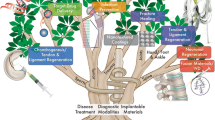
Abstract
Nanotechnology is the application and manipulation of structures, typically particles or molecules within the ‘nano’ range (one billionth of a metre (nm)). Nanoparticles measure 100 nm or less and have a greater surface area to weight ratio, meaning they can alter the properties of many conventional materials. Nanoparticles can be used in conjugation with traditional materials or to create novel structures with unique electrical, chemical and mechanical properties. These natural and artificial nanostructures offer new approaches to the management of disease; from diagnostics to treatment and preventative applications. These include advances in targeted drug delivery, repair mechanisms and healing, antimicrobial coats on implant surfaces, osteointegration of implants and the use of nanoscaffolds for tissue integration and regeneration. This chapter examines current concepts in nanomedicine and the potential applications of nanotechnology in the field of orthopaedics with a particular focus on surgery of the knee.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
3.1 Introduction
Nanotechnology is the application and manipulation of structures, typically particles or molecules within the ‘nano’ range. Subatomic particles (protons, electrons and neutrons) are the smallest building blocks of atoms, which bond together to form molecules. Elements are many molecules of the same atom, whilst compounds are many molecules of a mixture of atoms. Technically, a single atom is the smallest unit of matter, but matter is regarded as being molecular. The prefix nano in the metric system represents a distance of one billionth of a metre (nm) and is represented numerically as one times ten to the power minus nine (10−9 or 0.000000001 m). Nanoparticles have one dimension that measures 100 nm or less and contain 4–400 atoms [1]. The properties of many conventional materials change when formed from or are exposed to nanoparticles as they have a greater surface area to weight ratio making them potentially more reactive to other materials [2]. Nanostructures are 1–100 nm and comprised of molecular nanomaterials which may be natural or artificial. Natural nanostructures include light amplifying pigment particles such as those that occur in the corneas of moths [3], adhesive compounds forming pads on the feet of geckos which aid climbing [4] and nanotubules in some plants which have diverse functions, from a defence against UV radiation in mountain flowers to a self-cleaning mechanism in the lotus flower [5]. The most common artificial nanostructures in current nanotechnologies include graphene nanotubes of single, double or multiple layers which can be oriented into one complete tube inside another (Russian doll configuration) [6] or constructed into a continuous graphene sheet rolled upon itself (parchment configuration) [7]. The various configurations offer a variety of electrical, chemical and mechanical properties.
3.2 Current Concepts in Nanomedicine
Potential nanotechnology applications are currently being explored in medicine generally; however, this chapter is particularly concerned with applications in orthopaedics [1, 8, 9]. Some examples which give an idea of the scope of applications in medicine include nanoconstituent and nanoarchitecture modifications to implant coatings [10,11,12,13,14,15], diagnostics [16] and patient monitoring [17]. Advances in pharmacokinetics include improving drug targeting [18], efficacy optimisation, potency and side effect reduction [19]. Examples of how these techniques work include polymeric micelle nanoparticles with surface receptors that can specifically identify particular tumours and deliver drugs directly to tumour cells avoiding generalised cell destruction [20]. Another example of a targeting modality involves the attachment of a chemotherapy drug to a nanodiamond which has been used to treat brain tumours [21] and leukaemia [22]. Nanoparticles may be combined with specific antibodies known as ‘quantum dots’ (Invitrogen) to target neoplastic or infected cells [23]. Docetaxel (Cristal Therapeutics) for the treatment of solid tumours is a good example of the possibilities of nanotechnology and has recently commenced phase I clinical trials in 2015 [24].
In the field of infection control and prevention, nanotechnology has been used to improve the antimicrobial properties of healthcare clothing and equipment. Integrating nanosilicon particles into materials such as scrubs or surgical gowns has been shown to greatly enhance their antimicrobial capacity [25, 26]. Furthermore, polymer-coated iron oxide nanoparticles disrupt clusters of bacteria, with the potential to facilitate more effective treatment of chronic bacterial infections [27]. Protein-filled nanoparticles have been used in the form of an inhalational vaccine to promote an enhanced immune response [28].
Regenerative and preventative medicine has also been influenced by nanotechnology. Cerium oxide nanoparticles act as an antioxidant to remove oxygen-free radicals following trauma [29], and protein-linked nanodiamonds increase bone growth around dental or joint implants [30]. Nickel nanoparticles combined with a polymer form a self-healing, synthetic skin, which could potentially be used in the development of prosthetics [31]. Of particular interest is the phenomenon the material exhibits when cut, where it spontaneously heals itself within 30 min if held together. It also exhibits electrical resistance properties which change with pressure, giving it the ability to function as a form of synthetic touch. The development of advanced imaging systems may allow disease to be detected and potentially treated even in its early stages [32]. Combining nanoparticles with dyes or marker substances to allow the intraoperative visualisation of diseased tissue may greatly improve resection accuracy [33]. Implantable nanowires give real-time monitoring of physiological parameters which may aid chronic disease management and access to emergency treatment [34].
Nanoarrays have superseded microarray analysis, which was once regarded as the future of biomolecular analysis [35]. Limitations of microarrays include large sample volumes, longer incubation times, limited detection, bulky instrumentation, laborious sample amplification and labelling ultimately resulting in high running costs and delays. Nanotechnology may improve the speed and quality of diagnostic tests by moving complex tests from specialised centres to the bedside or office. Current operational protocols exist for nanoarray technology in label-free analysis of nucleic acids, protein detection (using conventional optical fluorescence microscopy or novel label-free atomic force microscopy) [35]. Furthermore, multiple tests can be combined onto a single ‘lab-on-a-chip’ and processed rapidly using handheld devices [36].
The examples above are not exhaustive but demonstrate the wide and variable uses of nanotechnology and the great potential for further development and use.
3.3 Current Concepts in Nano-Orthopaedic Research
Nanotechnology may provide the means of manipulating the organic and inorganic nanostructures of the bone and its surrounding soft tissues, representing a new avenue for the treatment of musculoskeletal disorders. Ongoing research into the application of nanotechnology within the field of orthopaedics is diverse; however, much of this remains at the laboratory stage with few clinical studies testing technologies in vivo [1, 8]. The current literature suggests three main and overlapping areas of exploration in orthopaedic nanotechnology: nanoscaffolds, implant and tissue integration and drug delivery.
