyletyl)-1,3-dihydroisoindoline hydrobromide (IsoA): It was obtained as a white solid, 90% yield; mp 165–166 °C; 1H NMR (DMSO-D6, 300 MHz) δ (PPM) 2.85 (t, H-11), 3.65 (t, H-10), 4.72 (dd, H-1,3), 7.36 (m, H-4,5,6,7,13,14,15,16,17); 13C NMR (CDCl3, 75 MHz) δ 58.4 (C-1,3), 123.5 (C-4,7), 127.4 (C-5,6), 137.9 (C-8,9), 55.4 (C-10), 33.5 (C-11), 134.9 (C-12), 129.2 (C-13,14,16,17), 127.5 (C-15). IR (ATR, cm−1) ύ: 3031 (C–H, Aromatic), 2908 (C–H, Aliphatic), 2546 (NH+), 1705 (C=O), 1600 (C=C), 1427 (CH2), 1391 (C–N). MS (m/z): 224.1447 (M+1).
2-(2-(3,4-Dimethoxyphenyl)etyl)-1,3-dihydroisoindoline hydrobromide (IsoB): It was obtained as a white solid, 80% yield; mp 197–198 °C; 1H NMR (DMSO-D6, 300 MHz) δ (PPM) 3.00 (t, H-11), 3.64 (t, H-10), 3.71 (s, H-18), 3.74 (s, H-19), 4.71 (s, H-1,3), 6.95 (m, H-13,16,17), 7.40 (m, H-4,5,6,7); 13C NMR (CDCl3, 75 MHz) δ 58.5 (C-1,3), 129.1 (C-4,7), 123.5 (C-5,6), 134.9 (C-8,9), 55.7 (C-10), 31.8 (C-11), 129.8 (C-12), 112.6 (C-13), 148.4 (C-14), 149.4 (C-15), 113.2 (C-16), 121.3 (C-17), 56.2 (C-18,19). IR (ATR, cm−1) ύ: 3063 (C–H, Aromatic), 2990 (C–H, Aliphatic), 2842 (O–CH3, Aliphatic), 2547 (NH+), 1600 (C=C), 1462 (CH2), 1453 (CH3), 1390 (C–N), 1228 (O–CH3). MS (m/z): 284.1624 (M+1).
2-(2-Phenyletyl) isoindolin-1,3-dione (DioxoA): It was obtained as a white solid, 85% yield; mp 130–131 °C; 1H NMR (CDCl3, 300 MHz) δ (PPM) 2.98 (t, H-11), 3.92 (t, H-10), 7.26 (m, H-13,14,15,16,17), 7.70 (m, H-5,6), 7.82 (m, H-4,7); 13C NMR (CDCl3, 75 MHz) δ 168.1 (C-1,3), 123.2 (C-4,7), 133.9 (C-5,6), 132.0 (C-8,9), 39.2 (C-10), 34.6 (C-11), 137.9 (C-12), 128.5 (C-13,17), 128.8 (C-14,16), 126.6 (C-15). IR (ATR, cm−1) ύ: 3031 (C–H, Aromatic), 2935 (C–H, Aliphatic), 1705 (C=O), 1600 (C=C), 1427 (CH2), 1391 (C–N). MS (m/z): 274.0752 (M+Na).
2-(2-(3,4-Dimethoxyphenyl)etyl) isoindolin-1,3-dione (DioxoB): It was obtained as a light yellow solid, 90% yield; mp 171–172 °C; 1H NMR (CDCl3, 300 MHz) δ (PPM) 2.93 (t, H-11), 3.90 (t, H-10), 3.80 (s, H-19), 3.83 (s, H-18), 6.78 (m, H-13,16,17), 7.70 (m, H-5,6), 7.82 (m, H-4,7); 13C NMR (CDCl3, 75 MHz) δ 168.2 (C-1,3), 123.19 (C-4,7), 132.0 (C-5,6), 130.4 (C-8,9), 39.3 (C-10), 34.0 (C-11), 133.9 (C-12), 111.1 (C-13), 148.7 (C-14), 147.6 (C-15), 111.8 (C-16), 120.8 (C-17), 55.7 (C-18,19). IR (ATR, cm−1) ύ: 3063 (C–H, Aromatic), 2943 (C–H, Aliphatic), 2842 (O–CH3, Aliphatic), 1705 (C=O), 1600 (C=C), 1466 (CH2), 1427 (CH3), 1394 (C–N), 1228 (O–CH3). MS (m/z): 334.0956 (M+Na).
