Abstract
Ataxia-telangiectasia (A-T) and Nijmegen breakage syndrome (NBS) are well-known single-gene disorders, which have similar cellular phenotypes, including chromosome instability, radioresistant DNA synthesis, and hypersensitivity to radiation. Such phenotypic similarity implies direct physical association and/or functional interaction between respective gene products. Indeed, the NBS1 protein responsible for NBS interacts with ATM kinase implicated in A-T and regulates ATM activation upon DNA damage; however, NBS1-mediated homologous recombination does not seem to require ATM. Moreover, ATM is activated by oxidative stress independently of NBS1. Thus, ATM and NBS1 are likely to have distinct functions in radiation-induced DNA damage responses or other cellular responses to genomic stresses such as oxidative stress, which should underlie different clinical manifestations of A-T and NBS.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
13.1 Clinical Features of A-T, NBS, and ATLD
Ataxia-telangiectasia (A-T; OMIM#208900; Table 13.1) is a rare neurodegenerative disease with worldwide incidence of 1 in 40,000–200,000 live births characterized by poor coordination, hypersensitivity to radiation, and chromosomal instability, which enhances the risk of cancer. A-T was first described in 1958 [1]; later, Gotoff et al. reported that A-T patients showed hypersensitivity to radiotherapy [2]. Typical clinical manifestations of this disorder include severe neurodegeneration due to progressive cerebellar atrophy and telangiectasia (small dilated blood vessels), especially in the eyes and occasionally on the facial skin. In addition, patients have general immunodeficiency, predisposition to malignancies (particularly lymphoma), and hypersensitivity to ionizing radiation (IR); some of them also show growth retardation, premature aging, and insulin resistance [3,4,5]. The cellular phenotype in A-T is characterized by chromosomal instability, radioresistant DNA synthesis (RDS), and hypersensitivity to DNA-damaging agents, especially those inducing double-strand breaks (DSBs) [3,4,5]; it has also been reported in other genetic conditions such as A-T variants and A-T-like disorder.
The most famous A-T variant is a rare autosomal recessive Nijmegen breakage syndrome (NBS; OMIN#251260; Table 13.1). NBS was first described in 1979 in a Dutch boy with microcephaly, growth retardation, IgA deficiency, and chromosomal rearrangements, which are also observed in A-T [6]. The boy’s brother had similar clinical manifestations; therefore Weemaes et al. reported the condition as a genetic disease and named it Nijmegen breakage syndrome [7]. Typical clinical features of NBS are developmental microcephaly, which results in birdlike face, mild growth retardation, premature ovarian failure, immunodeficiency, and predisposition to cancer, most frequently in hematological organs [8, 9]. NBS is very similar to A-T in the cellular phenotype, namely, hypersensitivity to radiation, RDS, and genomic instability caused by chromosomal aberrations. The estimated worldwide incidence of NBS is 1 in 100,000 live births; however, NBS is more common in Eastern Europe, where its frequency can be as high as about 1:150 in some populations, because the origin of the founder mutation is in Poland.
A-T-like disorder (ATLD; OMIM#604391; Table 13.1) has been reported as an A-T-related disease [10, 11]. ATLD patients were first described by Hernandez et al. in 1993 [12]. A common feature of ATLD and A-T is progressive cerebellar ataxia; however, ATLD patients show normal levels of total IgG, IgA, and IgM and do not have telangiectasia. Although immunodeficiency and cancer predisposition typical for A-T and NBS are uncommon in ATLD, cellular phenotypes are similar. Therefore, interactions between the factors responsible for DNA damage responses in A-T and related syndromes have been expected before the discovery of the encoding genes.
13.2 Interaction Between ATM and NBS1 in DSB Damage Responses
Several critical studies have identified mutations responsible for A-T in the ATM gene located at 11q22-23 [13, 14]. ATM is a 350-kDa protein of 3056 amino acids belonging to the family of phosphatidylinositol 3-kinase-like protein kinases [15]. This family also includes the catalytic subunit of the DNA-dependent protein kinase (DNA-PKcs) involved in the nonhomologous end-joining (NHEJ) pathway of DSB repair [16] and the A-T and Rad3-related (ATR) protein, which responds primarily to stalled replication forks (replication stress) [17]. These protein kinases preferably phosphorylate serine or threonine residues followed by glutamine (S/TQ motif) and have redundant functions. The ATM gene is widely conserved in eukaryotes and has an ortholog (TEL1/tel1) in yeast [18]. ATR is also conserved in yeast (MEC1 and rad3 genes in budding and fission yeast, respectively), but DNA-PKcs is not [18].
