Abstract
Depression is a highly prevalent form of mental illness that is one of the leading causes of disability worldwide. Because stressful life events frequently trigger its symptoms, depression is often characterized as a stress-related disorder, and chronic exposure to stress has been hypothesized to lead to long-term alterations of the physiological systems thought to mediate the stress response. Understanding the biological changes resulting from chronic stress is important because these long-term modifications may underlie the symptoms of depression. The corticotropin-releasing factor (CRF) system has long been considered to be one of the body’s major regulators of the stress response. Two genes encoding distinct G-protein-coupled CRF receptors have been identified: the CRF1 receptor and CRF2 receptor. Endogenous ligands for these receptors, including CRF, urocortin 1, urocortin 2, and urocortin 3, display different binding affinities for the two CRF-receptor subtypes, as well as distinct behavioral profiles in animal models of depression and anxiety. These findings have led to the hypothesis that CRF1 and CRF2 receptors may play distinct roles in the regulation of stress-related behavior, with the CRF1 receptor underlying the activational components of the stress response and the CRF2 receptor acting as a compensatory coping mechanism. The present chapter will review the role of CRF-related ligands and CRF receptors in depression and proposes targeting the CRF system as a potential pharmacotherapy for depressive disorders.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
44.1 Introduction
Depression is a highly prevalent form of mental illness that affects an estimated 350 million people [1]. In the coming decades, major depression is projected to become the second leading cause of disability worldwide, as well as the leading cause of disability in high-income nations [1]. Because stressful life events frequently trigger depressive symptoms, this illness is often characterized as a stress-related psychiatric disorder. A classic definition of stress is any response to demands, usually noxious, placed on the body [2]. An alternate definition describes stress as any alteration in the psychological homeostatic process [3]. Although body’s response to acute stressors allows it to adapt to environmental demands, chronic exposure to stress has been hypothesized to lead to long-term alterations of the physiological systems that are thought to mediate the stress response. It is these long-term changes that may also underlie the symptoms of stress-related psychiatric disorders such as depression.
Corticotropin-releasing factor (CRF) is a 41-amino-acid neuropeptide that has long been considered to be one of the body’s major regulators of the stress response. It is involved in mediating the neuroendocrine response to stress [4], as well as autonomic [5, 6] and behavioral responses to environmental demands [7, 8]. CRF is the main regulator of the hypothalamic-pituitary-adrenal (HPA) axis stress response, which has been traditionally used by biologists as a method of quantifying stress [4]. When the body is faced with a stressor, CRF neurons are activated in the paraventricular nucleus of the hypothalamus where they send axon terminals to the median eminence. From this area, CRF is released into the portal blood system and carried to the anterior lobe of the pituitary gland where it stimulates the synthesis and release of adrenocorticotropic hormone (ACTH). ACTH subsequently stimulates the release of glucocorticoids by the outer shell of the adrenals. In addition, CRF in the medulla can activate the sympathetic nervous system, stimulating the release of adrenaline from the adrenal medulla and other parts of the sympathetic nervous system [5, 6].
Chronic elevations in CRF and the hormones involved in the endocrine stress response can result in various detrimental physiological effects. Increased CRF levels can lead to the decreased toxicity of natural killer cells in the immune system [9] and induce stress-like changes in gastrointestinal, cardiovascular, and metabolic functions [10–12] via activation of the HPA axis and sympathetic nervous system. ACTH secretion directly influences immune function and acts within the brain to regulate sleep [13, 14]. Hypersecretion of glucocorticoids can result in infection via suppressed immune function, whereas low levels of these hormones can result in inflammatory conditions in laboratory animals [14]. Although the neuroendocrine stress response is important in the regulation of physiological responses to stress, the behavioral response to stress appears to occur independent of HPA axis activation. Hypophysectomy and blockade of the HPA axis response via dexamethasone suppression do not alter the behavioral response to stress produced by central administration of CRF [15, 16]. Thus, it appears that a central site of action is responsible for coordinating stress-related behavior.
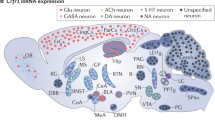
Two genes encoding distinct G-protein-coupled CRF receptors have been identified (Fig. 44.1). The CRF1 receptor is found mainly in the pituitary, amygdala, hippocampus, cerebellum, and cortex and is generally associated with increases in stress-related behaviors [8]. CRF, which preferentially binds to the CRF1 receptor [17], leads to increases in the behavioral stress response in animal models [18–22]. Clinical research has also shown that depressed individuals show increased levels of CRF in cerebrospinal fluid [23]. A number of nonpeptide CRF1 receptor antagonists have been developed with the hope that these drugs may be of therapeutic value in the treatment of depression and other stress-related psychiatric illnesses [24–26], although none have demonstrated clinical utility to date.
Schematic representation of CRF-receptor subtypes and their associated ligands. Corticotropin-releasing factor (CRF) shows preferential binding affinity for the CRF1 receptor. Urocortin 1 (Ucn 1) is equipotent in binding to the CRF1 and CRF2 receptor. Urocortin 2 (Ucn 2) and urocortin 3 (Ucn 3) are 1,000-fold more selective in binding to the CRF2 receptor compared to Ucn 1. However, Ucn 2 induces low levels of activity at the CRF1 receptor, whereas Ucn 3 does not induce CRF1 receptor signaling
The CRF2 receptor is found mainly in the lateral septum, ventromedial hypothalamus, and choroid plexus and exists in three splice variants: the CRF2a, CRF2b, and CRF2c receptors [27, 28], and the discovery of additional neuropeptides belonging to the CRF family has aided in characterizing the role of the CRF2 receptor in the stress response (Fig. 44.2). Urocortin 1 (Ucn 1) is a 40-amino-acid neuropeptide that is thought to be an endogenous ligand for the CRF2 receptor, as it shows equally high binding affinity for both the CRF1 and CRF2 receptors [29] and produces a distinct behavioral profile compared to CRF. Central injections of this peptide more potently reduce feeding in food-deprived rats but only mildly increase locomotor activation compared to CRF [30]. Ucn 1 injections also lead to delayed increases in stress-related behaviors [31].
Amino acid sequence structure of mammalian neuropeptides within the corticotropin-releasing factor peptide family. Represented are the structures of human corticotropin-releasing factor (hCRF), ovine corticotropin-releasing factor (oCRF), human urocortin 1 (hUcn 1), rat urocortin 1 (rUcn 1), human urocortin 2 (hUcn 2), mouse urocortin 2 (mUcn 2), human urocortin 3 (hUcn 3), and mouse urocortin 3 (mUcn 3)
Urocortin 2 (Ucn 2) is another CRF-related neuropeptide composed of 38 amino acids [32]. Ucn 2 shares a similar sequence with stresscopin-related peptide, differing only in the cleavage site of the mature peptide [33]. A putative human sequence, originally identified as human urocortin-related peptide, shares 76 % amino acid identity with the identified mouse sequence and is proposed to be the human ortholog to mouse Ucn 2 [34]. Although Ucn 2 is equipotent in its binding affinity at the CRF2 receptor when compared to Ucn 1, it is 1,000-fold more selective in binding to the CRF2 receptor [32]. A third CRF-related neuropeptide known as urocortin 3 (Ucn 3) has also been identified [34]. Ucn 3 is a 38-amino-acid neuropeptide that shares a similar sequence with stresscopin, differing only in the cleavage site of the mature peptide [33]. Compared to Ucn 2, Ucn 3 displays a similar potency but higher selectivity in binding to the CRF2 receptor [34]. Doses of up to 3 nM of Ucn 3 do not induce adenylate cyclase in CRF1 transfectants in vitro, a marker of CRF1 receptor activity [34]. Ucn 3 immunoreactive projections have been found in the hypothalamus, lateral septum, bed nucleus of the stria terminalis, and amygdala [35], areas believed to mediate the behavioral stress response [36–38]. These areas also are known to express high levels of the CRF2 receptor [39], supporting the notion that Ucn 3 is an endogenous ligand for the CRF2 receptor. The role of Ucn 2 and Ucn 3 in regulating stress-related behaviors is still unclear. Some studies have shown that administration of Ucn 2 and Ucn 3 attenuates the behavioral response to stress [40–42], whereas others have found that these selective CRF2 receptor ligands enhance stress-related behavior [43].
