Abstract
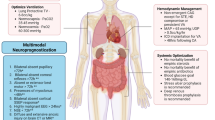
This chapter will review the elements of cardiac arrest resuscitation that begin after return of spontaneous circulation (ROSC). In-hospital mortality of patients who achieve ROSC long enough to be admitted to an ICU averages 60 % with wide inter-institutional variability (40–80 %) (Carr et al. Resuscitation 80:30–34, 2009). The pathophysiology of post-cardiac arrest syndrome (PCAS) is composed of four major components: post-cardiac arrest brain injury, post-cardiac arrest myocardial dysfunction, systemic ischemia/reperfusion response, and persistent precipitating pathology (Neumar et al. Circulation 118(23):2452–2483, 2008). It is important to recognize that each component is potentially reversible and responsive to therapy. A comprehensive multidisciplinary management strategy that addresses all components of post-cardiac arrest syndrome is needed to optimize patient outcomes (Callaway et al. Circulation 132(Suppl 1):S465–S482, 2015). In addition, a reliable strategy to prognosticate neurologic outcome in persistently comatose patients is essential to prevent premature limitation of care and make possible appropriate stewardship of patient care resources (Callaway et al. Circulation 132(Suppl 1):S465–S482, 2015).
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Cardiac Arrest
- Post Cardiac Arrest Syndrome
- Targeted Temperature Management
- Percutaneous Coronary Intervention
- Cardiogenic Shock
- Goal-Directed Resuscitation
- Neuroprognostication
Introduction
This chapter will review the elements of cardiac arrest resuscitation that begin after return of spontaneous circulation (ROSC). In-hospital mortality of patients who achieve ROSC long enough to be admitted to an ICU averages 60 % with wide inter-institutional variability (40–80 %) [1]. The pathophysiology of post-cardiac arrest syndrome (PCAS) is composed of four major components: post-cardiac arrest brain injury, post-cardiac arrest myocardial dysfunction, systemic ischemia/reperfusion response, and persistent precipitating pathology [2]. It is important to recognize that each component is potentially reversible and responsive to therapy. A comprehensive multidisciplinary management strategy that addresses all components of post-cardiac arrest syndrome is needed to optimize patient outcomes [3]. In addition, a reliable strategy to prognosticate neurologic outcome in persistently comatose patients is essential to prevent premature limitation of care and make possible appropriate stewardship of patient care resources [3].
Case Presentation
A 68-year old male was mowing his lawn, complained to his wife that he was having chest pain and then collapsed. She called “911” and when first responder EMTs arrived 5 min later, they found him to be unresponsive, not breathing and without a pulse. EMTs initiated cardiopulmonary resuscitation (CPR) and an automated external defibrillator (AED) was applied to the patient. The initial rhythm analysis advised a “shock”, and a shock was delivered. After two additional minutes of CPR the paramedics arrived and found the patient to have a palpable pulse, a systolic blood pressure of 70 mmHg, a narrow complex sinus tachycardia at a rate of 110 on the monitor, and agonal respirations. Prior to transport, a supraglottic airway was placed, bag-valve ventilation was performed using 100 % oxygen, an intravenous line was placed and 1-L normal saline bolus was initiated. Time from 911 call to return of spontaneous circulation (ROSC) was 9 min.
On arrival to the local hospital, the patient became pulseless again and the monitor revealed a rhythm of ventricular fibrillation. The patient was defibrillated with a biphasic defibrillator set at 200 J. Patient achieved return of spontaneous circulation (ROSC) with narrow complex tachycardia at a rate of 120 and a blood pressure of 75/40. The patient was given 500 cc IV crystalloid bolus and epinephrine infusion was initiated at titrated to MAP >65 mmHg. A femoral arterial line and an internal jugular central venous line were placed. Endotracheal intubation was performed and placement confirmed with waveform capnography and the PetCO2 was 40 mmHg. The patient had no eye opening or motor response to painful stimuli and pupils were fixed and dilated. Arterial blood gas demonstrated the following: pH = 7.18 PCO2 = 39 HCO3 − = 16 PaO2 = 340, SpO2 = 100 %, Lactate = 4.0. FiO2 was decreased to achieve SpO2 94–96 %. A temperature sensing bladder catheter was placed and read 36.0 °C. A 12 lead ECG was immediately obtained (Fig. 2.1).
Question
What interventions should be performed next?
Answer
Immediate coronary angiography with percutaneous coronary intervention (PCI) and hypothermic targeted temperature management.
