Abstract
One of the most important current issues in vaccinology is the need for vaccine delivery systems and adjuvants as an immune stimulator (immunostimulant). Polymeric nanoparticles with entrapped vaccine antigens, such as proteins, peptides, and DNA, have recently been shown to possess significant potential as vaccine delivery systems and immunostimulants. Novel nanoparticle-based vaccines are being evaluated in a variety of vaccine therapy including infectious diseases, cancers, or autoimmune diseases. Biodegradable nanoparticles that can control physicochemical properties, such as particle size, surface charge, and polymer composition, are promising candidate adjuvant systems to enhance vaccine efficacy. In this review, polymeric nanoparticles as vaccine delivery systems and immunostimulants are addressed with focus on (1) targeting of antigens to antigen-presenting cells (APCs), (2) control of the intracellular trafficking and biodistribution of nanoparticles, and (3) activation of APCs by particles for the development of effective vaccines. Understanding the strategies and mechanisms of immune induction by nanoparticle-based vaccines will help in the design guide of nanoparticle for the development of novel adjuvants. The development of safe and efficacious novel adjuvants is strongly desired. Vaccine delivery systems mainly function to target antigens to APCs, and immunostimulants directly activate these cells through specific receptors. The targeting antigen specifically to dendritic cells (DCs) and their subsequent activation with nanoparticles has demonstrated exciting potential for developing new vaccine technology. Uptake of nanoparticles by DCs can be controlled by altering properties of the nanoparticles, including size and surface characteristics. Moreover, novel chemical strategies can be employed to modulate DC maturation and immune presentation of antigens. This approach will enable both preventative and therapeutic vaccination for immune diseases requiring cellular immunity.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
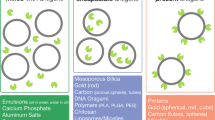
The purpose of vaccination is to generate a strong immune response, thus providing long-term protection against infection. When compared to traditional vaccines, which mainly consisted of attenuated pathogens, whole inactivated organisms, or inactivated bacterial toxins, the new generation of vaccines such as subunit antigenic proteins or peptides is less reactogenic and immunogenic and thus requires the use of adjuvants to induce optimal immune responses [1–5]. Adjuvants are compounds that enhance the immune response against co-inoculated antigens, with the word adjuvant coming from the Latin word adjuvare, which means to help or to enhance. In the past, many kinds of adjuvant have been developed, and they can be divided into two classes on the basis of their mechanism of action: vaccine delivery systems and immunostimulants [6]. Vaccine delivery systems generally have a particulate form (e.g., emulsions, liposomes, micelles, and polymeric nano-/microparticles) and function mainly to target associated antigens into antigen-presenting cells (APCs) such as dendritic cells (DCs) and macrophages. In contrast, immunostimulants mostly consist of pathogen-associated molecule (e.g., lipopolysaccharide, monophosphoryl lipid A, cholera toxin, CpG ODN), which activate cells of the innate immune system via specific receptors.
Until recently, hydroxide and phosphate salts of aluminum and calcium were the only adjuvants licensed for human use. Aluminum hydroxide or phosphate salts, commonly called alum, have dominated adjuvant use since the discovery of its adjuvant effect in the 1920s [7]. The mechanism of action of alum adjuvant is complex and not yet fully understood. It likely involves various mechanisms including the formation of depot, increasing targeting of antigens to APCs, and nonspecific activation of immune systems. Many adjuvants function in a manner similar to alum by providing an antigen depot. Antigen depots enhance immunogenicity of antigens by concentrating the peptides and extending the time antigen resides in the body, thus increasing the probability of interaction with immune cells. However, the use of alum-type adjuvant for vaccination has some disadvantages [8, 9]. They induce local reactions, induce IgE antibody responses, and generally fail to induce cell-mediated immunity, particularly cytotoxic T lymphocyte (CTL) responses. Therefore, the development of more efficient and safe adjuvants to obtain high and long-lasting immune responses is of primary importance.
Polymeric nanoparticles formulated from synthetic or biodegradable polymers are widely explored as carriers for controlled delivery of different agents including proteins, peptides, plasmid DNA (pDNA), and low-molecular-weight compounds [10–12]. Numerous investigators have shown that the biological distribution of drugs, proteins, and DNA can be modified, both at the cellular and organ levels, using nano-/microparticle delivery systems [13, 14]. For the development of vaccines, biodegradable nanoparticles show great promise as delivery systems. Controlled delivery systems consisting of nanoparticles can potentially delivery either the antigens or immunostimulants to the desired location at predetermined rates and durations to generate an optimal immune response. The carrier may also protect the vaccine from degradation until it is released. Other potential advantages of the controlled delivery approach include reduced systemic side effects and the possibility of co-encapsulating multiple antigenic epitopes or both antigen and immunostimulant in a single carrier. Biodegradable polymers provide sustained release of the encapsulated antigen and degrade in the body to nontoxic, low-molecular-weight products that are easily eliminated.
This review focuses on biodegradable polymeric nanoparticles as vaccine delivery systems and immunostimulants by summarizing the preparation of antigen-conjugated particles and the mechanism of nanoparticle-based vaccines. Theoretically, nanoparticles are solid particles ranging in size from 1 to 1,000 nm, while microparticles are particles that have sizes that range from 1 to 1,000 μm [15]. In the design of optimal vaccine delivery systems, polymeric nanoparticles have the advantage that their physicochemical properties such as particle size, shape, surface charge, and polymer composition can be regulated. Using these systems, it is possible to target antigen delivery to APCs, activate these APCs, and control intracellular release and distribution of the antigen (Fig. 12.1). By understanding immune activation, we can rationally design particulate adjuvant to not only deliver antigen but also directly activate innate immune cells providing the pro-inflammatory context for antigen recognition. The generation of more potent particulate adjuvants may allow the development of prophylactic and therapeutic vaccines against cancers and chronic infectious diseases.
Desired function of particulate antigens as vaccine delivery systems and immunostimulants for induction and regulation of antigen-specific immune responses. Antigen-conjugated nanoparticles administered by a systemic route may (1) be directly taken up by APCs, such as dendritic cells and macrophages; (2) activate APCs through specific receptors (may be related to Toll-like receptors). Particle size affects DC uptake and activation processes. Particles can be conjugated with DC-specific antibodies to increase targeting. (3) pH-sensitive particles can control intracellular distribution of antigen. The particles disrupt endosomes and release antigens to the cytoplasm. (4) Particles taken up by APCs migrate to lymph nodes, (5) where they mature and present antigen to T cells. (6) Small particles (>50 nm) can enter lymphatic vessels directly and migrate to lymph nodes with the lymphatic flow, where they are taken up by immature DCs resident in the nodes
2 Preparation of Biodegradable Polymeric Nanoparticles for Antigen Delivery
2.1 Aliphatic Polyester-Based Nanoparticles
Biodegradable polymeric nanoparticles have attracted much attention for their potential in biomedical applications. The biodegradation rate and the release kinetics of loaded drugs can be controlled by the composition ratio and the molecular weight of the polymer and block/graft copolymers [16–18]. Furthermore, by modulating the polymer characteristics, one can control the release of a therapeutic agent from the nanoparticles to achieve a desired therapeutic level in a target tissue for the required duration for optimal therapeutic efficacy. The commonly used biodegradable polymers are aliphatic polyesters, such as poly(lactic acid) (PLA), poly(glycolic acid) (PGA), poly(ε-caprolactone) (PCL), poly(hydroxybutyrate) (PHB), and their copolymers (Fig. 12.2) [19]. In particular, poly(lactide-co-glycolide) (PLGA) has been the most extensively investigated for developing nano-/microparticles encapsulating therapeutic drugs in controlled release applications [20–22] due to their inherent advantages. The copolymers have the advantage of sustaining the release of the encapsulated therapeutic agent over a period of days to several weeks. As polyesters in nature, these polymers undergo hydrolysis upon administration into the body, forming biologically compatible and metabolizable moieties (lactic acid and glycolic acid) that are eventually removed from the body by the citric acid cycle.
Antigen-conjugated nanoparticles are being investigated as vaccine delivery system alternatives to the currently used alum with an objective to develop better vaccine systems and minimize the frequency of immunization. The encapsulation of antigenic proteins or peptides into PLGA nanoparticle delivery system can be carried out through mainly three methods: the water-in-oil-in-water (w/o/w) emulsion technique, phase separation, and spray drying. The w/o/w double emulsion process is popularly used to load proteins into nanoparticles [23, 24]. In this process, an antigen is first dissolved in an aqueous solution, which is then emulsified in an organic solvent to make a primary water-in-oil emulsion. This initial emulsion is further mixed in an emulsifier-containing aqueous solution to make a w/o/w double emulsion. The ensuing removal of the solvent leaves nano-/microparticles in the aqueous continuous phase, making it possible to collect them by filtration or centrifugation. However, the possible denaturation of the proteins at the oil–water interface limits the usage of this method. It has been reported that this interface causes conformational changes in bovine serum albumin (BSA) [25, 26]. Moreover, it has a disadvantage in that the entrapment efficiency is very low. The prevention of protein denaturation and degradation, as well as high entrapment efficiency, would be of particular importance in the preparation of nanoparticles containing water-soluble drugs such as a protein. Improved protein integrity has been achieved by the addition of stabilizers such as carrier proteins (e.g., albumin), surfactants during the primary emulsion phase, or molecules such as trehalose and mannitol to the protein phase. The use for vaccines of these protein-loaded PLGA nanoparticles is described in the following sections.
