Abstract
The design of bioactive scaffolding materials with favorable properties is paramount for successful application in biomedical engineering. Polymeric hydrogels attract significant attention as leading candidates for scaffold engineering due to their specific compositional and structural similarities to the natural extracellular matrix. The ability to control porosity, surface morphology, and size of hydrogel scaffolds has created new approaches to overcome various issues in tissue engineering such as vascularization, tissue architecture, and simultaneous multiple cells seeding. This review imparts an overview of hydrogel scaffolds based on synthetic and natural polymeric components (alginate, gelatin, and 2-hydroxyethyl methacrylate). We made hydrogel scaffolds with unique properties. Their in vitro and in vivo biological response, morphology, mechanical properties, porosity, hydrophilicity, and degradability were tested to find optimal patterns of tissue regeneration.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
6.1 Tissue Regeneration Engineering and Polymeric Scaffolds
Tissue regeneration and engineering received significant scientific interest (curiosity) in the last decades and they can improve the levels of classical treatments. A biomaterial as a “temporary matrix that promotes a specific environment and architecture for tissue growth and development” is defined in the field of tissue engineering (Roseti et al. 2017).
The principal therapeutic platform for regenerative medicine is tissue engineering. The expansion of substitute products using biomaterials that can regenerate and repair diseased tissues and organs is a significant issue of new technological approaches. Therefore, these medical devices are fabricated to overcome the limited regeneration capacities of human tissues and organs.
The regenerative medicine field is dedicated to the general goal of damaged organs and tissues repairing and regenerating. Patient living cells isolation, their in vitro spreading inside polymeric scaffold, and reimplantation of tissue-mimick structures in the patient are the courses of the regenerative process (Langer and Vacanti 1993). The versatile properties of polymeric biomaterials, especially hydrogels, have found significant application in regenerative medicine as scaffolding materials into which cell cultures are introduced and serve as devices for the delivery of cells and genes (Slaughter et al. 2009). These biomaterials may be made biocompatible and exhibit adjustable mechanical properties and degradability. They are incorporated with biological signs to be able to carry out the processes of adhesion, migration, and proliferation of cells and growth factors, to enable the binding sites of peptides or cytokines. The biomimetic polymeric biomaterial thus created can mimic an extracellular matrix (ECM) environment.
Regenerative engineering aims to advance complex tissue revitalization processes and biological systems and encompasses the fields of stem cell science, advanced biomaterials, and developmental biology (Laurencin and Khan 2012). Polymeric hydrogels can be fabricated into 3D mimetic scaffolding for cell growth support thanks to their resemblance to a native extracellular matrix making them attractive biomaterials for regenerative engineering. The application of nano- and microtechnologies leads to the possibility of managing the properties and functionalities of hydrogel materials. This contributes to the biomimetic production of more refined patterns and architectures. Thus, our scientific perspectives expand to the level of nanoscale cellular interactions.
Most human tissues have a limited capacity for regeneration. Severe tissue damage due to trauma, degenerative diseases, or congenital abnormalities can lead to irreversible disability or death. Therefore, patients with serious tissue damage, in that case, depend on organ transplantation. Despite the increased volume of organ transplants, there is a limitation in the possibilities of recipients and donors of organs. Then tissue engineering and regenerative medicine take over the ″role″ (Amado et al. 2017; Vacanti and Langer 1999; Mason and Dunnill 2008).
The ideal scaffold should mimic a native extracellular matrix (ECM) and direct stem cells to regenerate functional tissues. In that sense, hydrogel materials are one of the most beneficial biomaterials with tunable water/fluid level, a high degree of biocompatibility, and simple adjustability to restore ECM (Slaughter et al. 2009). Various kinds of hydrogels with favorable properties are created to fix different type of tissues (Huebsch et al. 2010; Engler et al. 2006). Biophysical cues, like porosity, elasticity, and degradability, can be introduced into hydrogel scaffolds in a specific spatiotemporally manner to systematically regulate the cell’s behavior (Guvendiren and Burdick 2012; Yang et al. 2016). Advanced chemical strategies are used to improve biocompatibility and achieve hydrogel functionality (Amado et al. 2017; Phelps et al. 2012).
Spatially patterned hydrogel scaffolds with nanoscale biophysical and biochemical cues are used to evaluate cell behavior (Yang et al. 2016; Wade et al. 2015). Nanofiber-based hydrogel that mimics ECM with adaptable architecture and mechanics is synthesized in the interaction of advanced polymer processing technologies. In this way, the sensitivity of cells to mechanical stimuli as well as subsequent responses can be tested (Baker et al. 2015).
The potential of regenerative medicine is based on the regeneration and replacement ability of diseased tissues and organs (Atala 2008; Mendelson and Frenette 2014). Researches in the field of regenerative medicine have results that indicate that can be reported successful regeneration and replacement of many tissues and organs, including skin, heart, kidneys, and liver, as well as the potential to even improve some birth defects (Amado et al. 2017; Bailey et al. 2014; Knoepfler 2015; Tang et al. 2016).
Powerful biomaterials, mainly combinations of scaffolding, growth factors, and stem cells, have the function of replacing damaged tissue and showing that they function as original tissue or have the ability to stimulate native tissue regeneration to establish successful regenerative medicine platforms (Amado et al. 2017; Gao and Cui 2016; Guan et al. 2017). These platforms focus on tissue environmental changes due to the incorporation of exogenous materials and biological factors with the sole purpose of accelerating and promoting the body’s healing process. Extracellular matrix materials and biomimetics have been used for more than a decade, more than just providing physical support (Amado et al. 2017; Alves da Silva et al. 2017; Goncalves et al. 2017; Pina et al. 2017). Materials and biomimetics can in their own way stimulate the regeneration process, but they can also be biomolecules on their own that affect cell growth (Guan et al. 2017). In addition to the necessary physical support to the cells, it is advantageous for the scaffolding biomaterial to include biological signs or signals that enhance or improve tissue regeneration and performance (Dzobo et al. 2016; Evans et al. 2010; Sadtler et al. 2016). Different tissues possess the different regenerative capacities. So, some do not need the addition of cells, but only biomaterial and biological agents. Other tissues have limited regeneration capacities and need biomaterial, biomolecules, and cells for regeneration. Cartilage and cornea are tissues and organs with limited or no regenerative capacity, while the liver and lungs have a high regenerative capacity (Amado et al. 2017; Atala 2008; Atala 2012; Kotton and Morrisey 2014).
Native tissues have a wide range of physical characteristics, of which elasticity and permeability stand out. For example, human tissue shows tissue-specific elasticity in the range of about seven orders of magnitude, starting at only 167 Pa for breast tissue (Guan et al. 2017; Paszek et al. 2005), to as high as 54 GPa for hard tissue (Choi et al. 1990). There are also various optimum pore sizes of implants for inducing regeneration of different types of tissues: 5 μm in pore diameter for vascularization (Brauker et al. 1995), 5–15 μm for fibroblast ingrowth (Klawitter and Hulbert 1971), 20–125 μm for adult skin regeneration (Yannas et al. 1989), and 100–350 μm for bone regeneration (Annabi et al. 2010). Cells can recognize mechanical signals and through mechanical transduction reach further processes differentiated into different families (Guan et al. 2017; Huebsch et al. 2010; Engler et al. 2006). Hydrogel materials can contain biophysical responsiveness in a controlled way to control cellular manner, mimicking these physical characteristics on a micro and nano scale. This approach gives an obvious understanding of the mechanism of cell development and their reactions in various diseases (Guan et al. 2017).
One of the three most important elements in the basic concept of regenerative medicine is scaffolding materials. They form the basis of regenerative medicine engineering. Surgical procedures involving the use of scaffolds as medical devices are performed daily to replace or repair tissue damaged by disease or trauma. Highly porous scaffolding biomaterials combined with the body cells can form templates for tissue regeneration, which lead to the growth of new tissue. The scaffold has a prominent role in the design and fabrication of 2D and 3D models, including surface ligands and molecular architecture, nanoparticle-cell interactions (Amado et al. 2017).
Scaffold modeling is a crucial part of tissue engineering and regenerative medicine. A fundamental tool to guide tissue formation both in vitro and in vivo should be an optimal designed 3D scaffold. Properties like high surface-area-to-volume ratio, porosity, pore size, pore design, pore interconnectivity, permeability, and degradation should be taken under consideration when designing scaffold material for various and tailored applications. These permit a desirable biological network for cell migration, nutrient transportation, and therefore the mechanical stiffness, and strength are therefore obtained (Budama-Kilinc et al. 2017; Parker et al. 2002; Fang et al. 2005). Growth factors and drug release process should even be considered to attain optimized tissue growth as scaffold degraded. Moreover, some researches have shown the advantages for tissue regeneration of using curvature and concave surfaces compared to convex and planar ones (Zadpoor 2015). Two scaffolding design approaches may be used to fulfill the aforementioned demands. The first one is predicated on the native tissue. The second relies on the unit’s digital cell model, both addressing tailored scaffolding geometry. The geometry obtained can then be applied to computer-aided engineering studies to optimize the performances of the tailored bioengineering scaffold (Amado et al. 2017).
The artificial scaffold is made and its properties are optimized according to the complex structure of the tissue. The scaffolding designed in this way should be suitable for cell adhesion, proliferation, and ECM formation. This is how the ECM recovers. Medical devices should be designed to create, induce or congest tissue reactions (Amado et al. 2017; Haycock 2011). The perfect scaffolding should have optimal and favorable biocompatibility, biodegradability, mechanics, interconnection of pores of appropriate sizes that will accommodate cells, as well as an optimal exchange of nutrients and waste products with its three-dimensional space for cell growth in an organized manner (Amado et al. 2017; Seol et al. 2013). Tailoring biomaterials for enhanced biofunctionality can be accomplished by employing a kind of approaches that involve the introduction of chemical, topographical, or mechanical cues via top-down or bottom-up approaches (Camarero-Espinosa and Cooper-White 2016). It is very important to choose favorable biomaterials, as well as techniques and methods of obtaining them. There is a whole range of natural and synthetic components used for scaffold syntheses such as biometals, ceramics, bioactive glass, phosphates, and polymers. Bioactive ceramic scaffolds are favorable for bone tissue regeneration due to their biological functionality. However, ceramics as scaffolding materials is restricted owing to difficult processability and inherent brittleness (Seol et al. 2013). Rezwan’s group (Rezwan et al. 2006) showed that conventional material processing methods are adapted and extended for the incorporation of inorganic bioactive part into porous and interconnected 3D polymeric networks (Amado et al. 2017). Advanced biomaterials are hybrids with adjustable bioactivity and biodegradability (Rezwan et al. 2006). Addressing these issues, research has focused on the mechanical testing of polymer-bioglass composites. Consequently, scaffolds of identical density are compared and it has been confirmed that the addition of bioglass reduces the elastic gradient and relieves tension. Therefore, the highest content of bioglass seems to have a beneficial effect because it does not significantly impair the mechanics of the scaffold and improves bioactivity (Fiedler et al. 2015). The creation of biodegradable, bioactive, “living” composite biomaterials loaded with biomolecules, which is characterized by great adaptability to the biological environment (Rezwan et al. 2006), is a promising approach. Biomolecules are added to speed up the healing process, and they are sensitive to elevated temperatures and extreme chemical conditions. Therefore, their loading during scaffolding production is not easy. Another interesting approach is the immobilization of proteins and growth factors by functionalizing the scaffold surface in the postprocessing phase (Amado et al. 2017; Cosson et al. 2015).
