Abstract
Transcranial Doppler ultrasonography (TCD) allows easy bedside monitoring of cerebral circulation and can be used repeatedly and continuously at low cost. A high level of skill is required to obtain a sonogram of an individual blood vessel through the transtemporal bone window with this technique. However, the use of transcranial color duplex imaging and the power motion mode has further facilitated the measurement of blood flow velocity in the brain by this method. Cerebral autoregulation and cerebrovascular CO2 reactivity can be determined by TCD and are useful prognostic indicators in patients with cerebral infarction, subarachnoid hemorrhage, or head trauma. Transcranial Doppler ultrasonography is also suitable in evaluating cerebrovascular stenosis, vasospasm following subarachnoid hemorrhage, vascular patency following cerebral infarction and cerebral circulation in patients with intracranial hypertension. Furthermore, microemboli that have disseminated to the brain during carotid endarterectomy or cardiovascular surgery can be detected by TCD as microembolic signals. New techniques to differentiate between gaseous and solid microemboli are currently under development. We anticipate that the utility of TCD as a useful bedside monitoring tool for evaluating cerebral circulation will become increasingly recognized.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Transcranial Doppler ultrasonography
- Cerebral autoregulation
- Cerebrovascular CO2 reactivity
- Vasospasm
- Microembolic signal
1 Introduction
Transcranial Doppler ultrasonography (TCD) was established in 1982 by Aaslid et al., who reported successful transcranial measurement of blood flow velocity in the internal carotid artery (ICA), middle cerebral artery (MCA), anterior cerebral artery (ACA), and posterior cerebral artery (PCA) using 2-MHz pulsed wave Doppler [1]. TCD allows easy bedside monitoring of the cerebral circulation and can be used repeatedly and continuously at low cost without requiring a special dye.
In this chapter, we explain the measurement principles of and locations assessed by TCD, the parameters of physiological cerebral circulation, and the cerebrovascular responses that TCD can measure. We also provide an account of the changes that occur in cerebral blood flow velocity under various pathologic conditions, including vascular stenosis, vasospasm, and intracranial hypertension, and show how they are evaluated. In addition, we describe the characteristics of and methods for evaluating the intracranially disseminated microembolic signals that can be detected by TCD. Finally, we discuss the utility of TCD in surgical cases.
2 TCD Measurement Principles, Locations Assessed, and Procedures
Let us first look at the principles which underlie measurement in TCD. Rather than continuous ultrasonic waves, pulse waves are used to ultrasonically assess cerebral blood flow velocity. Based on the principle that ultrasonic waves are reflected by sites with substantially different acoustic impedances, TCD can isolate ultrasonic waves reflected by red blood cells circulating in a blood vessel. The frequency of these waves varies according to flow velocity (the Doppler effect), allowing the flow velocity of the circulating blood cells to be determined. Based on the known propagation velocity of ultrasonic waves in brain tissue (1,530 m/s), blood flow velocity at a given depth can be determined by measuring the propagation time of the pulsed ultrasonic waves reflected by blood cells. Ultrasonic waves at a frequency ≤2 MHz can pass through the skull, with lower frequencies penetrating deeper into the brain.
In terms of locations assessed, TCD can be used to insonate the ACA (A1), MCA (M1 and M2), PCA, and terminal portion of the ICA, as well as the anterior and posterior communicating arteries, through the temporal bone window. The ophthalmic artery can be visualized through the transorbital window, while the basilar artery and vertebral artery can be visualized through the transforaminal window. The external carotid artery can be insonated from the submandibular region (Fig. 19.1).
Insonation area of cervicocerebral vasculature by transcranial Doppler. Yellow, through transtemporal window; blue, through transorbital window; red, through transforaminal window; and green, through submandibular region. MCA indicates middle cerebral artery, and M1, M2 and M3 are segments of this artery; ACA indicates anterior cerebral artery, and A1 and A2 are segments of this artery; P1 and P2 are segments of posterior cerebral artery: CCA, ICA, and ECA indicate common, internal, and external carotid arteries; TICA indicates the terminal portion of ICA; siphon indicates siphon portion of ICA; SCA indicates superior cerebellar artery; AComA and PComA indicates anterior and posterior communicating arteries; BA indicates basilar artery; AICA and PICA indicate anterior and posterior inferior cerebellar arteries; OA indicate ophthalmic artery; VA indicates vertebral artery; SubCA indicates subclavian artery. (Adapted and modified from reference [36])
Doppler signals obtained by TCD can be visualized as sonograms by adjusting the depth of each target blood vessel (Fig. 19.2). From these sonograms, peak systolic velocity (PSV), end-diastolic velocity (EDV), and mean flow velocity (Vmean) can be determined, and, subsequently from these values, the pulsatility index (PI) can be calculated:
Usually, the Vmean value in the MCA, where the ultrasonic irradiation angle is almost parallel to the blood flow, provides the most accurate estimate of blood flow velocity. Blood flow velocity in the MCA can be detected at a depth of 35–65 mm, with a Vmean of 45–70 cm/s. The MCA is the only artery whose Vmean can be constantly determined at a depth of ≥20 mm. However, since 10 % of patients lack a temporal bone window, insonation of the MCA is difficult in some cases, especially in elderly and female patients [2].
