Abstract
Essential tremor (ET) is one of the most common movement disorders in adults. Several drugs have been proven as effective tools in the treatment of tremor associated with ET; however, their therapeutic efficacy varies in each patient. Irrespective of the pharmacotherapy, around 10 % of patients with ET experience severe tremor that causes a marked deterioration of their quality of life. So far, deep brain stimulation (DBS) has been applied and established as a powerful tool in the treatment of medically refractory tremor in ET patients. Its traditional target for ET is the ventral intermediate nucleus of the thalamus. During the recent years, there is a growing body of evidence suggesting that the posterior subthalamic area, which includes the zona incerta and the prelemniscal radiation, also serves as an alternative DBS target for ET, as does the subthalamic nucleus. Here, we introduce the current advances in understanding the pathophysiology of ET, the functional anatomy of the DBS targets for ET, and the possible mechanisms by which DBS suppresses tremor associated with ET. Overall therapeutic impacts and adverse effects related to the DBS surgeries for ET are also described. This review would help to gain more insight into the DBS surgeries in patients with ET.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Deep Brain Stimulation
- Essential Tremor
- Globus Pallidus Internus
- Inferior Olivary Nucleus
- Deep Brain Stimulation Surgery
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
11.1 Introduction
Essential tremor (ET) is the most common movement disorder in adults (Deuschl et al. 2011). The postural and action–intention components affecting distal and proximal musculature are the typical manifestations of advanced ET. ET affects the upper extremities, head, voice, legs, and trunk. The primary treatment for ET is pharmacotherapy. Two drugs, primidone and propranolol, have been established as effective (level-A evidence by the criteria of the American Academy of Neurology) (Zesiewicz et al. 2011). However, 30–50 % of patients will not respond to both drugs (Koller and Vetere-Overfield 1989). Five drugs, topiramate, alprazolam, atenolol, gabapentin, and sotalol, have been shown to be compatible to level-B evidence (probably effective). Irrespective of these medications, 25–55 % of patients manifest medication-refractory ET (Louis 2001). Around 10 % of patients experience significant physical impairment and markedly decreased quality of life. Although the evidence for surgical therapies remains at level C (possibly effective) due to a lack of class-I and class-II studies, thalamotomies and deep brain stimulations have been applied to drug-resistant ET patients, and they have been reported to be highly efficacious for upper limb tremor in patients with ET (Deuschl et al. 2011).
Although the therapeutic efficacy of ablation surgery may be comparable to that of DBS (Schuurman et al. 2000, 2008), DBS is currently preferred over thalamotomy due to its reversibility and adjustability and to the undesirable and irreversible tissue damage that is caused by the ablation surgery (Tasker 1998). The ventral intermediate (VIM) nucleus of the thalamus has been used as a classic target for ET since 1987 (Miocinovic et al. 2013). However, axial tremor, the action component of distal tremor, and proximal tremor respond poorly to VIM DBS (Benabid et al. 1991, 1996). In addition, VIM DBS manifests a high incidence of dysarthria and disequilibrium (Benabid et al. 1991, 1996; Pahwa et al. 1999; Taha et al. 1999) and tolerance to the stimulation (i.e., habituation) (Benabid et al. 1991, 1996; Hariz et al. 1999). The posterior subthalamic area (PSA), which is composed of the prelemniscal radiation (Raprl) and the caudal zona incerta (cZI), has been a target of early ablation surgery in patients with tremor (Ito 1975; Krauss et al. 1994; Mundinger 1969; Velasco et al. 1972). Recently, this structure has been revived as another option for DBS for ET (Lehman and Augustine 2013). Subthalamic nucleus (STN) DBS has also been considered for ET (Lind et al. 2008).
11.2 Pathophysiology of Essential Tremor
The precise pathogenesis of ET is poorly understood. In the harmaline animal model, abnormally synchronized (4–10 Hz) oscillations have been identified in the inferior olivary nucleus (ION), and these are transmitted to the dentate and interpositus nuclei in the cerebellum (Park et al. 2010; Wilms et al. 1999). The calcium-dependent neuronal synchrony in the ION is sufficient to drive the cerebellothalamocortical circuit to produce tremor (Park et al. 2010), and a functional imaging study has shown the abnormal activation of the ION in ET (Boecker et al. 1996). These results suggest the dysfunction of the olivocerebellar circuit is the primary cause of ET (Deuschl and Bergman 2002). There are no morphological changes in the ION, supporting the idea that ET is due to a functional abnormality within the central nervous system (Deuschl et al. 2001; Louis et al. 2013). The ION adjusts or modulates planned movements during their execution in response to unconditioned afferent information; in other words, it is a movement error detector (Plaha et al. 2004).
The cerebellar nuclei connect to the ventrolateral thalamus through the cerebellothalamic tract and consecutively to the motor cortex. Plaha et al. (2008) have presumed that excessive movement correction in response to limb displacement detection and overcorrection might create abnormal oscillation in the ION in ET. Louis and Vonsattel (2008) have proposed that the cerebellum is integrally involved in the pathophysiology of ET, and some neurodegenerative features in the cerebellum have been shown (Louis et al. 2009). This hypothesis is supported by the findings of a recent neuroimaging study that ET is associated with γ-aminobutyric acid (GABA)ergic neurotransmission dysfunction in the cerebellum (Boecker et al. 2010; Gironell et al. 2012).
Although the olivocerebellar system and the thalamus are key structures, corticomuscular coherence studies have suggested the existence of several central pacemakers in the cerebellum, thalamus, and motor cortex (Govindan et al. 2006; Hua and Lenz 2005; Raethjen and Deuschl 2012; Schelter et al. 2009; Schnitzler et al. 2009). Recent studies using magnetoencephalography (MEG) have revealed that all of the centers simultaneously work and are not fixed and that its constituents may vary over time (Raethjen et al. 2007; Schnitzler et al. 2009; Raethjen and Deuschl 2012). The intermittent cortical involvement may shift the mode of cooperation between all of the constituents of the tremor network (Raethjen et al. 2007; Raethjen and Deuschl 2012). The so-called burst and tonic modes of activity have been observed in thalamic neurons. In the burst mode, the transfer of information has a high signal-to-noise ratio that is conveyed in a nonlinear manner such that new signals are readily identifiable but not readily analyzed. In the tonic mode, there is a linear transfer of the activity of specific afferents, but the signal-to-noise ratio is low (Godwin et al. 1996). These patterns of activity have been seen in the lateral thalamus (Tsoukatos et al. 1997; Zirh et al. 1998). The interaction within the network seems to determine the emerging type of movement (Raethjen and Deuschl 2012), including ET.
The contribution of the basal ganglia loop in generating ET has been controversial (Gerasimou et al. 2012; Lou and Jankovic 1991). The fact that the stimulation of VIM, PSA, and STN could also affect neurons and fibers that are included in the basal ganglia loop has suggested that stimulation of both the cerebellothalamic and pallidothalamic fibers might be responsible for the therapeutic effects on tremor (Deuschl and Bergman 2002).
11.3 Anatomy and Electrophysiology of DBS Surgery
The VIM nucleus, which receives strong cerebellothalamic afferents, is a major target of tremor in functional neurosurgery (Asanuma et al. 1983a, b; Ilinsky and Kultas-Ilinsky 2002; Kultas-Ilinsky and Ilinsky 1991). Vim DBS has demonstrated promising results for the treatment of ET (Rehncrona et al. 2003; Sydow et al. 2003). Recently, many studies have demonstrated that the PSA (Fytagoridis et al. 2012; Kitagawa et al. 2000; Murata et al. 2003; Plaha et al. 2004, 2008, 2011; Velasco et al. 2001) and STN (Blomstedt et al. 2011a, b; Lind et al. 2008; Stover et al. 2005) could be alternative targets. Recent evidence has revealed that the effects of DBS for ET in these subthalamic structures yielded good results.
11.3.1 The VIM Nucleus
11.3.1.1 Functional Anatomy of VIM
The ventrolateral (VL) thalamus is comprised of ventral oral posterior (Vop) nucleus, ventralis oralis internus (Voi), and the VIM nucleus (Hassler 1959). Anterior and lateral to these nuclei lie the reticular nucleus of the thalamus and the internal capsule (El-Tahawy et al. 2004). The VL thalamus mediates motor control. It receives afferent fibers from the cerebellum, basal ganglia, cerebral cortices, and spinal cord, and it projects efferent fibers to the cerebral cortices and basal ganglia. The VL has two subcortical afferent territories: the pallidothalamic and cerebellothalamic territories (Ilinsky and Kultas-Ilinsky 1987; Kuo and Carpenter 1973; Nakano 2000; Sidibé et al. 1997). The density of the pallidothalamic territory decreases in an anterior to posterior gradient and that of the cerebellothalamic territory decreases in a posterior to anterior gradient in the VL thalamus (Sakai et al. 1996). These two territories are widely interdigitated (Asanuma et al. 1983a, b; Sakai et al. 1996). The Vop preferentially receives inhibitory pallidothalamic inputs from the globus pallidus internus (GPi), and the VIM predominantly receives excitatory inputs from the cerebellum. The efferents from the VIM nucleus preferentially project to the primary motor, premotor, and proper supplementary motor area, which, in turn, provide reciprocal excitatory corticothalamic inputs (Bromberg et al. 1981; Hoover and Strick 1999). The VIM nucleus projects predominantly to the deep cortical areas of the motor cortex (Area 4 and possibly, Area 3a), which respond to the passive motor movements of joints (Anderson and Turner 1991; Butler et al. 1992; Jones 2007; Miyagishima et al. 2007; Vitek et al. 1994). The VIM neurons are somatotopographically organized; the face, forelimb, and hindlimb receptive fields are arranged medially to laterally (Strick 1976; Vitek et al. 1994; Kurata 2005). The Vc nucleus, which is the major termination structure of the medial lemniscus, projects to the primary somatosensory cortex (El-Tahawy et al. 2004). The subthalamic area (STA) is located ventrally to the VL thalamus.
11.3.1.2 Electrophysiological Findings During VIM DBS
As the microelectrode descends toward the thalamic target, the caudate has a very slow rate of spontaneous discharge (0–10 Hz) (Vitek et al. 1998), and the thalamus is relatively quiet in the awake patient but shows occasional slow bursting activity (Starr et al. 1998). Microelectrode entry into the motor thalamus can be indicated by the identification of movement-responsive cells and/or cells discharging at tremor frequency (Lenz et al. 1994). Microelectrode recording can identify the Vc nucleus, which is a tactile relay nucleus, and its anterior border with VIM as well as the ventral border with STA (El-Tahawy et al. 2004). Neurons that respond to voluntary movements (voluntary cells) are predominantly present in the Voa and Vop (El-Tahawy et al. 2004). Voluntary cells do not respond to verbal commands but rather to the voluntary act itself, and they are sometimes difficult to distinguish from kinesthetic cells (El-Tahawy et al. 2004; Raeva et al. 1999). Kinesthetic cells receive afferents from muscle spindles that are located in the tendons and muscle bellies or from stretch receptors that are located in the tendons, joint capsules or deep tissues, and they respond to passive joint movements and proprioceptive afferents. These cells are located just anterior to the tactile receptive field (Ohye and Narabayashi 1979; Ohye et al. 1989). Tactile cells in the Vc nucleus respond to superficial light touch. Stimulation of the Vc nucleus induces paresthesia due to activation of the medial lemniscal axons (El-Tahawy et al. 2004).
