Abstract
The stem cell field witnessed a genuine breakthrough when a combination of solely four transcription factors (Oct3/4, Sox2, Klf4 and c-Myc, OSKM) proved enough to revert, in vitro, the differentiated status of a variety of cell types back to pluripotency, giving rise to so-called induced pluripotent stem (iPS) cells. Ten years after this revolutionary discovery, attempts to induce pluripotency have not been limited to the culture dish. Some studies have interrogated the downstream effects of the overexpression of OSKM reprogramming factors in the living organism. In this Chapter, we dissect the proof-of-principle studies that demonstrated that cellular reprogramming to pluripotency can be induced in vivo, in spite of unfavorable pro-differentiation signals present within the tissues. The links of in vivo reprogramming to pluripotency with tumorigenesis and teratoma formation, and the cross-talk with cellular senesce and tissue injury are also discussed.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
5.1 Introduction
Pluripotency is defined as the capacity of an undifferentiated cell to differentiate into cell types representative of all three germ layers (endoderm, mesoderm and ectoderm) that form embryonic and, eventually, adult tissues. In the mammalian organism and under normal circumstances, pluripotent stem cells are only found at early developmental stages, primarily in the inner cell mass (ICM) of the blastocyst, from where the so-called embryonic stem cells (ESCs) can be isolated and established in culture. As development continues, differentiation potential is progressively lost, and the majority of cells in the adult organism are terminally differentiated to perform specific functions within the tissue hierarchy. Although some tissues count with specific populations of stem cells to maintain tissue homeostasis, those are multi- or oligopotent (i.e. can only differentiate into a few cell types, most commonly within the same lineage), and no pluripotent cells remain naturally in the adult [1].
It is precisely their ample differentiation potential that has attracted great interest in pluripotent stem cells. Since they can be re-differentiated into specific progenitor and mature cell types in the laboratory, they are seen as invaluable research tools in developmental biology and to investigate cellular responses to drugs and other substances. More importantly, they are considered by many the “holy grail” in regenerative medicine, since they could potentially serve as starting source to generate new cells that replace those lost due to tissue injury or degeneration in a variety of conditions [2]. For all such reasons, the generation of pluripotent stem cells has been largely pursued and explored in the cell culture laboratory. By contrast, the generation of pluripotent stem cells directly in vivo has only recently seen the first proof-of-principle studies although, partly thanks to the knowledge generated in the culture dish, it is rapidly advancing to unveil its potential applications.
5.1.1 Sources of Pluripotent Stem Cells: From ESCs to Induced Reprogramming
Pluripotent stem cells, in particular ESCs, can be isolated from the ICM of mouse [3, 4] and human [5] blastocysts, and maintained as such in culture [6] (Fig. 5.1a). However, ethical implications brought by the destruction of embryonic material, as well as tight regulations that restrict their use and the capacity to fund and patent research in which ESCs are involved [7, 8], have prompted the search for less controversial sources of pluripotent stem cells (Fig. 5.1). Thanks to John Gurdon’s pioneering work on nuclear transfer [9,10,11] and Davis’ and Weintraub’s discoveries on the roles of transcription factors in cell fate decisions [12, 13], among many others, it is now understood that cell differentiation is not driven by irreversible changes to the genetic information of the cell, but by changes to the epigenetic landscape that can be reverted. Therefore, terminally differentiated cells retain all genetic information necessary to recapitulate the development of an entire organism. The differentiated status of adult cells is stable, but not irreversibly fixed, and it can be “reprogrammed” back to pluripotency as long and the appropriate switches are activated. Somatic cell nuclear transfer (SCNT), a process in which the nucleus of a somatic cell is introduced in an enucleated egg [14], has been one of the most popular approaches to achieve the pluripotent conversion (Fig. 5.1b). The oocyte contains molecular cues able to epigenetically reprogram the somatic nucleus back to pluripotency. The reprogrammed nucleus is in turn able to support the development of an entire new adult organism, and this technique is behind popular breakthroughs such as the first cloning of an adult frog [11] and the birth of Dolly the sheep [15]. Pluripotent stem cells have also been obtained in the laboratory by fusion events between somatic and embryonic carcinoma cells (ECCs), which are pluripotent cells isolated from germ cell tumors (Fig. 5.1c) [16]. However, none of these approaches is devoid of technical hurdles. Indeed, it took more than 20 years to adapt the SCNT protocol from amniotes to mammalian cells (sheep), and even harder efforts have been required to translate it to human cells, a procedure which is still today technically daunting [17, 18]. In addition, the specific molecular mechanisms and factors driving the conversion to pluripotency were never elucidated in the above studies.
Sources of pluripotent stem cells. Several strategies can be utilized to isolate naturally-occurring pluripotent stem cells or generate them artificially from other cell sources. (a) Naturally-occurring ESCs can be isolated from the ICM of the blastocyst and maintained in culture. (b) Pluripotent stem cells can be generated via transfer of a somatic cell nucleus into an enucleated oocyte. Factors present in the oocyte reprogram the somatic nucleus to a pluripotent state able to support the development of a whole adult organism. This procedure is known as Somatic Cell Nuclear Transfer (SCNT). (c) Fusion of a somatic cell with a pluripotent ECC generates an intermediate hybrid in which the pluripotent phenotype eventually outweighs the differentiated state. (d) Somatic cells can be reprogrammed to the pluripotent state via overexpression of defined transcription factors (Oct3/4, Sox2, Klf4, c-Myc, OSKM), generating so-called iPS cells
Precisely aiming to identify the molecular cues that trigger and orchestrate the induction of pluripotency, Yamanaka and Takahashi embarked on the ambitious challenge to screen a pool of transcription factors, all present in the oocyte and/or in ESCs and many of them with already-known roles in the maintenance of pluripotency. In a groundbreaking study published in 2006, which was awarded the 2012 Nobel Prize of Physiology and Medicine together with John Gurdon’s contributions to the field, they identified a cocktail of four transcription factors (Oct3/4, Sox2, Klf4 and cMyc, also known as OSKM or Yamanaka factors) as the most efficient combination to reprogram mouse embryonic and adult fibroblasts back to a pluripotent-like state (Fig. 5.1d) [19]. Their protocol was later refined to generate bona fide pluripotent cells that contributed to all adult tissues in murine chimeras [20], while the same and similar combinations of transcription factors (i.e. substituting KLF4 and cMYC by NANOG and LIN28) were shown to induce pluripotency in human cells [21, 22]. The resulting cells were named induced pluripotent stem (iPS) cells and have completely revolutionized the fields of stem cell research and regenerative medicine.