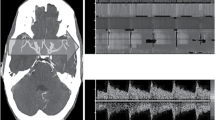
Although a high level of skill is required to obtain a sonogram of an individual blood vessel through the transtemporal bone window by TCD, recent technical innovations have facilitated the visualization of blood vessels. One such innovation is transcranial color duplex imaging, where the depth and blood flow of blood vessels are transcranially visualized by color Doppler imaging (Fig. 19.3). With this technique, the depth, location, and sample volume of the target vessel can be determined. Another innovation is the power motion mode, which enables the identification and visualization of all blood vessels in the Doppler beam by collecting blood flow information from multiple sample volumes (usually 8) within the range of the set depth (Fig. 19.4).
Normal vessel appearance on transtemporal transcranial color duplex imaging M1 and M2 indicate M1 and M2 segments of the middle cerebral artery; TICA indicates terminal portion of the internal carotid artery; A1 and A2 indicate segments of the anterior cerebral artery; P1 and P2 indicate segments of the posterior cerebral artery; SCA indicates superior cerebellar artery; BAT indicates basilar artery. (Adapted and modified from reference [36])
3 Physiological Parameters Measurable by TCD
TCD measures only the blood flow velocity of insonated cerebral blood vessels, not actual blood flow. Thus, assuming that the diameter of the target blood vessel is not significantly affected by physiological changes, any change in cerebral blood flow velocity should reflect a relative change in cerebral blood flow. In fact, the diameter of the MCA, as measured by magnetic resonance imaging or visually by craniotomy, does not substantially change, even with a change in blood pressure, CO2 load, or stand-up load [3–5]. Furthermore, Vmean as determined by TCD correlates well with cerebral blood flow velocity as measured by N2O inhalation (as described by Kety and Schmidt) or 133Xe inhalation [6], suggesting that changes in Vmean reflect relative changes in cerebral blood flow.
3.1 Evaluation of Cerebral Autoregulation
Cerebral autoregulation (CA) is a mechanism that maintains the cerebral blood flow at a constant level against varying mean arterial blood pressure (MAP). There are two types of CA: static CA, which maintains cerebral blood flow against a mild change in MAP, and dynamic CA, which maintains cerebral blood flow against a rapid change in MAP. Evaluating CA is important because impaired CA results in either decreased blood pressure, which is associated with an increased risk of cerebral ischemia, or increased blood pressure, which is associated with an increased risk of cerebral hemorrhage.
3.1.1 Evaluation of Static CA
Slow and continuous intravenous infusion of phenylephrine in increments of 20 mmHg gradually increases MAP. Mean arterial pressure and Vmean are measured before and after phenylephrine infusion. The percent change in cerebral vascular resistance (%CVR) per percent change in MAP (%MAP) is calculated as static CA (sCA%) using the following formulas:
Here, sCA% ≥20 is defined as normal vascular response [7].
It is typically understood that cerebral blood flow is regulated to maintain the MAP between 60 and 150 mmHg [8]. However, recent studies using TCD have shown that Vmean increases slightly depending on even this range of MAP at a constant rate [9].
3.1.2 Evaluation of Dynamic CA
Even after a rapid change in MAP, dynamic CA settles the cerebral blood flow to a constant level within 5 s. Dynamic CA can be evaluated by TCD by inducing a rapid change in blood pressure by mechanical or chemical stimulation or by making use of spontaneous fluctuations in MAP.
3.1.2.1 Suprasystolic Thigh Cuff Method
After inflating a thigh cuff to achieve a blood pressure of 30 mmHg above the systolic level and maintaining it for 2–3 min, rapid release of the cuff decreases MAP by about 15 mmHg. As a parameter of dynamic CA against this rapid change in MAP, the rate of regulation (RoR) is calculated as follows:
The change in MAP is measured over 2.5 s, from 1 to 3.5 s after cuff release, where CVR is calculated by multiplying MAP by Vmean−1 and Δt is 2.5 s (Fig. 19.5a) [10]. Vmean decreases with decrease in MAP over the first 1 s after cuff release, after which CVR decreases with continued decreases in MAP (Fig. 19.5b) and Vmean recovers to the level before cuff release. The normal value for RoR is 20 and a value close to 0 indicates impaired dynamic CA [10]. The autoregulation index is calculated by normalizing the pattern of change in Vmean over time so that evaluation can be made by determining which pattern most accurately describes the observed change in Vmean (Fig. 19.5c). An autoregulation index of ≥5 is defined as normal dynamic CA [10].
