Abstract
Sarco(endo)plasmic reticulum calcium ATPase (SERCA2a) plays an integral role in Ca2+ cycling in the heart. After a myocardial contraction has occurred, SERCA2a is primarily responsible for transporting Ca2+ out of the cytosol into the sarcoplasmic reticulum. Consequently, SERCA2a is key in determining relaxation time and inotropy of subsequent contractions. There are ten different SERCA isoforms in the body, where SERCA2a is the isoform expressed in the heart. Both SERCA2a expression and activity are reduced in models of disease. As such, a large body of research has examined SERCA2a and how it might be used as a means to restore heart function in models of disease. In this chapter, we examine various regulatory mechanisms of SERCA2a and how these mechanisms affect SERCA2a and cardiac function. Transcriptional, protein (e.g., phospholamban and sarcolipin), hormonal (e.g., thyroid hormone and adiponectin), and posttranslational modification (e.g., nitration, glutathionylation, SUMOylation, acetylation, glycosylation, and O-glcNAcylation) processes as they regulate SERCA2a are discussed. Additionally, exercise and its effect on the regulatory mechanisms of SERCA2a is examined.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Sarco(endo)plasmic reticulum calcium ATPase
- Heart failure
- Phospholamban
- Sarcolipin
- Thyroid hormone
- Adiponectin
- Posttranslational modifications
- Exercise
1 Introduction
1.1 Role of Calcium in Muscular Contractions
Calcium (Ca2+) is a key component of the excitation–contraction coupling (ECC) process in both cardiac and skeletal muscle. When Ca2+ is released from the sarcoplasmic reticulum (SR), free intracellular Ca2+ in the cytosol increases approximately tenfold. This facilitates Ca2+ binding to troponin C, which allows the tropomyosin filament to rotate and expose the myosin-actin binding site [1]. Myosin and actin are then able to interact and initiate cross bridge cycling, where adenosine triphosphate (ATP) hydrolysis moves the myosin along the actin filaments through a series of conformational changes [2]. Cross bridge cycling instigates the power stroke, resulting in muscular contraction. In cardiac muscle, the release of Ca2+ is initiated through Ca2+ induced Ca2+ release, a process where entry of Ca2+ through the L-type Ca2+ channel causes a further release of Ca2+ from the SR [1, 3].
Following contraction, Ca2+ must be removed from the cytoplasm to initiate myocardial relaxation. This occurs through four main transporters: the sarcolemmal Ca2+ ATPase, the mitochondrial Ca2+ uniport, the Na+/Ca2+ exchanger, and the Sarco(endo)plasmic reticulum Ca2+ ATPase (SERCA) [4]. In the mammalian heart, SERCA2a is primarily responsible for removing Ca2+ from the cytoplasm and subsequently transporting it back into the SR [4]. The amount of SERCA2a Ca2+ removal varies between species. For example, SERCA2a accounts for 92 %, 75 %, and 70 % of Ca2+ removal in rat, rabbit, and human hearts, respectively [4, 5].
SERCA2a is a ~110-kDa transmembrane protein that is part of the P-type ATPase category. As such, it functions to actively transport Ca2+ across the SR membrane and into the lumen through ATP hydrolysis [6]. SERCA2a is comprised of three distinct regions: the cytoplasmic head, the transmembrane helices, and the luminal loops [7]. Together, the transmembrane helices and luminal loops create the transmembrane domain [8], while the cytoplasmic head can be further subdivided into three different domains: the actuator domain, phosphorylation domain, and nucleotide domain. Each of these domains plays an integral role in the function of SERCA2a. The transmembrane domain contains two binding sites for Ca2+, and depending on protein conformation, these binding sites can exist in a high- or low-affinity state [9]. The actuator domain, which is the smallest domain, facilitates the major conformational changes that occur as Ca2+ is transported into the lumen [9]. Lastly, the interface between the phosphorylation and nucleotide domains form the catalytic site where ATP hydrolysis occurs [10].
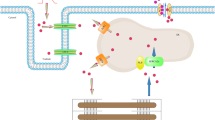
SERCA2a’s major role in Ca2+ transport has made it of primary interest when examining cardiomyopathy. This chapter aims to discuss the regulation of SERCA2a in the heart, its role in heart failure and the mechanisms affecting SERCA2a expression and function. It also examines SERCA2a as a therapeutic target for the prevention or treatment of heart failure. Finally, we describe how exercise may affect cardiac function by regulating SERCA2a function. An overall summary of the mechanisms and pathways affecting SERCA2a can be found in Figs. 11.1 and 11.2.
Summary of SERCA2a transcriptional regulation. Factors affected by exercise are also noted. Abbreviations: miRNA, Micro RNA; MEF2, Myocyte enhancing factor-2; NFAT, Nuclear factor of activated T-cells; SP1, Specificity protein 1; T3/T4, Thyroid hormone; PI3K/Akt, Phosphatidylinositide 3-kinase/protein kinase 3 pathway; TFAM, Mitochondrial transcription factor A; TFB2M, Mitochondrial transcription factor B2
Summary of SERCA2a protein regulation. Factors and pathways affected by exercise are also noted. Abbreviations: T3/T4, Thyroid hormone; PLN, Phospholamban; SLN, Sarcolipin; PKA, Protein Kinase A; CAMKII, Ca2+/Calmodulin-dependent protein kinase II; STK16, Serine/threonine kinase 16; SUMO, SUMOylation; Gluth, Glutathionylation; Acetyl, Acetylation; O-glc, O-GlcNAcylation; Glycos, Glycosylation
2 Transcriptional Regulation
Multiple isoforms of SERCA have been identified, all of which are encoded by one of three SERCA genes: ATP2A1, ATP2A2, and ATP2A3. The human ATP2A2 gene is responsible for encoding the SERCA2a-c isoforms [11], which are expressed in varying quantities throughout the body. ATP2A2 is located on chromosomal region 12q23-q24.1 and is organized into 22 exons [12, 13]. Alternative splicing at exon 20 produces either SERCA2a or SERCA2b [12], where SERCA2a is expressed predominantly in cardiac and smooth muscle and SERCA2b is expressed in both muscle and non-muscle cells [14]. In skeletal muscle, this process is partially mediated by a transcriptional factor known as myogenin [15]; however, little research has explored alternative splicing in cardiac muscle. SERCA2c arises from a splice variant inserted between exon 20 and exon 21 and is expressed in confined regions of the cardiomyocyte [9, 12]. The exact role of SERCA2c is yet to be fully elucidated.
Numerous factors regulate the transcription of ATP2A2. Two of these factors, mitochondrial transcription factors A (TFAM) and B2 (TFB2M), regulate ATP2A2 transcription in the heart by binding to the -122 to -114 and the -122 to -117 regions, respectively [16]. Myocardial SERCA2a transcription is significantly correlated to TFAM and TFB2M expression, suggesting TFAM and TFB2M play an essential role in the regulation of SERCA2a gene transcription. In fact, overexpression of TFAM and TFB2M in rat myocardial infarction models increased SERCA2a transcriptional activity twofold and prevented stress-induced reductions of SERCA2a mRNA levels [16]. Furthermore, mutation of ATP2A2 TFAM and TFB2M binding regions significantly reduced SERCA2 gene transcription [16]. In contrast, diabetic hearts and models of heart failure experience a reduction in TFAM levels [17, 18].
Specificity Protein 1 (SP1) is another transcription factor important to the gene regulation of SERCA2. Evidence suggests SP1 promoter sites are essential for full SERCA2a gene transcription [19, 20]. However, SP1 also mediated the decrease of SERCA2a mRNA seen in pressure overloaded hearts [21]. Therefore, SP1 is partially involved in both the basal and pressure-overloaded induced changes in SERCA2a transcriptional activity.
