Abstract
Non-small cell lung carcinoma (NSCLC) remains the leading cause of death from cancer in both men and women. Distant reoccurrence remains the major cause of morbidity and mortality in the patients with lung cancer. The term metastasis is defined as the transfer of disease from one organ to part or to another not directly connected to it. Metastasis is the primary clinical challenge as it is unpredictable in onset and it exponentially increases the clinical impact to the host. Tumor metastasis is a multistage process in which malignant cells spread from primary tumor to discontiguous organs. It involves a rest and growth in different micro-environments, which are treated clinically with different strategies depending on the tumor histotope and metastatic location. Some isolated metastases may be resected, whereas metastases to other organs may be treated with radioisotopes and are virtually unresectable. Because of the cellular heterogeneity therapies have varying degrees of efficacy that are challenging not only for the oncologist but also for our understanding of the metastatic process. This chapter will focus on differences regarding morphology and biomarker expression between the primary tumor and metastases of lung adenocarcinoma. The mutation status of metastases can differ from that of the primary tumor and also among metastases. The review will also present the frequency and the significance of pathologic variables between primary tumor and metastases.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Non-small cell lung carcinoma (NSCLC) remains the leading cause of death from cancer in both men and women [1]. Distant reoccurrence remains the major cause of morbidity and mortality in the patients with lung cancer [2]. The term metastasis was coined in 1829 by Jean Claude Récamier [3]. Today it is defined as the transfer of disease from one organ to another not directly connected to it. Metastasis is the primary clinical challenge as it is unpredictable in onset and it exponentially increases the clinical impact to the host [4]. Tumor metastasis is a multistage process in which malignant cells spread from primary tumor to discontiguous organs [2, 5]. It involves a rest and growth in different micro-environments, which are treated clinically with different strategies depending on the tumor histotype and anatomic location of the metastases. Because of the cellular heterogeneity therapies have varying efficacy challenging not only the oncologist but also our understanding of the metastatic process. Each step is rate limiting and is influenced by the interaction between tumor cells and the local micro-environment [3]. If a cell fails each one of the steps, the process stops. Therefore, development of each metastasis represents the survival of selected population of cells that preexist in the primary tumors. Tumor formation starts with cellular selection and transformation, resulting in the growth of the tumor. When the tumor reaches a critical mass new vascularization occurs through an intricate interaction of angiogenesis phenomena. Tumors acquire the propensity to invade through the basement membrane into the stroma, lymphatics, and capillaries through a process of motility and intravasation. Tumor cells migrate in the capillaries, venules, lymphatic vessels to form microemboli and cellular aggregates that have the property to spread and disseminate to distant organ sites. At the distant organ sites the tumor emboli arrest in the capillary beds, they adhere to the vascular walls and when they reach a critical mass they start to extravasate into the neighboring organ parenchyma through a process similar to the intravasation into the capillaries. Through complex interactions between the tumor cells and the local micro-environment the tumor cells start to proliferate, form new vessels through angiogenesis, and acquire properties that are significant for the formation of metastases in distant organs [3].
In many patients the process of metastasis has occurred by the time of diagnosis, even if this is not apparent clinically. In some instances the tumor metastases can occur early in the tumor progression stages, when the primary tumor is small or undetectable. However, in the majority of tumors the process of metastasis occurs later in the tumor progression stages when the primary tumor is much larger. The process of tumor metastasis has important features that have recently been uncovered and explored [5, 6].
Lung Cancer Metastases
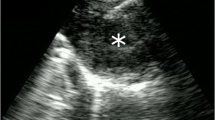
Lung cancer can spread to any part of the human body. Metastatic spread may result in the presenting symptoms or may occur later in the course of disease. The most frequent sites of distant metastases are the brain, liver, adrenal glands, and bones [7] (Fig. 16.1). Surprisingly the distal recurrences and metastasis to distant organs for lung cancer are extremely high (41–45%) and although studies have shown that chemotherapy, targeted therapy, or systemic immune checkpoint inhibitors (preferred) could lower the incidence of metastasis (Table 16.1), the recurrence rate still remains high [8, 9]. The IALT study [9] shows that the incidence of brain metastases is the most common among the patients with lung cancer (irrespective of the type of treatment) and represents almost a third of all the tumors that spread to distant organs.
