Abstract
Malignant tumors frequently exploit innate immunity to evade immune surveillance. The priming, function, and polarization of antitumor immunity fundamentally depends upon context provided by the innate immune system, particularly antigen presenting cells. Such context is determined in large part by sensing of pathogen specific and damage associated features by pathogen recognition receptors (PRRs). PRR activation induces the delivery of T cell priming cues (e.g. chemokines, co-stimulatory ligands, and cytokines) from antigen presenting cells, playing a decisive role in the cancer immunity cycle. Indeed, endogenous PRR activation within the tumor microenvironment (TME) has been shown to generate spontaneous antitumor T cell immunity, e.g., cGAS-STING mediated activation of antigen presenting cells after release of DNA from dying tumor cells. Thus, instigating intratumor PRR activation, particularly with the goal of generating Th1-promoting inflammation that stokes endogenous priming of antitumor CD8+ T cells, is a growing area of clinical investigation. This approach is analogous to in situ vaccination, ultimately providing a personalized antitumor response against relevant tumor associated antigens. Here I discuss clinical stage intratumor modalities that function via activation of PRRs. These approaches are being tested in various solid tumor contexts including melanoma, colorectal cancer, glioblastoma, head and neck squamous cell carcinoma, bladder cancer, and pancreatic cancer. Their mechanism (s) of action relative to other immunotherapy approaches (e.g., antigen-defined cancer vaccines, CAR T cells, dendritic cell vaccines, and immune checkpoint blockade), as well as their potential to complement these approaches are also discussed. Examples to be reviewed include TLR agonists, STING agonists, RIG-I agonists, and attenuated or engineered viruses and bacterium. I also review common key requirements for effective in situ immune activation, discuss differences between various strategies inclusive of mechanisms that may ultimately limit or preclude antitumor efficacy, and provide a summary of relevant clinical data.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Pattern recognition receptor
- TLR agonist
- Oncolytic virus
- Type-I IFN
- Innate immunotherapy
- In situ vaccination
- Intratumoral therapy
3.1 Pattern Recognition Receptors (PRRs) Induce Innate Inflammation
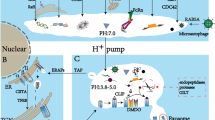
Pattern recognition receptors (PRRs) recognize rigid features known as pathogen associated molecular patterns (‘PAMPs’) or damage associated molecular patterns (‘DAMPs’) either in the extracellular space, endosome, or cytoplasm to induce appropriate inflammation during pathogen infection and/or tissue damage. Canonical PRRs include Toll-like Receptors (TLRs), of which there are 10 (TLRs 1-10) in humans; RIG-I like receptors (RLRs) including MDA5 and RIG-I; cytosolic double stranded DNA sensors (e.g., cGAS-STING); the AIM2-like receptors; the NOD-like receptors; and C-type lectin receptors. For information on PRRs, their locations, and specificities, see Fig. 3.1. Upon recognition of PAMPs or DAMPs by PRRs, signaling to the Tank Binding Kinase 1 (TBK1) and IKK-α/β kinases primarily lead to IRF3 phosphorylation and NFκB activation, respectively [1, 2], to concertedly lead to the synthesis of pro-inflammatory cytokines (e.g., type I IFNs, TNF, IL-6) and, in DCs, induce co-stimulatory ligand expression (e.g. CD86, CD80).
PRR cellular locations, specificities, and downstream signaling. Yellow indicates PRRs, blue indicates signaling adapters/kinases, and red indicates transcription factors that mediate transcription of inflammatory genes. PAMPs that activate PRRs are depicted in italicized red text. Toll-like Receptors 1, 2 and 4–6 are located on the cell surface and recognize bacterial features such as lipids, proteins, and lipoproteins. TLRs 3 and 7–9 are localized to endosomes, and recognize viral nucleic acids. TLR4 is both extracellular and endosomal. The specificity and function of TLR10 (not shown) is currently obscure, but in contrast to other TLRs, may negatively regulate inflammation [3]. The RIG-I like receptors, RIG-I and MDA5, recognize cytosolic viral double stranded (ds) RNA and have recently been shown to become activated at endoplasmic reticulum (ER) derived microsomes [4]. Cytosolic DNA sensing by cGAS-STING is mediated at the ER. The AIM2 inflammasome recognizes dsDNA in the cytosol to initiate cleavage of caspase-1, followed by cleavage of pro-IL-1β and pro-IL-18 to their mature, secreted state. The NLRP3 inflammasome (a NOD like receptor) recognizes various DAMP and PAMP features, including viral dsRNA and single stranded RNA, and similarly leads to caspase-1 activation. Several variations of inflammasomes recognizing diverse features are not shown. The C-type lectin receptors Dectin-1 and 2 recognize bacterial and fungal features; several additional C-type lectins with various specificities are not shown. The transcription factors IRF3 and IRF7 largely drive transcription of type I interferons (IFNs) while NFkB and AP-1 induce other pro-inflammatory cyotkines. The activated transcription factors also induce co-stimulatory ligand expression, as well as anti-viral/anti-bacterial gene products
3.2 PRR Signaling Dictates CD8+ T Cell Priming, Recruitment, and Function During Viral Infection
Leveraging antitumor functions of CD8+ T cells to eliminate malignant cells in an antigen-specific manner is the goal of most cancer immunotherapy strategies. In a natural infectious setting, CD8+ T cells are enlisted to eliminate intracellular pathogens, e.g., viruses. Provided below, and depicted in Fig. 3.2, is an example of how a typical acute viral infection leads to priming of antiviral CD8+ T cells via the activation of PRRs. The concepts of antiviral CD8+ T cell priming and effector functions during an infectious process are analogous to events that must occur to enable priming and effector function of antitumor CD8+ T cells.
-
Step 1: Viral infection of epithelium occurs (Fig 3.2a).
-
Step 2: Local inflammation is induced after recognition of viral features (e.g. viral nucleic acids) by PRRs expressed on tissue resident macrophages, infected epithelium, or by other tissue resident innate immune populations (Fig 3.2b).
-
Step 3: PRR mediated inflammatory signals leads to surface expression of adhesion molecules on the local endothelium (Fig 3.2c).
-
Step 4: The induction of adhesion molecules on endothelium in concert with chemokines/cytokines facilitates recruitment of additional innate immune cells (Fig. 3.2d). Much of the innate inflammation at this stage functions to limit viral replication and spread, and may lead to killing of infected cells by innate immune populations including NK cells, neutrophils, and macrophages. In addition, during this process conventional DCs consume antigens in the infected site, while receiving activating signals from inflammatory cytokines from infected cells and/or direct PRR signaling (Fig 3.2d) that induces their ‘activation’—which includes the induction of co-stimulatory signals.
-
Step 5: Antigen-bearing DCs then migrate to the draining lymph node or other lymphatic organ to prime and expand populations of CD8+ T cells recognizing viral antigen from the infection site (Fig 3.2e).
-
Step 6: Activated CD8+ T cells chemotract to recognize and kill remaining infected cells, and inflammation from the infection induces antigen presentation machinery and stress signals in infected cells that further enable T cell mediated killing. A pool of memory T cells persist after the infection is cleared for future pathogen recognition and elimination (Fig 3.2f).
Notably variations in the routes by which these steps occur are pathogen and tissue specific; alternate modes of CD8+ T cell priming have been demonstrated, e.g. via antigen transfer between migratory vs lymph node resident DCs [5, 6]; and other mechanisms of antigen transfer at sites distant from the infection may occur [7]. These processes, originally defined in the context of natural viral infection [8], have been shown to largely apply to immune surveillance, that is, the recognition and elimination of malignant cells by the immune system.
3.3 The Cancer Immunity Cycle and PRR Signaling
The host immune system recognizes malignant cells on the basis of protein coding genetic mutations; abnormal post-translational modifications; aberrantly expressed proteins (e.g., cancer-testis antigens); and in some cancer types, oncogenic viral proteins. Recognition of such antigens is mediated by cell surface MHC class I for CD8+ T cells, and surface MHC class II for CD4+ T cells, with CD8+ T cells typically being the primary antitumor effectors during immune surveillance. While co-evolution between malignant cells and the host immune system eliminates immunogenic malignant cells and results in outgrowth of ‘immunoedited’ tumors that are less immunogenic [9], and heterogeneity in the expression of tumor associated antigens is common [10], the success of immune checkpoint blockade in several tumor types implies that other potentially reversable regulatory nodes prevent immune recognition and destruction of solid tumors.
The cancer immunity cycle outlines established steps by which antitumor T cells can become activated endogenously to eliminate malignant cells [11] (Fig. 3.3). Dying cancer cells release antigens that are taken up by dendritic cells (DCs) to be loaded on to MHC-class I or II. Tumor antigen presenting DCs present antigen along with co-stimulatory signals to T cells, typically within the tumor draining lymph node. If the appropriate co-stimulatory signals along with cognate antigen are delivered to tumor antigen-specific T cells at this step, activated tumor-specific T cells may traffic to the tumor site, recognize tumor antigen-expressing malignant cells, and mediate killing of malignant cells through several mechanisms. The cytotoxic mechanisms of T cells include the release of perforin and granzymes, apoptotic signals (FAS-ligand), cytokines that mediate apoptotic signaling, e.g., TNF, as well as cytokines that induce upregulation of MHC class I and antigen processing machinery in tumor cells, particularly IFN-γ.

adapted from Chen and Mellman Immunity 2013 [11] with permission. Red boxes denote mechanisms by which PRR signaling impacts cancer immune surveillance. (1) Cancer cells routinely die due to genotoxic stress, chemo/radiation, nutrient deprivation, hypoxia, and other reasons; leading to the release of tumor antigens. (2) Migrating antigen presenting cells, including migratory conventional dendritic cells capable of cross presenting antigens to CD8+ T cells (see Fig. 3.4), take up antigen in the tumor microenvironment to be processed and presented on MHC-class I or II. PRRs potentiate this step by increasing antigen presentation on DCs, increasing antigen uptake (e.g. via calreticulin and HSP surface expression on apoptotic cells) and potentially recruiting additional migratory DCs into tumors. (3) Within the draining lymph node or other secondary lymphoid organ, tumor antigen loaded DCs present antigen to T cells, leading to their activation. PRR signaling induces the expression of co-stimulatory signals on DCs to potentiate T cell priming; see Fig. 3.4 for detailed explanation. (4) T cells traffic to the site of the tumor by surveying endothelial ligand (e.g. ICAM-1 and VCAM-1) expression and chemokine signals, and (5) infiltrate the tumor tissue. PRRs enhance endothelial cell T cell adhesion ligand expression and chemokine secretion from the tumor site to facilitate T cell infiltration. (6) T cells recognize cognate tumor antigen presented on tumor cells; PRRs facilitate this process by inducing inflammation that causes induction of antigen presentation machinery in cancer cells. (7) T cells kill cancer cells expressing their cognate antigen via granzymes and perforin, FAS ligand, and secretion of cytotoxic cytokines; PRRs induce inflammation that enhances antitumor T cell function and cytotoxicity
PRR signaling supports the cancer immunity cycle through multiple mechanisms,
However, several factors determine whether tumor-specific T cells will ultimately become tolerized and anergic after DC mediated antigen presentation, whether sufficient signals enable trafficking of tumor-reactive T cells to the tumor site, as well as whether antitumor T cells can function within the immune subversive tumor microenvironment (TME). These issues are dictated by that status of the innate immune system during the cancer immunity cycle, including that of DCs and tumor associated macrophages/myeloid derived suppressor cells (MDSCs). PRRs play a multifaceted role in determining the pace, and efficacy of the cancer immunity lifecycle. PRR signaling enhances antigen presentation and co-stimulatory signals on antigen presenting cells (Fig. 3.4), culminating in more effective priming of tumor antigen-specific T cells. In addition, intratumor activation of PRRs induces chemokines that facilitate the recruitment of newly primed antitumor T cells, and further supports their function by enhancing tumor antigen presentation and an inflammatory milieu that potentiates T cell effector functions. For detailed explanation of the role of PRR signaling at each step of the cancer immunity cycle, see Fig. 3.3. Accordingly, an emerging clinical strategy aimed at rectifying stalled cancer immune lifecycles in patients is that of targeting the activation of PRRs within the TME to provoke the expression of: co-stimulatory signals on DCs during antigen presentation, T cell recruiting chemokines within the tumor site, and inflammation within the TME that supports antitumor CD8+ T cell function.
Dendritic cell (DC) activation is dictated by PPR signaling, which enables CD8+ T cell cross-priming. An example of cross presentation is shown, which occurs via loading of engulfed exogenous antigen onto MHC-class I for presentation to CD8+ T cells, typically by cDC1s (CD103+, BATF3+ in mice; CD141+ in humans). In the context of viral infection, PRRs expressed by viral antigen presenting DCs sense PAMPs and DAMPs at the site of inflammation/infection and receive signals from locally produced cytokines. These signals lead to upregulation of antigen processing and presentation machinery (signal 1), induction of co-stimulatory ligands including the CD28 ligands CD80 and CD86 (signal 2), and secretion of cytokines like IL-12 and type I IFNs that lead to further activation and differentiation of the cognate antigen-specific CD8+ T cell (signal 3). Upon receiving these signals, CD8+ T cells become activated and can traffic to the site of infection to eliminate virally infected cells. Similarly, during the cancer immunity cycle, migratory cDCs take up tumor associated antigens, traffic to the draining lymph node, and present exogenously acquired antigen on MHC-class I to T cells. As occurs during viral infection, PRR signaling bolsters the efficiency of tumor antigen uptake, processing, and presentation on MHC-class I on DCs (Signal 1); the induction of co-stimulatory ligands expressed on the DC surface (Signal 2); as well as the induction of pro-inflammatory cytokines required for optimal antitumor CD8+ T cell priming (Signal 3)
3.4 Endogenous Activation of PRRs in Cancer
Endogenous signals from cells that are stressed or dying necrotically can induce DC activation in the absence of foreign pathogen associated features [12]; lending explanation for how T cell priming and activation in the contexts of spontaneous antitumor immunity, transplantation rejection, and/or autoimmunity occurs. Recent work has documented the importance of several PRRs in the context of tumor biology that lead to DC activation, and generalized inflammation within tumors. These include the following PAMPs and DAMPs, which represent only a subset of relevant documented endogenous PRR ligands:
-
1.
Double stranded DNA (dsDNA) from dying tumor cells can be recognized by cGAS-STING, particularly within DCs that take up debris from dead tumor cells. STING signaling culminates in IFNβ/antiviral responses that mediates activation of systemic antitumor T cell immunity and tumor regression [13, 14].
-
2.
High-mobility-group box 1 (HMGB1) is a nuclear protein that is released during cell death, including after chemotherapy/radiation, to engage TLR4 on DCs [15].
-
3.
Cell surface calreticulin facilitates phagocytosis of apoptotic tumor cells by DCs and macrophages and determines the immunogenicity of phagocytosed cells [16,17,18].
-
4.
Heat Shock Proteins (HSPs) released from dying cancer cells are widely reported to bind to TLRs 2 and 4 to induce inflammation [19,20,21,22,23,24].
-
5.
Endogenous retroviruses have been shown to reactivate in some cancers presumably due to epigenetic dysregulation or loss of innate signaling in malignant cells [25], and can induce TLR and RLR signaling due to cytoplasmic presence of replicating retroviral RNA [26].
-
6.
Uric acid/monosodium urate crystals, a byproduct of purine metabolism that causes gout, have been shown to induce activation of the NLRP3 inflammasome [27], TLR2, and TLR4 [28]. Uric acid mediates DC activation [29].
-
7.
The tumor microbiome has recently been defined, demonstrating evidence of microbial presence (e.g., intracellular bacteria and viruses) in various tumor types at baseline [30, 31]. The presence of such microbes is likely to impact endogenous PRR signaling in tumors, though this remains to be determined.
Thus, PRRs in tumors are not inert, but rather may recognize features associated with cell death; tissue damage; and in some cases, endogenous pathogens. Collectively, their activity in cancer likely explains how spontaneous antitumor T cells are primed to eliminate malignant cells. In contrast, a lack of co-stimulation from DCs to antitumor T cells is frequent in cancer [32, 33], causing tolerance and suppression as opposed to activation. This contradiction may be due to insufficient PRR signals from endogenous PAMPs/DAMPs, tolerance/desensitization of PRR signaling due to chronic PAMP exposure, or other mechanisms of tumor mediated immune suppression. Thus, given their roles in orchestrating co-stimulatory signal expression in antigen presenting cells, targeting PRRs to induce inflammation compatible with T cell priming and co-stimulation is a therapeutically viable strategy to engage antitumor CD8+ T cell immunity.
3.5 Engaging PRRs for Cancer Immunotherapy
3.5.1 Inducing Innate Inflammation in Tumors: A Historical Perspective
The first widespread medical use of a PRR activator in cancer is that of Coley’s toxin [34, 35] in the late 1800s, though the use of pathogens for cancer therapy, as well as anecdotal correlations of pathogen infection and spontaneous tumor regression, was documented much earlier [34, 36, 37]. Based upon clinical case review of a patient that experienced sarcoma tumor regression after bacterial infection at the tumor site, William Coley tested if bacterial infection of sarcomas may mediate tumor regression in patients. After initially using live bacterium, Coley switched to inactivated bacterium; which caused regression in some patients. This cocktail of inactivated bacteria became known as ‘Coley’s toxins’, but the approach was ultimately overshadowed by advances in radiation therapy, and suffered from limitations in standardizing the treatment [34].
