Abstract
Oral and Maxillofacial surgery (OMS) covers a wide variety of procedures such as dentoalveolar surgeries like extractions and dental implants, treatments for temporomandibular joint dysfunctions (TMD), and reconstruction of facial defects from trauma and craniofacial anomalies. This chapter will explore the biological components of platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) and provide a literature review of the current data available. PRP and PRF are being used in many areas of oral surgery and implantology including socket preservation, bone augmentation, sinus lifts, implant osteointegration, soft tissue healing, and post-extraction bone healing. While concrete evidence of actual osteointegration improvement with PRP/PRF is lacking, they are minimally invasive, have essentially no risk to the patient, and can be inexpensive to produce. This chapter will explore its use in dentoalveolar (specifically extractions, ridge augmentation, and dental implants), in reconstruction (cleft/craniofacial, bone and soft tissue defects), as well as in pathology (medication-related osteonecrosis of the jaw) and TMJ disorders. Like much of dental research, without large-scale clinical trials, the data to fully support its use in everyday practice is limited.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Oral and Maxillofacial surgery (OMS) covers a wide variety of procedures, from dentoalveolar surgeries such as extractions and dental implants, to soft tissue reconstruction, to orthognathic jaw surgery. The American Association of Oral and Maxillofacial Surgeons tries to explain the scope to dental students by dividing into six categories, dentoalveolar surgery, infections, pathology, trauma, orthognathic surgery, cleft/craniofacial reconstruction, TMJ, and facial cosmetics. The field, thus, has long searched for methods to aid in post-surgical healing, remodeling, and regeneration.
When teeth are extracted, bone remodeling is essential to the recovery process. Third molar extraction is a common procedure in Oral and Maxillofacial surgery. Approximately ten million wisdom teeth are extracted from five million patients every year in the United States [1]. Similarly, dental implants are a part of daily practice and often the ideal treatment for replacing missing teeth. Brânemark et al. first described the use of the modern-day implant in North America in 1982 [2]. With technological advancements, such as cone beam computed tomography (CBCT) and intra-oral scanning, practitioners can plan the treatment of more advance cases and have improved clinical outcomes. More complex cases often require technically demanding hard and/or soft tissue augmentation. As the need for bone augmentation increases, the dental literature has become flooded with numerous techniques and materials. One, of recent excitement, is the use of platelet-rich plasma and platelet-rich fibrin. Marx first described the use of platelet-rich plasma (PRP) and platelet-rich fibrin (PRF) in the dental field in 1998 where he reported positive healing of the alveolar bone with its use [3]. Platelet-rich plasma/fibrin has since gained substantial popularity in the dental and medical community.
PRP is a concentration of platelet and plasma proteins derived from whole blood that is placed in a centrifuge to remove the red blood cells. PRP production involves the use of anticoagulants. PRF, however, is made without the use of anticoagulants, and the blood is immediately placed into the centrifuge after phlebotomy. This allows the coagulation cascade to occur causing a PRF matrix to be formed in the test tube that traps cytokines and other growth factors (see Chap. 3, PRP Preparation). PRP is believed to work via the degranulation of the alpha granules in platelets which contain several growth factors [4]. PRP contains a variety of growth factors/cytokines such as transforming growth factor beta (TGF-beta), platelet-derived growth factor (PDGF), insulin-like growth factor (IGF), and epidermal growth factor (EGF). While both PRP and PRF contain many of the same growth factors, much research is being invested into the quantity. Given the matrix formed in PRF, it is believed that the growth factors are released slowly over time as compared to PRP, but some of the amount of these cytokines may be lost in the process. A study preformed observed the growth factors released from PRP and PRF over a period. The highest produced growth factors were PDGF-AA, PDGF-BB, TGFB1, VEGF, and PDGF-AB. PRP was demonstrated to provide the highest growth factor in the short term. Over a 10-day period, however, they noted that PRF released the highest amounts of total growth factor [5].