Despite the seemingly contradictory findings regarding CRF2 receptors and stress-related behavior, which will be discussed more in depth later in this chapter, characterization of the CRF receptors suggests that these CRF1 and CRF2 receptors may have distinct roles in the regulation of depressive behaviors. Preclinical studies strongly suggest that activation of the CRF1 receptor increases depression-related behaviors [44–46]. Although there is no general consensus regarding the role of CRF2 receptors in the behavioral stress response, preclinical evidence suggests that underactivation of this receptor may be involved in the regulation of increased depression-like behavior in animals [47, 48]. The present chapter will review the role of CRF-related ligands and CRF receptors in depression and proposes targeting the CRF system as a potential pharmacotherapy for depressive disorders.
44.2 Corticotropin-Releasing Factor and the Behavioral Stress Response
Much of the data regarding CRF itself and nonselective CRF-receptor antagonists focus more on animal models of anxiety rather than depression. These results should be strongly considered when examining the role of CRF in depression, however, given the multifaceted complexity and high incidence of comorbidity between these two disorders [49–51]. CRF injected into unstressed animals under familiar conditions leads to increased locomotor activation [18, 19], whereas in unfamiliar settings, centrally administered CRF can lead to behavioral suppression [18]. In addition, CRF administration can lead to even greater reductions in operant responding during the conflict test [20], a model of anxiety in which a reward is accompanied by presentation of an aversive stimulus in order to suppress responding for the reward. Other examples of stress-related behavior induced by central administration of CRF include an enhanced acoustic startle response [21, 52], increases in the conditioned fear response [22], and decreased appetite [53, 54]. Furthermore, transgenic mice overproducing CRF show decreased exploration of a novel environment compared to wild types, an effect potentiated by exposure to social defeat stress [55]. Overexpression of CRF in the amygdala also leads to increases in stress-related behaviors in rats [56].
Further evidence that brain CRF systems play an important role in the regulation of the behavioral response to stress comes from studies using nonselective peptide CRF-receptor antagonists. These antagonists attenuate both CRF and stress-induced behavioral changes. α-Helical CRF(9–41), a CRF-receptor antagonist, decreases the CRF-enhanced acoustic startle response when centrally injected in rats [57]. This antagonist also increases exploratory behavior of the open arms of the elevated plus maze following administration in CRF-overproducing mice [55]. Open-arm preference in the elevated plus maze, as indicated by the ratio of open-arm to total-arm time and entries, has been proposed to relate inversely to anxiety [58]. A second peptide CRF-receptor antagonist, D-Phe-CRF(12–41), reduces both CRF- and stress-induced increases in locomotor activation [59]. Astressin, a third CRF-receptor antagonist, decreases CRF-induced locomotor activation and increases open-arm exploration in the elevated plus maze [60].
CRF-receptor antagonists have also been shown to reduce stress-induced behavioral changes. In the elevated plus maze, administration of α-helical CRF(9–41) leads to increased exploration of the open arms of the elevated plus maze in rats subjected to restraint stress, swim stress, or social conflict stress [61]. Astressin also increases open-arm exploration in the elevated plus maze in rats subjected to social conflict stress [60]. D-Phe-CRF(12-41) attenuates stress-induced increases in locomotor activation and decreases in exploration of the open arms of the elevated plus maze [59].
With regard to animal models of depression, D-Phe-CRF(12–41) reverses increases in intracranial self-stimulation reward thresholds induced by central CRF administration [62]. Injections of CRF [63, 64] and CRF promoter-induced overexpression of CRF [56] have also shown to increase immobility in rats observed in the forced swim test. The forced swim test is an animal model of depression in which immobility is thought to model a depressive-like state. Treatment with standard antidepressant drugs can reverse immobility, an effect correlated with antidepressant efficacy in humans [65]. These results suggest that increased CRF activity may be a key component in regulating depressive-like behaviors in animals.
44.3 CRF1 Receptors, Stress-Related Behavior, and Animal Models of Depression
Preclinical evidence strongly suggests that activation of the CRF1 receptor increases stress-related behavior [8]. As described above, CRF, which preferentially binds to the CRF1 receptor, leads to increases in the behavioral stress response independent of HPA axis activation. For example, ovine CRF, which shows an 80-fold higher affinity in binding to the CRF1 receptor vs. the CRF2 receptor [17], produces increased motor activation and decreases open-arm exploration in the elevated plus maze [40]. CRF1 receptor knockout mice lacking CRF1 receptors also show a decreased responsiveness to stressful stimuli [66–68] and less spontaneous motor activity [69]. These data demonstrating that activation of the CRF1 receptor increases the behavioral response to stress suggests the CRF1 receptor may be a key biological component in regulating stress-related psychiatric disorders.
A number of CRF1 receptor antagonists have been examined in animal models of depression, yielding mixed results. CP-154,526, one of the earliest nonpeptide CRF1 receptor antagonists to be developed [70], reversed escape deficit in rats exposed to inescapable shock without affecting controls in the learned helplessness task [71]. During this task, animals were exposed to a series of inescapable shocks and then given the opportunity to escape shock following a period of time. Decreased escape behavior has been proposed to indicate a depressive-like state [72]. When administered 60 min before a test session, acute and chronic injections of CP-154,526 and CRA1000, another nonpeptide CRF1 receptor antagonist, reduced escape failure in rats in a manner comparable to chronic treatment with the tricyclic antidepressant imipramine [73, 74]. Acute and chronic treatment with the CRF1 receptor antagonist R278995/CRA0450 also reduced escape failures [75]. However, the CRF1 receptor antagonists DMP696 and DMP904 were not effective in learned helplessness task [76].
Data obtained using the forced swim test have also been equivocal regarding the effectiveness of CRF1 antagonists in animal models of depression. For example, CP-154,526, R121919, and antalarmin, CRF1 antagonists that are structurally similar to CP-154,526 [77], have been found to be ineffective in reversing swim stress-induced immobility in the rat [78]. Similar results have also been found using R278995/CRA0450 [75], DMP696, and DMP904 [76]. In mice, antalarmin, DMP696, DMP904, and R121919 were also unable to reverse immobility in the forced swim test [45]. In contrast, the CRF1 receptor antagonist LWH234 reduced immobility, but did not affect stress-induced increases in ACTH [78]. Another study has found that SSR125543A and antalarmin can also attenuate immobility due to swim stress [79].
In the tail suspension test, subchronic dosing of R121919 and DMP696 has been shown to decrease immobility in mice within a similar manner to that of the selective serotonin reuptake inhibitors (SSRI) fluoxetine and paroxetine or the selective norepinephrine reuptake inhibitor reboxetine [45]. In contrast, antalarmin, DMP 904 [45], CP154,526 [80], and R278995/CRA0450 [75] were found to be ineffective in the tail suspension test.
These conflicting findings may be explained, in part, by the baseline behavior of the animals. Similar to nonselective peptide CRF-receptor antagonists, CRF1 receptor antagonists may only be effective in reversing stress-induced changes in behavior. The development of the Flinders sensitive line (FSL) rats, showing higher a baseline level of immobility compared to other rat strains [44], has led to support for this hypothesis. FSL rats receiving chronic treatment with SSR125543A show decreases in immobility in the forced swim test comparable to that observed following chronic injections of fluoxetine and the tricyclic antidepressant desipramine. These drugs did not affect immobility in Flinders resistant line (FRL) rats [81]. Similar results have also been observed in FSL and FRL rats receiving chronic treatment with CP-154,526, imipramine, and the SSRI citalopram [82]. Given these results, it appears that CRF1 receptor antagonists are most effective in animal models of depression when tested in animals that show behaviors indicative of a depressive-like state.