11.3.1.3 Surgical Anatomy of VIM for Essential Tremor
Vim DBS reduces abnormal tremor-electromyography coherence in ET postural tremor (Vaillancourt et al. 2003). The ideal target for abolishing the tremor is supposed to be located in the area where kinesthetic and tremor cells coexist (Lenz et al. 1994; Atkinson et al. 2002). The kinesthetic zone is located in the lower and lateral part of the VIM nucleus, which is a region of confluence of cerebellothalamic and spinothalamic tracts and which sends the majority of its axons to the motor cortex (Percheron et al. 1996). Ohye and colleagues have postulated that this area is optimal for radiofrequency lesioning to abolish tremor (Ohye and Narabayashi 1979; Ohye et al. 1989). Kiss et al. (2003) have reported that there is an expansion of the representation of movement-related (kinesthetic and deep-responding) neurons anteriorly in patients with tremor. Although DBS of the lateral portion of the VIM nucleus, where tremor cells might play a predominant role, provides the best control of parkinsonian tremor, as suggested previously (Atkinson et al. 2002; Hariz and Hirabayashi 1997), this is not the case for ET and post-stroke tremor, in which, presumably, the tremor cells are spread out in wide areas (Katayama et al. 2005) and they involve more proximal muscle components, which are represented more anteriorly and dorsally in the VIM nucleus (Ohye et al. 1989). A clinical study that examined the relationship between lead location and clinical outcome of 57 leads in 37 ET patients revealed that the lead locations in the anterior margin of the VIM nucleus corresponded to significant improvements in tremor scores (Papavassiliou et al. 2004). In such cases, thalamic DBS with bipolar stimulation or a low angle of the DBS electrode to the anterior commissure–posterior commissure (AC–PC) line (~45°) is advocated, as this could cover the more anterior (Katayama et al. 2005; Kobayashi et al. 2010; Yamamoto et al. 2004; Kiss et al. 2003) and dorsal areas (Kiss et al. 2003; Nguyen and Degos 1993).
11.3.2 Posterior Subthalamic Area (PSA)
11.3.2.1 Functional Anatomy of the PSA
The PSA and its vicinity comprises the nuclei area, which includes the Zi, the STN, and substance Q of Sano, and the fiber area, which includes the ansa lenticularis, Forel’s fields H, H1, and H2, Raprl, perirubral fibers, and rubrothalamic fibers (Carrillo-Ruiz et al. 2012). There also exist extended nuclei from mesencephalon that correspond to the substantia nigra (SN) and red nucleus (RN). The PSA is situated anterolateral of the red nucleus, posteromedial of the STN, inferior of the ventral thalamic nuclei, superior of the SN, and anteromedial of the posterior limb of the internal capsule (Xie et al. 2012; Fytagoridis et al. 2013a).
The Zi consists of four territories: rostral, dorsal, ventral, and caudal. Rostral Zi, which is attributed to visceral control, is located dorsomedial to the pallidofugal fibers and STN. Dorsal Zi is attributed to the wake and ventral Zi is under the guidance of the eye and head movements (Carrillo-Ruiz et al. 2012). The cZi, which is called the motor part of the Zi, extends posterior to the STN (Carrillo-Ruiz et al. 2012). The cZi is situated ventral to the Va thalamic nucleus, just ventral to the fascicularis thalamicus (Forel’s fields H), and dorsal to the fascicularis lenticularis (Forel’s fields H2) (Morel 2007; Plaha et al. 2008). Medial to the cZi is situated the cerebellothalamic tract and the red nucleus, and, lateral to the cZi, exists the internal capsule. The Zi receives inputs from motor, associative, and limbic cortices, the interpositus nucleus of the cerebellum, the substantia nigra reticulata (SNr), the globus pallidus internus (GPi), and the ascending reticular activating system, and it then connects to the centromedian and parafascicular (CM/Pf) and VL nuclei of the thalamus, SNr, GPi, the parvocellular RN, ION, the medial reticular formation, the pedunculopontine tegmental nucleus, the interpositus nucleus of the cerebellum, hypothalamus, the brainstem, including the pedunculopontine nucleus, the spinal cord, and the cerebral cortices (Carrillo-Ruiz et al. 2012; Heise and Mitrofanis 2004; Mitrofanis et al. 2004; Mitrofanis 2005; Plaha et al. 2008). cZI is an extension of the reticular thalamic nucleus, and it predominantly consists of GABAergic neurons. It affects both the basal ganglia and cerebellar outputs, medial reticular formation, and midbrain reticular formation, which are involved in controlling axial and proximal limb muscles (Blomstedt et al. 2009; Plaha et al. 2008). Current theories suggest that the cZi might play a key role in transmitting GABAergic input from the basal ganglia to the cerebellothalamocortical circuits and that DBS might alter or inhibit abnormal oscillations (Blomstedt et al. 2009; Fytagoridis et al. 2012; Plaha et al. 2008). Plaha et al. (2008) have suggested that Zi is an effective target for various types of tremors.
The Raprl is situated inferior to the Vo and VIM thalamic nuclei, in front of the lemniscus pathway, externally is the thalamic reticular nucleus, Zi, and STN, and the medial side is bordered by the RN (Carrillo-Ruiz et al. 2008, 2012; Lehman and Augustine 2013; Morel 2007). The Raprl contains cerebellothalamic, pallidothalamic, renticulothalamic, and rubrothalamic fibers (Carrillo-Ruiz et al. 2008, 2012).
11.3.2.2 Electrophysiological Findings During PSA DBS
When PSA DBS is performed, the transfrontal trajectory to the target is ~45° to the AC–PC plane, and an abrupt increase in impedance (from 400–500 to 600–700 Ω) is experienced when the electrode is passed beyond the ventral boundary of the thalamus into the subthalamic white matter (Murata et al. 2003; Plaha et al. 2008). Alternatively, single-unit-activity recordings have demonstrated frequencies of at least 15 Hz and/or responses to somatosensory stimulation or joint movements in the thalamus, while single-unit activity is absent or below 5 Hz with low background activity and does not respond to outer stimuli in the subthalamic area (Raprl) (Herzog et al. 2007; Kiss et al. 2003). In awake humans, late components of the somatosensory evoked potential from median nerve stimulation can be recorded from Raprl (Blomstedt et al. 2009). The extracellular action potential characteristics of the anterior thalamus and Zi are similar: low frequency and irregular discharge. The major difference is the neuronal density or the distance traversed before extracellular action potentials are encountered (Baker et al. 2004). In the Zi, the neuronal density is lower than that of the anterior thalamus. When the microelectrode enters into the STN, high frequency irregular discharges and increases in background activity are notably observed (Theodosopoulos et al. 2004). Just outside the bottom of the STN is an electrically quiet zone. When the microelectrode enters into the SNr, high frequency regular discharges with decreased background activity are detected.
11.3.3 Surgical Anatomy of the Subthalamic Area (STA) and STN
Herzog et al. (2007) have reported that most contacts that disrupt tremor-electromyography synchronization are located within the PSA, although they are still present in the VL thalamus. Stimulation of the PSA significantly increases the tremor frequency, which reflects a reduced contribution of the pathological central tremor oscillator (Deuschl and Bergman 2002; Herzog et al. 2007). The cerebellothalamic fibers pass through the lateral portion of the red nucleus and the bulk of fibers that continue in the rostrolateral direction pass through the field H of Forel and Raprl and enter the thalamus (Ilinsky and Kultas-Ilinsky 1984; Herzog et al. 2007). The fasciculus thalamicus (pallidothalamic tract) includes the fasciculus and ansa lenticularis (Forel H1 and H2, respectively). These two fibers merge and form the fasciculus thalamicus (Forel H) (Morel 2007). Therefore, the PSA is largely comprised of these two fibers: the cerebellothalamic fibers and Forel H. These fibers, especially the cerebellothalamic fibers, pass through the Zi and the Raprl (Morel 2007). Therefore, the effects of cZi stimulation on tremor might, in part, be due to the stimulation of cerebellothalamic and/or pallidothalamic fibers. In patients suffering from ET over the long term, the tremor and kinesthetic cells spread into Vo segments (Katayama et al. 2005; Kiss et al. 2003). The intention component of ET is supposed to be intensively affected by cerebellothalamic afferents to the VIM nucleus (Pedrosa et al. 2013). These facts suggest that it might be better to stimulate cerebellothalamic fibers themselves in order to alleviate ET. The most effective electrode might be situated in the border zone of the PSA and VIM for ET. This situation has been shown to be true for Parkinson’s disease (PD); the border zone of the cZi and the STN was most effective for DBS (Deuschl and Bergman 2002).
According to the stereotactic target of the STN proposed by Blomstedt et al. (2011a), the stimulation site is located at the border of the STN and fasciculus lenticularis from Morel’s atlas, and this location is close to the Zi and the fasciculus thalamicus. The effect of STN DBS might affect the tonic activation of adjacent tracts, as well as the cZi, which might lead to a tonic activation of VIM neurons and disrupt the tremor synchronous activity (Stover et al. 2005; Miocinovic et al. 2013). Stover et al. (2005) have postulated that this hypothesis is compatible with the results that the short-latency excitation of thalamic neurons begins just after STN stimulation in MPTP PD model monkeys. Lind et al. (2008) have reported that the most effective contacts are situated in the mid (56.3 %) and ventral (31.3 %) side of the STN.
11.4 Tentative Stereotactic Coordinates for DBS in Patients with ET
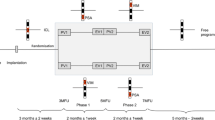
The current surgical targets for ET are the VIM (Fig. 11.1), STA (Fig. 11.2), and STN (Fig. 11.3). The tentative stereotactic coordinate for VIM DBS is 15 mm lateral to the midline at the level of the intercommissural line (ICL) and 6 mm anterior to the PC (Benabid et al. 1996). The Guiot approach that is widely used in France is the following: (11.0 or 11.5 + 1/2 or 1/3 of the third ventricular width) mm lateral to the midline at the level of the AC–PC plane and one-fourth of the AC–PC length anterior to the PC (Bardinet et al. 2011).
