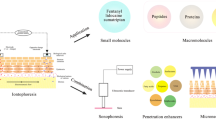
Abstract
Transdermal iontophoresis enables hydrophilic, charged, or neutral molecules to be administered through the skin in an effective, noninvasive, patient-friendly manner. This chapter presents the basic concepts, mechanisms, and an analysis of electrotransport across the skin as a function of (i) electrical parameters, such as current density; (ii) formulation parameters, such as the influence of drug concentration, pH, and the presence of competing ions; and (iii) the delivery system.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Molecular transport during iontophoresis can be attributed to three component mechanisms: passive diffusion, electromigration (EM), and convective solvent flow, also called electroosmosis (EO). In physical terms, the flux of a molecule, J i, across the skin, in the presence of an applied electric field, E, depends on both the concentration and potential gradients and can be described by a modified form of the Nernst-Planck equation that also takes into account the convective solvent flow (Pikal 2001) when an electric potential is applied to a membrane that contains fixed negative charges (e.g., the skin with isoelectric point (pI) of ~4–4.5 (Marro et al. 2001a)) (Srinivasan and Higuchi 1990; Kasting 1992):
where D i, c i, and u i are the diffusion coefficient, concentration, and electrical mobility of ion i and v w represents the linear velocity of the convective solvent flow (Gratieri and Kalia 2013). The diffusion coefficient and the electric mobility are related by the Nernst-Einstein equation:
Thus, the electric mobility represents an “ordered” diffusion dictated by the electric field – it competes against thermal disordering (RT term in the denominator) which will act to decrease its magnitude. It is clear that the higher the valence (z i), the higher is the electrical mobility. For charged molecules, passive diffusion across the stratum corneum is limited or negligible, meaning that molecular transport during iontophoresis is attributed to EM and EO – their relative contributions depending on the experimental conditions and the physicochemical properties of the molecule (Gratieri and Kalia 2013).
The penetration pathways of such charged molecules during iontophoresis may also be different from those during passive diffusion. Instead of following the tortuous intercellular lipid pathway between the corneocytes, it has been suggested that under the influence of an electric current, ions will follow the path of the least electrical resistance, e.g., they will preferentially take the appendageal pathways (i.e., hair follicles, sweat glands) (Cullander and Guy 1991). However, in addition to transport via these “shunt” pathways, structural changes in the membrane, which may correspond to transient reorientation of SC proteins and lipids in the presence of the electric field, may also facilitate ion transport (Jadoul et al. 1999). Lipids and proteins have dipole moments and will align themselves to the direction of the applied electric field. The reorientation of these SC components under the influence of the electric field may result in the formation of transient conduction pathways (“pores”) in the bulk SC (Gratieri and Kalia 2013). Therefore, although the appendageal structures are probably involved in iontophoretic transport, smaller negatively charged (given the skin’s permselectivity at physiological pH) transient “nano-pores” with estimated pore radii of ~20 nm may also be present (Aguilella et al. 1994) (Fig. 5.1).
Schematic representation of iontophoresis including the representation of transient pores created in the skin during current application. Under the influence of the applied field, it is envisaged that ions electromigrate through these pores – the presence of the fixed negative charges in the pore walls gives rise to electroosmotic phenomena (Pikal 1990). (Modified from (Gratieri and Kalia 2013). D is the drug, which can be either positively (D+) or negatively (D−) charged. N represents a neutral molecule. EM is the electromigration and EO the electroosmosis)
2 Factors Influencing Electrically Assisted Drug Delivery
2.1 Current Density
Electromigration refers to the ordered movement of the ions in the presence of the applied electric field in a process that can be described by Faraday’s law (Phipps et al. 1989; Phipps and Gyory 1992; Sage and Riviere 1992; Delgado-Charro and Guy 2001; Kalia et al. 2004):
where I is the applied current (amperes); t D is the transport number of the drug; A is the cross-sectional area through which transport occurs; F is the Faraday constant (Coulombs/mole); and z D is the drug valence.