3.3.1 Nanoscaffolds
Nanoscaffolds may be used for local drug or gene therapy delivery or act to regulate cellular processes and can be used as a growth material for tissue engineering purposes. Nanoscaffolds are typically comprised of electrospun nanofibre matrices [37]. These scaffolds are designed to be biomimetic particularly representing extracellular matrix structure and function [38]. This technology has the potential to be incorporated into implants to improve their integration with the bone [39, 40] and to combat biofilm-related infections of implants [14] and can be applied in tissue engineering to create artificial versions of natural substances [41].
3.3.2 Implant Integration
Biological integration of implants into the human body is highly sought after in orthopaedics. Aseptic loosening remains a major cause of revision in arthroplasty surgery [42,43,44,45]. Modification of existing materials such as titanium, tantalum, ceramics and hydroxyapatite at the nano level may facilitate biological activity [46, 47]. Evidence from previous research has indicated that if this can be safely harnessed it may decrease the incidence of revision in major joint arthroplasty [9, 14, 48, 49]. Infection is also a leading cause of implant failure and lack of integration. Nanoscale surface modification of orthopaedic implants has been found to be effective in reducing bacterial adherence, biofilm creation and disrupting bacterial cell homeostasis [14]. The fight against primary and secondary bone malignancy, which frequently requires the use of implants, may also be improved with the aid of nanotechnology. Tran et al. conducted an experimental in vitro study which examined the effects of three novel, hybrid implant surfaces of selenium and titanium on cancerous bone tissue. They found that the selenium adherent surfaces chemotherapeutic and osteointegrative when compared to untreated titanium implants [50].
3.4 Drug Delivery
3.4.1 Chemotherapeutics
The avoidance of healthy cells via the targeted delivery of therapeutic substances to diseased tissue is another possible role of nanotechnology which could revolutionise the management of some diseases. There is a potential to improve pharmacokinetics, efficacy, lower doses and lower drug-related toxicity [19]. Drugs contained within nanocapsules consisting of a nanoengineered coat with coded surface protein that unlock at the target cell are one method of applying this technology [18] (Fig. 3.1). The potential applications of such nanocoats could greatly improve orthopaedic care including the targeting of neoplastic bone disease and common orthopaedic conditions such as osteoarthritis and osteoporosis [51]. Bisphosphonates are currently the vessel of choice for improving the targeting of bone using nanotechnology due to their high affinity to the organ [51]. Their use with nanoparticles has been shown to limit metastasis, reduce tumour seeding and angiogenesis [51]. Bisphosphonates have been used in the treatment of bone metastasis to deliver chemotherapeutics directly to the organ, maintaining higher levels of the drug at target tissues and slowing its metabolic breakdown [52]. The treatment of primary bone tumours could also be influenced by nanotechnology. The delivery of chemotherapeutic substances to osteosarcoma has been improved with the use of nanoparticles and was able to tackle multidrug-resistant forms of the disease [53]. The combination of nanomedicine with gene therapy may have an even greater effect on treating such tumours [54]. Nanoparticles have been used to improve the efficacy of bisphosphonates in treating osteoporosis and have been shown to improve the retention time of interleukin receptor inhibitors in the treatment of osteoarthritis [51]. By similar means nanotechnology could be applied to improve drug delivery in the treatment of osteoarthritis, osteomyelitis and benign neoplastic conditions. The cells responsible for pigmented villonodular synovitis (PVNS) can be made more sensitive to radiotherapy resulting in a reduction of overall radiation dose and its associated risks [55].
3.4.2 Antimicrobial Applications
The use of nanocrystals of silver versus larger molecules in the surface coatings of arthroplasty implants to control and extend the release of antibiotics has been shown to reduce bacterial adhesion [56]. The use of synergistic nanomolecules such as nanophase gold which enhances the transcutaneous uptake of non-steroidal anti-inflammatories as also shown similar results. Currently, nanotechnology is utilised in wound dressings impregnated with silver nanocrystals which have a lower finite amount of silver but have been shown to have increased potency compared with larger molecules [57].
3.5 Nanotechnology Applications in Knee Surgery
3.5.1 Knee Arthroplasty
Total knee arthroplasty is well established with excellent success rates [58]. The standard expected of any new implant entering the market is a ten-year survival rate in greater than 90% of cases; however, aseptic loosening and infection remain leading causes of failure [58]. Aseptic loosening in total knee arthroplasty is a significant challenge and is more common in uncemented rather than cemented and hybrid implants [58]. It is the indication for over 40% of single stage revision knee replacements in the United Kingdom [58]. Target rates of infection in joint arthroplasty are quoted as <0.5%, but actual rates are under 2% [58]. Despite major advances, infection remains a major cause for implant failure and burden in revision surgery [58].
Better osteointegration is brought about by altering the mechanical nature of the implant, i.e. creating a more porous architecture for bone ingrowth or by altering chemical characteristics leading to selective bonding to bone and inhibition of fibrous healing [59]. Nanoengineered coatings may provide chemical, mechanical and ultimately biological enhancement to implant integration, improving long-term performance [60]. The nature of an implant surface dictates implant–host interaction [11, 48, 61,62,63] and nanotechnology has been employed in the effort to improve osteointegration [64,65,66,67] and counter bacterial adhesion and growth [68,69,70,71,72,73,74]. Osteoblast adherence to implants occurs on the nanoscale; therefore, altering the surface roughness of an orthopaedic implant from the macro to the nanoscale could improve osteointegration whilst inhibiting suboptimal fibrous tissue from forming [62, 75, 76] (Fig. 3.2). This has been demonstrated in animal studies with good results. Salou et al. assessed the pull-out resistance and histological characteristics between macro-surface implants created through standard manufacturing techniques and nanosurface implants of titanium nanotubules. Pull-out strength and histological evidence of osteointegration were improved with the nanoscale surfaces [77]. Addition of nanoparticles of hydroxyapatite or titanium may further enhance this process [60, 78].