First, the implications of Yamanaka and Takahashi’s work are huge for the efforts in understanding the biological mechanisms behind the process of reprogramming to pluripotency, and have opened the doors to extensive research in this topic [23, 24]. In addition, identification of the OSKM cocktail has also provided a relatively straightforward as well as versatile “recipe” to generate pluripotent stem cells in the laboratory. Indeed, iPS cells have been generated from a wide variety of terminally differentiated cell types, with little or no variation in the combination of transcription factors and experimental protocols utilized, of which the most popular nowadays are skin fibroblasts and peripheral blood cells [25,26,27,28,29]. The use of those as starting cell types avoids the ethical and legal hurdles associated to the use of embryonic material, while it allows derivation of patient-specific iPS cells through minimally invasive procedures, such as a simple skin biopsy or a blood test. Obtaining iPS cells from individuals suffering from a particular disease has opened tremendous opportunities to study the evolution of the specific condition through different developmental stages, as well as to interrogate responses to drugs and treatments [30]. In the context of regenerative medicine, the possibility to generate replacement cells from the very same patient in need for the transplantation is thought to diminish the chances for graft rejection [31].
5.2 iPS Cells Escape the Culture Dish. Proof-of-Principle Studies of In Vivo Reprogramming to Pluripotency
The first years after Yamanaka and Takahashi’s groundbreaking study focused primarily on (1) the optimization of the reprogramming protocol to increase its efficiency and ensure reprogramming to ground-state pluripotency, (2) further elucidation of the mechanisms behind reprogramming, (3) the characterization of genomic integrity and stability of iPS cell clones and their direct comparison to ESCs and (4) the establishment of specific protocols to derive a plethora of differentiated cell types from patient-specific iPS cells, to be tested as disease models and in cell therapies. All of such studies were performed in the culture dish. However, the question whether the OSKM cocktail would be able to induce adult cells to pluripotency in vivo remained unanswered, in spite of undeniable interest from the mechanistic point of view and the obvious implications in regenerative medicine that will be discussed in Chap. 6.
In the culture dish, the induction of reprogramming takes place under defined and controlled conditions that are set to promote and maintain the pluripotent state. For example, mouse embryonic fibroblasts (MEFs) are used as feeder cells in many iPS cell generation protocols [19]. Leukaemia inhibitor factor (LIF) [6] is also supplemented in the cell culture medium to avoid differentiation and maintain pluripotency. In certain reprogramming protocols, additional substances are required to reach ground-state pluripotency. GSK3 and Mek1/2 inhibitors—widely known as 2i conditions—have been used to force partially reprogrammed intermediates, unable to differentiate into all three lineages, to ground-state pluripotency [32]. On a very different picture, the induction of pluripotency directly in vivo cannot benefit from such controlled and pluripotency-favorable conditions, but has to overcome the effect of pro-differentiation signals naturally present in the tissue microenvironment. This was therefore the first uncertainty on the feasibility of in vivo reprogramming to pluripotency.
More importantly, the fact that pluripotent stem cells have both the capacity to proliferate actively and to differentiate towards all developmental lineages and tissue types adds an additional concern and questions whether generating cells with such capabilities within the living organism would be safe. In fact, previous experience in the transplantation of ESCs and iPS cells confirmed that the administration of pluripotent cells in vivo can generate teratomas, tumors composed of cells from all three germ layers [33, 34]. Indeed, the teratoma formation assay is routinely used as a tool to assess pluripotency [35].
In spite of these initial doubts, the field jumped its way onto the in vivo scenario in the early 2010s with two independent studies that used episomal plasmid DNA (pDNA)—in pre-metamorphic tadpoles [36] and mice [37, 38], respectively—to demonstrate that in vivo overexpression of reprograming factors can outweigh the pro-differentiation signals present in the tissue microenvironment and reprogram cells back to pluripotency. Since then, the number of strategies to induce pluripotency in various different tissues via OSKM overexpression has grown, but the outcomes of such studies differ significantly depending on the duration of OSKM expression, which will be discussed in Chap. 6 of this book. For a summary of the studies on in vivo reprogramming via OSKM overexpression see Table 6.2 in Chap. 6 of this book.
5.2.1 In Vivo Reprogramming to Pluripotency in the Developing Tadpole
The first proof-of-principle study to demonstrate that cells can be reprogrammed to pluripotency in vivo was performed in pre-metamorphic tadpoles (Fig. 5.2) [36]. Direct intramuscular injection of a reprogramming pDNA encoding three of the Yamanaka factors (Oct3/4, Sox2 and Klf4, with the absence of c-Myc) in the tail muscle generated clusters of highly proliferative cells that showed several hallmarks of pluripotency. Among them, expression of endogenous pluripotency markers, upregulation of key epigenetic and chromatin remodeling markers and high alkaline phosphatase (AP) activity. Beyond their molecular signature, the capacity of the reprogrammed cells to differentiate into different lineages was tested both in vivo and in vitro. When left to re-differentiate within the tissue, they gave rise to neuron-like cells, representative of the ectoderm lineage. Transplantation of in vivo reprogrammed cells generated in pCar-GFP transgenic tadpoles into wild-type (WT) counterparts confirmed the capacity of such reprogrammed cells to re-differentiate towards the mesoderm lineage and generate new muscle fibers. Notably, both events took place even without the administration of growth factors that favor differentiation towards specific lineages. In vitro culture of OSK-injected muscles gave rise to cell colonies with morphology similar to that of ESCs, and that showed high AP activity. The differentiation of such cells could be directed to all three germ layers, which confirmed reprogramming to a pluripotency.
