Abstract
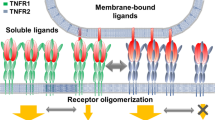
Tumor necrosis factor (TNF; tumor necrosis factor ligand superfamily member 2) induces a variety of intracellular signaling pathways including NF-κB activation through the binding to its two receptors, the TNF receptor superfamily member 1A (TNFR1; CD120A) and TNF receptor superfamily member 1B (TNFR2; CD120B). TNF has a crucial role in host defense against infectious diseases and carcinogenesis, but elevated concentrations of TNF cause various autoimmune diseases such as rheumatoid arthritis, Crohn’s disease, and ulcerative colitis. For clinical therapy trials, receptor-selective drugs are preferred because the blocking of both TNFRs can cause serious side effects. Crystal structure of the TNF and TNFR2 complex (TNF–TNFR2) was determined at 3.0 Å resolution. Although TNF trimer binds to three TNFR2 molecules similar to the known structure of the lymphotoxin-α (LT-α)–TNFR1 complex, structural comparison between TNFR2 and TNFR1 clearly showed several differences on the ligand-binding interfaces of the two receptors that may be useful information for the design of receptor-selective drugs. Furthermore, it was observed that the TNF–TNFR2 complexes form aggregates on the cell surface, suggesting two-dimensional network models for the signal initiation through TNFR2. Here we describe structural features of the TNF and TNFR superfamilies and the structural basis of the signal initiation triggered by the TNF–TNFR2 complex.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Tumor necrosis factor
- Tumor necrosis factor receptor
- Ligand–receptor complex
- Signal initiation
- Structural biology
1 Introduction
TNF is a well-known inflammatory cytokine that has important roles for various functions in immunity, inflammation, cell proliferation, differentiation, and apoptosis; therefore, immunomodulation by blockage of TNF can be a therapeutic approach. Anti-TNF therapies are approved for autoimmune diseases such as rheumatoid arthritis (Palladino et al. 2003), whereas TNF itself is also approved in isolated limb perfusion against some kinds of cancers including soft tissue sarcoma and metastatic melanoma because of its strong anti-tumor effect (van Horssen et al. 2006). These roles are sometimes called “double-edged swords” (Aggarwal 2003); therefore, understanding of TNF–TNFR function is still the focus of immunological research.
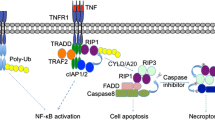
TNF is a trimeric protein and can interact with two different receptors, TNFR1 and TNFR2. TNFR1 is expressed on various types of cells, whereas the expression of TNFR2 is restricted to certain T cells (Ware et al. 1991). The signaling pathway of TNFR1 has two different forms: one leads to pro-survival signals such as activation of nuclear factor-kappa B (NF-κB) following the phosphorylation and degradation of inhibitor of kappa B (IκB), the other initiates a caspase cascade for apoptosis via cleaving caspase-8 (Micheau and Tschopp 2003). These two distinct pro-survival and apoptotic mechanisms are caused by forming two different signaling complexes (Oeckinghaus et al. 2011), and they are thought to be regulated by cell type or expression of intracellular adaptor molecules (Pimentel-Muinos and Seed 1999). The signaling pathway of TNFR2 is crosstalked with that of TNFR1 in the activation of NF-κB (Faustman and Davis 2010) and is important for T-cell survival.
Both TNF and anti-TNF agents can be therapies for different diseases. However, direct use could bring serious side effects because the TNF–TNFR signaling is crosstalked and their functions are complicated. In fact, systemic use of TNF promotes strong liver failure in human (Roberts et al. 2011), and anti-TNF therapy has a risk of bacterial or viral infection (Gomez-Reino et al. 2003; Lubel et al. 2007). On the basis of these studies, receptor-selective TNFR agonists or antagonists appear to be promising for both basic research and therapeutic use to develop a novel drug minimizing the side effects of current therapy. Until now, we successfully created several TNFR-selective agonistic or antagonistic mutants with phage display techniques (Abe et al. 2011; Mukai et al. 2009a, c; Shibata et al. 2004, 2008; Yamamoto et al. 2003). For example, TNFR1-selective antagonistic TNF mutant shows a strong antiinflammatory effect without loss of host-defense function against viral infection in mouse models (Shibata et al. 2009), suggesting that a TNFR1-selective blocker might be useful to overcome the problem of current anti-TNF therapy.