Kinetic test validation
The inhibitory effects on AChE were assessed by modifying the ultramicro assay developed by Bonting and Featherstone in 1955. We achieved a more efficient and faster technique, obtaining up to 12 kinetic curves at the same time. After running assays with the original and modified methods, a standard curve was constructed for AChE activity as well as for the AChE inhibition elicited by the reference compound. The values of the Michaelis–Menten constant (Km) for the AChE curves showed no significant difference between the two methods (Table 2), nor did the Ki values of the two antagonist curves. Since the modified method did not affect the results, it could be used to estimate the kinetic parameters of the new compounds.
Anticholinesterase activity assay
By employing the improved method, an assessment was made of acetylcholinesterase inhibition for three compounds: IsoA, IsoB, and DioxoA. Another compound (DioxoB) was considered, which had been evaluated in a previous work (paper in peer review). Consequently, the inhibition induced by two isoindolines and two dioxoisoindolines was compared (Table 2). The latter compounds are derivatives of two arylamines, the only difference being the addition of two carbonyls groups (Table 1). Dioxoisoindolines with different substituents in their structure are known to be fairly good inhibitors of AChE, due in part to their carbonyl groups in the pyrrolidine ring. This kind of moiety is important for recognition between the enzyme and inhibitors, forming H-bonds in the catalytic triad site.
It is thought that carbonyl groups are necessary in the molecule to achieve a good inhibitory effect. Despite not having carbonyl groups, nonetheless, the isoindolines inhibited AChE better than the isoindoline-1,3-diones (Table 2; Fig. 1). The comparison of the analog compounds IsoA and DioxoA revealed that the isoindoline afforded a 1.5-fold greater inhibition of the enzyme than the dioxoisoindoline. Regarding IsoB vs. DioxoB, the isoindoline derivative displayed a 5-fold greater inhibition than the corresponding dioxoisoindoline, likely due to the kind of interactions between the ligands and AChE. Although much research has examined the inhibitory effect of isoindolines-1,3-diones (as aforementioned), such is not the case with isoindolines. Therefore, one aim of the current contribution was to explore the latter molecules as a new kind of inhibitor.
Molecular docking
In silico experiments were performed to provide insights into the in vitro results. The competitive inhibitory activity of dioxoisoindolines allows for analysis by molecular docking, while the uncompetitive activity of isoindolines does not. Molecular docking was carried out on a 3D model of AChE to study the binding of well-known inhibitors (donepezil, galantamine, rivastigmine, or tacrine) and the dioxoisoindolines (Fig. 2). The ∆G is clearly exergonic for the two dioxoisoindolines and four reference compounds (Table 3), with very similar values for all these molecules. For the two dioxoisoindolines, the principal interactions and the main amino acid residues in AChE involved in such interactions are described (see Tables 4 and 5; Fig. 3).
Binding mode of the ligands with AChE of Electrophorus electricus, in the catalytic active site, peripheral anionic site, and aromatic patch (obtained by molecular docking): (A) Binding site of DioxoA, DioxoB, and donepezil in AChE; (A′) the dioxoisoindolines show a binding mode similar to donepezil; (B) the binding site of DioxoA, DioxoB, and rivastigmine in AChE; (B′) the dioxoisoindolines have a binding mode similar to rivastigmine
Binding mode and main amino acid residues in the catalytic active site, peripheral anionic site, and aromatic patch of AChE of Electrophorus electricus when interacting with the ligands (observed by docking simulation): (A) DioxoA interactions; (A′) DioxoA binding site; (B) DioxoB interactions; (B′) DioxoB binding site; (C) the orientations of DioxoA and DioxoB in AChE
After considering all the interactions, some conclusions were drawn. First, the binding sites for both dioxoisoindolines are the catalytic active site (consisting of a triad of amino acids; Fig. 3A′, B′), the peripheral anionic site, and the aromatic patch. The kind of inhibition can be explained by the fact that these molecules bind to the catalytic active site, thus competing with acetylcholine and accounting for the competitive inhibition found in vitro. Second, the principal interactions between the dioxoisoindolines and AChE are very similar to those described in literature: H-bonds with the oxygen atoms of the carbonyl groups as well as π–π interactions with the aromatic rings. Even the methoxy group supports the exergonic nature of the ∆G. Finally, the isoindoline-1,3-diones herein tested had a binding mode very similar to each other (Fig. 3C).
