Abstract
This chapter guides ambulatory educators through the key educational principles, components, and steps needed for a robust ambulatory curriculum with a longitudinal design and a diverse delivery mechanism. Ambulatory medical education for residents is structured into three major curricula designs—ambulatory block rotations, longitudinal continuity clinics, and ambulatory long blocks. Embedded into these curricular designs is a core curricular thread comprised of high-yield ambulatory topics and delivered through various teaching pedagogies. Highlighted in this chapter are specific formal instructional strategies as well as resident-directed learning modalities. The chapter concludes with a step-by-step guide of the essential elements in developing an ambulatory curriculum. Sample implementation tools provide deliverables for educators to utilize in their own ambulatory teaching environment. These include needs assessment tools, mini-CEX forms, and a goal and objective template for resident continuity clinics.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
The Accreditation Council for Graduate Medical Education (ACGME) issued significant requirement changes in 2009 for one-third of residency training to occur in the ambulatory setting [1]. The Alliance for Academic Internal Medicine (AAIM) and ACGME have advocated for decreasing the conflict between inpatient and outpatient experiences [1, 2]. These changes emphasize the need for the graduate medical education (GME) system to revitalize residents’ ambulatory education.
Reform of ambulatory training in internal medicine is twofold. First, it requires improving the system infrastructure of the clinic itself, and secondly it mandates enhancing the educational experience of residents within the clinic [3]. Part of that movement includes a longitudinal ambulatory curricular design that enhances the resident continuity clinic experience and provides residents with a foundation for learning ambulatory medicine. Most ambulatory medical education is structured into three curricula designs—ambulatory block rotations typically embedded through x + y scheduling , longitudinal continuity clinics, and ambulatory long blocks. Ambulatory blocks arranged in an x + y model provide a 1–2-week concentrated clinic experience in various ambulatory disciplines. Longitudinal continuity clinics allow the opportunity to manage a panel of patients on a weekly basis over the entire training period. The innovative ambulatory long blocks entrench residents in a 6–12-month ambulatory clinic immersion. More details on these ambulatory curricular designs are on chapter “Traditional and Block Scheduling Challenges and Solutions for Internal Medicine Residents.” Many resident continuity clinics provide some type of on-site instructional modality, usually as a preclinical conference or an ambulatory case-based discussion to disseminate a core curricular thread of high-yield ambulatory topics [3]. Residency clinic directors and program leadership have a responsibility to ensure a well-rounded longitudinal ambulatory experience focused around achievable learning objectives.
Learning Objectives
-
1.
Gain knowledge of the three major ambulatory curricular designs—ambulatory block rotations, longitudinal continuity clinics, and ambulatory long blocks.
-
2.
Learn the key principles and instructional modalities effective in ambulatory curricula.
-
3.
Provide a step-by-step guide and sample toolkits to develop and implement a robust ambulatory curriculum at one’s home institution.
Outline
-
Educational Principles and Steps in Ambulatory Curriculum Design
-
Curriculum Steering Committee for Educational Planning and Problem Identification
-
General and Targeted Educational Needs Assessment
-
Goals and Objectives for Continuity Clinics in Relationship to ACGME Competencies
-
Educational Strategies: Structured Core Curricular Content and Delivery Strategies
-
Implementation with Bidirectional Evaluation and Feedback
-
Ambulatory Faculty Development Needs
-
-
Ambulatory Curriculum Delivery
-
Core Curricular Content
-
Teaching Methods/Instructional Strategies: Formal Instruction
-
Small Group Sessions
-
Ambulatory Morning Report
-
Evidence-Based Learning
-
Ambulatory Journal Club
-
PICO Reports
-
-
Structured Clinical Observations
-
CEX/Mini-CEX
-
-
Patient Simulation Exercises
-
-
Teaching Methods/Instructional Strategies: Resident-Directed Learning
-
Team-Based Learning (TBL)
-
Problem-Based Learning (PBL)
-
Flipped Classroom
-
Web-Based Learning Modules
-
Quality Improvement Instruction and Application
-
-
-
Ambulatory Curriculum Design and Venue
-
Developing an Ambulatory Curriculum in One’s Own Academic Clinic
-
Step-by-Step Guide of Essential Elements in Developing an Ambulatory Curriculum
-
Existing Ambulatory Curricula
-
Educational Principles and Steps in Ambulatory Medicine Curriculum Design
Valuable resources exist to guide faculty in the development of medical education curriculum. Three well-cited books include Curriculum Development for Medical Education: A Six-Step Approach by Thomas et al. [4], Community-based Teaching: A Guide to Developing Education Programs for Medical Students and Residents in the Practitioner’s Office by the American College of Physicians [5], and The Toolkit Series: A Textbook for Internal Medicine Education Programs by the Alliance for Academic Internal Medicine [6]. Online resources are also available in three major categories to assist educators in curriculum development—resources from medical accrediting organizations [i.e., Association of American Medical Colleges, American Board of Internal Medicine (ABIM), Accreditation Council for Graduate Medical Education (ACGME)], topic-specific resources, and general medical education journals [7, 8].
A robust ambulatory medicine curriculum relies on a number of key principles and essential steps in educational curriculum planning as detailed below and in section “Conclusion.”
Curriculum Steering Committee for Educational Planning and Problem Identification
One faculty individual should be identified to oversee the ambulatory curriculum development process. Alternatively, the role can be shared by a couple of individuals, e.g., associate program director and clinic director. This person(s) is responsible for the day-to-day logistical planning of the curriculum, including scheduling of the curriculum in residents’ continuity clinics, recruiting relevant presenters, and ensuring collection and aggregation of curriculum evaluation. A curriculum steering committee of key ambulatory stakeholders should also be established to provide input and identify deficits or problems in the ambulatory curriculum. This committee focusing on improving ambulatory education will continually review and update the curricular content at least annually. This committee is distinct from the Program Evaluation Committee of the residency program. Key stakeholders should include the residency clinic directors, clinic preceptors, ambulatory chief resident, and residency program director. The latter two individuals make certain that the clinic curriculum aligns with ACGME requirements and is well-integrated into the residency program.
General and Targeted Educational Needs Assessment
The needs assessment process is an important step to inform relevant curricular content and design. This step must involve not only a general analysis of the institution’s educational and programmatic needs but also a targeted assessment of learners’ needs [4, 8]. This requires alignment of the program’s curriculum to ACGME/ABIM mandates and expert recommendations from major medical education organizations. Both general and targeted needs assessment can be done through various methods including, but not limited to stakeholder surveys, town hall meetings, focus group discussions, individualized faculty or resident interviews, In-Training Exam (ITE) performance on ambulatory topics, direct observation of stakeholders’ skills, and audits of current stakeholders’ performance. Additional curriculum needs assessments must conclude with a review of the literature for related ambulatory education curriculum and a collection of all the available resources. Appendices 1 and 2 provide samples of general and targeted needs assessment templates for ambulatory curriculum development.
Goals and Objectives for Continuity Clinics in Relationship to ACGME Competencies
The ACGME requires all training programs to develop specific goals and objectives for their ambulatory clinic curriculum. Goals are set in SMART format—specific, measurable, attainable, relevant, and timely [9, 10] (Table 1). Specific learning objectives make goals more concrete, prioritize curricular content, allow for direct evaluation, and tailor the individual clinic learning [8].
