Abstract
The mother provides various vital nutrients to the growing fetus during pregnancy. Maternal nutrient levels and fatty acids are critical for normal fetal growth and development. All fatty acids provide energy, but structural and metabolic functions primarily require the long-chain polyunsaturated fatty acids (LCPUFA). The biologically most active LCPUFA are docosahexaenoic acid (22:6, omega-3), eicosapentaenoic acid (20:5, omega-3), and arachidonic acid (AA, 20:4 omega-6) which are synthesized from their essential fatty acid precursors, alpha-linolenic acid (18:3, omega-3), and linoleic acid (18:2, omega-6). LCPUFA and their eicosanoid metabolites such prostaglandins and prostacyclins play a vital role in determining the length of gestation, initiation of labor, and placental growth and development. Storage of LCPUFA in maternal fat depots during early pregnancy serves as a sole source of LCPUFA for the growing fetus as the fetus has a limited capacity to synthesize LCPUFA due to lack of desaturases. Therefore, the amount of LCPUFA transported from the mother to fetus depends on maternal LCPUFA intake, metabolism, and placental uptake/transport of fatty acids. Accretion of maternal LCPUFA during pregnancy may reduce the risk of pregnancy complications such as preterm birth, intrauterine growth restriction, gestational diabetes mellitus, and preeclampsia. Maternal DHA and AA status positively influence fetal growth and brain development and also reduce the risk of developing non-communicable diseases in the offspring in adult life. This chapter describes the role of maternal LCPUFA in reducing the risk of adverse pregnancy outcomes.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Maternal Nutrition and Pregnancy Outcome
The nutritional status of the woman, prior to conception and during pregnancy, is recognized as an important determinant of pregnancy outcome. The pregnant mother provides nourishment for embryonic and fetal growth [1–4] and also prepares her body for labor and parturition [5].
The mother modifies her metabolism early from pregnancy to support the nutritional needs of the fetus [6]. Nutrients transported to the fetus are known to influence cell number and differentiation in the blastocyst that regulates fetal growth and organ development. However, maternal nutritional restriction can lead to fewer cells in the inner cell mass and cause blastocyst abnormalities [7]. Nutrient deficiencies also lead to serious complications of labor, preterm deliveries [8, 9] and contribute to high rates of maternal morbidity and mortality [10, 11]. It also leads to lower birth weight [12], restricted postnatal growth [13], altered organ/body weight ratios [14], and congenital malformations [8] in the offspring.
An adequate and balanced supply of both macro- and micronutrients is critical for maintaining pregnancy and appropriate fetal growth where macronutrients (carbohydrates, proteins, and lipid) provide energy for fetal growth while micronutrients play a major role in the metabolism of macronutrients and are involved in the cellular metabolism of the fetus [10, 15]. Fetal growth and development depends on the unique supply of dietary fatty acids from the mother [16]. Lipids/fats represent a balanced and wholesome diet important to maintain the health and its key components, fatty acids, represent essential nutrients during intrauterine life [6].
Lipids are esters of moderate to long-chain fatty acids, which are carboxylic acids with a long aliphatic hydrocarbon tail, either saturated or unsaturated. Based on the number of double bonds in the hydrocarbon chain, unsaturated fatty acids are further classified as monounsaturated fatty acids (MUFA) (presence of one double bond) and polyunsaturated fatty acids (PUFA) (presence of two or more double bonds).
Long-chain Polyunsaturated Fatty Acids (LCPUFA)
Long-chain polyunsaturated fatty acids (≥20 carbon atoms) are distinguished into two key families; omega-3 and omega-6. Omega-3 fatty acids contain a double bond (C=C) at the third carbon atom from the carboxylic end of the fatty acid chain and omega-6 fatty acids contain a double bond (C=C) at the sixth carbon atom. Among PUFA, linoleic acid (LA; 18:2 omega-6) and alpha-linolenic acid (ALA; 18:3 omega-3) are called ‘essential fatty acids’ because humans cannot synthesize them in the body and they have to be ingested through the diet [6]. All fatty acids within the omega-3 family are derived from ALA, while all omega-6 fatty acids are derived from LA. Biologically, most active forms of omega-3 PUFA are docosahexaenoic acid (DHA; 22:6 omega-3) and eicosapentaenoic acid (EPA; 20:5 omega-3). ALA is found in algal oil, flaxseed oil, rapeseed oil (canola), walnuts, and some green leafy vegetables while EPA and DHA are mainly found in marine fish or fish oils. AA is a physiologically important omega-6 fatty acid and is found abundantly in fats, oils, eggs, meat, poultry, cereals, vegetables, nuts, seeds, and human milk.
LCPUFA serve as important constituents of cell membrane phospholipids, play an important role in maintaining the fluidity, permeability, and conformation of cell membranes, perform membrane-associated functions, and act as intracellular mediators of gene expression [17]. AA and DHA are important structural fatty acids in neural tissue. They provide energy, act as the precursors of the metabolically active compounds such as the prostacyclins, prostaglandins, thromboxanes, leukotrienes, and resolvins, and perform functional and structural roles within the body. LCPUFA together with their above-mentioned metabolites are involved in the functioning of transporters, ion channels, and enzymes and in signal transduction pathways [18].
LCPUFA Biosynthesis
Liver is known to play a central role in the fatty acid synthesis and metabolism [19]. Fatty acid desaturases are the enzymes that catalyze the introduction of double bonds at specific positions in a fatty acid chain [20, 21]. Delta 5 (∆5) and Delta 6(∆6) desaturases participate in the synthesis of LCPUFA [22, 23]. DHA is endogenously synthesized from its precursor ALA via a series of ∆6 desaturase, ∆5 desaturase, elongase enzymes, and β-oxidation steps [24]. The same series of desaturases and elongases are involved in the conversion of LA into its longer-chain, more unsaturated derivative, AA. These LCPUFA are stored in the adipose tissue in the form of triglycerides.
LCPUFA Metabolism During Pregnancy
There are major changes in the maternal lipid metabolism throughout pregnancy to ensure a continuous supply of fatty acids to the growing fetus [25]. During early pregnancy, LCPUFA consumed through diet are accumulated and stored in the adipose tissue as a result of enhanced lipogenesis. Subsequently in the later stages of gestation, when the fetal growth rate is maximal, there is an increase in the lipolytic activity in the maternal adipose tissue [26, 27]. This increases plasma triacylglycerol concentrations, with smaller rises in phospholipids, cholesterol concentrations [26, 28], and plasma non-esterified fatty acids (a form of free fatty acids present in small proportion) which serve as a source of LCPUFA for the growing fetus. Additionally, there is mobilization of LCPUFA from the maternal adipose tissue depots and selective delivery of maternal circulating LCPUFA to the fetus through placenta [28].
LCPUFA Intake/Status during Pregnancy and Fetal LCPUFA Status
The fatty acid levels in maternal blood lipids serve as indicators of maternal status [29]. Several studies report a decline in the maternal essential fatty acid status from the first trimester of pregnancy until delivery [30]. Additionally, there is depletion in the levels of DHA in maternal total plasma [31], serum [32], plasma phospholipids, and erythrocytes [33, 34]. Report suggests a significant decline in the ratio of DHA to docosapentaenoic acid in maternal plasma phospholipids indicating maternal difficulty during pregnancy to cope up with high demands of DHA [34]. Although these studies provide evidence for compromised LCPUFA status in pregnancy, there is limited information on the maternal factors that influence essential fatty acid metabolism during pregnancy. Presumably, maternal dietary intake/status of LCPUFA is related to the amount of fatty acids delivered to the fetus through the placenta [35, 36]. Since the ability of fetus and placenta to synthesize LCPUFA is low, the fetus primarily depends on placental transfer of LCPUFA [32].
Maternal fatty acid intake can directly influence the plasma and tissue fatty acid profile of the offspring [37]. Infant plasma omega-3 and omega-6 fatty acids and conjugated LA are related to maternal plasma fatty acids [38] while the deficiency of AA and DHA in maternal blood throughout pregnancy results in a suboptimal neonatal DHA status [34]. A study in our department has shown higher levels of DHA and AA in cord blood as compared to maternal blood in terms of pregnancy suggesting that large quantities of maternal LCPUFA are diverted to the fetus [39]. Evidence from several observational studies and randomized control trials (RCT) suggests a positive association between intake of omega-3 fatty acids during pregnancy and birth outcome [40].
