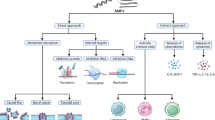
Abstract
Injury that breached the physical skin barrier increases the likelihood of infection. The wound healing process is divided into hemostasis, inflammation, proliferation, and tissue remodeling. Antimicrobial peptides play a major role for the antimicrobial defense at all these stages in wound healing, but the main sources of antimicrobial peptides vary with the different stages of wound healing coming from plasma proteins, neutrophils, and keratinocytes. Apart from being part of the antimicrobial defense, antimicrobial peptides play other important roles in wound healing as in angiogenesis, attraction of leukocytes, resolution of inflammation, and proliferation. Future studies will demonstrate whether antimicrobial peptides can be used therapeutically to improve the wound healing processes and reduce scar formation in chronic wounds.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1.1 Introduction
The intact skin constitutes a very efficient physical barrier toward surrounding microbes. Indeed, skin infections are rarely found in intact healthy skin. However, injury or wounding causes breach in the physical barrier of the skin increasing the likelihood of infections. Keeping the wound free of overt infection is a prerogative for successful wound healing (Edwards and Harding 2004). Indeed, chronic nonhealing cutaneous wounds are most often infected with Staphylococcus aureus or Pseudomonas aeruginosa (Edwards and Harding 2004). Antimicrobial peptides (AMPs) play a major role for the antimicrobial defense during wound healing. Indeed, studies of the remarkable ability of the African frog Xenopus laevis to keep its wounds free of infections under non-sterile conditions led to the first identification of antimicrobial peptides (AMPs) from the skin (Zasloff 1987).
Wound healing following injury is traditionally divided into four stages: (1) hemostasis, (2) inflammation, (3) proliferation, and (4) tissue remodeling (Singer and Clark 1999). AMPs are found at all stages of wound healing; however, the sources of AMPs are different at each of these stages of wound healing.
1.2 Generation of AMPs at the Different Stages of Wound Healing
1.2.1 Injury
Injury by itself leads to generation of AMPs. In frog skin, the injury-induced nervous stimulation leads to release of antimicrobial peptides from skin glands (Simmaco et al. 1998). Though similar mechanisms have not been described in mammals, injury does lead to activation of proteases that release membrane-bound growth factor like HB-EGF and amphiregulin that possess antimicrobial activity (Malmsten et al. 2007). Furthermore, these growth factors play a major role as inducers of the epidermal AMP expression at later stages in the wound healing process (Sørensen et al. 2006, 2008; Roupé et al. 2010). Surely, tissue injury may generate additional AMPs but a systematic study of antimicrobial peptides released by tissue injury is still to come.
1.2.2 Hemostasis
After injury, there is extravasation of plasma proteins into the wound with activation of complement and coagulation cascades. Activation of the complement system leads to generation of fragments of C3a with antimicrobial activity (Nordahl et al. 2004; Sonesson et al. 2007; Pasupuleti et al. 2007). The coagulation cascade is one of the principal host defenses in insects and activation of the human coagulation cascade leads to cleavage of several proteins like kininogen, fibrinogen, and thrombin involved in the coagulation cascade, which leads to generation of several antimicrobial peptides (Frick et al. 2006; Påhlman et al. 2013; Papareddy et al. 2010). Thrombin knockout mice have increased susceptibility to infection with Staphylococcus aureus infection in their limited life span (Mullins et al. 2009), which may indicate an important role of the thrombin-derived AMPs.
1.2.3 Inflammation
After hemostasis follows influx of neutrophils followed by monocytes and lymphocytes to the wounds in the inflammatory stage of wound healing (Singer and Clark 1999). Neutrophils contain large amounts of antimicrobial peptides (Levy 1996; Borregaard and Cowland 1997; Borregaard et al. 2007) important for the microbicidal activity of these cells (Flannagan et al. 2009). During the inflammatory phase, the major AMPs present in the wound will be derived from the neutrophils. The AMPs in neutrophils are found both in neutrophil granules and cytosol (Levy 1996; Borregaard and Cowland 1997). Neutrophils even produce an AMP like elafin after migration to the skin (Theilgaard-Mönch et al. 2004); however, the main antimicrobial peptides found in neutrophils are the α-defensins (HNPs) in azurophil granules (Ganz et al. 1985), cathelicidins in specific granules (Sørensen et al. 1997), and calgranulins (S100A8/S100A9) in the cytosol (Hessian et al. 1993).
The main antimicrobial activity of neutrophil defensins is exerted in the neutrophil phagolysosome (Joiner et al. 1989), but neutrophil defensins are also secreted to the exterior (Ganz 1987; Faurschou et al. 2002). Apart from their direct antibacterial and antiviral activity (Ganz et al. 1985; Daher et al. 1986), defensins also boost bacterial phagocytosis by macrophages (Soehnlein et al. 2008a). Neutrophil defensins have other functions of importance in wound healing. Human neutrophil defensins have chemotactic activity toward monocytes (Territo et al. 1989), T cells (Chertov et al. 1996), and immature dendritic cells (Yang et al. 2000a). Furthermore, these peptides are mitogenic for epithelial cells and fibroblasts (Murphy et al. 1993). Neutrophil defensins do not seem to have a nonredundant function in wound healing since mice neutrophils lack defensins (Eisenhauer and Lehrer 1992).
The cathelicidins present in specific granules (or large granules in rudiments) are stored as inactive proteins in the granules and the biological function is unleashed following extracellular cleavage with serine proteases from azurophil granules (Zanetti 2004). In porcine and bovine neutrophils, the cathelicidins are processed by elastase (Panyutich et al. 1997; Scocchi et al. 1992) while proteinase 3 is responsible for the processing of the human cathelicidin hCAP-18 to the antimicrobial peptide LL-37 (Sørensen et al. 2001), a peptide with broad-spectrum antimicrobial activity (Turner et al. 1998). The elastase-mediated processing porcine cathelicidins has been shown to be important for clearance of bacteria from wounds (Cole et al. 2001). Cathelicidins have other important functions in wound healing, both in the recruitment of mononuclear cells and in the tissue regeneration. It has long be recognized that neutrophils play a major role for the subsequent recruitment of monocytes (Ward 1968), and it has now been recognized that LL-37 plays a role for the recruitment of monocytes (Soehnlein et al. 2008b). Indeed, LL-37 has been shown to be a chemotactic factor toward monocytes as well as T cells and neutrophils (Yang et al. 2000b). Porcine and murine cathelicidins have importance for angiogenesis (Li et al. 2000; Koczulla et al. 2003) and both the porcine PR-39 and the human LL-37 induce expression of VEGF (Rodriguez-Martinez et al. 2008). Furthermore, treatment of wounds with the gene delivery of the human cathelicidin LL-37 promotes wound healing (Jacobsen et al. 2005; Steinstraesser et al. 2014; Carretero et al. 2008). Transactivation of the epidermal growth factor (EGFR) occurs in cutaneous wound healing (Tokumaru et al. 2000) and LL-37 has been shown to cause EGFR transactivation (Tjabringa et al. 2003) and thereby induce keratinocyte migration (Tokumaru et al. 2005). Furthermore, LL-37 suppresses both keratinocyte and neutrophil apoptosis (Chamorro et al. 2009; Nagaoka et al. 2006).