2.2 Amphiphilic Poly(Amino Acid) Nanoparticles
Self-assembling polymer or block/graft copolymers that can form nanostructure have been extensively investigated in the field of biotechnology and pharmaceuticals. In general, hydrophobic interactions, electrostatic forces, hydrogen bonds, van der Waals forces, or combinations of these interactions are available as the driving forces for the formation of the polymer complexes [27–31]. Nanoparticles fabricated by the self-assembly of amphiphilic block copolymers or hydrophobically modified polymers have been explored as drug carrier systems. In general, these amphiphilic copolymers consisting of hydrophilic and hydrophobic segments are capable of forming polymeric structures in aqueous solutions via hydrophobic interactions. These self-assembled nanoparticles are composed of an inner core of hydrophobic moieties and an outer shell of hydrophilic groups [32, 33].
In particular, poly(amino acids) have received considerable attention for their medical applications as potential polymeric drug carriers. Several amphiphilic block and graft copolymers based on poly(amino acid) have been employed, such as poly(α-l-glutamic acid) [34], poly(γ-glutamic acid) [35], poly(ε-lysine) [36], poly(l-aspartic acid) [37], poly(l-lysine) [38], poly(l-arginine) [39], and poly(l-asparagine) [40] as hydrophilic segments and poly(β-benzyl-l-aspartate) [41], poly(γ-benzyl-l-glutamate) [42], and poly(l-histidine) [43] as hydrophobic segments. In general, amphiphilic copolymers based on poly(amino acid) form micelles through self-association in water.
Poly(γ-glutamic acid) (γ-PGA) is a naturally occurring poly(amino acid) that is synthesized by certain strains of Bacillus [44] (Fig. 12.2). The polymer is made of d- and l-glutamic acid units linked through the α-amino and the γ-carboxylic acid groups, and its α-carboxylate side chains can be chemically modified to introduce various bioactive ligands or to modulate the overall function of the polymer [45–49]. Unlike general poly(amino acids), γ-PGA has unique characteristics with regard to enzymatic degradation and immunogenicity, compared to poly(amino acid) consisting of l-amino acid. It has been reported that γ-PGA is resistant against many proteases because γ-linked glutamic acids are not easily recognized by common proteases [50, 51]. Moreover, several studies have shown that γ-PGA by itself is a poor immunogen and does not induce booster responses, probably because of its simple homopolymeric structure, similar to those of polysaccharides [52–56]. Therefore, the potential applications of γ-PGA and its derivatives have been of interest in a broad range of fields, including medicine, food, cosmetic, and water treatment [57].
Akashi et al. prepared nanoparticles composed of hydrophobically modified γ-PGA [36, 58, 59]. γ-PGA (400 kDa) as the hydrophilic backbone and l-phenylalanine (Phe) as the hydrophobic segment were synthesized by grafting Phe to γ-PGA using water-soluble carbodiimide. The γ-PGA-graft-Phe copolymers (γ-PGA-Phe) with more than 50 % grafting degree formed monodispersed nanoparticles in water due to their amphiphilic properties (Fig. 12.3). To prepare nanoparticles, γ-PGA-Phe dissolved in dimethyl sulfoxide (DMSO) was added to various concentration of NaCl solution, and then the resulting solutions were dialyzed and freeze-dried. The γ-PGA-Phe formed monodispersed nanoparticles, and the particle size of the γ-PGA-Phe nanoparticles could be easily controlled (30–200 nm) by changing NaCl concentration [60]. In addition, the nanoparticles consisting of amphiphilic γ-PGA can efficiently and stably encapsulate various types of protein (11 different proteins with various molecular weights and isoelectric points, e.g., thyroglobulin, ovalbumin, lysozyme). Protein-loaded γ-PGA-Phe nanoparticles were prepared by encapsulation, covalent immobilization, or physical adsorption methods in order to study their potential applications as protein carriers [61]. To prepare the protein-encapsulated γ-PGA-Phe nanoparticles, proteins with various molecular weights and isoelectric points were dissolved in saline, and the γ-PGA-Phe dissolved in DMSO was added to the protein solutions. The resulting solutions were then centrifuged and repeatedly rinsed. The encapsulation of proteins into the nanoparticles was successfully achieved. The encapsulation efficiency was found to be in 50 % for most samples and was not markedly influenced by the physical properties of that protein [62]. Ovalbumin (OVA) encapsulated into the nanoparticles was not released (less than 10 %) over the pH range of 4–8, even after 10 days. Also, Portilla-Arias et al. reported the preparation of nanoparticles made of alkyl esters of γ-PGA and their potential application as drug and protein carrier [63]. Besides the particle formation of γ-PGA by using hydrophobic interaction, nanoparticles formed by complexation of γ-PGA with bivalent metal ion complex [64] or chemical cross-linking of carboxyl group of γ-PGA [65] have been reported.
2.3 Amphiphilic Polysaccharide Nanoparticles
Polysaccharidic hydrogel particles have been often used for designing protein-loaded systems for therapeutic applications. Polysaccharides are very hydrophilic polymers, and their hydrogels thus exhibit a good biocompatibility. Various types of hydrophobized polysaccharides, such as pullulan [66, 67], curdlan [68], dextran [69], alginic acid [70], and chitosan [71], have been used for preparation of nanoparticles. Akiyoshi et al. reported that self-aggregated hydrogel nanoparticles could be formed from cholesterol-bearing pullulan by an intra- and/or intermolecular association in diluted aqueous solutions [72]. Recently, much attention has been paid to chitosan as a drug or gene carrier because of its biocompatibility and biodegradability. Chitosan is a polysaccharide constituted by N-glucosamine and N-acetyl-glucosamine units, in which the number of N-glucosamine units exceeds 50 %. Chitosan can be degraded into nontoxic products in vivo, and thus, it has been widely used in various biomedical applications [73, 74]. Chitosan has cationic characters even in neutral condition to form complexes with negatively charged pDNA. Jeong et al. prepared nano-sized self-aggregates composed of hydrophobically modified chitosans with deoxycholic acids [75, 76]. The size of self-aggregates varied in the range of 130–300 nm in diameter, and their structures were found to depend strongly on the molecular weight of chitosan. To explore the potential applications of self-aggregates as a gene delivery carrier, complexes between chitosan self-aggregates and pDNA were prepared. The complex formation had strong dependency on the size and structure of chitosan self-aggregates and significantly influenced the transfection efficiency of cells. It is expected that these approaches to control the size and structure of chitosan-derived self-aggregates have a wide range of applications in gene delivery. Also, Kida et al. reported that novel polysaccharide-based nanoparticles were successfully prepared by the self-assembly of amphiphilic pectins, which were easily synthesized by the reaction of pectins with l-phenylalanine (Phe) as hydrophobic groups (Fig. 12.3) [77]. Pectin is a polymer of d-galacturonic acid. The galacturonic acid molecule has a carboxyl group on C5, some of which are esterified to form methyl esters. The pectin-graft-Phe could form about 200-nm-sized nanoparticles and were able to retain entrapped protein in the nanoparticles for 1 week without any significant leakage.
3 Uptake of Particulate Antigens by APCs
Biodegradable polymeric nanoparticles can be designed to fill various roles in antigen delivery, and they have been used to release antigens in a controlled manner. However, recent strategies for developing preventative and therapeutic vaccines have focused on the ability to deliver antigen to dendritic cells (DCs) in a targeted and prolonged manner. These strategies use nanoparticles because they can achieve longevity on intact antigen to increase the opportunity for DC uptake and processing. DCs are the most effective antigen-presenting cells (APCs) and have a crucial role in initiating T-cell-mediated immunity. DCs can control a substantial part of the adaptive immune response by internalizing and processing antigen through major histocompatibility complex (MHC) class I and class II pathways and then presenting antigenic peptides to CD4+ and CD8+ T lymphocytes [78]. Therefore, targeting DCs with an antigen delivery system provides tremendous potential in developing new vaccines [79]. Macrophages present endogenous antigens, such as those derived from viral expression, on MHC class I complexes. On the other hand, phagocytosed antigens are cleaved by lysosomal enzymes and expressed as MHC class II complexes. In contrast, dendritic cells can present soluble exogenous antigens as MHC class I complexes. This phenomenon has given rise to the theory of cross-priming, involving proteasomal degradation in the cytosol. Antigen uptake by DCs is enhanced by the association of the antigens with polymeric nanoparticles. It is mediated by several uptake mechanisms such as receptor-mediated endocytosis, macropinocytosis, and phagocytosis, depending on the nature of the particulate antigen [80]. Interactions between particulate formulations and cells in general depend on particle characteristics such as size, shape, and surface properties, including surface charge and hydrophobicity.