Structural studies of TNF and TNFR have greatly contributed to the understanding of the ligand–receptor binding and signal initiation mechanisms. The first crystal structure of TNF was reported in 1989 (Eck and Sprang 1989; Jones et al. 1989). TNF shows a β-jellyroll fold and forms a compact homotrimer shaped like a truncated pyramid. Following these reports, the structure of LT-α (also referred to as TNF-β) was determined (Eck et al. 1992). Overall trimeric structures of TNF and LT-α are very similar, excepting insertions or deletions of loop regions, and this feature is generally conserved among the structures of the TNF superfamily members, such as CD40 ligand, TNF-related apoptosis-inducing ligand (TRAIL), and TNF-like ligand 1A (TL1A or VEGI), which were published later (Karpusas et al. 1995; Jin et al. 2007; Mongkolsapaya et al. 1999; Hymowitz et al. 1999; Cha et al. 2000). In 1993, crystal structure of the LT-α–TNFR1 complex was determined (Banner et al. 1993). In the complex structure, three TNFR1 molecules symmetrically bind to the central LT-α trimer to form a 3:3 complex, revealing not only the recognition scheme between LT-α and TNFR1, but also the signal initiation triggered by the assembly of TNFR1s. However, to elucidate the receptor specificity of TNF, structural information of another TNF receptor, TNFR2, was also required. To date, we have solved crystal structures of receptor-selective TNF mutants and the TNF–TNFR2 complex, and investigated the receptor binding of TNF and the machinery of signal initiation (Shibata et al. 2008; Mukai et al. 2009a, b, c, 2010). Here, we summarize structural features of the TNF and TNFR superfamilies and describe our work on the TNF–TNFR2 complex.
2 Structure of TNF
Human TNF, which consists of 157 amino acids, is secreted as a stable homotrimer. TNF monomer has ten antiparallel β-strands and exhibits a β-jellyroll fold with two β-sheets (inner and outer sheets) (Fig. 9.1a) (Eck and Sprang 1989; Jones et al. 1989). The inner sheet is composed of five β-strands, A, A′, C, F, and H; the outer sheet is five strands, B, B′, D, E, and G. A disulfide bond is formed between Cys69 and Cys101, connecting the loop regions between strands C and D and between strands E and F. TNF monomers assemble into a trimer with a noncrystallographic threefold symmetry by edge-to-face interactions of β-sheets (Fig. 9.1b, c). The edge-to-face interaction is formed between adjacent molecules. The interaction is essentially van der Waals contacts between the side chains including Tyr59, Tyr119, and Tyr151 on the face of the inner sheet in a monomer (molecule B) and the main chain of the edge of β-strands in the adjacent monomer (molecule A) (Fig. 9.1c). In addition, a hydrophobic core is formed by the side chains of Leu, Ile, and Val residues between the dimer in the top region. As a result of these interactions in each dimer, TNF forms a stable trimer, which buries approximately 7000 Å2 of accessible surface area.
Structures of the tumor necrosis factor (TNF) superfamily. a Overall structure of the TNF monomer (PDB ID: 1TNF). β-Strands A, A′, C, F, and H form the inner sheet; β-strands B, B′, D, E, and G form the outer sheet. A disulfide bond between Cy69 and Cys101 is shown in the ball-and-stick representation. b Overall structure of the TNF trimer (molecules A, B, C). c Interactions between molecules A and B. Each monomer is shown in white and gray, respectively. The molecular surface of each monomer is shown as transparent. d Overall structure of the OX40L trimer (PDB ID: 2HEV). The OX40L trimer was generated by applying threefold crystallographic symmetry. All molecular graphics were prepared using PyMOL (DeLano 2010)
Although the β-jellyroll fold and the overall trimeric structure are generally conserved among the TNF superfamily members (Magis et al. 2012), there seems to be diversity in the trimer formation. For example, OX40L (also known as CD134 antigen) forms a relatively expanded homotrimer compared to TNF (Fig. 9.1d) (Compaan and Hymowitz 2006). In the crystal structure of OX40L, monomers are oriented and splayed out at an angle about 45° with respect to the threefold axis, whereas in most TNF superfamily members, the angle is about 25°–30°. As a result, the OX40L trimer shows much smaller binding interface (~2600 Å2 of accessible surface area buried upon trimer formation) than other TNF superfamily members. This structural difference in trimer assembly is the result of the low sequence identity between OX40L and the TNF superfamily members. The crystal structure of glucocorticoid-induced TNF receptor ligand (GITRL), which shares low sequence identity with the TNF superfamily members, also shows comparable assembly to OX40L (Chattopadhyay et al. 2007).
3 Overall Structure of the TNF–TNFR2 Complex
In 2010, we reported the crystal structure of the TNF–TNFR2 complex at 3.0 Å resolution (Fig. 9.2a) (Mukai et al. 2010). The overall structure of the TNF–TNFR2 is similar to those of other TNF superfamily members including LT-α–TNFR1 and TRAIL–DR5 (Banner et al. 1993; Mongkolsapaya et al. 1999; Hymowitz et al. 1999; Cha et al. 2000). The structure of TNFR2 is composed of four cysteine-rich domains (CRDs), termed CRD1 through CRD4, from its N-terminus to C-terminus (Fig. 9.2b, c). The CRD, which is conserved among most members of the TNFR superfamily, generally contains three disulfide bonds (Naismith and Sprang 1998; Bodmer et al. 2002). Among all the four CRDs of TNFR2, CRD2 and CRD3 bind to the shallow groove between the TNF dimer (~1400 Å2 of surface area buried in the binding interface). This binding manner is very similar to that observed in the LT-α–TNFR1 complex (~1200 Å2 of surface area buried). CRD1, also termed the pre-ligand-binding assembly domain (PLAD), is shown to be necessary for self-assembly of TNFR on the cell surface independent of ligand binding (Chan et al. 2000), but in this crystal structure, there is no interaction between the CRD1s.
