Abstract
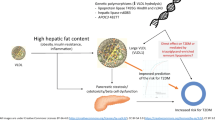
Triacylglycerol (TG)-enriched remnant lipoproteins (TRL) metabolism has a central role in cardiovascular disease, but more recently TRL particles got into evidence for their potential relationship with type 2 diabetes. TRL particle size and VLDL-triglyceride content have been implicated in the risk of type 2 diabetes and particularly a shift to larger VLDL particles (VLDL1) can improve risk prediction of type 2 diabetes. The chapter goes on to discuss research in humans that addresses these relationships, as well as potential direct and indirect mechanisms that may justify the use of TG-enriched remnant lipoprotein to predict future risk of type 2 diabetes. Obesity, insulin resistance and systemic inflammation play a role in increasing hepatic fat content and upregulating TRL particle size; however, it is less clear weather the connection VLDL1 and type 2 diabetes is direct (causal) or genetically mediated. Finally, the chapter discusses new perspectives in identifying new TG and TRL size-related biomarkers for the risk of type 2 diabetes and cardiovascular diseases, including untargeted lipidomics.
Access provided by Autonomous University of Puebla. Download reference work entry PDF
Similar content being viewed by others
Keywords
- Triacylglycerol-enriched remnant lipoproteins
- TRL
- TRL particle size
- Triacylglycerol
- Type 2 diabetes
- VLDL1
- Cardiovascular diseases
- Lipidomics
- NMR
- Mass spectrometry
- Risk prediction
Introduction
Clinical interest in the treatment of triacylglycerol (TG)-enriched remnant lipoproteins (TRL) has fluctuated between opposite extremes in recent decades. The hesitation between measuring and treating or not high levels of TRL has been driven by polarized evidence, sometimes suggesting that these lipoproteins may be causally associated with diabetes and atherosclerotic cardiovascular disease (CVD), and sometimes suggesting that such lipoproteins would represent only innocent bystanders of metabolism of high-density lipoproteins (HDL) (Chapman et al. 2011). Probably more important has been the stagnation on the basis of new clinical evidence or new specific therapies that could reinforce the benefit of reducing triglycerides. In addition, the measurement of TG-enriched remnant lipoproteins features other than TG content such as particle size, particle number and cholesterol content are still not commercially available in many countries.
In the 1980s and 1990s, most clinical guidelines suggested measuring and treating mild to moderately high triglyceride levels (200–500 mg/dL) (Pyorala et al. 1994). The wide interest in triglyceride-rich lipoproteins at the time was related to several factors, among them positive results from incipient clinical trials and the Zilversmith hypothesis (Zilversmit 1979), which explained atherogenesis and other metabolic diseases as a postprandial phenomenon and related to the increase in TG-enriched remnant lipoproteins.
However, from the late 1990s to recent years, most recommendations focused mainly on LDL (low-density lipoprotein) cholesterol and largely ignored the need for treatment of mild to moderately high levels of triglycerides. One of the main explanations for the lack of interest in TG-enriched remnant lipoproteins was the failure of most clinical trials with fibrates, which was interpreted by most clinicians as the failure of the “triglyceride hypothesis” (Group et al. 2014; Investigators et al. 2011). However, these clinical trials have not evaluated the effect of specific reduction of TG-enriched remnant lipoproteins on the risk diabetes.
In the last decade, the spotlight turned back to TG-enriched remnant lipoproteins, with the emergence of technologies combining niacin and EPA (CAT-2003), high-dose EPA (icosapent-ethyl), anti-apoC-III antisense therapies (volanesorsen), DGAT1 inhibitors (pradigastat), anti-angiopoietin-like protein 3 (ANGPTL3) antibodies (evinacumab), MTP inhibitors (lomitapide), LPL gene therapy (alipogene tiparvovec), and many others. With that, several novel population studies in parallel revealed TG-enriched remnant lipoproteins features showed strong association with the risk of diabetes and CVD. In this context, and with the evidence from genetic studies accumulated in the last 10 years, TG-enriched remnant lipoproteins are once again gaining importance in the scenario of diabetes and CVD risk prediction.
Risk Prediction of Diabetes and the Role of Lipoproteins
Glycemic status at baseline is the most important predictor for future diabetes and individuals characterized by prediabetes show a 2- to 10-fold higher risk for diabetes compared to non-prediabetic individuals (Richter et al. 2018). Conversely, among those without pre-diabetes, the glycemic status has a smaller value and thus long-term risk prediction of diabetes in this population is much less precise (Abdul-Ghani and DeFronzo 2009). With these evidences, it becomes clear that new predictors are necessary to improve the capacity of identifying individuals at high risk of developing type 2 diabetes, especially among individuals without pre-diabetes.
Lipoproteins are key factor in trafficking lipids among tissues and particularly LDL and VLDL particles are implicated in the trafficking of lipids to pancreatic beta cells. Beta cell dysfunction is influenced by increased fatty acid content and increased plasma levels of both VLDL-triglycerides and LDL-cholesterol (Hao et al. 2007; Oh et al. 2018). Large VLDL particles usually carry an elevated content of triglycerides and animals with this phenotype show increased pancreatic cell lipotoxicity (Zhang et al. 2019). Pancreatic cell lipotoxicity is a major driver of beta cell dysfunction, thus increasing the risk of type 2 diabetes (Robertson et al. 2004). More recently, TRL particle size and VLDL-triglyceride content have been implicated in the risk of type 2 diabetes and particularly a shift from to high VLDL1 concentration with elevated TRL particle size can improve risk prediction of type 2 diabetes in individuals without pre-diabetes (Carvalho et al. 2021).
The Role of Large VLDL Particles (High Density of VLDL1 Particles) in Risk Prediction of Diabetes: Results from Clinical Studies
The ELSA-Brasil study showed that, when participants without diabetes at baseline were divided in quartiles of TRL particle diameter, those larger TRL particles showed dysfunctional glucose homeostasis and lipid metabolism (Carvalho et al. 2021). Individuals with baseline HbA1c between 39 and 46 mmol/mol (5.7–6.4%) had stronger associations with insulin resistance (HOMA-IR), waist circumference, and hsCRP as compared to those with baseline HbA1c <5.7%. The study therefore hypothesizes that individuals with pre-diabetes status, baseline HbA1c of 5.7–6.4%, could increase the hepatic release of large VLDL particles or impair their catabolism (i.e., reduced lipoprotein lipase activity) due to a number of risk factors that they present, like obesity, hepatic steatosis, insulin resistance, and heightened inflammation (Carvalho et al. 2021).