Myocyte enhancing factor-2 (MEF2) also mediates genetic transcription of SERCA2a. MEF2 is a common target for hypertrophic pathways. Although its exact regulation of SERCA2a is yet to be fully elucidated [22], it appears to upregulate SERCA2a transcription in models of hypertrophy [23, 24]. MEF2C works in conjunction with nuclear factor of activated T-cells (NFAT). In ischemic and dilated hearts removed from transplant patients, MEF2C and NFAT protein levels were significantly correlated [25], where ischemic heart saw a significant increase in both proteins [25]. Additionally, in a study by Vlasblom et al. [23], co-transfection of MEF2C and NFAT stimulated SERCA2a promoter sites, but only when both factors were present. This was accompanied by a 2.5-fold increase in SERCA2a mRNA [23]. In contrast to these findings, diabetic patients with heart failure had significantly decreased MEF2C and SERCA2a protein levels when compared to heart failure patients without diabetes [26]. While more research is needed in this area, MEF2C is another factor to consider when examining the transcriptional regulation of SERCA2a.
MicroRNAs (miRNAs; miR) are a class of small, noncoding mRNA molecules that regulate RNA or protein expression [27, 28]. Since various miRNA recognition sites are located within the 3′ untranslated region of SERCA2, it has been suggested miRNA may affect cardiac function through regulation of SERCA2a protein expression. However, the interaction between SERCA2a and miRNAs is complex, with 43–144 miRNAs affecting SERCA2a expression during heart failure [27–29]. Furthermore, binding sites located on 3′ UTR can bind with multiple miRNAs, and miRNAs themselves can bind with up to 10 different sites [29].
Boštjančič et al. [29] identified ten different miRNAs upregulated in infarcted hearts. Of these 10 miRNAs, miR-25 and -185 have been identified as down regulators of SERCA2a specifically [28–30]. MiR-25 is upregulated 270 % in failing hearts [28], whereas reducing miR-25 expression restored end systolic pressure volume and ejection fraction in pressure-overloaded hearts [28]. Furthermore, miR-25 suppression increased total SERCA2a and SUMOylated SERCA2a levels [28].
In comparison, miR-22 and miR-1 are associated with enhanced SERCA2a expression [27, 31]. MiR-22 knockout mice experienced prolonged Ca2+ cytosolic decay and a 25 % lower SR Ca2+ load than controls [31]. While SERCA2a protein expression was not significantly altered in healthy knockout mice, 1 week of transverse aortic constriction decreased SERCA2a protein content 2.4-fold [31]. Accompanying this decrease was 50 % greater fibrosis levels, impaired fractional shortening, and increased LV end systolic dimensions [31]. MicroRNAs and their regulation of SERCA2a are yet to be fully understood; however, this remains a promising area of research.
Recent studies have begun investigating SERCA2a methylation and the role it may play in SERCA2a expression and function. Methylation is an epigenetic modification that involves the addition of a methyl group to DNA nucleotide [32]. Murine hearts with transverse aortic constriction (TAC) experienced a significant decrease of SERCA2a [33]. This was accompanied by decreased methylation at ATP2A2 promoter sites and increased methylation at ATP2A2 repression sites [33]. Moreover, methylation factors were altered after TAC, with displaced demethylases and recruited methyltransferases at the ATP2A2 promoter regions [33]. Prenatal environment can affect methylation and SERCA2a expression. For example, female mice exposed to estrogen diethylstilbestrol (DES) in utero had increased levels of DNA methylation at the calsequestrin-2 promoter after swim training [34]. Subsequently, SERCA2a and calsequestrin-2 protein expression increased, and cardiac hypertrophy was prevented in mice treated with DES [34].
3 Regulation of SERCA2a in Models of Disease
SERCA2a is a key factor in regulating cardiac contractility and relaxation. As such, there is a substantial amount of research examining SERCA2a in both animal and human heart models. Defective SERCA2a functioning via reduced mRNA, protein expression or activity levels leads to abnormal Ca2+ handling, reduced SR Ca2+ uptake and inefficient energy use [11, 35–37]. These traits are commonly characterized in patients with heart failure and eventually lead to impaired systolic and diastolic function of the heart [11, 37, 38]. In fact, a review of the literature reported significant decreases in SERCA2a mRNA and protein levels in various animal models of heart failure [39]. Moreover, failing human myocardium experienced up to a 60 % decrease in SERCA2a mRNA [39]. Decreases in SERCA2a expression in heart failure is accompanied by diminished activity levels. Arai et al. [35] reported a 50 % reduction in Ca2+ reuptake in right ventricular tissue removed from failing human hearts. However, this effect may be partially mediated by increases in circulating levels of myocardial C-type natriuretic peptide, a molecule known to increase in heart failure [40].
Diabetic hearts also experience a decrease in SERCA2a expression an activity. In diabetic sedentary mice, SERCA2a protein content and maximal SERCA2a activity was decreased by 21 % and 32 %, respectively [41]. This was accompanied by impaired diastolic function [41]. Vasanji et al. [42] reported a decrease in SERCA2a protein content and activity in diabetic hearts, but also noted a significant increase in phospholamban (see Sect. 4 for more details on phospholamban) to SERCA2a protein ratio levels. The underlying mechanisms linking diabetes to SERCA2a activity are not yet fully understood; however it may be partially mediated by reduced enzymatic activity of silent information regulation (SIRT) 1 [43].
Given its integral role in cardiac function, SERCA2a presents a promising target for cardiac treatment. In mice with established diabetic cardiomyopathy, conditional expression of SERCA2a restored cardiac function [44]. Furthermore, activation of SIRT1 in diabetic heart models increased SERCA2a protein and mRNA levels to near control values [43]. In turn, functional parameters of the heart were significantly improved [43]. Transgenic mice overexpressing SERCA1a in the heart demonstrated a 170 %, 50 %, and 66 % increase in maximum Ca2+ uptake velocity, peak rate of myocyte shortening, and relengthening, respectively [45]. However, Kalyanasundaram et al. [46] cautioned against using SERCA1a therapy as a heart failure treatment, reporting increased apoptosis, dilated cardiomyopathy, and early mortality in calsequestrin deficient mice over expressing SERCA1a in the heart.
SERCA2a therapy in human models of heart failure has also been well received. Overexpression of SERCA2a by adenoviral gene transfer in human ventricle cardiomyocytes increased SERCA2a protein number and activity, induced a faster contraction velocity, and enhanced relaxation [47]. Likewise, the CUPID trial found that patients with advanced heart failure experienced up to an 88 % risk reduction in adverse event occurrence, such as LV assistive device implant, heart transplant and death, 12 months after receiving an intracoronary infusion of SERCA2a [48]. A 3-year follow-up found those who receive high-dose infusions still had an 82 % risk reduction for recurrent cardiovascular events [49]. Thus, SERCA2a gene therapy for the treatment of the diseased human heart appears to be beneficial.
4 Protein Regulation of SERCA2a
Phospholamban (PLN) is a 52 amino acid protein that has been well established as an inhibitor of SERCA2a activity [50]. PLN binds to SERCA2a and decreases its affinity for Ca2+ [51]. This binding occurs when cytosolic Ca2+ levels are low and PLN is in a dephosphorylated state. In contrast, phosphorylation of PLN prevents PLN from binding to SERCA2a, allowing SERCA2a to remain active [51]. This occurs through two different mechanisms: Ca2+/Calmodulin kinase (CAMKII) phosphorylation and protein kinase A (PKA) phosphorylation [50, 52]. CAMKII is a serine/threonine protein kinase that is activated by an increase in cytosolic Ca2+ and phosphorylates PLN at the Threonine17 residue [50]. Similarly, PKA phosphorylates PLN at the Serine16 residue [5, 52]; however, PKA phosphorylation is governed through β-adrenergic stimulation. When β-Agonists bind to receptors, a signal transduction pathway is activated that increases production of cyclic AMP (cAMP) via adenylate cyclase [5, 52]. This ultimately activates PKA, which phosphorylates PLN [5, 52]. Phosphorylation of PLN through either of these mechanisms can increase SERCA2a activity up to threefold, increasing relaxation velocity and contributing to the positive inotropic and lusitropic effects of β-adrenergic stimulation [5, 53].