Structures of TNF and TNF receptors (TNFR). a Overall structure of the TNF–TNFR2 complex (PDB ID: 3ALQ). The TNF trimer and TNFR2 are shown in white and black, respectively. TNF and TNFR2 form a 3:3 complex. b Structures of TNFR2 (left) and TNFR1 (right) (PDB ID: 1EXT). TNFRs are composed of four CRDs (CRD1–CRD4). c Amino acid sequence alignment of TNFR1 and TNFR2. Cys residues are underlined and disulfide bonds are indicated by lines. Regions A and B are shaded. Fig. 9.2 (continued) A1, A2, B1, B2, and C2 represent the types of the module structures. d Structure of regions A and B of TNFR2. e Structure of regions A and B of TNFR1 (PDB ID: 1TNR). The side chain of Glu109 was missing in the coordinates of 1TNR and was modeled using PyMOL. d, e Drawn from the point of view of the binding interface between TNF and TNFR. (Modified from Y. Mukai et al. Science Signaling 3(148): ra83)
In CRD4 of TNFR2, the M174R mutation, which is known as M196R polymorphism, is associated with the presence of soluble TNFR2 and autoimmune diseases (Morita et al. 2001; Oregon-Romero et al. 2006). In the crystal packing of the TNF–TNFR2 complex, one TNFR2 molecule interacts with an adjacent TNFR2 molecule, but this dimer formation is in a head-to-tail manner. Thus, this dimer might form only under the specific condition in which TNFR2 is soluble. Met174 is located on this dimer interface, indicating that the mutation of Met174 may affect the assembly of soluble TNFR2.
4 Comparison of the Structures of TNFR2 and TNFR1
Extracellular domains of TNFR2 and TNFR1 have a similar structure composed of CRD1-4 (Fig. 9.2b). The CRD has two modules and each module is classified according to a type (A-C, N, and X) and a numeral indicating the number of disulfide bonds in the module (Fig. 9.2c) (Naismith and Sprang 1998; Bodmer et al. 2002). In the TNFR superfamily, the CRD domain generally consists of an A1-B2 or A2-B1 module. CRD1 and CRD2 of both receptors have the A1-B2 modules and are topologically similar. However, there is a local structural difference in CRD2 for ligand binding (region A in Fig. 9.2c). The region A of TNFR2, a loop region, is apart from the molecular surface of TNF, whereas that of TNFR1 is two amino acids longer and seems to interact with TNF (Fig. 9.2d, e; discussed later).
The topologies and structures of CRD3 and CRD4 of both receptors are totally different (CRD3 of TNFR2, the A2-B1 module; CRD3 of TNFR1, the A1-B2 module; CRD4 of TNFR2, the A1-B1 module; CRD4 of TNFR1, the A1-C2 module). Among these modules, the TNF–TNFR2 complex showed the first structure of the A2 module in the TNFR superfamily. The A2 module of CRD3 of TNFR2 has an additional disulfide bond (between Cys104 and Cys112) compared to the A1 module of CRD3 of TNFR1 (Fig. 9.2c). A loop region (around region B in Fig. 9.2c) in TNFR2 is deflected by this disulfide bond and projects to the binding surface of TNF (Fig. 9.2d; discussed later). On the other hand, around region B of TNFR1, there is a cleft between CRD2 and CRD3 (Fig. 9.2e).
To understand the ligand binding specificities of TNFR2 and TNFR1, we generated a model of the TNF–TNFR1 complex by superimposing the coordinates of LT-α in the LT-α–TNFR1 complex (PDB ID: 1TNR) (Banner et al. 1993) onto those of TNF in the TNF–TNFR2 complex (PDB ID: 3ALQ) (Mukai et al. 2010). The structures of TNF and LT-α are very similar with r.m.s.d. of 0.9 Å for the corresponding 387 Cα atoms except insertions or deletions (the sequence identity is 33%). TNF binds to both TNFR2 and TNFR1 through the same interface on itself, but there are electrostatic and structural differences between the TNF-binding interfaces on TNFRs. The interface is mainly separated into two regions, termed regions C and D (Fig. 9.3a, b).