In the early 1900s Mycobacterium bovis was isolated from a cow with tuberculosis mastitis. Laboratory passaging in bovine bile (to prevent clumping) led to a loss of virulence, and the strain of M Bovis was named Bacillus of Calmette and Guerin (BCG) after the scientists that developed the strain [38]. Coincidentally, Tuberculosis infection was noted to be associated with a lower frequency of cancer [39], raising the possibility for using M bovis for cancer therapy. In 1969 the first report of BCG’s use as a cancer therapy was reported by Mathe et al.in the treatment of lymphoblastoid leukemia where encouraging results were reported [40]. The first clinical trial of BCG for bladder cancer was published in 1976 [41] where a decrease in recurrence of superficial bladder cancer was observed. These observations were confirmed in 1980 [42], spurring widespread use of BCG as a intravesicular therapy for bladder cancer. BCG was FDA approved for the treatment of bladder cancer in 1990, and represents the first approved cancer immunotherapy. BCG mediates innate inflammation that engages CD4+ and CD8+ T cells with several TLRs being shown to mediate the initial innate response, including TLRs 2, 4, and 9 [43]. The success of BCG, along with discoveries on the role of PRR signaling in mediating immune surveillance, led to further studies applying intratumor PRR activators for cancer immunotherapy in several cancer types.
3.5.2 Non-Infectious Engagers of PRRs for Cancer Immunotherapy
PRR activating PAMPs have shown preclinical promise in engaging systemic antitumor immunity. In addition, therapies that evoke PRR signaling through indirect means are also being explored. Clinically tested approaches to engage immune surveillance through targeted PRR activation using non-replicating, non-infectious PAMPs are described below according to their PRR specificities.
3.5.2.1 TLR Agonists
The toll like receptors were first discovered in Drosophila, and later confirmed to induce innate inflammation in mammalian systems [8]. TLR signaling culminates in activation of TBK1 and IKKα/β to induce type I IFNs and NFkB dependent gene expression, respectively (Fig. 3.1).
TLR3
The double stranded RNA mimetics Poly I:C and Poly A:U, and derivatives thereof, have been widely tested as cancer immunotherapies in several solid tumor indications. Poly A:U was tested in the 1980–90 s wherein it was shown to extend relapse free survival after systemic delivery in breast cancer patients [44], but showed minimal efficacy in melanoma [45], and was associated with less favorable survival after systemic delivery in colorectal cancer patients [46].
The double stranded RNA mimetic, Poly I:C, effectively induces type I IFN in several tumor associated cell types and mediates generation of Th1 responses in mice [47, 48]. A poly-L-lysine stabilized version of Poly I:C in carboxymethyl-cellulose, Poly ICLC (Hiltonol), also engages MDA5 activation [49, 50] and has been tested in several trials. Poly ICLC has been delivered intramuscularly to boost systemic type I IFN responses [51, 52], as well as via intratumoral routes [53,54,55]. Poly ICLC was well tolerated in early trials, but limited efficacy as a monotherapy was reported overall. Ongoing work demonstrating potential clinical benefit focuses on combining Poly ICLC with other modalities including FLT3L, radiation, and PD-1 blockade [56]. Poly ICLC is also being used as a personalized cancer vaccine adjuvant, where sustained antitumor T cell responses were demonstrated [57].
TLR4
After the clinical use of Coley’s toxin in sarcomas, it was proposed that TLR4 activation via bacterial polysaccharides mediated that anti-sarcoma effects of Coley’s toxin in mice [58]. Lipopolysaccharide (LPS), also known as endotoxin, is the canonical bacterial polysaccharide used to activate TLR4 signaling in laboratory studies. Inducing TLR4 signaling leads to robust myeloid cell activation, particularly macrophages, and in preclinical models has been shown to induce robust antitumor effects [59,60,61]. The first clinical trial of LPS in cancer patients occurred via intravenous injection concomitant with ibuprofen to prevent inflammatory side effects, and showed induction of pro-inflammatory cytokines in the sera (TNF, IL-6 and MCSF) with moderate antitumor activity observed in 2 patients with colorectal cancer [62]. A follow-up trial of systemic LPS delivery showed only moderate antitumor efficacy [63]. Systemic toxicities associated with inflammation were a common issue for trials using LPS.
Usage of the lipid A subunit of LPS was later shown to induce antitumor activity with a more favorable toxicity profile [59, 64, 65]. Lipid A isolated from Salmonella, called monophosphoryl lipid A (MPL) was subsequently tested in cancer patients intravenously and was found to have minimal antitumor efficacy [66]. Several derivatives of MPL have been clinically tested in cancer patients with inconsistent or lacking indication of antitumor efficacy [67,68,69]. Despite limited efficacy of various MPL based strategies delivered intratumor, subcutaneous, or intravenously, MPL succeeded as an adjuvant for the HPV vaccine Cervarix® and was FDA approved for this use in 2009 [70]. Recent clinical efforts include the use of the TLR4 activating glycolipid (GSK1795091) in combination with an activating OX40 antibody, and a synthetic MPL mimetic (GLA-SE) in combination with radiation therapy [71, 72].
TLR7/8
Imiquimod is a small non-nucleoside TLR7/8 activator that originally demonstrated utility as an antiviral agent in preclinical models in the 1980s [73,74,75]. The antiviral effects observed were dependent upon mediating inflammation as opposed to direct action on viruses [74, 76,77,78,79,80,81,82]. Initial clinical trials delivering oral imiquimod in cancer patients failed to demonstrate efficacy beyond induction of inflammation [83, 84]. However, topical application of imiquimod cream for actinic keratosis [85,86,87,88,89,90,91] and basal cell carcinoma [92,93,94,95,96,97,98,99,100] was efficacious, and was FDA approved in 2004 for these indications. Several studies in various topical pre-cancerous and cancerous disease have since been conducted [67], with more recent testing occurring in breast cancer, melanoma, and other solid tumors alone or in combination with immune checkpoint blockade.
R848 (Resmiquimod) and motolimod (VTX-2337) are TLR7/8 agonists that are currently being clinically explored for cancer immunotherapy, in pre-cancerous actinic keratosis and head and neck squamous cell carcinoma, respectively [101]. Other agonists targeting TLR7 and TLR8 are currently being tested alone or in combination with immune checkpoint blockade in various solid tumors [102].
TLR9
TLR9 agonists induce potent type I IFN responses from plasmacytoid DCs (pDCs), and generally mimic unmethylated CpG DNA. Importantly, murine cell-type expression patterns of TLR9 is distinct from that of humans, with TLR9 largely being expressed in human pDCs and B cells, while murine expression of TLR9 is more ubiquitous in macrophage and DC populations [103]. Numerous clinical trials using TLR9 agonists have been conducted as monotherapy studies in solid tumors, exhibiting manageable safety profiles despite association with cytokine release syndrome related to IFN mediated inflammation [104]. Clinical efficacy signals in monotherapy trials have been limited, with more promising signals being observed when combined with other modalities [104].
Lefitolimod (MGN1703) was tested in two phase II trials in small cell lung cancer and metastatic colorectal cancer with subcutaneous delivery and did not meet survival endpoints [105, 106]. A phase III trial was conducted in a subgroup of metastatic colorectal cancer patients identified in the phase II trial, where negative results were posted.
Tilsotolimod (IMO-2125) has been tested in multiple solid tumors, most extensively in melanoma. A phase I/II trial in anti-PD-1 refractory melanoma showed evidence of efficacy of Tilsotolimod in combination with ipilimumab (anti-CTLA-4) or pembrolizumab (anti-PD-1) with an objective response rate (ORR) of 22% (News release, Idera Pharmaceuticals, April 21, 2020 press release). A follow-up phase III trial of Tilsotolimod in combination with ipilimumab in anti-PD-1 refractory melanoma was conducted but did not meet objective response rate endpoint (Idera pharmaceuticals, March 18, 2021 press release). A phase III trial in microsatellite stable colorectal cancer in combination with ipilumimab and nivolumab (anti-PD-1) is ongoing.
SD-101 has shown abscopal effects in indolent lymphoma patients after intratumor administration [107] and demonstrated an objective response rate (ORR) of 78% in treatment-naïve and 15% ORR in PD-1 refractory melanoma in combination with pembrolizumab [108]. Intratumor SD-101 in combination with pembrolizumab and paclitaxel in HER2-negative breast cancer showed non-significant improvement in pathological complete responses [109]. Several trials of SD-101 as an intratumor therapy are ongoing in combination with other modalities in melanoma, breast cancer, prostate cancer, and lymphoma.
CMP-001 is a virus like particle comprised of bacteriophage capsid with a CpG oligodeoxynucleotides. The drug is taken up by pDCs via FCgamma receptor anti-bacteriophage antibodies that bind the virus like particle leading to robust type-I IFN induction [110, 111]. In anti-PD-1 refractory melanoma patients, intratumor CMP-001 in combination with pembrolizumab achieved an ORR of 25% associated with abscopal effects noted [112, 113]. Ongoing clinical trials are testing CMP-001 in melanoma, head and neck squamous cell carcinoma, and lymphoma.
TLR9 agonists remain a very active area of clinical pursuit, particularly with newer routes of delivery, e.g., in the aforementioned case of bacteriophage-antibody mediated delivery via CMP-001; NZ-TLR, which uses a cold isostatic pressing to encapsulate a TLR9 agonist that permits extended release following intratumor injection; and AST-008, a spherical nucleic acid-based nanomaterial TLR9 agonist [104].
3.5.2.2 RLR Activation
The RLRs MDA5 and RIG-I are cytoplasmic sensors of viral RNA that have recently gained attention as potential targets for cancer immunotherapy.
MDA5
MDA5 recognizes long dsRNA in the cytosol, culminating a distinct type I IFN dominant activation of macrophages and DCs and cell death signaling in cancer cells [114,115,116]. Poly ICLC activates both TLR3 and MDA5 as mentioned in Sect. 3.5.2.1, with MDA5 activation being linked to the potent Th1 antitumor activity observed by Poly ICLC ([49, 50] (see TLR3 agonist description above for clinical status of Poly ICLC). An emerging route to target MDA5 activation is via synthetic RNA viruses and indirect reactivation of endogenous retroviruses (ERVs) using epigenetic modulators.
Synthetic positive-sense RNA viruses and replicons are commonly engineered from Semliki Forest virus, Sinbus virus, or Venezuelan equine encephalitis virus and delivers self-replicating RNA into the cytosol of cells, which can be recognized by both MDA5 and RIG-I [117]. Results from a phase I clinical trial testing a Simliki Forest virus-based HPV vaccine in HPV induced cancers efficiently induced HPV antigen-specific T cells and was well tolerated [118]. Synthetic coxsackievirus A21 RNA that engage MDA5 are currently in development for clinical use [119]. How well replicons/synthetic viral RNA engage MDA5 and other PRRs relative to oncolytic viruses/natural virus infection (see Sect. 3.5.3 below) remains unknown.
ERVs comprise up to 8% of the human genome [120] where they typically remain inactive, but have been shown to be reactivated in various cancer types [25]. Usage of demethylating agents was initially proposed to mediate antitumor effects by inducing expression of tumor suppressor genes [121]. However, several studies have shown that 5-aza-2-deoxycytidine, a DNA methylation inhibitor, causes re-expression of ERV gene products that induce dsRNA recognized by MDA5 in cancer cells, sensitizing tumor-bearing mice to anti-CTLA-4 therapy [122, 123]. Given that immunotherapy success is associated with ERV gene expression in tumors [124,125,126], it is possible that optimizing DNA demethylating agents for induction of ERV mediated MDA5 signaling will enhance immune checkpoint blockade therapy. DNA demethylating agents have been tested extensively in the clinic [127, 128], however it is unclear whether MDA5 engagement occurred and/or contributed to therapy effect.
RIG-I
In contrast to MDA5, RIG-I recognizes short dsRNA as well as 5’-ppp-RNA that lacks a 7-methylguanosine cap on the 5’ end of RNA commonly added to endogenous mRNAs. Several RIG-I agonists have been developed and are in clinical testing.
MK-4621 is a 5’-ppp synthetic RNA oligonucleotide that was delivered intratumoral in various solid tumor types where an interim analysis showed a favorable safety profile and induction of serum chemokine levels [129]. A second study testing MK-4621 complexed with JetPEI™ and pembrolizumab is also ongoing [130]. CV8102 is a single stranded, uncapped RNA complexed with cationic peptides that activates RIG-I along with TLR7/8. This drug was tested by intratumor injection in solid tumors alone or in combination with PD-1 blockade wherein the drug was well tolerated and early responses were observed [131]. GEN0101 is a drug composed of inactivated Sendai virus particles that engage RIG-I and have shown immunological responses to treatment, declines in prostate-specific antigen, and potential disease stabilization after intratumoral and subcutaneous injection in castration-resistant prostate cancer patients [132, 133]. Several other studies of GEN0101 have been conducted in melanoma and mesothelioma, however results from these trials have not been reported [134].
3.5.2.3 STING Agonists
Due to the role of endogenous STING signaling in tumors leading to spontaneous antitumor immunity [13], STING agonists have gained considerable attention as intratumoral agonists for clinical cancer immunotherapy.
DMXAA was originally developed as an anti-vascular drug that was later found to activate TBK1-IRF3 signaling [135] via STING [136]. A large phase III study was conducted in non-small cell lung cancer patients, but was discontinued [137]. Other clinical efforts with this agent have failed to show compelling clinical responses. However, despite preclinical data indicating its ability to engage antitumor CD8+ T cell immunity, it was later found to only induce mouse STING signaling, and not that of humans [138], possibly explaining its lack of clinical activity.
Other clinical trials of intratumor delivered STING agonists are ongoing and include GSK3745417, MK-2118, MK-1454, BMS-986301, IMSA-101, ADU-S100 and E7766; most of which are being combined with immune checkpoint blockade. At the time of writing, biological activity of STING agonists has been reported in patients [139, 140], but the clinical efficacy of these agents remains to be reported. Further development of modified versions of STING agonists in preclinical settings are ongoing that include the development of orally available STING agonists [141, 142], as well as higher potency STING agonists [143, 144].
3.5.3 Infectious Agents as Engagers of PRRs for Cancer Immunotherapy
In addition to BCG described above, attenuated, replication-competent viruses and bacteria being clinically developed for cancer immunotherapy also engage PRR signaling. A potential advantage of intratumoral therapy with infectious agents versus that of targeted PRR engagement with PAMPs is that infectious agents generally engage multiple PRRs within the spatiotemporal context of a natural infectious process, possibly recapitulating a more natural T cell priming scenario. However, infectious agents derived from natural animal viruses and bacterium also typically mediate some level of innate or adaptive immune interference (e.g. suppression of antiviral signaling or antigen presentation) that evolved to ensure the successful lifecycle of the pathogen [145,146,147,148]. It remains to be determined which approach (non-infectious agonists vs infectious agents) will be more effective in engaging immune surveillance and controlling tumor growth. Beyond the PRR-engaging attributes of these agents, it also must be noted that oncolytic viruses also mediate killing of cancer cells, adding an additional dimension of anticancer and immunogenic activity.
3.5.3.1 Oncolytic Viruses
While dubbed ‘oncolytic’ due to selective toxicity observed by various attenuated viruses in cancer cell lines [149], the antitumor potential of using viruses for cancer therapy may largely be due to their ability to elicit antitumor CD8+ T cells through PRR activation [114, 150,151,152]. Diverse virus species have been developed for cancer immunotherapy, ranging from large DNA viruses to small RNA viruses, that have distinct tissue tropisms, viral replication strategies, and mechanisms of immune subversion. Thus, as with targeting distinct PRRs for cancer therapy, different virus contexts are likely to mediate antitumor efficacy through different routes, with differing efficiencies. Clinically tested viral cancer immunotherapies are described below, however, numerous virus contexts beyond these agents are being considered for future clinical testing.
-
Herpes Simplex Viruses (HSV). HSV is a dsDNA viruses that engage a number of PRRs including STING, TLR2, TLR3, and TLR9 [153]. Talimogene laherparepvec (T-VEC), an attenuated oncolytic HSV1 (oHSV) expressing GMCSF, is the only FDA approved oncolytic virus to date, which demonstrated a 16.3% durable response rate and 33% 5-year response rate in a randomized phase III clinical trial of melanoma [154]. An abscopal effect was noted, with regression of non-injected lesions occurring in some patients [155]. Other monotherapy clinical trials of oHSVs have shown evidence of efficacy similar to what has been observed for T-VEC in early stage clinical trials [156]. While initial observations in combination with immune checkpoint blockade suggested promise [157], a phase III clinical trial testing T-VEC combined with pembrolizumab was recently discontinued due to futility [158].
The next generation of herpesvirus-based immunotherapies have been developed with intentions of improving oHSV immunotherapy efficacy, particularly in regards to preventing oHSV mediated disruption of antigen presentation (G47Δ [159]); enhancing oHSV toxicity selectively in cancer cells (rQNestin34.5v2 [160], RP1 [161]); enhancing IFN resistance of oHSV (ONCR-177 [162]); and ‘arming’ oHSV with PD-1 or CTLA4 blocking antibodies and immunostimulatory cytokines, particularly IL-12 (M032 [163], ONCR-177 [164], RP2 [165], MVR-T3011 [166]). Several of these agents are moving into early stage clinical trials in various solid tumor types as intratumorally delivered therapies.
