Abstract
Pulmonary arteriovenous malformations (PAVMs) are abnormal direct communications between the pulmonary artery and vein. Significant PAVMs can result in systemic hypoxemia with exertional dyspnea, paradoxical embolization with stroke, brain abscesses, and pulmonary hemorrhage with massive hemoptysis. Current guidelines recommend treatment for PAVMs when the feeding vessel is greater than 3 mm in diameter regardless of the presence of symptoms. Aortopulmonary collateral arteries (APCs) are frequently present in patients with cyanotic congenital heart disease and reduced pulmonary blood flow. Large or multiple collaterals can result in pulmonary overperfusion and symptomatic cardiac volume overload. Transcatheter embolotherapy has been established as the preferred treatment for both PAVMs and APCs. In this article, the physiopathology, clinical significance, occlusion technique, and potential complications for transcatheter embolization of these abnormal vessels are presented.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Target Vessel
- Collateral Artery
- Hereditary Hemorrhagic Telangiectasia
- Feeding Artery
- Transcatheter Embolization
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Transcatheter Embolization of Pulmonary Arteriovenous Malformations
1.1 Anatomic Description and Physiopathology
Pulmonary arteriovenous malformations (PAVMs) are direct high-flow, low-resistance fistulous communications between the pulmonary arteries and veins, bypassing the normal pulmonary capillary bed and resulting in an intrapulmonary right-to-left shunt.
Most PAVMs are congenital, with 80–95 % cases are associated with hereditary hemorrhagic telangiectasia.
Acquired PAVMs are even less frequent, occurring after heart surgery (Fontan or Glenn procedure), trauma, and pulmonary operations [1].
Most PAVMs are identified in the lower lobes, with the left lower lobe being the most common location. PAVMs are usually classified into single or multiple types. Approximately 80 % of PAVMs are simple, in which the feeding arteries arise from one or more branches of a single segmental pulmonary artery.
The majorities of the rest are complex PAVMs, which have multiple segmental feeding arteries from more than one pulmonary segment. A smaller percentage of PAVMs are diffuse, in which there is disseminated involvement of multiple pulmonary segments.
PAVMs can be further characterized according to according to their radiological appearance. The fistula-type PAVM has a feeding artery directly connected to a draining vein, with a venous sac.
Less commonly, PAVMs are plexiform with a multiseptated aneurysm or a cluster of vascular channels [2].
1.2 Clinical Manifestation
Clinical manifestation of patients with PAVM varies depending on the size, number, and flow through the PAVM.
Most PAVMs, especially if they are small ones, can be clinically silent for a long time. However, large or diffuse malformations can cause a wide spectrum of clinical manifestations including exertional dyspnea, fatigability, cyanosis, and neurologic disorders (infarcts, transient ischemic attack, and brain abscesses) secondary to paradoxical embolism as well as life-threatening hemoptysis due to sac rupture.
Because the pulmonary capillary bed is bypassed, the blood flowing through a PAVM is not oxygenated and directly drained into the pulmonary veins, resulting in systemic hypoxemia.
In addition, the absence of the normal filtering of the pulmonary capillary allows particulate matter (air bubbles or clots) to enter into the systemic circulation leading to serious neurologic complications.
1.3 Indications and Patient Selection
Transcatheter embolization of PAVMs is indicated for patients who have evidence of significant systemic hypoxemia or for patients at risk for or who have a documented history of a paradoxical embolic event and also for the prevention of pulmonary hemorrhage [1].
The current guidelines recommend transcatheter embolization of PAVMs for all symptomatic patients and for asymptomatic patients with discrete lesions with feeding arteries greater than 3 mm in diameter [3].
For patients with complex or diffuse PAVMs that cannot be safely or completely occluded, a reduction in the volume of right-to-left shunting by partial or staged transcatheter closure may also be indicated in order to reduce cyanosis and alleviate symptoms.