The gene mutated in NBS is NBS1, which has been mapped to chromosome 8q21–24; it contains 16 exons [19, 20] and is widely conserved in eukaryotes. Human NBS1 gene encodes 754-amino acid (aa) protein with weak homology to Xrs2 in budding yeast and stronger homology to yNbs1 in fission yeast. NBS1 has a forkhead-associated domain (aa 20–108) and two BRCA1 C-terminus (BRCT) domains (BRCT1, aa 111–197, and BRCT2, aa 219–327) at the C-terminal region (Fig. 13.1).
Structure of human NBS1 protein. NBS1 contains several interaction motifs in the N- and C-termini. The N-terminal FHA/BRCT domains interact with DNA damage-responding proteins such as MDC1, γ-H2AX, and TopBP1. The C-terminal motifs are indispensable for binding to MRE11, ATM, RAD18, RNF20, and RPA32. These interactions might be important for the maintenance of genomic stability
ATLD is caused by mutations in the MRE11 gene [10, 11], containing 20 exons and mapped to chromosome 11q21. The encoded 80-kDa MRE11 protein of 708 aa has a motif critical for nuclease activity (3′ to 5′ exo- and endonuclease) at the N-terminus and DNA-binding motifs at both central and C-terminal regions and is widely conserved in eukaryotes. It was shown that in budding yeast, yMre11 interacted with NBS1 ortholog Xrs2 [21]. In humans, MRE11 binds to NBS1 at the C-terminus (aa 682–693; Fig. 13.1) and to RAD50, forming the MRN complex [22]. Some patients with NBS-like disorder (NBSLD: OMIM#613078) have defective RAD50 and demonstrate cellular phenotypes characteristic for NBS, A-T, and ATLD, including radiation hypersensitivity, RDS, and chromosome instability [23]. The MRN complex functions in homologous recombination (HR) repair, which is, similar to NHEJ, a major DSB repair pathway. When DSBs are generated by IR, the MRN complex is rapidly recruited to DSB sites, and HR repair is initiated via resection of DSB ends, resulting in the formation of more than 30 single-stranded DNA (ssDNA) tails at both DSB ends. Then, the replication protein A (RPA) complex binds to ssDNA and is subsequently replaced with RAD51, which facilitates HR repair [24]. The MRN complex, particularly MRE11, is indispensable for the initial resection step in HR as evidenced by the findings in NBS1- or MRE11-deficient DT40 chicken and human cells [25, 26].
An intrinsic feature of A-T is RDS, which is a defect in the activation of the intra-S phase checkpoint. A-T cells are also known for failure to activate G1 and G2 checkpoints [27, 28]. A major pathway regulating the G1 checkpoint is the suppression of CDK/cyclin activity by cell cycle inhibitory protein p21, whose expression is induced by p53 activated after IR-induced DSB damage. ATM was found to participate in this pathway by phosphorylating p53 and promoting p21 transcription [29, 30]. ATM can also phosphorylate a number of other regulators of cell cycle checkpoints in response to DSB formation (Fig. 13.2). Most of ATM substrates have consensus sequences containing SQ/TQ motifs [31] that are found in the central region of NBS1. The serine residues at positions 278 and 343 are phosphorylated by ATM in response to IR, and the substitution of these residues with alanine results in the abrogation of the ATM-dependent intra-S checkpoint in response to DSB damage, which is similar to the cellular phenotype observed in NBS patients [32, 33]. Furthermore, ATM can perform autophosphorylation at serine 1981, which is essential for ATM monomerization and its sufficient activation (Fig. 13.2) [34]. Moreover, ATM is evidently activated by a direct association with NBS1 via a conserved motif (aa 734–754; Fig. 13.1) located at the NBS1 C-terminus (Fig. 13.2) [35]. NBS cells are deficient in the recruitment of ATM to DSB sites after IR and showed reduced activity of ATM kinase, indicating that the interaction between NBS1 and ATM is indispensable for sufficient ATM activation [35]. MRE11-defective ATLD cells and RAD50-defective NBSLD cells also show the reduction of ATM-dependent phosphorylation and activation of cell cycle checkpoint, suggesting that both MRE11 and RAD50 are also important for ATM activation via the MRN complex.