Proof-of-principle of in vivo reprogramming to pluripotency in pre-metamorphic tadpoles. (a) Direct intramuscular administration of pDNA encoding OSK reprogramming factors generated highly proliferative cell clusters within the muscle tissue that showed several hallmarks of pluripotency and re-differentiated spontaneously into representatives of ectoderm and mesoderm lineages. (b) Reprogrammed muscles cultured in vitro generated cell colonies that morphologically resembled those of iPS and ESCs and whose differentiation could be directed to all three embryonic lineages (ectoderm, mesoderm and endoderm) [36]
Within reprogrammed tissues, the morphology of the observed cell clusters was also very different from that of the regular muscle fibers. Nuclei were disorganized in such structures and significantly smaller than those in differentiated myofibers. However, proliferation was only observed within the clusters by PH3 expression for 14 days after injection and, in fact, the number and size of cell clusters peaked at day 7 to then decrease progressively, confirming that the reprogrammed cells did not persist as proliferative clusters within the tissues. An increase in the number of apoptotic cells was found in reprogrammed tissues at precisely the same time when clusters started to disappear. However, based on the results on cellular re-differentiation towards the ectoderm and mesoderm lineages mentioned above, it is likely that at least a percentage of the reprogrammed cells survived but re-differentiated spontaneously in response to the pro-differentiation signals present in the tissue. Importantly, the expression of reprogramming factors (OSK) was only detected for 7 days after pDNA injection. The impact of the duration of OSK expression in the fate of reprogrammed cells will be further discussed in Chap. 6.
Overall, this study demonstrated that pluripotency features can be artificially re-induced in a tissue within a developing living organism. Proof-of-concept in the fully developed adult is presented in Sect. 5.2.2.
5.2.2 In Vivo Reprogramming to Pluripotency in Adult Mouse Liver
Similar episomal pDNA cassettes (with the addition of c-Myc) were used to demonstrate that the pluripotent conversion can indeed take place in the adult, fully developed, mammalian organism [37, 38]. The mouse liver was the organ selected to direct such investigations, given the relative high efficiency of pDNA transfection that can be achieved via hydrodynamic tail vein (HTV) administration. This technique, which has been extensively exploited in the gene therapy field to specifically transfect hepatocytes, consists in a rapid intravenous injection of a large volume of fluid (10% of the body weight) containing the pDNA of interest [39]. Administration of such a large volume in only 5–7 s generates a transient heart failure that provokes the reversion of all the administered fluid to the hepatic circulation. The mechanisms by which pDNA is taken up by hepatocytes are not fully elucidated. Some studies point at a receptor-based mechanism, while others suggest the opening of pores in the hepatocyte membrane given the sudden influx of fluid. In addition, such a rapid cellular internalization of the nucleic acid avoids degradation driven by circulating nucleases and thus also contributes to the high levels of transgene expression achieved [40, 41].
Interestingly, very similar observations to those reported in pre-metamorphic tadpoles were made in the mouse study (Fig. 5.3), in spite of the significant differences between species and developmental stages involved in both models. In brief, clusters of cells expressing endogenous pluripotency markers appeared promptly in the liver after HTV injection of reprogramming pDNA. Moreover, the expression of some hepatocyte-specific markers was downregulated in reprogrammed tissues, which further indicated transient de-differentiation and loss of the specific cell phenotype [37]. Importantly, cells directly isolated from in vivo reprogrammed livers demonstrated potential to re-differentiate towards all three embryonic lineages when injected in the dorsal flank of immunocompromised mice. In such an environment, they generated teratomas [42, 43]. Since no ex vivo manipulations or exposure to LIF or other molecules that could favor the pluripotent conversion were used prior to implantation, this study confirmed that the pluripotent conversion took place within the tissue, and that the microenvironment of adult mammalian tissues is indeed permissive to epigenetic reprogramming to pluripotency. On the contrary, no teratomas were observed in the liver or any other organs of reprogrammed mice, monitored for a period of up to 120 days [37]. Similarly to what was observed in the tadpole, the expression of reprogramming factors and pluripotency markers was only detected for a few days, after which their levels reached again those observed in the control non-reprogrammed group, and the distinct clusters of pluripotent-like cells in the tissue were observed only up to day 4 after HTV administration. It is therefore possible that pluripotency is achieved in vivo via OSKM overexpression, but not maintained unless the reprogrammed cells are removed from their native microenvironment. The interactions between reprogramming and different pro-differentiation signals present in different tissues, those which the reprogrammed cells originally belonged to or not, are of great interest to further investigate in vivo reprogramming. However, given the very infant stage of the field at the moment, such interactions are still largely unexplored.
Proof-of-principle of in vivo reprogramming to pluripotency in an adult mammalian tissue (mouse liver). (a) HTV injection of reprogramming pDNA encoding OSKM transcription factors generated clusters of reprogrammed cells within the liver tissue, which expressed pluripotency markers and showed signs of hepatocyte de-differentiation, but which did not persist in the tissues for prolonged periods of time [37]. (b) Direct injection of cell suspensions extracted from in vivo reprogrammed mouse livers in the dorsal flak of nude mice generated teratomas, which confirmed the presence of cells with pluripotent potential within the reprogrammed tissue [37]. (c) In vivo induced pluripotent stem (i2PS) cells were extracted from reprogrammed livers and maintained in culture. Several studies confirmed bona fide pluripotency, among them: in vitro spontaneous differentiation towards the three embryonic lineages, teratoma assay and generation of chimeric mice via blastocyst injection [43]
Cells directly reprogrammed in the mouse liver can also be isolated and established in culture. When maintained under standard ESC culture conditions, they form dome-shaped compact colonies with very prominent nuclei that morphologically resemble ESC and in vitro generated iPS cells colonies. They are termed in vivo induced iPS cells (i2PS cells) in reference to their direct generation in the living organism and to distinguish them from their in vitro generated counterparts [43]. Such colonies express endogenous pluripotency markers and show high AP activity, both considered hallmarks of pluripotency. In addition, they spontaneously differentiate into cell types representative of all three germ layers when pro-pluripotency conditions (i.e. LIF supplement) are withdrawn. Their pluripotent potential has been further confirmed by the teratoma assay and the contribution to all adult tissues in chimeric mice generated via blastocyst injection. Overall, such studies proved that i2PS cells are bona fide pluripotent stem cells.
5.3 The “Reprogrammable Mouse” a Tool for the Study of In Vivo Reprogramming to Pluripotency
Delivery of reprogramming factors to target cells is one of the limiting steps that compromise the efficiency of reprogramming to pluripotency. In vitro, an extensive list of viral vectors including retrovirus [19], lentivirus [44], inducible lentivirus [45], excisable lentivirus [46], adenovirus [47] and Sendai virus [48] has been explored to optimize the induction of pluripotency. Non-viral vectors and vector-free methods such as cell electroporation have also been utilized to deliver not only reprogramming DNA in several forms [49, 50] but also mRNA [51], microRNA [52] and proteins [53].