Among subjects with intermediate hyperglycemia at baseline, TRL particle size present a borderline capacity for predicting diabetes when compared to a baseline model composed by age, sex, hypertension, parental history of type 2 diabetes, waist circumference, systolic blood pressure, HbA1c, triacylglycerol and HDL-cholesterol. The baseline model shows area under the receiver-operating characteristic curve (AUROC) of 0.708 [95% CI 0.685, 0.732], while the addition of TRL particle size slightly increases AUROC to 0.729 [95%CI 0.696, 0.768] (p for difference = 0.0647). In multivariate analyses, the study found an increase for incident diabetes by 32% in each 10 nm increment in TRLZ size (95% CI 7.3, 57.2, p = 0.0103) (Carvalho et al. 2021).
Contrarywise, TRL particle size showed the best association with diabetes risk in subjects with no glycemic abnormalities at baseline. Furthermore, TRL particle size increased the AUROC for predicting type 2 diabetes on top of the best available model in a large and multi-ethnic cohort with a sustained univariate and multivariate effect.
Although it is clear that conditions such as obesity, insulin resistance and systemic inflammation play a role in increasing hepatic fat content and upregulating TRL particle size, it is less clear weather the connection between larger VLDL particles (VLDL1) and type 2 diabetes is direct (causal) or indirect through genetic mediation. In the next paragraphs the focus is to discuss the evidence for direct or indirect associations between TRL particle size and type 2 diabetes.
The Role of Large VLDL Particles (High Density of VLDL1 Particles) in Risk Prediction of Diabetes: Rationale Suggesting a Causal Role
Inflammation stands as a critical player in the development of insulin resistance by affecting lipid metabolism in adipose tissues. Particularly, tumor necrosis factor (TNF)-α pathways inhibit lipoprotein lipase in adipose cells, resulting in increased non-esterified fatty acid level and causing overproduction of intestinally derived VLDL1 by stimuli of p38-mitogen-activated protein kinase (Akash et al. 2018; Qin et al. 2007). Furthermore, TNF-α active transcriptional factor, NF-kB, actively mediate the apoptosis of pancreatic ß-cells (Akash et al. 2018). Bearing these data, several anti-TNF-α treatments have been tested targeting insulin resistance mitigation and pancreatic ß-cell preservation. In experimental animal studies by Borst et al. (Borst and Bagby 2002), TNF-α inhibition improved insulin resistance, while the neutralization of TNF-α in an animal model by Tzanavari et al. (2010) improved the hepatic insulin resistance. In humans, Martin-Rodriguez et al. (2019) analyzed a healthy non-diabetic Caucasian population and showed a positive correlation between HOMA-IR and hepatic triglycerides, and also between plasma TNF-α concentrations and intrahepatic triglyceride content levels and HOMA-IR.
Insulin resistance is associated with increased production of glycerol 3-phosphate via increased gluconeogenesis and triglyceride synthesis via de novo lipogenesis. Both mechanisms trigger the expression of sterol regulatory element binding protein 1c (SREBP1c) (Browning and Horton 2004). The overlap between variations in metabolism and the change in TRL physiology in insulin resistance could clarify the reason why TRL particle size augment the predictive capacity for type 2 diabetes as compared to classic risk factors in non-prediabetic subjects. (Carvalho et al. 2021).
Many studies have suggested a potentially causal relationship between VLDL1 levels and the risk of diabetes (Qi et al. 2012). Another interesting finding is that the accumulation of fat in non-adipose tissue (e.g., liver and muscle) is highly associated with the risk of type 2 diabetes mellitus (Czech et al. 2013). All these effects are potentially due to the development of pancreatic steatosis and cytotoxicity.
In mouse, Zhang et al (2019) chose two hypertriglyceridemia models: apolipoprotein C3-transgenic (ApoC3-tg) and glycosylphosphatidylinositol-anchored high-density lipoprotein binding protein-1 knockout (Gpihbp1−/−). These genetic mutations are related with lipoprotein lipase activity, which leads to severe hypertriglyceridemia. Indeed, authors found that plasma from Gpihbp1−/− mice had much larger TRL particles, composed mainly of large chylomicron particles compared with ApoC3-tg mice, which has mainly small VLDL particles as adjusted by triglyceride content (Zhang et al. 2019). The pancreas of Gpihbp1−/− mice presented more free-fatty acids, hydrolysis products of TRLs, than ApoC3-tg mice suggesting that greater FFA production may predispose pancreatic necrosis, by cytotoxic effects in pancreatic acinar cells (Zhang et al. 2019).
Finally, several studies have demonstrated that decreasing the excess lipid from pancreas and liver improves insulin sensitivity, returning to a normal insulin secretion in early type 2 diabetes (Lim et al. 2011; Steven et al. 2016). Although these evidences are compelling to link TRL particle size to the risk of diabetes, they are not sufficient to state there is a causal role between these two elements. More recently, a large burden of evidence outlined a potential indirect role between TRL particle size and the risk of diabetes.
The Role of VLDL Particles and Triglycerides in Risk Prediction of Diabetes: What is the Role of Genetics?
The development of type 2 diabetes is a complex process resulting from the combination of genetic, environmental, behavioral, and aging factors. Family-based studies revealed that the complete understanding of the molecular mechanisms that are involved in the pathophysiology and susceptibility of type 2 diabetes is a challenge and is also influenced by genetic and epigenetic factors (Rich 1990). The risk of developing diabetes throughout lifespan is about 40% when one parent is affected, and this rate rises to 70% when both parents are diabetic (Rich 1990).
Genome-wide association studies (GWASs) were largely responsible for identifying more than 400 genetic variants at 250 distinct loci, including several single nucleotide polymorphisms (SNPs) associated with the risk of type 2 diabetes (Torres et al. 2014; Qi et al. 2012; Mahajan et al. 2018). These methods were able to identify genes associated with monogenic variants of type 2 diabetes such as lipodystrophy, severe insulin resistance (in non-obese individuals), and Maturity-Onset Diabetes of the Young (MODY). However, when the same methods were used to identify the most common forms of diabetes, only a few genes were shown as relevant (Billings and Florez 2010).