Goals and objectives for any ambulatory clinic curriculum must reflect the six domains of the ACGME milestones competencies [11]—patient care, medical knowledge, practice-based learning and improvement, interpersonal skills and communication, professionalism, and system-based practice (sample, Appendix 3). These educational goals and objectives should be reviewed with residents and preceptors on at least a semiannual basis. Residency program directors must verify residents’ clinical competence and performance trajectory in the six milestones core competencies within ambulatory education. The websites of both AAIM ( http://www.im.org/p/cm/ld/fid=464 ) and ACGME ( http://www.acgme.org/What-We-Do/Accreditation/Milestones/Overview ) publish milestones guidebooks and developmental toolkits in competency-based medical education for any program to adapt accordingly.
Educational Strategies: Structured Core Curricular Content and Delivery Strategies
A core curricular thread comprised of supplemental teaching modalities is a fundamental component of any ambulatory medicine curriculum . This helps to consolidate ambulatory concepts with learning in the clinical setting, promote self-directed learning beyond patient cases seen, and solidify clinical practice with evidence-based medicine [13,14,15,16,17,18]. A robust ambulatory curriculum should incorporate a balance of experiential training from direct patient care (e.g., acute care, chronic disease management, office-based procedures), formal educational instruction (e.g., teaching conferences, case-based small group sessions, web-based modules), and resident-driven learning strategies (e.g., problem-based learning, team-based learning, QI mini-projects, resident-led workshops, flipped classroom model).
Clear, achievable learning objectives should be established for each teaching pedagogy and its curricular contents updated at least annually. Emphasis must be placed on critical reasoning and active adult learning in small group settings; ambulatory curriculum has shifted away from traditional lecture-based teaching to problem-based learning [19,20,21]. Core curricular contents can be delivered in a variety of effective pedagogical venues including, but not limited to, ambulatory conference series, ambulatory medicine morning report, ambulatory medicine journal clubs, online learning modules, and patient simulation exercises.
Implementation with Bidirectional Evaluation and Feedback
Implementation of any ambulatory curriculum must first address barriers and identify resources and appropriate support. A rigorous evaluation system must then be established to routinely gauge its educational programming and primary stakeholders (i.e., residents, clinic staff, and faculty preceptors). Curricular metrics reflect outcomes-focused learning objectives and assess the level of milestones-specific competencies acquired by residents in the longitudinal care of their primary care patients [8]. Internal evaluation of the ambulatory curriculum should be done at least semiannually to ensure timely improvements to the overall program.
Bidirectional evaluations of both residents and faculty preceptors are an integral component of any ambulatory curriculum. Resident ambulatory evaluation data can originate from a variety of sources including, but not limited to, direct observation of patient encounters, mini-Clinical Evaluation Exercise (mini-CEX) , Objective Structured Clinical Examination (OSCE) , chart-simulated recall, and multisource feedback. These formative evaluations of residents are continuous throughout the academic year. The faculty clinic preceptor should complete a semiannual evaluation every 6 months on residents’ performance in ambulatory milestones competencies to align with the Clinical Competency Committee (CCC) report to ACGME. To ensure reciprocity, faculty evaluation data should ideally be collected primarily from residents’ and peers’ confidential feedback of teaching performance. ACGME Common Program Requirements stipulate at minimum a yearly evaluation of faculty performance and include “a review of the faculty’s clinical teaching abilities, commitment to the educational program, clinical knowledge, professionalism, and scholarly activities” [1] (see chapter “Clinic Evaluations and Milestones”).
Ambulatory Faculty Development Needs
Any ambulatory curriculum capitalizes on the clinical and teaching skills of the ambulatory faculty but will require a well-structured plan for ambulatory faculty development to ensure successful curriculum implementation. Faculty development programs are important to train clinic faculty on a variety of ambulatory teaching skills and instructional pedagogies. Ambulatory faculty must be able to skillfully diagnose patients’ complaints while assessing and teaching to their learner’s needs. To do so, faculty preceptors should be trained in effective ambulatory teaching models such as the One-Minute Preceptor and SNAPPS (Summarize, Narrow, Analyze, Probe, Plan, and Select) [22,23,24,25]. These validated models help to extract the highest-yield ambulatory concepts for learners in the busy ambulatory setting. See chapter “Medical Students in Clinic” for further details. The Education Committee of the American College of Physicians has even advocated for a “core faculty” group comprised of seasoned clinician educators who are “provided sufficient time, financial remuneration, academic status, and institutional recognition for teaching, evaluating, supervising and mentoring trainees” [26] (See for more details chapter “Supervising and Supporting Faculty” and chapter “Faculty Recruitment and Retention”).
Ambulatory Curriculum Delivery
Core Curricular Content
Clinical experience alone is limited in its ability to cover the breadth of knowledge in the outpatient setting given time constraints and differing patient experiences. Ambulatory didactics are needed to solidify ambulatory concepts beyond specific patient encounters and incorporate evidence-based medicine for high-quality care and lifelong learning [13, 14].
The standard curriculum must cover core ambulatory contents that will empower residents to practice outpatient medicine in any setting, whether in primary care or subspecialty medicine [27]. Ambulatory content can be further individualized to the clinical experiences of the specific academic institutions. Preventive medicine is a key component of primary care, and residents should be taught guideline-based and evidence-based preventative care measures. Curricula should further include such topics as billing and coding, panel management, team-based care, patient-physician communication, chronic disease management, electronic health record management, quality improvement/patient safety, and high-value care [28,29,30]. Depending on institutional needs and interests, programs may consider specialized topics addressing chronic pain and addiction medicine, social determinants of health, immigrant or refugee health, geriatrics, transgender health, or LGBT care. Maintaining a 12-month to 36-month core curricular thread of ambulatory topics will ensure a rigorous and balanced educational exposure (Appendix 6).
Teaching Methods and Instructional Strategies: Formal Instruction
Small Group Sessions
Small group sessions in the ambulatory setting can be a valuable tool to enhance outpatient learning. The small group allows for learner engagement, interactive didactics, and a forum to cover many broad clinical topics not commonly present in the clinic. Small groups can be utilized within the construct of a larger curriculum, e.g., Yale Office-Based Medicine Curriculum [31], or can be learner-directed [32] in the clinic. Small groups can focus on specific skills teaching [33] or work to improve subjective skills such as patient interviewing [34]. These small group sessions are particularly useful if there is a specific gap in education recognized by the program.
Ambulatory Morning Report
Morning report is a classic educational model that can be adapted to the ambulatory setting. Traditionally, morning report consists of case-based education where learners and teachers interact in a dynamic process to discuss patient care [35, 36]. However, there is no formal definition, and no effective format is noted in the literature [35]. In the ambulatory setting, morning report is an excellent venue to introduce common outpatient medical problems and share experiences among a larger group of residents [37]. A few studies noted that the topics presented in ambulatory morning reports are more general and more practical than inpatient topics [37, 38].
For those residency programs with an established inpatient morning report, adapting this educational modality to the clinic is simple. The key aspect is faculty and resident buy-in to ensure that the sessions are interactive and supported by faculty presence. Interactive discussions during morning report would then take place with chief resident or attending input. Despite being called “morning” report, there is no specific best time and/or frequency for morning report, as long as attendance can be assured [35]. Ambulatory morning report has been used to teach evidence-based medicine [39], morbidity and mortality [40], and more [35].
Evidence-Based Learning
Evidence-based medicine (EBM) uses current best scientific evidence to guide patient care decisions for management. Evidence-based learning consists of a four-step process [41]:
-
1.
Formulate a clear clinical question from a patient problem.
-
2.
Search the literature for relevant clinical articles.