-
Adenovirus. Adenovirus has a dsDNA genome and is recognized by TLR9 on pDCs[167], STING [168, 169], NOD like receptors [170, 171], with evidence for roles of other TLRs in vivo [172]. Immunogenic cell death (e.g., release of HMGB1, calreticulin, ATP, and HSP70) has also been proposed as a key mechanism driving the immunogenicity of oncolytic adenoviruses [173,174,175]. In 2005 China approved the replicating adenovirus H101 (Oncorine) for the treatment of nasopharyngeal carcinoma [176]. DNX-2401 is a modified adenovirus that selectively replicates in cancer cells with defective Retinoblastoma (Rb) and has shown promising phase I results in recurrent glioblastoma wherein 20% of patients surviving > 3 years [177]. A follow-up phase II study of DNX-2401 delivered at the time of biopsy in recurrent glioblastoma patients was conducted in combination with pembrolizumab, wherein 5/42 patients receiving the full DNX-2401 dose had confirmed responses [178]. A randomized phase III study is in planning [178]. Several ‘armed’ adenoviruses are in clinical testing in various indications; armed with GMCSF (CG0070 [179, 180] and ONCOS-102 [181]), immunostimulatory ligands CD40L and 41BBL (LOAd-703 [182]); hyaluronidase (to facilitate viral spread and CD8+ T cell recruitment within the tumor, VCN-01 [183]); IL-12 (AD5-yCD/mutTKSR39rep-hIL-12, [184]); OX40L (DNX-2440 [185]); and CXCL9, CXCL10, and IFN-α (NG-641 [186]). In addition, combination strategies of modified oncolytic adenoviruses with CAR T cell therapy (CAdVec) and chemoradiation (Colo-AD1) are being pursued [187].
-
Poxviruses. Poxviruses are large dsDNA viruses (130–300 Kb) that have sophisticated replication strategies and mechanisms to evade viral elimination by the host immune system [188]; attenuated vaccina viruses, are the most extensively tested oncolytic poxviruses. Poxviruses are recognized by several PRRs, including TLR2, TLR6, MDA5, and the NALP3 inflammasome [189, 190]. Interestingly, UV and heat inactivated Vaccina virus was shown to mediate stronger innate inflammation through STING signaling compared to replicating Vaccina, possibly reflecting strategies by which Vaccina interferes with innate signaling [191]. Pexa-Vec (JX-594), a Vaccinia virus, was tested as an intratumor therapy in hepatocellular carcinoma in a phase II clinical trial where evidence of disease control was reported [192]. However, a follow-up study revealed lack of overall survival benefit in this patient population [193]. A trial of Pexa-Vec in colorectal cancer was pursued with immune checkpoint inhibitor combination, but failed to show a significant improval in response [194]. As with other DNA viruses used for virotherapy, a current emphasis on arming poxviruses is driving ongoing clinical efforts, including with GM-CSF, chemokines, IL-15 and PD-1 blocking antibodies [195]. GL-ONC1 and vvDD are vaccina viruses that were delivered intravenously [196, 197], other studies in solid tumors are ongoing and evaluation of antitumor effects have not yet been reported. Myxoma viruses are also being developed for virotherapy in preclinical settings [195].
-
PVSRIPO. PVSRIPO, a (+)stranded RNA picornavirus, is the live attenuated type I Sabin strain of Polio with exchange of the Sabin Internal Ribosomal Entry Site (IRES) with that of human rhinovirus type II [198, 199]. This substitution neuroattenuates the virus, but does not impair its ability to kill malignant cells [198]. PVSRIPO requires poliovirus receptor (PVR) expression for viral entry, which is highly expressed on both antigen presenting cells and malignant cells [114, 198, 200]. PVSRIPO infection activates MDA5, leading to a sustained type I/III IFN dominant IFN signature in tumor-associated macrophages and dendritic cells that culminates in antitumor CD8+ T cell immunity [114, 115, 201]. Importantly, in preclinical models the antitumor efficacy of PVSRIPO was primarily dependent upon viral infection of TME constituents as opposed to malignant cells, indicating that PVSRIPO may function primarily as an engager of MDA5 within the TME [114]. A phase I clinical trial in recurrent GBM demonstrated a 21% survival rate at 36 months, relative to 4% survival in an eligibility criteria-matched historical control cohort of patients [202]. A small phase I trial in anti-PD-1 refractory melanoma demonstrated antitumor responses in both injected and non-injected lesions in 4/12 patients, with 6/12 patients resuming immune checkpoint blockade after PVSRIPO having durable disease control at 18 months of follow-up [203]. Ongoing clinical studies are focused on combining PVSRIPO with PD-1 blockade in melanoma, GBM, and other solid tumors [203,204,205].
-
Reovirus. Reoviruses are segmented dsRNA viruses with a long history of preclinical investigation backing its utility as an immunovirotherapy agent [206, 207]. Reovirus is recognized primarily by RIG-I and MDA5 [208]. The antitumor efficacy of Reovirus is independent of viral replication in preclinical models [209], implying that PRR recognition occurs upon viral entry, leading to antitumor CD8+ T cell priming [210]. Reolysin (aka pelareorep) has been delivered both intravenously and intratumorally in clinical trials. An initial phase I study observed local tumor responses in 7/19 patients, with one complete response in advanced solid tumors [211]. Phase II trials in combination with chemotherapy for malignant melanoma [212], breast cancer [213], non-small cell lung cancer [214], head and neck cancer [215], metastatic pancreatic cancer [216] have been conducted with some indication of efficacy in subsets of patients. Recent work has demonstrated that intravenously delivered Reovirus reaches brain tumors in patients and induces PD-1/PD-L1, possibly indicating its potential use as a systemic agent in combination with immune checkpoint blockade [217]. As with other oncolytic viruses, the ongoing focus of current Reovirus virotherapy is focused on combining with other immunomodulatory agents [218].
-
Coxsackievirus A21 is a (+)stranded RNA picornavirus primarily sensed by MDA5 [219], that has been clinically tested in both intravenous and intratumoral contexts as V937 (aka CAVATAK). Indications tested include non-muscle-invasive bladder cancer [220], in which tumor associated inflammation was observed, and melanoma [221], wherein 43.2% of patients had progression free survival at 1 year post treatment. Ongoing studies combining V937 and immune checkpoint blockade are being conducted in unresectable melanoma, and early results indicate the combination of V937 and pembrolizumab has a 47% ORR [222].
-
Vesicular Stomatitis Virus (VSV) is a (−) stranded RNA virus that was developed as an oncolytic virus due to the lack of type I IFN mediated suppression of attenuated VSV replication in human cancer cells [223]. VSV is recognized by RIG-I [224] and TLR7 [225]. However, VSV vectors are capable of causing neurological disease in non-human primates [226]; thus an interferon-β expressing VSV (VSV-IFNβ) was developed to restrict VSV replication beyond normal cells and was found to not cause neurotoxicity in non-human primates [227,228,229]. VSV-IFNβ was further modified with expression of a sodium iodide symporter (NIS) to enable imaging. Ongoing clinical studies in various indications include IV infusion in multiple myeloma, T cell lymphoma, and acute myeloid leukemia [230].
-
Measles Virus is a (−) stranded RNA virus that was originally proposed as an oncolytic virus candidate due to case reports of measles infection being linked to tumor regression [231]. Measles is recognized by MDA5 and RIG-I [232], however it is reported to intercept RLR recognition in antigen presenting cells [233]. Indeed natural (wildtype) measles infection also suppresses adaptive immunity [234]. The live attenuated vaccine strain of Measles (Edmonston-Zagreb strain) has been developed for cancer immunotherapy and tested in early stage clinical trials of T cell lymphoma [235], ovarian cancer [236], glioblastoma, breast cancer, head and neck squamous cell carcinoma, malignant peripheral nerve sheath tumors, bladder cancer, and multiple myeloma [237]. A NIS-expressing version of measles was also generated and tested in patients after intravenous administration [238].
-
Newcastle’s Disease Virus (NDV) is a (−) stranded RNA virus recognized primarily by RIG-I [239, 240] that naturally infects chickens. NDV has been shown to mediate both oncolysis and type I IFN-dependent priming of antitumor T cells in preclinical models [150, 241]. Several clinical trials used NDV-treated oncolysate, or lysed cancer cells, for vaccination in cancer patients [242], most of which were in melanoma where improved overall survival was demonstrated relative to historical controls. A phase III clinical trial demonstrated longer survival after NDV-pulsed autologous vaccine compared to surgical resection alone in colorectal cancer patients [243]. The MTH-68 strain of NDV was tested in various advanced cancer types in small cohorts of patients, including glioblastoma, with potential evidence of efficacy after intravenous administration [244, 245]. The PV701 strain was likewise tested intravenously in small cohorts patients with advanced cancers, documenting some objective responses [246, 247]. Extension of these studies have been complicated by changing regulatory guidelines restricting the use of NDV strains [241]. Ongoing clinical efforts to test NDV include a GMCSF expressing NDV variant (MEDI5395) being tested in various advanced cancers in combination with durvalumab (anti-PD-L1 antibody) [248].
3.5.3.2 Intracellular Bacterium
-
Bacille Calmette-Guerin (BCG) is standard of care therapy for non-muscle invasive bladder cancer, and was the first FDA approved cancer immunotherapy. See Sect. 3.5.1 for a description of the use of BCG in cancer therapy.
-
Listeria monocytogenes is a gram positive, intracellular bacterium that causes listeriosis, a foodborne illness. Listeria is recognized by TLR2, TLR5, NOD-like receptors, and STING [249]. Strains of Listeria have been developed for use as cancer vaccine vectors, with its intracellular lifecycle being an asset to deliver tumor associated antigens and engage antitumor T cell responses [250]. Listeria vaccine clinical trials have been conducted via intravenous delivery in pancreatic cancer, against mesothelin (CRS-207 [251]); in cervical cancer against HPV antigens [252, 253], and in mesothelioma against mesothelin (CRS-207 [254]). Encouraging objective responses have been observed in early stage clinical trials of mesothelioma and cervical cancer; however a phase III trial of Listeria E7 vaccine (AIM2CERV) in cervical cancer was closed by the sponsor [250], and CRS-207 development was recently discontinued after a failed lacking activity in combination with pembrolizumab [255]. Several Listeria-based approaches are in development with ongoing clinical trials.
3.6 The Role of Type I IFN in Mediating the Antitumor Efficacy of PRR Agonists
Type I IFNs are critical toward engaging DC priming of antitumor T cells [256]. Indeed, the efficacy of several PRR activators (both non-infectious agonists and infectious agents) has been shown to be dependent upon eliciting type I IFN signaling in tumors, including: Poly IC/Poly IC-LC [49, 114, 257, 258], RLR agonists [50, 259], TLR7/8 agonists [260], TLR9 agonists [261], STING agonists [262,263,264], PVSRIPO [114], and NDV [150]. IFNAR signaling both primes DC differentiation and expression of costimulatory ligands [47], while also boosting cytolytic function of antitumor CD8+ T cells locally [114, 265, 266]. However, it is critical to note that out-of-context type I IFN does not recapitulate the antitumor efficacy of broader signals delivered by type I IFN during PRR signaling [114, 267], which encompasses a myriad of other pro-inflammatory signals coinciding with type I IFN (Fig. 3.1). Indeed, while exogenous type I IFN treatment in cancer patients has shown some activity in the clinic, the efficacy of type I IFN treatment of tumors/cancer patients was limited [268]. PRR agonists, either infectious or non-infectious, offer potential to contextualize type I IFN signaling, and its T cell engaging capacity, within an inflammatory milieu supporting the production of chemokines, other DC/T cell modulating cytokines, and induction of pro-inflammatory signals within the TME that support CD8+ T cell effector functions. Whether this potential is fully realized clinically remains to be determined.
Yet, IFN signaling also mediates cancer cell chemoradiation resistance and induction of immune checkpoints that prevent antitumor T cell function [269,270,271]. Moreover, type I IFN contributes to T cell exhaustion and dysfunction during chronic viral infection [272], and type I IFN signaling in CD4+ T cells has been shown to negatively associate with immunotherapy response [273]. The context of IFN signaling may well determine whether it promotes or desensitizes antitumor immunity [274]: tumors with active IFN signaling at baseline may be resistant or non-responsive to PRR agonist therapy; and due to the role of IFNs in inducing immune checkpoint ligands [275], combination strategies to mitigate such negative feedback may be necessary to empower the antitumor effects of PRR engaging therapies. Indeed, most clinically pursued PRR engagers have been shown to induce PD-L1 and other immune checkpoint ligands, and are potentiated by immune checkpoint blockade in preclinical models [49, 114, 115, 150, 157, 267, 276].
3.7 Comparison of PRR Activators to Other Immunotherapies and Their Utility in Combination
PRR engaging immunotherapies intended to mediate in situ vaccination differ mechanistically from other anticancer modalities in several complementary ways. Complementary and distinct attributes of PRR activating immunotherapies compared to other established immunotherapy approaches are presented below:
-
Immune checkpoint blockade (ICB): Blockade of PD-L1, PD-1, CTLA4, and other immune inhibitory receptors function to resuscitate antitumor T cell function, and has achieved unprecedented clinical responses in immunogenic tumors with high mutation loads and/or oncogenic viral gene expression [277]. Generally, these modalities rely upon the presence of pre-existing antitumor T cells and are more efficacious in tumors that have higher baseline inflammation [278]. Inclusive of resistance mechanisms to ICB is that of innate immunosuppression, which limits co-stimulation, infiltration, and effector function of antitumor T cells [279]. In contrast, intratumoral therapy with PRR activators mediates innate inflammation within tumors, that enhances expression of co-stimulatory signals on antigen presenting cells, causes chemokine induction that enables trafficking of T cells to the site of the tumor, and directly bolsters the function of antitumor T cells, e.g., via type I IFNs [114, 280]. Numerous pre-clinical studies have shown that PRR activation within tumors leads to priming of antitumor T cells, which may broaden the potential of ICB therapy by bolstering antitumor T cell populations, while supporting their recruitment and function within the tumor microenvironment. Indeed, several studies have demonstrated synergy between PRR activators and ICB [281].
-
Cancer vaccines: Various cancer vaccine modalities have been developed including peptide vaccines, autologous dendritic cell vaccines, and mRNA vaccines. Indicating their clinical potential, prophylactic vaccination against HPV antigens has been remarkably successful in preventing cervical cancer [282]. Traditionally, cancer vaccines have been restricted to ‘shared’ tumor associated antigens common across numerous patients, e.g., HER2, EGFRviii, and MART1. With more recent feasibility of whole exome sequencing of biopsy tissue, personalized vaccines based upon patient-specific neoantigens are in development [57]. However, as with immune checkpoint blockade, cancer vaccines require that primed and expanded antitumor T cell populations induced by the vaccine traffic and function within the tumor. Moreover, these strategies require knowledge and accurate prediction of effectively presented, homogenously expressed, and targetable neoantigens. Notably, PRR activating adjuvants are used in cancer vaccines to enable priming and expansion of antitumor T cells in the periphery. In contrast, intratumoral delivery of PRR engaging therapies function to mediate vaccination using the tumor site in an antigen agnostic manner, by activating innate immunity and antigen presentation to prime T cells against antigens present within the tumor. Moreover, PRR agonists induce inflammation that enable trafficking and potentiation of antitumor T cell function. Intratumoral PRR agonist therapy is anticipated to complement cancer vaccines by enabling the recruitment, further tumor/tumor draining lymph node localized expansion of tumor antigen-specific T cells, and by providing inflammation in the tumor that supports antitumor T cell function.
-
Adoptive T cell transfer/CAR T cells: A direct route to bolster antitumor T cell populations in cancer patients is to deliver either expanded autologous antitumor T cells (or tumor infiltrating T cells) or autologous chimeric antigen receptor (CAR) T cells against specific tumor antigens. These approaches have shown promising antitumor efficacy in some cancer types [283, 284]. Distinct from a T cell-based approach to induce antitumor immunity in patients, intratumoral PRR activation leads to priming of T cells in the tumor bed and tumor draining lymph node while providing a supportive innate inflammatory framework for antitumor T cells to function. Intratumoral PRR activation has been shown to potentiate adoptive T cell therapy and CAR T cell therapy in pre-clinical models, primarily by enhancing recruitment of the ex-vivo expanded or engineered autologous T cells to the site of the tumor [285, 286].
3.8 The Future of PRR-Targeted Cancer Immunotherapies: Hurdles and Limitations
Beyond logistical regulatory and manufacturing issues, several hurdles remain for the success of PRR engaging immunotherapy to be realized. First, the optimal dosing of PRR engagers remains unclear, and is likely to be specific to each agent. For example, administration of higher doses of a STING agonist in mice impaired systemic antitumor immunity [287], implying that exaggerated activation of intratumor STING signaling may mediate a deleterious effect on antitumor T cell function. Whether this is true for other PRR engagers remains unknown. It also remains unclear as to which tumor types may benefit most from PRR engaging therapy: should immunologically quiescent tumors be targeted to enhanced intratumor inflammation and engage T cells? Or are immunologically active tumors more responsive to PRR-induced inflammation? As presented in this chapter, PRR agonists have been tested in both notoriously immunosuppressed tumors (e.g., glioblastoma) as well as immunogenic tumors (e.g., melanoma).