Despite GWASs have discovered many new genetic associations, these findings represent events of mid-frequency and common occurrences, not including rare frequency variants and minor variants of cumulative effect (Korte and Farlow 2013) {Billings and Florez 2010 #50}. Therefore, it is necessary to identify a part of the genetic variation that cannot be explained by all significant SNPs (Torres et al. 2014).
In an analysis focusing on the impact that the various polymorphisms have on the development of type 2 diabetes, a genotypic score was established to estimate the genetic predisposition to dyslipidemia based on well-established SNPs located in 95 loci for blood lipids, 25 of which had a direct influence on triglycerides. Each additional risk allele in the genotype scores of HDL cholesterol or triglycerides was associated with 2–3% increased risk for type 2 diabetes. Added the effects, this triglyceride genotype score was able to explain about 10% of the variation of plasma TRL in the evaluated population (Qi et al. 2012; Teslovich et al. 2010).
Most genetic polymorphism sites related to type 2 diabetes were identified by GWASs based on case-control cohorts of European descendants (Andersen et al. 2016). Most extensive data available comes from studies with Caucasian population, including more than 300,000 individuals, where the presence of one particular minor allele linked to rs662799 SNP associates with a 0.25 mmol/l in plasma TG levels (Triglyceride Coronary Disease Genetics et al. 2010). In other populations such as Latin American populations, the role of genetic loci in plasma TG levels and VLDL particles look more evident.
Among various polymorphisms associated with increased risk of type 2 diabetes in Latin American population the SLC16A11 gene polymorphisms have major importance. SLC16A11 messenger RNA is expressed in the liver and it influences lipid metabolism, mainly by promoting an increase in intracellular triacylglycerol levels. In an analysis that included Latin Americans, especially Mexicans, individuals that carry the risk haplotype develop type 2 diabetes approximately 2 years earlier than not carries. Another interesting finding was that the same patient had a higher incidence of type 2 diabetes, even with a body mass index nearly 1 kg/m2 lower and, finally, the odds ratio for type 2 diabetes among those with the risk haplotype was higher in younger individuals (≤45 years) than older individuals (OR 1.48 vs. 1.11) compared to those individuals without the risk haplotype (Consortium et al. 2014).
The Role of Large VLDL Particles (High Density of VLDL1 Particles) in Risk Prediction of Diabetes: Genetics as a Fundamental Player
Due to the specificity of common single nucleotide variants among different ethnic groups that have already been subjected to genotyping, more specific variants have been identified, often with different phenotypic impacts in each ethnic group (Andersen et al. 2016). A well-documented SNP identified as rs12310367 in the apolipoprotein C3 (APOC3) is directly related to alterations in the production of the protein component of TRLs, including VLDL (Valladolid-Acebes et al. 2021).
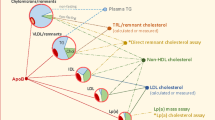
Overexpression of APOC3 is associated with high triglyceride levels and large VLDL particles, while reduction or loss of function mutations in the gene encoding APOC3 are associated with low plasma triglyceride levels and reduced risk of ischemic cardiovascular disease (Adiels et al. 2019). In individuals with abdominal obesity, plasma triglyceride concentrations are elevated as well as the presence of VLDL1 subspecies. The catabolism of VLDL1 is mostly dependent on APOC3 concentration. Furthermore, overexpression of APOC3 has been related to the promotion of VLDL assembly and secretion in hepatocytes in genetically modified mice in vitro experiments (Boren et al. 2015).
In addition to these findings, it has been reported that APOC3 metabolism is significantly unsettled in type 2 diabetes patients. These evidences suggest that glucose homeostasis is associated with APOC3 metabolism, and that the secretion rate of APOC3 seems to be a relevant actor in increasing TRL particle size and triglyceride content observed among individuals with type 2 diabetes (Boren et al. 2020).
Finally, apolipoprotein AV (ApoAV) is also associated with TG-rich lipoproteins. APOAV gene and its genetic variants influence both plasma triglyceride levels and VLDL remodeling. In addition, ApoAV also reduces plasma triglycerides by inhibiting VLDL-TG production and stimulating lipoprotein lipase-mediated VLDL-TG hydrolysis, thus reducing VLDL particle size (Schaap et al. 2004). Two minor alleles (C1131 and Trp19) of APOAV are related to reduced activity of APOAV and results in high plasma triglyceride levels (Hubacek 2016).
These genetic polymorphisms could underlie the indirect relationship between TRL particle size and the risk of type 2 diabetes. However, as pointed out, the genetic background does not fully answer this link and it is plausible to consider that both direct and indirect effects play a role. To better understand pathways to identify more specific markers to link TRL particle size and the risk of diabetes, the next section is dedicated to discuss the perspective of using lipidomics to study TRL metabolism and its associations with diseases.
Lipidomics as Tool to Study TRL Metabolism and the Risk of Diabetes
Advances in liquid chromatography tandem mass spectrometry (LC-MS) technologies have enabled an initial characterization of the human plasma lipidome (i.e., lipidomics (Quehenberger et al. 2010, 2011; Bowden et al. 2017)) and thereby its application to the discovery of novel lipid markers and targets for treatment of metabolic diseases (Rhee et al. 2011; Stegemann et al. 2014; O’Donnell et al. 2014). A direct link between TRL and lipidomics is to ascertain specific TG species as markers of health and disease status. The importance of such data relies on the composition of specific fatty acids esterified to TG, allowing a categorization of plasma TG species into different fatty acids (i.e., short, medium, long, and very long chains or degrees of unsaturation). This information could provide essential clues on their association with and effects on blood lipids, glucose-insulin homeostasis, insulin resistance, and diabetes.
To illustrate the potential of lipidomics in predicting T2DM, a selected list of five recent papers involving a comprehensive analysis of the plasma lipidome was compared (Fig. 1). Although investigating an extensive panel of lipids (180–800 species divided into 8–24 lipid classes), these studies revealed a surprisingly low number of overlapping lipid species associated with the incidence of T2DM (Fig. 1a). Nonetheless, there is a consistent prevalence of TG species among plasma lipid classes from which concentrations are positively correlated with T2DM incidence (Fig. 1b), despite the distinct populations (e.g., METSIM, SAFHS, PREDIMED, and REACTION cohorts) and periods for T2DM incidence (ranging from 3.8 to 21.2 years) reported. The data also revealed that most of these specific TG species are linked to fatty acids containing low number of carbon atoms and double bonds, with an averaged chain length and unsaturation of ca. 17 carbons and 0.7 double bonds (Fig. 1b). While far from conclusive, the data in Fig. 1 suggest that the prevalence of such TG species characterizing cases of incident T2DM might be linked to TRL levels.
