Abstract
Neuroendocrine prostate cancer (NEPC) is an androgen receptor (AR)-negative variant that most commonly arises from treated adenocarcinoma of the prostate. NEPC does not respond to AR-directed therapy and has only transient response to chemotherapy. It is estimated that up to 30% of late-stage prostate cancers harbor a predominance of neuroendocrine differentiation. However, due to a general lack of biopsy diagnoses for advanced disease, this may underrepresent the frequency of NEPC. The prognosis is poor due to late recognition, heterogeneous clinical features, and lack of effective therapy. Chemotherapy used for other small cell neuroendocrine cancers is the mainstay of treatment; however, more targeted approaches are being developed based on an emerging understanding of this aggressive form of prostate cancer. This chapter provides an in-depth overview of most recent genomic alterations of this lethal subtype of the disease.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Neuroendocrine prostate cancer (NEPC ) is the clinical term used for advanced prostate cancer with clinical features of small cell neuroendocrine carcinoma. It is also referred to as anaplastic prostate cancer or small cell carcinoma of prostate, an aggressive clinical variant that can arise de novo in pure form or more commonly after hormonal therapy for usual prostatic adenocarcinoma. Incidence rate of this cancer subtype is estimated to be 0.35 cases per million per year, and more than 50% of the patients with NEPC have distant metastasis at the time disease presentation [1]. In the Surveillance, Epidemiology, and End Results (SEER) database on 3,830,355 patients diagnosed with prostatic adenocarcinoma from 1973 to 2008, approximately 10% of distant metastatic patients were diagnosed as NEPC [1]. This frequency can be much higher because of lack of diagnostic biopsy on metastatic sites and also due to increased use of androgen deprivation therapy (ADT) for treatment of advanced prostate cancer, which predisposes to neuroendocrine differentiation [2]. Moreover, age-adjusted incidence of NEPC still continues to rise as per recent statistics [3].
NEPC has poor prognosis. It is suspected in patients with treated prostatic cancer showing rapid progression of the disease with visceral metastasis, elevated neuroendocrine serum markers, AR expression loss, and no appreciable PSA elevation. Most patient have fatal outcome in very short duration.
Neuroendocrine Cells in the Normal Prostate
Normal adult prostate comprises of epithelial and stromal components. Epithelial components include secretory (luminal) cells , basal cells , and neuroendocrine (NE) cells . In addition, there are pluripotent stem cells, which cannot be seen on conventional histology section by light microscopy. NE cells are a normal component of prostate and are found in both glandular and duct epithelium, comprising less than 1% of benign prostatic cells. Periurethral and duct regions have the highest density of NE cells [4]. There are two types of NE cells, namely, open-type cells (in contact with lumen) and closed-type cells (not in contact with lumen). Open-type cells have long surface microvilli which connect with lumen and interact with luminal content, whereas closed-type cells rest on basal lamina and have dendritic like processes which extend to adjacent epithelial cells and receive stimuli from nerve endings and underlying stromal cells [5].
The precise function of NE cells in prostate is not fully understood, but they are thought to play a role in regulation, secretion, differentiation, and proliferation of secretory and basal cells. Ultrastructurally, NE cells of prostate contain large dense core secretory granules measuring 50–500 nm diameter, which are storage site for diverse neurosecretory peptides and hormones such as chromogranin A and B, neuron-specific enolase (NSE), serotonin, somatostatin, bombesin, histamine, calcitonin, and other members of calcitonin gene family of peptides [6,7,8,9,10]. In clinical and research setting, NE cells are detected by using markers such as chromogranin, synaptophysin, NSE, and CD56 and showing negative expression of PSA, Ki-67, and androgen receptor (AR). Thus, they appear to be non-proliferative differentiated and androgen-independent cells.
Neuroendocrine Differentiation in Prostate Carcinoma
It is estimated that 5–10% of localized prostatic cancer show focal neuroendocrine differentiation (NED ), and this differentiation proportionately increases with disease progression [11]. Acinar adenocarcinoma of prostate demonstrates NE cells by immunostains in highly variable number of cases, which depend upon number of slides studies and type of marker used [12]. Focal NED is still controversial with regard to its clinical meaning as different studies have shown conflicting data with regard to prognostic value of NED markers in surgically treated prostate cancer [13]. Acinar adenocarcinoma of prostate demonstrates NE cells by immunostains in highly variable number of cases, depending upon number of slides studies and type of marker used [12]. It is not recommended to routinely use immunostains to detect focal NED in typical early-stage prostatic adenocarcinoma [13, 14]. Focal NED cells may not be necessarily resembling normal NE cells but usually have same morphological appearance as that of usual adenocarcinoma [15]. Allelotyping of microdissected cells from prostatic carcinoma had shown NE cells and exocrine tumor cells from prostate to share identical allelic profiles and common origin [16]. This phenomenon along with other supported studies have led to the notion that adenocarcinoma cells have the capacity to transdifferentiate into NE cells and play role in tumor growth and progression. Support of a transdifferentiation model of NEPC and its clonal origin from prostate adenocarcinoma includes evidence that when prostate adenocarcinoma cells are exposed to various cytokines (IL6, IL8, heparin-binding EGF) or an androgen-depleted environment in cell culture, they are able to differentiate into neuroendocrine cells transiently and then revert back to their original phenotype when the inducer is removed [17]. Also, prostate adenocarcinoma cell lines (LNCaP) have also been shown to become “neuroendocrine like” when transfected with the gene that encodes the transcription factor (and oncogene) N-myc (MYCN), with upregulation of neuroendocrine markers and downregulation of androgen receptor and androgen-regulated genes occurring via direct binding of N-myc to promoters of synaptophysin (SYP), neuron-specific enolase (NSE), and AR [18]. As further support of a transdifferentiation model of NEPC and clonal origin from prostate adenocarcinoma, the frequency of the prostate cancer-specific ERG gene rearrangement is similar to that of prostate adenocarcinoma . Histologic evaluation of mixed tumors reveals that neuroendocrine and small cell areas and prostate adenocarcinoma can coexist and intermingle within the same tumor focus. Tumors that are ERG fusion-positive demonstrate rearrangement in both the neuroendocrine and adenocarcinoma foci (Fig. 19.1). Similarly, when ERG-positive gene fusion status of primary tumors is compared with that of local recurrences or metastases with neuroendocrine differentiation, rearrangement is present in both areas , i.e., acinar and neuroendocrine (Fig. 19.2).
