Abstract
As a result of the AYA age range adopted by the US National Cancer Institute Progress Review Group, the authors of this second edition have risen to the challenge of extending the upper age limit from 29 to 39 years. This has uncovered some unanticipated revelations, especially in the realms of epidemiology and biology. For example, in the former, a remarkable and hitherto unknown incidence of prostate cancer in young adults has come to light, while in the latter, the age-related trajectory of characteristics that typify cancers in the AYA population has been expanded to bridge the gap between adolescents and older adults, as in acute lymphoblastic leukemia (ALL) and colorectal cancers. Another important finding is the overdiagnosis of some cancers in AYAs, as best evidenced by renal and thyroid carcinomas. These data have been amplified in the chapters on individual diseases.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Acute Lymphoblastic Leukemia
- Chronic Myeloid Leukemia
- Medical Expenditure Panel Survey
- Peer Support Program
- Biospecimen Bank
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
As a result of the AYA age range adopted by the US National Cancer Institute Progress Review Group, the authors of this second edition have risen to the challenge of extending the upper age limit from 29 to 39 years. This has uncovered some unanticipated revelations, especially in the realms of epidemiology and biology. For example, in the former, a remarkable and hitherto unknown incidence of prostate cancer in young adults has come to light, while in the latter, the age-related trajectory of characteristics that typify cancers in the AYA population has been expanded to bridge the gap between adolescents and older adults, as in acute lymphoblastic leukemia (ALL) and colorectal cancers. Another important finding is the overdiagnosis of some cancers in AYAs, as best evidenced by renal and thyroid carcinomas. These data have been amplified in the chapters on individual diseases.
The chapter on Access and Models of Care derives experiences from several parts of the world, offering examples for others to emulate while emphasizing the modified nostrum that “one size does not fit all.” Elements of special importance to AYAs with cancer – psychological support, sexuality, and oncofertility – receive separate detailed attention. High survival rates, at least in high-income countries, prompt a focus on survivorship. The chapters on rehabilitation and exercise, financial issues, late effects, health-related quality of life, and future health discuss critical elements of the cancer journey. For those who are destined to have that journey cut short, the contributions on ethical issues and palliative/end of life care are particularly relevant.
In 2009 several of the editors of the first edition of this book proposed a list of themes [1] to be addressed in the forthcoming decade. These have been expanded in Table 35.1 and are discussed briefly in the following:
-
1.
Elucidation of parameters other than age that define the AYA patient. In a broad sense, these require greater understanding of the biology of cancers and their AYA hosts. The former will yield to powerful technologies such as next-generation sequencing studies, as described by Pui and colleagues with respect to ALL [2]. The focus on host biology must surely be the physiological trajectory from childhood to adult life and how the inherent changes impact cancer and its treatment. Specimens of tumor and normal tissue from AYAs are more underrepresented in biorepositories than for any other age group.
-
2.
Development of and participation in clinical trials benefiting AYA patients. Collaborative initiatives involving pediatric and medical oncologists are beginning to bear fruit with respect to trial design, including changing limits on age eligibility, that are facilitating the availability of trials to AYAs with cancer. A nut that is proving at least as hard to crack is increasing the accrual of AYAs to these opportunities. There are many pitfalls on the pathway to enrollment [3] requiring multiple tactics to effect improvement, as exemplified by successes in the United Kingdom [4] and the United States [5].
-
3.
Specialization of health services delivery. It has become a mantra in the AYA cancer community that programs, including physical facilities, designed to meet the specific needs of AYA patients will result in better outcomes. The jury has been sequestered but the verdict not yet given, for the evidence has not been subject to the requisite rigorous analyses. These must range from patient-reported outcomes to formal economic evaluation. Moreover, assessments must encompass a spectrum of elements including locus of care, transitions [6], long-term follow up, and future health and well-being. In view of the considerable commitments, not least pecuniary, to mushrooming AYA programs, in-depth assessment of their value must be a high priority.
Fig. 35.1 Average cancer death rate during 2013 in 15- to 49-year-olds in 188 countries (Modified from Institute for Health Metrics and Evaluation (IHME) [36])
-
4.