Comparative analysis of five comprehensive lipidomic studies in the context of T2DM incidence. (a) Venn-diagram displaying the number of overlapping lipid species associated with T2DM incidence. (b) Detailed analysis of the number of lipids (#lipids) commonly associated with T2DM incidence to all studies, 4 or 3 out of 5 studies. Given that several lipid species belonged to TG (%TG), the average number of carbon atoms and double bonds in fatty acids linked to TG (TG-FA as X:Y, where X and Y denote the number of carbon atoms and double bonds, respectively) and the diagnostic TG species (TG sp. as X:Y) are shown (Kulkarni et al. 2017; Razquin et al. 2018; Suvitaival et al. 2018; Lu et al. 2019; Fernandez et al. 2020)
The assessment of TRL levels is challenging due to several factors including interindividual and intraindividual variation in plasma TG levels, highly heterogeneous size, density and composition of circulating TRL, and distinct sources of remnant lipoproteins (i.e., intestine or liver derived particles (Twickler et al. 2004)). The concentrations of TRL have been measured by different methods based on density, size, electrostatic charge, lipid and apolipoprotein components, or immunoaffinity (Cohn et al. 1999). For large-scale population studies, modern methods to access TRL levels include 1H-NMR lipoprotein spectroscopy analysis that can be applied to determine subclasses of TRL based on their size spectrum (Carvalho et al. 2021; Varga et al. 2021). The NMR is a low-cost and nondestructive technique that performs a quick analysis with highly reproducible data and free of batch analysis effects (i.e., no interaction of samples and equipment). While MS-based lipidomics is highly sensitive (can be used to monitor hundreds of compounds) and requires only a small volume of sample, there are some drawbacks in applying MS for population studies. For instance, the elevated costs associated with sample preparation (e.g., requirement for analytical internal standards to allow quantitative analysis), moderate data reproducibility and loss of sensitivity in batch analysis (due to variations in ionization process). Nonetheless, NMR lipoprotein analysis and MS-based lipidome profiling are rather complimentary (Emwas et al. 2019) and when combined may provide a powerful tool to discover new lipid markers and biological pathways relevant to TRL metabolism in a cost-effective manner. Such combined approach in large-scale studies would be ideally initiated by an NMR screening of all samples to identify divergent groups of patients, followed by a comprehensive and quantitative analysis by MS in a limited number of interesting and extreme samples. However, to advance into integrative approaches between lipidomics and other applied analytical methods (e.g., NMR or genomics), further improvements are still required, particularly concerning the standardization of methods for reporting quantitative and reproducible data (Bowden et al. 2017; Burla et al. 2018; O’Donnell et al. 2020).
Applications to Other Diseases or Conditions
In this study we review the use TRL particle size to predict the risk of type 2 diabetes and the potential mechanisms associated to this link. In summary, risk prediction of T2DM in primary prevention could be improved by using TRL particle size particularly among individuals with no abnormalities in glucose metabolism at baseline. Nonetheless, there are other potential applications for this biomarker. Of note, TRL particle size is also linked to the risk of myocardial infarction and peripheral artery disease ( Duran et al. 2020 ), and play a major role in atherogenesis and chronic coronary artery disease ( Twickler et al. 2004 ). Furthermore, the robust associations found between TRL particle size and the risk of type 2 diabetes offer a new perspective for the development of targeted interventions aiming to reduce TRL particle diameter and TG content per particle to control metabolic diseases.
Mini-Dictionary of Terms
-
Type 2 diabetes A chronic condition that affects the way the body processes blood sugar, due to both peripheral resistance to insulin action and dysfunctional production of insulin by pancreatic beta cells.
-
VLDL Very low-density lipoprotein is produced in the liver and released into the bloodstream to supply body tissues with triglycerides.
-
Genetic polymorphism. Defined as the inheritance of a trait controlled by a single genetic locus with two alleles, in which the least common allele has a frequency of about 1% or greater. Genetic polymorphism is a mutation in DNA sequence among individuals, groups, or populations.
-
GWAS A genome-wide association study is an observational study of a genome-wide set of genetic variants in different individuals to see if any variant is associated with a trait/condition.
-
1 H-NMR spectroscopy Proton NMR is a powerful tool for molecular structure characterization.
Key Facts of Type 2 Diabetes and Hypertriglyceridemia
In the last 20 years, the number of adults diagnosed with diabetes has more than doubled as the world population has aged and become more overweight or obese
Diabetes is the 7 th leading cause of death in the United States
At least 60% of individuals with type 2 diabetes show hypertriglyceridemia and other types dyslipidemia
Lipoproteins such as HDL-C, LDL-C and VLDL-C are implicated as risk factors for type 2 diabetes
Increased lipid content in pancreatic beta cells may induce lipotoxicity and apoptosis, leading to insulin secretory dysfunction.