Mixed small cell carcinoma and prostatic adenocarcinoma . H&E stain (left) shows a tumor with mixed small cell carcinoma and adenocarcinoma components. Immunohistochemistry (center) demonstrates that only adenocarcinoma cells are positive for AR and ERG, while ERG gene rearrangement by FISH (right) is present in both components (Reprinted with permission from Beltran H, Rickman DS, Park K, Chae SS, Sboner A, MacDonald TY, Wang Y, Sheikh KL, Terry S, Tagawa ST, et al.: Molecular characterization of neuroendocrine prostate cancer and identification of new drug targets. Cancer Discov 2011, 1:487–495)
ERG gene rearrangement and AURKA and MYCN amplification in prostate cancer. Left panel illustrates a needle biopsy from a patient with initial diagnosis of prostatic adenocarcinoma Gleason score 3 + 4 = 7 with amplification of AURKA (upper inset) but not MYCN (middle inset). Eight years after initial diagnosis and intermittent treatment, the patient developed pancytopenia and bone lytic lesions. The right panel shows a bone biopsy with metastatic small cell carcinoma (frozen tissue artifact present), consistent with spread from known prostatic primary. In addition to AURKA amplification (upper inset), clonal origin is confirmed by ERG rearrangement through translocation, also seen in his primary tumor (lower insets). The metastatic tumor demonstrates MYCN amplification (middle inset) (Reprinted from Neoplasia, Vol 15, Juan Miguel Mosquera et al., Concurrent AURKA and MYCN Gene Amplifications Are Harbingers of Lethal TreatmentRelated Neuroendocrine Prostate Cancer, p. 4, Copyright (2013), with permission from Elsevier)
De novo neuroendocrine prostate tumors are extremely rare cancers and composed of NE tumor cells without prior documentation of any known adenocarcinoma. Tumors that come under this category include carcinoid tumors of prostate, which have similar morphology to carcinoids at other anatomic sites, small cell carcinoma, and newly recognized entity large cell neuroendocrine carcinoma [19,20,21]. These tumors can present as pure form or admixed with variable component of prostatic adenocarcinoma.
The majority of studies on neuroendocrine tumors have shown that NE differentiation occur in hormone refractory prostate cancer after androgen deprivation study (ADT) [22,23,24,25]. It is considered to be the result of selective pressure caused by androgen deprivation as an escape route that enables adaptation in response to AR-targeted therapies [26,27,28]. Studies have shown that the NE component increases after a few months of introduction of ADT, and the diagnosis of castrate-resistant prostate carcinoma (CRPC) is made months or years after [22, 29, 30]. Androgen deprivation has been shown to activate epithelial mesenchymal transition (EMT) and neuroendocrine transdifferentiation, which are associated with resistance to treatment, tumor progression, distant metastasis, and aggressive behavior of the tumor [30]. Farach et al. recently showed that late stages of prostate cancer evolution involve neuronal transdifferentiation, which would enable cancer cells to acquire independence from the neural axis, critical in primary tumors [31]. It is estimated that at least a quarter of patients with late-stage disease and aggressively treated will develop NEPC, and incidence will rise with introduction of more potent antiandrogen agents [32, 33].
Classification of Primary Neuroendocrine Prostate Tumors
A recent updated classification of primary neuroendocrine tumors of prostate has been published in the WHO tumor classification of the urinary system (Table 19.1) [12].
Adenocarcinoma with neuroendocrine differentiation is the usual prostate adenocarcinoma with scattered neuroendocrine cells indistinguishable from typical adenocarcinoma cells on routine histology section. NE cells can be identified by immunohistochemistry with neuroendocrine markers such as chromogranin, synaptophysin, NSE, and CD56. These NE cells are seen in 10–100% of typical adenocarcinoma cases depending upon number of slides studies and type of marker used [12]. These NE cells have also been seen in intraepithelial lesion [34, 35]. Both high-grade and high-stage prostatic adenocarcinoma show increased neuroendocrine differentiation [22, 23, 36]. The effect of this NE differentiation on patient outcome is controversial, and routine use of IHC markers for NE differentiation is not recommended in surgical pathology reporting [12,13,14].
Adenocarcinoma with Paneth cell-like neuroendocrine differentiation is characterized by presence of brightly eosinophilic cytoplasmic granules in cytologically bland neuroendocrine cells with typical nuclear features such as “salt and pepper” chromatin and absence of nucleoli. This Paneth cell-like change has been recognized for many years [37]. These granules are positive for NE markers by immunohistochemistry [38, 39]. Paneth cell-like cells may be present in well-formed glands of Gleason pattern 6 or can be found in cords and solid sheets typically defined as Gleason pattern 4 or 5 [37, 39]. It is recommended that this Paneth cell-like pattern should be excluded while determining Gleason grade pattern. In some cases, Paneth cell-like change can be seen in adjacent cells which lack cytoplasmic granules in tumor cells with deeply amphophilic cytoplasm [40]. The cells of this Paneth cell variant morphologically lack prominent nucleoli of usual adenocarcinoma cells and are diffusely positive for NE immunostains and should be excluded from Gleason grading. There is a high frequency of AURKA amplification in localized prostatic carcinoma with Paneth cell-like change, which clinical significance warrants further investigation [41].
Well-differentiated neuroendocrine tumors (carcinoid tumor) of prostate are tumors analogous to carcinoid tumors in other sites such as lung. Pure carcinoid tumors of prostate are extremely rare. These should be diagnosed only when they originate from prostatic parenchyma, are not associated with concomitant adenocarcinoma, and must be positive for NE markers and negative for PSA [14]. Usual adenocarcinoma of prostate can express NE markers and can have bland cytological appearance, but the diagnosis of carcinoid should only be rendered if such tumors are not close to usual adenocarcinoma and are negative for PSA; otherwise they should be regarded as prostate adenocarcinoma with neuroendocrine differentiation. Several carcinoid-like prostate tumors appear to be variants of Paneth cell-like NE differentiation with paucity or absence of eosinophilic granules, in which PSA may be negative [42]. If such diagnosis of pure prostatic carcinoid is rendered, then grading should be done using mitotic rate and Ki-67 proliferation index as done with these tumors at other sites. These tumors may present with locally advanced disease, including some with pelvic lymph node metastasis, but in general, they still have favorable outcome.
Small cell neuroendocrine carcinoma of prostate is high-grade primary prostate tumor with cell morphology similar to small cell carcinoma of the lung, which includes high nuclear to cytoplasmic ratio, nuclear molding, lack of prominent nucleoli, crush artifact, geographic necrosis, apoptosis, and high mitotic rate (Fig. 19.3a). Pure small cell carcinoma of prostate at initial diagnosis is seen in 50–60% of cases, and the rest of them have a component of usual prostatic adenocarcinoma [43]. Transition between acinar and small cell component is abrupt, so it is quite easy to appreciate on routine histology (Fig. 19.3b, c). Morphological variations of small cell carcinoma include intermediate cell type with slightly more open chromatin and visible small nucleoli seen in 30–40% of the cases. Less common variation include presence of tumor giant cells and single file pattern [43]. Gleason grading is not done on the small cell component but in the acinar component, which shows Gleason score of >8 in 85% of the cases [43]. Classic morphology of small is quite distinct so routine use of immunostains is not necessary; approximately, 90% of the cases show immunopositivity for at least one NE marker [44, 45]. PSA and other prostate specific markers are focally positive in 17–25% of cases, usually cases in concomitant acinar component. Ki-67 labeling index is more than 50%. Positivity for p63 and HMWK is seen in 24 and 35% of cases, which are typically absent in usual adenocarcinoma [44]. TTF-1 is expressed in more than 50% of the cases, limiting its application in differentiating between primary small cell prostate carcinoma and metastasis from small cell carcinoma of the lung [43, 44, 46, 47]. Ancillary testing practical importance is the detection of prostate cancer-specific fusion between ETS family of genes and TMPRSS2, a common aberration found in small cell prostatic carcinoma (Fig. 19.3c) [48,49,50].