Due to its major role in SERCA2a regulation, PLN expression is closely related to SERCA2a activity. In fact, when compared to wild-type littermates, PLN knockout mice experienced significantly greater contraction and relaxation rates, accompanied by an increase in SERCA2a affinity for Ca2+ [54]. PLN expression varies in quantity throughout the body’s tissues. For example, in the murine heart, PLN is expressed threefold higher in right ventricle tissues compared to right atrial tissues [53]. Consequently, the relative ratio of PLN:SERCA2a is 4.2-fold lower in the atrium and is associated with significantly shortened relaxation and contraction times [53]. Similar findings have been found in the human heart. PLN protein expression is 44 % lower in the right atrium, and time to peak tension, time to relax and total contraction time are significantly decreased when compared to right ventricle tissues [55]. These data suggest that PLN expression, along with phosphorylation, plays a large role in cardiac function though regulation of SERCA2a activity in the heart.
In diseased states, both PLN content and phosphorylation in the heart are altered. As mentioned previously, PLN:SERCA2a ratio is increased in diabetic hearts [42]. Furthermore, PLN phosphorylation by both CAMKII and PKA is significantly decreased [42]. In ischemic and ischemia-reperfused hearts, CAMKII PLN phosphorylation is reduced, whereas PKA PLN phosphorylation is diminished in ischemia-reperfused hearts only [56]. Reduced PLN phosphorylation in heart failure may be partially due to lower levels of taurine, a beta-amino acid found in high concentrations in the heart [57].
Sarcolipin (SLN) is a homologue to PLN with high amino acid conservation in the transmembrane domain [58, 59]. Because of this, SLN and PLN likely interact with SERCA2a in a similar manner, although the precise regulatory mechanisms of SLN are not yet fully elucidated. SLN is a 31 amino acid protein and is thought to induce its inhibitory effect by binding directly to SERCA2a and reducing its affinity for Ca2+ [51, 60]. However, a study suggests SLN acts by reducing the V max of SECA2a Ca2+ uptake, and unlike PLN, it can interact with SERCA2a in the presence of high Ca2+ concentrations [61]. SLN also functions by interacting with PLN to create a super-inhibition of SERCA2a [58, 62]. SLN forms a complex with PLN that destabilizes PLN pentamers [50]. This promotes the formation of PLN monomers, the inhibitory form of PLN [50]. Thus, by enhancing the effects of PLN, SLN acts to further reduce SERCA2a activity.
Babu et al. [60] demonstrated SLN’s effect by over expressing SLN in rat myocytes through adenoviral gene transfer. These myocytes experienced a 31 % reduction in cell shortening compared to control myocytes [60]. SLN’s effect can be relieved through phosphorylation. SLN is phosphorylated by serine/threonine kinase 16 (STK 16) at Threonine5, which promotes dissociation of SLN from SERCA2a and subsequently increases SERCA2a activity [63]. This contributes to the relaxant effect of β-adrenergic stimulation [63]. SLN mRNA is mainly expressed in the atrial tissues of the heart [60]. In fact, Babu et al. [60] found SLN mRNA below detectable levels rat heart ventricle tissues. Similar results have been found in humans, with SLN mRNA being expressed only atrial tissues of the heart [64]. Given the different expression of SLN and PLN in cardiac muscle, it is thought that SLN is responsible for mediating SERCA2a activity where PLN is absent. SLN expression is deregulated in conditions of disease, where SLN mRNA and protein levels can be increased up to 12- and 6-fold, respectively in ventricle tissues [65]. Beyond SLN’s role in Ca2+ regulation, it is also involved in thermoregulation by promoting SERCA2a uncoupling in skeletal muscle [65]. This interaction is unique to SLN [61].
5 Hormonal Regulation of SERCA2a
Thyroid hormone can be found in two different forms in the body: levothyroxine (T4) and triiodothyronine (T3), where T3 is the active form and T4 is a prohormone that is converted into T3 or reverse T3 [66]. While intracellular T3 is about 20 times more potent than T4 [66], administration of both forms has been well documented to affect the expression and activity of SERCA2a [67–71]. This effect occurs through positive regulation of SERCA2a gene transcription [72]. Various animal models have demonstrated thyroid hormone’s impact on SERCA2a. For example, hypothyroid conditions imposed on rat and rabbit cardiomyocytes decreased SERCA2a mRNA content to 36–72 % of control levels, whereas hyperthyroid conditions increased SERCA2a mRNA up to 167 % of control levels [68, 70, 71, 73]. Furthermore, administration of T3 to hypothyroid rat hearts significantly increased SERCA2a mRNA levels 2 h after injection, and normalized it 5 h after injection [71]. Similar results have been found with SERCA2a protein levels, with hypothyroid conditions decreasing protein content 11 %–26 % [69, 73], and hyperthyroid conditions increasing content 34 %–88 % [67, 69].
In addition to its direct regulation of SERCA2a, thyroid hormone further affects SERCA2a activity by regulation of PLN. Thyroid hormone affects PLN in an opposite manner to SERCA2a, where a decrease of T3 or T4 upregulates PLN, and an increase downregulates PLN. Reed et al. [73] demonstrates this in mice hearts, where hypothyroidism increased PLN mRNA and protein levels 28 % and 20 %, respectively and hyperthyroidism decreased PLN mRNA and protein levels 13 % and 30 %, respectively. Similar findings have been reported with rat and rabbit hearts. Hyperthyroid conditions induced up to a 50 % decrease in PLN mRNA and a 25 % decrease in protein levels [68–70]. On the other hand, hypothyroid conditions increased PLN protein content 35 % in rat cardiomyocytes [69].
Coinciding to the changes in SERCA2a and PLN expression, thyroid hormone also induces a change in cardiac function. Chang et al. [67] found administering T4 to rats with aortic banding eliminated abnormal myocardial functioning and increased contractility, relaxation speed, and cytosolic Ca2+ removal when compared to controls. Additionally, both rabbit and rat hyperthyroid hearts have greater Ca2+ maximal uptake than euthyroid hearts [68, 69]. A review by Novitzky and Cooper [66] presents thyroid hormone as a possible treatment for patients with “stunned myocardium,” a condition where myocardial function is depressed due to global or regional ischemic events. These data demonstrate that through regulation of SERCA2a and PLN, thyroid hormone presents a possible means of reversing cardiac dysfunction and inhibiting cellular damage caused by ineffective Ca2+ cycling.
Another hormone responsible for the regulation of SERCA2a is adiponectin . Adiponectin is an adipocyte-derived peptide hormone that is inversely related to traditional cardiovascular risk factors, such as blood pressure, heart rate, and cholesterol and triglyceride levels [74, 75]. It also possesses antioxidant and anti inflammatory qualities [75, 76]. These cardioprotective properties are thought to occur through the modulation of SERCA2a activity [74]. Adiponectin appears to affect SERCA2a through PLN phosphorylation and the PI3K/Akt signaling pathway [74]. In a study by Safwat et al. [74], administration of globular adiponectin significantly restored SERCA2a activity in rats with induced ischemia/reperfusion injury. Additionally, the p-PLN/PLN ratio was significantly increased, suggesting PLN phosphorylation may be the mechanism adiponectin uses to increase SERCA2a activity [74]. Accompanying the increase in SERCA2a activity and PLN phosphorylation was a 139 % increase (p < 0.05) in p-Akt/Akt ratio [74]. Adiponectin induced benefits to cardiac function were abolished with administration of LY294002, an inhibitor of PI3K, confirming that PI3K/Akt pathway activation is essential for globular adiponectin to exert its effect on SERCA2a [74].