Twelve-lead ECG reveals an acute anteroseptal ST-segment elevation myocardial infarction (STEMI). The patient’s history of chest pain and recurrent episodes of VF support acute coronary syndrome (ACS) as the cause of cardiac arrest. Cardiology was consulted and patient was taken immediately to the coronary catheterization lab. Coronary angiography revealed left anterior descending artery occlusion that was successfully treated with balloon angioplasty and stent placement (Fig. 2.2).
An intravascular cooling catheter placed in coronary angiography laboratory and target temperature was set at 33 °C. Patient was admitted to the cardiac ICU and hypothermic targeted temperature management was maintained for 24 h followed by rewarming to 37 °C over 16 h (0.25 °C/h). Sedation included propofol and fentanyl infusion. Continuous EEG revealed a reactive baseline with intermittent seizure activity after rewarming that was treated with IV lorazepam and valproic acid. Seventy-two hours after rewarming neurologic exam revealed reactive pupil and positive cornea reflex, with withdrawal from painful stimuli. Patient began following commands 96 h after rewarming and was extubated on the 6th admission day. He was discharged to short-term rehabilitation on the ninth day with neurologic deficits limited to mild short-term memory deficit.
Principles of Management
Overview of Post-cardiac Arrest Syndrome
Post cardiac arrest syndrome is a unique pathologic state where varying degrees of post-arrest brain injury, myocardial dysfunction, systemic ischemia and reperfusion response, and persistent precipitating pathology are observed [2]. The severity of these manifestations will vary in each patient. When ROSC is achieved rapidly PCAS can be limited or even absent while prolonged cardiac arrest can result in PCAS that is refractory to all interventions. Between these two extremes, each component of PCAS when present is potentially treatable and reversible. Some post-cardiac arrest interventions, such as hypothermic-targeted temperature management, appear to have a favorable impact on multiple components of PCAS while more focused interventions such at early PCI specifically address the precipitating pathology. A comprehensive multidisciplinary approach that addresses all PCAS components in the appropriate timeframe is the best strategy to optimize outcomes.
Post Cardiac Arrest Brain Injury
Post-cardiac arrest brain injury is a common cause of morbidity and mortality. One study reported that brain damage was the cause of death in 68 % of patients that died after ICU admission following out-of hospital cardiac arrest and in 23 % of patient that died after ICU admission following in-hospital cardiac arrest [4]. The unique vulnerability of the brain is attributed to its limited tolerance of ischemia as well as unique response to reperfusion. The most vulnerable regions of the brain include the hippocampus, cerebellum, caudoputamen, and cortex. The mechanisms of brain damage triggered by cardiac arrest and resuscitation are complex, and many pathways are executed over hours to days following ROSC. The relatively protracted time course of injury cascades and histological changes suggests a broad therapeutic window for neuroprotective strategies following cardiac arrest. Early clinical manifestations include coma, seizures, myoclonus and late manifestations ranging from mild short-term memory deficits to persistent vegetative state and brain death.
Post-cardiac Arrest Myocardial Dysfunction
Post-cardiac arrest myocardial dysfunction is a significant cause of morbidity and mortality after both in- and out-of-hospital cardiac arrest [4–6]. Myocardial dysfunction is manifest by tachycardia, elevated left ventricular end-diastolic pressure, decreased ejection fraction, reduced cardiac output and hypotension. Cardiac output tends to improve by 24 h and can return to near normal by 72 h in survivors in the absence of other pathology [6]. The responsiveness of post-cardiac arrest global myocardial dysfunction to inotropic drugs is well documented in animal studies [7, 8]. If acute coronary syndrome or decompensated congestive heart failure were the precipitating pathology that caused cardiac arrest, the management of post-cardiac arrest myocardial dysfunction becomes more complex.
Systemic Ischemia/Reperfusion Response
The whole body ischemia/reperfusion of cardiac arrest with associated oxygen debt causes generalized activation of immunological and coagulation pathways increasing the risk of multiple organ failure and infection [9, 10]. This condition has many features in common with sepsis [11–14]. In addition, activation of blood coagulation without adequate activation of endogenous fibrinolysis may also contribute to microcirculatory reperfusion disorders after cardiac arrest [15, 16]. Finally, the stress of total body ischemia/reperfusion appears to adversely affect adrenal function [17, 18]. However, the relationship of adrenal dysfunction to outcome remains controversial. Clinical manifestations of systemic ischemic-reperfusion response include intravascular volume depletion, impaired vasoregulation, impaired oxygen delivery and utilization, as well as increased susceptibility to infection.