Stereotactic coordinate modified from Morel’s atlas (2007) illustrating the location of the Vim nucleus ( ). (a) Axial plane, on the AC–PC plane. (b) Coronal plane, 6 mm anterior to the PC. (c) Sagittal plane, 14.5 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Ce nucleus centralis externus, Dc nucleus dorsocaudalis, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vce & Vci nucleus ventrocaudalis externus & internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
). (a) Axial plane, on the AC–PC plane. (b) Coronal plane, 6 mm anterior to the PC. (c) Sagittal plane, 14.5 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Ce nucleus centralis externus, Dc nucleus dorsocaudalis, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vce & Vci nucleus ventrocaudalis externus & internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
Stereotactic coordinate modified from Morel’s atlas (2007) illustrating the location of the STA ( ). (a) Axial plane, 2.7 mm ventral to the AC-PC plane. (b) Coronal plane, 7 mm anterior to the PC. (c) Sagittal plane, 11.8 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Ce nucleus centralis externus, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNc substantia nigra, pars compacta, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vce & Vci nucleus ventrocaudalis externus & internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
). (a) Axial plane, 2.7 mm ventral to the AC-PC plane. (b) Coronal plane, 7 mm anterior to the PC. (c) Sagittal plane, 11.8 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Ce nucleus centralis externus, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNc substantia nigra, pars compacta, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vce & Vci nucleus ventrocaudalis externus & internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
Stereotactic coordinate modified from Morel’s atlas (2007) illustrating the location of the STh ( ). (a) Axial plane, 3.6 mm ventral to the AC-PC plane. (b) Coronal plane, 9 mm anterior to the PC. (c) Sagittal plane, 11.8 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNc substantia nigra, pars compacta, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vci nucleus ventrocaudalis internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
). (a) Axial plane, 3.6 mm ventral to the AC-PC plane. (b) Coronal plane, 9 mm anterior to the PC. (c) Sagittal plane, 11.8 mm lateral to the median plane (From Morel (2007) with permission.) Abbreviations: AC anterior commissure, al ansa lenticularis, Dim nucleus dorsointermedius, DVO AC-PC plane, fct fasciculus cerebello-thalamicus, fl fasciculus lenticularis, ft fasciculus thalamicus, GPi globus pallidus, internal segment, GPe globus pallidus, external segment, LPo nucleus lateropolaris thalami, stt spinothalamic tract, IC internal capsule, MCL midcommissural line, ml medial lemniscus, PC posterior commissure, PuT putamen, R reticular thalamic nucleus, RN red nucleus, SNc substantia nigra, pars compacta, SNr substantia nigra, pars reticulata, STh Subthalamic nucleus, Vci nucleus ventrocaudalis internus, Vim nucleus ventrointermedius, Vo nucleus ventrooralis, Zi zona incerta
In most studies, the PSA has been targeted directly (Murata et al. 2003; Plaha et al. 2008; Blomstedt et al. 2010). Murata et al. (2003) have reported the PSA coordinates as approximately 10 mm lateral and 3–4 mm behind the posterior border of the STN on the axial slice with the greatest STN diameter. Plaha et al. (2004) have targeted the point medial to the posterior dorsal third of the STN. Blomstedt et al. (2010) have targeted the cZi with thin-slice T2-weighted magnetic resonance images: slightly posteromedial to the tail of the STN at the level of the maximal diameter of the red nucleus. The stereotactic locations of the STA that best alleviated tremor (active contact) were 10.9–12.7 mm lateral to the midline, 6.1–7.0 mm posterior of the midcommissural line, and 1.5–3.0 mm below ICL (Murata et al. 2003; Hamel et al. 2007; Fytagoridis and Blomstedt 2010; Barbe et al. 2011). These targets are supposed to be located in the Raprl. Plaha et al. (2008) have targeted the cZi, and they reported that the stereotactic targets of the cZi were 14.2 mm lateral to the midline, 5.7 mm posterior to the mid-commissural line, and 2.1 mm below the ICL.
Blomstedt et al. (2011a, b) have targeted the STN with thin-slice T2-weighted images at the level of the maximal diameter of the red nucleus, at a line joining the anterior borders of these nuclei, and around 1.5 mm lateral from the visualized medial border of the STN. Lind et al. (2008) have reported that the position of active contact is 12 mm lateral to the midline, 16 mm posterior to the AC, and 4 mm below the ICL.
11.5 Definition of the Active Target During DBS Surgery
Intraoperative macrostimulation under local anesthesia is a reliable method to evaluate the effects of the optimal locations for each patient. The tremor stops immediately after the stimulation. Adverse events, such as dysesthesia and limb ataxia, which diminish within 10 s during the stimulation (200–300 Hz, 1 s trains of 0.1- or 0.2-ms pulse widths, the stimulation current is usually limited to a maximum of ~100 μA with high-impedance microelectrodes), are acceptable (El-Tahawy et al. 2004; Krack et al. 2002; Morigaki et al. 2010). Electrode model 3389 (Medtronic, Inc., Minneapolis, MN, USA) is usually used for VIM and STN, and model 3387 or 3389 is used for STA as it enabled stimulation of the VL thalamus alternatively (Plaha et al. 2004).
11.6 Stimulation Parameters
The mean parameters used in VIM, PSA, and STN DBS for ET are the following:
-
VIM DBS: 145–185 Hz (at least 100 Hz), 60–117 μs, 2.0–3.7 V (Koller et al. 1997, 1999, 2001; Pilitsis et al. 2008; Rehncrona et al. 2003; Tröster et al. 1999).
-
PSA DBS: 130–170 Hz (usually 130 Hz), 60–112.5 μs (usually 60 μs), 1.9–2.5 V (Blomstedt et al. 2010, 2011a; Fytagoridis et al. 2013a; Herzog et al. 2007; Murata et al. 2003; Plaha et al. 2004, 2011).
-
STN DBS: 130–180 Hz, 60–90 μs, 1.5–3 V (Blomstedt et al. 2011a; Lind et al. 2008; Meng et al. 2013; Stover et al. 2005).
11.7 The Possible Mechanisms by Which DBS Alleviates Tremor
Several hypotheses have been proposed with regard to the mechanisms of high-frequency DBS. Conduction or depolarization block is the simplest hypothesis, and it is supported by the findings that ablation surgery has similar effects as DBS (Benabid et al. 1996). Activation of inhibitory presynaptic afferents and inhibition of projection neurons (Wu et al. 2001; Anderson et al. 2006), inhibition of neuronal activity near the stimulation site and activation of axonal elements that leave the target structure (Vitek 2002), activation of adjacent fiber tracts surrounding or running through the stimulated site (Johnson et al. 2009), and the superposition of continuous stimuli onto rhythmically oscillating subcortical–cortical loops (Montgomery and Baker 2000) are other hypotheses. Some authors have hypothesized that high-frequency stimulation in the VIM increases glutamate release from glial cells and excites local interneurons, thereby increasing the production of inhibitory neurotransmitters (e.g., GABA and glycine) and resulting in a decrease in the firing rates of projection neurons (Kang et al. 1998; Tawfik et al. 2010; Tian et al. 2005). When we consider the effect of VIM, as well as PSA (especially Rarpl) stimulation, the conduction or depolarization block might be a plausible mechanism. However, positron emission tomography analyses have demonstrated that VIM DBS increases regional blood flow in the supplemental motor area (Ceballos-Baumann et al. 2001; Perlmutter et al. 2002). Taking into consideration that the cerebellothalamic and thalamocortical fibers are both glutamatergic (excitatory), a different mechanism might be at work. DBS might modulate abnormal oscillation coupling by superposing continuous stimuli onto rhythmically oscillating loops (Montgomery & Baker’s theory) or activate adjacent or surrounding fiber components (Vitek’s or Johnson’s theory).
11.8 Patient Selection
Factors to consider in DBS include tremor severity, refractoriness to medication, tremor type, patient characteristics, including age, comorbid conditions, surgical risk, patient preference, social and employment factors, and social support (Cooper and Bowes 2012). One of the most important aspects is cognitive function. This is especially important for bilateral procedures, particularly bilateral STN DBS (Hariz 2002). Patients with borderline mental conditions have experienced irreversible and unadjustable dementia after bilateral STN DBS. Although most cases involve unilateral surgery (left side), VIM, Raprl, and cZi DBS have not been shown to affect higher cognitive processes as long as in 6-year follow-up periods (Heber et al. 2013).
Unilateral thalamotomy could be an option when a patient does not want to implant devices, a patient has difficulty in consulting medical care frequently, extensive lesioning is predicted due to a proximal inclusion, a patient has an increased risk of infection (immune-compromised patients), and habituation or tolerance occurs after DBS (Bahgat et al. 2013).
With regard to VIM DBS, tremor-suppressing medications could be discontinued after bilateral VIM DBS, but they should be continued after unilateral DBS. Unilateral VIM DBS is insufficient to eliminate the necessity for tremor-suppressing medications, and discontinuation has been shown to worsen the tremor (Favilla et al. 2013).
11.9 Therapeutic Impact of DBS for ET
In general, resting tremors are better controlled than action tremors, distal limb tremors are better than proximal limb tremors, and upper limb tremors are better than lower limb tremors (Benabid et al. 1996, 1998; Lozano 2000). The short- and long-term efficacy of VIM DBS is promising. However, tolerance to the stimulation and insufficient effects on axial and proximal tremor are the biggest problems. The PSA is an effective target for tremor suppression in early ablation surgery (Spiegel et al. 1963). Although there are not enough results concerning long-term efficacy, PSA DBS seems promising in a number of recent publications. Moreover, PSA stimulation showed a powerful effect, even for axial and proximal tremor, and several short-term and a few long-term results have described that ET patients with PSA DBS did not manifest tolerance to the stimulation. Here, we review the short- and long-term outcomes that are related to VIM, PSA (Raprl & cZi), and STN DBS for patients with ET.
11.9.1 Therapeutic Impact of VIM DBS
Only one randomized controlled trial with a direct comparison of thalamotomy with DBS is available (Schuurman et al. 2000, 2008). The results demonstrated that VIM DBS was equally effective as VIM thalamotomy. However, half of the ET patients experienced diminished effects of the stimulation over the 5-year follow-up (Schuurman et al. 2008).
11.9.1.1 Short-Term Efficacy
11.9.1.1.1 Tremor Reduction (Assessors Blind)
Numerous case series are available, and the short- and long-term effects of VIM DBS are usually favorable (Morigaki et al. 2010). Among them, blinded assessments have shown a marked reduction in tremor scores and significant improvements in disability scores (Koller et al. 1997, 1999, 2001; Lyons et al. 1998; Pahwa et al. 1999; Tröster et al. 1999; Schuurman et al. 2000; Hariz 2002; Rehncrona et al. 2003; Fields et al. 2003).