Summary Points
-
TRL particle size and VLDL-triglyceride content have been implicated in the risk of type 2 diabetes
-
Particularly a shift to larger VLDL particles ( VLDL1 ) can improve risk prediction of type 2 diabetes
-
Obesity, insulin resistance, and systemic inflammation play a role in increasing hepatic fat content and upregulating TRL particle size
-
Genetic polymorphisms could explain both increased TRL particle size and the risk of type 2 diabetes
-
Data from mass spectrometry studies suggest TG species characterizing cases of incident T2DM might be linked to TRL levels
Abbreviations
- ANGPTL3:
-
Anti-angiopoietin-like protein 3
- ApoAV:
-
Apolipoprotein AV
- ApoC3:
-
Apolipoprotein C3
- AUROC:
-
Area under the receiver-operating characteristic curve
- CV:
-
Cardiovascular
- CVD:
-
Cardiovascular disease
- DGAT1:
-
Diacylglycerol O-Acyltransferase 1
- ELSA-Brasil:
-
Adult Health Logitudinal Study (Estudo Longitudinal de Saúde do Adulto) - Brazil
- EPA:
-
Eicosapentaenoic acid
- Gpihbp1:
-
Glycosylphosphatidylinositol-anchored HDL binding protein-1
- GWAS:
-
Genome-wide association studies
- HbA1c:
-
Glycosylated hemoglobin
- HDL:
-
High-density lipoprotein
- HDL-C:
-
High-density lipoprotein cholesterol
- HOMA-IR:
-
Homeostasis model assessment for insulin resistance
- LDL:
-
Low-density lipoprotein
- LDL:
-
Low-density lipoprotein cholesterol
- LPL:
-
Lipoprotein lipase
- MTP:
-
Microsomal triglyceride transfer protein
- NMR:
-
Nuclear magnetic resonance
- SNP:
-
Single nucleotide polymorphism
- Srebp-1c:
-
Sterol regulatory element-binding protein 1c
- T2DM:
-
Type 2 diabetes mellitus
- TG:
-
Triacylglycerol
- TRL:
-
Triacylglycerol-enriched remnant lipoproteins (TRL)
- TNFα:
-
Tumor necrose factor α
- VLDL:
-
Very low-density lipoprotein
References
Abdul-Ghani MA, DeFronzo RA. Plasma glucose concentration and prediction of future risk of type 2 diabetes. Diabetes Care. 2009;32:5.
Adiels M, Taskinen MR, Bjornson E, Andersson L, Matikainen N, Soderlund S, Kahri J, Hakkarainen A, Lundbom N, Sihlbom C, Thorsell A, Zhou H, Pietilainen KH, Packard C, Boren J. Role of apolipoprotein C-III overproduction in diabetic dyslipidaemia. Diabetes Obes Metab. 2019;21:1861–70.
Akash MSH, Rehman K, Liaqat A. Tumor necrosis factor-alpha: role in development of insulin resistance and pathogenesis of type 2 diabetes mellitus. J Cell Biochem. 2018;119:105–10.
Andersen MK, Pedersen CE, Moltke I, Hansen T, Albrechtsen A, Grarup N. Genetics of type 2 diabetes: the power of isolated populations. Curr Diab Rep. 2016;16:65.
Billings LK, Florez JC. The genetics of type 2 diabetes: what have we learned from GWAS? Ann N Y Acad Sci. 2010;1212:59–77.
Boren J, Watts GF, Adiels M, Soderlund S, Chan DC, Hakkarainen A, Lundbom N, Matikainen N, Kahri J, Verges B, Barrett PH, Taskinen MR. Kinetic and related determinants of plasma triglyceride concentration in abdominal obesity: Multicenter Tracer Kinetic Study. Arterioscler Thromb Vasc Biol. 2015;35:2218–24.
Boren J, Packard CJ, Taskinen MR. The roles of ApoC-III on the metabolism of Triglyceride-Rich lipoproteins in humans. Front Endocrinol (Lausanne). 2020;11:474.
Borst SE, Bagby GJ. Neutralization of tumor necrosis factor reverses age-induced impairment of insulin responsiveness in skeletal muscle of Sprague-Dawley rats. Metabolism. 2002;51:1061–4.
Bowden JA, Heckert A, Ulmer CZ, Jones CM, Koelmel JP, Abdullah L, Ahonen L, Alnouti Y, Armando AM, Asara JM, Bamba T, Barr JR, Bergquist J, Borchers CH, Brandsma J, Breitkopf SB, Cajka T, Cazenave-Gassiot A, Checa A, Cinel MA, Colas RA, Cremers S, Dennis EA, Evans JE, Fauland A, Fiehn O, Gardner MS, Garrett TJ, Gotlinger KH, Han J, Huang Y, Neo AH, Hyotylainen T, Izumi Y, Jiang H, Jiang H, Jiang J, Kachman M, Kiyonami R, Klavins K, Klose C, Kofeler HC, Kolmert J, Koal T, Koster G, Kuklenyik Z, Kurland IJ, Leadley M, Lin K, Maddipati KR, McDougall D, Meikle PJ, Mellett NA, Monnin C, Moseley MA, Nandakumar R, Oresic M, Patterson R, Peake D, Pierce JS, Post M, Postle AD, Pugh R, Qiu Y, Quehenberger O, Ramrup P, Rees J, Rembiesa B, Reynaud D, Roth MR, Sales S, Schuhmann K, Schwartzman ML, Serhan CN, Shevchenko A, Somerville SE, St John-Williams L, Surma MA, Takeda H, Thakare R, Thompson JW, Torta F, Triebl A, Trotzmuller M, Ubhayasekera SJK, Vuckovic D, Weir JM, Welti R, Wenk MR, Wheelock CE, Yao L, Yuan M, Zhao XH, Zhou S. Harmonizing lipidomics: NIST interlaboratory comparison exercise for lipidomics using SRM 1950-Metabolites in Frozen Human Plasma. J Lipid Res. 2017;58:2275–88.
Browning JD, Horton JD. Molecular mediators of hepatic steatosis and liver injury. J Clin Invest. 2004;114:147–52.
Burla B, Arita M, Arita M, Bendt AK, Cazenave-Gassiot A, Dennis EA, Ekroos K, Han X, Ikeda K, Liebisch G, Lin MK, Loh TP, Meikle PJ, Oresic M, Quehenberger O, Shevchenko A, Torta F, Wakelam MJO, Wheelock CE, Wenk MR. MS-based lipidomics of human blood plasma: a community-initiated position paper to develop accepted guidelines. J Lipid Res. 2018;59:2001–17.
Carvalho LSF, Bensenor IM, Nogueira ACC, Duncan BB, Schmidt MI, Blaha MJ, Toth PP, Jones SR, Santos RD, Lotufo PA, Sposito AC, ELSA-Brasil study. Increased particle size of triacylglycerol-enriched remnant lipoproteins, but not their plasma concentration or lipid content, augments risk prediction of incident type 2 diabetes. Diabetologia. 2021;64:385–96.