Conclusions
We developed and tested a method for evaluating the inhibitory activity of ligands on AChE. The slight modifications to Bonting and Featherston afforded a faster and more efficient method, while yielding similar results. The in vitro assays demonstrated that the isoindolines have higher affinity and a greater ability to inhibit AChE than the dioxoisoindolines. These pharmacodynamic properties are probably due to the distinct kind of key interactions carried out on AChE by isoindolines vs. dioxoisoindolines mediated for the presence of carbonyl group. IsoB showed affinity for AChE similar to neostigmine. Further research is needed to analyze the pharmacodynamic and pharmacokinetic profiles of this compound.
References
Achary R, Jung I-A, Son S-M, Lee H-K (2017) Stereoselective synthesis of functionalized 1,3-disubstituted isoindolines via Rh(III)-catalyzed tandem oxidative olefination-cyclization of 4-aryl-cyclic sulfamidate-5-carboxylates. J Org Chem. https://doi.org/10.1021/acs.joc.7b00799
Aliabadi A, Foroumadi A, Mohammadi-Farani A (2013) Synthesis and evaluation of anti-acetylcholinesterase Alzheimer effects. Iran J Basic Med Sci 16:1049–1054
Alipour M, Khoobi M, Foroumadi A, Nadri H, Moradi A, Sakhteman A, Ghandi M, Shafiee A (2012) Novel coumarin derivatives bearing N-benzyl pyridinium moiety: potent and dual binding site acetylcholinesterase inhibitors. Bioorganic Med Chem 20:7214–7222. https://doi.org/10.1016/j.bmc.2012.08.052
Anand P, Singh B (2013) A review on cholinesterase inhibitors for Alzheimer’s disease. Arch Pharm Res 36:375–399. https://doi.org/10.1007/s12272-013-0036-3
Andrade-Jorge E, Bahena-Herrera JR, Garcia-Gamez J, Padilla-Martínez II, Trujillo-Ferrara JG (2017) Novel synthesis of isoindoline/isoindoline-1,3-dione derivatives under solventless conditions and evaluation with the human D2 receptor. Med Chem Res 26:2420–2431. https://doi.org/10.1007/s00044-017-1942-6
Andrade-Jorge E, Bribiesca-Carlos J, Martínez-Martínez FJ, Soriano-Ursúa MA, Padilla-Martínez II, Trujillo-Ferrara JG (2018) Crystal structure, DFT calculations and evaluation of 2-(2-(3,4-dimethoxyphenyl)ethyl)isoindoline-1,3-dione as AChE inhibitor. Chem Cent J 12:74. https://doi.org/10.1186/s13065-018-0442-1
Bajda M, Więckowska A, Hebda M, Guzior N, Sotriffer C, Malawska B (2013) Structure-based search for new inhibitors of cholinesterases. Int J Mol Sci 14:5608–5632. https://doi.org/10.3390/ijms14035608
Barnard EA (1974) Neuromuscular transmission—enzymatic destruction of acetylcholine. In:Hubbard J.I. (eds) The peripheral nervous system. Springer, Boston, MA, pp 201–224
Barrio P, Ibáñez I, Herrera L, Román R, Catalán S, Fustero S (2015) Asymmetric synthesis of fluorinated isoindolinones through palladium-catalyzed carbonylative amination of enantioenriched benzylic carbamates. Chemistry 21:11579–11584. https://doi.org/10.1002/chem.201500773
Birks JS (2006) Cholinesterase inhibitors for Alzheimer’s disease. In: Birks JS (ed) Cochrane database of systematic reviews. John Wiley & Sons, Ltd., Chichester, p CD005593
Bonting SL, Featherstone RM (1956) Ultramicro assay of the cholinesterases. Arch Biochem Biophys 61:89–98. https://doi.org/10.1016/0003-9861(56)90319-8
Bourne Y, Grassi J, Bougis PE, Marchot P (1999) Conformational flexibility of the acetylcholinesterase tetramer suggested by X-ray crystallography. J Biol Chem 274:30370–30376. https://doi.org/10.1074/jbc.274.43.30370
Çizmecioğlu M, Pabuççuoğlu V, Ballar P, Pabuççuoğlu A, Soyer Z (2011) Synthesis and screening of cyclooxygenase inhibitory activity of some 1,3-dioxoisoindoline derivatives. Arzneimittelforschung 61:186–190. https://doi.org/10.1055/s-0031-1296187