Histologic features of small cell carcinoma . (a) Classic histomorphology of small cell carcinoma includes tumor cells with hyperchromatic nuclei, nuclear molding, and “crush” artifact. (b) Mixed small cell carcinoma—acinar adenocarcinoma. (c) Although ERG immunostain highlights nuclei only in the adenocarcinoma component, a FISH assay for ERG (insets) demonstrates break apart signal in both small cell carcinoma and acinar adenocarcinoma areas of this tumor
Being an aggressive tumor, approximately 60% of patients have with distant metastasis at time of presentation and less often paraneoplastic syndromes such as those associated with ectopic adrenocorticotropic hormone, hypercalcemia, or inappropriate antidiuretic hormone production. Clinically localized small cell prostate cancer is treated aggressively with multimodal therapy including chemo- and radiation therapy, whereas metastatic small cell is treated with platinum-based combination chemotherapy [51,52,53]. A 2- and 5-year survival rate is 27.5% and 14.3%, respectively [54].
Large cell neuroendocrine carcinoma (LCNC) is a new entity added in prostate neuroendocrine tumors in the updated WHO 2016 classification. These are exceptionally rare high-grade tumors with cells in large nests with peripheral palisading, geographical necrosis, and cytologically resembling acinar high-grade adenocarcinoma (large cell size, abundant cytoplasm, prominent nucleoli, coarse clumpy chromatin) [55]. Neuroendocrine differentiation is supported by positivity of at least one NE marker (CD56, synaptophysin, or chromogranin) [14]. Ki-67 proliferation index is more than 50%. PSA and PSAP are either negative or focally positive in tumor areas. Pure or de novo large cell neuroendocrine tumors are exceptionally very rare tumors; the majority of cases reported are associated with prior prostate adenocarcinoma with long-standing history of hormonal therapy. For rendering diagnosis of this entity, both NE immunostains and morphological features should be considered. Most cases are associated with rapid progression, widespread dissemination, and eventually death due to metastatic disease [20, 55].
A recent proposed classification from a working committee to classify prostate cancer with neuroendocrine differentiation also includes CRPC with small cell carcinoma-like clinical presentation, which morphology is heterogeneous and includes pure or mixed small cell carcinoma, LCNC, and usual high-grade prostate adenocarcinoma with or without evidence of NE differentiation by immunohistochemistry [14, 56]. Patients with this aggressive variant of CRPC present with any combination of these manifestations: visceral metastases, lytic bone metastases, bulky lymphadenopathy, low PSA, elevated serum chromogranin, and history of hormonal therapy [33, 51, 56, 57].
Molecular Alterations in NE Differentiation in Prostate Carcinoma
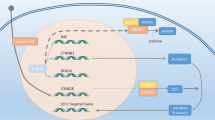
In the past few years, significant amount of molecular data has emerged from genome, transcriptome, and epigenetic analysis of prostate cancer and has increased our understanding of the molecular basis of this disease. Several molecular aberrations have been implicated in this neuroendocrine development in prostate cancer progression including AR independence, AURKA amplification +/− MYCN amplification [18, 56, 58], REST downregulation or loss, TP53 loss, RB1 loss, PTEN loss, MYCL amplification, SMAD4 mutations, overexpression of stem cell transcription factor genes, upregulation of mitotic or proliferative genes, and upregulation of genes encoding NE markers [57, 59,60,61,62,63].
Androgen Receptor
Androgen receptors (AR) plays an important role in regulation of genes responsible for normal development and function of prostate, and specifically stromal AR controls prostatic epithelial cell proliferation, survival, and differentiation [64, 65]. Aberrations in AR gene such as amplification, point mutation, and splice variants which leads to increased activity are seen only in setting of metastatic and castration-resistant prostate cancer and not seen in clinically localized prostate cancer [66, 67]. The absence of AR gene lesions in localized tumors, and their emergence during treatment is hypothesized as a mechanism of resistance to drugs targeting androgen axis in advanced disease. Approximately 80% of castrate-resistant prostate carcinoma have been documented to bear an extra copy of AR gene, and in 30% cases, this is to the level of gene amplification, whereas this phenomenon is very rare in untreated prostate cancer [68]. Recently, it is shown that AR gene copy number change emerges during development of prostatic small cell carcinoma and is strongly associated with TMPRSS2-ERG rearrangement [69].
AR mutation are present in 10–30% in CRPC while being very rare in early stage untreated prostate cancer [68]. Majority of these mutations are gain of function mutation. These mutations most commonly affect ligand-binding specificity of AR leading to its activation [70]. Most common AR mutation seen in CRPC is T877A, other less common being L701H, V715M, V730M and H874Y.
AR splice variants are suspected to be major culprit behind development of resistance to ADT. Till now, more than 22 AR splice variants have been documented, but clinical relevance is seen in only 2 constitutively activated variants, namely, AR-V7 and ARV567es [71, 72]. ADT has been shown to cause inhibition of AR pathways, which in turn causes upregulation of AR-V7 and ARV567es [73, 74]. Expression level of these variants is known to be associated with poor patient outcome and also with CRPC [75].
Enzalutamide and abiraterone are potent AR-targeted therapies approved for the treatment of men with castration-resistant prostate cancer (CRPC) [76, 77]. Although the use of these agents improves the survival and quality of life of individuals with CRPC, most patients ultimately develop resistance to them [78]. Prostate adenocarcinomas may eventually completely escape androgen blockade and become truly hormone refractory (AR-independent), associated with the development of a predominantly neuroendocrine clinical phenotype (NEPC). In a recent study by Beltran et al., sequencing analysis of CRPC tumors that histologically were characterized as either adenocarcinomas or NEPC further supports divergent evolution of NECP from one or more CRPC cells rather than linear or independent clonal evolution, with decreased AR signaling and epithelial plasticity. In that study, genome-wide DNA methylation analysis also revealed marked epigenetic differences between NEPC and CRPC and also designated samples of CRPC with clinical features of AR independence as NEPC, suggesting that epigenetic modifiers may play a role in the induction and/or maintenance of this treatment-resistant state [79].
AURKA and MYCN
AURKA amplification has been reported in 65% of prostatic carcinoma (hormone naïve and treated) which subsequently developed NEPC after androgen deprivation therapy (ADT). Such gene amplification was present in 86% of distant metastases. Concurrent amplification of MYCN was present in 70% of primary tumors, 69% of CRPC, and 83% of metastases [56]. This is significant when compared to prevalence of these amplifications in only 5% of unselected prostatic carcinoma cases (Fig. 19.4). It has also been shown that transfection of AURKA and MYCN causes NE differentiation in normal benign prostate cell lines and use of AURKA inhibitors causes inhibition of MYCN transfected NEPC cell lines and shrinkage of NEPC xenograft [18, 56, 80]. AURKA amplification is also reported to be present in 45% of prostatic adenocarcinoma with Paneth cell-like neuroendocrine differentiation when compared to tumors without Paneth cell-like differentiation where it is present only in 7% cases [41]. These finding suggest that AURKA and MYCN play significant role in development of NEPC and can be exploited as therapeutic target. AURKA inhibitors are currently in stage of clinical trials, and a ray of hope is seen for NEPC patients in whom targeting hormone pathway is no longer effective [81]. In addition, recent data demonstrate that N-Myc overexpression in preclinical models drives aggressive prostate cancer that mimic NEPC at the molecular level and sensitizes cells to AURKA and EZH2 inhibition [82].