1.4 Treatment Options
Therapeutic options for PAVMs include transcatheter embolization with coils or Amplatzer devices and surgical excision.
Currently, transcatheter embolization has become the mainstay of treatment for PAVMs. Surgical resection is currently rarely necessary and reserved for patients who are not candidates for embolization (e.g., in patients with diffuse lesions) or when embolization fails or unavailable.
The primary aim of embolotherapy is to eliminate or reduce the right-to-left shunting to relieve desaturation symptoms, prevent pulmonary hemorrhage, and, most importantly, prevent neurologic complications associated with paradoxical embolism.
1.5 Pre-procedural Imaging
1.5.1 Contrast-Enhanced Echocardiography
Contrast-enhanced echocardiography is useful in the assessment of PAVM since it helps to distinguish between intracardiac and extracardiac shunts. Intracardiac shunts are characterized by the visualization of bubbles in the left heart chambers within 1–2 cardiac cycles after appearing in the right atrium. In patients with PAVMs, this event occurs after a delay of 3–8 cardiac cycles.
1.5.2 Chest Computed Tomography
Multidetector CT (MDCT) has been established as the primary imaging modality in the detection of PAVM. CT angiography, especially with three-dimensional reconstruction, can provide important details to inform subsequent catheter-based treatment including the location, number, and size of the arterial feeding vessels and the presence of multiple, smaller malformations.
1.5.3 Contrast-Enhanced Magnetic Resonance Angiography (MRA)
Contrast-enhanced magnetic resonance angiography (MRA) has high sensitivity and specificity and should be considered in young patients where radiation exposure will be of greater concern. It is potentially able to provide precise information on the number, location, and complexity of PAVMs.
1.6 Technique (Step by Step)
1.6.1 Diagnostic Pulmonary Angiography
Following femoral venous access is obtained, weight-adjusted unfractionated heparin (100 U/Kg) is given intravenously.
Routine right heart catheterization is performed to assess the pulmonary artery pressure.
The initial diagnostic pulmonary angiogram is usually performed in the anteroposterior (AP) projection and ipsilateral 40° oblique (this projection places the heart over the injected lung and spreads the basal segments) using a 6-Fr pigtail catheter or other catheters.
Complete angiography in both lungs prior to any attempt at embolization is mandatory in order to identify all feeder vessels to a PAVM, their diameter, and length. This determines the occlusion strategy.
1.6.2 Occluding Materials
The choice of the occlusion device is primarily based on the anatomy morphology and size of the vessel as well as on the personal experience and preference of the interventionalist. In general, PAVM with feeding artery diameters of 3–8 mm is treated with coils, whereas those with diameters ≥9 mm may be treated with Amplatzer duct occluder or vascular plugs.
1.6.2.1 Coils
Magnetic resonance-compatible steel or platinum pushable or detachable coils are used in the majority of cases. It is recommended to choose coils that are at least 20–30 % larger than the vessel to be occluded. The main drawbacks of coil occlusion include the risk of embolization, the need for multiple coils, the potential for recanalization, and the resulting long procedure time without complete occlusion. Pictures regarding coils are reported in the chapter on ductus arteriosus closure.
1.6.2.2 ADO
Before the advent of AVP, the ADO device is used for the occlusion of medium-sized to large PAVMs. Several reports in the literature have described successful transcatheter treatment of large PAVMs using the ADO device. However, their application is limited by the need for relatively large long sheaths or large guiding catheters. Pictures regarding ADO are reported in the chapter on ductus arteriosus closure.
1.6.2.3 AVP
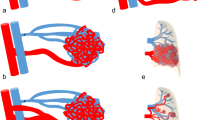
The AVPs are particularly suitable for embolization of large high-flow feeding vessels. They are a woven nitinol wire cylinder that can be delivered via small catheters such as standard 5–8-Fr coronary guiding catheters (Fig. 31.1a, b). The recent developed AVP IV (Fig. 31.1c) can even be introduced through a diagnostic catheter. During embolization, at least a 30–50 % oversizing of the device to the feeding vessel is recommended for the prevention of device migration and total occlusion. The only potential drawback to the AVP appears to be the relatively long length of the occluder that may limit its use if the target vessel is too short.