In addition, PRR-induced inflammation plays both anti- and pro-tumor roles [288]. For example, TLR3 signaling in the tumor microenvironment has been shown to enhance cancer metastases [288]; VEGF, matrix metalloproteinases, and other inflammatory features induced by PRR signaling may facilitate tumor vascularization; interferon responses induce APOBEC which can add to the evolutionary potential of cancer cells by increasing mutation rates [289]; PRR signaling promotes NFkB signaling, which can enable cancer cell survival and resistance to T cell mediated killing [290, 291]; and PRR signaling may exacerbate T cell exhaustion and dysfunction. In some respects, combination therapies like immune checkpoint blockade, anti-VEGF therapies, and other mechanisms may complement PRR engaging therapies to mitigate these effects. Overcoming and defining these limitations will be critical to optimize PRR activation for future cancer therapy.
References
Fitzgerald KA, McWhirter SM, Faia KL, Rowe DC, Latz E, Golenbock DT et al (2003) IKKepsilon and TBK1 are essential components of the IRF3 signaling pathway. Nat Immunol 4(5):491–496. https://doi.org/10.1038/ni921
Kawai T, Akira S (2007) Signaling to NF-kappaB by toll-like receptors. Trends Mol Med 13(11):460–469. https://doi.org/10.1016/j.molmed.2007.09.002
Fore F, Indriputri C, Mamutse J, Nugraha J (2020) TLR10 and Its unique anti-inflammatory properties and potential use as a target in therapeutics. Immune Netw. 20(3):e21. https://doi.org/10.4110/in.2020.20.e21
Esser-Nobis K, Hatfield LD, Gale M Jr (2020) Spatiotemporal dynamics of innate immune signaling via RIG-I-like receptors. Proc Natl Acad Sci USA 117(27):15778–15788. https://doi.org/10.1073/pnas.1921861117
Allan RS, Waithman J, Bedoui S, Jones CM, Villadangos JA, Zhan Y et al (2006) Migratory dendritic cells transfer antigen to a lymph node-resident dendritic cell population for efficient CTL priming. Immunity 25(1):153–162. https://doi.org/10.1016/j.immuni.2006.04.017
Yewdall AW, Drutman SB, Jinwala F, Bahjat KS, Bhardwaj N (2010) CD8+ T cell priming by dendritic cell vaccines requires antigen transfer to endogenous antigen presenting cells. PLoS ONE 5(6):e11144. https://doi.org/10.1371/journal.pone.0011144
Grabowska J, Lopez-Venegas MA, Affandi AJ, den Haan JMM (2018) CD169(+) macrophages capture and dendritic cells instruct: the interplay of the gatekeeper and the general of the immune system. Front Immunol 9:2472. https://doi.org/10.3389/fimmu.2018.02472
Janeway CA Jr TP, Walport M, Shlomchik MJ (2001) Immunobiology. Garland Science, New York
Dunn GP, Old LJ, Schreiber RD (2004) The three Es of cancer immunoediting. Annu Rev Immunol 22:329–360. https://doi.org/10.1146/annurev.immunol.22.012703.104803
Dagogo-Jack I, Shaw AT (2018) Tumour heterogeneity and resistance to cancer therapies. Nat Rev Clin Oncol 15(2):81–94. https://doi.org/10.1038/nrclinonc.2017.166
Chen DS, Mellman I (2013) Oncology meets immunology: the cancer-immunity cycle. Immunity 39(1):1–10. https://doi.org/10.1016/j.immuni.2013.07.012
Gallucci S, Lolkema M, Matzinger P (1999) Natural adjuvants: endogenous activators of dendritic cells. Nat Med 5(11):1249–1255. https://doi.org/10.1038/15200
Corrales L, Glickman LH, McWhirter SM, Kanne DB, Sivick KE, Katibah GE et al (2015) Direct activation of STING in the tumor microenvironment leads to potent and systemic tumor regression and immunity. Cell Rep 11(7):1018–1030. https://doi.org/10.1016/j.celrep.2015.04.031
Corrales L, McWhirter SM, Dubensky TW Jr, Gajewski TF (2016) The host STING pathway at the interface of cancer and immunity. J Clin Invest 126(7):2404–2411. https://doi.org/10.1172/JCI86892
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A et al (2007) Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med 13(9):1050–1059. https://doi.org/10.1038/nm1622
Gardai SJ, McPhillips KA, Frasch SC, Janssen WJ, Starefeldt A, Murphy-Ullrich JE et al (2005) Cell-surface calreticulin initiates clearance of viable or apoptotic cells through trans-activation of LRP on the phagocyte. Cell 123(2):321–334. https://doi.org/10.1016/j.cell.2005.08.032
Obeid M, Tesniere A, Ghiringhelli F, Fimia GM, Apetoh L, Perfettini JL et al (2007) Calreticulin exposure dictates the immunogenicity of cancer cell death. Nat Med 13(1):54–61. https://doi.org/10.1038/nm1523
Chao MP, Jaiswal S, Weissman-Tsukamoto R, Alizadeh AA, Gentles AJ, Volkmer J et al (2010) Calreticulin is the dominant pro-phagocytic signal on multiple human cancers and is counterbalanced by CD47. Sci Transl Med 2(63):63ra94. https://doi.org/10.1126/scitranslmed.3001375
Ohashi K, Burkart V, Flohe S, Kolb H (2000) Cutting edge: heat shock protein 60 is a putative endogenous ligand of the toll-like receptor-4 complex. J Immunol 164(2):558–561. https://doi.org/10.4049/jimmunol.164.2.558
Vabulas RM, Ahmad-Nejad P, da Costa C, Miethke T, Kirschning CJ, Hacker H et al (2001) Endocytosed HSP60s use toll-like receptor 2 (TLR2) and TLR4 to activate the toll/IL-1 receptor signaling pathway in innate immune cells. J Biol Chem 276(33):31332–31339. https://doi.org/10.1074/jbc.M103217200
Vabulas RM, Ahmad-Nejad P, Ghose S, Kirschning CJ, Issels RD, Wagner H (2002) HSP70 as endogenous stimulus of the toll/IL-1 receptor signal pathway. J Biol Chem 277(17):15107–15112. https://doi.org/10.1074/jbc.M111204200
Asea A, Rehli M, Kabingu E, Boch JA, Bare O, Auron PE et al (2002) Novel signal transduction pathway utilized by extracellular HSP70: role of toll-like receptor (TLR) 2 and TLR4. J Biol Chem 277(17):15028–15034. https://doi.org/10.1074/jbc.M200497200
Dybdahl B, Wahba A, Lien E, Flo TH, Waage A, Qureshi N et al (2002) Inflammatory response after open heart surgery: release of heat-shock protein 70 and signaling through toll-like receptor-4. Circulation 105(6):685–690. https://doi.org/10.1161/hc0602.103617
Roelofs MF, Boelens WC, Joosten LA, Abdollahi-Roodsaz S, Geurts J, Wunderink LU et al (2006) Identification of small heat shock protein B8 (HSP22) as a novel TLR4 ligand and potential involvement in the pathogenesis of rheumatoid arthritis. J Immunol 176(11):7021–7027. https://doi.org/10.4049/jimmunol.176.11.7021
Rooney MS, Shukla SA, Wu CJ, Getz G, Hacohen N (2015) Molecular and genetic properties of tumors associated with local immune cytolytic activity. Cell 160(1–2):48–61. https://doi.org/10.1016/j.cell.2014.12.033
Smith CC, Beckermann KE, Bortone DS, De Cubas AA, Bixby LM, Lee SJ et al (2018) Endogenous retroviral signatures predict immunotherapy response in clear cell renal cell carcinoma. J Clin Invest 128(11):4804–4820. https://doi.org/10.1172/JCI121476
Gasse P, Riteau N, Charron S, Girre S, Fick L, Petrilli V et al (2009) Uric acid is a danger signal activating NALP3 inflammasome in lung injury inflammation and fibrosis. Am J Respir Crit Care Med 179(10):903–913. https://doi.org/10.1164/rccm.200808-1274OC
Liu-Bryan R, Scott P, Sydlaske A, Rose DM, Terkeltaub R (2005) Innate immunity conferred by Toll-like receptors 2 and 4 and myeloid differentiation factor 88 expression is pivotal to monosodium urate monohydrate crystal-induced inflammation. Arthritis Rheum 52(9):2936–2946. https://doi.org/10.1002/art.21238
Kool M, Soullie T, van Nimwegen M, Willart MA, Muskens F, Jung S et al (2008) Alum adjuvant boosts adaptive immunity by inducing uric acid and activating inflammatory dendritic cells. J Exp Med 205(4):869–882. https://doi.org/10.1084/jem.20071087
Nejman D, Livyatan I, Fuks G, Gavert N, Zwang Y, Geller LT et al (2020) The human tumor microbiome is composed of tumor type-specific intracellular bacteria. Science 368(6494):973–980. https://doi.org/10.1126/science.aay9189
Dohlman AB, Arguijo Mendoza D, Ding S, Gao M, Dressman H, Iliev ID, et al (2021) The cancer microbiome atlas: a pan-cancer comparative analysis to distinguish tissue-resident microbiota from contaminants. Cell Host Microbe 29(2):281–298 e5. https://doi.org/10.1016/j.chom.2020.12.001
Zang X, Allison JP (2007) The B7 family and cancer therapy: costimulation and coinhibition. Clin Cancer Res 13(18 Pt 1):5271–5279. https://doi.org/10.1158/1078-0432.CCR-07-1030
Driessens G, Kline J, Gajewski TF (2009) Costimulatory and coinhibitory receptors in anti-tumor immunity. Immunol Rev 229(1):126–144. https://doi.org/10.1111/j.1600-065X.2009.00771.x
Hoption Cann SA, van Netten JP, van Netten C (2003) Dr William Coley and tumour regression: a place in history or in the future. Postgrad Med J 79(938):672–680
Coley WB (1910) The Treatment of Inoperable Sarcoma by Bacterial Toxins (the Mixed Toxins of the Streptococcus erysipelas and the Bacillus prodigiosus). Proc R Soc Med 3(Surg Sect):1–48
Jackson R (1974) Saint Peregrine, O.S.M.—the patron saint of cancer patients. Can Med Assoc J. 111(8):824
Hoption Cann SA, van Netten JP, van Netten C, Glover DW (2002) Spontaneous regression: a hidden treasure buried in time. Med Hypotheses 58(2):115–119. https://doi.org/10.1054/mehy.2001.1469
Meyer JP, Persad R, Gillatt DA (2002) Use of bacille Calmette-Guerin in superficial bladder cancer. Postgrad Med J 78(922):449–454. https://doi.org/10.1136/pmj.78.922.449
Peral R (1929) Cancer and tuberculosis. Am J Hyg 9:97–159
Mathe G, Amiel JL, Schwarzenberg L, Schneider M, Cattan A, Schlumberger JR et al (1969) Active immunotherapy for acute lymphoblastic leukaemia. Lancet 1(7597):697–699. https://doi.org/10.1016/s0140-6736(69)92648-8
Morales A, Eidinger D, Bruce AW (1976) Intracavitary Bacillus Calmette-Guerin in the treatment of superficial bladder tumors. J Urol 116(2):180–183. https://doi.org/10.1016/s0022-5347(17)58737-6
Lamm DL, Thor DE, Harris SC, Reyna JA, Stogdill VD, Radwin HM (1980) Bacillus Calmette-Guerin immunotherapy of superficial bladder cancer. J Urol 124(1):38–40. https://doi.org/10.1016/s0022-5347(17)55282-9
Redelman-Sidi G, Glickman MS, Bochner BH (2014) The mechanism of action of BCG therapy for bladder cancer–a current perspective. Nat Rev Urol 11(3):153–162. https://doi.org/10.1038/nrurol.2014.15
Lacour J, Lacour F, Spira A, Michelson M, Petit JY, Delage G et al (1980) Adjuvant treatment with polyadenylic-polyuridylic acid (Polya.Polyu) in operable breast cancer. Lancet 2(8187):161–4. https://doi.org/10.1016/s0140-6736(80)90057-4
Pawlicki M, Jonca M, Krzemieniecki K, Zuchowska-Vogelgesang B (1993) Results of adjuvant therapy with the preparation Poly-a Poly-u in patients with malignant melanoma during a 10-year observation. Wiad Lek 46(23–24):912–914
Lacour J, Laplanche A, Malafosse M, Gallot D, Julien M, Rotman N et al (1992) Polyadenylic-polyuridylic acid as an adjuvant in resectable colorectal carcinoma: a 6 1/2 year follow-up analysis of a multicentric double blind randomized trial. Eur J Surg Oncol 18(6):599–604
Longhi MP, Trumpfheller C, Idoyaga J, Caskey M, Matos I, Kluger C et al (2009) Dendritic cells require a systemic type I interferon response to mature and induce CD4+ Th1 immunity with poly IC as adjuvant. J Exp Med 206(7):1589–1602. https://doi.org/10.1084/jem.20090247
Trumpfheller C, Caskey M, Nchinda G, Longhi MP, Mizenina O, Huang Y et al (2008) The microbial mimic poly IC induces durable and protective CD4+ T cell immunity together with a dendritic cell targeted vaccine. Proc Natl Acad Sci U S A 105(7):2574–2579. https://doi.org/10.1073/pnas.0711976105
Sultan H, Wu J, Fesenkova VI, Fan AE, Addis D, Salazar AM, et al (2020) Poly-IC enhances the effectiveness of cancer immunotherapy by promoting T cell tumor infiltration. J Immunother Cancer 8(2). https://doi.org/10.1136/jitc-2020-001224
Sultan H, Wu J, Kumai T, Salazar AM, Celis E (2018) Role of MDA5 and interferon-I in dendritic cells for T cell expansion by anti-tumor peptide vaccines in mice. Cancer Immunol Immunother 67(7):1091–1103. https://doi.org/10.1007/s00262-018-2164-6
Salazar AM, Levy HB, Ondra S, Kende M, Scherokman B, Brown D, et al (1996) Long-term treatment of malignant gliomas with intramuscularly administered polyinosinic-polycytidylic acid stabilized with polylysine and carboxymethylcellulose: an open pilot study. Neurosurgery 38(6):1096–1103; discussion 103–104
Okada H, Butterfield LH, Hamilton RL, Hoji A, Sakaki M, Ahn BJ et al (2015) Induction of robust type-I CD8+ T-cell responses in WHO grade 2 low-grade glioma patients receiving peptide-based vaccines in combination with poly-ICLC. Clin Cancer Res 21(2):286–294. https://doi.org/10.1158/1078-0432.CCR-14-1790
Salazar AM, Erlich RB, Mark A, Bhardwaj N, Herberman RB (2014) Therapeutic in situ autovaccination against solid cancers with intratumoral poly-ICLC: case report, hypothesis, and clinical trial. Cancer Immunol Res 2(8):720–724. https://doi.org/10.1158/2326-6066.CIR-14-0024
de la Torre AN, Contractor S, Castaneda I, Cathcart CS, Razdan D, Klyde D et al (2017) A Phase I trial using local regional treatment, nonlethal irradiation, intratumoral and systemic polyinosinic-polycytidylic acid polylysine carboxymethylcellulose to treat liver cancer: in search of the abscopal effect. J Hepatocell Carcinoma 4:111–121. https://doi.org/10.2147/JHC.S136652
Kyi C, Roudko V, Sabado R, Saenger Y, Loging W, Mandeli J et al (2018) Therapeutic immune modulation against solid cancers with intratumoral poly-ICLC: a pilot trial. Clin Cancer Res 24(20):4937–4948. https://doi.org/10.1158/1078-0432.CCR-17-1866
Hammerich L, Marron TU, Upadhyay R, Svensson-Arvelund J, Dhainaut M, Hussein S et al (2019) Systemic clinical tumor regressions and potentiation of PD-1 blockade with in situ vaccination. Nat Med 25(5):814–824. https://doi.org/10.1038/s41591-019-0410-x
Hu Z, Leet DE, Allesoe RL, Oliveira G, Li S, Luoma AM et al (2021) Personal neoantigen vaccines induce persistent memory T cell responses and epitope spreading in patients with melanoma. Nat Med 27(3):515–525. https://doi.org/10.1038/s41591-020-01206-4
Shear M, Perrault A (1944) Chemical treatment of tumors. IX. Reactions of mice with primary subcutaneous tumors to injection of a hemorrhage-producing bacterial polysaccharide. J National Cancer Inst 4(5):461–476
Won EK, Zahner MC, Grant EA, Gore P, Chicoine MR (2003) Analysis of the antitumoral mechanisms of lipopolysaccharide against glioblastoma multiforme. Anticancer Drugs 14(6):457–466. https://doi.org/10.1097/00001813-200307000-00012
Chicoine MR, Won EK, Zahner MC (2001) Intratumoral injection of lipopolysaccharide causes regression of subcutaneously implanted mouse glioblastoma multiforme. Neurosurgery 48(3):607–614; discussion 14–15. https://doi.org/10.1097/00006123-200103000-00032
