Abstract
Liposuction (blunt suction lipectomy) is now well established and has generally gratifying aesthetic results. Since first described in 1977 by Illouz, changes or improvements to the technique of liposuction have been introduced regarding instruments (cannulas, pumps, syringes, and various devices), depth of suctioning (deep or superficial), volume of fluid infiltration (wet, super wet, tumescent), and osmolarity (isotonic, more or less hypotonic). Many other changes or “innovations” were also described that deserve being denounced. We report several complications resulting in severe skin necrosis, following liposuction and lipolysis methods of questionable scientific merits: ultrasonic liposuction, infiltration of hypo-osmolar solution, lipolysis without aspiration, or after unfortunately accidental infiltration of hypertonic saline solution. Ensuing skin necrosis required surgical debridement followed by prolonged secondary wound healing, resulting in severe aesthetic and functional sequelae with inevitable malpractice legal implications. It is essential that plastic surgeons be careful about using techniques widely advertised by the media but not yet scientifically validated; basic precautionary principles must be respected (light hypo-osmolar infiltration about 200 mOsm is safe), and the surgeons should not be dispensed from applying rigorous monitoring and strict safety measures in the operating room (checklist, traceability, qualification of nursing staff, etc.).
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction
Liposuction is a surgical procedure intended to remove fat deposits and shape the body. It is not a trivial surgery, not always benign [1, 2], not quite safe as claimed by glossy brochures as says Grazer. Nevertheless, since first described by Illouz in 1977 [3, 4], liposuction developed to become the most performed plastic surgery procedure worldwide. Numerous modifications and refinements of the basic original technique have been proposed regarding equipment (cannulas, infiltration pumps, aspiration syringes and machines), level of lipo-aspiration (deep or superficial), nature of the infiltration solution, and the injected volume. A non-negligible incidence of complications, namely, severe skin necrosis, has been reported following the performance of more or less scientifically validated liposuction procedures. Similar complications have also been reported following the unfortunate or accidental infiltration with hypertonic solutions. Alternatively, numerous nonsurgical lipolysis modalities have been proposed. Infiltration of hypo-osmolar solution without aspiration has not only been proved to be ineffective, but it has resulted in severe complications such as infection and scarring. As new technologies are being continuously described and introduced, enthusiasm about these technologies must be tempered and only procedures with solid scientific basis and proven efficacy must be performed [5].
This report, without being an inclusive review, is intended to highlight several serious side effects following some of these procedures we have observed in our function of medical experts for medicolegal cases. Therefore, liposuction is now well codified and generally has gratified results: simple precautionary principles must be respected to avoid these harmful effects, and for us, a light hypo-osmolar infiltration followed by aspiration is the technique of choice, safe, and effective: we will describe this procedure at the end of our paper.
2 Authors’ Cases
2.1 Ultrasound Liposuction
Ultrasonic liposuction, also called ultrasonic-assisted liposuction, or UAL for short, is one of the latest developments in the field. Liposuction with focused ultrasound energy cannulas has many supports in Europe [6] and South America but it has also numerous opponents because of its still questionable safety. Fat is removed from under the skin with the use of a vacuum-suction cannula (a hollow pen-like instrument) or using an ultrasonic probe that emulsify (breaks up into small pieces) the fat and then removes it with suction.
2.1.1 Case 1
This 44-year-old woman, employee in a pizzeria, underwent under local anesthesia ultrasound liposuction of the abdomen by a general practitioner. The procedure duration was 3 h 30 min. On examination, deep burn with extensive skin necrosis is observed on the left flank (Fig. 87.1). The physician tried to justify to no avail this complication by claiming that since the patient returned to work the following day, she was exposed too soon after the procedure to the oven heat. Delayed wound healing took 5 months to be completed at the expense of extensive scarring.