1.6.3 Techniques for Closing PAVM with Coils
To date, the most common approach to closing PAVM is embolization of the feeding artery using pushable fibered or detachable coils delivered via coaxial catheters.
Once a PAVM and its feeding arteries had been identified, selective catheterization of the target vessels is performed using a coaxial guide system with an outer 6-Fr 80 cm guide catheter and inner 5-Fr 100 cm end-hole coil delivery catheter (i.e., multipurpose catheter, Cook).
The added support provided by the guiding catheter prevents the inner coil delivery catheter from backing out of the target vessel during embolization, thereby allowing the coils to be delivered more precisely and in a tighter mass.
The use of such a coaxial guide system also allows smaller coils to be positioned within a larger anchor or scaffold coil.
Access to the middle and upper lobes can be challenging and is facilitated by the use of a 5-Fr Judkins left/right coronary catheter (cordis) or internal mammary catheter.
Once a feeding segmental artery is catheterized superselectively, the guiding catheter is advanced over the inner catheter to secure a stable position (i.e., placed in the parent segmental vessel), and the inner catheter is advanced into the vessel that feeds the malformation.
Hand-injected angiography(usually 4 frames/s) in multiple projections is performed to confirm position and define exact anatomy of the PAVM to determine site of implantation as well as size of the device to be used.
It is important to achieve as distal an embolization as possible in the feeding artery to avoid occluding branches to normal adjacent lung. This is especially true when multiple PAVMs are present and multiple indiscriminate proximal occlusions could result in a significant reduction in pulmonary blood supply.
Coil size is an important consideration. Undersized coils are at risk to pass through the malformation and becoming an embolic agent, while oversized coils may be difficult to form a tight nest. Many interventionalist empirically oversize the initial coil to the feeding vessel by at least 20 %. After placement of the first coil, additional coils must be positioned until blood flow to the PAVM has ceased. In order to create a dense, cross-sectional occlusion for durable result, packing of subsequent smaller coils in the center of the first deployed coil is essential (Fig. 31.2).
The “anchor or side-branch technique” and “scaffold technique” have been documented to be very useful in achieving complete cross-sectional occlusion and avoiding paradoxical embolization of the coil via the PAVM [1].
The “anchor technique” is characterized by the first 2 cm of the coil and is purposely anchored in a side branch close to the aneurysmal sac and the remainder of the coil positioned in the feeding artery and additional coils are densely packed so that cross-sectional occlusion is obtained. By securing the tip in a side branch, the risk of coil dislodgment is minimized.
The so-called scaffold technique is mainly used for high-flow vessels or when there is no anchoring vessel available. Initially, a high radial force, fibered coil with a diameter 2 mm larger than the feeding artery is placed to create a scaffold. Then several small diameter high radial force coils are placed as well into the endoskeleton, followed by several softer coils, until cross-sectional occlusion is obtained.
Packing of the aneurysm sac has been proposed as an alternative to feeding artery embolization when the feeding artery is too short to avoid sacrifice of large normal pulmonary artery branches or when the artery is a high-flow type with a higher risk of paradoxical embolization of coil.
Following the feeding artery that is catheterized superselectively with a 6-Fr guiding catheter, a coaxial microcatheter (i.e., a 2/2.6-Fr microcatheter (Excelsior; Boston Scientific)) is advanced coaxially through the catheter into the aneurysmal sac. Several microcoils (0.018 in.) are densely filled within the venous sac until a large matrix is established.
1.6.4 Techniques for Closing PAVM with Amplatzer Devices
For patients with PAVMs of large feeding artery or high-flow pattern, occlusion with coils is technically demanding and time consuming.