S100A8/S100A9 constitutes 40 % neutrophil cytosolic protein (Edgeworth et al. 1991) and is a potent antifungal agent (Steinbakk et al. 1990). In wounds, neutrophil-derived S100A8/S100A9 is probably released from dying neutrophils or from neutrophil extracellular traps (NETs) and contributes to killing of Candida albicans (Urban et al. 2009). Apart from the direct antifungal effect, S100A9 enhances microbicidal activity of neutrophils by enhancing phagocytosis (Simard et al. 2011) and S100A8/S100A9 is important for neutrophil accumulation in response to LPS (Vandal et al. 2003) and induces neutrophil chemotaxis and adhesion (Ryckman et al. 2003). S100A8/S100A9 mediates proinflammatory activities mediated by binding to TLR-4 (Vogl et al. 2007) or the receptor for advanced glycation end products (RAGE) (Hofmann et al. 1999). Additionally, calgranulins have functions that may limit tissue damage or are anti-inflammatory. S100A8/S100A9 is very sensitive to oxidation (Raftery et al. 2001; Lim et al. 2008) and may, thus, act as oxidant scavenger. S100A8 induces expression of the anti-inflammatory cytokine IL-10 and protects against tissue injury (Hiroshima et al. 2014) and may, thus, play a role in resolution of inflammation.
1.2.4 Proliferative Phase
As the inflammatory cells recede from the wound, the epidermal keratinocytes become a major source for AMPs during the proliferative phase of wound healing. While non-injured epidermis contains constitutively expressed AMPs like hBD-1 and RNase 7, the expression of many AMPs is induced during wound healing and inflammation. Indeed, many AMPs like hBD-2, hBD-3, RNase 7, and psoriasin were originally isolated from inflamed epidermis (Gläser et al. 2005; Harder et al. 1997, 2001; Harder and Schröder 2002). Though some epidermal expression of the human cathelicidin hCAP-18/LL-37 may also be found in the inflammatory stage of wound healing (Dorschner et al. 2001), the peak expression of epidermal AMPs is found during the proliferative phase of wound healing (Roupé et al. 2010). The AMPs with increased epidermal expression during the proliferative phase of wound healing include hBD-2 (Schmid et al. 2001), hBD-3 (Sørensen et al. 2006), psoriasin (S100A7) (Lee and Eckert 2007), S100A8/S100A9 (Thorey et al. 2001), S100A15 (Roupé et al. 2010), elafin (vanBergen et al. 1996), SLPI (Schmid et al. 2001; Wingens et al. 1998), lactoferrin (Roupé et al. 2010), midkine (Frick et al. 2011), and NGAL (Sørensen et al. 2006). Since the various defensins arise from a common ancestral gene (Bevins et al. 1996), it is remarkable that neutrophils and keratinocytes share many of the same AMPs and antimicrobial proteins (see Table 1.1); however, the AMPs in keratinocytes are induced only during wound healing and inflammation while the AMPs in neutrophils are synthesized during normal neutrophil differentiation in the bone barrow (Borregaard et al. 2005). However, this means that the antimicrobial proteins and peptides are present in the wound over and extended time, though the cellular source varies.
The expression of some AMPs during wound healing is dependent on inflammation, i.e., cytokines from infiltrating inflammatory cells as in the case of the IL-1-dependent hBD-2 expression (Liu et al. 2003; Sørensen et al. 2005). However, the expression of other AMPs, like hBD-3, is induced by the injury-induced EGFR activation in epidermal keratinocytes, even in the absence of inflammatory cells (Sørensen et al. 2006; Roupé et al. 2010), thus directly linking growth and tissue regeneration with AMP expression. Deficiency in the injury-induced hBD-3 expression has been linked to the severity of skin infections and nasal carriage of S. aureus (Zanger et al. 2010, 2011; Nurjadi et al. 2013). Additionally, many AMPs like S100A8/S100A9, SLPI, and NGAL are induced both by injury-induced GFR activation and proinflammatory cytokines (Roupé et al. 2010; Mork et al. 2003; Sørensen et al. 2003; Liang et al. 2006).
Though AMP expression mainly is induced during wound healing and inflammation, inflammatory stimuli seem to downregulate the expression of certain AMPs during wound healing. The antimicrobial chemokine CXCL14 is normally expressed in the epidermis (Maerki et al. 2009) but downregulated during wound healing and inflammation (Frick et al. 2011; Maerki et al. 2009). Likewise, RNase 7 protects healthy skin from Staphylococcus aureus infection (Simanski et al. 2010). The expression of RNase 7 is induced both by IFN-γ/IL-17 (Simanski et al. 2013) and significantly by EGFR activation in injured skin ex vivo (Wanke et al. 2011). Though RNase 7 is significantly induced through EGFR activation in injured skin ex vivo, the expression level of RNase 7 is the same in skin wounds in vivo as in non-injured skin (Roupé et al. 2010) indicating that some inflammatory mediators may downregulate the injury-induced RNase 7 expression.
The epidermal AMPs induced by wound healing generate a broad spectrum on antibacterial activity, e.g., hBD-3 against S. aureus and S. pyogenes (Harder et al. 2001), psoriasin against E. coli (Gläser et al. 2005), and calgranulins against C. albicans (Steinbakk et al. 1990). Though, for example, psoriasin has been implicated in defense against E. coli (Gläser et al. 2005) and hBD-3 and RNase 7 against S. aureus (Zanger et al. 2010; Simanski et al. 2010), the appearance of AMPs during the proliferative phase of wound healing raises the question of whether these peptides may play additional roles beyond antimicrobial defense of the wound. Notably, some AMPs seem to remain intracellular or cell associated while other AMPs are secreted. hBD-2 is readily secreted into the medium from multilayer epidermal keratinocyte cell cultures (Sørensen et al. 2005), while hBD-3 remains cell associated, both in multilayer epidermal keratinocytes cell cultures (Sørensen et al. 2005) and in whole epidermis (Sørensen et al. 2006). Though, the antimicrobial S100A proteins psoriasin (S100A7), calgranulins (S100A8/S100A9), and S100A15 are cytosolic, at least psoriasin is also found extracellularly (Gläser et al. 2005). For AMPs to interact with other cells, the AMPs must – at least partially – be found extracellularly.