-
3.
Critically appraise the evidence for its validity and usefulness.
-
4.
Implement useful findings in clinical practice.
With the advent of the six milestones competency domains, the ACGME requires programs to train residents not only in clinical skills and medical knowledge but also in quality, patient safety, EBM, and cost-effective care [42]. Residency programs must address residents’ barriers to practicing EBM including limited time; lack of experience in EBM; influences from other team members, e.g., faculty role models; and self-perceived inferior positional status and low likelihood to influence change at their institution [43]. To surmount these barriers, ambulatory curricula require EBM teaching to promote residents’ practice-based learning skills and lifelong learning.
Ambulatory Journal Club
Journal clubs are a popular modality to teach physicians how to critically appraise the medical literature and stay current with new evidence. Journal club discussions that are small group, structured, and facilitated by faculty can lead to an increase in resident knowledge of critical appraisal and clinical epidemiology [44,45,46]. Systematic reviews found that overall, journal clubs can enhance residents’ knowledge of epidemiology, biostatistics, reading habits, and references to the medical literature [47]. Further studies are still needed to determine if journal clubs improve clinical behavior. Nonetheless, ambulatory journal club is a vital instructional modality in any ambulatory curriculum to promote academic rigor and EBM practice among residents and faculty [28].
PICO Reports
Critical to practicing EBM is asking the right clinical question. Questions should be as specific as possible, including distinct patient characteristics, the clinical intervention being considered, and the desired outcome [41]. The PICO format helps to design such clinical questions to include the patient or problem, the intervention, the comparison group (usually the standard of care or main alternative), and the outcome [48]. The PICO report provides a template for clinicians to build a specific clinical question and a search strategy to determine the main concepts of the article and answer the question posed. It prompts residents to research a specific clinical question during an actual patient care encounter. This format can be extrapolated to house staff presentations as a way to complement ambulatory journal clubs. Residents can present the relevant article(s) and apply them appropriately in the clinical decision-making process.
Structured Clinical Observations
Mini-Clinical Evaluation Exercises (Mini-CEX)
The mini-CEX , as defined by the ABIM, consists of 10–20 min of direct assessment by a clinical faculty member. This allows for a quick view into a resident’s competence in certain area of practice. The mini-CEX is not intended to be a comprehensive assessment of a full patient encounter but rather serves as a focused assessment of a resident’s competence in a key encounter element (e.g., history gathering, physical examination skills, counseling). The ABIM website encourages the faculty to perform at least one mini-CEX per clinical rotation. After such an interaction, the faculty should then provide timely and specific feedback [51]. The literature reports the far-reach of this method of teaching and objective observation into the international platform and on a variety of contexts in clinical teaching settings.
The mini-CEX format has demonstrated reproducible and reliable results [52]. One main benefit is its ability to provide immediate feedback to the learner. Educators have reported this as valuable, given the lack of time to complete administrative and clinical tasks as well as teach and provide feedback [49, 50]. Mini-CEXs also provide an aspect of realism to the encounter that can be lost in other educational models such as an OSCE [50]. Since residents interact with patients on a daily basis, it is relatively simple to carve time-out within the academic year for this type of instructional modality.
Some pitfalls of the mini-CEX tool include the need for faculty development and rater training [49, 50]. Depending on the type of model implemented and the level of faculty expertise, a significant amount of faculty training maybe required to limit the variation and increase the value of the feedback/rating gathered. This pitfall can be reduced by choosing high-yield areas of evaluation (i.e., breaking bad news, communication skills) since they are already linked to other curricular goals [49]. Time is another concern of the mini-CEX tool. Several studies note that faculty time commitment can range between 19 and 31 min including feedback time [53, 54].
The ABIM website provides a generic template for the development and implementation of a mini-CEX tool into a residency program (Table 2) [51]. The form can be modified to the needs of a residency program, and a modified version of the form is located in the AAIM curriculum toolkit. One can denote on this form the level of satisfaction with the mini-CEX experience, which is useful for faculty development. Programs can also develop their own forms based on the clinical skills involved. Further research should focus on linking specific evaluations to the ACGME milestones.
Patient Simulation Exercises
Most residency programs use patient simulation exercises to teach emergent clinical scenarios such as “rapid response” and/or cardiopulmonary arrest (“Code Blue”) situations as well as to teach specific procedural skills such as central line placement. In the ambulatory setting, some programs use procedural simulation modalities to teach outpatient skills such as arthrocentesis and abdominal paracentesis. Simulations ensure that residents receive high-yield experiences such as mock exercises related to patient safety and improve on their practical skills which may be difficult to do during an 80-h workweek. Simulation can be adapted to a variety of clinical situations, whether it be management of a specific medical issue (e.g., back pain in the clinic) or crisis management (e.g., patient becomes acutely ill or medically unstable in the clinic) [55]. One advantage of the simulation modality is its removal of risk associated with learning a procedure on an actual patient [55]. It allows deliberate practice to occur with immediate feedback available [56]. However, further research in utilizing this type of educational model in ambulatory internal medicine is needed.
Teaching Methods and Instructional Strategies: Resident-Directed Learning
Team-Based Learning
Initially developed by Larry Michaelsen [57, 58], team-based learning (TBL ) is an adult learning pedagogy that uses small group instruction, problem solving, and a knowledge application process for residents to be active participants in their learning. There is a specific sequence of events, starting with an individual pre-class preparation and then individual and group testing based on the pre-class reading called the Readiness Assurance Process, followed by a team-based application exercise and feedback. TBL has been successful in undergraduate medical education [59] with increasing use in graduate medical education, especially in the ambulatory setting. At Northwell Health, the faculty converted all their ambulatory didactics to a modified TBL pedagogy. They found the use of TBL resulted in increased resident engagement, improved facilitated group learning, and preference by residents and faculty for TBL pedagogy over traditional didactic lectures [60]. A recent meta-analysis of seven unique TBL curricula in a variety of GME programs noted higher levels of learner engagement and positive or neutral responses by learners of the TBL pedagogy. However, many faculty reported increased time investment for developing TBL curricula. Despite visible knowledge gains, it is unclear how TBL compares to traditional instructional models in terms of content retention and faculty time investment [61].
Problem-Based Learning
Problem-based learning (PBL ) has been used in interdisciplinary medical education for the last 40 years [62]. It is an active, learner-centered educational strategy focused around a specific problem, whether it is a clinical-, a scientific-, or a community-based problem. Residents use the problem as a starting point to guide their individual learning needs [62]. Unlike TBL, learners are presented with a problem with no pre-work or preparation. They work either individually or in small groups through the scenario and identify unfamiliar terms or concepts. The group determines underlying mechanisms and formulates potential explanations for the problem scenario. The group identifies learning issues associated with the clinical encounter and related to the learning objectives identified by faculty. Following this stage is a period for individual study for accessing a range of educational resources. The group then reconvenes to share what they have learned and apply the learning to the problem scenario. This stage may uncover new learning points that require further individualized study. The final stage is to generalize the learning to the knowledge, skills, or attitudes of other relevant scenarios [62]. PBL has been studied extensively in the undergraduate medical literature, and unfortunately, review of the literature suggests no substantial evidence that PBL improves clinical performance or increases medical knowledge base; however, students and faculty find greater satisfaction in learning and teaching in this format [63].