Alternatively, the recently developed Amplatzer vascular plug (AVP) appears to be an effective tool for embolization of PAVMs, particularly in patients with large outflow or short feeding arteries in whom embolization using coils entails a great risk of paradoxical embolization.
The AVP is made from densely woven nitinol mesh wires that can be delivered via small catheters such as standard 5–8-Fr coronary guiding catheters and can be repositioned multiple times prior to its final release.
Following pulmonary artery pressure recording and angiography, the feeding artery is selectively cannulated using an appropriate-sized guiding catheter (5-Fr guiding catheter for AVPs 4–8 mm in diameter, 6 Fr for AVPs 10–12 mm in diameter, and 8 Fr for AVPs 14–16 mm in diameter).
Once a suitable position has been achieved as distally as possible within the feeding vessel and beyond any branches to normal lung, the AVP is then delivered to the target area.
The diameter of the AVP is selected to be 30–50 % larger than the diameter of the feeding artery, according to the manufacturer’s recommendation. Satisfactory positioning of the AVP is confirmed by repeat arteriography via the guiding catheter before its final detachment. If suboptimally positioned, the AVP is resheathed and redeployed in a more appropriate site. Since the AVP does not cause instantaneous thrombosis and in high-flow situations thrombosis typically takes up to 15 min, control angiography should be performed for at least 15 min after deployment of the occluder.
The Amplatzer duct occluder (ADO) can also be an alternative for closing large PAVM (Fig. 31.3). After catheterization of the feeding vessel, a long delivery sheath is introduced over a stiff exchange wire and placed in the feeding artery as close to the malformation as possible. The size of the ADO selected for embolization should be 2–4 mm larger than the caliber of the feeding vessel at site of implantation.
After embolization of the feeding artery or arteries by any of the above methods, repeated segmental and lobar angiography should be performed to assess for complete occlusion and any accessory feeding vessels that might also require embolization.
1.7 Expected Results
-
1.
Pulmonary angiogram post-embolization confirmed complete occlusion of the PAVMs.
-
2.
A significant improvement in systemic arterial oxygen saturation and sustained relief of clinical symptoms attributed to the PAVMs on follow-up are obtained after embolization.
-
3.
Contrast-enhanced CT at follow-up showed that the PAVMs remained occluded, with a significant shrinkage of the vein sac or complete resolution of the malformations.
1.8 Complications and Its Management
To date, there is no mortality occurred during the procedure and long-term follow-up. The complications of transcatheter embolization of PAVMs documented in the literature have been infrequent and are listed as follows:
1.8.1 Device Embolization
Device migration with paradoxical embolization is one of the most severe complications and occurs in 0.7–3 % of treated patients, especially in cases of high-flow malformations with large outflow vessels. Paradoxical coil embolism into the cerebral artery, left popliteal artery, and left carotid artery has been reported. The choice of appropriate-sized coils is crucial to minimize the risk of coil embolization. The “anchoring” and “scaffolding” techniques are also frequently applied to overcome the problem of coil migration.
1.8.2 Pulmonary Infarction
Pulmonary infarction has been observed in about 3 % of patients. It usually occurs when the embolization causes occlusion of normal branches secondary to overly proximal positioning of embolization materials. To minimize this event, the embolization materials should be placed as close to the PAVM and as distal to normal side branches as possible.
1.8.3 Air Embolization
Air embolization is not infrequently encountered during the procedure. This usually occurs when a catheter or wire is withdrawn rapidly out of the sheath. When blood cannot replace the space previously occupied by the retrieved catheter, air will be suck into the delivery sheath. Air accidentally enters into the coronary arteries causing acute chest pain, bradycardia, and temporary ECG changes. This usually resolves within l5 min. A continuous flushing of catheters, observation for back-bleeding, and removal of catheters or wires “underwater” can largely prevent this complication.
