Abstract
Contrast-enhanced digital breast tomosynthesis (CEDBT) may improve contrast-enhanced lesion conspicuity and relative contrast quantification by improving three-dimensional visualization of lesion morphology, and reducing the integration of attenuation information along the axial direction. Improved visualization of patterns of contrast-enhancement and improved iodine quantification may help differentiate between malignant and benign enhancing lesions. The dependence of dual-energy contrast-enhanced lesion detectability on imaging chain design is investigated. Lesion detectability and relative iodine quantification is comparable for subtraction in either reconstruction or projection domains for both phantom and patient images. SART generally produces greater SDNR than FBP, and scatter correcting projections further improves SDNR.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
- Contrast-enhanced digital mammography
- Contrast-enhanced digital breast tomosynthesis
- Digital breast tomosynthesis
- X-ray imaging
- SDNR
1 Introduction
Contrast-enhanced digital mammography (CEDM) has been investigated recently to improve the conspicuity of mammographically occult breast pathologies. Similarly, contrast-enhanced digital breast tomosynthesis (CEDBT) has been proposed to improve breast cancer diagnosis by providing three-dimensional (3D) morphological information in addition to 3D physiological information through contrast-enhancement. A recent clinical study [1] showed superiority of CEDM, CEDBT and dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) over non-enhanced full-field digital mammography (FFDM) and non-enhanced DBT; however, none of the contrast-enhanced modalities was demonstrated to be superior to the others as assessed by the area under the receiver operating characteristic (ROC) curves.
While this result may suggest the addition of CEDBT to CEDM is unnecessary, this study did not report the specificity or false positive rate of any modality. Although numerous previous studies have reported sensitivities for CEDM ranging from 92 %−100 %, specificities are lower and more varied, ranging from 41 %−87 %, due to enhancement of benign pathologies [2–5].
The specificity of DCE-MRI similarly varies, however may be improved by the inclusion of additional factors to differentiate true and false positives. Differentiation of false positives from true positives in DCE-MRI is afforded by several characteristics; namely (1) accurate assessment of tumor margins, (2) observation of punctate or stippled enhancement of non-mass lesions, and (3) observation of contrast-kinetic curves [6].
Whereas planar mammography collapses all attenuation information to a single plane, DBT reduces this integrating effect by reconstructing projection images into a series of image slices, typically 1 mm thick, arranged parallel to the detector plane. This effectively reduces superposition of tissue structures, and provides improved localization of pathologies in 3D space. These results may provide CEDBT a technical advantage over CEDM in measuring all three benign/malignant differentiating characteristics.
First, the addition of 3D morphological information and reduction of superimposed structural noise provided by DBT has been shown to significantly improve tumor sizing and margin assessment. [7] Secondly, punctate or stippled enhancement patterns, generally indicative of benign fibrocystic changes, are characterized by multiple enhancing punctate foci 1−2 mm in diameter. [8] CEDBT may improve differentiation of these smaller individual foci from diffuse background parenchymal enhancement (BPE) by the addition of 3D information. Finally, while CEDM has been unable to reliably demonstrate contrast kinetic curves, initial results in CEDBT have shown promise. [9] By reducing the integration of signal from iodinated lesions along the axial direction, CEDBT may improve accurate quantification of iodinated lesions, and thus may improve observation of contrast kinetic information.
While the performance of DBT in identifying tumor margins has been investigated, further work remains in characterizing the performance of CEDBT in identifying small iodinated enhancements (stippled enhancement patterns) and accurately quantifying relative iodine concentration (kinetic curves).
We aim to investigate the ability of dual-energy CEDBT to identify small iodinated enhancements and accurately quantify relative iodine concentration, and the dependence of these tasks on imaging chain design. Specifically, lesion detectability, characterized by object signal-difference-to-noise-ratio (SDNR), is measured for dual-energy subtracted 3D CEDBT phantom images. Imaging chain design, including various image processing and reconstruction strategies, are investigated. We investigate iodine quantification by correlating iodine SDNR with known iodine concentration.
Additionally, SDNR for iodinated lesions is characterized for initial patients in an Institutional Review Board-approved clinical study. CEDBT datasets acquired for these patients are similarly processed and SDNR characterized with different imaging chain designs.