Mechanisms of ATM activation. (a) DSB damage induces autophosphorylation of ATM at serine 1981, which allows the interaction of ATM monomer with MRN complex and subsequent recruitment to DSB sites. As a result, ATM could sufficiently phosphorylate checkpoint regulators. (b) Oxidative stress induces ATM dimerization through disulfide bonds and subsequent activation. Such activated ATM could phosphorylate anti-ROS regulatory proteins
13.3 Distinct Functions of ATM and NBS1 and Their Relevance to Clinical Phenotypes
Although cellular phenotypes are similar in A-T and NBS, their clinical manifestations, especially neurodegeneration, are different. Thus, A-T patients show progressive cerebellar ataxia, while NBS patients have microcephaly. In A-T patients, progressive cerebellar ataxia mostly leads to gait imbalance at the end of the first decade [36, 37], accompanied with oculomotor abnormalities, swallowing difficulty, and speech defects. Pathology studies indicate that a loss of Purkinje and granular neurons may cause progressive cerebellar cortical degeneration in A-T [38, 39]. Although Atm-deficient mice do not display the typical ataxia phenotype [39], neural stem cells derived from induced pluripotent cells of A-T patients had abnormal responses to hypoxia and attenuated neuronal differentiation, especially to GABAergic neurons and oligodendrogenesis [40]. Moreover, ATM-deficient human and mouse cells showed increased generation of endogenous reactive oxygen species (ROS) and accumulation of oxidative damage, suggesting that ATM could have an important role in antioxidative responses [41, 42]. Guo et al. reported that ROS directly induced ATM kinase activation independently of MRN complex through stabilization of ATM dimers by the formation of disulfide bonds (Fig. 13.2) [43]. Moreover, several recent studies have described ATM roles in cytoplasmic organelles such as peroxisomes and mitochondria [44,45,46]. Thus, Walker et al. showed that ROS activated peroxisomal ATM, which phosphorylated serine-threonine kinase LKB1 and induced 5′-AMP-activated protein kinase (AMPK) and tuberin (TSC2), dampening mTORC1-mediated signaling. This cascade of events led to a decrease in protein synthesis and enhancement of autophagy (pexophagy) via ATM-dependent phosphorylation of PEX5, which interacts with p62 (an autophagy adaptor) [44, 45]. ATM was also found in mitochondria, where it was suggested to play a role in mitochondrial autophagy (mitophagy) and stabilization of mitochondrial DNA [46,47,48]; however, ATM substrates in mitochondria and mechanistic aspects of its activity there remain to be investigated. Overall, these data indicate that deregulation of ATM activation in anti-oxidative stress signaling may lead to distinct neuronal phenotypes such as cerebellar ataxia in A-T. ATLD patients show similar progressive cerebellar ataxia, while ATM activation by oxidative stress is suggested to be independent of MRE11; another common role of ATM and MRE11 may be related to the neurodegenerative phenotype.
Immunodeficiency is also a typical feature in A-T. The patients have decreased levels of IgA, IgE, and IgG and are defective in B- and T-cell differentiation [49, 50]. Lymphocytes from A-T patients often contain clonal translocations, mainly in chromosome 7 and 14 loci of the T-cell receptor and Ig heavy chain genes [51, 52]. V(D)J recombination occurs only at the G0 and G1 phases of the cell cycle because of the G1-/G0-specific expression of V(D)J recombination-specific nuclease RAG2; therefore, abnormal regulation of cell cycle checkpoints in A-T may induce incomplete V(D)J recombination and consequently lead to immunodeficiency [53]. Another prominent clinical hallmark of A-T is predisposition to cancer, especially to that of hematopoietic origin, including Hodgkin’s and non-Hodgkin’s lymphoma, and several forms of leukemia [54, 55], which can be triggered by incomplete differentiation of immune organ. Furthermore, accumulating evidence suggests that ATM-mediated cell cycle checkpoint regulation is important for the prevention of cancer progression [56]; consequently, ATM-inactivating mutations may promote cancer development.