Schuurman et al. (2000) have reported that the contralateral tremors of 13 ET patients were completely suppressed at 6 months postoperatively. In Koller’s series (Koller et al. 1997), VIM stimulation resulted in 31 % of the ET patients obtaining contralateral tremor remission, and 79 % of the ET patients experienced marked tremor improvement (50–100 %) at the 3-month follow-up. Hariz et al. (2002) have reported that unilateral VIM DBS improved the total Fahn-Tolosa-Marin (FTM)-tremor rating scale (TRS) tremor score by 47 % from baseline at the 12-month follow-up. Unilateral VIM DBS improved the FTM-TRS tremor scores by 50.8–78.0, 53–78.7, and 20.6 % from baseline at the 3-, 12-, and 24-month follow-ups, respectively (Fields et al. 2003; Hariz 2002; Rehncrona et al. 2003; Tröster et al. 1999). The improvement in upper limb tremors contralateral to the DBS improved 79 % at the 12-month follow-up (Hariz 2002). Both the contralateral upper postural and activity/intention components improved 66.7 % at the 24-month follow-up (Rehncrona et al. 2003). Bilateral VIM DBS improved the FTM-TRS motor scores (items 1–10) and the postural + intention tremor by 64.9 and 66.7 %, respectively, at the 3-month follow-up (Pahwa et al. 1999). Head tremor was improved in 71 % of patients (Koller et al. 1999).
Although the assessors were not blind, several publications have indicated the efficacy of bilateral VIM DBS for axial tremors (Koller et al. 1999; Limousin et al. 1999; Obwegeser et al. 2000; Ondo et al. 1998; Putzke et al. 2005; Sydow et al. 2003; Taha et al. 1999). However, its therapeutic efficacy has been reported to vary. With respect to voice tremor, some studies have reported a significant and marked (more than 80 %) improvement (Obwegeser et al. 2000; Taha et al. 1999), whereas others have reported minimal changes in either short- or long-term follow-up studies (Limousin et al. 1999; Putzke et al. 2005; Sydow et al. 2003).
11.9.1.1.2 Motor Function of the Upper Limb
VIM stimulation improved FTM-TRS writing, spiral-drawing, straight line-drawing, and liquid-pouring scores by 56.7, 48.4, 56.3, and 63.3 %, respectively, at the 3-month follow-up (Koller et al. 1997). Unilateral VIM DBS improved FTM-TRS hand function scores by 39 % at the 12-month follow-up (Hariz 2002).
11.9.1.1.3 Improvement in Activity of Daily Living/Disability Scores
The therapeutic effects have been reported with several different scales. The Frenchay activity index score improved by 18 % at the 6-month follow-up after VIM DBS (Schuurman et al. 2000). VIM stimulation improved the global disability score by 57.6 % at the 3-month follow-up (Koller et al. 1997). Unilateral VIM DBS improved the Parkinson’s Disease Questionnaire (PDQ-39) Activities of Daily Living (ADL) score by 55.5 and 43.6 % at the 3- and 12-month follow-ups, respectively (Fields et al. 2003). Unilateral VIM DBS improved the FTM-TRS ADL score (items 15–21) by 54 % at the 12-month follow-up (Hariz 2002). Several factors of the ADL taxonomy scale significantly improved (Hariz 2002).
11.9.1.1.4 Improvements in Other Symptoms
VIM DBS has been shown to improve cognitive screening measures, visual attention, fine visuomotor and visuoperceptual functions, verbal memory, delayed prose recall, social life, interest/hobbies, and mood state/emotional reactions 3 and 12 months after unilateral VIM DBS (Fields et al. 2003; Hariz 2002; Tröster et al. 1999). However, Heber et al. (2013) have reported that neither stereotactic surgery nor electric stimulation affected higher cognitive functions, including memory and verbal fluency, at 1- and 6-year follow-up evaluations.
11.9.1.2 Long-Term Efficacy
There has been two publication with a blind assessment. Rehncrona et al. (2003) have found that FTM-TRS tremor (item 1–9) and hand function (items 11–14) scores improved by 47 and 71 %, respectively, compared to those presurgery at a mean follow-up period of 6.5 years after unilateral VIM DBS. The contralateral upper postural and activity/intention components improved 66.7 and 50 %, respectively.
Several publications with unblinded assessors have shown similar results. Sydow et al. (2003) have reported a 41 % reduction in FTM-TRS tremor scores and a 39 % improvement in the ADL scores with a follow-up period of 6.5 years. Pahwa et al. (2006) have reported that VIM DBS at a 5-year follow-up period resulted in a 75 % improvement in targeted hand tremors by unilateral stimulation, a 65 % improvement in the left limb, and an 86 % improvement in the right limb by bilateral stimulation, with a 36 and 51 % improvement in ADL scores by unilateral and bilateral stimulation, respectively. Total FTM-TRS, tremor score, contralateral hand function, and ADL scores improved significantly, except for voice tremor, at the 86-month follow-up (Blomstedt et al. 2007; Hariz et al. 2008). However, the DBS efficacy on tremor decreased, and almost all of the improvements in ADL at 1 year were no longer sustained (Hariz et al. 2008). Zhang et al. (2010) have reported a 80.4 and 69.7 % improvement of FTM-TRS tremor and handwriting scores, respectively, in a series of 34 patients (bilateral/unilateral DBS; 11/23 patients) with a follow-up period of about 5 years. Hariz et al. (2008) have reported an 18 % reduction in FTM-TRS total scores in a follow-up period of 7 years by unilateral stimulation. Nazzaro et al. (2012) have reported a 55, 44, and 31 % significant reduction in FTM-TRS total tremor scores for the follow-up periods of 1, 4, and 9 years by unilateral stimulation, respectively. FTM-TRS ADL improved 73, 52, and 37 %, and the PDQ-39 quality of life domains of the ADLs improved 27, 23, and 19 %, respectively. The PDQ-39 evaluation revealed ADL, emotional well-being, stigma, and cognition were significantly improved up to 7 years, but only stigma remained significant at 9 years and the mobility score significantly worsened.
11.9.2 Therapeutic Impact of PSA DBS
In a few early studies, the subthalamic area has been identified as a better location than the thalamus for alleviating ET (Mohadjer et al. 1990; Mundinger 1969; Velasco et al. 1972). The short-term results of DBS in this area seem promising, and the results include tremors that are difficult to be controlled by VIM DBS, such as proximal postural tremors and distal intention tremors (Xie et al. 2012). Publications concerning long-term results are limited (Fytagoridis et al. 2012).
11.9.2.1 Short-Term Efficacy of PSA DBS for ET
11.9.2.1.1 Tremor Reduction
Murata et al. (2003) have reported that unilateral PSA (Raprl and cZi) DBS immediately alleviated intractable proximal and distal tremors in patients with eight ET by 81 % as assessed with the modified tremor rating scale (FTM-TRS), and no worsening was observed during the mean 22-month follow-up periods. Voice, neck, and/or orthostatic axial tremors were also improved.
Using the FTM-TRS evaluation method and comparing the results with tremor severity at baseline, unilateral PSA DBS improved total tremor scores by 60–80.1 % at 12 months (Blomstedt et al. 2010; Plaha et al. 2004). The tremor score (items 1–9) improved by 61.2–84.2 % (Blomstedt et al. 2010; Plaha et al. 2004); upper limb postural and action components improved by 84.4 % (Plaha et al. 2004). Unilateral PSA DBS improved intention tremor by 63.4 and 68.4 % for a left- and right-side tremor, respectively, in patients with eight ET, two multiple sclerosis (MS), and one spinocerebellar ataxia (SCA) (Hamel et al. 2007).
Bilateral PSA DBS reduced the FTM-TRS total tremor scores by 63.5 % at a mean of 17 months postoperatively in patients with 10 ET (Herzog et al. 2007). The ipsilateral upper tremor improved by 8.7 % and the contralateral upper tremor improved by 95 %; the rest, postural, and activity/intention components improved by 100, 83.3, and 94.1 %, respectively (Herzog et al. 2007).
Unilateral cZi DBS improved total tremor scores by 60.9–76.9 %, tremor scores by 59.4–65.1 %, upper extremity tremors by 95.0–100 % (rest, postural, and action/intention components improved by 100, 95.8–100, and 93.8–94.1 %, respectively) 1 year postoperatively (Blomstedt et al. 2011a, b; Fytagoridis et al. 2012; Sandvik et al. 2012).
Bilateral cZi DBS improved total tremor scores by 75.9 % and upper extremity tremors by 85.6 % in six ET patients 1 year postoperatively (Plaha et al. 2008). Both distal (75.9 %) and proximal (71.2 %) intention tremors have been reported to be improved. Another study has shown that bilateral cZi DBS improved total tremor scores by 73.8 %, upper extremity tremors by 86.6 % (postural and action components by 88.2 and 82.2 %, respectively) at a 31.7-month follow-up (Plaha et al. 2011).
Some studies have adopted a more objective index. PSA DBS reduced the total power of accelerometry by 99 %, whereas DBS at the ventral thalamic border reduced it by 68 % and DBS at thalamus proper reduced it by 2.5 % at least 6 months after the operation (Herzog et al. 2007). Using a 3D ultrasound kinematic analysis tool in 21 ET patients, bilateral PSA DBS improved hand tremors by 86 % at least 3 months after the operation (Barbe et al. 2011).
Head tremor has been reported to be greatly improved: 75.0–100 % in short-term studies and 75 % in one long-term (48.5 months) follow-up study as well (Blomstedt et al. 2010, 2011b; Fytagoridis et al. 2012; Plaha et al. 2004, 2008, 2011). Face and trunk tremors were improved by 90.4 and 100 %, respectively, in Plaha’s series (cZi DBS, 31.7-month follow-up) (Plaha et al. 2011). The effects of PSA DBS on voice tremor seem to be worsening over the years: 66.7–98.7 % improvements in short-term follow-up periods (Blomstedt et al. 2010, 2011b; Fytagoridis et al. 2012), while a 33.3 % improvement was observed in a long-term follow-up duration (Fytagoridis et al. 2012; Plaha et al. 2011). However, we should be aware of the small sample size in the study of the long-term results.
11.9.2.1.2 Motor Function of the Upper Limb
Two early case series demonstrated that unilateral PSA DBS improves hand writing in all patients (Kitagawa et al. 2000; Murata et al. 2003). Using FTM-TRS, unilateral PSA DBS improved motor function scores of the upper limb (items 10–14); writing, spiral drawing, pouring water, and drawing lines improved by 68, 66.7, 76.9, and 58.3 %, respectively (Plaha et al. 2004), while bilateral cZi DBS improved them by 60.1–64.2, 81.9, 52.9 and 71.7 %, respectively (Blomstedt et al. 2011b; Plaha et al. 2008, 2011). Unilateral cZi DBS improved contralateral hand function (items 11–14) by 78.8–100 % at a 1-year follow-up (Blomstedt et al. 2011a, b; Fytagoridis et al. 2012; Sandvik et al. 2012).