AURKA and MYCN amplifications in primary prostatic adenocarcinoma may predict the subsequent development of neuroendocrine prostate cancer (NEPC). This four-image panel illustrates several specimens from a patient at different stages of disease progression to NEPC. (a and b) Images of hormone naïve prostate cancer with areas of Gleason score 3 + 3 = 6 (a) and 4 + 5 = 9 (b) at initial diagnosis. Concurrent AURKA (upper inset) and MYCN (middle inset) amplifications are present in both areas. (c) Subsequent local recurrence in the bladder demonstrates high-grade adenocarcinoma without neuroendocrine differentiation, exhibiting both AURKA and MYCN amplifications (upper and middle insets, respectively). (d) Five years after hormonal treatment, the patient presented with metastatic large cell neuroendocrine carcinoma in pelvic soft tissue. The tumor has both AURKA and MYCN amplifications (upper and middle insets, respectively). Clonal origin is confirmed by ERG rearrangement through translocation in all tumors (lower inset). (Reprinted from Neoplasia, Vol 15, Juan Miguel Mosquera et al., Concurrent AURKA and MYCN Gene Amplifications Are Harbingers of Lethal TreatmentRelated Neuroendocrine Prostate Cancer, p. 4, Copyright (2013), with permission from Elsevier)
REST downregulation : Repressor element-1 silencing transcription factor (REST) also known as neuron restrictive silencing factor (NRSF) is a transcriptional repressor of neuronal-specific genes and has been shown to play crucial role in during embryogenesis and neural development [83,84,85]. It is proposed to be one of the key mediators for NE differentiation caused by androgen depletion [86]. Recently, it has been shown that REST downregulation is essential for NE differentiation of prostate adenocarcinoma induced by hypoxia through activation of autophagy [87]. REST is identified to be crucial regulator for CRPC to acquire EMT-like and stem cell phenotype and may serve as a potential therapeutic target for CRPC [88].
TP53 Loss
Aberration on TP53 gene has been seen in approximately 53% of metastatic CRPC [72]. NE cells of small cell neuroendocrine carcinoma are highly proliferative, compared to NE cells of benign prostate and those present in usual prostate adenocarcinoma, and lead to early metastasis [89]. It is postulated that TP53 mutation leads to inactivation of IL8–CXCR2–p53 signaling pathway, resulting in the loss of important growth inhibitory mechanism and the hyper-proliferation of NE cells in prostatic small cell carcinoma [90]. It is reported that TP53 mutation also leads to Aurora kinase A expression , which has a critical role in rapid proliferation and aggressive behavior of small cell prostatic carcinoma [58].
RB1 Loss
Rb protein loss has been seen in almost 90% of prostate small cell carcinoma cases with RB1 allelic loss in 85% of cases, whereas this Rb protein loss is rare in high-grade acinar tumors, suggesting that it is a critical event in the development of small cell carcinomas, prostate cancer progression, and metastasis [91, 92]. Rb loss along with hypoxia also leads to aberrant expression of hypoxia-regulated genetic programs that causes invasiveness and enhanced neuroendocrine differentiation in prostate cancer [93].
PTEN Loss
PTEN is one of the commonest inactivated tumor suppressor genes in human malignancies. PTEN aberrations such as deletion and mutation are seen in approximately 50% of primary prostate cancers with even higher incidence in advanced prostate cancers [94,95,96,97,98]. PTEN deletion is more frequent event in prostate cancer compared to point mutation [99]. PTEN loss mediates prostate tumor growth and metastasis via AKT activation, which may contribute to neuroendocrine differentiation [100, 101]. PTEN loss is associated with worst survival outcome in ADT-treated CRPC as well as those treated with radical prostatectomy [102, 103].
Recently, using next-generation RNA sequencing, an NEPC-specific RNA splicing signature has been identified, which is controlled by serine/arginine repetitive matrix 4 (SRRM4), which drives the progression of NEPC. This has been proposed to be a novel potential therapeutic target for NEPC [104]. IL6 is also hypothesized to induce neuroendocrine differentiation in prostate cancer cells via peroxisome proliferator-activated receptor γ and adipocyte differentiation-related protein (a major component of adiposome) which could be exploited as novel drug targets for CRPC [105].
Recurrent MYCL amplification, SMAD4 mutation along with other rare molecular aberrations have also been linked to neuroendocrine differentiation of prostate cancer [60, 62].
Clinical Presentation and Therapy
Primary or de novo NEPC (most commonly with small cell histomorphology) is rare (<1%) and tends to occur at younger age, and most patients present with overt metastases. There are no well-defined risk factors. Patients that do present with localized disease usually have few symptoms. Distant spread is often to visceral organs (such as liver and brain) or lytic bone lesions, unlike acinar prostatic adenocarcinoma that tends to metastasize to bone and produce sclerotic lesions. Presenting symptoms of primary NEPC may include constitutional symptoms, hydronephrosis, bone pain, abdominal pain, hematochezia, or hematuria. Occasionally, patients may have paraneoplastic syndrome due to ectopic production of hormones such as adrenocorticotropic hormone and antidiuretic hormone.
Differential diagnoses of pure NEPC include small cell carcinoma from other primary sites such as the lung, specifically in the setting of widespread metastatic disease. Accurate diagnosis can be challenging in this clinical scenario. Histologically, tumors from other sites may have similar morphological appearance as well as similar immunostaining profile (negative for AR and positive for NE markers). Detection of ERG gene rearrangement by FISH is helpful in such scenarios as this rearrangement is positive in more than 50% of prostatic NEPC whereas universally negative in small cell carcinoma from other sites such as the lung and bladder [48, 106].
Much more commonly, NEPC arises in the setting of androgen deprivation therapy of prostate adenocarcinoma. Resistance eventually develops to antihormonal drugs, and some hormone refractory tumors progress toward NEPC [22]. Clinically, suspicion of NEPC should be made in a patient with advanced prostate cancer showing rapid progression, especially development of visceral metastases, without appropriate rise of serum PSA level. Serum NE markers such as chromogranin A and NSE are frequently elevated in advanced prostate cancer, but extremely high values support the diagnosis of NEPC. Circulating tumor cell analysis has recently been shown to enable detection and characterization of NEPC, but it still remains as a research tool [107, 108]. Metastatic tumor biopsy is the gold standard for diagnosing NEPC.
Patients with treatment-related neuroendocrine prostate cancer will likely not respond to hormonal agents but may initially respond to platinum-based chemotherapy . Therefore, treatment of NEPC is somewhat similar to that of small cell carcinoma of lung. Radiotherapy is occasionally added for local control or palliation of symptoms. Currently, there has also been growing concern for toxicities of continuous ADT (CADT). Treatment of NEPC is still an area of active research. Currently phase II clinical trial of PARP inhibitor olaparib with or without cediranib in men with metastatic castration-resistant prostate cancer-inducing NEPC is still ongoing (https://clinicaltrials.gov/ct2/show/NCT02893917).