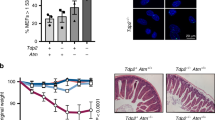
A-T is often accompanied by the deficiency in glucose metabolism and insulin-related responses; the patients often show poor weight gain, progressive decrease in body mass index (BMI), and dystrophy [57]. In fact, ATM was found to participate in several signaling pathways regulated by insulin [58, 59], and ApoE-deficient mice heterozygous for the Atm null allele had glucose intolerance and insulin resistance similar to those in type 2 diabetes [60]. Furthermore, Atm−/− mice showed reduction of insulin secretion and impaired differentiation of fibroblasts to adipocytes due to insufficient induction of C/EBPα and PPARγ [61, 62]. These findings suggest an important role of ATM in glucose metabolism mediated via adipocyte differentiation; however, the signals triggering ATM kinase activation in metabolic regulation remain unclear.
13.4 Novel Role of NBS1 and Its Contribution to NBS-Specific Symptoms
As mentioned above, NBS1 forms the MRN complex with MRE11 and RAD50 functioning in HR repair. The C-terminus of NBS1 contains motifs responsible for the binding to MRE11 and ATM, which are conserved among eukaryotes. Another conserved C-terminal sequence was found to be critical for the binding to E3 ubiquitin ligase RNF20 (aa 704–708; Fig. 13.1) [63], which ubiquitinates histone H2B at lysine 119 and is important for transcriptional regulation. RNF20 accumulates at DSB damage sites, and RNF20-dependent ubiquitination of H2B induced by IR is required for the recruitment of BRCA1 and RAD51 to DSB damage sites and HR repair. Furthermore, the interaction between NBS1 and RNF20 is essential for IR-induced focus formation of RPA complex (their accumulation to damaged chromatin) following DSB end resection, suggesting that NBS1 association with RNF20 is involved in the regulation of HR repair through end resection. Thus, while the NBS1 function in HR repair through assembly with MRE11 and RNF20 has been established, the role of its binding partner ATM in HR is unclear. There is evidence to suggest that ATM might be dispensable for HR repair, while some findings indicate the opposite [64,65,66]; therefore, further investigation is required.
In NBS, the characteristic clinical feature is microcephaly, which is not observed in A-T and ATLD patients, suggesting that physiological functions of NBS1 are distinct from those of ATM and MRE11. Microcephaly is also common for Seckel syndrome patients deficient in ATR, which is a member of the ATM kinase family and regulates cell cycle checkpoint response to replication stress. ATR is recruited to DNA damage sites induced by replication stress through the binding with ATRIP, which interacts with the RPA complex recognizing and coating ssDNA ends generated on stalled forks [67]. In parallel, TopBP1 binds to the RAD9-RAD1-HUS1 (9-1-1) checkpoint clamp, which is loaded onto DNA by the RAD17-replication factor C clamp loader complex [17]. These events result in the catalytic activation of ATR through direct binding of the ATR-ATRIP complex to the activation domain of TopBP1. Shiotani et al. reported that NBS1 could activate ATR through binding with RPA32, one of the three RPA subunits (aa 549–561; Fig. 13.1) [68]. NBS1, via its N-terminus, is likely to interact with TopBP1 and facilitate TopBP1 recruitment to DNA damage sites [69]. Overall, these data indicate that NBS1 has a critical role in ATR activation and that both ATR and NBS1 are important for cell cycle checkpoint induction by replication stress. In addition, accumulating evidence suggests that ATR and NBS1 are involved in centrosome maintenance. Centrosome is an organelle with a key role in equal chromosome segregation to daughter cells, which prevents aneuploidy. The MCPH1 gene responsible for autosomal recessive primary microcephaly disorder has a role in centrosome maintenance, and its defects induce abnormal centrosome amplification [70]. MCPH1 is also involved in ATR-dependent DNA damage responses [71], suggesting a role of ATR in the centrosome cycle. Cumulatively, these data implicate NBS1, ATR, and MCPH1 in normal brain development and prevention of microcephaly [70, 72].