In vivo, the delivery challenge is even more daunting considering the additional biological barriers that vectors have to overcome to reach the appropriate target, and the presence of a variety of enzymes in biological fluids that can trigger degradation of the cargo. Naked pDNA has been used when the administration method allows relatively high uptake in the target tissue, as it is the case of liver transfection via HTV injection [37, 38]. Direct pDNA injection has also been used to reprogram tissues known to be naturally permissive to the uptake of the nucleic acid, such as skeletal muscle [36, 54]. To target other organs that do not allow such a phenomena—for example, the brain cortex—retroviral vectors have been used [55].
In spite of the examples above, the issue of delivery remains one of the main obstacles for the induction of pluripotency in vivo. In light of such complications, and to be able to separate the impact of inefficient delivery from the intrinsic poor efficiency and stochastic character of the reprogramming process, various proof-of-principle studies have relied on the use of genetically engineered mice that contain OSKM reprogramming factors inserted in the genome to induce pluripotency in vivo [56,57,58,59,60,61,62].
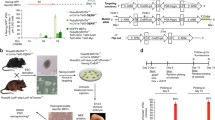
Different approaches have been followed to engineer so-called “reprogrammable mice”, including secondary systems through generation of iPS cells with integrating viral vectors [63] and direct insertion of the OSKM cassette in ESCs [64]. Wernig et al. first constructed a secondary system based on the infection of MEFs, which contained the reverse tetracycline-dependent transactivator M2rtTA in the ubiquitously expressed Rosa26 locus (Rosa26-M2rtTA MEFs), with four integrating lentiviruses encoding each of the OSKM factors under the control of a doxycycline-inducible promoter (tetOP) [63]. Addition of the drug to the culture medium generated iPS cells that contained OSKM factors inserted in the genome and were subsequently used to generate reprogrammable mice via blastocyst injection. In a different strategy, Stadtfeld et al. utilized gene targeting mediated by Flp recombinase to avoid the complications associated with secondary systems [64]. A doxycycline-inducible polycistronic OSKM cassette was placed in the 3′ untranslated region of the collagen type I, alpha 1 gene (Col1a1) in Rosa26-M2rtTA ESCs that were, similarly to the previous approach, used to generate chimeric reprogrammable mice. Both strategies are illustrated in Fig. 5.4.
Genetic engineering strategies to generate reprogrammable mice. In vitro and in vivo applications. Different genetic engineering strategies have been used to build reprogrammable mice with OSKM transgenes inserted in their genome. (a) MEFs expressing the tetracycline-depended transactivator in M2rtTA in the ubiquitously expressed Rosa26 locus (Rosa26-M2rtTA MEFs) were infected with fours lentivirus vectors expressing each of the OSKM transgenes under the control of a doxycycline-inducible (tetOP) promoter. Primary iPS cells obtained upon doxycycline (Dox) supplementation were used to generate chimeric mice via blastocyst injection, termed “reprogrammable mice” [63]. (b) Gene targeting via Flp recombinase was used to insert a polycistronic OSKM cassette under the control of a doxycycline-inducible promoter (tetOP) in the collagen type I, alpha 1 gene (Col1A1) in ESCs that expressed an optimized tetracycline-dependent transactivator in the ubiquitously expressed Rosa26 locus (Rosa26-M2rtTA ESCs)). Reprogrammable mice were generated via the injection of such genetically engineered cells in donor blastocysts [64]. Embryonic and somatic cells extracted from both reprogrammable mouse models generate iPS cells upon the addition of doxycycline in the culture medium. (c) Reprogrammable mice can also be used to induce adult cells to pluripotency within the adult organism upon systemic or localized administration of doxycycline [56, 61]
The reprogrammable mouse is an excellent source of “reprogrammable cells” for in vitro studies. Not only MEFs, but also somatic cells obtained from adult reprogrammable mice, can be reprogrammed to pluripotency in the culture dish when doxycycline is added to the culture medium. In addition, the OSKM cassette can also be induced in vivo with the administration of the drug (Fig. 5.4c). Doxycycline administration in drinking water induces widespread OSKM expression, since the transgenes are ubiquitously inserted in the genomes of all cells [56]. Targeted expression of reprogramming factors in specific tissues can also be achieved via localized doxycycline administration, for example by intramuscular administration [61].
The advantages brought by this model are numerous. First, it avoids the need to use viral or other delivery vectors, and with that it circumvents the problems associated with poor and heterogeneous OSKM delivery and ensures efficient reprogramming. In addition, genetic homogeneity of the reprogrammed cells is also higher in terms of number and location of transgene integrations. This allows direct comparison of the reprogramming process, its mechanisms and efficiency in different tissues and cell types of different developmental origin and maturation status; also thanks to the fact that the OSKM transgenes are ubiquitously present in all cells throughout the organism. In fact, induction of OSKM expression in the reprogrammable mouse highlighted that certain tissues are more resilient to reprogramming than others. In the skeletal muscle, OSKM expression was not enough to induce the generation of teratomas at doxycycline doses that efficiently formed such tissue aberrations in stomach, intestine and pancreas [60].
In addition, the doxycycline-inducible promoter (tetO) driving OSKM expression in the reprogrammable mouse model is an excellent tool to customize the pattern of expression of the factors. Their expression can be easily switched on an off at different times via administration or withdrawal of the drug. Thanks to this inducible system, the impact that the duration of OSKM expression has on the extent of reprogramming (partial vs complete reprogramming to pluripotency) and on the overall fate of in vivo reprogrammed cells in the tissues has been elucidated [65]. Full understanding of this relationship is key to ensure the safety of in vivo reprogramming to pluripotency and facilitate the path towards potential clinical applications, and therefore it will be further dissected in Chap. 6 of this book.
5.4 Downstream Effects of OSKM Expression in the Reprogrammed Tissue Microenvironment
In vivo overexpression of OSKM factors generates cells with pluripotency features within reprogrammed tissues, as demonstrated in proof-of-principle studies described in Sect. 5.2 of this Chapter [36, 37]. However, this is not the only downstream effect that OSKM induction triggers in the cells that express the factors and in those in the surrounding tissue.