Flipped Classroom
Similar to TBL and PBL, a flipped classroom is a learner-centered instructional strategy that reverses the traditional educational arrangement by delivering instructional content outside the classroom. This information can be in the form of audio, video, text, or images. It requires the learner to be an active participant in acquiring knowledge and in using it for evaluation of self-performance and peer feedback. It redefines in-class activities to include an application activity, traditionally considered “homework,” to engage learners in the educational content. Residents are able to utilize this knowledge in interactive formats, such as traditional PBL or TBL, or involve simulation activities, role-play, patient encounters, or debates [64]. Teachers take on the role of facilitator by organizing interactive experiences, challenging students to think creatively, and providing expert insight and feedback. This interaction is less didactic and more personalized to the learners [65]. This pedagogy has also been adapted in residency programs of other medical subspecialties [66] and health professional schools with success [65]. The flipped classroom modality leverages technology to meet the needs of learners and allows learners access to the much-needed material for knowledge mastery.
Web-Based Learning
Educational tools that utilize web-based learning (e-learning ) are useful to augment any ambulatory curriculum, especially in the age of millennial learners. E-learning modules help with work hour constraints and present general information regardless of the expertise of the assigned attendings. Web-based module formats are effective at teaching a variety of topics to learners, with improved knowledge [67, 68] and communication skills [69]. Many educational models use e-learning as an adjunct to established ambulatory curricula. The major advantages of web-based learning include the portability of knowledge through a universal web access point and its adaptability to many levels of learners. This instructional modality does not add to the attending workload and can be sustained with limited maintenance [70]. The literature has cited residents’ preference for web-based learning as well. One study showed greater resident satisfaction with web-based learning compared to print materials [71]. Multiple models of e-learning exist in the literature including education in end-of-life and palliative care [70], nephrology at the point of care [72], education about DKA [73], dermatology [74], and cultural competency [75]. Many modules also focus on specific topics available to health systems and universities. These include the Institute for Healthcare Improvement’s Open School [76], Centers to Advance Palliative Care Modules [77], and American Academy of Dermatology Basic Dermatology Curriculum [78]. With available technical support, residency programs can create their own e-learning tools that directly complement established education in the clinic.
Quality Improvement Instruction and Application
Quality improvement (QI) and patient safety (PS) education have become important in ambulatory education as programs develop curricula for their residents to meet specific ACGME milestones in QI skills. Training residents in QI not only helps to meet milestones but also gives residents experiential learning in QI/PS issues encountered in independent practice. It is important to integrate QI projects into the resident continuity clinic experience, not only to develop basic skills in quality improvement and panel management, but resident-driven QI projects can help residents become more invested in their continuity clinics [79, 80]. For more information on developing a QI curriculum, please refer to chapter “Quality Improvement Projects and Indicators” on quality improvement.
Ambulatory Curriculum Design and Venue
Ambulatory medicine education is often delivered to residents by two major curricular designs—longitudinal continuity clinics [88,82,83] and ambulatory block rotations which include the x + y burst model [13, 17, 95,85,87]. Most recently, ambulatory long blocks have emerged as an innovative third design to sustain the continuity of the ambulatory clinical experience [99,89,90]. Clinical experiential training remains the crux of these curricular designs. Embedded within these curricular designs are various instructional venues to allow for dedicated time blocks for formal ambulatory teaching with no patient care assignments. These include academic half-days, pre-clinic or post-clinic conferences, and daily protected didactics, i.e., ambulatory morning reports and noon conferences. These supplementary educational venues consolidate the experiential learning, extend the curriculum beyond clinical cases, and connect clinical practice with evidence-based medicine [13, 14]. Consult chapter “Traditional and Block Scheduling Challenges and Solutions for Internal Medicine Residents” for more information on the various residency schedules.
Developing an Ambulatory Curriculum in One’s Own Academic Clinic
Step-by-Step Guide of Essential Elements in Developing an Ambulatory Curriculum
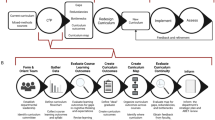
For a successful ambulatory curriculum , the authors recommend that clinic directors assemble a team dedicated to identifying the ambulatory educational needs for the program and the residents, develop goals and objectives for continuity clinics, create and implement a core curriculum, and, finally, establish a forum for feedback, assessment, and faculty development (Fig. 1).
Existing Ambulatory Curricula
Existing ambulatory curricula can be purchased to facilitate the development process of an ambulatory curriculum. The two most popular curricula are the Internal Medicine Ambulatory Care Curriculum offered through Johns Hopkins and the Yale Office-Based Medicine Curriculum. The Internal Medicine Ambulatory Care Curriculum through the Physician Education and Assessment Center (PEAC) at Johns Hopkins consists of 43 modules relevant to outpatient medicine. Topics are in a case-based format with a pretest and posttest to assess resident knowledge. Each module has links to relevant journal articles, abstracts, images, and videos [91]. This curriculum can help complement the core residency ambulatory content and fulfill any clinical knowledge gaps at any institution. Over 180 residency programs have subscribed to this curriculum. Alternatively, the Yale Office-Based Medicine Curriculum exists to help house staff assess and manage common ambulatory problems through an evidence-based syllabus. It covers 3 years of ambulatory training with over 144 clinical cases with case-related questions. There are two formal guides: a house staff guide composed of the case, clinical questions, and key references and a faculty guide composed of teaching points with answers. The Yale Office-Based Medicine Curriculum is used by over 190 internal medicine and family medicine residency programs [31]. Both of these curricula have an annual subscription fee for institutions to purchase for use in their residency program.
Conclusion
Since ambulatory education makes up one-third of residency training, the experiential component of outpatient training must be supplemented by a structured core curricular thread. This curricular thread is guided by the needs of both the learners and institutions, has achievable learning objectives specific to ACGME competencies, and covers basic outpatient skills such as electronic health record management, chronic disease management, and team-based care. Most trainees after residency or fellowship will practice in the outpatient setting and require these core skills for success. Assorted instructional strategies from formal instruction to resident-directed learning modalities can help address the diverse learning styles of learners and unique teaching techniques used by faculty.
References
Accreditation Council for Graduate Medical Education. ACGME Common Program Requirements—Faculty Evaluation. 29 Sept 2013. https://www.acgme.org/Portals/0/PFAssets/ProgramRequirements/CPRs_07012016.pdf. Accessed 14 Aug 2016.
Meyers FJ, Weinberger SE, Fitzgibbons JP, Glassroth J, Duffy FD, Clayton CP, et al. Redesigning residency training in internal medicine: the consensus report of the Alliance for Academic Internal Medicine Education Redesign Task Force. Acad Med. 2007;82(12):1211–9.
Nadkarni M, Reddy S, Bates CK, Fosburgh B, Babbott S, Holmboe E. Ambulatory-based education in internal medicine: current organization and implications for transformation. Results of a national survey of resident continuity clinic directors. J Gen Intern Med. 2011;26(1):16–20.
Thomas PA, Kern DE, Hughes MT, Chen BY. Curriculum development for medical education: a six-step approach. 3rd ed. Baltimore: Johns Hopkins University Press; 2016.
Deutsch SL, Noble J. Community-based teaching: a guide to developing education programs for medical students and residents in the practitioner’s office. American College of Physicians: Philadelphia; 1997.
Aboff B, Chick D, Holmboe E, McKinney S, Schultz H, Yacht A, et al. Developing a curriculum. In: Ficalora R, Costa S, editors. The toolkit series: a textbook for internal medicine education programs. 11th ed. Alliance for Academic Internal Medicine; 2011. p. 265–83.