Persistent Precipitating Pathology
Post-cardiac arrest syndrome is commonly associated with persisting acute pathology that caused or contributed to the cardiac arrest itself. The diagnosis and treatment of acute coronary syndrome, pulmonary diseases, hemorrhage, sepsis, and various toxidromes is often complicated in the setting of post-cardiac arrest syndrome. However, early identification and effective therapeutic intervention is essential if optimal outcomes are to be achieved.
Hemodynamic Optimization
Post-cardiac arrest patients typically exhibit a mixed cardiogenic, distributive, and hypovolemic state of shock. In addition, persistence of the pathology that caused the cardiac arrest can cause a refractory shock state unless definitively treated. Early hemodynamic optimization is essential to prevent re-arrest, secondary brain injury and multi-organ failure. A goal-directed approach using physiologic parameters to achieve adequate oxygen delivery has been associated with improved outcomes [19, 20]. This involves optimizing preload, arterial oxygen content, afterload, ventricular contractility, and systemic oxygen utilization. Appropriate monitoring includes continuous intra-arterial pressure monitoring, arterial and central venous blood gases, urine output, lactate clearance, and bedside echocardiography. When feasible, diagnostic studies to rule out treatable persistent precipitating pathology should be performed, and treatment initiated while resuscitation is ongoing.
The optimal MAP for post-cardiac arrest patients has not been defined by prospective clinical trials, and should be individualize for each patient. Cerebrovascular auto regulation can be disrupted or right-shifted in post-cardiac arrest patients suggesting a higher cerebral perfusion pressure is needed to provide adequate brain blood flow [21]. In contrast, ongoing ACS and congestive heart failure can be exacerbated by targeting a MAP higher than what is needed to maintain adequate myocardial perfusion. Higher systolic and mean arterial pressures during the first 24 h after ROSC are associated with better outcomes in descriptive studies [22–24]. In terms of goal-directed strategies, good outcomes have been achieved in published studies where the MAP target range was low as 65–75 mmHg [20] to as high as 90–100 mm [25, 26] for patients admitted after out-of-hospital cardiac arrest.
For patients with evidence of inadequate oxygen delivery or hypotension, preload optimization is the first line intervention. Preload optimization is typically achieved using IV crystalloid boluses guided by non-invasive bedside assessment of volume responsiveness. Patients treated with a goal-directed volume resuscitation strategy following out-of-hospital cardiac arrest typically have positive fluid balance of 2–3 in the first 6 h and 4–6 L positive fluid balance in the first 24 h [19, 20].
Vasopressor and inotrope infusions should be initiated early in severe shock states and when there is an inadequate response to preload optimization. No agent or combination of agents has been demonstrated to be superior or improve outcomes. A reasonable approach is norepinephrine as the first line vasopressor supplemented by dobutamine for inotropic support guided by bedside echocardiography.
When shock is refractory to preload optimization, vasopressors, and inotropes it is critical to identify and treat any persistent acute pathology that caused the cardiac arrest including acute coronary syndrome (ACS), pulmonary embolism (PE), or hemorrhage. If no such persistent pathology exists or the patient is not stable enough to undergo definitive intervention, then mechanical circulatory support should be considered (see section “Evidence Contour”).
Ventilation and Oxygenation
The ventilation and oxygenation goals for post-cardiac arrest patients should be normoxia and normocarbia. Both low (<60 mmHg) and high (>300 mmHg) arterial PO2 are associated with worse outcomes in post-cardiac arrest patients [27]. Low PaO2 can cause secondary brain hypoxia while high PaO2 can increase oxidative injury in the brain. The impact of PaCO2 on cerebrovascular blood flow is maintained in post-cardiac arrest patients; therefore hypocarbia can cause secondary brain ischemia and is associated with worse outcomes [28, 29]. Currently there are no studies to specify which ventilator modes or tidal volumes are optimal in patients resuscitated from cardiac arrest but generally an approach using assist control mode with a tidal volume goal in 6–8 cc/kg range is considered standard. Titration of mechanical ventilation should be aimed at achieving a PaCO2 of 45 mmHg and a range for PaO2 between 75 and 150 mmHg.
Management of STEMI and ACS
Acute coronary syndrome is a common cause of out-of-hospital cardiac arrest, but making the diagnosis in an unconscious post-arrest patient presents unique challenges. A previous history of coronary artery disease, significant risk factors, and/or symptoms prior to arrest can contribute to clinical suspicion, but the absence of these does not exclude ACS as the cause. A standard 12-lead ECG should be obtained as soon as feasible after ROSC, with additional right-sided and/or posterior leads as indicated. Immediate PCI is indicated in post-ROSC patients meeting STEMI criteria regardless of neurologic status [3]. In addition, immediate coronary angiography should be considered in post-cardiac arrest patients that do not meet STEMI criteria but there is a high clinical suspicion for ACS (see section “Evidence Contour”). Medical management of ACS is the same as for non-post-cardiac arrest patients.