Role of LCPUFA in Pregnancy
The different kinds of fatty acids consumed by the mother during gestation are known to influence pregnancy and fetal outcome [6] due to their fundamental roles as structural elements and functional modulators [17]. LCPUFA are required to support the development of the fetus in utero. LCPUFA are required in all stages of pregnancy [1] and play important role in determining length of gestation, initiation of labor, and in placental growth and development [41] (Fig. 35.1).
Role of LCPUFA during pregnancy. LCPUFA Long-chain polyunsaturated fatty acids. Maternal LCPUFA intake during pregnancy plays an important role in maintaining length of gestation, initiation of labor, placental angiogenesis, and development. However, lower levels of maternal LCPUFA may lead to preterm labor, intrauterine growth retardation, and pregnancy complications such as gestational diabetes mellitus and preeclampsia. Adequate amounts of maternal LCPUFA are essential for fetal growth and organ development, brain development, and overall health
Initiation of Labor
LCPUFA metabolites such as prostaglandins are critical for initiation of labor and parturition process [42]. The rise in prostaglandins is involved in pathway of uterine contractility [43] and their levels increase during labor in the fetal membranes [44].
Among LCPUFA, AA serves as a precursor of the potent 2-series prostaglandins (PGs) E2 and PGF2α, and thromboxane A2 which are required for connective tissue remodeling associated with cervical maturation and rupture of membranes [45, 46]. On the other hand, EPA acts as a precursor for the 3-series of prostaglandins and produces PGE3 and PGI3, which promote myometrium relaxation [42]. These 3-series PGs do not possess any uterotonic activity and inhibit the synthesis of prostaglandins belonging to series 2 [47]. The eicosanoids from omega-3 and omega-6 fatty acids possess opposing modes of action. It is also known that EPA and DHA competitively displace AA in the membrane phospholipids, reduce production of PGE2 and PGF2α, and thereby inhibit the parturition process [48] (Fig. 35.2).
The premature production of PGE-2 and PGF-2α may lead to remodeling of the cervix, ultimately triggering labor by activating matrix metalloproteinases (MMPs) [49]. It has been reported that the concentrations of AA elevate in the amniotic fluid during labor and is accompanied by the elevated levels of PGE2 and PGF2α in the maternal circulation preceding the onset of spontaneous labor [50]. Administration of vaginal PGE2 has been a successful way to induce labor since the 1960s [51, 52].
As the pregnancy progresses, there is a rise in omega-3 fatty acids within the utero-placental unit followed by local production of series-3 prostaglandins, a critical element in cervical ripening that plays essential roles in normal initiation of labor [53]. Reports suggest that inclusion of EPA in the diet leads to a reduction in the production of proinflammatory eicosanoids and increased production of prostacyclin (PGI2), promotes myometrial relaxation [54], and prevents preterm labor [55].
Length of Gestation
There is growing evidence that omega-3 fatty acids and their eicosanoid metabolites play vital roles in determining the duration of gestation [54, 56] and parturition process [45]. Improved omega-3 fatty acids status during pregnancy shows promise as series-3 prostaglandins are important in the maintenance of normal length of gestation [57]. Maternal DHA supplementation has shown to increase the length of gestation and infant size [46, 54, 56].
Some RCTs report that 600 mg DHA/d [56] and 800 mg DHA/d [58] significantly increase duration of gestation. On the other hand, 400 mg DHA/d supplementation showed no effect on the gestation duration [59]. No randomized controlled trial has found a reduction in gestation duration or size at birth [56].
LCPUFA in Placental Growth and Development
Placenta is at the interface between mother and fetus and is a key moderator of fetal growth and development [60]. The proper growth, development, and establishment of the placenta with its circulatory system are essential for successful maintenance of mother’s health and for the development of the embryo [5].
During pregnancy, vasculogenesis and angiogenesis are critical processes in placental development [61]. Vasculogenesis involves the formation of new blood vessels from angioblast precursor cells, leading to the formation of an initial vascular network. Angiogenesis is the process of development of new vessels from pre-existing blood vessel [62] that plays an important role in the development of capillary network in both maternal and fetal compartments [63]. These processes are regulated by various growth factors, including vascular endothelial growth factor (VEGF) family, placental growth factor (PlGF), transforming growth factor ß (TGF ß) family, and angiopoietins along with proteases such as MMPs as well as their respective receptors [64, 65].
Maternal supply of DHA plays an important role in placental angiogenic processes and vascular remodeling by increasing the expression of VEGF, angiopoeitin, and tissue inhibitors of metalloproteinases (TIMP) genes [66]. Angiogenic activities of LCPUFA are reported on the first trimester placental trophoblast cell line and have been shown to be highest for DHA followed by EPA and AA [67]. It has been observed that DHA induces maximum tube (capillary-like structures) formation by stimulating cell proliferation in the placenta as compared to other fatty acids [66]. DHA is also known to alter the expression of several genes, such as adipose differentiation-related protein, fatty acid-binding protein-4 (FABP4), FABP3 and cyclooxygenase-2, which are involved in angiogenesis [67]. Studies from our department in women with preeclampsia have shown a negative association between placental DHA levels and maternal anti-angiogenic factor soluble fms-like tyrosine kinase-1(sFLT-1) levels [68]. A recent review reports that maternal omega-3 fatty acid supplementation during pregnancy is associated with enhanced placental growth and reductions in placental inflammation, oxidative stress in rats [41].
Transport of Maternal LCPUFA to Fetus Through Placenta
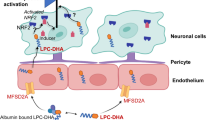
The fetus has a limited ability to synthesize LCPUFA because the capacity of the fetal liver for desaturation and chain elongation is not mature in early gestation in humans. Therefore, the fetus is dependent upon the mother for a supply of preformed DHA and AA through placenta. However, maternal lipoproteins which are rich in triglycerides do not directly cross the placental unit and therefore require placental lipoprotein lipases for their hydrolysis to form free fatty acids [26]. These fatty acids are mainly derived from maternal fatty acids bound to albumin, from lipoproteins bound by apoprotein receptors, or from triglyceride-rich lipoproteins released by the triglyceride hydrolases or lipoprotein lipases [69]. These enzymes must be active to facilitate the placental uptake of free fatty acids [70].
The free fatty acids need to get bound with the fatty acid-binding proteins (FABPs; cytosolic and membrane bound FABPs) to get entry into placental cells [46] where they cross the microvillous and basal membranes of placenta by simple diffusion [35]. Additionally, a number of placental fatty acid transport proteins (FATPs) and carrier proteins are present for the transfer of hydrophobic fatty acids from the maternal circulation to the fetal circulation [71] (Fig. 35.3).
Studies from various laboratories have clearly demonstrated the presence of different FATPs both in the cytosol and in the cell membranes and stated their role in the uptake and intracellular transport [72]. Several transport proteins such as plasma membrane fatty acid-binding protein (FATP), fatty acid translocase, or CD36 are located in the placenta to facilitate fatty acid transfer and meet the increased nutrients demand of the fetus during gestation [70, 73]. FATP 1 and FATP 4 have shown to be positively correlated with placental DHA uptake and are important for selective maternal–fetal transfer of DHA [74]. Thus, the placenta plays a critical role in modulating the transport of maternal fatty acids to fetus [41, 75].
Consequences of LCPUFA Inadequacy/Insufficiency
A number of RCTs have demonstrated that the maternal DHA intake during pregnancy can prolong high-risk pregnancies, reduce early preterm delivery, improve birth outcome by increasing birth weight, and head circumference and birth length [1]. However, low concentrations of maternal LCPUFA have shown to be associated with adverse pregnancy outcome, reduced birth weight, and an increased risk of small for gestational age infants [76].
Preterm Labor
Preterm birth is defined as birth before 37 weeks of gestation or fewer than 259 days since the first day of the woman’s last menstrual period. As mentioned above, the balance between omega-3 and omega-6 fatty acids plays an important role in the maintenance of normal length of gestation. However, an imbalance between omega-3 and omega-6 fatty acids may lead to disturbances in the production of prostaglandins which are critical in cervical ripening and initiation of labor [57].