More consistent results have also been seen in animals examined in the chronic mild stress model. BALB/c mice exposed to a series of mild stressors, including restraint, food restriction, and changes in housing, show a deteriorated physical state and decreased body weight. Chronic treatment with antalarmin or fluoxetine reverses the decrease in physical state [83]. Chronic treatment with SSR125543A or fluoxetine can also reverse deterioration of physical state in mice. In addition, both of these drugs attenuate the stress-induced reduction of cell proliferation in the dentate gyrus [84]. Interestingly, fluoxetine treatment led to an increase in cell proliferation in the dentate gyrus in nonstressed mice, whereas SSR125543A had no effects on cell proliferation in these animals [84], further supporting the hypothesis that CRF1 antagonists may only be effective in altering depressive-like behaviors related to stressful conditions.
Recent data also suggest that CRF1 antagonists may be a useful alternative to those resistant to the therapeutic properties of traditional antidepressants [46]. In a series of experiments, mice exposed to chronic mild stress were examined in a number of stress-related behavioral tests following treatment with fluoxetine. Animals were then further divided into responder and nonresponder groups to fluoxetine treatment. Mice that did not respond to fluoxetine showed increases in nest-building behavior, an indication of increased motivation, and decreases in aggression when administered SSR125543A [46]. The findings of this study suggest that while traditional antidepressants may be beneficial to some, CRF1 receptors may provide an alternative target for those who do not benefit from these medications.
44.4 CRF1 Antagonists in Clinical Trials
The earliest clinical trials examining the effectiveness of nonpeptide CRF1 antagonists in the treatment of depression were performed at the Max Planck Institute of Psychiatry in Munich, Germany, examining the CRF1 antagonist NBI-30775. The initial open-label trial designed to assess the safety of NBI-30775 did not show significant alterations in liver enzymes or heart rate in patients with major depression. Moreover, consistent with the hypothesis that behavioral measures of stress occur independently of HPA axis activation, NBI-30775 did not alter the normal neuroendocrine response in response to intravenous administration of CRF. These patients also showed reduced scores in the Hamilton depression (HAM-D) and Hamilton anxiety (HAM-A) scales [85].
A subsequent trial showed that a 30-day treatment of low- or high-dosing regimens of NBI-30775 did not affect various endocrine measures, including HPA axis, hypothalamic-pituitary-gonadal axis and plasma renin activity, and aldosterone, human growth hormone, and insulin-like growth factor vasopressin and thyroid hormone levels. In addition, reports of adverse side effects such as headache, nausea and dizziness that were observed during the trial did not appear to be the direct result of the experimental compound [86]. NBI-30775 has also been shown to normalize electroencephalogram sleep patterns in patients diagnosed with major depression [87]. Finally, subsequent analysis of plasma leptin levels and body weight of the patients examined in the Zobel et al. study [85] showed that neither of these measures was affected by NBI-30775 treatment [88]. Although these data suggested that NBI-30775 is relatively safe and may be clinically useful, an unpublished study in the UK found elevated liver enzyme levels in two patients. This finding led to the termination of the development of NBI-30775, according to a media release from Janssen Pharmaceuticals.
Phase I clinical trials have been conducted to assess the effects of another CRF1 receptor antagonist, NBI-34041, on neuroendocrine function [89]. For 14 days, 24 healthy male subjects received either NBI-34041 or placebo, and the HPA axis response to CRF and psychosocial stress was examined. NBI-34041 reversed the increases in ACTH and cortisol due to intravenous CRF or psychosocial stress but did not impair normal HPA axis function. Although these initial results demonstrate that NBI-34041 is effective in reversing physiological responses to stress without affecting basal hormone levels, further work is clearly needed to assess the safety and efficacy of this drug in the treatment of depression. Currently, there is no available literature concerning clinical trials for NBI-34041 in depression.
CP-316,311 is an additional CRF1 receptor antagonist developed by Pfizer that has undergone clinical testing. Patients with recurring major depression were examined in a 6-week fixed dose double-blind placebo- and sertraline-controlled trial [90]. Although bioavailability data demonstrated adequate serum concentrations of CP-316,311 and urinary cortisol levels showed evidence of CRF1 receptor blockade, patients administered CP-316,311 did not show any significant differences in HAM-D scores compared to those given placebo. Development of CP-316,311 was discontinued due to this negative result.
A multicenter clinical trial has also been conducted to determine the effectiveness of the CRF1 antagonist pexacerfont in the treatment of generalized anxiety disorder [91]. Similar to CP-316,311, patients given pexacerfont had similar HAM-A scores compared to those given placebo, despite achieving efficacious serum concentrations of the drug. Clinical trials are also underway for CRF1 antagonists in the treatment of post-traumatic stress disorder, substance use disorders, and stress-induced food cravings [92–95]. Although there remains interest in the field of developing CRF1 antagonists with therapeutic value for depression and other stress-related psychiatric disorders, none have demonstrated clinical utility to date.
44.5 CRF2 Receptors, Stress-Related Behavior, and Animal Models of Depression
Although the main focus in the development of antidepressants that target the CRF system has been on the CRF1 receptor, CRF2 receptors may present a compelling alternative given the lack of clinical success of CRF1 receptor antagonists. The CRF2 receptor is found mainly in the lateral septum, ventromedial hypothalamus, and choroid plexus [27, 28]. Activation of the CRF2 receptor is most strongly associated with alterations in feeding behavior [30, 96]. Due to conflicting experimental findings, however, there is currently no general consensus regarding the role of CRF2 receptors in the behavioral stress response.
CRF2 receptor knockout mice show an anxiogenic-like phenotype when examined in the elevated plus maze, open-field, and light-dark emergence tests [97, 98]. Central infusion of CRF2 receptor antisense decreases stress-coping behaviors and induces an anxiogenic-like response in rats [99]. Furthermore, rats examined in a model of post-traumatic stress disorder in which they were exposed to predator order over a 10-week period showed chronic upregulation of CRF1 receptors and downregulation of CRF2 receptors in the bed nucleus of the stria terminalis (BNST) [100]. This effect was attenuated by injections of Lentivirus overexpressing CRF2 receptors [100]. As described previously, amidated 38-amino-acid synthetic peptides encoded by the Ucn 2 [32] and Ucn 3 [34] genes have been identified as selective CRF2 receptor agonists. Central injections of Ucn 2 and Ucn 3 lead to suppressed motor activity in the locomotor activity test and an increase in open-arm exploration in the elevated plus maze [40, 41]. Ucn 3 also increases exploratory behavior in mice examined in the open-field test [42].
In contrast, there have also been findings that suggest an anxiogenic role for the CRF2 receptor. Contrary to the findings discussed above, studies have found that central injections of antisauvagine 30 (ASVG-30) produced anxiolytic-like effects in the rat [101] and the mouse [43]. In addition, antisense inhibition of CRF2 receptors in the lateral septum attenuates fear conditioning [102], and Ucn 2 has also been shown to produce a decrease in open-arm exploration in the elevated plus maze in mice [43]. However, further research has yielded additional insight to these conflicting results.
One possible explanation for these seemingly contradictory findings is that the doses used in these experiments may not be selective for the CRF2 receptor. For example, ASVG-30 blocks footshock-induced freezing equally in CRF2 receptor knockout mice and controls [103]. In contrast, the CRF2 receptor antagonist astressin2-B did not affect freezing in these mice [103]. ASVG-30 does have a moderate binding affinity for the CRF1 receptor, whereas astressin2-B is much more selective for the CRF2 receptor [104, 105], and review of the previous literature shows that many of the studies that found anxiolytic-like effects following ASVG-30 administration used doses approximately threefold greater than the IC50 of this compound. Although Ucn 2 has been shown to induce an anxiogenic-like response when tested in the elevated plus maze [43], this ligand does have a low affinity for binding to the CRF1 receptor [32]. In contrast, Ucn 3, which does not induce receptor signaling at the CRF1 receptor, [34], appears to reduce behavioral measures of stress in the elevated plus maze on a more consistent basis [41, 106]. It is possible that the anxiolytic- and anxiogenic-like properties of ASVG-30 and Ucn 3, respectively, may be due to low levels of binding activity at the CRF1 receptor.