a Electrostatic surface potentials of TNFR2 (left) and TNFR1 (right). Blue, positive charge; red, negative charge (contoured at ±7.0 kT). Each electrostatic surface potential was calculated with CCP4 mg (McNicholas et al. 2011). Regions C and D are circled. b Location of regions C and D in the TNF–TNFR2 complex. Regions C and D indicated by squares. c, d Interactions between TNF and TNFR2 around regions C and D, respectively. e, f Interactions between TNF and TNFR1 around regions C and D, respectively (modeled). A model of the TNF–TNFR1 complex was generated by superposing the LT-α portion in the LT-α–TNFR1 complex onto the TNF portion in the TNF–TNFR2 complex. Green TNF, blue TNFR2, pink TNFR1
Region C in TNFR2 has clustered acidic amino acid residues (Asp54, Glu57, and Glu70) and is more negatively charged than that of TNFR1 (Fig. 9.3a). Although a cobalt ion (Co2+) from the crystallization reagent binds to the acidic cluster, Arg31 of TNF seems to interact with Asp54, Glu57, and Glu70 in region C of TNFR2 under the condition without metal ions (Fig. 9.3a, c). In the model of the TNF–TNFR1 complex, on the other hand, electrostatic interactions between Arg31 of TNF and region C of TNFR1 might be weaker than those in TNF–TNFR2 because TNFR1 has basic residues such as Arg53 and His69 (structurally corresponding to Asp54 and Glu70 of TNFR2, respectively) in region C (Fig. 9.3a, e). This result indicates that Arg31 of TNF has an important role in the specificity for TNFR2 and is consistent with the previous report that the R31D mutant of TNF reduces the affinity for TNFR2 but retains the affinity for TNFR1 (Reed et al. 1997). Arg32 of TNF, which makes a hydrogen bond with Ser73 of TNFR2, seems to interact with Ser72 of TNFR1 in almost the same way (Fig. 9.3e), indicating that Arg32 of TNF contributes to the binding to both receptors.
Region D of TNFR2, which is near region A and B, shows a wide positively charged area compared to that of TNFR1 (Fig. 9.3a) that is caused by diversity in the modules present. In the A2 module structure (CRD3) of TNFR2 (the corresponding module is the A1 module (CRD3) in TNFR1), basic amino acids (Lys108 and Arg113) are exposed to the binding interface and generate a positively charged surface with Arg77 of CRD2 (Figs. 9.2d, 9.3a). Arg113 and Arg77 of TNFR2 interact with Asp143, Gln149, and Glu23 of TNF (Fig. 9.3d). In contrast, in the model of the TNF–TNFR1 complex, Arg77 of TNFR1, which structurally corresponds not to Arg77 but to Arg113 of TNFR2, appears to interact with Asp143 of TNF (Fig. 9.3f). Lys75 of TNFR1 seems to form a hydrogen bond with Glu23 of TNF and compensates the interactions observed between Arg77 of TNFR2 and Glu23 of TNF.
5 Structural Implication for the Design of Receptor-Selective Drugs
Elevated concentrations of TNF are closely associated with various autoimmune diseases (Feldmann and Maini 2003), and it is strongly implied that TNFR1 is involved in arthritis pathogenesis (Keffer et al. 1991; Mori et al. 1996). Therefore, a TNFR1-specific blockade would be a potential therapeutic strategy with low side effects.
Comparison of the structures of TNFR2 and TNFR1 highlighted two major structural differences for ligand binding that would be useful information for the design of receptor-specific drugs. Previous mutational analysis showed that the interactions between region B of TNFRs and the loop region of TNF (amino acid residues 143–149) are important for binding (Loetscher et al. 1993; Mukai et al. 2009c; Van Ostade et al. 1994). In the TNF–TNFR2 complex, the loop region of TNF fits to the region B in the A2 module of CRD3 (Fig. 9.4a). On the other hand, region B in TNFR1 (the A1 module of CRD3) is apart from TNF, and there is a cleft close to the TNF-binding region (Figs. 9.2e, 9.4c). Another structural difference between TNFR2 and TNFR1 was observed in region A. In the TNF–TNFR2 complex, there is a space at the binding interface on TNF from the shorter loop of TNFR2 (amino acid residues 79–81; Figs. 9.2c, d, 9.4b). On the other hand, region A of TNFR1, which is two amino acids longer (amino acid residues 77–81; Fig. 9.2c) than that of TNFR2 (Fig. 9.2e), is expected to interact with TNF through a wide surface area by van der Waals contacts (Fig. 9.4d). This recognition scheme is also observed in the LT-α–TNFR1 complex (Banner et al. 1993). These two regions of TNFRs (Fig. 9.4) would be targets for creating new drug candidates that specifically bind to TNFR1 or TNFR2.