Preterm birth is characterized by lower production of prostaglandins by the reproductive tissue [45]. If omega-3 fatty acid accumulation within the feto-placental unit is low and local production of prostaglandins is high, the cervix ripens prematurely with increase in uterine contractions, leading to preterm delivery [57]. Mothers delivering preterm babies are reported to have low levels of omega-3 fatty acids [77]. Additionally, it is reported that the percent total LA, AA, EPA, and omega-6/omega-3 ratio are higher while total omega-3 fatty acids are lower in preterm mothers compared to full-term mothers [77]. An imbalance in the levels of omega-3 and omega-6 fatty acids has been reported in the preterm delivery [47] where a high ratio of omega-6/omega-3 fatty acids results in increased production of PGE2 and PGF2α leading to initiation of labor and preterm labor [54].
Studies from our department have reported reduced erythrocyte DHA levels in mothers of preterm babies as compared to mothers of term babies [78] and reduced levels of placental AA and DHA in preterm deliveries [79]. A study in preterm and full-term human newborns found differences in maternal erythrocyte AA content and hypothesized that high content of maternal erythrocyte AA and AA/EPA ratio may be considered as an early signal of preterm delivery [80]. Similar observations are reported in the fatty acid profile of erythrocyte membrane of Brazilian mothers at delivery [81] and in the fatty acid composition of the colostrum of Iraqi mothers delivering preterm [82].
Supplementation of omega-3 fatty acids during pregnancy has shown to reduce early preterm birth before 34 weeks of gestation by 31 % [83]. Omega-3 fatty acid supplementation has also been reported to reduce the rate of recurrent preterm birth in a randomized trial [84].
Intrauterine Growth Restriction
Normal fetal growth depends on the genetically predetermined growth potential and is modulated by fetal, placental, maternal, and external factors [85]. Intrauterine growth restriction (IUGR) is characterized by the failure of the fetus to reach its genetic growth potential [85, 86] and is associated with increased perinatal mortality and morbidity [86].
LCPUFA status is altered in pregnancies complicated by IUGR [87]. Reports suggest alterations in lipid status in the mother, fetus, and placenta in IUGR pregnancies, i.e., a decrease in the conversion of LA and ALA into AA and DHA, respectively [88, 89]. Abnormal maternal lipoprotein concentrations of cholesterol, low-density lipoprotein (LDL)-cholesterol have been reported in IUGR [90].
A lower proportion of AA and DHA in fetal blood in comparison with maternal blood has been reported in IUGR pregnancies which may be related to inadequate transplacental supply and a fetal lack of desaturases enzymes [88]. Reports suggest that placentas of infants with IUGR have a specific placental phenotype indicating alterations in placental structure and functions [91]. Altered placental lipoprotein lipase activity and placental FABP expression has been reported in IUGR pregnancies indicating disrupted lipid metabolism in these pregnancies [92]. However, only minor changes in passive membrane permeability and composition have been reported in the syncytiotrophoblast membranes in IUGR pregnancies [93]. A case control study reports an increase in AA in the placenta and umbilical artery phospholipids of fetal growth retardation speculating that the differential arterial composition may be responsible for the increased cardiovascular risk of fetal growth-restricted infants in adulthood [33].
Gestational Diabetes Mellitus
Gestational diabetes mellitus (GDM) is characterized by an abnormal glucose tolerance diagnosed for the first time during pregnancy [94]. GDM is associated with adverse obstetric and perinatal outcomes [95] and these mothers are at a risk of developing type 2 diabetes in later life [96]. Intake of specific types of dietary fat has been implicated in GDM risk where diets high in saturated fatty acids increase the risk of developing GDM [97] while PUFA are protective [98].
Reduction in plasma phospholipid of omega-6 fatty acids has been reported in GDM mothers [99]. In GDM, decreased proportion of LCPUFA in fetal plasma has been reported resulting from decreased supply, impaired placental transfer, or altered intrauterine metabolism [100]. Altered maternal metabolism, as a result of maternal hyperglycemia in GDM, affects placental metabolism and leads to an aberrant fetal metabolism [101]. In GDM pregnancies, fetal plasma and red blood cells show an altered lipid pattern compared to controls, with reduced AA and DHA levels [102]. On the other hand, elevated levels of DHA and AA in placental phospholipids are reported in GDM, which subsequently results into impaired LCPUFA transport to the fetus [103]. The composition of placental glycerol phospholipids is known to be altered in GDM and might reflect an aberrant fatty acid transfer across the placenta affecting fetal body composition. Placental mRNA and protein expression of CD36 has shown to be higher while FABP1 mRNA and FABP3 protein expression has shown to be lower in GDM [104].
Disturbance in normal fetal growth and development induced by GDM is associated with long-term adverse effects in the offspring, such as adiposity and type 2 diabetes [105]. GDM is associated with increased fetal weight and the risk for later metabolic and cardiovascular diseases [106]. However, omega-3 fatty acid supplementation in GDM pregnancy is reported to have beneficial effects on maternal high-sensitivity C-reactive protein, malondialdehyde levels, and hyperbilirubinemia of newborn babies [107].
Preeclampsia
Preeclampsia is a pregnancy complication manifested by hypertension, proteinuria, and the varying degrees of ischemic peripheral organ damage, which typically arise in the third trimester of gestation [108]. There are limited studies which have reported lower levels of omega-3 fatty acids from erythrocytes in preeclampsia [109, 110]. It has previously been shown that low erythrocyte levels of omega-3 fatty acids and high levels of omega-6 fatty acids particularly AA are associated with an increased risk of preeclampsia [111] while higher levels of omega-3 fatty acids at mid-gestation are associated with lower maternal blood pressures and pregnancy-associated hypertension [112]. A report suggests that high intakes of energy, sucrose, and PUFA independently increase the risk for preeclampsia [113]. Report suggests that lower concentrations of maternal and fetal LCPUFA in mothers with preeclampsia may be due to the decreased maternal LCPUFA synthesis that further leads to deficiency in the offspring [114]. Some studies report no change in the LCPUFA status [109] while others report higher DHA levels [115]. Further, it is likely that altered membrane lipid fatty acid composition may lead to altered placental development in preeclampsia [116]. Reports suggest a possible role of impaired placental fatty acid oxidation in the pathogenesis of preeclampsia [117]. Recent study from our department also indicates that disturbances in placental fatty acid metabolism exist in preeclampsia [118].
Maternal LCPUFA and Fetal Development
Maternal LCPUFA and its storage in fetal adipose tissue provide an important source of LCPUFA during the critical first months of life for rapid cellular growth and activity [28, 119]. It is known that prior to 25 weeks of gestation, the fetus accumulates only a small amount of lipids and thereafter exponentially accumulates large amount of lipids [28]. It has been reported that the fetus requires approximately 50 mg/kg/day of omega-3 fatty acids and 400 mg/kg/day of omega 6 fatty acids during the early weeks of life [120, 121].
Fetal Size and Weight
If adequate nutrition is available, the fetus can reach its growth potential, resulting in the birth of a healthy newborn of appropriate size. Among LCPUFA, DHA has shown to play important role in determining birth weight [46, 122], fetal growth, and development [1, 58]. Placental phosphatidylethanolamine with AA is known to be associated with fetal growth [123]. Low plasma phospholipid concentrations of EPA, DHA, and dihomo-gamma-linolenic acid (DGLA) and high concentrations of AA during early pregnancy have shown to be associated with reduced birth weight and/or an increased risk of small for gestational length infants [76]. DHA supplementation in large studies has shown slightly higher birth weight by about 50 g at delivery [32]. A meta-analysis of 15 RCTs indicates that maternal omega-3 fatty acid supplementations lightly increase birthweight as compared to placebo but show no differences in birth length and head circumference [40]. A double-blind RCT showed that supplementation with 600 mg/day DHA increases birthweight by 172 g [56]. A recent study reports no association between maternal omega-3 fatty acid compositions in gestational week 24 with fetal weight gain [124]. A study investigating birthweight in a fishing community reports increase in the duration of gestation with increased intake of marine fats but decrease in birthweight [125]. No studies have reported a reduction in infant size at birth by LCPUFA supplementation [56].