Numerous cytokine-line functions have been attributed to hBD-2. hBD-2 activates dendritic cells through TLR-4 (Biragyn et al. 2002) and is a chemoattractant toward immature dendritic cells and memory T cells through CCR6 (Yang et al. 1999) and toward neutrophils, monocytes, and macrophages through CCR2 (Röhrl et al. 2010). hBD-2 has been found to promote intestinal wound healing in vitro (Otte et al. 2008) and stimulate proliferation, migration, and cytokine production of epidermal keratinocytes (Niyonsaba et al. 2007).
Likewise, non-antimicrobial functions have been attributed to hBD-3 including chemoattractant properties (Röhrl et al. 2010), antagonism of CXCR4 (Feng et al. 2006), and activation of mast cells with increase of vascular permeability (Chen et al. 2007). However, the fact that hBD-3 appears to remain cell associated in the skin (Sørensen et al. 2005 2006) questions whether these functions play a major role during wound healing.
The non-antimicrobial functions of psoriasin include chemotactic activity toward T lymphocytes and neutrophils (Jinquan et al. 1996) mediated by binding to RAGE (Wolf et al. 2008). This also promotes proliferation of endothelial cells (Shubbar et al. 2012). Psoriasin induces VEGF (Shubbar et al. 2012) and the expression of keratinocyte differentiation markers (Hattori et al. 2014) as wells as strengthens the tight junction barrier in the skin (Hattori et al. 2014).
Though SLPI (secretory leukocyte protease inhibitor) is also found in neutrophils, keratinocytes are the major source of SLPI in wound healing (Jacobsen et al. 2008). SLPI is found to be secreted both in multilayer epidermal keratinocytes cell culture (Sørensen et al. 2003) and whole epidermis (Sørensen et al. 2006). SLPI has antimicrobial activity against bacteria (Hiemstra et al. 1996), fungi (Tomee et al. 1997), and HIV-1 (McNeely et al. 1995). During wound healing, the secreted SLPI has nonredundant functions (Ashcroft et al. 2000) by inhibiting the elastase-mediated cleavage the epithelial growth factor proepithelin to the growth-inhibitory epithelin (Zhu et al. 2002).
1.2.5 Tissue Remodeling Phase
Tissue remodeling in cutaneous wound healing involves increased expression of collagen VI (Betz et al. 1993) that has antimicrobial activity (Abdillahi et al. 2012). Interestingly, collagen VI expression in fibroblasts is induced by neutrophil defensins (Li et al. 2006). The regulation of expression of antimicrobial proteins and peptides in the underlying connective tissue of skin will likely receive more interest after the finding that the normal skin microbiome extends to the connective tissue (Nakatsuji et al. 2013).
1.2.6 Chronic Wounds
Though many studies demonstrate how microbial products induce AMP expression in keratinocytes mainly through TLR activation (Abtin et al. 2008; Büchau et al. 2007, 2008; Li et al. 2013; Nagy et al. 2005; Gariboldi et al. 2008; Gerstel et al. 2009; Liu et al. 2002), the possible significance of this in acute wound healing in noninfected wounds is not clear. The bacteria-induced AMP expression may be more important in chronic wounds with infections (Edwards and Harding 2004). Furthermore, in this instance, the bacterial proteases could play contradictory roles, either by induction of AMP expression through protease-activated receptors (Chung et al. 2004) or by AMP degradation (Schmidtchen et al. 2002). Chronic wounds like chronic venous ulcers are characterized by chronic inflammation with continuous recruitment of inflammatory cells, and indeed neutrophil AMPs like neutrophils defensins are found in high amounts (Lundqvist et al. 2008). The epidermal expression of hBD-2 and psoriasin is induced in chronic venous ulcers (Butmarc et al. 2004; Dressel et al. 2010), while the expression of LL-37 is decreased (Heilborn et al. 2003). In diabetic wounds, the high glucose levels may suppress the expression of both hBD-2 (Lan et al. 2012) and hBD-3 (Lan et al. 2011) in keratinocytes. To understand the role of AMPs in chronic wound pathology or chronic wound infections, more detailed studies are needed to delineate the AMP expression in different types of chronic wounds and how this is related to wound infection or underlying disease such as diabetes.
1.3 Concluding Remarks and Future Perspective
AMPs provide part of the antimicrobial defense during wound healing. Topical application of antimicrobials do not improve normal wound healing (Lipsky and Hoey 2009), demonstrating adequate antimicrobial defenses. While the AMPs originating from the coagulation and complement cascades, the neutrophils, and epidermal keratinocytes undoubtedly contribute to the antimicrobial defense in the wound healing process, it is difficult to decipher the role of individual AMPs due to overlapping antimicrobial activities. Apart from SLPI (Ashcroft et al. 2000), no AMP has been demonstrated to possess nonredundant functions during wound healing.
Though mice models provide useful insight, it is important to note that differences exist between humans and mice – also when it comes to both wound healing and AMPs. Wound contractions are important for wound healing in rodents such as mice, but not in humans (Davidson 1998). Neutrophils and keratinocytes are major sources of AMPs during wound healing, but mice have far fewer neutrophils than humans (Mestas and Hughes 2004) and the mouse epidermis contains far fewer keratinocytes than human epidermis. Accordingly, though no directly comparative studies exist, it seems reasonable that the mouse wounds will contain fewer AMPs than human wounds. There will also be qualitative difference in the AMPs. The mouse contains many more different β-defensins than humans (Schutte et al. 2002), while there will be no neutrophil α-defensins in mouse wounds (Eisenhauer and Lehrer 1992). The neutrophil α-defensins play a role for the antimicrobial function of the neutrophils (Sørensen et al. 2014), and this will undoubtedly be important for the antimicrobial defense also in wounds.
While even infected wounds only in some instances benefit from topical treatment with antibiotics (Lipsky and Hoey 2009), gene delivery of AMPs has been found to have beneficial effects for wound healing (Jacobsen et al. 2005; Steinstraesser et al. 2014; Carretero et al. 2008). This clearly indicates that AMPs have beneficial effects in wound healing beyond its antimicrobial properties. AMPs are generated at all stages of wound healing and it does seem like AMPs participate in the regulation of some aspects of the wound healing processes, for instance, LL-37 plays a role for recruitment of monocytes (Soehnlein et al. 2008b). Resolution of inflammation is now recognized as a regulated process (Serhan and Savill 2005; Ortega-Gomez et al. 2013), and in wounds, AMPs may play an important role here. Dying and necrotic neutrophils are anti-inflammatory due to the release of neutrophil defensins (Miles et al. 2009) and calgranulin S100A8, which induce the anti-inflammatory cytokine IL-10. Later, IL-10 may play a role for downregulation of AMP expression in keratinocytes (Howell et al. 2005). Both defensins and LL-37 promote proliferation of keratinocytes (Niyonsaba et al. 2007; Heilborn et al. 2003). Accordingly, AMPs may play a role for inflammation, resolution of inflammation, and proliferation during wound healing. One of the paradoxes of psoriasis, a disease with very prominent AMP expression (Harder and Schröder 2005), is the lack of scarring following the chronic inflammation (Nickoloff et al. 2006). Future studies will further address the role of AMPs for regulation of the wound healing process and scar formation. This will hopefully pave the way for new treatment modalities for chronic wounds and wound infection.