Focus on oncofertility. If there is one issue that is peculiarly apposite for AYA oncology, this is surely it. Emblematic of the reproductive age span, the AYA population has a dominant interest in the preservation of their fertility. Responding to that need, Teresa Woodruff (who coined the term oncofertility [7]) and her colleagues formed the Oncofertility Consortium in 2006. As stated on their website https://oncofertility.northwestern.edu, “The Oncofertility Consortium is a national interdisciplinary initiative designed to explore the reproductive future of cancer survivors.” This has provided a stimulus for others. In Canada the Cancer Knowledge Network launched the Oncofertility Referral Network in 2014 and is working in collaboration with the Canadian Fertility and Andrology Society to develop a national database that will provide performance metrics in this important area.
-
5.
Professional training in AYA oncology. A stated priority of the standards committee of LIVESTRONG is to foster the development of educational programs, leading to formal certification, in AYA oncology for a wide spectrum of health-care professionals. Independently, initiatives in the United Kingdom, Australia, and Canada have risen to the challenge. In the United Kingdom, the University of Coventry offers three modules of e-learning, available to all health-care professionals, leading to a postgraduate certificate in teenage and young adult cancer care (http://www.coventry.ac.uk). A similar two semester course is offered by the Royal Children’s Hospital in Melbourne, Australia, that provides a graduate certificate of adolescent health and well-being oncology stream (http://www.rch.org.au). As indicated in the Introduction, the Royal College of Physicians and Surgeons of Canada has acknowledged adolescent and young adult oncology as an area of focused competence with a full-time 1-year program for physicians that leads to a diploma in this subject. Additionally, the American Society of Clinical Oncology has 11 current online modules on AYA oncology available at http://university.asco.org/focus-under-forty.
-
6.
The economic cost of medical care is a greater burden on AYAs than on any other age group. In general, they have the least economic resources and, among cancer survivors, the greatest financial hardship [8]. This issue has become all the more acute with the dramatic increase in the cost of cancer drugs that has affected both parenteral and oral medications [9, 10]. In the United States, the most common cause of personal bankruptcy is medical expenditure [11], and a large group of prominent oncologists worldwide has published a request for government regulation on cancer drug costs [12].
-
7.
The role of health insurance for AYAs has also become all the more acute, especially since delays in and suboptimal medical care lead to more advanced stages of cancer in AYAs [13–15]. Since the first edition of this book, the United States made health insurance available to most 18- to 25-year-olds via their parents’ health insurance policies. An estimated 4,000 AYAs were diagnosed with cancer during the first 15 months after insurance companies in the United States were required to cover, up to the age of 26, patients who would otherwise not have been insured [16]. The lack of health insurance for AYAs is more problematic in the United States than elsewhere but underlies the socioeconomic differences in cancer survival outcomes and prevention described in this book.
-
8.
Application of developmental behavior therapy to understanding the experience of cancer in young adulthood. The high prevalence and likely underestimation of psychological distress in AYA survivors of cancer is well described [17]. Regrettably this is related in part to unsatisfied needs for psychological support. This is particularly problematic in the age group 20–29 years [18], defining a population for whom services are especially necessary. The contributions of peer support programs have been important in reducing this deficit, as have the numerous social media targeting the AYA cancer survivor community. Nevertheless, high proportions of these young people report distress, compounded by unmet needs for information, counseling, and practical support. Developing a valid tool for the detection of psychological distress in this population remains in itself an unmet need [19].
-
9.
A specific need is to improve adherence to treatment and diagnostic evaluation. AYAs are the age group that has the least compliance with oral medication and, in the United States at least, the least health insurance to cover the costs of clinical, hospital, and drug costs. In AYAs with leukemia, decreased adherence to oral medications has been associated with lower disease-free survival rates [20, 21]. In adolescents with ALL, only one-third of blood samples showed concentrations of the 6-mercaptopurine active metabolite within the therapeutic reference range [22]. Nonadherence to oral 6-mercaptopurine has been found to increase at an odds ratio of 1.07 per year of age [23]. Young adults with chronic myeloid leukemia, for whom oral therapy with BCR-ABL tyrosine kinase inhibitors is critical, have been shown to have a lower adherence than older adults [24].
-
10.
Support and utilization of the peer advocacy community. The field of AYA oncology has been advanced considerably as a result of the highly effective national initiatives undertaken by communities of advocates and support groups. These have been especially well developed in Australia [25], the United Kingdom [26], and the United States [27]. Particularly notable contributions have been made by LIVESTRONG in the United States that include position statements on quality of care [28] and the training of health professionals [29]. It is anticipated that more initiatives of this sort will be forthcoming. Moreover, as these entities work increasingly and synergistically with organizations of health-care professionals, the pace of progress in AYA oncology will only accelerate, to the benefit of young people with cancer at large.