11.9.2.1.3 Improvement in Activity of Daily Living Scores
Unilateral PSA DBS improved FTM-TRS ADL scores (items 15–21) by 66.4–88.8 % 12 months postoperatively (Blomstedt et al. 2010; Plaha et al. 2004). Bilateral PSA DBS improved ADL scores by 85.7 % in patients with eight ET, two MS, and one SCA (Hamel et al. 2007). Unilateral cZi DBS improved ADL scores by 64.1–76.5 % at a 1-year follow-up (Fytagoridis et al. 2012; Blomstedt et al. 2011a; Sandvik et al. 2012). Bilateral cZi DBS improved ADL scores by 80–84.5 % (Plaha et al. 2008, 2011).
A SF-36-survey physiological component score was improved by 23.7 %, and the mental component score improved by 22.4 % (Plaha et al. 2011). In another report, cZi DBS did not improve SF-36 subscores, and the authors postulated that SF-36 might be unsuitable for evaluating changes in ET patients in this condition (Sandvik et al. 2012).
The Quality of Life in Essential Tremor Questionnaire (QUEST) score 1 year after cZi DBS was improved in the summary index (SI), ADL, and psychosocial scores by 35.5, 40.2, and 40.9 %, respectively (Sandvik et al. 2012).
11.9.2.2 Long-Term Efficacy of PSA DBS for ET
With regard to the long-term efficacy, three ET patients (mean 5-year follow-up duration) with unilateral cZi DBS exhibited improved total tremor scores by 57.4 %, improved tremor scores (items 1–9) by 46.9 %, improved contralateral hand tremor by 100 %, improved hand function (items 11–14) by 87.5 %, and improved ADL scores (items 15–21) by 76.5 % (Blomstedt et al. 2011a). Eighteen ET patients (mean 48.5-month follow-up duration) with unilateral cZi DBS exhibited improved total tremor scores by 52.4 %, improved tremor scores (items 1–9) by 48.0 %, improved hand tremors by 91.8 % (improved rest, postural, and action/intention components by 100, 95.8, 85.3 %, respectively), improved hand function (items 11–14) by 39 % (contralateral side, 78.5 %; ipsilateral side, −13 %), and improved ADL scores by 65.8 % (Fytagoridis et al. 2012). Four ET patients with bilateral cZi DBS exhibited improved total tremor scores by 72.6 %, improved tremor scores (items 1–9) by 81.5 %, improved total hand function (items 11–14) by 60 %, and improved ADL scores (items 15–21) by 82.4 % with a mean 6.25-year follow-up duration (Plaha et al. 2011).
11.9.2.3 PSA DBS in Patients with Failed VIM DBS
Kitagawa et al. (2000) have reported the efficacy of unilateral PSA DBS in an ET patient with failed unilateral VIM thalamotomy. High-frequency (120–130 Hz) stimulation totally abolished the patient’s tremor. Blomstedt et al. (2012) have described two patients with early failure of VIM DBS and three failures after several years of good effects. It was confirmed that the failure in these patients was not due to the misplacement of electrodes. Before cZi DBS, VIM DBS improved total tremor scores and hand tremor/functions (items 5, 11–14) by 17 and 28.7 %, respectively. Unilateral cZi DBS moderately improved them: 31.7 and 54.3 % from baseline, respectively. Combined cZi and VIM stimulation that was tried in a single patient further improved these scores.
11.9.3 Therapeutic Impact of STN DBS for ET
Almost all publications about STN DBS are related to Parkinson’s tremor, and those that are associated with ET tremor are limited. However, some authors have postulated that STN DBS is also effective for ET (Stover et al. 2005; Lind et al. 2008; Blomstedt et al. 2011a; Meng et al. 2013).
Unilateral STA DBS improved FTM-TRS total tremor scores by 72.5 %, improved tremor scores (items 1–9) by 33.3 %, improved contralateral hand tremors by 66.7 %, improved hand function (items 11–14) by 77.8 %, and improved ADL by 100 % 1 year after the operation in a single patient (Blomstedt et al. 2011a). Meng et al. (2013) have described one patient with unilateral STN and another with bilateral STN DBS. The former exhibited an improved total tremor score by 75.5 % after a 6-month follow-up, and the latter exhibited a 66.7 % improved after a 24-month follow-up. Lind has described ten ET patients with unilateral STN DBS with a 1- to 3-year follow-up. They reported that all of the patients experienced favorable effects (slight tremor to complete disappearance of the tremor), but one patient changed to VIM DBS due to the development of a dystonic twist, two experienced minor speech disturbances, and two experienced balance disturbances (Lind et al. 2008). Lind et al. (2008) have reported complete tremor disappearance in all three patients with long-term follow-up (mean, 8.7 years).
11.10 Microlesioning and Stimulation-Related Problems
Stimulation-induced side effects are important because they determine the intensity of the stimulation and whether it can be used or not. Generally, sensory side effects have a high degree of habituation over time and are not a major threat to the therapeutic results (Fytagoridis et al. 2013a). Motor side effects are less susceptible to habituation and more prone to impede the results of the treatment. Theoretically, stimulation of the internal capsule (corticospinal or corticobulbar tracts) causes muscle contraction and dysarthria (Baker et al. 2004; Tamma et al. 2002). Dysarthria can also be induced by stimulation of cerebellothalamic fibers (Fytagoridis et al. 2013a). Stimulation of the medial lemniscus or Vc thalamic nucleus could result in paresthesia (Murata et al. 2003). Stimulation of the third nerve complex results in conjugate and disconjugate eye movements or eyelid closure (Baker et al. 2004). Stimulation of the oculomotor region of the STN just medial to the somatic sensorimotor region or rostral interstitial nucleus causes the same adverse effects (Tamma et al. 2002). Horizontal gaze deviation is considered to be a motor side effect of the corticofugal tract, which transverses the anterior limb of the internal capsule (Tamma et al. 2002). Cerebellar signs, such as limb ataxia, hypotonia, gait disturbance, and disequilibrium, are attributed to the stimulation of cerebellothalamic fibers. Hyperhydrosis might be due to the disruption of sympathetic efferent fibers in the Zi or activation of basal and posteromedial structures of the STN (Fytagoridis and Blomstedt 2010; Lind et al. 2008; Lipp et al. 2005; Tamma et al. 2002).
11.10.1 Adverse Effects Related to VIM DBS
According to a recent systematic review, the stimulation-related complications of 430 patients who received Vim DBS were paresthesia (18.84 %), dysarthria (8.84 %), headache (7.21 %), disequilibrium (3.95 %), and paresis (3.02 %) (Flora et al. 2010). The stimulation-related adverse events concerning long-term (more than 5 years) follow-ups have been described as follows: paresthesias (0–38 %), dysarthria (0–36 %), gait disturbance (0–19 %), dystonia/hypertonia (0–16 %), balance disturbance (0–8 %), and cognitive dysfunction (0–3 %) (Rehncrona et al. 2003; Sydow et al. 2003; Pahwa et al. 2006; Tarsy et al. 2005; Hariz et al. 2008; Schuurman et al. 2008). Most adverse events were mild and could be adjusted (Flora et al. 2010). Among these adverse effects, the nonadjustable and long-lasting complications included paresthesia (0–19 %), dysarthria (0–19 %), dystonia (0–6 %), gait disturbance (0–4 %), and upper limb ataxia (0–4 %). Bilateral stimulation can cause persistent complications that include dysarthria, disequilibrium, and gait disturbance, even if the stimulus parameters are optimized (Pahwa et al. 2006). Therefore, unilateral or staged bilateral procedures are safe and recommended.
11.10.2 Adverse Events Related to PSA DBS
Transient dysphasia (22.5 %), clumsiness (5 %), hemiparesis (2.5 %), and persistent dizziness (2.5 %) have been reported as nonstimulation-induced (due to microlesioning) complications after PSA surgery (Fytagoridis and Blomstedt 2010). The high rate of transient dysphasia might be due to a microlesional effect/edema caused by the passage of the electrode into the thalamus of the dominant hemisphere (Fytagoridis and Blomstedt 2010). When the active electrode is placed too close to the red nucleus, nonadjustable visual disturbances and dizziness occur (Fytagoridis and Blomstedt 2010). Fytagoridis et al. (2013b) have reported reduced verbal fluency that was statistically significant at 3 days and not significant at 1 year after cZi DBS in 17 patients. They hypothesized that this might have been due to microlesion/edema of the ventral thalamus.
Paresthesia (hand ≒ face > leg ≒ arm), dizziness, blurred vision, muscle contractures, dysarthria, ataxia/dysmetria, diplopia, ptosis, and hyperhidrosis are stimulation-induced side effects (Fytagoridis et al. 2013a). There exists a large anatomical variation in their emergence, or, in other words, it is hard to predict the adverse events that will occur from the anatomical location of the contacts (Fytagoridis et al. 2013a). This might be due to the stimulation of axonal components that spread electrical impulses farther than expected (Johnson et al. 2009). These side effects are totally reversible, adjustable, and usually do not affect the final results.
Bilateral lead implantation in Raprl induced somnolence in all five patients with PD and the deterioration of depression in two out of five patients with PD (Carrillo-Ruiz et al. 2008), and it has been reported to induce a 40 % incidence of hypophonic speech and disequilibrium (Plaha et al. 2011). Similarly, bilateral cZi stimulation induced dysarthria and hypophonic speech in three out of the 15 ET patients (20 %) in a relatively long-term (mean, 31 months) follow-up study (Plaha et al. 2011). These side effects were completely reversible but persistent and present at all times in one patient (6.7 %). In this study, the anatomical location of this side effect was supposed to be induced by stimulation that was dorsomedial to the STN (Plaha et al. 2006). PSA DBS bears a risk of speech, balance, and sensory disturbances, which is more pronounced with bilateral procedures. Staged surgery for bilateral PSA DBS might be safe and recommended.
11.10.3 Adverse Events Related to STN DBS
The adjustable complications induced by STN-DBS include arm dystonia, dysarthria, dizziness, and balance disturbances (Lind et al. 2008; Blomstedt et al. 2011a, b). Motor contraction and dysarthria are frequent (81 %), paresthesia occurs (32.5 %), and oculomotor side effects (24 %) are caused by stimulation of the third nerve or the rostral interstitial nucleus (Tamma et al. 2002). Vegetative side effects (nausea, heat sensation, sweating, or bradycardia) are also common (40.5 %). One patient experienced an unadjustable dystonic twist of the contralateral foot (Lind et al. 2008). Bilateral stimulation did not cause further side effects (Plaha et al. 2008, 2011).