Other studies examining adiponectin and SERCA2a activity have shown similar results to Safwat et al. [74]. Adiponectin gene therapy significantly increased SERCA expression in skeletal muscle of diabetic rats [77]. This restoration was furthered by a 9 week swimming exercise protocol [77]. Additionally, treatment of H9C2 cardiomyoblasts in an adiponectin-enriched medium significantly increased SERCA2a expression and decreased in inflammatory markers compared to cardiomyoblasts in an adiponectin depleted culture [78]. In contrast, induction of ER stress through tunicamycin treatment reduced SERCA2a expression, adiponectin, and adiponectin receptor 1 by as much as 50 % [78].
6 Posttranslational Modification Regulation of SERCA2a
Various posttranslational modifications have been found to affect the activity of SERCA2a. Some of these modifications are currently being researched, and as such, the process and effects of these modifications are yet to be fully elucidated. This section will examine current knowledge of nitration, glutathionylation, SUMOylation, acetylation, glycosylation and O-glcNAcylation and their role in SERCA2a function.
Nitration is a chemical process where a nitro group is added to a protein. Nitration inhibits SERCA2a activity through the polyol pathway, a pathway that contributes to oxidative stress in hyperglycemic conditions [79, 80]. In fact, levels of nitrotyrosine on SERCA2a were significantly increased in high-glucose perfused rat hearts compared to hearts perfused with normal glucose levels [80]. Studies on the human heart found nitrotyrosine levels to be nearly doubled in idiopathic dilated cardiomyopathic hearts compared to age matched controls [79]. This was accompanied by a significant positive correlation between time to half relaxation and nitrotyrosine to SERCA2a ratio [79]. This suggests SERCA2a nitration can substantially affect cardiac function [79]. However, nitration’s exact role in normal regulation of SERCA2a is yet to be defined.
Glutathionylation is the process where a disulfide bond is formed between the cysteine of a protein and glutathione (GSH) [81]. In SERCA2a, glutathionylation occurs predominately on cysteine674 [82–84] and subsequently increases SERCA2a activity and Ca2+ uptake [82, 84, 85]. It is well documented that nitric oxide (NO) causes muscle relaxation through cGMP and protein kinase G. However, NO appears to induce relaxation by increasing SERCA2a glutathionylation as well [86]. Exposure to low amounts of oxidative species including NO, Perioxynitrate (ONOO−) and nitroxyl can increase SERCA2a activity 45–60 % in cardiac muscle cells [83–86]. However, it should be noted that NO cannot act alone, and must be combined with the superoxide radical to form ONOO− before it can react with cytosolic GSH and glutathionylate cys674 [82].
While low amounts (10–100 μM) of oxidative species increases SERCA2 activity, transgenic mice exposed to high amounts (>100 μM) experienced a decrease SERCA2 activity [82]. Glutathiolyation can normally be reversed either chemically or enzymatically, but in cases such as atherosclerosis where there is a chronic increase in oxidative species, cys 674 is irreversibly oxidized to sulfonylation [82, 84–86]. Consequently, further glutathiolation and activation of SERCA2a is prevented [82, 84]. This causes a subsequent decrease in SERCA2a activity, which can lead to heart failure. Substances known to reverse glutathiolation, such as dithiothreitol, can help prevent SERCA2 inactivation, but are unable to reverse oxidation once it has occurred [85, 86].
SUMOylation and its effect on SERCA2a is a promising area of research when examining SERCA2a protein stability and function. SUMOylation occurs through the binding of small ubiquitin-like modifier 1 (SUMO1) to the lysine 480 and lysine585 residues of SERCA2a [87, 88]. This modification is thought to have cardioprotective properties [87, 88]. In heart failure, there is a 30 %–40 % decrease in SUMO1, which is accompanied by a decrease in total SERCA2a SUMOylation [87]. Moreover, downregulation of SUMO1 using small hairpin RNA reduced SERCA2a protein levels by 40 % [87]. This is likely due to lower levels of SERCA2a SUMOylation reducing SERCA2a half life from 5.9 to 4.9 days [87]. SUMOylation proved to be a potential therapeutic means when injection of SUMO1 to pressure overloaded hearts significantly improved cardiac performance and restored SERCA2a function and mRNA expression to almost normal levels [87, 88]. The mechanisms SUMOylation uses to rescue SERCA2a function are yet to be fully elucidated. However, it is thought that SUMOylation competes with other posttranslational modifications, such as ubiquitination or acetylation, to increase SERCA2a’s stability and prevent degradation [87]. SERCA2a SUMOylation also appears to increase SERCA2a ATPase activity by increasing its sensitivity to ATP [87].
Acetylation/deacetylation involves the attachment, or removal, of an acetyl group from a molecule. Its precise role in SERCA2a regulation has yet to be examined, although it may regulate SERCA2a in a manner opposite to SUMOylation [89]. Three potential acetylation sites were identified within the nucleotide-binding domain of SERCA2a: lysine464, lysine510, and lysine533 [90]. Therefore, acetylation/deacetylation could play a role in cardiac muscle Ca2+ cycling [90]. Kho et al. [87] reported increased SERCA2a acetylation in failing hearts, which could be reversed with sirtuin-1 deacetylase, but no data was given to validate this statement. Although current evidence is limited, acetylation/deacetylation is a potential regulator of SERCA2a activity.
Glycosylation occurs when a saccharide is attached to a protein. This can be done enzymatically or nonenzymatically, where the nonenzymatic reaction is better known as glycation. An increase in glycosylation has been associated with a 25–45 % decrease in SERCA2a mRNA and protein levels [91, 92] and a 40 % increase in PLN levels [92]. This combination results in an overall decrease in SERCA2a activity, reducing Ca2+ transport into the SR. Since elevated levels of glucose appears to increase SERCA2a glycosylation, this area remains of particular interest when examining the relationship between diabetes and heart disease [91, 92].
O-glcNAcylation is a specific form of glycosylation where a single O-linked N-acetylglucosamine is either added or removed from a serine or threonine residue [91, 93, 94]. O-glcNAcylation reduces SERCA2a activity through direct regulation SERCA2a and modification of PLN [91, 93, 95]. High-glucose treated rat cardiomyocytes had substantially increased levels of nuclear O-glcNAclyation, accompanied by a 28–37 % and 25 % reduction in SERCA2a mRNA and protein expression, respectively [91]. Additionally, cardiomyocytes injected with an O-glcNAc-transferase had a 47 % decrease in SERCA2a expression when compared to controls [91]. In contrast, reducing cellular O-glcNAcylation through an adenovirus expressing O-glcNAcase increased SERCA2a protein expression 40 %, reduced PLN protein 50 %, and increased PLN phosphorylation twofold [94]. SERCA2a O-glcNAcylation may be partially mediated by SP1, as SP1 is known to be heavily O-glcNAcylated and is directly involved in the transcription of SERCA2a [20, 96].
7 Regulation of SERCA2a in Models of Exercise
It has been well documented that exercise increases cardiac function through enhanced SERCA2a Ca2+ uptake, especially in models of cardiovascular disease [97]. This can occur as a result of direct regulation of SERCA2a transcription and activity, or through modifications of the regulatory processes discussed earlier in this chapter. Here, we examine the various processes by which exercise regulates SERCA2a.