Structural differences between the TNF–TNFR2 and TNF–TNFR1 complexes. a, b Binding interface of TNF–TNFR2 around regions B and A, respectively. c, d Binding interface of TNF–TNFR1 around regions B and A, respectively (modeled). A cleft observed on TNFR1 and a space on TNF are indicated by dashed circles
6 Network Model of the TNF–TNFR2 Complexes
According to previous reports, the PLAD of some TNFR superfamily members is crucial for ligand-independent self-assembly on the cell surface, which is required for efficient signal initiation (Chan et al. 2000; Siegel et al. 2000). However, in the crystal structure of the TNF–TNFR2 complex, the PLADs are more than 30 Å apart from each other. In other structures of the TNF–TNFR complexes, there is no structural insight for the assembly of TNFRs mediated through the PLADs (Banner et al. 1993; Mongkolsapaya et al. 1999; Hymowitz et al. 1999; Cha et al. 2000; Compaan and Hymowitz 2006). To understand the dynamic behavior of TNFR2 stimulated by TNF on the cell surface, we investigated the assembled state of TNFR2 by transfecting human embryonic kidney (HEK) 293T cells with three different types of plasmids encoding hemagglutinin (HA)-tagged wild-type TNFR2 (HA-TNFR2), TNFR2 lacking its PLAD (HA-TNFR2ΔPLAD), or TNFR2 lacking its intracellular domain (HA-TNFR2ΔCD) (Mukai et al. 2010). The TNFR2 self-complexes (with or without TNF) were captured by using the chemical cross-linker 3,3′-dithiobis (sulfosuccinimidyl propionate) (DTSSP), and detected by Western blotting analysis with antibodies against HA and TNF. In the absence of TNF, we detected not only monomeric TNFR2 but also dimeric and trimeric TNFR2 self-complexes, which is consistent with previous reports (Chan et al. 2000). Moreover, after stimulation by TNF, the formation of TNF–TNFR2 aggregates with a molecular mass greater than 1000 kDa was observed. On the other hand, a similar experiment with HA-TNFR2ΔPLAD showed that there is no TNFR2 self-complex in the absence or presence of TNF. Also, TNF rarely bound to TNFR2 without PLAD and did not induce the formation of TNF–TNFR2 aggregates, indicating that PLAD is necessary for the self-assembly of TNFR2 as well as the binding to TNF. This phenomenon is also observed in TNFR1 (Chan et al. 2000). The experiment with HA-TNFR2ΔCD showed that TNFR2ΔCD can still form self-complexes, but cannot form aggregates in the presence of TNF. These results suggested that TNF binds to the PLAD-dependent TNFR2 self-complex and induces the formation of TNF–TNFR2 aggregates on the cell surface, which is also mediated by the PLADs. For the formation of TNF–TNFR2 aggregates, the intracellular domain of TNFR2 is also important.
Previous reports and our results showed that TNFR2 and TNFR1 form homodimeric or homotrimeric self-complexes on the cell surface, respectively (Chan et al. 2000). On the other hand, crystallographic studies on ligand-free TNFR1 revealed that TNFR1 forms two different types of dimeric structures (Naismith et al. 1995, 1996), and structural insight into the self-complex of TNFR2 still remains unknown. Thus, we suggested two possible models (dimer and trimer models) for the signal initiation mediated by the TNFR2 self-complexes (Fig. 9.5). TNF trimers bind to dimeric or trimeric TNFR2 self-complexes, and other TNFR2 self-complexes subsequently bind to the TNFs. As a result, the TNF–TNFR2 complexes form a two-dimensional network on the cell surface. The networks generated by the TNFR2 dimers and trimers would maintain six- and threefold symmetry, respectively. The structural arrangement of intracellular domain of TNFR2 in the network might be necessary for efficient signaling through the intracellular signaling molecules such as TNFR-associated factor 2 (TRAF2) (Rothe et al. 1994). A signaling network model was also proposed in the cell by the studies of TNFR-associated factor 6 (TRAF6), which mediates Lys63-linked polyubiquitination of itself and induces NF-κB activation (Ye et al. 2002; Yin et al. 2009). TRAF6 is composed of a N-terminal RING/zinc-finger domain with E3 ligase activity and a C-terminal coiled-coil/TRAF-C domain, which interacts with receptors and adaptor proteins. It was shown that TRAF6 forms high-order oligomerization at the cell surface upon receptor stimulation, and dimerization of TRAF6 through its N-terminal domain is crucial for this oligomerization as well as for auto-ubiquitination (Yin et al. 2009). The C-terminal coiled-coil region also forms a trimer, and a “lattice” assembly model of TRAF6 in the activated state is generated on the basis of the N-terminal dimerization and the C-terminal trimerization. This “lattice” structure of TRAF6 molecules seems to enable the TRAF6 auto-ubiquitination in trans, and subsequent signal transduction.