A review of the unmet needs of AYA with cancer was undertaken by the Institute of Medicine in the United States at a workshop in July 2013 [30]. Particular attention was paid to the psychosocial aspects, integrating data from the AYA HOPE Study [31], an online survey conducted by LIVESTRONG, information provided by the Behavioral Risk Factors and Surveillance System [32] that focused on employment, and the Medical Expenditure Panel Survey [33] that identified the health and economic burden experienced by AYA survivors of cancer. Clearly many needs remain unmet.
This second edition of Cancer in Adolescents and Young Adults highlights the need to revise the classification system for cancer in AYAs [34], an anticipated outcome of the effort of preparing this edition. As noted by Heidi Adams in her Foreword, interest in AYA oncology has gathered a considerable “head of steam.” The metric of the number of publications is useful and will continue as a yardstick. The editors, for example, continue to stimulate interest [35] with others and, will draw attention to the need for good performance indicators, such as clinical trial accruals, increased availability of cancer and host tissue in biospecimen banks, accelerated translational research, and utilization of oncofertility services, as well as rigorous economic evaluation. The need for biospecimens of AYA tumor and normal tissue merits emphasis since AYA tumor and normal tissue samples are more underrepresented in biorepositories than for any other patient age. Without adequate specimens, theme #1 above and in the table cannot be addressed effectively.
As enunciated by others, “it should be clear to all that real results can only be achieved if there is genuine cooperation between, and leadership by, both pediatric oncologists and medical oncologists. While, historically, adult and pediatric healthcare professionals may be unaccustomed to working with each other, their respective experiences and resources should be pooled for the benefit of the AYA patient. It is encouraging to know that willing hands are reaching out to cross the divide.”
There is no room for complacency. The great majority of AYAs with cancer, residing in low- and middle-income countries, cannot avail themselves of the advances described in this volume. Figures 35.1 and 35.2 are derived from a resource developed recently by the Institute for Health Metrics and Evaluation in conjunction with the University of Washington for global comparison of disabilities [36]. Their geographical-visualization world map for cancer illustrates that, for the year 2013, the death rate in 188 countries varies more than tenfold, from 6 to 63 deaths per 100,000 populations per year. The highest cancer death rates among 15- to 49-year-olds worldwide were in Southeast Asia and Eastern Europe, and the lowest rates were in the Middle East, Africa, and the Americas (Fig. 35.1). The 15- to 39-year age data were not available from this resource.
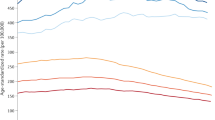
Average number of years lived with cancer (upper panel) and average number of disability-adjusted (lower panel) during 2013 in 15- to 49-year-olds in 188 countries (Modified from Institute for Health Metrics and Evaluation (IHME) [36])
In considering the burden of disease while alive, countries with the most number of years lived with cancer, between the ages 15 and 49, included the United States, Canada, Australia, France, Italy, Belarus, Hungary, Papua New Guinea, and Guyana (Fig. 35.2, upper panel) [36]. Those with the least number of years lived with cancer in this age group were in Africa, the Middle East, India, China, and Southeast Asia (Fig. 35.2, upper panel). The total impact of cancer, as measured by the sum of years lived with cancer plus the years lost due to premature death from cancer (“disability-adjusted life years”), was greatest in Asia and eastern Europe and least in the Middle East, most countries of Africa, North and Central America, most countries of South America, and the Nordic Countries (Fig. 35.2, lower panel).
A comparison of the death rates (Fig. 35.1) with the years lived with cancer (Fig. 35.2, upper panel) provides some explanations for the wide variation in the death rate. The lower mortality rate throughout most of Africa is likely due primarily to a lower incidence. The high death rate and few years of life lived with cancer in Mongolia and Myanmar implicate very poor survival. With both a high rate of deaths and years lived with cancer, the age group in Papua New Guinea and Guyana may also face poor survival. The lower death rates in North America, Western Europe, and Australia can be attributed to better therapy, prolonged survival, and higher cure rates. These regions may also have a higher incidence of cancers that are potentially preventable, such a melanoma and cancer of the lung, oral cavity/oropharynx, anorectum, and uterine cervix [37].