Implant integration with the bone; immediately after bone (B) preparation blood components (BC) surround the prosthesis (P) within the bone (1); platelet-derived factors (PF) coat the prosthesis and prevent integration with healing tissue (2); suboptimal fibrous tissue develops with poor pull-out strength (3); enhanced implant integration with nanosurface modification (NC) prevents PF from binding and allows for better implant bone interface bonding (4–6)
Surface topography can influence bacterial behaviour, and nanotechnology has been shown to reduce adherence [48, 79] (Fig. 3.3). Lab-based research has demonstrated marked reductions in the adherence of multiple bacterial species [80], and silver nanosurfaces have been found to be bactericidal by interfering in bacterial cell homeostasis [74, 81]. Improving the quality of orthopaedic cement, a substance which has remained relatively unchanged for decades, as well as the cement bone interface may also be achieved with nanotechnology leading to lower risk of failure and cement fracture. Khandaker et al. added nanoform magnesium oxide to bone cement and found marked improvement in fracture toughness of the cement which could have implications for implant longevity [82]. Ricker et al. investigated the effects of added barium sulphate and magnesium oxide nanoparticles on methyl methacrylate bone cement. They noted reductions in the harm caused during the curing process and an increase in osteointegration with the nanoparticles [83]. Valuable evidence for improved osteointegration using nanotechnology has come from the field of dentistry. Modifications to the surface of implants with bioactive ceramics to improve interaction at the bone implant interface and coating material such as various phosphates, hydroxyapatite and bioactive glasses have been shown to hold promise [59].
3.5.2 Repair and Restoration of Cartilage
One of the more complex aspects of knee surgery is the management of cartilage defects. Restoring, replacing and rejuvenating articular cartilage are all aspirations of the knee surgeon but are currently impossible. Techniques including microfracture, drilling and transplants give rise to suboptimal fibrous scar tissue which does not provide the same biomechanical properties as true cartilage [84]. Innovative techniques such as patch graft repairs with autologous stem cells are laborious, expensive and inconsistent in their results. Nanoscaffolds may provide opportunities to improve this aspect of knee surgery. Creating a three-dimensional structure formed of biodegradable polymers that function as a scaffold for stem cell adherence programmed differentiation according to tissue requirements and eventual integration into the surrounding native tissue [85]. This could be achieved through programmed obsolescence (e.g. hydrolysis) and has been realised in other areas of the body [86]. Kon et al. used a nanostructured scaffold to surgically pack a chronic degenerative chondral lesion in a high demand knee. The response to treatment was monitored clinically with pain-free function at a year following surgery and by MRI which demonstrated healing [87]. Alternatively, a more robust or self-healing synthetic mimic, which retains the biomechanical properties of cartilage, could be created. This is exemplified by newer nanoplastics developed for use in prosthetics, with the ability to self-repair following micro or even macro level damage [41]. These can be created as multilayered structures which may better represent interfaces between tissues such as cartilage and bone [88]. Nanocomposites have been developed using Type I collagen and hydroxyapatite with promising results [88].
3.5.3 Anterior Cruciate Ligament Injury
ACL ruptures are common, with an estimated incidence rate of 37 per 100,000 person-years or approximately 118,000 ruptures in the USA alone [89]. Up to two thirds of these patients (79,000) experience instability that limits their daily activity or sport and recreation [90] with up to 76.6% of such patients requiring surgery [90]. A review of approximately 13,000 ACL reconstructions on the Swedish knee ligament register reported a 1.6% incidence of revision surgery at 2-year follow-up [91].
Success of an ACL reconstruction relies upon two key ideologies: the constituents of the graft and the integration of the graft with the host [92, 93]. The former primarily addresses the strength of the mobile segment of the repair, its kinematics through ranges of movement and its longevity. The latter is concerned with the degree and speed with which biological integration occurs in the static segments (proximal and distal) of the graft embedded within bone tunnels and the minimisation of factors that would weaken the integration over time. ACL reconstruction represents a unique area in which to test the possible applications of current nanotechnological concepts and to consider new avenues for their development which could aid in addressing these two points. The current focus of investigation includes the creation of artificial ligament replacements which is less common than autograft repair but is still used and the enhancement of bone graft integration [85, 94,95,96,97]. The manufacturing of artificial grafts which incorporate into host tissue and function as a native ACL is still at the exploratory stage.
The incorporation of a graft into bone tunnels provides long-term fixation; however, this remains the weak link in ACL reconstruction, accounting for early failures and limiting the speed of rehabilitation [98]. Multiple tissue engineering strategies using nanotechnology are being developed for improved bone graft interface healing and include local delivery of bioactive compounds such as collagen using scaffolds, coating of implants and grafts and augmentation of the canal [99]. Chou et al. undertook an in vivo study looking at the pull-out strength and histological features of collagen and biodegradable poly lactic-co-glycolic acid coated nanofibre membrane graft in the form of a scaffold. Histologically the researchers noted a reduction in tunnel size and greater graft-bone integration in the form of fibre-bone anchors using the scaffold. Pull-out strength was much greater in those treated with the scaffold [100]. Han et al. examined the tissue integration of tendon graft wrapped in polycaprolactone/nanohydroxyapatite/collagen nanofibre and non-wrapped tendon in vitro and in vivo. Wrapped semimembranosus ACL graft was found to have better integration, mineralisation and mechanical stretch [101]. Grant et al. undertook a study in which human tendon impregnated with various combinations of gold and hydroxyapatite nanoparticles was grafted into animal models in place of an ACL. These were compared with nonimpregnated grafts after approximately 3 months, and it was found that grafts with gold nanoparticles had greater new growth of fibrous connective tissue and higher vascularity [102]. These results support the findings by Smith et al. who undertook a similar study of gold and hydroxyapatite nanoparticles and found improved cell viability [103].
Some ACL tears are amenable to repair, but ligament healing forms a fibrous scare resulting in inferior biomechanical properties [100, 104]. It may be possible to enhance this or to create ligament substitutes from nanoengineered materials which may improve integration and physical properties and decrease donor site morbidity. In addition, nanoscaffolds could be used to augment existing grafts to enhance integration properties with bone [93], which could enhance the pace of healing and the ability to return to activities compared to existing techniques [99, 100].
3.6 Trauma Applications
Given the nanocomposite nature of bone, osseous trauma can be difficult to treat with traditional surgical methods of fixation which lack nanoscale properties. This is especially the case in areas of poor healing such as the femoral head and talus which are at risk of avascular necrosis, stripped soft tissue covering, bone loss and superimposed infection. The key principles of this technology for healing include attractive mechanical characteristics, surface modification of implants to aid fixation and scaffolds for tissue integration or defect filling.