Conclusion
In summary, NEPC is a highly aggressive form of prostate cancer that most commonly arises in the setting of hormonal treatment and very rarely de novo. Most of these tumors progress rapidly and develop visceral metastases and lytic bone lesions in the setting of low PSA. Due to widespread use of hormone therapy in treatment of prostate cancer, incidence of NEPC is anticipated to rise. Biopsy is the gold standard for diagnosing NEPC. Chemotherapy is the mainstay of treatment as used in small cell neuroendocrine carcinoma of other sites. More targeted approaches are being developed based on an emerging molecular understanding of this aggressive form of prostate cancer.
Abbreviations
- AR:
-
Androgen receptor
- CRPC:
-
Castration-resistant prostate cancer
- NEPC:
-
Neuroendocrine prostate cancer
References
Marcus DM, Goodman M, Jani AB, Osunkoya AO, Rossi PJ. A comprehensive review of incidence and survival in patients with rare histological variants of prostate cancer in the United States from 1973 to 2008. Prostate Cancer Prostatic Dis. 2012;15:283–8.
Li Q, Zhang CS, Zhang Y. Molecular aspects of prostate cancer with neuroendocrine differentiation. Chin J Cancer Res. 2016;28:122–9.
Alanee S, Moore A, Nutt M, Holland B, Dynda D, El-Zawahry A, McVary KT. Contemporary incidence and mortality rates of neuroendocrine prostate cancer. Anticancer Res. 2015;35:4145–50.
Bostwick DG, Cheng L: Urologic surgical pathology. 3rd edition. Saunders: London. pp. 1 online resource (ix, 966 pages):1 online resource (ix, 966 pages).
Aumuller G, Doll A, Wennemuth G, Dizeyi N, Abrahamsson PA, Wilhelm B. Regional distribution of neuroendocrine cells in the urogenital duct system of the male rat. Prostate. 2012;72:326–37.
Alberti C. Neuroendocrine differentiation in prostate carcinoma: focusing on its pathophysiologic mechanisms and pathological features. G Chir. 2010;31:568–74.
di Sant’Agnese PA. Neuroendocrine cells of the prostate and neuroendocrine differentiation in prostatic carcinoma: a review of morphologic aspects. Urology. 1998;51:121–4.
di Sant’Agnese PA. Neuroendocrine differentiation in carcinoma of the prostate. Diagnostic, prognostic, and therapeutic implications. Cancer. 1992;70:254–68.
di Sant’Agnese PA, de Mesy Jensen KL, Ackroyd RK. Calcitonin, katacalcin, and calcitonin gene-related peptide in the human prostate. An immunocytochemical and immunoelectron microscopic study. Arch Pathol Lab Med. 1989;113:790–6.
Sunday ME, Kaplan LM, Motoyama E, Chin WW, Spindel ER. Gastrin-releasing peptide (mammalian bombesin) gene expression in health and disease. Lab Investig. 1988;59:5–24.
Mucci NR, Akdas G, Manely S, Rubin MA. Neuroendocrine expression in metastatic prostate cancer: evaluation of high throughput tissue microarrays to detect heterogeneous protein expression. Hum Pathol. 2000;31:406–14.
International Agency for Research on Cancer (IARC), Moch H. WHO classification of tumours of the urinary system and male genital organs. 4th ed. Geneva: WHO.
Surcel CI, van Oort IM, Sooriakumaran P, Briganti A, De Visschere PJ, Futterer JJ, Ghadjar P, Isbarn H, Ost P, van den Bergh RC, et al. Prognostic effect of neuroendocrine differentiation in prostate cancer: a critical review. Urol Oncol. 2015;265:e261–7.
Epstein JI, Amin MB, Beltran H, Lotan TL, Mosquera JM, Reuter VE, Robinson BD, Troncoso P, Rubin MA. Proposed morphologic classification of prostate cancer with neuroendocrine differentiation. Am J Surg Pathol. 2014;38:756–67.
Nakada SY, di Sant’Agnese PA, Moynes RA, Hiipakka RA, Liao S, Cockett AT, Abrahamsson PA. The androgen receptor status of neuroendocrine cells in human benign and malignant prostatic tissue. Cancer Res. 1993;53:1967–70.
Sauer CG, Roemer A, Grobholz R. Genetic analysis of neuroendocrine tumor cells in prostatic carcinoma. Prostate. 2006;66:227–34.
Yuan TC, Veeramani S, Lin MF. Neuroendocrine-like prostate cancer cells: neuroendocrine transdifferentiation of prostate adenocarcinoma cells. Endocr Relat Cancer. 2007;14:531–47.
Beltran H, Rickman DS, Park K, Chae SS, Sboner A, MacDonald TY, Wang Y, Sheikh KL, Terry S, Tagawa ST, et al. Molecular characterization of neuroendocrine prostate cancer and identification of new drug targets. Cancer Discov. 2011;1:487–95.
Humphrey PA. Histological variants of prostatic carcinoma and their significance. Histopathology. 2012;60:59–74.
Okoye E, Choi EK, Divatia M, Miles BJ, Ayala AG, Ro JY. De novo large cell neuroendocrine carcinoma of the prostate gland with pelvic lymph node metastasis: a case report with review of literature. Int J Clin Exp Pathol. 2014;7:9061–6.
Acosta-Gonzalez G, Qin J, Wieczorek R, Melamed J, Deng FM, Zhou M, Makarov D, Ye F, Pei Z, Pincus MR, Lee P. De novo large cell neuroendocrine carcinoma of the prostate, case report and literature review. Am J Clin Exp Urol. 2014;2:337–42.
Hirano D, Okada Y, Minei S, Takimoto Y, Nemoto N. Neuroendocrine differentiation in hormone refractory prostate cancer following androgen deprivation therapy. Eur Urol. 2004;45:586–92. discussion 592
Berruti A, Mosca A, Porpiglia F, Bollito E, Tucci M, Vana F, Cracco C, Torta M, Russo L, Cappia S, et al. Chromogranin A expression in patients with hormone naive prostate cancer predicts the development of hormone refractory disease. J Urol. 2007;178:838–43. quiz 1129
di Sant’Agnese PA. Neuroendocrine differentiation in prostatic carcinoma: an update on recent developments. Ann Oncol. 2001;12(Suppl 2):S135–40.
Abrahamsson PA. Neuroendocrine differentiation in prostatic carcinoma. Prostate. 1999;39:135–48.
Lin D, Wyatt AW, Xue H, Wang Y, Dong X, Haegert A, Wu R, Brahmbhatt S, Mo F, Jong L, et al. High fidelity patient-derived xenografts for accelerating prostate cancer discovery and drug development. Cancer Res. 2014;74:1272–83.
Aparicio A, Tzelepi V. Neuroendocrine (small-cell) carcinomas: why they teach us essential lessons about prostate cancer. Oncology (Williston Park). 2014;28:831–8.
Wang HT, Yao YH, Li BG, Tang Y, Chang JW, Zhang J. Neuroendocrine Prostate Cancer (NEPC) progressing from conventional prostatic adenocarcinoma: factors associated with time to development of NEPC and survival from NEPC diagnosis-a systematic review and pooled analysis. J Clin Oncol. 2014;32:3383–90.