It is evident from the equation that the applied current (I) is a parameter that can directly affect the rate and extent of drug delivery. The introduction of the second driving force – the electrical potential gradient – in addition to the concentration gradient across the skin (Gratieri and Kalia 2013), means that drug delivery is enhanced, and the flux can be strictly correlated with duration, intensity, and profile of current application. As such, complex drug delivery kinetics – determined solely by the current profile – are feasible. This was demonstrated in studies carried out in Yorkshire swine investigating the feasibility of delivering zolmitriptan (MW 287.4 Da) – used for the treatment of migraine. An iontophoretic patch system and a complex multistep current profile were used. The study showed that the drug levels in the blood (7.1 ± 1.7 and 11.9 ± 2.0 ng/ml at t = 30 and t = 40 min, respectively) closely followed the variations in the applied current (four-step profile with current intensities ranging from 0.35 to 0.05 mA/cm2) (Patel et al. 2009).
Many other studies have demonstrated that the iontophoretic flux of a drug can be enhanced by increasing the applied current (Green et al. 1992; Lau et al. 1994; Abla et al. 2005; Panzade et al. 2012); linear correlations between flux and current density have been reported either small molecules as thyrotropin (362 Da) (Burnette and Marrero 1986) or for larger molecules, e.g., triptorelin (1311.5 Da) (Schuetz et al. 2005). In this way, the modulation of the applied current and the patch size enables easy individualization of therapy (Djabri et al. 2012a). This was recently observed with rasagiline (RAS) and selegiline (SEL), which are dose-dependent selective irreversible inhibitors of monoamine oxidase B (MAO-B), with therapeutic applications for the treatment of Parkinson’s disease and in the treatment of major depressive disorder (Kalaria et al. 2012). Permeation experiments performed across porcine and human skin in vitro demonstrated that while passive delivery from aqueous solution was minimal, drug delivery was directly correlated with current density (I d = 0.15, 0.3, and 0.5 mA/cm2) producing a linear increase in steady-state iontophoretic flux (J ss, RAS = 49.1 I d + 27.9 (r 2 = 0.96) and J ss, SEL = 27.8 i d + 25.8 (r 2 = 0.98)). Drug extraction from the skin showed that there was also a statistically significant increase in the amounts of RAS and SEL retained within the membrane as a function of current density (Fig. 5.2).
Total delivery (cumulative permeation + skin deposition) and steady state flux (Jtot) of (a) RAS (20 mM) and (b) SEL (20 mM) as a function of current density (at 0.15, 0.3, and 0.5 mA/cm2) across porcine skin after 7 h of transdermal iontophoresis (mean ± SD; n ≥ 5). (Adapted and reproduced with permission from Kalaria et al. 2012)
However, straightforward linear correlations are not always observed. For example, a poor correlation was observed between 9-desglycinamide-8-arginine-vasopressin (DGAVP) flux and applied current; a more than sixfold increment in current density did not even double the flux (Craanevanhinsberg et al. 1994).
It is also evident from Eq. 5.3 that a drug’s transport number influences the electromigration efficiency. This parameter is related to the ability of the drug to function as a charge carrier, and the transport number represents the fraction of the total charge carried by each species (0 < t D < 1) (Mudry et al. 2006a, b, c). It depends on how drug concentration, mobility, and valence compare with those of the other ions present in the pharmaceutical formulation (buffering agents, viscosity modifiers, and preservatives) generated by electrode reactions and present in the skin (Mudry et al. 2006a). Specifically,
where I d is the applied current density (= I/A) and z D, u D, and c D refer to the charge, mobility, and concentration of the drug in the membrane, respectively; the denominator is the sum of the products of these parameters for each ion in the system contributing to charge transfer across the membrane (Kalia et al. 2004; Kasting and Keister 1989). It is obvious that the presence of endogenous competing counterions decreases the iontophoretic transport of the drug.
2.2 Formulation
2.2.1 Drug Concentration
Drug concentration is a commonly studied experimental parameter in iontophoretic experiments, as it might be envisaged that an increase in the amount of drug in the formulation would result in increased drug delivery. However, linear correlations are not always encountered, and behavior is complicated by drug-membrane interactions. For certain molecules, the flux-concentration profiles reach a plateau above which further increases in concentration have only a limited or negligible effect on flux.