Berendt MJ, North RJ, Kirstein DP (1978) The immunological basis of endotoxin-induced tumor regression. Requirement for a pre-existing state of concomitant anti-tumor immunity. J Exp Med 148(6):1560–1569. https://doi.org/10.1084/jem.148.6.1560
Engelhardt R, Mackensen A, Galanos C (1991) Phase I trial of intravenously administered endotoxin (Salmonella abortus equi) in cancer patients. Cancer Res 51(10):2524–2530
Otto F, Schmid P, Mackensen A, Wehr U, Seiz A, Braun M et al (1996) Phase II trial of intravenous endotoxin in patients with colorectal and non-small cell lung cancer. Eur J Cancer 32A(10):1712–1718. https://doi.org/10.1016/0959-8049(96)00186-4
Ha DK, Leung SW, Fung KP, Choy YM, Lee CY (1985) Role of lipid A of endotoxin in the production of tumour necrosis factor. Mol Immunol 22(3):291–294. https://doi.org/10.1016/0161-5890(85)90164-6
Nowotny A, Golub S, Key B (1971) Fate and effect of endotoxin derivtives in tumor-bearing mice. Proc Soc Exp Biol Med 136(1):66–69. https://doi.org/10.3181/00379727-136-35194
Vosika GJ, Barr C, Gilbertson D (1984) Phase-I study of intravenous modified lipid A. Cancer Immunol Immunother 18(2):107–112. https://doi.org/10.1007/BF00205743
Vacchelli E, Galluzzi L, Eggermont A, Fridman WH, Galon J, Sautes-Fridman C et al (2012) Trial watch: FDA-approved Toll-like receptor agonists for cancer therapy. Oncoimmunology. 1(6):894–907. https://doi.org/10.4161/onci.20931
de Bono JS, Dalgleish AG, Carmichael J, Diffley J, Lofts FJ, Fyffe D et al (2000) Phase I study of ONO-4007, a synthetic analogue of the lipid A moiety of bacterial lipopolysaccharide. Clin Cancer Res 6(2):397–405
Isambert N, Fumoleau P, Paul C, Ferrand C, Zanetta S, Bauer J et al (2013) Phase I study of OM-174, a lipid A analogue, with assessment of immunological response, in patients with refractory solid tumors. BMC Cancer 13:172. https://doi.org/10.1186/1471-2407-13-172
Schiffman M, Wacholder S (2012) Success of HPV vaccination is now a matter of coverage. Lancet Oncol 13(1):10–12. https://doi.org/10.1016/S1470-2045(11)70324-2
Seo YD, Zhou J, Morse K, Patino J, Mackay S, Kim EY et al (2018) Effect of intratumoral (IT) injection of the toll-like receptor 4 (TLR4) agonist G100 on a clinical response and CD4 T-cell response locally and systemically. J Clin Oncol 36(5):71
Shetab Boushehri MA, Lamprecht A (2018) TLR4-based immunotherapeutics in cancer: a review of the achievements and shortcomings. Mol Pharm 15(11):4777–4800. https://doi.org/10.1021/acs.molpharmaceut.8b00691
Chen M, Griffith BP, Lucia HL, Hsiung GD (1988) Efficacy of S26308 against guinea pig cytomegalovirus infection. Antimicrob Agents Chemother 32(5):678–683. https://doi.org/10.1128/AAC.32.5.678
Harrison CJ, Jenski L, Voychehovski T, Bernstein DI (1988) Modification of immunological responses and clinical disease during topical R-837 treatment of genital HSV-2 infection. Antiviral Res 10(4–5):209–223. https://doi.org/10.1016/0166-3542(88)90032-0
Bernstein DI, Harrison CJ (1989) Effects of the immunomodulating agent R837 on acute and latent herpes simplex virus type 2 infections. Antimicrob Agents Chemother 33(9):1511–1515. https://doi.org/10.1128/AAC.33.9.1511
Harrison CJ, Stanberry LR, Bernstein DI (1991) Effects of cytokines and R-837, a cytokine inducer, on UV-irradiation augmented recurrent genital herpes in guinea pigs. Antiviral Res 15(4):315–322. https://doi.org/10.1016/0166-3542(91)90012-g
Bernstein DI, Miller RL, Harrison CJ (1993) Adjuvant effects of imiquimod on a herpes simplex virus type 2 glycoprotein vaccine in guinea pigs. J Infect Dis 167(3):731–735. https://doi.org/10.1093/infdis/167.3.731
Bernstein DI, Miller RL, Harrison CJ (1993) Effects of therapy with an immunomodulator (imiquimod, R-837) alone and with acyclovir on genital HSV-2 infection in guinea-pigs when begun after lesion development. Antiviral Res 20(1):45–55. https://doi.org/10.1016/0166-3542(93)90058-q
Reiter MJ, Testerman TL, Miller RL, Weeks CE, Tomai MA (1994) Cytokine induction in mice by the immunomodulator imiquimod. J Leukoc Biol 55(2):234–240. https://doi.org/10.1002/jlb.55.2.234
Gibson SJ, Imbertson LM, Wagner TL, Testerman TL, Reiter MJ, Miller RL et al (1995) Cellular requirements for cytokine production in response to the immunomodulators imiquimod and S-27609. J Interferon Cytokine Res 15(6):537–545. https://doi.org/10.1089/jir.1995.15.537
Megyeri K, Au WC, Rosztoczy I, Raj NB, Miller RL, Tomai MA et al (1995) Stimulation of interferon and cytokine gene expression by imiquimod and stimulation by Sendai virus utilize similar signal transduction pathways. Mol Cell Biol 15(4):2207–2218. https://doi.org/10.1128/MCB.15.4.2207
Testerman TL, Gerster JF, Imbertson LM, Reiter MJ, Miller RL, Gibson SJ et al (1995) Cytokine induction by the immunomodulators imiquimod and S-27609. J Leukoc Biol 58(3):365–372. https://doi.org/10.1002/jlb.58.3.365
Witt PL, Ritch PS, Reding D, McAuliffe TL, Westrick L, Grossberg SE et al (1993) Phase I trial of an oral immunomodulator and interferon inducer in cancer patients. Cancer Res 53(21):5176–5180
Savage P, Horton V, Moore J, Owens M, Witt P, Gore ME (1996) A phase I clinical trial of imiquimod, an oral interferon inducer, administered daily. Br J Cancer 74(9):1482–1486. https://doi.org/10.1038/bjc.1996.569
Persaud AN, Shamuelova E, Sherer D, Lou W, Singer G, Cervera C et al (2002) Clinical effect of imiquimod 5% cream in the treatment of actinic keratosis. J Am Acad Dermatol 47(4):553–556. https://doi.org/10.1067/mjd.2002.123492
Salasche SJ, Levine N, Morrison L (2002) Cycle therapy of actinic keratoses of the face and scalp with 5% topical imiquimod cream: an open-label trial. J Am Acad Dermatol 47(4):571–577. https://doi.org/10.1067/mjd.2002.126257
Harrison LI, Skinner SL, Marbury TC, Owens ML, Kurup S, McKane S et al (2004) Pharmacokinetics and safety of imiquimod 5% cream in the treatment of actinic keratoses of the face, scalp, or hands and arms. Arch Dermatol Res 296(1):6–11. https://doi.org/10.1007/s00403-004-0465-4
Lebwohl M, Dinehart S, Whiting D, Lee PK, Tawfik N, Jorizzo J et al (2004) Imiquimod 5% cream for the treatment of actinic keratosis: results from two phase III, randomized, double-blind, parallel group, vehicle-controlled trials. J Am Acad Dermatol 50(5):714–721. https://doi.org/10.1016/j.jaad.2003.12.010
Stockfleth E, Christophers E, Benninghoff B, Sterry W (2004) Low incidence of new actinic keratoses after topical 5% imiquimod cream treatment: a long-term follow-up study. Arch Dermatol 140(12):1542. https://doi.org/10.1001/archderm.140.12.1542-a
Szeimies RM, Gerritsen MJ, Gupta G, Ortonne JP, Serresi S, Bichel J et al (2004) Imiquimod 5% cream for the treatment of actinic keratosis: results from a phase III, randomized, double-blind, vehicle-controlled, clinical trial with histology. J Am Acad Dermatol 51(4):547–555. https://doi.org/10.1016/j.jaad.2004.02.022
Korman N, Moy R, Ling M, Matheson R, Smith S, McKane S et al (2005) Dosing with 5% imiquimod cream 3 times per week for the treatment of actinic keratosis: results of two phase 3, randomized, double-blind, parallel-group, vehicle-controlled trials. Arch Dermatol 141(4):467–473. https://doi.org/10.1001/archderm.141.4.467
Beutner KR, Geisse JK, Helman D, Fox TL, Ginkel A, Owens ML (1999) Therapeutic response of basal cell carcinoma to the immune response modifier imiquimod 5% cream. J Am Acad Dermatol 41(6):1002–1007. https://doi.org/10.1016/s0190-9622(99)70261-6
Marks R, Gebauer K, Shumack S, Amies M, Bryden J, Fox TL et al (2001) Imiquimod 5% cream in the treatment of superficial basal cell carcinoma: results of a multicenter 6-week dose-response trial. J Am Acad Dermatol 44(5):807–813. https://doi.org/10.1067/mjd.2001.113689
Shumack S, Robinson J, Kossard S, Golitz L, Greenway H, Schroeter A et al (2002) Efficacy of topical 5% imiquimod cream for the treatment of nodular basal cell carcinoma: comparison of dosing regimens. Arch Dermatol 138(9):1165–1171. https://doi.org/10.1001/archderm.138.9.1165
Sterry W, Ruzicka T, Herrera E, Takwale A, Bichel J, Andres K et al (2002) Imiquimod 5% cream for the treatment of superficial and nodular basal cell carcinoma: randomized studies comparing low-frequency dosing with and without occlusion. Br J Dermatol 147(6):1227–1236. https://doi.org/10.1046/j.1365-2133.2002.05069.x
Geisse J, Caro I, Lindholm J, Golitz L, Stampone P, Owens M (2004) Imiquimod 5% cream for the treatment of superficial basal cell carcinoma: results from two phase III, randomized, vehicle-controlled studies. J Am Acad Dermatol 50(5):722–733. https://doi.org/10.1016/j.jaad.2003.11.066
Huber A, Huber JD, Skinner RB Jr, Kuwahara RT, Haque R, Amonette RA (2004) Topical imiquimod treatment for nodular basal cell carcinomas: an open-label series. Dermatol Surg 30(3):429–430. https://doi.org/10.1111/j.1524-4725.2004.30116.x
Marks R, Owens M, Walters SA (2004) Australian multi-centre trial G. Efficacy and safety of 5% imiquimod cream in treating patients with multiple superficial basal cell carcinomas. Arch Dermatol 140(10):1284–1285. https://doi.org/10.1001/archderm.140.10.1284-b
Vidal D, Alomar A (2004) Efficacy of imiquimod 5% cream for basal cell carcinoma in transplant patients. Clin Exp Dermatol 29(3):237–239. https://doi.org/10.1111/j.1365-2230.2004.01456.x
Vidal D, Matias-Guiu X, Alomar A (2004) Open study of the efficacy and mechanism of action of topical imiquimod in basal cell carcinoma. Clin Exp Dermatol 29(5):518–525. https://doi.org/10.1111/j.1365-2230.2004.01601.x
Ferris RL, Saba NF, Gitlitz BJ, Haddad R, Sukari A, Neupane P et al (2018) Effect of adding motolimod to standard combination chemotherapy and cetuximab treatment of patients with squamous cell carcinoma of the head and neck: the active8 randomized clinical trial. JAMA Oncol 4(11):1583–1588. https://doi.org/10.1001/jamaoncol.2018.1888
Frega G, Wu Q, Le Naour J, Vacchelli E, Galluzzi L, Kroemer G et al (2020) Trial watch: experimental TLR7/TLR8 agonists for oncological indications. Oncoimmunology. 9(1):1796002. https://doi.org/10.1080/2162402X.2020.1796002
Rehli M (2002) Of mice and men: species variations of Toll-like receptor expression. Trends Immunol 23(8):375–378. https://doi.org/10.1016/s1471-4906(02)02259-7
Karapetyan L, Luke JJ, Davar D (2020) Toll-like receptor 9 agonists in cancer. Onco Targets Ther 13:10039–10060. https://doi.org/10.2147/OTT.S247050
Thomas M, Ponce-Aix S, Navarro A, Riera-Knorrenschild J, Schmidt M, Wiegert E et al (2018) Immunotherapeutic maintenance treatment with toll-like receptor 9 agonist lefitolimod in patients with extensive-stage small-cell lung cancer: results from the exploratory, controlled, randomized, international phase II IMPULSE study. Ann Oncol 29(10):2076–2084. https://doi.org/10.1093/annonc/mdy326
Schmoll HJ, Wittig B, Arnold D, Riera-Knorrenschild J, Nitsche D, Kroening H et al (2014) Maintenance treatment with the immunomodulator MGN1703, a Toll-like receptor 9 (TLR9) agonist, in patients with metastatic colorectal carcinoma and disease control after chemotherapy: a randomised, double-blind, placebo-controlled trial. J Cancer Res Clin Oncol 140(9):1615–1624. https://doi.org/10.1007/s00432-014-1682-7
Frank MJ, Reagan PM, Bartlett NL, Gordon LI, Friedberg JW, Czerwinski DK et al (2018) In Situ vaccination with a TLR9 agonist and local low-dose radiation induces systemic responses in untreated indolent lymphoma. Cancer Discov 8(10):1258–1269. https://doi.org/10.1158/2159-8290.CD-18-0743
Ribas A, Medina T, Kummar S, Amin A, Kalbasi A, Drabick JJ et al (2018) SD-101 in combination with pembrolizumab in advanced melanoma: results of a phase Ib. Multicenter Study. Cancer Discov. 8(10):1250–1257. https://doi.org/10.1158/2159-8290.CD-18-0280
Chien AJ, Soliman HH, Ewing CA, Boughey JC, Campbell MJ, Rugo HS et al (2021) Evaluation of intra-tumoral (IT) SD-101 and pembrolizumab (Pb) in combination with paclitaxel (P) followed by AC in high-risk HER2-negative (HER2-) stage II/III breast cancer: Results from the I-SPY 2 trial. J Clin Oncol 39(15):508. https://doi.org/10.1200/JCO.2021.39.15_suppl.508
Lemke-Miltner CD, Blackwell SE, Yin C, Krug AE, Morris AJ, Krieg AM et al (2020) Antibody opsonization of a TLR9 agonist-containing virus-like particle enhances In Situ immunization. J Immunol 204(5):1386–1394. https://doi.org/10.4049/jimmunol.1900742
Sabree SA, Voigt AP, Blackwell SE, Vishwakarma A, Chimenti MS, Salem AK, et al (2021) Direct and indirect immune effects of CMP-001, a virus-like particle containing a TLR9 agonist. J Immunother Cancer 9(6). https://doi.org/10.1136/jitc-2021-002484
Milhem M, Zakharia Y, Davar D, Buchbinder E, Medina T, Daud A et al (2020) O85 durable responses in anti-PD-1 refractory melanoma following intratumoral injection of a toll-like receptor 9 (TLR9) agonist, CMP-001, in combination with pembrolizumab. J Immunother Cancer 8(Suppl 1):A2. https://doi.org/10.1136/LBA2019.4
Ribas A, Medina T, Kirkwood JM, Zakharia Y, Gonzalez R, Davar D et al (2021) Overcoming PD-1 blockade resistance with CpG-A Toll-like receptor 9 agonist vidutolimod in patients with metastatic melanoma. Cancer Discov. https://doi.org/10.1158/2159-8290.CD-21-0425
Brown MC, Mosaheb MM, Mohme M, McKay ZP, Holl EK, Kastan JP et al (2021) Viral infection of cells within the tumor microenvironment mediates antitumor immunotherapy via selective TBK1-IRF3 signaling. Nat Commun 12(1):1858. https://doi.org/10.1038/s41467-021-22088-1
Brown MC, Holl EK, Boczkowski D, Dobrikova E, Mosaheb M, Chandramohan V, et al (2017) Cancer immunotherapy with recombinant poliovirus induces IFN-dominant activation of dendritic cells and tumor antigen-specific CTLs. Sci Transl Med 9(408). https://doi.org/10.1126/scitranslmed.aan4220
Yu X, Wang H, Li X, Guo C, Yuan F, Fisher PB et al (2016) Activation of the MDA-5-IPS-1 viral sensing pathway induces cancer cell death and Type I IFN-dependent antitumor immunity. Cancer Res 76(8):2166–2176. https://doi.org/10.1158/0008-5472.CAN-15-2142
Akhrymuk I, Frolov I, Frolova EI (2016) Both RIG-I and MDA5 detect alphavirus replication in concentration-dependent mode. Virology 487:230–241. https://doi.org/10.1016/j.virol.2015.09.023
