Abstract
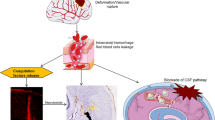
Intracranial bleeding is a common and serious consequence of traumatic brain injury (TBI). In the present study, we investigated cerebral hematoma occurrence, brain edema formation, blood–brain barrier (BBB) disruption, and heme oxygenase-1 (HO-1) expression after TBI. Moderate severity (1.8–2.2 atmospheres [ATM]) TBI was induced by lateral fluid percussion in male adult Sprague–Dawley rats. Sham rats underwent only a craniotomy. Rats were euthanized 24 h later for brain histology and immunoblotting analysis. We found TBI-induced cerebral hematomas and iron deposition in the ipsilateral hemisphere in all rats. TBI also caused marked BBB disruption (p < 0.05) and brain swelling (p < 0.05). HO-1, a key enzyme for heme degradation, was upregulated significantly after TBI (419 ± 89 vs 194 ± 59 pixels in the sham, p < 0.05). These results suggest that cerebral hematomas might play a role in brain injury after TBI. Future studies should determine the role of iron released from the cerebral hematoma in TBI.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
Introduction
Each year in the United States, approximately 1.6 million people suffer a traumatic brain injury (TBI) and there are more than 5 million Americans currently living with TBI-related disabilities [10]. There are currently no effective therapies for TBI patients. Intracranial bleeding is a common and serious consequence of TBI. MRI has shown a preponderance of hemorrhagic lesions and few ischemic lesions in the acute phase and 56 % of TBI patients were reported to have at least one intracranial bleed [12]. The release of iron from the breakdown of hemoglobin during hematoma resolution may result in a build-up of non-heme iron in brain tissue and brain damage.
In the present study we established a TBI model with cerebral hematoma. The lateral fluid percussion (LFP) model produces both focal and diffuse injury with vascular disruption, neuronal cell death and glial proliferation [1, 2, 7, 14, 15, 17, 20].
Materials and Methods
Animal Preparation and Experimental Group
The protocols for these animal studies were approved by the University of Michigan Committee on the Use and Care of Animals at the University of Michigan. Adult male Sprague–Dawley rats (Charles River Laboratories, Portage, MI, USA) weighing 260–340 g were used in this study. Animals were euthanized at 24 h post-TBI or sham operation for brain histology and Western blot analysis.
Lateral Fluid Percussion Injury
Traumatic brain injury was induced by lateral fluid percussion injury, as described previously [3, 15]. In brief, rats were anesthetized with pentobarbital (50 mg/kg, i.p.), and rectal temperature was maintained at 37.5 °C by using a feedback-controlled heating pad. The animals were placed in a stereotaxic frame, and the scalp and temporal muscle were reflected. A 4.8-mm diameter hole was drilled between the bregma and lambda on the right convexity (anterior edge 2.0 mm posterior to the bregma; lateral edge adjacent to the left lateral ridge), and a hollow female Luer–Lock fitting secured with dental cement. Lateral fluid percussion injury was induced by a transient (21–23 ms) fluid pulse impact against the exposed dura by using a fluid-percussion device (AmScien Instruments, Richmond, VA, USA). The impact pressure was measured by an extra-cranial transducer and controlled to 1.8–2.2 atmospheres (ATM). After impact, the dura was checked to ensure that it had remained intact. Sham-operated control animals underwent all surgical procedures, except the fluid-percussion impact. Animals that did not survive the injury were predetermined to be excluded from the study.
Histological and Immunohistochemical Study
Rats were reanesthetized with pentobarbital (60 mg/kg, i.p.), followed by intracardiac perfusion with 4 % paraformaldehyde in 0.1 mol/L phosphate-buffered saline, pH 7.4. Brains were removed, kept in 4 % paraformaldehyde for 24 h, and immersed in 25 % sucrose for 3–4 days at 4 °C. The brains were then embedded in an optimal cutting temperature compound (Sakura Finetek USA, Torrance, CA, USA) and sectioned on a cryostat (18 µm). Brain swelling was assessed morphometrically. Coronal sections from 1 mm posterior to the anterior edge of the craniotomy site were stained with hematoxylin and eosin. On the microscopic images, the area of the ipsilateral or contralateral hemisphere was measured using ImageJ software. Brain swelling was estimated by the ratio of the volume of (ipsilateral – contralateral)/contralateral hemisphere. Immunohistochemical staining was performed using avidin–biotin complex technique. The primary antibody was polyclonal rabbit anti-rat HO-1 IgG (1:200 dilution, StressGene) and the secondary antibody was biotinylated goat anti-rabbit IgG (1:500 dilution, Vector Laboratories). Normal rabbit IgG was used as negative control. Brain iron deposition was determined by enhanced Perls’ reaction [22].