Yanagihara et al. reported that another conserved region (aa 639–669; Fig. 13.1) at the NBS1 C-terminus contributes to its binding with RAD18, an E3-ubiqutin ligase for proliferating cell nuclear antigen (PCNA) [73]. PCNA ubiquitination is implicated in DNA polymerase η (Polη)-dependent DNA translesion synthesis (TLS) after UV-induced DNA damage, which is regulated by RAD18. Depletion of NBS1 by siRNA increased UV sensitivity and reduced RAD18-dependent PCNA ubiquitination and subsequent accumulation of Polη at UV-induced DNA damage sites. These data suggest the involvement of NBS1 in RAD18/Polη-dependent TLS, while MRE11 and ATM are known to be dispensable for the TLS pathway. However, cells derived from most NBS patients are not sensitive to UV, because a major NBS1 mutation does not affect its RAD18-binding site and thus, does not prevent the activation of the RAD18/Polη-dependent TLS pathway.
NBS as well as A-T patients have predisposition to cancer, particularly to T-cell and B-cell lymphomas, which is likely due to genomic instability as evidenced by translocation between chromosomes 7 and 14 observed in T lymphocytes [9, 51]. As NBS1 is essential to ATM activation in response to DSB damage, it could also be involved in immune development through the ATM-dependent cell cycle checkpoint. Therefore, NBS1 defects can also lead to incomplete differentiation in immune organs and consequent lymphoid malignancy. Considering NBS1 role in the RAD18/Polη-dependent TLS pathway, deficiency of NBS1 may compromise TLS activation and lead to nucleotide misincorporation during regular DNA synthesis, causing genetic defects. Thus, NBS patients may suffer increased predisposition to malignancy due to deregulation of the RAD18/Polη-dependent TLS pathway.
13.5 Conclusion
ATM, NBS1, and MRE11 exert significant effects on IR-induced DNA damage responses through direct physical associations with and functional activation of each other. Therefore, mutations in the encoding genes underlie radiation hypersensitive genetic disorders such as A-T, ATLD, and NBS, which share common features of chromosomal instability and radioresistant DNA synthesis. However, clinical phenotypes of A-T, ATLD, and NBS are different, especially concerning neurodegeneration. While A-T and ATLD are characterized with progressive cerebellar ataxia, NBS has a typical microcephaly phenotype, suggesting distinct functional roles of the involved genes. Thus, ATM could be activated by oxidative stress as well as DSB damage, while NBS1 and perhaps the MRN complex may be dispensable for oxidative stress responses. At the same time, NBS1 has a role in TLS following UV-induced DNA damage, but ATM and MRE11 do not. Therefore, distinct functional activities of ATM, NBS1, and MRE11 may underlie the differences in clinical phenotypes of A-T, ATLD, and NBS, including neurodegeneration. However, future studies focusing on distinct functions of these genes are required.
References
Boder E, Sedgwick RP. Ataxia-telangiectasia; a familial syndrome of progressive cerebellar ataxia, oculocutaneous telangiectasia and frequent pulmonary infection. Pediatrics. 1958;21:526–54.
Gotoff SP, Amirmokri E, Liebner EJ. Ataxia telangiectasia. Neoplasia, untoward response to x-irradiation, and tuberous sclerosis. Am J Dis Child. 1967;114:617–25.
McKinnon PJ. Ataxia-telangiectasia: an inherited disorder of ionizing-radiation sensitivity in man. Progress in the elucidation of the underlying biochemical defect. Hum Genet. 1987;75:197–208.
Shiloh Y. Ataxia-telangiectasia: closer to unraveling the mystery. Eur J Hum Genet. 1995;3:116–38.
Shiloh Y. Ataxia-telangiectasia and the Nijmegen breakage syndrome: related disorders but genes apart. Annu Rev Genet. 1997;31:635–62.
Hustinx TW, Scheres JM, Weemaes CM, et al. Karyotype instability with multiple 7/14 and 7/7 rearrangements. Hum Genet. 1979;49:199–208.
Weemaes CM, Hustinx TW, Scheres JM, et al. A new chromosomal instability disorder: the Nijmegen breakage syndrome. Acta Paediatr Scand. 2000;70:557–64.
The International Nijmegen Breakage Syndrome Study Group. Nijmegen breakage syndrome. Arch Dis Child. 2000;82:400–6.