11.11 Tolerance (Habituation)
The recurrence of ET seems to be higher than that of PD tremors (Benabid et al. 1996; Tasker 1998; Pilitsis et al. 2008). Poor outcomes have been documented in up to 40 % of ET patients with VIM DBS (Hariz and Hirabayashi 1997; Benabid et al. 1998; Hariz et al. 1999; Koller et al. 2001; Kumar et al. 2003). A gradual loss of tremor control is due to suboptimal lead placement, misdiagnosis, disease progression, and habituation (Deuschl et al. 2011). The tolerance could be explained by disease progression or the adaptation of the biological response by the stimulated neuronal network (Benabid et al. 1996; Deuschl et al. 2011; Barbe et al. 2011; Shih et al. 2013). Therefore, the intermittent use of implantable pulse generators is recommended in order to avoid the development of habituation and to save battery life (Morigaki et al. 2010, Lozano and Levy 2012). Acute changes of the stimulation parameters could suppress the habituated tremor. However, it adapts to the changed parameters over a time of 10 weeks, which causes tremor recurrence (Barbe et al. 2011). Barbe et al. (2011) have hypothesized that frequently switching between two equivalent but slightly different stimulation settings might be useful for reducing habituation. The prevalence of tolerance for VIM DBS has been estimated to be 10–40 % (Pahwa et al. 2006; Benabid et al. 1998; Papavassiliou et al. 2004; Pilitsis et al. 2008; Benabid et al. 1996). A recent long-term follow-up study (mean, 55.9 months) with strict criteria demonstrated that 73.3 % of the patients with 45 ET experienced waning benefits of VIM DBS over time (Shih et al. 2013). In contrast, many authors referred to the fact that there was no or less tolerance to the maintenance of the constant chronic stimulation of the PSA (Kitagawa et al. 2000; Murata et al. 2003; Plaha et al. 2004, 2008, 2011). Although we need further evidence, the loss of habituation might be a potential benefit of PSA DBS.
11.12 Which Is the Optimal Target in the Treatment for ET?
PSA (Raprl and cZi) DBS showed better tremor control and hand function with the use of lower voltages, which resulted in a reduction of side effects, such as dysarthria and disequilibrium (Lozano and Levy 2012). Using the same electrode different contacts, PSA stimulation preceded thalamic stimulation in patients with ET (Murata et al. 2003; Hamel et al. 2007; Herzog et al. 2007; Barbe et al. 2011). One study with 34 VIM DBS and 34 PSA DBS for ET patients implied that PSA DBS preceded to VIM DBS. However, there is no statistical evidence so far (Blomstedt et al. 2011b). Blomstedt et al. have compared the effects of cZi with STN DBS in ET by implanting two ipsilateral electrodes simultaneously, one in the STN and one in the cZi (Blomstedt et al. 2011a). Although they reported that both STN and cZi DBS were effective, cZi was the preferable target because the best effect was achieved at lower energy consumption with less adverse events.
VIM DBS developed tolerance (habituation) to stimulation despite the amplitude increase, and tremor recurrence may occur within weeks or years (Plaha et al. 2004). Plaha et al. (2011) have postulated that tolerance was a major property of VIM itself. Although further evidence with more patients is required for PSA DBS with both short- and long-term follow-up periods, PSA DBS might be preceded by VIM DBS in efficacy and safety. There might be a possibility that VIM and PSA DBS manifest synergic effects on ET (Blomstedt et al. 2012).
11.13 Conclusions
VIM DBS is a standard target for medically intractable tremor. Its short- and long-term efficacies are promising. PSA is a new target for DBS. Short-term efficacy of PSA DBS seems the same or better than VIM DBS, and two publications have reported satisfactory long-term outcomes. The complications and side effects related to PSA are limited, and notably, PSA DBS has been reported to be effective for proximal tremor and free from tolerance. In these points, PSA might be a preferred target for ET. However, further short- and long-term studies with large numbers of patients are required, and it is necessary to compare the effects and complications of PSA DBS with the established target of VIM DBS to elucidate its real therapeutic impact.
References
Anderson ME, Turner RS (1991) Activity of neurons in cerebellar-receiving and pallidal-receiving areas of the thalamus of the behaving monkey. J Neurophysiol 66:879–893
Anderson TR, Hu B, Iremonger K et al (2006) Selective attenuation of afferent synaptic transmission as a mechanism of thalamic deep brain stimulation-induced tremor arrest. J Neurosci 26:841–850
Asanuma C, Thach WR, Jones EG (1983a) Distribution of cerebellar terminations and their relation to other afferent terminations in the ventral lateral thalamic region of the monkey. Brain Res 286:237–265
Asanuma C, Thach WT, Jones EG (1983b) Anatomical evidence for segregated focal groupings of efferent cells and their terminal ramifications in the cerebellothalamic pathway of the monkey. Brain Res 286:267–297
Atkinson JD, Collins DL, Bertrand G et al (2002) Optimal location of thalamotomy lesions for tremor associated with Parkinson disease: a probabilistic analysis based on postoperative magnetic resonance imaging and an integrated digital atlas. J Neurosurg 96:854–866
Bahgat D, Magill ST, Berk C et al (2013) Thalamotomy as a treatment option for tremor after ineffective deep brain stimulation. Stereotact Funct Neurosurg 91:18–23
Baker KB, Boulis NM, Rezai AR et al (2004) Target selection using microelectrode recording. In: Israel Z, Burchiel KJ (eds) Microelectrode recording in movement disorder surgery. Thieme, New York, pp 138–151
Barbe MT, Liebhart L, Runge M et al (2011) Deep brain stimulation of the ventral intermediate nucleus in patients with essential tremor: stimulation below intercommissural line is more efficient but equally effective as stimulation above. Exp Neurol 230:131–137
Bardinet E, Belaid H, Grabli D et al (2011) Thalamic stimulation for tremor: can target determination be improved? Mov Disord 26:307–312
Benabid AL, Pollak P, Gervason C et al (1991) Long-term suppression of tremor by chronic stimulation of the ventral intermediate thalamic nucleus. Lancet 337:403–406
Benabid AL, Pollak P, Gao D et al (1996) Chronic electrical stimulation of the ventralis intermedius nucleus of the thalamus as a treatment of movement disorders. J Neurosurg 84:203–214
Benabid AL, Benazzouz A, Hoffmann D et al (1998) Long-term electrical inhibition of deep brain targets in movement disorders. Mov Disord 13(Suppl 3):s119–s125
Blomstedt P, Hariz GM, Hariz MI et al (2007) Thalamic deep brain stimulation in the treatment of essential tremor: a long-term follow-up. Br J Neurosurg 21:504–509
Blomstedt P, Sandvik U, Fytagoridis A et al (2009) The posterior subthalamic area in the treatment of movement disorders: Past, present, and future. Neurosurgery 64:1029–1042
Blomstedt P, Sandvik U, Tisch S (2010) Deep brain stimulation in the posterior subthalamic area in the treatment of essential tremor. Mov Disord 25:1350–1356
Blomstedt P, Sandvik U, Linder J et al (2011a) Deep brain stimulation of the subthalamic nucleus versus the zona incerta in the treatment of essential tremor. Acta Neurochir 153:2329–2335
Blomstedt P, Sandvik U, Hariz MI et al (2011b) Influence of age, gender and severity of tremor on outcome after thalamic and subthalamic DBS for essential tremor. Parkinsonism Relat Disord 17:617–620
Blomstedt P, Lindvall P, Linder J et al (2012) Reoperation after failed deep brain stimulation for essential tremor. World Neurosurg 78:554E1–554E5
Boecker H, Wills AJ, Ceballos-Baumann A et al (1996) The effect of ethanol on alcohol-responsive essential tremor: a positron emission tomography study. Ann Neurol 39:650–658
Boecker H, Weindl A, Brooks DJ et al (2010) GABAergic dysfunction in essential tremor: an 11C-flumazenil PET study. J Nucl Med 51:1030–1035
Bromberg MB, Penny JB Jr, Stephenson BS et al (1981) Evidence for glutamate as the neurotransmitter of corticothalamic and corticorubral pathways. Brain Res 215:369–374
Butler EG, Horne MK, Hawkins NJ (1992) The activity of monkey thalamic and motor cortical neurones in a skilled, ballistic movement. J Physiol 445:25–48
Carrillo-Ruiz JD, Velasco F, Jimènez F et al (2008) Bilateral electrical stimulation of prelemniscal radiations in the treatment of advanced Parkinson’s disease. Neurosurgery 62:347–359
Carrillo-Ruiz JD, Velasco F, Jiménez F et al (2012) Prelemniscal radiations neuromodulation in Parkinson disease’s treatment. In: Carrillo-Ruiz J (ed) Topics in neuromodulation treatment. InTech, Rijeka, Croatia, pp 63–86. ISBN 978-953-51-0395-0
Ceballos-Baumann AO, Boecker H, Fogel W et al (2001) Thalamic stimulation for essential tremor activates motor and deactivates vestibular cortex. Neurology 56:1347–1354
Cooper S, Bowes M (2012) Surgical considerations for tremor and dystonia. Cleve Clin J Med 79(Suppl 2):S40–S43
Deuschl G, Bergman H (2002) Pathophysiology of nonparkinsonian tremors. Mov Disord 17:S41–S48
Deuschl G, Raethjen J, Lindemann M et al (2001) The pathophysiology of tremor. Muscle Nerve 24:716–735
Deuschl G, Raethjen J, Hellriegel H et al (2011) Treatment of patients with essential tremor. Lancet Neurol 10:148–161
El-Tahawy H, Lozano AM, Dostrovsky JO (2004) Electrophysiological findings in Vim and Vc. In: Israel Z, Burchiel KJ (eds) Microelectrode recording in movement disorder surgery. Thieme, New York, 4:pp 63–71
Favilla CG, Topiol DD, Zesiewicz TA et al (2013) Impact of discontinuing tremor suppressing medications following thalamic deep brain stimulation. Parkinsonism Relat Disord 19:171–175
Fields JA, Tröster AI, Woods SP et al (2003) Neuropsychological and quality of life outcomes 12 months after unilateral thalamic stimulation for essential tremor. J Neurol Neurosurg Psychiatry 74:305–311
Flora ED, Perera CL, Cameron AL et al (2010) Deep brain stimulation for essential tremor: a systematic review. Mov Disord 25:1550–1559