References
Abdillahi SM, Balvanovic S, Baumgarten M, Mörgelin M (2012) Collagen VI encodes antimicrobial activity: novel innate host defense properties of the extracellular matrix. J Innate Immun 4:371–376
Abtin A, Eckhart L, Mildner M, Gruber F, Schröder JM, Tschachler E (2008) Flagellin is the principal inducer of the antimicrobial peptide S100A7c (psoriasin) in human epidermal keratinocytes exposed to Escherichia coli. FASEB J 22:2168–2176
Ashcroft GS, Lei K, Jin W, Longenecker G, Kulkarni AB, Greenwell-Wild T, Hale-Donze H, McGrady G, Song XY, Wahl SM (2000) Secretory leukocyte protease inhibitor mediates non-redundant functions necessary for normal wound healing. Nat Med 6:1147–1153
Betz P, Nerlich A, Wilske J, Tubel J, Penning R, Eisenmenger W (1993) Immunohistochemical localization of collagen types I and VI in human skin wounds. Int J Legal Med 106:31–34
Bevins CL, Jones DE, Dutra A, Schaffzin J, Muenke M (1996) Human enteric defensin genes: chromosomal map position and a model for possible evolutionary relationships. Genomics 31:95–106
Biragyn A, Ruffini PA, Leifer CA, Klyushnenkova E, Shakhov A, Chertov O, Shirakawa AK, Farber JM, Segal DM, Oppenheim JJ et al (2002) Toll-like receptor 4-dependent activation of dendritic cells by beta-defensin 2. Science 298:1025–1029
Borregaard N, Cowland JB (1997) Granules of the human neutrophilic polymorphonuclear leukocyte. Blood 89:3503–3521
Borregaard N, Theilgaard-Monch K, Cowland JB, Stahle M, Sørensen OE (2005) Neutrophils and keratinocytes in innate immunity – cooperative actions to provide antimicrobial defense at the right time and place. J Leukoc Biol 77:439–443
Borregaard N, Sørensen OE, Theilgaard-Mönch K (2007) Neutrophil granules: a library of innate immunity proteins. Trends Immunol 28:340–345
Büchau AS, Hassan M, Kukova G, Lewerenz V, Kellermann S, Würthner JU, Wolf R, Walz M, Gallo RL, Ruzicka T (2007) S100A15, an antimicrobial protein of the skin: regulation by E-coli through toll-like receptor 4. J Invest Dermatol 127:2596–2604
Büchau AS, Schauber J, Hultsch T, Stuetz A, Gallo RL (2008) Pimecrolimus enhances TLR2/6-induced expression of antimicrobial peptides in keratinocytes. J Invest Dermatol 128:2646–2654
Butmarc J, Yufit T, Carson P, Falanga V (2004) Human beta-defensin-2 expression is increased in chronic wounds. Wound Repair Regen 12:439–443
Carretero M, Escamez MJ, Garcia M, Duarte B, Holguin A, Retamosa L, Jorcano JL, Rio MD, Larcher F (2008) In vitro and in vivo wound healing-promoting activities of human cathelicidin LL-37. J Invest Dermatol 128:223–236
Chamorro CI, Weber G, Gronberg A, Pivarcsi A, Stahle M (2009) The human antimicrobial peptide LL-37 suppresses apoptosis in keratinocytes. J Invest Dermatol 129:937–944
Chen X, Niyonsaba F, Ushio H, Hara M, Yokoi H, Matsumoto K, Saito H, Nagaoka I, Ikeda S, Okumura K et al (2007) Antimicrobial peptides human beta-defensin (hBD)-3 and hBD-4 activate mast cells and increase skin vascular permeability. Eur J Immunol 37:434–444
Chertov O, Michiel DF, Xu L, Wang JM, Tani K, Murphy WJ, Longo DL, Taub DD, Oppenheim JJ (1996) Identification of defensin-1, defensin-2, and CAP37/azurocidin as T- cell chemoattractant proteins released from interleukin-8-stimulated neutrophils. J Biol Chem 271:2935–2940
Chung WO, Hansen SR, Rao D, Dale BA (2004) Protease-activated receptor signaling increases epithelial antimicrobial peptide expression. J Immunol 173:5165–5170
Cole AM, Shi J, Ceccarelli A, Kim YH, Park A, Ganz T (2001) Inhibition of neutrophil elastase prevents cathelicidin activation and impairs clearance of bacteria from wounds. Blood 97:297–304
Daher KA, Selsted ME, Lehrer RI (1986) Direct inactivation of viruses by human granulocyte defensins. J Virol 60:1068–1074
Davidson JM (1998) Animal models for wound repair. Arch Dermatol Res 290(Suppl):S1–S11
Dorschner RA, Pestonjamasp VK, Tamakuwala S, Ohtake T, Rudisill J, Nizet V, Agerberth B, Gudmundsson GH, Gallo RL (2001) Cutaneous injury induces the release of cathelicidin anti-microbial peptides active against group A Streptococcus. J Invest Dermatol 117:91–97
Dressel S, Harder J, Cordes J, Wittersheim M, Meyer-Hoffert U, Sunderkotter C, Glaser R (2010) Differential expression of antimicrobial peptides in margins of chronic wounds. Exp Dermatol 19:628–632
Edgeworth J, Gorman M, Bennett R, Freemont P, Hogg N (1991) Identification of p8,14 as a highly abundant heterodimeric calcium binding protein complex of myeloid cells. J Biol Chem 266:7706–7713
Edwards R, Harding KG (2004) Bacteria and wound healing. Curr Opin Infect Dis 17:91–96
Eisenhauer PB, Lehrer RI (1992) Mouse neutrophils lack defensins. Infect Immun 60:3446–3447
Faurschou M, Sørensen OE, Johnsen AH, Askaa J, Borregaard N (2002) Defensin-rich granules of human neutrophils: characterization of secretory properties. Biochim Biophys Acta 1591:29–35
Feng Z, Dubyak GR, Lederman MM, Weinberg A (2006) Cutting edge: human beta defensin 3 – a novel antagonist of the HIV-1 coreceptor CXCR4. J Immunol 177:782–786
Flannagan RS, Cosio G, Grinstein S (2009) Antimicrobial mechanisms of phagocytes and bacterial evasion strategies. Nat Rev Microbiol 7:355–366
Frick IM, Åkesson P, Herwald H, Mörgelin M, Malmsten M, Nagler DK, Björck L (2006) The contact system – a novel branch of innate immunity generating antibacterial peptides. EMBO J 25:5569–5578
Frick IM, Nordin SL, Baumgarten M, Mörgelin M, Sørensen OE, Olin AI, Egesten A (2011) Constitutive and inflammation-dependent antimicrobial peptides produced by epithelium are differentially processed and inactivated by the commensal Finegoldia magna and the pathogen Streptococcus pyogenes. J Immunol 187:4300–4309