A key factor is the presence or absence of competing ions (Kasting and Keister 1989). Studies have described the use of a salt bridge to eliminate the presence of competing cations in the donor compartment rendering delivery independent of drug concentration. For example, it was observed that cumulative permeation of RAS after iontophoresis for 7 h using a salt bridge at 0.5 mA/cm2 was independent of drug concentration. For the three concentrations studied (10, 20 and 40 mM), the cumulative permeation was statistically equivalent (1200.4 ± 154.6, 1262.6 ± 125.0 and 1321.5 ± 335.2 μg/cm2, respectively); similar behavior was observed for SEL (the corresponding values were 748.3 ± 115.2, 848.8 ± 108.3, and 859.8 ± 230.1 μg/cm2, respectively) (Kalaria et al. 2012). Although the use of salt bridges precluded the presence of competing cations in the donor compartment, chloride ions present in the receptor were the principal charge carrier due to their high mobility and concentration as they migrated across the skin toward the anode – as would be the case in vivo (Kalaria et al. 2012).
In cases where a salt bridge is not used, Eq. 5.4 suggests that the increase of the drug concentration, or drug molar fraction, should enhance the transdermal flux via an increase in t D , therefore, increasing EM. This was recently demonstrated with the cathodal iontophoresis of phenobarbital in vitro across porcine skin. The results showed that drug fluxes were inversely related to the Cl- concentration present in the donor solution after 5 h of current application (0.5 mA/cm2) (Fig. 5.3a). Therefore, the lower the co-ion concentration, the greater the drug molar fraction in the vehicle and the greater the drug transport number in a linearly proportional manner (r 2 ≈ 0.80) (Fig. 5.3b) (Djabri et al. 2012b).
Cathodal delivery of phenobarbital from different donor solutions (pH 7.4) containing various amounts of competing co-ions. (a) Flux values (mean ± SD) determined after 5 h of iontophoresis (0.4 mA). (b) Transport number of phenobarbital (t PHEN, mean ± SD) as a function of molar fraction (XPHEN). Values of the latter parameter were calculated from the concentrations of phenobarbital, HEPES, and chloride. The sources of Cl−included NaCl (used as background electrolyte), HCl (used to adjust the donor solution pH), and the electrode electrochemical reaction. The dashed line is the linear regression through all data points except those obtained with HEPES: t PHEN = 0.002 (±0.001) + 0.033 (±0.002) XPHEN (r 2 > 0.8). Adapted and reproduced with permission from Djabri et al. (2012b)
It may also be assumed that an increase in drug concentration would result in an increased EO flux, according to Eq. 5.5, which expresses the EO drug flux:
where v w is the electroosmotic solvent flow, and c D is the concentration of the drug in the vehicle (Pikal 1992). This should have a direct impact on the delivery of positively charged and neutral molecules. However, the real situation may be far more complex than the cited equations suggest, as other factors may be involved: not only the existence of competing ions, as mentioned before, but also the effect of drug physicochemical properties and their impact on the ability of the molecule to interact with structures along the iontophoretic transport pathway.
Studying the anodal iontophoresis of granisetron (GST; MW: 348.9, pKa 9.4) across porcine skin in vitro, it was demonstrated that cumulative delivery from 5 to 10 mM solutions was statistically equivalent; however, statistically significant increases were seen when drug concentration was raised to 20 or 40 mM (Cazares-Delgadillo et al. 2010). The reduced delivery efficiency at lower concentrations could be explained by the presence of Na+ in the formulation, which possesses higher mobility than granisetron, effectively negating the effect of any increase in formulation concentration (Kasting 1992). As the formulation pH (6.6–6.8) was higher than the skin’s pI, there was an EO contribution to delivery. However, co-iontophoresis of acetaminophen, a neutral molecule used to report on convective solvent flow, showed that EM was the predominant transport mechanism accounting for 71–86 % of total granisetron delivery. It was also observed that a fourfold increase in granisetron concentration from 10 to 40 mM resulted in a twofold reduction in acetaminophen permeation indicating that skin permselectivity was decreased (Cazares-Delgadillo et al. 2010). As for other lipophilic cations, including the peptides, leuprolide, and nafarelin, it is likely that the positively charged molecules were bound to skin structures along the iontophoretic transport pathway neutralizing the intrinsic negative charges, thereby reducing the volume of solvent flow (Lu et al. 1993; Delgado-Charro and Guy 1994; Hoogstraate et al. 1994; Delgado-Charro and Guy 1995; Delgado-Charro et al. 1995; Hirvonen et al. 1996; Rodriguez Bayon and Guy 1996; Hirvonen and Guy 1997; Nair and Panchagnula 2003). In these cases, the impact on drug delivery can depend on the relative contribution of EM and EO to the iontophoretic transport of the molecule in question (Hirvonen and Guy 1997; Marro et al. 2001b).