Two-dimensional network models for the signal initiation through TNFR2. a Dimer model. b Trimer model. Overhead views of the cell surface. TNFR2 molecules interact with each other through the PLADs and form dimers or trimers, respectively. TNF and TNFR2 are shown in gray and black, respectively. (Modified from Y. Mukai et al. Science Signaling 3(148):ra83)
Abbreviations
- CRD:
-
cysteine-rich domain
- HA:
-
hemagglutinin
- IκB:
-
inhibitor of kappa B
- LT-α:
-
lymphotoxin-α
- NF-κB:
-
nuclear factor-kappa B
- PDB:
-
protein data bank
- PLAD:
-
pre-ligand-binding assembly domain
- r.m.s.d.:
-
root mean square deviation
- TNF:
-
tumor necrosis factor
- TNFR:
-
TNF receptor
- TNFR1:
-
TNF receptor superfamily member 1A
- TNFR2:
-
TNF receptor superfamily member 1B
- TRAF6:
-
TNFR-associated factor 6
References
Abe Y, Yoshikawa T, Inoue M, Nomura T, Furuya T, Yamashita T, Nagano K, Nabeshi H, Yoshioka Y, Mukai Y, Nakagawa S, Kamada H, Tsutsumi Y, Tsunoda S (2011) Fine tuning of receptor-selectivity for tumor necrosis factor-alpha using a phage display system with one-step competitive panning. Biomaterials 32(23):5498–5504
Aggarwal BB (2003) Signalling pathways of the TNF superfamily: a double-edged sword. Nat Rev Immunol 3(9):745–756
Banner DW, D’Arcy A, Janes W, Gentz R, Schoenfeld HJ, Broger C, Loetscher H, Lesslauer W (1993) Crystal structure of the soluble human 55 kd TNF receptor–human TNFβ complex: implications for TNF receptor activation. Cell 73(3):431–445
Bodmer JL, Schneider P, Tschopp J (2002) The molecular architecture of the TNF superfamily. Trends Biochem Sci 27(1):19–26
Cha SS, Sung BJ, Kim YA, Song YL, Kim HJ, Kim S, Lee MS, Oh BH (2000) Crystal structure of TRAIL-DR5 complex identifies a critical role of the unique frame insertion in conferring recognition specificity. J Biol Chem 275(40):31171–31177
Chan FK, Chun HJ, Zheng L, Siegel RM, Bui KL, Lenardo MJ (2000) A domain in TNF receptors that mediates ligand-independent receptor assembly and signaling. Science 288(5475):2351–2354
Chattopadhyay K, Ramagopal UA, Mukhopadhaya A, Malashkevich VN, Dilorenzo TP, Brenowitz M, Nathenson SG, Almo SC (2007) Assembly and structural properties of glucocorticoid-induced TNF receptor ligand: implications for function. Proc Natl Acad Sci U S A 104(49):19452–19457
Compaan DM, Hymowitz SG (2006) The crystal structure of the costimulatory OX40-OX40L complex. Structure 14(8):1321–1330
DeLano WL (2010) The PyMOL molecular graphics system. http://www.pymol.org/
Eck MJ, Sprang SR (1989) The structure of tumor necrosis factor-α at 2.6 Å resolution. Implications for receptor binding. J Biol Chem 264(29):17595–17605
Eck MJ, Ultsch M, Rinderknecht E, de Vos AM, Sprang SR (1992) The structure of human lymphotoxin (tumor necrosis factor-β) at 1.9 Å resolution. J Biol Chem 267(4):2119–2122
Faustman D, Davis M (2010) TNF receptor 2 pathway: drug target for autoimmune diseases. Nat Rev Drug Discov 9(6):482–493
Feldmann M, Maini RN (2003) Lasker Clinical Medical Research Award. TNF defined as a therapeutic target for rheumatoid arthritis and other autoimmune diseases. Nat Med 9(10):1245–1250
Gomez-Reino JJ, Carmona L, Valverde VR, Mola EM, Montero MD, Group B (2003) Treatment of rheumatoid arthritis with tumor necrosis factor inhibitors may predispose to significant increase in tuberculosis risk: a multicenter active-surveillance report. Arthritis Rheum 48(8):2122–2127
Hymowitz SG, Christinger HW, Fuh G, Ultsch M, O’Connell M, Kelley RF, Ashkenazi A, de Vos AM (1999) Triggering cell death: the crystal structure of Apo2L/TRAIL in a complex with death receptor 5. Mol Cell 4(4):563–571
Jin T, Guo F, Kim S, Howard A, Zhang YZ (2007) X-ray crystal structure of TNF ligand family member TL1A at 2.1 Å. Biochem Biophys Res Commun 364(1):1–6
Jones EY, Stuart DI, Walker NP (1989) Structure of tumour necrosis factor. Nature (Lond) 338(6212):225–228
Karpusas M, Hsu YM, Wang JH, Thompson J, Lederman S, Chess L, Thomas D (1995) 2 Å crystal structure of an extracellular fragment of human CD40 ligand. Structure 3(12):1426