Ganz T (1987) Extracellular release of antimicrobial defensins by human polymorphonuclear leukocytes. Infect Immun 55:568–571
Ganz T, Selsted ME, Szklarek D, Harwig SSL, Daher K, Bainton DF, Lehrer RI (1985) Defensins. Natural peptide antibiotics of human neutrophils. J Clin Invest 6:1427–1435
Gariboldi S, Palazzo M, Zanobbio L, Selleri S, Sommariva M, Sfondrini L, Cavicchini S, Balsari A, Rumio C (2008) Low molecular weight hyaluronic acid increases the self-defense of skin epithelium by induction of beta-defensin 2 via TLR2 and TLR4. J Immunol 181:2103–2110
Gerstel U, Czapp M, Bartels J, Schroder JM (2009) Rhamnolipid-induced shedding of flagellin from Pseudomonas aeruginosa provokes hBD-2 and IL-8 response in human keratinocytes. Cell Microbiol 11:842–853
Gläser R, Harder J, Lange H, Bartels J, Christophers E, Schröder JM (2005) Antimicrobial psoriasin (S100A7) protects human skin from Escherichia coli infection. Nat Immunol 6:57–64
Harder J, Schröder JM (2002) RNase 7, a novel innate immune defense antimicrobial protein of healthy human skin. J Biol Chem 277:46779–46784
Harder J, Schröder JM (2005) Psoriatic scales: a promising source for the isolation of human skin-derived antimicrobial proteins. J Leukoc Biol 77:476–486
Harder J, Bartels J, Christophers E, Schröder JM (1997) A peptide antibiotic from human skin. Nature 387:861
Harder J, Bartels J, Christophers E, Schröder JM (2001) Isolation and characterization of human beta -defensin-3, a novel human inducible peptide antibiotic. J Biol Chem 276:5707–5713
Hattori F, Kiatsurayanon C, Okumura K, Ogawa H, Ikeda S, Okamoto K, Niyonsaba F (2014) The antimicrobial protein S100A7/psoriasin enhances the expression of keratinocyte differentiation markers and strengthens the skin’s tight junction barrier. Br J Dermatol 171:742–753
Heilborn JD, Nilsson MF, Kratz G, Weber G, Sørensen O, Borregaard N, Stahle-Backdahl M (2003) The cathelicidin anti-microbial peptide LL-37 is involved in re-epithelialization of human skin wounds and is lacking in chronic ulcer epithelium. J Invest Dermatol 120:379–389
Hessian PA, Edgeworth J, Hogg N (1993) MRP-8 and MRP-14, two abundant Ca(2+)-binding proteins of neutrophils and monocytes. J Leukoc Biol 53:197–204
Hiemstra PS, Maassen RJ, Stolk J, Heinzel-Wieland R, Steffens GJ, Dijkman JH (1996) Antibacterial activity of antileukoprotease. Infect Immun 64:4520–4524
Hiroshima Y, Hsu K, Tedla N, Chung YM, Chow S, Herbert C, Geczy CL (2014) S100A8 induces IL-10 and protects against acute lung injury. J Immunol 192:2800–2811
Hofmann MA, Drury S, Fu C, Qu W, Taguchi A, Lu Y, Avila C, Kambham N, Bierhaus A, Nawroth P et al (1999) RAGE mediates a novel proinflammatory axis: a central cell surface receptor for S100/calgranulin polypeptides. Cell 97:889–901
Howell MD, Novak N, Bieber T, Pastore S, Girolomoni G, Boguniewicz M, Streib J, Wong C, Gallo RL, Leung DYM (2005) Interleukin-10 downregulates anti-microbial peptide expression in atopic dermatitis. J Invest Dermatol 125:738–745
Jacobsen F, Mittler D, Hirsch T, Gerhards A, Lehnhardt M, Voss B, Steinau HU, Steinstraesser L (2005) Transient cutaneous adenoviral gene therapy with human host defense peptide hCAP-18/LL-37 is effective for the treatment of burn wound infections. Gene Ther 12:1494–1502
Jacobsen LC, Sørensen OE, Cowland JB, Borregaard N, Theilgaard-Mönch K (2008) The secretory leukocyte protease inhibitor (SLPI) and the secondary granule protein lactoferrin are synthesized in myelocytes, colocalize in subcellular fractions of neutrophils, and are coreleased by activated neutrophils. J Leukoc Biol 83:1155–1164
Jinquan T, Vorum H, Larsen CG, Madsen P, Rasmussen HH, Gesser B, Etzerodt M, Honore B, Celis JE, Thestrup-Pedersen K (1996) Psoriasin: a novel chemotactic protein. J Invest Dermatol 107:5–10
Joiner KA, Ganz T, Albert J, Rostrosen D (1989) The opsonizing ligand on salmonella typhimurium influences incorporation of specific, but not azurophil, granule constituents into neutrophil phagosomes. J Cell Biol 109:2771–2782
Koczulla R, Von Degenfeld G, Kupatt C, Krotz F, Zahler S, Gloe T, Issbrucker K, Unterberger P, Zaiou M, Lebherz C et al (2003) An angiogenic role for the human peptide antibiotic LL-37/hCAP-18. J Clin Invest 111:1665–1672
Lan CC, Wu CS, Huang SM, Kuo HY, Wu IH, Wen CH, Chai CY, Fang AH, Chen GS (2011) High-glucose environment inhibits p38MAPK signaling and reduces human beta-defensin-3 expression in keratinocytes. Mol Med 17:771–779
Lan CC, Wu CS, Huang SM, Kuo HY, Wu IH, Liang CW, Chen GS (2012) High-glucose environment reduces human beta-defensin-2 expression in human keratinocytes: implications for poor diabetic wound healing. Br J Dermatol 166:1221–1229
Lee KC, Eckert RL (2007) S100A7 (Psoriasin) – mechanism of antibacterial action in wounds. J Invest Dermatol 127:945–957
Levy O (1996) Antibiotic proteins of polymorphonuclear leukocytes. Eur J Haematol 56:263–277
Li J, Post M, Volk R, Gao Y, Li M, Metais C, Sato K, Tsai J, Aird W, Rosenberg RD et al (2000) PR39, a peptide regulator of angiogenesis. Nat Med 6:49–55
Li J, Raghunath M, Tan D, Lareu RR, Chen Z, Beuerman RW (2006) Defensins HNP1 and HBD2 stimulation of wound-associated responses in human conjunctival fibroblasts. Invest Ophthalmol Vis Sci 47:3811–3819
Li D, Lei H, Li Z, Li H, Wang Y, Lai Y (2013) A novel lipopeptide from skin commensal activates TLR2/CD36-p38 MAPK signaling to increase antibacterial defense against bacterial infection. PLoS One 8:e58288