Maternal LCPUFA and Brain Development
DHA and AA are found in very high concentrations in cell membranes for fetal neural and retinal development and are known to accrete extensively in these tissues during prenatal period [40, 120, 121]. Brain development is known to accelerate during the second half of pregnancy, lasting until late adolescence [126]. The brain growth spurt that takes place from the third trimester of pregnancy until 18 months after birth also correlates well with DHA accretion in brain phospholipids [127]. During this time, the developing brain is sensitive to acute variations in the supply of DHA. Maternal diet, DHA stores, placental transport, and genetic polymorphisms are reported to influence DHA accretion in the fetal brain.
Several human and animal studies indicate that LCPUFA play a vital role in the development and maintenance of the central nervous system and improved cognitive development and spatial memory [128–131]. However, DHA deficiency has shown to cause retarded visual acuity [132], cognitive impairment, cerebellar dysfunction [133], and various other neurological disorders [134].
High-dosage LCPUFA supplementation at mid-pregnancy has shown to be associated with improved intelligence quotient scores of neurodevelopment [135]. Supplementation studies conducted in pregnancy and/or lactation using DHA suggest that DHA could help in improving cognitive outcome of children in later life [131]. Animal studies indicate that LCPUFA promote early brain development and regulate behavioral aspects, memory, and cognitive functions [136]. These studies have proved that supplementation has many beneficial effects such as increased visual acuity [137], reduced hyperactivity [138], and enhanced cognitive functions, memory, and attention [136]. Studies based on a rat model of Alzheimer’s disease suggest that DHA can be used as a therapeutic agent to improve cognitive decline [139].
Maternal LCPUFA and Fetal Health
Maternal plasma triacylglycerols and non-esterified fatty acids are known to correlate with fetal growth and fat mass [140]. Maternal fasting triglyceride levels are significant predictors of the fatty acid composition of the child’s muscle membrane [141]. During gestation and lactation, higher levels of AA, EPA, and DHA are positively associated with child’s pre- and postnatal growth [142–144].
A review suggests that maternal intake of omega-3 and omega-6 fatty acids in gestation and lactation can impact the developing infant tissue neuroendocrine and metabolic pathways [145]. Recent studies in humans and animals suggest that inadequate levels of omega-3 fatty acids during the prenatal and postnatal periods influences metabolic diseases [146], lean mass [147], and blood pressure in the offspring [148]. Further, prenatal and early postnatal exposures to low omega-3 fatty acids and high omega-6 fatty acids influence adiposity in children [149]. Children with a lower proportion of LCPUFA in their muscle membrane are at a higher risk for developing insulin resistance [150].
An enhanced maternal–fetal omega-3 PUFA status has shown to be associated with lower childhood adiposity [149]. A review suggests that the provision/supplementation of LCPUFA during critical periods of growth, especially from the 2nd trimester of pregnancy to 5 year, can prevent coronary artery diseases in adult life [151].
Animal studies demonstrate that maternal and post-weaning diet containing omega-3 fatty acids improve the lipid profile in the offspring [152, 153]. The beneficial effects of gestational/prenatal omega-3 fatty acid supplementation in reducing risk for metabolic syndrome markers in the hamster [154] and Wistar rat offspring [155, 156] have also been reported. Maternal supplementation with DHA is reported to decrease blood lipid [157] and improve blood pressure in the adult rat offspring [156].
LCPUFA Recommendations During Pregnancy
Fetal DHA requirement increases exponentially with gestational age due to fetal development. Therefore, a daily intake of DHA during pregnancy is recommended by World Health Organization and the Food and Agriculture Organization of the United Nations [158]. It is advisable that pregnant women should ingest at least 300 mg/day of DHA in order to achieve a better pregnancy outcome [159].
In 2002, the Food and Nutrition Board of the US Institute of Medicine established adequate intake levels (AI) for omega-3 and omega-6 fatty acids[160]. The recommendations suggest that human diets should contain minimum 3 % LA and 0.5 % ALA [161]. The recommended dietary allowances for essential fatty acids are 4.5 % of total energy for pregnant women and 5.7 % of total energy for lactating women. It has been suggested that the intake in Indian pregnant and lactating women should be 300 mg; of which, 200 mg should be in the form of DHA [Indian Council of Medical Research, India [162]. In populations consuming fish, it is recommended that during pregnancy two portions of fish should be consumed per week, with one portion of an oily fish such as mackerel, herring, sardines, or salmon [159].
Conclusion
Dietary intake of LCPUFA before and during pregnancy is critical for maternal health and optimal fetal growth. Accretion of AA and DHA in maternal tissues during pregnancy is the major determinant of length of gestation, parturition, placental growth, and development. Insufficiency/decline in the LCPUFA is associated with adverse pregnancy outcomes such as preterm birth, intrauterine growth retardation, GDM, and preeclampsia. Maternal LCPUFA status positively influences postnatal growth, neuro-cognitive development and helps to improve the health of the offspring.
Abbreviations
- AA:
-
Arachidonic acid
- ALA:
-
Alpha-linolenic acid
- DHA:
-
Docosahexaenoic acid
- GDM:
-
Gestational diabetes mellitus
- IUGR:
-
Intrauterine growth restriction
- LA:
-
Linoleic acid
- LCPUFA:
-
Long-chain polyunsaturated fatty acids
- PUFA:
-
Polyunsaturated fatty acids
References
Morse NL. Benefits of docosahexaenoic acid, folic acid, vitamin D and iodine on foetal and infant brain development and function following maternal supplementation during pregnancy and lactation. Nutrients. 2012;4(7):799–840.
Allen LH. Multiple micronutrients in pregnancy and lactation: an overview. Am J Clin Nutr. 2005;81(5):1206s–12s.
Moore VM, Davies MJ. Diet during pregnancy, neonatal outcomes and later health. ReprodFertil Dev. 2005;17(3):341–8.
Odent M. Nutrition in pregnancy: keeping in mind the priorities. Pract Midwife. 2014;17(9):10–2.
Mistry HD, Williams PJ. The importance of antioxidant micronutrients in pregnancy. Oxid Med Cell Longev. 2011;2011:841749.
Cetin I, Alvino G, Cardellicchio M. Long chain fatty acids and dietary fats in fetal nutrition. J Physiol. 2009;587(Pt 14):3441–51.
Kwong WY, Wild AE, Roberts P, Willis AC, Fleming TP. Maternal undernutrition during the preimplantation period of rat development causes blastocyst abnormalities and programming of postnatal hypertension. Development. 2000;127(19):4195–202.
Kontic-Vucinic O, Sulovic N, Radunovic N. Micronutrients in women’s reproductive health: II. Minerals and trace elements. Int J Fertil Womens Med. 2006;51(3):116–24.
Keen CL, Clegg MS, Hanna LA, Lanoue L, Rogers JM, Daston GP, et al. The plausibility of micronutrient deficiencies being a significant contributing factor to the occurrence of pregnancy complications. J Nutr. 2003;133(5 Suppl 2):1597s–605s.
Wu G, Imhoff-Kunsch B, Girard AW. Biological mechanisms for nutritional regulation of maternal health and fetal development. Paediatr Perinat Epidemiol. 2012;26(Suppl 1):4–26.
Rush D. Nutrition and maternal mortality in the developing world. Am J Clin Nutr. 2000;72(1 Suppl):212s–40s.
Muthayya S. Maternal nutrition & low birth weight—what is really important? Indian J Med Res. 2009;130(5):600–8.
Chen JH, Martin-Gronert MS, Tarry-Adkins J, Ozanne SE. Maternal protein restriction affects postnatal growth and the expression of key proteins involved in lifespan regulation in mice. PLoS ONE. 2009;4(3):e4950.
Watkins AJ, Lucas ES, Wilkins A, Cagampang FR, Fleming TP. Maternal periconceptional and gestational low protein diet affects mouse offspring growth, cardiovascular and adipose phenotype at 1 year of age. PLoS One. 2011;6(12):e28745.