Hypothermic Targeted Temperature Management
Hypothermic-targeted temperature management (HTTM) is recommended for comatose adult patients who achieve ROSC following cardiac arrest independent of presenting cardiac rhythm (shockable vs. non-shockable) and location (Out of Hospital Cardiac Arrest (OHCA) vs. In-hospital Cardiac Arrest (IHCA)) [3]. Based on current clinical evidence, providers should select a constant target temperature between 32 and 36 °C and maintain that temperature for at least 24 h. Rewarming should be no faster than 0.5 C/h and fever should be prevented for at least 72 h after ROSC.
Although there are no absolute contraindications to HTTM after cardiac arrest, relative contraindications may include uncontrolled bleeding or refractory severe shock. Induction of hypothermia may lead to intense shivering, hyperglycemia, diuresis and associated electrolyte derangements such as hypokalemia and hypophosphatemia [30]. Rewarming may be associated with mild hyperkalemia and must be monitored closely.
When the decision is made to treat the comatose post-cardiac arrest patient with HTTM, efforts to achieve and maintain target temperature should be as soon as feasible. In the ED, practical methods of rapidly inducing hypothermia include ice packs (applied to the neck, inguinal areas, and axilla), fan cooling of dampened exposed skin, cooling blankets underneath and on top of the patient, and disabling of ventilator warming circuits. Rapid intravenous infusion of limited volumes (1–2 L) of 4 °C saline facilitates induction of hypothermia, but additional measures are needed to maintain hypothermia. No one cooling strategy or device has been demonstrated to result in superior clinical outcomes. A number of automated surface cooling devices are now available that use chest and thigh pads and continuous temperature feedback from bladder or esophageal temperature probes. Although more invasive, automated endovascular cooling systems are also available that require placement of a central venous catheter and offer tighter control of temperature at target. Target core body temperature is best monitored by an indwelling esophageal temperature probe, but can be monitored by a temperature-sensitive bladder catheter if adequate urine output is present.
Shivering, which inhibits cooling, can be prevented with sedation and neuromuscular blockade. If neuromuscular blockade is continued during the maintenance phase of therapeutic hypothermia, continuous electroencephalographic monitoring is strongly encouraged to detect seizures, a common occurrence in post-cardiac arrest patients [3].
Glucose Control
Hyperglycemia is common in post-cardiac arrest patients, and average levels above 143 mg/dL have been strongly associated with poor neurologic outcomes [31]. One randomized trial in post-cardiac arrest patients compared strict (72–108 mg/dL) versus moderate (108–144 mg/dL) glucose control and found no difference in 30-day mortality [32]. Based on available evidence, moderate glucose management strategies in place for most critically ill patients do not need to be modified for post-cardiac arrest patients.
Seizure Management
Seizures, nonconvulsive status epilepticus, and other epileptiform activity occurs in 12–22 % of comatose post-cardiac arrest patients, and may contribute to secondary brain injury and prevent awaking from coma [3]. There is no direct evidence that post-cardiac arrest seizure prophylaxis is effective or improves outcomes. However, prolonged epileptiform discharges are associated with secondary brain injury in other conditions, making detection and treatment of nonconvulsive status epilepticus a priority [33]. Continuous EEG, initiated as soon as possible following ROSC, should be strongly considered in all comatose survivors of cardiac arrest treated with HTTM, to monitor for potentially treatable electrographic status epilepticus and to assist with neuroprognostication. In the absence of continuous EEG monitoring, an EEG for the diagnosis of seizure should be promptly performed and interpreted in comatose post-arrest patients. The same anticonvulsant regimens for the treatment of seizures and status epilepticus and myoclonus caused by other etiologies are reasonable to use in post-cardiac arrest patients.