It is well known that PDGF/IGF-1, when added to bone defects and implants, promotes osteoblasts and osteointegration [6]. Although numerous studies have demonstrated statistical significance from a biological basis, none to our knowledge have formulated a concrete clinical difference [7, 8]. A systematic review was conducted to determine the efficacy of PRP for non-transfusion use in the fields of dentistry, orthopedics, and wound care. The authors retrieved a total of 1240 references and found statistically significant results regarding the use of PRP in treatment of intra-bony defects as well as bone augmentation for implant placement. However, the authors in this study noted a high risk of bias in the individual studies due to lack of randomization and blinding [9].
Platelet-rich products are being utilized and studied in each of the disciplines of OMS. This chapter will explore its use in dentoalveolar (specifically extractions, ridge augmentation, and dental implants), in reconstruction (cleft/craniofacial, bone and soft tissue defects), as well as in pathology (medication-related osteonecrosis of the jaw) and TMJ disorders. Its use in facial cosmetics will be explored in other chapters of this book (see Chap. 5, Hair Restoration, and Chap. 6, Facial Rejuvenation).
Dentoalveolar
Extraction Sockets
PRP and PRF have been hypothesized to aid in bone healing after extraction sockets. Since extraction of third molars is so common, they are useful models for investigating this theory. Mandibular third molar extractions specifically are generally more painful and have more postoperative complications than maxillary third molars. PRF has long thought to provide benefit in regard to reducing the incidents of alveolar osteitis, pain, trismus, and swelling following extraction of third molars. The reason for this is due to the enhanced healing by the growth factors. In 2017 a study was published in the Journal of Oral and Maxillofacial Surgery in which they conducted a systematic review and meta-analysis to determine the efficacy of platelet-rich fibrin after third molar extractions [10]. They concluded that limited evidence exists and there is a need for standardized randomized controlled trials to truly determine the efficacy of PRF. The meta-analysis only found six papers published in this topic with all of them from outside of the United States. There has been a huge push for the use of platelet-rich fibrin in all aspects of medicine with dentistry included.
A Cochrane review was published in 2020 that included 62 trials and 4643 participants to explore surgical techniques of mandibular third molar extractions. The authors found “lacing platelet-rich plasma (PRP) or platelet-rich fibrin (PRF) in sockets may reduce the incidence of alveolar osteitis (OR 0.39, 95% CI 0.22–0.67; 2 studies) [11].” Zhu et al. published a meta-analysis in 2021 that included 42 studies, stating that PRF significantly reduced the incidence of both alveolar osteitis and postoperative pain [12]. Malhotra et al. preformed a study exploring bone regeneration in extraction sockets of third molars and found that faster bone formation in the PRF sockets compared to the control [13]. The data is still imperfect in regard to clear benefit; it appears biologically plausible that platelet-rich products are beneficial in the wound healing process of third molar extractions.
Implant Osteointegration
A systematic review conducted in 2014 determined the 10-year survival rate of dental implants is approximately 94.6% [14]. As clinicians, it is hard to ask for better odds, yet as dentistry advances, patients are expecting a guarantee. Current research is looking at how to shorten the integration time and time to prosthesis. PRP and PRF can possibly serve a role in this purpose.
A split mouth randomized clinical trial was conducted involving PRF and implants in the posterior maxilla. Implant stability was determined using resonance frequency analysis at 2, 4, and 6 weeks after placement. The authors found statistically significant increased ISQ at the 6-week period with implants placed using PRF [15]. The study is limited in that it only includes 20 patients. While the statistically significant result does not necessarily correlate to meaning clinically significant, it does demonstrate that biologically, PRF is having some sort of measurable effect. Another study performed using 72 dental implants in 9 beagles attempted to analyze the bone remodeling using PRP and PRF. After 3-month follow-up, the authors concluded that there was no increase in primary or secondary implant stability, but they did see a biological improvement in the peri-implant bone volume and structural integration [16].
In a randomized, single-blinded, controlled clinical trial, involving placing 41 immediate implants, half received PRF at the peri-implant region and half did not; the authors found no increased implant stability when using radiofrequency analysis [17]. Although clinical effects have yet to be established, a biological effect is being consistently observed. In one in vitro study in which roughened titanium dental implants were treated with PRP, the authors found that the number of cells observed around the implant at day 5 was double that of the non-PRP coated [18]. In another study where titanium implants were placed in the femurs of rats using PRF, the authors found that the PRF caused an osseoinductive response as compared to the control [19].