Chapman MJ, Ginsberg HN, Amarenco P, Andreotti F, Boren J, Catapano AL, Descamps OS, Fisher E, Kovanen PT, Kuivenhoven JA, Lesnik P, Masana L, Nordestgaard BG, Ray KK, Reiner Z, Taskinen MR, Tokgozoglu L, Tybjaerg-Hansen A, Watts GF, Panel European Atherosclerosis Society Consensus. Triglyceride-rich lipoproteins and high-density lipoprotein cholesterol in patients at high risk of cardiovascular disease: evidence and guidance for management. Eur Heart J. 2011;32:1345–61.
Cohn JS, Marcoux C, Davignon J. Detection, quantification, and characterization of potentially atherogenic triglyceride-rich remnant lipoproteins. Arterioscler Thromb Vasc Biol. 1999;19:2474–86.
Consortium, Sigma Type 2 Diabetes, Williams AL, Jacobs SB, Moreno-Macias H, Huerta-Chagoya A, Churchhouse C, Marquez-Luna C, Garcia-Ortiz H, Gomez-Vazquez MJ, Burtt NP, Aguilar-Salinas CA, Gonzalez-Villalpando C, Florez JC, Orozco L, Haiman CA, Tusie-Luna T, Altshuler D. Sequence variants in SLC16A11 are a common risk factor for type 2 diabetes in Mexico. Nature. 2014;506:97–101.
Czech MP, Tencerova M, Pedersen DJ, Aouadi M. Insulin signalling mechanisms for triacylglycerol storage. Diabetologia. 2013;56:949–64.
Duran EK, Aday AW, Cook NR, Buring JE, Ridker PM, Pradhan AD. Triglyceride-Rich lipoprotein cholesterol, small dense LDL cholesterol, and incident cardiovascular disease. J Am Coll Cardiol. 2020;75:2122–35.
Emwas AH, Roy R, McKay RT, Tenori L, Saccenti E, Gowda GAN, Raftery D, Alahmari F, Jaremko L, Jaremko M, Wishart DS. NMR spectroscopy for metabolomics research. Metabolites. 2019;9:123.
Fernandez C, Surma MA, Klose C, Gerl MJ, Ottosson F, Ericson U, Oskolkov N, Ohro-Melander M, Simons K, Melander O. Plasma lipidome and prediction of type 2 diabetes in the population-based Malmo Diet and Cancer Cohort. Diabetes Care. 2020;43:366–73.
Group, Hps Thrive Collaborative, Landray MJ, Haynes R, Hopewell JC, Parish S, Aung T, Tomson J, Wallendszus K, Craig M, Jiang L, Collins R, Armitage J. Effects of extended-release niacin with laropiprant in high-risk patients. N Engl J Med. 2014;371:203–12.
Hao M, Head WS, Gunawardana SC, Hasty AH, Piston DW. Direct effect of cholesterol on insulin secretion: a novel mechanism for pancreatic beta-cell dysfunction. Diabetes. 2007;56:2328–38.
Hubacek JA. Apolipoprotein A5 fifteen years anniversary: lessons from genetic epidemiology. Gene. 2016;592:193–9.
Investigators, Aim-High, Boden WE, Probstfield JL, Anderson T, Chaitman BR, Desvignes-Nickens P, Koprowicz K, McBride R, Teo K, Weintraub W. Niacin in patients with low HDL cholesterol levels receiving intensive statin therapy. N Engl J Med. 2011;365:2255–67.
Korte A, Farlow A. The advantages and limitations of trait analysis with GWAS: a review. Plant Methods. 2013;9:29.
Kulkarni H, Mamtani M, Wong G, Weir JM, Barlow CK, Dyer TD, Almasy L, Mahaney MC, Comuzzie AG, Duggirala R, Meikle PJ, Blangero J, Curran JE. Genetic correlation of the plasma lipidome with type 2 diabetes, prediabetes and insulin resistance in Mexican American families. BMC Genet. 2017;18:48.
Lim EL, Hollingsworth KG, Aribisala BS, Chen MJ, Mathers JC, Taylor R. Reversal of type 2 diabetes: normalisation of beta cell function in association with decreased pancreas and liver triacylglycerol. Diabetologia. 2011;54:2506–14.
Lu J, Lam SM, Wan Q, Shi L, Huo Y, Chen L, Tang X, Li B, Wu X, Peng K, Li M, Wang S, Xu Y, Xu M, Bi Y, Ning G, Shui G, Wang W. High-coverage targeted lipidomics reveals novel serum lipid predictors and lipid pathway dysregulation antecedent to type 2 diabetes onset in normoglycemic Chinese adults. Diabetes Care. 2019;42:2117–26.
Mahajan A, Taliun D, Thurner M, Robertson NR, Torres JM, Rayner NW, Payne AJ, Steinthorsdottir V, Scott RA, Grarup N, Cook JP, Schmidt EM, Wuttke M, Sarnowski C, Magi R, Nano J, Gieger C, Trompet S, Lecoeur C, Preuss MH, Prins BP, Guo X, Bielak LF, Below JE, Bowden DW, Chambers JC, Kim YJ, Ng MCY, Petty LE, Sim X, Zhang W, Bennett AJ, Bork-Jensen J, Brummett CM, Canouil M, Ec Kardt KU, Fischer K, Kardia SLR, Kronenberg F, Lall K, Liu CT, Locke AE, Luan J, Ntalla I, Nylander V, Schonherr S, Schurmann C, Yengo L, Bottinger EP, Brandslund I, Christensen C, Dedoussis G, Florez JC, Ford I, Franco OH, Frayling TM, Giedraitis V, Hackinger S, Hattersley AT, Herder C, Ikram MA, Ingelsson M, Jorgensen ME, Jorgensen T, Kriebel J, Kuusisto J, Ligthart S, Lindgren CM, Linneberg A, Lyssenko V, Mamakou V, Meitinger T, Mohlke KL, Morris AD, Nadkarni G, Pankow JS, Peters A, Sattar N, Stancakova A, Strauch K, Taylor KD, Thorand B, Thorleifsson G, Thorsteinsdottir U, Tuomilehto J, Witte DR, Dupuis J, Peyser PA, Zeggini E, Loos RJF, Froguel P, Ingelsson E, Lind L, Groop L, Laakso M, Collins FS, Jukema JW, Palmer CNA, Grallert H, Metspalu A, Dehghan A, Kottgen A, Abecasis GR, Meigs JB, Rotter JI, Marchini J, Pedersen O, Hansen T, Langenberg C, Wareham NJ, Stefansson K, Gloyn AL, Morris AP, Boehnke M, McCarthy MI. Fine-mapping type 2 diabetes loci to single-variant resolution using high-density imputation and islet-specific epigenome maps. Nat Genet. 2018;50:1505–13.