2.2.2 pH
In principle, the ionization state of the skin will determine the EO solvent flow, and in vitro studies have tried to use modification of formulation pH as a means to change skin pH. However, this is a strategy more suited to enhancing the ionization state of the drug and so affects mobility and hence EM, since manipulation of skin ionization state is rather more difficult to achieve in vivo due to the skin’s intrinsic buffering capacity (Levin and Maibach 2008). Although modulation of formulation pH can certainly be used to improve transport, in practice, extreme pH values need to be avoided to prevent irritation or chemical burns. Acceptable pH values for skin application have a mildly acidic to neutral pH (5–7.4).
Acyclovir, for example, is an antiviral agent used in the treatment of cutaneous viral infections caused by herpes simplex virus (HSV-1). Although it is a small molecule (225.20 Da), it is unable to diffuse efficiently through the SC and subsequently enter into the basal epidermis, where viral replication occurs. In order to enhance the permeation of this molecule, iontophoresis has been applied by many authors (Volpato et al. 1995; Volpato et al. 1998; de Jalon et al. 2001; Stagni et al. 2004; Padula et al. 2005; Morrel et al. 2006; Shukla et al. 2009; Siddoju et al. 2011). However, it has been shown that at pH 7.4, the amount of drug recovered in the stratum corneum and epidermis after iontophoresis was similar to that obtained after passive diffusion (Volpato et al. 1998). This is because acyclovir is essentially uncharged at physiological pH (pKa1 2.27; pKa2 9.25); hence EO is the only enhancing mechanism. However, even delivery by EO is compromised due to its low aqueous solubility (1.3 mg/ml at pH 7.4, 25 °C). For this reason, other studies employed formulations with extreme pH to have the drug molecule in an ionized state (Fig. 5.4). For example, after 10 min cathodal iontophoresis of acyclovir gel at pH 11 to hairless rats in vivo, fourfold more ACV was detected in the SC as compared with passive delivery (30.70 ± 4.83 and 7.83 ± 1.59 μg/cm2, respectively) (Siddoju et al. 2011). Improved delivery to the dermis was observed in rabbits in vivo after 1 h of cathodal iontophoresis at pH 11 (Shukla et al. 2009). However, although the authors reported there were no additional signs of skin irritation on the conditions used, it is rather implausible that a formulation with such an irritant pH can be of practical use.
Acyclovir ionization state, assuming an analytical concentration of Ca of 0.1 M. (Reproduced with permission from Shukla et al. (2009)
2.3 Delivery System
The iontophoretic delivery system comprises a microprocessor/power source and two electrode compartments. The “active” electrode contains the drug formulation, and the circuit is completed by the return electrode placed at an adjacent area on the skin. The system design may have an impact on patient compliance and hence on the efficiency of the treatment. However, the formulation and the electrodes may also affect drug delivery rates and safety.