Czarnecka K, Szymański P, Girek M, Mikiciuk-Olasik E, Skibiński R, Kabziński J, Majsterek I, Malawska B, Jończyk J, Bajda M (2017) Tetrahydroacridine derivatives with fluorobenzoic acid moiety as multifunctional agents for Alzheimer’s disease treatment. Bioorg Chem 72:315–322. https://doi.org/10.1016/j.bioorg.2017.05.003
Davood A, Shafaroodi H, Amini M, Nematollahi A, Shirazi M, Iman M (2012) Design, synthesis and protection against pentylenetetrazole-induced seizure of N-aryl derivatives of the phthalimide pharmacophore. Med Chem 8:953–963. https://doi.org/10.2174/157340612802084289
Duthey B (2013) Background Paper 6. 11 Alzheimer disease and other dementias, update on 2004. World Heal Organ 1–77
Dvir H, Silman I, Harel M, Rosenberry TL, Sussman JL (2010) Acetylcholinesterase: from 3D structure to function. Chem Biol Interact 187:10–22. https://doi.org/10.1016/j.cbi.2010.01.042
Ellman GL, Courtney KD, Andres V, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95. https://doi.org/10.1016/0006-2952(61)90145-9
Forli S, Huey R, Pique ME, Sanner MF, Goodsell DS, Olson AJ (2016) Computational protein-ligand docking and virtual drug screening with the AutoDock suite. Nat Protoc 11:905–919
Frisch MJ, Trucks GW, Schlegel HB, Scuseria GE, Robb MA, Cheeseman JR, Scalmani G, Barone V, Mennucci B, Petersson GA, Nakatsuji H, Caricato M, Li X, Hratchian HP, Izmaylov AF, Bloino J, Zheng G, Sonnenberg JL, Hada M, Ehara M, Toyota K, Fukuda R, Hasegawa J (2009) Gaussian 09, Revision E. 01; Gaussian, Inc., Wallingford, CT
Grathwohl SA, Kälin RE, Bolmont T, Prokop S, Winkelmann G, Kaeser SA, Odenthal J, Radde R, Eldh T, Gandy S, Aguzzi A, Staufenbiel M, Mathews PM, Wolburg H, Heppner FL, Jucker M (2009) Formation and maintenance of Alzheimer’s disease beta-amyloid plaques in the absence of microglia. Nat Neurosci 12:1361–1363. https://doi.org/10.1038/nn.2432
Gupta S, Mohan CG (2014) Dual binding site and selective acetylcholinesterase inhibitors derived from integrated pharmacophore models and sequential virtual screening. Biomed Res Int 2014:291214. https://doi.org/10.1155/2014/291214
Guzior N, Bajda M, Skrok M, Kurpiewska K, Lewiński K, Brus B, Pišlar A, Kos J, Gobec S, Malawska B (2015) Development of multifunctional, heterodimeric isoindoline-1,3-dione derivatives as cholinesterase and β-amyloid aggregation inhibitors with neuroprotective properties. Eur J Med Chem 92:738–749. https://doi.org/10.1016/j.ejmech.2015.01.027
Guzior N, Wieckowska A, Panek D, Malawska B (2014) Recent development of multifunctional agents as potential drug candidates for the treatment of Alzheimer’s disease. Curr Med Chem 22:373–404. https://doi.org/10.2174/0929867321666141106122628
Hebda M, Bajda M, Więckowska A, Szałaj N, Pasieka A, Panek D, Godyń J, Wichur T, Knez D, Gobec S, Malawska B (2016) Synthesis, molecular modelling and biological evaluation of novel heterodimeric, multiple ligands targeting cholinesterases and amyloid beta. Molecules 21:1–24. https://doi.org/10.3390/molecules21040410
Heneka MT, Carson MJ, Khoury JEl, Landreth GE, Brosseron F, Feinstein DL, Jacobs AH, Wyss-Coray T, Vitorica J, Ransohoff RM, Herrup K, Frautschy SA, Finsen B, Brown GC, Verkhratsky A, Yamanaka K, Koistinaho J, Latz E, Halle A (2015) Neuroinflammation in Alzheimer’s disease. Lancet Neurol 14:388–405. https://doi.org/10.1016/S1474-4422(15)70016-5
Humphrey W, Dalke A, Schulten K (1996) VMD: visual molecular dynamics. J Mol Graph 14:33–38. https://doi.org/10.1016/0263-7855(96)00018-5