Komdeur FL, Singh A, van de Wall S, Meulenberg JJM, Boerma A, Hoogeboom BN et al (2021) First-in-human Phase I clinical trial of an SFV-based RNA replicon cancer vaccine against HPV-induced cancers. Mol Ther 29(2):611–625. https://doi.org/10.1016/j.ymthe.2020.11.002
Edward K, Agnieszka D, Jacqueline H, Lingxin K, De Ana A, Jeffrey B et al (2021). Nature Portfolio. https://doi.org/10.21203/rs.3.rs-523458/v1
Feschotte C, Gilbert C (2012) Endogenous viruses: insights into viral evolution and impact on host biology. Nat Rev Genet 13(4):283–296. https://doi.org/10.1038/nrg3199
Navada SC, Steinmann J, Lubbert M, Silverman LR (2014) Clinical development of demethylating agents in hematology. J Clin Invest 124(1):40–46. https://doi.org/10.1172/JCI69739
Roulois D, Loo Yau H, Singhania R, Wang Y, Danesh A, Shen SY et al (2015) DNA-demethylating agents target colorectal cancer cells by inducing viral mimicry by endogenous transcripts. Cell 162(5):961–973. https://doi.org/10.1016/j.cell.2015.07.056
Chiappinelli KB, Strissel PL, Desrichard A, Li H, Henke C, Akman B et al (2015) Inhibiting DNA methylation causes an interferon response in cancer via dsRNA including endogenous retroviruses. Cell 162(5):974–986. https://doi.org/10.1016/j.cell.2015.07.011
Rycaj K, Plummer JB, Yin B, Li M, Garza J, Radvanyi L et al (2015) Cytotoxicity of human endogenous retrovirus K-specific T cells toward autologous ovarian cancer cells. Clin Cancer Res 21(2):471–483. https://doi.org/10.1158/1078-0432.CCR-14-0388
Wang-Johanning F, Rycaj K, Plummer JB, Li M, Yin B, Frerich K et al (2012) Immunotherapeutic potential of anti-human endogenous retrovirus-K envelope protein antibodies in targeting breast tumors. J Natl Cancer Inst 104(3):189–210. https://doi.org/10.1093/jnci/djr540
Krishnamurthy J, Rabinovich BA, Mi T, Switzer KC, Olivares S, Maiti SN et al (2015) Genetic engineering of T cells to target HERV-K, an ancient retrovirus on melanoma. Clin Cancer Res 21(14):3241–3251. https://doi.org/10.1158/1078-0432.CCR-14-3197
Wrangle J, Wang W, Koch A, Easwaran H, Mohammad HP, Vendetti F et al (2013) Alterations of immune response of non-small cell lung cancer with azacytidine. Oncotarget 4(11):2067–2079. https://doi.org/10.18632/oncotarget.1542
Linnekamp JF, Butter R, Spijker R, Medema JP, van Laarhoven HWM (2017) Clinical and biological effects of demethylating agents on solid tumours—a systematic review. Cancer Treat Rev 54:10–23. https://doi.org/10.1016/j.ctrv.2017.01.004
Middleton MR, Wermke M, Calvo E, Chartash E, Zhou H, Zhao X et al (2018) LBA16—Phase I/II, multicenter, open-label study of intratumoral/intralesional administration of the retinoic acid–inducible gene I (RIG-I) activator MK-4621 in patients with advanced or recurrent tumors. Ann Oncol 29:viii712. https://doi.org/10.1093/annonc/mdy424.016
Elion DL, Cook RS (2019) Activation of RIG-I signaling to increase the pro-inflammatory phenotype of a tumor. Oncotarget 10(24):2338–2339. https://doi.org/10.18632/oncotarget.26729
Eigentler T, Bauernfeind FG, Becker JC, Brossart P, Fluck M, Heinzerling L et al (2020) A phase I dose-escalation and expansion study of intratumoral CV8102 as single-agent or in combination with anti-PD-1 antibodies in patients with advanced solid tumors. J Clin Oncol 38(15_suppl):3096. https://doi.org/10.1200/JCO.2020.38.15_suppl.3096
Fujita K, Nakai Y, Kawashima A, Ujike T, Nagahara A, Nakajima T et al (2017) Phase I/II clinical trial to assess safety and efficacy of intratumoral and subcutaneous injection of HVJ-E in castration-resistant prostate cancer patients. Cancer Gene Ther 24(7):277–281. https://doi.org/10.1038/cgt.2017.15
Fujita K, Kato T, Hatano K, Kawashima A, Ujike T, Uemura M et al (2020) Intratumoral and s.c. injection of inactivated hemagglutinating virus of Japan envelope (GEN0101) in metastatic castration-resistant prostate cancer. Cancer Sci 111(5):1692–1698. https://doi.org/10.1111/cas.14366
Iurescia S, Fioretti D, Rinaldi M (2020) The innate immune signalling pathways: turning RIG-I sensor activation against cancer. Cancers (Basel) 12(11):3158. https://doi.org/10.3390/cancers12113158
Roberts ZJ, Goutagny N, Perera PY, Kato H, Kumar H, Kawai T et al (2007) The chemotherapeutic agent DMXAA potently and specifically activates the TBK1-IRF-3 signaling axis. J Exp Med 204(7):1559–1569. https://doi.org/10.1084/jem.20061845
Prantner D, Perkins DJ, Lai W, Williams MS, Sharma S, Fitzgerald KA et al (2012) 5,6-Dimethylxanthenone-4-acetic acid (DMXAA) activates stimulator of interferon gene (STING)-dependent innate immune pathways and is regulated by mitochondrial membrane potential. J Biol Chem 287(47):39776–39788. https://doi.org/10.1074/jbc.M112.382986
Le Naour J, Zitvogel L, Galluzzi L, Vacchelli E, Kroemer G (2020) Trial watch: STING agonists in cancer therapy. Oncoimmunology 9(1):1777624. https://doi.org/10.1080/2162402X.2020.1777624
Conlon J, Burdette DL, Sharma S, Bhat N, Thompson M, Jiang Z et al (2013) Mouse, but not human STING, binds and signals in response to the vascular disrupting agent 5,6-dimethylxanthenone-4-acetic acid. J Immunol 190(10):5216–5225. https://doi.org/10.4049/jimmunol.1300097
Harrington KJ, Brody J, Ingham M, Strauss J, Cemerski S, Wang M et al (2018) LBA15—preliminary results of the first-in-human (FIH) study of MK-1454, an agonist of stimulator of interferon genes (STING), as monotherapy or in combination with pembrolizumab (pembro) in patients with advanced solid tumors or lymphomas. Ann Oncol 29:viii712. https://doi.org/10.1093/annonc/mdy424.015
Meric-Bernstam F, Sandhu SK, Hamid O, Spreafico A, Kasper S, Dummer R et al (2019) Phase Ib study of MIW815 (ADU-S100) in combination with spartalizumab (PDR001) in patients (pts) with advanced/metastatic solid tumors or lymphomas. J Clin Oncol 37(15_suppl):2507. https://doi.org/10.1200/JCO.2019.37.15_suppl.2507
Chin EN, Yu C, Vartabedian VF, Jia Y, Kumar M, Gamo AM et al (2020) Antitumor activity of a systemic STING-activating non-nucleotide cGAMP mimetic. Science 369(6506):993–999. https://doi.org/10.1126/science.abb4255
Pan BS, Perera SA, Piesvaux JA, Presland JP, Schroeder GK, Cumming JN et al (2020) An orally available non-nucleotide STING agonist with antitumor activity. Science 369(6506):aba6098. https://doi.org/10.1126/science.aba6098
Ager CR, Boda A, Rajapakshe K, Lea ST, Di Francesco ME, Jayaprakash P, et al (2021) High potency STING agonists engage unique myeloid pathways to reverse pancreatic cancer immune privilege. J Immunother Cancer 9(8). https://doi.org/10.1136/jitc-2021-003246
Ager CR, Reilley MJ, Nicholas C, Bartkowiak T, Jaiswal AR, Curran MA (2017) Intratumoral STING activation with T-cell checkpoint modulation generates systemic antitumor immunity. Cancer Immunol Res 5(8):676–684. https://doi.org/10.1158/2326-6066.CIR-17-0049
Mosaheb MM, Brown MC, Dobrikova EY, Dobrikov MI, Gromeier M (2020) Harnessing virus tropism for dendritic cells for vaccine design. Curr Opin Virol 44:73–80. https://doi.org/10.1016/j.coviro.2020.07.012
Vossen MT, Westerhout EM, Soderberg-Naucler C, Wiertz EJ (2002) Viral immune evasion: a masterpiece of evolution. Immunogenetics 54(8):527–542. https://doi.org/10.1007/s00251-002-0493-1
Yewdell JW, Bennink JR (1999) Mechanisms of viral interference with MHC class I antigen processing and presentation. Annu Rev Cell Dev Biol 15:579–606. https://doi.org/10.1146/annurev.cellbio.15.1.579
Bowie AG, Unterholzner L (2008) Viral evasion and subversion of pattern-recognition receptor signalling. Nat Rev Immunol 8(12):911–922. https://doi.org/10.1038/nri2436
Parato KA, Senger D, Forsyth PA, Bell JC (2005) Recent progress in the battle between oncolytic viruses and tumours. Nat Rev Cancer 5(12):965–976. https://doi.org/10.1038/nrc1750
Zamarin D, Holmgaard RB, Subudhi SK, Park JS, Mansour M, Palese P et al (2014) Localized oncolytic virotherapy overcomes systemic tumor resistance to immune checkpoint blockade immunotherapy. Sci Transl Med 6(226):226ra32. https://doi.org/10.1126/scitranslmed.3008095
Li X, Wang P, Li H, Du X, Liu M, Huang Q et al (2017) The efficacy of oncolytic adenovirus is mediated by t-cell responses against virus and tumor in Syrian Hamster model. Clin Cancer Res 23(1):239–249. https://doi.org/10.1158/1078-0432.CCR-16-0477
Kaufman HL, Kohlhapp FJ, Zloza A (2015) Oncolytic viruses: a new class of immunotherapy drugs. Nat Rev Drug Discov 14(9):642–662. https://doi.org/10.1038/nrd4663
Paludan SR, Bowie AG, Horan KA, Fitzgerald KA (2011) Recognition of herpesviruses by the innate immune system. Nat Rev Immunol 11(2):143–154. https://doi.org/10.1038/nri2937
Andtbacka RH, Kaufman HL, Collichio F, Amatruda T, Senzer N, Chesney J et al (2015) Talimogene laherparepvec improves durable response rate in patients with advanced melanoma. J Clin Oncol 33(25):2780–2788. https://doi.org/10.1200/JCO.2014.58.3377
Andtbacka RH, Ross M, Puzanov I, Milhem M, Collichio F, Delman KA et al (2016) Patterns of clinical response with talimogene laherparepvec (T-VEC) in patients with melanoma treated in the OPTiM Phase III clinical trial. Ann Surg Oncol 23(13):4169–4177. https://doi.org/10.1245/s10434-016-5286-0
Koch MS, Lawler SE, Chiocca EA (2020) HSV-1 oncolytic viruses from bench to bedside: an overview of current clinical trials. Cancers (Basel) 12(12):3514. https://doi.org/10.3390/cancers12123514
Ribas A, Dummer R, Puzanov I, VanderWalde A, Andtbacka RHI, Michielin O, et al (2017) Oncolytic virotherapy promotes intratumoral T cell infiltration and improves anti-PD-1 immunotherapy. Cell 170(6):1109–1119 e10. https://doi.org/10.1016/j.cell.2017.08.027
Najjar YG (2021) Search for effective treatments in patients with advanced refractory melanoma continues: can novel intratumoral therapies deliver? J Immunother Cancer 9(7). https://doi.org/10.1136/jitc-2021-002820
Todo T (2019) ATIM-14. Results of phase II clinical trial of oncolytic herpes virus G47Δ in patients with glioblastoma. Neuro-Oncology 21(Supplement_6):vi4-vi. https://doi.org/10.1093/neuonc/noz175.014
Chiocca EA, Nakashima H, Kasai K, Fernandez SA, Oglesbee M (2020) Preclinical Toxicology of rQNestin34.5v.2: An Oncolytic Herpes Virus with Transcriptional Regulation of the ICP34.5 Neurovirulence Gene. Mol Ther Meth Clin Dev 17:871–893. https://doi.org/10.1016/j.omtm.2020.03.028
Thomas S, Kuncheria L, Roulstone V, Kyula JN, Mansfield D, Bommareddy PK et al (2019) Development of a new fusion-enhanced oncolytic immunotherapy platform based on herpes simplex virus type 1. J Immunother Cancer 7(1):214. https://doi.org/10.1186/s40425-019-0682-1
Kennedy EM, Farkaly T, Grzesik P, Lee J, Denslow A, Hewett J et al (2020) Design of an interferon-resistant oncolytic HSV-1 incorporating redundant safety modalities for improved tolerability. Mol Ther Oncolytics 18:476–490. https://doi.org/10.1016/j.omto.2020.08.004
Patel DM, Foreman PM, Nabors LB, Riley KO, Gillespie GY, Markert JM (2016) Design of a Phase I clinical trial to evaluate M032, a genetically engineered HSV-1 expressing IL-12, in patients with recurrent/progressive glioblastoma multiforme, anaplastic astrocytoma, or gliosarcoma. Hum Gene Ther Clin Dev 27(2):69–78. https://doi.org/10.1089/humc.2016.031
Haines BB, Denslow A, Grzesik P, Lee JS, Farkaly T, Hewett J et al (2021) ONCR-177, an oncolytic HSV-1 designed to potently activate systemic antitumor immunity. Cancer Immunol Res 9(3):291–308. https://doi.org/10.1158/2326-6066.CIR-20-0609
Harrington KJ, Aroldi F, Sacco JJ, Milhem MM, Curti BD, Vanderwalde AM et al (2021) Abstract LB180: Clinical biomarker studies with two fusion-enhanced versions of oncolytic HSV (RP1 and RP2) alone and in combination with nivolumab in cancer patients indicate potent immune activation. Cancer Res 81(13 Supplement):LB180. https://doi.org/10.1158/1538-7445.AM2021-LB180
Zheng Y, Yan R, Tang Y, Zhan B, Huang Y, Ni D et al (2021) Abstract 2597: non-clinical studies of systemic delivery of oncolytic virus arms with IL-12 and anti-PD-1 antibody. Can Res 81(13 Supplement):2597. https://doi.org/10.1158/1538-7445.AM2021-2597
Zhu J, Huang X, Yang Y (2007) Innate immune response to adenoviral vectors is mediated by both Toll-like receptor-dependent and -independent pathways. J Virol 81(7):3170–3180. https://doi.org/10.1128/JVI.02192-06
Anghelina D, Lam E, Falck-Pedersen E (2016) Diminished innate antiviral response to adenovirus vectors in cGAS/STING-deficient mice minimally impacts adaptive immunity. J Virol 90(13):5915–5927. https://doi.org/10.1128/JVI.00500-16
Wang F, Alain T, Szretter KJ, Stephenson K, Pol JG, Atherton MJ et al (2016) S6K-STING interaction regulates cytosolic DNA-mediated activation of the transcription factor IRF3. Nat Immunol 17(5):514–522. https://doi.org/10.1038/ni.3433
Suzuki M, Cela R, Bertin TK, Sule G, Cerullo V, Rodgers JR et al (2011) NOD2 signaling contributes to the innate immune response against helper-dependent adenovirus vectors independently of MyD88 in vivo. Hum Gene Ther 22(9):1071–1082. https://doi.org/10.1089/hum.2011.002
Muruve DA, Petrilli V, Zaiss AK, White LR, Clark SA, Ross PJ et al (2008) The inflammasome recognizes cytosolic microbial and host DNA and triggers an innate immune response. Nature 452(7183):103–107. https://doi.org/10.1038/nature06664
Atasheva S, Yao J, Shayakhmetov DM (2019) Innate immunity to adenovirus: lessons from mice. FEBS Lett 593(24):3461–3483. https://doi.org/10.1002/1873-3468.13696
Di Somma S, Iannuzzi CA, Passaro C, Forte IM, Iannone R, Gigantino V et al (2019) The oncolytic virus dl922-947 triggers immunogenic cell death in mesothelioma and reduces xenograft growth. Front Oncol 9:564. https://doi.org/10.3389/fonc.2019.00564
Liikanen I, Ahtiainen L, Hirvinen ML, Bramante S, Cerullo V, Nokisalmi P et al (2013) Oncolytic adenovirus with temozolomide induces autophagy and antitumor immune responses in cancer patients. Mol Ther 21(6):1212–1223. https://doi.org/10.1038/mt.2013.51
Ma J, Ramachandran M, Jin C, Quijano-Rubio C, Martikainen M, Yu D et al (2020) Characterization of virus-mediated immunogenic cancer cell death and the consequences for oncolytic virus-based immunotherapy of cancer. Cell Death Dis 11(1):48. https://doi.org/10.1038/s41419-020-2236-3
Garber K (2006) China approves world’s first oncolytic virus therapy for cancer treatment. J Natl Cancer Inst 98(5):298–300. https://doi.org/10.1093/jnci/djj111