1.8.4 Pleurisy
Pleurisy is the most frequent complication of embolization occurring in approximately 15–31 % of patients. Delayed pleurisy (4–6 weeks after the procedure) with fever and infiltrates has been reported mainly with larger PAVMs. It is thought that this is due to delayed thrombosis of the aneurysmal sac and is usually self-limited and responsive to nonsteroidal anti-inflammatory drugs.
1.8.5 PAVM Recanalization
Recurrence of PAVMs can occur in 15 % of cases, but is not considered a real complication or failure of the treatment, since it can result from recanalization of previously occluded PAVMs, collateralization from adjacent arteries, or missed accessory pathways. Recanalization of PAVM can be attributed to coil elongation (use of oversized coils), poor coil packing, or use of an insufficient number of coils. This complication can be reduced by good closure technique and by selecting appropriate occluder for large PAVM.
1.9 Post-procedural Care and Follow-Up
Most patients can be discharged on the next day following the procedure. For patients with large feeding arteries and received large occluder, daily oral aspirin (5 mg/kg/day) is recommended for 6 months to prevent thromboembolic complications. Prophylactic antibiotics are not routinely recommended for all treated patients. In patients with incomplete occlusion with residual shunting, physicians should be aware of the risk of mechanical hemolytic anemia. Care should also be taken to early detect femoral thrombosis and local hematoma at puncture site.
Long-term follow-up of treated patients with imaging modality and clinical and physiologic evaluation should be performed in order to document recanalization of embolized PAVMs early, as well as to detect growth or enlargement of the untreated small lesions. It is recommended that a combination of clinical evaluation, physiologic testing, and contrast-enhanced CT scan is the best algorithm of follow-up.
2 Transcatheter Embolization of Aortopulmonary Collateral Arteries
2.1 Anatomic Description and Physiopathology
Aortopulmonary collateral arteries (APCs) can be detected in association with various congenital heart diseases (CHDs), from simple malformations to complex cyanotic CHDs such as tetralogy of Fallot, pulmonary atresia, and single ventricle with pulmonary stenosis, resulting in varying degrees of left-to-right shunting.
They may be masked by another predominant cardiac lesion and are not discovered until after surgical repair of the major lesions.
The APCs typically originate from the anterior wall of the descending thoracic aorta at the level of the carina. However, they can also arise from the lower descending thoracic and abdominal aorta or innominate arteries (Fig. 31.4a–c).
A 10-year-old boy who had previously undergone surgical correction for TOF was referred for transcatheter occlusion of APCs. Selective angiogram in the innominate artery (a), the left subclavian (b), and the descending aorta (c) demonstrating multiple APCs. Repeated angiogram (d–f) after AVP and coil deployed, confirming complete occlusion of the major APCs
They frequently run a retroesophageal course. Occasionally, the collateral arteries may arise from the coronary artery.
In patients with cyanotic congenital heart disease and reduced pulmonary blood flow, the additional pulmonary blood flow provided by APCs can relieve systemic hypoxemia prior to surgical correction. However, APCs’ flow can result in significant volume overloading of the left ventricle, compete with and limit blood flow via the pulmonary arteries, and increase pulmonary arterial pressure and vascular resistance during the postoperative period of corrective surgery.
2.2 Clinical Manifestation
Small APCs are usually clinically silent, but large or multiple APCs can result in pulmonary overperfusion and symptomatic cardiac volume overload manifested as exertional dyspnea, recurrent pleural effusion, protein-losing enteropathy, frequent lower airway infection, and hemoptysis.
2.3 Indications and Patient Selection [3]
2.3.1 Indications
Transcatheter occlusion of APCs is indicated for the treatment of aortopulmonary collateral vessels with documented large left-to-right shunting in biventricular or single-ventricle physiology that results in congestive heart failure, pulmonary overcirculation, and respiratory compromise, or development of pleural effusion or protein-losing enteropathy.