A primary lung cancer (left panel) involving the lung of a non-smoker patient treated for recurrent NSCLC with multiple cycles of chemotherapy and radiation. The patient had involvement of multiple organs (liver, adrenal, and bone) that led to multiple organ failure and disseminated disease in multiple organs
Liver Metastases
Symptomatic hepatic metastases are uncommon early in the course of the disease; asymptomatic liver metastases may be detected at presentation by liver enzyme abnormalities, CT or PET imaging. Among the patients with otherwise resectable NSCLC in the chest, CT evidence of liver metastases has been identified in approximately 3% of the cases. Newer imaging techniques (PET or integrated PET/CT) identify unsuspected metastases in the liver or the adrenal glands respectively in about 4% of the patients. The incidence of liver metastasis is much higher later in the course of disease once the tumor progresses and spreads to distant organs. Autopsy studies have shown that hepatic metastases are present in more than 50% of the patients with either NSCLC or small cell cancer.
Adrenal Metastases
The adrenal glands are a frequent site of metastasis but are rarely symptomatic. Only a fraction of adrenal masses detected on staging scans represent metastases. In a series of 330 patients with operable NSCLC, 10% had isolated adrenal masses [10]. Only 8 out of 32 (25%) were malignant, while the remainder had benign lesions like adrenal adenoma, adrenal nodule hyperplasia, or hemorrhagic cysts. Conversely, negative imaging studies do not exclude adrenal masses and a study of patients that had SCC found that at least 17% of adrenal biopsies showed metastatic involvement despite normal CT scans [11]. The lack of specificity of initial CT identifying an adrenal mass creates a special problem in patients with an otherwise resectable lung cancer. Involvement of the adrenal glands is more frequent in patients with widely disseminated disease. In an autopsy series that have been previously published, adrenal gland metastases have been identified in 40% of patients with lung cancer.
Bone Metastases
Metastases from lung cancer to bone are frequently symptomatic. Patients present with pain and elevated levels of alkaline phosphatases. Twenty percent of patients with NSCLC have bone metastases at presentation and osteolytic appearances are more common than osteoblastic ones. The most common sites of involvement are the vertebral bodies. Bone metastases are even more common in patients with SCLC, and represent 30–40%. Modern imaging studies (PET and PET/CT) have improved the ability to identify metastases to many organs including bone, with greater sensitivity than CT or bone scan.
Brain Metastases
Lung cancer is the malignancy that most commonly gives rise to brain metastasis which is a devastating complication [12]. Brain metastases are a major cause of morbidity and mortality in human malignancies in patients wit h NSCLC. The frequency of brain metastasis is greatest with adenocarcinoma and least with squamous cell carcinoma . Approximately 10% of the patients have brain metastases at the time of diagnosis, and approximately 40% of all patients with lung cancer will develop brain metastases during the course of the disease [13]. Patients with locally advanced NSCLC who are treated with chemotherapy and chest radiotherapy with or without surgery have a very high rate of developing brain metastases [14,15,16,17]. These patients also have a risk that ranges from 15 to 30% of failing first in the brain. Brain metastases from NSCLC have received increasing attention, because combined-modality therapy has led to improvements in intrathoracic local control and prolonged overall survival [18,19,20]. The risk for brain metastasis increases with larger primary tumor size and regional node involvement (which is a well-known phenomenon at the basis TNM staging system). For carefully selected patients, surgical resection may be feasible. Surgical resection of brain metastases may be feasible in cases that have operable NSCLC in the chest and solitary brain metastases. In patients with SCLC, metastases to brain are present in 20–30% at initial diagnosis. Without prophylactic irradiation, relapse in the brain occurs in 50% within the next 2 years after the diagnosis. Randomized trials have shown that the frequency of brain metastases can be significantly reduced with prophylactic cranial irradiation. It is important to identify the patients with NSCLC who are at greater risk of developing metastases because such metastases may exist in the absence of neurologic symptoms [21]. Furthermore, prophylactic cranial irradiation may be an effective modality preventing brain metastases in patients with NSCLC who receive adjuvant chemoradiation [16]. Despite advances in diagnosis, therapeutic modalities, and clinical practice guidelines, it remains unclear whether patients with NSCLC should be screened for brain metastases or not [22, 23].