“Soft” material routes like sol-gel processing may be a platform to include biomolecules during scaffold fabrication. But, highly porous, interconnected pore structures for bioactive organic/inorganic hybrids have not yet been achieved, which is important for scaffolding application. Further, an important issue is a reason for the local impact of growth factors on the cell and tissue systems, especially long-term effects (Amado et al. 2017; Rezwan et al. 2006). The foremost, crucial parameters that determine the performance of a designed implant are mechanical characteristics which depend on the process and structural characteristics of the biomaterials. In such a way, desired mechanical properties can accomplish by modifying the structural characteristics of a biomaterial. Cell biological behavior testing is required to check biocompatibility and bioactivity after surface modifications (Amado et al. 2017; Haycock 2011). The study of the interactions of biochemical and geometrical cues on stem cell differentiation and alignment should be also considered. The potential to spatially control stem cell orientation and differentiation toward multiple phenotypes simultaneously, i.e., myocyte, tenocyte, and osteoblast allow in vitro cells grown to more closely mimic aspects of native structure organization (Amado et al. 2017;Ker et al. 2011). Although the precise mechanism behind geometry-induced cell alignment is presently unknown, cells alignment observed on fibers may likely be attributed to a mix of factors including physical space constraint and relative stiffness of the underlying substrate; ultimately effecting changes in both cell spreading and cell stiffness, cells could also be predisposed toward a selected orientation through the modulation of mechanotransduction pathways via cytoskeletal rearrangements (Amado et al. 2017; Sun et al. 2004).
A more robust choice to create graded structures that resemble the biological interface is to form multilayer scaffolds as combinations of several biomaterials. The newest technologies deal with the development of multilayer scaffolds and the controlled release of bioactive agents to promote in situ regeneration of biological tissues and aim to perfect the available traditional treatments. Long-term evaluation is indispensable with a special focus on studying the biological and mechanical properties of the designed tissues to verify the potential of those novel approaches (Amado et al. 2017; López-Ruiz et al. 2016).
The scaffold design should enable the creation of a bioactive dynamic system, which will be a favorable environment for cells. One of the types of scaffolds is nanofibers that are obtained by the technique of surface modification, which contribute to an improved understanding of in vitro and in vivo cellular behavior. This approach implies the interconnection of knowledge of science and technology (Amado et al. 2017; Cheung et al. 2015; Kariduraganavar 2016).
In organ engineering, it is important to take care that the regeneration of functional tissue takes place, whereby it is necessary to achieve cell viability and differentiation, stimulate proliferation, the direction of modulation, and the rate of cell migration and cell adhesion regulation (Amado et al. 2017). Cell viability is determined through morphological changes or membrane permeability, as a physiological condition based on cell culture staining. Cells are cultured on a three-dimensional biocompatible scaffold. This is followed by a process of degradation and resorption at a projected rate whereby soft and hard tissues are regenerated in vitro or in vivo conditions (Amado et al. 2017; Hutmacher 2001).
The bioengineering approach in scaffolding design in vivo is guided by the conditions of oxygen diffusion and the flow of nutrient components so that the thickness of the scaffold is adjusted to several hundred microns (Amado et al. 2017; Cosson et al. 2015). Great care must be taken with scaling in the transition to clinical applications from in vivo testing. An important topic is the process of tissue vascularization. Good blood circulation to the tissues leads to a favorable flow of nutrients and other components and leads to the proper integration of cells and the healing process. The latest biocreation techniques, especially when it comes to bulkier medical devices scaffolds, lead to more advanced solutions to vascularization issues (Amado et al. 2017;Lim et al. 2017).
The most widespread biomaterials used for the design of scaffolding and medical devices in regenerative engineering are polymers (Budama-Kilinc et al. 2017; Piskin 1994; Ji et al. 2006). The properties of materials that recommend them to be used toward biomaterials are composition, hydrophilicity, swelling, surface energy, adhesiveness, the possibility of degradation, and erosion mechanism. Polymeric scaffolds have emerged as the biomaterials of choice due to their specific properties that can be adjusted to different synthesis processes and techniques (the length of polymeric chains is a key factor that further determines all properties relevant to biomedical applications). Due to all the above, it is possible to very finely achieve the most favorable bioactivity and biocompatibility of scaffolds. Research on the development of artificial skin and cartilage has been conducted in that direction (Eaglstein and Falanga 1998), bone and cartilage (Boyan et al. 1999), liver (Mayer et al. 2000), heart valves and arteries (Mayer et al. 1997), bladder (Oberpenning et al. 1999), pancreas (Tziampazis and Sambanis 1995), nerves (Mohammad et al. 2000), corneas (Germain et al. 1999), and various other soft tissues (Diedwardo et al. 1999).
One of the scaffolding polymeric materials classifications is synthetic, biologic, degradable, or nondegradable concerning their application (Budama-Kilinc et al. 2017; Ramakrishna et al. 2001). The behavior of polymers results from their properties-composition, structure, conformation, and arrangement of basic repeating units.
Natural polymers are often reviewed as the first biodegradable biomaterials used clinically (Nair and Laurencin 2007). Natural materials are considered to be bioactive properties and thus lead to better interaction with cells. This leads to improved cell performance in the biological system. They are included in natural polymers proteins (silk, collagen, gelatin, fibrinogen, elastin, keratin, actin, and myosin), polysaccharides (cellulose and derivatives, amylose, dextran, chitin, and glycosaminoglycans), or polynucleotides (DNA, RNA) (Yannas 2004).
Synthetic polymeric materials have proven to be very favorable in the function of restoring the structure and performance of damaged tissues. Their properties essential for this purpose such as porosity, degradation time, and mechanical properties can be adjusted in various ways and adapted to specific applications. One of the advantages of synthetic polymers is that they are often cheaper than biological. Their production takes place in large uniform batches, and the shelf life is longer. Also, a wide range of commercially available synthetic polymers possesses physicochemical and mechanical properties that mimic the properties of biological tissues. Synthetic polymers represent the largest group of biodegradable polymers, and that they can be produced under controlled conditions. Their properties are predictable and repeatable, and they include strength to different types of loads, multiple module types, and degree of degradation (Gunatillake et al. 2006). Polylactides and polyglycolides (homo- and copolymers) are among the foremost commonly used synthetic polymers in tissue engineering (Ma 2004). Polyhydroxyalkanoates belong to a category of microbial polyesters and are widely investigated for tissue and regenerative engineering applications (Chen and Wang 2002).
Bioactive ceramics and specified silicate and phosphate glasses (bioactive glasses) and glass-ceramics (apatite-wollastonite) can react with physiological fluids and through cellular activity form firm interconnections to hard and in some cases soft tissue (Hench 1998). However, the biocompatibility and biodegradability of these compositions are often insufficient, diminishing their potential use within the clinical part. By combining synthetic and natural polymeric components in different ways or by using composite materials that improve the properties of scaffolds, such phenomena are promoted and thus enable controlled degradation (Cascone et al. 2001) and improve biocompatibility in tissue engineering (Ciardelli et al. 2005). Especially, degradable polymers and bioactive inorganics in synergy represent the platform to achieve mechanical and biological performance in hard tissue (Roether et al. 2002).
In the last 10 years, hydrogels as three-dimensional polymer networks that have taken precedence as leading biomaterials in the field of tissue engineering, where they are used as scaffolding to guide the growth of new tissues. The potential impact of hydrogel materials in the biomedical field has been significantly increased based on the possibilities of tailored design, especially those of biodegradability. This is followed by a very important area of the system for the controlled release of active agents (Budama-Kilinc et al. 2017; Cabodi et al. 2005). When considering properties essential for tissue regeneration-biocompatibility, cell-controlled degradability, and internal cell interactions, naturally occurring polymer-based hydrogels have an advantage. As for obtaining this type of polymer, there is variation in batches, but their structure and functional properties are precisely controlled. Hydrogels possess a structural identity similar to the macromolecular based constituents within the body and highly biocompatible behavior (Jhon and Andrade 1973). Hydrogels are made of synthetic or natural polymers or combinations thereof, where covalent or noncovalent bonds are established by the cross-linking agent(s) (Hoffman 2001). For hydrogels to be used in tissue engineering, they must meet a whole range of standards to perform their role and contribute to the formation of new tissues. These criteria refer to the classical physical parameters (degradation and mechanics) similarly to biological parameters (cell adhesion). It is commonly presumed that the degradation rates of tissue scaffolds must be matched to the speed of varied cellular processes to optimize tissue regeneration (Hubbell 1999; Lee and Mooney 2001). Therefore, the degradation behavior of biodegradable hydrogels should be defined, reproducible, and tunable via hydrogel chemistry and structure. Biocompatible hydrogels are currently employed in cartilage healing, bone regeneration, wound dressings, and as drug delivery systems (Peppas and Khare 1993). Hydrogel loaded with growth factors can act to support the development and differentiation of cells within the newly formed tissues (Tabata 2003). Hydrogels are often favorable for promoting cell migration, angiogenesis, optimal water/fluid content, and rapid nutrient flow (Bryant and Anseth 2001). Hydrogel scaffolds are the subject of intensive research in the engineering of replacement connective tissues, primarily because of their biochemical similarity with the highly hydrophilic glycosaminoglycan components of connective tissues. Hydrogel-forming polymers of the natural source are collagen (Wallace and Rosenblatt 2003), gelatin (Kim et al. 2004), fibrin (Eyrich et al. 2007), hyaluronic acid (Solchaga et al. 2002), alginate (Kong et al. 2003), and chitosan (Francis Suh and Matthew 2000). Synthetic polymers are polylactides (Schmedlen et al. 2002), polypropylene fumarate-derived copolymers (Behravesh and Mikos 2003), polyethylene glycol derivatives, and polyvinyl alcohol (Bryant et al. 2004).
Alginate is a naturally derived macromolecule; polysaccharide extracted from brown algae, such as Macrocystis pyrifera, Laminaria hyperborea, Ascophyllum nodosum. Naturally, it has an anionic character and consists of β-D-mannuronic acid and α-L-guluronic acid repeating units (Das and Subuddhi 2020). It manifests vital properties like biocompatibility, biodegradability, nontoxicity, nonimmunogenicity, and transparency. Gelation is accomplished easily, which enables alginate to be widely used in biomedical applications such as drug delivery, cell encapsulation, wound healing, and tissue engineering (Das and Subuddhi 2020; Lee and Mooney 2012). A modified version of alginate is sodium alginate which is a salt of alginic acid. Alginate is polymeric material with good scaffold-forming properties that can be useful to treat the loss or failure of organs.