2 Methods
2.1 Image Acquisition
All image acquisitions were performed on a Siemens MAMMOMAT Inspiration Digital Breast Tomosynthesis prototype, modified for dual-energy contrast-enhanced imaging. The x-ray source is capable of producing 49 kVp x-ray beams and is equipped with a tungsten anode with a rhodium (Rh) filter and titanium (Ti) or copper (Cu) filters for low- and high-energy imaging, respectively. The amorphous selenium (a-Se) flat panel imager has also been designed for dual-energy imaging, wherein the photoconductor thickness has been increased from 200 µm to 300 µm to improve detective quantum efficiency at high energies.
2.2 Phantom Image Acquisition
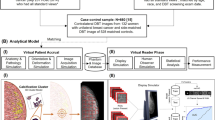
Phantom imaging was performed using a CIRS (Norfolk, VA) model 020 BR3D breast simulating phantom with a custom solid iodine feature plate (see Fig. 1). This insert contains 16 cylindrical objects of four diameters (2, 3, 5 and 8 mm) and four concentrations of iodine (1, 2, 3 and 5 mg/ml). Four 1-cm tissue simulating slices were used, including the 1-cm solid iodine insert, for a total phantom thickness for 4 cm. Low- and high energy DBT scans of the phantom were acquired using W/Rh 28 kVp and W/Cu 49 kVp spectra, with approximately equal mean glandular doses (MGD) assigned to low- and high-energy scans, for a total MGD of 1.5 mGy. [10] The phantom was not moved and compression was maintained between scans.
2.3 Patient Image Acquisition
Three patients with BI-RADS 4-5 suspicious findings were recruited as part of an Institutional Review Board-approved clinical study investigating CEDBT. After obtaining informed consent, each patient was injected with 1.5−2.0 ml of iodinated contrast medium per kilogram body weight at a rate of 2 ml/sec using a power-injector. After approximately 2 min, the affected breast was positioned and minimally compressed (<5 daN). A pair of dual-energy CEDM and CEDBT images were subsequently acquired, with approximately 33 % of the total dose allocated to the high-energy acquisitions. Each of the four acquisitions was separated by approximately 30 s, for a total study time of approximately 4.5 min post-injection.
2.4 Imaging Chain Design
Dual-energy subtracted reconstructions were produced from the low- and high-energy projections through six different imaging chain designs (see Fig. 1). Subtraction was performed in either the reconstruction or projection domain. While subtraction in the projection domain may remove the effect of reconstruction artifacts on subtracted images, system geometry instability may result in misregistered projections. Reconstruction was performed using either filtered back-projection (FBP) or an ordered-subset simultaneous algebraic reconstruction technique (OS-SART). [11] In the case of SART reconstructions, raw projections were either corrected for scatter radiation using a previously described scatter correction algorithm [12] or left uncorrected. Scatter radiation, manifest as a low-frequency drop in the modulation transfer function and additive quantum noise at all spatial frequencies, may obscure iodinated lesions and prevent accurate quantification of iodine. Since the filters applied in FBP typically remove the effect of scatter radiation, scatter correction was not applied to projections used in FBP reconstructions (Fig. 2).
2.5 SDNR Analysis
In-plane SDNR of the solid iodine objects was measured for each dual-energy subtracted reconstruction as
where q O and q B represent the signal intensity in an ROI of equal size in an area of uniform object and background respectively, and σ B is the standard deviation of the pixel intensity in the ROI of background [13].
The dependence of object detectability on imaging chain design was investigated by measuring SDNR for iodine objects of every diameter; SDNR was similarly measured for iodinated lesions in patient images. Accuracy of relative iodine quantification was investigated by plotting phantom SDNR as a function of known iodine concentration and calculating the Pearson correlation coefficient r.
3 Results
3.1 Subtracted Reconstructions
Subtracted reconstructions were produced according to each of the six imaging strategies outlined for both phantom and patient datasets. Weighting factors w s were derived analytically [11] and tuned to produce maximal tissue cancelation (w s ± 0.1). Example phantom and patient reconstruction slices are presented in Fig. 3.