Molecular Characteristics of Metastases in Comparison with Primary Tumor
Recent studies have advanced the hypothesis that there may be important differences in the primary tumor , lung tumor, and metastases of lung adenocarcinoma, regarding morphology, biomarker expression, and genotype [24]. The mutation status of metastases can differ from the primary tumors and also among metastases [3, 25]. The frequency of differences and the significance of the differences in pathologic variables between primary lung tumors and metastases and also previously systemically treated tumors have yet to be fully investigated [25, 26]. Both the cells within the primary tumor and the metastatic lesions can continue to diversify if the lesions grow and result in molecular differences between the primary and the metastatic tumor. To determine whether the genetic profiles are similar between the primary lung cancer and their paired metastases to the brain, we examined pairs of primary metastatic lung carcinomas by high-throughput genetic mutation profiling. We evaluated four-micron formalin-fixed paraffin embedded specimens from patients with lung cancer (women 52% and men 48%) with a median age of 65 years. The tumors investigated were 12 adenocarcinomas and nine squamous cell carcinomas and the corresponding brain metastases they developed after a median of 12.5 months (range 2–90 months) over a 35-month median follow-up time. We employed the sequenom mass spectrometry-based system (IPLEX protocol-oncomap analyses) for 252 genetic mutations in the following genes: ABL1, BRAF, EGFR, FGFR3, HRAS, KRAS, MET, N-ras, PBGFRA, PI3K, and RET. Some of the lower confidence mutations identified by IPLEX protocol were validated by homogeneous mass-extended (HME) technology . We found that nine patients (39.1%) had mutations only in the primary tumors Table 16.2. In five patients (21.7%) mutations were identified only in the brain metastases and in only three patients (13%) mutations were identified in both lung and brain metastases (Table 16.2). Except K-ras G12C mutation that was identified in two patients, all mutations were unique in each patient.
In summary, there is a great variation in the molecular abnormalities between individual primary NSCLC and their metastases to the brain. Understanding these differences will allow us to clarify the mechanism of metastatic progression of NSCLC to brain and potentially identify novel targets of therapy.
Protein Expression Characteristics of Metastatic Lung Carcinoma to Brain and Primary Metastases
We compared the expression of certain proteins between brain metastases and the primary tumors (Fig. 16.2). The results of the study showed that metastatic NSCLC to the brain have a higher expression of MIB1 (p = 0.02), a lower VEGF-A (p = 0.03), and a higher EGFR (p = 0.03) expression in brain metastases than the matched primary NSCL cancers (Fig. 16.2).
MET in Primary Lung Cancers and Corresponding Distant Brain Metastases
MET amplification has been detected in 20% of NSCL cancers with EGFR mutations progressing after an initial response to tyrosine-kinase inhibitors (TKI) therapy. MET is amplified, mutated, and overexpressed or uniquely activated in many tumors. MET expression was associated with worse prognosis in many cancers including NSCLC [27]. We investigated MET expression, phosphorylation, and gene copy gain in both primary NSCLC and brain metastases. MET FISH reveals a lower copy gain in the primary lung tumors versus a higher copy gain in the corresponding metastatic lesions (Fig. 16.3). Surprisingly we found that the expression of both the receptors is focal and heterogeneous. Furthermore, immunohistochemistry images on consecutive sections revealed colocalization of deletion of EGFR mutated cells and activated MET cells. Our studies confirm the hypothesis of clonal selection and the genotype differences between primary tumors and brain metastases (Fig. 16.4). We found that the heterogeneous Met expression, activation, and gene copy gain in primary NSCLC is significantly enriched in paired brain metastases. These results suggest that the enrichment of Met-activated lung tumor cells in brain metastases may result from an increased capacity for Met activated primary tumor cells to migrate and establish metastases. The initial response to EGFR tyrosine-kinase therapy and the initial disease control (partial response or stable disease as defined by RECIST criteria) is anticipated in tumors harboring no MET activation (scenario A, Fig. 16.5) or a low percentage of MET activation (scenario B, Fig. 16.5). By contrast, primary resistance (progressive diseases defined by RECIST criteria) is consistent with tumors harboring a high percentage of MET activated cells with concomitant EGFR tyrosine-kinase resistant cells (scenario C, Fig. 16.5) [27].