Rao KR, Padmavathi IJ, Raghunath M. Maternal micronutrient restriction programs the body adiposity, adipocyte function and lipid metabolism in offspring: a review. Rev Endocr Metab Disord. 2012;13(2):103–8.
Herrera E. Implications of dietary fatty acids during pregnancy on placental, fetal and postnatal development—a review. Placenta. 2002;23 Suppl A:S9–19.
Dutta-Roy AK. Transport mechanisms for long-chain polyunsaturated fatty acids in the human placenta. Am J Clin Nutr. 2000;71(1 Suppl):315s–22s.
Muskiet FAJ. Frontiers in neuroscience pathophysiology and evolutionary aspects of dietary fats and long-chain polyunsaturated fatty acids across the life cycle. In: Montmayeur JP, le Coutre J, editors. Fat detection: taste, texture, and post ingestive effects. Boca Raton (FL): CRC Press, Taylor& Francis Group, LLC; 2010.
Zhou H, Liu R. ER stress and hepatic lipid metabolism. Front Genet. 2014;5:112.
Rodriguez A, Sarda P, Nessmann C, Boulot P, Leger CL, Descomps B. Delta6- and delta5-desaturase activities in the human fetal liver: kinetic aspects. J Lipid Res. 1998;39(9):1825–32.
Vrablik TL, Watts JL. Emerging roles for specific fatty acids in developmental processes. Genes Dev. 2012;26(7):631–7.
Nakamura MT, Nara TY. Structure, function, and dietary regulation of delta6, delta5, and delta9 desaturases. Annu Rev Nutr. 2004;24:345–76.
Slagsvold JE, Thorstensen K, Kvitland M, Erixon D, Knagenhjelm N, Mack M, et al. Fatty acid desaturase expression in human leucocytes correlates with plasma phospholipid fatty acid status. Scand J Clin Lab Invest. 2009;69(4):496–504.
Chilton FH, Murphy RC, Wilson BA, Sergeant S, Ainsworth H, Seeds MC, et al. Diet-gene interactions and PUFA metabolism: a potential contributor to health disparities and human diseases. Nutrients. 2014;6(5):1993–2022.
Butte NF. Carbohydrate and lipid metabolism in pregnancy: normal compared with gestational diabetes mellitus. Am J Clin Nutr. 2000;71(5 Suppl):1256s-61s.
Herrera E, Amusquivar E, Lopez-Soldado I, Ortega H. Maternal lipid metabolism and placental lipid transfer. Horm Res. 2006;65 (Suppl) 3:59–64.
Herrera E, Ortega-Senovilla H. Maternal lipid metabolism during normal pregnancy and its implications to fetal development. Clinical Lipidology. 2000;5(6):899–911.
Haggarty P. Fatty acid supply to the human fetus. Annu Rev Nutr. 2010;30:237–55.
Lauritzen L, Carlson SE. Maternal fatty acid status during pregnancy and lactation and relation to newborn and infant status. Matern Child Nutr. 2011;7 (Suppl) 2:41–58.
Holman RT, Johnson SB, Ogburn PL. Deficiency of essential fatty acids and membrane fluidity during pregnancy and lactation. Proc Natl AcadSci USA. 1991;88(11):4835–9.
Montgomery C, Speake BK, Cameron A, Sattar N, Weaver LT. Maternal docosahexaenoic acid supplementation and fetal accretion. Br J Nutr. 2003;90(1):135–45.
Larque E, Gil-Sanchez A, Prieto-Sanchez MT, Koletzko B. Omega 3 fatty acids, gestation and pregnancy outcomes. Br J Nutr. 2012;107 Suppl 2:S77–84.
Matorras R, Lopez De Larrucea A, Sanjurjo P, Ignacio Ruiz J, Echevarria Y, Nieto A, et al. Increased tissue concentrations of arachidonic acid in umbilical artery and placenta in fetal growth retardation. Acta Obstet Gynecol Scand. 2001;80(9):807–12.
Al MD, van Houwelingen AC, Kester AD, Hasaart TH, de Jong AE, Hornstra G. Maternal essential fatty acid patterns during normal pregnancy and their relationship to the neonatal essential fatty acid status. Br J Nutr. 1995;74(1):55–68.
Haggarty P. Placental regulation of fatty acid delivery and its effect on fetal growth–a review. Placenta. 2002;23 Suppl A:S28–38.
Haggarty P. Effect of placental function on fatty acid requirements during pregnancy. Eur J Clin Nutr. 2004;58(12):1559–70.
Amusquivar E, Herrera E. Influence of changes in dietary fatty acids during pregnancy on placental and fetal fatty acid profile in the rat. Biol Neonate. 2003;83(2):136–45.
Elias SL, Innis SM. Infant plasma trans, n-6, and n-3 fatty acids and conjugated linoleic acids are related to maternal plasma fatty acids, length of gestation, and birth weight and length. Am J Clin Nutr. 2001;73(4):807–14.
Kilari AS, Mehendale SS, Dangat KD, Yadav HR, Kulakarni AV, Dhobale MV, et al. Long chain polyunsaturated fatty acids in mothers and term babies. J Perinat Med. 2009;37(5):513–8.
Imhoff-Kunsch B, Briggs V, Goldenberg T, Ramakrishnan U. Effect of n-3 long-chain polyunsaturated fatty acid intake during pregnancy on maternal, infant, and child health outcomes: a systematic review. Paediatr Perinat Epidemiol. 2012;26 Suppl 1:91–107.
Jones ML, Mark PJ, Waddell BJ. Maternal dietary omega-3 fatty acids and placental function. Reproduction. 2014;147(5):R143–52.
Olsen SF, Hansen HS, Sorensen TI, Jensen B, Secher NJ, Sommer S, et al. Intake of marine fat, rich in (n-3)-polyunsaturated fatty acids, may increase birthweight by prolonging gestation. Lancet. 1986;2(8503):367–9.
Kota SK, Gayatri K, Jammula S, Kota SK, Krishna SV, Meher LK, et al. Endocrinology of parturition. Indian J Endocrinol Metab. 2013;17(1):50–9.
Olsen SF, Joensen HD. High liveborn birth weights in the Faroes: a comparison between birth weights in the Faroes and in Denmark. J Epidemiol Community Health. 1985;39(1):27–32.
Allen KG, Harris MA. The role of n-3 fatty acids in gestation and parturition. Exp Biol Med (Maywood). 2001;226(6):498–506.
Greenberg JA, Bell SJ, Ausdal WV. Omega-3 fatty acid supplementation during pregnancy. Rev Obstet Gynecol. 2008;1(4):162–9.
Facchinetti F, Fazzio M, Venturini P. Polyunsaturated fatty acids and risk of preterm delivery. Eur Rev Med Pharmacol Sci. 2005;9(1):41–8.
Roman AS, Schreher J, Mackenzie AP, Nathanielsz PW. Omega-3 fatty acids and decidual cell prostaglandin production in response to the inflammatory cytokine IL-1beta. Am J Obstet Gynecol. 2006;195(6):1693–9.
Yoshida M, Sagawa N, Itoh H, Yura S, Takemura M, Wada Y, et al. Prostaglandin F(2alpha), cytokines and cyclic mechanical stretch augment matrix metalloproteinase-1 secretion from cultured human uterine cervical fibroblast cells. Mol Hum Reprod. 2002;8(7):681–7
Karim SM. The role of prostaglandins in human parturition. Proc R Soc Med. 1971;64(1):10–2.
Thomas J, Fairclough A, Kavanagh J, Kelly AJ. Vaginal prostaglandin (PGE2 and PGF2a) for induction of labour at term. Cochrane Database Syst Rev. 2014;6:Cd003101.
Kelly AJ, Malik S, Smith L, Kavanagh J, Thomas J. Vaginal prostaglandin (PGE2 and PGF2a) for induction of labour at term. Cochrane Database Syst Rev. 2009;4:Cd003101.
Olson DM, Mijovic JE, Sadowsky DW. Control of human parturition. Semin Perinatol. 1995;19(1):52–63
Coletta JM, Bell SJ, Roman AS. Omega-3 fatty acids and pregnancy. Rev Obstet Gynecol. 2010;3(4):163–71.
Fereidooni B, Jenabi E. The use of omega 3 on pregnancy outcomes: a single-center study. J Pak Med Assoc. 2014;64(12):1363–5.