3.6.1 Surface Modification
Modification of existing fracture fixation techniques using nanotechnology to enhance incorporation into the host tissue, to reduce the need for foreign material implantation or to reduce the need for repeated procedures to remove implants once healing is complete is key research areas. The biocompatibility of an implant is determined by its surface characteristics, and nanoscale coating applied to their surface may offer a solution in terms of accelerated bony healing and minimal tissue reaction to foreign material. Surface characteristics include the surface area or roughness, hydrophobicity and immunogenicity which determine the implant’s ability to integrate into the body and influence healing [105]. Surface modification at the nanoscale can be achieved by several methods, including altering the structure of endogenous substances such as collagen, creation of artificial nanomaterials applied to the surface of implants or anodization of existing materials, primarily metals [105].
Alteration of metallic and ceramic implant surfaces at the nanoscale has been shown to improve osteoblasts adhesion and proliferation, calcium deposition and alkaline phosphatase activity [105]. A recent study used bioactive and degradable nanocomposite coating on k-wire fixation of animal tibia in vivo and evaluated these at 1 and 2 months postoperatively [106]. The results indicated minimal soft tissue reaction and an increase in healing rate in those treated with the nanocoat. Hydroxyapatite-coated screws have been trialled in hip fracture surgery and have been shown to provide superior fixation in osteoporotic bone [107] as an effective coating for half pins in external fixation constructs. These applications are particularly relevant around the knee where removal or metalwork may be required before subsequent surgery, for example, knee replacement following high tibial osteotomy or tibial plateau fixation. In addition, fixation of osteochondral fractures and meniscal tears within the knee are perfectly suitable for nanoengineered fixation devices due to the intra-articular environment which better mimic the tissue and incorporate over time as the tissue heals.
3.6.2 Scaffolds
Orthopaedic fixation devices could be engineered to have properties that encourage healing and regeneration which current implants do not offer. Key to fracture healing is the extracellular matrix which not only serves as a scaffold for growth and healing but also acts as a source of growth factors and other key constituents of repair [108]. Implantation of impregnated, degradable scaphoids could enhance bone healing by providing an immediate source of bone-forming cells and materials with minimal tissue reaction. Peptides which undergo self-assembly into nanostructures (termed self-assembling peptides) have been shown to enhance cell replication and proliferation and promote bone regeneration and healing whilst inhibiting demineralization. Another option for surface modification to improve bone healing is with carbon nanotubes, multiple forms of which have been shown to improve bone repair and provide exceptional mechanical stability; however, peptides are more versatile in terms of architecture and are less hydrophobic. Coating of titanium or hydroxyapatite implants with components of the ECM such as collagen and chondroitin sulphate may greatly improve the quality of fracture fixation and speed of bony healing [108]. Recent advances in biologically engineered hydrogels at the nano level have been shown to dramatically improve the osseous forming components following fracture. Hydrogel biomaterials are highly porous structures which can mimic the extracellular matrix and enhancing these at the nanoscale may greatly improve bone healing. Xavier et al. undertook a study in which collagen-based hydrogels impregnated with nanosilicates of orthosilicic acid (bioavailable silicon utilised by living organisms), magnesium and lithium were created and used in the healing of non-united fractures. They found a marked increase in the activity of alkaline phosphatase and the formation of mineralised matrix. They concluded that adequate osteogenesis could occur even in the absence of osteoinductive and growth factors [109]. These substances could be injected into osseous defects both in the immediate postfracture period and in chronic non-unions, optimising healing whilst gradually being replaced by native tissue. Nanocomposite hydrogels may also be used to induce stem cells into a desired cell type by mimicking bone-inducing growth factors [110].
Gao et al. examined the potential applications of nanotechnology in treating avascular necrosis of the femoral head by applying nanoscale decompression cores containing mesenchymal stem cells in 12 patients with early stages of the disease and found that the treatment was effective in alleviating symptomology and improving radiographic appearance [111]. Yang et al. also looked at the applications of nanotechnology on avascular necrosis of the femoral head. Patients were treated with core decompression in combination with a nanohydroxyapatite and polyamide rod and a porous bioglass bone graft, and an equal number were treated with core decompression with an autologous cancellous bone graft. The clinical failure rate was lower in the non-particle-enhanced approach, and overall, symptomology and functionality were better in this group [112].
3.7 Bone Grafting
There has been much interest in the world of nanotechnology around bone graft substitutes using nanoengineered scaffolds and other techniques. These products would be particularly useful around the knee both in trauma surgery and in revision knee arthroplasty as bone loss can be an issue in some cases following implant removal. Currently bone graft is used for small defects, and larger defects are managed with augments or wedges that are usually metal or polyethylene. The current augmentation techniques are effective but do not reconstitute the patient’s bone stock. The use of nanoengineered structural scaffolds with biological properties could be very effective in this area to fill these defects and provide structural stability, whilst natural bone stock is restored during the integration process. Nanoparticles of various bone graft substances are in development, and these have shown promising results in addition to nanoscaffolds in combination with bone morphogenic proteins, the latter having been shown in vivo to be a highly effective osteogenic and osteoconductive graft substance [37]. Other in vivo studies have looked at the potential of filling bone defects with nanotechnology and have shown exciting results. Recent studies have examined the effects of a nanoscale filling material in the form of porous hydroxyapatite as a substitute for bone graft and found that normal bony healing resulted, including a mature haversian system [113].
3.8 Safety Considerations
The question of safety relating to the use of nanotechnology is not without justification. Nanoparticles can be toxic and have been associated with a host of human disease and may result in massive environmental damage with widespread use. Asbestos was once hailed as a miracle material due to its versatility and was used extensively in construction and other industry in the early half of the last century, resulting in disease in the form of asbestosis and mesothelioma [114]. The open questions relating to the safety of nanotechnology have led to developments of the field of nanotoxicology which aims to study this in detail. Although many of the technologies used are based on biological systems or compounds already in use, differences in forms or sizes of materials are responsible for the increased risk. Nanoparticles are more likely to pass undetected by the respiratory immune system [115] and have been known to pass across vascular barriers and potentially alter clotting [116]. Nanoparticles can pass the blood–brain barrier and may be implicated in degenerative brain disease [117]. In orthopaedics, questions arise relating to the toxicity of wear particles which are a proven risk even when none nanomaterial is utilised in joint replacement surgery [118]. Questions also remain over the long-term toxic effects of nanomaterials in vivo [27]. Despite the exciting and imminent therapeutic advancements offered by nanotechnology, urgent and exhaustive research into the medical and environmental risks associated with its wider use is required [27].