Alternatively, these findings may be the result of site-specific actions. Astressin, a nonselective CRF-receptor antagonist, but not antisauvagine-30, impairs CRF-enhanced fear conditioning when injected into the hippocampus. Both of these antagonists, however, attenuate fear conditioning when injected into the lateral septum [107]. Lesions of the lateral septum also produce anxiolytic-like effects in rat models of anxiety [108, 109]. Furthermore, mice exposed to high levels of stress show enhanced anxiety-like behavior when injected with Ucn 2 in the lateral septum [110].
Another possibility is that CRF2 receptors may regulate specific aspects of the stress-coping response, such as sensory information. In C57BL/6J and 129S6/SvEvTac mice, both the CRF1 receptor antagonist NBI-03775 and antisauvagine-30 attenuated enhancement of the acoustic startle response by CRF. In addition, Ucn 2 also increased the acoustic startle response, but with less efficacy than CRF [111]. Further investigation, however, showed that although NBI-30775 and ASVG-30 reduced CRF-induced increases in startle and CRF-induced deficits in prepulse inhibition, CRF2 receptor activation via Ucn 2 and Ucn 3 injections enhanced prepulse inhibition of the acoustic startle response [112]. Also, rats injected with ASVG-30 in the anterolateral BNST show decreases in open-arm exploration similar to those seen in vehicle-injected controls following exposure to water-avoidance stress, whereas injections of the CRF1 receptor antagonist CP376395 into the anterolateral BNST appears to reverse this effect [113]. However, both ASVG-30 and CP376395 decreased the acoustic startle reflex in this same study [113]. These data suggest that although it is possible that CRF2 receptors may have some stress-inducing properties, they appear to be a critical component tempering the stress response.
With regard to depressive-like behaviors specifically, the role of CRF2 receptors remains unclear. When observed in the forced swim test, CRF2 receptor knockout mice display increased depression-like behavior as indicated by increased immobility [47]. In contrast, female, but not male, Ucn 2 knockout mice show less immobility time in the tail suspension and forced swim tests [114]. The difference in behavioral profiles between these strains of mice may be due to the body-wide absence of CRF2 receptors and a different compensation in CRF1 signaling in the CRF2 receptor knockout mice. Ucn 2 knockout mice still have CRF2 receptors available for Ucn 1 and Ucn 3 to bind and in fact show upregulated CRF2 receptor expression in the dorsal raphe [114]. Conflicting results have also been found following administration of CRF2 receptor-specific ligands. Ucn 2 injected into the dorsal raphe has been shown to potentiate learned helplessness behavior in response to inescapable shock, possibly due to interactions with the serotonergic system [115]. However, another study showed that Ucn 2 and Ucn 3 decreased immobility and increased climbing and swimming in mice examined in the forced swim test [48]. Clearly, further work is needed to fully understand the role of CRF2 receptors in depression.
44.6 Conclusions
The data presented are clear evidence that the CRF receptors and CRF-related ligands are important in mediating heightened stress, which in turn may lead to stress-related psychiatric disorders. Although further study is needed, characterization of the CRF1 and CRF2 receptors suggests that these behavioral changes may be the result of an imbalance of CRF1 and CRF2 receptor activity, rather than simply CRF activation. The increases in CRF typically observed during the stress response appear to lead to an overactivation of the CRF1 receptor given the binding profile of this neuropeptide [17]. This hypothesis is further supported by the data indicating an anti-stress function for CRF2 receptor activation [40–42, 100, 112], leading to the hypothesis that the CRF1 receptor is responsible for coordinating the activational components of stress, whereas the CRF2 receptor acts as compensatory coping mechanism to oppose this action.
Currently, the effort with regard to medication development targeting the CRF system has focused on small molecule CRF1 antagonists. Observations of both clinical and preclinical studies suggest that CRF1 receptor antagonists are potentially effective candidate medications in the treatment of stress-related psychiatric illnesses. Patients diagnosed with affective disorders have shown increased CRF levels in cerebrospinal fluid and the hypothalamus, decreased CRF binding in the frontal cortex, and impaired HPA axis function [23, 116–118]. Preclinical evidence demonstrates that reducing brain CRF activity via antagonism of CRF1 receptors can attenuate the behavioral changes observed in animal models of depression.
Although the evidence is compelling, there are still some issues that still need to be considered in the development of CRF1 receptor antagonists. One highly encouraging characteristic of these drugs is their specificity in altering behavior only under stressed conditions, a feature that bodes well for side effect liability. Major side effects were not observed in clinical studies examining NBI-30775 [85]. However, animal studies have suggested that some CRF1 antagonists may have slight sedative effects [75], endocrine disruptive actions [119], and transient abuse-related potential [120]. Another concern is that most structures have poor aqueous solubility and pharmacokinetic properties due to the fact that they are excessively lipophilic. Despite the efforts of the pharmaceutical industry, no CRF1 receptor antagonists have demonstrated clinical utility to date. It is unclear if this lack of success is due to the lack of effectiveness of the compounds themselves, or the multifaceted complexity of the disorders they are designed to target, such as major depression. Nonetheless, the hope exists that further development of CRF1 receptor antagonists and clinical trials that address these shortcomings may one day lead to new pharmacotherapies for the treatment of depression.
An alternative approach to targeting the CRF system in the development of new antidepressant medications may be to increase CRF2 receptor activity. Although there is still no general consensus regarding the role of the CRF2 receptor in the behavioral stress response, much of the data regarding the behavioral profiles of CRF-related neuropeptides and CRF-receptor knockout mice have led to a hypothesis that the CRF-receptor subtypes have an opposing role in the regulation of the stress-related behaviors. For example, CRF and Ucn 1, CRF-related neuropeptides with equal affinity for the CRF1 and CRF2 receptors [29], have been shown to increase overall behavioral activity in rats in a differential manner compared to Ucn 2 and Ucn 3. For example, de Groote et al. [121] found that CRF and Ucn 1 increase measures of exploratory behavior and grooming, whereas Ucn 2 and Ucn 3 only increase exploratory behavior. In addition, chronic exposure to stress leads to opposing profiles of CRF1 and CRF2 receptor expression [100]. In addition, it appears that some of the conflicting evidence may be due to the low-level binding activity at the CRF1 receptor [103] and site-specific actions [107].
CRF2 receptor-specific agonists have also been shown to reverse the effects of CRF. Ucn 2 and Ucn 3 decrease the stimulatory effect of CRF on locomotor activity in a familiar environment, and Ucn 2 injections attenuate CRF-induced decreases in exploratory behavior in the open field [122]. Although the precise mechanism of this action remains unclear, one hypothesis is that activation of the CRF2 receptor may simply lead to a functional antagonism of the behaviors produced by CRF1 receptor activation. Activation of the CRF2 receptor may oppose the stress-inducing actions that result from CRF1 receptor activation. Although this hypothesis must be further tested, the development of small molecule CRF2 receptor agonists may also provide a novel approach for the treatment of depression.
The experiments discussed in this chapter suggest that the underlying mechanisms for increases in depressive behaviors may be the overactivation of CRF1 receptors and possible underactivation of CRF2 receptors. Studies describing the effects of CRF1 receptor antagonists imply that antagonizing the effects associated with activation of this receptor can attenuate the behavioral stress response. Although these compounds have also shown promising results when tested in preclinical models of depression, clinical trials have been unsuccessful thus far. Although data regarding CRF2 receptor regulation of depressive behaviors is less clear, there is evidence that CRF2 receptor ligands act opposing the effects of CRF1 receptor activation. Thus, the development of small molecule CRF2 receptor agonists may also be worth exploring as potential novel antidepressants. In conclusion, the data presented regarding CRF and its receptors and related ligands strongly suggest that targeting the CRF receptors has the potential to generate novel pharmacotherapies for depression.