Neuroprognostication
Accurate neuroprognostication can be extremely challenging in persistently comatose post-cardiac arrest patients, but is essential for appropriate patient care and resource utilization. Decisions to limit care based on neurologic prognosis should not be made before 72 h after ROSC and at least 12 h following rewarming and cessation of all sedative and paralytic medications [34]. Available neuroprognostication tools include clinical examination, electrophysiologic measurements, imaging studies, and serum biomarkers. The performance of these tools is highly dependent on the interval between the achievement of ROSC and the measurement. For example, bilateral absence of pupillary light reflex has a false positive rate (FPR) for predicting poor neurologic outcome of 32 % [95 % CI 19–48 %] at the time of hospital admission versus a FPR of 1 % [0–3 %] when measured 72 h after ROSC [35]. In addition to timing, major confounders such as sedation and neuromuscular blockade, persistent hypothermia, severe hypotension, hypoglycemia and other profound metabolic derangements must be excluded before an assessment for neuroprognostication is performed. Finally, all available clinical data on the reliability of prognostication tools is limited by the potential for a self-fulfilling prophecy that occurs when these tools are used to limit care.
Most experts agree that recovery of Glasgow Motor Score (GMS) of flexion or better (i.e. >2) is a good prognostic sign that precludes the need for further prognostic evaluation. In patients that do not recover a GMS >2 by 72 h after ROSC, the most reliable predictors of poor neurologic outcome (defined by a Cerebral Performance Category score of 3–5) are listed in Table 2.1.
It is recommended that decisions to limit care never be based on the results of a single prognostication tool [3]. Although a number of published guidelines from professional societies are available, the field is rapidly evolving and therefore post-arrest neuroprognostication should be guided by consultation with an experienced neurocritical care specialist [34, 37]. Establishing a consistent institutional approach based on available resources and multidisciplinary expertise will optimize both resource utilization and patient outcomes.
Organ Donation
Patients that are initially resuscitated from cardiac arrest but subsequently die or meet brain death criteria should be evaluated as potential organ donors. Multiple studies have found no difference in immediate or long-term function of transplanted organs from donors who reach brain death after cardiac arrest when compared with donors who reach brain death from other causes [38]. In addition, patients who have withdrawal of life support after initial resuscitation from cardiac arrest based on reliable neuroprognostication of futility or as part of advanced directives are candidates for donation after cardiac death (DCD). The list of potential organs successfully donated from the patients has expanded from primarily kidneys and liver to include heart, lung and intestine. Finally, tissue donation (cornea, skin, and bone) is almost always possible if post-cardiac arrest patients die.
Evidence Contour
Patient Selection for Emergency Coronary Angiography
There are no prospective randomized controlled trials demonstrating benefit of immediate coronary angiography and PCI in post-cardiac arrest patients with or without STEMI. However, multiple observational studies have reported better survival in both STEMI and NSTEMI post-cardiac arrest patients that undergo immediate coronary angiography and PCI (when indicated) compared to those that do not undergo immediate coronary angiography [39–41]. The strength of the recommendation for post-cardiac arrest patients that meet STEMI criteria is based on extrapolation of the positive survival benefits for non-cardiac arrest patients. Conversely, the reluctance of interventional cardiologists to perform immediate coronary angiography in NSTEMI patients is similarly based on lack of proven benefit in non-cardiac arrest patients. However, it should be recognized that the post-arrest patients are higher risk and do not always have ST-elevation with an acutely occluded culprit lesion [42]. In a large international post-cardiac arrest registry that included patients undergoing immediate coronary angiography with and without STEMI, an occluded culprit vessel was found in 74.3 % of patients with STEMI and 22.9 % of patients without STEMI [41]. This high incidence of occluded culprit lesions combined with post-cardiac arrest myocardial dysfunction and the need to maintain adequate cerebral perfusion pressure to prevent secondary brain injury argues strongly for immediate coronary angiography in any post-cardiac arrest patient when there is a clinical suspicion of ACS, especially when associated with hemodynamic instability.
Patient Selection for Hypothermic TTM
Although international guidelines consistently recommend treating all comatose post-cardiac arrest patients with hypothermic TTM, this practice has not been universally implemented. The two major clinical trials demonstrating efficacy of HTTM limited enrollment to witnessed out-of-hospital cardiac arrest with as shockable (VF/VT) presenting rhythm [26, 43]. There have been no prospective randomized clinical trials comparing HTTM to normothermia (or no active temperature management) in out-of-hospital cardiac arrest patients with non-shockable presenting rhythms or in in-hospital cardiac arrest patients with any presenting rhythm. Therefore these recommendations represent an extrapolation of the evidence in patients with witnessed out-of-hospital ventricular fibrillation. This extrapolation is supported by clinical observational studies that suggest benefit in these patient populations and robust body animal data demonstrating the neuroprotective effect of HTTM in cardiac arrest models regardless of arrest rhythm [44, 45]. In addition, HTTM has a relatively safe side effect profile limited primarily to shivering and electrolyte shifts. For intubated comatose cardiac arrest survivors managed in the ICU setting, the incremental intensity of care and cost is modest. One potential concern about treating all comatose post-cardiac arrest patients with HTTM is a delay in prognostication of poor outcome and decision to limit care. However, there is international consensus that neuroprognostication should not be performed before 72 after ROSC. So, awaiting completion of HTTM therapy does itself delay neuroprognostication. Moreover, HTTM could delay the metabolism of sedative and paralytic agents. Therefore, some experts have recommended delaying prognostication until 72 h after rewarming, which could cause significant delays in neuroprognostication. However, the initiation of HTTM should not impact decisions to limit care that are based criteria other than neurologic prognosis, such as terminal illness or previously unrecognized advanced directives. In such cases the decision to discontinue HTTM can be considered in the same way as the decision to discontinue mechanical ventilation or intravenous pressor therapy.