3.9 Conclusions
Currently the published data supports the applicability of a wide variety of nanotechniques which have the potential to revolutionise the management of a plethora of medical and surgical pathologies, once considered refractory to treatment or even incurable. In knee surgery, this potential is diverse in terms of disease type, surgical or nonsurgical options, method of drug or device delivery and overall strategy of applying new technologies. Synergistic strategies encourage organic and inorganic cooperation to improve healing following trauma, better graft integration following ligament repair or reconstruction and creating a nourishing microenvironment for stem cell differentiation and tissue integration. Furthermore, targeting strategies that improve pharmacokinetics in musculoskeletal could aid in the treatment of neoplasia and in symptomatic care of patients with chronic or degenerative disease. Implants used for trauma or arthroplasty may be enhanced by nanotechnology with a concomitant reduction in revision procedures. Infection-resistant materials or coatings, highly integrative implants and revolutionary materials with the ability to repair or regenerate may represent the advent of a new era in arthroplasty. These potential advances are exciting, but enthusiasm for their use must be tempered until the risks of nanotechnology are fully investigated.
References
Pleshko N, Grande DA, Myers KR (2012) Nanotechnology in orthopaedics. J Am Acad Orthop Surg 20(1):60–62
Favier I, Teuma E, Gómez M (2009) Palladium and ruthenium nanoparticles: reactivity and coordination at the metallic surface. C R Chim 12(5):533–545
Park S-C, Kim N, Ji S, Lim H (2016) Fabrication and characterization of moth-eye mimicking nanostructured convex lens. Microelectron Eng 158:35–40
Ma S, Wang D, Liang Y, Sun B, Gorb SN, Zhou F (2015) Gecko-inspired but chemically switched friction and adhesion on nanofibrillar surfaces. Small 11(9–10):1131–1137
Karthick B, Maheshwari R (2008) Lotus-inspired nanotechnology applications. Resonance 13(12):1141–1145
Kawase T, Tanaka K, Shiono N, Seirai Y, Oda M (2004) Onion-type complexation based on carbon nanorings and a buckminsterfullerene. Angew Chem Int Ed 43(13):1722–1724
Culpepper ML, DiBiasio CM, Panas RM, Magleby S, Howell LL (2006) Simulation of a carbon nanotube-based compliant parallel-guiding mechanism: a nanomechanical building block. Appl Phys Lett 89:203111. https://doi.org/10.1063/1.2388143
Brown CP (2013) Advancing musculoskeletal research with nanoscience. Nat Rev Rheumatol 9(10):614–623
Korkusuz F (2013) Editorial comment: nanoscience in musculoskeletal medicine. Clin Orthop Relat Res 471(8):2530–2531
Bernthal NM, Stavrakis AI, Billi F et al (2010) A mouse model of post-arthroplasty staphylococcus aureus joint infection to evaluate in vivo the efficacy of antimicrobial implant coatings. PLoS One 5(9):e12580
Katainen J, Paajanen M, Ahtola E, Pore V, Lahtinen J (2006) Adhesion as an interplay between particle size and surface roughness. J Colloid Interface Sci 304(2):524–529
Zhu H, Guo Z, Liu W (2014) Adhesion behaviors on superhydrophobic surfaces. Chem Commun (Camb) 50(30):3900–3913
Goldman M, Juodzbalys G, Vilkinis V (2014) Titanium surfaces with nanostructures influence on osteoblasts proliferation: a systematic review. J Oral Maxillofac Res 5(3):e1
Gallo J, Holinka M, Moucha CS (2014) Antibacterial surface treatment for orthopaedic implants. Int J Mol Sci 15(8):13849–13880
Holinka J, Pilz M, Kubista B, Presterl E, Windhager R (2013) Effects of selenium coating of orthopaedic implant surfaces on bacterial adherence and osteoblastic cell growth. Bone Joint J 95-B(5):678–682
Jain KK (2005) Nanotechnology in clinical laboratory diagnostics. Clin Chim Acta 358(1–2):37–54
Savaliya R, Shah D, Singh R et al (2015) Nanotechnology in disease diagnostic techniques. Curr Drug Metab
Ruggiero C, Pastorino L, Herrera OL (2010) Nanotechnology based targeted drug delivery. Conf Proc IEEE Eng Med Biol Soc 2010:3731–3732
Hamidi M, Azadi A, Rafiei P, Ashrafi H (2013) A pharmacokinetic overview of nanotechnology-based drug delivery systems: an ADME-oriented approach. Crit Rev Ther Drug Carrier Syst 30(5):435–467
Zhang Y, Huang Y, Li S (2014) Polymeric micelles: nanocarriers for cancer-targeted drug delivery. AAPS PharmSciTech 15(4):862–871
Kateb B, Chiu K, Black KL et al (2011) Nanoplatforms for constructing new approaches to cancer treatment, imaging, and drug delivery: what should be the policy? Neuroimage 54(Suppl 1):S106–S124
Man HB, Kim H, Kim HJ et al (2014) Synthesis of nanodiamond-daunorubicin conjugates to overcome multidrug chemoresistance in leukemia. Nanomedicine 10(2):359–369
Rosenthal SJ, Chang JC, Kovtun O, McBride JR, Tomlinson ID (2011) Biocompatible quantum dots for biological applications. Chem Biol 18(1):10–24
Von Hoff DD, Mita MM, Ramanathan RK et al (2016) Phase I study of PSMA-targeted docetaxel-containing nanoparticle BIND-014 in patients with advanced solid tumors. Clin Cancer Res 22(13):3157–3163
Freeman AI, Halladay LJ, Cripps P (2012) The effect of silver impregnation of surgical scrub suits on surface bacterial contamination. Vet J 192(3):489–493
Parthasarathi V, Thilagavathi G (2013) Developing antiviral surgical gown using nonwoven fabrics for health care sector. Afr Health Sci 13(2):327–332