Western Blot Analysis
Animals were anesthetized before undergoing transcardiac perfusion with 0.1 mol/L phosphate-buffered saline. The brains were removed and a 4-mm thick coronal brain slice was cut approximately 5 mm from the frontal pole. The slice was separated into ipsilateral or contralateral cortex and basal ganglia. Western blot analysis was performed as previously described [24]. The primary antibodies were polyclonal rabbit anti-rat HO-1 IgG antibody (1:2,500 dilution; StressGen, Farmingdale, NY, USA) and polyclonal sheep anti-rat albumin antibody (1:20,000 dilution; Bethyl Lab, Montgomery, USA). The secondary antibodies were peroxidase-conjugated goat anti-rabbit antibody (Bio-Rad Laboratories, Hercules, CA, USA) and rabbit anti-sheep antibody (Millipore, Billerica, MA, USA).
Statistical Analysis
All data in this study are presented as mean ± standard deviation. Data were analyzed using Student’s t test or Kruskal–Wallis test. Statistical significance was set at p < 0.05.
Results
All animals undergoing lateral fluid percussion had intracerebral hematomas in the ipsilateral cortex and caudate at 24 h (Fig. 1a). TBI caused ipsilateral brain swelling (3.3 ± 0.9 % vs −0.04 ± 1.2 % in the sham group, p < 0.05, Fig. 1b). Release of iron from the degradation of heme occurred around clots 24 h after brain trauma, as indicated by Perls’ staining. Iron-positive cells were found in the ipsilateral hemisphere, especially around hematomas (Fig. 2a). TBI also resulted in blood–brain barrier disruption. Albumin levels were increased in the ipsilateral hemisphere of TBI rats (1,248 ± 710 vs 204 ± 171 pixels in the sham group, p < 0.05, Fig. 2b).
(a) Perls’ staining showing iron deposition in the ipsilateral hemisphere 24 h after TBI, scale bar = 50 μm; (b) Albumin levels in the ipsilateral hemisphere of sham rats (lanes 1–3) or in the ipsilateral hemisphere (lanes 4–6) or in the contralateral hemisphere (lanes 7–9) of TBI rats. Values are mean ± SD, n = 3, *p < 0.05 vs sham. Arrows indicate perls’ positive cells
Immunoreactivity of HO-1 was increased markedly in the ipsilateral cortex and caudate of TBI rats (Fig. 3a, b). Most HO-1 positive cells were microglia-like cells. HO-1 protein levels were determined by Western blot analysis and we found that HO-1 levels in the ipsilateral cortex were significantly higher in TBI rats (419 ± 89 vs 194 ± 59 pixels in the sham, p < 0.05, Fig. 3c).
HO-1 immunoreactivity in the ipsilateral cortex of sham rat (a) or TBI rat (b). Scale bar = 200 μm. HO-1 protein levels (c) in the ipsilateral hemisphere of sham-operated rats (lanes 1–3) and in the ipsilateral hemisphere (lanes 4–6) and the contralateral hemisphere (lanes 7–9) of TBI rats at 24 h. Values are mean ± SD, n = 3, *p < 0.05 vs the other groups
Conclusion
In this study, we found that TBI resulted in cerebral hematomas, brain swelling, and BBB disruption. HO-1 upregulation and brain iron deposition were also found in the ipsilateral hemisphere 24 h after TBI.