Keratinized Soft Tissue
The utilization of PRF has been associated with better epithelialization and improved soft tissue healing. The growth factors that constitute PRP and PRF promote fibroblasts and other healing mechanisms. With this information it is logical that PRP and PRF cause a better soft tissue response after surgical procedure. Many studies have demonstrated both a faster remodeling and an increased thickness in keratinized mucosa when using PRP or PRF. A randomized, split-mouth design was conducted for eight patients who needed bilateral widening of keratinized mucosa around dental implants in the mandible. On one side of the mouth, a free gingival graft was placed, while on the other, a PRF membrane was placed. The mean amount of keratinized mucosa at the implant at the PRF-only site was 3.3 mm ± 0.9 and 3.8 mm ± 1.0 at the free gingival graft site [20]. The use of PRF membranes may provide an alternative to restoring the keratinized gingiva around implants. PRF membranes are a great alternative, being less invasive, do not require a donor site, and have less postoperative pain.
On a study involving 126 immediately placed dental implants and the use of PRP, the authors found a statistically significant soft tissue healing score as compared to the control at 3 and 7 days. The study does note no difference found at 5-year follow-up, however [21]. In the exploration of soft tissue healing, many studies also found decrease pain and swelling associated with PRP and PRF at the surgical procedure. While both of these tend to be difficult to measure and are relatively subjective, any benefit could be an added bonus for the patient. As experienced providers know, keratinized gingiva is very important at dental implant sites and difficult to get back if lost. Maintaining as much keratinized gingiva as possible is very valuable when placing dental implants.
Sinus Lifts
The maxillary bone tends to resorb in the apical and palatal direction. In the posterior maxilla, the lack of vertical bone height may prevent implant placement. When minimal vertical bone height exists between the crest of the edentulous ridge and the maxillary sinus, the provider may need to perform a sinus lift [22].
Internal sinus lifts can be performed when there is already at least 5 mm of bone between the ridge and the maxillary sinus. There must be adequate bone height below the sinus for the implant to be stable when it is inserted in the alveolar bone. This approach is executed by making the osteotomy just short of the sinus floor. Hand osteotomes can then be used to “up-fracture” the remaining cortical bone at the sinus floor, and graft material can be packed at the osteotomy site [23, 24]. Minimizing the extent of the elevation decreases the risk of creating a hole in the sinus floor and perforating the sinus membrane. Some proponents have argued just packing a PRF pellet at osteotomy site and pushing it to the base of the sinus membrane before putting in the implant [25]. The PRF pellet might potentially be a good alternative to packing bone particulate graft material or conjunction.
An external sinus lift is performed using a window that is created in the lateral sinus wall after reflecting an extensive mucoperiosteal flap often involving releasing incisions. After flap elevation, the sinus may be visible through the lateral wall showing a transparent/blue appearance. A rectangular- or oval-shaped window is created with a large round diamond bur or now more commonly with an ultrasonic piezotome using great care to prevent perforating the underlying sinus membrane [26]. Utilization of a Dentium Advanced Sinus Kit or other sinus membrane kits can also aid in forming the osteo-window without sinus communication. Bone graft material is placed into the new space created between the apical aspect of the edentulous ridge and the sinus. The provider should wait 5–6 months after sinus augmentation and then 3 months after implant placement prior to prosthetic treatment. If the sinus elevation is not extensive, and enough bone height already exists to achieve primary stability, the implant can be placed at the time of the sinus augmentation. Some have advocated the use of PRF membranes either along the sinus membrane or along the osteotomy window defect (Fig. 8.1).
A recent study looked at the use of Unilab Surgibone with and without PRP on bone healing of the sinus floor. They measured histologic and residency frequency analysis for implant stability. Bone biopsies were conducted at time of implant placement on average 7 months following the sinus augmentation. Out of the ten patients, they found no statistically significant effect in either measure [27]. A Cochrane systematic review in 2010 found no statistical efficacy for its use in dental implant sinus lifts but did note limited data existed [28].
Ridge Augmentation
Bone quality is an important factor in successful osteointegration. Lekohlm and Zarb classify bone quality into four categories depending on the ratio of compact bone and spongy bone as well as the subjective bone resistance when drilling [29] (Table 8.1).
