Abstract
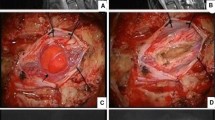
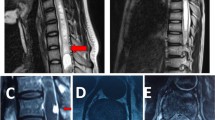
A 42-year-old female presented asymptomatic (accidentally discovered, at 8 years follow-up imaging, after prior treatments of intracranial multiple hemangioblastomas). The patient was treated with upfront (primary); Linac-based (shaped-beam) SRS for cervical spinal cord (C4) hemangioblastoma. The target volume of 1.5 cc received a marginal dose of 12.0 Gy normalized to 90% isodose line. At 12 months post-SRS, the patient remained asymptomatic. Follow-up MRI showed a mild decrease in tumor size. At 24 months post-SRS, the patient was asymptomatic and neurologically intact. Follow-up MRI showed more decrease in tumor size. Continued clinical and radiological follow-up was advised.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Spinal cord hemangioblastoma
- Spinal cord tumor
- Intramedullary spinal tumor
- Linac-based SRS
- Shaped-beam
- Primary radiosurgery
- Spine radiosurgery
-
Demographics: Female; 42 years
-
Initial Presentation:
-
Asymptomatic
-
On regular follow-up after prior treatments of intracranial multiple hemangioblastomas
-
-
Diagnosis: Spinal cord hemangioblastoma
-
Pre-radiosurgery Treatment: Surgery and radiation therapy of other intracranial multiple hemangioblastomas; 8 years before radiosurgery treatment
-
Pre-radiosurgery Presentation: Asymptomatic (accidentally discovered, at 8 years follow up imaging, after prior treatments of intracranial multiple hemangioblastomas)
-
Radiosurgery Treatment:
Upfront (Primary); Linac-based (Shaped-beam) SRS for cervical spinal cord (C4) hemangioblastoma
-
Radiosurgery Dosimetry:
-
Target volume: 1.5 cc
-
Marginal dose: 12.0 Gy
-
Marginal isodose: 90%
-
Maximum dose: 13.3 Gy
-
Minimum dose: 12.0 Gy
-
Average dose: 12.7 Gy
-
Number of isocenters: 1
-
-
Follow-Up Period: 24 months post-SRS
-
Clinical Outcome:
-
12 months post-SRS: Asymptomatic
-
24 months post-SRS: Asymptomatic
-
-
Complications: None
-
Radiological Outcome:
-
12 months post-SRS (MRI): Mild decrease in tumor size
-
24 months post-SRS (MRI): More decrease in tumor size
-
-
Post-radiosurgery Treatment: Continued clinical and radiological follow-up




Further Reading
Avanzo M, Romanelli P. Spinal radiosurgery: technology and clinical outcomes. Neurosurg Rev. 2009;32(1):1–12; discussion 12–13, 1.
Bridges KJ, Jaboin JJ, Kubicky CD, et al. Stereotactic radiosurgery versus surgical resection for spinal hemangioblastoma: a systematic review. Clin Neurol Neurosurg. 2017;154:59–66.
Daly ME, Choi CY, Gibbs IC, et al. Tolerance of the spinal cord to stereotactic radiosurgery: insights from hemangioblastomas. Int J Radiat Oncol Biol Phys. 2011;80:213–20.
Hernández-Durán S, Hanft S, Komotar RJ, et al. The role of stereotactic radiosurgery in the treatment of intramedullary spinal cord neoplasms: a systematic literature review. Neurosurg Rev. 2016;39(2):175–83; discussion 183.
Liu EK, Silverman JS, Sulman EP, et al. Stereotactic radiation for treating primary and metastatic neoplasms of the spinal cord. Front Oncol. 2020;9(10):907.
Selch MT, Tenn S, Agazaryan N, et al. Image-guided linear accelerator-based spinal radiosurgery for hemangioblastoma. Surg Neurol Int. 2012;3:73.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Abdelaziz, O.S., De Salles, A.A.F. (2023). Spinal Cord Hemangioblastoma. In: NeuroRadiosurgery: Case Review Atlas. Springer, Cham. https://doi.org/10.1007/978-3-031-16199-5_71
Download citation
DOI: https://doi.org/10.1007/978-3-031-16199-5_71
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-16198-8
Online ISBN: 978-3-031-16199-5
eBook Packages: MedicineMedicine (R0)