Intracranial bleeding is a common and serious consequence of TBI and contributes to the injury. The primary brain injury after trauma may manifest as diffuse axonal injury, intraparenchymal contusions, intracranial hematomas, diffused axonal injury, and skull fractures [9, 12]. Brain edema after TBI is a common and serious consequence of severe traumatic brain injury [6]. BBB disruption was reported previously after TBI [4, 19]. A brain contusion results in immediate cell death in a limited region of the brain. But secondary cell loss and chronic atrophy can occur at sites other than at or near the primary injury [13]. It may be related to regional metabolic distress that was mediated by accumulated iron-induced oxidative stress and metabolic dysfunction [25].
Iron deposition occurs in TBI brain, as indicated in this study using Perls’ staining. We have gathered substantial evidence that iron plays a major role in brain injury after intracerebral hemorrhage and subarachnoid hemorrhage. The release of iron from the breakdown of hemoglobin during hematoma resolution in the rat results in a build-up in the levels of non-heme iron in brain tissue. The high level of non-heme iron remains in the brain for at least 28 days [22]. Through enhanced Perls’ reaction, iron-positive cells were found in the perihematomal zone as early as the 1st day [22], as found in our study with TBI. Increases in brain iron levels cause brain edema, oxidative stress, BBB disruption, brain atrophy, and neurological deficits following intracranial hemorrhage (ICH) [8, 16, 21, 23]. Our previous studies showed that free iron levels in cerebrospinal fluid (CSF) increase almost 14-fold on the third day after ICH, and remain high for at least 28 days after experimental ICH [18]. The duration of iron overload after lateral fluid percussion remains to be elucidated.
Brain HO-1 levels are increased after TBI. HO-1, also called heat shock protein 32, is an enzyme for heme degradation into iron, carbon monoxide, and biliverdin. It can be induced in the brain by heat shock, heme and hemoglobin, a variety of oxidants [23], and TBI [5]. In the rat, marked HO-1 upregulation at day 3 accompanied by the elevation of nonheme iron, transferrin, transferrin receptor, and ferritin levels after subarachnoid hemorrhage [11].
In conclusion, TBI induced cerebral hematomas, brain edema formation, BBB disruption, and iron deposition. Cerebral hematomas and brain iron overload could be therapeutic targets for TBI.
References
Bramlett HM, Dietrich WD (2002) Quantitative structural changes in white and gray matter 1 year following traumatic brain injury in rats. Acta Neuropathol 103:607–614
Cortez SC, McIntosh TK, Noble LJ (1989) Experimental fluid percussion brain injury: vascular disruption and neuronal and glial alterations. Brain Res 482:271–282
Dixon CE, Lyeth BG, Povlishock JT, Findling RL, Hamm RJ, Marmarou A, Young HF, Hayes RL (1987) A fluid percussion model of experimental brain injury in the rat. J Neurosurg 67:110–119
Fukuda K, Panter SS, Sharp FR, Noble LJ (1995) Induction of heme oxygenase-1 (HO-1) after traumatic brain injury in the rat. Neurosci Lett 199:127–130
Fukuda K, Richmon JD, Sato M, Sharp FR, Panter SS, Noble LJ (1996) Induction of heme oxygenase-1 (HO-1) in glia after traumatic brain injury. Brain Res 736:68–75
Ghajar J (2000) Traumatic brain injury. Lancet 356:923–929
Hicks R, Soares H, Smith D, McIntosh T (1996) Temporal and spatial characterization of neuronal injury following lateral fluid-percussion brain injury in the rat. Acta Neuropathol 91:236–246
Hua Y, Nakamura T, Keep R, Wu J, Schallert T, Hoff J, Xi G (2006) Long-term effects of experimental intracerebral hemorrhage: the role of iron. J Neurosurg 104:305–312
Khoshyomn S, Tranmer BI (2004) Diagnosis and management of pediatric closed head injury. Semin Pediatr Surg 13:80–86