Carlson SE, Colombo J, Gajewski BJ, Gustafson KM, Mundy D, Yeast J, et al. DHA supplementation and pregnancy outcomes. Am J Clin Nutr. 2013;97(4):808–15.
Quinlivan JA, Pakmehr S. Fish oils as a population based strategy to reduce early preterm birth. Reprod Syst Sex Disord. 2013;2:116.
Makrides M, Gibson RA, McPhee AJ, Yelland L, Quinlivan J, Ryan P, et al. Effect of DHA supplementation during pregnancy on maternal depression and neurodevelopment of young children: a randomized controlled trial. JAMA. 2010;304(15):1675–83.
Ramakrishnan U, Stein AD, Parra-Cabrera S, Wang M, Imhoff-Kunsch B, Juarez-Marquez S, et al. Effects of docosahexaenoic acid supplementation during pregnancy on gestational age and size at birth: randomized, double-blind, placebo-controlled trial in Mexico. Food Nutr Bull. 2010;31(2 Suppl):S108–16.
Gabory A, Roseboom TJ, Moore T, Moore LG, Junien C. Placental contribution to the origins of sexual dimorphism in health and diseases: sex chromosomes and epigenetics. Biol Sex Differ. 2013;4(1):5.
Reynolds LP, Redmer DA. Angiogenesis in the placenta. Biol Reprod. 2001;64(4):1033–40.
Carmeliet P. Angiogenesis in life, disease and medicine. Nature. 2005;438(7070):932–6.
Demir R, Yaba A, Huppertz B. Vasculogenesis and angiogenesis in the endometrium during menstrual cycle and implantation. Acta Histochem. 2010;112(3):203–14.
Carmeliet P. Angiogenesis in health and disease. Nat Med. 2003;9(6):653–60.
Pepper MS. Role of the matrix metalloproteinase and plasminogen activator-plasmin systems in angiogenesis. Arterioscler Thromb Vasc Biol. 2001;21(7):1104–17.
Johnsen GM, Basak S, Weedon-Fekjaer MS, Staff AC, Duttaroy AK. Docosahexaenoic acid stimulates tube formation in first trimester trophoblast cells, HTR8/SVneo. Placenta. 2011;32(9):626–32.
Basak S, Duttaroy AK. Effects of fatty acids on angiogenic activity in the placental extravillious trophoblast cells. Prostaglandins Leukot Essent Fatty Acids. 2013;88(2):155–62.
Sundrani DP, Reddy US, Joshi AA, Mehendale SS, Chavan-Gautam PM, Hardikar AA, et al. Differential placental methylation and expression of VEGF, FLT-1 and KDR genes in human term and preterm preeclampsia. Clin Epigenetics. 2013;5(1):6.
Hanebutt FL, Demmelmair H, Schiessl B, Larque E, Koletzko B. Long-chain polyunsaturated fatty acid (LC-PUFA) transfer across the placenta. Clin Nutr. 2008;27(5):685–93.
Duttaroy AK. Fetal growth and development: roles of fatty acid transport proteins and nuclear transcription factors in human placenta. Indian J Exp Biol. 2004;42(8):747–57.
van der Vusse GJ, van Bilsen M, Glatz JF. Cardiac fatty acid uptake and transport in health and disease. Cardiovasc Res. 2000;45(2):279–93.
Stahl A, Gimeno RE, Tartaglia LA, Lodish HF. Fatty acid transport proteins: a current view of a growing family. Trends Endocrinol Metab. 2001;12(6):266–73.
Gil-Sanchez A, Koletzko B, Larque E. Current understanding of placental fatty acid transport. Curr Opin Clin Nutr Metab Care. 2012;15(3):265–72.
Larque E, Krauss-Etschmann S, Campoy C, Hartl D, Linde J, Klingler M, et al. Docosahexaenoic acid supply in pregnancy affects placental expression of fatty acid transport proteins. Am J Clin Nutr. 2006;84(4):853–61.
Lager S, Powell TL. Regulation of nutrient transport across the placenta. J Pregnancy. 2012;2012:179827.
Smits LJ, Elzenga HM, Gemke RJ, Hornstra G, van Eijsden M. The association between interpregnancy interval and birth weight: what is the role of maternal polyunsaturated fatty acid status? BMC Pregnancy Childbirth. 2013;13:23.
Reece MS, McGregor JA, Allen KG, Harris MA. Maternal and perinatal long-chain fatty acids: possible roles in preterm birth. Am J Obstet Gynecol. 1997;176(4):907–14.
Joshi SR, Mehendale SS, Dangat KD, Kilari AS, Yadav HR, Taralekar VS. High maternal plasma antioxidant concentrations associated with preterm delivery. Ann Nutr Metab. 2008;53(3–4):276–82.
Dhobale MV, Wadhwani N, Mehendale SS, Pisal HR, Joshi SR. Reduced levels of placental long chain polyunsaturated fatty acids in preterm deliveries. Prostaglandins Leukot Essent Fatty Acids. 2011;85(3–4):149–53.
Araya J, Rojas M, Fernandez P, Mateluna A. Essential fatty acid content of maternal erythrocyte phospholipids. A study in preterm and full-term human newborns. Rev Med Chil. 1998;126(4):391–6.
Pontes PV, Torres AG, Trugo NM, Fonseca VM, Sichieri R. n-6 and n-3 long-chain polyunsaturated fatty acids in the erythrocyte membrane of Brazilian preterm and term neonates and their mothers at delivery. Prostaglandins Leukot Essent Fatty Acids. 2006;74(2):117–23.
Al-Tamer YY, Mahmood AA. Fatty-acid composition of the colostrum and serum of fullterm and preterm delivering Iraqi mothers. Eur J Clin Nutr. 2004;58(8):1119–24.
Koletzko B, Cetin I, Brenna JT. Dietary fat intakes for pregnant and lactating women. Br J Nutr. 2007;98(5):873–7.
Olsen SF, Secher NJ, Tabor A, Weber T, Walker JJ, Gluud C. Randomised clinical trials of fish oil supplementation in high risk pregnancies. Fish Oil Trials In Pregnancy (FOTIP) Team. BJOG. 2000;107(3):382–95.
Baschat AA. Pathophysiology of fetal growth restriction: implications for diagnosis and surveillance. Obstet Gynecol Surv. 2004;59(8):617–27.
Cetin I, Foidart JM, Miozzo M, Raun T, Jansson T, Tsatsaris V, et al. Fetal growth restriction: a workshop report. Placenta. 2004;25(8–9):753–7.
Vilbergsson G, Wennergren M, Samsioe G, Percy P, Percy A, Mansson JE, et al. Essential fatty acid status is altered in pregnancies complicated by intrauterine growth retardation. World Rev Nutr Diet. 1994;76:105–9.
Cetin I, Giovannini N, Alvino G, Agostoni C, Riva E, Giovannini M, et al. Intrauterine growth restriction is associated with changes in polyunsaturated fatty acid fetal-maternal relationships. Pediatr Res. 2002;52(5):750–5.
Uauy R, Mena P, Wegher B, Nieto S, Salem N Jr. Long chain polyunsaturated fatty acid formation in neonates: effect of gestational age and intrauterine growth. Pediatr Res. 2000;47(1):127–35.
Sattar N, Greer IA, Galloway PJ, Packard CJ, Shepherd J, Kelly T, et al. Lipid and lipoprotein concentrations in pregnancies complicated by intrauterine growth restriction. J ClinEndocrinol Metab. 1999;84(1):128–30.
Sibley CP, Turner MA, Cetin I, Ayuk P, Boyd CA, D’Souza SW, et al. Placental phenotypes of intrauterine growth. Pediatr Res. 2005;58(5):827–32.
Magnusson AL, Waterman IJ, Wennergren M, Jansson T, Powell TL. Triglyceride hydrolase activities and expression of fatty acid binding proteins in the human placenta in pregnancies complicated by intrauterine growth restriction and diabetes. J Clin Endocrinol Metab. 2004;89(9):4607–14.