Aerobic exercise in hypertensive rats significantly increased cell contractility and Ca2+ transport [97]. These changes were partially due to increased PLN phosphorylation and SERCA2a mRNA expression [97]. Similar results were demonstrated in mice with induced heart failure. Aerobic interval training improved atrial myocyte shortening by 89 % and restored SERCA2a function to near control levels [98]. Additionally, genetic mouse models of sympathetic hyperactivity-induced heart failure experienced greater peak Ca2+ transient levels and reduced diastolic Ca2+ decay time after 8 weeks of aerobic training [99]. These results were enhanced with administration of carvidilol, a beta-blocker used to treat heart failure [99]. Similar benefits have been demonstrated in diabetic models as well. For example, voluntary wheel running in diabetic mice attenuated the decrease in diastolic function and SERCA2a content and activity [41]. Even when disease is absent, cardiac function increases in response to exercise. Kemi et al. [100] reported a 60 % and 50 % increase in fractional myocyte shortening and Ca2+ transient amplitude, respectively, in aerobic interval trained mice. With these adaptations was a 25 % increase in SERCA2a protein content [100]. Wisløff et al. [101] report comparable findings in exercise trained mice, where SERCA2a protein content increased 82 % and Ca2+ cycling and sensitivity was significantly increased compared to sedentary mice. The effects of exercise training on SERCA2a require a stimulus to be maintained. For example, Carneiro-Júnior et al. [97] noted cardiac adaptations to exercise were reversed to control levels after 4 weeks of detraining. Despite these data, some studies have reported that exercise training in aging models was not able to change age related degradations to SERCA2a and cardiac function [102].
Exercise may partially mediate its effect of SERCA2a through regulation of TFAM and TFB2M [16]. Aerobic fitness is positively correlated with mitochondrial biogenesis [103], and thus, requires an increase in mitochondrial transcription factors such as TFAM and TFB2M. TFAM protein expression was significantly higher in elite athletes compared to moderately active individuals [103], and in male participants, TFB2M mRNA levels nearly doubled after 10 days of exercise training with restricted blood flow [103]. Moreover, exercise training in hyperglycemic mice restored TFAM protein to control levels [104]. Therefore, it is likely exercise affects SERCA2a transcription through regulation of TFAM and TFB2M.
Exercise also affects SERCA2a activity by regulating PLN phosphorylation [105]. In aged, ovariectomized rats, exercise training reversed reduced PLN phosphorylation at Threonine17 and normalized SERCA2a activity [105]. Furthermore, aerobic exercise in hypertensive rats significantly increased PLN phosphorylation at both Serine16 and Threonine17 [106]. This contributed to an improved inotropic and lusitropic response to β-adrenergic stimulation [106]. Exercise’s effect on PLN phosphorylation may be partially mediated through CaMKII phosphorylation [100]. Aerobic interval training increases CaMKII Threonine287 phosphorylation, indicating activation [100]; this would contribute to the increase in PLNThr17 phosphorylation observed [100]. Accompanying the increase in PLN phosphorylation, exercise reduces PLN:SERCA2a expression ratios, further enhancing SERCA2a activity [100].
Exercise has varying effects on circulating thyroid hormone, where intense exercise reduces free T3 (fT3) and T3 and increases T4, free T4 (fT4), and thyroid stimulating hormone [107–109]. These changes are acute and most likely due to suppression of T4 to T3 conversion [108]; given proper recovery, thyroid hormone levels are restored within 72 h [108]. In contrast, chronic exercise is associated with a significant increase in thyroid hormone levels. Four weeks of treadmill training increased T3 and T4 in hypothyroid rats to near control levels [110]. This would suggest a subsequent upregulation of SERCA2a. In fact, 4 weeks of wheel running in adult male rats significantly increased thyroid hormone receptor β1 mRNA nearly twofold, which would augment transcription of downstream thyroid hormone target genes, such as SERCA2a [111]. As such, it is likely exercise partially mediates SERCA2a expression through thyroid hormone regulation.
More research is needed to fully understand how adiponectin responds to exercise; however, studies suggest physical activity increases adiponectin levels. Cross-sectional studies report positive correlations between physical activity levels and adiponectin [112, 113], and intervention studies produce similar results. For example, obese individuals randomized to a controlled physical activity-behavior-diet-based lifestyle intervention for 3 months experienced a 34 % increase in adiponectin concentration [114]. Nevertheless, not all studies agree with these results. In a systematic review by Simpson & Singh [115], less than half the studies on chronic exercise and adiponectin reported significant results. While this does not mean exercise does not regulate adiponectin, more rigorous and long-term studies are needed.
Researchers examining exercise and posttranslational modifications have mainly focused on O-glcNAcylation. Six weeks of exercise training in mice decreased O-glcNAcylation 40–75 %, which was paired with a 30 % increase in SERCA mRNA [93, 96]. Moreover, mice trained at a high running capacity had a significantly lower O-glcNAcylated SERCA2a to total SERCA2a ratio than mice trained at a low running capacity [116]. Swim-trained mice experienced a reduction in O-glcNAcylated SP1, suggesting SP1 may be involved in exercise regulation of SERCA2a [96]. It is possible physical activity reduces O-glcNAcylation through regulation of glucose levels, as O-glcNAcylation increases in the presence of glucose [91]. Research on exercise’s effect of other posttranslational modifications if needed to further understand how exercise regulates SERCA2a.
8 Conclusion
Regulation of SERCA2a is governed by numerous factors, such as gene transcription, posttranslational modifications, and endogenous proteins. Given its critical role in heart function and failure, an abundance of research has focused on SERCA2a’a function, regulation, and how it can be used as a therapeutic target. Some of these areas, such as SUMOylation, acetylation, and microRNAs, have yet to be fully elucidated. Exercise has also presented itself as a possible means of effective therapy, although more research is needed on the exact mechanisms here as well. Overall, SERCA2a remains a promising target to maintain and restore heart function and enhance longevity and quality of life.
References
Bers DM (2002) Cardiac excitation-contraction coupling. Nature 415:198–205
Lodish H, Berk A, Zipursky SL et al (2000) Molecular cell biology, 4th edn. W. H Freeman, San Francisco, CA
Fabiato A (1983) Calcium-induced release of calcium from the cardiac sarcoplasmic reticulum. Am J Physiol 245:C1–C14
Bers DM (1997) Ca transport during contraction and relaxation in mammalian ventricular muscle. Basic Res Cardiol 92(Suppl 1):1–10