Thomas PA, Kern DE. Internet resources for curriculum development in medical education: an annotated bibliography. J Gen Intern Med. 2004;19(5 Pt 2):599–605.
Green ML. Identifying, appraising, and implementing medical education curricula: a guide for medical educators. Ann Intern Med. 2001;135(10):889–96.
Doran GT. There’s a S.M.A.R.T. way to write management’s goals and objectives. Manag Rev. 1981;70:35–6.
Meyer PJ. Attitude is everything: if you want to succeed above and beyond. Waco: Meyer Resource Group; 2003.
Accreditation Council for Graduate Medical Education. ACGME milestones. https://www.acgme.org/What-We-Do/Accreditation/Milestones/Overview. Accessed 17 Nov 2016.
Johns Hopkins School of Medicine. Writing better objective. http://www.hopkinscme.edu/Uploads/StaticFiles/WritingBetterObjectives.pdf. Accessed 13 Aug 2016.
Irby DM. Teaching and learning in ambulatory care settings: a thematic review of the literature. Acad Med. 1995;70(10):898–931.
Bowen JL, Irby DM. Assessing quality and costs of education in the ambulatory setting: a review of the literature. Acad Med. 2002;77(7):621–80.
Lesky LG, Borkan SC. Strategies to improve teaching in the ambulatory medicine setting. Arch Intern Med. 1990;150(10):2133–7.
Skeff KM. Enhancing teaching effectiveness and vitality in the ambulatory setting. J Gen Intern Med. 1988;3(2 Suppl):S26–33.
Holmboe ES, Bowen JL, Green M, Gregg J, DiFrancesco L, Reynolds E, et al. Reforming internal medicine residency training. A report from the Society of General Internal Medicine’s task force for residency reform. J Gen Intern Med. 2005;20(12):1165–72.
Lesky LG, Hershman WY. Practical approaches to a major educational challenge. Training students in the ambulatory setting. Arch Intern Med. 1995;155(9):897–904.
Branch WT Jr. Teaching models in an ambulatory training program. J Gen Intern Med. 1990;5(1 Suppl):S15–26.
Jones R, Higgs R, de Angelis C, Prideaux D. Changing face of medical curricula. Lancet. 2001;357(9257):699–703.
Kulasegaram KM, Martimianakis MA, Mylopoulos M, Whitehead CR, Woods NN. Cognition before curriculum: rethinking the integration of basic science and clinical learning. Acad Med. 2013;88(10):1578–85.
Furney SL, Orsini AN, Orsetti KE, Stern DT, Gruppen LD, Irby DM. Teaching the one-minute preceptor. A randomized controlled trial. J Gen Intern Med. 2001;16(9):620–4.
Wolpaw TM, Wolpaw DR, Papp KK. SNAPPS: a learner-centered model for outpatient education. Acad Med. 2003;78(9):893–8.
Aagaard E, Teherani A, Irby DM. Effectiveness of the one-minute preceptor model for diagnosing the patient and the learner: proof of concept. Acad Med. 2004;79(1):42–9.
Irby DM, Aagaard E, Teherani A. Teaching points identified by preceptors observing one-minute preceptor and traditional preceptor encounters. Acad Med. 2004;79(1):50–5.
Weinberger SE, Smith LG, Collier VU. Education Committee of the American College of Physicians. Redesigning training for internal medicine. Ann Intern Med. 2006;144(12):927–32.
Bharel M, Jain S, Hollander H. Comprehensive ambulatory medicine training for categorical internal medicine residents. J Gen Intern Med. 2003;18(4):288–93.
DaRosa DA, Dunnington GL, Stearns J, Ferenchick G, Bowen JL, Simpson DE. Ambulatory teaching “lite”: less clinic time, more educationally fulfilling. Acad Med. 1997;72(5):358–61.
Stevens DP, Bowen JL, Johnson JK, Woods DM, Provost LP, Holman HR, et al. A multi-institutional quality improvement initiative to transform education for chronic illness care in resident continuity practices. J Gen Intern Med. 2010;25(Suppl 4):S574–80.
Mladenovic J, Shea JA, Duffy FD, Lynn LA, Holmboe ES, Lipner RS. Variation in internal medicine residency clinic practices: assessing practice environments and quality of care. J Gen Intern Med. 2008;23(7):914–20.
Yale University. Yale office-based medicine curriculum. 2016. https://medicine.yale.edu/intmed/obm/about/. Accessed 1 Sept 2016.
Kernan WN, Quagliarello V, Green ML. Student faculty rounds: a peer-mediated learning activity for internal medicine clerkships. Med Teach. 2005;27(2):140–4.
Leung J, Bhutani M, Leigh R, Pelletier D, Good C, Sin DD. Empowering family physicians to impart proper inhaler teaching to patients with chronic obstructive pulmonary disease and asthma. Can Respir J. 2015;22(5):266.
Chou C, Lee K. Improving residents’ interviewing skills by group videotape review. Acad Med. 2002;77(7):744.
McNeill M, Ali SK, Banks DE, Mansi IA. Morning report: can an established medical education tradition be validated? J Grad Med Educ. 2013;5:374.
Demopoulos B, Pelzman F, Wenderoth S. Ambulatory morning report: an underutilized educational modality. Teach Learn Med. 2001;13(1):49–52.
Spickard A 3rd, Hales JB, Ellis S. Outpatient morning report: a new educational venue. Acad Med. 2000;75(2):197.
Malone ML, Jackson TC. Educational characteristics of ambulatory morning report. J Gen Intern Med. 1993;8(9):512.
Luciano GL, Visintainer PF, Kleppel R, Rothberg MB. Ambulatory morning report: a case-based method of teaching EBM through experiential learning. South Med J. 2016;109(2):108.
Wong C, Evans G. The ambulatory morbidity and mortality conference meets the morning report. Med Educ. 2012;46:501.
Rosenberg W, Donald A. Evidence based medicine: an approach to clinical problem-solving. BMJ. 1995;310(6987):1122–6.
Fazio SB, Steinmann AF. A new era for residency training in internal medicine. JAMA Intern Med. 2016;176(2):161–2.
van Dijk N, Hooft L, Wieringa-de Waard M. What are the barriers to residents’ practicing evidence-based medicine? A systematic review. Acad Med. 2010;85(7):1163–70.
Green ML. Graduate medical education training in clinical epidemiology, critical appraisal, and evidence-based medicine: a critical review of curricula. Acad Med. 1999;74(6):686–94.
Linzer M, Brown JT, Frazier LM, DeLong ER, Siegel WC. Impact of a medical journal club on house-staff reading habits, knowledge, and critical appraisal skills. A randomized control trial. JAMA. 1988;260(17):2537–41.
Green ML, Ellis PJ. Impact of an evidence-based medicine curriculum based on adult learning theory. J Gen Intern Med. 1997;12(12):742–50.
Ebbert JO, Montori VM, Schultz HJ. The journal club in postgraduate medical education: a systematic review. Med Teach. 2001;23(5):455–61.
Richardson WS, Wilson MC, Nishikawa J, Hayward RS. The well-built clinical question: a key to evidence-based decisions. ACP J Club. 1995;123(3):A12–3.
Liao K, Pu S, Liu M, Yang C, Kuo H. Development and implementation of a mini-Clinical Evaluation Exercise (mini-CEX) program to assess the clinical competencies of internal medicine residents: from faculty development to curriculum evaluation. BMC Med Educ. 2013;13:31.
Alves de Lima A, Conde D, Aldunate L, van der Vleuten C. Teachers’ experiences of the role and function of the mini clinical evaluation exercise in post-graduate training. Int J Med Educ. 2010;1:68.