Powell TL, Jansson T, Illsley NP, Wennergren M, Korotkova M, Strandvik B. Composition and permeability of syncytiotrophoblast plasma membranes in pregnancies complicated by intrauterine growth restriction. Biochim Biophys Acta. 1999;1420(1–2):86–94.
Buchanan TA, Xiang A, Kjos SL, Watanabe R. What is gestational diabetes? Diabetes Care. 2007;30 Suppl 2:S105–11.
Kalra P, Kachhwaha CP, Singh HV. Prevalence of gestational diabetes mellitus and its outcome in western Rajasthan. Indian J Endocrinol Metab. 2013;17(4):677–80.
O’Sullivan JB. Diabetes mellitus after GDM. Diabetes. 1991;40 Suppl 2:131–5.
Bo S, Menato G, Lezo A, Signorile A, Bardelli C, De Michieli F, et al. Dietary fat and gestational hyperglycaemia. Diabetologia. 2001;44(8):972–8.
Radesky JS, Oken E, Rifas-Shiman SL, Kleinman KP, Rich-Edwards JW, Gillman MW. Diet during early pregnancy and development of gestational diabetes. Paediatr Perinat Epidemiol. 2008;22(1):47–59.
Wijendran V, Bendel RB, Couch SC, Philipson EH, Thomsen K, Zhang X, et al. Maternal plasma phospholipid polyunsaturated fatty acids in pregnancy with and without gestational diabetes mellitus: relations with maternal factors. Am J Clin Nutr. 1999;70(1):53–61.
Herrera E, Ortega-Senovilla H. Disturbances in lipid metabolism in diabetic pregnancy - Are these the cause of the problem? Best Pract Res Clin Endocrinol Metab. 2010;24(4):515–25.
Osmond DT, Nolan CJ, King RG, Brennecke SP, Gude NM. Effects of gestational diabetes on human placental glucose uptake, transfer, and utilisation. Diabetologia. 2000;43(5):576–82.
Thomas BA, Ghebremeskel K, Lowy C, Offley-Shore B, Crawford MA. Plasma fatty acids of neonates born to mothers with and without gestational diabetes. Prostaglandins Leukot Essent Fatty Acids. 2005;72(5):335–41.
Bitsanis D, Ghebremeskel K, Moodley T, Crawford MA, Djahanbakhch O. Gestational diabetes mellitus enhances arachidonic and docosahexaenoic acids in placental phospholipids. Lipids. 2006;41(4):341–6.
Dube E, Gravel A, Martin C, Desparois G, Moussa I, Ethier-Chiasson M, et al. Modulation of fatty acid transport and metabolism by maternal obesity in the human full-term placenta. Biol Reprod. 2012;87(1):1–14.
Symonds ME, Pearce S, Bispham J, Gardner DS, Stephenson T. Timing of nutrient restriction and programming of fetal adipose tissue development. Proc Nutr Soc. 2004;63(3):397–403.
Garcia Carrapato MR. The offspring of gestational diabetes. J Perinat Med. 2003;31(1):5–11.
Jamilian M, Samimi M, Kolahdooz F, Khalaji F, Razavi M, Asemi Z. Omega-3 fatty acid supplementation affects pregnancy outcomes in gestational diabetes: a randomized, double-blind, placebo-controlled trial. J Matern Fetal Neonatal Med. 2015;1–7.
Alvino G, Cozzi V, Radaelli T, Ortega H, Herrera E, Cetin I. Maternal and fetal fatty acid profile in normal and intrauterine growth restriction pregnancies with and without preeclampsia. Pediatr Res. 2008;64(6):615–20.
Mahomed K, Williams MA, King IB, Mudzamiri S, Woelk GB. Erythrocyte omega-3, omega-6 and trans fatty acids in relation to risk of preeclampsia among women delivering at Harare Maternity Hospital, Zimbabwe. Physiol Res. 2007;56(1):37–50.
Qiu C, Sanchez SE, Larrabure G, David R, Bralley JA, Williams MA. Erythrocyte omega-3 and omega-6 polyunsaturated fatty acids and preeclampsia risk in Peruvian women. Arch Gynecol Obstet. 2006;274(2):97–103.
Williams MA, Zingheim RW, King IB, Zebelman AM. Omega-3 fatty acids in maternal erythrocytes and risk of preeclampsia. Epidemiology. 1995;6(3):232–7.
Lim WY, Chong M, Calder PC, Kwek K, Chong YS, Gluckman PD, et al. Relations of plasma polyunsaturated fatty acids with blood pressures during the 26th and 28th week of gestation in women of Chinese, Malay, and Indian ethnicity. Medicine (Baltimore). 2015;94(9):e571.
Clausen T, Slott M, Solvoll K, Drevon CA, Vollset SE, Henriksen T. High intake of energy, sucrose, and polyunsaturated fatty acids is associated with increased risk of preeclampsia. Am J Obstet Gynecol. 2001;185(2):451–8.
Mackay VA, Huda SS, Stewart FM, Tham K, McKenna LA, Martin I, et al. Preeclampsia is associated with compromised maternal synthesis of long-chain polyunsaturated fatty acids, leading to offspring deficiency. Hypertension. 2012;60(4):1078–85.
Bakheit KH, Ghebremeskel K, Pol K, Elbashir MI, Adam I. Erythrocyte omega-3 and omega-6 fatty acids profile in Sudanese women with pre-eclampsia. J Obstet Gynaecol. 2010;30(2):151–4.
Kulkarni A, Chavan-Gautam P, Mehendale S, Yadav H, Joshi S. Global DNA methylation patterns in placenta and its association with maternal hypertension in pre-eclampsia. DNA Cell Biol. 2011;30(2):79–84.
Rakheja D, Bennett MJ, Rogers BB. Long-chain L-3-hydroxyacyl-coenzyme a dehydrogenase deficiency: a molecular and biochemical review. Lab Invest. 2002;82(7):815–24.
Wadhwani N, Patil V, Pisal H, Joshi A, Mehendale S, Gupte S, et al. Altered maternal proportions of long chain polyunsaturated fatty acids and their transport leads to disturbed fetal stores in preeclampsia. Prostaglandins Leukot Essent Fatty Acids. 2014;91(1–2):21–30.
Herrera E. Lipid metabolism in pregnancy and its consequences in the fetus and newborn. Endocrine. 2002;19(1):43–55.
Clandinin MT, Chappell JE, Leong S, Heim T, Swyer PR, Chance GW. Intrauterine fatty acid accretion rates in human brain: implications for fatty acid requirements. Early Hum Dev. 1980;4(2):121–9.
Clandinin MT, Chappell JE, Heim T, Swyer PR, Chance GW. Fatty acid utilization in perinatal de novo synthesis of tissues. Early Hum Dev. 1981;5(4):355–66.
De Giuseppe R, Roggi C, Cena H. n-3 LC-PUFA supplementation: effects on infant and maternal outcomes. Eur J Nutr. 2014;53(5):1147–54.
Uhl O, Demmelmair H, Segura MT, Florido J, Rueda R, Campoy C, et al. Effects of obesity and gestational diabetes mellitus on placental phospholipids. Diabetes Res Clin Pract. 2015;109:364–71.
Carlsen K, Pedersen L, Bonnelykke K, Stark KD, Lauritzen L, Bisgaard H. Association between whole-blood polyunsaturated fatty acids in pregnant women and early fetal weight. Eur J Clin Nutr. 2013;67(9):978–83.
Grandjean P, Bjerve KS, Weihe P, Steuerwald U. Birthweight in a fishing community: significance of essential fatty acids and marine food contaminants. Int J Epidemiol. 2001;30(6):1272–8.
Simpson JL, Bailey LB, Pietrzik K, Shane B, Holzgreve W. Micronutrients and women of reproductive potential required dietary intake and consequences of dietary deficiency or excess: Part II–vitamin D, vitamin A, iron, zinc, iodine, essential fatty acids. J Matern Fetal Neonatal Med. 2011;24(1):1–24.
Martinez M. Abnormal profiles of polyunsaturated fatty acids in the brain, liver, kidney and retina of patients with peroxisomal disorders. Brain Res. 1992;583(1–2):171–82.
Hussain G, Schmitt F, Loeffler JP, Gonzalez de Aguilar JL. Fatting the brain: a brief of recent research. Front Cell Neurosci. 2013;7:144.