Akagi et al. demonstrated the use of nanoparticles composed of amphiphilic poly(amino acid) derivatives as adjuvants [81–84]. To evaluate the uptake of OVA-encapsulated γ-PGA-Phe nanoparticles (OVA-NPs) by DCs, murine bone marrow-derived DCs were incubated with 250-nm-sized OVA-NPs for 30 min at 37 °C. The cells were then analyzed by flow cytometry (FCM) and confocal laser scanning microscopy (CLSM). OVA-NPs were efficiently taken up into DCs, whereas the uptake of OVA alone was barely detectable at the same concentration of OVA. OVA-NPs were more efficiently taken up than OVA alone by DCs, and the uptake of OVA-NPs was inhibited at 4 °C [81]. These results suggest that OVA-NPs were phagocytosed mainly via endocytosis by the DCs. In the case of OVA alone, an approximately 30-fold higher concentration was required to elicit a similar amount of intracellular OVA as compared to OVA-NPs. Likewise, it has been reported that PLGA nanoparticles or liposomes are efficiently phagocytosed by the DCs in culture, resulting in their intracellular localization [85–87]. Foged et al. investigated DC uptake of model fluorescent polystyrene particles with a broad size range (0.04–15 μm). The results showed that DC internalized particles in the tested size range with different efficiencies. The optimal particle size for DC uptake was 500 nm and below. In the smaller particle size, the higher percentage of the DCs interacted with the polystyrene spheres [88]. Kanchan et al. also reported that PLA nanoparticles (200–600 nm) were efficiently taken up by macrophages in comparison to microparticles (2–8 μm) [89]. In contrast, in hydrogel particles composed of polyacrylamide, there was no difference in uptake by APCs between 3.5-μm and 35-nm-sized particles [90]. This disparity in uptake may be related to fundamental differences in the material properties of those carriers.
Particle shape and surface charge are equally important particulate physicochemical factors and play a crucial role for the interaction between particles and APCs. In general, cationic particles induced high phagocytosis activity of APCs, because of anionic nature of cell membranes [88]. Recently, particle shape has been identified as having a significant effect on the ability of macrophages to internalize particles via actin-driven movement of the macrophage membrane. Champion et al. observed that the cellular uptake of particles strongly depends on the shape of particles. The wormlike particles with very high aspect ratios exhibited negligible phagocytosis when compared to traditional spherical particles [91, 92]. These results suggest that uptake of particles by APCs strongly depends on the local geometry at the interface of particle and the cells.
4 Control of Intracellular Distribution of Nanoparticles
In general, particulate materials can be easily internalized into the cells via endocytosis, depending on their sizes, shapes, and surface charges. However, the internalized materials are mostly trafficked from acidic endosomes to lysosomes, where the degradation may occur. Thus, degraded exogenous antigens are presented by the MHC class II presentation pathway, and a part of the pathway involves antibody-medicated immune responses. In contrast, antigens within the cytosol are processed into proteasomes and presented by the MHC class I pathway, a pathway involved in CTL response [93–95] (Fig. 12.4). Therefore, the induction of antigen-specific cellular immunity by exogenous antigens is needed in the regulation of intracellular distribution of antigens. The escape of internalized antigens from endosomes to the cytoplasm is an important subject to control the antigen processing/presentation pathways.
Pathways of intracellular trafficking of particulate antigens in APCs. Antigens can be encapsulated within particles. Antigen-conjugated nanoparticles can be internalized into the cells via endocytosis, depending on their sizes, shapes, and surface charges. Polymers sensitive to pH can disrupt or destabilize the endosomal membrane and release antigen into the cytoplasm. Polymer hydrophobicity is also an important factor for endosome escape of antigens. Antigens taken up by APCs are processed into peptide epitopes and directed through two discrete pathways to MHC classes I and II, which present peptide for interaction with either CD8+ or CD4+ T cells, respectively
4.1 pH-Responsive Nanoparticles
The release of biomolecules from acidic endosomes requires a membrane-disruptive agent, which can release the internalized compounds into the cytoplasm. Approaches include the use of membrane-penetrating peptides, pathogen-derived pore-forming proteins, and “endosome-escaping” polymers or lipids that disrupt the endosomal membrane in response to the pH reduction, which occurs in these compartments. Thus, in recent years, there has been significant interest in developing pH-sensitive nanoparticles that can enhance the cytoplasmic delivery of various biomolecules [96–99]. Standley et al. reported an acid-degradable particle composed of acrylamide and acid-degradable cross-linker for protein-based vaccines. These particles released encapsulated protein in a pH-dependent manner. They were stable at the physiological pH of 7.4 but degrade quickly in the pH 5.0 environment of endosomes. The degradation of particles led to the endosome escape of encapsulated proteins. The colloid osmotic mechanism is to generate a quick degradation of the particles into many molecules, thus increasing the osmotic pressure within the endosomes, leading to a rapid influx of water across the membrane resulting in its disruption. In fact, the MHC class I presentation levels achieved with these particles were vastly enhanced as a result of their ability to deliver more protein into the cytoplasm of APCs. In mouse immunization study, these acid-sensitive particles could induce antigen-specific CTL responses and showed antitumor activity [100, 101]. Hu et al. also reported the endosome escape of pH-responsive core–shell nanoparticles. pH-sensitive poly(diethylaminoethyl methacrylate) (PDEAEMA)-core/poly(ethylene glycol) dimethacrylate (PAEMA)-shell nanoparticles were capable of efficient cytosolic delivery of membrane-impermeable molecules such as calcein and OVA to DCs. These particles effectively disrupted endosomes and delivered molecules to the cytosol of cells without cytotoxicity and enhanced priming of CD8+ T cells by DCs pulsed with OVA/PDEAEMA-core nanoparticles [102]. Polycations that absorb protons in response to the acidification of endosomes can disrupt these vesicles via the proton sponge effect. The proton sponge effect arises from a large number of weak conjugate bases with buffering capacities between 7.2 and 5.0, such as polyethylenimine (PEI), leading to proton absorption in acid organelles and an osmotic pressure buildup across the organelle membrane. This osmotic pressure causes swelling and/or rupture of the acidic endosomes and a release of the internalized molecules into the cytoplasm [103].
4.2 Amphiphilic Polymers for Cytosolic Delivery
Synthetic poly(alkylacrylic acid) [104, 105] and poly(alkylacrylic acid-co-alkyl acrylate) [106, 107] also have pH-dependent, membrane-disruptive properties. These polymers contain a combination of carboxyl groups and hydrophobic alkyl groups and are protonated at the endosomal pH range. Upon a decrease in pH, they increase their hydrophobicity and penetrate into the endosomal membranes and disrupt them. The hydrophobicity of the polymers is important for disrupting lipid membranes. Foster et al. have applied these amphiphilic polymers to nanoparticle delivery systems [108]. A pH-responsive nanoparticle (180 nm) incorporating OVA-conjugated poly(propylacrylic acid) (PPAA) (PPAA-OVA) was evaluated to test whether improved cytosolic delivery of a protein antigen could enhance CD8+ CTL and prophylactic tumor vaccine responses. Nanoparticles containing PPAA-OVA were formed by ionic complexation of cationic poly(dimethylaminoethyl methacrylate) (PDMAEMA) with the anionic PPAA-OVA conjugate (PPAA-OVA/PDMAEMA). The PPAA-OVA/PDMAEMA nanoparticles were stably internalized and could access the MHC class I pathway in the cytosol by triggering endosome escape. In an EG.7-OVA mouse tumor protection model, PPAA-OVA/PDMAEMA-immunized mice delayed tumor growth for nearly 5 weeks, while control mice injected with PBS and free OVA developed tumors in less than 10 days. This response was attributed to the eightfold increase in production of OVA-specific CD8+ T lymphocytes and an 11-fold increase in production of anti-OVA IgG. However, these vinyl polymers are not biodegradable and, thus, their molecular weight presents a limitation for medical applications.
Recently, our group developed novel biodegradable nanoparticles composed of hydrophobically modified γ-PGA (γ-PGA-Phe). The nanoparticles showed a highly negative zeta potential (−25 mV) due to the ionization of the carboxyl groups of γ-PGA located near the surfaces. Protein-encapsulated γ-PGA-Phe nanoparticles efficiently delivered proteins from the endosomes to the cytoplasm in DCs [109]. To evaluate their potential applications as membrane-disruptive nanoparticles, the nanoparticles were characterized with respect to their hemolytic activity against erythrocytes as a function of pH. The nanoparticles showed hemolytic activity with decreasing pH from 7 to 5.5 and were membrane inactive at physiological pH. As the pH decreased, the hemolytic activity of the nanoparticles gradually increased, reaching a peak at pH 5.5. This activity was dependent on the hydrophobicity of γ-PGA. The mechanism responsible for the pH-dependent hemolysis by the nanoparticles involved a conformational change of γ-PGA-Phe and corresponding increase in the surface hydrophobicity. Increased polymer hydrophobicity resulted in increased membrane disruption. The γ-PGA-Phe has carboxyl side-chain groups, so the pKa of the proton of the carboxyl groups is also a very important factor for the pH sensitivity of the γ-PGA-Phe [84].
It has also been reported that antigen delivery to DCs via PLGA particles increased the amount of protein that escaped from endosomes into the cytoplasm. How PLGA particles encapsulated proteins or peptides become accessible to the cytoplasm is still not clear. It is suggested that the gradual acidification of endosomes would lead to the protonation of the PLGA polymer, resulting in enhanced hydrophobicity and attachment and rupture of the endosomal membrane [110].
5 Activation of APCs by Nanoparticles
Research on biomaterial adjuvant potential has been focused largely on determining the degree of DC maturation induced by exposure to polymeric nanoparticles or liposomes [111–113]. The maturation of DCs is associated with increased expression of several cell surface markers, including the co-stimulatory molecules CD40, CD80, CD83, CD86, and MHC class I and class II. It is well known that DC maturation can be induced by inflammatory factors such as lipopolysaccharide (LPS), bacterial DNA, or inflammatory cytokines such as TNF-α, and the process is highly important for the innate immune responses [114, 115]. Therefore, in addition to the antigen delivery to DCs, DC maturation is crucial in the development of effective vaccines.