The ideal formulation for iontophoretic application would be easy to apply, have good electrical conductivity, have good bioadhesion avoiding leakage, be compatible with the electrodes and the device, promote high drug stability, not be irritant to the skin, and not contain competing ions. In this way, hydrogels have been proposed as base formulations for iontophoretic delivery because of the high water content and consequent good electrical conductivity (Fang et al. 1999; Fang et al. 2001; Fang et al. 2002; Merclin et al. 2004; Jyoung et al. 2009; Taveira et al. 2009) but also because of their adhesiveness and biocompatibility (Alvarez-Figueroa and Blanco-Mendez 2001; Haak et al. 1994). However, in some cases anti-adherent hydrogel films that could be easily removed might be desirable. Such a formulation, composed of the polyelectrolyte poly(methyl vinyl ether-co-maleic acid) cross-linked in a 2:1 ratio with PEG 10,000, was investigated as a potential rapid photodynamic antimicrobial chemotherapy treatment for infected wounds using iontophoresis for the delivery of the photosensitizers meso-Tetra (N-methyl-4-pyridyl) porphine tetra tosylate (TMP), methylene blue (MB), and TMP with sodium dodecyl sulfate. The study demonstrated that formulation properties such as hydrogel hardness, compressibility, adhesiveness, and ionic conductivity could be influenced by the concentration of a component in the formulation. The authors concluded that hydrogels prepared from aqueous blends containing 10 % of the polymer loaded with TMP or MB were the most flexible (should conform most easily to wounds), least adhesive (reducing the potential trauma to the wound upon removal), and released the greatest amount of photosensitizer (ensuring the greatest extent of microbial kill in the wound) (Fallows et al. 2012). Indeed, studies demonstrate that network structure and composition can be manipulated to influence the permeation and diffusion characteristics of a drug within the hydrogel (Banga and Chien 1993), changes that should take into account the charge of both the polymer and the drug. Normally, drug release is reduced when the molecule has the opposite charge to the polymer and favored when they have the same charge (Tatavarti et al. 2004).
To improve iontophoretic delivery efficiency, the use of ion-exchange materials, such as ion-exchange membrane, has been proposed (Patel et al. 2007; Patel et al. 2009; Xu et al. 2009). The membranes used should have the opposite charge to that of the ionized drug, and when placed between the skin and the donor electrode, they would hinder the migration of competing counterions, selectively enhancing drug transport across the skin (Xu et al. 2009). A recent study showed that the use of drug in a complex with ion-exchange fibers might be more promising than the use of ion-exchange membranes. It was observed that when cathodal iontophoresis of diclofenac across rat skin in vitro and in vivo was carried out, drug bound to ion-exchange fibers with an ionic bond had a higher transference number than those having the drug bound to other ion-exchange materials or simply in solution (Che et al. 2012). Further studies with other molecules should be performed to confirm the promising results. As the field is constantly evolving, novel ion-exchange materials with higher efficiency on enhancing drug permeation may also be developed in the future.
Conclusion
The work performed to date using many different molecules has given us a better understanding of the advantages and limitations of the technique and the principal factors that impact on its efficiency. Analysis of the molecular properties is a first step in trying to predict feasibility of drug delivery and in identifying which parameters might affect transport rates. First, if it is positively charged, the relative contributions of EM and EO to the total flux need to be determined. If EO plays an important role, conditions that might reduce interactions with the skin penetration pathway should be used. If EM is the main transport mechanism, the pH should preferably favor drug ionization. Second, the impact of drug concentration in the formulation and current density must be evaluated since these would help to determine the treatment conditions; if the amount of compound delivered is directly proportional to the applied current or concentration, the duration of current application and the area of the skin surface in contact with the active electrode compartment can be calculated to deliver a specific dose of the drug molecule. In this way, it is possible to control drug delivery kinetics and allow individualization of the therapy. Although a better understanding of iontophoretic transport mechanisms is essential, it must be accompanied by progress in the enabling technologies required to develop iontophoretic patch systems. Only then will it be possible to create the patient-friendly, safe therapeutic systems that will enable the clinical applications described in the next chapter to be realized.