Fytagoridis A, Blomstedt P (2010) Complications and side effects of deep brain stimulation in the posterior subthalamic area. Stereotact Funct Neurosurg 88:88–93
Fytagoridis A, Sandvik U, Åström M et al (2012) Long term follow-up of deep brain stimulation of the caudal zona incerta for essential tremor. J Neurol Neurosurg Psychiatry 83:258–262
Fytagoridis A, Åström M, Wårdell K et al (2013a) Stimulation-induced side effects in the posterior subthalamic area: distribution, characteristics and visualizaion. Clin Neurol Neurosurg 115:65–71
Fytagoridis A, Sjöberg RL, Åström M et al (2013b) Effects of deep brain stimulation in the caudal zona incerta on verbal fluency. Stereotact Funct Neurosurg 91:24–29
Gerasimou G, Costa DC, Papanastasiou E et al (2012) SPECT study with I-123-ioflupane (Da TSCAN) in patients with essential tremor. Is there any correlation with Parkinson’s disease. Ann Nucl Med 26:337–344
Gironell A, Figueiras FP, Pagonabarraga J et al (2012) Gaba and serotonin molecular neuroimaging in essential tremor: a clinical correlation study. Parkinsonism Relat Disord 18:876–880
Godwin DW, Vaughan JW, Sherman SM (1996) Metabotropic glutamate receptors switch visual response mode of lateral geniculate nucleus cells from burst to tonic. J Neurophysiol 76:1800–1816
Govindan RB, Raethjen J, Arning K et al (2006) Time delay and partial coherence analyses to identify cortical connectivities. Biol Cybern 94:262–275
Hamel W, Herzog J, Kopper F et al (2007) Deep brain stimulation in the subthalamic area is more effective than nucleus ventralis intermedius stimulation for bilateral intention tremor. Acta Neurochir (Wien) 149:749–758
Hariz MI (2002) Complications of deep brain stimulation surgery. Mov Disord 17(Suppl 3):s162–s166
Hariz MI, Hirabayashi H (1997) Is there a relationship between size and site of the stereotactic lesion and symptomatic results of pallidotomy and thalamotomy? Stereotact Funct Neurosurg 69:28–45
Hariz MI, Shamsgovara P, Johansson F et al (1999) Tolerance and tremor rebound following long-term chronic thalamic stimulation for Parkinsonian and essential tremor. Stereotact Funct Neurosurg 72:208–218
Hariz GM, Blomstedt P, Koskinen LO (2008) Long-term effect of deep brain stimulation for essential tremor on activities of daily living and health-related quality of life. Acta Neurol Scand 118:387–394
Hassler R (1959) Introduction to stereotaxic operation with an atlas of the human brain. In: Schaltenbrand G, Bailey P (eds) Anatomy of the thalamus. Thieme, Stuttgart, pp 230–290
Heber IA, Coenen VA, Reetz K et al (2013) Cognitive effects of deep brain stimulation for essential tremor: evaluation at 1 and 6 years. J Neural Transm 120:1569–1577
Heise CE, Mitrofanis J (2004) Evidence for a glutamatergic projection from the zona incerta to the basal ganglia of rats. J Comp Neurol 468:482–495
Herzog J, Hamel W, Wenzelburger R et al (2007) Kinematic analysis of thalamic versus subthalamic neurostimulation in postural and intention tremor. Brain 130:1608–1625
Hoover JE, Strick PL (1999) The organization of cerebellar and basal ganglia outputs to primary motor cortex as revealed by retrograde transneuronal transport of herpes simplex virus type 1. J Neurosci 19:1446–1463
Hua SE, Lenz FA (2005) Posture-related oscillations in human cerebellar thalamus in essential tremor are enabled by voluntary motor circuits. J Neurophysiol 93:117–127
Ilinsky IA, Kultas-Ilinsky K (1984) An autoradiographic study of topographical relationships between pallidal and cerebellar projections to the cat thalamus. Exp Brain Res 54:95–106
Ilinsky IA, Kultas-Ilinsky K (1987) Sagittal cytoarchitectonic maps of the Macaca mulatta thalamus with a revised nomenclature of the motor-related nuclei validated by observasions on their connectivity. J Comp Neurol 262:331–364
Ilinsky IA, Kultas-Ilinsky K (2002) Motor thalamic circuits in primates with emphasis on the area targeted in treatment of movement disorders. Mov Disord 17(Suppl 3):s9–s14
Ito Z (1975) Stimulation and destruction of the prelemniscal radiation or its adjacent area in various extrapyramidal disorders. Cofin Neurol 37:41–48
Johnson MD, Vitek JL, Mclntyre CC (2009) Pallidal stimulation that improves parkinsonian motor symptoms also modulates neuronal firing patterns in primary motor cortex in the MPTP-treated monkey. Exp Neurol 219:359–362
Jones EG (2007) The thalamus, vol II, 2nd edn. Cambridge University Press, New York, pp 1297–1447
Kang J, Jiang L, Goldman SA et al (1998) Astrocyte-mediated potentiation of inhibitory synaptic transmission. Nat Neurosci 1:683–692
Katayama Y, Kano T, Kobayashi K et al (2005) Difference in surgical strategies between thalamotomy and thalamic deep brain stimulation for tremor control. J Neurol 252(Suppl 4):17–22
Kiss ZH, Davis KD, Tasker RR et al (2003) Kinaesthetic neurons in thalamus of humans with and without tremor. Exp Brain Res 150:85–94
Kitagawa M, Murata J, Kikuchi S et al (2000) Deep brain stimulation of subthalamic area for severe proximal tremor. Neurology 55:114–116
Kobayashi K, Katayama Y, Sumi K et al (2010) Effects of electrode implantation angle on thalamic stimulation for treatment of tremor. Neuromodulation 13:31–36
Koller WC, Vetere-Overfield B (1989) Acute and chronic effects of propranolol and primidone in essential tremor. Neurology 39:1587–1588
Koller W, Pahwa R, Busenbark K et al (1997) High-frequency unilateral thalamic stimulation in the treatment of essential and parkinsonian tremor. Ann Neurol 42:292–299
Koller WC, Lyons KE, Wilkinson SB et al (1999) Efficacy of unilateral deep brain stimulation of the VIM nucleus of the thalamus for essential head tremor. Mov Disord 14:847–850
Koller WC, Lyons KE, Wilkinson SB et al (2001) Long-term safety and efficacy of unilateral deep brain stimulation of the thalamus in essential tremor. Mov Disord 16:464–468
Krack P, Dostrovsky J, Ilinsky I et al (2002) Surgery of the motor thalamus: problems with the present nomenclatures. Mov Disord 17(Suppl 3):2–8
Krauss JK, Mohadjer M, Nobbe F et al (1994) The treatment of posttraumatic tremor by stereotactic surgery. Symptomatic and functional outcome in a series of 35 patients. J Neurosurg 80:810–819
Kultas-Ilinsky K, Ilinsky IA (1991) Fine structure of the ventral lateral nucleus (VL) of the Macaca mulatta thalamus: cell types and synaptology. J Comp Neurol 314:319–349
Kumar R, Lozano AM, Sime E et al (2003) Long-term follow-up of thalamic deep brain stimulation for essential and parkinsonian tremor. Neurology 61:1601–1604
Kuo JS, Carpenter MB (1973) Organization of pallidothalamic projections in the rhesus monkey. J Comp Neurol 151:201–236
Kurata K (2005) Activity properties and location of neurons in the motor thalamus that project to the cortical motor areas in monkeys. J Neurophysiol 94:550–566
Lehman RM, Augustine JR (2013) Evolution and rebirth of functional stereotaxy in the subthalamus. World Neurosurg 80:521–533
Lenz FA, Kwan HC, Martin RL et al (1994) Single unit analysis of the human ventral thalamus nuclear group. Tremor related activity in functionally identified cells. Brain 117:531–543
Limousin P, Speelman JD, Gielen F et al (1999) Multicentre European study of thalamic stimulation in parkinsonian and essential tremor. J Neurol Neurosurg Psychiatry 66:289–296
Lind G, Schechtmann G, Lind C et al (2008) Subthalamic stimulation for essential tremor. Short- and long-term results and critical target area. Stereotact Funct Neurosurg 86:253–258
Lipp A, Tank J, Trottenberg T et al (2005) Sympathetic activation due to deep brain stimulation in the region of the STN. Neurology 65:774–775
Lou RS, Jankovic J (1991) Essential tremor: clinical correlates in 350 patients. Neurology 41:234–238
Louis ED (2001) Clinical practice. Essential tremor. N Engl J Med 345:887–891
Louis ED, Vonsattel JP (2008) The emerging neuropathology of essential tremor. Mov Disord 23:174–182
Louis ED, Yi H, Erickson-Davis C et al (2009) Structural study of Purkinje cell axonal torpedoes in essential tremor. Neurosci Lett 450:287–291
Louis ED, Babij R, Cortés E et al (2013) The inferior olivary nucleus: a postmortem study of essential tremor. Case versus controls. Mov Disord 28:779–786
Lozano AM (2000) Vim thalamic stimulation for tremor. Arch Med Res 31:266–269
Lozano AM, Levy R (2012) Reoperation of deep brain stimulation in patients with essential tremor. World Neurosurg 78:442–444
Lyons KE, Pahwa R, Busenbark KL et al (1998) Improvements in daily functioning after deep brain stimulation of the thalamus for intractable tremor. Mov Disord 13:690–692
Meng FG, Kao CC, Chen N et al (2013) Deep brain stimulation of the subthalamic nucleus for essential tremor. Chin Med J (Engl) 126:395–396
Miocinovic S, Somayajula S, Chitnis S et al (2013) History, applications, and mechanisms of deep brain stimulation. JAMA Neurol 70:163–171
Mitrofanis J (2005) Some certainty for the “zone of uncertainty”? Exploring the function of the zona incerta. Neuroscience 130:1–15
Mitrofanis J, Ashkan K, Wallace BA et al (2004) Chemoarchitectonic heterogeneities in the primate zona incerta: clinical and functional implications. J Neurocytol 33:429–440
Miyagishima T, Takahashi A, Kikuchi S et al (2007) Effect of ventralis intermedius thalamotomy on the area in the sensorimotor cortex activated by passive hand movements: fMR imaging study. Stereotact Funct Neurosurg 85:225–234
Mohadjer M, Goerke H, Milios E et al (1990) Long-term results of stereotaxy in the treatment of essential tremor. Stereotact Funct Neurosurg 54–55:125–129
Montgomery EB Jr, Baker KB (2000) Mechanisms of deep brain stimulation and future technical developments. Neurol Res 22:259–266
Morel A (2007) Subthalamic fiber tracts. In: Morel A (ed) Stereotactic atlas of the human thalamus and basal ganglia. Informa Healthcare USA, Inc., New York, pp 111–118
Morigaki R, Nagahiro S, Kaji R et al (2010) Current use of thalamic surgeries for treating movement disorders. In: Song JL (ed) Thlamus: anatomy, functions and disorders. Nova Science Publisher, New York, pp 1–31
Mundinger F (1969) Results f 500 subthalamotomies in the region of the zona incerta. In: Third Symposium on Parkinson’s disease. E & S Livingstone, Edinburgh/London, pp 261–265