Typical changes in mean arterial pressure (MAP), mean flow velocity (Vmean) (a), and cerebrovascular resistance in response to suprasystolic thigh cuff deflation to determine dynamic cerebral autoregulation (b). MAP and Vmean decreased simultaneously during first second after tight cuff was released following earlier recovery of Vmean during next seconds than MAP (a). All tracings are shown in normalized units relative to control prerelease values from −4 to 0 s. Straight line (bold line) through cerebral vascular resistance curve (b) was determined by regression analysis of data obtained from 1 to 3.5 s after thigh cuff release and used to calculate rate of regulation. Autoregulation index was calculated by normalizing pattern of change in Vmean over time so that evaluation could be made by determining which pattern most accurately described observed change in Vmean (c) (Adapted and modified from reference [10])
3.1.2.2 Valsalva Maneuver
The effect of the Valsalva maneuver on the systemic and cerebral circulation is manifested in four stages: stage I, in which holding of inspiration increases intrathoracic pressure, causing blood to be pumped out of the chest cavity and MAP and Vmean to increase; stage IIa, in which decreased venous return results in decreased cardiac output and MAP, while increased intrathoracic pressure results in increased intracranial pressure and decreased Vmean; stage IIb, in which sympathicotonia results in increased cardiac output and recovery of MAP, while Vmean also improves as a result of improved blood pressure and dynamic CA; stage III, in which a decrease in intrathoracic pressure following expiration of intrathoracic air results in decreased MAP due to blood inflow into the chest cavity; and stage IV, in which improved venous return leads to an increase in MAP and Vmean (Fig. 19.6). To evaluate dynamic CA, the autoregulatory slope index (ASI) is calculated by incorporating the duration of stage IIa and the degree of improvement in MAP and Vmean into the following formula:
Recordings of MAP and Vmean during Valsalva maneuver. Phase I, increased intrathoracic and MAP; phase IIa, fall in arterial blood pressure due to decreased atrial filling; phase IIb, rise in MAP due to increased heart rate; phase III, sudden decrease in MAP due to release of intrathoracic pressure; and phase IV, overshoot in MAP with resumed atrial filling. Derivation of autoregulatory slope index is shown: d v , difference between minimum Vmean and Vmean reading 3 s later, and d p , difference between MAP readings in the same time interval (Adapted and modified from reference [11])
The normal range of ASI in healthy individuals has been reported to be 22 ± 14 % [11].
3.1.2.3 Postural Alterations
Standing up from a supine, sitting, or squatting position can cause MAP to change by up to 35 mmHg. Dynamic CA can be evaluated based on changes in MAP and Vmean determined by this postural alterations method.
3.1.2.4 Transient Hyperemic Response Ratio
The transient hyperemic response ratio (THRR) is calculated by dividing the mean PSV from the average of two heart beats after the release of 5-s common carotid artery compression (PSV hyperemia), as measured by ipsilateral TCD, by the mean PSV from the average of five heart beats before compression (PSV baseline), as follows:
With normal dynamic CA, cerebral blood vessels on the compressed side will be dilated to increase blood flow during carotid artery compression, resulting in transient hyperemia after releasing compression. The normal range for THRR is 1.2 ± 0.04, and a value close to 1 indicates impaired dynamic CA [12].
3.1.2.5 Spontaneous Fluctuations in Blood Pressure
Blood pressure fluctuates finely, even at rest. CA has been evaluated by examining the correlation between low-frequency MAP fluctuation (≤2.0 Hz) and Vmean. The correlation coefficient between the average values of Vmean and MAP over 5–10 s is calculated as the mean velocity index (Fig. 19.7a). Impaired dynamic CA is associated with a higher positive correlation between Vmean and MAP (Fig. 19.7b), while normal dynamic CA is associated with no or a negative correlation (Fig. 19.7c) [13].
Signal processing steps used to obtain subsequent samples of mean velocity index (Mx) (a). Two examples of linear regression plots with positive and negative values of Mx corresponding to non-autoregulating (b) and autoregulating (c) systems, respectively (Adapted and modified from reference [13])
3.1.3 Effect of Anesthetics on CA
When evaluating CA by TCD during surgery, consideration should be given to the type of anesthetic being used. Volatile inhalation anesthetics typically used in clinical practice such as desflurane, sevoflurane, and isoflurane are known to impair CA in a dose-dependent manner. In contrast, intravenous anesthetic propofol reduces Vmean, but does not affect CA. Opioids such as fentanyl and remifentanil do not affect Vmean or CA [14].
3.1.4 Significance of Evaluating CA
Evaluation of CA by TCD has been performed under various pathologic conditions. Impaired CA is observed in the presence of cerebral vascular spasms in patients with post-subarachnoid hemorrhage [15]. Cerebral infarction, even involving small lesions, is also associated with impaired CA. The degree of impaired CA initially worsens over the first 5 days after the onset of cerebral infarction, but gradually improves over the 3 months that follow. There is also a correlation between the degree of impaired CA after cerebral infarction and the severity and prognosis of brain disorder [16]. Furthermore, CA evaluation has proven prognostic utility in patients with head trauma [17–19].