3.2 SDNR
SDNR was measured for each solid iodine insert in each dual-energy subtracted phantom reconstruction. As shown in Fig. 4, subtracting in the reconstruction domain produced SDNR comparable to subtracting in the projection domain. SART generally outperformed FBP, except for very low iodine concentration targets (<2 mg/ml), where FBP and SART results were comparable. The application of a ramp filter in FBP reduces contrast, thus degrading SDNR. Scatter correcting projections before SART reconstruction improved SDNR especially for low iodine concentrations (<3 mg/ml), though this is likely due to the placement of these low concentration objects at the center of the phantom, where scatter radiation is greatest. Iodinated lesion SDNR was similarly measured for each subtracted reconstruction for each of the three patients imaged (see Fig. 5); similar trends were observed, with no advantage of subtraction in one domain over the other.
SDNR of embedded iodine inserts in the phantom, measured for each subtraction scheme. Subtraction in reconstruction domain was essentially equivalent to subtraction in projection domain. SART (A2-A3/B2-B3) generally outperformed FBP when subtracting in either domain. Scatter correcting projections (A3/B3) before SART reconstruction improved SDNR in all cases.
SDNR of iodinated masses in each of three patients imaged with CEDBT. SART reconstruction outperformed FBP in all cases; scatter corrected projections increased SDNR in SART reconstructions. Subtraction in reconstruction domain was essentially equivalent to subtraction in projection domain. Data from Patient A could not be scatter corrected due to technical limitations of the correction algorithm.
Accuracy of relative iodine quantification was investigated by plotting SDNR as a function of iodine concentration; data were linearly fitted and Pearson’s correlation coefficients r were calculated (see Fig. 6). Each algorithm performed nearly identically when comparing subtraction domains. Good correlation (r > 0.98) was seen for all imaging chain designs.
Measured SDNR of 8 mm iodine objects for each subtraction scheme. Data were linearly fitted and Pearson correlation coefficients were calculated; r > 0.98 was demonstrated in all cases. Subtraction schemes in corresponding subtraction domains (e.g., A1/B1) produced virtually identical SDNR results, and thus appear to overlap in the plot.
4 Discussion
Subtraction in the reconstruction domain was shown to produce essentially equivalent iodine SDNR when compared with subtraction in the projection domain for both phantom and patient images. While subtraction in either domain is thus feasible, subtraction in the reconstruction domain may allow for faster interleaved scans in which alternating low- and high-energy projections are acquired during a single scan, from which low- and high-energy reconstructions are generated and subsequently subtracted. [13] Further, patient motion did not result in low- and high-energy projection misregistration sufficient to impact SDNR.
SART was shown to generally outperform FBP, though judicious choice of reconstruction filters may improve FBP performance. Scatter correcting projections improves SDNR for SART reconstructions, with the greatest improvement for iodine targets at the center of the phantom, where scatter radiation is greatest.
Strong correlation between iodine concentration and SDNR was observed for subtraction in either projection or reconstruction domain for FBP, suggesting that accurate relative iodine quantification may be achievable for dynamic CEDBT.
Finally, while these results describe the impact of subtraction scheme on contrast-enhanced lesion SDNR, the effect on residual noise remains to be studied. Future work will investigate the impact of subtraction domain, reconstruction algorithm, scatter presence and the impact of appropriate weighting factor on residual structural noise.