Martin-Rodriguez JL, Gonzalez-Cantero J, Gonzalez-Cantero A, Marti-Bonmati L, Alberich-Bayarri A, Gonzalez-Cejudo T, Gonzalez-Calvin JL. Insulin resistance and NAFLD: relationship with intrahepatic iron and serum TNF-alpha using 1H MR spectroscopy and MRI. Diabetes Metab. 2019;45:473–9.
O’Donnell VB, Murphy RC, Watson SP. Platelet lipidomics: modern day perspective on lipid discovery and characterization in platelets. Circ Res. 2014;114:1185–203.
O’Donnell VB, Ekroos K, Liebisch G, Wakelam M. Lipidomics: current state of the art in a fast moving field. Wiley Interdiscip Rev Syst Biol Med. 2020;12:e1466.
Oh YS, Bae GD, Baek DJ, Park EY, Jun HS. Fatty acid-induced lipotoxicity in pancreatic beta-cells during development of type 2 diabetes. Front Endocrinol (Lausanne). 2018;9:384.
Pyorala K, De Backer G, Graham I, Poole-Wilson P, Wood D. Prevention of coronary heart disease in clinical practice: recommendations of the Task Force of the European Society of Cardiology, European Atherosclerosis Society and European Society of Hypertension. Atherosclerosis. 1994;110:121–61.
Qi Q, Liang L, Doria A, Hu FB, Qi L. Genetic predisposition to dyslipidemia and type 2 diabetes risk in two prospective cohorts. Diabetes. 2012;61:745–52.
Qin B, Qiu W, Avramoglu RK, Adeli K. Tumor necrosis factor-alpha induces intestinal insulin resistance and stimulates the overproduction of intestinal apolipoprotein B48-containing lipoproteins. Diabetes. 2007;56:450–61.
Quehenberger O, Armando AM, Brown AH, Milne SB, Myers DS, Merrill AH, Bandyopadhyay S, Jones KN, Kelly S, Shaner RL, Sullards CM, Wang E, Murphy RC, Barkley RM, Leiker TJ, Raetz CR, Guan Z, Laird GM, Six DA, Russell DW, McDonald JG, Subramaniam S, Fahy E, Dennis EA. Lipidomics reveals a remarkable diversity of lipids in human plasma. J Lipid Res. 2010;51:3299–305.
Quehenberger O, Armando AM, Dennis EA. High sensitivity quantitative lipidomics analysis of fatty acids in biological samples by gas chromatography-mass spectrometry. Biochim Biophys Acta. 2011;1811:648–56.
Razquin C, Toledo E, Clish CB, Ruiz-Canela M, Dennis C, Corella D, Papandreou C, Ros E, Estruch R, Guasch-Ferre M, Gomez-Gracia E, Fito M, Yu E, Lapetra J, Wang D, Romaguera D, Liang L, Alonso-Gomez A, Deik A, Bullo M, Serra-Majem L, Salas-Salvado J, Hu FB, Martinez-Gonzalez MA. Plasma lipidomic profiling and risk of type 2 diabetes in the PREDIMED Trial. Diabetes Care. 2018;41:2617–24.
Rhee EP, Cheng S, Larson MG, Walford GA, Lewis GD, McCabe E, Yang E, Farrell L, Fox CS, O’Donnell CJ, Carr SA, Vasan RS, Florez JC, Clish CB, Wang TJ, Gerszten RE. Lipid profiling identifies a triacylglycerol signature of insulin resistance and improves diabetes prediction in humans. J Clin Invest. 2011;121:1402–11.
Rich SS. Mapping genes in diabetes. Genetic epidemiological perspective. Diabetes. 1990;39:1315–9.
Richter B, Hemmingsen B, Metzendorf MI, Takwoingi Y. Development of type 2 diabetes mellitus in people with intermediate hyperglycaemia. Cochrane Database Syst Rev. 2018;10:CD012661.
Robertson RP, Harmon J, Tran PO, Poitout V. Beta-cell glucose toxicity, lipotoxicity, and chronic oxidative stress in type 2 diabetes. Diabetes. 2004;53(Suppl 1):S119–24.
Schaap FG, Rensen PC, Voshol PJ, Vrins C, van der Vliet HN, Chamuleau RA, Havekes LM, Groen AK, van Dijk KW. ApoAV reduces plasma triglycerides by inhibiting very low density lipoprotein-triglyceride (VLDL-TG) production and stimulating lipoprotein lipase-mediated VLDL-TG hydrolysis. J Biol Chem. 2004;279:27941–7.
Stegemann C, Pechlaner R, Willeit P, Langley SR, Mangino M, Mayr U, Menni C, Moayyeri A, Santer P, Rungger G, Spector TD, Willeit J, Kiechl S, Mayr M. Lipidomics profiling and risk of cardiovascular disease in the prospective population-based Bruneck study. Circulation. 2014;129:1821–31.
Steven S, Hollingsworth KG, Small PK, Woodcock SA, Pucci A, Aribisala B, Al-Mrabeh A, Daly AK, Batterham RL, Taylor R. Weight loss decreases excess pancreatic triacylglycerol specifically in type 2 diabetes. Diabetes Care. 2016;39:158–65.
Suvitaival T, Bondia-Pons I, Yetukuri L, Poho P, Nolan JJ, Hyotylainen T, Kuusisto J, Oresic M. Lipidome as a predictive tool in progression to type 2 diabetes in Finnish men. Metabolism. 2018;78:1–12.