Liang SC, Tan XY, Luxenberg DP, Karim R, Dunussi-Joannopoulos K, Collins M, Fouser LA (2006) Interleukin (IL)-22 and IL-17 are coexpressed by Th17 cells and cooperatively enhance expression of antimicrobial peptides. J Exp Med 203:2271–2279
Lim SY, Raftery M, Cai H, Hsu K, Yan WX, Hseih HL, Watts RN, Richardson D, Thomas S, Perry M et al (2008) S-nitrosylated S100A8: novel anti-inflammatory properties. J Immunol 181:5627–5636
Lipsky BA, Hoey C (2009) Topical antimicrobial therapy for treating chronic wounds. Clin Infect Dis 49:1541–1549
Liu AY, Destoumieux D, Wong AV, Park CH, Valore EV, Liu L, Ganz T (2002) Human beta-defensin-2 production in keratinocytes is regulated by interleukin-1, bacteria, and the state of differentiation. J Invest Dermatol 118:275–281
Liu L, Roberts AA, Ganz T (2003) By IL-1 signaling, monocyte-derived cells dramatically enhance the epidermal antimicrobial response to lipopolysaccharide. J Immunol 170:575–580
Lundqvist K, Sørensen OE, Schmidtchen A (2008) Increased levels of human neutrophil alpha-defensins in chronic venous leg ulcers. J Dermatol Sci 51:131–134
Maerki C, Meuter S, Liebi M, Muhlemann K, Frederick MJ, Yawalkar N, Moser B, Wolf M (2009) Potent and broad-spectrum antimicrobial activity of CXCL14 suggests an immediate role in skin infections. J Immunol 182:507–514
Malmsten M, Davoudi M, Walse B, Rydengard V, Pasupuleti M, Mörgelin M, Schmidtchen A (2007) Antimicrobial peptides derived from growth factors. Growth Factors 25:60–70
McNeely TB, Dealy M, Dripps DJ, Orenstein JM, Eisenberg SP, Wahl SM (1995) Secretory leukocyte protease inhibitor: a human saliva protein exhibiting anti-human immunodeficiency virus 1 activity in vitro. J Clin Invest 96:456–464
Mestas J, Hughes CC (2004) Of mice and not men: differences between mouse and human immunology. J Immunol 172:2731–2738
Miles K, Clarke DJ, Lu W, Sibinska Z, Beaumont PE, Davidson DJ, Barr TA, Campopiano DJ, Gray M (2009) Dying and necrotic neutrophils are anti-inflammatory secondary to the release of alpha-defensins. J Immunol 183:2122–2132
Mork G, Schjerven H, Mangschau L, Soyland E, Brandtzaeg P (2003) Proinflammatory cytokines upregulate expression of calprotectin (L1 protein, MRP-8/MRP-14) in cultured human keratinocytes. Br J Dermatol 149:484–491
Mullins ES, Kombrinck KW, Talmage KE, Shaw MA, Witte DP, Ullman JM, Degen SJ, Sun W, Flick MJ, Degen JL (2009) Genetic elimination of prothrombin in adult mice is not compatible with survival and results in spontaneous hemorrhagic events in both heart and brain. Blood 113:696–704
Murphy CJ, Foster BA, Mannis MJ, Selsted ME, Reid TW (1993) Defensins are mitogenic for epithelial cells and fibroblasts. J Cell Physiol 155:408–413
Nagaoka I, Tamura H, Hirata M (2006) An antimicrobial cathelicidin peptide, human CAP18/LL-37, suppresses neutrophil apoptosis via the activation of formyl-peptide receptor-like 1 and P2X7. J Immunol 176:3044–3052
Nagy I, Pivarcsi A, Koreck A, Szell M, Urban E, Kemeny L (2005) Distinct strains of Propionibacterium acnes induce selective human beta-defensin-2 and interleukin-8 expression in human keratinocytes through toll-like receptors. J Invest Dermatol 124:931–938
Nakatsuji T, Chiang HI, Jiang SB, Nagarajan H, Zengler K, Gallo RL (2013) The microbiome extends to subepidermal compartments of normal skin. Nat Commun 4:1431
Nickoloff BJ, Bonish BK, Marble DJ, Schriedel KA, DiPietro LA, Gordon KB, Lingen MW (2006) Lessons learned from psoriatic plaques concerning mechanisms of tissue repair, remodeling, and inflammation. J Investig Dermatol Symp Proc 11:16–29
Niyonsaba F, Ushio H, Nakano N, Ng W, Sayama K, Hashimoto K, Nagaoka I, Okumura K, Ogawa H (2007) Antimicrobial peptides human beta-defensins stimulate epidermal keratinocyte migration, proliferation and production of proinflammatory cytokines and chemokines. J Invest Dermatol 127:594–604
Nordahl EA, Rydengard V, Nyberg P, Nitsche DP, Morgelin M, Malmsten M, Bjorck L, Schmidtchen A (2004) Activation of the complement system generates antibacterial peptides. Proc Natl Acad Sci U S A 101:16879–16884
Nurjadi D, Herrmann E, Hinderberger I, Zanger P (2013) Impaired beta-defensin expression in human skin links DEFB1 promoter polymorphisms with persistent Staphylococcus aureus nasal carriage. J Infect Dis 207:666–674
Ortega-Gomez A, Perretti M, Soehnlein O (2013) Resolution of inflammation: an integrated view. EMBO Mol Med 5:661–674
Otte JM, Werner I, Brand S, Chromik AM, Schmitz F, Kleine M, Schmidt WE (2008) Human beta defensin 2 promotes intestinal wound healing in vitro. J Cell Biochem 104:2286–2297
Påhlman LI, Mörgelin M, Kasetty G, Olin AI, Schmidtchen A, Herwald H (2013) Antimicrobial activity of fibrinogen and fibrinogen-derived peptides – a novel link between coagulation and innate immunity. Thromb Haemost 109:930–939
Panyutich P, Shi J, Boutz PL, Zhao C, Ganz T (1997) Porcine polymorphonuclear leukocytes generate extracellular microbial activity by elastase-mediated activation of secreted proprotegrins. Infect Immun 65:978–985
Papareddy P, Rydengard V, Pasupuleti M, Walse B, Morgelin M, Chalupka A, Malmsten M, Schmidtchen A (2010) Proteolysis of human thrombin generates novel host defense peptides. PLoS Pathog 6:e1000857
Pasupuleti M, Walse B, Nordahl EA, Morgelin M, Malmsten M, Schmidtchen A (2007) Preservation of antimicrobial properties of complement peptide C3a, from invertebrates to humans. J Biol Chem 282:2520–2528
Raftery MJ, Yang Z, Valenzuela SM, Geczy CL (2001) Novel intra- and inter-molecular sulfinamide bonds in S100A8 produced by hypochlorite oxidation. J Biol Chem 276:33393–33401