2.1.2 Case 2
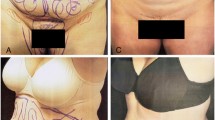
This 36-year-old woman underwent ultrasound liposuction by a general practitioner resulting in serious burns of the inner thighs (Fig. 87.2). Six months of conservative therapy were required for healing of the right thigh. The left thigh, however, required a STSG that was later excised following tissue expansion and scar revision with flaps. Nevertheless, the patient was left with an obvious scar on the medial aspect of the left thigh with lesser scarring on the right [7].
(a) 36-year-old woman underwent ultrasound liposuction, sustaining burns of the inner thighs. (b) The left thigh required a split-thickness skin graft (STSG). (c) The left thigh had tissue expansion before revision. (d) Healing of the right thigh took 6 months of conservative therapy. The left thigh had excision of STSG following tissue expansion and scar revision with flaps
In both cases, the expert legal opinion confirmed the total responsibility of the two physicians.
2.2 Liposuction following Injection by Mistake of Hyperosmolar Solution
2.2.1 Case 3
A 44-year-old female with medial upper thighs lipodystrophy underwent medial thigh lift with associated liposuction by a plastic surgeon. Within few days, skin necrosis developed more on right than left with obvious scars shown by Fig. 87.3 [8].
2.2.2 Case 4
A young woman 24 years of age (Fig. 87.4) was operated on with liposuction only by another well-experienced plastic surgeon in the same clinic and the same operating theater as in Case 3. Similarly, this patient developed rapidly skin necrosis over the right medial thigh that slowly healed to result 7 months later in serious scarring.
The occurrence of skin necrosis in two successive patients 1 month apart operated by two different surgeons but in the same clinic and operating theater and with the same nurse was highly suspicious. It was realized then that the fluid used for infiltration was in fact a 30 % hyper-osmolar solution usually used for treatment of hydatid cysts. Unfortunately, the iso- and hyper-osmolar containers were placed on the same shelf in the pharmacy (Fig. 87.5). The same nurse that was hired temporarily for replacement has prepared the infiltration solution. Apparently hyper-osmolar saline solution was used and was inadvertently injected. Skin necrosis of the second patient was more pronounced on the right side probably because liposuction was performed first at the left, resulting without knowing in early aspiration of some infiltration solution, thus reducing its harmful effect. The expert legal opinion was that the nurse is to be blamed. For the judge, the head of the treating team, namely, the surgeon, had to instruct each member of his team about his or her duties; however, it is not possible for him to check the prepared solution and to know its final composition before injection. This is an important legal consideration to declare that the surgeon is not guilty of negligence and that he did not commit any surgical error. The clinic, employer of the temporary nurse, was held responsible; however, this ruling should not dispense the surgeon from preoperative checking of all material used [9–11].
2.2.3 Case 5
The figures illustrate the result following inadvertent subcutaneous injection of hyper-osmolar solution before aspiration. Necrotic tissues had to be subsequently excised (Fig. 87.6; republished with permission [12]).
3 Lipolysis and Lipotomy
Many lipolysis procedures are widely advertised in magazines for women promoting nonsurgical incisions and resulting in a dream body shape and a sublime silhouette. These are “lunchtime procedures” utilizing the latest technologies such as laser (thermal laser technologies, lipo laser, micro lipolaser, UltraPulse fractional laser), ultrasound (focused external ultrasound or UltraShape), external application of high-intensity focused ultrasound (HIFU) (Liposonix) for body sculpting equipment and the nonsurgical ultrasound lipoplasty [13] cryolipolysis (selective cryolipolysis controlled cooling of the subcutaneous fat), infrared, or finally radiofrequency (BodyTite bipolar radiofrequency).
All these nonsurgical techniques aiming at localized adipolysis have never been validated scientifically even though they have been unfortunately mentioned in the official plastic surgery journal reporting with conflicting and poorly verifiable results.
-
1.
Injection lipolysis
These various procedures such as Lipodissolve, Lipostabil, or phosphatidylcholine have many documented side effects (pain and hyperpigmentation) and are not authorized in France [14].
-
2.