In vitro studies have shown that γ-PGA-Phe nanoparticle-pulsed DCs result in DC maturation by upregulation of co-stimulatory molecule expression and cytokine production. To determine whether the uptake of γ-PGA-Phe nanoparticles mediates the phenotypic maturation of DCs, DCs were incubated with γ-PGA-Phe nanoparticles for 24 or 48 h, and the expression of surface molecules was measured by flow cytometry. Upon exposure of these DCs to the nanoparticles, the expression of co-stimulatory molecules (maturation markers) was increased in a dose-dependent manner. The expression levels of co-stimulatory molecules in nanoparticle-pulsed DCs were similar to those of LPS-pulsed DCs. The effect of nanoparticles on DCs was not inhibited by treatment with polymyxin B (PmB), an inhibitor of LPS, suggesting that nanoparticle-induced DC maturation is not due to LPS contamination. These results suggest that γ-PGA-Phe nanoparticles have great potential as adjuvant for DC maturation [81–83]. Interestingly, the difference in DC activation was detected by changing the size of nanoparticles. The induction of maturation markers was increased with decreasing particle size. These results indicate that DC maturation was significantly affected by the size of nanoparticles. The mechanisms responsible for DC maturation by γ-PGA-Phe nanoparticles may be related to Toll-like receptors (TLRs) of DCs. TLRs are abundantly expressed on professional APCs. TLRs play a major role in pathogen recognition and in the initiation of the inflammatory and immune responses [116]. The stimulation of TLRs by TLR ligands induces the surface expression of co-stimulatory molecules, and this phenotypic modulation is a typical feature of DC maturation. Recently, soluble γ-PGA-induced innate immune responses have been reported in a TLR4-dependent manner in DCs [117, 118]. Treatment with high molecular mass γ-PGA (2,000 kDa), but not a low molecular one (10 kDa), induced a significant upregulation of CD40, CD80, and CD86 expression in wild-type DCs. The stimulatory capacity of γ-PGA was not significantly affected by pretreatment with PmB. In contrast, DCs from TLR4-defective mice did not show an enhanced expression of maturation markers in response to the 2,000 kDa γ-PGA treatment. These results suggest that not only the DC uptake process of γ-PGA-Phe nanoparticles but also the surface interactions between γ-PGA-Phe nanoparticles and DCs are important for induction of DC maturation. The DC uptake of 30-nm-sized nanoparticles was lower than for 200-nm-sized nanoparticles, but the effect of DC activation by the nanoparticles was high in the small sizes. Thus, it is considered that the surface interactions between the nanoparticles and DCs predominately affect the DC maturation. Tomayo et al. have also reported that poly(anhydride) nanoparticles act as agonists of various TLRs. The nanoparticles were useful as Th1 adjuvants in immunoprophylaxis and immunotherapy through TLR exploitation [119].
The efficacy of antigen-loaded γ-PGA-Phe nanoparticles on the induction of antigen-specific humoral and cellular immune responses was examined using OVA as a model antigen [82]. The immune responses were investigated in mice after subcutaneous immunization with OVA-encapsulated γ-PGA-Phe nanoparticles (OVA-NPs). The mice immunized with OVA-NPs showed a more potent CTL response than those obtained from mice immunized with OVA plus complete Freund’s adjuvant (CFA). It has been demonstrated that the γ-PGA-Phe nanoparticles are also effective for vaccines against human immunodeficiency virus (HIV) [81], influenza virus [120], or cancers [121].
Similar results on DC maturation by particulate materials have been obtained with PLGA nano-/microparticles [122, 123], liposomes [87], cationic polystyrene microparticles [124], polystyrene nanoparticles [125], and acid-degradable cationic nanoparticles [126]. Elamanchili et al. examined DC maturation by PLGA nanoparticles. The results showed that after PLGA nanoparticle pulsing, DCs exhibited a modest increase in the expression of MHC class II and CD86 compared to untreated controls. In addition, DCs pulsed with PLGA nanoparticles containing an immunomodulator, monophosphoryl lipid A (MPLA), further induced DC maturation [86]. The PLGA-based nanoparticulate system offers the flexibility for incorporation of broad range of TLR ligands. Copland et al. investigated whether formulation of antigen in mannosylated liposomes enhanced uptake and DC maturation. Exposure to liposomes containing OVA resulted in enhanced expression of maturation markers when compared to exposure to antigen in solution. Expression was highest following exposure to mannosylated liposomes [87]. These particulate systems hold promise as a vaccine delivery system and immunostimulant.
PLGA or PLA nano-/microparticles are suitable vehicles for the delivery of recombinant proteins, peptides, and pDNA to generate immune responses in vivo. Several studies have shown that PLGA nanoparticles can be used to modulate immune responses against encapsulated antigens due to their ability to efficiently target APCs and to facilitate appropriate processing and in presenting antigens to T cells [24, 127–135]. Gutierro et al. investigated the immune responses by BSA-loaded PLGA nanoparticles after subcutaneous, oral, and intranasal administration to evaluate parameters that can affect the immune response [136]. The vaccination of 1,000 nm particles generally elicited a higher serum IgG response than that obtained with the vaccination of 500- or 200-nm-sized particles, the immune response for 500 nm particles being similar than that obtained with 200 nm by the subcutaneous and the oral route and higher by the intranasal route.
Many different vaccine antigens encapsulated into PLGA nanoparticles were shown to induce broad and potent immune responses. For example, hepatitis B therapeutic vaccines were designed and formulated by loading the hepatitis B core antigen (HBcAg) into PLGA nanoparticles (300 nm) with or without monophospholipid A (MPLA) adjuvant [137]. A single immunization with HBcAg-encapsulated PLGA nanoparticles containing MPLA induced a stronger cellular immune response than those induced by HBcAg alone and HBcAg mixed with MPLA in a murine model. More importantly, the level of HBcAg-specific immune responses could be increased further significantly by a booster immunization with the PLGA nanoparticles. These results suggested that co-delivery of HBcAg and MPLA in PLGA nanoparticles promoted HBcAg-specific cellular immune responses. These findings suggest that appropriate design of the vaccine formulation and careful planning of the immunization schedule are important in the successful development of effective therapeutic vaccines for hepatitis B virus.
6 Targeting of APCs in Lymph Nodes with Nanoparticulate Systems
To improve the therapeutic potential of the nanoparticle-based nanoparticles for vaccine delivery, it is important to understand the physicochemical properties of nanoparticles affecting the biodistribution. To date, several reports have discussed the biodistribution of polymeric nanoparticles administered into the body [138–140]. The polymeric nanoparticles can be surface modified and functionalized to improve their biodistribution and also conjugated to targeting ligands which can direct nanoparticles to specific cells/tissues where drug delivery is desired. Polymer- and liposome-based delivery systems have focused primarily on vaccine delivery to peripheral DCs, where they first internalize the particles and then migrate to lymph nodes to activate T cells [141]. However, targeting DCs in vivo is very difficult because, in normal tissues, they exist in significantly lower numbers than other APCs such as macrophages. To overcome this problem, Kwon et al. prepared acid-degradable particles conjugated with anti-DEC-205 (anti-CD205) monoclonal Abs (mAbs). DEC-205 is an endocytosis receptor that is only expressed by lymphoid, interstitial, epidermal Langerhans DCs and thymic endothelial cells. Anti-DEC-205 mAb-conjugated particles increased receptor-mediated uptake of the particles by DCs as well as migration of particle-carrying DCs to lymph nodes and stimulation of naive T cells leading to enhanced cellular immune response [142]. Some subsets of DCs including plasmacytoid DCs (pDCs), which are known to play an important role in bridging the innate and adaptive immunities, do not express DEC-205. Therefore, the use of particles conjugated with anti-DEC-205 mAb is not suitable for targeting of pDCs. To further enhance targeting efficiency for DCs and reduce an unexpected toxicity, the use of a particle conjugated with a specific DC targeting molecule would be more beneficial.
A substantial fraction of resident DCs in lymph nodes are phenotypically immature and capable of internalizing antigens and particulate materials. Thus, resident APCs in lymph node may also be utilized as targets for vaccine antigens [143]. Therefore, antigen direct delivery to lymph nodes might provide an attractive alternative, because DCs are present in much higher concentration in these lymph nodes. It has been reported that delivery of particulate antigens to lymph nodes is affected by the size of nanoparticles [144]. Reddy et al. investigated the delivery of 20-, 45-, and 100-nm-sized poly(ethylene glycol) (PEG)-stabilized poly(propylene sulfide) (PPS) nanoparticles to DCs in the lymph nodes. The 20 nm particles were most readily taken up into the lymphatics following interstitial injection. The nanoparticles were internalized by up to 40–50 % of lymph node DCs, and the site of internalization was in the lymph nodes rather than at the injection site [145]. In mouse immunization study, OVA-conjugated 20 nm particles produced strong levels of immune response compared to 100 nm particles. The results indicate that by controlling size, PPS nanoparticles can be effectively taken up into the lymphatics as well as retained in lymph nodes without using any specific targeting ligand. In addition, these findings suggest that antigen delivery to lymph nodes is an important strategy for vaccine developments. Vila et al. also demonstrated that the size of PLA–PEG particles affects the nasal transport of the encapsulated protein and lymph node uptake of nasal-administered particles. The tissue levels following nasal administration of tetanus toxoid (TT) encapsulated into PLA–PEG particles (200 nm, 1.5, 5, and 10 μm) were investigated. The efficacy of transport to lymph nodes was related to the particle size, reaching the most important transport for the smallest (200 nm) particle size [146]. The results suggest that the PLA–PEG nanoparticles could be transported through the nasal mucosa and reach the subepithelial layer which is highly irrigated by lymph and capillary vessels. From these observations, it was found that uptake of particles in regional lymph nodes after systemic or mucosal administration is affected by the size of particles.