Murata J, Kitagawa M, Uesugi H et al (2003) Electrical stimulation of the posterior subthalamic area for the treatment of intractable proximal tremor. J Neurosurg 99:708–715
Nakano K (2000) Neural circuits and topographic organization of the basal ganglia and related regions. Brain Dev 22(Suppl 1):S5–S16
Nazzaro JM, Pahwa R, Lyons KE (2012) Long-term benefits in quality of life after unilateral thalamic deep brain stimulation for essential tremor. J Neurosurg 117:156–161
Nguyen JP, Degos JD (1993) Thalamic stimulation and proximal tremor. A specific target in the nucleus ventrointermedius thalami. Arch Neurol 50:498–500
Obwegeser AA, Uitti RJ, Turk MF (2000) Thalamic stimulation for the treatment of midline tremors in essential tremor patients. Neurology 54:2342–2344
Ohye C, Narabayashi H (1979) Physiological study of presumed ventralis intermedius neurons in the human thalamus. J Neurosurg 50:290–297
Ohye C, Shibazaki T, Hirai T (1989) Further physiological observations on the ventralis intermedius neurons in the human thalamus. J Neurophysiol 61:488–500
Ondo W, Jankovic J, Schwartz K et al (1998) Unilateral thalamic deep brain stimulation for refractory essential tremor and Parkinson’s disease tremor. Neurology 51:1063–1069
Pahwa R, Lyons KL, Wilkinson SB et al (1999) Bilateral thalamic stimulation for the treatment of essential tremor. Neurology 53:1447–1450
Pahwa R, Lyons KE, Wilkinson SB et al (2006) Long-term evaluation of deep brain stimulation of the thalamus. J Neurosurg 104:506–512
Papavassiliou E, Rau G, Heath S et al (2004) Thalamic deep brain stimulation for essential tremor: relation of lead location to outcome. Neurosurgery 54:1120–1129
Park YG, Park HY, Lee CJ et al (2010) Ca(V)3.1 is a tremor rhythm pacemaker in the inferior olive. Proc Natl Acad Sci U S A 107:10731–10736
Pedrosa DJ, Auth M, Eggers C et al (2013) Effects of low-frequency thalamic deep brain stimulation in essential tremor patients. Exp Neurol 248:205–212
Percheron G, François C, Talbi B et al (1996) The primate motor thalamus. Brain Res Rev 22:93–181
Perlmutter JS, Mink JW, Bastian AJ et al (2002) Blood flow responses to deep brain stimulation of thalamus. Neurology 58:1388–1394
Pilitsis JG, Metman LV, Toleikis JR et al (2008) Factors involved in long-term efficacy of deep brain stimulation of the thalamus for essential tremor. J Neurosurg 109:640–646
Plaha P, Patel NK, Gill SS (2004) Stimulation of the subthalamic region for essential tremor. J Neurosurg 101:48–54
Plaha P, Ben-Shlomo Y, Patel NK et al (2006) Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving contralateral parkinsonism. Brain 129:1732–1747
Plaha P, Khan S, Gill SS (2008) Bilateral stimulation of the caudal zona incerta nucleus for tremor control. J Neurol Neurosurg Psychiatry 79:504–513
Plaha P, Javed S, Agombar D et al (2011) Bilateral caudal zona incerta nucleus stimulation for essential tremor: outcome and quality of life. J Neurol Neurosurg Psychiatry 82:899–904
Putzke JD, Uitti RJ, Obwegeser AA et al (2005) Bilateral thalamic deep brain stimulation: midline tremor control. J Neurol Neurosurg Psychiatry 76:684–690
Raethjen J, Deuschl G (2012) The oscillating central network of essential tremor. Clin Neurophysiol 123:61–64
Raethjen J, Govindan RB, Kopper F et al (2007) Cortical involvement in the generation of essential tremor. J Neurophysiol 97:3219–3228
Raeva SN, Vainberg NA, Dubynin VA et al (1999) Changes in the spike activity of neurons in the ventrolateral nucleus of the thalamus in humans during performance of a voluntary movement. Neurosci Behav Physiol 29:505–513
Rehncrona S, Johnels B, Widner H et al (2003) Long-term efficacy of thalamic deep brain stimulation for tremor: double-blind assessments. Mov Disord 18:163–170
Sakai ST, Inase M, Tanji J (1996) Comparison of cerebellothalamic and pallidothalamic projections in the monkey (Macaca fuscata): a double anterograde labeling study. J Comp Neurol 368:215–228
Sandvik U, Hariz GM, Blomstedt P (2012) Quality of life following DBS in the caudal zona incerta in patients with essential tremor. Acta Neurochir 154:495–499
Schelter B, Timmer J, Eichler M (2009) Assessing the strength of directed influences among neural signals using renormalized partial directed coherence. J Neurosci Methods 179:121–130
Schnitzler A, Münks C, Butz M et al (2009) Synchronized brain network associated with essential tremor as revealed by magnetoencephalography. Mov Disord 24:1629–1635
Schuurman PR, Bosch DA, Bossuyt PM et al (2000) A comparison of continuous thalamic stimulation and thalamotomy for suppression of severe tremor. N Engl J Med 342:461–468
Schuurman PR, Bosch DA, Merkus MP et al (2008) Long-term follow-up of thalamic stimulation versus thalamotomy for tremor suppression. Mov Disord 23:1146–1153
Shih LC, LaFaver K, Lim C et al (2013) Loss of benefit in VIM thalamic deep brain stimulation (DBS) for essential tremor (ET): how prevalent is it? Parkinsonism Relat Disord 19:676–679
Sidibé M, Bevan MD, Bolam JP et al (1997) Efferent connections of the internal globus pallidus in the squirrel monkey: I. Topography and synaptic organization of the pallidothalamic projection. J Comp Neurol 382:323–347
Spiegel EA, Wycis HT, Szekely EG et al (1963) Campotomy in various extrapyramidal disorders. J Neurosurg 20:871–884
Starr PA, Vitek JL, Bakay RA (1998) Ablative surgery and deep brain stimulation for Parkinson’s disease. Neurosurgery 43:989–1013
Stover NP, Okun MS, Evatt ML et al (2005) Stimulation of the subthalamic nucleus in a patient with Parkinson disease and essential tremor. Arch Neurol 62:141–143
Strick PL (1976) Activity of ventrolateral thalamic neurons during arm movement. J Neurophysiol 39:1032–1044
Sydow O, Thobois S, Alesch F et al (2003) Multicentre European study of thalamic stimulation in essential tremor: a six year follow up. J Neurol Neurosurg Pscychiatry 74:1387–1391
Taha JM, Janszen MA, Favre J (1999) Thalamic deep brain stimulation for the treatment of head, voice, and bilateral limb tremor. J Neurosurg 91:68–72
Tamma F, Caputo E, Chiesa V et al (2002) Anatomo-clinical correlation of intraoperative stimulation-induced side-effects during HF-DBS of the subthalamic nucleus. Neurol Sci 23(Suppl 2):s109–s110
Tarsy D, Scollins L, Corapi K et al (2005) Progression of Parkinson’s disease following thalamic deep brain stimulation for tremor. Stereotact Funct Neurosurg 83:222–227
Tasker RR (1998) Deep brain stimulation is preferable to thalamotomy for tremor suppression. Surg Neurol 49:145–153
Tawfik VL, Chang SY, Hitti FL et al (2010) Deep brain stimulation results in local glutamate and adenosine release: investigation into the role of astrocytes. Neurosurgery 67:367–375
Theodosopoulos PV, Turner RS, Starr PA (2004) Electrophysiological findings in STN and SNr. In: Israel Z, Burchiel KJ (eds) Microelectrode recording in movement disorder surgery. Thieme, New York, pp 82–89
Tian GF, Azmi H, Takano T et al (2005) An astrocytic basis of epilepsy. Nat Med 11:973–981
Tröster AI, Fields JA, Pahwa R et al (1999) Neuropsychological and quality of life outcome after thalamic stimulation for essential tremor. Neurology 53:1774–1780
Tsoukatos J, Kiss ZH, Davis KD et al (1997) Patterns of neuronal firing in the human lateral thalamus during sleep and wakefulnee. Exp Brain Res 113:273–282
Vaillancourt DE, Sturman MM, Verhagen Metman L et al (2003) Deep brain stimulation of the VIM thalamic nucleus modifies several features of essential tremor. Neurology 61:919–925
Velasco FC, Molina-Negro P, Bertrand C et al (1972) Further definition of the subthalamic target for arrest of tremor. J Neurosurg 36:184–191
Velasco F, Jiménez F, Pérez ML et al (2001) Electrical stimulation of the prelemniscal radiation in the treatment of Parkinson’s disease: an old target revised with new techniques. Neurosurgery 49:293–308
Vitek JL (2002) Mechanisms of deep brain stimulation: excitation or inhibition. Mov Disord 17(Suppl 3):s69–s72
Vitek JL, Ashe J, DeLong MR et al (1994) Physiologic properties and somatotopic organization of the primate motor thalamus. J Neurophysiol 71:1498–1513
Vitek JL, Bakay RA, Hashimoto T et al (1998) Microelectrode-guided pallidotomy: technical approach and its application in medically intractable Parkinson’s disease. J Neurosurg 881027–1043
Wilms H, Sievers J, Deuschl G (1999) Animal models of tremor. Mov Disord 14:557–571
Wu YR, Levy R, Ashby P et al (2001) Does stimulation of the GPi control dyskinesia by activating inhibitory axons? Mov Disord 16:208–216
Xie T, Bernard J, Warnke P (2012) Post subthalamic area deep brain stimulation for tremors: a mini-review. Transl Neurodegener 1:20
Yamamoto T, Katayama Y, Kano T et al (2004) Deep brain stimulation for the treatment of parkinsonian, essential, and poststroke tremor: a suitable stimulation method and changes in effective stimulation intensity. J Neurosurg 101:201–209
Zesiewicz TA, Elble RJ, Louis ED et al (2011) Evidence-based guideline update: treatment of essential tremor: report of the Quality Standards subcommittee of the American Academy of Neurology. Neurology 77:1752–1755
Zhang K, Bhatia S, Oh MY et al (2010) Long-term results of thalamic deep brain stimulation for essential tremor. J Neurosurg 112:1271–1276
Zirh TA, Lenz FA, Reich SG et al (1998) Patterns of bursting occurring in thalamic cells during parkinsonian tremor. Neuroscience 83:107–121
Acknowledgements
This work was supported in part by the Grants from the Ministry of Education, Culture, Sports, Science and Technology of Japan (grant-in-aid for Scientific Research, 23500428; 21390269; 23659458; 24390223; 26461272).
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Morigaki, R., Goto, S. (2015). Deep Brain Stimulation for Essential Tremor. In: Itakura, T. (eds) Deep Brain Stimulation for Neurological Disorders. Springer, Cham. https://doi.org/10.1007/978-3-319-08476-3_11
Download citation
DOI: https://doi.org/10.1007/978-3-319-08476-3_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-08475-6
Online ISBN: 978-3-319-08476-3
eBook Packages: MedicineMedicine (R0)