Preexisting Met activation may predict poor response to subsequent EGFR TKI therapy in EGFR mutant NSCLC. Initial response to EGFR TKI therapy: Initial disease control (partial response or stable disease, as defined by RECIST criteria) is anticipated in tumors harboring no Met activation (A) or a low percentage of Met activation (B). By contrast, primary resistance (progressive disease as defined by RECIST) is consistent with tumors harboring a high percentage of Met activated, EGFR TKI resistant cells. (C) Disease control in tumors without Met activation may remain relatively durable but, initial disease control in tumors with low level Met activation is not durable, as focal regions of Met activated, EGFR TKI resistant cells can proliferate despite EGFR TKI therapy
Genetic Abnormalities in Primary Lung Cancers and Locoregional Lymph Node Metastases
Recent studies looked into the EGFR, KRAS, and BRAF mutations in primary lung adenocarcinomas and corresponding locoregional lymph node metastases [28]. The study revealed that 72% (31 out of 43 patients with mutated tumors in total 32% of all investigated cases) with mutations showed discordant results. The discordant mutational status in the primary tumor and the corresponding lymph node metastases were 6 out of 7 cases with EGFR mutation and 25 out of 36 cases with KRAS mutations. The lack of the correlation in the mutation status between primary tumors and metastases is most likely real and not due to technical problems for several reasons: (a) all tumor specimens analyzed were required to contain at least 70% tumor cells, (b) the results were confirmed by a second run, (c) the mutant rate in the primary tumors was not different to previous published data, and (d) the results were in accordance with those from other reports.
Predictive Markers Associated with an Increased Risk of Brain Metastases
We performed a controlled study of patients who were newly diagnosed with NSCLC, who developed brain metastases . These patients were initially diagnosed with early stage operable lung cancer. After surgical removal of the primary tumor the patients were followed up for a median period of 35.5 months [12]. These patients developed brain metastases as a site of distant release after a median period of 12.5 months. These patients were compared with a control group of patients who had NSCLC and no evidence of brain metastases in the same follow-up period. NSCLC and their corresponding metastases were examined for expression levels of Ki-67, caspase-3, VEGF-A, VEGF-C, E-cadherin, and EGFR respectively. The study showed an increased risk of developing brain metastases in patients who had a high expression of Ki-67, caspase-3, VEGF-C, and e-cadherin but not with VEGF-A and EGFR (Fig. 16.6). Patients with an increased Ki-67 labeling index developed metastases after a median time of 1.2 years as opposed to 5 years for the patients with the low labeling index. Furthermore, patients with a lower caspase labeling index had an increased rate of developing brain metastases as opposed to patients with a high labeling index. The results of the study indicated that patients with NSCLC and high Ki-67, low caspase-3, high VEGF-C, and low e-cadherin in their tumors may benefit from close surveillance because they may have an increased risk of developing brain metastases. Higher Ki-67 and lower caspase labeling indices characterize patients who are at greater risk of developing metastatic NSCLC to the brain. The identification of this subgroup of patients is very important as these patients may benefit from early and close physical and imaging follow-up. In addition, this subset of patients may benefit from prophylactic brain irradiation. Another study looked into 100 consecutive patients with EGFR mutations that were treated with gefitinib or erlotinib that followed the patients for a period of time and looked into the incidence of brain metastases [29]. The authors have surprisingly shown that there are differences between different types of EGFR mutations (exon 19 deletion versus L858R point mutation) in the characteristics of the primary tumors and propensity to spread to brain. The time to progression was 16.2 months with exon 19 deletions versus 11.8 months in patients with l858R (p = 0.026) also, the overall survival was much longer in patients with exon-19 deletions than L858R (40.6 versus 23.9 months, p = 0.014).
Conclusion
There may be important differences between the primary tumor and metastases of lung adenocarcinoma regarding morphology, biomarker expression and genotype. The mutation status of metastases can differ from that of the primary tumor and also among metastases. The frequency of differences and the significance of the differences in pathologic variables between the primary tumors and metastases and also previously systemically treated tumors have also yet to be investigated.
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2017. CA Cancer J Clin. 2017;67:7–30.
Nguyen DX, Bos PD, Massague J. Metastasis: from dissemination to organ-specific colonization. Nat Rev Cancer. 2009;9:274–84.
Talmadge JE, Fidler IJ. AACR centennial series: the biology of cancer metastasis: historical perspective. Cancer Res. 2010;70:5649–69.
Ettinger DS, et al. NCCN guidelines insights: non-small cell lung cancer, version 4.2016. J Natl Compr Cancer Netw. 2016;14:255–64.
Irmisch A, Huelsken J. Metastasis: new insights into organ-specific extravasation and metastatic niches. Exp Cell Res. 2013;319:1604–10.
Pienta KJ, Robertson BA, Coffey DS, Taichman RS. The cancer diaspora: metastasis beyond the seed and soil hypothesis. Clin Cancer Res. 2013;19:5849–55.
Goncalves PH, et al. Risk of brain metastases in patients with nonmetastatic lung cancer: analysis of the metropolitan Detroit surveillance, epidemiology, and end results (SEER) data. Cancer. 2016;122:1921–7.