7 Conclusion
Many of the vaccines currently in development are based on purified subunits, recombinant proteins, or synthetic peptides. This new generation of antigens is less immunogenic than traditional vaccines and has better delivery systems, and immunostimulants are required to induce acceptable immune responses. Polymeric nano-/microparticles have been shown to possess significant potential as antigen delivery systems. In particular, biodegradable polymeric nanoparticles with entrapped antigens, such as proteins, peptides, or DNA, represent an exciting approach to control the intracellular release of antigens and to optimize the desired immune response via selective targeting of the antigen to APCs. The efficient delivery of antigens to APCs, especially in DCs, is one of the most important issues in the development of effective vaccines. Using nanoparticle-based vaccine delivery systems, it is possible to target delivery to DCs. The nanoparticle surfaces can be conjugated with DC-specific antibodies or ligands to increase targeting specificity. Polymeric nanoparticles are suitable for conjugation with antigens and can protect the antigen from degradation in vivo. Following uptake of the nanoparticles by DCs, the antigens are released intracellularly in a manner that can activate MHC class I and II pathways and, therefore, induce both CD4+ and CD8+ T-cell immunity. To deliver exogenous antigen for inducing cellular immunity through the MHC class I pathway can be an important problem, as internalized antigen-conjugated nanoparticles are mostly trafficked from endosomes to lysosomes. To avoid lysosomal trafficking, pH-responsive nanoparticles have been studied to disrupt endosomes in a pH-dependent fashion. For successfully targeting lymph-node-resident DCs, it is crucial to engineer nanoparticles that can be readily taken up into lymphatic vessels after subcutaneous injection and can then be retained in draining lymph nodes. It has been well established that particle size is among the most crucial factors for DC and lymphatic uptake.
Polymeric nanoparticles can also be used as synthetic immunostimulants to induce DC maturation and initiate adaptive immune responses. The mechanisms of DC activation by nanoparticles, as an immunostimulant, are not fully understood. DC maturation by nanoparticles may be related to Toll-like receptors (TLRs) of DCs. However, it has been reported that LPS contamination of gold nanoparticle preparations can stimulate DC maturation [147]. It is well known that LPS mainly interacts with TLR4 and induces DC maturation. In addition, LPS might act in synergy with these nanoparticles to activate/mature DCs. A trace of LPS in the nanoparticle might induce endotoxic effects. For clinical application of nanoparticle-based vaccine, this problem is a fundamental issue that cannot be avoided. To avoid misinterpretation of results, the production processes and handling of polymeric nanoparticles for vaccine use have to get plenty of attention.
There is a growing interest in identifying the relationship between the size of nanoparticles and their adjuvant activities, but the results from recent studies remain controversial. Many investigators are in agreement that the size of the particles is crucial to their adjuvant activities. Some factors may affect to the conflicting findings which include (1) polymeric materials used to form the particles, (2) nature of antigens used, (3) methods of antigen conjugation, and (4) immunization routes of antigens [148]. To clear the factor of particles that influence the adjuvant activity, there is a need to more comprehensively compare immune responses induced by precisely size-controlled nanoparticles prepared with the same materials and loaded with the same antigens by the proper method.
References
Singh M, O’Hagan DT (1999) Advances in vaccine adjuvants. Nat Biotechnol 17:1075–1081
Singh M, O’Hagan DT (2002) Recent advances in vaccine adjuvants. Pharm Res 19:715–728
Peek LJ, Middaugh CR, Berkland C (2008) Nanotechnology in vaccine delivery. Adv Drug Deliv Rev 60:915–928
Rice-Ficht AC, Arenas-Gamboa AM, Kahl-McDonagh MM, Ficht TA (2010) Polymeric particles in vaccine delivery. Curr Opin Microbiol 13:106–112
De Koker S, Lambrecht BN, Willart MA, van Kooyk Y, Grooten J, Vervaet C, Remon JP, De Geest BG (2011) Designing polymeric particles for antigen delivery. Chem Soc Rev 40:320–339
O’Hagan DT, Valiante NM (2003) Recent advances in the discovery and delivery of vaccine adjuvants. Nat Rev Drug Discov 2:727–735
Marrack P, McKee AS, Munks MW (2009) Towards an understanding of the adjuvant action of aluminium. Nat Rev Immunol 9:287–293
Gupta RK (1998) Aluminum compounds as vaccine adjuvants. Adv Drug Deliv Rev 32:155–172
Brewer JM (2006) How do aluminium adjuvants work? Immunol Lett 102:10–15
Hans ML, Lowman AM (2002) Biodegradable nanoparticles for drug delivery and targeting. Curr Opin Solid State Mater Sci 6:319–327
Greenland JR, Letvin NL (2007) Chemical adjuvants for plasmid DNA vaccines. Vaccine 25:3731–3741
Lu JM, Wang X, Marin-Muller C, Wang H, Lin PH, Yao Q, Chen C (2009) Current advances in research and clinical applications of PLGA-based nanotechnology. Expert Rev Mol Diagn 9:325–341
Panyam J, Labhasetwar V (2003) Biodegradable nanoparticles for drug and gene delivery to cells and tissue. Adv Drug Deliv Rev 55:329–347
Vasir JK, Labhasetwar V (2007) Biodegradable nanoparticles for cytosolic delivery of therapeutics. Adv Drug Deliv Rev 59:718–728
Kreuter J (1996) Nanoparticles and microparticles for drug and vaccine delivery. J Anat 189:503–505
O’Hagan DT, Jeffery H, Davis SS (1994) The preparation and characterization of poly(lactide-co-glycolide) microparticles: III. Microparticle/polymer degradation rates and the in vitro release of a model protein. Int J Pharm 103:37–45
Li X, Deng X, Yuan M, Xiong C, Huang Z, Zhang Y, Jia W (2000) In vitro degradation and release profiles of poly-DL-lactide-poly(ethylene glycol) microspheres with entrapped proteins. J Appl Polym Sci 78:140–148
Liggins RT, Burt HM (2001) Paclitaxel loaded poly(L-lactic acid) microspheres: properties of microspheres made with low molecular weight polymers. Int J Pharm 222:19–33
Lemoine D, Francois C, Kedzierewicz F, Preat V, Hoffman M, Maincent P (1996) Stability study of nanoparticles of poly(ε-caprolactone), poly(D,L-lactide) and poly(D,L-lactide-co-glycolide). Biomaterials 17:2191–2197
Jiang W, Gupta RK, Deshpande MC, Schwendeman SP (2005) Biodegradable poly(lactic-co-glycolic acid) microparticles for injectable delivery of vaccine antigens. Adv Drug Deliv Rev 57:391–410
Mohamed F, van der Walle CF (2008) Engineering biodegradable polyester particles with specific drug targeting and drug release properties. J Pharm Sci 97:71–87
Kumari A, Yadav SK, Yadav SC (2009) Biodegradable polymeric nanoparticles based drug delivery systems. Colloids Surf B 75:1–18
Tamber H, Johansen P, Merkle HP, Gander B (2005) Formulation aspects of biodegradable polymeric microspheres for antigen delivery. Adv Drug Deliv Rev 57:357–376
Mundargi RC, Babu VR, Rangaswamy V, Patel P, Aminabhavi TM (2008) Nano/micro technologies for delivering macromolecular therapeutics using poly(D,L-lactide-co-glycolide) and its derivatives. J Control Release 125:193–209
Sah H (1999) Stabilization of proteins against methylene chloride/water interface induced denaturation and aggregation. J Control Release 58:143–151
Panyam J, Dali MM, Sahoo SK, Ma W, Chakravarthi SS, Amidon GL, Levy RJ, Labhasetwar V (2003) Polymer degradation and in vitro release of a model protein from poly(D, L-lactide-co-glycolide) nano- and microparticles. J Control Release 92:173–187
Kakizawa Y, Kataoka K (2002) Block copolymer micelles for delivery of gene and related compounds. Adv Drug Deliv Rev 54:203–222
Zhang L, Eisenberg A (1995) Multiple morphologies of crew-cut aggregates of polystyrene-b-poly(acrylic acid) block copolymers. Science 1268:1728–1731