MacLennan DH, Kranias EG (2003) Phospholamban: a crucial regulator of cardiac contractility. Nat Rev Mol Cell Biol 4:566–577
Tran K, Smith NP, Loiselle DS, Crampin EJ (2009) A thermodynamic model of the cardiac sarcoplasmic/endoplasmic Ca(2+) (SERCA) pump. Biophys J 96:2029–2042
Martonosi AN, Pikula S (2003) The structure of the Ca2+-ATPase of sarcoplasmic reticulum. Acta Biochim Pol 50:337–365
Sacchetto R, Bertipaglia I, Giannetti S et al (2012) Crystal structure of sarcoplasmic reticulum Ca2+-ATPase (SERCA) from bovine muscle. J Struct Biol 178:38–44
Wuytack F, Raeymaekers L, Missiaen L (2002) Molecular physiology of the SERCA and SPCA pumps. Cell Calcium 32:279–305
Toyoshima C, Inesi G (2004) Structural basis of ion pumping by Ca2+-ATPase of the sarcoplasmic reticulum. Annu Rev Biochem 73:269–292
Kawase Y, Hajjar RJ (2008) The cardiac sarcoplasmic/endoplasmic reticulum calcium ATPase: a potent target for cardiovascular diseases. Nat Clin Pract Cardiovasc Med 5:554–565
Gélébart P, Martin V, Enouf J, Papp B (2003) Identification of a new SERCA2 splice variant regulated during monocytic differentiation. Biochem Biophys Res Commun 303:676–684
Otsu K, Fujii J, Periasamy M et al (1993) Chromosome mapping of five human cardiac and skeletal muscle sarcoplasmic reticulum protein genes. Genomics 17:507–509
Loukianov E, Ji Y, Baker DL et al (1998) Sarco(endo)plasmic reticulum Ca2+ ATPase isoforms and their role in muscle physiology and pathology. Ann N Y Acad Sci 853:251–259
Van den Bosch L, Eggermont J, De Smedt H et al (1994) Regulation of splicing is responsible for the expression of the muscle-specific 2a isoform of the sarco/endoplasmic-reticulum Ca(2+)-ATPase. Biochem J 302(Pt 2):559–566
Watanabe A, Arai M, Koitabashi N et al (2011) Mitochondrial transcription factors TFAM and TFB2M regulate Serca2 gene transcription. Cardiovasc Res 90:57–67
Choi YS, Kim S, Pak YK (2001) Mitochondrial transcription factor A (mtTFA) and diabetes. Diabetes Res Clin Pract 54(Suppl 2):S3–S9
Ikeuchi M, Matsusaka H, Kang D et al (2005) Overexpression of mitochondrial transcription factor a ameliorates mitochondrial deficiencies and cardiac failure after myocardial infarction. Circulation 112:683–690
Baker DL, Dave V, Reed T, Periasamy M (1996) Multiple Sp1 binding sites in the cardiac/slow twitch muscle sarcoplasmic reticulum Ca-ATPase gene promoter Are required for expression in Sol8 muscle cells. J Biol Chem 271:5921–5928
Flesch M (2001) On the trail of cardiac specific transcription factors. Cardiovasc Res 50:3–6
Takizawa T, Arai M, Tomaru K et al (2003) Transcription factor Sp1 regulates SERCA2 gene expression in pressure-overloaded hearts: a study using in vivo direct gene transfer into living myocardium. J Mol Cell Cardiol 35:777–783
Zarain-Herzberg A, Fragoso-Medina J, Estrada-Avilés R (2011) Calcium-regulated transcriptional pathways in the normal and pathologic heart. IUBMB Life 63:847–855
Vlasblom R, Muller A, Musters RJP et al (2004) Contractile arrest reveals calcium-dependent stimulation of SERCA2a mRNA expression in cultured ventricular cardiomyocytes. Cardiovasc Res 63:537–544
Zhang Z-Y, Liu X-H, Hu W-C et al (2010) The calcineurin-myocyte enhancer factor 2c pathway mediates cardiac hypertrophy induced by endoplasmic reticulum stress in neonatal rat cardiomyocytes. Am J Physiol Heart Circ Physiol 298:H1499–H1509
Cortés R, Rivera M, Roselló-Lletí E et al (2012) Differences in MEF2 and NFAT transcriptional pathways according to human heart failure aetiology. PLoS One 7, e30915
Razeghi P, Young ME, Cockrill TC et al (2002) Downregulation of myocardial myocyte enhancer factor 2C and myocyte enhancer factor 2C-regulated gene expression in diabetic patients with nonischemic heart failure. Circulation 106:407–411
Kumarswamy R, Lyon AR, Volkmann I et al (2012) SERCA2a gene therapy restores microRNA-1 expression in heart failure via an Akt/FoxO3A-dependent pathway. Eur Heart J 33:1067–1075
Wahlquist C, Jeong D, Rojas-Muñoz A et al (2014) Inhibition of miR-25 improves cardiac contractility in the failing heart. Nature 508:531–535
Boštjančič E, Zidar N, Glavač D (2012) MicroRNAs and cardiac sarcoplasmic reticulum calcium ATPase-2 in human myocardial infarction: expression and bioinformatic analysis. BMC Genomics 13:552
Earls LR, Fricke RG, Yu J et al (2012) Age-dependent microRNA control of synaptic plasticity in 22q11 deletion syndrome and schizophrenia. J Neurosci Off J Soc Neurosci 32:14132–14144
Gurha P, Abreu-Goodger C, Wang T et al (2012) Targeted deletion of microRNA-22 promotes stress-induced cardiac dilation and contractile dysfunction. Circulation 125:2751–2761
Handy DE, Castro R, Loscalzo J (2011) Epigenetic modifications: basic mechanisms and role in cardiovascular disease. Circulation 123:2145–2156
Angrisano T, Schiattarella GG, Keller S et al (2014) Epigenetic switch at atp2a2 and myh7 gene promoters in pressure overload-induced heart failure. PLoS One 9, e106024
Haddad R, Kasneci A, Sebag IA, Chalifour LE (2013) Cardiac structure/function, protein expression, and DNA methylation are changed in adult female mice exposed to diethylstilbestrol in utero. Can J Physiol Pharmacol 91:741–749
Arai M, Alpert NR, MacLennan DH et al (1993) Alterations in sarcoplasmic reticulum gene expression in human heart failure. A possible mechanism for alterations in systolic and diastolic properties of the failing myocardium. Circ Res 72:463–469
Mercadier JJ, Lompré AM, Duc P et al (1990) Altered sarcoplasmic reticulum Ca2(+)-ATPase gene expression in the human ventricle during end-stage heart failure. J Clin Invest 85:305–309
Park WJ, Oh JG (2013) SERCA2a: a prime target for modulation of cardiac contractility during heart failure. BMB Rep 46:237–243
Aronson D, Krum H (2012) Novel therapies in acute and chronic heart failure. Pharmacol Ther 135:1–17
Hasenfuss G (1998) Alterations of calcium-regulatory proteins in heart failure. Cardiovasc Res 37:279–289
Moltzau LR, Aronsen JM, Meier S et al (2013) SERCA2 activity is involved in the CNP-mediated functional responses in failing rat myocardium. Br J Pharmacol 170:366–379
Epp RA, Susser SE, Morissette MP et al (2013) Exercise training prevents the development of cardiac dysfunction in the low-dose streptozotocin diabetic rats fed a high-fat diet. Can J Physiol Pharmacol 91:80–89
Vasanji Z, Dhalla NS, Netticadan T (2004) Increased inhibition of SERCA2 by phospholamban in the type I diabetic heart. Mol Cell Biochem 261:245–249
Sulaiman M, Matta MJ, Sunderesan NR et al (2010) Resveratrol, an activator of SIRT1, upregulates sarcoplasmic calcium ATPase and improves cardiac function in diabetic cardiomyopathy. Am J Physiol Heart Circ Physiol 298:H833–H843
Suarez J, Scott B, Dillmann WH (2008) Conditional increase in SERCA2a protein is able to reverse contractile dysfunction and abnormal calcium flux in established diabetic cardiomyopathy. Am J Physiol Regul Integr Comp Physiol 295:R1439–R1445
Loukianov E, Ji Y, Grupp IL et al (1998) Enhanced myocardial contractility and increased Ca2+ transport function in transgenic hearts expressing the fast-twitch skeletal muscle sarcoplasmic reticulum Ca2+-ATPase. Circ Res 83:889–897