Ibach B, Haen E (2004) Acetylcholinesterase inhibition in Alzheimer’s disease. Curr Pharm Des 10:231–251. https://doi.org/10.2174/1381612043386509
Ignasik M, Bajda M, Guzior N, Prinz M, Holzgrabe U, Malawska B (2012) Design, synthesis and evaluation of novel 2-(aminoalkyl)-isoindoline-1,3-dione derivatives as dual-binding site acetylcholinesterase inhibitors. Arch Pharm 345:509–516. https://doi.org/10.1002/ardp.201100423
Iqbal K, Liu F, Gong C-X, Grundke-Iqbal I (2010) Tau in Alzheimer disease and related tauopathies. Curr Alzheimer Res 7:656–664. https://doi.org/10.2174/156720510793611592
Kamkwalala A, Newhouse P (2016) Beyond acetylcholinesterase inhibitors: novel cholinergic treatments for Alzheimer’s disease. Curr Alzheimer Res 13:1–1. https://doi.org/10.2174/1567205013666160930112625
Kiametis AS, Silva MA, Romeiro LAS, Martins JBL, Gargano R (2017) Potential acetylcholinesterase inhibitors: molecular docking, molecular dynamics, and in silico prediction. J Mol Model 23:67–72. https://doi.org/10.1007/s00894-017-3228-9
Kim HS, Kim Y, Doddareddy MR, Seo SH, Rhim H, Tae J, Pae AN, Choo H, Cho YS (2007) Design, synthesis, and biological evaluation of 1,3-dioxoisoindoline-5-carboxamide derivatives as T-type calcium channel blockers. Bioorg Med Chem Lett 17:476–481. https://doi.org/10.1016/j.bmcl.2006.10.042
Korolev I (2014) Alzheimer’s disease: a clinical and basic science review. Med Stud Res J 4:24–33
Kukkola PJ, Bilci NA, Ikler T, Savage P, Shetty SS, DelGrande D, Jeng AY (2001) Isoindolines: a new series of potent and selective endothelin—a receptor antagonists. Bioorg Med Chem Lett 11:1737–1740. https://doi.org/10.1016/S0960-894X(01)00273-6
Kumar A, Singh A, Ekavali (2015) A review on Alzheimer’s disease pathophysiology and its management: an update. Pharmacol Rep 67:195–203. https://doi.org/10.1016/j.pharep.2014.09.004
Lahiri DK, Farlow MR, Greig NH, Sambamurti K (2002) Current drug targets for Alzheimer’s disease treatment. Drug Dev Res 56:267–281. https://doi.org/10.1002/ddr.10081
Li F, Liu Y, Yuan Y, Yang B, Liu Z, Huang L (2017) Molecular interaction studies of acetylcholinesterase with potential acetylcholinesterase inhibitors from the root of Rhodiola crenulata using molecular docking and isothermal titration calorimetry methods. Int J Biol Macromol 104:527–532. https://doi.org/10.1016/j.ijbiomac.2017.06.066
Mandelkow E-M, Mandelkow E (1994) Tau protein and Alzheimer’s disease. Neurobiol Aging 15:85–86. https://doi.org/10.1016/0197-4580(94)90178-3
Mary A, Renko DZ, Guillou C, Thal C (1998) Potent acetylcholinesterase inhibitors: design, synthesis, and structure–activity relationships of bis-interacting ligands in the galanthamine series. Bioorg Med Chem 6:1835–1850. https://doi.org/10.1016/S0968-0896(98)00133-3
Mohammadi-Farani A, Abdi N, Moradi A, Aliabadi A (2017) 2-(2-(4-Benzoylpiperazin-1-yl)ethyl)isoindoline-1,3-dione derivatives: synthesis, docking and acetylcholinesterase inhibitory evaluation as anti-alzheimer agents. Iran J Basic Med Sci 20:59–66. https://doi.org/10.22038/ijbms.2017.8095
Mohammadi-Farani A, Ahmadi A, Nadri H, Aliabadi A (2013) Synthesis, docking and acetylcholinesterase inhibitory assessment of 2- (2- (4-Benzylpiperazin- potential anti-Alzheimer effects. DARU J Pharm Sci 21:1–10. https://doi.org/10.1186/2008-2231-21-47
Morris GM, Goodsell DS, Halliday RS, Huey R, Hart WE, Belew RK, Olson AJ (1998) Automated docking using a Lamarckian genetic algorithm and an empirical binding free energy function. J Comput Chem 19:1639–1662. 10.1002/(SICI)1096-987X(19981115)19:14<1639::AID-JCC10>3.0.CO;2-B