Dou H, Jiang M, Peng H, Chen D, Hong Y (2003) pH-dependent self-assembly: micellization and micelle-hollow-sphere transition of cellulose-based copolymers. Angew Chem Int Ed 42:1516–1519
Reihs T, Muller M, Lunkwitz K (2004) Preparation and adsorption of refined polyelectrolyte complex nanoparticles. J Colloid Interface Sci 271:69–79
Kang N, Perron ME, Prudhomme RE, Zhang Y, Gaucher G, Leroux JC (2005) Stereocomplex block copolymer micelles: core-shell nanostructures with enhanced stability. Nano Lett 5:315–319
Gaucher G, Dufresne MH, Sant VP, Kang N, Maysinger D, Leroux JC (2005) Block copolymer micelles: preparation, characterization and application in drug delivery. J Control Release 109:169–188
Letchford K, Burt H (2007) A review of the formation and classification of amphiphilic block copolymer nanoparticulate structures: micelles, nanospheres, nanocapsules and polymersomes. Eur J Pharm Biopharm 65:259–269
Holowka EP, Pochan DJ, Deming TJ (2005) Charged polypeptide vesicles with controllable diameter. J Am Chem Soc 127:12423–12428
Matsusaki M, Hiwatari K, Higashi M, Kaneko T, Akashi N (2004) Stably-dispersed and surface-functional bionanoparticles prepared by self-assembling amphipathic polymers of hydrophilic poly(γ-glutamic acid) bearing hydrophobic amino acids. Chem Lett 33:398–399
Matsusaki M, Fuchida T, Kaneko T, Akashi M (2005) Self-assembling bionanoparticles of poly(ε-lysine) bearing cholesterol as a biomesogen. Biomacromolecules 6:2374–2379
Arimura H, Ohya Y, Ouchi T (2005) Formation of core-shell type biodegradable polymeric micelles from amphiphilic poly(aspartic acid)-block-polylactide diblock copolymer. Biomacromolecules 6:720–725
Akiyoshi K, Ueminami A, Kurumada S, Nomura Y (2000) Self-association of cholesteryl-bearing poly(L-lysine) in water and control of its secondary structure by host-guest interaction with cyclodextrin. Macromolecules 33:6752–6756
Holowka EP, Sun VZ, Kamei DT, Deming TJ (2007) Polyarginine segments in block copolypeptides drive both vesicular assembly and intracellular delivery. Nat Mater 6:52–57
Jeong JH, Kang HS, Yang SR, Kim JD (2003) Polymer micelle-like aggregates of novel amphiphilic biodegradable poly(asparagine) grafted with poly(caprolactone). Polymer 44:583–591
Kataoka K, Matsumoto T, Yokoyama M, Okano T, Sakurai Y, Fukushima S, Okamoto K, Kwon GS (2000) Doxorubicin-loaded poly(ethylene glycol)-poly(β-benzyl-L-aspartate) copolymer micelles: their pharmaceutical characteristics and biological significance. J Control Release 64:143–153
Lin J, Zhang S, Chen T, Lin S, Jin H (2007) Micelle formation and drug release behavior of polypeptide graft copolymer and its mixture with polypeptide block copolymer. Int J Pharm 336:49–57
Lee ES, Shin HJ, Na K, Bae YH (2003) Poly(L-histidine)-PEG block copolymer micelles and pH-induced destabilization. J Control Release 90:363–374
Kubota H, Matsunobu T, Uotani K, Takebe H, Satoh A, Tanaka T, Taniguchi M (1993) Production of poly(γ-glutamic acid) by Bacillus subtilis F-2-01. Biosci Biotech Biochem 57:1212–1213
King EC, Watkins WJ, Blacker AJ, Bugg TDH (1998) Covalent modification in aqueous solution of poly-γ-D-glutamic acid from Bacillus licheniformis. J Polym Sci A Polym Chem 36:1995–1999
Morillo M, de Ilarduya AM, Munoz-Guerra S (2001) Comblike alkyl esters of biosynthetic poly(γ-glutamic acid) 1 Synthesis and characterization. Macromolecules 34:7868–7875
Prodhomme EJF, Tutt AL, Glennie MJ, Bugg TDH (2003) Multivalent conjugates of poly-γ-D-glutamic acid from Bacillus licheniformis with antibody F(ab′) and glycopeptide ligands. Bioconj Chem 14:1148–1155
Tachibana Y, Kurisawa M, Uyama H, Kobayashi S (2003) Thermo- and pH-responsive biodegradable poly(α-N-substituted γ-glutamine)s. Biomacromolecules 4:1132–1134
Shimokuri T, Kaneko T, Serizawa T, Akashi M (2004) Preparation and thermosensitivity of naturally occurring polypeptide poly(γ-glutamic acid) derivatives modified by alkyl groups. Macromol Biosci 4:407–411
Oppermann FB, Fickaitz S, Steinbiichel A (1998) Biodegradation of polyamides. Polym Degrad Stab 59:337–344
Obst M, Steinbuchel A (2004) Microbial degradation of poly(amino acid)s. Biomacromolecules 5:1166–1176
Schneerson R, Kubler-Kielb J, Liu TY, Dai ZD, Leppla SH, Yergey A, Backlund P, Shiloach J, Majadly F, Robbins JB (2003) Poly(γ-D-glutamic acid) protein conjugates induce IgG antibodies in mice to the capsule of Bacillus anthracis: a potential addition to the anthrax vaccine. Proc Natl Acad Sci U S A 100:8945–8950
Rhie GE, Roehrl MH, Mourez M, Collier RJ, Mekalanos JJ, Wang JY (2003) A dually active anthrax vaccine that confers protection against both bacilli and toxins. Proc Natl Acad Sci U S A 100:10925–10930
Wang TT, Fellows PF, Leighton TJ, Lucas AH (2004) Induction of opsonic antibodies to the gamma-D-glutamic acid capsule of Bacillus anthracis by immunization with a synthetic peptide-carrier protein conjugate. FEMS Immunol Med Microbiol 40:231–237
Joyce J, Cook J, Chabot D, Hepler R, Shoop W, Xu Q, Stambaugh T, Aste-Amezaga M, Wang S, Indrawati L, Bruner M, Friedlander A, Keller P, Caulfield M (2006) Immunogenicity and protective efficacy of Bacillus anthracis poly-γ-D-glutamic acid capsule covalently coupled to a protein carrier using a novel triazine-based conjugation strategy. J Biol Chem 281:4831–4843
Kubler-Kielb J, Liu TY, Mocca C, Majadly F, Robbins JB, Schneerson R (2006) Additional conjugation methods and immunogenicity of Bacillus anthracis poly-γ-D-glutamic acid-protein conjugates. Infect Immun 74:4744–4749
Shih IL, Van YT (2001) The production of poly(γ-glutamic acid) from microorganisms and its various application. Bioresour Technol 79:207–225
Kaneko T, Higashi M, Matsusaki M, Akagi T, Akashi M (2005) Self-assembled soft nanofibrils of amphipathic polypeptides and their morphological transformation. Chem Mater 17:2484–2486
Akagi T, Baba M, Akashi M (2007) Preparation of nanoparticles by the self-organization of polymers consisting of hydrophobic and hydrophilic segments: potential applications. Polymer 48:6729–6747
Kim H, Akagi T, Akashi M (2009) Preparation of size tunable amphiphilic poly(amino acid) nanoparticles. Macromol Biosci 9:842–848
Akagi T, Kaneko T, Kida T, Akashi M (2005) Preparation and characterization of biodegradable nanoparticles based on poly(γ-glutamic acid) with L-phenylalanine as a protein carrier. J Control Release 108:226–236
Akagi T, Kaneko T, Kida T, Akashi M (2006) Multifunctional conjugation of proteins on/into core-shell type nanoparticles prepared by amphiphilic poly(γ-glutamic acid). J Biomater Sci Polym Ed 17:875–892
Portilla-Arias JA, Camargo B, Garcia-Alvarez M, de Ilarduya AM, Munoz-Guerra S (2009) Nanoparticles made of microbial poly(γ-glutamate)s for encapsulation and delivery of drugs and proteins. J Biomater Sci Polym Ed 20:1065–1079
Bodnar M, Kjoniksen AL, Molnar RM, Hartmann JF, Daroczi L, Nystrom B, Borbely J (2008) Nanoparticles formed by complexation of poly-γ-glutamic acid with lead ions. J Hazard Mater 153:1185–1192
Radu JEF, Novak L, Hartmann JF, Beheshti N, Kjoniksen AL, Nystrom B, Borbely J (2008) Structural and dynamical characterization of poly-γ-glutamic acid-based cross-linked nanoparticles. Colloid Polym Sci 286:365–376
Akiyoshi K, Kobayashi S, Shichibe S, Mix D, Baudys M, Kim SW, Sunamoto J (1998) Self-assembled hydrogel nanoparticle of cholesterol-bearing pullulan as a carrier of protein drugs: complexation and stabilization of insulin. J Control Release 54:313–320
Jung SW, Jeong Y, Kim SH (2003) Characterization of hydrophobized pullulan with various hydrophobicities. Int J Pharm 254:109–121
Na K, Park KH, Kim SW, Bae YH (2000) Self-assembled hydrogel nanoparticles from curdlan derivatives: characterization, anti-cancer drug release and interaction with a hepatoma cell line (HepG2). J Control Release 69:225–236
Gref R, Rodrigues J, Couvreur P (2002) Polysaccharides grafted with polyesters: novel amphiphilic copolymers for biomedical applications. Macromolecules 35:9861–9867
Leonard M, Boisseson MRD, Hubert P, Dalenccon F, Dellacherie E (2004) Hydrophobically modified alginate hydrogels as protein carriers with specific controlled release properties. J Control Release 98:395–405