References
Abla N, Naik A, Guy RH, Kalia YN (2005) Contributions of electromigration and electroosmosis to peptide iontophoresis across intact and impaired skin. J Control Release 108:319–330
Aguilella V, Kontturi K, Murtomaki L, Ramirez P (1994) Estimation of the pore-size and charge-density in human cadaver skin. J Control Release 32:249–257
Alvarez-Figueroa MJ, Blanco-Mendez J (2001) Transdermal delivery of methotrexate: iontophoretic delivery from hydrogels and passive delivery from microemulsions. Int J Pharm 215:57–65
Banga AK, Chien YW (1993) Hydrogel-based iontotherapeutic delivery devices for transdermal delivery of peptide/protein drugs. Pharm Res 10:697–702
Burnette RR, Marrero D (1986) Comparison between the iontophoretic and passive transport of thyrotropin releasing hormone across excised nude mouse skin. J Pharm Sci 75:738–743
Cazares-Delgadillo J, Ganem-Rondero A, Quintanar-Guerrero D, Lopez-Castellano AC, Merino V, Kalia YN (2010) Using transdermal iontophoresis to increase granisetron delivery across skin in vitro and in vivo: Effect of experimental conditions and a comparison with other enhancement strategies. Eur J Pharm Sci 39:387–393
Che X, Wang LH, Yuan Y, Gao YN, Wang QF, Yang Y et al (2012) A novel method to enhance the efficiency of drug transdermal iontophoresis delivery by using complexes of drug and ion-exchange fibers. Int J Pharm 428:68–75
Craanevanhinsberg WHM, Bax L, Flinterman NHM, Verhoef J, Junginger HE, Bodde HE (1994) Iontophoresis of a model peptide across human skin in-vitro. Effects of iontophoresis protocol, pH, and ionic-strength on peptide flux and skin impedance. Pharm Res 11:1296–1300
Cullander C, Guy RH (1991) Sites of iontophoretic current flow into the skin: identification and characterization with the vibrating probe electrode. J Invest Dermatol 97:55–64
de Jalon EG, Blanco-Prieto MJ, Ygartua P, Santoyo S (2001) Topical application of acyclovir-loaded microparticles: quantification of the drug in porcine skin layers. J Control Release 75:191–197
Delgado-Charro MB, Guy RH (1994) Characterization of convective solvent flow during iontophoresis. Pharm Res 11:929–935
Delgado-Charro MB, Guy RH (1995) Iontophoretic delivery of nafarelin across the skin. Int J Pharm 117:165–172
Delgado-Charro MB, Guy RH (2001) Transdermal iontophoresis for controlled drug delivery and non-invasive monitoring. Stp Pharma Sci 11:403–414
Delgado-Charro MB, Rodriguezbayon AM, Guy RH (1995) Iontophoresis of nafarelin – effects of current-density and concentration on electrotransport in-vitro. J Control Release 35:35–40
Djabri A, Guy RH, Delgado-Charro MB (2012a) Transdermal iontophoresis of ranitidine: an opportunity in paediatric drug therapy. Int J Pharm 435:27–32a
Djabri A, Guy RH, Delgado-Charro MB (2012b) Passive and iontophoretic transdermal delivery of phenobarbital: Implications in paediatric therapy. Int J Pharm 435:76–82b
Fallows SJ, Garland MJ, Cassidy CM, Tunney MM, Singh TRR, Donnelly RF (2012) Electrically-responsive anti-adherent hydrogels for photodynamic antimicrobial chemotherapy. J Photochem Photobiol B-Biol 114:61–72
Fang JY, Hsu LR, Huang YB, Tsai YH (1999) Evaluation of transdermal iontophoresis of enoxacin from polymer formulations: in vitro skin permeation and in vivo microdialysis using Wistar rat as an animal model. Int J Pharm 180:137–149
Fang JY, Sung KC, Hu OYP, Chen HY (2001) Transdermal delivery of nalbuphine and nalbuphine pivalate from hydrogels by passive diffusion and iontophoresis. Drug Res 51:408–413
Fang JY, Sung KC, Wang JJ, Chu CC, Chen KT (2002) The effects of iontophoresis and electroporation on transdermal delivery of buprenorphine from solutions and hydrogels. J Pharm Pharmacol 54:1329–1337