Terry S, Maille P, Baaddi H, Kheuang L, Soyeux P, Nicolaiew N, Ceraline J, Firlej V, Beltran H, Allory Y, et al. Cross modulation between the androgen receptor axis and protocadherin-PC in mediating neuroendocrine transdifferentiation and therapeutic resistance of prostate cancer. Neoplasia. 2013;15:761–72.
Nouri M, Ratther E, Stylianou N, Nelson CC, Hollier BG, Williams ED. Androgen-targeted therapy-induced epithelial mesenchymal plasticity and neuroendocrine transdifferentiation in prostate cancer: an opportunity for intervention. Front Oncol. 2014;4:370.
Farach A, Ding Y, Lee M, Creighton C, Delk NA, Ittmann M, Miles B, Rowley D, Farach-Carson MC, Ayala GE. Neuronal trans-differentiation in prostate cancer cells. Prostate. 2016;76:1312–25.
Aparicio A, Logothetis CJ, Maity SN. Understanding the lethal variant of prostate cancer: power of examining extremes. Cancer Discov. 2011;1:466–8.
Beltran H, Tagawa ST, Park K, MacDonald T, Milowsky MI, Mosquera JM, Rubin MA, Nanus DM. Challenges in recognizing treatment-related neuroendocrine prostate cancer. J Clin Oncol. 2012;30:e386–9.
Parimi V, Goyal R, Poropatich K, Yang XJ. Neuroendocrine differentiation of prostate cancer: a review. Am J Clin Exp Urol. 2014;2:273–85.
Sun Y, Niu J, Huang J. Neuroendocrine differentiation in prostate cancer. Am J Transl Res. 2009;1:148–62.
Puccetti L, Supuran CT, Fasolo PP, Conti E, Sebastiani G, Lacquaniti S, Mandras R, Milazzo MG, Dogliani N, De Giuli P, Fasolis G. Skewing towards neuroendocrine phenotype in high grade or high stage androgen-responsive primary prostate cancer. Eur Urol. 2005;48:215–21. Discussion 221–213
Adlakha H, Bostwick DG. Paneth cell-like change in prostatic adenocarcinoma represents neuroendocrine differentiation: report of 30 cases. Hum Pathol. 1994;25:135–9.
Kuroda N, Katto K, Shiotsu T, Lee GH. Prostatic adenocarcinoma with Paneth cell-like change. APMIS. 2007;115:857–8.
Tamas EF, Epstein JI. Prognostic significance of paneth cell-like neuroendocrine differentiation in adenocarcinoma of the prostate. Am J Surg Pathol. 2006;30:980–5.
So JS, Gordetsky J, Epstein JI. Variant of prostatic adenocarcinoma with Paneth cell-like neuroendocrine differentiation readily misdiagnosed as Gleason pattern 5. Hum Pathol. 2014;45:2388–93.
Park K, Chen Z, MacDonald TY, Siddiqui J, Ye H, Erbersdobler A, Shevchuk MM, Robinson BD, Sanda MG, Chinnaiyan AM, et al. Prostate cancer with Paneth cell-like neuroendocrine differentiation has recognizable histomorphology and harbors AURKA gene amplification. Hum Pathol. 2014;45:2136–43.
Reyes A, Moran CA. Low-grade neuroendocrine carcinoma (carcinoid tumor) of the prostate. Arch Pathol Lab Med. 2004;128:e166–8.
Wang W, Epstein JI. Small cell carcinoma of the prostate. A morphologic and immunohistochemical study of 95 cases. Am J Surg Pathol. 2008;32:65–71.
Yao JL, Madeb R, Bourne P, Lei J, Yang X, Tickoo S, Liu Z, Tan D, Cheng L, Hatem F, et al. Small cell carcinoma of the prostate: an immunohistochemical study. Am J Surg Pathol. 2006;30:705–12.
Schron DS, Gipson T, Mendelsohn G. The histogenesis of small cell carcinoma of the prostate. An immunohistochemical study. Cancer. 1984;53:2478–80.
Agoff SN, Lamps LW, Philip AT, Amin MB, Schmidt RA, True LD, Folpe AL. Thyroid transcription factor-1 is expressed in extrapulmonary small cell carcinomas but not in other extrapulmonary neuroendocrine tumors. Mod Pathol. 2000;13:238–42.
Ordonez NG. Value of thyroid transcription factor-1 immunostaining in distinguishing small cell lung carcinomas from other small cell carcinomas. Am J Surg Pathol. 2000;24:1217–23.
Lotan TL, Gupta NS, Wang W, Toubaji A, Haffner MC, Chaux A, Hicks JL, Meeker AK, Bieberich CJ, De Marzo AM, et al. ERG gene rearrangements are common in prostatic small cell carcinomas. Mod Pathol. 2011;24:820–8.
Tomlins SA, Rhodes DR, Perner S, Dhanasekaran SM, Mehra R, Sun XW, Varambally S, Cao X, Tchinda J, Kuefer R, et al. Recurrent fusion of TMPRSS2 and ETS transcription factor genes in prostate cancer. Science. 2005;310:644–8.
Guo CC, Dancer JY, Wang Y, Aparicio A, Navone NM, Troncoso P, Czerniak BA. TMPRSS2-ERG gene fusion in small cell carcinoma of the prostate. Hum Pathol. 2011;42:11–7.
Aparicio AM, Harzstark AL, Corn PG, Wen S, Araujo JC, Tu SM, Pagliaro LC, Kim J, Millikan RE, Ryan C, et al. Platinum-based chemotherapy for variant castrate-resistant prostate cancer. Clin Cancer Res. 2013;19:3621–30.
Yumiba S, Asakura T, Okada T, Satoh M, Nin M, Tsujihata M. Etoposide and carboplatin effective for treatment of small cell carcinoma of prostate : a report of two cases. Hinyokika Kiyo. 2016;62:639–45.
Yossi S, Brahmi T, Enachescu C, Selmaji I, Lapierre A, Samlali H, Chapet O. Management of neuroendocrine prostate carcinoma: literature review. Cancer Radiother. 2016;20:330–5.
Deorah S, Rao MB, Raman R, Gaitonde K, Donovan JF. Survival of patients with small cell carcinoma of the prostate during 1973–2003: a population-based study. BJU Int. 2012;109:824–30.
Evans AJ, Humphrey PA, Belani J, van der Kwast TH, Srigley JR. Large cell neuroendocrine carcinoma of prostate: a clinicopathologic summary of 7 cases of a rare manifestation of advanced prostate cancer. Am J Surg Pathol. 2006;30:684–93.
Mosquera JM, Beltran H, Park K, MacDonald TY, Robinson BD, Tagawa ST, Perner S, Bismar TA, Erbersdobler A, Dhir R, et al. Concurrent AURKA and MYCN gene amplifications are harbingers of lethal treatment-related neuroendocrine prostate cancer. Neoplasia. 2013;15:1–10.
Terry S, Beltran H. The many faces of neuroendocrine differentiation in prostate cancer progression. Front Oncol. 2014;4:60.