3.2 Evaluation of Cerebrovascular CO2 Reactivity
Cerebrovascular CO2 reactivity (CO2 R) can be evaluated by challenge with chemicals such as acetazolamide or by changing the arterial partial pressure of CO2 (PaCO2) through respiratory regulation. Acetazolamide increases the tissue concentration of CO2 by inhibiting carbonic anhydrase, an enzyme catalyzing the conversion of CO2 and water to bicarbonate, thereby inducing metabolic acidosis in tissue.
Pa CO2 can be changed by rebreathing of CO2, administering CO2, or changing the respiratory rate consciously to hypoventilation, apnea, and hyperventilation. CO2 R is calculated as follows:
Here, Δ represents the change in each parameter before and after changing PaCO2.
3.2.1 Effect of Anesthetics on CO2 R
When evaluating CO2 R by TCD during surgery, consideration should be given to the effect of anesthetics on CO2 R, as in the case of evaluating CA. Volatile inhalation anesthetics such as desflurane, sevoflurane, and isoflurane are known to increase CO2 R by increasing Vmean. In contrast, CO2 R can be maintained with the intravenous anesthetic propofol, although the CO2 R value will be slightly lower due to a reduced baseline Vmean. Opioids do not affect CO2 R [20].
3.2.2 Significance of Evaluating CO2 R
CO2 R is decreased in patients with hypertension [21], obstructive apnea syndrome [22], central apnea syndrome complicated by heart failure [23], or carotid artery stenosis [24]. In addition, a correlation exists between an increased blood cholesterol level, a known precipitating factor for arteriosclerosis, and reduced CO2 R in patients with a history of mild cerebral infarction or transient ischemic attack [25]. In patients with carotid artery stenosis and reduced CO2 R, an increased incidence of cerebral infarction has been observed during follow-up [26–28]. Furthermore, impaired CO2 R has been shown to correlate with the prognosis in patients with head trauma complicated by cerebral hemorrhage [29].
In patients with kidney disorder, however, controversy remains as to whether CO2 R is maintained [30] or impaired [31]. Similarly in diabetic patients, some studies have reported an increased CO2 R during general anesthesia [32], while others have reported a decreased CO2 R [33]. Given that decreased CO2 R during anesthesia is likely associated with postoperative cognitive dysfunction [34], evaluating CO2 R is also important in predicting the risk of brain disorder and patient outcome.
4 Pathologic Conditions Evaluable by TCD
4.1 Intracranial Vascular Stenosis
Intracranial vascular stenosis can be detected by TCD as a localized area with an increase in PSV and Vmean. It has been reported that ≥50 % stenosis in the MCA corresponds to a Vmean of 80–100 cm/s and 70 % stenosis corresponds to a Vmean of 110–120 cm/s [35]. A change in blood flow velocity in the distal part of the narrowing vessel can be detected as a decrease in Vmean to <30 cm/s and a decrease in PI to <0.6 (vasodilatation). A decreased Vmean and an increased PI are evident at the proximal part of the stenosis (Fig. 19.8). In the presence of severe stenosis in the ICA, the blood flow in the ipsilateral ACA is reversed, flowing from the contralateral side to the stenotic side through the circle of Willis.
Spectrogram changes in right middle cerebral artery with stenosis are displayed on corresponding magnetic resonance angiograph. Significant increase in flow velocities in stenotic region (peak systolic velocity 120 cm/s) and decrease in post-stenotic region are evident (Adapted and modified from Neurosonology 19:113–131, 2006, in Japanese; URL: https://www.jstage.jst.go.jp/article/neurosonology/19/3/19_3_113/_pdf)
4.2 Vasospasm
Vasospasm caused by subarachnoid hemorrhage can be easily detected and evaluated by TCD and occurs along a longer length of blood vessels than intracranial stenotic lesions. Vasospasm in the MCA can be most accurately detected by TCD as an area with increased Vmean and PSV. The criteria for identifying vasospasm are shown in Table 19.1. Since vasospasm is present even before a patient develops clinical symptoms or cerebral infarction, evaluating Vmean by TCD in post-subarachnoid hemorrhage patients is important in the early detection and treatment planning of vasospasm [36].
4.3 Acute Ischemic Stroke, Occlusion, Recanalization, and Reperfusion
TCD is useful in evaluating cerebrovascular patency in patients with cerebral infarction. The thrombolysis in brain ischemia [37] and consensus on grading intracranial flow obstruction criteria [38] are used to evaluate blood flow (Fig.19.9), and cerebrovascular patency based on these criteria is considered to correlate strongly with patient outcome.