Abbreviations
- ACTH:
-
Adrenocorticotropic hormone
- ASVG-30:
-
Antisauvagine-30
- BNST:
-
Bed nucleus of the stria terminalis
- CRF:
-
Corticotropin-releasing factor
- FRL:
-
Flinders resistant line
- FSL:
-
Flinders sensitive line
- HAM-A:
-
Hamilton anxiety scale
- HAM-D:
-
Hamilton depression scale
- HPA axis:
-
Hypothalamic-pituitary-adrenal axis
- SSRI:
-
Selective serotonin reuptake inhibitor
- Ucn 1:
-
Urocortin 1
- Ucn 2:
-
Urocortin 2
- Ucn 3:
-
Urocortin 3
References
World Health Organization Depression Fact Sheet. 2012. http://www.who.int/mediacentre/factsheets/fs369/en/. Last accessed 18 Sept 2014.
Selye H. A syndrome produced by diverse noxious agents. Nature. 1936;32:138.
Burchfield SR. The stress response: a new perspective. Psychosom Med. 1979;41:661–72.
Vale W, Spiess J, Rivier C, Rivier J. Characterization of a 41-residue ovine hypothalamic peptide that stimulates secretion of corticotropin and beta-endorphin. Science. 1981;213:1394–7.
Vale W, Rivier C, Brown MR, Spiess J, Koob G, Swanson L, Bilezikjian L, Bloom F, Rivier J. Chemical and biological characterization of corticotropin releasing factor. Recent Prog Horm Res. 1983;39:245–70.
Dunn AJ, Berridge CW. Physiological and behavioral responses to corticotropin-releasing factor administration: is CRF a mediator of anxiety or stress responses? Brain Res Rev. 1990;15:71–100.
Koob GF, Heinrichs SC, Menzaghi F, Pich EM, Britton KT. Corticotropin releasing factor, stress, and behavior. Sem Neurosci. 1994;6:221–9.
Koob GF, Heinrichs SC. A role for corticotropin releasing factor and urocortin in behavioral responses to stressors. Brain Res. 1999;848:141–52.
Irwin M, Vale W, Rivier C. Central corticotropin-releasing factor mediates the suppressive effect of stress on natural killer cytotoxicity. Endocrinology. 1990;126:2837–44.
Taché Y, Gunion M, Stephens R. CRF: central nervous system action to influence gastrointestinal function and role in the gastrointestinal response to stress. In: De Souza EB, Nemeroff CB, eds. Corticotropin-releasing factor: basic and clinical studies of a neuropeptide. Boca Raton, FL: CRC Press. 1989. p. 299–307.
Brown MR. Brain peptide regulation of autonomic nervous and neuroendocrine functions. In: Brown MR, Koob G, Rivier C, eds. Stress Neurobiology and Neuroendocrinology. New York, NY: Marcel Dekker Inc. 1991. p. 193–216.
Fisher LA. Central actions of corticotropin-releasing factor on autonomic nervous activity and cardiovascular functioning. Cibia Found Symp. 1993;discussion:243–57.
Chastrette N, Cespublio R, Jouvet M. Proopiomelancortin(POMC)-derived peptides and sleep in the rat. Part 1. Hypnogenic properties of ACTH derivatives. Neuropeptides. 1990;15:61–74.
Rivier C. Alcohol stimulates ACTH secretion in the rat: mechanisms of action and interactions with other stimuli. Alcohol Clin Exp Res. 1996;20:240–54.
Eaves M, Thatcher-Britton K, Rivier J, Vale W, Koob GF. Effects of corticotropin releasing factor on locomotor activity in hypophysectomized rats. Peptides. 1985;6:923–6.
Britton KT, Lee G, Dana R, Risch SC, Koob GF. Activating and ‘anxiogenic’ effects of corticotropin releasing factor are not inhibited by blockade of the pituitary-adrenal system with dexamethasone. Life Sci. 1986;39:1281–6.
Behan DP, Grigoriadis DE, Lovenberg T, Chalmers D, Heinrichs S, Liaw C, De Souza EB. Neurobiology of corticotropin releasing factor (CRF) receptors and CRF- binding protein: implications for the treatment of CNS disorders. Mol Psychiatry. 1996;1:265–77.
Sutton RE, Koob GF, Le Moal M, Rivier J, Vale W. Corticotropin releasing factor produces behavioural activation in rats. Nature. 1982;297:331–3.
Koob GF, Swerdlow N, Seeligson M, Eaves M, Sutton R, Rivier J, Vale W. Effects of alpha-flupenthixol and naloxone on CRF-induced locomotor activation. Neuroendocrinology. 1984;39:459–64.
Britton KT, Morgan J, Rivier J, Vale W, Koob GF. Chlordiazepoxide attenuates response suppression induced by corticotropin-releasing factor in the conflict test. Psychopharmacology (Berl). 1985;86:170–4.
Swerdlow NR, Geyer MA, Vale WW, Koob GF. Corticotropin-releasing factor potentiates acoustic startle in rats: blockade by chlordiazepoxide. Psychopharmacology (Berl). 1986;88:147–52.
Cole BJ, Koob GF. Propranolol antagonizes the enhanced conditioned fear produced by corticotropin releasing factor. J Pharmacol Exp Ther. 1988;247:902–10.
Nemeroff CB, Widerlov E, Bissette G, Walleus H, Karlsson I, Eklund K, Kilts CD, Loosen PT, Vale W. Elevated concentrations of CSF corticotropin-releasing factor-like immunoreactivity in depressed patients. Science. 1984;226:1342–4.
Valdez GR. Development of CRF1 receptor antagonists as antidepressants and anxiolytics: progress to date. CNS Drugs. 2006;20:887–96.
Zorrilla EP, Koob GF. The therapeutic potential of CRF1 antagonists for anxiety. Expert Opin Investig Drugs. 2004;13:799–828.
Zorrilla EP, Koob GF. Progress in corticotropin-releasing factor-1 antagonist development. Drug Discov Today. 2010;15:371–83.
Chalmers DT, Lovenberg TW, De Souza EB. Localization of novel corticotropin-releasing factor receptor (CRF2) mRNA expression to specific subcortical nuclei in rat brain: comparison with CRF1 receptor mRNA expression. J Neurosci. 1995;15:6340–50.
Perrin M, Donaldson C, Chen R, Blount A, Berggren T, Bilezikjian L, Sawchenko P, Vale W. Identification of a second corticotropin-releasing factor receptor gene and characterization of a cDNA expressed in heart. Proc Natl Acad Sci U S A. 1995;92:2969–73.
Vaughan J, Donaldson C, Bittencourt J, Perrin MH, Lewis K, Sutton S, Chan R, Turnbull AV, Lovejoy D, Rivier C, Rivier J, Sawchenko PE, Vale W. Urocortin, a mammalian neuropeptide related to fish urotensin I and to corticotropin-releasing factor. Nature. 1995;378:287–92.
Spina M, Merlo-Pich E, Chan RK, Basso AM, Rivier J, Vale W, Koob GF. Appetite-suppressing effects of urocortin, a CRF-related neuropeptide. Science. 1996;273:1561–4.
Spina MG, Merlo-Pich E, Akwa Y, Balducci C, Basso AM, Zorrilla EP, Britton KT, Rivier J, Vale WW, Koob GF. Time-dependent induction of anxiogenic-like effects after central infusion of urocortin or corticotropin-releasing factor in the rat. Psychopharmacology (Berl). 2002;160:113–21.
Reyes TM, Lewis K, Perrin MH, Kunitake KS, Vaughan J, Arias CA, Hogenesch JB, Gulyas J, Rivier J, Vale WW, Sawchenko PE. Urocortin II: a member of the corticotropin-releasing factor (CRF) neuropeptide family that is selectively bound by type 2 CRF receptors. Proc Natl Acad Sci U S A. 2001;98:2843–8.
Hsu SY, Hsueh AJ. Human stresscopin and stresscopin-related peptide are selective ligands for the type 2 corticotropin-releasing hormone receptor. Nat Med. 2001;7:605–11.
Lewis K, Li C, Perrin MH, Blount A, Kunitake K, Donaldson C, Vaughan J, Reyes TM, Gulyas J, Fischer W, Bilezikjian L, Rivier J, Sawchenko PE, Vale WW. Identification of urocortin III, an additional member of the corticotropin-releasing factor (CRF) family with high affinity for the CRF2 receptor. Proc Natl Acad Sci U S A. 2001;98:7570–5.