2.3.2 Relative Indications
-
1.
Transcatheter occlusion of APCs may be considered in the presence of moderate-sized collaterals found in asymptomatic single-ventricle patients undergoing routine pre-Glenn or pre-Fontan cardiac catheterization.
-
2.
Transcatheter occlusion of APCs may be considered in patients with pulmonary atresia and aortopulmonary collaterals that have adequate dual supply from native pulmonary arteries.
2.3.3 Contraindications
-
1.
Transcatheter occlusion is not recommended for the presence of APCs of any size in biventricle or single-ventricle patients who have significant cyanosis due to decreased pulmonary flow.
-
2.
Transcatheter occlusion is not recommended for patients in whom the responsible collateral arteries directly supply a large area of pulmonary parenchyma, when embolization could result in infarction of the lung parenchyma.
2.4 Treatment Options
Therapeutic options for APCs include transcatheter embolization and surgical ligation. Surgical ligation can be technically challenging because of the identification, and dissection of the APCs can be very difficult, especially when they are transdiaphragmatic, and the operative field can be flooding by APCs supplying. Transcatheter occlusion is currently the preferred method for the management of APCs. The primary goal of embolotherapy is to control excessive flow of blood to the lungs.
2.5 Pre-procedural Imaging
Conventional angiography remains the gold standard for morphological assessment of the APCs. Noninvasive imaging modalities such as contrast-enhanced magnetic resonance angiography (MRA) and multidetector-row computed tomography (MDCT) with three-dimensional reconstruction are also useful for the assessment of APCs. Both of them can clearly identify the number, origins, course, and diameter of the APCs.
2.6 Technique (Step by Step)
2.6.1 Aortography and Pulmonary Angiography
Access is obtained in both the femoral artery and vein. Systemic anticoagulation (heparin 100 U/Kg) is provided, and the activated clotting time is maintained within the therapeutic range. A standard right heart catheterization is performed to assess the degree of shunting and evaluate the pulmonary artery pressure. A diagnostic aortogram and pulmonary angiogram is performed with a 5-Fr pigtail catheter. The goal is to identify the anatomic characteristics of the APCs including the number, origin, course, diameter, and flow distribution pattern of the APCs and the presence or absence of native pulmonary arterial supply in the region of the “target” vessel. Since there is considerable anatomic variation among APCs in their origins (it can arise anywhere along the aorta or its major side branches), course, and branching patterns, selective angiography at multiple sites is required to fully assess for APCs. In some circumstance, it may also be necessary to perform selective angiography of the right or left subclavian artery, and even the coronary arteries, to fully disclose the collateral arteries.
2.6.2 Occlusion Techniques and Devices
Currently, transcatheter occlusion of APCs is performed most commonly with detachable or undetachable coils and Amplatzer Vascular Plug (AVP). Device selection is made according to the angiographic features of the target vessels.
Following diagnostic aortogram, the target collateral arteries are selectively engaged using a coaxial guide system with an outer 6-Fr Judkins right guiding catheter (Cordis, USA) or Cobra catheter (Terumo, Japan) and inner 5-Fr multipurpose catheter (COOK Corp., USA). The use of coaxial catheters allows for deep coil delivery and reduces the risk of proximal coil malposition. Once a suitable position has been achieved as deeply as possible within the target vessel, the appropriate-sized coils are then delivered to the target vessel. If undetachable coils are used for occlusion, the target vessels are selectively catheterized with a 5-Fr Judkins right guide catheter or Cobra catheter through which a microcatheter is introduced. The use of a coaxial microcatheter avoids the risk that a catheter may be dislocated by tension during the advancement of microcoils and the subsequent problem of coil deployment in an inappropriate systemic artery. With desired catheter position obtained, microcoils are delivered into the target vessel by saline flush.