Kalyanasundaram A, Lacombe VA, Belevych AE et al (2013) Up-regulation of sarcoplasmic reticulum Ca(2+) uptake leads to cardiac hypertrophy, contractile dysfunction and early mortality in mice deficient in CASQ2. Cardiovasc Res 98:297–306
del Monte F, Harding SE, Schmidt U et al (1999) Restoration of contractile function in isolated cardiomyocytes from failing human hearts by gene transfer of SERCA2a. Circulation 100:2308–2311
Jessup M, Greenberg B, Mancini D et al (2011) Calcium upregulation by percutaneous administration of gene therapy in cardiac disease (CUPID) a phase 2 trial of intracoronary gene therapy of sarcoplasmic reticulum Ca2+-ATPase in patients with advanced heart failure. Circulation 124:304–313
Zsebo K, Yaroshinsky A, Rudy JJ et al (2014) Long-term effects of AAV1/SERCA2a gene transfer in patients with severe heart failure: analysis of recurrent cardiovascular events and mortality. Circ Res 114:101–108
Bhupathy P, Babu GJ, Periasamy M (2007) Sarcolipin and phospholamban as regulators of cardiac sarcoplasmic reticulum Ca2+ ATPase. J Mol Cell Cardiol 42:903–911
Periasamy M, Bhupathy P, Babu GJ (2008) Regulation of sarcoplasmic reticulum Ca2+ ATPase pump expression and its relevance to cardiac muscle physiology and pathology. Cardiovasc Res 77:265–273
Levitzki A (1988) From epinephrine to cyclic AMP. Science 241:800–806
Koss KL, Ponniah S, Jones WK et al (1995) Differential phospholamban gene expression in murine cardiac compartments. Molecular and physiological analyses. Circ Res 77:342–353
Luo W, Grupp IL, Harrer J et al (1994) Targeted ablation of the phospholamban gene is associated with markedly enhanced myocardial contractility and loss of beta-agonist stimulation. Circ Res 75:401–409
Bokník P, Unkel C, Kirchhefer U et al (1999) Regional expression of phospholamban in the human heart. Cardiovasc Res 43:67–76
Netticadan T, Temsah R, Osada M, Dhalla NS (1999) Status of Ca2+/calmodulin protein kinase phosphorylation of cardiac SR proteins in ischemia-reperfusion. Am J Physiol 277:C384–C391
Ramila KC, Jong CJ, Pastukh VM et al (2015) Role of protein phosphorylation in excitation-contraction coupling in taurine deficient hearts. Am J Physiol Heart Circ Physiol 308(3):H232–H239, ajpheart.00497.2014
Asahi M, Kurzydlowski K, Tada M, MacLennan DH (2002) Sarcolipin inhibits polymerization of phospholamban to induce superinhibition of sarco(endo)plasmic reticulum Ca2+-ATPases (SERCAs). J Biol Chem 277:26725–26728
Asahi M, Sugita Y, Kurzydlowski K et al (2003) Sarcolipin regulates sarco(endo)plasmic reticulum Ca2+-ATPase (SERCA) by binding to transmembrane helices alone or in association with phospholamban. Proc Natl Acad Sci U S A 100:5040–5045
Babu GJ, Zheng Z, Natarajan P et al (2005) Overexpression of sarcolipin decreases myocyte contractility and calcium transient. Cardiovasc Res 65:177–186
Sahoo SK, Shaikh SA, Sopariwala DH et al (2013) Sarcolipin protein interaction with sarco(endo)plasmic reticulum Ca2+ATPase (SERCA) is distinct from phospholamban protein, and only sarcolipin Can promote uncoupling of the SERCA pump. J Biol Chem 288:6881–6889
Zvaritch E, Backx PH, Jirik F et al (2000) The transgenic expression of highly inhibitory monomeric forms of phospholamban in mouse heart impairs cardiac contractility. J Biol Chem 275:14985–14991
Gramolini AO, Trivieri MG, Oudit GY et al (2006) Cardiac-specific overexpression of sarcolipin in phospholamban null mice impairs myocyte function that is restored by phosphorylation. Proc Natl Acad Sci U S A 103:2446–2451
Minamisawa S, Wang Y, Chen J et al (2003) Atrial chamber-specific expression of sarcolipin is regulated during development and hypertrophic remodeling. J Biol Chem 278:9570–9575
Bal NC, Maurya SK, Sopariwala DH et al (2012) Sarcolipin is a newly identified regulator of muscle-based thermogenesis in mammals. Nat Med 18:1575–1579
Novitzky D, Cooper DKC (2014) Thyroid hormone and the stunned myocardium. J Endocrinol 223:R1–R8
Chang KC, Figueredo VM, Schreur JH et al (1997) Thyroid hormone improves function and Ca2+ handling in pressure overload hypertrophy. Association with increased sarcoplasmic reticulum Ca2+-ATPase and alpha-myosin heavy chain in rat hearts. J Clin Invest 100:1742–1749
Kimura Y, Otsu K, Nishida K et al (1994) Thyroid hormone enhances Ca2+ pumping activity of the cardiac sarcoplasmic reticulum by increasing Ca2+ ATPase and decreasing phospholamban expression. J Mol Cell Cardiol 26:1145–1154
Kiss E, Jakab G, Kranias EG, Edes I (1994) Thyroid hormone-induced alterations in phospholamban protein expression. Regulatory effects on sarcoplasmic reticulum Ca2+ transport and myocardial relaxation. Circ Res 75:245–251
Nagai R, Zarain-Herzberg A, Brandl CJ et al (1989) Regulation of myocardial Ca2+-ATPase and phospholamban mRNA expression in response to pressure overload and thyroid hormone. Proc Natl Acad Sci U S A 86:2966–2970
Rohrer D, Dillmann WH (1988) Thyroid hormone markedly increases the mRNA coding for sarcoplasmic reticulum Ca2+-ATPase in the rat heart. J Biol Chem 263:6941–6944
Hartong R, Wang N, Kurokawa R et al (1994) Delineation of three different thyroid hormone-response elements in promoter of rat sarcoplasmic reticulum Ca2+ATPase gene. Demonstration that retinoid X receptor binds 5′ to thyroid hormone receptor in response element 1. J Biol Chem 269:13021–13029
Reed TD, Babu GJ, Ji Y et al (2000) The expression of SR calcium transport ATPase and the Na(+)/Ca(2+)Exchanger are antithetically regulated during mouse cardiac development and in Hypo/hyperthyroidism. J Mol Cell Cardiol 32:453–464
Guo J, Bian Y, Bai R et al (2013) Globular adiponectin attenuates myocardial ischemia/reperfusion injury by upregulating endoplasmic reticulum Ca2+-ATPase activity and inhibiting endoplasmic reticulum stress. J Cardiovasc Pharmacol 62:143–153
Pischon T, Girman CJ, Hotamisligil GS et al (2004) Plasma adiponectin levels and risk of myocardial infarction in men. JAMA 291:1730–1737
Villarreal-Molina MT, Antuna-Puente B (2012) Adiponectin: anti-inflammatory and cardioprotective effects. Biochimie 94:2143–2149
Safwat Y, Yassin N, Gamal El Din M, Kassem L (2013) Modulation of skeletal muscle performance and SERCA by exercise and adiponectin gene therapy in insulin-resistant rat. DNA Cell Biol 32:378–385
Boddu NJ, Theus S, Luo S et al (2014) Is the lack of adiponectin associated with increased ER/SR stress and inflammation in the heart? Adipocyte 3:10–18
Lokuta AJ, Maertz NA, Meethal SV et al (2005) Increased nitration of sarcoplasmic reticulum Ca2+-ATPase in human heart failure. Circulation 111:988–995
Tang WH, Cheng WT, Kravtsov GM, Tong XY et al (2010) Cardiac contractile dysfunction during acute hyperglycemia due to impairment of SERCA by polyol pathway-mediated oxidative stress. Am J Physiol 299:C643–C653
Ghezzi P (2005) Oxidoreduction of protein thiols in redox regulation. Biochem Soc Trans 33:1378
Adachi T, Weisbrod RM, Pimentel DR et al (2004) S-Glutathiolation by peroxynitrite activates SERCA during arterial relaxation by nitric oxide. Nat Med 10:1200–1207
Lancel S, Zhang J, Evangelista A et al (2009) Nitroxyl activates SERCA in cardiac myocytes via glutathiolation of cysteine 674. Circ Res 104:720–723