Alginate hydrogels are also being actively researched for their beneficial properties to mediate the regeneration and engineering of various tissues and organs, including skeletal muscle, nerve, pancreas, and liver (Lee and Mooney 2012). Current strategies for skeletal muscle regeneration apply to cell transplantation, growth factor delivery, or a fusion of both approaches (Saxena et al. 1999; Levenberg et al. 2005), and alginate hydrogels have found potential in these platforms. The combined delivery and release of vascular endothelial growth factor and insulin-like growth factor-1 from alginate hydrogels were used to regulate both angiogenesis and myogenesis (Lee and Mooney 2012). The localized and sustained delivery of both growth factors led to significant muscle regeneration and functional muscle formation, because of cell activation and proliferation, and cellular protection from apoptosis by the released factors (Borselli et al. 2010). Long-term survival and outward migration of primary myoblasts into damaged muscle tissue in vivo from RGD-alginate hydrogels were significantly improved by the sustained delivery of hepatocyte growth factor and fibroblast growth factor2 from the hydrogels (Hill et al. 2006a, b). This led to extensive repopulation of host muscle tissues and enhancement of the regeneration of muscle fibers at the wound site (Hill et al. 2006a, b).
Alginate hydrogels have also been tested as biomaterials that can act to repair the central and peripheral nervous system. Alginate-based highly anisotropic capillary gels, introduced into acute cervical spinal cord lesions in adult rats, were integrated into the spinal cord parenchyma without significant inflammatory responses and directed axonal regrowth (Prang et al. 2006). Alginate gels, covalently cross-linked with ethylenediamine, can be useful to restore a 50 mm gap in cat sciatic nerves (Lee and Mooney 2012; Hashimoto et al. 2005) and promote the outgrowth of regenerating axons and astrocyte reactions at the stump of transected spinal cords in young rats (Kataoka et al. 2004). Alginate gels are also used as glue for the repair of peripheral nerve gaps that could not be sutured (Suzuki et al. 2000).
Alginate has shown great use and potential as a biomaterial for several biomedical applications, for wound healing, drug delivery systems, in vitro cell culture, and tissue engineering (Lee and Mooney 2012). The foremost attractive features of alginate for these applications include biocompatibility, mild gelation conditions, and easy modifications to make alginate derivatives with new properties. There are documents on the safe clinical use of alginate as a wound healing and dressing, as well as pharmaceutical compositions. It can be safely implanted in a variety of applications, including islet transplantation for type 1 diabetes (Soon-Shiong and Heintz 1994) and chondrocyte transplantation for urinary incontinence and vesicoureteral (Diamond and Caldamone 1999; Kershen et al. 2000). A chemically modified alginate can be also widely used as a carrier to advance periodontal regeneration (Sculean et al. 2001). However, alginate gels have limited mechanical stiffness and more general physical properties. An ongoing challenge is matching the physical properties of alginate gels to the necessity in an exceedingly particular application. Consideration of the range of various available cross-linking strategies, using molecules with various chemical structures, molecular weights, and cross-linking functionality will often yield gels suitable for every application. Determined research concepts evaluate cell encapsulation strategies (Lee and Mooney 2012). But, covalent cross-linking reactions can cause toxicity to the cells to be encapsulated, and an appropriate choice of cell-compatible chemical reagents (initiator, activator), and thorough removal of unreacted components and by-products will likely be needed in those applications (Lee and Mooney 2012; Smeds and Grinstaff 2001).
Dynamical control over delivery can potentially improve the drug’s safety and effectiveness and assure new therapeutic platforms. On-demand drug release from alginate gels in response to external cues like mechanical signals (Lee et al. 2000) and magnetic fields (Lee and Mooney 2012; Zhao et al. 2011) can be exploited to design active depots of the many drugs, including therapeutic cells. The introduction of appropriate cell-interactive features to alginate is additionally crucial in many tissue engineering applications. The kind of adhesion ligands and their spatial organization in gels are key variables, as they can adjust cell phenotype and also the resultant function of regenerated tissues. While RGD peptides are extensively exploited thus far as a cell adhesion ligand, multiple ligands and/or a mix of ligands and soluble factors could also be required to properly produce replacement tissues and organs.
Gelatin is a natural polymer obtained by partial hydrolysis of collagen, which is considered to be nonimmunogenic, biodegradable, easy to process, and biocompatible for clinic use (Mohammadzadehmoghadam and Dong 2019; Lien et al. 2009; Aldana and Abraham 2017; Babitha et al. 2017). Most ECM is made of gelatin and carbohydrates. However, gelatin is rarely used as the sole constituent owing to its high brittleness, and thus needs to be functionalized using cross-linking, grafting, and blending methods (Mohammadzadehmoghadam and Dong 2019; Hersel et al. 2003; Zhang et al. 2006; Wongputtaraksa et al. 2012; Taddei et al. 2013; Poursamar et al. 2016).
Gelatin is often made through thermal and chemical denaturation of collagen with pronounced properties of nontoxic, nonirritant, and biodegradability, likewise nearly as good living body compatibility (Bigi et al. 1998; Bajpai and Kankane 2007). Gelatin contains an Arg-Gly-Asp (RGD) sequence which improved cell adhesion and migration (Huang et al. 2005). It possesses a high degree of biological functional groups and potential for tissue scaffolding applications. Gelatin can be used in pharmaceuticals, wound dressings, and adhesives in clinics because of its good cell viability and lack of antigenicity. Improved formability and low costs allow selection and mass production (Kim et al. 2005).
Gelatin can be also used as a coating agent to enhance cell attachment as a technique of vascular tissue regeneration (Nair and Thottappillil 2015). Gelatin shows gel-forming, thickening, emulsifying, and foaming proprieties. The mechanical ones depend on the supramolecular structure (Kozlov and Burdygina 1983). Syntheses of anionic or cationic gelatin are based on extraction conditions and fundamentally for filling molecules through electrostatic interaction. Since gelatin stability at high temperatures and a wide range of pH allow synthetic polymers to be grafted on the gelatin backbone. The methods are known as “grafting from”, polymerization on the functional surface of the substrate, “grafting to,” grafting of a fully functionalized polymer to the substrate, or “grafting through” (Sadeghi and Heidari 2011).
Gelatin-based formulations are employed in biomedicine and therapeutic agent controlled delivery (Sajkiewicz and Kołbuk 2014). Polyethyleneimine-functionalized gelatin can increase transfection efficiency thanks to positive nanoparticles that facilitate DNA loading (Kuo et al. 2011). It indicates the possibility to use hydrogel as vectors for gene controlled delivery.
Methacryloyl group-grafted gelatin, also known as gelatin methacrylate (GelMA) had been used for the microfabricated blood vessel. Gelatin electrospun fibers loaded with antibiotic drugs show a strong antibacterial activity but this gelatin has to be reinforced with materials such as graphene oxide and boron nitride, to improve poor mechanical proprieties (Bakhsheshi-Rad et al. 2017; Nagarajan et al. 2017; Nagarajan et al. 2016a, b).
Gelatin copolymer acts as a natural cell surface that reacts under mechanical stimulation when the electrospinning process is used to create tubular scaffolding and allows obtaining a similar morphology as the native ECM structure (Thomas and Nair 2012). Panzavolta’s group obtained electrospun gelatin nanofibers cross-linked with genipin (low-toxicity agent) which reduces the extensibility of the electrospun mats, producing appreciable improvements in elastic modulus and breaking stress (Panzavolta et al. 2011). Long-term studies on cross-linked electrospun gelatin are still in progress to confirm its efficacy as a biomaterial scaffold for blood vessel tissue engineering.
2-Hydroxyethyl methacrylate (HEMA) is a famous monomer due to its versatility for syntheses of polymeric biomaterials-hydrogels and hydrogel scaffolds. HEMA-based polymeric materials show favorable biocompatibility and tunable hydrophilicity. Therefore, they have multiple applications in pharmaceutical and biomedical fields such as coatings, intraocular lenses, scaffolds, and controlled drug release systems. To tune the biocompatibility, swelling, and mechanical properties of HEMA-based hydrogels, they can be combined with hydrophilic polymeric components (Prasitsilp et al. 2003; Hejcl et al. 2008; Kubinova et al. 2015; Babić and Tomić 2020; Tomić and Vuković 2020).
6.2 Design and Properties of Alginate/Gelatin/2-Hydroxyethyl Methacrylate Hydrogel Scaffolds
6.2.1 Alginate/Gelatin/2-Hydroxyethyl Methacrylate Polymeric Hydrogel Scaffolds
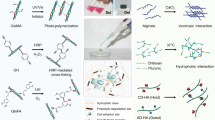
Two series of novel, porous, and degradable hydrogel scaffolds were successfully synthesized using a combination of natural polymers-alginate and gelatin, and synthetic monomer 2-hydroxyethyl methacrylate (AGH), by cryogelation and porogenation. The synthesis path is shown in Scheme 6.1.
Hydrogel scaffolds were made in three steps.In the first step, porous and the mechanically strong polymeric network was obtained by free-radical cross-linking polymerization of 2-hydroxyethyl methacrylate in the presence of an initiator, activator, and cross-linking agent. In the second step, an additional polymeric network was created by the cross-linking of gelatin. The third step is alginate chains are loaded to intertwine in the networks.
6.2.1.1 Biocompatibility of AGH Hydrogel Scaffolds
The main focus during the design of the scaffolding polymeric biomaterials which can be used in regenerative engineering and medicine is the first step related to in vitro and in vivo biocompatibility testing of the hydrogel matrices. The biocompatibility of AGH hydrogel scaffolds was evaluated in a cytotoxicity test on normal human fibroblasts (MRC5). The results of this assay for AGH samples are shown in Fig. 6.1. A50G50Hcryo, A30G70Hcryo, AHcryo, A50G50Hpor, and A30G70Hpor samples showed very favorable cellular viability in contact with cell culture. The AHpor sample showed a lower level of cell survival (for higher extract concentration). It has been shown that all scaffolds, when delivered directly to cells, support the accumulation of cells on their surface (Fig. 6.1). The obtained data confirm that AGH hydrogel scaffolds demonstrate favorable level of cytocompatibility. Therefore, these scaffolding materials are suitable for applications as biomaterials in tissue regeneration.
To address whether the alginate/gelatin/methacrylate hydrogels could be used for human use, we assessed their in vivo toxicity using the zebrafish model. The zebrafish model was accepted as a valid alternative to mammalian models (rats mice) for toxicity and biocompatibility evaluation of novel biomaterial sowing to the high molecular, genetic, physiological, and immunological similarity to humans, and good correlation in response to pharmaceuticals and bioactive agents (Lieschke and Currie 2007; MacRae and Peterson 2015), simplifying thus the route to clinical trials and reducing the failure at later stages of testing (Barros et al. 2008; MacRae and Peterson 2015).