It behooves us, as an international community of stakeholders, to advocate for inclusion of these young people in the evolving success of AYA oncology to which this book is dedicated. As stated by others [38], “though rules and recommendations might be defined to improve our chances of success, the human element remains essential; no progress will be made without the fundamental influence of forward-thinking, charismatic heads willing to dedicate their professional lives to AYA patients.”
References
Albritton K, Barr R, Bleyer A (2010) The adolescence of young adult oncology. Semin Oncol 36:478–488
Pui C-H, Yang JJ, Hunger SP et al (2015) Childhood acute lymphoblastic leukemia: progress through collaboration. J Clin Oncol 33:2938–2948
Freyer DR, Seibel NL (in press) The clinical trials gap for adolescents and young adults with cancer: recent progress and conceptual framework for continued research. Curr Pediatr Rep. doi:10.1007s40124-0075-y
Fern LA, Lewandowski JA, Coxon KM et al (2014) Available, accessible, aware, appropriate, and acceptable: a strategy to improve participation of teenagers and young adults in cancer trials. Lancet Oncol 15:e341–e350
Weiss AR, Nichols CR, Freyer DR (2015) Enhancing adolescent and young adult oncology research within the National Clinical Trials Network: rationale, progress and emerging strategies. Semin Oncol 42:740–747
Wilkins KL, D’Agostino N, Penney AM, Barr RD, Nathan PC (2014) Supporting adolescents and young adults with cancer through transitions: position statement from the Canadian Task Force on adolescents and young adults with cancer. J Pediatr Hematol Oncol 36:545–551
Woodruff TK (2007) The emergence of a new interdiscipline: oncofertility. Cancer Treat Rep 138:3–11
Yabroff KR, Dowling EC, Guy GP Jr et al (2016) Financial hardship associated with cancer in the United States: findings from a population-based sample of adult cancer survivors. J Clin Oncol. Pii; JCO620468 34:259–267
Light DW, Kantarjian H (2013) Market spiral pricing of cancer drugs. Cancer 119:3900–3902
Conti RM, Padula WV, Larson RA (2015) Changing the cost of care for chronic myeloid leukemia: the availability of generic imatinib in the USA and the EU. Ann Hematol 94(Suppl 2):S249–S257
LaMontagne C (2015) NerdWallet Health finds medical bankruptcy accounts for majority of personal bankruptcies. http://www.nerdwallet.com/blog/health/medical-bills/nerdwallet-health-study-estimates-56-million-americans-65-struggle-medical-bills-2013. Accessed 29 Dec 2015
Tefferi A, Kantarjian H, Rajkumar SV et al (2015) In support of a patient-driven initiative and petition to lower the high price of cancer drugs. Mayo Clin Proc 90:996–1000
Martin S, Ulrich C, Munsell M, Taylor S, Lange G, Bleyer A (2007) Delays in cancer diagnosis in under-insured young adults and older adolescents. Oncologist 12:816–824
Wessler JM, Crouch G, Bleyer A, Merino M (2010) Lagtime to oncologic diagnoses: a comparison between military and non-military health care systems. Pediatr Blood Cancer 54: Abstr 195
Robbins AS, Lerro CC, Barr RD (2014) Insurance status and distant-stage disease among adolescent and young adult patients with cancer aged 15–39 years. National Cancer Database, 2004 through 2010. Cancer 120:1212–1219
Bleyer A, Ulrich C, Martin S (2012) Young adults, cancer, health insurance, socioeconomic status and the Patient Protection and Affordable Care Act. Cancer 118:6018–6021
Zebrack BJ, Corbett V, Embry L et al (2014) Psychological distress and unsatisfied need for psychosocial support in adolescent and young adult cancer patients during the first year following diagnosis. Psychooncology 23:1267–1275
Zebrack BJ, Block R, Hayes-Lattin B et al (2013) Psychosocial service use and unmet need among recently diagnosed adolescent and young adult cancer patients. Cancer 119:201–214
Recklitis CJ, Blackmon JE, Chang G (2016) Screening young adult cancer survivors for distress with the distress thermometer: comparisons with a structured clinical diagnostic interview. Cancer 122:296–303