Tong X, Ying J, Pimentel DR et al (2008) High glucose oxidizes SERCA cysteine-674 and prevents inhibition by nitric oxide of smooth muscle cell migration. J Mol Cell Cardiol 44:361–369
Jardim-Messeder D, Camacho-Pereira J, Galina A (2012) 3-Bromopyruvate inhibits calcium uptake by sarcoplasmic reticulum vesicles but not SERCA ATP hydrolysis activity. Int J Biochem Cell Biol 44:801–807
Adachi T (2010) Modulation of vascular sarco/endoplasmic reticulum calcium ATPase in cardiovascular pathophysiology. In: Vanhoutte PM (ed) Advances in pharmacology. Academic Press, San Diego, CA, pp 165–195
Kho C, Lee A, Jeong D et al (2011) SUMO1-dependent modulation of SERCA2a in heart failure. Nature 477:601–605
Tilemann L, Lee A, Ishikawa K et al (2013) SUMO-1 gene transfer improves cardiac function in a large-animal model of heart failure. Sci Transl Med 5:211ra159
Van Rechem C, Boulay G, Pinte S et al (2010) Differential regulation of HIC1 target genes by CtBP and NuRD, via an acetylation/SUMOylation switch, in quiescent versus proliferating cells. Mol Cell Biol 30:4045–4059
Foster DB, Liu T, Rucker J et al (2013) The cardiac acetyl-lysine proteome. PLoS One 8, e67513
Clark RJ, McDonough PM, Swanson E et al (2003) Diabetes and the accompanying hyperglycemia impairs cardiomyocyte calcium cycling through increased nuclear O-GlcNAcylation. J Biol Chem 278:44230–44237
Bidasee KR, Zhang Y, Shao CH et al (2004) Diabetes increases formation of advanced glycation End products on sarco(endo)plasmic reticulum Ca2+-ATPase. Diabetes 53:463–473
Bennett CE, Johnsen VL, Shearer J, Belke DD (2013) Exercise training mitigates aberrant cardiac protein O-GlcNAcylation in streptozotocin-induced diabetic mice. Life Sci 92:657–663
Hu Y, Belke D, Suarez J et al (2005) Adenovirus-mediated overexpression of O-GlcNAcase improves contractile function in the diabetic heart. Circ Res 96:1006–1013
Yokoe S, Asahi M, Takeda T, Otsu K, Taniguchi N, Miyoshi E, Suzuki K (2010) Inhibition of phospholamban phosphorylation by O-GlcNAcylation: implications for diabetic cardiomyopathy. Glycobiology 20:1217–1226
Belke DD (2011) Swim-exercised mice show a decreased level of protein O-GlcNAcylation and expression of O-GlcNAc transferase in heart. J Appl Physiol 111:157–162
Carneiro-Júnior MA, Quintão-Júnior JF, Drummond LR et al (2013) The benefits of endurance training in cardiomyocyte function in hypertensive rats are reversed within four weeks of detraining. J Mol Cell Cardiol 57:119–128
Johnsen AB, Høydal M, Røsbjørgen R, Stølen T, Wisløff U (2013) Aerobic interval training partly reverse contractile dysfunction and impaired Ca2+ handling in atrial myocytes from rats with post infarction heart failure. PLoS One 8, e66288
Vanzelli AS, Medeiros A, Rolim N et al (2013) Integrative effect of carvedilol and aerobic exercise training therapies on improving cardiac contractility and remodeling in heart failure mice. PLoS One 8, e62452
Kemi OJ, Ellingsen O, Ceci M, Grimaldi S, Smith GL, Condorelli G, Wisløff U (2007) Aerobic interval training enhances cardiomyocyte contractility and Ca2+ cycling by phosphorylation of CaMKII and Thr-17 of phospholamban. J Mol Cell Cardiol 43:354–361
Wisløff U, Loennechen JP, Currie S, Smith GL, Ellingsen Ø (2002) Aerobic exercise reduces cardiomyocyte hypertrophy and increases contractility, Ca2+ sensitivity and SERCA-2 in rat after myocardial infarction. Cardiovasc Res 54:162–174
Thomas MM, Vigna C, Betik AC, Tupling AR, Hepple RT (2011) Cardiac calcium pump inactivation and nitrosylation in senescent rat myocardium are not attenuated by long-term treadmill training. Exp Gerontol 46:803–810
Norrbom J, Wallman SE, Gustafsson T, Rundqvist H, Jansson E, Sundberg CJ (2010) Training response of mitochondrial transcription factors in human skeletal muscle. Acta Physiol (Oxf) 198:71–79
Lumini-Oliveira J, Magalhães J, Pereira CV, Moreira AC, Oliveira PJ, Ascensão A (2011) Endurance training reverts heart mitochondrial dysfunction, permeability transition and apoptotic signaling in long-term severe hyperglycemia. Mitochondrion 11:54–63
Bupha-Intr T, Laosiripisan J, Wattanapermpool J (2009) Moderate intensity of regular exercise improves cardiac SR Ca2+ uptake activity in ovariectomized rats. J Appl Physiol (1985) 107:1105–1112
MacDonnell SM, Kubo H, Crabbe DL, Renna BF, Reger PO, Mohara J, Smithwick LA, Koch WJ, Houser SR, Libonati JR (2005) Improved myocardial beta-adrenergic responsiveness and signaling with exercise training in hypertension. Circulation 111:3420–3428
Ciloglu F, Peker I, Pehlivan A, Karacabey K, Ilhan N, Saygin O, Ozmerdivenli R (2005) Exercise intensity and its effects on thyroid hormones. Neuro Endocrinol Lett 26:830–834
Hackney AC, Kallman A, Hosick KP, Rubin DA, Battaglini CL (2012) Thyroid hormonal responses to intensive interval versus steady-state endurance exercise sessions. Horm Athens Greece 11:54–60
Neto R, de Souza dos Santos M, Rangel I, Ribeiro M, Cavalcanti-de-Albuquerque J, Ferreira A, Cameron L, Carvalho D, Werneck de Castro J (2013) Decreased serum T3 after an exercise session is independent of glucocorticoid peak. Horm Metab Res 45:893–899
Shin M-S, Ko I-G, Kim S-E, Kim B-K, Kim T-S, Lee S-H, Hwang D-S, Kim C-J, Park J-K, Lim B-V (2013) Treadmill exercise ameliorates symptoms of methimazole-induced hypothyroidism through enhancing neurogenesis and suppressing apoptosis in the hippocampus of rat pups. Int J Dev Neurosci 31:214–223
Kinugawa K, Yonekura K, Ribeiro RCJ, Eto Y, Aoyagi T, Baxter JD, Camacho SA, Bristow MR, Long CS, Simpson PC (2001) Regulation of thyroid hormone receptor isoforms in physiological and pathological cardiac hypertrophy. Circ Res 89:591–598
St-Pierre DH, Faraj M, Karelis AD, Conus F, Henry JF, St-Onge M, Tremblay-Lebeau A, Cianflone K, Rabasa-Lhoret R (2006) Lifestyle behaviours and components of energy balance as independent predictors of ghrelin and adiponectin in young non-obese women. Diabetes Metab 32:131–139
Tsukinoki R, Morimoto K, Nakayama K (2005) Association between lifestyle factors and plasma adiponectin levels in Japanese men. Lipids Health Dis 4:27
Balagopal P, George D, Yarandi H, Funanage V, Bayne E (2005) Reversal of obesity-related hypoadiponectinemia by lifestyle intervention: a controlled, randomized study in obese adolescents. J Clin Endocrinol Metab 90:6192–6197
Simpson KA, Singh MAF (2008) Effects of exercise on adiponectin: a systematic review. Obesity 16:241–256
Johnsen VL, Belke DD, Hughey CC, Hittel DS, Hepple RT, Koch LG, Britton SL, Shearer J (2013) Enhanced cardiac protein glycosylation (O-GlcNAc) of selected mitochondrial proteins in rats artificially selected for low running capacity. Physiol Genomics 45:17–25
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Hamm, N.C. et al. (2016). Regulation of Cardiac Sarco(endo)plasmic Reticulum Calcium-ATPases (SERCA2a) in Response to Exercise. In: Chakraborti, S., Dhalla, N. (eds) Regulation of Ca2+-ATPases,V-ATPases and F-ATPases. Advances in Biochemistry in Health and Disease, vol 14. Springer, Cham. https://doi.org/10.1007/978-3-319-24780-9_11
Download citation
DOI: https://doi.org/10.1007/978-3-319-24780-9_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-24778-6
Online ISBN: 978-3-319-24780-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)