Given that the organisms at embryonic developmental stages are more sensitive to the chemical insults than as an adult, we subjected zebrafish embryos at the 6 hpf stage indirectly, to the material’s extracts (embryo water in which the ground materials were extracted over 72 h at 37 °C and 180 rpm and applied as 100%, 50%, 25%, and 10% suspensions) and to the ground material (200 μg/mL) for 5 days. Obtained data showed that all AGHcryo and AGHpor scaffolding biomaterials tested, regardless of the method was no toxic to the zebrafish embryos, since there were no lethality, developmental malformation, cardiovascular disorders, or signs of hepatotoxicity (the liver necrosis and the yolk retention) (Fig. 6.2), indicating the safety of the tested materials. We showed the safety and biocompatibility (no inflammation and no immunosuppression) of 2-hydroxyethyl methacrylate hydrogels using the zebrafish model (Tomić et al. 2020). In this study, we showed that AGH hydrogel scaffolds present also nontoxic materials, indicating their favorable potential in biomedical applications. Otherwise, the alginate-based materials have been applied as safe biomaterials for the food packing and oral delivery to zebrafish larvae or adults (Onal and Langdon 2000; Lin et al. 2016) and more recently as the carriers of drugs to improve their therapeutic outcome (controlled release, reduced toxicity, increase in efficacy) (Tzankova et al. 2017; Gao et al. 2017).
6.2.1.2 Structural Properties of AGH Hydrogel Scaffolds
Fourier transform infrared spectroscopy (FTIR) gives information about the structural characteristics of created scaffolds. FTIR spectra are tracked to find the most important bands indicating the presence of functional groups originated from scaffold components (alginate, gelatin, and 2-hydroxyethyl methacrylate). Peaks indicating the presence of HEMA in the polymeric network are on the following wavenumbers 3360 cm−1, 2940 cm−1, 1640 cm−1, and 1710 cm−1 and are assigned to asymmetric and symmetric stretching vibrations (terminal hydroxyl group), methylene stretching, and terminal vinyl, and a carbonyl group. The peak at 1640 cm−1 can be assigned to the asymmetric stretching of COO− of alginate (Wang et al. 2016). Also, the FTIR spectra show characteristic bands for alginate at 1027 cm−1 and 1086 cm−1 for its glucuronic (G) and manuronic (M) acid units. The bands at 879 cm−1 and 822 cm−1 demonstrate β-glycosidic linkages between G and M units of alginate. Besides these, characteristic bands of gelatin at 1620 cm−1 and 1536 cm−1 were observed, which correspond to amide I and amide II groups (Sharma et al. 2016). The peak at about 1150 cm−1, related to C-O vibration, indicates cross-linking of gelatin, and confirms its successful incorporation into the polymeric structure. Also, the broad peak from 2900 cm−1 to 3600 cm−1 illustrates a strong -OH bond resulting from the interaction between alginate and gelatin (Wang et al. 2016).
6.2.1.3 Water Uptake Capacity of AGH Hydrogel Scaffolds
AGH hydrogel scaffold water uptake capacity shows the hydration of dry scaffold. The AGH matrices swell up to 90% within 10 min, reaching equilibrium within 30 min. Once the scaffold was water equilibrated, further, it remains at equilibrium for a longer period. In that way shows their capacity for water uptake and the ability to retain water over a long period. AGH hydrogel scaffolds show a time-favorable hydration profile which is suitable for use in tissue regeneration.
6.2.2 Alginate/Gelatin/2-Hydroxyethyl Methacrylate Hydrogel Scaffolds Made by Cryogelation
6.2.2.1 Morphology of AGHcryo Hydrogel Scaffolds
The demands that scaffolds need to meet for proper cell attachment are to easily deliver oxygen, nutrients, water-soluble metabolites, and waste products between the inside and outside of the hydrogel scaffold. To fulfill these demands, the scaffold must exhibit a large number of interconnected pores. To examine the morphology of created scaffolds based on alginate, gelatin, and 2-hydroxyethyl methacrylate, prepared by cryogelation (AGHcryo), a scanning electron microscopy (SEM) was performed. The obtained SEM micrographs are displayed in Fig. 6.3. As can be seen, the interior of the scaffolds is highly porous, with open, interconnected pores, with spherical to elliptical shapes. The pore size was found to vary between 10 and 100 μm, which can provide efficient vascularization, proliferation, and differentiation of cells.
The surface morphology of AGHcryo scaffolds can be described as rough and porous, similar to the interior architecture of the tested scaffolds. When compared to the scaffolding materials with smooth and nonporous walls, AGHcryo scaffolds are expected to enhance the attachment of cells and their mutual interaction. The internal and surface morphology of scaffolds with different gelatin content shows different patterns that can be attributed to the more cross-links of gelatin. Obtained data for morphological testing indicate that AGHcryo scaffolds are suitable for tissue regeneration and biomedical applications.
6.2.2.2 Mechanical Properties of AGHcryo Hydrogel Scaffolds
Mechanical properties are very valuable properties of the scaffolds for tissue engineering. Therefore, the scaffold should possess good strength. To evaluate the mechanical properties of hydrogel scaffolds based on alginate, gelatin, and 2-hydroxyethyl methacrylate, prepared by cryogelation (AGHcryo), Young’s modulus (E) was determined. The results revealed E values of AGHcryo samples in the range of 1.251–9.755 MPa, thus clearly indicating that scaffold composition determines their mechanical properties. The lowest E value exhibited the AHcryo sample (1.251 MPa), while A50G50Hcryo showed the highest value (9.755 MPa). The presence of gelatin resulted in a more compact, mechanically stronger structure, but with the further increase of gelatin content value of Young’s modulus was decreased. Certainly, according to known data related to the mechanical characteristics of native tissues, AGHcryo scaffolds possess great potential for tissue regeneration application, especially for soft tissues and skin. The desired mechanical strength can be adjusted by synthesis optimization and adjusting the component ratios.
6.2.2.3 Porosity of AGHcryo Hydrogel Scaffolds
The porosity of hydrogel scaffolds based on alginate, gelatin, and 2-hydroxyethyl methacrylate, prepared by cryogelation (AGHcryo) was evaluated by the bulk density method. The porosity values of hydrogel scaffolds depend on the composition of scaffolds. The results obtained reveal a high level of porosity of all tested samples, over 80%. The highest porosity showed the AHcryo sample (84.63%), while the lowest value has an A50G50Hcryo sample (82.26%). The presence of gelatin slightly decreased the porosity, most probably due to the more cross-links of gelatin. Results indicate that the porosity of the AGHcryo hydrogel scaffolds obtained by cryogelation can be adjusted and adapted by modifications of scaffold composition and variations of components ratio. Generally, there is no change in porosity due to the increased surface area and hydrophilicity of gelatin and alginate.
6.2.2.4 Hydrophilicity of AGHcryo Hydrogel Scaffolds
The surface hydrophilicity of the alginate/gelatin/2-hydroxyethyl methacrylate hydrogel scaffolds, prepared by cryogelation was assessed by the contact angle measuring through droplet water spread on a surface. As it is well known, the hydrophilicity of material is reflected in contact angle low values. The results obtained from the static water contact angle are presented in Fig. 6.4. A50G50Hcryo hydrogel scaffold was found to be fully hydrophilic, due to the completely wet surface and disappearance of the water drop. The contact angle values for A30G70Hcryo and AHcryo samples are 81.55 and 81.20. The surface hydrophilicity of AGHcryo scaffolds certainly depends on the composition and ratio of natural polymers used for the syntheses. Obtained data showed favorable hydrophilicity of AGHcryo hydrogel scaffolds. Thus the hydrophilic character of hydrogels based on alginate, gelatin, and 2-hydroxyethyl methacrylate, prepared by cryogelation can provide efficient attachment, proliferation, and further growth of the cells.
6.2.2.5 In Vitro Degradation Properties of AGHcryo Hydrogel Scaffolds
The in vitro degradation process was monitored in controlled, physiologically conditions-simulated buffer fluid of pH 7.40 and at a temperature of 37 °C. The weight loss, as an indicator of degradation of alginate/gelatin/2-hydroxyethyl methacrylate hydrogel scaffolds, prepared using cryogelation was investigated for 3 months. The tested scaffolds degraded up to 11% after 3 months. The highest weight loss was detected for the AHcryo scaffold (11.33%), while the lowest weight loss exhibited A30G70Hpor (3.41%). The decrease of alginate content and the increase of gelatin in scaffolds resulted in decreased biodegradability. As it is assumed, the degree of cross-linking of gelatin has a prominent influence on the scaffolds biodegradability.
6.2.3 Alginate/Gelatin/2-Hydroxyethyl Methacrylate Hydrogel Scaffolds Made by Porogenation
6.2.3.1 Morphology of AGHpor Hydrogel Scaffolds
Hydrogel scaffolds designed for tissue regeneration must be highly porous with an open interconnected pore, to permit a large surface area relative to the scaffold’s volume. The porosity is directly coherent to the function of the scaffold. Pronounced and interconnected porosity will promote cell growth, uniform cell distribution, and assist the neovascularization of the matrix. According to the latest studies, scaffolds should have a distribution of pores ranging from micrometers to 100 μm, improving the capillarity of the scaffolds and enabling the ingrowth of cells (Kim et al. 2019). Morphological properties of the alginate/gelatin/2-hydroxyethyl methacrylate hydrogel scaffolds, prepared by porogenation (AGHpor) were tested using scanning electron microscopy (SEM) (Fig. 6.5). SEM micrographs of the cross-sections revealed a uniform porous structure with interconnected pores. No phase separation and occurrence of crystalline regions phenomena were detected, which indicate the compactness and compatibility between components of the resulting polymeric network scaffolds. The addition and increase of gelatin content in the scaffolds reflected in a more porous, almost like a honeycomb, structure with the smaller pores finely distributed in larger pores. Scaffold’s architecture can be depicted as the interior is porous, with open, interconnected pores, with spherical to elliptical shapes, thus providing efficient nutrient flow and distribution, the proper vascularization, proliferation, and differentiation support for the cells.
Also, micrographs of the scaffold’s surfaces revealed a range of pore sizes from a few microns to 200 μm, as well as their interconnections. The larger ones are filled with small pores, which indicate that the surface porosity can contribute to the interactions between these scaffolding materials and the cells, which implies their faster attachment.
6.2.3.2 Mechanical Properties of AGHpor Hydrogel Scaffolds
Mechanical properties are a very valuable parameter for scaffolding engineering because scaffolding must withstand handling and should show initial load-bearing capacity. To achieve this, the challenge is to combine hydrogel scaffolding of natural/synthetic origin. Strength tests were performed to assess the mechanical performance of the scaffolds. The focus of current researches in tissue engineering is to make a porous scaffold that mimics the native extracellular matrix (ECM). Among the demands, mechanical properties are essential factors to consider in scaffolds production. Mechanical strength is defined by the impact resistance of final products to maintain the integrity of the scaffold during implantation (Tran et al. 2018). The material application for tissue engineering requires the resemblance of deformable characteristics between the biomaterial and the analog tissue. The cell attachment, growth, and function in such a 3D structure depend on the scaffold mechanical properties (Lim et al. 2019). Elastic modulus, as a representative of the stiffness of the biomaterial, is an indicator of similarity between the biomaterial aimed to replace or repair particular tissue.