5.4.1 In Vivo Reprogramming to Pluripotency and Tumorigenesis
The proliferative nature of pluripotent stem cells and their potential to differentiate into cell types from all three embryonic lineages are often regarded as excellent features that offer opportunities in stem cell research and regenerative medicine. However, such capabilities can also compromise the safety of in vivo reprogramming to pluripotency if excessive proliferation and uncontrolled re-differentiation take place in the living organism. Indeed, in vivo OSKM overexpression can lead to the generation of dysplastic lesions and teratomas within reprogrammed tissues [56].
Teratomas are defined as tumors that originate from the uncontrolled expansion and random differentiation of pluripotent cells and that are therefore composed of tissue types representing all three germ layers [66]. Abad et al. reported the occurrence of such tissue abnormalities following ubiquitous induction of OSKM expression in the reprogrammable mouse model [56]. Administration of doxycycline in the drinking water induced reprogramming of a variety of cell types, from hematopoietic and non-hematopoietic lineages, across different tissues. Reprograming and de-differentiation were confirmed by expression of the pluripotency marker NANOG, which was found concomitantly with loss of specific cell type markers. However, OSKM overexpression also led to the appearance of tumor masses, the majority of which were classified as teratomas that contained NANOG+ reprogrammed cells.
Indeed, the process of reprogramming to pluripotency shares various common events with the early stages of tumorigenesis. Those include the acquisition of self-renewal properties, loss of cell differentiation status and re-expression of genes typically enriched in embryonic developmental stages [67], as well as metabolic changes in the cell that involve significant upregulation of glycolytic pathways [68]. Similar telomere changes have also been observed during reprogramming and the onset of tumorigenesis, which indeed support the acquisition of self-renewal properties. Telomeres are short repetitive DNA sequences at the end of the chromosomes that protect them from degradation but are shortened through cell division [69]. Therefore, telomere length determines the lifespan of a cell. Increased activity of telomerase—the enzyme in charge of telomere elongation and normally only active during embryonic development and in adult stem cell compartments—is one of the hallmarks of tumorigenesis, and leads to immortalization of the cancerous cells [70]. During reprogramming, telomere elongation is a mandatory step to achieve bona fide pluripotency and it also determines the efficiency of reprogramming [71]. Although this was initially observed in vitro, it is now known that cells within in vivo reprogrammed areas have longer telomeres that those in non-reprogrammed tissues and show high telomerase activity [62].
Similarities between common types of tumors and those generated upon OSKM overexpression in the respective organ have also been reported. Kidney tumors in reprogrammable mice shared common histological, gene expression and DNA methylation features with Wilms tumor, a common pediatric kidney tumor [57]. While such observation adds to the list of shared features between induced reprogramming to pluripotency and tumorigenesis, it should be considered with care since the genetically modified nature of reprogrammable mice prevents any clinical relevance.
Generation of teratomas following OSKM overexpression has been reported in a number of studies [56, 57, 59, 62, 60], not all of which made use of the reprogrammable mouse model [55]. However, other studies have demonstrated that reprogramming can be induced in the absence of tumorigenesis and therefore the causal relationship between in vivo OSKM overexpression and teratoma formation should not be interpreted as general [37, 61, 54]. The main determinants that trigger or prevent teratoma formation are discussed in Chap. 6 of this book.
5.4.2 In Vivo Reprogramming to Pluripotency, Tissue Damage and Cellular Senescence
In addition to telomere shortening, reprogramming via OSKM overexpression is able to reverse various other hallmarks of ageing, including increased expression of aged-related stress response genes, double-stranded DNA breaks, mitochondrial dysfunction and abnormal architecture of the nuclear envelope. In fact, complete reprogramming to pluripotency is not necessary to attain such cell “rejuvenation”, which can be achieved with partial reprogramming [61]. However, the relationship between cell reprogramming and cellular senescence is much more intricate, especially at the tissue level.
While reprogrammed cells are “molecularly rejuvenated”, in vivo expression of OSKM factors induces senescence in surrounding cells within the tissue, which secrete senescence-related cytokines [59]. Interestingly, the presence of such senescence signals, of which IL-6 is the main player, renders the tissue microenvironment more permissive to the induction of reprogramming [59, 60]. Indeed, the efficiency of in vivo reprogramming has proven to increase in a variety of scenarios, including the administration of pharmacological agents that promote senescence [59], physiological ageing [59], progeria (a condition of extremely premature ageing) [59] and tissue injury [59, 60], all of which share cellular senescence as a common factor.
Therefore, the cross-talk between senescence and reprogramming seems to be beneficial for the latter, which could be of great interest to develop in vivo reprogramming strategies for tissue regeneration.
5.5 Conclusions
Proof-of-principle studies in a developing amniote and an adult, fully developed, mammalian model have demonstrated that specific reprogramming transcription factors are indeed able to induce pluripotency features in vivo, even in the presence of pro-differentiation signals in the tissue microenvironment. However, it is also clear from these and other studies that forced expression of such genes triggers additional downstream effects in in vivo reprogrammed cells and their surrounding tissue. While confirmation that pluripotent cells can be generated in vivo envisions a plethora of potential applications in regenerative medicine, knowledge on the links between reprogramming, tumorigenesis and cellular senescence, among other events, is still limited and warrants further investigation.
References
Brunt KR, Weisel RD, Li RK. Stem cells and regenerative medicine - future perspectives. Can J Physiol Pharmacol. 2012;90(3):327–35. doi:10.1139/y2012-007.
Ilic D, Polak JM. Stem cells in regenerative medicine: introduction. Br Med Bull. 2011;98:117–26. doi:10.1093/bmb/ldr012.
Martin GR. Isolation of a pluripotent cell line from early mouse embryos cultured in medium conditioned by teratocarcinoma stem cells. Proc Natl Acad Sci U S A. 1981;78(12):7634–8.
Evans MJ, Kaufman MH. Establishment in culture of pluripotential cells from mouse embryos. Nature. 1981;292(5819):154–6.
Thomson JA, Itskovitz-Eldor J, Shapiro SS, Waknitz MA, Swiergiel JJ, Marshall VS, Jones JM. Embryonic stem cell lines derived from human blastocysts. Science. 1998;282(5391):1145–7.
Nichols J, Evans EP, Smith AG. Establishment of germ-line-competent embryonic stem (ES) cells using differentiation inhibiting activity. Development. 1990;110(4):1341–8.