Reck M, et al. Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer. N Engl J Med. 2016;375:1823–33.
Dunant A, Pignon JP, Le Chevalier T. Adjuvant chemotherapy for non-small cell lung cancer: contribution of the international adjuvant lung trial. Clin Cancer Res. 2005;11:5017s–21s.
Oliver TW Jr, et al. Isolated adrenal masses in nonsmall-cell bronchogenic carcinoma. Radiology. 1984;153:217–8.
Pagani JJ. Normal adrenal glands in small cell lung carcinoma: CT-guided biopsy. AJR Am J Roentgenol. 1983;140:949–51.
Saad AG, et al. Immunohistochemical markers associated with brain metastases in patients with nonsmall cell lung carcinoma. Cancer. 2008;113:2129–38.
Schuette W. Treatment of brain metastases from lung cancer: chemotherapy. Lung Cancer. 2004;45:S253–7.
Gaspar LE, et al. Time from treatment to subsequent diagnosis of brain metastases in stage III non-small-cell lung cancer: a retrospective review by the Southwest Oncology Group. J Clin Oncol. 2005;23:2955–61.
Mamon HJ, et al. High risk of brain metastases in surgically staged IIIA non-small-cell lung cancer patients treated with surgery, chemotherapy, and radiation. J Clin Oncol. 2005;23:1530–7.
Pottgen C, et al. Prophylactic cranial irradiation in operable stage IIIA non small-cell lung cancer treated with neoadjuvant chemoradiotherapy: results from a German multicenter randomized trial. J Clin Oncol. 2007;25:4987–92.
Bradley JD, et al. Phase II trial of postoperative adjuvant paclitaxel/carboplatin and thoracic radiotherapy in resected stage II and IIIA non-small-cell lung cancer: promising long-term results of the Radiation Therapy Oncology Group--RTOG 9705. J Clin Oncol. 2005;23:3480–7.
Robnett TJ, Machtay M, Stevenson JP, Algazy KM, Hahn SM. Factors affecting the risk of brain metastases after definitive chemoradiation for locally advanced non-small-cell lung carcinoma. J Clin Oncol. 2001;19:1344–9.
Palmieri D, Chambers AF, Felding-Habermann B, Huang S, Steeg PS. The biology of metastasis to a sanctuary site. Clin Cancer Res. 2007;13:1656–62.
Aragon-Ching JB, Zujewski JA. CNS metastasis: an old problem in a new guise. Clin Cancer Res. 2007;13:1644–7.
Ferrigno D, Buccheri G. Cranial computed tomography as a part of the initial staging procedures for patients with non-small-cell lung cancer. Chest. 1994;106:1025–9.
Shen KR, Meyers BF, Larner JM, Jones DR. Special treatment issues in lung cancer: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132:290S–305S.
Shi AA, et al. Does initial staging or tumor histology better identify asymptomatic brain metastases in patients with non-small cell lung cancer? J Thorac Oncol. 2006;1:205–10.
Tanvetyanon T, Boyle TA. Clinical implications of genetic heterogeneity in multifocal pulmonary adenocarcinomas. J Thorac Dis. 2016;8:E1734–8.
Wu C, et al. High discrepancy of driver mutations in patients with NSCLC and synchronous multiple lung ground-glass nodules. J Thorac Oncol. 2015;10:778–83.
Schneider F, et al. Morphological and molecular approach to synchronous non-small cell lung carcinomas: impact on staging. Mod Pathol. 2016;29:735–42.
Benedettini E, et al. Met activation in non-small cell lung cancer is associated with de novo resistance to EGFR inhibitors and the development of brain metastasis. Am J Pathol. 2010;177:415–23.
Schmid K, et al. EGFR/KRAS/BRAF mutations in primary lung adenocarcinomas and corresponding locoregional lymph node metastases. Clin Cancer Res. 2009;15:4554–60.
Heon S, et al. Development of central nervous system metastases in patients with advanced non-small cell lung cancer and somatic EGFR mutations treated with gefitinib or erlotinib. Clin Cancer Res. 2010;16:5873–82.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Chirieac, L.R. (2018). Biology of Lung Cancer Metastases. In: Cagle, P., et al. Precision Molecular Pathology of Lung Cancer. Molecular Pathology Library. Springer, Cham. https://doi.org/10.1007/978-3-319-62941-4_16
Download citation
DOI: https://doi.org/10.1007/978-3-319-62941-4_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-62940-7
Online ISBN: 978-3-319-62941-4
eBook Packages: MedicineMedicine (R0)