Young’s modulus (E) of hydrogel alginate/gelatin/2-hydroxyethyl methacrylate scaffolds, prepared by porogenation was determined and the obtained values depend on the composition of the scaffolds. As was expected, the reverse trend of calculated E values was noticed compared to the determined porosity of the hydrogel scaffolds. The lowest E value exhibited A50G50Hpor (0.988 MPa), the scaffold with the highest level of porosity. The increase of gelatin content resulted in a more compact, mechanically stronger structure, thus the A30G70Hpor sample showed the highest value of Young’s modulus (4.056 MPa). AHpor scaffold has E value near the highest calculated (3.102 MPa).
The obtained data indicate that the mechanical properties can be tuned through control of the scaffold’s composition. According to known data, the native skin has Young’s modulus in a range of 4.6–20.0 MPa, while the E value of cartilage is 12.0 MPa (Joodaki and Panzer 2018; Żak et al. 2011). Thus, alginate/gelatin/2-hydroxyethyl methacrylate scaffolds, prepared by porogenation can realize the requirements for the specific biomedical application. Additionally, by altering scaffold composition and the ratio of components, favorable mechanical strength could be reached.
6.2.3.3 Porosity of AGHpor hydrogel Scaffolds
The specifically defined porosity of the scaffolding materials is certainly one of the crucial requests that must be fulfilled to create an adequate 3D matrix for cell attachment, viability, and growth to successfully regenerate damaged tissue. The level of porosity of a biomaterial can be evaluated by the bulk density method, as it was performed in this study. The results obtained for AGHpor hydrogel scaffolds show that AGHpor tested scaffolds exhibited values of porosity in the range of 28–70%, thus confirming the results of the morphological study. The presence of gelatin increased the porosity of the hydrogels. The minimum value showed AHpor (28.48%), due to the intertwined chains of alginate in the polymeric matrix which decreases available free space. The highest porosity exhibited for the A50G50Hpor sample (69.92%). Further increase of gelatin content slightly decreased the porosity of the hydrogel scaffolds, probably due to the more cross-links of gelatin. Thus, scaffold composition and component variations play a notable role in tailoring the specific and targeted porosity of these biomaterials.
6.2.3.4 Hydrophilicity of AGHpor Hydrogel Scaffolds
The extracellular matrix hydrophilicity is a valuable parameter affecting cell adhesion processes in tissue engineering. Low surface wettability influences the attachment, colonization, and growth of cells (Cho et al. 2015). Focal adhesion represents the interaction between cells and scaffold or the specific sites of their contacts. When the scaffold surface has a hydrophobic character, it disables the focal adhesion. Nowadays, the development of scaffolding materials is focused on surface modifications to achieve desirable hydrophilicity (Chang and Wang 2011).
The surface hydrophilicity of hydrogel scaffolds is assessed by measuring the contact angle through the water droplet spread on a surface. A lower contact angle indicates higher surface hydrophilicity. Figure 6.6 shows the static water contact angle results obtained reveal the hydrophilic character of AGHpor hydrogel scaffolds. As can be observed, A50G50Hpor and A30G70Hpor hydrogel scaffolds are completely hydrophilic, where water has completely wetted their surface, with the drop disappearing immediately after being placed on the surface of the hydrogel. AHpor sample shows a slightly small wetting angle. The obtained results suggest that the AGHpor hydrogel scaffolds are suitable as scaffolding biomaterials to enable favorable adhesion, proliferation, and differentiation of various types of cells.
6.2.3.5 In Vitro Degradation Properties of AGHpor Hydrogel Scaffolds
Scaffold degradation and the matching rate between scaffold degradation and new tissue growth are crucial factors for advanced tissue regeneration (Zhang et al. 2014). Synthetic biodegradable polymers can be used extensively for scaffold fabrication due to desirable mechanical support to the 3D matrix, and the possibility to control the degradation (Sung et al. 2004). Natural polymers, biopolymers, e.g., alginate and gelatin, are suitable candidates for porous ECM-mimicking scaffolds, owing to their biodegradable and biocompatible nature (Bettinger et al. 2007).
The weight loss, as an indicator of degradation, for alginate/gelatin/2-hydroxyethyl methacrylate hydrogel scaffolds is investigated during 3 months, in simulated buffer fluid of pH 7.40, at 37 °C. The scaffolds are degraded up to 3% after 3 months. The highest weight loss exhibited A30G70Hpor (3.07%), suggesting that the increase of gelatin content contributed to the biodegradability of the hydrogels. AHpor and A50G50Hpor degraded at a similar rate, with weight loss of around 1.60%.
From the obtained data for the rate of weight loss of AGHpor scaffolding biomaterials, it can be said that the composition of the scaffolds affects the degradation process in such a way that the desired degradation rate can be achieved by varying and fine adjustment of the component ratio.
6.3 Summary and Future Perspectives
In our researches, two series of scaffolding biomaterials, based on alginate/gelatin/methacrylate, were synthesized by free-radical polymerization/cross-linking reaction using special methods of cryogelation and porogenaion. All samples showed favorable properties thus suitable for tissue regeneration and engineering-biocompatibility, water uptake, morphology, mechanical properties, porosity, hydrophilicity, and degradation.
6.3.1 AGHcryo Hydrogel Scaffolds
We have successfully developed hydrogel scaffolds of alginate, gelatin, and 2-hydroxyethyl methacrylate by free-radical cross-linking polymerization using cryogelation. Results obtained for cytotoxicity, it can see that AGHcryo hydrogel scaffolds do not show significant changes in cell viability with the composition scaffold, and are exceptionally cytocompatible, and therefore suitable as polymeric biomaterials for tissue regeneration. The in vivo zebrafish embryos assay test showed that the AGHcryo scaffolding materials tested were no toxic effects, since there was no lethality, developmental malformation, cardiovascular disorders, or signs of hepatotoxicity, which means they are safe to use in tissue regeneration. The spectroscopic characteristics of the AGHcryo scaffolding materials demonstrated the presence of bands indicating that the polymeric networks were constructed of alginate, gelatin, and 2-hydroxyethyl methacrylate components. Water uptake behavior for AGHcryo hydrogel scaffolds demonstrated a time-favorable hydration profile which is suitable for use in tissue regeneration. The morphology of AGHcryo hydrogel scaffolds is highly porous, with open, spherical to elliptical shapes, interconnected pores, with pore size in the range of 10–100 μm, which can provide efficient vascularization, proliferation, and differentiation of cells that meet the requirements to be used for tissue regeneration. The mechanical properties of AGHcryo scaffold samples, represented by the modulus of elasticity, are in the range of 1.251–9.755 MPa, and depend on the composition of the scaffolds. These values indicate the great potential of AGHcryo scaffolding materials for tissue regeneration, especially for soft tissues and skin. The porosity data of AGHcryo scaffold samples are in the range of 80–85%. This parameter can be adjusted and adapted by modifications of scaffold composition and variations of components ratio. A50G50Hcryo hydrogel scaffold was found to be fully hydrophilic. The contact angle values for A30G70Hcryo and AHcryo samples are 81.55 and 81.20. Obtained data showed favorable hydrophilicity of AGHcryo hydrogel scaffolds. Thus the hydrophilic character of alginate/gelatin/2-hydroxyethyl methacrylate hydrogels, prepared by cryogelation can provide efficient cell attachment, proliferation, and further growth. The in vitro degradation process was monitored for 3 months. The tested AGHcryo hydrogel scaffolds degraded up to 11% after 3 months. The highest weight loss was detected for the AHcryo scaffold, while the lowest weight loss exhibited A30G70Hpor.
6.3.2 AGHpor Hydrogel Scaffolds
We have designed alginate/gelatin/2-hydroxyethyl methacrylate hydrogel scaffolds by free-radical polymerization/cross-linking using porogenation. The cytotoxicity assay for AGHpor hydrogel scaffolds shows satisfied cell viability (only AHpor for higher extract concentration shows lower cell viability). In vivo zebrafish embryos assay test showed that the AGHpor scaffolding materials were no toxic effects since there was no lethality, developmental malformation, cardiovascular disorders, or signs of hepatotoxicity. Therefore, AGHpor scaffolding materials are safe to use in tissue regeneration applications as polymeric biomaterials. The spectroscopic characteristics of the AGHpor scaffolding materials demonstrated the presence of bands indicating that the polymeric networks were built of alginate, gelatin, and 2-hydroxyethyl methacrylate components. Water uptake behavior for AGHpor hydrogel scaffolds displayed a time-favorable hydration profile which is suitable for use in tissue regeneration. Morphology of AGHpor hydrogel scaffolds indicates highly porous structures, with open, spherical to elliptical shapes, interconnected pores. Pore size is in the range of 10–100 μm. This morphology pattern can provide efficient vascularization, proliferation, and differentiation of cells, which are prerequisites for tissue regeneration. The modulus of elasticity of AGHpor scaffolds is in the range of 0.988–4.056 MPa and depends on the scaffold composition. These values indicate the good potential of AGHpor hydrogel scaffolds for tissue regeneration, particularly for soft tissues. The porosity data of AGHpor scaffold samples is in the range of 28–70%. This feature can be tuned and adapted by modifications of scaffold composition and variations of components ratio. A50G50Hpor and A30G70Hpor hydrogel scaffolds were found to be fully hydrophilic. AHpor sample showed a slightly small wetting angle. The obtained results suggest that AGHpor hydrogels are favorable scaffolding biomaterials for cell adhesion, proliferation, and differentiation. The tested AGHpor hydrogel scaffolds degraded up to 3% after 3 months. The highest weight loss exhibited A30G70Hpor (3.07%), suggesting that the increase of gelatin content contributed to the biodegradability of the hydrogels. AHpor and A50G50Hpor degraded at a similar rate, with weight loss of around 1.60%.
As the most important achievements of these extensive researches, it can be stated that AGH hydrogel scaffolds created by cryogelation showed slightly more favorable properties for tissue regeneration compared to AGH hydrogel scaffolds created by porogenation. Another important fact is that more advantageous properties for tissue regeneration are achieved when the polymeric chains of alginate are intermingled into polymeric networks of gelatin and 2-hydroxyethyl methacrylate than into a polymeric network of 2-hydroxyethyl methacrylate. Thanks to the significant progress already made, along with others that will be made in the near future. The safe and effective clinical application of alginate/gelatin/methacrylate polymeric scaffolding systems is expected to accelerate and expand soon.
Hydrogel scaffolding materials have a significant role in regenerative medicine and tissue engineering. The future advances and success of hydrogel scaffolds are based on the new classes of polymers syntheses or the modification of natural polymers to solve certain biological and medical obstacles. Most scientific research shows that hydrogel scaffolding studies have a great future. New aspects to hydrogel scaffold design are increased in the investigation of these biomaterials, with an emphasis on rapid response, self-assembly, high and good mechanical properties, and super-porosity.