Evans MD, Kelley J. US attitudes toward human embryonic stem cell research. Nat Biotechnol. 2011;29(6):484–8. doi:10.1038/nbt.1891.
Wilmut I. Consternation and confusion following EU patent judgment. Cell Stem Cell. 2011;9(6):498–9. doi:10.1016/j.stem.2011.11.002.
Gurdon JB. The developmental capacity of nuclei taken from differentiating endoderm cells of Xenopus laevis. J Embryol Exp Morphol. 1960;8:505–26.
Gurdon JB. The developmental capacity of nuclei taken from intestinal epithelium cells of feeding tadpoles. J Embryol Exp Morphol. 1962;10:622–40.
Gurdon JB, Laskey RA, Reeves OR. The developmental capacity of nuclei transplanted from keratinized skin cells of adult frogs. J Embryol Exp Morphol. 1975;34(1):93–112.
Davis RL, Weintraub H, Lassar AB. Expression of a single transfected cDNA converts fibroblasts to myoblasts. Cell. 1987;51(6):987–1000. doi:10.1016/0092-8674(87)90585-x.
Weintraub H, Tapscott SJ, Davis RL, Thayer MJ, Adam MA, Lassar AB, Miller AD. Activation of muscle-specific genes in pigment, nerve, fat, liver, and fibroblast cell lines by forced expression of MyoD. Proc Natl Acad Sci U S A. 1989;86(14):5434–8.
Briggs R, King TJ. Transplantation of living nuclei from blastula cells into enucleated frogs’ eggs. Proc Natl Acad Sci U S A. 1952;38(5):455–63.
Wilmut I, Schnieke AE, McWhir J, Kind AJ, Campbell KH. Viable offspring derived from fetal and adult mammalian cells. Nature. 1997;385(6619):810–3. doi:10.1038/385810a0.
Miller RA, Ruddle FH. Pluripotent teratocarcinoma-thymus somatic cell hybrids. Cell. 1976;9(1):45–55. doi:10.1016/0092-8674(76)90051-9.
Egli D, Chen AE, Saphier G, Ichida J, Fitzgerald C, Go KJ, Acevedo N, Patel J, Baetscher M, Kearns WG, Goland R, Leibel RL, Melton DA, Eggan K. Reprogramming within hours following nuclear transfer into mouse but not human zygotes. Nat Commun. 2011;2:488. doi:10.1038/ncomms1503.
Noggle S, Fung HL, Gore A, Martinez H, Satriani KC, Prosser R, Oum K, Paull D, Druckenmiller S, Freeby M, Greenberg E, Zhang K, Goland R, Sauer MV, Leibel RL, Egli D. Human oocytes reprogram somatic cells to a pluripotent state. Nature. 2011;478(7367):70–5. doi:10.1038/nature10397.
Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006;126(4):663–76. doi:10.1016/j.cell.2006.07.024.
Okita K, Ichisaka T, Yamanaka S. Generation of germline-competent induced pluripotent stem cells. Nature. 2007;448(7151):313–7. doi:10.1038/nature05934.
Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T, Tomoda K, Yamanaka S. Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell. 2007;131(5):861–72. doi:10.1016/j.cell.2007.11.019.
Yu J, Vodyanik MA, Smuga-Otto K, Antosiewicz-Bourget J, Frane JL, Tian S, Nie J, Jonsdottir GA, Ruotti V, Stewart R, Slukvin II, Thomson JA. Induced pluripotent stem cell lines derived from human somatic cells. Science. 2007;318(5858):1917–20. doi:10.1126/science.1151526.
Polo Jose M, Anderssen E, Walsh Ryan M, Schwarz Benjamin A, Nefzger Christian M, Lim Sue M, Borkent M, Apostolou E, Alaei S, Cloutier J, Bar-Nur O, Cheloufi S, Stadtfeld M, Figueroa Maria E, Robinton D, Natesan S, Melnick A, Zhu J, Ramaswamy S, Hochedlinger K. A molecular roadmap of reprogramming somatic cells into iPS cells. Cell. 2012;151(7):1617–32. doi:10.1016/j.cell.2012.11.039.
Buganim Y, Faddah DA, Jaenisch R. Mechanisms and models of somatic cell reprogramming. Nat Rev Genet. 2013;14(6):427–39. doi:10.1038/nrg3473.
Aoi T, Yae K, Nakagawa M, Ichisaka T, Okita K, Takahashi K, Chiba T, Yamanaka S. Generation of pluripotent stem cells from adult mouse liver and stomach cells. Science. 2008;321(5889):699–702. doi:10.1126/science.1154884.
Loh YH, Agarwal S, Park IH, Urbach A, Huo H, Heffner GC, Kim K, Miller JD, Ng K, Daley GQ. Generation of induced pluripotent stem cells from human blood. Blood. 2009;113(22):5476–9. doi:10.1182/blood-2009-02-204800.
Ruiz S, Brennand K, Panopoulos AD, Herrerias A, Gage FH, Izpisua-Belmonte JC. High-efficient generation of induced pluripotent stem cells from human astrocytes. PLoS One. 2010;5(12):e15526. doi:10.1371/journal.pone.0015526.
Lowry WE, Richter L, Yachechko R, Pyle AD, Tchieu J, Sridharan R, Clark AT, Plath K. Generation of human induced pluripotent stem cells from dermal fibroblasts. Proc Natl Acad Sci U S A. 2008;105(8):2883–8. doi:10.1073/pnas.0711983105.
Staerk J, Dawlaty MM, Gao Q, Maetzel D, Hanna J, Sommer CA, Mostoslavsky G, Jaenisch R. Reprogramming of human peripheral blood cells to induced pluripotent stem cells. Cell Stem Cell. 2010;7(1):20–4. doi:10.1016/j.stem.2010.06.002.
Bellin M, Marchetto MC, Gage FH, Mummery CL. Induced pluripotent stem cells: the new patient? Nat Rev Mol Cell Biol. 2012;13(11):713–26. doi:10.1038/nrm3448.
de Lazaro I, Yilmazer A, Kostarelos K. Induced pluripotent stem (iPS) cells: a new source for cell-based therapeutics? J Control Release. 2014;185:37–44. doi:10.1016/j.jconrel.2014.04.011.