Park JH, Kwona S, Nam JO, Park RW, Chung H, Seo SB, Kim IS, Kwon IC, Jeong SY (2004) Self-assembled nanoparticles based on glycol chitosan bearing 5h-cholanic acid for RGD peptide delivery. J Control Release 95:579–588
Akiyoshi K, Deguchi S, Moriguchi N, Yamaguchi S, Sunamoto J (1993) Self-aggregates of hydrophobized polysaccharides in water. Formation and characteristics of nanoparticles. Macromolecules 26:3062–3068
Hsieh CY, Tsai SP, Wang DM, Chang YN, Hsieh HJ (2005) Preparation of γ-PGA/chitosan composite tissue engineering matrices. Biomaterials 26:5617–5623
Kang HS, Park SH, Lee YG, Son I (2007) Polyelectrolyte complex hydrogel composed of chitosan and poly(γ-glutamic acid) for biological application: preparation, physical properties, and cytocompatibility. J Appl Polym Sci 103:386–394
Kim YH, Gihm SH, Park CR, Lee KY, Kim TW, Kwon IC, Chung H, Jeong SY (2001) Structural characteristics of size-controlled self-aggregates of deoxycholic acid-modified chitosan and their application as a DNA delivery carrier. Bioconj Chem 12:932–938
Lee KY, Jo WH, Kwon IC, Kim YH, Jeong SY (1998) Structural determination and interior polarity of self-aggregates prepared from deoxycholic acid-modified chitosan in water. Macromolecules 31:378–383
Kida T, Inoue K, Akagi T, Akashi M (2007) Preparation of novel polysaccharide nanoparticles by the self-assembly of amphiphilic pectins and their protein-encapsulation ability. Chem Lett 36:940–941
Banchereau J, Steinman RM (1998) Dendritic cells and the control of immunity. Nature 392:245–252
Gamvrellis A, Leong D, Hanley JC, Xiang SD, Mottram P, Plebanski M (2004) Vaccines that facilitate antigen entry into dendritic cells. Immunol Cell Biol 82:506–516
Zhang S, Li J, Lykotrafitis G, Bao G, Suresh S (2009) Size-dependent endocytosis of nanoparticles. Adv Mater 21:419–424
Akagi T, Wang X, Uto T, Baba M, Akashi M (2007) Protein direct delivery to dendritic cells using nanoparticles based on amphiphilic poly(amino acid) derivatives. Biomaterials 28:3427–3436
Uto T, Wang X, Sato K, Haraguchi M, Akagi T, Akashi M, Baba M (2007) Targeting of antigen to dendritic cells with poly(γ-glutamic acid) nanoparticles induce antigen-specific humoral and cellular immunity. J Immunol 178:2979–2986
Uto T, Akagi T, Hamasaki T, Akashi M, Baba M (2009) Modulation of innate and adaptive immunity by biodegradable nanoparticles. Immunol Lett 125:46–52
Akagi T, Kim H, Akashi M (2010) pH-dependent disruption of erythrocyte membrane by amphiphilic poly(amino acid) nanoparticles. J Biomater Sci Polym Ed 21:315–328
Lutsiak ME, Robinson DR, Coester C, Kwon GS, Samuel J (2002) Analysis of poly(D, L-lactic-co-glycolic acid) nanosphere uptake by human dendritic cells and macrophages in vitro. Pharm Res 19:1480–1487
Elamanchili P, Diwan M, Cao M, Samuel J (2004) Characterization of poly(D,L-lactic-co-glycolic acid) based nanoparticulate system for enhanced delivery of antigens to dendritic cells. Vaccine 22:2406–2412
Copland MJ, Baird MA, Rades T, McKenzie JL, Becker B, Reck F, Tyler PC, Davies NM (2003) Liposomal delivery of antigen to human dendritic cells. Vaccine 21:883–890
Foged C, Brodin B, Frokjaer S, Sundblad A (2005) Particle size and surface charge affect particle uptake by human dendritic cells in an in vitro model. Int J Pharm 298:315–322
Kanchan V, Panda AK (2007) Interactions of antigen-loaded polylactide particles with macrophages and their correlation with the immune response. Biomaterials 28:5344–5357
Cohen JA, Beaudette TT, Tseng WW, Bachelder EM, Mende I, Engleman EG, Fréchet JM (2009) T-cell activation by antigen-loaded pH-sensitive hydrogel particles in vivo: the effect of particle size. Bioconj Chem 20:111–119
Champion JA, Mitragotri S (2006) Role of target geometry in phagocytosis. Proc Natl Acad Sci U S A 103:4930–4934
Champion JA, Mitragotri S (2009) Shape induced inhibition of phagocytosis of polymer particles. Pharm Res 26:244–249
O’Hagan DT (1998) Recent advances in immunological adjuvants: the development of particulate antigen delivery systems. Expert Opin Invest Drugs 7:349–359
Storni T, Kundig TM, Senti G, Johansen P (2005) Immunity in response to particulate antigen-delivery systems. Adv Drug Deliv Rev 57:333–355
Shen H, Ackerman AL, Cody V, Giodini A, Hinson ER, Cresswell P, Edelson RL, Saltzman WM, Hanlon DJ (2006) Enhanced and prolonged cross-presentation following endosomal escape of exogenous antigens encapsulated in biodegradable nanoparticles. Immunology 117:78–88
Plank C, Zauner W, Wagner E (1998) Application of membrane-active peptides for drug and gene delivery across cellular membranes. Adv Drug Deliv Rev 34:21–35
Shai Y (1999) Mechanism of the binding, insertion and destabilization of phospholipid bilayer membranes by α-helical antimicrobial and cell non-selective membrane-lytic peptides. Biochim Biophys Acta 1462:55–70
Yessine MA, Leroux JC (2004) Membrane-destabilizing polyanions: interaction with lipid bilayers and endosomal escape of biomacromolecules. Adv Drug Deliv Rev 56:999–1021
Chen R, Yue Z, Eccleston ME, Williams S, Slater NK (2005) Modulation of cell membrane disruption by pH-responsive pseudo-peptides through grafting with hydrophilic side chains. J Control Release 108:63–72
Murthy N, Xu M, Schuck S, Kunisawa J, Shastri N, Fréchet JM (2003) A macromolecular delivery vehicle for protein-based vaccines: acid-degradable protein-loaded microgels. Proc Natl Acad Sci U S A 29:4995–5000
Standley SM, Kwon TJ, Murthy N, Kunisawa J, Shastri N, Guillaudeu SJ, Lau L, Fréchet JM (2004) Acid-degradable particles for protein-based vaccines: enhanced survival rate for tumor-challenged mice using ovalbumin model. Bioconj Chem 15:1281–1288
Hu Y, Litwin T, Nagaraja AR, Kwong B, Katz J, Watson N, Irvine DJ (2007) Cytosolic delivery of membrane-impermeable molecules in dendritic cells using pH-responsive core-shell nanoparticles. Nano Lett 7:3056–3064
Boussif O, Lezoualc’h F, Zanta MA, Mergny MD, Scherman D, Demeneix B, Behr JP (1995) A versatile vector for gene and oligonucleotide transfer into cells in culture and in vivo. Proc Natl Acad Sci U S A 92:7297–7301
Murthy N, Robichaud JR, Tirrell DA, Stayton PS, Hoffman AS (1999) The design and synthesis of polymers for eukaryotic membrane disruption. J Control Release 61:137–143
Jones RA, Cheung CY, Black FE, Zia JK, Stayton PS, Hoffman AS, Wilson MR (2003) Poly(2-alkylacrylic acid) polymers deliver molecules to the cytosol by pH-sensitive disruption of endosomal vesicles. Biochem J 372:65–75
Kusonwiriyawong C, van de Wetering P, Hubbell JA, Merkle HP, Walter E (2003) Evaluation of pH-dependent membrane-disruptive properties of poly(acrylic acid) derived polymers. Eur J Pharm Biopharm 56:237–246
Yessine MA, Meier C, Petereit HU, Leroux JC (2006) On the role of methacrylic acid copolymers in the intracellular delivery of antisense oligonucleotides. Eur J Pharm Biopharm 63:1–10
Foster S, Duvall CL, Crownover EF, Hoffman AS, Stayton PS (2010) Intracellular delivery of a protein antigen with an endosomal-releasing polymer enhances CD8 T-cell production and prophylactic vaccine efficacy. Bioconj Chem 21:2205–2212
Yoshikawa T, Okada N, Oda A, Matsuo K, Matsuo K, Mukai Y, Yoshioka Y, Akagi T, Akashi M, Nakagawa S (2008) Development of amphiphilic γ-PGA-nanoparticle based tumor vaccine: potential of the nanoparticulate cytosolic protein delivery carrier. Biochem Biophys Res Commun 366:408–413
Panyam J, Zhou WZ, Prabha S, Sahoo SK, Labhasetwar V (2002) Rapid endo-lysosomal escape of poly(dl-lactide-co-glycolide) nanoparticles: implications for drug and gene delivery. FASEB J 16:1217–1226
Reddy ST, Swartz MA, Hubbell JA (2006) Targeting dendritic cells with biomaterials: developing the next generation of vaccines. Trends Immunol 27:573–579
Jones KS (2008) Biomaterials as vaccine adjuvants. Biotechnol Prog 24:807–814
Babensee JE (2007) Interaction of dendritic cells with biomaterials. Semin Immunol 20:101–108