Gratieri T, Kalia YN (2013) Mathematical models to describe iontophoretic transport in vitro and in vivo and the effect of current application on the skin barrier. Adv Drug Deliv Rev 65:315–329
Green P, Shroot B, Bernerd F, Pilgrim WR, Guy RH (1992) In vitro and in vivo iontophoresis of a tripeptide across nude rat skin. J Control Release 20:209–218
Haak RP, Gyory JR, Theeuwes F, Landrau FA, Roth N, Meyers RM (1994) Iontophoretic delivery device and methods of hydrating same. US5320598
Hirvonen J, Guy RH (1997) Iontophoretic delivery across the skin: electroosmosis and its modulation by drug substances. Pharm Res 14:1258–1263
Hirvonen J, Kalia YN, Guy RH (1996) Transdermal delivery of peptides by iontophoresis. Nat Biotechnol 14:1710–1713
Hoogstraate AJ, Srinivasan V, Sims SM, Higuchi WI (1994) Iontophoretic enhancement of peptides – behavior of leuprolide versus model permeants. J Control Release 31:41–47
Jadoul A, Bouwstra J, Preat V (1999) Effects of iontophoresis and electroporation on the stratum corneum – review of the biophysical studies. Adv Drug Deliv Rev 35:89–105
Jyoung JY, Shim BS, Cho DE, Hwang IS (2009) Iontophoretic transdermal delivery of alendronate in hairless mouse skin. Polymer-Korea 33:237–242
Kalaria DR, Patel P, Patravale V, Kalia YN (2012) Comparison of the cutaneous iontophoretic delivery of rasagiline and selegiline across porcine and human skin in vitro. Int J Pharm 438:202–208
Kalia YN, Naik A, Garrison J, Guy RH (2004) Iontophoretic drug delivery. Adv Drug Deliv Rev 56:619–658
Kasting GB (1992) Theoretical-models for iontophoretic delivery. Adv Drug Del Rev 9:177–199
Kasting GB, Keister JC (1989) Application of electrodiffusion theory for a homogeneous membrane to iontophoretic transport through skin. J Control Release 8:195–210
Lau DT, Sharkey JW, Petryk L, Mancuso FA, Yu Z, Tse FL (1994) Effect of current magnitude and drug concentration on iontophoretic delivery of octreotide acetate (Sandostatin) in the rabbit. Pharm Res 11:1742–1746
Levin J, Maibach H (2008) Human skin buffering capacity: an overview. Skin Res Technol 14:121–126
Lu MF, Lee D, Carlson R, Rao GS, Hui HW, Adjei L et al (1993) The effects of formulation variables on iontophoretic transdermal delivery of leuprolide to humans. Drug Dev Ind Pharm 19:1557–1571
Marro D, Guy RH, Delgado-Charro MB (2001a) Characterization of the iontophoretic permselectivity properties of human and pig skin. J Control Release 70:213–7a
Marro D, Kalia YN, Delgado-Charro MB, Guy RH (2001b) Contributions of electromigration and electroosmosis to iontophoretic drug delivery. Pharm Res 18:1701–8b
Merclin N, Bramer T, Edsman K (2004) Iontophoretic delivery of 5-aminolevulinic acid and its methyl ester using a carbopol gel as vehicle. J Control Release 98:57–65
Morrel EM, Spruance SL, Goldberg DI (2006) Topical iontophoretic administration of acyclovir for the episodic treatment of herpes labialis: a randomized, double-blind, placebo-controlled, clinic-initiated trial. Clin Infect Dis 43:460–467
Mudry B, Guy RH, Begona Delgado-Charro M (2006a) Prediction of iontophoretic transport across the skin. J Control Release 111:362–7a
Mudry B, Guy RH, Delgado-Charro MB (2006b) Transport numbers in transdermal iontophoresis. Biophys J 90:2822–30b
Mudry B, Guy RH, Delgado-Charro MB (2006c) Electromigration of ions across the skin: determination and prediction of transport numbers. J Pharm Sci 95:561–9c
Nair V, Panchagnula R (2003) Physicochemical considerations in the iontophoretic delivery of a small peptide: in vitro studies using arginine vasopressin as a model peptide. Pharm Res 48:175–182