Morris GM, Ruth H, Lindstrom W, Sanner MF, Belew RK, Goodsell DS, Olson AJ (2009) AutoDock4 and AutoDockTools4: automated docking with selective receptor flexibility. J Comput Chem 30:2785–2791. https://doi.org/10.1002/jcc.21256
Murphy MP, LeVine H (2010) Alzheimer’s disease and the amyloid-β peptide. J Alzheimer’s Dis 19:311–323. https://doi.org/10.3233/JAD-2010-1221
Musiał A, Bajda M, Malawska B (2007) Recent developments in cholinesterases inhibitors for Alzheimer’s disease treatment. Curr Med Chem 14:2654–2679. https://doi.org/10.2174/092986707782023217
Nwidu LL, Elmorsy E, Thornton J, Wijamunige B, Wijesekara A, Tarbox R, Warren A, Carter WG (2017) Anti-acetylcholinesterase activity and antioxidant properties of extracts and fractions of Carpolobia lutea. Pharm Biol 55:1875–1883. https://doi.org/10.1080/13880209.2017.1339283
Ozadali-Sari K, Tüylü Küçükkılınç T, Ayazgok B, Balkan A, Unsal-Tan O (2017) Novel multi-targeted agents for Alzheimer’s disease: synthesis, biological evaluation, and molecular modeling of novel 2-[4-(4-substitutedpiperazin-1-yl)phenyl]benzimidazoles. Bioorg Chem 72:208–214. https://doi.org/10.1016/j.bioorg.2017.04.018
Prince M, Bryce R, Albanese E, Wimo A, Ribeiro W, Ferri CP (2013) The global prevalence of dementia: a systematic review and metaanalysis. Alzheimers Dement 9:63–75.e2. https://doi.org/10.1016/j.jalz.2012.11.007
Raveendra RS, Prashanth Pa, Prasad BD, Nayaka SC, Suresha GP, Nagabhushana BM, Bhagya NP (2014) Synthesis, characterization and antibacterial activity of isoindoline-1,3-dione derivatives. SOP Trans Org Chem 01:543–547
Shakir R, Muhi-Eldeen Za, Matalka KZ, Qinna Na (2012) Analgesic and toxicity studies of aminoacetylenic isoindoline-1,3-dione derivatives. ISRN Pharmacol 2012:1–7. https://doi.org/10.5402/2012/657472
Shazi S (2012) Molecular interaction of the antineoplastic drug, methotrexate with human brain acetylcholinesterase: a docking study CNS Neurol Disord Drug Targets 11:142–147. https://doi.org/10.2174/187152712800269669
Si W, Zhang T, Zhang L, Mei X, Dong M, Zhang K, Ning J (2016) Design, synthesis and bioactivity of novel phthalimide derivatives as acetylcholinesterase inhibitors. Bioorg Med Chem Lett 26:2380–2382. https://doi.org/10.1016/j.bmcl.2015.07.052
Van Goethem S, Matheeussen V, Joossens J, Lambeir A-M, Chen X, De Meester I, Haemers A, Augustyns K, Van der Veken P (2011) Structure–activity relationship studies on isoindoline inhibitors of dipeptidyl peptidases 8 and 9 (DPP8, DPP9): is DPP8-selectivity an attainable goal? J Med Chem 54:5737–5746. https://doi.org/10.1021/jm200383j
Wenk GL (2003) Neuropathologic changes in Alzheimer’s disease. J Clin Psychiatry 64:7–10
Zhao Q, Yang G, Mei X, Yuan H, Ning J (2009) Novel acetylcholinesterase inhibitors: synthesis and structure-activity relationships of phthalimide alkyloxyphenyl N,N-dimethylcarbamate derivatives. Pestic Biochem Physiol 95:131–134. https://doi.org/10.1016/j.pestbp.2009.04.018
Acknowledgements
This work was supported by SIP (m1930), Instituto Politécnico Nacional, and by CONACYT-Mexico.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Andrade-Jorge, E., Sánchez-Labastida, L.A., Soriano-Ursúa, M.A. et al. Isoindolines/isoindoline-1,3-diones as AChE inhibitors against Alzheimer’s disease, evaluated by an improved ultra-micro assay. Med Chem Res 27, 2187–2198 (2018). https://doi.org/10.1007/s00044-018-2226-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00044-018-2226-5