Li Z, Sun Y, Chen X, Squires J, Nowroozizadeh B, Liang C, Huang J. p53 mutation directs AURKA overexpression via miR-25 and FBXW7 in prostatic small cell neuroendocrine carcinoma. Mol Cancer Res. 2015;13:584–91.
Clegg N, Ferguson C, True LD, Arnold H, Moorman A, Quinn JE, Vessella RL, Nelson PS. Molecular characterization of prostatic small-cell neuroendocrine carcinoma. Prostate. 2003;55:55–64.
Borges GT, Vencio EF, Quek SI, Chen A, Salvanha DM, Vencio RZ, Nguyen HM, Vessella RL, Cavanaugh C, Ware CB, et al. Conversion of prostate adenocarcinoma to small cell carcinoma-like by reprogramming. J Cell Physiol. 2016;231:2040–7.
Lapuk AV, Wu C, Wyatt AW, McPherson A, McConeghy BJ, Brahmbhatt S, Mo F, Zoubeidi A, Anderson S, Bell RH, et al. From sequence to molecular pathology, and a mechanism driving the neuroendocrine phenotype in prostate cancer. J Pathol. 2012;227:286–97.
Kadakia KC, Tomlins SA, Sanghvi SK, Cani AK, Omata K, Hovelson DH, Liu CJ, Cooney KA. Comprehensive serial molecular profiling of an “N of 1” exceptional non-responder with metastatic prostate cancer progressing to small cell carcinoma on treatment. J Hematol Oncol. 2015;8:109.
Priemer DS, Montironi R, Wang L, Williamson SR, Lopez-Beltran A, Cheng L. Neuroendocrine tumors of the prostate: emerging insights from molecular data and updates to the 2016 World Health Organization classification. Endocr Pathol. 2016;27:123–35.
Heinlein CA, Chang C. The roles of androgen receptors and androgen-binding proteins in nongenomic androgen actions. Mol Endocrinol. 2002;16:2181–7.
Cunha GR, Cooke PS, Kurita T. Role of stromal-epithelial interactions in hormonal responses. Arch Histol Cytol. 2004;67:417–34.
Linja MJ, Savinainen KJ, Saramaki OR, Tammela TL, Vessella RL, Visakorpi T. Amplification and overexpression of androgen receptor gene in hormone-refractory prostate cancer. Cancer Res. 2001;61:3550–5.
Ho Y, Dehm SM. Androgen receptor rearrangement and splicing variants in resistance to endocrine therapies in prostate cancer. Endocrinology. 2017;158(6):1533–42.
Waltering KK, Urbanucci A, Visakorpi T. Androgen receptor (AR) aberrations in castration-resistant prostate cancer. Mol Cell Endocrinol. 2012;360:38–43.
Wang L, Williamson SR, Zhang S, Huang J, Montironi R, Davison DD, Wang M, Yao JL, Lopez-Beltran A, Osunkoya AO, et al. Increased androgen receptor gene copy number is associated with TMPRSS2-ERG rearrangement in prostatic small cell carcinoma. Mol Carcinog. 2015;54:900–7.
Steketee K, Timmerman L, Ziel-van der Made AC, Doesburg P, Brinkmann AO, Trapman J. Broadened ligand responsiveness of androgen receptor mutants obtained by random amino acid substitution of H874 and mutation hot spot T877 in prostate cancer. Int J Cancer. 2002;100:309–17.
Lu C, Luo J. Decoding the androgen receptor splice variants. Transl Androl Urol. 2013;2:178–86.
Robinson D, Van Allen EM, Wu YM, Schultz N, Lonigro RJ, Mosquera JM, Montgomery B, Taplin ME, Pritchard CC, Attard G, et al. Integrative clinical genomics of advanced prostate cancer. Cell. 2015;161:1215–28.
Nadiminty N, Tummala R, Liu C, Yang J, Lou W, Evans CP, Gao AC. NF-kappaB2/p52 induces resistance to enzalutamide in prostate cancer: role of androgen receptor and its variants. Mol Cancer Ther. 2013;12:1629–37.
Mostaghel EA, Marck BT, Plymate SR, Vessella RL, Balk S, Matsumoto AM, Nelson PS, Montgomery RB. Resistance to CYP17A1 inhibition with abiraterone in castration-resistant prostate cancer: induction of steroidogenesis and androgen receptor splice variants. Clin Cancer Res. 2011;17:5913–25.
Hornberg E, Ylitalo EB, Crnalic S, Antti H, Stattin P, Widmark A, Bergh A, Wikstrom P. Expression of androgen receptor splice variants in prostate cancer bone metastases is associated with castration-resistance and short survival. PLoS One. 2011;6:e19059.
Scher HI, Fizazi K, Saad F, Taplin ME, Sternberg CN, Miller K, de Wit R, Mulders P, Chi KN, Shore ND, et al. Increased survival with enzalutamide in prostate cancer after chemotherapy. N Engl J Med. 2012;367:1187–97.
de Bono JS, Logothetis CJ, Molina A, Fizazi K, North S, Chu L, Chi KN, Jones RJ, Goodman OB Jr, Saad F, et al. Abiraterone and increased survival in metastatic prostate cancer. N Engl J Med. 2011;364:1995–2005.
Watson PA, Arora VK, Sawyers CL. Emerging mechanisms of resistance to androgen receptor inhibitors in prostate cancer. Nat Rev Cancer. 2015;15:701–11.
Beltran H, Prandi D, Mosquera JM, Benelli M, Puca L, Cyrta J, Marotz C, Giannopoulou E, Chakravarthi BV, Varambally S, et al. Divergent clonal evolution of castration-resistant neuroendocrine prostate cancer. Nat Med. 2016;22:298–305.
Lee JK, Phillips JW, Smith BA, Park JW, Stoyanova T, McCaffrey EF, Baertsch R, Sokolov A, Meyerowitz JG, Mathis C, et al. N-Myc drives neuroendocrine prostate cancer initiated from human prostate epithelial cells. Cancer Cell. 2016;29:536–47.
Vlachostergios PJ, Papandreou CN. Targeting neuroendocrine prostate cancer: molecular and clinical perspectives. Front Oncol. 2015;5:6.
Dardenne E, Beltran H, Benelli M, Gayvert K, Berger A, Puca L, Cyrta J, Sboner A, Noorzad Z, MacDonald T, et al. N-Myc induces an EZH2-mediated transcriptional program driving neuroendocrine prostate cancer. Cancer Cell. 2016;30:563–77.
Chong JA, Tapia-Ramirez J, Kim S, Toledo-Aral JJ, Zheng Y, Boutros MC, Altshuller YM, Frohman MA, Kraner SD, Mandel G. REST: a mammalian silencer protein that restricts sodium channel gene expression to neurons. Cell. 1995;80:949–57.
Schoenherr CJ, Anderson DJ. The neuron-restrictive silencer factor (NRSF): a coordinate repressor of multiple neuron-specific genes. Science. 1995;267:1360–3.
Chen ZF, Paquette AJ, Anderson DJ. NRSF/REST is required in vivo for repression of multiple neuronal target genes during embryogenesis. Nat Genet. 1998;20:136–42.