Lang FF, Conrad C, Gomez-Manzano C, Yung WKA, Sawaya R, Weinberg JS et al (2018) Phase I study of DNX-2401 (Delta-24-RGD) oncolytic adenovirus: replication and immunotherapeutic effects in recurrent malignant glioma. J Clin Oncol 36(14):1419–1427. https://doi.org/10.1200/JCO.2017.75.8219
Zadeh G, Daras M, Cloughesy TF, Colman H, Kumthekar PU, Chen CC, et al (2020) LTBK-04. phase 2 multicenter study of the oncolytic adenovirus DNX-2401 (TASADENOTUREV) in combination with pembrolizumab for recurrent glioblastoma; captive study (KEYNOTE-192). Neuro-Oncology. 22(Supplement_2):ii237-ii. https://doi.org/10.1093/neuonc/noaa215.989
Friedlander TW, Weinberg VK, Yeung A, Burke J, Lamm DL, McKiernan JM et al (2012) Activity of intravesical CG0070 in Rb-inactive superficial bladder cancer after BCG failure: updated results of a phase I/II trial. J Clin Oncol 30(15_suppl):4593. https://doi.org/10.1200/jco.2012.30.15_suppl.4593
Packiam Vignesh T, Barocas Daniel A, Chamie K, Davis Ronald L, Karim Kader A, Lamm Donald L et al (2019) MP43–02 CG0070, an oncolytic adenovirus, for bcg-unresponsive non-muscle-invasive bladder cancer (NMIBC): 18 month follow-up from a multicenter phase II trial. J Urol 201(4):617. https://doi.org/10.1097/01.JU.0000556225.57786.36
Ranki T, Pesonen S, Hemminki A, Partanen K, Kairemo K, Alanko T et al (2016) Phase I study with ONCOS-102 for the treatment of solid tumors—an evaluation of clinical response and exploratory analyses of immune markers. J Immunother Cancer 4:17. https://doi.org/10.1186/s40425-016-0121-5
Musher BL, Smaglo BG, Abidi W, Othman M, Patel K, Jing J et al (2020) A phase I/II study combining a TMZ-CD40L/4–1BBL-armed oncolytic adenovirus and nab-paclitaxel/gemcitabine chemotherapy in advanced pancreatic cancer: an interim report. J Clin Oncol 38(4_suppl):716. https://doi.org/10.1200/JCO.2020.38.4_suppl.716
Garcia-Carbonero R, Gil Martín M, Alvarez Gallego R, Macarulla Mercade T, Riesco Martinez MC, Guillen-Ponce C et al (2019) Systemic administration of the hyaluronidase-expressing oncolytic adenovirus VCN-01 in patients with advanced or metastatic pancreatic cancer: first-in-human clinical trial. Ann Oncol 30:v271–v272. https://doi.org/10.1093/annonc/mdz247.037
Barton KN, Siddiqui F, Pompa R, Freytag SO, Khan G, Dobrosotskaya I et al (2021) Phase I trial of oncolytic adenovirus-mediated cytotoxic and IL-12 gene therapy for the treatment of metastatic pancreatic cancer. Mol Ther Oncolytics 20:94–104. https://doi.org/10.1016/j.omto.2020.11.006
Jiang H, Rivera-Molina Y, Gomez-Manzano C, Clise-Dwyer K, Bover L, Vence LM et al (2017) Oncolytic adenovirus and tumor-targeting immune modulatory therapy improve autologous cancer vaccination. Cancer Res 77(14):3894–3907. https://doi.org/10.1158/0008-5472.CAN-17-0468
Champion BR, Besneux M, Patsalidou M, Silva A, Zonca M, Marino N et al (2019) Abstract 5013: NG-641: an oncolytic T-SIGn virus targeting cancer-associated fibroblasts in the stromal microenvironment of human carcinomas. Can Res 79(13 Supplement):5013. https://doi.org/10.1158/1538-7445.AM2019-5013
Peter M, Kuhnel F (2020) Oncolytic adenovirus in cancer immunotherapy. Cancers (Basel) 12(11):3354. https://doi.org/10.3390/cancers12113354
Seet BT, Johnston JB, Brunetti CR, Barrett JW, Everett H, Cameron C et al (2003) Poxviruses and immune evasion. Annu Rev Immunol 21:377–423. https://doi.org/10.1146/annurev.immunol.21.120601.141049
Delaloye J, Roger T, Steiner-Tardivel QG, Le Roy D, Knaup Reymond M, Akira S et al (2009) Innate immune sensing of modified vaccinia virus Ankara (MVA) is mediated by TLR2-TLR6, MDA-5 and the NALP3 inflammasome. PLoS Pathog 5(6):e1000480. https://doi.org/10.1371/journal.ppat.1000480
Yang Y, Huang CT, Huang X, Pardoll DM (2004) Persistent Toll-like receptor signals are required for reversal of regulatory T cell-mediated CD8 tolerance. Nat Immunol 5(5):508–515. https://doi.org/10.1038/ni1059
Dai P, Wang W, Yang N, Serna-Tamayo C, Ricca JM, Zamarin D et al (2017) Intratumoral delivery of inactivated modified vaccinia virus Ankara (iMVA) induces systemic antitumor immunity via STING and Batf3-dependent dendritic cells. Sci Immunol. 2(11):1713. https://doi.org/10.1126/sciimmunol.aal1713
Heo J, Reid T, Ruo L, Breitbach CJ, Rose S, Bloomston M et al (2013) Randomized dose-finding clinical trial of oncolytic immunotherapeutic vaccinia JX-594 in liver cancer. Nat Med 19(3):329–336. https://doi.org/10.1038/nm.3089
Moehler M, Heo J, Lee HC, Tak WY, Chao Y, Paik SW et al (2019) Vaccinia-based oncolytic immunotherapy Pexastimogene Devacirepvec in patients with advanced hepatocellular carcinoma after sorafenib failure: a randomized multicenter Phase IIb trial (TRAVERSE). Oncoimmunology. 8(8):1615817. https://doi.org/10.1080/2162402X.2019.1615817
Monge C, Xie C, Brar G, Akoth E, Webb S, Mabry D et al (2020) A phase I/II study of JX-594 oncolytic virus in combination with immune checkpoint inhibition in refractory colorectal cancer. Eur J Cancer 138:S57–S58. https://doi.org/10.1016/S0959-8049(20)31231-4
Torres-Dominguez LE, McFadden G (2019) Poxvirus oncolytic virotherapy. Expert Opin Biol Ther 19(6):561–573. https://doi.org/10.1080/14712598.2019.1600669
Mell LK, Brumund KT, Daniels GA, Advani SJ, Zakeri K, Wright ME et al (2017) Phase I trial of intravenous oncolytic vaccinia virus (GL-ONC1) with cisplatin and radiotherapy in patients with locoregionally advanced head and neck carcinoma. Clin Cancer Res 23(19):5696–5702. https://doi.org/10.1158/1078-0432.CCR-16-3232
Downs-Canner S, Guo ZS, Ravindranathan R, Breitbach CJ, O’Malley ME, Jones HL et al (2016) Phase 1 study of intravenous oncolytic poxvirus (vvDD) in patients with advanced solid cancers. Mol Ther 24(8):1492–1501. https://doi.org/10.1038/mt.2016.101
Gromeier M, Lachmann S, Rosenfeld MR, Gutin PH, Wimmer E (2000) Intergeneric poliovirus recombinants for the treatment of malignant glioma. Proc Natl Acad Sci U S A 97(12):6803–6808
Brown MC, Dobrikova EY, Dobrikov MI, Walton RW, Gemberling SL, Nair SK et al (2014) Oncolytic polio virotherapy of cancer. Cancer 120(21):3277–3286. https://doi.org/10.1002/cncr.28862
McKay ZP, Brown MC, Gromeier M (2021) Aryl hydrocarbon receptor signaling controls CD155 expression on macrophages and mediates tumor immunosuppression. J Immunol 206(6):1385–1394. https://doi.org/10.4049/jimmunol.2000792
Mosaheb MM, Dobrikova EY, Brown MC, Yang Y, Cable J, Okada H et al (2020) Genetically stable poliovirus vectors activate dendritic cells and prime antitumor CD8 T cell immunity. Nat Commun 11(1):524. https://doi.org/10.1038/s41467-019-13939-z
Desjardins A, Gromeier M, Herndon JE 2nd, Beaubier N, Bolognesi DP, Friedman AH et al (2018) Recurrent glioblastoma treated with recombinant poliovirus. N Engl J Med 379(2):150–161. https://doi.org/10.1056/NEJMoa1716435
Beasley GM, Nair SK, Farrow NE, Landa K, Selim MA, Wiggs CA, et al (2021) Phase I trial of intratumoral PVSRIPO in patients with unresectable, treatment-refractory melanoma. J Immunother Cancer. 9(4). https://doi.org/10.1136/jitc-2020-002203
Inman BA, Balar AV, Milowsky MI, Pruthi RS, Polasek MJ, Morris SR et al (2021) Abstract CT242: LUMINOS-103: A basket trial evaluating the safety and efficacy of PVSRIPO in patients with advanced solid tumors. Cancer Res 81(13 Supplement):CT242. https://doi.org/10.1158/1538-7445.AM2021-CT242
Neighbours L, McKay ZP, Gromeier M, Nichols G, Kelly AT, Corum D et al (2021) Safety and efficacy of murine PVSRIPO plus anti-PD-1 immune checkpoint inhibitor (ICI) in a melanoma tumor model. J Clin Oncol 39(15):2560. https://doi.org/10.1200/JCO.2021.39.15_suppl.2560
Norman KL, Hirasawa K, Yang AD, Shields MA, Lee PW (2004) Reovirus oncolysis: the Ras/RalGEF/p38 pathway dictates host cell permissiveness to reovirus infection. Proc Natl Acad Sci U S A 101(30):11099–11104. https://doi.org/10.1073/pnas.0404310101
Norman KL, Lee PW (2000) Reovirus as a novel oncolytic agent. J Clin Invest 105(8):1035–1038. https://doi.org/10.1172/JCI9871
Abad AT, Danthi P (2020) Recognition of reovirus RNAs by the innate immune system. Viruses 12(6):667. https://doi.org/10.3390/v12060667
Prestwich RJ, Ilett EJ, Errington F, Diaz RM, Steele LP, Kottke T et al (2009) Immune-mediated antitumor activity of reovirus is required for therapy and is independent of direct viral oncolysis and replication. Clin Cancer Res 15(13):4374–4381. https://doi.org/10.1158/1078-0432.CCR-09-0334
Prestwich RJ, Errington F, Ilett EJ, Morgan RS, Scott KJ, Kottke T et al (2008) Tumor infection by oncolytic reovirus primes adaptive antitumor immunity. Clin Cancer Res 14(22):7358–7366. https://doi.org/10.1158/1078-0432.CCR-08-0831
Morris DG, Feng X, DiFrancesco LM, Fonseca K, Forsyth PA, Paterson AH et al (2013) REO-001: a phase I trial of percutaneous intralesional administration of reovirus type 3 dearing (Reolysin(R)) in patients with advanced solid tumors. Invest New Drugs 31(3):696–706. https://doi.org/10.1007/s10637-012-9865-z
Mahalingam D, Fountzilas C, Moseley J, Noronha N, Tran H, Chakrabarty R et al (2017) A phase II study of REOLYSIN((R)) (pelareorep) in combination with carboplatin and paclitaxel for patients with advanced malignant melanoma. Cancer Chemother Pharmacol 79(4):697–703. https://doi.org/10.1007/s00280-017-3260-6
Bernstein V, Ellard SL, Dent SF, Tu D, Mates M, Dhesy-Thind SK et al (2018) A randomized phase II study of weekly paclitaxel with or without pelareorep in patients with metastatic breast cancer: final analysis of Canadian Cancer Trials Group IND.213. Breast Cancer Res Treat 167(2):485–93. https://doi.org/10.1007/s10549-017-4538-4
Morris D, Tu D, Tehfe MA, Nicholas GA, Goffin JR, Gregg RW et al (2016) A randomized phase II study of Reolysin in patients with previously treated advanced or metatstatic non small cell lung cancer (NSCLC) receiving standard salvage chemotherapy—canadian cancer trials group IND 211. J Clin Oncol 34(15):e20512. https://doi.org/10.1200/JCO.2016.34.15_suppl.e20512
Karnad AB, Haigentz M, Miley T, Coffey M, Gill G, Mita M (2011) Abstract C22: a phase II study of intravenous wild-type reovirus (Reolysin®) in combination with paclitaxel plus carboplatin in patients with platinum refractory metastatic and/or recurrent squamous cell carcinoma of the head and neck. Mol Cancer Ther 10(11 Supplement):C22. https://doi.org/10.1158/1535-7163.TARG-11-C22
Noonan AM, Farren MR, Geyer SM, Huang Y, Tahiri S, Ahn D et al (2016) Randomized phase 2 trial of the oncolytic virus pelareorep (Reolysin) in upfront treatment of metastatic pancreatic adenocarcinoma. Mol Ther 24(6):1150–1158. https://doi.org/10.1038/mt.2016.66
Samson A, Scott KJ, Taggart D, West EJ, Wilson E, Nuovo GJ et al (2018) Intravenous delivery of oncolytic reovirus to brain tumor patients immunologically primes for subsequent checkpoint blockade. Sci Transl Med. 10(422):aam7577. https://doi.org/10.1126/scitranslmed.aam7577
Muller L, Berkeley R, Barr T, Ilett E, Errington-Mais F (2020) Past, present and future of oncolytic reovirus. Cancers (Basel) 12(11):3219. https://doi.org/10.3390/cancers12113219
Feng Q, Hato SV, Langereis MA, Zoll J, Virgen-Slane R, Peisley A et al (2012) MDA5 detects the double-stranded RNA replicative form in picornavirus-infected cells. Cell Rep 2(5):1187–1196. https://doi.org/10.1016/j.celrep.2012.10.005
Annels NE, Mansfield D, Arif M, Ballesteros-Merino C, Simpson GR, Denyer M et al (2019) Phase I trial of an ICAM-1-targeted immunotherapeutic-coxsackievirus A21 (CVA21) as an oncolytic agent against non muscle-invasive bladder cancer. Clin Cancer Res 25(19):5818. https://doi.org/10.1158/1078-0432.CCR-18-4022
Andtbacka RHI, Curti B, Daniels GA, Hallmeyer S, Whitman ED, Lutzky J, et al (2021) Clinical responses of oncolytic coxsackievirus A21 (V937) in patients with unresectable melanoma. J Clin Oncol. JCO2003246. https://doi.org/10.1200/JCO.20.03246
Silk AW, Day SJ, Kaufman HL, Bryan J, Norrell JT, Imbergamo C et al (2021) Abstract CT139: intratumoral oncolytic virus V937 in combination with pembrolizumab (pembro) in patients (pts) with advanced melanoma: Updated results from the phase 1b CAPRA study. Cancer Res 81(13 Supplement):CT139. https://doi.org/10.1158/1538-7445.AM2021-CT139
Stojdl DF, Lichty BD, tenOever BR, Paterson JM, Power AT, Knowles S et al (2003) VSV strains with defects in their ability to shutdown innate immunity are potent systemic anti-cancer agents. Cancer Cell 4(4):263–275. https://doi.org/10.1016/s1535-6108(03)00241-1
Yoneyama M, Kikuchi M, Natsukawa T, Shinobu N, Imaizumi T, Miyagishi M et al (2004) The RNA helicase RIG-I has an essential function in double-stranded RNA-induced innate antiviral responses. Nat Immunol 5(7):730–737. https://doi.org/10.1038/ni1087
Lund JM, Alexopoulou L, Sato A, Karow M, Adams NC, Gale NW et al (2004) Recognition of single-stranded RNA viruses by Toll-like receptor 7. Proc Natl Acad Sci U S A 101(15):5598–5603. https://doi.org/10.1073/pnas.0400937101
Johnson JE, Nasar F, Coleman JW, Price RE, Javadian A, Draper K et al (2007) Neurovirulence properties of recombinant vesicular stomatitis virus vectors in non-human primates. Virology 360(1):36–49. https://doi.org/10.1016/j.virol.2006.10.026
Jenks N, Myers R, Greiner SM, Thompson J, Mader EK, Greenslade A et al (2010) Safety studies on intrahepatic or intratumoral injection of oncolytic vesicular stomatitis virus expressing interferon-beta in rodents and nonhuman primates. Hum Gene Ther 21(4):451–462. https://doi.org/10.1089/hum.2009.111
Obuchi M, Fernandez M, Barber GN (2003) Development of recombinant vesicular stomatitis viruses that exploit defects in host defense to augment specific oncolytic activity. J Virol 77(16):8843–8856. https://doi.org/10.1128/jvi.77.16.8843-8856.2003
Patel MR, Jacobson BA, Ji Y, Drees J, Tang S, Xiong K et al (2015) Vesicular stomatitis virus expressing interferon-beta is oncolytic and promotes antitumor immune responses in a syngeneic murine model of non-small cell lung cancer. Oncotarget 6(32):33165–33177. https://doi.org/10.18632/oncotarget.5320
Cook J, Peng KW, Geyer SM, Ginos BF, Dueck AC, Packiriswamy N et al (2021) Clinical activity of systemic VSV-IFNβ-NIS oncolytic virotherapy in patients with relapsed refractory T-cell lymphoma. J Clin Oncol 39(15_suppl):2500. https://doi.org/10.1200/JCO.2021.39.15_suppl.2500
Bluming AZ, Ziegler JL (1971) Regression of Burkitt’s lymphoma in association with measles infection. Lancet 2(7715):105–106. https://doi.org/10.1016/s0140-6736(71)92086-1