Silva J, Barrandon O, Nichols J, Kawaguchi J, Theunissen TW, Smith A. Promotion of reprogramming to ground state pluripotency by signal inhibition. PLoS Biol. 2008;6(10):2237–47. doi:10.1371/journal.pbio.0060253.
Kawai H, Yamashita T, Ohta Y, Deguchi K, Nagotani S, Zhang X, Ikeda Y, Matsuura T, Abe K. Tridermal tumorigenesis of induced pluripotent stem cells transplanted in ischemic brain. J Cereb Blood Flow Metab. 2010;30(8):1487–93. doi:10.1038/jcbfm.2010.32.
Ben-David U, Benvenisty N. The tumorigenicity of human embryonic and induced pluripotent stem cells. Nat Rev Cancer. 2011;11(4):268–77. doi:10.1038/nrc3034.
Hentze H, Soong PL, Wang ST, Phillips BW, Putti TC, Dunn NR. Teratoma formation by human embryonic stem cells: evaluation of essential parameters for future safety studies. Stem Cell Res. 2009;2(3):198–210. doi:10.1016/j.scr.2009.02.002.
Vivien C, Scerbo P, Girardot F, Le Blay K, Demeneix BA, Coen L. Non-viral expression of mouse Oct4, Sox2, and Klf4 transcription factors efficiently reprograms tadpole muscle fibers in vivo. J Biol Chem. 2012;287(10):7427–35. doi:10.1074/jbc.M111.324368.
Yilmazer A, de Lazaro I, Bussy C, Kostarelos K. In vivo cell reprogramming towards pluripotency by virus-free overexpression of defined factors. PLoS One. 2013;8(1):e54754. doi:10.1371/journal.pone.0054754.
Yilmazer A, de Lazaro I, Bussy C, Kostarelos K. In vivo reprogramming of adult somatic cells to pluripotency by overexpression of Yamanaka factors. J Vis Exp. 2013;17(82):e50837.
Liu F, Song Y, Liu D. Hydrodynamics-based transfection in animals by systemic administration of plasmid DNA. Gene Ther. 1999;6(7):1258–66. doi:10.1038/sj.gt.3300947.
Andrianaivo F, Lecocq M, Wattiaux-De Coninck S, Wattiaux R, Jadot M. Hydrodynamics-based transfection of the liver: entrance into hepatocytes of DNA that causes expression takes place very early after injection. J Gene Med. 2004;6(8):877–83. doi:10.1002/jgm.574.
Sebestyen MG, Budker VG, Budker T, Subbotin VM, Zhang G, Monahan SD, Lewis DL, Wong SC, Hagstrom JE, Wolff JA. Mechanism of plasmid delivery by hydrodynamic tail vein injection. I. Hepatocyte uptake of various molecules. J Gene Med. 2006;8(7):852–73. doi:10.1002/jgm.921.
Banga A, Akinci E, Greder LV, Dutton JR, Slack JMW. In vivo reprogramming of Sox9+ cells in the liver to insulin-secreting ducts. Proc Natl Acad Sci U S A. 2012;109(38):15336–41. doi:10.1073/pnas.1201701109.
de Lazaro I, Bussy C, Yilmazer A, Jackson MS, Humphreys NE, Kostarelos K. Generation of induced pluripotent stem cells from virus-free in vivo reprogramming of BALB/c mouse liver cells. Biomaterials. 2014;35(29):8312–20. doi:10.1016/j.biomaterials.2014.05.086.
Sommer CA, Stadtfeld M, Murphy GJ, Hochedlinger K, Kotton DN, Mostoslavsky G. Induced pluripotent stem cell generation using a single lentiviral stem cell cassette. Stem Cells. 2009;27(3):543–9. doi:10.1634/stemcells.2008-1075.
Hamilton B, Feng Q, Ye M, Welstead GG. Generation of induced pluripotent stem cells by reprogramming mouse embryonic fibroblasts with a four transcription factor, doxycycline inducible lentiviral transduction system. J Vis Exp. 2009;33:1447. https://doi.org/10.3791/1447.
Sommer CA, Sommer AG, Longmire TA, Christodoulou C, Thomas DD, Gostissa M, Alt FW, Murphy GJ, Kotton DN, Mostoslavsky G. Excision of reprogramming transgenes improves the differentiation potential of iPS cells generated with a single excisable vector. Stem Cells. 2010;28(1):64–74. doi:10.1002/stem.255.
Tashiro K. Optimization of adenovirus vectors for transduction in embryonic stem cells and induced pluripotent stem cells. Yakugaku Zasshi. 2011;131(9):1333–8. doi:10.1248/yakushi.131.1333.
Fusaki N, Ban H, Nishiyama A, Saeki K, Hasegawa M. Efficient induction of transgene-free human pluripotent stem cells using a vector based on Sendai virus, an RNA virus that does not integrate into the host genome. Proc Jpn Acad Ser B Phys Biol Sci. 2009;85(8):348–62. doi:10.2183/pjab.85.348.
Okita K, Nakagawa M, Hyenjong H, Ichisaka T, Yamanaka S. Generation of mouse induced pluripotent stem cells without viral vectors. Science. 2008;322(5903):949–53. doi:10.1126/science.1164270.
Davis RP, Nemes C, Varga E, Freund C, Kosmidis G, Gkatzis K, de Jong D, Szuhai K, Dinnyes A, Mummery CL. Generation of induced pluripotent stem cells from human foetal fibroblasts using the sleeping beauty transposon gene delivery system. Differentiation. 2013;86(1-2):30–7. doi:10.1016/j.diff.2013.06.002.
Plews JR, Li J, Jones M, Moore HD, Mason C, Andrews PW, Na J. Activation of pluripotency genes in human fibroblast cells by a novel mRNA based approach. PLoS One. 2010;5(12):e14397. doi:10.1371/journal.pone.0014397.
Anokye-Danso F, Trivedi CM, Juhr D, Gupta M, Cui Z, Tian Y, Zhang Y, Yang W, Gruber PJ, Epstein JA, Morrisey EE. Highly efficient miRNA-mediated reprogramming of mouse and human somatic cells to pluripotency. Cell Stem Cell. 2011;8(4):376–88. doi:10.1016/j.stem.2011.03.001.