Li C, Vaughan J, Sawchenko PE, Vale WW. Urocortin III-immunoreactive projections in the rat brain: partial overlap with sites of type 2 corticotropin-releasing factor receptor expression. J Neurosci. 2002;22:991–1001.
Möller C, Wiklund L, Sommer W, Thorsell A, Heilig M. Decreased experimental anxiety and voluntary ethanol consumption in rats following central but not basolateral amygdala lesions. Brain Res. 1997;760:94–101.
Gewirtz JC, McNish KA, Davis M. Lesions of the bed nucleus of the stria terminalis block sensitization of the acoustic startle reflex produced by repeated stress, but not fear-potentiated startle. Prog Neuropsychopharmacol Biol Psychiatry. 1998;22:625–48.
Hatalski CG, Guirguis C, Baram TZ. Corticotropin releasing factor mRNA expression in the hypothalamic paraventricular nucleus and the central nucleus of the amygdala is modulated by repeated acute stress in the immature rat. J Neuroendocrinol. 1998;10:663–9.
Van Pett K, Viau V, Bittencourt JC, Chan RK, Li HY, Arias C, Prins GS, Perrin M, Vale W, Sawchenko PE. Distribution of mRNAs encoding CRF receptors in brain and pituitary of rat and mouse. J Comp Neurol. 2000;428:191–212.
Valdez GR, Inoue K, Koob GF, Rivier J, Vale WW, Zorrilla EP. Human urocortin II: mild locomotor suppressive and delayed anxiolytic-like effects of a novel corticotropin-releasing factor related peptide. Brain Res. 2002;943:142–50.
Valdez GR, Zorrilla EP, Rivier J, Vale WW, Koob GF. Locomotor suppressive and anxiolytic-like effects of urocortin 3, a highly selective type 2 corticotropin-releasing factor agonist. Brain Res. 2003;980:206–12.
Venihaki M, Sakihara S, Subramanian S, Dikkes P, Weninger SC, Liapakis G, Graf T, Majzoub JA. Urocortin III, a brain neuropeptide of the corticotropin-releasing hormone family: modulation by stress and attenuation of some anxiety-like behaviours. J Neuroendocrinol. 2004;16:411–22.
Pelleymounter MA, Joppa M, Ling N, Foster AC. Pharmacological evidence supporting a role for central corticotropin-releasing factor(2) receptors in behavioral, but not endocrine, response to environmental stress. J Pharmacol Exp Ther. 2002;302:145–52.
Overstreet DH, Friedman E, Mathe AA, Yadid G. The Flinders Sensitive Line rat: a selectively bred putative animal model of depression. Neurosci Biobehav Rev. 2005;29:739–59.
Nielsen DM, Carey GJ, Gold LH. Antidepressant-like activity of corticotropin-releasing factor type-1 receptor antagonists in mice. Eur J Pharmacol. 2004;499:135–46.
Dournes C, Beeske S, Belzung C, Griebel G. Deep brain stimulation in treatment-resistant depression in mice: comparison with the CRF1 antagonist, SSR125543. Prog Neuropsychopharmacol Biol Psychiatry. 2013;40:213–20.
Bale TL, Vale WW. Increased depression-like behaviors in corticotropin-releasing factor receptor-2-deficient mice: sexually dichotomous responses. J Neurosci. 2003;23:5295–301.
Tanaka M, Telegdy G. Antidepressant-like effects of the CRF family peptides, urocortin 1, urocortin 2 and urocortin 3 in a modified forced swimming test in mice. Brain Res Bull. 2008;75:509–12.
Lenze EJ, Mulsant BH, Mohlman J, Shear MK, Dew MA, Schulz R, Miller MD, Tracey B, Reynolds 3rd CF. Generalized anxiety disorder in late life: lifetime course and comorbidity with major depressive disorder. Am J Geriatr Psychiatry. 2005;13:77–80.
Lenze EJ, Mulsant BH, Shear MK, Alexopoulos GS, Frank E, Reynolds 3rd CF. Comorbidity of depression and anxiety disorders in later life. Depress Anxiety. 2001;14:86–93.
Lenze EJ, Mulsant BH, Shear MK, Schulberg HC, Dew MA, Begley AE, Pollock BG, Reynolds 3rd CF. Comorbid anxiety disorders in depressed elderly patients. Am J Psychiatry. 2000;157:722–8.
Borelli KG, Albrechet-Souza L, Fedoce AG, Fabri DS, Resstel LB, Brandao ML. Conditioned fear is modulated by CRF mechanisms in the periaqueductal gray columns. Horm Behav. 2013;63:791–9.
Krahn DD, Gosnell BA, Grace M, Levine AS. CRF antagonist partially reverses CRF- and stress-induced effects on feeding. Brain Res Bull. 1986;17:285–90.
Arase K, York DA, Shimizu H, Shargill N, Bray GA. Effects of corticotropin-releasing factor on food intake and brown adipose tissue thermogenesis in rats. Am J Physiol. 1988;255:E255–9.
Stenzel-Poore MP, Heinrichs SC, Rivest S, Koob GF, Vale WW. Overproduction of corticotropin-releasing factor in transgenic mice: a genetic model of anxiogenic behavior. J Neurosci. 1994;14:2579–84.
Flandreau EI, Bourke CH, Ressler KJ, Vale WW, Nemeroff CB, Owens MJ. Escitalopram alters gene expression and HPA axis reactivity in rats following chronic overexpression of corticotropin-releasing factor from the central amygdala. Psychoneuroendocrinology. 2013;38:1349–61.
Swerdlow NR, Britton KT, Koob GF. Potentiation of acoustic startle by corticotropin-releasing factor (CRF) and by fear are both reversed by alpha-helical CRF (9-41). Neuropsychopharmacology. 1989;2:285–92.
Cruz AP, Frei F, Graeff FG. Ethopharmacological analysis of rat behavior on the elevated plus-maze. Pharmacol Biochem Behav. 1994;49:171–6.
Menzaghi F, Howard RL, Heinrichs SC, Vale W, Rivier J, Koob GF. Characterization of a novel and potent corticotropin-releasing factor antagonist in rats. J Pharmacol Exp Ther. 1994;269:564–72.
Spina MG, Basso AM, Zorrilla EP, Heyser CJ, Rivier J, Vale W, Merlo-Pich E, Koob GF. Behavioral effects of central administration of the novel CRF antagonist astressin in rats. Neuropsychopharmacology. 2000;22:230–9.
Heinrichs SC, Menzaghi F, Pich EM, Baldwin HA, Rassnick S, Britton KT, Koob GF. Anti-stress action of a corticotropin-releasing factor antagonist on behavioral reactivity to stressors of varying type and intensity. Neuropsychopharmacology. 1994;11:179–86.
Macey DJ, Koob GF, Markou A. CRF and urocortin decreased brain stimulation reward in the rat: reversal by a CRF receptor antagonist. Brain Res. 2000;866:82–91.
Swiergiel AH, Zhou Y, Dunn AJ. Effects of chronic footshock, restraint and corticotropin-releasing factor on freezing, ultrasonic vocalization and forced swim behavior in rats. Behav Brain Res. 2007;183:178–87.
Dunn AJ, Swiergiel AH. Effects of acute and chronic stressors and CRF in rat and mouse tests for depression. Ann N Y Acad Sci. 2008;1148:118–26.
Porsolt RD, Le Pichon M, Jalfre M. Depression: a new animal model sensitive to antidepressant treatments. Nature. 1977;266:730–2.
Smith GW, Aubry JM, Dellu F, Contarino A, Bilezikjian LM, Gold LH, Chen R, Marchuk Y, Hauser C, Bentley CA, Sawchenko PE, Koob GF, Vale W, Lee KF. Corticotropin releasing factor receptor 1-deficient mice display decreased anxiety, impaired stress response, and aberrant neuroendocrine development. Neuron. 1998;20:1093–102.