References
Aldana AA, Abraham GA (2017) Current advances in electrospun gelatin-based scaffolds for tissue engineering applications. Int J Pharm 523:441–453
Alves da Silva M, Martins A, Costa-Pinto AR, Monteiro N, Faria S, Reis RL, Neves NM (2017) Electrospun nanofibrous meshes cultured with Wharton’s jelly stem cell: an alternative for cartilage regeneration, without the need of growth factors. Biotechnol J. https://doi.org/10.1002/biot.201700073
Amado S, Morouço P, Pascoal-Faria P, Alves N (2017) Tailoring Bioengineered scaffolds for regenerative medicine. In: Dobrzański LA (ed) Biomaterials in regenerative medicine. IntechOpen, London. https://doi.org/10.5772/intechopen.69857. Available from: https://www.intechopen.com/chapters/56531
Annabi N, Nichol JW, Zhong X, Ji C et al (2010) Controlling the porosity and microarchitecture of hydrogels for tissue engineering. Tissue Eng Part B16:371–383
Atala A (2008) Advances in tissue and organ replacement. Curr Stem Cell Res Ther 3:21–31
Atala A (2012) Regenerative medicine strategies. J Pediatr Surg 47:17–28
Babić MM, Tomić SLj (2020) Semi-interpenetrating networks based on (Meth)acrylate, itaconic acid, and poly(vinyl Pyrrolidone) hydrogels for biomedical applications. In: Jana S, Jana S (eds) Interpenetrating polymer network: biomedical applications. Springer, Singapore, pp 263–288
Babitha S, Rachita L, Karthikeyan K, Shoba E, Janani I, Poornima B et al (2017) Electrospun protein nanofibers in healthcare: a review. Int J Pharm 523:52–90
Bailey AM, Mendicino M, Au P (2014) An FDA perspective on preclinical development of cell-based regenerative medicine products. Nat Biotechnol 32:721–723
Bajpai AK, Kankane S (2007) Preparation and characterization of macroporous poly(2-hydroxyethyl methacrylate)-based biomaterials: water sorption property and in vitro blood compatibility. J Appl Polym Sci 104:1559–1571
Baker BM, Trappmann B, Wang WY, Sakar MS, Kim IL, Shenoy VB, Burdick JA, Chen CS (2015) Cell-mediated fibre recruitment drives extracellular matrix mechanosensing in engineered fibrillar microenvironments. Nat Mater 14:1262–1268
Bakhsheshi-Rad HR, Hadisi Z, Hamzah E, Ismail AF, Aziz M, Kashefian M (2017) Drug delivery and cytocompatibility of ciprofloxacin loaded gelatin nanofibers-coated Mg alloy. Mater Lett 207:179–182
Barros TP, Alderton WK, Reynolds HM, Roach AG, Berghmans S (2008) Zebrafish: an emerging technology for in vivo pharmacological assessment to identify potential safety liabilities in early drug discovery. Br J Pharmacol 154:1400–1413
Behravesh E, Mikos AG (2003) Three-dimensional culture of differentiating marrow stromal osteoblasts in biomimetic poly(propylene fumarate-co-ethylene glycol)-based macroporous hydrogels. J Biomed Mater Res A 66:698–706
Bettinger CJ, Borenstein JT, Langer R (2007) Micro- and nanofabricated scaffolds. In: Lanza R, Langer R, Vacanti J (eds) Principles of tissue engineering, 3rd edn. Elsevier Academic Press, San Diego, CA, pp 341–358
Bigi A, Panzavolta S, Rovery N (1998) Hydroxyapatite-gelatin films: a structural and mechanical characterization. Biomaterials 19:739–744
Borselli C, Storrie H, Benesch-Lee F, Shvartsman D, Cezar C, Lichtman JW, Vandenburgh HH, Mooney DJ (2010) Functional muscle regeneration with combined delivery of angiogenesis and myogenesis factors. Proc Natl Acad Sci U S A 107:3287–3292
Boyan BD, Lohmann CH, Romero J, Schwartz Z (1999) Bone and cartilage tissue engineering. Clin Plast Surg 26:629–645
Brauker JH, Carr-Brendel VE, Martinson LA, Crudele J, Johnston WD, Johnson RC (1995) Neovascularization of synthetic membranes directed by membrane microarchitecture. J Biomed Mater Res 29:1517–1524
Bryant SJ, Anseth KS (2001) The effects of scaffold thickness on tissue engineered cartilage in photocrosslinked poly(ethylene oxide) hydrogels. Biomaterials 22:619–626
Bryant SJ, Davis-Arehart KA, Luo N, Shoemaker RK, Arthur JA, Anseth KS (2004) Synthesis and characterization of photopolymerized multifunctional hydrogels: water-soluble poly(vinyl alcohol) and chondroitin sulfate macromers for chondrocyte encapsulation. Macromolecules 37:6726–6733
Budama-Kilinc Y, Cakir-Koc R, Aslan B, Özkan B, Mutlu H, Üstün E (2017) Hydrogels in regenerative medicine. In: Dobrzański LA (ed) Biomaterials in regenerative medicine. IntechOpen. https://doi.org/10.5772/intechopen.70409
Cabodi M, Choi NW, Gleghorn JP, Lee CSD, Bonassar LJ, Stroock AD (2005) A microfluidic biomaterial. J Am Chem Soc 127:13788–13789
Camarero-Espinosa S, Cooper-White J (2016) Tailoring biomaterial scaffolds for osteochondral repair. Int J Pharm 523:476–489
Cascone MG, Barbani N, Cristallini C, Giusti P, Ciardelli G, Lazzeri L (2001) Bioartificial polymeric materials based on polysaccharides. Aust J Biol Sci 12:267–281
Chang H-I and Wang Y (2011) Cell responses to surface and architecture of tissue engineering scaffolds. In: Eberli D (ed) Regenerative medicine and tissue engineering-cells and biomaterials, BoD – books on demand. https://doi.org/10.5772/21983
Chen LJ, Wang M (2002) Production and evaluation of biodegradable composites based on PHB-PHV copolymer. Biomaterials 23:2631–2639
Cheung DYC, Duan B, Butcher JT (2015) Bioprinting of cardiac tissues. In: Atala A, Yoo JJ (eds) Essentials of 3D biofabrication and translation. Academic Press, Elsevier Science, London, pp 351–370
Cho SJ, Jung SM, Kang M, Shin HS, Youk JH (2015) Preparation of hydrophilic PCL nanofiber scaffolds via electrospinning of PCL/PVP-b-PCL block copolymers for enhanced cell biocompatibility. Polymer 69:95–102. https://doi.org/10.1016/j.polymer.2015.05.037
Choi K, Kuhn J, Ciarelli M, Goldstein S (1990) The elastic moduli of human subchondral, trabecular, and cortical bone tissue and the size-dependency of cortical bone modulus. J Biomech 23:1103–1113
Ciardelli G, Chiono V, Vozzi G, Pracella M, Ahluwalia A, Barbani N, Cristallini C, Giusti P (2005) Blends of poly(ε-caprolactone) and polysaccharides in tissue engineering applications. Biomacromolecules 6:1961–1976
Cosson S, Otte EA, Hezaveh H, Cooper-White JJ (2015) Concise review: tailoring bioengineered scaffolds for stem cell applications in tissue engineering and regenerative medicine. Stem Cells Transl Med 4:156–164
Das S, Subuddhi U (2020) Alginate-based interpenetrating network carriers for biomedical applications. In: Jana S, Jana S (eds) Interpenetrating polymer network: biomedical applications. Springer, Singapore, pp 79–118
Diamond DA, Caldamone AA (1999) Endoscopic treatment of vesicoureteric reflux in children using autologous chondrocytes-preliminary results. J Urol 162:1185–1188
Diedwardo CA, Petrosko P, Acarturk TO, Dimilia PA, Laframboise WA, Johnson PC (1999) Muscle tissue engineering. Clin Plast Surg 26:647–656
Dzobo K, Turnley T, Wishart A et al (2016) Fibroblast-derived extracellular matrix induces chondrogenic differentiation in human adipose-derived mesenchymal stromal/stem cells in vitro. Int J Mol Sci. https://doi.org/10.3390/ijms17081259
Eaglstein WH, Falanga V (1998) Tissue engineering and the development of Apligraf a human skin equivalent. AdvWound Care 11:1–8
Engler AJ, Sen S, Sweeney HL, Discher DE (2006) Matrix elasticity directs stem cell lineage specification. Cell 126:677–689
Evans ND, Gentleman E, Chen X, Roberts CJ, Polak JM, Stevens MM (2010) Extracellular matrix-mediated osteogenic differentiation of murine embryonic stem cells. Biomaterials 31:3244–3252
Eyrich D, Brandl F, Appel B et al (2007) Long-term stable fibrin gels for cartilage engineering. Biomaterials 28:55–65
Fang Z, Starly B, Sun W (2005) Computer-aided characterization for effective mechanical properties of porous tissue scaffolds. CAD Comput Aided Design 37:65–72
Fiedler T, Videira AC, Bártolo P, Strauch M, Murch GE, Ferreira JMF (2015) On the mechanical properties of PLC-bioactive glass scaffolds fabricated via BioExtrusion. Mater Sci Eng C 57:288–293
Gao G, Cui X (2016) Three-dimensional bioprinting in tissue engineering and regenerative medicine. Biotechnol Lett 38:203–211
Gao C, Tang F, Gong G, Zhang J, Hoi MPM, Lee SMY, Wang R (2017) pH-responsive prodrug nanoparticles based on a sodium alginate derivative for selective co-release of doxorubicin and curcumin into tumor cells. Nanoscale 9:12533–12542
Germain L, Auger FA, Grandbois E et al (1999) Reconstructed human cornea produced in vitro by tissue engineering. Pathobiology 67:140–147
Goncalves AI, Rodrigues MT, Gomes ME (2017) Tissue engineered magnetic cell sheet patches for advanced strategies in tendon regeneration. Acta Biomater 63:110–122
Guan X, Avci-Adali M, Alarcin E et al (2017) Development of hydrogels for regenerative engineering. Biotechnol J 12(5):1600394. https://doi.org/10.1002/biot.201600394
Gunatillake P, Mayadunne R, Adhikari R (2006) Recent developments in biodegradable synthetic polymers. Biotechnol Annu Rev 12:301–347
Guvendiren M, Burdick JA (2012) Stiffening hydrogels to probe short- and long-term cellular responses to dynamic mechanics. Nat Commun 3:792
Hashimoto T, Suzuki Y, Suzuki K, Nakashima T, Tanihara M, Ide C (2005) Peripheral nerve regeneration using non-tubular alginate gel crosslinked with covalent bonds. J Mater Sci Mater Med 16:503–509
Haycock JW (2011) 3D cell culture: a review of current approaches and techniques. Methods Mol Biol 695:1–15
Hejcl A, Urdzikova L, Sedy J, Lesny P, Pradny M, Michalek J, Burian M, Hajek M, Zamecnik J, Jendelova P, Sykova E (2008) Acute and delayed implantation of positively charged 2-hydroxyethyl methacrylate scaffolds in spinal cord injury in the rat. J Neurosurg Spine 8:67–73
Hench LL (1998) Bioceramics. J Am Ceram Soc 81:1705–1727