References
Chou, C.-P., Lewin, J.M., Chiang, C.-L., Hung, B.-H., Yang, T.-L., Huang, J.-S., Liao, J.-B., Pan, H.-B.: Clinical evaluation of contrast-enhanced digital mammography and contrast enhanced tomosynthesis – comparison to contrast-enhanced breast MRI. Eur. J. Radiol. 84(12), 2501–2508 (2015)
Dromain, C., Thibault, F., Muller, S., Rimareix, F., Delaloge, S., Tardivon, A., Balleyguier, C.: Dual-energy contrast-enhanced digital mammography: initial clinical results. Eur. Radiol. 21, 565–574 (2011)
Jochelson, M.S., Dershaw, D.D., Sung, J.S., Heerdt, A.S., Thornton, C., Moskowitz, C.S., Ferrara, J., Morris, E.A.: Bilateral contrast-enhanced dual-energy digital mammography: feasibility and comparison with conventional digital mammography and MR imaging in women with known breast carcinoma. Radiology 266, 743–751 (2013)
Lobbes, M.B.I., Lalji, U., Houwers, J., Nijssen, E.C., Nelemans, P.J., Van Roozendaal, L., Smidt, M.L., Heuts, E., Wildberger, J.E.: Contrast-enhanced spectral mammography in patients referred from the breast cancer screening programme. Eur. Radiol. 24, 1668–1676 (2014)
Luczyńska, E., Heinze-Paluchowska, S., Dyczek, S., Blecharz, P., Rys, J., Reinfuss, M.: Contrast-enhanced spectral mammography: comparison with conventional mammography and histopathology in 152 women. Korean J. Radiol. 15, 689–696 (2014)
Baltzer, P.A.T., Benndorf, M., Dietzel, M., Gajda, M., Runnebaum, I.B., Kaiser, W.A.: False-positive findings at contrast-enhanced breast MRI: a BI-RADS descriptor study. Am. J. Roentgenol. 194, 1658–1663 (2010)
Förnvik, D., Zackrisson, S., Ljungberg, O., Svahn, T., Timberg, P., Tingberg, A., Andersson, I.: Breast tomosynthesis: accuracy of tumor measurement compared with digital mammography and ultrasonography. Acta Radiol. 51, 240–247 (2010)
Petralia, G., Bonello, L., Priolo, F., Summers, P., Bellomi, M.: Breast MR with special focus on DW-MRI and DCE-MRI. Cancer Imaging 11, 76–90 (2011)
Froeling, V., Diekmann, F., Renz, D.M., Fallenberg, E.M., Steffen, I.G., Diekmann, S., Lawaczeck, R., Schmitzberger, F.F.: Correlation of contrast agent kinetics between iodinated contrast-enhanced spectral tomosynthesis and gadolinium-enhanced MRI of breast lesions. Eur. Radiol. 23, 1528–1536 (2013)
Hu, Y.-H., Scaduto, D.A., Zhao, W.: Optimization of clinical protocols for contrast enhanced breast imaging. In: Nishikawa, R.M. Whiting, B.R. (eds.) SPIE Medical Imaging, p. 86680G. International Society for Optics and Photonics, Orlando, FL (2013)
Lu, Y., Peng, B., Scaduto, D.A., Zhao, W., Gindi, G.: Application of the ordered-subsets transmission reconstruction algorithm to contrast-enhanced dual-energy digital breast tomosynthesis. In: Proceedings of IEEE Nuclear Science Symposium and Medical Imaging Conference, IEEE NSS/MIC, Seattle, WA (2014)
Lu, Y., Peng, B., Lau, B.A., Hu, Y., Scaduto, D.A., Zhao, W., Gindi, G.: A scatter correction method for contrast-enhanced dual-energy digital breast tomosynthesis. Phys. Med. Biol. 60, 6323–6354 (2015)
Hu, Y.-H., Zhao, W.: Experimental quantification of lesion detectability in contrast enhanced dual energy digital breast tomosynthesis, vol. 8313, pp. 83130A1–83130A10 (2012)
Acknowledgments
We gratefully acknowledge financial support from NIH (1 R01 CA148053 and 1 R01 EB002655), and Siemens Healthcare.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this paper
Cite this paper
Scaduto, D.A. et al. (2016). Dependence of Contrast-Enhanced Lesion Detection in Contrast-Enhanced Digital Breast Tomosynthesis on Imaging Chain Design. In: Tingberg, A., Lång, K., Timberg, P. (eds) Breast Imaging. IWDM 2016. Lecture Notes in Computer Science(), vol 9699. Springer, Cham. https://doi.org/10.1007/978-3-319-41546-8_18
Download citation
DOI: https://doi.org/10.1007/978-3-319-41546-8_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-41545-1
Online ISBN: 978-3-319-41546-8
eBook Packages: Computer ScienceComputer Science (R0)