Teslovich TM, Musunuru K, Smith AV, Edmondson AC, Stylianou IM, Koseki M, Pirruccello JP, Ripatti S, Chasman DI, Willer CJ, Johansen CT, Fouchier SW, Isaacs A, Peloso GM, Barbalic M, Ricketts SL, Bis JC, Aulchenko YS, Thorleifsson G, Feitosa MF, Chambers J, Orho-Melander M, Melander O, Johnson T, Li X, Guo X, Li M, Shin Cho Y, Jin Go M, Jin Kim Y, Lee JY, Park T, Kim K, Sim X, Twee-Hee Ong R, Croteau-Chonka DC, Lange LA, Smith JD, Song K, Hua Zhao J, Yuan X, Luan J, Lamina C, Ziegler A, Zhang W, Zee RY, Wright AF, Witteman JC, Wilson JF, Willemsen G, Wichmann HE, Whitfield JB, Waterworth DM, Wareham NJ, Waeber G, Vollenweider P, Voight BF, Vitart V, Uitterlinden AG, Uda M, Tuomilehto J, Thompson JR, Tanaka T, Surakka I, Stringham HM, Spector TD, Soranzo N, Smit JH, Sinisalo J, Silander K, Sijbrands EJ, Scuteri A, Scott J, Schlessinger D, Sanna S, Salomaa V, Saharinen J, Sabatti C, Ruokonen A, Rudan I, Rose LM, Roberts R, Rieder M, Psaty BM, Pramstaller PP, Pichler I, Perola M, Penninx BW, Pedersen NL, Pattaro C, Parker AN, Pare G, Oostra BA, O’Donnell CJ, Nieminen MS, Nickerson DA, Montgomery GW, Meitinger T, McPherson R, McCarthy MI, McArdle W, Masson D, Martin NG, Marroni F, Mangino M, Magnusson PK, Lucas G, Luben R, Loos RJ, Lokki ML, Lettre G, Langenberg C, Launer LJ, Lakatta EG, Laaksonen R, Kyvik KO, Kronenberg F, Konig IR, Khaw KT, Kaprio J, Kaplan LM, Johansson A, Jarvelin MR, Janssens AC, Ingelsson E, Igl W, Kees Hovingh G, Hottenga JJ, Hofman A, Hicks AA, Hengstenberg C, Heid IM, Hayward C, Havulinna AS, Hastie ND, Harris TB, Haritunians T, Hall AS, Gyllensten U, Guiducci C, Groop LC, Gonzalez E, Gieger C, Freimer NB, Ferrucci L, Erdmann J, Elliott P, Ejebe KG, Doring A, Dominiczak AF, Demissie S, Deloukas P, de Geus EJ, de Faire U, Crawford G, Collins FS, Chen YD, Caulfield MJ, Campbell H, Burtt NP, Bonnycastle LL, Boomsma DI, Boekholdt SM, Bergman RN, Barroso I, Bandinelli S, Ballantyne CM, Assimes TL, Quertermous T, Altshuler D, Seielstad M, Wong TY, Tai ES, Feranil AB, Kuzawa CW, Adair LS, Taylor HA Jr, Borecki IB, Gabriel SB, Wilson JG, Holm H, Thorsteinsdottir U, Gudnason V, Krauss RM, Mohlke KL, Ordovas JM, Munroe PB, Kooner JS, Tall AR, Hegele RA, Kastelein JJ, Schadt EE, Rotter JI, Boerwinkle E, Strachan DP, Mooser V, Stefansson K, Reilly MP, Samani NJ, Schunkert H, Cupples LA, Sandhu MS, Ridker PM, Rader DJ, van Duijn CM, Peltonen L, Abecasis GR, Boehnke M, Kathiresan S. Biological, clinical and population relevance of 95 loci for blood lipids. Nature. 2010;466:707–13.
Torres JM, Gamazon ER, Parra EJ, Below JE, Valladares-Salgado A, Wacher N, Cruz M, Hanis CL, Cox NJ. Cross-tissue and tissue-specific eQTLs: partitioning the heritability of a complex trait. Am J Hum Genet. 2014;95:521–34.
Triglyceride Coronary Disease Genetics, Consortium, Collaboration Emerging Risk Factors, Sarwar N, Sandhu MS, Ricketts SL, Butterworth AS, Di Angelantonio E, Boekholdt SM, Ouwehand W, Watkins H, Samani NJ, Saleheen D, Lawlor D, Reilly MP, Hingorani AD, Talmud PJ, Danesh J. Triglyceride-mediated pathways and coronary disease: collaborative analysis of 101 studies. Lancet. 2010;375:1634–9.
Twickler TB, Dallinga-Thie GM, Cohn JS, Chapman MJ. Elevated remnant-like particle cholesterol concentration: a characteristic feature of the atherogenic lipoprotein phenotype. Circulation. 2004;109:1918–25.
Tzanavari T, Giannogonas P, Karalis KP. TNF-alpha and obesity. Curr Dir Autoimmun. 2010;11:145–56.
Valladolid-Acebes I, Berggren PO, Juntti-Berggren L. Apolipoprotein CIII Is an important piece in the type-1 diabetes Jigsaw Puzzle. Int J Mol Sci. 2021;22.
Varga TV, Liu J, Goldberg RB, Chen G, Dagogo-Jack S, Lorenzo C, Mather KJ, Pi-Sunyer X, Brunak S, Temprosa M, Group Diabetes Prevention Program Research. Predictive utilities of lipid traits, lipoprotein subfractions and other risk factors for incident diabetes: a machine learning approach in the Diabetes Prevention Program. BMJ Open Diabetes Res Care. 2021;9.
Zhang Y, He W, He C, Wan J, Lin X, Zheng X, Li L, Li X, Yang X, Yu B, Xian X, Zhu Y, Wang Y, Liu G, Lu N. Large triglyceride-rich lipoproteins in hypertriglyceridemia are associated with the severity of acute pancreatitis in experimental mice. Cell Death Dis. 2019;10:728.
Zilversmit DB. Atherogenesis: a postprandial phenomenon. Circulation. 1979;60:473–85.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 Springer Nature Switzerland AG
About this entry
Cite this entry
de Carvalho, L.S.F., Asari, A.I.A., de Sousa Teles, B.S.B., de Britto Chaves Filho, A., Yoshinaga, M.Y. (2023). Biomarkers in Disease: Diabetes Methods, Discoveries, and Applications. In: Patel, V.B., Preedy, V.R. (eds) Biomarkers in Diabetes. Biomarkers in Disease: Methods, Discoveries and Applications. Springer, Cham. https://doi.org/10.1007/978-3-031-08014-2_20
Download citation
DOI: https://doi.org/10.1007/978-3-031-08014-2_20
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-08013-5
Online ISBN: 978-3-031-08014-2
eBook Packages: Biomedical and Life SciencesReference Module Biomedical and Life Sciences