American Board of Internal Medicine. Mini-CEX clinical evaluation for trainees: direct observation assessment tool. 2016. http://www.abim.org/program-directors-administrators/assessment-tools/mini-cex.aspx. Accessed Aug 2016.
Pelgrim EA, Kramer AW, Mokkink HG, van den Elsen L, Grol RP, van der Vleuten CP. In-training assessment using direct observation of single-patient encounters: a literature review. Adv Health Sci Educ Theory Pract. 2011;16(1):131.
Kogan JR, Bellini LM, Shea JA. Feasibility, reliability, and validity of the mini-clinical evaluation exercise (mCEX) in a medicine core clerkship. Acad Med. 2003;78(10 Suppl):S33.
Hauer KE. Enhancing feedback to students using the mini-CEX (Clinical Evaluation Exercise). Acad Med. 2000;75(5):524.
McLaughlin S, Fitch MT, Goyal DG, Hayden E, Kauh CY, Laack TA, et al. Simulation in graduate medical education 2008: a review for emergency medicine. Acad Emerg Med. 2008;15:1117.
Gaba DM. The future vision of simulation in healthcare. Qual Saf Health Care. 2004;13(Suppl 1):i2.
Parmelee D, Michaelsen LK, Cook S, Hudes PD. Team-based learning: a practical guide: AMEE guide no. 65. Med Teach. 2012;34(5):e275–87.
Parmelee DX, Michaelsen LK. Twelve tips for doing effective Team-Based Learning (TBL). Med Teach. 2010;32(2):118–22.
Searle NS, Haidet P, Kelly PA, Schneider VF, Seidel CL, Richards BF. Team learning in medical education: initial experiences at ten institutions. Acad Med. 2003;78(10 Suppl):S55–8.
Balwan S, Fornari A, DiMarzio P, Verbsky J, Pekmezaris R, Stein J, et al. Use of team-based learning pedagogy for internal medicine ambulatory resident teaching. J Grad Med Educ. 2015;7(4):643–8.
Poeppelman RS, Liebert CA, Vegas DB, Germann CA, Volerman A. A narrative review and novel framework for application of team-based learning in graduate medical education. J Grad Med Educ. 2016;8(4):510–7.
Davis MH. AMEE Medical Education Guide No. 15: problem-based learning: a practical guide. Med Teach. 1999;21(2):130–40.
Dolmans D, Michaelsen L, van Merrienboer J, van der Vleuten C. Should we choose between problem-based learning and team-based learning? No, combine the best of both worlds! Med Teach. 2015;37(4):354–9.
Prober CG, Khan S. Medical education reimagined: a call to action. Acad Med. 2013;88(10):1407–10.
McLaughlin JE, Roth MT, Glatt DM, Gharkholonarehe N, Davidson CA, Griffin LM, et al. The flipped classroom: a course redesign to foster learning and engagement in a health professions school. Acad Med. 2014;89(2):236–43.
Young TP, Bailey CJ, Guptill M, Thorp AW, Thomas TL. The flipped classroom: a modality for mixed asynchronous and synchronous learning in a residency program. West J Emerg Med. 2014;15(7):938–44.
Truncali A, Lee JD, Ark TK, Gillespie C, Triola M, Hanley K, et al. Teaching physicians to address unhealthy alcohol use: a randomized controlled trial assessing the effect of a Web-based module on medical student performance. J Subst Abus Treat. 2011;40(2):203.
Desai T, Stankeyeva D, Chapman A, Bailey J. Nephrology fellows show consistent use of, and improved knowledge from, a nephrologist-programmed teaching instrument. J Nephrol. 2011;24(3):345.
Lee CA, Chang A, Chou CL, Boscardin C, Hauer KE. Standardized patient-narrated web-based learning modules improve students’ communication skills on a high-stakes clinical skills examination. J Gen Intern Med. 2011;26(11):1374.
Ross DD, Shpritz DW, Wolfsthal SD, Zimrin AB, Keay TJ, Fang H, et al. Creative solution for implementation of experiential, competency-based palliative care training for internal medicine residents. J Cancer Educ. 2011;26:436.
Bell DS, Fonarow GC, Hays RD, Mangione CM. Self-Study from web-based and printed guideline materials. A randomized controlled trial among resident physicians. Ann Intern Med. 2000;132(12):938.
William JH, Huang GC. How we make nephrology easier to learn: computer-based modules at the point-of-care. Med Teach. 2014;36:13.
Yu CH, Straus S, Brydges R. The ABCs of DKA: development and validation of a computer-based simulator and scoring system. J Gen Intern Med. 2015;30(9):1319.
McCleskey PE. Clinic teaching made easy: a prospective study of the American Academy of Dermatology core curriculum in primary care learners. J Am Acad Dermatol. 2013;69(2):273.
Staton LJ, Estrada C, Panda M, Ortiz D, Roddy D. A multimethod approach for cross-cultural training in an internal medicine residency program. Med Educ Online. 2013;18:20352.
Institute for Healthcare Improvement. IHI Open School courses. 2016. http://www.ihi.org/education/ihiopenschool/courses/Pages/default.aspx. Accessed 1 Sept 2016.
Centers to Advance Palliative Care. CAPC CME courses. https://www.capc.org/. Accessed 1 Sept 2016.
American Academy of Dermatology. Basic dermatology curriculum. 2016. https://www.aad.org/education/basic-derm-curriculum. Accessed 1 Sept 2016.
Zafar MA, Diers T, Schauer DP. Connecting resident education to patient outcomes: the evolution of a quality improvement curriculum in an internal medicine residency. Acad Med. 2014;89(10):1341.
Potts S, Shields S, Upshur C. Preparing future leaders: an integrated quality improvement residency curriculum. Fam Med. 2016;48(6):477.
Thomas KG, West CP, Popkave C, Bellini LM, Weinberger SE, Kolars JC, et al. Alternative approaches to ambulatory training: internal medicine residents’ and program directors’ perspectives. J Gen Intern Med. 2009;24(8):904–10.
Julian K, Riegels NS, Baron RB. Perspective: creating the next generation of general internists: a call for medical education reform. Acad Med. 2011;86(11):1443–7.
Zebrack JR, Fletcher KE, Beasley BW, Whittle J. Ambulatory training since duty hour regulations: a survey of program directors. Am J Med. 2010;123(1):89–94.
Bard FJ, Shu Z, Morrice JD, Leykum KL. Annual block scheduling for internal medicine residents with 4+1 templates. J Oper Res Soc. 2016;67(7):911–27.
Chaudhry SI, Balwan S, Friedman KA, Sunday S, Chaudhry B, DiMisa D, et al. Moving forward in GME reform: a 4 + 1 model of resident ambulatory training. J Gen Intern Med. 2013;28(8):1100–4.
Shalaby M, Yaich S, Donnelly J, Chippendale R, DeOliveira MC, Noronha C. X + Y scheduling models for internal medicine residency programs-a look back and a look forward. J Grad Med Educ. 2014;6(4):639–42.
Huddle TS, Heudebert GR. Internal medicine training in the 21st century. Acad Med. 2008;83(10):910–5.
Warm EJ, Schauer DP, Diers T, Mathis BR, Neirouz Y, Boex JR, et al. The ambulatory long-block: an accreditation council for graduate medical education (ACGME) educational innovations project (EIP). J Gen Intern Med. 2008;23(7):921–6.