Hersel U, Dahmen C, Kessler H (2003) RGD modified polymers: biomaterials for stimulated cell adhesion and beyond. Biomaterials 24:4385–4415
Hill E, Boontheekul T, Mooney DJ (2006a) Designing scaffolds to enhance transplanted myoblast survival and migration. Tissue Eng 12:1295–1304
Hill E, Boontheekul T, Mooney DJ (2006b) Regulating activation of transplanted cells controls tissue regeneration. Proc Natl Acad Sci U S A 103:2494–2499
Hoffman AS (2001) Hydrogels for biomedical applications. Ann N Y Acad Sci 944:62–73
Huang Y, Onyeri S, Siewe M, Moshfeghian A, Madihally SV (2005) In vitro characterization of chitosan–gelatin scaffolds for tissue engineering. Biomaterials 26:7616–7627
Hubbell JA (1999) Bioactive biomaterials. Curr Opin Biotechnol 10:123–129
Huebsch N, Arany PR, Mao AS, Shvartsman D, Ali OA, Bencherif SA, Rivera-Feliciano J, Mooney DJ (2010) Harnessing traction-mediated manipulation of the cell/matrix interface to control stem-cell fate. Nat Mater 9:518–526
Hutmacher DW (2001) Scaffold design and fabrication technologies for engineering tissues-state of the art and future perspectives. J Biomat Sci Polym E 12:107–124
Jhon MS, Andrade JD (1973) Water and hydrogels. J Biomed Mater Res 7:509–522
Ji Y, Ghosh K, Shu XZ, Li B, Sokolov JC, Prestwich GD, Clark RAF, Rafailovich MH (2006) Electrospun three-dimensional hyaluronic acid nanofibrous scaffolds. Biomaterials 27:3782–3792
Joodaki H, Panzer MB (2018) Skin mechanical properties and modeling: a review. Proc Inst Mech Eng H. https://doi.org/10.1177/0954411918759801
Kariduraganavar MY (2016) Advances in polymers and tissue engineering scaffolds. In: Inamuddin (ed) Green polymer composites technology properties and applications. CRC Press, Boca Raton, FL, pp 343–354
Kataoka K, Suzuki Y, Kitada M, Hashimoto T, Chou H, Bai HL, Ohta M, Wu S, Suzuki K, Ide C (2004) Alginate enhances elongation of early regenerating axons in spinal cord of young rats. Tissue Eng 10:493–504
Ker EDF, Nain AS, Weiss LE, Wang J, Suhan J, Amon CH et al (2011) Bioprinting of growth factors onto aligned sub-micron fibrous scaffolds for simultaneous control of cell differentiation and alignment. Biomaterials 32:8097–8107
Kershen RT, Fefer SD, Atala A (2000) Tissue-engineered therapies for the treatment of urinary incontinence and vesicoureteral reflux. World J Urol 18:51–55
Khang G (2017) Biomaterials and manufacturing methods for scaffolds in regenerative medicine: update 2015. In: Khang G (ed) Handbook of intelligent scaffolds for tissue engineering and regenerative medicine. Taylor & Francis Group, Singapore, pp 1–53
Kim UJ, Park J, Li C, Jin HJ, Valluzzi R, Kaplan DL (2004) Structure and properties of silk hydrogels. Biomacromolecules 5:786–792
Kim H-W, Kim H-E, Salih V (2005) Stimulation of osteoblast responses to biomimetic nanocomposites of gelatin-hydroxyapatite for tissue engineering scaffolds. Biomaterials 26:5221–5230
Kim T-R, Kim M-S, Goh TS, Lee JS, Kim YH, Yoon S-Y, Lee C-S (2019) Evaluation of structural and mechanical properties of porous artificial bone scaffolds fabricated via advanced TBA-based freeze-gel casting technique. Appl Sci 9(9):1965. https://doi.org/10.3390/app9091965
Klawitter J, Hulbert S (1971) Application of porous ceramics for the attachment of load bearing internal orthopedic applications. J Biomed Mater Res 5:161–229
Knoepfler PS (2015) From bench to FDA to bedside: us regulatory trends for new stem cell therapies. Adv Drug Del Rev 82-83:192–196
Kong HJ, Smith MK, Mooney DJ (2003) Designing alginate hydrogels to maintain viability of immobilized cells. Biomaterials 24:4023–4029
Kotton DN, Morrisey EE (2014) Lung regeneration: mechanisms, applications and emerging stem cell populations. Nat Med 20:822–832
Kozlov PV, Burdygina GI (1983) The structure and properties of solid gelatin and the principles of their modification. Polymer 24:651–666
Kubinova S, Horak D, Hejcl A, Plichta Z, Kotek J, Proks V, Forostyak S, Sykova E (2015) SIKVAV-modified highly superporous PHEMA scaffolds with oriented pores for spinal cord injury repair. J Tissue Eng Regen Med 9:1298–1309
Kuo W-T, Huang H-Y, Chou M-J, Wu M-C, Huang Y-Y (2011) Surface modification of gelatin nanoparticles with polyethyleneimine as gene vector. J Nanomater 2011:1–5
Langer R, Vacanti J (1993) Tissue engineering. Science 260:920–926
Laurencin CT, Khan Y (2012) Regenerative engineering. Sci Transl Med 4:160ed9
Lee KY, Mooney DJ (2001) Hydrogels for tissue engineering. Chem Rev 101:1869–1879
Lee KY, Mooney DJ (2012) Alginate: properties and biomedical applications. Prog Polym Sci 37:106–126
Lee KY, Peters MC, Anderson KW, Mooney DJ (2000) Controlled growth factor release from synthetic extracellular matrices. Nature 408:998–1000
Levenberg S, Rouwkema J, Macdonald M, Garfein ES, Kohane DS, Darland DC, Marini R, van Blitterswijk CA, Mulligan RC, D’Amore PA, Langer R (2005) Engineering vascularized skeletal muscle tissue. Nat Biotechnol 23:879–884
Lien SM, Ko LY, Huang TJ (2009) Effect of pore size on ECM secretion and cell growth in gelatin scaffold for articular cartilage tissue engineering. Acta Biomater 5:670–679
Lieschke GJ, Currie PD (2007) Animal models of human disease: zebrafish swim into view. Nat Rev Genet 8:353–367
Lim K, Morouço P, Levato R, Melchels F, Malda J (2017) Organ biofabrication. Comprehen Biomater II 5:236–266
Lim Y-S, Ok Y-J, Hwang S-Y, Kwak J-Y, Yoon S (2019) Marine collagen as a promising biomaterial for biomedical applications. Mar Drugs 17:467
Lin LJ, Chiang CJ, Chao YP, Wang SD, Chiou YT, Wang HY et al (2016) Development of alginate microspheres containing chuanxiong for oral administration to adult zebrafish. BioMed Res Int. https://doi.org/10.1155/2016/4013071
López-Ruiz E, Jiménez G, García MÁ, Antich C, Boulaiz H, Marchal JA, Peran M (2016) Polymers, scaffolds and bioactive molecules with therapeutic properties in osteochondral pathologies: what’s new? Expert Opin Ther Pat 26:877–890
Ma PX (2004) Scaffolds for tissue fabrication. Mater Today 7:30–40
MacRae CA, Peterson RT (2015) Zebrafish as tools for drug discovery. Nat Rev Drug Discov 14:721–731
Mason C, Dunnill P (2008) A brief definition of regenerative medicine. Regen Med 3:1–5
Mayer JE, Shin’oka T, Shum-Tim D (1997) Tissue engineering of cardiovascular structures. Curr Opin Cardiol 12:528–532
Mayer J, Karamuk E, Akaike T, Wintermantel E (2000) Matrices for tissue engineering-scaffold structure for a bioartificial liver support system. J Control Release 64:81–90
Mendelson A, Frenette PS (2014) Hematopoietic stem cell niche maintenance during homeostasis and regeneration. Nat Med 20:833–846
Mohammad J, Shenaq J, Rabinovsky E, Shenaq S (2000) Modulation of peripheral nerve regeneration: a tissue engineering approach. The role of amnion tube nerve conduit across a 1-centimeter nerve gap. Plast Reconstr Surg 105:660–666
Mohammadzadehmoghadam S, Dong Y (2019) Fabrication and characterization of electrospun silk fibroin/gelatin scaffolds crosslinked with glutaraldehyde vapor. Front Mater 6:91. https://doi.org/10.3389/fmats.2019.00091
Nagarajan S, Pochat-Bohatier C, Teyssier C, Balme S, Miele P, Kalkura N, Cavaillès V, Bechelany M (2016a) Design of graphene oxide/gelatin electrospun nanocomposite fibers for tissue engineering applications. RSC Adv 6:109150–109156
Nagarajan S, Soussan L, Bechelany M, Teyssier C, Cavaillès V, Pochat-Bohatier C, Miele P, Kalkura N, Janot JM, Balme S (2016b) Novel biocompatible electrospun gelatin fiber mats with antibiotic drug delivery properties. J Mater Chem B 4:1134–1141
Nagarajan S, Belaid H, Pochat-Bohatier C, Teyssier C, Iatsunskyi I, Coy E, Balme S, Cornu D, Miele P, Kalkura NS, Cavailles V, Bechelany M (2017) Design of boron nitride/gelatin electrospun nanofibers for bone tissue engineering. ACS Appl Mater Interfaces 9:33695–33706
Nair LS, Laurencin CT (2007) Biodegradable polymers as biomaterials. Prog Polym Sci 32:762–798
Nair P, Thottappillil N (2015) Scaffolds in vascular regeneration: current status. Vasc Health Risk Manag 11:79–91
Oberpenning F, Meng J, Yoo JJ, Atala A (1999) De novo reconstitution of a functional mammalian urinary bladder by tissue engineering. Nat Biotechnol 17:149–155
OECD, OECD Guidelines for the Testing of Chemicals (2013) Test No 236
Onal U, Langdon C (2000) Characterization of two microparticle types for delivery of food to altricial fish larvae. Aquac Nutr 6:159–170
Panzavolta S, Gioffrè M, Focarete ML, Gualandi C, Foroni L, Bigi A (2011) Electrospun gelatin nanofibers: optimization of genipin cross-linking to preserve fiber morphology after exposure to water. Acta Biomater 7:1702–1709
Parker GJM, Wheeler-Kingshott CAM, Barker GJ (2002) Diffusion tensor imaging. IEEE T Med Imaging 21:505–512
Paszek MJ, Zahir N, Johnson KR, Lakins JN, Rozenberg GI, Gefen A, Reinhart-King CA, Margulies SS, Dembo M, Boettiger D, Hammer DA, WeaverVM (2005) Tensional homeostasis and the malignant phenotype. Cancer Cell 8:241–254
Peppas NA, Khare AR (1993) Preparation, structure and diffusional behavior of hydrogels in controlled release. Adv Drug Deliv Rev 11:1–35
Phelps EA, Enemchukwu NO, Fiore VF, Sy JC, Murty N, Sulchek TA, Barker TH, Garcia AJ (2012) Maleimide cross-linked bioactive peg hydrogel exhibits improved reaction kinetics and cross-linking for cell encapsulation and in situ delivery. Adv Mater 24:64–70
Pina S, Canadas RF, Jimenez G, Peran M, Marchal JA, Reis RL, Oliveira JM (2017) Biofunctional ionic-doped calcium phosphates: silk fibroin composites for bone tissue engineering scaffolding. Cells Tissues Organs 204:150–163
Piskin E (1994) Biodegradable polymers as biomaterials. J Biomat Sci Polym E 6:775–795