Bone grafting procedures are utilized to augment the region generally when insufficient bone exists at a potential implant site. Sometimes bone grafting is used when there is sufficient bone to stabilize an implant but not enough to cover all the implants surfaces [30, 31]. Guided bone regeneration (GBR) generally consists of utilizing bone particulate substances. Bone augmentation can be done months prior to implant placement to facilitate future implant placement. The primary purpose of these procedures is to provide a scaffold and maintain volume for new bone formation.
Allografts are biomaterials generally composed of cadaver bone. An important difference from autogenous bone is the loss of endogenous cells and growth factors resulting from processing and sterilizing the allograft, thereby reducing or eliminating osteoinductive capacity. Consequently, the allograft will serve as an effective osteoconductive scaffold for new bone regeneration [32]. PRP is believed to act as a reservoir for stem cells and therefore provide that osteoinductive capacity that is found in autologous grafts (see Fig. 8.2). A xenograft is a graft that is obtained from another species. The xenografts used in alveolar bone regeneration are osteoconductive bone graft substitute made of inorganic components but derived from non-human sources. The use of bone graft substitutes eliminates the need for harvesting of autogenous bone or harvesting a smaller volume of autogenous bone while providing structure and slow resorption characteristics that stabilize and “protect” the autogenous component of the bone graft. In addition, the use of bone graft substitutes eliminates donor site morbidity. To take best advantage of these characteristics, clinicians often mix and/or layer autogenous bone and biomaterial bone graft substitute components [33]. It is expected that implants can be placed into previously placed block or particulate bone grafts 5–6 months post graft placement; however, there is older data that shows implant stability may be more predictable when placed 6–9 months following bone grafting [34,35,36,37]. When particulate grafting occurs simultaneous with implant placement, the implant will often begin prosthetic treatment approximately 3–4 months after implant placement [38].
It has been demonstrated that PRF gradually releases autologous growth factors and is more effective for the proliferation of differentiation of osteoblasts than PRP in vivo [39]. PRF can act as a resorbable membrane for guided bone regeneration in that it prevents the emigration of non-desirable cells into the bone defect as well as provide a source of healing by promoting cytokines [40]. Therefore, the use of PRF can be used as a membrane itself or in conjunction with other membranes. An additional use of PRF with bone particulate is the fabrication of “sticky bone” which is PRF and allograft. The fibrin acts as a glue to hold the particulate together and can be molded into the desired morphology (see Fig. 8.3). The protocol for preparation of sticky bone is described in Chap. 8, PRP Cases.
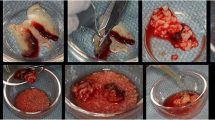
Creation of sticky bone using PRF and bony particulate. Venipuncture is preformed to obtain 10 ccs of blood and placed in the centrifuge at 2500 rpms for 3.5 min. The top plasma/fibrin layer is removed with an empty syringe which is approximately 1 cc. Generally, you can expect to obtain 1 cc of autologous fibrin glue for each 10 cc test tube of venous blood. Mix the autologous fibrin glue immediately with bone particles on a metal dish. Mold the bone into the desired thickness with a periosteal elevator. Leave the coated bone undisturbed on the metal dish for 5–10 min. The bone particulate will form “sticky bone” (PRF + allograft)
Reconstruction
Clefts
In a similar fashion to ridge augmentation, PRP is being investigated for benefit in alveolar cleft bone grafting. Sakio et al. reported on a study 29 patients with unilateral alveolar clefts, with 6 in the control, and 23 in the PRP group. All patients underwent iliac cancellous bone grafts. The authors [41] found no significant difference in mean resorption of the bone on follow-up imaging, suggesting that PRP does not decrease bone resorption following the procedure. A similar study was preformed 3 years later by Chen and colleges. They aimed to analyze the newly formed bone volume 6 months after secondary alveoloplasty using iliac cancellous bone graft, with and without platelet-rich plasma in 40 patients, this time with 20 patients in each group. The authors found no statistical difference in bone formation on postoperative bone volume [42]. The current literature, therefore, does not show benefit with PRP in terms of bone volume. It would be helpful if other studies explored any soft tissue benefit when using PRP or if the alveolar cleft that was grafted with PRP has increased dental implant survival long term.