Health Quality Ontario (2006) Nanotechnology: an evidence-based analysis. Ont Health Technol Assess Ser 6(19):1–43
Makidon PE, Nigavekar SS, Bielinska AU et al (2010) Characterization of stability and nasal delivery systems for immunization with nanoemulsion-based vaccines. J Aerosol Med Pulm Drug Deliv 23(2):77–89
Bailey ZS, Nilson E, Bates JA et al (2016) Cerium oxide nanoparticles improve outcome after in vitro and in vivo mild traumatic brain injury. J Neurotrauma. https://doi.org/10.1089/neu.2016.4644
Grausova L, Bacakova L, Kromka A et al (2009) Nanodiamond as promising material for bone tissue engineering. J Nanosci Nanotechnol 9(6):3524–3534
Tee BC, Wang C, Allen R, Bao Z (2012) An electrically and mechanically self-healing composite with pressure- and flexion-sensitive properties for electronic skin applications. Nat Nanotechnol 7(12):825–832
Cormode DP, Skajaa T, Fayad ZA, Mulder WJ (2009) Nanotechnology in medical imaging: probe design and applications. Arterioscler Thromb Vasc Biol 29(7):992–1000
Orringer DA, Koo YE, Chen T, Kopelman R, Sagher O, Philbert MA (2009) Small solutions for big problems: the application of nanoparticles to brain tumor diagnosis and therapy. Clin Pharmacol Ther 85(5):531–534
Ali SM, Aijazi T, Axelsson K, Nur O, Willander M (2011) Wireless remote monitoring of glucose using a functionalized ZnO nanowire arrays based sensor. Sensors (Basel) 11(9):8485–8496
Chen H, Li J (2007) Nanotechnology: moving from microarrays toward nanoarrays. Methods Mol Biol 381:411–436
Miled MA, Massicotte G, Sawan M (2012) Dielectrophoresis-based integrated lab-on-chip for nano and micro-particles manipulation and capacitive detection. IEEE Trans Biomed Circuits Syst 6(2):120–132
Schofer MD, Roessler PP, Schaefer J et al (2011) Electrospun PLLA nanofiber scaffolds and their use in combination with BMP-2 for reconstruction of bone defects. PLoS One 6(9):e25462
Deng M, James R, Laurencin CT, Kumbar SG (2012) Nanostructured polymeric scaffolds for orthopaedic regenerative engineering. IEEE Trans Nanobioscience 11(1):3–14
Sartori M, Giavaresi G, Parrilli A et al (2015) Collagen type I coating stimulates bone regeneration and osteointegration of titanium implants in the osteopenic rat. Int Orthop 39(10):2041–2052
Li Y, Jiao Y, Li X, Guo Z (2015) Improving the osteointegration of Ti6Al4V by zeolite MFI coating. Biochem Biophys Res Commun 460(2):151–156
Amendola V, Meneghetti M (2009) Self-healing at the nanoscale. Nanoscale 1(1):74–88
Kelly EW, Coghlan J, Bell S (2004) Five- to thirteen-year follow-up of the GSB III total elbow arthroplasty. J Shoulder Elbow Surg 13(4):434–440
Kinov P, Bukarev D, Dimov V, Kazakov K, Tivchev P (2007) Revision total hip arthroplasty with cementing technique—five-year results. Chir Narzadow Ruchu Ortop Pol 72(4):293–296
Poss R, Brick GW, Wright RJ, Roberts DW, Sledge CB (1988) The effects of modern cementing techniques on the longevity of total hip arthroplasty. Orthop Clin North Am 19(3):591–598
Evans BG, Salvati EA, Huo MH, Huk OL (1993) The rationale for cemented total hip arthroplasty. Orthop Clin North Am 24(4):599–610
Gittens RA, Olivares-Navarrete R, Schwartz Z, Boyan BD (2014) Implant osseointegration and the role of microroughness and nanostructures: lessons for spine implants. Acta Biomater 10(8):3363–3371
Mavrogenis AF, Dimitriou R, Parvizi J, Babis GC (2009) Biology of implant osseointegration. J Musculoskelet Neuronal Interact 9(2):61–71
Rieger E, Dupret-Bories A, Salou L et al (2015) Controlled implant/soft tissue interaction by nanoscale surface modifications of 3D porous titanium implants. Nanoscale 7(21):9908–9918
Zan X, Kozlov M, McCarthy TJ, Su Z (2010) Covalently attached, silver-doped poly(vinyl alcohol) hydrogel films on poly(l-lactic acid). Biomacromolecules 11(4):1082–1088
Tran PA, Sarin L, Hurt RH, Webster TJ (2010) Titanium surfaces with adherent selenium nanoclusters as a novel anticancer orthopedic material. J Biomed Mater Res A 93(4):1417–1428
Gu W, Wu C, Chen J, Xiao Y (2013) Nanotechnology in the targeted drug delivery for bone diseases and bone regeneration. Int J Nanomedicine 8:2305–2317
Ramanlal Chaudhari K, Kumar A, Megraj Khandelwal VK et al (2012) Bone metastasis targeting: a novel approach to reach bone using zoledronate anchored PLGA nanoparticle as carrier system loaded with docetaxel. J Control Release 158(3):470–478
Susa M, Iyer AK, Ryu K et al (2009) Doxorubicin loaded polymeric nanoparticulate delivery system to overcome drug resistance in osteosarcoma. BMC Cancer 9:399
Sun K, Wang J, Zhang J, Hua M, Liu C, Chen T (2011) Dextran-g-PEI nanoparticles as a carrier for co-delivery of adriamycin and plasmid into osteosarcoma cells. Int J Biol Macromol 49(2):173–180
Yang L, Webster TJ (2009) Nanotechnology controlled drug delivery for treating bone diseases. Expert Opin Drug Deliv 6(8):851–864
Rai M, Yadav A, Gade A (2009) Silver nanoparticles as a new generation of antimicrobials. Biotechnol Adv 27(1):76–83
Zhao L, Wang H, Huo K et al (2011) Antibacterial nano-structured titania coating incorporated with silver nanoparticles. Biomaterials 32(24):5706–5716
United Kingdom Department of Health (2016) National joint registry for England, wales, Northern Ireland and The Isle of Man, 13th Annual Report. www.njrcentre.org.uk. Accessed May 2017.