Thrombolysis in brain ischemia (TIBI) and consensus on grading intracranial flow obstruction (COGIF) criteria: patients with absent flow (TIBI grade 0, COGIF grade 1), minimal flow with zero EDV (TIBI grade 1, COGIF grade 2), and low flow with either blunted (TIBI grade 2) or dampened (TIBI grade 3, COGIF grade 3) configuration show worse prognosis than patients with flow velocities equal to those of contralateral side (TIBI grade 5, COGIF grade 4a), flow velocities that increased segmentally (TIBI grade 4, COGIF grade 4c), or flow velocities that increased focally (COGIF grade 4b) (Adapted and modified from reference [36])
4.4 Evaluation of Intracranial Pressure
TCD can be used to evaluate cerebral perfusion pressure and also to indirectly evaluate intracranial pressure (ICP). The initial sign of increased ICP is a combination of decreased EDV and increased PI. End-diastolic velocity becomes zero after ICP has exceeded diastolic blood pressure and decreases to negative values, with further increases in ICP (reverse diastolic flow), resulting in decreased PSV and eventually blood flow undetectable on TCD (Fig. 19.10). The sensitivity and specificity of undetectable blood flow on TCD for brain death are 95 % and 100 %, respectively.
Increased progressive waveform changes with intracranial pressure (ICP), eventually leading to cerebral circulatory arrest. If ICP significantly to level obviating spontaneous cerebral circulation (i.e., cerebral circulatory arrest or brain death), transcranial Doppler will show one of following specific flow patterns: (1) alternating flow with systolic forward flow, followed by complete reversal during diastole, indicating net zero forward flow, or (2) systolic peaks with only systolic hit to stagnant blood column but no flow: CPP, cerebral perfusion pressure. (Adapted and modified from reference [36])
5 Detection of Microembolic Signals
The concept of microembolic signals (MES) was first introduced in 1965 by Austen et al., who detected signals that were stronger and shorter than those of blood flow sound in a cardiopulmonary bypass circuit using continuous ultrasonic waves [39]. Because they used a bubble-type oxygenation device for the cardiopulmonary bypass circuit, they assumed that these MES represented gaseous microemboli. In 1986, MES were detected during TCD-monitored carotid endarterectomy (CEA) [40]. This was the first study to detect intraoperatively disseminated microemboli in the brain by TCD. However, since this was observed after cutting the ICA, it was again considered that these MES represented gaseous microemboli. Subsequently, in 1990, MES with different acoustic properties than those of gaseous microemboli were detected during CEA. Because they were detected before cutting the ICA, these MES were considered to originate from solid microemboli such as a thrombus or atheroma. Patients in whom solid microemboli-derived MES were detected developed transient ischemic attack or cerebral infarction after surgery [41]. Subsequently, TCD was also applied in cardiovascular surgery to measure and detect MES.
5.1 Definition of MES
MES are defined as signals with a characteristic sound on a TCD sonogram. They are characterized by a signal intensity of ≥3 dB stronger than the background blood flow sound and a duration of <300 msec [42, 43] (Fig. 19.11). To detect MES, gain and ultrasonic power should be set as low as possible so that the background flow spectrum is barely visible.
Microembolic signals (MES) comprise sine waves of constant frequency. Gaseous and solid MES can be differentiated to some extent by analyzing their frequencies. For MES detected on sonogram in (a), MES comprising seven sine waves were detected over 10 ms (b). Therefore, their frequency was calculated as 700 Hz, indicating gaseous MES. For MES detected on sonogram in (c), MES comprising ≤2 sine waves were detected over 10 ms (d). Therefore, their frequency was calculated as ≤200 Hz, indicating solid MES [45]
5.2 Differentiation Between Gaseous and Solid MES
A number of attempts have been made since around 2002 to differentiate between gaseous and solid MES [44]. Because gaseous microemboli have very low acoustic impedance, Doppler signals are strongly reflected at the interface. Thus, MES representing gaseous microemboli are observed as strong signals on TCD [41]. However, it is difficult to differentiate relatively small gaseous microemboli from solid microemboli.
Microembolic signals comprise sine waves at a constant frequency (Fig. 19.11). It is believed that gaseous and solid MES can be differentiated to some extent by analyzing their frequencies, as gaseous MES emit relatively high-frequency sound (>400–500 Hz) (Fig. 19.11a, b), while solid MES emit sound at a lower frequency (≦400Hz) (Fig. 19.11c, d) [45]. Russel et al. differentiated the two types of MES by using ultrasonic waves of two different frequencies (2 MHz and 2.5 MHz) based on the fact that gaseous MES reflect 2-MHz ultrasonic waves more strongly than 2.5-MHz ones (Fig. 19.12a), while solid MES reflect ultrasonic waves of both frequencies to a similar extent (Fig. 19.12b) [44].