Rodriguez-Martinez S, Cancino-Diaz JC, Vargas-Zuniga LM, Cancino-Diaz ME (2008) LL-37 regulates the overexpression of vascular endothelial growth factor (VEGF) and c-IAP-2 in human keratinocytes. Int J Dermatol 47:457–462
Röhrl J, Yang D, Oppenheim JJ, Hehlgans T (2010) Human beta-defensin 2 and 3 and their mouse orthologs induce chemotaxis through interaction with CCR2. J Immunol 184:6688–6694
Roupé KM, Nybo M, Sjöbring U, Alberius P, Schmidtchen A, Sørensen OE (2010) Injury is a major inducer of epidermal innate immune responses during wound healing. J Invest Dermatol 130:1167–1177
Ryckman C, Vandal K, Rouleau P, Talbot M, Tessier PA (2003) Proinflammatory activities of S100: proteins S100A8, S100A9, and S100A8/A9 induce neutrophil chemotaxis and adhesion. J Immunol 170:3233–3242
Schmid P, Grenet O, Medina J, Chibout SD, Osborne C, Cox DA (2001) An intrinsic antibiotic mechanism in wounds and tissue-engineered skin. J Invest Dermatol 116:471–472
Schmidtchen A, Frick IM, Andersson E, Tapper H, Björck L (2002) Proteinases of common pathogenic bacteria degrade and inactivate the antibacterial peptide LL-37. Mol Microbiol 46:157–168
Schutte BC, Mitros JP, Bartlett JA, Walters JD, Jia HP, Welsh MJ, Casavant TL, McCray PB Jr (2002) Discovery of five conserved beta -defensin gene clusters using a computational search strategy. Proc Natl Acad Sci U S A 99:2129–2133
Scocchi M, Skerlavaj B, Romeo D, Gennaro R (1992) Proteolytic cleavage by neutrophil elastase converts inactive storage proforms to antibacterial bactenecins. Eur J Biochem 209:589–595
Serhan CN, Savill J (2005) Resolution of inflammation: the beginning programs the end. Nat Immunol 6:1191–1197
Shubbar E, Vegfors J, Carlstrom M, Petersson S, Enerback C (2012) Psoriasin (S100A7) increases the expression of ROS and VEGF and acts through RAGE to promote endothelial cell proliferation. Breast Cancer Res Treat 134:71–80
Simanski M, Dressel S, Glaser R, Harder J (2010) RNase 7 protects healthy skin from Staphylococcus aureus colonization. J Invest Dermatol 130:2836–2838
Simanski M, Rademacher F, Schroder L, Schumacher HM, Glaser R, Harder J (2013) IL-17A and IFN-gamma synergistically induce RNase 7 expression via STAT3 in primary keratinocytes. PLoS One 8:e59531
Simard JC, Simon MM, Tessier PA, Girard D (2011) Damage-associated molecular pattern S100A9 increases bactericidal activity of human neutrophils by enhancing phagocytosis. J Immunol 186:3622–3631
Simmaco M, Mignogna G, Barra D (1998) Antimicrobial peptides from amphibian skin: what do they tell us? Biopolymers 47:435–450
Singer AJ, Clark RA (1999) Cutaneous wound healing. N Engl J Med 341:738–746
Soehnlein O, Kai-Larsen Y, Frithiof R, Sorensen OE, Kenne E, Scharffetter-Kochanek K, Eriksson EE, Herwald H, Agerberth B, Lindbom L (2008a) Neutrophil primary granule proteins HBP and HNP1-3 boost bacterial phagocytosis by human and murine macrophages. J Clin Invest 118:3491–3502
Soehnlein O, Zernecke A, Eriksson EE, Rothfuchs AG, Pham CT, Herwald H, Bidzhekov K, Rottenberg ME, Weber C, Lindbom L (2008b) Neutrophil secretion products pave the way for inflammatory monocytes. Blood 112:1461–1471
Sonesson A, Ringstad L, Nordahl EA, Malmsten M, Morgelin M, Schmidtchen A (2007) Antifungal activity of C3a and C3a-derived peptides against Candida. Biochim Biophys Acta 1768:346–353
Sørensen O, Arnljots K, Cowland JB, Bainton DF, Borregaard N (1997) The human antibacterial Cathelicidin, hCAP-18, is synthesized in myelocytes and metamyelocytes and localized to specific granules in neutrophils. Blood 90:2796–2803
Sørensen OE, Follin P, Johnsen AH, Calafat J, Tjabringa GS, Hiemstra PS, Borregaard N (2001) Human cathelicidin, hCAP-18, is processed to the antimicrobial peptide LL-37 by extracellular cleavage with proteinase 3. Blood 97:3951–3959
Sørensen OE, Cowland JB, Theilgaard-Mönch K, Liu L, Ganz T, Borregaard N (2003) Wound healing and expression of antimicrobial peptides/polypeptides in keratinocytes, a consequence of common growth factors. J Immunol 170:5583–5589
Sørensen OE, Thapa DR, Rosenthal A, Liu L, Roberts AA, Ganz T (2005) Differential regulation of β-defensin expression in human skin by microbial stimuli. J Immunol 174:4870–4879
Sørensen OE, Thapa DR, Roupe KM, Valore EV, Sjobring U, Roberts AA, Schmidtchen A, Ganz T (2006) Injury-induced innate immune response in human skin mediated by transactivation of the epidermal growth factor receptor. J Clin Invest 116:1878–1885
Sørensen OE, Schmidtchen A, Roupe KM (2008) EGF receptor: role for innate immunity during wound healing in human skin. Expert Rev Dermatol 3:587–593
Sørensen OE, Clemmensen SN, Dahl SL, Østergaard O, Heegaard NH, Glenthøj A, Nielsen FC, Borregaard N (2014) Papillon-Lefevre syndrome patient reveals species-dependent requirements for neutrophil defenses. J Clin Invest 124:4539–4548
Steinbakk M, Naess-Andresen CF, Lingaas E, Dale I, Brandtzaeg P, Fagerhol MK (1990) Antimicrobial actions of calcium binding leukocyte L1 protein, calprotectin. Lancet 336:763–765
Steinstraesser L, Lam MC, Jacobsen F, Porporato PE, Chereddy KK, Becerikli M, Stricker I, Hancock RE, Lehnhardt M, Sonveaux P et al (2014) Skin electroporation of a plasmid encoding hCAP-18/LL-37 host defense peptide promotes wound healing. Mol Ther 22:734–742
Territo MC, Ganz T, Selsted ME, Lehrer RI (1989) Monocyte-chemotactic activity of defensins from human neutrophils. J Clin Invest 84:2017–2020
Theilgaard-Mönch K, Knudsen S, Follin P, Borregaard N (2004) The transcriptional activation program of human neutrophils in skin lesions supports their important role in wound healing. J Immunol 172:7684–7693