Warm EJ. Interval examination: the ambulatory long block. J Gen Intern Med. 2010;25(7):750–2.
Reynolds EE. Fostering educational innovation through measuring outcomes. J Gen Intern Med. 2011;26(11):1241–2.
Johns Hopkins University Physician Education and Assessment Center. Internal medicine curriculum. 2016. https://ilc.peaconline.org/. Accessed Oct 2016.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Appendices
Appendix 1: A General Needs Assessment of Ambulatory Medicine Curriculum
Problem identification—What is the current approach? Barriers to implementation? | Ideal approach? | Goals and objectives | Resources needed for implementation? |
|---|---|---|---|
. | . | . | . |
Appendix 2: Targeted Needs Assessment of Learners
Key learners | Impact of curriculum | Relevant info needed from learners | Methods for learner needs assessment | Resources needed for implementation |
|---|---|---|---|---|
. | . | . | . | . |
Appendix 3: Example Goals and Objectives
Internal Medicine Residency Training Program
Resident Continuity Clinics
Resident Clinic Director: ____________
Rotation description: The continuity clinic rotation teaches residents to care for a longitudinal panel of primary care patients over their 3-year residency. In their primary care continuity clinics, residents will manage patients with a mix of acute care issues and chronic medical conditions, including but not limited to diabetes, hypertension, coronary artery disease, and COPD. Residents will also perform office-based procedures under the supervision of a clinic attending.
Principal Educational Goals by Relevant Competency
The principal educational goals for residents on this rotation are indicated for each of the six ACGME competencies in the tables below. The first column of the table lists the goals; the second column maps the goals to the reporting milestones competencies; the third column lists the most relevant learning activities for that goal; and the fourth column indicates the correlating evaluation methods for that goal.
PGY-1/2/3 (Goals Are for All Levels Unless Indicated)
Principal educational goals | Milestones competency | Learning activities | Evaluation methods |
|---|---|---|---|
A. Patient care | |||
Ability to take a complete medical history and perform a careful and accurate physical examination | PC1 | DPC | FE, MC, CEX, SPE |
Ability to write or dictate concise, accurate, and informative histories, physical examinations, and progress notes | PC1, ICS2, ICS3 | DPC | FE |
Define and prioritize patients’ medical problems and generate appropriate differential diagnoses | PC1, PC2, PC3, MK1 | DPC, FR | FE |
Develop rational, evidence-based management strategies | PC2, PC3, MK1, SPB2, SPB3, PROF3, PBL4 | DPC, FR, MR, EBM | FE |
PGY-1—Ability to make basic interpretation of chest and abdominal x-rays and electrocardiograms PGY-2/3—Develop and demonstrate proficiency in above | MK2 | DPC, FR, MR DPC, FR, MR | FE, IE FE, IE |
PGY-1—Ability to perform pelvic examination under supervision PGY-2/3—Ability to perform pelvic examination | PC4, MK2 PC4, MK2 | DPC, ACS, AM DPC, ACS, AM | FE FE |
Ability to recognize the physical findings of important medical illnesses | PC1, PC2, PC3 | DPC, MR, MM | FE, MC, CEX |
Willingness and ability to help patients engage in strategies of disease prevention | PC2, MK1, MK2, SBP3, PROF1, PROF3, ICS1 | DPC | FE, SPE, MC |
B. Medical knowledge | |||
Expand clinically applicable knowledge base of the basic and clinical sciences underlying the care of medical patients in the outpatient setting | PC1, PC2, MK1 | AM, DPC, PIP, JC, NC, MR | FE, IE, PIP |
Access and critically evaluate current medical information and scientific evidence relevant to patient care in outpatient setting | SPB2, PBLI4 | DPC, JC, NC, EBM, MR | FE, IE |
PGY-1—Understand basic pathophysiology, clinical manifestations, diagnosis, and management of medical illnesses seen by a general internist in the ambulatory setting PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, PC2,MK1 PC1, PC2, PC3, MK1 | DPC, NC DPC, NC | FE, IE FE, IE |
PGY-1—Recognize the indications for and basic interpretation of chest and abdominal x-rays, electrocardiograms, and pulmonary function tests PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, MK2, SBP3 PC1, MK2, SBP3 | DPC, MR, ACS DPC, ACS, MR | FE, IE FE, IE |
PGY-1—Learn indications for and basic interpretation of standard laboratory tests, including blood counts, coagulation studies, blood chemistry tests, urinalysis, body fluid analyses, and microbiologic tests PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, MK2, SBP3 PC1, MK2, SBP3 | DPC, MR DPC, MR | FE, IE FE, IE |
PGY-1—Familiarity with basic principles of disease prevention, including adult immunizations, cardiovascular risk assessment, prevention of cardiovascular disease, screening for cancer, prevention of osteoporosis, and cessation of tobacco PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC2, MK1, MK2, SBP3, PROF3, ICS1 PC2, MK1, MK2, SBP3, ICS1 | DPC, ACS, PIP, AM DPC, ACS, PIP | FE, PIP FE, PIP |
Appreciation of the evolution of chronic conditions over time | PC1, PC2, PC3, | DPC, NC, AM, ACS | FE |
PGY-1 —Basic familiarity with pathophysiology, clinical manifestations, and nonoperative management of common musculoskeletal conditions, including occupational and sports-related injuries PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, PC2, PC3, MK1 PC1, PC2, PC3, MK1 | DPC, ACS, CC, NC, AM DPC, ACS, NC, AM | FE, IE FE, IE |
PGY-1—Basic familiarity with pathophysiology, clinical manifestations, and medical management of common gynecological conditions, including acute salpingitis, vaginitis, dysmenorrhea, irregular menses, and menopausal symptoms PGY-2/3-Develop and demonstrate in-depth knowledge of above | PC1, PC2, PC3, MK1 PC1, PC2, PC3, MK1 | DPC, ACS, AM, NC DPC, ACS, AM, NC | FE, IE FE, IE |
PGY-1 —Basic familiarity with pathophysiology, clinical manifestations, and medical management of common otolaryngological conditions, including acute and chronic sinusitis and allergic rhinitis PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, PC2, PC3, MK1 PC1, PC2, PC3, MK1 | DPC, ACS, NC, AM DPC, ACS,AM, | FE, IE FE, IE |
PGY-1—Basic familiarity with pathophysiology, clinical manifestations, and management of common ophthalmologic conditions, including minor ocular injuries and conjunctivitis PGY-2/3—Develop and demonstrate in-depth knowledge of above | PC1, PC2, PC3, MK1 PC1, PC2, PC3, MK1 | DPC, ACS, NC, AM DPC, ACS, NC, AM | FE, IE FE, IE |
Familiarity with special features of diagnosis, interpretation of tests, and management of illnesses in a geriatric population | PC1, PC2, PC3, MK1, MK2, PROF3 | DPC, SL, AM, NC | FE, IE |
C. Interpersonal skills and communication | |||
Communicate effectively with patients and families | PROF1, PROF3, ICS1 | DPC | FE, SPE, PE |
Communicate effectively with physician colleagues at all levels | PC5, SBP1, SBP4, PBLI3, ICS2 | DPC, PC | FE, PR |
Present information on patients concisely and clearly, both verbally and in writing | PROF1, PROF3, ICS1, ICS3 | DPC, MR | FE, PR, NE, MRF, ABF |
D. Professionalism | |||