Lipotomy (hypo-osmolar lipotomy)
Adipocytolysis is presented by the authors as an alternative to liposuction technique, utilizing osmosis physiological mechanism.
3.1 What Is Osmosis?
From Greek osmos = pushing. It is a diffusion process (physiological fact) when two solutions with different concentrations are separated by partial permeability membrane; there is a transfer from the hypotonic toward the hypertonic solution through this membrane (water only but not dissolved substance).
3.2 Physical Mechanism of Lipotomy
Normal osmolar intra-tissue (isotonia) is about 300 mOsm. With hypo-osmolar solution (90/150 mOsm), the water is transferred into fat cells and increases intramembrane pressure (reverse osmosis). Swelling and cellular explosion with interstitial triglyceride release (glycerol and fatty acids) residues that should be picked up by lymph or eliminated by urine (Fig. 87.7). This theory is very controversial and the authors insist on associated dispositions like musculation, sport activities, and external ultrasound to eliminate free fatty acids. So no fat aspiration is performed [15, 16]. Lipotomy procedures have different names (Table 87.1).
Frequently these procedures are followed by superficial burns, abscess, oily collections, necrosis, and severe troubles of healing. In a clinical case, a 14-year-old female had a postoperative problem that was polymicrobial subcutaneous abscess that needed two surgical evacuations and had very bad aesthetic result (Fig. 87.8) [17].
Other cases observed in medicolegal situations include a 60-year-old woman, 1.63 m, 95 kg after abdominal hypo-osmolar lipotomy with very bad result after a long healing evolution (Fig. 87.9), and a relative of the precedent, 41-year-old, 1.60 m, 72 kg, had bilateral hip lipodystrophy with the same technique. Postoperatively there was temperature elevation, abscess, and necrosis that occurred 5 months after, and after 1 year, it showed a worsening of lipodystrophy (Fig. 87.10).
Lipolysis by hypo-osmolar lipotomy without liposuction is in fact a noninvasive technique invented for medical practitioners but has no true scientific evaluation (tolerance, efficiency) and had bad results and risk of serious complications. It is a non-validated technique in France.
4 Merits of Light Hypo-osmolar Liposuction
Beware of confusing hypo-osmolar lipotomy (adipo-cytolyse without aspiration) with harmful effects described and hypo-osmolar liposuction with infiltration before aspiration is performed by a light hypotonic solution (200–220 mOsm), so aspiration of burst adipocytes and fat liquefied is easier.
Some examples of hypotonic solutions:
-
1.
Saline 1,000 mL plus distilled water 200 mL = 230 mOsm
-
2.
Saline 1,000 mL plus distilled water 300 mL = 200 mOsm
-
3.
Saline 1,000 mL plus distilled water 1,000 mL = 150 mOsm
Wetting Solutions
-
1.
Majority use isotonic solutions (Fournier, Klein, Mang, Cook, Asken, Hetter, Hunstadt, Avelar, Rebello, Georgiade).
-
2.
Minority use hypotonic solutions: Illouz: light hypotonia: 230 mOsm.
-
3.
Strong hypotonia is used by Zocchi:150 mOsm.
-
4.
Severe hypotonia: 90/150 mOsm is used by medical practitioners and is very dangerous, because there is no aspiration, only biological reabsorption.
Authors’ Wetting Solution
-
Saline 1,000 mL plus distilled water: 300 mL plus lidocaine and epinephrine, light hypo-osmolarity = 200 mOsm
Liposuction begins 20 min after infiltration; temperature solution = room temperature. Fat is more clear (Fig. 87.11) and easier to aspirate, and fat is medium in quantity (3 or 4 l) (Fig. 87.12). Skin retraction is better; return to activity is earlier and better results are observed after 1 month.
So do not reject the hypo-osmolarity concept. Many plastic surgeons, adding water to their solution, are unknowingly using a hypo-osmolar procedure. Liposuction, after a moderate hypo-osmolar infiltration about 200 mOsm, is a good technique, safe, and efficient.