Langlois JA, Rutland-Brown W, Wald MM (2006) The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehabil 21:375–378
Lee JY, Keep RF, He Y, Sagher O, Hua Y, Xi G (2010) Hemoglobin and iron handling in brain after subarachnoid hemorrhage and the effect of deferoxamine on early brain injury. J Cereb Blood Flow Metab 30:1793–1803
Maas AI, Stocchetti N, Bullock R (2008) Moderate and severe traumatic brain injury in adults. Lancet Neurol 7:728–741
Marcoux J, McArthur DA, Miller C, Glenn TC, Villablanca P, Martin NA, Hovda DA, Alger JR, Vespa PM (2008) Persistent metabolic crisis as measured by elevated cerebral microdialysis lactate-pyruvate ratio predicts chronic frontal lobe brain atrophy after traumatic brain injury. Crit Care Med 36:2871–2877
Marmarou A, Foda MA, van den Brink W, Campbell J, Kita H, Demetriadou K (1994) A new model of diffuse brain injury in rats. Part I: pathophysiology and biomechanics. Neurosurg 80:291–300
McIntosh TK, Vink R, Noble L, Yamakami I, Fernyak S, Soares H, Faden AL (1989) Traumatic brain injury in the rat: characterization of a lateral fluid-percussion model. Neuroscience 28:233–244
Nakamura T, Keep RF, Hua Y, Schallert T, Hoff JT, Xi G (2004) Deferoxamine-induced attenuation of brain edema and neurological deficits in a rat model of intracerebral hemorrhage. J Neurosurg 100:672–678
Pierce JE, Trojanowski JQ, Graham DI, Smith DH, McIntosh TK (1996) Immunohistochemical characterization of alterations in the distribution of amyloid precursor proteins and beta-amyloid peptide after experimental brain injury in the rat. J Neurosci 16:1083–1090
Wan S, Hua Y, Keep RF, Hoff JT, Xi G (2006) Deferoxamine reduces CSF free iron levels following intracerebral hemorrhage. Acta Neurochir Suppl 96:215–218
Schmidt RH, Grady MS (1993) Regional patterns of blood-brain barrier breakdown following central and lateral fluid percussion injury in rodents. J Neurotrauma 10:415–430
Thompson HJ, Lifshitz J, Marklund N, Grady MS, Graham DI, Hovda DA, McIntosh TK (2005) Lateral fluid percussion brain injury: a 15-year review and evaluation. J Neurotrauma 22:42–75
Wu J, Hua Y, Keep R, Schallert T, Hoff J, Xi G (2002) Oxidative brain injury from extravasated erythrocytes after intracerebral hemorrhage. Brain Res 953:45
Wu J, Hua Y, Keep RF, Nakamura T, Hoff JT, Xi G (2003) Iron and iron-handling proteins in the brain after intracerebral hemorrhage. Stroke 34:2964–2969
Xi G, Keep RF, Hoff JT (2006) Mechanisms of brain injury after intracerebral haemorrhage. Lancet Neurol 5:53–63
Xi G, Keep RF, Hua Y, Xiang JM, Hoff JT (1999) Attenuation of thrombin-induced brain edema by cerebral thrombin preconditioning. Stroke 30:1247–1255
Xu Y, McArthur DL, Alger JR, Etchepare M, Hovda DA, Glenn TC, Huang S, Dinov I, Vespa PM (2010) Early nonischemic oxidative metabolic dysfunction leads to chronic brain atrophy in traumatic brain injury. J Cereb Blood Flow Metab 30:883–894
Acknowledgments
This study was supported by grants NS-017760, NS-039866, and NS-057539 from the National Institutes of Health (NIH) and 0840016 N from the American Heart Association (AHA). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH and AHA.
Conflict of InterestWe declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer-Verlag Wien
About this paper
Cite this paper
Okubo, S., Xi, G., Keep, R.F., Muraszko, K.M., Hua, Y. (2013). Cerebral Hemorrhage, Brain Edema, and Heme Oxygenase-1 Expression After Experimental Traumatic Brain Injury. In: Katayama, Y., Maeda, T., Kuroiwa, T. (eds) Brain Edema XV. Acta Neurochirurgica Supplement, vol 118. Springer, Vienna. https://doi.org/10.1007/978-3-7091-1434-6_14
Download citation
DOI: https://doi.org/10.1007/978-3-7091-1434-6_14
Published:
Publisher Name: Springer, Vienna
Print ISBN: 978-3-7091-1433-9
Online ISBN: 978-3-7091-1434-6
eBook Packages: MedicineMedicine (R0)