Gas bubble reflecting 4.8-dB greater ultrasound at 2.0-MHz insonation (red) than at 2.5 MHz (blue) (a). Solid microemboli (80-μm plastic microsphere) reflecting only 0.6-dB greater ultrasound at 2.5-MHz insonation (blue) than at 2.0-MHz insonation (red) (b) (Adapted and modified from reference [44])
6 Usefulness of Intraoperative Monitoring by TCD
Transcranial Doppler ultrasonography is a useful monitoring tool that allows for the bedside monitoring of various parameters. However, it has limited use intraoperatively during neurosurgical procedures. Its utility has therefore been demonstrated mainly in CEA and cardiovascular surgery.
6.1 Usefulness of TCD in CEA
It is helpful to monitor Vmean in the MCA on the operated side during CEA. During CEA, an extreme decrease in Vmean from the baseline indicates the need to maintain blood pressure with drugs or use a shunt tube. A study investigating the relationship between Vmean of the MCA during carotid occlusion during CEA under local anesthesia and the occurrence of neurological complications suggested that a Vmean of <25 cm/s or a decrease to <48 % of the baseline value represents a risk of neurological complications [46]. A decrease in Vmean to <10 % of the baseline value during carotid occlusion and an increase in PI to >100 % after clamp release are associated with cerebral infarction in the perioperative period [47]. Furthermore, the detection of >50 MES during CEA is associated with cerebral ischemia [48].
Taken together, the evidence level of TCD in CEA is classes II to III, with a recommendation level of type B [49].
6.2 Usefulness of TCD in Coronary Artery Bypass Grafting Surgery
MES have been reported to occur during cardiovascular surgery in a number of cases, and their association with cerebral disorder or postoperative cognitive dysfunction has been examined. In coronary artery bypass grafting surgery (CABG) using cardiopulmonary bypass MES have been frequently detected during aortic cannulation, release of aortic cross-clamping, and heart displacement to identify the anastomotic site [50]. Furthermore, MES are even more frequently detected during valvular surgery involving cardiotomy [51].
The relationship between MES and postoperative cognitive dysfunction was confirmed in only 5 of 15 reports (1994–2009) that examined this relationship primarily in CABG cases [52]. Thus, the evidence level of MES detection by TCD during cardiovascular surgery is classes II to III, with a recommendation level of type B, while the recommendation level for the clinical significance of MES detection is type U [49].
One possible reason for the ambiguous relationship between MES detection and postoperative cognitive dysfunction after cardiovascular surgery is the small sample size. Moreover, there have been no studies on the differential effect of gaseous and solid MES—which affect the brain differently—on the occurrence of postoperative cognitive dysfunction [52]. Fat globules aspirated from the surgical field during cardiovascular surgery can be disseminated to the brain via cardiopulmonary bypass [53]. Early and robust formation of cerebral edema in a rat model of fat emboli to the brain indicates the seriousness of such lipid dissemination [54]. It is, however, unclear whether fat emboli are detectable as MES. Further efforts to detect and differentiate MES to the maximum extent possible and prevent the dissemination of microemboli to the brain may improve the usefulness of TCD during cardiovascular surgery.
7 Conclusion
Inexpensive and noninvasive Vmean monitoring by TCD, which can provide various types of information at the bedside, is extremely useful in perioperative patient management. The use of transcranial color duplex imaging and power motion mode has further facilitated the determination of Vmean. New techniques for differentiating MES are also under development. We anticipate that the utility of TCD as a useful bedside monitoring tool will be increasingly recognized.
References
Aaslid R, Markwalder TM, Nornes H (1982) Noninvasive transcranial Doppler ultrasound recording of flow velocity in basal cerebral arteries. J Neurosurg 57(6):769–774
Itoh T, Matsumoto M, Handa N et al (1993) Rate of successful recording of blood flow signals in the middle cerebral artery using transcranial Doppler sonography. Stroke 24(8):1192–1195
Giller CA, Bowman G, Dyer H et al (1993) Cerebral arterial diameters during changes in blood pressure and carbon dioxide during craniotomy. Neurosurgery 32(5):737–742
Valdueza JM, Balzer JO, Villringer A et al (1997) Changes in blood flow velocity and diameter of the middle cerebral artery during hyperventilation: assessment with MR and transcranial Doppler sonography. AJNR Am J Neuroradiol 18(10):1929–1934