The AVP is particularly suited for embolization of large, short, high-flow, or tortuous collateral arteries where coil migration is possible or multiple coils may be needed. An appropriate-sized guiding catheter or long sheath is advanced over a hydrophilic coated guidewire into the collateral artery as deeply as possible. The AVP is then advanced via the guiding catheter or sheath into the vessel. Hand-injected angiogram is performed 15 min later to confirm coils or AVP position within collateral arteries (Fig. 31.4d–f).
It is important to recognize that APCs may have multiple sources of arterial supply, and occlusion devices should be delivered as selectively and as deeply into the target vessel as possible to block all potential arterial supply to the final pulmonary exit point.
2.7 Expected Results
-
1.
Cardiac catheterization post-embolization confirmed complete occlusion of the APCs with the pulmonary arterial pressure and oxygen saturation decreased, while the systemic pressure elevated to the normal level.
-
2.
Significant improvement or resolution of symptoms attributed to the APCs at physician follow-up is obtained after embolization.
2.8 Complications and Its Management
2.8.1 Device Embolization
Device embolization into an important systemic artery occurs in about l % of embolization attempts, mainly with coils. It usually occurs when a coil can’t be fully accommodated by the target vessel that led to coil bouncing out of the collateral during or after implantation. In order to avoid such a complication, the selected coils should be of appropriate size and it should be placed as deeply into the target vessel as possible. When coil embolization occurs, retrieval of the coil with a snare may be considered.
2.8.2 Pulmonary Infarction
The complication of pulmonary infarction occurs when the APCs constitute the sole supply to the affected lung or the responsible collateral arteries supply directly a large area of pulmonary parenchyma. Prior to embolization, a careful analysis has to be made based on the collateral circulation to ensure that the collateral arteries targeted for embolization are not the sole source of flow of blood to a parenchymal segment.
2.8.3 Hemolysis
Hemolysis has been rarely reported with embolization of APCs. This rare complication occurs if there is significant residual shunting across the occluder. Once it occurs, the patient should be monitored and treated medically. If hemolysis is so significant that medical treatments is not effective, the residual shunt should be eliminated by further embolization, and surgical removal is an alternative option.
2.9 Post-procedural Care and Follow-Up
Most patients can be discharged in a few days following the procedure. A pre-discharge imaging study including echocardiography, chest X-ray should be performed to assess the cardiac function and occluder position. Long-term follow-up of treated patients with imaging modality and clinical evaluation is recommended.
References
Fahey JT, Pollak JS, White RI (2009) Complications of catheter-based interventions for pulmonary arteriovenous malformations. In: Hijazi ZM, Feldman T, Cheatham JP, Sievert H (eds) Complications during percutaneous interventions for congenital and structural heart disease. Informa, London, pp 195–204
Jones TK (2012) Closure of coronary artery fistula, pulmonary arteriovenous malformation and patent ductus arteriosus. In: Carroll JD, Webb JG (eds) Structural heart disease interventions. Lippincott Williams & Wilkins, Philadelphia, pp 215–218
Feltes TF, Bacha E, Beekman RR (2011) Indications for cardiac catheterization and intervention in pediatric cardiac disease: a scientific statement from the American Heart Association. Circulation 123(22):2607–2652
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer-Verlag Italia
About this chapter
Cite this chapter
Tang, L., Fang, Zf., Zhou, Sh. (2015). Vessel Embolization: Transcatheter Embolization of Pulmonary Arteriovenous Malformations and Aortopulmonary Collateral Arteries. In: Butera, G., Chessa, M., Eicken, A., Thomson, J. (eds) Cardiac Catheterization for Congenital Heart Disease. Springer, Milano. https://doi.org/10.1007/978-88-470-5681-7_31
Download citation
DOI: https://doi.org/10.1007/978-88-470-5681-7_31
Published:
Publisher Name: Springer, Milano
Print ISBN: 978-88-470-5680-0
Online ISBN: 978-88-470-5681-7
eBook Packages: MedicineMedicine (R0)