Large Bone Defects
In addition to being used in small maxillary and mandibular ridge augmentations, PRP is being used in large bone defects in conjunction with other reconstruction techniques. Custom cribs of titanium mesh are being fabricated to help facilitate bone growth in maxillary and mandibular reconstruction. Marx et al. have described this in detail using both bone particular (CCFDAB) and bone harvested from anterior iliac crests along with rhBMP-2 to stimulate bone formation [43]. In addition to the rhBMP-2, Marx et al. incorporate PRP. Marx and colleagues define the “tissue engineering triangle” as a source of cells, a signal, and a matrix. The recombinant human bone morphogenic protein-2 (rhBMP-2) is a chemoattractant providing the stem cells, crushed cancellous freeze-dried allogenic bone (CCFDAB) provides the osteoconductive matrix, and the PRP provides the signal through its growth factors [43]. PRF membranes have also been used to lay over the titanium mesh to aid in soft tissue closure. PRF can also be used after the mesh is removed, laying over the newly formed bone.
Pathology
The growth factors of PRP have thought to be beneficial in cases of osteonecrosis of the jaws (ONJ). Osteoradionecrosis of the jaws (ORNJ) and medication-related osteonecrosis of the jaws (MRONJ) are a growing problem. In 2016 a paper was published that reviewed the current literature regarding PRP and both preventing and treating ONJ. The study found several papers that used PRP as a prevention strategy, placing PRP in dental extraction sockets of high-risk patients and, as treatment, placing PRP after debridement of established osteonecrosis cases. The study stated there was inconclusive evidence to show benefit and randomized controlled trials were needed [44]. Some clinicals have reported PRP use after laser therapy in treating patients with MRONJ [45]. In 2018, a study was performed in rats which showed local application of autologous PRP was a viable therapy in preventing the occurrence of MRONJ following tooth extractions [46]. A systematic review in 2019 showed PRP as an adjuvant to surgical debridement can produce significant benefit in treatment of MRONJ, with one study finding 80.2% of patients completely healed [47].
TMJ
The use of PRP in temporomandibular joint disorders that are associated with chronic pain is gaining popularity as a treatment modality, especially as treating TMD can often be difficult [48]. A randomized controlled trial found injection of PRP in comparison to hyaluronic acid demonstrated more pain reduction [49]. A study was performed to determine the effects of PRP injections in cases of TMJ arthritis in domestic pigs. The authors found a “A significant reduction in signs of histological inflammation, such as hyperplasia of the synovial membrane, leucocyte infiltration, cartilage surface alterations, and an increase in cartilage-specific glycosaminoglycan content, was observed [50].”
Conclusion
Oral and Maxillofacial surgery covers a wide plethora of procedures, but dentoalveolar surgery is the most numerous in daily practice and therefore is likely why most available data on PRP and PRF pertains to extractions and dental implants. PRP/PRF has potential to help with postoperative healing after extractions as well as improve bone and soft tissue formation for future dental implant site development. Investigations are starting to be done for use in TMJ disorders and bone reconstruction. PRP/PRF may also prove beneficial for some of the other procedures in the field, including soft tissue defects and flap reconstruction. As the reader can appreciate, the literature on this topic is lacking and therefore unable to provide definitive guidelines for its use. The safety and low cost of PRP/PRF along with the biological plausibility make it still a valuable treatment modality for practitioners. Over the next decade, the authors of this chapter expect to see a robust wave of literature of randomized controlled trials that will hopefully help develop meaningful clinical indications.
For now, the PRP/PRF literature appears centered around dental implant surgery. Dental implant osteointegration is already arbitrarily very successful. Implant success rate is estimated around 95% [14]. Most dental implant research focuses on how to improve success in less than ideal situations (i.e., inadequate bone height, uncontrolled diabetics). PRP and PRF may just be an additional tool in the dentists’ arsenal to aid in these circumstances. While concrete evidence of actual osteointegration improvement with PRP/PRF is lacking, evidence does exist in terms of soft tissue healing and is likely to be a big area of future research. Soft tissue involving implants has been a long-studied area given the belief that it is directly related to the longevity of the implant’s success. While the PRP/PRF may have clinical effects to primary or secondary stability, its use in promoting soft tissue healing cannot be ignored. PRP/PRF are minimally invasive, have essentially no risk to the patient, and can be inexpensive to produce. While some still believe there used to be use a better word here, the risk/benefit analysis with the current data supports its use in specific instances. Like much of dental research, without large-scale clinical trials, the data to fully support its use in everyday practice is limited.