Chung WL, Chen JJ, Su HM. Fish oil supplementation of control and (n-3) fatty acid-deficient male rats enhances reference and working memory performance and increases brain regional docosahexaenoic acid levels. J Nutr. 2008;138(6):1165–71.
Helland IB, Smith L, Saarem K, Saugstad OD, Drevon CA. Maternal supplementation with very-long-chain n-3 fatty acids during pregnancy and lactation augments children’s IQ at 4 years of age. Pediatrics. 2003;111(1):e39–44.
Jensen CL, Voigt RG, Llorente AM, Peters SU, Prager TC, Zou YL, et al. Effects of early maternal docosahexaenoic acid intake on neuropsychological status and visual acuity at five years of age of breast-fed term infants. J Pediatr. 2010;157(6):900–5.
Neuringer M. Cerebral cortex docosahexaenoic acid is lower in formula-fed than in breast-fed infants. Nutr Rev. 1993;51(8):238–41.
Jamieson EC, Farquharson J, Logan RW, Howatson AG, Patrick WJ, Weaver LT, et al. Infant cerebellar gray and white matter fatty acids in relation to age and diet. Lipids. 1999;34(10):1065–71.
Haag M. Essential fatty acids and the brain. Can J Psychiatry. 2003;48(3):195–203.
Agostoni C. Docosahexaenoic acid (DHA): from the maternal-foetal dyad to the complementary feeding period. Early Hum Dev. 2010;86 Suppl 1:3–6.
Rombaldi Bernardi J, de Souza Escobar R, Ferreira CF, Silveira PP. Fetal and neonatal levels of omega-3: effects on neurodevelopment, nutrition, and growth. Sci World J. 2012;2012:202473.
Smithers LG, Gibson RA, McPhee A, Makrides M. Higher dose of docosahexaenoic acid in the neonatal period improves visual acuity of preterm infants: results of a randomized controlled trial. Am J Clin Nutr. 2008;88(4):1049–56.
Gale CR, Robinson SM, Godfrey KM, Law CM, Schlotz W, O’Callaghan FJ. Oily fish intake during pregnancy–association with lower hyperactivity but not with higher full-scale IQ in offspring. J Child Psychol Psychiatry. 2008;49(10):1061–8.
Hashimoto M, Hossain S. Neuroprotective and ameliorative actions of polyunsaturated fatty acids against neuronal diseases: beneficial effect of docosahexaenoic acid on cognitive decline in Alzheimer’s Disease. J Pharmacol Sci. 2011;116(2):150–62.
Herrera E, Ortega-Senovilla H. Lipid metabolism during pregnancy and its implications for fetal growth. Curr Pharm Biotechnol. 2014;15(1):24–31.
Kubo A, Corley DA, Jensen CD, Kaur R. Dietary factors and the risks of oesophageal adenocarcinoma and Barrett’s oesophagus. Nutr Res Rev. 2010;23(2):230–46.
Innis SM. Perinatal biochemistry and physiology of long-chain polyunsaturated fatty acids. The Journal of Pediatrics. 2003;143(4):1–8.
Innis SM. Fatty acids and early human development. Early Hum Dev. 2007;83(12):761–6.
Helland IB, Saugstad OD, Smith L, Saarem K, Solvoll K, Ganes T, et al. Similar effects on infants of n-3 and n-6 fatty acids supplementation to pregnant and lactating women. Pediatrics. 2001;108(5):e82-e.
Innis SM. Metabolic programming of long-term outcomes due to fatty acid nutrition in early life. Matern Child Nutr. 2011;2(7Suppl):112–23.
Bernardi JR, Ferreira CF, Senter G, Krolow R, de Aguiar BW, Portella AK, et al. Early life stress interacts with the diet deficiency of omega-3 fatty acids during the life course increasing the metabolic vulnerability in adult rats. PLoS ONE. 2013;8(4):e62031.
Moon RJ, Harvey NC, Robinson SM, Ntani G, Davies JH, Inskip HM, et al. Maternal plasma polyunsaturated fatty acid status in late pregnancy is associated with offspring body composition in childhood. J Clin Endocrinol Metab. 2013;98(1):299–307.
Armitage JA, Khan IY, Taylor PD, Nathanielsz PW, Poston L. Developmental programming of the metabolic syndrome by maternal nutritional imbalance: how strong is the evidence from experimental models in mammals? J Physiol. 2004;561(Pt 2):355–77.
Donahue SM, Rifas-Shiman SL, Gold DR, Jouni ZE, Gillman MW, Oken E. Prenatal fatty acid status and child adiposity at age 3 y: results from a US pregnancy cohort. Am J Clin Nutr. 2011;93(4):780–8.
Baur LA, O’Connor J, Pan DA, Storlien LH. Relationships between maternal risk of insulin resistance and the child’s muscle membrane fatty acid composition. Diabetes. 1999;48(1):112–6.
Das UN. A perinatal strategy to prevent coronary heart disease nutrition. 2003;19(11-12):1022–7.
Hussain A, Nookaew I, Khoomrung S, Andersson L, Larsson I, Hulthen L, et al. A maternal diet of fatty fish reduces body fat of offspring compared with a maternal diet of beef and a post-weaning diet of fish improves insulin sensitivity and lipid profile in adult C57BL/6 male mice. Acta Physiol (Oxf). 2013;209(3):220–34.
Bremer AA, Stanhope KL, Graham JL, Cummings BP, Ampah SB, Saville BR, et al. Fish oil supplementation ameliorates fructose-induced hypertriglyceridemia and insulin resistance in adult male rhesus macaques. J Nutr. 2014;144(1):5–11.
Kasbi-Chadli F, Boquien CY, Simard G, Ulmann L, Mimouni V, Leray V, et al. Maternal supplementation with n-3 long chain polyunsaturated fatty acids during perinatal period alleviates the metabolic syndrome disturbances in adult hamster pups fed a high-fat diet after weaning. J Nutr Biochem. 2014;25(7):726–33.
Khaire A, Rathod R, Kemse N, Kale A, Joshi S. Supplementation with omega-3 fatty acids during gestation and lactation to a vitamin B12—deficient or—supplemented diet improves pregnancy outcome and metabolic variables in Wistar rats. Reprod Fertil Dev. 2015a;27(2):341–50.
Khaire A, Rathod R, Kale A, Joshi S. Vitamin B and omega-3 fatty acids together regulate lipid metabolism in Wistar rats. Prostaglandins Leukot Essent Fatty Acids. 2015b.
Gong Q, Zhang X, Xu C. Effect of pregnancy rats supplemented with docosahexaenoic acid on carnitine palmitoyl transferase-I gene expression in offspring. Wei Sheng Yan Jiu. 2009;38(6):685–791.
WHO. Diet, nutrition and the prevention of chronic diseases report of a joint WHO/FAO Expert Consultation, WHO Technical Report Series No. 916, WHO, Geneva.
Koletzko B, Boey CC, Campoy C, Carlson SE, Chang N, Guillermo-Tuazon MA, et al. Current information and Asian perspectives on long-chain polyunsaturated fatty acids in pregnancy, lactation, and infancy: systematic review and practice recommendations from an early nutrition academy workshop. Ann Nutr Metab. 2014;65(1):49–80.
Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. Washington, D. C.: National Academies Press; 2002
Goyal USB, Verma S. Contribution of various foods to fat and fatty acids intake among urban and semi-urban women of Punjab. J Hum Ecol. 2005;18:217–20.
Indian Council of Medical Research (ICMR). Nutrient requirements and recommended dietary allowances for Indians. A report of the expert group of the ICMR, National Institute of Nutrition, Hyderabad, India. 2009.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Khaire, A., Joshi, S. (2016). Maternal Long-chain Polyunsaturated Fatty Acids and Pregnancy Outcome. In: Hegde, M., Zanwar, A., Adekar, S. (eds) Omega-3 Fatty Acids. Springer, Cham. https://doi.org/10.1007/978-3-319-40458-5_35
Download citation
DOI: https://doi.org/10.1007/978-3-319-40458-5_35
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-40456-1
Online ISBN: 978-3-319-40458-5
eBook Packages: MedicineMedicine (R0)