Keffer J, Probert L, Cazlaris H, Georgopoulos S, Kaslaris E, Kioussis D, Kollias G (1991) Transgenic mice expressing human tumour necrosis factor: a predictive genetic model of arthritis. EMBO J 10(13):4025–4031
Loetscher H, Stueber D, Banner D, Mackay F, Lesslauer W (1993) Human tumor necrosis factor alpha (TNF α) mutants with exclusive specificity for the 55-kDa or 75-kDa TNF receptors. J Biol Chem 268(35):26350–26357
Lubel JS, Testro AG, Angus PW (2007) Hepatitis B virus reactivation following immunosuppressive therapy: guidelines for prevention and management. Intern Med J 37(10):705–712
Magis C, van der Sloot AM, Serrano L, Notredame C (2012) An improved understanding of TNFL/TNFR interactions using structure-based classifications. Trends Biochem Sci 37(9):353–363
McNicholas S, Potterton E, Wilson KS, Noble ME (2011) Presenting your structures: the CCP4mg molecular-graphics software. Acta Crystallogr D Biol Crystallogr 67(pt 4):386–394
Micheau O, Tschopp J (2003) Induction of TNF receptor 1-mediated apoptosis via two sequential signaling complexes. Cell 114(2):181–190
Mongkolsapaya J, Grimes JM, Chen N, Xu XN, Stuart DI, Jones EY, Screaton GR (1999) Structure of the TRAIL-DR5 complex reveals mechanisms conferring specificity in apoptotic initiation. Nat Struct Biol 6(11):1048–1053
Mori L, Iselin S, De Libero G, Lesslauer W (1996) Attenuation of collagen-induced arthritis in 55-kDa TNF receptor type 1 (TNFR1)-IgG1-treated and TNFR1-deficient mice. J Immunol 157(7):3178–3182
Morita C, Horiuchi T, Tsukamoto H, Hatta N, Kikuchi Y, Arinobu Y, Otsuka T, Sawabe T, Harashima S, Nagasawa K, Niho Y (2001) Association of tumor necrosis factor receptor type II polymorphism 196R with systemic lupus erythematosus in the Japanese: molecular and functional analysis. Arthritis Rheum 44(12):2819–2827
Mukai Y, Nakamura T, Yoshioka Y, Shibata H, Abe Y, Nomura T, Taniai M, Ohta T, Nakagawa S, Tsunoda S, Kamada H, Yamagata Y, Tsutsumi Y (2009a) Fast binding kinetics and conserved 3D structure underlie the antagonistic activity of mutant TNF: useful information for designing artificial proteo-antagonists. J Biochem (Tokyo) 146(2):167–172
Mukai Y, Nakamura T, Yoshioka Y, Tsunoda S, Kamada H, Nakagawa S, Yamagata Y, Tsutsumi Y (2009b) Crystallization and preliminary X-ray analysis of the tumour necrosis factor alpha-tumour necrosis factor receptor type 2 complex. Acta Crystallogr Sect F: Struct Biol Crystallogr Commun 65(pt 3):295–298
Mukai Y, Shibata H, Nakamura T, Yoshioka Y, Abe Y, Nomura T, Taniai M, Ohta T, Ikemizu S, Nakagawa S, Tsunoda S, Kamada H, Yamagata Y, Tsutsumi Y (2009c) Structure-function relationship of tumor necrosis factor (TNF) and its receptor interaction based on 3D structural analysis of a fully active TNFR1-selective TNF mutant. J Mol Biol 385(4):1221–1229
Mukai Y, Nakamura T, Yoshikawa M, Yoshioka Y, Tsunoda S, Nakagawa S, Yamagata Y, Tsutsumi Y (2010) Solution of the structure of the TNF-TNFR2 complex. Sci Signal 3(148):ra83
Naismith JH, Sprang SR (1998) Modularity in the TNF-receptor family. Trends Biochem Sci 23(2):74–79
Naismith JH, Devine TQ, Brandhuber BJ, Sprang SR (1995) Crystallographic evidence for dimerization of unliganded tumor necrosis factor receptor. J Biol Chem 270(22):13303–13307
Naismith JH, Devine TQ, Kohno T, Sprang SR (1996) Structures of the extracellular domain of the type I tumor necrosis factor receptor. Structure 4(11):1251–1262
Oeckinghaus A, Hayden MS, Ghosh S (2011) Crosstalk in NF-κB signaling pathways. Nat Immunol 12(8):695–708
Oregon-Romero E, Vazquez-Del Mercado M, Navarro-Hernandez RE, Torres-Carrillo N, Martinez-Bonilla G, Estrada-Garcia I, Rangel-Villalobos H, Munoz-Valle JF (2006) Tumor necrosis factor receptor 2 M196R polymorphism in rheumatoid arthritis and osteoarthritis: relationship with sTNFR2 levels and clinical features. Rheumatol Int 27(1):53–59