Runge S, Sparrer KM, Lassig C, Hembach K, Baum A, Garcia-Sastre A et al (2014) In vivo ligands of MDA5 and RIG-I in measles virus-infected cells. PLoS Pathog 10(4):e1004081. https://doi.org/10.1371/journal.ppat.1004081
Mesman AW, Zijlstra-Willems EM, Kaptein TM, de Swart RL, Davis ME, Ludlow M et al (2014) Measles virus suppresses RIG-I-like receptor activation in dendritic cells via DC-SIGN-mediated inhibition of PP1 phosphatases. Cell Host Microbe 16(1):31–42. https://doi.org/10.1016/j.chom.2014.06.008
Mina MJ, Kula T, Leng Y, Li M, de Vries RD, Knip M et al (2019) Measles virus infection diminishes preexisting antibodies that offer protection from other pathogens. Science 366(6465):599–606. https://doi.org/10.1126/science.aay6485
Heinzerling L, Kunzi V, Oberholzer PA, Kundig T, Naim H, Dummer R (2005) Oncolytic measles virus in cutaneous T-cell lymphomas mounts antitumor immune responses in vivo and targets interferon-resistant tumor cells. Blood 106(7):2287–2294. https://doi.org/10.1182/blood-2004-11-4558
Galanis E, Hartmann LC, Cliby WA, Long HJ, Peethambaram PP, Barrette BA et al (2010) Phase I trial of intraperitoneal administration of an oncolytic measles virus strain engineered to express carcinoembryonic antigen for recurrent ovarian cancer. Cancer Res 70(3):875–882. https://doi.org/10.1158/0008-5472.CAN-09-2762
Engeland CE, Ungerechts G (2021) Measles virus as an oncolytic immunotherapy. Cancers (Basel). 13(3):544. https://doi.org/10.3390/cancers13030544
Galanis E, Atherton PJ, Maurer MJ, Knutson KL, Dowdy SC, Cliby WA et al (2015) Oncolytic measles virus expressing the sodium iodide symporter to treat drug-resistant ovarian cancer. Cancer Res 75(1):22–30. https://doi.org/10.1158/0008-5472.CAN-14-2533
Rehwinkel J, Tan CP, Goubau D, Schulz O, Pichlmair A, Bier K et al (2010) RIG-I detects viral genomic RNA during negative-strand RNA virus infection. Cell 140(3):397–408. https://doi.org/10.1016/j.cell.2010.01.020
Kato H, Sato S, Yoneyama M, Yamamoto M, Uematsu S, Matsui K et al (2005) Cell type-specific involvement of RIG-I in antiviral response. Immunity 23(1):19–28. https://doi.org/10.1016/j.immuni.2005.04.010
Burman B, Pesci G, Zamarin D (2020) Newcastle disease virus at the forefront of cancer immunotherapy. Cancers (Basel) 12(12):3552. https://doi.org/10.3390/cancers12123552
Schlag P, Manasterski M, Gerneth T, Hohenberger P, Dueck M, Herfarth C et al (1992) Active specific immunotherapy with Newcastle-disease-virus-modified autologous tumor cells following resection of liver metastases in colorectal cancer. First evaluation of clinical response of a phase II-trial. Cancer Immunol Immunother 35(5):325–330. https://doi.org/10.1007/BF01741145
Liang W, Wang H, Sun TM, Yao WQ, Chen LL, Jin Y et al (2003) Application of autologous tumor cell vaccine and NDV vaccine in treatment of tumors of digestive tract. World J Gastroenterol 9(3):495–498. https://doi.org/10.3748/wjg.v9.i3.495
Csatary LK, Gosztonyi G, Szeberenyi J, Fabian Z, Liszka V, Bodey B et al (2004) MTH-68/H oncolytic viral treatment in human high-grade gliomas. J Neurooncol 67(1–2):83–93. https://doi.org/10.1023/b:neon.0000021735.85511.05
Csatary LK, Moss RW, Beuth J, Torocsik B, Szeberenyi J, Bakacs T (1999) Beneficial treatment of patients with advanced cancer using a newcastle disease virus vaccine (MTH-68/H). Anticancer Res 19(1B):635–638
Pecora AL, Rizvi N, Cohen GI, Meropol NJ, Sterman D, Marshall JL et al (2002) Phase I trial of intravenous administration of PV701, an oncolytic virus, in patients with advanced solid cancers. J Clin Oncol 20(9):2251–2266. https://doi.org/10.1200/JCO.2002.08.042
Laurie SA, Bell JC, Atkins HL, Roach J, Bamat MK, O’Neil JD et al (2006) A phase 1 clinical study of intravenous administration of PV701, an oncolytic virus, using two-step desensitization. Clin Cancer Res 12(8):2555–2562. https://doi.org/10.1158/1078-0432.CCR-05-2038
Dy GK, Davar D, Galanis E, Townsley D, Karanovic D, Schwaederle M et al (2020) Abstract CT244: a phase 1 study of IV MEDI5395, an oncolytic virus, in combination with durvalumab in patients with advanced solid tumors. Cancer Res 80(16 Supplement):CT244. https://doi.org/10.1158/1538-7445.AM2020-CT244
Eitel J, Suttorp N, Opitz B (2010) Innate immune recognition and inflammasome activation in listeria monocytogenes infection. Front Microbiol 1:149. https://doi.org/10.3389/fmicb.2010.00149
Oladejo M, Paterson Y, Wood LM (2021) Clinical experience and recent advances in the development of listeria-based tumor immunotherapies. Front Immunol 12:642316. https://doi.org/10.3389/fimmu.2021.642316
Tsujikawa T, Crocenzi T, Durham JN, Sugar EA, Wu AA, Onners B et al (2020) Evaluation of cyclophosphamide/GVAX pancreas followed by listeria-mesothelin (CRS-207) with or without nivolumab in patients with pancreatic cancer. Clin Cancer Res 26(14):3578–3588. https://doi.org/10.1158/1078-0432.CCR-19-3978
Basu P, Mehta A, Jain M, Gupta S, Nagarkar RV, John S et al (2018) A randomized phase 2 study of ADXS11-001 listeria monocytogenes-listeriolysin O immunotherapy with or without cisplatin in treatment of advanced cervical cancer. Int J Gynecol Cancer 28(4):764–772. https://doi.org/10.1097/IGC.0000000000001235
Huh WK, Brady WE, Fracasso PM, Dizon DS, Powell MA, Monk BJ et al (2020) Phase II study of axalimogene filolisbac (ADXS-HPV) for platinum-refractory cervical carcinoma: an NRG oncology/gynecologic oncology group study. Gynecol Oncol 158(3):562–569. https://doi.org/10.1016/j.ygyno.2020.06.493
Hassan R, Alley E, Kindler H, Antonia S, Jahan T, Honarmand S et al (2019) Clinical response of live-attenuated, listeria monocytogenes expressing mesothelin (CRS-207) with chemotherapy in patients with malignant pleural mesothelioma. Clin Cancer Res 25(19):5787–5798. https://doi.org/10.1158/1078-0432.CCR-19-0070
Alley EW, Tanvetyanon T, Jahan TM, Gandhi L, Peikert T, Stevenson J et al (2019) A phase II single-arm study of CRS-207 with pembrolizumab (pembro) in previously treated malignant pleural mesothelioma (MPM). J Clin Oncol 37(8):29. https://doi.org/10.1200/JCO.2019.37.8_suppl.29
Diamond MS, Kinder M, Matsushita H, Mashayekhi M, Dunn GP, Archambault JM et al (2011) Type I interferon is selectively required by dendritic cells for immune rejection of tumors. J Exp Med 208(10):1989–2003. https://doi.org/10.1084/jem.20101158
Di S, Zhou M, Pan Z, Sun R, Chen M, Jiang H et al (2019) Combined adjuvant of poly I: C improves antitumor effects of CAR-T cells. Front Oncol 9:241. https://doi.org/10.3389/fonc.2019.00241
Ngoi SM, Tovey MG, Vella AT (2008) Targeting poly(I:C) to the TLR3-independent pathway boosts effector CD8 T cell differentiation through IFN-alpha/beta. J Immunol 181(11):7670–7680. https://doi.org/10.4049/jimmunol.181.11.7670
Poeck H, Besch R, Maihoefer C, Renn M, Tormo D, Morskaya SS et al (2008) 5’-Triphosphate-siRNA: turning gene silencing and Rig-I activation against melanoma. Nat Med 14(11):1256–1263. https://doi.org/10.1038/nm.1887
Inglefield JR, Dumitru CD, Alkan SS, Gibson SJ, Lipson KE, Tomai MA et al (2008) TLR7 agonist 852A inhibition of tumor cell proliferation is dependent on plasmacytoid dendritic cells and type I IFN. J Interferon Cytokine Res 28(4):253–263. https://doi.org/10.1089/jir.2007.0097
Mai J, Li Z, Xia X, Zhang J, Li J, Liu H et al (2021) Synergistic activation of antitumor immunity by a particulate therapeutic vaccine. Adv Sci (Weinh). 8(12):2100166. https://doi.org/10.1002/advs.202100166
Deng L, Liang H, Xu M, Yang X, Burnette B, Arina A et al (2014) STING-dependent cytosolic DNA sensing promotes radiation-induced type i interferon-dependent antitumor immunity in immunogenic tumors. Immunity 41(5):843–852. https://doi.org/10.1016/j.immuni.2014.10.019
Klarquist J, Hennies CM, Lehn MA, Reboulet RA, Feau S, Janssen EM (2014) STING-mediated DNA sensing promotes antitumor and autoimmune responses to dying cells. J Immunol 193(12):6124–6134. https://doi.org/10.4049/jimmunol.1401869
Sivick KE, Desbien AL, Glickman LH, Reiner GL, Corrales L, Surh NH et al (2019) Magnitude of therapeutic STING activation determines CD8(+) T cell-mediated anti-tumor immunity. Cell Rep 29(3):785–789. https://doi.org/10.1016/j.celrep.2019.09.089
Kolumam GA, Thomas S, Thompson LJ, Sprent J, Murali-Krishna K (2005) Type I interferons act directly on CD8 T cells to allow clonal expansion and memory formation in response to viral infection. J Exp Med 202(5):637–650. https://doi.org/10.1084/jem.20050821
Le Bon A, Durand V, Kamphuis E, Thompson C, Bulfone-Paus S, Rossmann C et al (2006) Direct stimulation of T cells by type I IFN enhances the CD8+ T cell response during cross-priming. J Immunol 176(8):4682–4689. https://doi.org/10.4049/jimmunol.176.8.4682
Zamarin D, Ricca JM, Sadekova S, Oseledchyk A, Yu Y, Blumenschein WM et al (2018) PD-L1 in tumor microenvironment mediates resistance to oncolytic immunotherapy. J Clin Invest 128(4):1413–1428. https://doi.org/10.1172/JCI98047
Kirkwood J (2002) Cancer immunotherapy: the interferon-alpha experience. Semin Oncol 29(3 Suppl 7):18–26. https://doi.org/10.1053/sonc.2002.33078
Benci JL, Johnson LR, Choa R, Xu Y, Qiu J, Zhou Z et al (2019) Opposing functions of interferon coordinate adaptive and innate immune responses to cancer immune checkpoint blockade. Cell 178(4):933–948. https://doi.org/10.1016/j.cell.2019.07.019
Benci JL, Xu B, Qiu Y, Wu TJ, Dada H, Twyman-Saint Victor C et al (2016) Tumor interferon signaling regulates a multigenic resistance program to immune checkpoint blockade. Cell 167(6):1540–1554. https://doi.org/10.1016/j.cell.2016.11.022
Boukhaled GM, Harding S, Brooks DG (2021) Opposing roles of type I interferons in cancer immunity. Annu Rev Pathol 16:167–198. https://doi.org/10.1146/annurev-pathol-031920-093932
Snell LM, McGaha TL, Brooks DG (2017) Type I interferon in chronic virus infection and cancer. Trends Immunol 38(8):542–557. https://doi.org/10.1016/j.it.2017.05.005
Magen A, Nie J, Ciucci T, Tamoutounour S, Zhao Y, Mehta M et al (2019) Single-Cell Profiling Defines Transcriptomic Signatures Specific to Tumor-Reactive versus Virus-Responsive CD4(+) T Cells. Cell Rep 29(10):3019–3032. https://doi.org/10.1016/j.celrep.2019.10.131
Trinchieri G (2010) Type I interferon: friend or foe? J Exp Med 207(10):2053–2063. https://doi.org/10.1084/jem.20101664
Terawaki S, Chikuma S, Shibayama S, Hayashi T, Yoshida T, Okazaki T et al (2011) IFN-alpha directly promotes programmed cell death-1 transcription and limits the duration of T cell-mediated immunity. J Immunol 186(5):2772–2779. https://doi.org/10.4049/jimmunol.1003208
Reilley MJ, Morrow B, Ager CR, Liu A, Hong DS, Curran MA (2019) TLR9 activation cooperates with T cell checkpoint blockade to regress poorly immunogenic melanoma. J Immunother Cancer 7(1):323. https://doi.org/10.1186/s40425-019-0811-x
Yarchoan M, Hopkins A, Jaffee EM (2017) Tumor mutational burden and response rate to PD-1 Inhibition. N Engl J Med 377(25):2500–2501. https://doi.org/10.1056/NEJMc1713444
Sharma P, Allison JP (2015) The future of immune checkpoint therapy. Science 348(6230):56–61. https://doi.org/10.1126/science.aaa8172
Kalbasi A, Ribas A (2020) Tumour-intrinsic resistance to immune checkpoint blockade. Nat Rev Immunol 20(1):25–39. https://doi.org/10.1038/s41577-019-0218-4
Le Bon A, Etchart N, Rossmann C, Ashton M, Hou S, Gewert D et al (2003) Cross-priming of CD8+ T cells stimulated by virus-induced type I interferon. Nat Immunol 4(10):1009–1015. https://doi.org/10.1038/ni978
Shekarian T, Valsesia-Wittmann S, Brody J, Michallet MC, Depil S, Caux C et al (2017) Pattern recognition receptors: immune targets to enhance cancer immunotherapy. Ann Oncol 28(8):1756–1766. https://doi.org/10.1093/annonc/mdx179
Lei J, Ploner A, Elfstrom KM, Wang J, Roth A, Fang F et al (2020) HPV vaccination and the risk of invasive cervical cancer. N Engl J Med 383(14):1340–1348. https://doi.org/10.1056/NEJMoa1917338
Yee C, Thompson JA, Byrd D, Riddell SR, Roche P, Celis E et al (2002) Adoptive T cell therapy using antigen-specific CD8+ T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc Natl Acad Sci U S A 99(25):16168–16173. https://doi.org/10.1073/pnas.242600099
Mullard A (2021) FDA approves fourth CAR-T cell therapy. Nat Rev Drug Discov 20(3):166. https://doi.org/10.1038/d41573-021-00031-9
Guedan S, Alemany R (2018) CAR-T cells and oncolytic viruses: joining forces to overcome the solid tumor challenge. Front Immunol 9:2460. https://doi.org/10.3389/fimmu.2018.02460
Rosewell Shaw A, Suzuki M (2018) Oncolytic viruses partner with T-Cell therapy for solid tumor treatment. Front Immunol 9:2103. https://doi.org/10.3389/fimmu.2018.02103
Sivick KE, Desbien AL, Glickman LH, Reiner GL, Corrales L, Surh NH et al (2018) Magnitude of therapeutic sting activation determines CD8(+) T cell-mediated anti-tumor immunity. Cell Rep. 25(11):3074–3085. https://doi.org/10.1016/j.celrep.2018.11.047
Huang B, Zhao J, Unkeless JC, Feng ZH, Xiong H (2008) TLR signaling by tumor and immune cells: a double-edged sword. Oncogene 27(2):218–224. https://doi.org/10.1038/sj.onc.1210904
Huff AL, Wongthida P, Kottke T, Thompson JM, Driscoll CB, Schuelke M et al (2018) APOBEC3 ssserapy. Mol Ther Oncolytics. 11:1–13. https://doi.org/10.1016/j.omto.2018.08.003
Verzella D, Pescatore A, Capece D, Vecchiotti D, Ursini MV, Franzoso G et al (2020) Life, death, and autophagy in cancer: NF-kappaB turns up everywhere. Cell Death Dis 11(3):210. https://doi.org/10.1038/s41419-020-2399-y
Luo JL, Kamata H, Karin M (2005) IKK/NF-kappaB signaling: balancing life and death–a new approach to cancer therapy. J Clin Invest 115(10):2625–2632. https://doi.org/10.1172/JCI26322
Competing Interests
M.C.B. is an inventor on intellectual property licensed to, and a paid advisor of, Istari Oncology, which is developing a recombinant poliovirus, PVSRIPO, for cancer immunotherapy.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Brown, M. (2022). Engaging Pattern Recognition Receptors in Solid Tumors to Generate Systemic Antitumor Immunity. In: Hays, P. (eds) Cancer Immunotherapies. Cancer Treatment and Research, vol 183. Springer, Cham. https://doi.org/10.1007/978-3-030-96376-7_3
Download citation
DOI: https://doi.org/10.1007/978-3-030-96376-7_3
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-96375-0
Online ISBN: 978-3-030-96376-7
eBook Packages: MedicineMedicine (R0)