Tomisa AP, Launey ME, Lee JS, Mankani MH, Wegst UG, Saiz E (2011) Nanotechnology approaches to improve dental implants. Int J Oral Maxillofac Implants 26(Suppl):25–44. discussion 45-9
Raimondo T, Puckett S, Webster TJ (2010) Greater osteoblast and endothelial cell adhesion on nanostructured polyethylene and titanium. Int J Nanomedicine 5:647–652
Bahl S, Shreyas P, Trishul MA, Suwas S, Chatterjee K (2015) Enhancing the mechanical and biological performance of a metallic biomaterial for orthopedic applications through changes in the surface oxide layer by nanocrystalline surface modification. Nanoscale 7(17):7704–7716
Webster TJ, Ejiofor JU (2004) Increased osteoblast adhesion on nanophase metals: Ti, Ti6Al4V, and CoCrMo. Biomaterials 25(19):4731–4739
Price RL, Ellison K, Haberstroh KM, Webster TJ (2004) Nanometer surface roughness increases select osteoblast adhesion on carbon nanofiber compacts. J Biomed Mater Res A 70(1):129–138
Singh AV, Vyas V, Patil R et al (2011) Quantitative characterization of the influence of the nanoscale morphology of nanostructured surfaces on bacterial adhesion and biofilm formation. PLoS One 6(9):e25029
Shida T, Koseki H, Yoda I, Horiuchi H, Sakoda H, Osaki M (2013) Adherence ability of staphylococcus epidermidis on prosthetic biomaterials: An in vitro study. Int J Nanomedicine 8:3955–3961
Ivanova EP, Truong VK, Wang JY et al (2010) Impact of nanoscale roughness of titanium thin film surfaces on bacterial retention. Langmuir 26(3):1973–1982
Truong VK, Lapovok R, Estrin YS et al (2010) The influence of nano-scale surface roughness on bacterial adhesion to ultrafine-grained titanium. Biomaterials 31(13):3674–3683
Cheng H, Li Y, Huo K, Gao B, Xiong W (2014) Long-lasting in vivo and in vitro antibacterial ability of nanostructured titania coating incorporated with silver nanoparticles. J Biomed Mater Res A 102(10):3488–3499
Gao A, Hang R, Huang X et al (2014) The effects of titania nanotubes with embedded silver oxide nanoparticles on bacteria and osteoblasts. Biomaterials 35(13):4223–4235
Mei S, Wang H, Wang W et al (2014) Antibacterial effects and biocompatibility of titanium surfaces with graded silver incorporation in titania nanotubes. Biomaterials 35(14):4255–4265
Dong W, Zhu Y, Zhang J et al (2013) Investigation on the antibacterial micro-porous titanium with silver nano-particles. J Nanosci Nanotechnol 13(10):6782–6786
Panacek A, Balzerova A, Prucek R et al (2013) Preparation, characterization and antimicrobial efficiency of ag/PDDA-diatomite nanocomposite. Colloids Surf B Biointerfaces 110:191–198
Knetsch MLW, Koole LH (2011) New strategies in the development of antimicrobial coatings: The example of increasing usage of silver and silver nanoparticles. Polymer 3:340–366
Kvitek L, Panacek A, Soukupova J et al (2008) Effect of surfactants and polymers on stability and antibacterial activity of silver nanoparticles (NPs). J Phys Chem C 112:5825–5834
Biggs MJ, Richards RG, Gadegaard N, Wilkinson CD, Dalby MJ (2007) The effects of nanoscale pits on primary human osteoblast adhesion formation and cellular spreading. J Mater Sci Mater Med 18(2):399–404
Miyauchi T, Yamada M, Yamamoto A et al (2010) The enhanced characteristics of osteoblast adhesion to photofunctionalized nanoscale TiO2 layers on biomaterials surfaces. Biomaterials 31(14):3827–3839
Salou L, Hoornaert A, Louarn G, Layrolle P (2015) Enhanced osseointegration of titanium implants with nanostructured surfaces: an experimental study in rabbits. Acta Biomater 11:494–502
Durmus NG, Webster TJ (2012) Nanostructured titanium: the ideal material for improving orthopedic implant efficacy? Nanomedicine (Lond) 7(6):791–793
Antoci V Jr, Adams CS, Parvizi J, Ducheyne P, Shapiro IM, Hickok NJ (2007) Covalently attached vancomycin provides a nanoscale antibacterial surface. Clin Orthop Relat Res 461:81–87
Puckett SD, Taylor E, Raimondo T, Webster TJ (2010) The relationship between the nanostructure of titanium surfaces and bacterial attachment. Biomaterials 31(4):706–713
Fu J, Ji J, Fan D, Shen J (2006) Construction of antibacterial multilayer films containing nanosilver via layer-by-layer assembly of heparin and chitosan-silver ions complex. J Biomed Mater Res A 79(3):665–674
Khandaker M, Li Y, Morris T (2013) Micro and nano MgO particles for the improvement of fracture toughness of bone-cement interfaces. J Biomech 46(5):1035–1039. https://doi.org/10.1016/j.jbiomech.2012.12.006. Epub 2013 Jan 16
Ricker A, Liu-Snyder P, Webster TJ (2008) The influence of nano MgO and BaSO4 particle size additives on properties of PMMA bone cement. Int J Nanomedicine 3(1):125–132
Argatov I, Mishuris G (2016) Articular contact mechanics from an asymptotic modeling perspective: a review. Front Bioeng Biotechnol 4:83
Li H, Jiang J, Wu Y, Chen S (2012) Potential mechanisms of a periosteum patch as an effective and favourable approach to enhance tendon-bone healing in the human body. Int Orthop 36(3):665–669
Ch'ng S, Wong GL, Clark JR (2014) Reconstruction of the trachea. J Reconstr Microsurg 30(3):153–162
Kon E, Delcogliano M, Filardo G, Altadonna G, Marcacci M (2009) Novel nano-composite multi-layered biomaterial for the treatment of multifocal degenerative cartilage lesions. Knee Surg Sports Traumatol Arthrosc 17(11):1312–1315. https://doi.org/10.1007/s00167-009-0819-8. Epub 2009 May 26
Takakuda K, Koyama Y, Matsumoto HN et al (2007) Material design of bioabsorbable inorganic/organic composites for bone regeneration. J Nanosci Nanotechnol 7(3):738–741
Gianotti SM, Marshall SW, Hume PA, Bunt L (2009) Incidence of anterior cruciate ligament injury and other knee ligament injuries: a national population-based study. J Sci Med Sport 12(6):622–627
Joseph AM, Collins CL, Henke NM, Yard EE, Fields SK, Comstock RD (2013) A multisport epidemiologic comparison of anterior cruciate ligament injuries in high school athletics. J Athl Train 48(6):810–817