Timpl P, Spanagel R, Sillaber I, Kresse A, Reul JM, Stalla GK, Blanquet V, Steckler T, Holsboer F, Wurst W. Impaired stress response and reduced anxiety in mice lacking a functional corticotropin-releasing hormone receptor. Nat Genet. 1998;19:162–6.
Contarino A, Dellu F, Koob GF, Smith GW, Lee KF, Vale W, Gold LH. Reduced anxiety-like and cognitive performance in mice lacking the corticotropin-releasing factor receptor 1. Brain Res. 1999;835:1–9.
Contarino A, Dellu F, Koob GF, Smith GW, Lee KF, Vale WW, Gold LH. Dissociation of locomotor activation and suppression of food intake induced by CRF in CRFR1-deficient mice. Endocrinology. 2000;141:2698–702.
Schulz DW, Mansbach RS, Sprouse J, Braselton JP, Collins J, Corman M, Dunaiskis A, Faraci S, Schmidt AW, Seeger T, Seymour P, Tingley 3rd FD, Winston EN, Chen YL, Heym J. CP-154,526: a potent and selective nonpeptide antagonist of corticotropin releasing factor receptors. Proc Natl Acad Sci U S A. 1996;93:10477–82.
Mansbach RS, Brooks EN, Chen YL. Antidepressant-like effects of CP-154,526, a selective CRF1 receptor antagonist. Eur J Pharmacol. 1997;323:21–6.
Maier SF, Seligman MEP. Learned helplessness: theory and evidence. J Exp Psychol Gen. 1976;105:3–46.
Takamori K, Kawashima N, Chaki S, Nakazato A, Kameo K. Involvement of corticotropin-releasing factor subtype 1 receptor in the acquisition phase of learned helplessness in rats. Life Sci. 2001;69:1241–8.
Takamori K, Kawashima N, Chaki S, Nakazato A, Kameo K. Involvement of the hypothalamus-pituitary-adrenal axis in antidepressant activity of corticotropin-releasing factor subtype 1 receptor antagonists in the rat learned helplessness test. Pharmacol Biochem Behav. 2001;69:445–9.
Chaki S, Nakazato A, Kennis L, Nakamura M, Mackie C, Sugiura M, Vinken P, Ashton D, Langlois X, Steckler T. Anxiolytic- and antidepressant-like profile of a new CRF1 receptor antagonist, R278995/CRA0450. Eur J Pharmacol. 2004;485:145–58.
Li YW, Fitzgerald L, Wong H, Lelas S, Zhang G, Lindner MD, Wallace T, McElroy J, Lodge NJ, Gilligan P, Zaczek R. The pharmacology of DMP696 and DMP904, non-peptidergic CRF1 receptor antagonists. CNS Drug Rev. 2005;11:21–52.
Webster EL, Lewis DB, Torpy DJ, Zachman EK, Rice KC, Chrousos GP. In vivo and in vitro characterization of antalarmin, a nonpeptide corticotropin-releasing hormone (CRH) receptor antagonist: suppression of pituitary ACTH release and peripheral inflammation. Endocrinology. 1996;137:5747–50.
Jutkiewicz EM, Wood SK, Houshyar H, Hsin LW, Rice KC, Woods JH. The effects of CRF antagonists, antalarmin, CP154,526, LWH234, and R121919, in the forced swim test and on swim-induced increases in adrenocorticotropin in rats. Psychopharmacology (Berl). 2005;180:215–23.
Griebel G, Simiand J, Steinberg R, Jung M, Gully D, Roger P, Geslin M, Scatton B, Maffrand JP, Soubrie P. 4-(2-Chloro-4-methoxy-5-methylphenyl)-N-[(1S)-2-cyclopropyl-1-(3-fluoro-4- methylphenyl)ethyl]5-methyl-N-(2-propynyl)-1, 3-thiazol-2-amine hydrochloride (SSR125543A), a potent and selective corticotrophin-releasing factor(1) receptor antagonist. II. Characterization in rodent models of stress-related disorders. J Pharmacol Exp Ther. 2002;301:333–45.
Yamano M, Yuki H, Yasuda S, Miyata K. Corticotropin-releasing hormone receptors mediate consensus interferon-alpha YM643-induced depression-like behavior in mice. J Pharmacol Exp Ther. 2000;292:181–7.
Overstreet DH, Griebel G. Antidepressant-like effects of CRF1 receptor antagonist SSR125543 in an animal model of depression. Eur J Pharmacol. 2004;497:49–53.
Overstreet DH, Keeney A, Hogg S. Antidepressant effects of citalopram and CRF receptor antagonist CP-154,526 in a rat model of depression. Eur J Pharmacol. 2004;492:195–201.
Ducottet C, Griebel G, Belzung C. Effects of the selective nonpeptide corticotropin-releasing factor receptor 1 antagonist antalarmin in the chronic mild stress model of depression in mice. Prog Neuropsychopharmacol Biol Psychiatry. 2003;27:625–31.
Alonso R, Griebel G, Pavone G, Stemmelin J, Le Fur G, Soubrie P. Blockade of CRF(1) or V(1b) receptors reverses stress-induced suppression of neurogenesis in a mouse model of depression. Mol Psychiatry. 2004;9:278–86. 224.
Zobel AW, Nickel T, Kunzel HE, Ackl N, Sonntag A, Ising M, Holsboer F. Effects of the high-affinity corticotropin-releasing hormone receptor 1 antagonist R121919 in major depression: the first 20 patients treated. J Psychiatr Res. 2000;34:171–81.
Kunzel HE, Zobel AW, Nickel T, Ackl N, Uhr M, Sonntag A, Ising M, Holsboer F. Treatment of depression with the CRH-1-receptor antagonist R121919: endocrine changes and side effects. J Psychiatr Res. 2003;37:525–33.
Held K, Kunzel H, Ising M, Schmid DA, Zobel A, Murck H, Holsboer F, Steiger A. Treatment with the CRH1-receptor-antagonist R121919 improves sleep-EEG in patients with depression. J Psychiatr Res. 2004;38:129–36.
Kunzel HE, Ising M, Zobel AW, Nickel T, Ackl N, Sonntag A, Holsboer F, Uhr M. Treatment with a CRH-1-receptor antagonist (R121919) does not affect weight or plasma leptin concentration in patients with major depression. J Psychiatr Res. 2005;39:173–7.
Ising M, Zimmermann US, Kunzel HE, Uhr M, Foster AC, Learned-Coughlin SM, Holsboer F, Grigoriadis DE. High-affinity CRF1 receptor antagonist NBI-34041: preclinical and clinical data suggest safety and efficacy in attenuating elevated stress response. Neuropsychopharmacology. 2007;32:1941–9.
Binneman B, Feltner D, Kolluri S, Shi Y, Qiu R, Stiger T. A 6-week randomized, placebo-controlled trial of CP-316,311 (a selective CRH1 antagonist) in the treatment of major depression. Am J Psychiatry. 2008;165:617–20.
Coric V, Feldman HH, Oren DA, Shekhar A, Pultz J, Dockens RC, Wu X, Gentile KA, Huang SP, Emison E, Delmonte T, D’Souza BB, Zimbroff DL, Grebb JA, Goddard AW, Stock EG. Multicenter, randomized, double-blind, active comparator and placebo-controlled trial of a corticotropin-releasing factor receptor-1 antagonist in generalized anxiety disorder. Depress Anxiety. 2010;27:417–25.
Effects of corticotropin-releasing hormone receptor 1 (CRH1) antagonism on stress-induced craving in alcoholic women with high anxiety. 2014. http://clinicaltrials.gov/ct2/show/NCT01187511. Last accessed 18 Sept 2014.
Pexacerfont to reduce stress-induced tobacco craving. 2014. http://clinicaltrials.gov/ct2/show/NCT01557556. Last accessed 18 Sept 2014.
Corticotropin-releasing hormone receptor 1 (CRH1) antagonism in anxious alcoholics. 2014. http://clinicaltrials.gov/ct2/show/NCT01227980. Last accessed 18 Sept 2014.