References
Normando D. Third molars: to extract or not to extract? Dental Press J Orthod. 2015;20(4):17–8.
Branemark P, Zarb G, Albrektsson T. Tissue-integrated prostheses: ossesointegration in clinical dentistry. Chicago, IL: Quintessence Publishing; 1985.
Marx RE, Carlson ER, Eichstaedt RM, Schimmele SR, Strauss JE, Georgeff KR. Platelet-rich plasma: growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;85(6):638–46.
Scully D, Naseem KM, Matsakas A. Platelet biology in regenerative medicine of skeletal muscle. Acta Physiol (Oxf). 2018;223(3):e13071.
Kobayashi E, Fluckiger L, Fujioka-Kobayashi M, Sawada K, Sculean A, Schaller B, Miron RJ. Comparative release of growth factors from PRP, PRF, and advanced-PRF. Clin Oral Investig. 2016;20(9):2353–60.
Ortolani E, Guerriero M, Coli A, Di Giannuario A, Minniti G, Polimeni A. Effect of PDGF, IGF-1 and PRP on the implant osseointegration. An histological and immunohistochemical study in rabbits. Ann Stomatol (Roma). 2014;5(2):66–8.
Strauss FJ, Stahli A, Gruber R. The use of platelet-rich fibrin to enhance the outcomes of implant therapy: a systematic review. Clin Oral Implants Res. 2018;29(Suppl 18):6–19.
Stahli A, Strauss FJ, Gruber R. The use of platelet-rich plasma to enhance the outcomes of implant therapy: a systematic review. Clin Oral Implants Res. 2018;29(Suppl 18):20–36.
Pachito DV, de Oliveira Cruz Latorraca C, Riera R. Efficacy of Platelet-Rich Plasma for non-transfusion use: overview of systematic reviews. Int J Clin Pract. 2019;73:e13402.
Al-Hamed FS, Tawfik MA, Abdelfadil E, Al-Saleh MAQ. Efficacy of platelet-rich fibrin after mandibular third molar extraction: a systematic review and meta-analysis. J Oral Maxillofac Surg. 2017;75(6):1124–35.
Bailey E, Kashbour W, Shah N, Worthington HV, Renton TF, Coulthard P. Surgical techniques for the removal of mandibular wisdom teeth. Cochrane Database Syst Rev. 2020;7(7):Cd004345.
Zhu J, Zhang S, Yuan X, He T, Liu H, Wang J, Xu B. Effect of platelet-rich fibrin on the control of alveolar osteitis, pain, trismus, soft tissue healing, and swelling following mandibular third molar surgery: an updated systematic review and meta-analysis. Int J Oral Maxillofac Surg. 2021;50(3):398–406.
Malhotra A, Kapur I, Das D, Sharma A, Gupta M, Kumar M. Comparative evaluation of bone regeneration with platelet-rich fibrin in mandibular third molar extraction socket: a randomized split-mouth study. Natl J Maxillofac Surg. 2020;11(2):241–7.
Moraschini V, Poubel LA, Ferreira VF, Barboza E. Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years: a systematic review. Int J Oral Maxillofac Surg. 2015;44(3):377–88.
Tabrizi R, Arabion H, Karagah T. Does platelet-rich fibrin increase the stability of implants in the posterior of the maxilla? A split-mouth randomized clinical trial. Int J Oral Maxillofac Surg. 2018;47(5):672–5.
Huang Y, Li Z, Van Dessel J, Salmon B, Huang B, Lambrichts I, Politis C, Jacobs R. Effect of platelet-rich plasma on peri-implant trabecular bone volume and architecture: a preclinical micro-CT study in beagle dogs. Clin Oral Implants Res. 2019;30(12):1190–9.
Diana C, Mohanty S, Chaudhary Z, Kumari S, Dabas J, Bodh R. Does platelet-rich fibrin have a role in osseointegration of immediate implants? A randomized, single-blind, controlled clinical trial. Int J Oral Maxillofac Surg. 2018;47(9):1178–88.