Svensson C, Ceder J, Iglesias-Gato D, Chuan YC, Pang ST, Bjartell A, Martinez RM, Bott L, Helczynski L, Ulmert D, et al. REST mediates androgen receptor actions on gene repression and predicts early recurrence of prostate cancer. Nucleic Acids Res. 2014;42:999–1015.
Lin TP, Chang YT, Lee SY, Campbell M, Wang TC, Shen SH, Chung HJ, Chang YH, Chiu AW, Pan CC, et al. REST reduction is essential for hypoxia-induced neuroendocrine differentiation of prostate cancer cells by activating autophagy signaling. Oncotarget. 2016;7:26137–51.
Chang YT, Lin TP, Campbell M, Pan CC, Lee SH, Lee HC, Yang MH, Kung HJ, Chang PC. REST is a crucial regulator for acquiring EMT-like and stemness phenotypes in hormone-refractory prostate cancer. Sci Rep. 2017;7:42795.
Erasmus CE, Verhagen WI, Wauters CA, van Lindert EJ. Brain metastasis from prostate small cell carcinoma: not to be neglected. Can J Neurol Sci. 2002;29:375–7.
Chen H, Sun Y, Wu C, Magyar CE, Li X, Cheng L, Yao JL, Shen S, Osunkoya AO, Liang C, Huang J. Pathogenesis of prostatic small cell carcinoma involves the inactivation of the P53 pathway. Endocr Relat Cancer. 2012;19:321–31.
Tan HL, Sood A, Rahimi HA, Wang W, Gupta N, Hicks J, Mosier S, Gocke CD, Epstein JI, Netto GJ, et al. Rb loss is characteristic of prostatic small cell neuroendocrine carcinoma. Clin Cancer Res. 2014;20:890–903.
Thangavel C, Boopathi E, Liu Y, Haber A, Ertel A, Bhardwaj A, Addya S, Williams N, Ciment SJ, Cotzia P, et al. RB loss promotes prostate cancer metastasis. Cancer Res. 2017;77:982–95.
Labrecque MP, Takhar MK, Nason R, Santacruz S, Tam KJ, Massah S, Haegert A, Bell RH, Altamirano-Dimas M, Collins CC, et al. The retinoblastoma protein regulates hypoxia-inducible genetic programs, tumor cell invasiveness and neuroendocrine differentiation in prostate cancer cells. Oncotarget. 2016;7:24284–302.
Cairns P, Okami K, Halachmi S, Halachmi N, Esteller M, Herman JG, Jen J, Isaacs WB, Bova GS, Sidransky D. Frequent inactivation of PTEN/MMAC1 in primary prostate cancer. Cancer Res. 1997;57:4997–5000.
Qu X, Randhawa G, Friedman C, Kurland BF, Glaskova L, Coleman I, Mostaghel E, Higano CS, Porter C, Vessella R, et al. A three-marker FISH panel detects more genetic aberrations of AR, PTEN and TMPRSS2/ERG in castration-resistant or metastatic prostate cancers than in primary prostate tumors. PLoS One. 2013;8:e74671.
Pesche S, Latil A, Muzeau F, Cussenot O, Fournier G, Longy M, Eng C, Lidereau R. PTEN/MMAC1/TEP1 involvement in primary prostate cancers. Oncogene. 1998;16:2879–83.
Beltran H, Yelensky R, Frampton GM, Park K, Downing SR, MacDonald TY, Jarosz M, Lipson D, Tagawa ST, Nanus DM, et al. Targeted next-generation sequencing of advanced prostate cancer identifies potential therapeutic targets and disease heterogeneity. Eur Urol. 2013;63:920–6.
Grasso CS, Wu YM, Robinson DR, Cao X, Dhanasekaran SM, Khan AP, Quist MJ, Jing X, Lonigro RJ, Brenner JC, et al. The mutational landscape of lethal castration-resistant prostate cancer. Nature. 2012;487:239–43.
Wise HM, Hermida MA, Leslie NR. Prostate cancer, PI3K, PTEN and prognosis. Clin Sci (Lond). 2017;131:197–210.
Conley-LaComb MK, Saliganan A, Kandagatla P, Chen YQ, Cher ML, Chinni SR. PTEN loss mediated Akt activation promotes prostate tumor growth and metastasis via CXCL12/CXCR4 signaling. Mol Cancer. 2013;12:85.
Ham WS, Cho NH, Kim WT, Ju HJ, Lee JS, Choi YD. Pathological effects of prostate cancer correlate with neuroendocrine differentiation and PTEN expression after bicalutamide monotherapy. J Urol. 2009;182:1378–84.
Ferraldeschi R, Nava Rodrigues D, Riisnaes R, Miranda S, Figueiredo I, Rescigno P, Ravi P, Pezaro C, Omlin A, Lorente D, et al. PTEN protein loss and clinical outcome from castration-resistant prostate cancer treated with abiraterone acetate. Eur Urol. 2015;67:795–802.
Lahdensuo K, Erickson A, Saarinen I, Seikkula H, Lundin J, Lundin M, Nordling S, Butzow A, Vasarainen H, Bostrom PJ, et al. Loss of PTEN expression in ERG-negative prostate cancer predicts secondary therapies and leads to shorter disease-specific survival time after radical prostatectomy. Mod Pathol. 2016;29:1565–74.
Li Y, Donmez N, Sahinalp C, Xie N, Wang Y, Xue H, Mo F, Beltran H, Gleave M, Wang Y, et al. SRRM4 drives neuroendocrine transdifferentiation of prostate adenocarcinoma under androgen receptor pathway inhibition. Eur Urol. 2017;71:68–78.
Lin LC, Gao AC, Lai CH, Hsieh JT, Lin H. Induction of neuroendocrine differentiation in castration resistant prostate cancer cells by adipocyte differentiation-related protein (ADRP) delivered by exosomes. Cancer Lett. 2017;391:74–82.
Scheble VJ, Braun M, Beroukhim R, Mermel CH, Ruiz C, Wilbertz T, Stiedl AC, Petersen K, Reischl M, Kuefer R, et al. ERG rearrangement is specific to prostate cancer and does not occur in any other common tumor. Mod Pathol. 2010;23:1061–7.
Beltran H, Jendrisak A, Landers M, Mosquera JM, Kossai M, Louw J, Krupa R, Graf RP, Schreiber NA, Nanus DM, et al. The initial detection and partial characterization of circulating tumor cells in neuroendocrine prostate cancer. Clin Cancer Res. 2016;22:1510–9.
Rescigno P, Rodrigues DN, de Bono JS. Circulating biomarkers of neuroendocrine prostate cancer: an unmet challenge. BJU Int. 2017;119:3–4.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Beg, S., Mosquera, J.M. (2018). Neuroendocrine Prostate Cancer. In: Robinson, B., Mosquera, J., Ro, J., Divatia, M. (eds) Precision Molecular Pathology of Prostate Cancer. Molecular Pathology Library. Springer, Cham. https://doi.org/10.1007/978-3-319-64096-9_19
Download citation
DOI: https://doi.org/10.1007/978-3-319-64096-9_19
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-64094-5
Online ISBN: 978-3-319-64096-9
eBook Packages: MedicineMedicine (R0)