Pexacerfont for stress-induced food craving. 2013. http://clinicaltrials.gov/ct2/show/NCT01656577. Last accessed 18 Sept 2014.
Pelleymounter MA, Joppa M, Carmouche M, Cullen MJ, Brown B, Murphy B, Grigoriadis DE, Ling N, Foster AC. Role of corticotropin-releasing factor (CRF) receptors in the anorexic syndrome induced by CRF. J Pharmacol Exp Ther. 2000;293:799–806.
Bale TL, Contarino A, Smith GW, Chan R, Gold LH, Sawchenko PE, Koob GF, Vale WW, Lee KF. Mice deficient for corticotropin-releasing hormone receptor-2 display anxiety-like behaviour and are hypersensitive to stress. Nat Genet. 2000;24:410–4.
Kishimoto T, Radulovic J, Radulovic M, Lin CR, Schrick C, Hooshmand F, Hermanson O, Rosenfeld MG, Spiess J. Deletion of crhr2 reveals an anxiolytic role for corticotropin- releasing hormone receptor-2. Nat Genet. 2000;24:415–9.
Isogawa K, Akiyoshi J, Tsutsumi T, Kodama K, Horinouti Y, Nagayama H. Anxiogenic-like effect of corticotropin-releasing factor receptor 2 antisense oligonucleotides infused into rat brain. J Psychopharmacol. 2003;17:409–13.
Elharrar E, Warhaftig G, Issler O, Sztainberg Y, Dikshtein Y, Zahut R, Redlus L, Chen A, Yadid G. Overexpression of corticotropin-releasing factor receptor type 2 in the bed nucleus of stria terminalis improves posttraumatic stress disorder-like symptoms in a model of incubation of fear. Biol Psychiatry. 2013;74:827–36.
Takahashi LK, Ho SP, Livanov V, Graciani N, Arneric SP. Antagonism of CRF(2) receptors produces anxiolytic behavior in animal models of anxiety. Brain Res. 2001;902:135–42.
Ho SP, Takahashi LK, Livanov V, Spencer K, Lesher T, Maciag C, Smith MA, Rohrbach KW, Hartig PR, Arneric SP. Attenuation of fear conditioning by antisense inhibition of brain corticotropin releasing factor-2 receptor. Brain Res Mol Brain Res. 2001;89:29–40.
Zorrilla EP, Roberts AJ, Rivier JE, Koob GF. Anxiolytic-like effects of antisauvagine-30 in mice are not mediated by CRF2 receptors. PLoS One. 2013;8:e63942.
Hoare SR, Sullivan SK, Fan J, Khongsaly K, Grigoriadis DE. Peptide ligand binding properties of the corticotropin-releasing factor (CRF) type 2 receptor: pharmacology of endogenously expressed receptors, G-protein-coupling sensitivity and determinants of CRF2 receptor selectivity. Peptides. 2005;26:457–70.
Hoare SR, Sullivan SK, Schwarz DA, Ling N, Vale WW, Crowe PD, Grigoriadis DE. Ligand affinity for amino-terminal and juxtamembrane domains of the corticotropin releasing factor type I receptor: regulation by G-protein and nonpeptide antagonists. Biochemistry. 2004;43:3996–4011.
Valdez GR, Sabino V, Koob GF. Increased anxiety-like behavior and ethanol self-administration in dependent rats: reversal via corticotropin-releasing factor-2 receptor activation. Alcohol Clin Exp Res. 2004;28:865–72.
Radulovic J, Ruhmann A, Liepold T, Spiess J. Modulation of learning and anxiety by corticotropin-releasing factor (CRF) and stress: differential roles of CRF receptors 1 and 2. J Neurosci. 1999;19:5016–25.
Menard J, Treit D. Lateral and medial septal lesions reduce anxiety in the plus-maze and probe-burying tests. Physiol Behav. 1996;60:845–53.
Yadin E, Thomas E, Grishkat HL, Strickland CE. The role of the lateral septum in anxiolysis. Physiol Behav. 1993;53:1077–83.
Henry B, Vale W, Markou A. The effect of lateral septum corticotropin-releasing factor receptor 2 activation on anxiety is modulated by stress. J Neurosci. 2006;26:9142–52.
Risbrough VB, Hauger RL, Pelleymounter MA, Geyer MA. Role of corticotropin releasing factor (CRF) receptors 1 and 2 in CRF-potentiated acoustic startle in mice. Psychopharmacology (Berl). 2003;170:178–87.
Risbrough VB, Hauger RL, Roberts AL, Vale WW, Geyer MA. Corticotropin-releasing factor receptors CRF1 and CRF2 exert both additive and opposing influences on defensive startle behavior. J Neurosci. 2004;24:6545–52.
Tran L, Schulkin J, Greenwood-Van Meerveld B. Importance of CRF receptor-mediated mechanisms of the bed nucleus of the stria terminalis in the processing of anxiety and pain. Neuropsychopharmacology. 2014;39:2633–45.
Chen A, Zorrilla E, Smith S, Rousso D, Levy C, Vaughan J, Donaldson C, Roberts A, Lee KF, Vale W. Urocortin 2-deficient mice exhibit gender-specific alterations in circadian hypothalamus-pituitary-adrenal axis and depressive-like behavior. J Neurosci. 2006;26:5500–10.
Hammack SE, Schmid MJ, LoPresti ML, Der-Avakian A, Pellymounter MA, Foster AC, Watkins LR, Maier SF. Corticotropin releasing hormone type 2 receptors in the dorsal raphe nucleus mediate the behavioral consequences of uncontrollable stress. J Neurosci. 2003;23:1019–25.
Galard R, Catalan R, Castellanos JM, Gallart JM. Plasma corticotropin-releasing factor in depressed patients before and after the dexamethasone suppression test. Biol Psychiatry. 2002;51:463–8.
Nemeroff CB, Owens MJ, Bissette G, Andorn AC, Stanley M. Reduced corticotropin releasing factor binding sites in the frontal cortex of suicide victims. Arch Gen Psychiatry. 1988;45:577–9.
Raadsheer FC, Hoogendijk WJ, Stam FC, Tilders FJ, Swaab DF. Increased numbers of corticotropin-releasing hormone expressing neurons in the hypothalamic paraventricular nucleus of depressed patients. Neuroendocrinology. 1994;60:436–44.
Bornstein SR, Webster EL, Torpy DJ, Richman SJ, Mitsiades N, Igel M, Lewis DB, Rice KC, Joost HG, Tsokos M, Chrousos GP. Chronic effects of a nonpeptide corticotropin-releasing hormone type I receptor antagonist on pituitary-adrenal function, body weight, and metabolic regulation. Endocrinology. 1998;139:1546–55.
Broadbear JH, Winger G, Rice KC, Woods JH. Antalarmin, a putative CRH-RI antagonist, has transient reinforcing effects in rhesus monkeys. Psychopharmacology (Berl). 2002;164:268–76.
de Groote L, Penalva RG, Flachskamm C, Reul JM, Linthorst AC. Differential monoaminergic, neuroendocrine and behavioural responses after central administration of corticotropin-releasing factor receptor type 1 and type 2 agonists. J Neurochem. 2005;94:45–56.
Ohata H, Shibasaki T. Effects of urocortin 2 and 3 on motor activity and food intake in rats. Peptides. 2004;25:1703–9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer India
About this chapter
Cite this chapter
Valdez, G.R. (2016). Corticotropin-Releasing Factor Receptors as a Potential Target in the Developments of Antidepressant Drugs. In: López-Muñoz, F., Srinivasan, V., de Berardis, D., Álamo, C., Kato, T. (eds) Melatonin, Neuroprotective Agents and Antidepressant Therapy. Springer, New Delhi. https://doi.org/10.1007/978-81-322-2803-5_44
Download citation
DOI: https://doi.org/10.1007/978-81-322-2803-5_44
Published:
Publisher Name: Springer, New Delhi
Print ISBN: 978-81-322-2801-1
Online ISBN: 978-81-322-2803-5
eBook Packages: MedicineMedicine (R0)