5 Conclusion
Be careful to use techniques that are not yet validated but advertised by the media. Simple precautionary principles must be respected (light hypo-osmolar solution followed by aspiration is safe). Apply rigorous monitoring and safety measures in the operating room (checklist, traceability, qualification of nurse staff). Do not forget medicolegal aspect and choose good insurance.
References
Mole B. Liposuction and extensive cutaneous necrosis. Ann Chir Plast Esthet. 1994;39(2):251–4.
Gibbons M, Lim R. Necrotizing fasciitis after tumescent liposuction. Ann Surg. 1998;64(5):458–60.
Illouz YG. Surgical remodelling of the silhouette by aspiration lipolysis or selective lipectomy. Aesthetic Plast Surg. 1985;9(1):7–21.
Illouz YG. Liposculpture et chirurgie de la silhouette. In: EMC, editor. Techniques Chirurgicales: Chirurgie Plastique Reconstructive et Esthétique. Paris: Elsevier Masson; 2008. p. 45–120.
Stephan PJ, Kenkel JM. Updates and advances in liposuction. Aesthet Surg J. 2010;30(1):83–97.
Zocchi M. Basic physics for ultrasound-assisted lipoplasty. Clin Plast Surg. 1999;26(2):209–20.
Grolleau JL, Rougé D, Chavoin JP, Costagliola M. Severe cutaneous necrosis after ultrasound lipolysis; medico legal aspects and review. Ann Chir Plast Esthet. 1997;42(1):31–6.
Chaput B, Fade G, Grolleau JL AA, Garrido I. Liposuction: an exceptional case of skin necrosis secondary to an error of infiltration. Plast Reconstr Surg. 2012;129(4):765e–6.
Campbell B, Callum K, Peacock N. Operating with the law a practical guide for surgeons and lawyers. London: Trinity Press; 2011.
Rougé D, Escat J, Costagliola M. Responsabilité Médicale: de la Chirurgie à l’Esthétique. Paris: Arnette; 1992.
Costagliola M, Chaput B. What are the limits of the surgeon’s responsibility in the operating theater?, Aesthetic Plast Surg. 2014;38(4):830–1. doi: 10.1007/s00266-014-0331-5. Epub 2014 May 31.
Kerfant N, Philandrianos C, Alliez A, Casanova D. Inadvertent subcutaneous injection of hypertonic saline solution during lipofilling. Aesthetic Plast Surg. 2013;37(4):709–10.
Fodor PB. Reflections on lipoplasty: history and personal experience. Aesthet Surg J. 2009;29(3):226–31.
Journal Oficiel Ministère du travail, emploi et santé. Interdiction des techniques de lipolyse adipocytaires à visée esthétique; Décret n° 2011-382, 11 Avril 2011. http://legifrance.gouv.fr/eli/decret/2011/4/11/ETSP1107628D/jo/texte Accessed 9 Apr 2015.
Hoeflin S. Lipoplasty with hypotonic pharmacologic lipo-dissolution. Aesthet Surg J. 2002;22(6):573–6.
Song A, Benett J, Marra K, Cimino W, Rubin P. Scientific basis of the use of hypotonic solutions with ultrasonic liposuction. Aesthetic Plast Surg. 2006;30(2):233–8.
Benjoar M, Lepage C, Hivelin M. Lantiéri Complications d’injection de solutés hypo osmotiques chez une patiente mineure. Ann Chir Plast Esthet. 2008;54(2):161–4.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Costagliola, M., Atiyeh, B., Rampillon, F., Chaput, B. (2016). Harmful Effects of Liposuction and Lipolysis Procedures Questionable Safety and Scientific Validity: A Medico-Legal Perspective and Advantages of “Light” Hypo-osmolar Liposuction. In: Shiffman, M., Di Giuseppe, A. (eds) Liposuction. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-48903-1_87
Download citation
DOI: https://doi.org/10.1007/978-3-662-48903-1_87
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-48901-7
Online ISBN: 978-3-662-48903-1
eBook Packages: MedicineMedicine (R0)