Thorey IS, Roth J, Regenbogen J, Halle JP, Bittner M, Vogl T, Kaesler S, Bugnon P, Reitmaier B, Durka S et al (2001) The Ca2 + −binding proteins S100A8 and S100A9 are encoded by novel injury-regulated genes. J Biol Chem 276:35818–35825
Tjabringa GS, Aarbiou J, Ninaber DK, Drijfhout JW, Sørensen OE, Borregaard N, Rabe KF, Hiemstra PS (2003) The antimicrobial peptide LL-37 activates innate immunity at the airway epithelial surface by transactivation of the epidermal growth factor receptor. J Immunol 171:6690–6696
Tokumaru S, Higashiyama S, Endo T, Nakagawa T, Miyagawa JI, Yamamori K, Hanakawa Y, Ohmoto H, Yoshino K, Shirakata Y et al (2000) Ectodomain shedding of epidermal growth factor receptor ligands is required for keratinocyte migration in cutaneous wound healing. J Cell Biol 151:209–220
Tokumaru S, Sayama K, Shirakata Y, Komatsuzawa H, Ouhara K, Hanakawa Y, Yahata Y, Dai XJ, Tohyama M, Nagai H et al (2005) Induction of keratinocyte migration via transactivation of the epidermal growth factor receptor by the antimicrobial peptide LL-37. J Immunol 175:4662–4668
Tomee JF, Hiemstra PS, Heinzel-Wieland R, Kauffman HF (1997) Antileukoprotease: an endogenous protein in the innate mucosal defense against fungi. J Infect Dis 176:740–747
Turner J, Cho Y, Dihn NN, Waring A, Lehrer RI (1998) Activities of LL-37, a Cathelin-associated antimicrobial peptide of human neutrophils. Antimicrob Agents Chemother 42:2206–2214
Urban CF, Ermert D, Schmid M, Abu-Abed U, Goosmann C, Nacken W, Brinkmann V, Jungblut PR, Zychlinsky A (2009) Neutrophil extracellular traps contain calprotectin, a cytosolic protein complex involved in host defense against Candida albicans. PLoS Pathog 5:e1000639
vanBergen BH, Andriessen MPM, Spruijt KIJ, van de Kerkhof PCM, Schalkwijk J (1996) Expression of SKALP/elafin during wound healing in human skin. Arch Dermatol Res 288:458–462
Vandal K, Rouleau P, Boivin A, Ryckman C, Talbot M, Tessier PA (2003) Blockade of S100A8 and S100A9 suppresses neutrophil migration in response to lipopolysaccharide. J Immunol 171:2602–2609
Vogl T, Tenbrock K, Ludwig S, Leukert N, Ehrhardt C, van Zoelen MAD, Nacken W, Foell D, van der Poll T, Sorg C et al (2007) Mrp8 and Mrp14 are endogenous activators of Toll- like receptor 4, promoting lethal, endotoxin-induced shock. Nat Med 13:1042–1049
Wanke I, Steffen H, Christ C, Krismer B, Gotz F, Peschel A, Schaller M, Schittek B (2011) Skin commensals amplify the innate immune response to pathogens by activation of distinct signaling pathways. J Invest Dermatol 131:382–390
Ward PA (1968) Chemotaxis of mononuclear cells. J Exp Med 128:1201–1221
Wingens M, van Bergen BH, Hiemstra PS, Meis JF, van Vlijmen WIM, Zeeuwen PL, Mulder J, Kramps HA, van Ruissen F, Schalkwijk J (1998) Induction of SLPI (ALP/HUSI-I) in epidermal keratinocytes. J Invest Dermatol 111:996–1002
Wolf R, Howard OM, Dong HF, Voscopoulos C, Boeshans K, Winston J, Divi R, Gunsior M, Goldsmith P, Ahvazi B et al (2008) Chemotactic activity of S100A7 (Psoriasin) is mediated by the receptor for advanced glycation end products and potentiates inflammation with highly homologous but functionally distinct S100A15. J Immunol 181:1499–1506
Yang D, Chertov O, Bykovskaia N, Chen Q, Buffo MJ, Shogan J, Anderson M, Schroder JM, Wang JM, Howard OMZ et al (1999) beta-defensins: linking innate and adaptive immunity through dendritic and T cell CCR6. Science 286:525–528
Yang D, Chen Q, Chertov O, Oppenheim JJ (2000a) Human neutrophil defensins selectively chemoattract naive T and immature dendritic cells. J Leukoc Biol 68:9–14
Yang D, Chen Q, Schmidt AP, Anderson GM, Wang JM, Wooters J, Oppenheim JJ, Chertov O (2000b) LL-37, the Neutrophil Granule- and epithelial cell-derived cathelicidin, utilizes formyl peptide receptor -like 1 (FPRL1) as a receptor to chemoattract human peripheral blood neutrophil, monocytes, and T cells. J Exp Med 192:1069–1074
Zanetti M (2004) Cathelicidins, multifunctional peptides of the innate immunity. J Leukoc Biol 75:39–48
Zanger P, Holzer J, Schleucher R, Scherbaum H, Schittek B, Gabrysch S (2010) Severity of Staphylococcus aureus infection of the skin is associated with inducibility of human beta-defensin 3 but not human beta-defensin 2. Infect Immun 78:3112–3117
Zanger P, Nurjadi D, Vath B, Kremsner PG (2011) Persistent nasal carriage of Staphylococcus aureus is associated with deficient induction of human beta-defensin 3 after sterile wounding of healthy skin in vivo. Infect Immun 79:2658–2662
Zasloff M (1987) Magainins, a class of antimicrobial peptides from Xenopus skin: isolation, characterization of two active forms, and partial cDNA sequence of a precursor. Proc Natl Acad Sci U S A 84:5449–5453
Zhu J, Nathan C, Jin W, Sim D, Ashcroft GS, Wahl SM, Lacomis L, Erdjument-Bromage H, Tempst P, Wright CD et al (2002) Conversion of proepithelin to epithelins: roles of SLPI and elastase in host defense and wound repair. Cell 111:867–878
Acknowledgments
This work was supported by grants from the Alfred Österlunds Stiftelse, the Royal Physiografic Society Lund, Greta och Johan Kocks Stiftelse, Petrus och Augusta Hedlunds Stiftelse, and the Swedish Research Council.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Sørensen, O.E. (2016). Antimicrobial Peptides in Cutaneous Wound Healing. In: Harder, J., Schröder, JM. (eds) Antimicrobial Peptides. Birkhäuser Advances in Infectious Diseases. Springer, Cham. https://doi.org/10.1007/978-3-319-24199-9_1
Download citation
DOI: https://doi.org/10.1007/978-3-319-24199-9_1
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-24197-5
Online ISBN: 978-3-319-24199-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)