Lee JH, Nam J, Nam KW, Kim HJ, Yoo JJ. Pre-treatment of titanium alloy with platelet-rich plasma enhances human osteoblast responses. Tissue Eng Regen Med. 2016;13(4):335–42.
Yosif AM, Al-Hijazi A. Evaluation of the effect of Autolougues Platelet Rich Fibrin Matrix on osseointegration of the titanium implant immunohistochemical evaluation for PDGF-I&IGF-A. J Baghdad Coll Dent. 2013;25(1):70.
Temmerman A, Cleeren GJ, Castro AB, Teughels W, Quirynen M. L-PRF for increasing the width of keratinized mucosa around implants: a split-mouth, randomized, controlled pilot clinical trial. J Periodontal Res. 2018;53(5):793–800.
Taschieri S, Lolato A, Ofer M, Testori T, Francetti L, Del Fabbro M. Immediate post-extraction implants with or without pure platelet-rich plasma: a 5-year follow-up study. Oral Maxillofac Surg. 2017;21(2):147–57.
Kent JN, Block MS. Simultaneous maxillary sinus floor bone grafting and placement of hydroxylapatite-coated implants. J Oral Maxillofac Surg. 1989;47(3):238–42.
Schleier P, Bierfreund G, Schultze-Mosgau S, Moldenhauer F, Küpper H, Freilich M. Simultaneous dental implant placement and endoscope-guided internal sinus floor elevation: 2-year post-loading outcomes. Clin Oral Implants Res. 2008;19(11):1163–70.
Summer R. A new concept in maxillary implant surgery; the osteome technique. Compend Contin Educ Dent. 1994;2:152–62.
Aoki N, Kanayama T, Maeda M, Horii K, Miyamoto H, Wada K, Ojima Y, Tsuchimochi T, Shibuya Y. Sinus augmentation by platelet-rich fibrin alone: a report of two cases with histological examinations. Case Rep Dent. 2016;2016:2654645.
Lin YH, Yang YC, Wen SC, Wang HL. The influence of sinus membrane thickness upon membrane perforation during lateral window sinus augmentation. Clin Oral Implants Res. 2016;27(5):612–7.
Cabbar F, Guler N, Kurkcu M, Iseri U, Sencift K. The effect of bovine bone graft with or without platelet-rich plasma on maxillary sinus floor augmentation. J Oral Maxillofac Surg. 2011;69(10):2537–47.
Esposito M, Grusovin MG, Rees J, Karasoulos D, Felice P, Alissa R, Worthington H, Coulthard P. Effectiveness of sinus lift procedures for dental implant rehabilitation: a Cochrane systematic review. Eur J Oral Implantol. 2010;3(1):7–26.
Lekohlm U, Zarb G. Patient selection. Quintessence Publishing; 1985.
Benic GI, Bernasconi M, Jung RE, Hämmerle CH. Clinical and radiographic intra-subject comparison of implants placed with or without guided bone regeneration: 15-year results. J Clin Periodontol. 2017;44(3):315–25.
Benic GI, Hämmerle CH. Horizontal bone augmentation by means of guided bone regeneration. Periodontol 2000. 2014;66(1):13–40.
Sheikh Z, Hamdan N, Ikeda Y, Grynpas M, Ganss B, Glogauer M. Natural graft tissues and synthetic biomaterials for periodontal and alveolar bone reconstructive applications: a review. Biomater Res. 2017;21:9.
Wang HL, Misch C, Neiva RF. “Sandwich” bone augmentation technique: rationale and report of pilot cases. Int J Periodontics Restorative Dent. 2004;24(3):232–45.
Triplett RG, Schow SR. Autologous bone grafts and endosseous implants: complementary techniques. J Oral Maxillofac Surg. 1996;54(4):486–94.
Anitua E, Murias-Freijo A, Alkhraisat MH. Implant site under-preparation to compensate the remodeling of an autologous bone block graft. J Craniofac Surg. 2015;26(5):e374–7.
Levin L, Schwartz-Arad D, Nitzan D. Smoking as a risk factor for dental implants and implant-related surgery. Refuat Hapeh Vehashinayim (1993). 2005;22(2):37–43, 85.