Padula C, Sartori F, Marra F, Santi P (2005) The influence of iontophoresis on acyclovir transport and accumulation in rabbit ear skin. Pharm Res 22:1519–1524
Panzade P, Heda A, Puranik P, Patni M, Mogal V (2012) Enhanced transdermal delivery of granisetron by using iontophoresis. Iran J Pharm Res 11:503–512
Patel SR, Zhong H, Sharma A, Kalia YN (2007) In vitro and in vivo evaluation of the transdermal iontophoretic delivery of sumatriptan succinate. Eur J Pharm Biopharm 66:296–301
Patel SR, Zhong H, Sharma A, Kalia YN (2009) Controlled non-invasive transdermal iontophoretic delivery of zolmitriptan hydrochloride in vitro and in vivo. Eur J Pharm Biopharm 72:304–309
Phipps JB, Gyory JR (1992) Transdermal ion migration. Adv Drug Deliv Rev 9:137–176
Phipps JB, Padmanabhan RV, Lattin GA (1989) Iontophoretic delivery of model inorganic and drug ions. J Pharm Sci 78:365–369
Pikal MJ (1990) Transport Mechanisms in Iontophoresis. 1. A theoretical-model for the effect of electroosmotic flow on flux enhancement in transdermal iontophoresis. Pharm Res 7:118–126
Pikal MJ (1992) The role of electroosmotic flow in transdermal iontophoresis. Adv Drug Deliv Rev 9:201–237
Pikal MJ (2001) The role of electroosmotic flow in transdermal iontophoresis. Adv Drug Deliv Rev 46:281–305
Rodriguez Bayon AM, Guy RH (1996) Iontophoresis of nafarelin across human skin in vitro. Pharm Res 13:798–800
Sage BH, Riviere JE (1992) Model systems in iontophoresis transport efficacy. Adv Drug Deliv Rev 9:265–287
Schuetz YB, Naik A, Guy RH, Vuaridel E, Kalia YN (2005) Transdermal iontophoretic delivery of triptorelin in vitro. J Pharm Sci 94:2175–2182
Shukla C, Friden P, Juluru R, Stagni G (2009) In vivo quantification of acyclovir exposure in the dermis following iontophoresis of semisolid formulations. J Pharm Sci 98:917–925
Siddoju S, Sachdeva V, Friden PM, Yu YY, Banga AK (2011) Acyclovir skin depot characterization following in vivo iontophoretic delivery. Skin Res Technol 17:234–244
Srinivasan V, Higuchi WI (1990) A model for iontophoresis incorporating the effect of convective solvent flow. Int J Pharm 60:133–138
Stagni G, Ali ME, Weng D (2004) Pharmacokinetics of acyclovir in rabbit skin after IV-bolus, ointment, and iontophoretic administrations. Int J Pharm 274:201–211
Tatavarti AS, Mehta KA, Augsburger LL, Hoag SW (2004) Influence of methacrylic and acrylic acid polymers on the release performance of weakly basic drugs from sustained release hydrophilic matrices. J Pharm Sci 93:2319–2331
Taveira SF, Nomizo A, Lopez RFV (2009) Effect of the iontophoresis of a chitosan gel on doxorubicin skin penetration and cytotoxicity. J Control Release 134:35–40
Volpato NM, Santi P, Colombo P (1995) Iontophoresis enhances the transport of acyclovir through nude-mouse skin by electrorepulsion and electroosmosis. Pharm Res 12:1623–1627
Volpato NM, Nicoli S, Laureri C, Colombo P, Santi P (1998) In vitro acyclovir distribution in human skin layers after transdermal iontophoresis. J Control Release 50:291–296
Xu QF, Ibrahim SA, Higuchi WI, Li SK (2009) Ion-exchange membrane assisted transdermal iontophoretic delivery of salicylate and acyclovir. Int J Pharm 369:105–113
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Gratieri, T., Kalia, Y.N. (2017). Iontophoretic Transport Mechanisms and Factors Affecting Electrically Assisted Delivery. In: Dragicevic, N., I. Maibach, H. (eds) Percutaneous Penetration Enhancers Physical Methods in Penetration Enhancement. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-53273-7_5
Download citation
DOI: https://doi.org/10.1007/978-3-662-53273-7_5
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-53271-3
Online ISBN: 978-3-662-53273-7
eBook Packages: MedicineMedicine (R0)