Optimizing Hypothermic TTM
Most experts agree that the optimal time to initiation, target temperature, and duration of HTTM is unknown. Although it theoretically makes sense to achieve target temperature as soon as feasible, there is no clinical data to support this approach. Even in the two landmark clinical trials, the time to target temperature was discordant. In the study by Bernard the time to target temperature was reported to be ≤2 h while in the HACA trial the median time to target temperature was 8 h (IQR 4–16 h) [26, 43]. Rapid infusion of cold intravenous saline immediately after ROSC by paramedics in the field had no impact on outcomes in two randomized clinical trials [46, 47]. Observational studies examining time to target temperature are not informative because neurologically devastated patients are easier to cool due to loss of temperature auto regulation. Based on available evidence achieving target temperature within 4 h of ROSC is a reasonable goal.
The target temperature of 32–34 °C in the original guidelines was based on the target temperature used in the Bernard and HACA studies [26, 43]. Subsequent to that, a large multicenter studied published by Nielsen et al. did not detect superior outcomes in comatose post-cardiac arrest patients who were cooled to 33 °C compared to 36 °C [48]. It is for this reason that the recommended target temperature range was expanded to 32–36 °C. Although it is theoretically easier to use a higher target temperature, it does not obviate the need for use of active cooling techniques guided by continuous temperature monitoring. The recommended duration of therapy is again based on the durations used in major clinical trials. There have been no prospective comparisons of HTTM duration in randomized clinical trials. No specific cooling technique has been demonstrated to result in superior patient outcomes. Therefore the best strategy is the one that is most feasible to consistently implement at your own institution. Overall, the optimization of HTTM requires additional research, and it is likely that a personalized approach based on severity of injury and response to therapy will emerge as the best strategy.
Mechanical Support for Refractory Post-cardiac Arrest Cardiogenic Shock
In post-cardiac arrest patients with refractory cardiogenic shock a number of options can be considered for mechanical circulatory support. An intra-aortic balloon pump can enhance cardiac output by approximately 0.5 L/min in cardiogenic shock. Despite early evidence of improved outcomes when IABP was used post-MI, recent studies have not shown a 30-day or 12 month mortality benefit [49, 50]. The newer peripheral ventricular assist devices Tandem HeartTM PVAD (Fig. 2.3) and ImpellaTM Recovery (Fig. 2.4) are reported to augment cardiac output by 3.5 and 2.5 L/min, respectively. These devices gain access to the central circulation via large cannulas, which then use either a centrifugal pump (Tandem HeartTM) or catheter motor with inlet and output (ImpellaTM) via the aorta. In centers with specialty expertise complete circulatory support may be performed using veno-arterial extracorporeal membrane oxygenation (VA-ECMO) as a bridge to transplantation or bridge to recovery [51].
References
Carr B, Kahn J, Merchant RM. Inter-hospital variability in post-cardiac arrest mortality. Resuscitation. 2009;80:30–4.
Neumar R, Nolan JP, Adrie C. Post-Cardiac Arrest Syndrome: epidemiology, pathophysiology, treatment, and prognostication. A consensus statement from the International Liaison Committee on Resuscitation (American Heart Association, Australian and New Zealand Council on Resuscitation, European Resuscitation Council, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Council of Asia, and the Resuscitation Council of Southern Africa). Circulation. 2008;118(23):2452–83.
Callaway C, Donnino M, Fink E. Post Cardiac Arrest Care: 2015 American Heart Association Guidelines Update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2015;132 Suppl 1:S465–82.
Laver S, Farrow C, Turner D. Mode of death after admission to an intensive care unit following cardiac arrest. Intensive Care Med. 2004;30:2126–8.
Herlitz J, Ekstrom B, Wennerblom B. Hospital mortality after out-of-hospital cardiac arrest among patients found in ventricular fibrillation. Resuscitation. 1995;29(1):11–21.