Levin L, Nitzan D, Schwartz-Arad D. Success of dental implants placed in intraoral block bone grafts. J Periodontol. 2007;78(1):18–21.
Freilich M, Shafer D, Halepas S. Chapter 21: Dental implants. In: Ferneini E, Goupil M, editors. Evidence-based oral surgery. Springer Nature; 2019.
He L, Lin Y, Hu X, Zhang Y, Wu H. A comparative study of platelet-rich fibrin (PRF) and platelet-rich plasma (PRP) on the effect of proliferation and differentiation of rat osteoblasts in vitro. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(5):707–13.
Borie E, Oliví DG, Orsi IA, Garlet K, Weber B, Beltrán V, Fuentes R. Platelet-rich fibrin application in dentistry: a literature review. Int J Clin Exp Med. 2015;8(5):7922–9.
Sakio R, Sakamoto Y, Ogata H, Sakamoto T, Ishii T, Kishi K. Effect of platelet-rich plasma on bone grafting of alveolar clefts. J Craniofac Surg. 2017;28(2):486–8.
Chen S, Liu B, Yin N, Wang Y, Li H. Assessment of bone formation after secondary alveolar bone grafting with and without platelet-rich plasma using computer-aided engineering techniques. J Craniofac Surg. 2020;31(2):549–52.
Marx RE, Armentano L, Olavarria A, Samaniego J. rhBMP-2/ACS grafts versus autogenous cancellous marrow grafts in large vertical defects of the maxilla: an unsponsored randomized open-label clinical trial. Int J Oral Maxillofac Implants. 2013;28(5):e243–51.
Lopez-Jornet P, Sanchez Perez A, Amaral Mendes R, Tobias A. Medication-related osteonecrosis of the jaw: is autologous platelet concentrate application effective for prevention and treatment? A systematic review. J Craniomaxillofac Surg. 2016;44(8):1067–72.
Fornaini C, Cella L, Oppici A, Parlatore A, Clini F, Fontana M, Lagori G, Merigo E. Laser and platelet-rich plasma to treat medication-related osteonecrosis of the jaws (MRONJ): a case report. Laser Ther. 2017;26(3):223–7.
Toro LF, de Mello-Neto JM, Santos F, Ferreira LC, Statkievicz C, Cintra L, Issa JPM, Dornelles RCM, de Almeida JM, Nagata MJH, Garcia VG, Theodoro LH, Casatti CA, Ervolino E. Application of autologous platelet-rich plasma on tooth extraction site prevents occurence of medication-related osteonecrosis of the jaws in rats. Sci Rep. 2019;9(1):22.
de Souza Tolentino E, de Castro TF, Michellon FC, Passoni ACC, Ortega LJA, Iwaki LCV, da Silva MC. Adjuvant therapies in the management of medication-related osteonecrosis of the jaws: systematic review. Head Neck. 2019;41(12):4209–28.
Anitua E, Fernández-de-Retana S, Alkhraisat MH. Platelet rich plasma in oral and maxillofacial surgery from the perspective of composition. Platelets. 2021;32(2):174–82.
Fernández-Ferro M, Fernández-Sanromán J, Blanco-Carrión A, Costas-López A, López-Betancourt A, Arenaz-Bua J, Stavaru Marinescu B. Comparison of intra-articular injection of plasma rich in growth factors versus hyaluronic acid following arthroscopy in the treatment of temporomandibular dysfunction: a randomised prospective study. J Cranio-Maxillofac Surg. 2017;45(4):449–54.
Naujokat H, Sengebusch A, Loger K, Möller B, Açil Y, Wiltfang J. Therapy of antigen-induced arthritis of the temporomandibular joint via platelet-rich plasma injections in domestic pigs. J Craniomaxillofac Surg. 2021;49(8):726–31.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Halepas, S., Chen, X.J., Koch, A. (2022). PRP in Oral and Maxillofacial Surgery and Dental Implants. In: Ferneini, E.M., Landesberg, R., Halepas, S. (eds) Platelet Rich Plasma in Medicine. Springer, Cham. https://doi.org/10.1007/978-3-030-94269-4_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-94269-4_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-94268-7
Online ISBN: 978-3-030-94269-4
eBook Packages: MedicineMedicine (R0)