Bhatia S, Landier W, Shangguan M et al (2012) Nonadherence to oral mercaptopurine and risk of relapse in Hispanic and non-Hispanic white children with acute lymphoblastic leukemia. A report from the Children’s Oncology Group. J Clin Oncol 30:2094–2101
Ganesan P, Sagar TG, Dubashi B et al (2011) Nonadherence to imatinib adversely affects event-free survival in chronic phase chronic myeloid leukemia. Am J Hematol 86:471–474
Kremelke K, Juergens C, Alz H, Reinhardt D (2015) Patients’ adherence in the maintenance therapy of children and adolescents with acute lymphoblastic leukemia. Klin Padiatr 227:326–334
Landier W, Chen Y, Hageman L et al (2015) 6-Mercaptopurine intake during maintenance for childhood acute lymphoblastic leukemia – a comparison of self-report and electronic monitoring. A report from the Children’s Oncology Group study AALL03N1. Ann Manag Am Soc Hematol Abstr 82
Anderson KR, Chambers CR, Lam N et al (2015) Medication adherence among adults prescribed dasatinib or nilotinib for the treatment of chronic myeloid leukemia. J Oncol Pharm Pract 21:19–25
Osborn M, Little C, Bowering S, Orme L (2013) Youth cancer services in Australia. Development and implementation. J Adolesc Young Adult Oncol 2:118–124
Fern L, Whelan J (2013) National Cancer Research Institute Teenage and Young Adult Clinical Studies Group: the United Kingdom approach to research. J Adolesc Young Adult Oncol 2:161–165
Johnson RH (2013) AYA in the USA. J Adolesc Young Adult Oncol 2:167–174
Zebrack B, Mathews-Bradshaw B, Siegel S (2010) Quality cancer care for adolescents and young adults: a position statement. J Clin Oncol 28:4862–4867
Hayes-Lattin B, Mathews-Bradshaw B, Siegel S (2010) Adolescent and young adult oncology training for health professionals: a position statement. J Clin Oncol 28:4858–4861
Nass SJ, Beaupin LJ, Demark-Wahnefried W et al (2015) Identifying and addressing the needs of adolescents and young adults with cancer: summary of an Institute of Medicine workshop. Oncologist 20:186–195
Keegan THM, Lichtensztajn DY, Kato I et al (2012) Unmet adolescent and young adult cancer survivors information and service needs: a population-based cancer registry study. J Cancer Surviv 6:239–250
Tai E, Buchanan N, Townsend J et al (2012) Health status of adolescent and young adult cancer survivors. Cancer 118:4884–4891
Guy GP Jr, Ekwueme DU, Yabroff KR et al (2013) Economic burden of cancer survivorship among adults in the United States. J Clin Oncol 31:3749–3757
Barr RD, Holowaty EJ, Birch JM (2006) Classification schemes for tumors diagnosed in adolescents and young adults. Cancer 106:1425–1430
Barr RD, Ferrari A, Ries L, Whelan J, Bleyer WA (2016) A narrative review of cancer in adolescents and young adults. Current status and a view of the future. JAMA Pediatr 170;495–501
Institute for Health Metrics and Evaluation (IHME) (2015) GBD compare. IHME, University of Washington, Seattle, Available from http://vizhub.healthdata.org/gbd-compare. Accessed 20 Jan 2016
Ferrari A, Thomas D, Franklin ARK et al (2010) Starting an adolescent and young adult program: some success stories and some obstacles to overcome. J Clin Oncol 28:4850–4857
Barr RD, Ries LAG, Lewis DR, Harlan LC, Keegan THM, Pollock BR, Bleyer A, for the U.S. National Cancer Institute Next Steps for Adolescent and Young Adult Oncology Epidemiology Working Group (2016) U.S. incidence and incidence trends of the most frequent cancers in adolescent and young adult Americans, including “non-malignant” tumors. Cancer 122;1000–1008
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing
About this chapter
Cite this chapter
Barr, R.D., Ries, L., Ferrari, A., Whelan, J., Bleyer, A. (2017). Conclusions, Perspectives, and Future Considerations. In: Bleyer, A., Barr, R., Ries, L., Whelan, J., Ferrari, A. (eds) Cancer in Adolescents and Young Adults. Pediatric Oncology. Springer, Cham. https://doi.org/10.1007/978-3-319-33679-4_35
Download citation
DOI: https://doi.org/10.1007/978-3-319-33679-4_35
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-33677-0
Online ISBN: 978-3-319-33679-4
eBook Packages: MedicineMedicine (R0)