Andernord D, Bjornsson H, Petzold M et al (2014) Surgical predictors of early revision surgery after anterior cruciate ligament reconstruction: results from the Swedish national knee ligament register on 13,102 patients. Am J Sports Med 42(7):1574–1582
Kiapour AM, Murray MM (2014) Basic science of anterior cruciate ligament injury and repair. Bone Joint Res 3(2):20–31
Vavken P, Fleming BC, Mastrangelo AN, Machan JT, Murray MM (2012) Biomechanical outcomes after bioenhanced anterior cruciate ligament repair and anterior cruciate ligament reconstruction are equal in a porcine model. Arthroscopy 28(5):672–680
Liwen L, Hui W, Ming N et al (2014) Enhanced osteointegration of medical titanium implant with surface modifications in micro/nanoscale structures. J Orthop Transl 2:35–42
Kadonishi Y, Deie M, Takata T, Ochi M (2012) Acceleration of tendon-bone healing in anterior cruciate ligament reconstruction using an enamel matrix derivative in a rat model. J Bone Joint Surg Br 94(2):205–209
Haenle M, Fritsche A, Zietz C et al (2011) An extended spectrum bactericidal titanium dioxide (TiO2) coating for metallic implants: in vitro effectiveness against MRSA and mechanical properties. J Mater Sci Mater Med 22(2):381–387
Hu H, Zhang W, Qiao Y, Jiang X, Liu X, Ding C (2012) Antibacterial activity and increased bone marrow stem cell functions of zn-incorporated TiO2 coatings on titanium. Acta Biomater 8(2):904–915
Stevenson S, Emery SE, Goldberg VM (1996) Factors affecting bone graft incorporation. Clin Orthop Relat Res 324:66–74
Liu Y, Ramanath HS, Wang DA (2008) Tendon tissue engineering using scaffold enhancing strategies. Trends Biotechnol 26(4):201–209
Chou YC, Yeh WL, Chao CL, Hsu YH et al (2016) Enhancement of tendon-bone healing via the combination of biodegradable collagen-loaded nanofibrous membranes and a three-dimensional printed bone-anchoring bolt. Int J Nanomedicine 11:4173–4186. https://doi.org/10.2147/IJN.S108939
Han F, Zhang P, Sun Y, Lin C, Zhao P, Chen J (2015) Hydroxyapatite-doped polycaprolactone nanofiber membrane improves tendon-bone interface healing for anterior cruciate ligament reconstruction. Int J Nanomedicine 10:7333–7343
Grant SA, Smith SE, Schmidt H, Pfeiffer F, Kuroki K, Sherman S, White R, Grant DA (2017) In vivo bone tunnel evaluation of nanoparticle-grafts using an ACL reconstruction rabbit model. J Biomed Mater Res A. https://doi.org/10.1002/jbm.a.36000
Smith SE, White RA, Grant DA, Grant SA (2016) Gold and hydroxyapatite nano-composite scaffolds for anterior cruciate ligament reconstruction: in vitro characterization. J Nanosci Nanotechnol 16(1):1160–1169
Evans S, Shaginaw J, Bartolozzi A (2014) Acl reconstruction—it's all about timing. Int J Sports Phys Ther 9(2):268–273
Zhang ZG, Li ZH, Mao XZ, Wang WC (2011) Advances in bone repair with nanobiomaterials: mini-review. Cytotechnology 63(5):437–443. https://doi.org/10.1007/s10616-011-9367-4. Epub 2011 Jul 12
Mehdikhani-Nahrkhalaji M, Fathi MH, Mortazavi V, Mousavi SB et al (2012) Novel nanocomposite coating for dental implant applications in vitro and in vivo evaluation. J Mater Sci Mater Med 23(2):485–495. https://doi.org/10.1007/s10856-011-4507-0. Epub 2011 Nov 30
Moroni A, Faldini C, Pegreffi F, Giannini S (2004) HA-coated screws decrease the incidence of fixation failure in osteoporotic trochanteric fractures. Clin Orthop Relat Res 425:87–92
Forster Y, Rentsch C, Schneiders W et al (2012) Surface modification of implants in long bone. Biomatter 2(3):149–157
Xavier JR, Thakur T, Desai P, Jaiswal MK, Sears N, Cosgriff-Hernandez E, Kaunas R, Gaharwar AK (2015) Bioactive nanoengineered hydrogels for bone tissue engineering: a growth-factor-free approach. ACS Nano 9(3):3109–3118. https://doi.org/10.1021/nn507488s. Epub 2015 Feb 25
Paul A, Manoharan V, Krafft D, Assmann A et al (2016) Nanoengineered biomimetic hydrogels for guiding human stem cell osteogenesis in three dimensional microenvironments. J Mater Chem B Mater Biol Med 4(20):3544–3554. Epub 2016 Feb 4
Gao H, Zhang G, Wang J, Zhao F et al (2015) Clinical effects of novel nanoscaled core decompression rods combined with umbilical cord mesenchymal stem cells on the treatment of early osteonecrosis of the femoral head. J Nanomat:902836. https://doi.org/10.1155/2015/902836
Yang P, Bian C, Huang X, Shi A, Wang C, Wang K (2014) Core decompression in combination with nano-hydroxyapatite/polyamide 66 rod for the treatment of osteonecrosis of the femoral head. Arch Orthop Trauma Surg 134(1):103–112. https://doi.org/10.1007/s00402-013-1885-4. Epub 2013 Nov
Nandi SK, Kundu B, Ghosh SK, De DK, Basu D (2008) Efficacy of nano-hydroxyapatite prepared by an aqueous solution combustion technique in healing bone defects of goat. J Vet Sci 9(2):183–191
Bartrip PW (2004) History of asbestos related disease. Postgrad Med J 80(940):72–76
Viswanath B, Kim S (2016) Influence of nanotoxicity on human health and environment: the alternative strategies. Rev Environ Contam Toxicol
Kim D, Finkenstaedt-Quinn S, Hurley KR, Buchman JT, Haynes CL (2014) On-chip evaluation of platelet adhesion and aggregation upon exposure to mesoporous silica nanoparticles. Analyst 139(5):906–913
Rollerova E, Tulinska J, Liskova A et al (2015) Titanium dioxide nanoparticles: some aspects of toxicity/focus on the development. Endocr Regul 49(2):97–112
Korovessis P, Petsinis G, Repanti M, Repantis T (2006) Metallosis after contemporary metal-on-metal total hip arthroplasty. Five to nine-year follow-up. J Bone Joint Surg Am 88(6):1183–1191
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Kwaees, T.A., Pearce, A., Ring, J., Sutton, P., Charalambous, C.P. (2018). Nanotechnology and Its Applications in Knee Surgery. In: Jackson, M., Ahmed, W. (eds) Micro and Nanomanufacturing Volume II. Springer, Cham. https://doi.org/10.1007/978-3-319-67132-1_3
Download citation
DOI: https://doi.org/10.1007/978-3-319-67132-1_3
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-67130-7
Online ISBN: 978-3-319-67132-1
eBook Packages: EngineeringEngineering (R0)