Kim D, Kim CH, Moon JI, Chung YG, Chang MY, Han BS, Ko S, Yang E, Cha KY, Lanza R, Kim KS. Generation of human induced pluripotent stem cells by direct delivery of reprogramming proteins. Cell Stem Cell. 2009;4(6):472–6. doi:10.1016/j.stem.2009.05.005.
de Lazaro I, Yilmazer A, Nam Y, Qubisi S, Razak F, Cossu G, Kostarelos K. Non-viral induction of transient cell reprogramming in skeletal muscle to enhance tissue regeneration. bioRxiv. 2017. doi:10.1101/101188.
Gao X, Wang X, Xiong W, Chen J. In vivo reprogramming reactive glia into iPSCs to produce new neurons in the cortex following traumatic brain injury. Sci Rep. 2016;6:22490. doi:10.1038/srep22490.
Abad M, Mosteiro L, Pantoja C, Canamero M, Rayon T, Ors I, Grana O, Megias D, Dominguez O, Martinez D, Manzanares M, Ortega S, Serrano M. Reprogramming in vivo produces teratomas and iPS cells with totipotency features. Nature. 2013;502:340–5. doi:10.1038/nature12586.
Ohnishi K, Semi K, Yamamoto T, Shimizu M, Tanaka A, Mitsunaga K, Okita K, Osafune K, Arioka Y, Maeda T, Soejima H, Moriwaki H, Yamanaka S, Woltjen K, Yamada Y. Premature termination of reprogramming in vivo leads to cancer development through altered epigenetic regulation. Cell. 2014;156(4):663–77. doi:10.1016/j.cell.2014.01.005.
Choi HW, Kim JS, Hong YJ, Song H, Seo HG, Do JT. In vivo reprogrammed pluripotent stem cells from teratomas share analogous properties with their in vitro counterparts. Sci Rep. 2015;5:13559. doi:10.1038/srep13559.
Mosteiro L, Pantoja C, Alcazar N, Marion RM, Chondronasiou D, Rovira M, Fernandez-Marcos PJ, Munoz-Martin M, Blanco-Aparicio C, Pastor J, Gomez-Lopez G, De Martino A, Blasco MA, Abad M, Serrano M. Tissue damage and senescence provide critical signals for cellular reprogramming in vivo. Science. 2016;354(6315):aaf4445. doi:10.1126/science.aaf4445.
Chiche A, Le Roux I, von Joest M, Sakai H, Aguin SB, Cazin C, Salam R, Fiette L, Alegria O, Flamant P, Tajbakhsh S, Li H. Injury-induced senescence enables in vivo reprogramming in skeletal muscle. Cell Stem Cell. 2017;20:407. doi:10.1016/j.stem.2016.11.020.
Ocampo A, Reddy P, Martinez-Redondo P, Platero-Luengo A, Hatanaka F, Hishida T, Li M, Lam D, Kurita M, Beyret E, Araoka T, Vazquez-Ferrer E, Donoso D, Roman JL, Xu J, Rodriguez Esteban C, Nunez G, Nunez Delicado E, Campistol JM, Guillen I, Guillen P, Izpisua Belmonte JC. In vivo amelioration of age-associated hallmarks by partial reprogramming. Cell. 2016;167(7):1719–1733.e12. doi:10.1016/j.cell.2016.11.052.
Marion RM, Lopez de Silanes I, Mosteiro L, Gamache B, Abad M, Guerra C, Megias D, Serrano M, Blasco MA. Common telomere changes during in vivo reprogramming and early stages of tumorigenesis. Stem Cell Rep. 2017;8(2):460–75. doi:10.1016/j.stemcr.2017.01.001.
Wernig M, Lengner CJ, Hanna J, Lodato MA, Steine E, Foreman R, Staerk J, Markoulaki S, Jaenisch R. A drug-inducible transgenic system for direct reprogramming of multiple somatic cell types. Nat Biotechnol. 2008;26(8):916–24. doi:10.1038/nbt1483.
Stadtfeld M, Maherali N, Borkent M, Hochedlinger K. A reprogrammable mouse strain from gene-targeted embryonic stem cells. Nat Methods. 2010;7(1):53–5. doi:10.1038/nmeth.1409.
de Lazaro I, Cossu G, Kostarelos K. Transient transcription factor (OSKM) expression is key towards clinical translation of in vivo cell reprogramming. EMBO Mol Med. 2017;9:733. doi:10.15252/emmm.201707650.
Stevens LC, Little CC. Spontaneous testicular teratomas in an inbred strain of mice. Proc Natl Acad Sci U S A. 1954;40(11):1080–7.
Ben-Porath I, Thomson MW, Carey VJ, Ge R, Bell GW, Regev A, Weinberg RA. An embryonic stem cell-like gene expression signature in poorly differentiated aggressive human tumors. Nat Genet. 2008;40(5):499–507. doi:10.1038/ng.127.
Folmes CD, Nelson TJ, Martinez-Fernandez A, Arrell DK, Lindor JZ, Dzeja PP, Ikeda Y, Perez-Terzic C, Terzic A. Somatic oxidative bioenergetics transitions into pluripotency-dependent glycolysis to facilitate nuclear reprogramming. Cell Metab. 2011;14(2):264–71. doi:10.1016/j.cmet.2011.06.011.
Blackburn EH, Gall JG. A tandemly repeated sequence at the termini of the extrachromosomal ribosomal RNA genes in tetrahymena. J Mol Biol. 1978;120(1):33–53. doi:10.1016/0022-2836(78)90294-2.
Martinez P, Blasco MA. Telomeric and extra-telomeric roles for telomerase and the telomere-binding proteins. Nat Rev Cancer. 2011;11(3):161–76. doi:10.1038/nrc3025.
Marion RM, Strati K, Li H, Tejera A, Schoeftner S, Ortega S, Serrano M, Blasco MA. Telomeres acquire embryonic stem cell characteristics in induced pluripotent stem cells. Cell Stem Cell. 2009;4(2):141–54. doi:10.1016/j.stem.2008.12.010.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
de Lázaro, I. (2017). In Vivo Cell Reprogramming to Pluripotency. In: Yilmazer, A. (eds) In Vivo Reprogramming in Regenerative Medicine. Stem Cell Biology and Regenerative Medicine. Humana Press, Cham. https://doi.org/10.1007/978-3-319-65720-2_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-65720-2_5
Published:
Publisher Name: Humana Press, Cham
Print ISBN: 978-3-319-65719-6
Online ISBN: 978-3-319-65720-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)