Poursamar SA, Lehner AN, Azami M, Ebrahimi-Barough S, Samadikuchaksaraei A, Antunes APM (2016) The effects of crosslinkers on physical, mechanical, and cytotoxic properties of gelatin sponge prepared via in-situ gas foaming method as a tissue engineering scaffold. Mater Sci Eng C 63:1–9
Prang P, Muller R, Eljaouhari A, Heckmann K, Kunz W, Weber T, Faber C, Vroemen M, Bogdahn U, Weidner N (2006) The promotion of oriented axonal regrowth in the injured spinal cord by alginate-based anisotropic capillary hydrogels. Biomaterials 27:3560–3569
Prasitsilp M, Siriwittayakorn T, Molloy R, Suebsanit N, Siriwittayakorn P, Veeranondha S (2003) Cytotoxicity study of homopolymers and copolymers of 2-hydroxyethyl methacrylate and some alkyl acrylates for potential use as temporary skin substitutes. J Mater Sci Mater Med 14:595–600
Ramakrishna S, Mayer J, Wintermantel E, Leong KW (2001) Biomedical applications of polymer-composite materials: a review. Compos Sci Technol 61:1189–1224
Rezwan K, Chen QZ, Blaker JJ, Boccaccini AR (2006) Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 27:3413–3431
Roether JA, Boccaccini AR, Hench LL, Maquet V, Gautier S, Jerome R (2002) Development and in vitro characterization of novel bioresorbable and bioactive composite materials based on polylactide foams and bioglass® for tissue engineering applications. Biomaterials 23:3871–3878
Roseti L, Parisi V, Petretta M, Cavallo C, Desando G, Bartolotti I, Grigolo B (2017) Scaffolds for bone tissue engineering: state of the art and new perspectives. Mat Sci Eng C Bio S 78:1246–1262
Sadeghi M, Heidari B (2011) Crosslinked graft copolymer of methacrylic acid and gelatin as a novel hydrogel with pHresponsiveness properties. Materials 4:543–552
Sadtler K, Singh A, Wolf MT, Wang T, Pardoll DM, Elisseeff JH (2016) Design, clinical translation and immunological response of biomaterials in regenerative medicine. Nat Rev Mater 1:16040
Sajkiewicz P, Kołbuk D (2014) Electrospinning of gelatin for tissue engineering-molecular conformation as one of the overlooked problems. J Biomater Sci Polym Ed 25:2009–2022
Saxena AK, Marler J, Benvenuto M, Willital GH, Vacanti JP (1999) Skeletal muscle tissue engineering using isolated myoblasts on synthetic biodegradable polymers: preliminary studies. Tissue Eng 5:525–532
Schmedlen RH, Masters KS, West JL (2002) Photocrosslinkable polyvinyl alcohol hydrogels that can be modified with cell adhesion peptides for use in tissue engineering. Biomaterials 23:4325–4332
Sculean A, Auschill TM, Donos N, Brecx M, Arweiler NB (2001) Effect of an enamel matrix protein (Emdogain®) on ex vivo dental plaque vitality. J Clin Periodontol 28:1074–1078
Seol YJ, Park DY, Park JY, Kim SW, Park SJ, Cho DW (2013) A new method of fabricating robust freeform 3D ceramic scaffolds for bone tissue regeneration. Biotechnol Bioeng 110:1444–1455
Sharma C, Dinda AK, Potdar PD, Chou CF, Mishra NC (2016) Fabrication and characterization of novel nano-biocomposite scaffold of chitosan-gelatin-alginate-hydroxyapatite for bone tissue engineering. Mater Sci Eng 64:416–427
Slaughter BV, Khurshid SS, Fisher OZ, Khademhosseini A, Peppas NA (2009) Hydrogels in regenerative medicine. Adv Mater 21:3307–3329
Smeds KA, Grinstaff MW (2001) Photocrosslinkable polysaccharides for in situ hydrogel formation. J Biomed Mater Res 54:115–121
Solchaga LA, Gao J, Dennis JE et al (2002) Treatment of osteochondral defects with autologous bone marrow in a hyaluronan-based delivery vehicle. Tissue Eng 8:333–347
Soon-Shiong P, Heintz RE (1994) Insulin independence in a type 1 diabetic patient after encapsulated islet transplantation. Lancet 343:950–951
Suh JKF, Matthew HWT (2000) Application of chitosan-based polysaccharide biomaterials in cartilage tissue engineering: a review. Biomaterials 21:2589–2598
Sun W, Darling A, Starly B, Nam J (2004) Computer-aided tissue engineering: overview, scope and challenges. Appl Biochem Biotechnol 39:29–47
Sung H-J, Meredith C, Johnso C, Galis ZS (2004) The effect of scaffold degradation rate on three-dimensional cell growth and angiogenesis. Biomaterials 25:5735–5742
Suzuki K, Suzuki Y, Tanihara M, Ohnishi K, Hashimoto T, Endo K, Nishimura Y (2000) Reconstruction of rat peripheral nerve gap without sutures using freeze-dried alginate gel. J Biomed Mater Res 49:528–533
Tabata Y (2003) Tissue regeneration based on growth factor release. Tissue Eng 9:5–15
Taddei P, Chiono V, Anghileri A, Vozzi G, Freddi G, Ciardelli G (2013) Silk fibroin/gelatin blend films crosslinked with enzymes for biomedical applications. Macromol Biosci 13:1492–1510
Tang XL, Li Q, Rokosh G, Sanganalmath SH, Chen N, Ou Q, Stowers H, Hunt G, Bolli R (2016) Long-term outcome of administration of c-kitPOS cardiac progenitor cells after acute myocardial infarction: transplanted cells do not become cardiomyocytes, but structural and functional improvement and proliferation of endogenous cells persist for at least one year. Circ Res 118:1091–1105
Thomas LV, Nair PD (2012) Influence of mechanical stimulation in the development of a medial equivalent tissue-engineered vascular construct using a gelatin-g-vinyl acetate co-polymer scaffold. J Biomater Sci Polym Ed 23:2069–2087
Tomić SLj, Vuković JS (2020) Antimicrobial properties of (meth)acrylate-based hydrogels. In: Paquette N (ed) An introduction to antibacterial properties. Nova Science Publishers, New York. https://novapublishers.com/shop/an-introduction-to-antibacterialproperties/
Tomić SLj, Babić MM, Djokić L, Pavić A, Nikodinović-Runić J (2020) Effect of composition and method of preparation of 2-hydroxyethyl methacrylate/gelatin hydrogels on biological in vitro (cell line) and in vivo (zebrafish) properties. J Polym Res 27(10):1–8. https://doi.org/10.1007/s10965-020-02219-w
Tran TT, Hamid ZA, Cheong KY (2018) A review of mechanical properties of scaffold in tissue engineering: Aloe vera composites. J Phys Conf Ser 1082:012080
Tzankova V, Aluani D, Kondeva-Burdina M, Yordanov Y, Odzhakov F, Apostolov A, Yoncheva K (2017) Hepatoprotective and antioxidant activity of quercetin- loaded chitosan/alginate particles in vitro and in vivo in a model of paracetamol-induced toxicity. Biomed Pharmacother 92:569–579
Tziampazis E, Sambanis A (1995) Tissue engineering of a bioartificial pancreas: modeling the cell environment and device function. Biotechnol Prog 11:115–126
Vacanti JP, Langer R (1999) Tissue engineering: the design and fabrication of living replacement devices for surgical reconstruction and transplantation. Lancet 354:S32–S34
Wade RJ, Bassin EJ, Gramlich WM, Burdick JA (2015) Nanofibrous hydrogels with spatially patterned biochemical signals to control cell behavior. Adv Mater 27:1356–1362
Wallace DG, Rosenblatt J (2003) Collagen gel systems for sustained delivery and tissue engineering. Adv Drug Deliv Rev 55:1631–1649
Wang K, Nune KC, Misra RDK (2016) The functional response of alginate-gelatin- nanocrystalline cellulose injectable hydrogels toward delivery of cells and bioactive molecules. Acta Biomater 36:143–151
Wongputtaraksa T, Ratanavaraporn J, Pichyangkura R, Damrongsakkul S (2012) Surface modification of Thai silk fibroin scaffolds with gelatin and chitooligosaccharide for enhanced osteogenic differentiation of bone marrow-derived mesenchymal stem cells. J Biomed Mater Res Part B Appl Biomater 100:2307–2315
Yang C, DelRio FW, Ma H, Killaars AR, Basta LP, Kyburz KA, Anseth KS (2016) Spatially patterned matrix elasticity directs stem cell fate. Proc Natl Acad Sci U S A 113:E4439–E4445
Yannas IV (2004) Classes of materials used in medicine: natural materials. In: Ratner BD, Hoffman AS, Schoen FJ, Lemons J (eds) Biomaterials science-an introduction to materialsin medicine. Elsevier Academic Press, San Diego, CA, pp 127–136
Yannas I, Lee E, Orgill D, Skrabut E, Murphy G (1989) Synthesis and characterization of a model extracellular matrix that induces partial regeneration of adult mammalian skin. Proc Natl Acad Sci U S A 86:933–937
Zadpoor AA (2015) Bone tissue regeneration: the role of scaffold geometry. Biomater Sci UK 3:231–245
Żak M, Kuropka P, Kobielarz M, Dudek A, Kaleta-Kuratewicz K, Szotek S (2011) Determination of the mechanical properties of the skin of pig foetuses with respect to its structure. Acta Bioeng Biomech 13:37–43
Zhang YZ, Venugopal J, Huang ZM, Lim CT, Ramakrishna S (2006) Crosslinking of the electrospun gelatin nanofibers. Polymer 47:2911–2917
Zhang H, Zhou L, Zhang W (2014) Control of scaffold degradation in tissue engineering: a review. Tissue Eng Part B Rev 20(5):492–502. https://doi.org/10.1089/ten.TEB.2013.0452
Zhao XH, Kim J, Cezar CA, Huebsch N, Lee K, Bouhadir K, Mooney DJ (2011) Active scaffolds for on-demand drug and cell delivery. Proc Natl Acad Sci U S A 108:67–72
Acknowledgments
This research is supported by the SCOPES program of the Swiss National Science Foundation and the Swiss Agency for Development and Cooperation [Grant No IZ73ZO_152327]. This work is supported by the Ministry for Education, Science, and Technological Development of the Republic of Serbia (Contracts Nos. 451-03-9/2021-14/172062 and 451-03-9/2021-14/172026).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Tomić, S.L., Vukomanović, M., Nikodinović-Runić, J., Babić, M.M., Vuković, J.S. (2022). Hydrogel Scaffolds Based on Alginate, Gelatin, and 2-Hydroxyethyl Methacrylate for Tissue Regeneration. In: Jana, S., Jana, S. (eds) Marine Biomaterials. Springer, Singapore. https://doi.org/10.1007/978-981-16-5374-2_6
Download citation
DOI: https://doi.org/10.1007/978-981-16-5374-2_6
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-16-5373-5
Online ISBN: 978-981-16-5374-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)