Chrzanowska KH, Gregorek H, Dembowska-Bagińska B, et al. Nijmegen breakage syndrome (NBS). Orphanet J Rare Dis. 2012;7:e13.
Stewart GS, Maser RS, Stankovic T, et al. The DNA double-strand break repair gene hMRE11 is mutated in individuals with an ataxia-telangiectasia-like disorder. Cell. 1999;99:577–87.
Taylor AM, Groom A, Byrd PJ. Ataxia-telangiectasia-like disorder (ATLD)-its clinical presentation and molecular basis. DNA Repair (Amst). 2004;3:1219–25.
Hernandez D, McConville CM, Stacey M, et al. A family showing no evidence of linkage between the ataxia telangiectasia gene and chromosome 1q22-23. J Med Genet. 1993;30:135–40.
Savitsky K, Bar-Shira A, Gilad S, et al. A single ataxia telangiectasia gene with a product similar to PI-3 kinase. Science. 1995;268:1749–53.
Shiloh Y, Ziv Y. The ATM protein kinase: regulating the cellular response to genotoxic stress, and more. Nat Rev Mol Cell Biol. 2013;14:197–210.
Lovejoy CA, Cortez D. Common mechanisms of PIKK regulation. DNA Repair. 2009;8:1004–8.
Kong X, Shen Y, Jiang N, et al. Emerging roles of DNA-PK besides DNA repair. Cell Signal. 2011;23:1273–80.
Nam EA, Cortez D. ATR signalling: more than meeting at the fork. Biochem J. 2011;436:527–36.
Gobbini E, Cesena D, Galbiati A, et al. Interplays between ATM/Tel1 and ATR/Mec1 in sensing and signaling DNA double-strand breaks. DNA Repair (Amst). 2013;12:791–9.
Matsuura S, Tauchi H, Nakamura A, et al. Positional cloning of the gene for Nijmegen breakage syndrome. Nat Genet. 1998;19:179–81.
Tauchi H, Matsuura S, Kobayashi J, et al. Nijmegen breakage syndrome gene, NBS1, and molecular links to factors for genome stability. Oncogene. 2002;21:8967–80.
Chamankhah M, Wei YF, Xiao W. Isolation of hMRE11B: failure to complement yeast mre11 defects due to species-specific protein interactions. Gene. 1998;225:107–16.
Tauchi H, Kobayashi J, Morishima K, et al. The forkhead-associated domain of NBS1 is essential for nuclear foci formation after irradiation but not essential for hRAD50 hMRE11 NBS1 complex DNA repair activity. J Biol Chem. 2001;276:12–5.
Barbi G, Scheres JMJC, Schindler D, et al. Chromosome instability and X-ray hypersensitivity in a microcephalic and growth-retarded child. Am J Med Genet. 1991;40:44–50.
Thompson LH. Recognition, signaling, and repair of DNA double-strand breaks produced by ionizing radiation in mammalian cells: the molecular choreography. Mutat Res. 2012;751:158–246.
Fujimori A, Tachiiri S, Sonoda E, et al. Rad52 partially substitutes for the Rad51 paralog XRCC3 in maintaining chromosomal integrity in vertebrate cells. EMBO J. 2001;20:5513–20.
Tauchi H, Kobayashi J, Morishima K, et al. Nbs1 is essential for DNA repair by homologous recombination in higher vertebrate cells. Nature. 2002;420:93–8.
Khanna KK, Beamish H, Yan J, et al. Nature of G1/S cell cycle checkpoint defect in ataxia-telangiectasia. Oncogene. 1995;11:609–18.
Beamish H, Williams R, Chen P, et al. Defect in multiple cell cycle checkpoints in ataxia-telangiectasia postirradiation. J Biol Chem. 1996;271:20486–93.
Banin S, Moyal L, Shieh S, et al. Enhanced phosphorylation of p53 by ATM in response to DNA damage. Science. 1998;281:1674–7.
Canman CE, Lim DS, Cimprich KA, et al. Activation of the ATM kinase by ionizing radiation and phosphorylation of p53. Science. 1998;281:1677–9.
Matsuoka S, Ballif BA, Smogorzewska A, et al. ATM and ATR substrate analysis reveals extensive protein networks responsive to DNA damage. Science. 2007;316:1160–6.