Interact professionally toward patients, families, colleagues, and all members of the healthcare team | SBP1, PBLI3, PROF1, ICS1, ICS2 | DPC | FE, PR, NE, PE, SPE |
Acceptance of professional responsibility as the primary care physician for patients under his/her care | PC3, PBLI1, PROF2, PROF4 | DPC | FE |
Appreciation of the social context of illness | PC2, MK1, PROF3, ICS1 | DPC | FE, SPE |
Understand ethical concepts of confidentiality, consent, autonomy, and justice in the outpatient setting | PROF1, PROF4 | DPC, EC | FE, PE |
Understand professionalism concepts of integrity, altruism, and conflict of interest in the outpatient setting | PROF1, PROF4 | DPC, EC | FE |
E. Practice-based learning and improvement | |||
Identify and acknowledge gaps in personal knowledge and skills in the care of ambulatory patients | PC2, PC3, PBLI1, PBLI3 | DPC, PIP | FE, PIP |
Develop and implement strategies for filling gaps in knowledge and skills | SPB2, PBLI1, PBLI2, PBLI4 | DPC | FE, IE, HEC |
Commitment to professional scholarship, including systematic and critical perusal of relevant print and electronic literature, with emphasis on integration of basic science with clinical medicine, and evaluation of information in light of the principles of evidence-based medicine related to the outpatient world | PBLI2, PBLI4, PROF4 | DPC, EBM, JC | FE, JCF, ABF |
F. System-based practice | |||
Understand and utilize the multidisciplinary resources necessary to care optimally for clinic patients | PC3, PC5, SBP1, SBP4 | DPC | FE |
Collaborate with other members of the healthcare team to assure comprehensive patient care | SBP1, SBP4, PBLI3, PROF1 | DPC | FE |
Use evidence-based, cost-conscious strategies in the care of outpatients | MK2, SBP3 | DPC, SS | FE |
Effective collaboration with other members of the healthcare team, including nurses, clinical pharmacists, occupational therapists, physical therapists, nutrition specialists, patient educators, speech pathologists, respiratory therapists, enterostomy nurses, social workers, and providers of home health services | SBP1, SBP4, PROF1 | DPC | FE |
Knowing when and how to request medical consultation and how to utilize the advice provided | PC5, SBP1, PROF1 | DPC | FE |
Consideration of the cost-effectiveness of outpatient diagnostic and treatment strategies | MK2, SBP3 | DPC | FE |
Knowing when to refer patients to specialists in orthopedics, gynecology, otolaryngology, and ophthalmology | PC5 | DPC, ACS, AM | FE |
Knowing when to consult or refer a patient to a medical subspecialist | PC5 | DPC, ACS | FE |
PGY-2/3—Willingness and ability to teach medical students and PGY-1 residents | PROF2, ICS2 | DPC, RAE | FE, PR |
Appendix 4: Checklist for Curriculum Implementation
-
Identify resources
-
Personnel required: faculty, staff, others
-
Time: faculty, learners, support staff
-
Facilities: space, equipment, sites
-
Funding/costs: direct and indirect costs
-
-
Obtain support
-
Internal: program director, department chair, learners, faculty
-
External: professional societies, if applicable (e.g., SGIM, AAIM)
-
-
Develop administrative mechanisms to support the curriculum
-
Administrative structure of team
-
◦ Necessary for delineating responsibilities and decision-making
-
-
Communication
-
◦ Content to learners and faculty: includes goals and objectives, information about curriculum, facilities, scheduling, changes, evaluation results
-
◦ Mechanisms: email, meetings, website, etc.
-
-
Operations
-
◦ Preparation and distribution of schedules and curricular materials
-
◦ Method of collecting, collating, and distributing evaluation data
-
◦ Process for revisions
-
-
-
Anticipate and address barriers
-
Financial
-
Competing demands
-
People: attitudes of learners and faculty, faculty without enough time, authority, etc.
-
-
Introduce curriculum in stepwise fashion
-
Pilot project
-
Phase-in
-
Full implementation
-
Adapted from: Kern DE, et al.: Curriculum Development for Medical Education – A Six-Step Approach, 2nd edition. Baltimore: The Johns Hopkins Univ. Press. 2009
Appendix 5: Sample Mini-CEX for Gynecological Examination
Resident: ____________________________
Date: _______________________________
Supervisor: __________________________
Please rate the resident on the following criteria:
Poor/not done | Minimal/adequate | Excellent | |
|---|---|---|---|
1. Proper patient positioning | 1 | 2 | 3 |
2. Communication with patient during exam | 1 | 2 | 3 |
3. Inspection of the external genitalia | 1 | 2 | 3 |
4. Use of speculum (insertion and removal) | 1 | 2 | 3 |
5. Inspection of vaginal walls and cervix | 1 | 2 | 3 |
6. Obtained sample for Pap smear and/or wet mount/culture | 1 | 2 | 3 |
7. Bimanual examination | 1 | 2 | 3 |
8. Examination for inguinal adenopathy | 1 | 2 | 3 |
9. Overall rating | 1 | 2 | 3 |
Do you feel this resident is competent in performance of the pelvic exam? Yes No
Please provide any additional comments below:
Appendix 6: Sample 18-Month Curriculum for x + y Clinic Design, Repeated Twice over Residency
Block | Theme |
|---|---|
1 | Introduction to office-based practice I |
2 | Screening, prevention, population health |
3 | Pain management/musculoskeletal |
4 | Cardiology |
5 | Psychiatric disease |
6 | Pulmonary |
7 | Infectious disease/HIV |
8 | Endocrine |
9 | Gastroenterology |
10 | Renal |
11 | Geriatrics |
12 | Women’s health |
13 | Neurology/dermatology |
14 | ENT/ophthalmology/hematology |
15 | Palliative |
16 | High-value cost-conscious care |
17 | Urban curriculum |
18 | Career development and wellness |
Sample 36-month curriculum for traditional, weekly half-day clinic design
Month | Topics | ||
|---|---|---|---|
Year 1 | Year 2 | Year 3 | |
July | Billing and coding | Billing and coding | Billing and coding |
August | Preventative services: vaccine/cancer screen | Preventative services: vaccine/cancer screen | Preventative services: vaccine/cancer screen |
September | Type 2 diabetes mellitus | Preoperative evaluation | Sexually transmitted diseases |
October | Hypertension | Coronary artery disease | Geriatric wellness |
November | Hyperlipidemia | Obesity | Congestive heart failure |
December | Panel management | Panel management | Panel management |
January | Depression/anxiety | Hypogonadism and erectile dysfunction | Chronic pelvic pain and dysmenorrhea |
February | Chronic pain syndrome | Gout vs. osteoarthritis | Women’s health |
March | URI vs. sinusitis | Fibromyalgia | Hepatitis C |
April | Asthma and COPD | CVA/TIA | Atrial fibrillation |
May | Thyroid disease: hypo-/hyperthyroidism | GERD | Community-acquired pneumonia vs. influenza |
June | Transitions of care | Migraines vs. tension headaches | Osteoporosis and vitamin D deficiency |
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Lo, M.C., Chisty, A., Mullen, E. (2018). Ambulatory Curriculum Design and Delivery for Internal Medicine Residents. In: Lu, L., Barrette, EP., Noronha, C., Sobel, H., Tobin, D. (eds) Leading an Academic Medical Practice. Springer, Cham. https://doi.org/10.1007/978-3-319-68267-9_15
Download citation
DOI: https://doi.org/10.1007/978-3-319-68267-9_15
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-68266-2
Online ISBN: 978-3-319-68267-9
eBook Packages: MedicineMedicine (R0)