Jilek S, Merkle HP, Walter E (2005) DNA-loaded biodegradable microparticles as vaccine delivery systems and their interaction with dendritic cells. Adv Drug Deliv Rev 57:377–390
Black M, Trent A, Tirrell M, Olive C (2010) Advances in the design and delivery of peptide subunit vaccines with a focus on toll-like receptor agonists. Expert Rev Vaccines 9:157–173
Kawai T, Akira S (2005) Pathogen recognition with Toll-like receptors. Curr Opin Immunol 17:338–344
Kim TW, Lee TY, Bae HC, Hahm JH, Kim YH, Park C, Kang TH, Kim CJ, Sung MH, Poo H (2007) Oral administration of high molecular mass poly-γ-glutamate induces NK cell-mediated antitumor immunity. J Immunol 179:775–780
Lee TY, Kim YH, Yoon SW, Choi JC, Yang JM, Kim CJ, Schiller JT, Sung MH, Poo HR (2009) Oral administration of poly-γ-glutamate induces TLR4- and dendritic cell-dependent antitumor effect. Cancer Immunol Immunother 58:1781–1794
Tamayo I, Irache JM, Mansilla C, Ochoa-Repáraz J, Lasarte JJ, Gamazo C (2010) Poly(anhydride) nanoparticles act as active Th1 adjuvants through Toll-like receptor exploitation. Clin Vaccine Immunol 17:1356–1362
Okamoto S, Matsuura M, Akagi T, Akashi M, Tanimoto T, Ishikawa T, Takahashi M, Yamanishi K, Mori Y (2009) Poly(γ-glutamic acid) nano-particles combined with mucosal influenza virus hemagglutinin vaccine protects against influenza virus infection in mice. Vaccine 27:5896–5905
Yamaguchi S, Tatsumi T, Takehara T, Sasakawa A, Yamamoto M, Kohga K, Miyagi T, Kanto T, Hiramatsu N, Akagi T, Akashi M, Hayashi N (2010) EphA2-derived peptide vaccine with amphiphilic poly(gamma-glutamic acid) nanoparticles elicits an anti-tumor effect against mouse liver tumor. Cancer Immunol Immunother 59:759–767
Yoshida M, Babensee JE (2004) Poly(lactic-co-glycolic acid) enhances maturation of human monocyte-derived dendritic cells. J Biomed Mater Res 71:45–54
Jilek S, Ulrich M, Merkle HP, Walter E (2004) Composition and surface charge of DNA-loaded microparticles determine maturation and cytokine secretion in human dendritic cells. Pharm Res 21:1240–1247
Thiele L, Rothen-Rutishauser B, Jilek S, Wunderli-Allenspach H, Merkle HP, Walter E (2001) Evaluation of particle uptake in human blood monocyte-derived cells in vitro. Does phagocytosis activity of dendritic cells measure up with macrophages? J Control Release 76:59–71
Matsusaki M, Larsson K, Akagi T, Lindstedt M, Akashi M, Borrebaeck CA (2005) Nanosphere induced gene expression in human dendritic cells. Nano Lett 5:2168–2173
Kwon YJ, Standley SM, Goh SL, Frechet JM (2005) Enhanced antigen presentation and immunostimulation of dendritic cells using acid-degradable cationic nanoparticles. J Control Release 105:199–212
Raghuvanshi RS, Katare YK, Lalwani K, Ali MM, Singh O, Panda AK (2002) Improved immune response from biodegradable polymer particles entrapping tetanus toxoid by use of different immunization protocol and adjuvants. Int J Pharm 245:109–121
Ataman-Onal Y, Munier S, Ganee A, Terrat C, Durand PY, Battail N, Martinon F, Le Grand R, Charles MH, Delair T, Verrier B (2006) Surfactant-free anionic PLA nanoparticles coated with HIV-1 p24 protein induced enhanced cellular and humoral immune responses in various animal models. J Control Release 112:175–185
Hamdy S, Elamanchili P, Alshamsan A, Molavi O, Satou T, Samuel J (2007) Enhanced antigen-specific primary CD4+ and CD8+ responses by codelivery of ovalbumin and toll-like receptor ligand monophosphoryl lipid A in poly(D,L-lactic-co-glycolic acid) nanoparticles. J Biomed Mater Res A 81:652–662
Solbrig CM, Saucier-Sawyer JK, Cody V, Saltzman WM, Hanlon DJ (2007) Polymer nanoparticles for immunotherapy from encapsulated tumor-associated antigens and whole tumor cells. Mol Pharm 4:47–57
Wendorf J, Chesko J, Kazzaz J, Ugozzoli M, Vajdy M, O’Hagan D, Singh M (2008) A comparison of anionic nanoparticles and microparticles as vaccine delivery systems. Hum Vaccin 4:44–49
Hamdy S, Molavi O, Ma Z, Haddadi A, Alshamsan A, Gobti Z, Elhasi S, Samuel J, Lavasanifar A (2008) Co-delivery of cancer-associated antigen and Toll-like receptor 4 ligand in PLGA nanoparticles induces potent CD8+ T cell-mediated anti-tumor immunity. Vaccine 26:5046–5057
Caputo A, Sparnacci K, Ensoli B, Tondelli L (2008) Functional polymeric nano/microparticles for surface adsorption and delivery of protein and DNA vaccines. Curr Drug Deliv 5:230–242
Nayak B, Panda AK, Ray P, Ray AR (2009) Formulation, characterization and evaluation of rotavirus encapsulated PLA and PLGA particles for oral vaccination. J Microencapsul 26:154–165
Slutter B, Plapied L, Fievez V, Sande MA, Des Rieux A, Schneider YJ, Van Riet E, Jiskoot W, Préat V (2009) Mechanistic study of the adjuvant effect of biodegradable nanoparticles in mucosal vaccination. J Control Release 138:113–121
Gutierro I, Hernandez RM, Igartua M, Gascón AR, Pedraz JL (2002) Size dependent immune response after subcutaneous, oral and intranasal administration of BSA loaded nanospheres. Vaccine 21:67–77
Chong CS, Cao M, Wong WW, Fischer KP, Addison WR, Kwon GS, Tyrrell DL, Samuel J (2005) Enhancement of T helper type 1 immune responses against hepatitis B virus core antigen by PLGA nanoparticle vaccine delivery. J Control Release 102:85–99
Wilson KD, Raney SG, Sekirov L, Chikh G, de Jong SD, Cullis PR, Tam YK (2007) Effects of intravenous and subcutaneous administration on the pharmacokinetics, biodistribution, cellular uptake and immunostimulatory activity of CpG ODN encapsulated in liposomal nanoparticles. Int Immunopharmacol 7:1064–1075
He C, Hua Y, Yin L, Tang C, Yin C (2010) Effects of particle size and surface charge on cellular uptake and biodistribution of polymeric nanoparticles. Biomaterials 31:3657–3666
Decuzzi P, Godin B, Tanaka T, Lee SY, Chiappini C, Liu X, Ferrari M (2010) Size and shape effects in the biodistribution of intravascularly injected particles. J Control Release 141:320–327
Manolova V, Flace A, Bauer M, Schwarz K, Saudan P, Bachmann MF (2008) Nanoparticles target distinct dendritic cell populations according to their size. Eur J Immunol 38:1404–1413
Kwon YJ, James E, Shastri N, Fréchet JM (2005) In vivo targeting of dendritic cells for activation of cellular immunity using vaccine carriers based on pH-responsive microparticles. Proc Natl Acad Sci U S A 102:18264–18268
Reddy ST, van der Vlies AJ, Simeoni E, Angeli V, Randolph GJ, O’Neil CP, Lee LK, Swartz MA, Hubbell JA (2007) Exploiting lymphatic transport and complement activation in nanoparticle vaccines. Nat Biotechnol 25:1159–1164
Oussoren C, Storm G (2001) Liposomes to target the lymphatics by subcutaneous administration. Adv Drug Deliv Rev 50:143–156
Reddy ST, Rehor A, Schmoekel HG (2006) In vivo targeting of dendritic cells in lymph nodes with poly(propylene sulfide) nanoparticles. J Control Release 112:26–34
Vilaa A, Sancheza A, Evorab C, Soriano I, McCallion O, Alonso MJ (2005) PLA-PEG particles as nasal protein carriers: the influence of the particle size. Int J Pharm 292:43–52
Vallhov H, Qin J, Johansson SM, Ahlborg N, Muhammed MA, Scheynius A, Gabrielsson S (2006) The importance of an endotoxin-free environment during the production of nanoparticles used in medical applications. Nano Lett 6:1682–1686
Oyewumi MO, Kumar A, Cui Z (2010) Nano-microparticles as immune adjuvants: correlating particle sizes and the resultant immune responses. Expert Rev Vaccines 9:1095–1107
Acknowledgments
The authors thank Dr. M. Baba and Dr. T. Uto (Kagoshima University, Japan) for their helpful discussion.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer Japan
About this chapter
Cite this chapter
Akagi, T., Akashi, M. (2014). Functional Nanoparticles for Vaccine Delivery Systems. In: Akashi, M., Akagi, T., Matsusaki, M. (eds) Engineered Cell Manipulation for Biomedical Application. Nanomedicine and Nanotoxicology. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55139-3_12
Download citation
DOI: https://doi.org/10.1007/978-4-431-55139-3_12
Published:
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55138-6
Online ISBN: 978-4-431-55139-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)