Lim DS, Kim ST, Xu B, et al. ATM phosphorylates p95/nbs1 in an S-phase checkpoint pathway. Nature. 2000;404:613–7.
Zhao S, Weng YC, Yuan SS, et al. Functional link between ataxia-telangiectasia and Nijmegen breakage syndrome gene products. Nature. 2000;405:473–7.
Bakkenist CJ, Kastan MB. DNA damage activates ATM through intermolecular autophosphorylation and dimer dissociation. Nature. 2003;421:499–506.
Falck J, Coates J, Jackson SP. Conserved modes of recruitment of ATM, ATR and DNA-PKcs to sites of DNA damage. Nature. 2005;434:605–11.
Crawford TO. Ataxia telangiectasia. Semin Pediatr Neurol. 1998;5:287–94.
Shiloh Y, Lederman HM. Ataxia-telangiectasia (A-T): an emerging dimension of premature ageing. Ageing Res Rev. 2016;33:76–88. pii: S1568-1637(16)30078-30082.
Gatti RA, Vinters HV. Cerebellar pathology in ataxia-telangiectasia: the significance of basket cells. Kroc Found Ser. 1985;19:225–32.
Lavin MF. The appropriateness of the mouse model for ataxia-telangiectasia: neurological defects but no neurodegeneration. DNA Repair (Amst). 2013;12:612–9.
Carlessi L, Fusar Poli E, De Filippis L, et al. ATM-deficient human neural stem cells as an in vitro model system to study neurodegeneration. DNA Repair (Amst). 2013;12:605–11.
Reichenbach J, Schubert R, Schindler D, et al. Elevated oxidative stress in patients with ataxia telangiectasia. Antioxid Redox Signal. 2002;4:465–9.
Kamsler A, Daily D, Hochman A, et al. Increased oxidative stress in ataxia telangiectasia evidenced by alterations in redox state of brains from Atm-deficient mice. Cancer Res. 2001;61:1849–54.
Guo Z, Kozlov S, Lavin MF, et al. ATM activation by oxidative stress. Science. 2010;330:517–21.
Zhang J, Kim J, Alexander A, et al. A tuberous sclerosis complex signalling node at the peroxisome regulates mTORC1 and autophagy in response to ROS. Nat Cell Biol. 2013;15:1186–96.
Zhang J, Tripathi DN, Jing J, et al. ATM functions at the peroxisome to induce pexophagy in response to ROS. Nat Cell Biol. 2015;17:1259–69.
Valentin-Vega YA, Maclean KH, Tait-Mulder J, et al. Mitochondrial dysfunction in ataxia-telangiectasia. Blood. 2012;119:1490–500.
Valentin-Vega YA, Kastan MB. A new role for ATM: regulating mitochondrial function and mitophagy. Autophagy. 2012;8:840–1.
Ambrose M, Goldstine JV, Gatti RA. Intrinsic mitochondrial dysfunction in ATM-deficient lymphoblastoid cells. Hum Mol Genet. 2007;16:2154–64.
Gatti RA, Bick M, Tam CF, et al. Ataxia-telangiectasia: a multiparameter analysis of eight families. Clin Immunol Immunopathol. 1982;23:501–16.
Nowak-Wegrzyn A, Crawford TO, Winkelstein JA, et al. Immunodeficiency and infections in ataxia-telangiectasia. J Pediatr. 2004;144:505–11.
Taylor AM, Metcalfe JA, Thick J, et al. Leukemia and lymphoma in ataxia telangiectasia. Blood. 1996;87:423–38.
Isoda T, Takagi M, Piao J, et al. Process for immune defect and chromosomal translocation during early thymocyte development lacking ATM. Blood. 2012;120:789–99.
Dujka ME, Puebla-Osorio N, Tavana O, et al. ATM and p53 are essential in the cell- cycle containment of DNA breaks during V(D)J recombination in vivo. Oncogene. 2010;29:957–65.
Murphy RC, Berdon WE, Ruzal-Shapiro C, et al. Malignancies in pediatric patients with ataxia telangiectasia. Pediatr Radiol. 1999;29:225–30.
Olsen JH, Hahnemann JM, Borresen-Dale AL, et al. Cancer in patients with ataxia-telangiectasia and in their relatives in the Nordic countries. J Natl Cancer Inst. 2001;93:121–7.