Laurent I, Monchi M, Chiche J. Reversible myocardial dysfunction in survivors of out-of-hospital cardiac arrest. J Am Coll Cardiol. 2002;40(1):2110–6.
Kern KB, Hilwig R, Berg RA. Postresuscitation left ventricular systolic and diastolic dysfunction: treatment with dobutamine. Circulation. 1997;95(12):2610–3.
Huang L, Weil M, Tang W. Comparison between dobutamine and levosimendan for management of postresuscitation myocardial dysfunction. Crit Care Med. 2005;33(3):487–91.
Cerchiari E, Safar P, Klein E. Visceral, hematologic and bacteriologic changes and neurologic outcome after cardiac arrest in dogs. The visceral post-resuscitation syndrome. Resuscitation. 1993;25:119–36.
Adams J. Endothelium and cardiopulmonary resuscitation. Crit Care Med. 2006;34(12):S45–465.
Adrie C, Adib-Conquy M, Laurent I. Successful cardiopulmonary resuscitation after cardiac arrest as a “sepsis-like” syndrome. Circulation. 2002;106(5):562–8.
Adrie C, Laurent I, Monchi M. Postresuscitation disease after cardiac arrest: a sepsis-like syndrome? Curr Opin Crit Care. 2004;10(3):208–12.
Gando S, Nanzaki S, Morimoto Y. Out-of-hospital cardiac arrest increases soluble vascular endothelial adhesion molecules and neutrophil elastase associated with endothelial injury. Intensive Care Med. 2000;26(1):38–44.
Geppert A, Zorn G, Karth G. Soluble selectins and the systemic inflammatory response syndrome after successful cardiopulmonary resuscitation. Crit Care Med. 2000;28(7):2360–5.
Bottinger B, Motsch J, Bohrer H. Activation of blood coagulation after cardiac arrest is not balanced adequately by activation of endogenous fibrinolysis. Circulation. 1995;92(9):2572–8.
Adrie C, Monchi M, Laurent I. Coagulopathy after successful cardiopulmonary resuscitation following cardiac arrest: implication of the protein C anticoagulant pathway. J Am Coll Cardiol. 2005;46(1):21–8.
Hekimian G, Baugnon T, Thuong M. Cortisol levels and adrenal reserve after successful cardiac arrest resuscitation. Shock. 2004;22(2):116–9.
Schultz C, Rivers EP, Feldkamp C. A characterization of hypothalamic-pituitary-adrenal axis function during and after human cardiac arrest. Crit Care Med. 1993;21(9):1339–47.
Gaieski DF, et al. Early goal directed hemodynamic optimization combined with therapeutic hypothermia in comatose survivors of out-of-hospital cardiac arrest. Resuscitation. 2009;80:418–24.
Sunde K, Pytte M, Jacobsen D. Implementation of a standardised treatment protocol for post resuscitation care after out-of-hospital cardiac arrest. Resuscitation. 2007;73(1):29–39.
Sundgreen C, Larsen F, Herzog T. Autoregulation of cerebral blood flow in patients resuscitated from cardiac arrest. Stroke. 2001;32:128–32.
Kilgannon JH, et al. Early arterial hypotension is common in the post-cardiac arrest syndrome and associated with increased in-hospital mortality. Resuscitation. 2008;79(3):410–6.
Beylin ME, et al. Higher mean arterial pressure with or without vasoactive agents is associated with increased survival and better neurological outcomes in comatose survivors of cardiac arrest. Intensive Care Med. 2013;39(11):1981–8.
Kilgannon JH, et al. Arterial blood pressure and neurologic outcome after resuscitation from cardiac arrest. Crit Care Med. 2014;42:2083–91.
Oddo M, et al. From evidence to clinical practice: effective implementation of therapeutic hypothermia to improve patient outcome after cardiac arrest. Crit Care Med. 2006;34(7):1865–73.
Bernard S, et al. Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Engl J Med. 2002;346(8):557–63.
Kilgannon JH, et al. Association between arterial hyperoxia following resuscitation from cardiac arrest and in-hospital mortality. JAMA. 2010;303(21):2165–71.
Kagstrom E, Smith M, Siesjo B. Cerebral circulatory responses to hypercapnia and hypoxia in the recovery period following complete and incomplete cerebral ischemia in the rat. Acta Physiol Scand. 1983;118(3):281–91.
Buunk G, van der Hoeven JG, Meinders AE. Cerebrovascular reactivity in comatose patients resuscitated from a cardiac arrest. Stroke. 1997;28:1569–73.