Palladino MA, Bahjat FR, Theodorakis EA, Moldawer LL (2003) Anti-TNF-α therapies: the next generation. Nat Rev Drug Discov 2(9):736–746
Pimentel-Muinos FX, Seed B (1999) Regulated commitment of TNF receptor signaling: a molecular switch for death or activation. Immunity 11(6):783–793
Reed C, Fu ZQ, Wu J, Xue YN, Harrison RW, Chen MJ, Weber IT (1997) Crystal structure of TNF-α mutant R31D with greater affinity for receptor R1 compared with R2. Protein Eng 10(10):1101–1107
Roberts NJ, Zhou S, Diaz LA Jr, Holdhoff M (2011) Systemic use of tumor necrosis factor alpha as an anticancer agent. Oncotarget 2(10):739–751
Rothe M, Wong SC, Henzel WJ, Goeddel DV (1994) A novel family of putative signal transducers associated with the cytoplasmic domain of the 75 kDa tumor necrosis factor receptor. Cell 78(4):681–692
Shibata H, Yoshioka Y, Ikemizu S, Kobayashi K, Yamamoto Y, Mukai Y, Okamoto T, Taniai M, Kawamura M, Abe Y, Nakagawa S, Hayakawa T, Nagata S, Yamagata Y, Mayumi T, Kamada H, Tsutsumi Y (2004) Functionalization of tumor necrosis factor-α using phage display technique and PEGylation improves its antitumor therapeutic window. Clin Cancer Res 10(24):8293–8300
Shibata H, Yoshioka Y, Ohkawa A, Minowa K, Mukai Y, Abe Y, Taniai M, Nomura T, Kayamuro H, Nabeshi H, Sugita T, Imai S, Nagano K, Yoshikawa T, Fujita T, Nakagawa S, Yamamoto A, Ohta T, Hayakawa T, Mayumi T, Vandenabeele P, Aggarwal BB, Nakamura T, Yamagata Y, Tsunoda S, Kamada H, Tsutsumi Y (2008) Creation and X-ray structure analysis of the tumor necrosis factor receptor-1-selective mutant of a tumor necrosis factor-α antagonist. J Biol Chem 283(2):998–1007
Shibata H, Yoshioka Y, Abe Y, Ohkawa A, Nomura T, Minowa K, Mukai Y, Nakagawa S, Taniai M, Ohta T, Kamada H, Tsunoda S, Tsutsumi Y (2009) The treatment of established murine collagen-induced arthritis with a TNFR1-selective antagonistic mutant TNF. Biomaterials 30(34):6638–6647
Siegel RM, Frederiksen JK, Zacharias DA, Chan FK, Johnson M, Lynch D, Tsien RY, Lenardo MJ (2000) Fas preassociation required for apoptosis signaling and dominant inhibition by pathogenic mutations. Science 288(5475):2354–2357
van Horssen R, Ten Hagen TL, Eggermont AM (2006) TNF-α in cancer treatment: molecular insights, antitumor effects, and clinical utility. Oncologist 11(4):397–408
Van Ostade X, Tavernier J, Fiers W (1994) Structure-activity studies of human tumour necrosis factors. Protein Eng 7(1):5–22
Ware CF, Crowe PD, Vanarsdale TL, Andrews JL, Grayson MH, Jerzy R, Smith CA, Goodwin RG (1991) Tumor necrosis factor (TNF) receptor expression in T lymphocytes. Differential regulation of the type I TNF receptor during activation of resting and effector T cells. J Immunol 147(12):4229–4238
Yamamoto Y, Tsutsumi Y, Yoshioka Y, Nishibata T, Kobayashi K, Okamoto T, Mukai Y, Shimizu T, Nakagawa S, Nagata S, Mayumi T (2003) Site-specific PEGylation of a lysine-deficient TNF-α with full bioactivity. Nat Biotechnol 21(5):546–552
Ye H, Arron JR, Lamothe B, Cirilli M, Kobayashi T, Shevde NK, Segal D, Dzivenu OK, Vologodskaia M, Yim M, Du K, Singh S, Pike JW, Darnay BG, Choi Y, Wu H (2002) Distinct molecular mechanism for initiating TRAF6 signalling. Nature (Lond) 418(6896):443–447
Yin Q, Lin SC, Lamothe B, Lu M, Lo YC, Hura G, Zheng L, Rich RL, Campos AD, Myszka DG, Lenardo MJ, Darnay BG, Wu H (2009) E2 interaction and dimerization in the crystal structure of TRAF6. Nat Struct Mol Biol 16(6):658–666
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer Japan
About this chapter
Cite this chapter
Nakamura, T., Mukai, Y., Tsutsumi, Y., Yamagata, Y. (2015). Structural Basis for Signal Initiation by TNF and TNFR. In: Inoue, Ji., Takekawa, M. (eds) Protein Modifications in Pathogenic Dysregulation of Signaling. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55561-2_9
Download citation
DOI: https://doi.org/10.1007/978-4-431-55561-2_9
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55560-5
Online ISBN: 978-4-431-55561-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)