Bartkova J, Rezaei N, Liontos M, et al. Oncogene-induced senescence is part of the tumorigenesis barrier imposed by DNA damage checkpoints. Nature. 2006;444:633–7.
Schubert R, Reichenbach J, Zielen S. Growth factor deficiency in patients with ataxia telangiectasia. Clin Exp Immunol. 2005;140:517–9.
Yang DQ, Kastan MB. Participation of ATM in insulin signalling through phosphorylation of eIF-4E-binding protein 1. Nat Cell Biol. 2000;2:893–8.
Miles PD, Treuner K, Latronica M, et al. Impaired insulin secretion in a mouse model of ataxia telangiectasia. Am J Physiol Endocrinol Metab. 2007;293:E70–4.
Wu D, Yang H, Xiang W, et al. Heterozygous mutation of ataxia-telangiectasia mutated gene aggravates hypercholesterolemia in apoE-deficient mice. J Lipid Res. 2005;46:1380–7.
Schneider JG, Finck BN, Ren J, et al. ATM-dependent suppression of stress signaling reduces vascular disease in metabolic syndrome. Cell Metab. 2006;4:377–89.
Takagi M, Uno H, Nishi R, et al. ATM regulates adipocyte differentiation and contributes to glucose homeostasis. Cell Rep. 2015;10:957–67.
Nakamura K, Kato A, Kobayashi J, et al. Regulation of homologous recombination by RNF20-dependent H2B ubiquitination. Mol Cell. 2011;41:515–28.
Sakamoto S, Iijima K, Mochizuki D, et al. Homologous recombination repair is regulated by domains at the N- and C-terminus of NBS1 and is dissociated with ATM functions. Oncogene. 2007;26:6002–9.
Kass EM, Helgadottir HR, Chen CC, et al. Double-strand break repair by homologous recombination in primary mouse somatic cells requires BRCA1 but not the ATM kinase. Proc Natl Acad Sci U S A. 2013;110:5564–9.
Kijas AW, Lim YC, Bolderson E, et al. ATM-dependent phosphorylation of MRE11 controls extent of resection during homology directed repair by signalling through exonuclease 1. Nucleic Acids Res. 2015;43:8352–67.
Zou L, Elledge SJ. Sensing DNA damage through ATRIP recognition of RPA-ssDNA complexes. Science. 2003;300:1542–8.
Shiotani B, Nguyen HD, Håkansson P, et al. Two distinct modes of ATR activation orchestrated by Rad17 and Nbs1. Cell Rep. 2013;3:1651–162.
Morishima K, Sakamoto S, Kobayashi J, et al. TopBP1 associates with NBS1 and is involved in homologous recombination repair. Biochem Biophys Res Commun. 2007;362:872–9.
Cox J, Jackson AP, Bond J, et al. What primary microcephaly can tell us about brain growth. Trends Mol Med. 2006;12:358–66.
Zhang B, Wang E, Dai H, et al. Phosphorylation of the BRCA1 C terminus (BRCT) repeat inhibitor of hTERT (BRIT1) protein coordinates TopBP1 protein recruitment and amplifies ataxia telangiectasia-mutated and Rad3-related (ATR) signaling. J Biol Chem. 2014;289:34284–95.
Shimada M, Sagae R, Kobayashi J, et al. Inactivation of the Nijmegen breakage syndrome gene leads to excess centrosome duplication via the ATR/BRCA1 pathway. Cancer Res. 2009;69:1768–75.
Yanagihara H, Kobayashi J, Tateishi S, et al. NBS1 recruits RAD18 via a RAD6-like domain and regulates pol η-dependent translesion DNA synthesis. Mol Cell. 2011;43:788–97.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Kobayashi, J. (2019). Ataxia-Telangiectasia and Nijmegen Breakage Syndrome. In: Nishigori, C., Sugasawa, K. (eds) DNA Repair Disorders. Springer, Singapore. https://doi.org/10.1007/978-981-10-6722-8_13
Download citation
DOI: https://doi.org/10.1007/978-981-10-6722-8_13
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-10-6721-1
Online ISBN: 978-981-10-6722-8
eBook Packages: MedicineMedicine (R0)