Polderman K. Of ions and temperature: the complicated interplay of temperature, fluids, and electrolyte on myocardial function. Crit Care. 2013;17(6):1018.
Losert H, et al. Strict normoglycaemic blood glucose levels in the therapeutic management of patients within 12 h after cardiac arrest might not be necessary. Resuscitation. 2008;76(2):214–20.
Oksanen T, Skrifvars M, Varpula T. Strict versus moderate glucose control after resuscitation from ventricular fibrillation. Intensive Care Med. 2007;33(12):2093–100.
Friedman D, Claassen J, Hirsch L. Continuous electroencephelogram monitoring in the intensive care unit. Anesth Analg. 2009;109(2):506–23.
Sandroni C, et al. Prognostication in comatose survivors of cardiac arrest: an advisory statement from the European Resuscitation Council and the European Society of Intensive Care Medicine. Resuscitation. 2014;85:1779–89.
Callaway C, et al. Part 4: Advanced life support: 2015 International consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations [review]. Circulation. 2015;132(16 Suppl 1):S84–145.
Westhall E, Rossetti A, van Rootselaar A. Standardized EEG interpretation accurately predicts prognosis after cardiac arrest. Neurology. 2016;86(16):1482–90.
Cronberg T, Brizzi M, Liedholm L. Neurological prognostication after cardiac arrest – recommendations from the Swedish resuscitation Council. Resuscitation. 2013;84(7):867–72.
Orioles A, Morrison W, Rossano J. An under-recognized benefit of cardiopulmonary resuscitation: organ transplantation [review]. Crit Care Med. 2013;41(12):2794–9.
Callaway CW, et al. Early coronary angiography and induced hypothermia are associated with survival and functional recovery after out-of-hospital cardiac arrest. Resuscitation. 2014;85(5):657–63.
Dumas F, Bougouin W, Geri G. Is early PCI associated with a clinical benefit in post-cardiac arrest patients without STEMI pattern? Insights from the Parisian registry (PROCAT II). Resuscitation. 2015;96 Suppl 1:37.
Kern K, Lotun K, Patel N. Outcomes of comatose cardiac arrest survivors with and without ST-segment elevation myocardial infarction: importance of coronary angiography. JACC Cardiovasc Interv. 2015;8(8):1031–40.
Spaulding CM, et al. Immediate coronary angiography in survivors of out-of-hospital cardiac arrest. N Engl J Med. 1997;336(23):1629–33.
Hypothermia after Cardiac Arrest Study Group. Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N Engl J Med. 2002;346(8):549–56.
Testori C, Sterz F, Behringer W. Mild therapeutic hypothermia is associated with favourable outcomes in patients after cardiac arrest with non-shockable rhythms. Resuscitation. 2011;82(9):1162–7.
Perman S, Grossestreuer A, Wiebe D. The utility of therapeutic hypothemia for post-cardiac arrest syndrome patients with an initial nonshockable rhythm. Circulation. 2015;132(22):2146–51.
Bernard S, Smith K, Cameron P. Induction of therapeutic hypothermia by paramedics after resuscitation from out-of-hospital ventricular fibrillation cardiac arrest: a randomized controlled trial. Circulation. 2010;122(7):737–42.
Kim F, et al. Effect of prehospital induction of mild hypothermia on survival and neurological status among adults with cardiac arrest: a randomized clinical trial. JAMA. 2014;311(1):45–52.
Nielsen N, et al. Targeted temperature management at 33°C versus 36°C after cardiac arrest. N Engl J Med. 2013;369(23):2197–206.
Thiele H, et al. Intraaortic balloon support for myocardial infarction with cardiogenic shock. N Engl J Med. 2012;367:1287–96.
Thiele H, et al. Intra-aortic balloon counterpulsation in acute myocardial infarction complicated by cardiogenic shock (IABP-SHOCK II): final 12 month results of a randomised open-label trial. Lancet. 2013;382:1638–45.
Stub D, et al. Refractory cardiac arrest treated with mechanical CPR, hypothermia, ECMO and early reperfusion (the CHEER trial). Resuscitation. 2015;86:88–94.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Otero, R.M., Neumar, R.W. (2017). Post-cardiac Arrest Management. In: Hyzy, R. (eds) Evidence-Based Critical Care. Springer, Cham. https://doi.org/10.1007/978-3-319-43341-7_2
Download citation
DOI: https://doi.org/10.1007/978-3-319-43341-7_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-43339-4
Online ISBN: 978-3-319-43341-7
eBook Packages: MedicineMedicine (R0)