Serrador JM, Picot PA, Rutt BK et al (2000) MRI measures of middle cerebral artery diameter in conscious humans during simulated orthostasis. Stroke 31(7):1672–1678
Wintermark M, Sesay M, Barbier E et al (2005) Comparative overview of brain perfusion imaging techniques. Stroke 36(9):e83–e99
Tiecks FP, Lam AM, Aaslid R et al (1995) Comparison of static and dynamic cerebral autoregulation measurements. Stroke 26(6):1014–1019
Paulson OB, Strandgaard S, Edvinsson L (1990) Cerebral autoregulation. Cerebrovasc Brain Metab Rev 2(2):161–192
Lucas SJ, Tzeng YC, Galvin SD et al (2010) Influence of changes in blood pressure on cerebral perfusion and oxygenation. Hypertension 55(3):698–705
Willie CK, Colino FL, Bailey DM et al (2011) Utility of transcranial Doppler ultrasound for the integrative assessment of cerebrovascular function. J Neurosci Methods 196(2):221–237
Tiecks FP, Douville C, Byrd S et al (1996) Evaluation of impaired cerebral autoregulation by the Valsalva maneuver. Stroke 27(7):1177–1182
Smielewski P, Czosnyka M, Kirkpatrick P et al (1996) Assessment of cerebral autoregulation using carotid artery compression. Stroke 27(12):2197–2203
Piechnik SK, Yang X, Czosnyka M et al (1999) The continuous assessment of cerebrovascular reactivity: a validation of the method in healthy volunteers. Anesth Analg 89(4):944–949
Dagal A, Lam AM (2009) Cerebral autoregulation and anesthesia. Curr Opin Anaesthesiol 22(5):547–552
Soehle M, Czosnyka M, Pickard JD et al (2004) Continuous assessment of cerebral autoregulation in subarachnoid hemorrhage. Anesth Analg 98(4):1133–1139
Aries MJ, Elting JW, De Keyser J et al (2010) Cerebral autoregulation in stroke: a review of transcranial Doppler studies. Stroke 41(11):2697–2704
Czosnyka M, Smielewski P, Kirkpatrick P et al (1996) Monitoring of cerebral autoregulation in head-injured patients. Stroke 27(10):1829–1834
Czosnyka M, Smielewski P, Lavinio A et al (2008) An assessment of dynamic autoregulation from spontaneous fluctuations of cerebral blood flow velocity: a comparison of two models, index of autoregulation and mean flow index. Anesth Analg 106(1):234–239
Lam JM, Hsiang JN, Poon WS (1997) Monitoring of autoregulation using laser Doppler flowmetry in patients with head injury. J Neurosurg 86(3):438–445
Brian JE Jr (1998) Carbon dioxide and the cerebral circulation. Anesthesiology 88(5):1365–1386
Serrador JM, Sorond FA, Vyas M et al (2005) Cerebral pressure-flow relations in hypertensive elderly humans: transfer gain in different frequency domains. J Appl Physiol 98(1):151–159
Reichmuth KJ, Dopp JM, Barczi SR et al (2009) Impaired vascular regulation in patients with obstructive sleep apnea: effects of continuous positive airway pressure treatment. Am J Respir Crit Care Med 180(11):1143–1150
Xie A, Skatrud JB, Khayat R et al (2005) Cerebrovascular response to carbon dioxide in patients with congestive heart failure. Am J Respir Crit Care Med 172(3):371–378
Widder B, Kleiser B, Krapf H (1994) Course of cerebrovascular reactivity in patients with carotid artery occlusions. Stroke 25(10):1963–1967
Wijnhoud AD, Koudstaal PJ, Dippel DW (2006) Relationships of transcranial blood flow Doppler parameters with major vascular risk factors: TCD study in patients with a recent TIA or nondisabling ischemic stroke. J Clin Ultrasound 34(2):70–76
Silvestrini M, Vernieri F, Pasqualetti P et al (2000) Impaired cerebral vasoreactivity and risk of stroke in patients with asymptomatic carotid artery stenosis. JAMA 283(16):2122–2127
Markus H, Cullinane M (2001) Severely impaired cerebrovascular reactivity predicts stroke and TIA risk in patients with carotid artery stenosis and occlusion. Brain 124(3):457–467
Vernieri F, Pasqualetti P, Matteis M et al (2001) Effect of collateral blood flow and cerebral vasomotor reactivity on the outcome of carotid artery occlusion. Stroke 32(7):1552–1558
Klingelhofer J, Sander D (1992) Doppler CO2 test as an indicator of cerebral vasoreactivity and prognosis in severe intracranial hemorrhages. Stroke 23(7):962–966
Skinner H, Mackaness C, Bedforth N et al (2005) Cerebral haemodynamics in patients with chronic renal failure: effects of haemodialysis. Br J Anaesth 94(2):203–205
Ishida K, Uchida M, Utada K et al (2011) Cerebrovascular carbon dioxide reactivity during general anesthesia in the patients with chronic renal failure. J Neurosurg Anesthesiol 23(4):459
Kawata R, Nakakimura K, Matsumoto M et al (1998) Cerebrovascular CO2 reactivity during anesthesia in patients with diabetes mellitus and peripheral vascular disease. Anesthesiology 89(4):887–893
Kadoi Y, Hinohara H, Kunimoto F et al (2003) Diabetic patients have an impaired cerebral vasodilatory response to hypercapnia under propofol anesthesia. Stroke 34(10):2399–2403
Kadoi Y, Kawauchi C, Kuroda M et al (2011) Association between cerebrovascular carbon dioxide reactivity and postoperative short-term and long-term cognitive dysfunction in patients with diabetes mellitus. J Anesth 25(5):641–647
Feldmann E, Wilterdink JL, Kosinski A et al (2007) The Stroke Outcomes and Neuroimaging of Intracranial Atherosclerosis (SONIA) trial. Neurology 68(24):2099–2106
Topcuoglu MA (2012) Transcranial Doppler ultrasound in neurovascular diseases: diagnostic and therapeutic aspects. J Neurochem 123(Suppl 2):39–51
Demchuk AM, Burgin WS, Christou I et al (2001) Thrombolysis in brain ischemia (TIBI) transcranial Doppler flow grades predict clinical severity, early recovery, and mortality in patients treated with intravenous tissue plasminogen activator. Stroke 32(1):89–93
Nedelmann M, Stolz E, Gerriets T et al (2009) Consensus recommendations for transcranial color-coded duplex sonography for the assessment of intracranial arteries in clinical trials on acute stroke. Stroke 40(10):3238–3244
Austen WG, Howry DH (1965) Ultrasound as a method to detect bubbles or particulate matter in the arterial line during cardiopulmonary bypass. J Surg Res 5:283–284
Padayachee TS, Gosling RG, Bishop CC et al (1986) Monitoring middle cerebral artery blood velocity during carotid endarterectomy. Br J Surg 73(2):98–100
Spencer MP, Thomas GI, Nicholls SC et al (1990) Detection of middle cerebral artery emboli during carotid endarterectomy using transcranial Doppler ultrasonography. Stroke 21(3):415–423
Stroke (1995) Basic identification criteria of Doppler microembolic signals. Consensus Committee of the Ninth International Cerebral Hemodynamic Symposium. Stroke 26(6):1123
Ringelstein EB, Droste DW, Babikian VL et al (1998) Consensus on microembolus detection by TCD. International Consensus Group on Microembolus Detection. Stroke 29(3):725–729
Russell D, Brucher R (2002) Online automatic discrimination between solid and gaseous cerebral microemboli with the first multi-frequency transcranial Doppler. Stroke 33(8):1975–1980
Hanzawa K, Furui E, Ohzeki H et al (1998) Frequency analysis of high intensity transient signals in CPB can distinguishes solid embolic signals from gaseous signals. Ann Thorac Surg 66:1490
Moritz S, Kasprzak P, Arlt M et al (2007) Accuracy of cerebral monitoring in detecting cerebral ischemia during carotid endarterectomy: a comparison of transcranial Doppler sonography, near-infrared spectroscopy, stump pressure, and somatosensory evoked potentials. Anesthesiology 107(4):563–569
Ackerstaff RG, Moons KG, van de Vlasakker CJ et al (2000) Association of intraoperative transcranial doppler monitoring variables with stroke from carotid endarterectomy. Stroke 31(8):1817–1823
Levi CR, O’Malley HM, Fell G et al (1997) Transcranial Doppler detected cerebral microembolism following carotid endarterectomy. High microembolic signal loads predict postoperative cerebral ischaemia. Brain 120(4):621–629
Sloan MA, Alexandrov AV, Tegeler CH et al (2004) Assessment: transcranial Doppler ultrasonography: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 62(9):1468–1481
Clark RE, Brillman J, Davis DA et al (1995) Microemboli during coronary artery bypass grafting. Genesis and effect on outcome. J Thorac Cardiovasc Surg 109(2):249–258
Braekken SK, Reinvang I, Russell D et al (1998) Association between intraoperative cerebral microembolic signals and postoperative neuropsychological deficit: comparison between patients with cardiac valve replacement and patients with coronary artery bypass grafting. J Neurol Neurosurg Psychiatry 65(4):573–576
Kruis RW, Vlasveld FA, Van Dijk D (2010) The (un)importance of cerebral microemboli. Semin Cardiothorac Vasc Anesth 14(2):111–118
Brooker RF, Brown WR, Moody DM et al (1998) Cardiotomy suction: a major source of brain lipid emboli during cardiopulmonary bypass. Ann Thorac Surg 65(6):1651–1655
Gohara T, Ishida K, Nakakimura K et al (2010) Temporal profiles of aquaporin 4 expression and astrocyte response in the process of brain damage in fat embolism model in rats. J Anesth 24(2):225–233
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer Japan
About this chapter
Cite this chapter
Ishida, K., Yamashita, A., Matsumoto, M. (2015). Role of Transcranial Doppler Ultrasonography in Neuroanesthesia. In: Uchino, H., Ushijima, K., Ikeda, Y. (eds) Neuroanesthesia and Cerebrospinal Protection. Springer, Tokyo. https://doi.org/10.1007/978-4-431-54490-6_19
Download citation
DOI: https://doi.org/10.1007/978-4-431-54490-6_19
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-54489-0
Online ISBN: 978-4-431-54490-6
eBook Packages: MedicineMedicine (R0)